Plant Extracts as Skin Care and Therapeutic Agents
Abstract
:1. Introduction
2. Plants as Photoprotective Agents against Ultraviolet-Radiation-Induced Inflammation and Skin Damage
3. Plants as Regenerative and Wound-Healing Agents
4. Plants as Anti-Aging Agents
5. Plants as Anti-Tyrosinase Agents
6. Plants as Aromatic Agents
7. Plants as Colorants and Dye Agents
| Chemical Class | Example of Class | Source | Color Produced | |
|---|---|---|---|---|
| Quinones | benzoquinone | 1,4-benzoquinone | Pyrus lindleyi | brown |
| anthraquinones | alizarin | Rubia tinctiorum | red | |
| napthoqinones | lawsone (2-hydroxy-1,4-naphthoquinone) | Lawsonia inermis | brown, purple grey and shades of orange | |
| juglone (5-hydroxy-1,4-naphthoquinon) | Juglans regia | |||
| Polyphenols | flavones | luteolin | Reseda luteola | yellow and brown |
| apigenin | Chamomilla recutita | |||
| chrysin | Passiflora incarnata | |||
| anthocyanins | protocyanins | Centaurea cyanus | red, violet or blue (depending on pH) | |
| malvidin, peonidin, delphinidin | Althaea rosea | |||
| 3-delphinidin sambubioside (hibiscin), 3-cyanidin sambubioside, 3-delphinidin glucoside | Hibiscus sabdariffa | |||
| 3-cyanidin glucoside (chrysanthemum), 3-cyanidin sambubioside | Sambucus nigra fructus | |||
| Betalains | betacyanins | betanin | Beta vulgaris Amaranthus cruentus Opuntia ficus-indica | red and purple |
| betaxanthins | vulgaxanthin I and II, indicaxanthin | Hylocereus polyrhizus, Opuntia ficus-indica, Beta vulgaris | yellow and orange | |
| Carotenoids | carotenes | α-, β-, γ-carotene, lycopene | Daucus carota, Solanum lycopersicum, Sorbus aucuparia | orange, red and yellow |
| xanthophylls | lutein, zeaxanthin, violaxanthin | Spinacia oleracea, Zea mays, Tagetes erecta |
8. Future Perspectives and Challenges
9. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Michalak, M.; Pierzak, M.; Kręcisz, B.; Suliga, E. Bioactive Compounds for Skin Health: A Review. Nutrients 2021, 13, 203. [Google Scholar] [CrossRef] [PubMed]
- Michalak, M. Plant-Derived Antioxidants: Significance in Skin Health and the Ageing Process. Int. J. Mol. Sci. 2022, 23, 585. [Google Scholar] [CrossRef] [PubMed]
- Menaa, F. Skin anti-aging benefits of phytoterapeutics-based emulsions. Pharm. Anal. Acta 2014, 5, 168. [Google Scholar] [CrossRef]
- Jadoon, S.; Karim, S.; Bin Asad, M.H.; Akram, M.R.; Khan, A.K.; Malik, A.; Chen, C.; Murtaza, G. Anti-Aging Potential of Phytoextract Loaded-Pharmaceutical Creams for Human Skin Cell Longetivity. Oxid. Med. Cell Longev. 2015, 2015, 709628. [Google Scholar] [CrossRef]
- Clydesdale, G.J.; Dandie, G.W.; Muller, H.K. Ultraviolet light induced injury: Immunological and inflammatory effects. Immunol. Cell Biol. 2001, 79, 547–568. [Google Scholar] [CrossRef]
- Brink, N.; Szamel, M.; Young, A.R.; Wittern, K.P.; Bergemann, J. Comparative quantification of IL-1beta, IL-10, IL-10r, TNF-alpha and IL-7 mRNA levels in UV-irradiated human skin in vivo. Inflamm. Res. 2000, 49, 290–296. [Google Scholar] [CrossRef]
- Rundhaug, J.E.; Fischer, S.M. Cyclo-oxygenase-2 plays a critical role in UV-induced skin carcinogenesis. Photochem. Photobiol. 2008, 84, 322–329. [Google Scholar] [CrossRef]
- Muller-Decker, K. Cyclooxygenase-dependent signaling is causally linked to non-melanoma skin carcinogenesis: Pharmacological, genetic, and clinical evidence. Cancer Metastasis Rev. 2011, 30, 343–361. [Google Scholar] [CrossRef]
- de Gruijl, F.R.; van Kranen, H.J.; Mullenders, L.H. UV-induced DNA damage, repair, mutations and oncogenic pathways in skin cancer. J. Photochem. Photobiol. B 2001, 63, 19–27. [Google Scholar] [CrossRef]
- He, Y.-Y.; Huang, J.-L.; Chignell, C.F. Delayed and Sustained Activation of Extracellular Signal-regulated Kinase in Human Keratinocytes by UVA: Implications in carcinogenesis. J. Biol. Chem. 2004, 279, 53867–53874. [Google Scholar] [CrossRef]
- Muthusamy, V.; Piva, T.J. The UV response of the skin: A review of the MAPK, NFκB and TNF signal transduction pathways. Arch. Dermatol. Res. 2010, 302, 5–17. [Google Scholar] [CrossRef]
- Meng, X.; Qiu, L.; Song, H.; Dang, N. MAPK pathway involved in epidermal terminal differentiation of normal human epidermal keratinocytes. Open Med. 2018, 13, 189–195. [Google Scholar]
- Chouinard, N.; Valerie, K.; Rouabhia, M.; Huot, J. UVB-mediated activation of p38 mitogen-activated protein kinase enhances resistance of normal human keratinocytes to apoptosis by stabilizing cytoplasmic p53. Biochem. J. 2002, 365, 133–145. [Google Scholar] [CrossRef]
- Lee, C.H.; Wu, S.B.; Hong, C.H.; Yu, H.S.; Wei, Y.H. Molecular mechanisms of UV-induced apoptosis and its effects on skin residential cells: The implication in UV-based phototherapy. Int. J. Mol. Sci. 2013, 14, 6414–6643. [Google Scholar] [PubMed]
- Solano, F. Photoprotection and Skin Pigmentation: Melanin-Related Molecules and Some Other New Agents Obtained from Natural Sources. Molecules 2020, 25, 1537. [Google Scholar] [CrossRef] [PubMed]
- Skarupova, D.; Vostalova, J.; Rajnochova Svobodova, A. Ultraviolet A protective potential of plant extracts and phytochemicals. Biomed. Pap. Med. Fac. Univ. Palacký Olomouc Czechoslov. 2020, 164, 1–22. [Google Scholar] [CrossRef]
- Torres-Contreras, A.M.; Garcia-Baeza, A.; Vidal-Limon, H.R.; Balderas-Renteria, I.; Ramírez-Cabrera, M.A.; Ramirez-Estrada, K. Plant Secondary Metabolites against Skin Photodamage: Mexican Plants, a Potential Source of UV-Radiation Protectant Molecules. Plants 2022, 11, 220. [Google Scholar] [CrossRef]
- Park, K.; Choi, H.S.; Hong, Y.H.; Jung, E.Y.; Suh, H.J. Cactus cladodes (Opuntia humifusa) extract minimizes the effects of UV irradiation on keratinocytes and hairless mice. Pharm. Biol. 2017, 55, 1032–1040. [Google Scholar] [CrossRef]
- Tobi, S.E.; Gilbert, M.; Paul, N.; McMillan, T.J. The green tea polyphenol, epi gallocatechin-3-gallate, protects against the oxidative cellular and genotoxic damage of UVA radiation. Int. J. Cancer. 2002, 102, 439–444. [Google Scholar] [CrossRef]
- Afaq, F.; Zaid, M.A.; Khan, N.; Dreher, M.; Mukhtar, H. Protective effect of pomegranate-derived products on UVB-mediated damage in human reconstituted skin. Exp. Dermatol. 2009, 18, 553–561. [Google Scholar] [CrossRef]
- Napagoda, M.T.; Malkanthi, B.M.A.S.; Abayawardana, S.A.K.; Qader, M.M.; Jayasinghe, L. Photoprotective potential in some medicinal plants used to treat skin diseases in Sri Lanka. BMC Complement. Altern. Med. 2016, 16, 479. [Google Scholar] [CrossRef] [PubMed]
- Svobodová, A.; Zdařilová, A.; Walterová, D.; Vostálová, J. Flavonolignans from Silybum marianum moderate UVA-induced oxidative damage to HaCaT keratinocytes. J. Dermatol. Sci. 2007, 48, 213–224. [Google Scholar] [CrossRef] [PubMed]
- Alonso-Lebrero, J.L.; Domínguez-Jiménez, C.; Tejedor, R.; Brieva, A.; Pivel, J.P. Photoprotective properties of a hydrophilic extract of the fern Polypodium leucotomos on human skin cells. J. Photochem. Photobiol. B 2003, 70, 31–37. [Google Scholar] [CrossRef]
- Calò, R.; Marabini, L. Protective effect of Vaccinium myrtillus extract against UVA- and UVB-induced damage in a human keratinocyte cell line (HaCaT cells). J. Photochem. Photobiol. B 2014, 132, 27–35. [Google Scholar] [CrossRef]
- Svobodová, A.; Zdařilová, A.; Vostálová, J. Lonicera caerulea and Vaccinium myrtillus fruit polyphenols protect HaCaT keratinocytes against UVB-induced phototoxic stress and DNA damage. J. Dermatol. Sci. 2009, 56, 196–204. [Google Scholar] [CrossRef] [PubMed]
- Sun, Z.; Park, S.Y.; Hwang, E.; Zhang, M.; Seo, S.A.; Lin, P.; Yi, T.H. Thymus vul garis alleviates UVB irradiation induced skin damage via inhibition of MAPK/AP-1 and activation of Nrf2-ARE antioxidant system. J. Cell Mol. Med. 2017, 21, 336–438. [Google Scholar] [CrossRef]
- Petruk, G.; Di Lorenzo, F.; Imbimbo, P.; Silipo, A.; Bonina, A.; Rizza, L.; Piccoli, R.; Monti, D.M.; Lanzetta, R. Protective effect of Opuntia ficus-indica L. cladodes against UVA-induced oxidative stress in normal human keratinocytes. Bioorg. Med. Chem. Lett. 2017, 27, 5485–5489. [Google Scholar] [CrossRef]
- West, B.J.; Deng, S.; Palu, A.K.; Jensen, C.J. Morinda citrifolia Linn. (Rubiaceae) leaf extracts mitigate UVB-induced erythema. J. Nat. Med. 2009, 63, 351–354. [Google Scholar] [CrossRef]
- Bazylko, A.; Borzym, J.; Parzonko, A. Determination of in vitro antioxidant and UV-protecting activity of aqueous and ethanolic extracts from Galinsoga parviflora and Galinsoga quadriradiata herb. J. Photochem. Photobiol. B 2015, 149, 189–195. [Google Scholar] [CrossRef]
- Cho, Y.-H.; Bahuguna, A.; Kim, H.-H.; Kim, D.-I.; Kim, H.-J.; Yu, J.-M.; Jung, H.-G.; Jang, J.-Y.; Kwak, J.-H.; Park, G.-H.; et al. Potential effect of compounds isolated from Coffea arabica against UV-B induced skin damage by protecting fibroblast cells. J. Photochem. Photobiol. B 2017, 174, 323–332. [Google Scholar] [CrossRef]
- Bulla, M.K.; Hernandes, L.; Baesso, M.L.; Nogueira, A.C.; Bento, A.C.; Bortoluzzi, B.B.; Serra, L.Z.; Cortez, D.A.G. Evaluation of photoprotective potential and percutaneous penetration by photoacoustic spectroscopy of the Schinus terebinthifolius raddi extract. Photochem. Photobiol. 2015, 91, 558–566. [Google Scholar] [CrossRef]
- de Lima-Saraiva, S.R.G.; da Silva Oliveira, F.G.; de Oliveira Junior, R.G.; de Souza Araújo, C.; de Oliveira, A.P.; Pacheco, A.G.M.; Rolim, L.A.; de Amorim, E.L.C.; César, F.C.S.; da Silva Almeida, J.R.G. Chemical analysis and evaluation of antioxidant, antimicrobial, and photoprotective activities of Schinopsis brasiliensis Engl. (Anacardiaceae). Sci. World J. 2017, 2017, 1713921. [Google Scholar] [CrossRef]
- Ebrahimzadeh, M.; Enayatifard, R.; Khalili, M.; Ghaffarloo, M.; Saeedi, M.; Charati, J.Y. Correlation between sun protection factor and antioxidant activity, phenol and flavonoid contents of some medicinal plants. Iran. J. Pharm. Res. 2014, 13, 1041–1047. [Google Scholar] [PubMed]
- Jarzycka, A.; Lewińska, A.; Gancarz, R.; Wilk, K.A. Assessment of extracts of Helichrysum arenarium, Crataegus monogyna, Sambucus nigra in photoprotective UVA and UVB; photostability in cosmetic emulsions. J. Photochem. Photobiol. B 2013, 128, 50–57. [Google Scholar] [CrossRef] [PubMed]
- Lefahal, M.; Zaabat, N.; Ayad, R.; Makhloufi, E.H.; Djarri, L.; Benahmed, M.; Laouer, H.; Nieto, G.; Akkal, S. In vitro assessment of total phenolic and flavonoid contents, antioxidant and photoprotective activities of crude methanolic extract of aerial parts of Capnophyllum peregrinum (L.) Lange (Apiaceae) growing in Algeria. Medicines 2018, 5, 26. [Google Scholar] [CrossRef] [PubMed]
- Martins, F.J.; Caneschi, C.A.; Vieira, J.L.F.; Barbosa, W.; Raposo, N.R.B. Antioxidant activity and potential photoprotective from amazon native flora extracts. J. Photochem. Photobiol. B 2016, 161, 34–39. [Google Scholar] [CrossRef] [PubMed]
- Mejía-Giraldo, J.C.; Winkler, R.; Gallardo, C.; Sánchez-Zapata, A.M.; Puertas-Mejía, M.A. Photoprotective potential of Baccharis antioquensis (Asteraceae) as natural sunscreen. Photochem. Photobiol. 2016, 92, 742–752. [Google Scholar] [CrossRef]
- Muzaffer, U.; Paul, V.I.; Prasad, N.R.; Karthikeyan, R.; Agilan, B. Protective effect of Juglans regia L. against ultraviolet B radiation induced inflammatory responses in human epidermal keratinocytes. Phytomedicine 2018, 42, 100–111. [Google Scholar] [CrossRef]
- Nunes, A.R.; Rodrigues, A.L.M.; de Queiróz, D.B.; Vieira, I.G.P.; Neto, J.F.C.; Junior, J.T.C.; Tintino, S.R.; de Morais, S.M.; Coutinho, H.D.M. Photoprotective potential of medicinal plants from Cerrado biome (Brazil) in relation to phenolic content and antioxidant activity. J. Photochem. Photobiol. B 2018, 189, 119–123. [Google Scholar] [CrossRef]
- He, H.; Li, A.; Li, S.; Tang, J.; Li, L.; Xiong, L. Natural components in sunscreens: Topical formulations with sun protection factor (SPF). Biomed. Pharmacother. 2021, 134, 111161. [Google Scholar] [CrossRef]
- Lekmine, S.; Boussekine, S.; Akkal, S.; Martín-García, A.I.; Boumegoura, A.; Kadi, K.; Djeghim, H.; Mekersi, N.; Bendjedid, S.; Bensouici, C.; et al. Investigation of Photoprotective, Anti-Inflammatory, Antioxidant Capacities and LC–ESI–MS Phenolic Profile of Astragalus gombiformis Pomel. Foods 2021, 10, 1937. [Google Scholar] [CrossRef] [PubMed]
- Quintero-Rincón, P.; Mesa-Arango, A.C.; Flórez-Acosta, O.A.; Zapata-Zapata, C.; Stashenko, E.E.; Pino-Benítez, N. Exploring the Potential of Extracts from Sloanea medusula and S. calva: Formulating Two Skincare Gels with Antioxidant, Sun Protective Factor, and Anti-Candida albicans Activities. Pharmaceuticals 2023, 16, 990. [Google Scholar] [CrossRef]
- Vijayakumar, R.; Salwa Abd Gani, S.; Hasanah Zaidan, U.; Effendi Halmi, I.; Karunakaran, T.; Razak Hamdan, M. Exploring the Potential Use of Hylocereus polyrhizus Peels as a Source of Cosmeceutical Sunscreen Agent for Its Antioxidant and Photoprotective Properties. Evid.-Based Complement. Altern. Med. 2020, 2020, 7520736. [Google Scholar] [CrossRef] [PubMed]
- Fuentes, J.L.; Pedraza Barrera, C.A.; Villamizar Mantilla, D.A.; Flórez González, S.J.; Sierra, L.J.; Ocazionez, R.E.; Stashenko, E.E. Flower Extracts from Ornamental Plants as Sources of Sunscreen Ingredients: Determination by In Vitro Methods of Photoprotective Efficacy, Antigenotoxicity and Safety. Molecules 2022, 27, 5525. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, A.S.; Mazzei, J.L.; Oliveira, C.G.; Evangelista, H.; Marques, M.R.C.; Ferraz, E.R.A.; Felzenszwalb, I. Protection against UV-induced toxicity and lack of mutagenicity of Antarctic Sanionia uncinata. Toxicology 2017, 376, 126–136. [Google Scholar] [CrossRef]
- Fernandes Ada, S.; Santos Alencar, A.; Evangelista, H.; Luiz Mazzei, J.; Felzenszwalb, J. Photoprotective and toxicological activities of extract from the Antarctic moss Sanionia uncinata. Pharmacogn. Mag. 2015, 11, 38–43. [Google Scholar]
- Hubner, A.; Sobreira, F.; Vetore Neto, A.; Pinto, C.A.S.d.O.; Dario, M.F.; Díaz, I.E.C.; Lourenço, F.R.; Rosado, C.; Baby, A.R.; Bacchi, E.M. The synergistic behavior of antioxidant phenolic compounds obtained from Winemaking waste’s valorization, increased the efficacy of a sunscreen system. Antioxidants 2019, 8, 530. [Google Scholar] [CrossRef]
- Mota, M.D.; da Boa Morte, A.N.; Silva, L.C.R.C.; Chinalia, F.A. Sunscreen protection factor enhancement through supplementation with Rambutan (Nephelium lappaceum L.) ethanolic extract. J. Photochem. Photobiol. B 2020, 205, 111837. [Google Scholar] [CrossRef]
- Mota, M.D.; Costa, R.Y.S.; Guedes, A.A.S.; Silva, L.C.R.C.; Chinalia, F.A. Guava-fruit extract can improve the UV-protection efficiency of synthetic filters in sun cream formulations. J. Photochem. Photobiol. B 2019, 201, 111639. [Google Scholar] [CrossRef]
- Catelan, T.B.S.; Gaiola, L.; Ferreira Duarte, B.; Lima Cardoso, C.A. Evaluation of the in vitro photoprotective potential of ethanolic extracts of four species of the genus Campomanesia. J. Photochem. Photobiol. B 2019, 197, 111500. [Google Scholar] [CrossRef]
- Fernandes, A.S.; Mazzei, J.L.; Evangelista, H.; Marques, M.R.C.; Ferraz, E.R.A.; Felzenszwalb, I. Protection against UV-induced oxidative stress and DNA damage by Amazon moss extracts. J. Photochem. Photobiol. B 2018, 183, 331–341. [Google Scholar] [CrossRef]
- Ahn, H.S.; Kim, H.J.; Na, C.; Jang, D.S.; Shin, Y.K.; Lee, S.H. The protective effect of Adenocaulon himalaicum Edgew. and its bioactive compound neochlorogenic acid againstUVB-induced skin damage in human dermal fibroblasts and epidermal keratinocytes. Plants 2021, 10, 1669. [Google Scholar] [CrossRef] [PubMed]
- Jung, J.M.; Kwon, O.Y.; Choi, J.K.; Lee, S.H. Alpinia officinarum Rhizome ameliorates the UVB induced photoaging through attenuating the phosphorylation of AKT and ERK. BMC Complement. Med. Ther. 2022, 22, 232. [Google Scholar] [CrossRef] [PubMed]
- Natewong, S.; Niwaspragrit, C.; Ratanachamnong, P.; Samatiwat, P.; Namchaiw, P.; Jaisin, Y. Photo-Protective and Anti-Inflammatory Effects of Antidesma thwaitesianum Müll. Arg. Fruit Extract against UVB-Induced Keratinocyte Cell Damage. Molecules 2022, 27, 5034. [Google Scholar] [CrossRef]
- Seregheti, T.M.Q.; Pinto, A.P.R.; Gonçalves, M.C.; Antunes, A.S.; Almeida, W.A.S.; Machado, R.S.; Silva, J.N.; Ferreira, P.M.P.; Pessoa, C.; Dos Santos, V.M.R.; et al. Antiproliferative and photoprotective activities of the extracts and compounds from Calea fruticosa. Braz. J. Med. Biol. Res. 2020, 53, e9375. [Google Scholar] [CrossRef]
- Park, S.; Eun-Soo Lee, E.-S.; Park, N.-H.; Hwang, K.; Cho, E.-G. Circadian Expression of TIMP3 Is Disrupted by UVB Irradiation and Recovered by Green Tea Extracts. Int. J. Mol. Sci. 2019, 20, 862. [Google Scholar] [CrossRef] [PubMed]
- Song, C.; Lorz, L.R.; Lee, J.; Cho, J.Y. In Vitro Photoprotective, Anti-Inflammatory, Moisturizing, and Antimelanogenic Effects of a Methanolic Extract of Chrysophyllum lucentifolium Cronquist. Plants 2022, 11, 94. [Google Scholar] [CrossRef]
- Gaweł-Bęben, K.; Kukula-Koch, W.; Hoian, U.; Czop, M.; Strzępek-Gomółka, M.; Antosiewicz, B. Characterization of Cistus × incanus L. and Cistus ladanifer L. Extracts as Potential Multifunctional Antioxidant Ingredients for Skin Protecting Cosmetics. Antioxidants 2020, 9, 202. [Google Scholar] [CrossRef]
- Kavvoura, D.-A.; Stefanakis, M.K.; Kletsas, D.; Katerinopoulos, H.E.; Pratsinis, H. Biological Activities of Ceratonia siliqua Pod and Seed Extracts: A Comparative Analysis of Two Cretan Cultivars. Int. J. Mol. Sci. 2023, 24, 12104. [Google Scholar] [CrossRef]
- Ivanović, S.; Avramović, N.; Dojćinović, B.; Trifunović, S.; Novaković, M.; Tešević, V.; Mandi, B. Chemical Composition, Total Phenols and Flavonoids Contents and Antioxidant Activity as Nutritive Potential of Roasted Hazelnut Skins (Corylus avellana L.). Foods 2020, 9, 430. [Google Scholar] [CrossRef]
- Hering, A.; Stefanowicz-Hajduk, J.; Gucwa, M.; Wielgomas, B.; Ochocka, J.R. Photoprotection and Antiaging Activity of Extracts from Honeybush (Cyclopia sp.)—In Vitro Wound Healing and Inhibition of the Skin Extracellular Matrix Enzymes: Tyrosinase, Collagenase, Elastase and Hyaluronidase. Pharmaceutics 2023, 15, 1542. [Google Scholar] [CrossRef] [PubMed]
- Gea-Botella, S.; Moreno-Chamba, B.; de la Casa, L.; Salazar-Bermeo, J.; Martí, N.; Martínez-Madrid, M.C.; Valero, M.; Saura, D. Carotenoids from Persimmon (Diospyros kaki Thunb.) Byproducts Exert Photoprotective, Antioxidative and Microbial Anti-Adhesive Effects on HaCaT. Pharmaceutics 2021, 13, 1898. [Google Scholar] [CrossRef] [PubMed]
- Ahmady, A.; Amini, M.H.; Zhakfar, A.M.; Babak, G.; Sediqi, M.N. Sun protective potential and physical stability of herbal sunscreen developed from afghan medicinal plants. Turk. J. Pharm. Sci. 2020, 17, 285–292. [Google Scholar] [CrossRef] [PubMed]
- Pintus, F.; Floris, S.; Fais, A.; Era, B.; Porcedda, C.; Tuberoso, C.I.G.; Caddeo, C. Euphorbia characias Extract: Inhibition of Skin Aging-Related Enzymes and Nanoformulation. Plants 2022, 11, 1849. [Google Scholar] [CrossRef] [PubMed]
- Hwang, E.; Gao, W.; Xiao, Y.K.; Ngo, H.T.T.; Yi, H.Y. Helianthus annuus L. flower prevents UVB-induced photodamage in human dermal fibroblasts by regulating the MAPK/AP-1, NFAT, and Nrf2 signaling pathways. J. Cell. Biochem. 2019, 120, 601–612. [Google Scholar] [CrossRef] [PubMed]
- Muzaffer, U.; Paul, V.I.; Agilan, B.; Prasad, N.R. Protective effect of Juglans regia L., against ultraviolet-B induced photoaging in human epidermal keratinocytes. Biomed. Pharmacother. 2019, 111, 724–732. [Google Scholar] [CrossRef]
- Jeon, J.S.; Kang, H.M.; Park, J.H.; Kang, J.S.; Lee, Y.J.; Park, Y.H.; Je, B.I.; Park, S.Y.; Choi, Y.W. A Comparative Study on Photo-Protective and Anti-Melanogenic Properties of Different Kadsura coccinea Extracts. Plants 2021, 10, 1633. [Google Scholar] [CrossRef]
- Bianchini Silva, L.S.; Perasoli, F.B.; Carvalho, K.V.; Vieira, K.M.; Paz Lopes, M.T.; Bianco de Souza, G.H.; Henrique Dos Santos, O.D.; Freitas, K.M. Melaleuca leucadendron (L.) L. flower extract exhibits antioxidant and photoprotective activities in human keratinocytes exposed to ultraviolet B radiation. Free Radic. Biol. Med. 2020, 159, 54–65. [Google Scholar] [CrossRef]
- Santhanam, R.; Karunakaran, T.; Sowndhararajan, K.; Zulkifli, M.F.; Kothandaraman, M.G.; Aravindhan, V.; Ismail, W.I.W. Photoprotective Potential, Cytotoxicity, and UPLC-QTOF/MS Analysis on Bioactive Solvent Fractions of Moringa concanensis Nimmo Bark. Evid.-Based Complement. Altern. Med. 2022, 2022, 3781189. [Google Scholar] [CrossRef]
- Her, Y.; Shin, B.-N.; Lee, Y.L.; Park, J.H.; Kim, D.W.; Kim, K.S.; Kim, H.; Song, M.; Kim, J.-D.; Won, M.-H.; et al. Oenanthe javanica Extract Protects Mouse Skin from UVB Radiation via Attenuating Collagen Disruption and Inflammation. Int. J. Mol. Sci. 2019, 20, 1435. [Google Scholar] [CrossRef]
- Jeong, D.; Lee, J.; Park, S.H.; Kim, Y.A.; Park, B.J.; Oh, J.; Sung, G.-H.; Aravinthan, A.; Kim, J.-H.; Kang, H.; et al. Antiphotoaging and Antimelanogenic Effects of Penthorum chinense Pursh Ethanol Extract due to Antioxidant- and Autophagy-Inducing Properties. Oxid. Med. Cell. Longev. 2019, 2019, 9679731. [Google Scholar] [CrossRef]
- Lorz, L.R.; Yoo, B.C.; Kim, M.-Y.; Cho, J.Y. Anti-Wrinkling and Anti-Melanogenic Effect of Pradosia mutisii Methanol Extract. Int. J. Mol. Sci. 2019, 20, 1043. [Google Scholar] [CrossRef]
- Hong, Y.H.; Kim, J.H.; Cho, J.Y. Photoaging Protective Effects of Ranunculus bulumei Methanol Extract. Evid.-Based Complement. Altern. Med. 2020, 2020, 1761785. [Google Scholar] [CrossRef]
- Ibrahim, N.; Abbas, H.; El-Sayed, N.S.; Gad, H.A. Rosmarinus officinalis L. hexane extract: Phytochemical analysis, nanoencapsulation, and in silico, in vitro, and in vivo anti-photoaging potential evaluation. Sci. Rep. 2022, 12, 13102. [Google Scholar] [CrossRef]
- Wang, P.-W.; Cheng, Y.-C.; Hung, Y.-C.; Lee, C.-H.; Fang, J.-Y.; Li, W.-T.; Wu, Y.-R.; Pan, T.-L. Red Raspberry Extract Protects the Skin against UVB-Induced Damage with Antioxidative and Anti-inflammatory Properties. Oxid. Med. Cell Longev. 2019, 2019, 9529676. [Google Scholar] [CrossRef] [PubMed]
- Krgović, N.; Jovanović, M.; Aradski, A.A.; Janković, T.; Stević, T.; Zdunić, G.; Laušević, S.D.; Šavikin, K. Bioassay-Guided Skin-Beneficial Effects of Fractionated Sideritis raeseri subsp. raeseri Extract. Plants 2022, 11, 2677. [Google Scholar] [CrossRef]
- Kwon, K.-R.; Alam, B.; Park, J.-H.; Kim, T.-H.; Lee, S.-H. Attenuation of UVB-Induced Photo-Aging by Polyphenolic-Rich Spatholobus suberectus Stem Extract Via Modulation of MAPK/AP-1/MMPs Signaling in Human Keratinocytes. Nutrients 2019, 11, 1341. [Google Scholar] [CrossRef]
- Park, H.-A.; Kim, M.Y.; Lee, N.-Y.; Lim, J.; Park, K.-B.; Lee, C.-K.; Nguyen, V.D.; Kim, J.; Park, J.-T.; Park, J.-I. Variation of Triterpenic Acids in 12 Wild Syzygium formosum and Anti-Inflammation Activity on Human Keratinocyte HaCaT. Plants 2021, 10, 2428. [Google Scholar] [CrossRef] [PubMed]
- Vostálová, J.; Tinková, E.; Biedermann, D.; Kosina, P.; Ulrichová, J.; Rajnochová Svobodová, A. Skin Protective Activity of Silymarin and its Flavonolignans. Molecules 2019, 24, 1022. [Google Scholar] [CrossRef] [PubMed]
- Era, B.; Floris, S.; Sogos, V.; Porcedda, C.; Piras, A.; Medda, R.; Fais, A.; Pintus, F. Anti-Aging Potential of Extracts from Washingtonia filifera Seeds. Plants 2021, 10, 151. [Google Scholar] [CrossRef]
- Hao, D.; Wen, X.; Liu, L.; Wang, L.; Zhou, X.; Li, Y.; Zeng, X.; He, G.; Jiang, X. Sanshool improves UVB-induced skin photodamage by targeting JAK2/STAT3-dependent autophagy. Cell. Death. Dis. 2019, 10, 19–31. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, A.C.; Costa, T.F.; Andrade, Z.A.; Medrado, A.R. Wound healing—A literature review. An. Bras. Dermatol. 2016, 91, 614–620. [Google Scholar] [CrossRef] [PubMed]
- Shedoeva, A.; Leavesley, D.; Upton, Z.; Fan, C. Wound Healing and the Use of Medicinal Plants. Evid.-Based Complement. Altern. Med. 2019, 2019, 2684108. [Google Scholar] [CrossRef]
- Bass, S.; Chowdhury, M.; Raj, S.; Raj Chaudhary, N. Effects of Phytomedicines on Wound Healing. Eur. J. Exper. Biol. 2021, 11, 133–138. [Google Scholar]
- Bindschadler, M.; McGrath, J.L. Sheet migration by wounded monolayers as an emergent property of single-cell dynamics. J. Cell Sci. 2007, 120, 876–884. [Google Scholar] [CrossRef]
- Parent, C.A.; Devreotes, P.N. A cell’s sense of direction. Science 1999, 284, 765–770. [Google Scholar] [CrossRef]
- Horwitz, R.; Webb, D. Cell migration. Curr. Biol. 2003, 13, 756–759. [Google Scholar] [CrossRef]
- Sivamani, R.K.; Garcia, M.S.; Rivkah Isseroff, R. Wound re-epithelialization: Modulating keratinocyte migration in wound healing. Front. Biosci. 2007, 12, 2849–2868. [Google Scholar]
- Seeger, M.A.; Paller, A.S. The Roles of Growth Factors in Keratinocyte Migration. Adv. Wound Care 2015, 4, 213–224. [Google Scholar] [CrossRef]
- Zulkefli, N.; Che Zahari, C.N.M.; Sayuti, N.H.; Kamarudin, A.A.; Saad, N.; Hamezah, H.S.; Bunawan, H.; Baharum, S.N.; Mediani, A.; Ahmed, Q.U.; et al. Flavonoids as Potential Wound-Healing Molecules: Emphasis on Pathways Perspective. Int. J. Mol. Sci. 2023, 24, 4607. [Google Scholar] [CrossRef]
- Liang, Y.; He, J.; Guo, B. Functional Hydrogels as Wound Dressing to Enhance Wound Healing. ACS Nano 2021, 15, 12687–12722. [Google Scholar] [CrossRef]
- Chittasupho, C.; Manthaisong, A.; Okonogi, S.; Tadtong, S.; Samee, W. Effects of Quercetin and Curcumin Combination on Antibacterial, Antioxidant, In Vitro Wound Healing and Migration of Human Dermal Fibroblast Cells. Int. J. Mol. Sci. 2022, 23, 142. [Google Scholar] [CrossRef]
- Bittner Fialová, S.; Rendeková, K.; Mučaji, P.; Nagy, M.; Slobodníková, L. Antibacterial Activity of Medicinal Plants and Their Constituents in the Context of Skin and Wound Infections, European Legislation and Folk Medicine-A Review. Int. J. Mol. Sci. 2021, 22, 10746. [Google Scholar] [CrossRef]
- Nowak, A.; Zagórska-Dziok, M.; Perużyńska, M.; Cybulska, K.; Kucharska, E.; Ossowicz-Rupniewska, P.; Piotrowska, K.; Duchnik, W.; Kucharski, Ł.; Sulikowski, T.; et al. Assessment of the Anti-Inflammatory, Antibacterial and Anti-Aging Properties and Possible Use on the Skin of Hydrogels Containing Epilobium angustifolium L. Extracts. Front. Pharmacol. 2022, 13, 896706. [Google Scholar] [CrossRef]
- Albahri, G.; Badran, A.; Hijazi, A.; Daou, A.; Baydoun, E.; Nasser, M.; Merah, O. The Therapeutic Wound Healing Bioactivities of Various Medicinal Plants. Life 2023, 13, 317. [Google Scholar] [CrossRef] [PubMed]
- Pain, S.; Altobelli, C.; Boher, A.; Cittadini, L.; Favre-Mercuret, M.; Gaillard, C.; Sohm, B.; Vogelgesang, B.; André-Frei, V. Surface rejuvenating effect of Achillea millefolium extract. Int. J. Cosmet. Sci. 2011, 33, 535–542. [Google Scholar] [CrossRef]
- Sajithlal, G.B. Influence of aloe vera on collagen turnover in healing of dermal wounds in rats. Indian J. Exp. Biol. 2000, 36, 896–901. [Google Scholar]
- Rezaei, M.; Dadgar, Z.; Noori-Zadeh, A.; Mesbah-Namin, S.A.; Pakzad, I.; Davodian, E. Evaluation of the antibacterial activity of the Althaea officinalis L. leaf extract and its wound healing potency in the rat model of excision wound creation. Avicenna J. Phytomed. 2015, 5, 105–112. [Google Scholar] [PubMed]
- Preethi, K.C.; Kuttan, R. Wound healing activity of flower extract of Calendula officinalis. J. Basic Clin. Physiol. Pharmacol. 2009, 20, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Yen, Y.H. Curcumin accelerates cutaneous wound healing via multiple biological actions: The involvement of TNF-α, MMP-9,-SMA, and collagen. Int. Wound J. 2018, 15, 605–617. [Google Scholar] [CrossRef] [PubMed]
- Mumtaz, R.; Zubair, M.; Khan, M.A.; Muzammil, S.; Siddique, M.H. Extracts of Eucalyptus alba Promote Diabetic Wound Healing by Inhibiting α-Glucosidase and Stimulating Cell Proliferation. Evid. Based Complement. Altern. Med. 2022, 2022, 4953105. [Google Scholar] [CrossRef] [PubMed]
- Ranzato, E.; Martinotti, S.; Burlando, B. Wound healing properties of jojoba liquid wax: An in vitro study. J. Ethnopharmacol. 2011, 134, 443–449. [Google Scholar] [CrossRef]
- Wang, C.; Shang, H.; Cui, W.; Zhou, F.; Zhang, S.; Wang, X.; Gao, P.; Wei, K.; Zhu, R. Pine pollen polysaccharides promote cel proliferation and accelerate wound healing by activating the JAK2-STAT3 signaling pathway. Int. J. Biol. Macromol. 2022, 210, 579–587. [Google Scholar] [CrossRef]
- Chen, G.; He, L.; Zhang, P.; Zhang, J.; Mei, X.; Wang, D.; Zhang, Y.; Ren, X.; Chen, Z. Encapsulation of green tea polyphenol nanospheres in PVA/alginate hydrogel for promoting wound healing of diabetic rats by regulating PI3K/AKT pathway. Mater. Sci. Eng. C 2020, 110, 110686. [Google Scholar] [CrossRef] [PubMed]
- Vasilenko, T.; Kováč, I.; Slezák, M.; Ďurkáč, J.; Peržel’ová, N.; Čoma, M.; Kaňuchová, M.; Urban, L.; Szabo, P.; Dvořánková, B.; et al. Agrimonia eupatoria L. Aqueous Extract Improves Skin Wound Healing: An In Vitro Study in Fibroblasts and Keratinocytes and In Vivo Study in Rats. In Vivo 2022, 36, 1236–1244. [Google Scholar] [CrossRef]
- Lee, S.-Y.; Won, K.-J.; Kim, D.-Y.; Kim, M.-J.; Won, Y.-R.; Kim, N.-Y.; Lee, H.-M. Wound Healing-Promoting and Melanogenesis-Inhibiting Activities of Angelica polymorpha Maxim. Flower Absolute In Vitro and Its Chemical Composition. Molecules 2021, 26, 6172. [Google Scholar] [CrossRef]
- Mazumdar, S.; Ghosh, A.K.; Dinda, M.; Das, A.K.; Das, S.; Jana, K.; Karmakar, P. Evaluation of wound healing activity of ethanol extract of Annona reticulata L. leaf both in vitro and in diabetic mice model. J. Tradit. Complement. Med. 2021, 11, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Akbari, F.; Azadbakht, M.; Bagheri, A.; Vahedi, L. In Vitro and In Vivo Wound Healing Activity of Astragalus floccosus Boiss. (Fabaceae). Adv. Pharmacol. Pharm. Sci. 2022, 2022, 7865015. [Google Scholar] [CrossRef]
- Emrich, S.; Schuster, A.; Schnabel, T.; Oostingh, G.J. Antimicrobial Activity and Wound-Healing Capacity of Birch, Beech and Larch Bark Extracts. Molecules 2022, 27, 2817. [Google Scholar] [CrossRef]
- Ruttanapattanakul, J.; Wikan, N.; Okonogi, S.; Na Takuathung, M.; Buacheen, P.; Pitchakarn, P.; Potikanond, S.; Nimlamool, W. Boesenbergia rotunda extract accelerates human keratinocyte proliferation through activating ERK1/2 and PI3K/Akt kinases. Biomed. Pharmacother. 2021, 133, 111002. [Google Scholar] [CrossRef]
- Salas-Oropeza, J.; Jimenez-Estrada, M.; Perez-Torres, A.; Castell-Rodriguez, A.E.; Becerril-Millan, R.; Rodriguez-Monroy, M.A.; Jarquin-Yañez, K.; Canales-Martinez, M.M. Wound Healing Activity of α-Pinene and α-Phellandrene. Molecules 2021, 26, 2488. [Google Scholar] [CrossRef]
- Nizioł-Łukaszewska, Z.; Zagórska-Dziok, M.; Ziemlewska, A.; Bujak, T. Comparison of the Antiaging and Protective Properties of Plants from the Apiaceae Family. Oxid. Med. Cell Longev. 2020, 2020, 5307614. [Google Scholar] [CrossRef]
- Rafsanjani, S.M.; Naeini, A.T.; Meimandi-Parizi, A.; Nowzari, F.; Wani, M.M.; Iraji, A. Wound healing effect of Carum carvi L. on the incised skin wound in male rats: Histopathology, total protein and biomechanical evaluations. Vet. Med. Sci. 2022, 8, 2726–2737. [Google Scholar] [CrossRef] [PubMed]
- Somwong, P.; Kamkaen, N. Wound-healing activity and quantification of bioactive compounds from Derris scandens extract. J. Adv. Pharm. Technol. Res. 2022, 13, 38–43. [Google Scholar] [PubMed]
- Park, S.M.; Won, K.J.; Hwang, D.I.; Kim, D.Y.; Kim, H.B.; Li, Y.; Lee, H.M. Potential Beneficial Effects of Digitaria ciliaris Flower Absolute on the Wound Healing-Linked Activities of Fibroblasts and Keratinocytes. Planta Med. 2020, 86, 348–355. [Google Scholar] [CrossRef]
- Assar, D.H.; Elhabashi, N.; Mokhbatly, A.A.A.; Ragab, A.E.; Elbialy, Z.I.; Rizk, S.A.; Albalawi, A.E.; Althobaiti, N.A.; Jaouni, S.A.; Atiba, A. Wound healing potential of licorice extract in rat model: Antioxidants, histopathological, immunohistochemical and gene expression evidences. Biomed. Pharmacother. 2021, 143, 112151. [Google Scholar] [CrossRef] [PubMed]
- Siriwattanasatorn, M.; Itharat, A.; Thongdeeying, P.; Ooraikul, B. In Vitro Wound Healing Activities of Three Most Commonly Used Thai Medicinal Plants and Their Three Markers. Evid. Based. Complement. Alternat. Med. 2020, 2020, 6795383. [Google Scholar] [CrossRef]
- Loggenberg, S.R.; Twilley, D.; De Canha, M.N.; Meyer, D.; Mabena, E.C.; Lall, N. Evaluation of Wound Healing and Antibacterial Potential of Greyia radlkoferi Szyszyl. Ethanolic Leaf Extract. Front. Pharmacol. 2022, 13, 806285. [Google Scholar] [CrossRef] [PubMed]
- Yoon, J.H.; Park, S.H.; Yoon, S.E.; Hong, S.Y.; Lee, J.B.; Lee, J.; Cho, J.Y. Hydrangea serrata Hot Water Extract and Its Major Ingredient Hydrangenol Improve Skin Moisturization and Wrinkle Conditions via AP-1 and Akt/PI3K Pathway Upregulation. Nutrients 2023, 15, 2436. [Google Scholar] [CrossRef]
- Hernandez-Hernandez, A.B.; Alarcon-Aguilar, F.J.; Garcia-Lorenzana, M.; Rodriguez-Monroy, M.A.; Canales-Martinez, M.M. Jatropha neopauciflora Pax Latex Exhibits Wound-Healing Effect in Normal and Diabetic Mice. J. Evid. Based. Integr. Med. 2021, 26, 2515690X20986762. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.Y.; Won, K.J.; Kim, H.B.; Kim, D.Y.; Kim, M.J.; Won, Y.R.; Lee, H.M. Chemical Composition of Salix koreensis Anderss Flower Absolute and Its Skin Wound Healing Activities In Vitro. Plants 2022, 11, 246. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.-C.; Nien, C.-J.; Chen, L.-G.; Huang, K.-Y.; Chang, W.-J.; Huang, H.-M. Effects of Sapindus mukorossi Seed Oil on Skin Wound Healing: In Vivo and in Vitro Testing. Int. J. Mol. Sci. 2019, 20, 2579. [Google Scholar] [CrossRef] [PubMed]
- de Freitas Figueiredo, F.; Filho, F.C.; Damazo, A.S.; Arunachalam, K.; Colodel, E.M.; Ribeiro, M.; Venturini, C.L.; Oliveira, D.M.; Machado, M.T.; Pavan, E.; et al. Sorocea guilleminiana Gaudich.: Wound healing activity, action mechanisms, and chemical characterization of the leaf infusion. J. Ethnopharmacol. 2020, 248, 112307. [Google Scholar] [CrossRef] [PubMed]
- Kang, M.C.; Yumnam, S.; Park, W.S.; So, H.M.; Kim, K.H.; Shin, M.C.; Ahn, M.-J.; Kim, S.Y. Ulmus parvifolia Accelerates Skin Wound Healing by Regulating the Expression of MMPs and TGF-β. J. Clin. Med. 2020, 9, 59. [Google Scholar] [CrossRef]
- Rahman, S.; Islam, R.; Rana, M.; Spitzhorn, L.-S.; Rahman, M.S.; Adjaye, J.; Asaduzzaman, S.M. Characterization of burn wound healing gel prepared from human amniotic membrane and Aloe vera extract. BMC Complement. Altern. Med. 2019, 19, 115. [Google Scholar] [CrossRef]
- Lopes, C.M.I.; Baratella-Evêncio, L.; DE Souza, I.A.; DE Oliveira, E.B.; Sá, J.G.A.; Santana, M.A.N.; Neto, P.P.M.; DE Santana, E.S.; DA Silva, L.A.; Vieira, J.R.C. Evaluation of cytotoxicity and wound healing activity of Avicennia schaueriana in cream. An. Acad. Bras. Cienc. 2019, 91, e20180171. [Google Scholar] [CrossRef]
- Amrati, F.E.-Z.; Chebaibi, M.; Galvão de Azevedo, R.; Conte, R.; Slighoua, M.; Mssillou, I.; Kiokias, S.; de Freitas Gomes, A.; Soares Pontes, G.; Bousta, D. Phenolic Composition, Wound Healing, Antinociceptive, and Anticancer Effects of Caralluma europaea Extracts. Molecules 2023, 28, 1780. [Google Scholar] [CrossRef]
- Moglad, E.H.; Hamad, A.M.; Fatima, F.; Devanathadesikan Seshadri, V.; Naz, M. Antimicrobial and wound healing activities of certain Sudanese medicinal plants. Saudi. J. Biol. Sci. 2020, 27, 1766–1772. [Google Scholar] [CrossRef]
- Teshome, N.; Degu, A.; Ashenafi, E.; Ayele, E.; Abebe, A. Evaluation of Wound Healing and Anti-Inflammatory Activity of Hydroalcoholic Leaf Extract of Clematis simensis Fresen (Ranunculaceae). Clin. Cosmet. Investig. Dermatol. 2022, 15, 1883–1897. [Google Scholar] [CrossRef]
- Ankomah, A.D.; Boakye, Y.D.; Agana, T.A.; Boamah, V.E.; Sampene Ossei, P.P.; Adu, F.; Agyare, C. Evaluation of Dermal Toxicity and Wound Healing Activity of Cnestis ferruginea Vahl ex DC. Adv. Pharmacol. Pharm. Sci. 2022, 2022, 5268613. [Google Scholar] [CrossRef]
- Saleem, U.; Khalid, S.; Zaib, S.; Anwar, F.; Akhtar, M.F.; Hussain, L.; Saleem, A.; Ahmad, B. Wound Healing Potential and In Silico Appraisal of Convolvulus arvensis L. Methanolic Extract. Biomed. Res. Int. 2022, 2022, 1373160. [Google Scholar] [CrossRef]
- Ahmed, A.S.; Taher, M.; Mandal, U.K.; Jaffri, J.; Susanti, D.; Mahmood, S.; Zakaria, Z.A. Pharmacological properties of Centella asiatica hydrogel in accelerating wound healing in rabbits. BMC Complement Altern. Med. 2019, 19, 213. [Google Scholar] [CrossRef]
- Salhi, N.; El Guourrami, O.; Rouas, L.; Moussaid, S.; Moutawalli, A.; Benkhouili, F.Z.; Ameggouz, M.; Alshahrani, M.M.; Al Awadh, A.A.; Bouyahya, A.; et al. Evaluation of the Wound Healing Potential of Cynara humilis Extracts in the Treatment of Skin Burns. Evid. Based. Complement. Alternat. Med. 2023, 2023, 5855948. [Google Scholar] [CrossRef]
- Bardaa, S.; Makni, K.; Boudaouara, O.; Bardaa, T.; Ktari, N.; Hachicha, S.; Ben Salah, R.; Kallel, R.; Sahnoun, Z.; Boufi, S. Development and Evaluation of the Wound Healing Effect of a Novel Topical Cream Formula Based on Ginkgo biloba Extract on Wounds in Diabetic Rats. Biomed. Res. Int. 2021, 2021, 6474706. [Google Scholar] [CrossRef]
- Ahmad, S.U.; Binti Aladdin, N.-A.; Jamal, J.A.; Shuid, A.N.; Mohamed, I.N. Evaluation of Wound-Healing and Antioxidant Effects of Marantodes pumilum (Blume) Kuntze in an Excision Wound Model. Molecules 2021, 26, 228. [Google Scholar] [CrossRef]
- Okur, M.E.; Karadağ, A.E.; Üstündağ Okur, N.; Özhan, Y.; Sipahi, H.; Ayla, S.; Daylan, B.; Demirci, B.; Demirci, F. In Vivo Wound Healing and In Vitro Anti-Inflammatory Activity Evaluation of Phlomis russeliana Extract Gel Formulations. Molecules 2020, 25, 2695. [Google Scholar] [CrossRef]
- Niknam, S.; Tofighi, Z.; Faramarzi, M.A.; Abdollahifar, M.A.; Sajadi, E.; Dinarvand, R.; Toliyat, T. Polyherbal combination for wound healing: Matricaria chamomilla L. and Punica granatum L. DARU J. Pharm. Sci. 2021, 29, 133–145. [Google Scholar] [CrossRef]
- Upadhyay, G.; Tiwari, N.; Maurya, H.; Upadhyay, J.; Joshi, R.; Ansari, M.N. In Vivo wound-healing and antioxidant activity of aqueous extract of Roylea elegans leaves against physically induced burn model in Wistar albino rats. 3 Biotech 2021, 11, 442. [Google Scholar] [CrossRef]
- Gul, H.; Naseer, R.D.; Abbas, I.; Khan, E.A.; Rehman, H.U.; Nawaz, A.; Azad, A.K.; Albadrani, G.M.; Altyar, A.E.; Albrakati, A.; et al. The Therapeutic Application of Tamarix aphylla Extract Loaded Nanoemulsion Cream for Acid-Burn Wound Healing and Skin Regeneration. Medicina 2023, 59, 34. [Google Scholar] [CrossRef]
- Abeje, B.A.; Bekele, T.; Getahun, K.A.; Asrie, A.B. Evaluation of Wound Healing Activity of 80% Hydromethanolic Crude Extract and Solvent Fractions of the Leaves of Urtica simensis in Mice. J. Exp. Pharmacol. 2022, 14, 221–241. [Google Scholar] [CrossRef]
- Carvalho, G.R.; Braz, D.S.; Gonçalves, T.C.O.; Aires, R.; Côco, L.Z.; Guidoni, M.; Fronza, M.; Endringer, D.C.; Júnior, A.D.S.; Campos-Toimil, M.; et al. Development and Evaluation of Virola oleifera Formulation for Cutaneous Wound Healing. Antioxidants 2022, 11, 1647. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Liu, Y.; Cai, K.; Zhang, B.; Tang, S.; Zhang, W.; Liu, W. Antibacterial polysaccharide-based hydrogel dressing containing plant essential oil for burn wound healing. Burn. Trauma 2021, 9, tkab041. [Google Scholar] [CrossRef] [PubMed]
- Qureshi, K.A.; Mohammed, S.A.A.; Khan, O.; Ali, H.M.; El-Readi, M.Z.; Mohammed, H.A. Cinnamaldehyde-Based Self-Nanoemulsion (CA-SNEDDS) Accelerates Wound Healing and Exerts Antimicrobial, Antioxidant, and Anti-Inflammatory Effects in Rats’ Skin Burn Model. Molecules 2022, 27, 5225. [Google Scholar] [CrossRef]
- George, J.; Sneed, K.; Pathak, Y. The Skin Aging Process and Anti-Aging Strategies. Biomed. J. Sci. Tech. Res. 2022, 42, 33377–33386. [Google Scholar] [CrossRef]
- Russell-Goldman, E.; Murphy, G.F. The Pathobiology of Skin Aging New Insights into an Old Dilemma. Am. J. Pathol. 2020, 190, 1356–1369. [Google Scholar] [CrossRef]
- Feingold, K.R.; Elias, P.M. Role of lipids in the formation and maintenance of the cutaneous permeability barier. Biochim. Biophys. Acta 2014, 1841, 280–294. [Google Scholar] [CrossRef]
- van Smeden, J.; Janssens, M.; Gooris, G.S.; Bouwstra, J.A. The important role of stratum corneum lipids for the cutaneous barrier function. Biochim. Biophys. Acta 2014, 1841, 295–313. [Google Scholar] [CrossRef]
- Gębalski, J.; Graczyk, F.; Załuski, D. Paving the way towards effective plant-based inhibitors of hyaluronidase and tyrosinase: A critical review on a structure–activity relationship. J. Enzyme Inhib. Med. Chem. 2022, 37, 1120–1195. [Google Scholar] [CrossRef]
- Thring, T.S.; Hili, P.; Naughton, D.P. Anti-collagenase, anti-elastase and anti-oxidant activities of extracts from 21 plants. BMC Complement. Altern. Med. 2009, 9, 27. [Google Scholar] [CrossRef]
- Zagórska-Dziok, M.; Bujak, T.; Ziemlewska, A.; Nizioł-Łukaszewska, Z. Positive Effect of Cannabis sativa L. Herb Extracts on Skin Cells and Assessment of Cannabinoid-Based Hydrogels Properties. Molecules 2021, 26, 802. [Google Scholar] [CrossRef]
- Poomanee, W.; Yaowiwat, N.; Pattarachaidaecharuch, T.; Leelapornpisid, P. Optimized multiherbal combination and in vivo anti-skin aging potential: A randomized double blind placebo controlled study. Sci. Rep. 2023, 13, 5633. [Google Scholar] [CrossRef]
- Ghimeray, A.K.; Jung, U.S.; Lee, H.Y.; Ki, Y.H.; Ryu, E.K.; Chang, M.S. In vitro antioxidant, collagenase inhibition, and in vivo anti-wrinkle effects of combined formulation containing Punica granatum, Ginkgo biloba, Ficus carica and Morus alba fruits extract. Clin. Cosmet. Investig. Dermatol. 2015, 8, 389–396. [Google Scholar] [CrossRef]
- Pieczykolan, A.; Pietrzak, W.; Dos Santos Szewczyk, K.; Gawlik-Dziki, U.; Wang, R. LC-ESI-MS/MS Polyphenolic Profile and In Vitro Study of Cosmetic Potential of Aerva lanata (L.) Juss. Herb Extracts. Molecules 2022, 27, 1259. [Google Scholar] [CrossRef]
- Gam, D.H.; Hong, J.W.; Kim, J.H.; Kim, J.W. Skin-Whitening and Anti-Wrinkle Effects of Bioactive Compounds Isolated from Peanut Shell Using Ultrasound-Assisted Extraction. Molecules 2021, 26, 1231. [Google Scholar] [CrossRef]
- Kim, K.Y.; Lee, E.J.; Whang, W.K.; Park, C.H. In vitro and in vivo anti-aging effects of compounds isolated from Artemisia iwayomogi. J. Anal. Sci. Technol. 2019, 10, 35. [Google Scholar] [CrossRef]
- Sriyab, S.; Laosirisathian, N.; Punyoyai, C.; Anuchapreeda, S.; Tima, S.; Chiampanichayakul, S.; Chaiyana, W. Nutricosmetic effects of Asparagus officinalis: A potent matrix metalloproteinase-1 inhibitor. Sci. Rep. 2021, 11, 8772. [Google Scholar] [CrossRef] [PubMed]
- Michalak, M.; Zagórska-Dziok, M.; Klimek-Szczykutowicz, M.; Szopa, A. Phenolic Profile and Comparison of the Antioxidant, Anti-Ageing, Anti-Inflammatory, and Protective Activities of Borago officinalis Extracts on Skin Cells. Molecules 2023, 28, 868. [Google Scholar] [CrossRef]
- Sadeer, N.B.; Sinan, K.I.; Cziáky, Z.; Jek, J.; Zengin, G.; Jeewon, R.; Abdallah, H.H.; Rengasamy, K.R.R.; Mahomoodally, M.F. Assessment of the Pharmacological Properties and Phytochemical Profile of Bruguiera gymnorhiza (L.) Lam Using In Vitro Studies, In Silico Docking, and Multivariate Analysis. Biomolecules 2020, 10, 731. [Google Scholar] [CrossRef]
- Nur, S.; Setiawan, H.; Hanafi, M.; Elya, B. Phytochemical composition, antioxidant, in vitro and in silico studies of active compounds of Curculigo latifolia extracts as promising elastase inhibitor. Saudi. J. Bio. Sci. 2023, 30, 103716. [Google Scholar] [CrossRef] [PubMed]
- Hong-in, P.; Chaiyana, W. Potential cosmeceutical lamellar liquid crystals containing black longan (Dimocarpus longan Lour.) seed extract for MMP-1 and hyaluronidase inhibition. Sci. Rep. 2022, 12, 7683. [Google Scholar] [CrossRef] [PubMed]
- Tungmunnithum, D.; Drouet, S.; Hano, C. Validation of a High-Performance Liquid Chromatography with Photodiode Array Detection Method for the Separation and Quantification of Antioxidant and Skin Anti-Aging Flavonoids from Nelumbo nucifera Gaertn. Stamen Extract. Molecules 2022, 27, 1102. [Google Scholar] [CrossRef]
- Marijan, M.; Mitar, A.; Jakupovic, L.; Prlic Kardum, J.; Zovko Končic, M. Optimization of Bioactive Phenolics Extraction and Cosmeceutical Activity of Eco-Friendly Polypropylene-Glycol– Lactic-Acid-Based Extracts of Olive Leaf. Molecules 2022, 27, 529. [Google Scholar] [CrossRef]
- Andradea, J.M.; Domínguez-Martín, E.M.; Nicolai, M.; Faustino, C.; Rodrigues, L.M.; Rijo, P. Screening the dermatological potential of Plectranthus species components: Antioxidant and inhibitory capacities over elastase, collagenase and tyrosinase. J. Enzyme Inhib. Med. Chem. 2021, 36, 258–270. [Google Scholar] [CrossRef]
- Altyar, A.E.; Ashour, M.L.; Youssef, F.S. Premna odorata: Seasonal Metabolic Variation in the Essential Oil Composition of Its Leaf and Verification of Its Anti-Ageing Potential via In Vitro Assays and Molecular Modelling. Biomolecules 2020, 10, 879. [Google Scholar] [CrossRef] [PubMed]
- Chaiyana, W.; Chansakaow, S.; Intasai, N.; Kiattisin, K.; Lee, K.-H.; Lin, W.-C.; Lue, S.-C.; Leelapornpisid, P. Chemical Constituents, Antioxidant, Anti-MMPs, and Anti-Hyaluronidase Activities of Thunbergia laurifolia Lindl. Leaf Extracts for Skin Aging and Skin Damage Prevention. Molecules 2020, 25, 1923. [Google Scholar] [CrossRef]
- Waqas, M.K.; Akhtar, N.; Rasul, A.; Sethi, A.; Abbas, K.; Hussain, T. Non-invasive in vivo evaluations of cosmetic emulsion containing phytoextract of grape seeds in the treatment of skin aging by using noninvasive bio-engineering techniques. Acta Pol. Pharm. Drug Res. 2018, 75, 97–105. [Google Scholar]
- Abdelfattah, M.A.O.; Dmirieh, M.; Bakrim, W.B.; Mouhtady, O.; Ghareeb, M.A.; Wink, M.; Sobeh, M. Antioxidant and anti-aging effects of Warburgia salutaris bark aqueous extract: Evidences from in silico, in vitro and in vivo studies. J. Ethnopharmacol. 2022, 292, 115187. [Google Scholar] [CrossRef] [PubMed]
- Bujak, T.; Zagórska-Dziok, M.; Ziemlewska, A.; Nizioł-Łukaszewska, Z.; Wasilewski, T.; Hordyjewicz-Baran, Z. Antioxidant and Cytoprotective Properties of Plant Extract from Dry Flowers as Functional Dyes for Cosmetic Products. Molecules 2021, 26, 2809. [Google Scholar] [CrossRef]
- Michailidis, D.; Angelis, A.; Nikolaou, P.E.; Mitakou, S.; Skaltsounis, A.L. Exploitation of Vitis vinifera, Foeniculum vulgare, Cannabis sativa and Punica granatum By-Product Seeds as Dermo-Cosmetic Agents. Molecules 2021, 26, 731. [Google Scholar] [CrossRef]
- Ito, S. A chemist’s view of melanogenesis. Pigment. Cell Res. 2003, 16, 230–236. [Google Scholar] [CrossRef]
- Solano, F. Melanins: Skin pigments and much more—Types, structural models, biological functions, and formation routes. New J. Sci. 2014, 2014, 498276. [Google Scholar] [CrossRef]
- Simon, J.D.; Peles, D.; Wakamatsu, K.; Ito, S. Current challenges in understanding melanogenesis: Bridging chemistry, biological control, morphology, and function. Pigment. Cell Melanoma Res. 2009, 22, 563–579. [Google Scholar] [CrossRef]
- d’Ischia, M.; Wakamatsu, K.; Cicoira, F.; Di Mauro, E.; Garcia-Borron, J.C.; Commo, S.; Galván, I.; Ghanem, G.; Kenzo, K.; Meredith, P.; et al. Melanins and melanogenesis: From pigment cells to human health and technological applications. Pigment. Cell Melanoma Res. 2015, 28, 520–544. [Google Scholar] [CrossRef] [PubMed]
- Hearing, V.J. Determination of melanin synthetic pathway. J. Investig. Dermatol. 2011, 131, E8–E11. [Google Scholar] [CrossRef] [PubMed]
- Chang, T.S. An updated review of tyrosinase inhibitors. Int. J. Mol. Sci. 2009, 10, 2440–2475. [Google Scholar] [CrossRef] [PubMed]
- Solano, F.; Briganti, S.; Picardo, M.; Ghanem, G. Hypopigmenting agents: An updated review on biological, chemical and clinical aspects. Pigment. Cell Res. 2006, 19, 550–571. [Google Scholar] [CrossRef] [PubMed]
- Couteau, C.; Coiffard, L. Overview of Skin Whitening Agents: Drugs and Cosmetic Products. Cosmetics 2016, 3, 27. [Google Scholar] [CrossRef]
- Smit, N.; Vicanova, J.; Pavel, S. The Hunt for Natural Skin Whitening Agents. Int. J. Mol. Sci. 2009, 10, 5326–5349. [Google Scholar] [CrossRef]
- Agbai, O.N.; Taylor, S.C. Melasma and Depigmentation Agents. Cosmeceuticals and Active Cosmetics. In Cosmeceuticals and Active Cosmetics; Sivamani, R.K., Jagdeo, J., Elsner, P., Maibach, H.I., Eds.; CRC Press: Boca Raton, FL, USA, 2016; pp. 343–356. [Google Scholar]
- Lee, B.D.; Eun, J.B. Optimum extraction conditions for arbutin from Asian peal peel by supercritical fluid extraction (SFE) using Box-Behnken design. J. Med. Plant Res. 2012, 6, 2348–2364. [Google Scholar]
- Lukas, B.; Schmiderer, C.; Mitteregger, U.; Novak, J. Arbutin in marjoram and oregano. Food Chem. 2010, 121, 185–190. [Google Scholar] [CrossRef]
- Kenndler, I.E.; Schwer, C.; Fritsche, B.; Pöhm, M. Determination of arbutin in Uvae-ursi folium (bearberry leaves) by capillary zone electrophoresis. J. Chromatogr. A 1990, 514, 383–388. [Google Scholar] [CrossRef]
- Pyka, A.; Bober, K.; Stolarczyk, A. Densitometric Determination of arbutin in cowberry leaves (Vaccinium vitis idaeae). Acta Pol. Pharmaceutic. Drug Res. 2007, 63, 395–400. [Google Scholar]
- Pop, C.; Vlase, L.; Tamas, M. Natural Resources Containing Arbutin. Determination of Arbutin in the Leaves of Bergenia crassifolia (L.) Fritsch. acclimated in Romania. Not. Bot. Hort. Agrobot. Cluj 2009, 37, 129–132. [Google Scholar]
- Nguyen, M.H.K.; Nguyen, H.X.; Nguyen, M.T.T.; Nguyen, N.T. Phenolic Constituents from the Heartwood of Artocapus altilis and their Tyrosinase Inhibitory Activity. Nat. Prod. Commun. 2012, 7, 185–186. [Google Scholar] [CrossRef] [PubMed]
- Soifoini, T.; Donno, D.; Jeannoda, V.; Rakoto, D.D.; Msahazi, A.; Farhat, S.M.M.; Oulam, M.Z.; Beccaro, G.L. Phytochemical Composition, Antibacterial Activity, and Antioxidant Properties of the Artocarpus altilis Fruits to Promote Their Consumption in the Comoros Islands as Potential Health-Promoting Food or a Source of Bioactive Molecules for the Food Industry. Foods 2021, 10, 2136. [Google Scholar] [CrossRef]
- Özer, Ö.; Mutlu, B.; Kıvçak, B. Antityrosinase Activity of Some Plant Extracts and Formulations Containing Ellagic Acid. Pharmaceut. Biol. 2007, 45, 519–524. [Google Scholar] [CrossRef]
- Jones, K.; Hughes, J.; Hong, M.; Jia, Q.; Orndorff, S. Modulation of melanogenesis by aloesin: A competitive inhibitor of tyrosinase. Pigment. Cell Res. 2002, 15, 335–340. [Google Scholar] [CrossRef]
- Li, X.; Guo, L.; Sun, Y.; Zhou, J.; Gu, Y.; Li, Y. Baicalein inhibits melanogenesis through activation of the ERK signaling pathway. Int. J. Mol. Med. 2010, 25, 923–927. [Google Scholar] [CrossRef]
- Zheng, Y.; Zhou, S.; Zhang, H.; Lu, Z.; Deng, R.; Feng, Y.; Li, P. Comparative Study of the Flavonoid Content in Radix Scutellaria from Different Cultivation Areas in China. Int. J. Anal. Chem. 2023, 2023, 3754549. [Google Scholar] [CrossRef]
- Eghlima, G.; Kheiry, A.; Sanikhani, M.; Hadian, J.; Aelaei, M.; Ebrahimi, S.N. Investigation of Phytochemical Variability, Antioxidant Activity and Ecological Conditions of Native Iranian Glycyrrhiza glabra L. Int. J. Hort. Sci. Technol. 2020, 7, 387–400. [Google Scholar]
- Matos, P.; Paranhos, A.; Batista, M.T.; Figueirinha, A. Synergistic Effect of DIBOA and Verbascoside from Acanthus mollis Leaf on Tyrosinase Inhibition. Int. J. Mol. Sci. 2022, 23, 13536. [Google Scholar] [CrossRef]
- Kadyrbayeva, G.; Zagórska, J.; Grzegorczyk, A.; Gaweł-Beben, K.; Strzepek-Gomółka, M.; Ludwiczuk, A.; Czech, K.; Kumar, M.; Koch, W.; Malm, A.; et al. The Phenolic Compounds Profile and Cosmeceutical Significance of Two Kazakh Species of Onions: Allium galanthum and A. turkestanicum. Molecules 2021, 26, 5491. [Google Scholar] [CrossRef] [PubMed]
- Fawzi Mahomoodally, M.; Picot-Allain, M.C.N.; Zengin, G.; Llorent-Martínez, E.J.; Abdullah, H.H.; Ak, G.; Senkardes, I.; Chiavaroli, A.; Menghini, L.; Recinella, L.; et al. Phytochemical Analysis, Network Pharmacology and in Silico Investigations on Anacamptis pyramidalis Tuber Extracts. Molecules 2020, 25, 2422. [Google Scholar] [CrossRef] [PubMed]
- Chaikhong, K.; Chumpolphant, S.; Rangsinth, P.; Sillapachaiyaporn, C.; Chuchawankul, S.; Tencomnao, T.; Prasansuklab, A. Antioxidant and Anti-Skin Aging Potential of Selected Thai Plants: In Vitro Evaluation and In Silico Target Prediction. Plants 2023, 12, 65. [Google Scholar] [CrossRef] [PubMed]
- Zeitoun, H.; Khan, Z.; Banerjee, K.; Salameh, D.; Lteif, R. Antityrosinase Activity of Combretum micranthum, Euphorbia hirta and Anacardium occidentale Plants: Ultrasound Assisted Extraction Optimization and Profiling of Associated Predominant Metabolites. Molecules. 2020, 25, 2684. [Google Scholar] [CrossRef]
- Anh, L.H.; Quan, N.V.; Lam, V.Q.; Iuchi, Y.; Takami, A.; Teschke, R.; Xuan, T.D. Antioxidant, Anti-tyrosinase, Anti-α-amylase, and Cytotoxic Potentials of the Invasive Weed Andropogon virginicus. Plants 2021, 10, 69. [Google Scholar] [CrossRef]
- Lee, J.-H.; Mei, H.-C.; Kuo, I.-C.; Lee, T.-H.; Chen, Y.-H.; Lee, C.-K. Characterizing Tyrosinase Modulators from the Roots of Angelica keiskei Using Tyrosinase Inhibition Assay and UPLC-MS/MS as the Combinatorial Novel Approach. Molecules 2019, 24, 3297. [Google Scholar] [CrossRef]
- Ilgün, S.; Karatoprak, G.S.; Polat, D.Ç.; ¸Safak, E.K.; Yıldız, G.; Küpeli Akko, E.; Sobarzo-Sánchez, E. Phytochemical Composition and Biological Activities of Arctium minus (Hill) Bernh.: A Potential Candidate as Antioxidant, Enzyme Inhibitor, and Cytotoxic Agent. Antioxidants 2022, 11, 1852. [Google Scholar] [CrossRef]
- Suroowan, S.; Llorent-Martínez, E.J.; Zengin, G.; Buskaran, K.; Fakurazi, S.; Abdalla, A.N.; Khalid, A.; Le Van, B.; Mahomoodally, M.F. Unveiling the Antioxidant, Clinical Enzyme Inhibitory Properties and Cytotoxic Potential of Tambourissa peltata Baker—An Understudied Endemic Plant. Molecules 2023, 28, 599. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.-Q.; Xu, C.-Y.; Liang, F.-Y.; Jin, P.-C.; Qian, Z.-Y.; Luo, Z.-S.; Qin, R.-G. Selecting and Characterizing Tyrosinase InhibiTors from Atractylodis macrocephalae Rhizoma Based on Spectrum-Activity Relationship and Molecular Docking. J. Anal. Methods Chem. 2021, 2021, 5596463. [Google Scholar] [CrossRef]
- del Pilar Fernández-Poyatos, M.; Ruiz-Medina, A.; Zengin, G.; Llorent-Martínez, E.J. Phenolic Characterization, Antioxidant Activity, and Enzyme Inhibitory Properties of Berberis thunbergii DC. Leaves: A Valuable Source of Phenolic Acids. Molecules 2019, 24, 4171. [Google Scholar] [CrossRef] [PubMed]
- Pandey, B.P.; Pradhan, S.P.; Adhikari, K.; Nepal, S. Bergenia pacumbis from Nepal, an astonishing enzymes inhibitor. BMC Complem. Med. Ther. 2020, 20, 198–209. [Google Scholar] [CrossRef] [PubMed]
- Dirar, A.M.; Wada, M.; Watanabe, T.; Devkota, H.P. Phenolic Compounds from the Aerial Parts of Blepharis linariifolia Pers. and Their Free Radical Scavenging and Enzyme Inhibitory Activities. Medicines 2019, 6, 113. [Google Scholar] [CrossRef]
- Luo, Y.; Wang, J.; Li, S.; Wu, Y.; Wang, Z.; Chen, S.; Chen, H. Discovery and identification of potential anti-melanogenic active constituents of Bletilla striata by zebrafish model and molecular docking. BMC Complem. Med. Ther. 2022, 22, 9. [Google Scholar] [CrossRef] [PubMed]
- Dall’Acqua, S.; Sinan, K.I.; Ferrarese, I.; Sut, S.; Bene, K.; Mahomoodally, M.F.; Sadeer, N.B.; Ak, G.; Zengin, G. Chromatographic Separation of Breynia retusa (Dennst.) Alston Bark, Fruit and Leaf Constituents from Bioactive Extracts. Molecules 2020, 25, 5537. [Google Scholar] [CrossRef]
- Mahomoodally, M.F.; Jugreet, S.; Sinan, K.I.; Zengin, G.; Ak, G.; Ceylan, R.; Jekő, J.; Cziáky, Z.; Angelini, P.; Angeles Flores, G.; et al. Pharmacological Potential and Chemical Characterization of Bridelia ferruginea Benth.—A Native Tropical African Medicinal Plant. Antibiotics 2021, 10, 223. [Google Scholar] [CrossRef]
- Placines, C.; Castañeda-Loaiza, V.; Rodrigues, M.J.; Pereira, C.G.; Stefanucci, A.; Mollica, A.; Zengin, G.; Llorent-Martínez, E.J.; Castilho, P.C.; Custódio, L. Phenolic Profile, Toxicity, Enzyme Inhibition, In Silico Studies, and Antioxidant Properties of Cakile maritima Scop. (Brassicaceae) from Southern Portugal. Plants 2020, 9, 142. [Google Scholar] [CrossRef]
- Yeom, S.-H.; Gam, D.-H.; Kim, J.-H.; Kim, J.-W. Development of Ultrasound-Assisted Extraction to Produce Skin-Whitening and anti-Wrinkle Substances from Safflower Seed. Molecules 2022, 27, 1296. [Google Scholar] [CrossRef]
- Viet, T.D.; Xuan, T.D.; Anh, L.H. α-Amyrin and β-Amyrin Isolated from Celastrus hindsii Leaves and Their Antioxidant, Anti-Xanthine Oxidase, and Anti-Tyrosinase Potentials. Molecules 2021, 26, 7248. [Google Scholar] [CrossRef]
- Lou, Y.; Xu, T.; Cao, H.; Zhao, Q.; Zhang, P.; Shu, P. Natural Antioxidants, Tyrosinase and Acetylcholinesterase Inhibitors from Cercis glabra Leaves. Molecules 2022, 27, 8667. [Google Scholar] [CrossRef]
- Rodrigues, M.J.; Custódio, L.; Mecha, D.; Zengin, G.; Cziáky, Z.; Sotkó, G.; Pereira, C.G. Nutritional and Phyto-Therapeutic Value of the Halophyte Cladium mariscus L. (Pohl.): A Special Focus on Seeds. Plants 2022, 11, 2910. [Google Scholar] [CrossRef] [PubMed]
- Van Quan, N.; Xuan, T.D.; Anh, L.H.; Tran, H.-D. Bio-Guided Isolation of Prospective Bioactive Constituents from Roots of Clausena indica (Dalzell) Oliv. Molecules 2019, 24, 4442. [Google Scholar] [CrossRef]
- Anwar, S.; Faisal Nadeem, M.; Pervaiz, I.; Khurshid, U.; Akmal, N.; Aamir, K.; Haseeb ur Rehman, M.; Almansour, K.; Alshammari, F.; Shaikh, M.F.; et al. A comprehensive phytochemical, biological, and toxicological studies of roots and aerial parts of Crotalaria burhia Buch.-Ham: An important medicinal plant. Front. Plant Sci. 2022, 13, 988352. [Google Scholar] [CrossRef] [PubMed]
- Dall’Acqua, S.; Sinan, K.I.; Sut, S.; Ferrarese, I.; Etienne, O.K.; Mahomoodally, M.F.; Lobine, D.; Zengin, G. Evaluation of Antioxidant and Enzyme Inhibition Properties of Croton hirtus L’Hér. Extracts Obtained with Different Solvents. Molecules 2021, 26, 1902. [Google Scholar] [CrossRef] [PubMed]
- Oh, H.-N.; Park, D.-H.; Park, J.-Y.; Song, S.-Y.; Lee, S.-H.; Yoon, G.; Moon, H.-S.; Oh, D.-S.; Rhee, S.-H.; Im, E.-O.; et al. Tyrosinase Inhibition Antioxidant Effect and Cytotoxicity Studies of the Extracts of Cudrania tricuspidata Fruit Standardized in Chlorogenic Acid. Molecules 2019, 24, 3266. [Google Scholar] [CrossRef]
- Zengin, G.; Cádiz-Gurrea, M.d.l.L.; Fernández-Ochoa, Á.; Leyva-Jiménez, F.J.; Carretero, A.S.; Momotko, M.; Yildiztugay, E.; Karatas, R.; Jugreet, S.; Mahomoodally, M.F.; et al. Selectivity Tuning by Natural Deep Eutectic Solvents (NADESs) for Extraction of Bioactive Compounds from Cytinus hypocistis—Studies of Antioxidative, Enzyme-Inhibitive Properties and LC-MS Profiles. Molecules 2022, 27, 5788. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.-C.; Su, S.-H.; Huang, J.-C.; Chao, C.-Y.; Sung, P.-J.; Chen, Y.-F.; Ko, H.-H.; Kuo, Y.-H. Tyrosinase Inhibitors Derived from Chemical Constituents of Dianella ensifolia. Plants 2022, 11, 2142. [Google Scholar] [CrossRef]
- Sagara, T.; Sugimoto, S.; Yamano, Y.; Nehira, T.; Masuda, K.; Otsuka, H.; Matsunam, K. Isolation of Three New Diterpenes from Dodonaea viscosa. Chem. Pharm. Bull. 2021, 69, 40–47. [Google Scholar] [CrossRef]
- Carradori, S.; Cairone, F.; Garzoli, S.; Fabrizi, G.; Iazzetti, A.; Giusti, A.M.; Menghini, L.; Uysal, S.; Ak, G.; Zengin, G.; et al. Phytocomplex Characterization and Biological Evaluation of Powdered Fruits and Leaves from Elaeagnus angustifolia. Molecules 2020, 25, 2021. [Google Scholar] [CrossRef]
- Sabera, F.R.; Ashour, R.M.; El-Halawanya, A.M.; Mahomoodally, M.F.; Akd, G.; Zengind, G.; Mahrous, E.A. Phytochemical profile, enzyme inhibition activity and molecular docking analysis of Feijoa sellowiana O. Berg. J. Enzym. Inhib. Med. Chem. 2021, 36, 618–626. [Google Scholar] [CrossRef]
- Shrestha, S.S.; Sut, S.; Ferrarese, I.; Di Marco, S.B.; Zengin, G.; De Franco, M.; Pant, D.R.; Mahomoodally, M.F.; Ferri, N.; Biancorosso, N.; et al. Himalayan Nettle Girardinia diversifolia as a Candidate Ingredient for Pharmaceutical and Nutraceutical Applications—Phytochemical Analysis and In Vitro Bioassays. Molecules 2020, 25, 1563. [Google Scholar] [CrossRef]
- Popoola, O.K.; Marnewick, J.L.; Iwuoha, E.I.; Hussein, A.A. Methoxylated Flavonols and ent-Kaurane Diterpenes from the South African Helichrysum rutilans and Their Cosmetic Potential. Plants 2023, 12, 2870. [Google Scholar] [CrossRef]
- Ozntamar-Pouloglou, K.-M.; Cheilari, A.; Zengin, G.; Graikou, K.; Ganos, C.; Karikas, G.-A.; Chinou, I. Heliotropium procubens Mill: Taxonomic Significance and Characterization of Phenolic Compounds via UHPLC–HRMS-In Vitro Antioxidant and Enzyme Inhibitory Activities. Molecules 2023, 28, 1008. [Google Scholar] [CrossRef]
- Arshad, A.; Ahemad, S.; Saleem, H.; Saleem, M.; Zengin, G.; Abdallah, H.H.; Tousif, M.I.; Ahemad, N.; Fawzi Mahomoodally, M. RP-UHPLC-MS Chemical Profiling, Biological and In Silico Docking Studies to Unravel the Therapeutic Potential of Heliotropium crispum Desf. as a Novel Source of Neuroprotective Bioactive Compounds. Biomolecules 2021, 11, 53. [Google Scholar] [CrossRef] [PubMed]
- Lim, W.Y.; Chan, E.W.C.; Phan, C.W.; Wong, C.W. Tyrosinase Inhibiting Extracts from Coastal Plants as Potential Additives in Skin Whitening Formulations. Curr. Appl. Sci. Technol. 2021, 21, 481–494. [Google Scholar]
- Sut, S.; Dall’Acqua, S.; Zengin, G.; Senkardes, I.; Uba, A.I.; Bouyahya, A.; Aktumsek, A. Novel Signposts on the Road from Natural Sources to Pharmaceutical Applications: A Combinative Approach between LC-DAD-MS and Offline LC-NMR for the Biochemical Characterization of Two Hypericum Species (H. montbretii and H. origanifolium). Plants 2023, 12, 648. [Google Scholar] [CrossRef] [PubMed]
- Yehia, S.M.; Ayoub, I.M.; Watanabe, M.; Devkota, H.P.; Singab, A.N.B. Metabolic profiling, antioxidant, and enzyme inhibition potential of Iris pseudacorus L. from Egypt and Japan: A comparative study. Sci Rep. 2023, 13, 5233. [Google Scholar] [CrossRef] [PubMed]
- Zengin, G.; Mahomoodally, M.F.; Sinan, K.I.; Ak, G.; Etienne, O.K.; Sharmeen, J.B.; Brunetti, L.; Leone, S.; Di Simone, S.C.; Recinella, L.; et al. Chemical Composition and Biological Properties of Two Jatropha Species: Different Parts and Different Extraction Methods. Antioxidants 2021, 10, 792. [Google Scholar] [CrossRef]
- Baysal, I.; Ekizoglu, M.; Ertas, A.; Temiz, B.; Agalar, H.G.; Yabanoglu-Ciftci, S.; Temel, H.; Ucar, G.; Turkmenoglu, F.P. Identification of Phenolic Compounds by LC-MS/MS and Evaluation of Bioactive Properties of Two Edible Halophytes: Limonium effusum and L. sinuatum. Molecules 2021, 26, 4040. [Google Scholar] [CrossRef]
- Saive, M.; Genva, M.; Istasse, T.; Frederich, M.; Maes, C.; Fauconnier, M.-L. Identification of a Proanthocyanidin from Litchi chinensis Sonn. Root with Anti-Tyrosinase and Antioxidant Activity. Biomolecules 2020, 10, 1347. [Google Scholar] [CrossRef]
- Fan, Z.; Li, L.; Bai, X.; Hhang, H.; Liu, Q.; Zhang, H.; Fu, Y.; Moyo, R. Extraction optimization, antioxidant activity, and tyrosinase inhibitory capacity of polyphenols from Lonicera japonica. Food Sci. Nutr. 2019, 7, 1786–1794. [Google Scholar] [CrossRef] [PubMed]
- Srisupap, S.; Chaicharoenpong, C. In vitro antioxidant and antityrosinase activities of Manilkara kauki. Acta Pharm. 2021, 71, 153–162. [Google Scholar] [CrossRef] [PubMed]
- Taviano, M.F.; Miceli, N.; Acquaviva, R.; Malfa, G.A.; Ragusa, S.; Giordano, D.; Cásedas, G.; Les, F.; López, V. Cytotoxic, Antioxidant, and Enzyme Inhibitory Properties of the Traditional Medicinal Plant Matthiola incana (L.) R. Br. Biology 2020, 9, 163. [Google Scholar] [CrossRef] [PubMed]
- He, R.-J.; Li, J.; Huang, Y.-L.; Wang, Y.-F.; Yang, B.-Y.; Liu, Z.-B.; Ge, L.; Yang, K.-D.; Li, D.-P. Structural Characterization and Assessment of Anti-Inflammatory and Anti-Tyrosinase Activities of Polyphenols from Melastoma normale. Molecules 2021, 26, 3913. [Google Scholar] [CrossRef]
- Kim, J.; Hong, S.-C.; Lee, E.H.; Lee, J.W.; Yang, S.-H.; Kim, J.-C. Preventive Effect of M. cochinchinensis on Melanogenesis via Tyrosinase Activity Inhibition and p-PKC Signaling in Melan-A Cell. Nutrients 2021, 13, 3894. [Google Scholar] [CrossRef]
- Ali, J.S.; Saleem, H.; Mannan, A.; Zengin, G.; Mahomoodally, M.F.; Locatelli, M.; Abidin, S.A.Z.; Ahemad, N.; Zia, M. Metabolic fingerprinting, antioxidant characterization, and enzyme-inhibitory response of Monotheca buxifolia (Falc.) A. DC. extracts. BMC Complement. Med. Ther. 2020, 20, 313. [Google Scholar] [CrossRef]
- Istifli, E.S. Chemical Composition, Antioxidant and Enzyme Inhibitory Activities of Onosma bourgaei and Onosma trachytricha and in Silico Molecular Docking Analysis of Dominant Compounds. Molecules 2021, 26, 2981. [Google Scholar] [CrossRef]
- Zengin, G.; Fernández-Ochoa, Á.; Cádiz-Gurrea, M.d.l.L.; Leyva-Jiménez, F.J.; Segura-Carretero, A.; Elbasan, F.; Yildiztugay, E.; Malik, S.; Khalid, A.; Abdalla, A.N.; et al. Phytochemical Profile and Biological Activities of Different Extracts of Three Parts of Paliurus spina-christi: A Linkage between Structure and Ability. Antioxidants 2023, 12, 255. [Google Scholar] [CrossRef]
- Elloumi, W.; Maalej, A.; Ortiz, S.; Michel, S.; Chamkha, M.; Boutefnouchet, S.; Sayadi, S. Pistacia lentiscus L. Distilled Leaves as a Potential Cosmeceutical Ingredient: Phytochemical Characterization, Transdermal Diffusion, and Anti-Elastase and Anti-Tyrosinase Activities. Molecules 2022, 27, 855. [Google Scholar] [CrossRef]
- Fonseca-Hernández, D.; Lugo-Cervantes, E.D.C.; Escobedo-Reyes, A.; Mojica, L. Black Bean (Phaseolus vulgaris L.) Polyphenolic Extract Exerts Antioxidant and Antiaging Potential. Molecules 2021, 26, 6716. [Google Scholar] [CrossRef]
- Di Petrillo, A.; González-Paramás, A.M.; Rosa, A.; Ruggiero, V.; Boylan, F.; Kumar, A.; Pintus, F.; Santos-Buelga, C.; Fais, A.; Era, B. Chemical composition and enzyme inhibition of Phytolacca dioica L. seeds extracts. J. Enzyme Inhib. Med. Chem. 2019, 34, 519–527. [Google Scholar] [CrossRef] [PubMed]
- Etsassala, N.G.E.R.; Waryo, T.; Popoola, O.K.; Adeloye, A.O.; Iwuoha, E.I.; Hussein, A.A. Electrochemical Screening and Evaluation of Lamiaceae Plant Species from South Africa with Potential Tyrosinase Activity. Sensors 2019, 19, 1035. [Google Scholar] [CrossRef]
- Xiong, Y.; Kim, H.K.; Özer, Ö.Ç.; van Duijn, B.; Korthout, H.A.A.J.; Zi, L.; Cai, A. Synergistic Inhibiting Effect of Phytochemicals in Rheum palmatum on Tyrosinase Based on Metabolomics and Isobologram Analyses. Molecules 2023, 28, 944. [Google Scholar] [CrossRef] [PubMed]
- Chiavaroli, A.; Sinan, K.I.; Zengin, G.; Mahomoodally, M.F.; Sadeer, N.B.; Etienne, O.K.; Cziáky, Z.; Jek, J.; Glamoclija, J.; SokoviĆ, M.; et al. Identification of Chemical Profiles and Biological Properties of Rhizophora racemosa G. Mey. Extracts Obtained by Different Methods and Solvents. Antioxidants 2020, 9, 533. [Google Scholar] [CrossRef] [PubMed]
- Sabitov, A.; Gaweł-Beben, K.; Sakipova, Z.; Strzepek-Gomółka, M.; Hoian, U.; Satbayeva, E.; Głowniak, K.; Ludwiczuk, A. Rosa platyacantha Schrenk from Kazakhstan—Natural Source of Bioactive Compounds with Cosmetic Significance. Molecules 2021, 26, 2578. [Google Scholar] [CrossRef]
- Desmiaty, Y.; Hanafi, M.; Saputri, F.C.; Elya, B.; Rifai, E.A.; Syahdi, R.R. Two triterpenoids from Rubus fraxinifolius leaves and their tyrosinase and elastase inhibitory activities. Sci. Rep. 2021, 11, 20452. [Google Scholar] [CrossRef]
- Dall’Acqua, S.; Sut, S.; Sinan, K.I.; Zengin, G.; Ferrarese, I.; Peron, G.; Yildiztugay, E.; Picot-Allain, C.; Mahomoodally, M.F. An Integrated NMR, LC-DAD-MS, LC-QTOF Metabolomic Characterization of Sartoria hedysaroides: Correlation of Antioxidant and Enzyme Inhibitory Activity with Chemical Composition by Multivariate Data Analysis. Antioxidants 2022, 11, 110. [Google Scholar] [CrossRef] [PubMed]
- Zagórska-Dziok, M.; Wójciak, M.; Ziemlewska, A.; Nizioł-Łukaszewska, Z.; Hoian, U.; Klimczak, K.; Szczepanek, D.; Sowa, I. Evaluation of the Antioxidant, Cytoprotective and Antityrosinase Effects of Schisandra chinensis Extracts and Their Applicability in Skin Care Product. Molecules 2022, 27, 8877. [Google Scholar] [CrossRef]
- Sinan, K.I.; Yagi, S.; Llorent-Martínez, E.J.; Ruiz-Medina, A.; Gordo-Moreno, A.I.; Stefanucci, A.; Mollica, A.; Bene, K.; Zengin, G. Understanding the Chemical Composition and Biological Activities of Different Extracts of Secamone afzelii Leaves: A Potential Source of Bioactive Compounds for the Food Industry. Molecules 2023, 28, 3678. [Google Scholar] [CrossRef]
- Parndaeng, K.; Pitakbut, T.; Wattanapiromsakul, C.; Hwang, J.S.; Udomuksorn, W.; Dej-adisai, S. Chemical Constituents from Streblus taxoides Wood with Their Antibacterial and Antityrosinase Activities Plus in Silico Study. Antibiotics 2023, 12, 319. [Google Scholar] [CrossRef]
- Aziz, M.; Ahmad, S.; Khurshid, U.; Pervaiz, I.; Lodhi, A.H.; Jan, N.; Khurshid, S.; Arshad, M.A.; Ibrahim, M.M.; Mersal, G.A.M.; et al. Comprehensive Biological Potential, Phytochemical Profiling Using GC-MS and LC-ESI-MS, and In-Silico Assessment of Strobilanthes glutinosus Nees: An Important Medicinal Plant. Molecules 2022, 27, 6885. [Google Scholar] [CrossRef]
- Oh, K.-E.; Shin, H.; Lee, M.K.; Park, B.; Lee, K.Y. Characterization and Optimization of the Tyrosinase Inhibitory Activity of Vitis amurensis Root Using LC-Q-TOF-MS Coupled with a Bioassay and Response Surface Methodology. Molecules 2021, 26, 446. [Google Scholar] [CrossRef] [PubMed]
- Pintatum, A.; Laphookhieo, S.; Logie, E.; Berghe, W.V.; Maneera, W. Chemical Composition of Essential Oils from Different Parts of Zingiber kerrii Craib and Their Antibacterial, Antioxidant, and Tyrosinase Inhibitory Activities. Biomolecules 2020, 10, 228. [Google Scholar] [CrossRef]
- Tomczyk, M.; Ceylan, O.; Locatelli, M.; Tartaglia, A.; Ferrone, V.; Sarikurkcu, C. Ziziphora taurica subsp. taurica: Analytical Characterization and Biological Activities. Biomolecules 2019, 9, 367. [Google Scholar] [CrossRef]
- Ali, B.; Al-Wabel, N.A.; Shams, S.; Ahamad, A.; Khan, S.A.; Anwar, F. Essential oils used in aromatherapy: A systemic review. Asian Pac. J. Trop. Biomed. 2015, 5, 601–611. [Google Scholar] [CrossRef]
- Elshafie, H.S.; Camele, I. An Overview of the Biological Effects of Some Mediterranean Essential Oils on Human Health. Biomed. Res. Int. 2017, 2017, 9268468. [Google Scholar] [CrossRef]
- Michalak, M. Aromatherapy and methods of applying essential oils. Arch. Physiother. Glob. Res. 2018, 22, 25–31. [Google Scholar]
- Guzmán, E.; Lucia, A. Essential Oils and Their Individual Components in Cosmetic Products. Cosmetics 2021, 8, 114. [Google Scholar] [CrossRef]
- Sharmeen, J.B.; Mahomoodally, F.M.; Zengin, G.; Maggi, F. Essential Oils as Natural Sources of Fragrance Compounds for Cosmetics and Cosmeceuticals. Molecules 2021, 26, 666. [Google Scholar] [CrossRef]
- Śmigielski, K.; Raj, A.; Krosowiak, K.; Gruska, R. Chemical Composition of the Essential Oil of Lavandula angustifolia Cultivated in Poland. J. Essent. Oil Bear. Plants 2009, 12, 338–347. [Google Scholar] [CrossRef]
- Khan, M.; Khan, S.T.; Khan, N.A.; Mahmood, A.; Al-Kedhairy, A.A.; Alkhathlan, H.Z. The composition of the essential oil and aqueous distillate of Origanum vulgare L. growing in Saudi Arabia and evaluation of their antibacterial activity. Arabian J. Chem. 2018, 11, 1189–1200. [Google Scholar] [CrossRef]
- Shabnum, S.; Wagay, M.G. Essential Oil Composition of Thymus vulgaris L. and their Uses. J. Res. Develop. 2011, 11, 23617694. [Google Scholar]
- Golparvar, A.R.; Hadipanah, A. Chemical compositions of the essential oil from peppermint (Mentha piperita L.) cultivated in Isfahan conditions. J. Herb. Drugs 2013, 4, 75–80. [Google Scholar]
- Wesołowska, A.; Jadczak, D.; Grzeszczuk, M. Essential oil composition of hyssop (Hyssopus officinalis L.) cultivated in north-western Poland. Herba Pol. 2020, 56, 57–65. [Google Scholar]
- Acimovic, M.; Tesevic, V.; Todosijevic, M.; Djisalov, J.; Oljaca, S. Compositional characteristics of the essential oil of Pimpinella anisum and Foeniculum vulgare grown in Serbia. Botanica Serbica 2015, 39, 9–14. [Google Scholar]
- Jiang, Z.T.; Sun, M.L.; Li, R.; Wang, Y. Essential oil Composition of Chinese Caraway (Carum carvi L.). J. Essen. Oil Bear. Pl. 2011, 14, 379–382. [Google Scholar] [CrossRef]
- Louiza, H.; Salah, M.; Malika, B. Chemical composition of Citrus limon (Eureka variety) essential oil and evaluation of its antioxidant and antibacterial activities. Afr. J. Biotechnol. 2018, 17, 356–361. [Google Scholar] [CrossRef]
- Deng, W.; Liu, K.; Cao, S.; Sun, J.; Zhong, B.; Chun, J. Chemical Composition, Antimicrobial, Antioxidant, and Antiproliferative Properties of Grapefruit Essential Oil Prepared by Molecular Distillation. Molecules 2020, 25, 217. [Google Scholar] [CrossRef]
- Chalchat, J.; Garry, R. Chemical composition of the leaf oil of Verbena officinalis L. J. Essen. Oil Res. 1996, 8, 419–420. [Google Scholar] [CrossRef]
- Chakraborty, A.; Sankaran, V.; Ramar, M.; Chellappan, D.R. Chemical analysis of leaf essential oil of Cinnamomum verum from Palni hills, Tamil Nadu. J. Chem. Pharm. Sci. 2015, 8, 476–479. [Google Scholar]
- Sadiki, F.Z.; El Idrissi, M. Chemical composition of essential oil of Anthemis nobilis L. flowers from Morocco. Appl. J. Envir. Eng. Sci. 2019, 5, 342–348. [Google Scholar]
- Almas, I.; Innocent, E.; Machumi, F.; Kisinza, W. Chemical Composition of Essential Oils from Eucalyptus globulus and Eucalyptus maculata Grown in Tanzania. Sci. Afr. 2021, 12, e00758. [Google Scholar] [CrossRef]
- Borotová, P.; Galovicová, L.; Vukovic, N.L.; Vukic, M.; Tvrdá, E.; Kacániová, M. Chemical and Biological Characterization of Melaleuca alternifolia Essential Oil. Plants 2022, 11, 558. [Google Scholar] [CrossRef] [PubMed]
- Hatami, T.; Johner, J.C.F.; Zabot, G.L.; Meireles, M.A.A. Supercritical fluid extraction assisted by cold pressing from clove buds: Extraction performance, volatile oil composition, and economic evaluation. J. Supercrit. Fluids 2019, 144, 39–47. [Google Scholar] [CrossRef]
- Sharopov, F.S.; Zhang, H.; Setzer, W.N. Composition of geranium (Pelargonium graveolens) essential oil from Tajikistan. Am. J. Essent. Oils Nat. Prod. 2014, 2, 13–16. [Google Scholar]
- Khalil, R.; Li, Z.G. Antimicrobial activity of essential oil of Salvia officinalis L. collected in Syria. Afr. J. Biotechnol. 2011, 10. [Google Scholar] [CrossRef]
- Dweck, A.C. Natural ingredients for colouring and styling. Int. J. Cosmet. Sci. 2002, 24, 287–302. [Google Scholar] [CrossRef] [PubMed]
- Yusuf, M.; Shabbir, M.; Mohammad, F. Natural Colorants: Historical, Processing and Sustainable Prospects. Nat. Prod. Bioprospect. 2017, 7, 123–145. [Google Scholar] [CrossRef] [PubMed]
- Mohana Priya, M.; Chidambara Rajan, P.; Lavanya, M. Use of natural pigments as colorants in cosmetics—A review. J. Emerg. Technol. Innov. Res. 2020, 7, 907–917. [Google Scholar]
- Delgado-Vargas, F.; Jiménez, A.R.; Paredes-López, O. Natural pigments: Carotenoids, anthocyanins, and betalains-characteristics, biosynthesis, processing, and stability. Crit. Rev. Food Sci. Nutr. 2000, 40, 173–289. [Google Scholar] [CrossRef]
- Michalak, M.; Glinka, R. Sources of vegetable dyes and their use in cosmetology. Pol. J. Cosmetol. 2017, 20, 196–205. [Google Scholar]
- Bhalekar, O.S.; Waghmare, S.A.; Kamble, H.V.; Dhamal, K.S. Natural colourants and dyes from plant origin. Int. J. Sci. Res. Eng. Dev. 2022, 5, 537–549. [Google Scholar]
- Brudzyńska, P.; Sionkowska, A.; Grisel, M. Plant-Derived Colorants for Food, Cosmetic and Textile Industries: A Review. Materials 2021, 14, 3484. [Google Scholar] [CrossRef]
- Cui, H.; Xie, W.; Hua, Z.; Cao, L.; Xiong, Z.; Tang, Y.; Yuan, Z. Recent Advancements in Natural Plant Colorants Used for Hair Dye Applications: A Review. Molecules 2022, 27, 8062. [Google Scholar] [CrossRef]
- Chandrasekar, R.; Sivagami, B.; Swapna, D. Herbal Cosmetics an Overview. Int. J. Pharm. Res. Rev. 2016, 5, 1–20. [Google Scholar]
- Prabhu, K.H.; Bhute, A.S. Plant based natural dyes and mordnats: A Review. J. Nat. Prod. Plant Resour. 2012, 2, 649–664. [Google Scholar]
- Morel, S.; Sapino, S.; Peira, E.; Chirio, D.; Gallarate, M. Regulatory Requirements for Exporting Cosmetic Products to Extra-EU Countries. Cosmetics 2023, 10, 62. [Google Scholar] [CrossRef]
- Sopyan, I.; Gozali, D.; Tiassetiana, S. Formulation of tomato extracts (Solanum lycopersicum L.) as a sunscreen lotion. Natl. J. Physiol. Pharm. Pharmacol. 2017, 8, 453–458. [Google Scholar] [CrossRef]
- Maheshwar, G.H.; Patil, B.S.; Prashant, D. Comparative sun protection factor determination of fresh fruits extract of cucumber vs marketed cosmetic formulation. Res. J. Pharm. Biol. Chem. Sci. 2010, 1, 55–59. [Google Scholar]
- Ortel, B.; Gange, R.W. An Action Spectrum for the Elicitation of Erythema in Skin persistently Sensitized by Photobound 8-Methoxypsoralen. J. Investig. Dermatol. 1990, 94, 781–785. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.C.; Liu, K.C.; Chiou, Y.L. Melanogenesis of murine melanoma cells induced by hesperetin, a Citrus hydrolysate-derived flavonoid. Food Chem. Toxicol. 2012, 50, 653–659. [Google Scholar] [CrossRef]
- Wang, H.Z.; Zhang, Y.; Xie, L.P.; Yu, X.Y.; Zhang, R.Q. Effects of genistein and daidzein on the cell growth, cell cycle, and differentiation of human and murine melanoma cells. J. Nutr. Biochem. 2002, 13, 421–426. [Google Scholar] [CrossRef]
- Kim, D.-S.; Park, S.-H.; Kwon, S.-B.; Li, K.; Youn, S.-W.; Park, K.-C. (-)-Epigallocatechin-3-gallate and hinokitiol reduce melanin synthesis via decreased MITF production. Arch. Pharm. Res. 2004, 27, 334–339. [Google Scholar] [CrossRef]
- Ye, Y.; Chou, G.-X.; Wang, H.; Chu, J.-H.; Yu, Z.-L. Flavonoids, apigenin and icariin exert potent melanogenic activities in murine B16 melanoma cells. Phytomedicine 2010, 18, 32–35. [Google Scholar] [CrossRef] [PubMed]
- An, S.M.; Kim, H.J.; Kim, J.-E.; Boo, Y.C. Flavonoids, taxifolin and luteolin attenuate cellular melanogenesis despite increasing tyrosinase protein levels. Phytother. Res. 2008, 22, 1200–1207. [Google Scholar] [CrossRef] [PubMed]
- Takekoshi, S.; Matsuzaki, K.; Kitatani, K. Quercetin stimulates melanogenesis in hair follicle melanocyte of the mouse. Tokai J. Exp. Clin. Med. 2013, 38, 129–134. [Google Scholar]
- Fujii, T.; Saito, M. Inhibitory effect of quercetin isolated from rose hip (Rosa canina L.) against melanogenesis by mouse melanoma cells. Biosci. Biotechnol. Biochem. 2009, 73, 1989–1993. [Google Scholar] [CrossRef]
- Magalhães, W.V.; Baby, A.R.; Robles Velasco, M.V.; Mendes Pereira, D.M.; Kaneko, T.M. Patenting in the cosmetic sector: Study of the use of herbal extracts. Braz. J. Pharm. Sci. 2011, 47, 693–700. [Google Scholar] [CrossRef]
- Yapar, E.A. Intellectual Property and Patent in Cosmetics. Marmara Pharm. J. 2017, 21, 419–424. [Google Scholar] [CrossRef]
- Césara, F.C.S.; Carnevale Netob, F.; Portoc e Patrícia, G.S.; Camposa, M.B.G.M. Patent analysis: A look at the innovative nature of plant-based cosmetics. Quim. Nova 2017, 40, 840–847. [Google Scholar] [CrossRef]
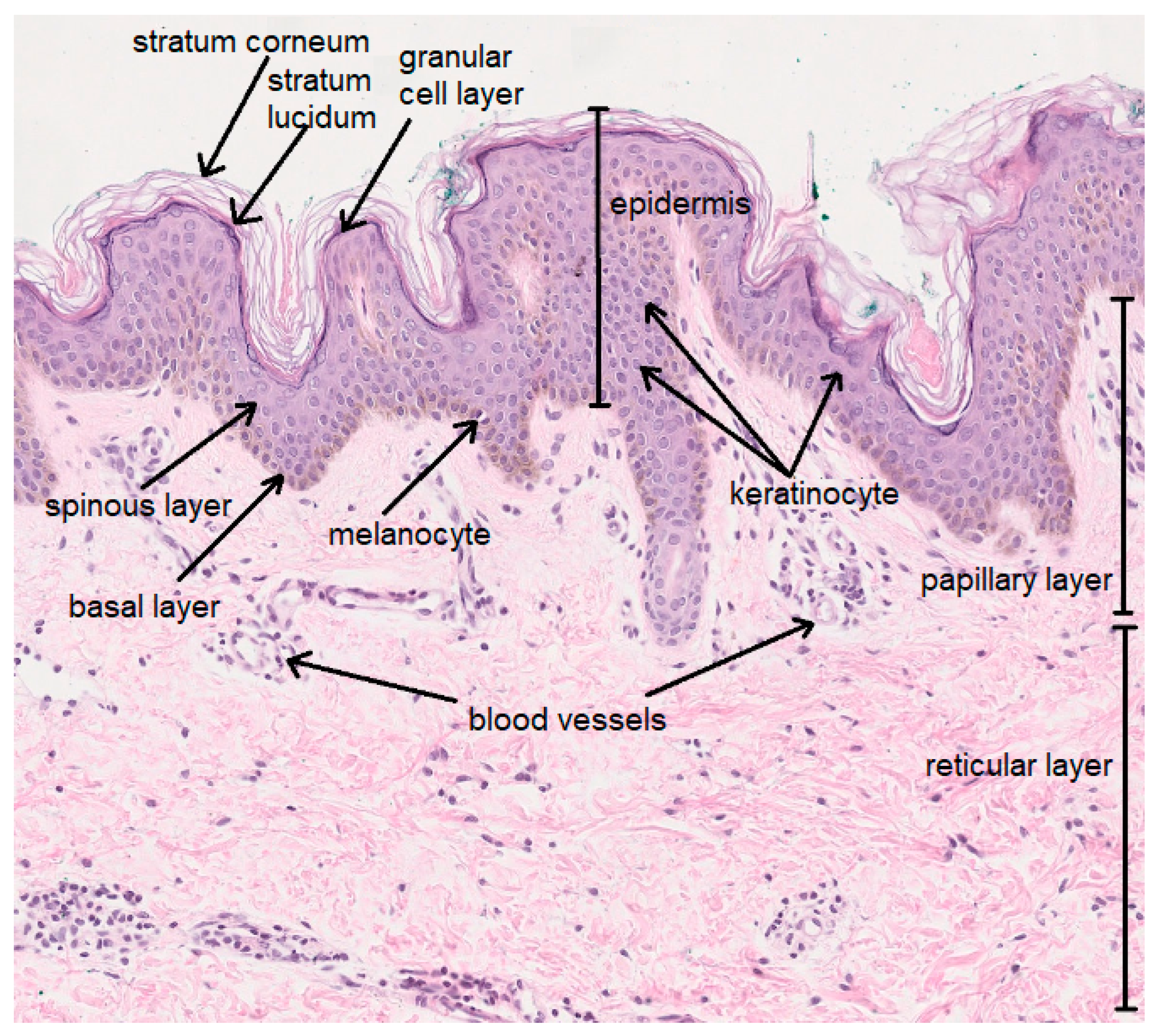
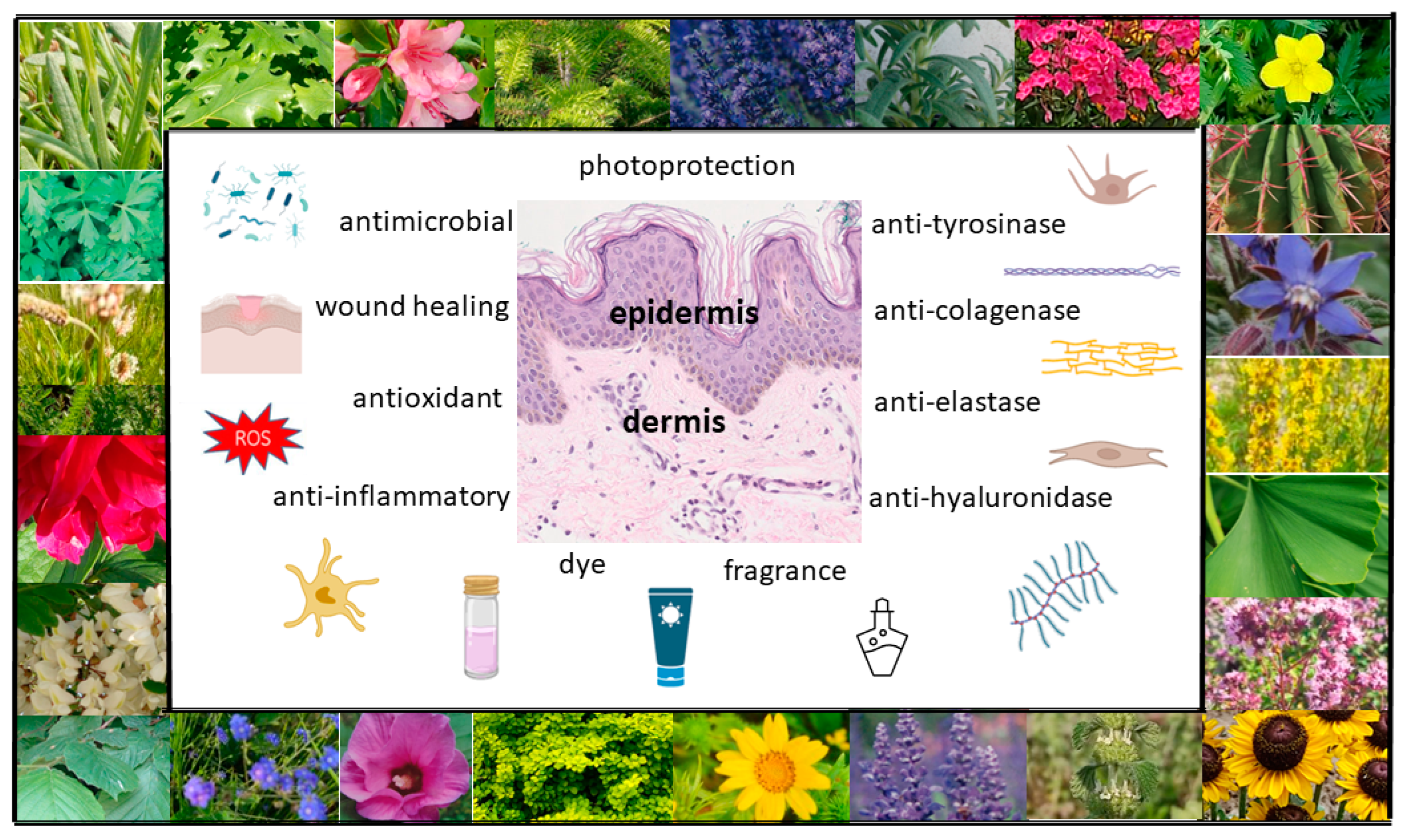
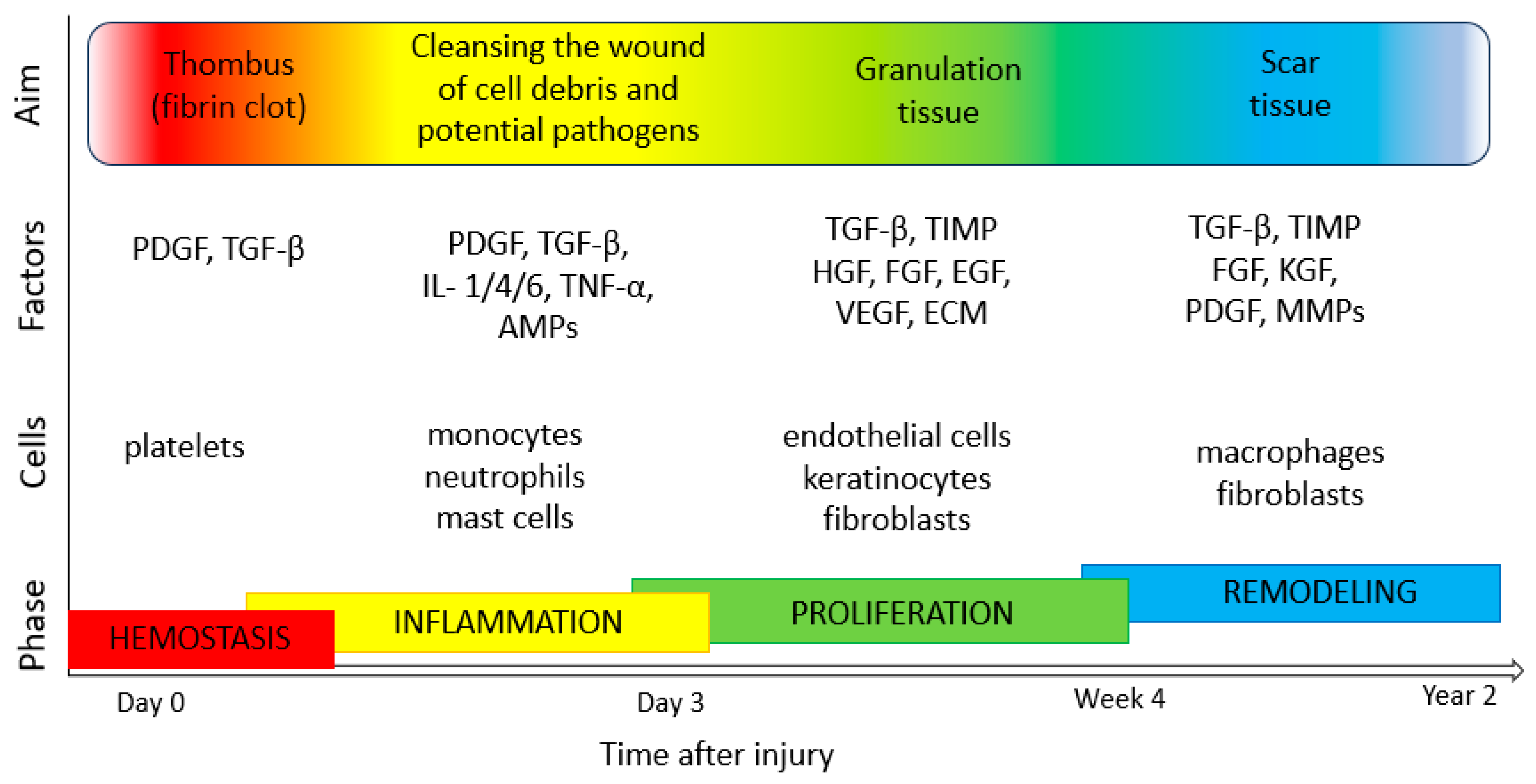
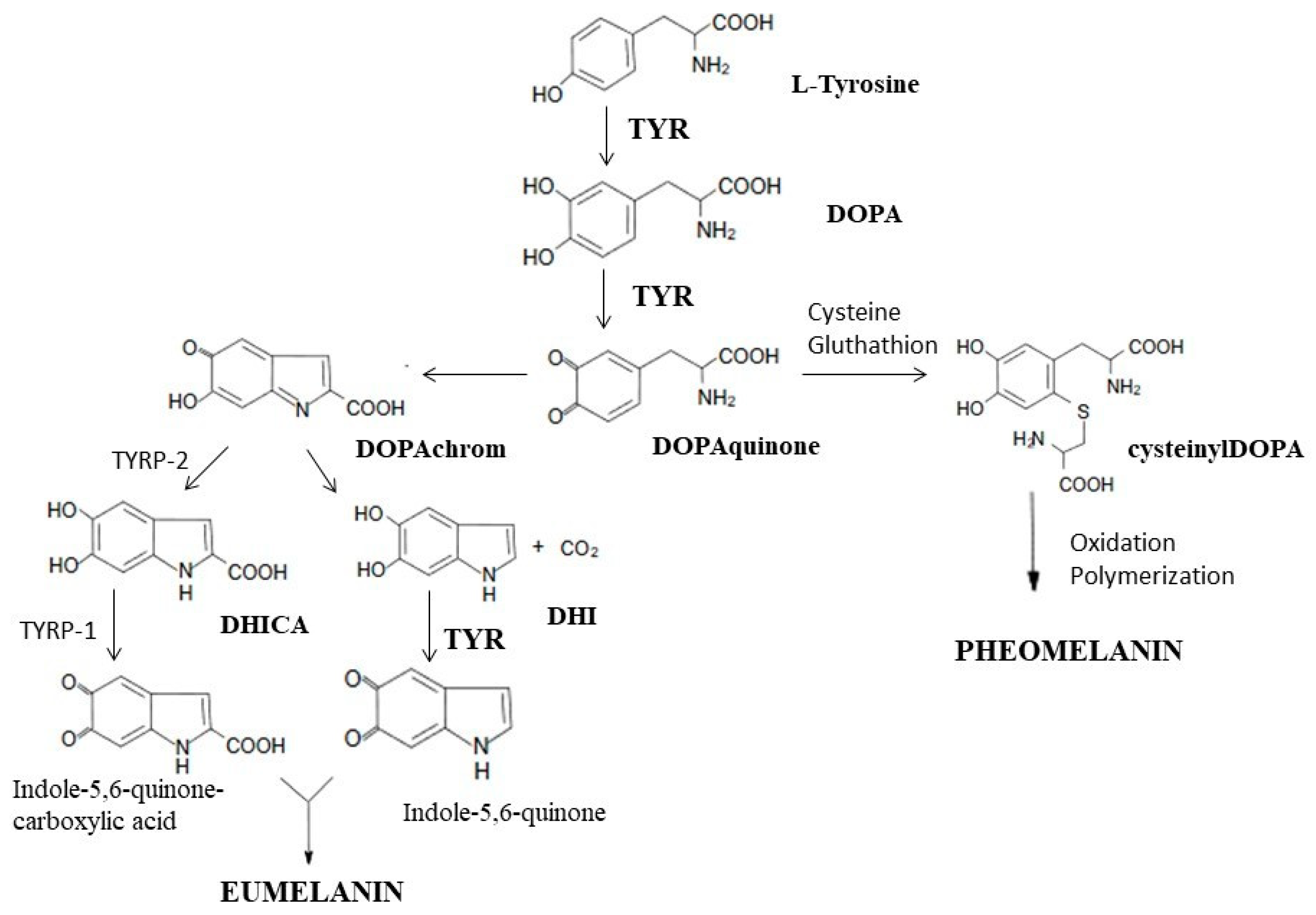
| Species (Family) | Plant Material | Method | Effect | Ref |
|---|---|---|---|---|
| Adenocaulon himalaicum (Asteraceae) | leaf, EE | in vitro, HaCaT exposed to UVB | ↑ filaggrin, involucrin, loricrin expression ↓ MMP-1; MAPK, AP-1 activation | [52] |
| Alpinia officinarum (Zingiberaceae) | rhizome, WE | in vivo, UVB-irradiated hairless mouse; in vitro, NIH-3T3 exposed to UVB | ↓ of MMP-1 expression and recovered the reduction in collagen content in mouse skin; ↓ IL-6, IL-8, MCP-3 expression and ↓ phospho-Akt and phospho-ERK in NIH-3T3 | [53] |
| Antidesma thwaitesianum (Euphorbiceae) | fruit extract | in vitro, UVB-irradiated HaCaT | protects cells from UVB-induced cytotoxicity; anti-inflammatory effect through ↓ NO and ROS generation; ↓ phospho-p38 and phospho-JNK | [54] |
| Astragalus gombiformis (Fabaceae) | aerial part, BE | in vitro, SPF via UV spectroscopy | SPF 37.78 | [41] |
| Calea fruticosa (Asteraceae) | aerial part, EE | in vitro, SPF via UV spectroscopy | SPF 9.66 | [55] |
| Camellia sinensis (Theaceae) | leaf extract | in vitro, NHEK exposed to UVB | efficacy in recovering TIMP-3 expression downregulated by UVB treatment | [56] |
| Chrysophyllum lucentifolium (Sapotaceae) | ME | in vitro, UVB and H2O2-treated HaCaT and HDF | ↓ expression of COX-2, MMP-1, and -9, HYAL-1, and -4 by downregulating the NF-κB and MAPK (ERK, JNK and p38) pathways; ↑ Col1a1 expression | [57] |
| Cistus incanus Cistus ladanifer (Cistaceae) | aerial part extract | in vitro, SPF via UV spectroscopy | SPF 3.33—4.37 | [58] |
| Ceratonia siliqua (Fabaceae) | pod and seed extract, WME | in vitro, SPF via UV spectroscopy | SPF 1.07–18.19 | [59] |
| Corylus avellana (Betulaceae) | hazelnut skin extract | in vitro, SPF via UV spectroscopy | extract ↑ SPF value of benzophenone 4.66–4.94 | [60] |
| Cyclopia spp. (Fabaceae) | leaf and branch, WAE | in vitro, SPF via UV spectroscopy | SPF 27.8 | [61] |
| Diospyros kaki (Ebenaceae) | fruit (pulp, skin and seed) extract | in vitro, HaCaT exposed to UVA and UVB | ↓ intracellular ROS production in cells; exerts a photoprotective and regenerative effect on UV-irradiated cells | [62] |
| Elaeagnus angustifolia (Elaeagnaceae) | leaf extract | in vitro, SPF via UV spectroscopy | SPF values of sunscreen formulation (with 2%, 4%, 6%, 8% extracts): 6.37–21.05 | [63] |
| Euphorbia characias (Euphorbiaceae) | leaf, EE | in vitro, SPF via UV spectroscopy | SPF 9.10 | [64] |
| Helianthus annuus (Asteraceae) | flower, EE | in vitro, UVB-irradiated HDF | ↓ MMP-1, 3 and ROS production; ↓ procollagen type I reduction; anti-photoaging action via the activation of Nrf2, upregulation of TGF-β, downregulation of AP-1 and MAPK phosphorylation; ↓ UVB-induced VEGF and IL-6, COX-2, iNOS and TNF-α secretion | [65] |
| Hylocereus polyrhizus (Cactaceae) | fruit peel, EE | in vitro, SPF via UV spectroscopy | SPF 35.02 | [43] |
| Juglans regia (Juglandaceae) | male flower, ME | in vitro, UVB-irradiated HaCaT | prevents the overexpression of MAPKs, AP-1, MMPs, Smad7; ↓ expression of TIMP-1/2, TGF-β1, Smad3 and procollagen type-1 in cells | [66] |
| Kadsura coccinea (Schisandraceae) | root, stem, leaf and fruit, EE | in vitro, UVA and UVB-irradiated HaCaT | alleviates anti-proliferative and cytotoxic effects of UVA/UVB irradiation on cells; ↓ intracellular ROS level and keratinocyte damage | [67] |
| Melaleuca leucadendron (Myrtaceae) | flower, EE | in vitro, UVB-induced HaCaT | ↓ COX-2 expression, ensures protection of DNA damage, prevents the increase in ROS; ↑ levels of the antioxidant enzymes SOD, GPx and CAT | [68] |
| Moringa concanensis (Moringaceae) | stem bark extract | in vitro, SPF via UV spectroscopy, UVA/UVB absorption spectra | SPF 10.46 and broad absorption spectrum (UVA and UVB) ranges | [69] |
| Oenanthe javanica (Apiaceae) | EE | in vivo, UVB-exposed mouse | ↑ collagen types I and III productions; ↓ MMP-1 and MMP-3, TNF-α and COX-2 expression | [70] |
| Penthorum chinense (Penthoraceae) | EE | in vitro, HaCaT under UVB or H2O2 treatment | ↑ the promoter activity of the type 1 procollagen gene Col1A1; ↓ MMPs, COX-2, IL-6 expression and HYAL induced by UVB irradiation or H2O2-induced oxidative stress; ↓ phospho-p38 and phospho-JNK | [71] |
| Pradosia mutisii (Sapotaceae) | ME | in vitro, HaCaT, HDF under UVB or H2O2 treatment | ↓ MMP-1 and MMP-9; ↑ Sirt-1 | [72] |
| Posoqueria latifolia (Rubiaceae) | flower, EE | in vitro, SPF via UV spectroscopy | SPF 35, broad-spectrum (UVA-UVB) protection efficacy | [44] |
| Ranunculus bulumei (Ranunculaceae) | aerial part, ME | in vitro, UVB-irradiated HaCaT | ↓ mRNA levels of MMP-9, COX-2; ↑mRNA levels of Sirt-1, type-1 procollagen; ↓ phospho-p38; inactivates AP-1 | [73] |
| Rosa centifolia (Rosacea) | flower, EE | in vitro, SPF via UV spectroscopy | SPF value of 32, broad-spectrum (UVA-UVB) protection efficacy | [44] |
| Rosmarinus officinalis (Lamiaceae) | leaf, HE | in vivo, UV-irradiated rat | ↓ level of GSH, SOD, CAT; ↓ IL-1β, IL-6, and NF-kB; ↓ MMP-1, GM-CSF, NEP | [74] |
| Rubus idaeus (Rosaceae) | EE | in vitro, HaCaT; in vivo, mouse exposed to UVB | alleviate UVB-caused erythema in the skin; ↓ formation of 8-OHdG; recover the expression of Nrf2 and antioxidant enzyme proteins SOD and CAT; ↓ phospho-p38 and NF-κB expression | [75] |
| Sideritis raeseri (Lamiaceae) | aerial part, WEE | in vitro, SPF via UV spectroscopy | SPF 4.54–18.01 | [76] |
| Sloanea medusula Sloanea calva (Elaeocarpaceae) | leaf, EE | in vitro, SPF via UV spectroscopy | S. medusula, SPF 32.5 S. calva, SPF 35.4 | [42] |
| Spatholobus suberectus (Leguminosa) | stem, WE, EE | in vitro, HaCaT exposed to UVB | ↓ ROS production; block MAPK, NF-κB and c-Jun; ↑ Col1a1, ELN, HAS2 expression | [77] |
| Syzygium formosum (Myrtaceae) | leaf, EE | in vitro, HaCaT exposed to UVB | ↓ IL-1 β, IL-6, IL-8 and COX-2 expression | [78] |
| Silybum marianum (Asteraceae) | sylimarin and flavonolignans | in vitro, SPF via UV spectroscopy | absorbs UVB and UVA; SPF 2.01–6.07 | [79] |
| Washingtonia filifera (Arecaceae) | seed, EE, WE, ME | in vitro, H2O2-induced HaCaT; in vitro SPF via UV spectroscopy | ↓ ROS generation; SPF 1.52–3.35. | [80] |
| Zanthoxylum bungeanum (Rutaceae) | sanshool, a major component | in vitro, UVB-irradiated HDF; in vivo, mouse | ↓ activation of JAK2-STAT3 signaling; ↓ MMP-1 and MMP-3 secretion | [81] |
| Plant (Family) | Plant Material | Cell/Animal | Effect | Ref |
|---|---|---|---|---|
| Agrimonia eupatoria (Rosaceae) | WE | in vitro, NIH 3T3, HDF and HaCaT; in vivo, rat | ↑ ECM deposition, ↑ keratinocyte proliferation/differentiation; ↑ wound TS and contraction rates | [105] |
| Angelica polymorpha (Umbelliferae) | flower absolute | in vitro, HaCaT | ↑ cell migration, proliferation and collagen IV synthesis; ↑ phosphorylation of ERK1/2, JNK, MAPK p38 and Akt | [106] |
| Annona reticulata (Annonaceae) | leaf, EE | in vitro, HaCaT | ↑ VEGF and Akt; ↑ cell migration and proliferation | [107] |
| Astragalus floccosus (Leguminosae) | root, ME | in vitro, NHDF; in vivo, rat | ↑ scratch wound healing, cell proliferation, fibrosis and epithelization | [108] |
| Betula pendula (Betulaceae) | bark, WE | in vitro, HaCaT | strong activities against S. aureus, C. acnes and S. epidermidis; ↑ wound closure | [109] |
| Boesenbergia rotunda (Zingiberaceae) | rhizome, EE | in vitro, HaCaT | ↑ ERK1/2 and Akt; ↑ cell migration and proliferation | [110] |
| Bursera morelensis (Burseraceae) | terpenes α-pinene and α-phellandrene | in vivo, mouse | ↑ wound contraction due to collagen deposition from the early stages; provided better structure in scar tissue | [111] |
| Centella asiatica (Apiaceae) | WGE | in vitro, HaCaT | positively affected wound healing and cell migration | [112] |
| Cumin carvi (Apiaceae) | seed, WEE | in vivo, rat | healing effects: ↑ total protein content and biomechanical factors; ↑ re-epithelialization, granular tissue, connective tissue, collagen and angiogenesis index; ↓ inflammatory factors | [113] |
| Cyclopia spp. (Fabaceae) | leaf and branch, WE, WEE | in vitro, HaCaT | ↑ cell migration | [61] |
| Derris scandens (Fabaceae) | stem, WE, EE | in vitro, HSF | ↑ cell migration and wound closure in a scratch assay | [114] |
| Digitaria ciliaris (Poaceae) | flower, EE | in vitro, CCD986sk HaCaT | ↑ cell proliferation and migration; ↑ collagen I and IV syntheses; ↑ phosphorylation of ERK1/2 and p38 MAPK | [115] |
| Fagus sylvatica (Fagaceae) | bark, WE | in vitro, HaCaT | strong activities against S. aureus, C. acnes and S. epidermidis; ↑ wound closure | [109] |
| Glycyrrihza glabra (Fabaceae) | root, EE | in vivo, rat | ↑ collagen synthesis, ↑ α-SMA, PDGFR-α, FGFR1 and Cytokeratin 14 expression; ↑ angiogenesis and collagen deposition through up-regulation of bFGF, VEGF and TGF-β gene expression levels | [116] |
| Garcinia mangostana (Clusiaceae) | pericarp, EE | in vitro, 3T3-CCL92 | ↑ fibroblast proliferation and wound recovery | [117] |
| Greyia radlkoferi (Melianthaceae) | leaf, EE | in vitro, HaCaT | antibacterial activity against wound-associated bacteria (S. aureus) | [118] |
| Hydrangea serrata (Hydrangeaceae) | leaf, WE | in vitro, HaCaT | improved transcription levels of keratin Ker5, Ker6 and Ker16 | [119] |
| Jatropha neopauciflora (Euphorbiaceae) | latex | in vivo, normal and diabetic mouse | accelerated and improved the wound-healing process | [120] |
| Nigella sativa (Ranunculaceae) | seed, EE | in vitro, 3T3-CCL92 | ↑ cell proliferation and wound recovery | [117] |
| Rosmarinus officinalis (Lamiaceae) | leaf, HE | in vitro, HaCaT | ↑ migration and repopulation of keratinocytes at the scratched area and considerably narrowed the scratched gap | [74] |
| Salix koreensis (Salicaceae) | flower absolute | in vitro, HaCaT | ↑ cell proliferation, migration and collagen I and IV production; ↑ phosphorylation of Akt, JNK, ERK1/2 and p38 MAPK | [121] |
| Sapindus mukorossi (Sapindaceae) | kernel oil | in vitro, CCD-966SK | ↑ cell proliferation and migration; anti-inflammatory and anti-microbial activities; ↑ wound healing, ↓ size of the wound | [122] |
| Sorocea guilleminina (Moraceae) | leaf, WE | in vitro, N3T3; in vivo rat | ↑ cell proliferation/migration rate, ↑ wound contraction | [123] |
| Ulmus parvifolia (Ulmaceae) | root bark, ME | in vitro, HaCaT; in vivo, mouse | ↑ cell migration; upregulated the expression of the MMP-2 and -9 protein, ↑ TGF-β | [124] |
| Plant material | Formulation | Cell/animal | Effect | Ref |
| Aloe vera | gel with EE | in vitro, HaCaT, HFF1; in vivo, rat | ↑ cell proliferation; promoted wound healing; accelerated re-epithelialization and wound contraction | [125] |
| Avicennia schaueriana | cream with leaf WE | in vivo, mouse | ↑ re-epithelialization and the number of fibroblasts, exhibiting a healing activity on skin injuries | [126] |
| Caralluma europaea | ointment with aerial part WEE | in vivo, rat | ↑ wound healing | [127] |
| Cassia obtusifolia | gel with aerial part EE | in vivo, rat and mouse | ↑ wound healing | [128] |
| Clematis simensis | ointment with leaf WEE | in vivo, mouse and rat | ↑ wound contraction and epithelialization; extract reduced inflammation and demonstrated antioxidant activity | [129] |
| Cnestis ferruginea | creams with root bark ME | in vivo, rat | ↓ wound size; affected the formation of well-regenerated tissue | [130] |
| Convolvulus arvensis | ointment with stem ME | in vivo, rat | ↑ wound closure; improved skin architecture; healing potential comparable to that of gentamycin | [131] |
| Centella asiatica | hydrogel with asiaticoside-rich fraction | in vivo, rabbit | ↑ wound healing | [132] |
| Cynara humilis | ointment with root WE and EE | in vivo, rat | ↑ wound contraction, epithelialization, ↑ collagen production; ↓ the number of inflammatory cells during wound healing | [133] |
| Epilobium angustifolium | hydrogel with EE, IE and WE | in vitro, HDF | ↑ wound healing; activity against S. pneumoniae, E. coli, E. faecalis, E. faecium, S. lutea and B. pseudomycoides | [94] |
| Ginkgo biloba | O/W cream with leaf WE | in vivo, diabetic rats | ↑ wound closure associated with increased collagen synthesis | [134] |
| Loranthus acaci | gel with aerial part EE | in vivo, rat and mouse | ↑ wound healing | [128] |
| Marantodes pumilum | ointment with leaf and root WE | in vivo, rat | ↑ wound healing; re-epithelialization, collagen deposition, fibronectin content and fibroblast cells, and fiber transformation from collagen III to I | [135] |
| Phlomis russeliana | gel with aerial part extract | in vivo, mouse | ↑ dermal and epidermal regeneration, collagen formation, ↑ TGF-β, VEGF and FGF levels | [136] |
| Punica granatum, Matricaria chamomilla | ointment with methanol fraction of pomegranate and chamomile flowers | in vivo, rat | ↑ wound healing; activity against S. aureus, S. epidermidis and P. aeruginosa of plant extracts | [137] |
| Roylea elegans | cream with leaf WE | in vivo, rat | ↑ wound contraction formation of collagen, and tissue re-epithelialization; ↑ protein, GSH, SOD and CAT levels, ↓ MPO levels; ↑ IL-10, ↓ TNF-α and IL-6 | [138] |
| Tamarix aphylla | nanoemulsion W/O with leaf ME | in vivo, rabbit | ↑ acid-burn wound-healing process (improved cell attachment at the edge of the wound, collagen content), ↓ healing duration | [139] |
| Urtica simensis | ointment with leaf WME | in vivo, mouse | ↑ wound contraction, ↓ periods of epithelialization | [140] |
| Virola oleifera | cream with resin | in vivo, rat | ↑ wound contraction; ↓ LPO and protein oxidation | [141] |
| Plant essential oils | polysaccharide-based hydrogel with eucalyptus, ginger and cumin EO | in vitro, L929 cells; in vivo, mouse | antibacterial activity against S. aureus and E. coli; ↑ cell migration and improved burn wound healing | [142] |
| Cinnamaldehyde | nanoemulsion | in vivo, rat | ↓ wound size; ↑ CAT and SOD, ↓ NAP3; activity against S. aureus and S. typhimurium | [143] |
| Species (Family) | Part/Extract | Method | Results | Ref |
|---|---|---|---|---|
| Aegopodium podagraria (Apiaceae) | WGE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA and COL activity | [112] |
| Aerva lanata (Amaranthaceae) | EE, WE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA, COL and HYAL activity | [153] |
| Arachis hypogaea (Fabaceae) | peanut shells, UAE | enzyme reaction assay, spectrophotometric method in vitro | ↓ COL activity | [154] |
| Artemisia iwayomogi (Asteraceae) | 1% water fraction | in vivo study on 21 women volunteers | anti-wrinkle effect after using O/W cream for 8 weeks; ↓ depth of fine wrinkles on facial skin | [155] |
| Asparagus officinalis (Asparagaceae) | aerial parts, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ MMP-1, ELA and HYAL activity | [156] |
| Borago officinalis (Boraginacea) | aerial parts, ME, WME | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA, COL activity | [157] |
| Bruguiera gymnorhiza (Rhizophoraceae) | leaf, root, twig, fruit, EAE, ME | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA activity | [158] |
| Cannabis sativa (Cannabaceae) | herb, WEE, MAE, UAE | enzyme reaction assay, spectrophotometric method in vitro; application analysis on 15 volunteers in vivo | ↓ COL and ELA activity; ↓ TEWL; ↑ skin moisture level | [150] |
| Cyclopia spp. (Fabaceae) | leaf, branches, WE, WEE, WAE, BE | enzyme reaction assay, spectrophotometric method in vitro | ↓ COL and HYAL, weak influence on ELA activity | [61] |
| Curculigo latifolia (Hypoxidaceae) | root, steam, leaf, EAE, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA activity | [159] |
| Dimocarpus longan (Sapindaceae) | seed extracts, PET, EAE, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ MMP-1 and HYAL activity | [160] |
| Euphorbia characias (Euphorbiaceae) | leaf, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA, COL and HYAL activity | [64] |
| Hydrangea serrata (Hydrangeaceae) | leaf, WE | in vitro, HaCaT and HDF; clinical study (22 subjects) | ↑ skin barrier components and HAS, ↓ mRNA levels of HYAL-1, -2, -3; ↑ mRNA expression of Col1a1; ↑ skin moisture level, ↓ skin wrinkles | [119] |
| Nelumbo nucifera (Nelumbonaceae) | whole flower, stamen, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA, COL and HYAL activity | [161] |
| Olea europaea (Oleacea) | leaf, WE, PPG, LA; MAE, UAE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA and COL activity | [162] |
| Plectranthus spp. (Lamiaceae) | aerial part, WE, ME, AE, EAE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA and COL activity | [163] |
| Pradosia mutisii (Sapotaceae) | ME | in vitro, HaCaT and HDF | ↑ expression of moisturizing-related genes HAS-2, TGM-1 and Col1a1 gene | [72] |
| Premna odorata (Verbenaceae) | leaf, EO | enzyme reaction assay, spectrophotometric method in vitro | considerable anti-ELA and anti-HYAL and mild anti-COL potential | [164] |
| Rosmarinus officinalis (Lamiaceae) | leaf, HE | enzyme reaction assay, fluorometric and spectrophotometric methods in vitro | ↓ ELA, COL and HYAL activity | [74] |
| Spatholobus suberectus (Fabaceae) | stem, WE, EE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA activity | [77] |
| Thunbergia laurifolia (Acanthacea) | leaf, EE, SE, RE | enzyme reaction assay, fluorometric and spectrophotometric methods in vitro; in vitro, 3T3 cells | ↓ MMP-1, MMP-2, -9 and HYAL activity | [165] |
| Vitis vinifera (Vitaceae) | fruit, WEE | single-blind placebo-controlled in vivo study, 11 volunteers | improvement in skin moisture and elasticity after 12 weeks of applying W/O emulsion | [166] |
| Washingtonia filifera (Arecaceae) | pulp, seed, WE, EE, ME | in vitro, HaCaT | ↓ ELA and COL activity | [80] |
| Warburgia salutaris (Canellacea) | bark, WE | enzyme reaction assay, spectrophotometric method in vitro | activity against HYAL > ELA > COL | [167] |
| Papaver rhoeas Punica granatum Clitoria ternatea Carthamus tinctorius Gomphrena globasa | flower, WEE | enzyme reaction assay, spectrophotometric method in vitro; application analysis on 15 volunteers in vivo | ↓ ELA and COL activity; SPF 20–31; ↓ TEWL; ↑ skin moisture level | [168] |
| Cannabis sativa Foeniculum vulgare Punica granatum Vitis vinifera | seed, EE, WEE, SFE UAE | enzyme reaction assay, spectrophotometric method in vitro | ↓ ELA and COL activity | [169] |
| Phyllanthus emblica Momordica cochinchinensis Centella asiatica | leaf, fruit extract | randomized double-blind placebo-controlled in vivo study, 60 women | significant improvement in skin hydration, elasticity and wrinkles in eye and cheek areas after 60 days of emulsion application containing an extract combination | [151] |
| Plant Species | Family | Part of Plant | Ref |
|---|---|---|---|
| Acanthus mollis | Acanthaceae | leaves | [192] |
| Aerva lanata | Amaranthaceae | aerial parts | [153] |
| Allium galanthum | Amaryllidaceae | bulbus | [193] |
| Allium turkestanicum | |||
| Anacamptis pyramidalis | Orchidaceae | tubers | [194] |
| Anacardium occidentale | Anacardiaceae | leaves | [195] |
| Anacardium occidentale | Anacardiaceae | fruits | [196] |
| Andropogon virginicus | Poaceae | aerial parts | [197] |
| Angelica keiskei | Umbelliferae | leaves, roots | [198] |
| Arachis hypogaea | Fabaceae | peanut shell | [154] |
| Areca catechu | Palmaceae | fruits | [195] |
| Arctium minus | Asteraceae | flower heads, leaves, roots | [199] |
| Artemisia verlotiorum | Asteraceae | whole plant | [200] |
| Atractylodis macrocephalae | Asteraceae | rhizomes | [201] |
| Berberis thunbergii | Berberidaceae | leaves | [202] |
| Bergenia pacumbis | Saxifragaceae | plant and its rhizomes | [203] |
| Blepharis linariifolia | Acanthaceae | aerial parts | [204] |
| Bletilla striata | Orchidaceae | tubers, fibrous roots | [205] |
| Breynia retusa | Phyllanthaceae | leaves | [206] |
| Bridelia ferruginea | Phyllanthaceae | leaves, stem bark | [207] |
| Bruguiera gymnorhiza | Rhizophoraceae | leaves, roots, fruits | [158] |
| Cakile maritima | Brassicaceae | fruits, leaves, stems | [208] |
| Cannabis sativa | Cannabaceae | seeds | [169] |
| Carthamus tinctorius | Asteraceae | seeds | [209] |
| Celastrus hindsii | Celastracea | leaves | [210] |
| Cercis glabra | Fabaceae | leaves | [211] |
| Cladium mariscus | Cyperaceae | seeds | [212] |
| Clausena indica | Rutaceae | roots | [213] |
| Combretum micranthum | Combretaceae | leaves | [196] |
| Crotalaria burhia | Fabaceae | aerial parts, roots | [214] |
| Croton hirtus | Euphorbiaceae | aerial parts | [215] |
| Cudrania tricuspidata | Moraceae | fruits | [216] |
| Cytinus hypocistis | Cytinaceae | aerial parts | [217] |
| Dianella ensifolia | Liliaceae | roots | [218] |
| Dodonaea viscosa | Sapindaceae | stems | [219] |
| Elaeagnus angustifolia | Elaeagnaceae | fruits, leaves | [220] |
| Euphorbia hirta | Euphorbiaceae | whole plant | [196] |
| Feijoa sellowiana | Myrtaceae | leaves | [221] |
| Foeniculum vulgare | Apiaceae | seeds | [169] |
| Glochidion zeylanicum | Phyllanthaceae | leaves | [195] |
| Girardinia diversifolia | Urticaceae | shoot tips | [222] |
| Helichrysum rutilans | Asteraceae | aerial parts | [223] |
| Heliotropium procumbens | Boraginaceae | aerial parts | [224] |
| Heliotropium crispum | Boraginaceae | whole plant | [225] |
| Hibiscus tiliaceus | Malvaceae | leaves | [226] |
| Hypericum montbretii | Hypericaceae | aerial parts | [227] |
| Hypericum origanifolium | |||
| Iris pseudacorus | Iridaceae | aerial parts, rhizomes | [228] |
| Jatropha curcas | Euphorbiaceae | stems, bark, leaves | [229] |
| Jatropha gossipiifolia | |||
| Limonium effusum | Plumbaginaceae | aerial parts | [230] |
| Limonium sinuatum | |||
| Litchi chinensis | Sapindaceae | roots | [231] |
| Lonicera japonica | Caprifoliaceae | whole plant | [232] |
| Mangifera caloneura | Anacardiaceae | leaves | [195] |
| Manilkara kauki | Sapotaceae | fruits, leaves, seeds, stem bark, woods | [233] |
| Matthiola incana | Brassicacea | leaves, flower buds | [234] |
| Melastoma normale | Melastomacea | roots | [235] |
| Momordica cochinchinensis | Cucurbitacea | fruits (pulp, aril, seed) | [236] |
| Monotheca buxifolia | Sapotaceae | leaves, stems | [237] |
| Nelumbo nucifera | Nelumbonaceae | whole flower, stamen | [161] |
| Onosma bourgaei, | Boraginaceae | aerial parts | [238] |
| Onosma trachytricha | |||
| Paliurus spina-christi | Rhamnaceae | fruits, leaves, stems | [239] |
| Pistacia lentiscus | Anacardiaceae | leaves | [240] |
| Phaseolus vulgari | Fabaceae | seed coat | [241] |
| Phytolacca dioica | Phytolaccacea | fruits | [242] |
| Plectranthus ecklonii, P. namaensis, P. zuluensis | Lamiacea | aerial parts | [243] |
| Punica granatum | Punicaceae | seeds | [169] |
| Rheum palmatum | Polygonacea | roots, rhizomes | [244] |
| Rhizophora racemosa | Rhizophoraceae | leaves, stem bark | [245] |
| Rhizophora apiculata | Rhizophoraceae | leaves | [226] |
| Rhizophora mucronata | |||
| Rosa platyacantha | Rosaceae | flowers, leaves, buds | [246] |
| Rubus fraxinifolius | Rosaceae | leaves | [247] |
| Salvia chamelaeagnea, | Lamiacea | aerial parts | [243] |
| Salvia dolomitica | |||
| Sartoria hedysaroides | Fabaceae | aerial parts | [248] |
| Schisandra chinensis | Schisandraceae | fruits | [249] |
| Secamone afzelii | Asclepiadaceae | leaves | [250] |
| Streblus taxoides | Moraceae | wood | [251] |
| Strobilanthes glutinosus | Acanthaceae | whole plant | [252] |
| Tambourissa peltat | Monimiaceae | fruits, flowers, leaves | [200] |
| Vitis amurensis | Vitaceae | root | [253] |
| Vitis vinifera | Vitaceae | seeds | [169] |
| Warburgia salutaris | Canellacea | barks | [167] |
| Zingiber kerrii | Zingiberaceae | rhizomes | [254] |
| Ziziphora taurica | Lamiaceae | aerial parts | [255] |
| Family | Aromatic Plants | Extraction of EO | Single Constituent | Aroma Description | Ref. |
|---|---|---|---|---|---|
| Lamiaceae | Lavandula officinalis | hydrodistillation of air-dried flowers | linalool, linalyl acetate, geraniol, β-caryophyllene, lavandulyl acetate | fresh, herbaceous, floral | [261] |
| Origanum vulgare | hydrodistillation of air-dried aerial parts | carvacrol, γ-terpinene, p-cymene, trans-sabinene hydrate, thymol | warm, spicy, camphoraceous | [262] | |
| Thymus vulgaris | hydrodistillation of shade-dried flowers and leaves | thymol, γ-terpinene, p-cymene, linalool, myrcene, α-pinene, α-thujene | strong, spicy, herbaceous | [263] | |
| Mentha piperita | hydrodistillation of shade-dried aerial parts | camphane, menthone, menthol, β-pinene, pulegone, β-cubebene, α-pinene, γ-terpinene, γ-carane, piperiton | fresh, sweetish, menthol | [264] | |
| Hyssopus officinalis | steam distillation, simple hydrodistillation and hydrodistillation in Dean–Stark apparatus of air-dried flowering aerial parts | elemol, spathulenol, α-eudesmol, γ-eudesmol, virdiflorol, hedycaryol, isopinocamphone, cis-jasmone. | fresh, herbal, slightly sweet, camphorous | [265] | |
| Apiaceae | Pimpinella anisum | hydrodistillationof mature fruits | trans-anethole, γ-himachalene, trans-pseudoisoeugenyl 2-methylbutyrate, cis-dihydrocarvone, methyl chavicol, α-himachalen, β-himachalene | fresh, warm, sweet, mildly pungent | [266] |
| Carum carvi | hydrodistillation and microwave-assisted hydrodistillation of air-dried seeds | carvone, limonene, apiole, andrographolide, aromadendrene, β-cadinene, friedelanol, barrigenol, 3-benzyloxyphenol | pungent, anise-like, herbaceous | [267] | |
| Rutaceae | Citrus limon | hydrodistillation of peels | limonene, α-citral, β-pinene, α-terpinene, β-elemene, neryl acetate | sharp, lemon, sweet | [268] |
| Citrus paradisi | molecular distillation from cold-pressed fruits | limonene, β-myrcene, α-pinene, sabinene (0.60%), carvone (0.41%), cis-limonene oxide (0.43%), and trans-limonene oxide (0.33%), caryophyllene (0.20%), β-cubebene (0.14%), α-copaene (0.13%), | fresh, sharp, citrus | [269] | |
| Verbenaceae | Verbena officinalis | steam distillation of leaves | limonene, 1,8-cineole, ar-curcumeme, caryophyllene oxide, spathulenol | lemony scent with sweet, fruity undertones | [270] |
| Lauraceae | Cinnamomum verum | hydrodistillation of shade-dried leaves | eugenol, linalol, benzyl benzoate, | sweet, spicy, slightly woody, clove-like | [271] |
| Asteraceae | Anthemis nobilis | hydrodistillation of shade-dried flowers | en-yn-dicycloether, β-caryophyllene, aristolene epoxide, germacrene D, widdrol, cis-caryophyllene | crisp, sweet, herbal, floral, soft fruity (reminiscent of apples) | [272] |
| Myrtaceae | Eucalyptus globulus | steam distillation of dried leaves | eucalyptol, α-pinene, p-cymene, β- myrcene, terpinen-4-ol, γ-terpinene | fresh, camphoraceous, medicinal | [273] |
| Melaleuca alternifolia | steam distillation of young branches and leaves | terpinen-4-ol,-terpinene, 1,8-cineole, p-cymene | fresh, camphoraceous | [274] | |
| Syzygium aromaticum | supercritical fluid extraction assisted by cold pressing buds | eugenol, eugenyl acetate, β- caryophyllene, α-humulene | clove, strong | [275] | |
| Geraniaceae | Pelargonium graveolens | hydrodistillation of fully grown aerial parts | citronellol, geraniol, caryophyllene oxide, menthone, linalool, β-bourbonene, iso-menthone, geranyl formate | floral, sweet, rose-like with minty undertones | [276] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Michalak, M. Plant Extracts as Skin Care and Therapeutic Agents. Int. J. Mol. Sci. 2023, 24, 15444. https://doi.org/10.3390/ijms242015444
Michalak M. Plant Extracts as Skin Care and Therapeutic Agents. International Journal of Molecular Sciences. 2023; 24(20):15444. https://doi.org/10.3390/ijms242015444
Chicago/Turabian StyleMichalak, Monika. 2023. "Plant Extracts as Skin Care and Therapeutic Agents" International Journal of Molecular Sciences 24, no. 20: 15444. https://doi.org/10.3390/ijms242015444
APA StyleMichalak, M. (2023). Plant Extracts as Skin Care and Therapeutic Agents. International Journal of Molecular Sciences, 24(20), 15444. https://doi.org/10.3390/ijms242015444






