Sleep and Anabolic/Catabolic Hormonal Profile in Sedentary Middle-Aged Adults: The FIT-AGEING Study
Abstract
1. Introduction
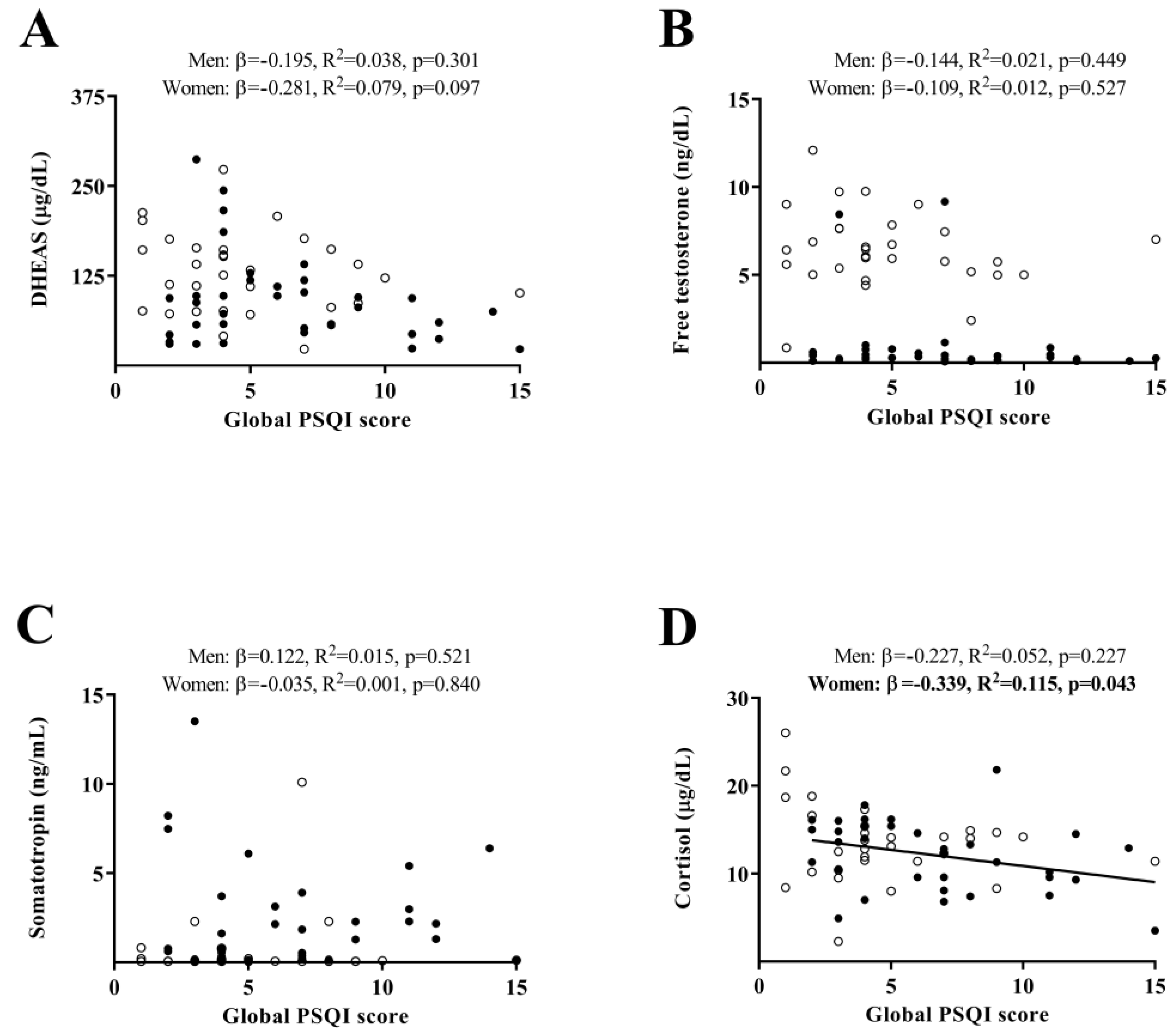
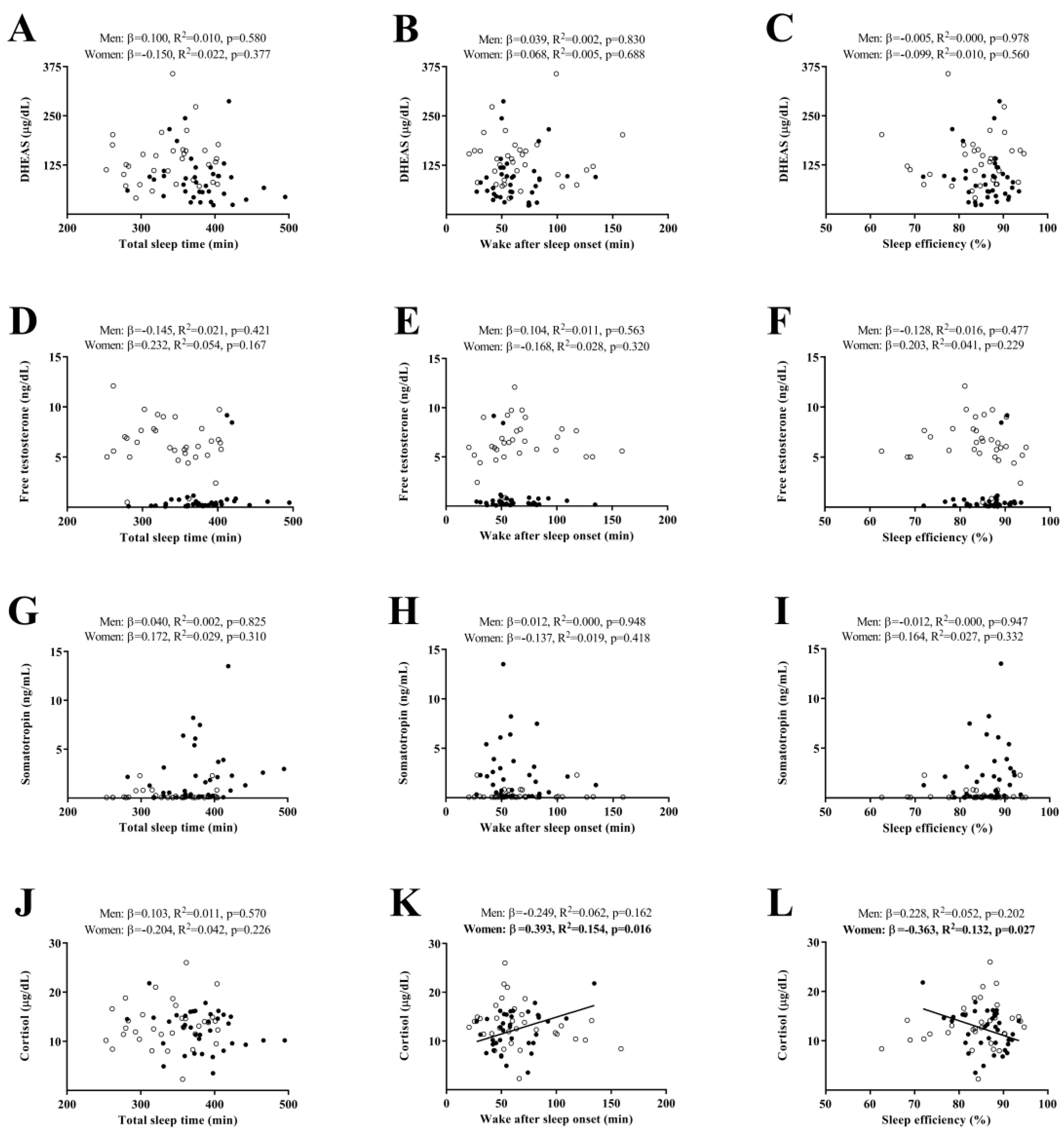
2. Results
3. Discussion
4. Materials and Methods
4.1. Study Protocol and Participants
4.2. Measurements
4.2.1. Anthropometry and Body Composition
4.2.2. Sleep Quantity and Quality
4.2.3. Blood Sampling
4.3. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- van den Beld, A.W.; Kaufman, J.-M.; Zillikens, M.C.; Lamberts, S.W.J.; Egan, J.M.; van der Lely, A.J. The Physiology of Endocrine Systems with Ageing. Lancet Diabetes Endocrinol. 2018, 6, 647–658. [Google Scholar] [CrossRef] [PubMed]
- Chahal, H.; Drake, W. The Endocrine System and Ageing. J. Pathol. 2007, 211, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Bartke, A. Growth Hormone and Aging: Updated Review. World J. Mens. Health 2019, 37, 19. [Google Scholar] [CrossRef]
- Luboshitzky, R.; Shen-Orr, Z.; Herer, P. Middle-Aged Men Secrete Less Testosterone at Night Than Young Healthy Men. J. Clin. Endocrinol. Metab. 2003, 88, 3160–3166. [Google Scholar] [CrossRef]
- Yiallouris, A.; Tsioutis, C.; Agapidaki, E.; Zafeiri, M.; Agouridis, A.P.; Ntourakis, D.; Johnson, E.O. Adrenal Aging and Its Implications on Stress Responsiveness in Humans. Front. Endocrinol. 2019, 10, 54. [Google Scholar] [CrossRef]
- Ohlsson, C.; Labrie, F.; Barrett-Connor, E.; Karlsson, M.K.; Ljunggren, Ö.; Vandenput, L.; Mellström, D.; Tivesten, Å. Low Serum Levels of Dehydroepiandrosterone Sulfate Predict All-Cause and Cardiovascular Mortality in Elderly Swedish Men. J. Clin. Endocrinol. Metab. 2010, 95, 4406–4414. [Google Scholar] [CrossRef] [PubMed]
- Rutkowski, K.; Sowa, P.; Rutkowska-Talipska, J.; Kuryliszyn-Moskal, A.; Rutkowski, R. Dehydroepiandrosterone (DHEA): Hypes and Hopes. Drugs 2014, 74, 1195–1207. [Google Scholar] [CrossRef] [PubMed]
- Ceresini, G.; Morganti, S.; Rebecchi, I.; Freddi, M.; Ceda, G.P.; Banchini, A.; Solerte, S.B.; Ferrari, E.; Ablondi, F.; Valenti, G. Evaluation of the Circadian Profiles of Serum Dehydroepiandrosterone (DHEA), Cortisol, and Cortisol/DHEA Molar Ratio after a Single Oral Administration of DHEA in Elderly Subjects. Metabolism 2000, 49, 548–551. [Google Scholar] [CrossRef] [PubMed]
- Anaissie, J.; DeLay, K.J.; Wang, W.; Hatzichristodoulou, G.; Hellstrom, W.J. Testosterone Deficiency in Adults and Corresponding Treatment Patterns across the Globe. Transl. Androl. Urol. 2017, 6, 183–191. [Google Scholar] [CrossRef] [PubMed]
- Dote-Montero, M.; Amaro-Gahete, F.J.; De-la-O, A.; Jurado-Fasoli, L.; Gutierrez, A.; Castillo, M.J. Study of the Association of DHEAS, Testosterone and Cortisol with S-Klotho Plasma Levels in Healthy Sedentary Middle-Aged Adults. Exp. Gerontol. 2019, 121, 55–61. [Google Scholar] [CrossRef]
- Labrie, F.; Martel, C.; Bélanger, A.; Pelletier, G. Androgens in Women Are Essentially Made from DHEA in Each Peripheral Tissue According to Intracrinology. J. Steroid Biochem. Mol. Biol. 2017, 168, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.; Gwenin, C. Cortisol Level Dysregulation and Its Prevalence—Is It Nature’s Alarm Clock? Physiol. Rep. 2021, 8, e14644. [Google Scholar] [CrossRef]
- Samaras, N.; Papadopoulou, M.-A.; Samaras, D.; Ongaro, F. Off-Label Use of Hormones as an Antiaging Strategy: A Review. Clin. Interv. Aging 2014, 9, 1175. [Google Scholar] [CrossRef]
- Dote-Montero, M.; De-la-O, A.; Jurado-Fasoli, L.; Ruiz, J.R.; Castillo, M.J.; Amaro-Gahete, F.J. The Effects of Three Types of Exercise Training on Steroid Hormones in Physically Inactive Middle-Aged Adults: A Randomized Controlled Trial. Eur. J. Appl. Physiol. 2021, 121, 2193–2206. [Google Scholar] [CrossRef] [PubMed]
- Sasaki, N.; Fujiwara, S.; Yamashita, H.; Ozono, R.; Teramen, K.; Kihara, Y. Impact of Sleep on Osteoporosis: Sleep Quality Is Associated with Bone Stiffness Index. Sleep Med. 2016, 25, 73–77. [Google Scholar] [CrossRef] [PubMed]
- Piovezan, R.D.; Abucham, J.; dos Santos, R.V.T.; Mello, M.T.; Tufik, S.; Poyares, D. The Impact of Sleep on Age-Related Sarcopenia: Possible Connections and Clinical Implications. Ageing Res. Rev. 2015, 23, 210–220. [Google Scholar] [CrossRef]
- Beccuti, G.; Pannain, S. Sleep and Obesity. Curr. Opin. Clin. Nutr. Metab. Care 2011, 14, 402–412. [Google Scholar] [CrossRef]
- Penev, P.D. Update on Energy Homeostasis and Insufficient Sleep. J. Clin. Endocrinol. Metab. 2012, 97, 1792–1801. [Google Scholar] [CrossRef]
- Chaput, J.P. Sleep Patterns, Diet Quality and Energy Balance. Physiol. Behav. 2014, 134, 86–91. [Google Scholar] [CrossRef] [PubMed]
- Zuraikat, F.M.; Makarem, N.; Redline, S.; Aggarwal, B.; Jelic, S.; St-Onge, M.-P. Sleep Regularity and Cardiometabolic Heath: Is Variability in Sleep Patterns a Risk Factor for Excess Adiposity and Glycemic Dysregulation? Curr. Diab. Rep. 2020, 20, 38. [Google Scholar] [CrossRef]
- Matricciani, L.; Paquet, C.; Fraysse, F.; Grobler, A.; Wang, Y.; Baur, L.; Juonala, M.; Nguyen, M.T.; Ranganathan, S.; Burgner, D.; et al. Sleep and Cardiometabolic Risk: A Cluster Analysis of Actigraphy-Derived Sleep Profiles in Adults and Children. Sleep 2021, 44, zsab014. [Google Scholar] [CrossRef] [PubMed]
- Besedovsky, L.; Lange, T.; Haack, M. The Sleep-Immune Crosstalk in Health and Disease. Physiol. Rev. 2019, 99, 1325–1380. [Google Scholar] [CrossRef] [PubMed]
- Khosro, S.; Alireza, S.; Omid, A.; Forough, S. Night Work and Inflammatory Markers. Indian J. Occup. Environ. Med. 2011, 15, 38–41. [Google Scholar] [CrossRef] [PubMed]
- Gabryelska, A.; Łukasik, Z.M.; Makowska, J.S.; Białasiewicz, P. Obstructive Sleep Apnea: From Intermittent Hypoxia to Cardiovascular Complications via Blood Platelets. Front. Neurol. 2018, 9, 635. [Google Scholar] [CrossRef] [PubMed]
- Pákó, J.; Kunos, L.; Mészáros, M.; Tárnoki, D.L.; Tárnoki, Á.D.; Horváth, I.; Bikov, A. Decreased Levels of Anti-Aging Klotho in Obstructive Sleep Apnea. Rejuvenation Res. 2019. ahead of print. [Google Scholar] [CrossRef] [PubMed]
- Nakanishi, K.; Nishida, M.; Taneike, M.; Yamamoto, R.; Adachi, H.; Moriyama, T.; Yamauchi-Takihara, K. Implication of Alpha-Klotho as the Predictive Factor of Stress. J. Investig. Med. 2019, 67, 1082–1086. [Google Scholar] [CrossRef] [PubMed]
- Kredlow, M.A.; Capozzoli, M.C.; Hearon, B.A.; Calkins, A.W.; Otto, M.W. The Effects of Physical Activity on Sleep: A Meta-Analytic Review. J. Behav. Med. 2015, 38, 427–449. [Google Scholar] [CrossRef]
- Strand, L.B.; Laugsand, L.E.; Wisløff, U.; Nes, B.M.; Vatten, L.; Janszky, I. Insomnia Symptoms and Cardiorespiratory Fitness in Healthy Individuals: The Nord-Trøndelag Health Study (HUNT). Sleep 2013, 36, 99–108. [Google Scholar] [CrossRef]
- Wang, T.Y.; Wu, Y.; Wang, T.; Li, Y.; Zhang, D. A Prospective Study on the Association of Sleep Duration with Grip Strength among Middle-Aged and Older Chinese. Exp. Gerontol. 2018, 103, 88–93. [Google Scholar] [CrossRef]
- Copinschi, G.; Caufriez, A. Sleep and Hormonal Changes in Aging. Endocrinol. Metab. Clin. N. Am. 2013, 42, 371–389. [Google Scholar] [CrossRef]
- Noël, S. Morbidity of Irregular Work Schedules. Rev. Med. Brux. 2009, 30, 309–317. [Google Scholar] [PubMed]
- Van Cauter, E.; Knutson, K.L. Sleep and the Epidemic of Obesity in Children and Adults. Eur. J. Endocrinol. 2008, 159, S59–S66. [Google Scholar] [CrossRef] [PubMed]
- Van Cauter, E.; Spiegel, K.; Tasali, E.; Leproult, R. Metabolic Consequences of Sleep and Sleep Loss. Sleep Med. 2008, 9, S23–S28. [Google Scholar] [CrossRef] [PubMed]
- Cappuccio, F.P.; D’Elia, L.; Strazzullo, P.; Miller, M.A. Sleep Duration and All-Cause Mortality: A Systematic Review and Meta-Analysis of Prospective Studies. Sleep 2010, 33, 585–592. [Google Scholar] [CrossRef]
- Barrett-Connor, E.; Dam, T.-T.; Stone, K.; Harrison, S.L.; Redline, S.; Orwoll, E. The Association of Testosterone Levels with Overall Sleep Quality, Sleep Architecture, and Sleep-Disordered Breathing. J. Clin. Endocrinol. Metab. 2008, 93, 2602–2609. [Google Scholar] [CrossRef] [PubMed]
- Patel, P.; Shiff, B.; Kohn, T.P.; Ramasamy, R. Impaired Sleep Is Associated with Low Testosterone in US Adult Males: Results from the National Health and Nutrition Examination Survey. World J. Urol. 2019, 37, 1449–1453. [Google Scholar] [CrossRef]
- Burschtin, O.; Wang, J. Testosterone Deficiency and Sleep Apnea. Urol. Clin. N. Am. 2016, 43, 233–237. [Google Scholar] [CrossRef]
- Redwine, L.; Hauger, R.L.; Gillin, J.C.; Irwin, M. Effects of Sleep and Sleep Deprivation on Interleukin-6, Growth Hormone, Cortisol, and Melatonin Levels in Humans 1. J. Clin. Endocrinol. Metab. 2000, 85, 3597–3603. [Google Scholar] [CrossRef]
- Brandenberger, G.; Weibel, L. The 24-h Growth Hormone Rhythm in Men: Sleep and Circadian Influences Questioned. J. Sleep Res. 2004, 13, 251–255. [Google Scholar] [CrossRef]
- Van Cauter, E.; Copinschi, G. Interrelationships between Growthhormone and Sleep. Growth Horm. IGF Res. 2000, 10, S57–S62. [Google Scholar] [CrossRef]
- Asarnow, L.D. Depression and Sleep: What Has the Treatment Research Revealed and Could the HPA Axis Be a Potential Mechanism? Curr. Opin. Psychol. 2020, 34, 112–116. [Google Scholar] [CrossRef] [PubMed]
- van Dalfsen, J.H.; Markus, C.R. The Influence of Sleep on Human Hypothalamic–Pituitary–Adrenal (HPA) Axis Reactivity: A Systematic Review. Sleep Med. Rev. 2018, 39, 187–194. [Google Scholar] [CrossRef] [PubMed]
- Mohammadi, H.; Rezaei, M.; Faghihi, F.; Khazaie, H. Hypothalamic–Pituitary–Gonadal Activity in Paradoxical and Psychophysiological Insomnia. J. Med. Signals Sens. 2019, 9, 59. [Google Scholar] [CrossRef]
- Mohammadi, H.; Rezaei, M.; Sharafkhaneh, A.; Khazaie, H.; Ghadami, M.R. Serum Testosterone/Cortisol Ratio in People with Obstructive Sleep Apnea. J. Clin. Lab. Anal. 2020, 34, e23011. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Piotrowska, K.; Chavoshan, B.; Wallace, J.; Liu, P.Y. Sleep Duration Is Associated With Testis Size in Healthy Young Men. J. Clin. Sleep Med. 2018, 14, 1757–1764. [Google Scholar] [CrossRef]
- Ruge, M.; Skaaby, T.; Andersson, A.-M.; Linneberg, A. Cross-Sectional Analysis of Sleep Hours and Quality with Sex Hormones in Men. Endocr. Connect. 2019, 8, 141–149. [Google Scholar] [CrossRef]
- Bani-Issa, W.; Radwan, H.; Al Marzooq, F.; Al Awar, S.; Al-Shujairi, A.M.; Samsudin, A.R.; Khasawneh, W.; Albluwi, N. Salivary Cortisol, Subjective Stress and Quality of Sleep Among Female Healthcare Professionals. J. Multidiscip. Healthc. 2020, 13, 125–140. [Google Scholar] [CrossRef]
- Jurado-Fasoli, L.; Amaro-Gahete, F.J.; De-la-O, A.; Dote-Montero, M.; Gutiérrez, Á.; Castillo, M.J. Association between Sleep Quality and Body Composition in Sedentary Middle-Aged Adults. Medicina 2018, 54, 91. [Google Scholar] [CrossRef]
- Jurado-Fasoli, L.; Mochon-Benguigui, S.; Castillo, M.J.; Amaro-Gahete, F.J. Association between Sleep Quality and Time with Energy Metabolism in Sedentary Adults. Sci. Rep. 2020, 10, 4598. [Google Scholar] [CrossRef]
- Mochón-Benguigui, S.; Carneiro-Barrera, A.; Castillo, M.J.; Amaro-Gahete, F.J. Is Sleep Associated with the S-Klotho Anti-Aging Protein in Sedentary Middle-Aged Adults? The FIT-AGEING Study. Antioxidants 2020, 9, 738. [Google Scholar] [CrossRef]
- Mochón-Benguigui, S.; Carneiro-Barrera, A.; Castillo, M.J.; Amaro-Gahete, F.J. Role of Physical Activity and Fitness on Sleep in Sedentary Middle-Aged Adults: The FIT-AGEING Study. Sci. Rep. 2021, 11, 539. [Google Scholar] [CrossRef] [PubMed]
- Luboshitzky, R.; Herer, P.; Levi, M.; Shen-Orr, Z.; Lavie, P. Relationship between Rapid Eye Movement Sleep and Testosterone Secretion in Normal Men. J. Androl. 1999, 20, 731–737. [Google Scholar] [CrossRef] [PubMed]
- Van Cauter, E. Age-Related Changes in Slow Wave Sleep and REM Sleep and Relationship With Growth Hormone and Cortisol Levels in Healthy Men. JAMA 2000, 284, 861. [Google Scholar] [CrossRef]
- Saaresranta, T.; Polo, O. Sleep-Disordered Breathing and Hormones. Eur. Respir. J. 2003, 22, 161–172. [Google Scholar] [CrossRef]
- Brandenberger, G.; Gronfier, C.; Chapotot, F.; Simon, C.; Piquard, F. Effect of Sleep Deprivation on Overall 24 h Growth-Hormone Secretion. Lancet 2000, 356, 1408. [Google Scholar] [CrossRef]
- Nollet, M.; Wisden, W.; Franks, N.P. Sleep Deprivation and Stress: A Reciprocal Relationship. Interface Focus 2020, 10, 20190092. [Google Scholar] [CrossRef]
- Kanikowska, D.; Roszak, M.; Rutkowski, R.; Sato, M.; Sikorska, D.; Orzechowska, Z.; Bręborowicz, A.; Witowski, J. Seasonal Differences in Rhythmicity of Salivary Cortisol in Healthy Adults. J. Appl. Physiol. 2019, 126, 764–770. [Google Scholar] [CrossRef]
- Kruisbrink, M.; Robertson, W.; Ji, C.; Miller, M.A.; Geleijnse, J.M.; Cappuccio, F.P. Association of Sleep Duration and Quality with Blood Lipids: A Systematic Review and Meta-Analysis of Prospective Studies. BMJ Open 2017, 7, e018585. [Google Scholar] [CrossRef]
- Song, M.J.; Kim, J.H. Family Caregivers of People with Dementia Have Poor Sleep Quality: A Nationwide Population-Based Study. Int. J. Environ. Res. Public Health 2021, 18, 13079. [Google Scholar] [CrossRef]
- Buysse, D.J.; Hall, M.L.; Strollo, P.J.; Kamarck, T.W.; Owens, J.; Lee, L.; Reis, S.E.; Matthews, K.A. Relationships between the Pittsburgh Sleep Quality Index (PSQI), Epworth Sleepiness Scale (ESS), and Clinical/Polysomnographic Measures in a Community Sample. J. Clin. Sleep Med. 2008, 4, 563–571. [Google Scholar] [CrossRef] [PubMed]
- Berger, I.; Obeid, J.; Timmons, B.W.; DeMatteo, C. Exploring Accelerometer Versus Self-Report Sleep Assessment in Youth With Concussion. Glob. Pediatr. Health 2017, 4, 2333794X1774597. [Google Scholar] [CrossRef] [PubMed]
- Sadeh, A. The Role and Validity of Actigraphy in Sleep Medicine: An Update. Sleep Med. Rev. 2011, 15, 259–267. [Google Scholar] [CrossRef] [PubMed]
- Goelema, M.S.; Regis, M.; Haakma, R.; van den Heuvel, E.R.; Markopoulos, P.; Overeem, S. Determinants of Perceived Sleep Quality in Normal Sleepers. Behav. Sleep Med. 2019, 17, 388–397. [Google Scholar] [CrossRef] [PubMed]
- Amaro-Gahete, F.J.; De-la-O, A.; Jurado-Fasoli, L.; Espuch-Oliver, A.; Robles-Gonzalez, L.; Navarro-Lomas, G.; de Haro, T.; Femia, P.; Castillo, M.J.; Gutierrez, A. Exercise Training as S-Klotho Protein Stimulator in Sedentary Healthy Adults: Rationale, Design, and Methodology. Contemp. Clin. Trials Commun. 2018, 11, 10–19. [Google Scholar] [CrossRef] [PubMed]
- WHO Obesidad y Sobrepeso. Available online: https://www.who.int/es/news-room/fact-sheets/detail/obesity-and-overweight (accessed on 17 June 2022).
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A New Instrument for Psychiatric Practice and Research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef] [PubMed]
- Migueles, J.H.; Cadenas-Sanchez, C.; Ekelund, U.; Delisle Nyström, C.; Mora-Gonzalez, J.; Löf, M.; Labayen, I.; Ruiz, J.R.; Ortega, F.B. Accelerometer Data Collection and Processing Criteria to Assess Physical Activity and Other Outcomes: A Systematic Review and Practical Considerations. Sport. Med. 2017, 47, 1821–1845. [Google Scholar] [CrossRef]
- van Hees, V.T.; Fang, Z.; Langford, J.; Assah, F.; Mohammad, A.; da Silva, I.C.M.; Trenell, M.I.; White, T.; Wareham, N.J.; Brage, S. Autocalibration of Accelerometer Data for Free-Living Physical Activity Assessment Using Local Gravity and Temperature: An Evaluation on Four Continents. J. Appl. Physiol. 2014, 117, 738–744. [Google Scholar] [CrossRef] [PubMed]
- van Hees, V.T.; Sabia, S.; Anderson, K.N.; Denton, S.J.; Oliver, J.; Catt, M.; Abell, J.G.; Kivimäki, M.; Trenell, M.I.; Singh-Manoux, A. A Novel, Open Access Method to Assess Sleep Duration Using a Wrist-Worn Accelerometer. PLoS ONE 2015, 10, e0142533. [Google Scholar] [CrossRef]
- Shrivastava, D.; Jung, S.; Saadat, M.; Sirohi, R.; Crewson, K. How to Interpret the Results of a Sleep Study. J. Community Hosp. Intern. Med. Perspect. 2014, 4, 24983. [Google Scholar] [CrossRef] [PubMed]
- Vermeulen, A.; Verdonck, L.; Kaufman, J.M. A Critical Evaluation of Simple Methods for the Estimation of Free Testosterone in Serum. J. Clin. Endocrinol. Metab. 1999, 84, 3666–3672. [Google Scholar] [CrossRef]
- Edwards, B.; O’Driscoll, D.; Ali, A.; Jordan, A.; Trinder, J.; Malhotra, A. Aging and Sleep: Physiology and Pathophysiology. Semin. Respir. Crit. Care Med. 2010, 31, 618–633. [Google Scholar] [CrossRef] [PubMed]
- Carneiro-Barrera, A.; Amaro-Gahete, F.J.; Acosta, F.M.; Ruiz, J.R. Body Composition Impact on Sleep in Young Adults: The Mediating Role of Sedentariness, Physical Activity, and Diet. J. Clin. Med. 2020, 9, 1560. [Google Scholar] [CrossRef] [PubMed]
- Sidhu, S.; Parikh, T.; Burman, K.D. Endocrine Changes in Obesity. In Perioperative Anesthetic Care of the Obese Patient; CRC Press: Boca Raton, FL, USA, 2016; pp. 51–59. [Google Scholar]
| N | All | N | Men | N | Women | ||||
|---|---|---|---|---|---|---|---|---|---|
| Age (years) | 74 | 53.66 | (5.14) | 35 | 54.39 | (5.27) | 39 | 53.01 | (5.00) |
| Anthropometry and body composition | |||||||||
| Height (cm) | 74 | 167.8 | (9.81) | 35 | 175.8 | (6.48) | 39 | 160.7 | (6.10) * |
| Weight (kg) | 74 | 75.73 | (14.98) | 35 | 87.38 | (10.95) | 39 | 65.28 | (9.32) * |
| Body mass index (kg/m2) | 74 | 26.72 | (3.76) | 35 | 28.32 | (3.61) | 39 | 25.27 | (3.31) * |
| Fat mass index (kg/m2) | 74 | 10.75 | (3.13) | 35 | 10.03 | (3.23) | 39 | 11.39 | (2.93) |
| Lean mass index (kg/m2) | 74 | 15.21 | (2.88) | 35 | 17.49 | (2.02) | 39 | 13.17 | (1.80) * |
| Hormones | |||||||||
| DHEAS (μg/dL) | 73 | 109.8 | (66.95) | 34 | 135.1 | (66.45) | 39 | 87.74 | (59.87) * |
| Free testosterone (ng/dL) | 73 | 3.40 | (3.50) | 34 | 6.37 | (2.37) | 39 | 0.81 | (1.90) * |
| Total testosterone (ng/dL) | 73 | 182.0 | (182.6) | 34 | 342.1 | (128.8) | 39 | 42.44 | (76.66) * |
| SHBG (nmol/L) | 73 | 47.02 | (23.76) | 34 | 35.79 | (16.36) | 39 | 56.81 | (25.01) * |
| Somatotropin (ng/mL) | 73 | 1.44 | (2.54) | 34 | 0.60 | (1.77) | 39 | 2.17 | (2.88) * |
| Cortisol (μg/dL) | 73 | 12.86 | (4.18) | 34 | 13.43 | (4.49) | 39 | 12.36 | (3.87) |
| Sleep quantity and quality | |||||||||
| Global PSQI score | 67 | 5.61 | (3.47) | 31 | 4.77 | (3.15) | 36 | 6.33 | (3.62) |
| Total sleep time (min) | 71 | 359.9 | (48.85) | 34 | 337.9 | (46.30) | 37 | 380.1 | (42.44) * |
| Wake after sleep onset (min) | 71 | 63.90 | (27.44) | 34 | 65.80 | (32.45) | 37 | 62.15 | (22.19) |
| Sleep efficiency (%) | 71 | 85.01 | (6.29) | 34 | 83.88 | (7.53) | 37 | 86.06 | (4.75) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mochón-Benguigui, S.; Carneiro-Barrera, A.; Dote-Montero, M.; Castillo, M.J.; Amaro-Gahete, F.J. Sleep and Anabolic/Catabolic Hormonal Profile in Sedentary Middle-Aged Adults: The FIT-AGEING Study. Int. J. Mol. Sci. 2022, 23, 14709. https://doi.org/10.3390/ijms232314709
Mochón-Benguigui S, Carneiro-Barrera A, Dote-Montero M, Castillo MJ, Amaro-Gahete FJ. Sleep and Anabolic/Catabolic Hormonal Profile in Sedentary Middle-Aged Adults: The FIT-AGEING Study. International Journal of Molecular Sciences. 2022; 23(23):14709. https://doi.org/10.3390/ijms232314709
Chicago/Turabian StyleMochón-Benguigui, Sol, Almudena Carneiro-Barrera, Manuel Dote-Montero, Manuel J. Castillo, and Francisco J. Amaro-Gahete. 2022. "Sleep and Anabolic/Catabolic Hormonal Profile in Sedentary Middle-Aged Adults: The FIT-AGEING Study" International Journal of Molecular Sciences 23, no. 23: 14709. https://doi.org/10.3390/ijms232314709
APA StyleMochón-Benguigui, S., Carneiro-Barrera, A., Dote-Montero, M., Castillo, M. J., & Amaro-Gahete, F. J. (2022). Sleep and Anabolic/Catabolic Hormonal Profile in Sedentary Middle-Aged Adults: The FIT-AGEING Study. International Journal of Molecular Sciences, 23(23), 14709. https://doi.org/10.3390/ijms232314709








