ThymicPeptides Reverse Immune Exhaustion in Patients with Reactivated Human Alphaherpesvirus1 Infections
Abstract
1. Introduction
2. Results
2.1. Participants
2.2. Frequencies of Basic Lymphocyte Subsets in Patients with Reactivated HHV-1 Infections and Controls
2.3. Frequencies of CD25+, PD-1+, and PD-L1+ T and B Lymphocytes in Patients with Reactivated HHV-1 Infections and Controls
2.4. Frequencies of PD-1+ and PD-L1+ B and T Lymphocytes in Patients with Reactivated HHV-1 Infections before and after 2 Months of Thymostimulin Therapy
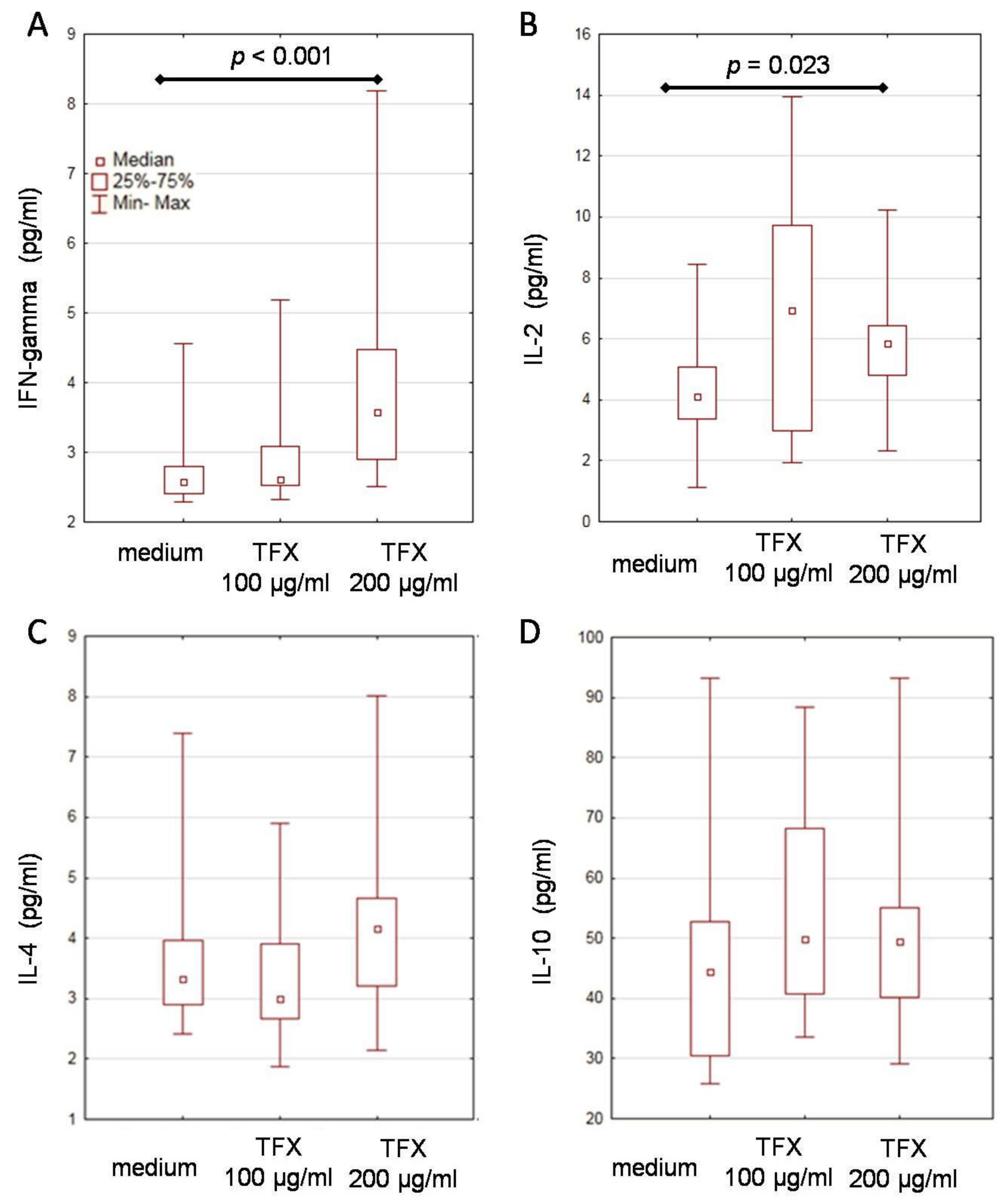
2.5. Stimulation of PBMCs with Thymic Peptides in Patients with Reactivated HHV-1 Infections
3. Discussion
4. Materials and Methods
4.1. Patients with Reactivated HHV-1 Infections and the Control Group
4.2. Material
4.3. Immunophenotyping
4.4. Cytokine Secretion in Cultures of PBMCs Stimulated with Thymic Peptides
4.5. Measurement of the Concentrations of IFN-γ, IL-2, IL-4, IL-10, anti-HHV-1 IgM Antibodies, anti-HHV-1 IgG Antibodies, anti-HHV-2 IgM Antibodies, and anti-HHV-2 IgG Antibodies
4.6. Statistical Analysis
5. Conclusions
Smentary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| APC | antigen-presenting cells |
| CTLA-4 | cytolytic T-lymphocyte antigen-4 |
| ELISA | enzyme-linked immunosorbent assay |
| HHV-1 | human alphaherpesvirus 1 |
| IFN-γ | interferon gamma |
| IL | interleukin |
| LAG-3 | lymphocyte activation gene-3 |
| NK | natural killer cell |
| NKT-like | natural killer T-like cell |
| PBMC | peripheral blood mononuclear cells |
| PD-1 | Programmed cell death protein 1 |
| PD-L1 | programmed death ligand 1 |
| SD | standard deviation |
| TFX | thymostimulinum |
| Th | T helper cells |
| TIM-3 | T-cell immunoglobulin mucin-containing domain-3 |
| TNF-α | tumor necrosis factor alpha |
| TRAIL | tumor necrosis-factor-related apoptosis-inducing ligand |
References
- Denes, C.E.; Miranda-Saksena, M.; Cunningham, A.L.; Diefenbach, R.J. Cytoskeletons in the Closet—Subversion in Alphaherpesvirus Infections. Viruses 2018, 10, 79. [Google Scholar] [CrossRef] [PubMed]
- Schulte, J.M.; Bellamy, A.R.; Hook, E.W.; Bernstein, D.I.; Levin, M.J.; Leone, P.A.; Sokol-Anderson, M.L.; Ewell, M.G.; Wolff, P.A.; Heineman, T.C.; et al. HSV-1 and HSV-2 Seroprevalence in the United States among Asymptomatic Women Unaware of Any Herpes Simplex Virus Infection (Herpevac Trial for Women). South. Med. J. 2014, 107, 79–84. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Wang, X.-H.; Luo, Z.; Liu, L.-F.; Yan, C.; Yan, C.-Y.; Chen, G.-D.; Gao, H.; Duan, W.-J.; Kurihara, H.; et al. Traditional Chinese Medicine as a Potential Source for HSV-1 Therapy by Acting on Virus or the Susceptibility of Host. Int. J. Mol. Sci. 2018, 19, 3266. [Google Scholar] [CrossRef] [PubMed]
- Roy, M.; Lebeau, L.; Chessa, C.; Damour, A.; Ladram, A.; Oury, B.; Boutolleau, D.; Bodet, C.; Lévêque, N. Comparison of Anti-Viral Activity of Frog Skin Anti-Microbial Peptides Temporin-Sha and [K3]SHa to LL-37 and Temporin-Tb against Herpes Simplex Virus Type 1. Viruses 2019, 11, 77. [Google Scholar] [CrossRef]
- Sharifi-Rad, J.; Iriti, M.; Setzer, W.N.; Sharifi-Rad, M.; Roointan, A.; Salehi, B. Antiviral activity of Veronica persica Poir. on herpes virus infection. Cell. Mol. Biol. 2018, 64, 11–17. [Google Scholar] [CrossRef]
- Egan, K.P.; Wu, S.; Wigdahl, B.; Jennings, S.R. Immunological control of herpes simplex virus infections. J. Neurovirol. 2013, 19, 328–345. [Google Scholar] [CrossRef]
- Blackburn, S.D.; Crawford, A.; Shin, H.; Polley, A.; Freeman, G.J.; Wherry, E.J. Tissue-Specific Differences in PD-1 and PD-L1 Expression during Chronic Viral Infection: Implications for CD8 T-Cell Exhaustion. J. Virol. 2010, 84, 2078–2089. [Google Scholar] [CrossRef]
- Griffin, J.; Moulton, M.; Elmezayen, R.; Moorman, J. Negative Immunomodulators–Blunting Immunostimulation and Facilitating Infection. In Immune Response Activation; InTech: London, UK, 2014. [Google Scholar]
- Keir, M.E.; Butte, M.J.; Freeman, G.J.; Sharpe, A.H. PD-1 and Its Ligands in Tolerance and Immunity. Annu. Rev. Immunol. 2008, 26, 677–704. [Google Scholar] [CrossRef]
- Goldstein, A.L. History of the Discovery of the Thymosins. Ann. N. Y. Acad. Sci. 2007, 1112, 1–13. [Google Scholar] [CrossRef]
- Tuthill, C.; Rios, I.; McBeath, R. Thymosin alpha 1: Past clinical experience and future promise. Ann. N. Y. Acad. Sci. 2010, 1194, 130–135. [Google Scholar] [CrossRef]
- Mamedov, M.K.; Safarova, S.M.; Dadasheva, A.E. Impact of thymosin-alpha1 on reproduction of herpes simplex virus in cell system and on course of acute experimental infection in mice. Georgian Med. News 2012, 71–75. [Google Scholar]
- Li, J.; Liu, C.H.; Wang, F.S. Thymosin alpha 1: Biological activities, applications and genetic engineering production. Peptides 2010, 31, 2151–2158. [Google Scholar] [CrossRef] [PubMed]
- Matteucci, C.; Minutolo, A.; Sinibaldi-Vallebona, P.; Palamara, A.T.; Rasi, G.; Mastino, A.; Garaci, E. Transcription profile of human lymphocytes following in vitro treatment with thymosin alpha-1. Ann. N. Y. Acad. Sci. 2010, 1194, 6–19. [Google Scholar] [CrossRef] [PubMed]
- Robert, S.; King, C.W.T. Thymosin Apha 1–A Peptide Immune Modulator with a Broad Range of Clinical Applications. Clin. Exp. Pharmacol. 2013, 03, 133. [Google Scholar]
- Reddy, M.; Eirikis, E.; Davis, C.; Davis, H.M.; Prabhakar, U. Comparative analysis of lymphocyte activation marker expression and cytokine secretion profile in stimulated human peripheral blood mononuclear cell cultures: An in vitro model to monitor cellular immune function. J. Immunol. Methods 2004, 293, 127–142. [Google Scholar] [CrossRef]
- Macleod, B.L.; Bedoui, S.; Hor, J.L.; Mueller, S.N.; Russell, T.A.; Hollett, N.A.; Heath, W.R.; Tscharke, D.C.; Brooks, A.G.; Gebhardt, T. Distinct APC Subtypes Drive Spatially Segregated CD4+ and CD8+ T-Cell Effector Activity during Skin Infection with HSV-1. PLoS Pathog. 2014, 10, e1004303. [Google Scholar] [CrossRef]
- Jeon, S.; St Leger, A.J.; Cherpes, T.L.; Sheridan, B.S.; Hendricks, R.L. PD-L1/B7-H1 regulates the survival but not the function of CD8+ T cells in herpes simplex virus type 1 latently infected trigeminal ganglia. J. Immunol. 2013, 190, 6277–6286. [Google Scholar] [CrossRef]
- Kahan, S.M.; Wherry, E.J.; Zajac, A.J. T cell exhaustion during persistent viral infections. Virology 2015, 479–480, 180–193. [Google Scholar] [CrossRef]
- Miranda-Saksena, M.; Denes, C.E.; Diefenbach, R.J.; Cunningham, A.L. Infection and Transport of Herpes Simplex Virus Type 1 in Neurons: Role of the Cytoskeleton. Viruses 2018, 10, 92. [Google Scholar] [CrossRef]
- Khan, A.A.; Srivastava, R.; Chentoufi, A.A.; Geertsema, R.; Thai, N.T.U.; Dasgupta, G.; Osorio, N.; Kalantari, M.; Nesburn, A.B.; Wechsler, S.L.; et al. Therapeutic Immunization with a Mixture of Herpes Simplex Virus 1 Glycoprotein D-Derived “Asymptomatic” Human CD8+ T-Cell Epitopes Decreases Spontaneous Ocular Shedding in Latently Infected HLA Transgenic Rabbits: Association with Low Frequency of Local PD-1+ TIM-3+ CD8+ Exhausted T Cells. J. Virol. 2015, 89, 6619–6632. [Google Scholar]
- Crawford, A.; Wherry, E.J. The diversity of costimulatory and inhibitory receptor pathways and the regulation of antiviral T cell responses. Curr. Opin. Immunol. 2009, 21, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Torti, N.; Oxenius, A. T cell memory in the context of persistent herpes viral infections. Viruses 2012, 4, 1116–1143. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Wu, S.; Wang, Y.; Pan, S.; Lan, B.; Liu, Y.; Zhang, L.; Leng, Q.; Chen, D.; Zhang, C.; et al. The Us3 Protein of Herpes Simplex Virus 1 Inhibits T Cell Signaling by Confining Linker for Activation of T Cells (LAT) Activation via TRAF6 Protein. J. Biol. Chem. 2015, 290, 15670–15678. [Google Scholar] [CrossRef]
- Mott, K.R.; Bresee, C.J.; Allen, S.J.; BenMohamed, L.; Wechsler, S.L.; Ghiasi, H. Level of herpes simplex virus type 1 latency correlates with severity of corneal scarring and exhaustion of CD8+ T cells in trigeminal ganglia of latently infected mice. J. Virol. 2009, 83, 2246–2254. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Chung, Y.; Bishop, C.; Daugherty, B.; Chute, H.; Holst, P.; Kurahara, C.; Lott, F.; Sun, N.; Welcher, A.A.; et al. Regulation of T cell activation and tolerance by PDL2. Proc. Natl. Acad. Sci. USA 2006, 103, 11695–11700. [Google Scholar] [CrossRef]
- Latchman, Y.E.; Liang, S.C.; Wu, Y.; Chernova, T.; Sobel, R.A.; Klemm, M.; Kuchroo, V.K.; Freeman, G.J.; Sharpe, A.H. PD-L1-deficient mice show that PD-L1 on T cells, antigen-presenting cells, and host tissues negatively regulates T cells. Proc. Natl. Acad. Sci. USA 2004, 101, 10691–10696. [Google Scholar] [CrossRef]
- Gianchecchi, E.; Delfino, D.V.; Fierabracci, A. Recent insights into the role of the PD-1/PD-L1 pathway in immunological tolerance and autoimmunity. Autoimmun. Rev. 2013, 12, 1091–1100. [Google Scholar] [CrossRef]
- Brown, J.A.; Dorfman, D.M.; Ma, F.-R.; Sullivan, E.L.; Munoz, O.; Wood, C.R.; Greenfield, E.A.; Freeman, G.J. Blockade of Programmed Death-1 Ligands on Dendritic Cells Enhances T Cell Activation and Cytokine Production. J. Immunol. 2003, 170, 1257–1266. [Google Scholar] [CrossRef]
- Sharpe, A.H.; Wherry, E.J.; Ahmed, R.; Freeman, G.J. The function of programmed cell death 1 and its ligands in regulating autoimmunity and infection. Nat. Immunol. 2007, 8, 239–245. [Google Scholar] [CrossRef]
- Antoine, P.; Olislagers, V.; Huygens, A.; Lecomte, S.; Liesnard, C.; Donner, C.; Marchant, A. Functional Exhaustion of CD4+ T Lymphocytes during Primary Cytomegalovirus Infection. J. Immunol. 2012, 189, 2665–2672. [Google Scholar] [CrossRef]
- Shankar, E.M.; Che, K.F.; Messmer, D.; Lifson, J.D.; Larsson, M. Expression of a Broad Array of Negative Costimulatory Molecules and Blimp-1 in T Cells following Priming by HIV-1 Pulsed Dendritic Cells. Mol. Med. 2011, 17, 229–240. [Google Scholar] [CrossRef] [PubMed]
- Barathan, M.; Mohamed, R.; Vadivelu, J.; Chang, L.Y.; Vignesh, R.; Krishnan, J.; Sigamani, P.; Saeidi, A.; Ram, M.R.; Velu, V.; et al. CD8+ T cells of chronic HCV-infected patients express multiple negative immune checkpoints following stimulation with HCV peptides. Cell. Immunol. 2017, 313, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Saeidi, A.; Zandi, K.; Cheok, Y.Y.; Saeidi, H.; Wong, W.F.; Lee, C.Y.Q.; Cheong, H.C.; Yong, Y.K.; Larsson, M.; Shankar, E.M. T-Cell Exhaustion in Chronic Infections: Reversing the State of Exhaustion and Reinvigorating Optimal Protective Immune Responses. Front. Immunol. 2018, 9, 2569. [Google Scholar] [CrossRef] [PubMed]
- Saeidi, A.; Tien Tien, V.L.; Al-Batran, R.; Al-Darraji, H.A.; Tan, H.Y.; Yong, Y.K.; Ponnampalavanar, S.; Barathan, M.; Rukumani, D.V.; Ansari, A.W.; et al. Attrition of TCR Vα7.2+ CD161++ MAIT Cells in HIV-Tuberculosis Co-Infection Is Associated with Elevated Levels of PD-1 Expression. PLoS ONE 2015, 10, e0124659. [Google Scholar] [CrossRef] [PubMed]
- Yong, Y.K.; Saeidi, A.; Tan, H.Y.; Rosmawati, M.; Enström, P.F.; Al Batran, R.; Vasuki, V.; Chattopadhyay, I.; Murugesan, A.; Vignesh, R.; et al. Hyper-Expression of PD-1 Is Associated with the Levels of Exhausted and Dysfunctional Phenotypes of Circulating CD161++TCR iVα7.2+ Mucosal-Associated Invariant T Cells in Chronic Hepatitis B Virus Infection. Front. Immunol. 2018, 9, 472. [Google Scholar] [CrossRef]
- Matteucci, C.; Minutolo, A.; Pollicita, M.; Balestrieri, E.; Grelli, S.; D’Ettorre, G.; Vullo, V.; Bucci, I.; Luchini, A.; Aquaro, S.; et al. Thymosin α1 potentiates the release by CD8+ cells of soluble factors able to inhibit HIV-1 and human T lymphotropic virus 1 infection in vitro. Expert Opin. Biol. Ther. 2015, 15, 83–100. [Google Scholar] [CrossRef]
- Pierluigi, B.; D’Angelo, C.; Fallarino, F.; Moretti, S.; Zelante, T.; Bozza, S.; De Luca, A.; Bistoni, F.; Garaci, E.; Romani, L. Thymosin α1: The regulator of regulators? Ann. N. Y. Acad. Sci. 2010, 1194, 1–5. [Google Scholar] [CrossRef]
- Jiang, Y.-F.; Ma, Z.-H.; Zhao, P.-W.; Pan, Y.; Liu, Y.-Y.; Feng, J.-Y.; Niu, J.-Q. Effect of Thymosin-α 1 on T-helper 1 Cell and T-helper 2 Cell Cytokine Synthesis in Patients with Hepatitis B Virus e Antigen-positive Chronic Hepatitis B. J. Int. Med. Res. 2010, 38, 2053–2062. [Google Scholar] [CrossRef]
- Decman, V.; Kinchington, P.R.; Harvey, S.A.K.; Hendricks, R.L. Gamma Interferon Can Block Herpes Simplex Virus Type 1 Reactivation from Latency, Even in the Presence of Late Gene Expression. J. Virol. 2005, 79, 10339–10347. [Google Scholar] [CrossRef]
- Pellegatta, S.; Di Ianni, N.; Pessina, S.; Paterra, R.; Anghileri, E.; Eoli, M.; Finocchiaro, G. ABCC3 Expressed by CD56dim CD16+ NK Cells Predicts Response in Glioblastoma Patients Treated with Combined Chemotherapy and Dendritic Cell Immunotherapy. Int. J. Mol. Sci. 2019, 20, 5886. [Google Scholar] [CrossRef]
- Korona-Glowniak, I.; Grywalska, E.; Grzegorczyk, A.; Roliński, J.; Glowniak, A.; Malm, A. Bacterial Colonization in Patients with Chronic Lymphocytic Leukemia and Factors Associated with Infections and Colonization. J. Clin. Med. 2019, 8, 861. [Google Scholar] [CrossRef] [PubMed]
| Variable | Statistics | Patients (n = 50) | Controls (n = 20) |
|---|---|---|---|
| Age (years) | median (min–max) | 40.05 (19–66) | 44 (18–69) |
| mean ± SD | 41.21 ± 12.42 | 42.87 ± 15.81 | |
| anti-HHV-1IgM, n (%) | Yes | 8 (16%) | 0 |
| No | 42 (84%) | 20 (100%) | |
| anti-HHV-1 IgM, U/mL | median (min–max) | 27.72 (12.11–62.7) | - |
| mean ± SD | 27.45 ± 18.33 | - | |
| anti-HHV-1IgG, n (%) | Yes | 50 (100%) | 0 |
| No | 0 | 20 (100%) | |
| anti-HHV-1 IgG, U/mL | median (min–max) | 70.62 (22.41–1701.82) | - |
| mean ± SD | 167.09 ± 301.18 | - | |
| anti-HHV-2IgM, n (%) | Yes | 0 | 0 |
| No | 50 (100%) | 20 (100%) | |
| anti- HHV-2 IgG, n (%) | Yes | 0 | 0 |
| No | 50 (100%) | 20 (100%) |
| Variable | Patients with Reactivated HHV-1 Infections (n = 50) | Control Group (n = 20) | p (Patients before TFX vs. Controls) | p (Patients before vs. after TFX) | ||
|---|---|---|---|---|---|---|
| before TFX | after TFX | |||||
| CD3+ T lymphocytes (%) | median (min–max) | 69.62 (62.55–74.97) | 73.66 (62.23-83.19) | 71.94 (61.61–74.53) | NS | 0.001 |
| mean ± SD | 69.31 ± 3.35 | 73.31 ± 4.29 | 70.44 ± 3.53 | |||
| CD19+ B lymphocytes (%) | median (min–max) | 10.44 (6.12–16.96) | 15.31 (0.29–19.46) | 13.62 (8.69–16.88) | 0.002 | <0.001 |
| mean ± SD | 10.60 ± 3.22 | 13.95 ± 4.12 | 13.33 ± 2.46 | |||
| CD4+CD3+ T lymphocytes (%) | median (min–max) | 39.16 (25.19–59.88) | 40.25 (23.07–55.45) | 38.34 (33.40–57.43) | NS | NS |
| mean ± SD | 39.92 ± 6.62 | 38.76 ± 9.36 | 41.06 ± 6.36 | |||
| CD8+CD3+ T lymphocytes (%) | median (min–max) | 29.42 (11.17–49.29) | 28.81 (9.01–52.22) | 27.71 (12.78–37.16) | NS | NS |
| mean ± SD | 28.62 ± 7.07 | 31.04 ± 11.35 | 28.48 ± 6.10 | |||
| CD4+CD3+/CD8+CD3+ ratio | median (min–max) | 1.29 (0.51–4.86) | 1.49 (0.50–6.15) | 1.34 (0.92–4.49) | NS | NS |
| mean ± SD | 1.58 ± 0.84 | 1.57 ± 1.04 | 1.58 ± 0.79 | |||
| NK cells (%) | median (min–max) | 17.77 (10.16–27.72) | 10.19 (3.43–18.56) | 14.26 (9.16–24.08) | 0.025 | <0.001 |
| mean ± SD | 17.51 ± 3.85 | 10.30 ± 3.96 | 15.09 ± 4.42 | |||
| NKT-like cells (%) | median (min–max) | 4.19 (0.84–16.06) | 4.31 (0.91–17.83) | 3.29 (1.86–4.91) | 0.048 | NS |
| mean ± SD | 5.21 ± 3.35 | 5.43 ± 3.33 | 3.30 ± 1.02 | |||
| T regulatory cells (CD4+CD25+ FOXP3) (%) | median (min–max) | 6.61 (3.13–16.85) | 6.63 (3.11–13.66) | 4.26 (3.23–7.45) | <0.001 | 0.020 |
| mean ± SD | 8.32 ± 3.82 | 7.10 ± 2.72 | 4.45 ± 1.06 | |||
| Variable | Patients with Reactivated HHV-1 Infections before TFX (n = 50) | Control Group (n = 20) | p | |
|---|---|---|---|---|
| CD3+CD25+ T lymphocytes | median (min–max) | 46.71(26.99–68.01) | 37.06(18.65–47.13) | <0.001 |
| mean ± SD | 47.17 ± 10.15 | 35.23 ± 8.33 | ||
| CD19+CD25+ B lymphocytes | median (min–max) | 36.00(16.05–58.87) | 18.64(10.88–27.50) | <0.001 |
| mean ± SD | 36.59 ± 11.10 | 18.29 ± 4.16 | ||
| CD4+CD25+ T lymphocytes | median (min–max) | 46.12(28.49–75.50) | 35.79(30.64–47.50) | <0.001 |
| mean ± SD | 49.01 ± 10.50 | 36.11 ± 3.97 | ||
| CD19+PD-1+ B lymphocytes | median (min–max) | 6.35(1.91–25.47) | 2.94(0.5–5.45) | <0.001 |
| mean ± SD | 8.44 ± 5.99 | 3.05 ± 1.36 | ||
| CD4+PD-1+ T lymphocytes | median (min–max) | 21.24(8.17–78.51) | 8.73(6.19–11.34) | <0.001 |
| mean ± SD | 25.03 ± 12.98 | 8.37 ± 1.46 | ||
| CD8+PD-1+ T lymphocytes | median (min–max) | 17.73(8.40–40.73) | 7.23(5.01–10.11) | <0.001 |
| mean ± SD | 19.42 ± 7.34 | 7.32 ± 1.62 | ||
| CD19+PD-L1+B lymphocytes | median (min–max) | 3.34(0.71–23.95) | 2.39(0.12–4.70) | 0.044 |
| mean ± SD | 5.48 ± 5.23 | 2.33 ± 1.24 | ||
| CD4+PD-L1+ T lymphocytes | median (min–max) | 14.67(6.78–63.81) | 8.37(2.58–13.31) | <0.001 |
| mean ± SD | 19.21 ± 12.78 | 7.99 ± 2.37 | ||
| CD8+PD-L1+ T lymphocytes | median (min–max) | 11.43(2.35–33.67) | 3.34(0.71–23.95) | <0.001 |
| mean ± SD | 12.39 ± 6.80 | 3.36 ± 1.24 | ||
| Variable | Before TFX (n = 50) | After TFX (n = 50) | p | |
|---|---|---|---|---|
| CD19+PD-1+ B lymphocytes | median (min–max) | 6.35(1.91–25.47) | 3.42 (0.83–14.36) | <0.001 |
| mean ± SD | 8.44 ± 5.99 | 4.60 ± 3.37 | ||
| CD4+PD-1+ T lymphocytes | median (min–max) | 21.24(8.17–78.51) | 8.1 (1.14–27.96) | <0.001 |
| mean ± SD | 25.03 ± 12.98 | 11.13 ± 7.9 | ||
| CD8+PD-1+ T lymphocytes | median (min–max) | 17.73(8.40–40.73) | 8.81(2.18–27.8) | <0.001 |
| mean ± SD | 19.42 ± 7.34 | 8.96 ± 5.14 | ||
| CD19+PD-L1+ B lymphocytes | median (min–max) | 3.34(0.71–23.95) | 4.42(0.61–9.86) | NS |
| mean ± SD | 5.48 ± 5.23 | 4.57 ± 2.60 | ||
| CD4+PD-L1+ T lymphocytes | median (min–max) | 14.67(6.78–63.81) | 7.67(1.45–23.99) | <0.001 |
| mean ± SD | 19.21 ± 12.78 | 8.23 ± 4.98 | ||
| CD8+PD-L1+ T lymphocytes | median (min–max) | 11.43(2.35–33.67) | 3.44(0.82–17.35) | <0.001 |
| mean ± SD | 12.39 ± 6.80 | 4.97 ± 3.55 | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hymos, A.; Grywalska, E.; Klatka, J.; Klatka, M.; Korona-Głowniak, I.; Roliński, J. ThymicPeptides Reverse Immune Exhaustion in Patients with Reactivated Human Alphaherpesvirus1 Infections. Int. J. Mol. Sci. 2020, 21, 2379. https://doi.org/10.3390/ijms21072379
Hymos A, Grywalska E, Klatka J, Klatka M, Korona-Głowniak I, Roliński J. ThymicPeptides Reverse Immune Exhaustion in Patients with Reactivated Human Alphaherpesvirus1 Infections. International Journal of Molecular Sciences. 2020; 21(7):2379. https://doi.org/10.3390/ijms21072379
Chicago/Turabian StyleHymos, Anna, Ewelina Grywalska, Janusz Klatka, Maria Klatka, Izabela Korona-Głowniak, and Jacek Roliński. 2020. "ThymicPeptides Reverse Immune Exhaustion in Patients with Reactivated Human Alphaherpesvirus1 Infections" International Journal of Molecular Sciences 21, no. 7: 2379. https://doi.org/10.3390/ijms21072379
APA StyleHymos, A., Grywalska, E., Klatka, J., Klatka, M., Korona-Głowniak, I., & Roliński, J. (2020). ThymicPeptides Reverse Immune Exhaustion in Patients with Reactivated Human Alphaherpesvirus1 Infections. International Journal of Molecular Sciences, 21(7), 2379. https://doi.org/10.3390/ijms21072379






