Updates on the Risk of Neuropsychiatric and Gastrointestinal Comorbidities in Rosacea and Its Possible Relationship with the Gut–Brain–Skin Axis
Abstract
:1. Introduction
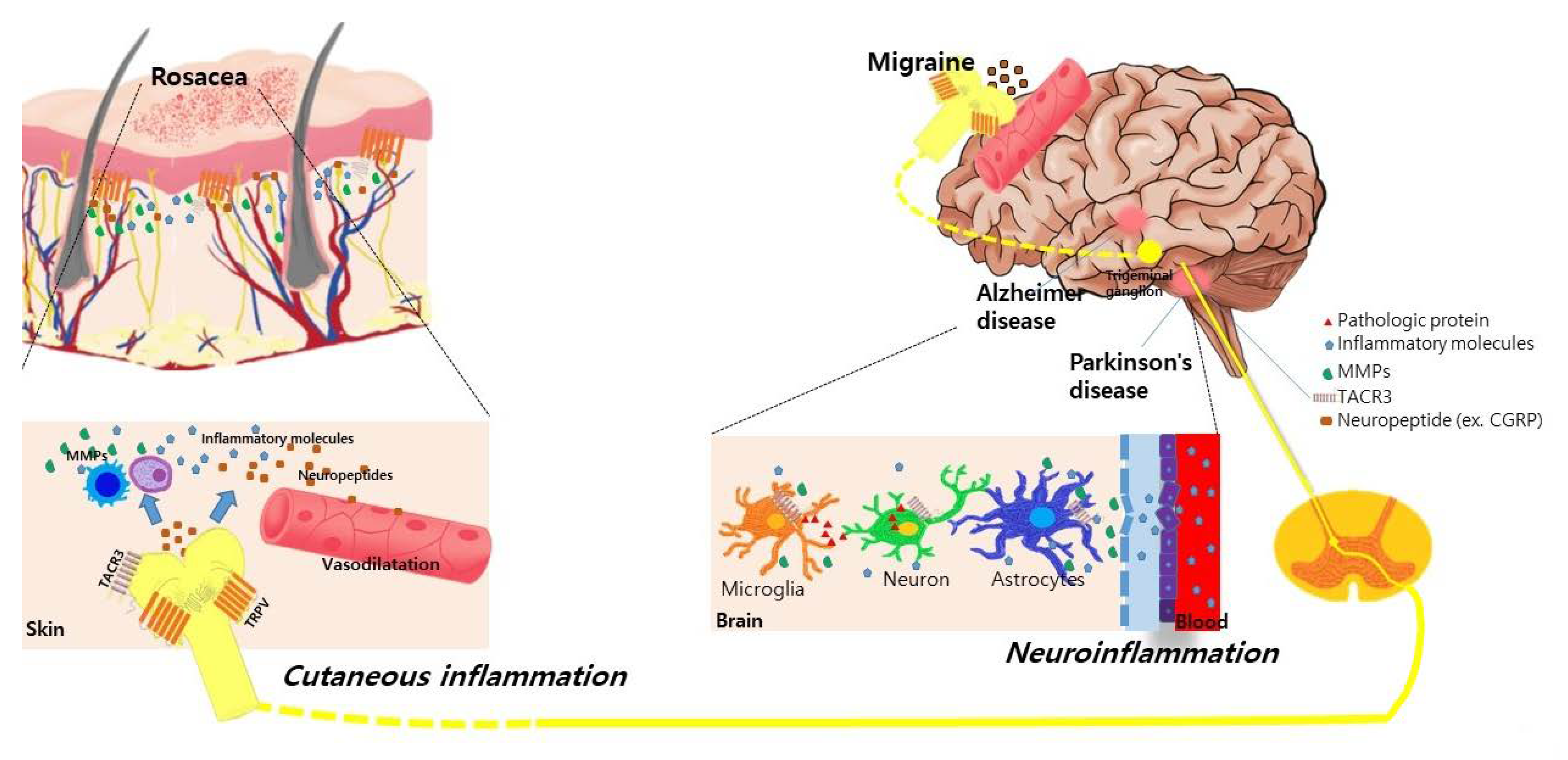
2. The Risk of Neurologic Diseases in Rosacea
3. The Risk of Psychiatric Diseases in Rosacea
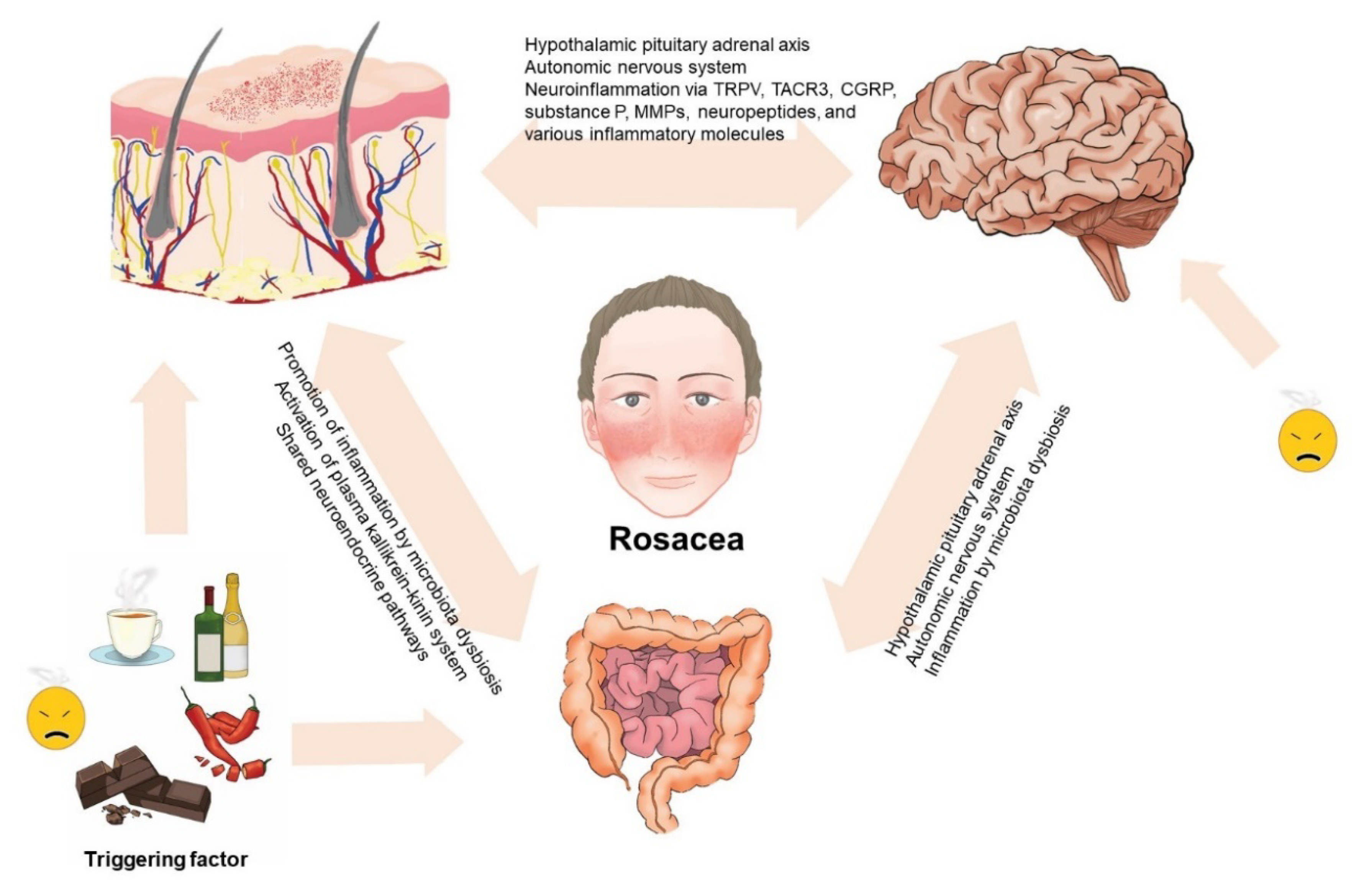
4. The Risk of Gastrointestinal Disorders in Rosacea
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| AMP | antimicrobial peptide |
| CD | Crohn’s disease |
| CGRP | calcitonin gene-related peptide |
| CI | confidence interval |
| HR | hazard ratio |
| IBD | inflammatory bowel disease |
| IL | interleukin |
| IRR | incidence rate ratio |
| MMP | matrix metalloproteinase |
| OR | odds ratio |
| PKKS | plasma kallikrein–kinin system |
| RR | relative risk |
| SIBO | small intestinal bacterial overgrowth |
| Th | T helper |
| TRPV | transient receptor potential vanilloid type |
| UC | ulcerative colitis |
References
- Holmes, A.D.; Steinhoff, M. Integrative concepts of rosacea pathophysiology, clinical presentation and new therapeutics. Exp. Dermatol. 2016, 26, 659–667. [Google Scholar] [CrossRef]
- Woo, Y.R.; Lim, J.H.; Cho, D.; Park, H.J. Rosacea: Molecular Mechanisms and Management of a Chronic Cutaneous Inflammatory Condition. Int. J. Mol. Sci. 2016, 17, 1562. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hua, T.-C.; Chung, P.-I.; Chen, Y.-J.; Wu, L.-C.; Chen, Y.-D.; Hwang, C.-Y.; Chu, S.-Y.; Chen, C.-C.; Lee, D.-D.; Chang, Y.-T.; et al. Cardiovascular comorbidities in patients with rosacea: A nationwide case-control study from Taiwan. J. Am. Acad. Dermatol. 2015, 73, 249–254. [Google Scholar] [CrossRef]
- Egeberg, A.; Hansen, P.R.; Gislason, G.H.; Thyssen, J.P. Assessment of the risk of cardiovascular disease in patients with rosacea. J. Am. Acad. Dermatol. 2016, 75, 336–339. [Google Scholar] [CrossRef] [PubMed]
- Bowe, W.P.; Logan, A.C. Acne vulgaris, probiotics and the gut-brain-skin axis—Back to the future? Gut Pathog. 2011, 3, 1–11. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fischer, M.; Gemende, I.; Marsch, W.C.; Fischer, P.A. Skin function and skin disorders in Parkinson’s disease. J. Neural Transm. 2001, 108, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Egeberg, A.; Hansen, P.R.; Gislason, G.H.; Thyssen, J.P. Exploring the Association between Rosacea and Parkinson Disease. JAMA Neurol. 2016, 73, 529–534. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mathieu, R.; Guido, N.; Ibler, E.; Serrano, L.; Rangel, S.; Schlosser, B.; West, D.; Laumann, A.; Nardone, B. Rosacea and subsequent diagnosis for Parkinson’s disease: A large, urban, single center, US patient population retrospective study. J. Eur. Acad. Dermatol. Venereol. 2017, 32, e141–e144. [Google Scholar] [CrossRef]
- Egeberg, A.; Hansen, P.R.; Gislason, G.H.; Thyssen, J.P. Patients with rosacea have increased risk of dementia. Ann. Neurol. 2016, 79, 921–928. [Google Scholar] [CrossRef]
- Spoendlin, J.; Voegel, J.J.; Jick, S.S.; Meier, C.R. Migraine, triptans, and the risk of developing rosacea. J. Am. Acad. Dermatol. 2013, 69, 399–406. [Google Scholar] [CrossRef]
- Egeberg, A.; Ashina, M.; Gaist, D.; Gislason, G.H.; Thyssen, J.P. Prevalence and risk of migraine in patients with rosacea: A population-based cohort study. J. Am. Acad. Dermatol. 2017, 76, 454–458. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.A.; Gupta, A.K.; Chen, S.J.; Johnson, A.M. Comorbidity of rosacea and depression: An analysis of the National Ambulatory Medical Care Survey and National Hospital Ambulatory Care Survey—Outpatient Department data collected by the U.S. National Center for Health Statistics from 1995 to 2002. Br. J. Dermatol. 2005, 153, 1176–1181. [Google Scholar] [CrossRef] [PubMed]
- Egeberg, A.; Hansen, P.R.; Gislason, G.H.; Thyssen, J.P. Patients with Rosacea Have Increased Risk of Depression and Anxiety Disorders: A Danish Nationwide Cohort Study. Dermatology 2016, 232, 208–213. [Google Scholar] [CrossRef] [PubMed]
- Chung, C.; Chiang, C.-P.; Tsao, C.-H.; Chien, W.-C.; Wang, W.-M. Risk of psychiatric disorders in rosacea: A nationwide, population-based, cohort study in Taiwan. J. Dermatol. 2018, 46, 110–116. [Google Scholar] [CrossRef]
- Jayaraj, R.L.; Beiram, R.; Azimullah, S.; Mf, N.M.; Ojha, S.; Adem, A.; Jalal, F.Y. Lycopodium Attenuates Loss of Dopaminergic Neurons by Suppressing Oxidative Stress and Neuroinflammation in a Rat Model of Parkinson’s Disease. Molecules 2019, 24, 2182. [Google Scholar] [CrossRef] [Green Version]
- Spindola, A.; Targa, A.D.S.; Rodrigues, L.S.; Winnischofer, S.M.B.; Lima, M.M.S.; Sogayar, M.C.; Trombetta-Lima, M. Increased Mmp/Reck Expression Ratio Is Associated with Increased Recognition Memory Performance in a Parkinson’s Disease Animal Model. Mol. Neurobiol. 2019, 57, 837–847. [Google Scholar] [CrossRef]
- Schwab, V.D.; Sulk, M.; Seeliger, S.; Nowak, P.; Aubert, J.; Mess, C.; Rivier, M.; Carlavan, I.; Rossio, P.; Metze, D.; et al. Neurovascular and Neuroimmune Aspects in the Pathophysiology of Rosacea. J. Investig. Dermatol. Symp. Proc. 2011, 15, 53–62. [Google Scholar] [CrossRef] [Green Version]
- Jang, Y.H.; Sim, J.H.; Kang, H.Y.; Kim, Y.C.; Lee, E.-S. Immunohistochemical expression of matrix metalloproteinases in the granulomatous rosacea compared with the non-granulomatous rosacea. J. Eur. Acad. Dermatol. Venereol. 2011, 25, 544–548. [Google Scholar] [CrossRef]
- Karpouzis, A.; Avgeridis, P.; Tripsianis, G.; Gatzidou, E.; Kourmouli, N.; Veletza, S. Assessment of Tachykinin Receptor 3′ Gene Polymorphism rs3733631 in Rosacea. Int. Sch. Res. Notices 2015, 2015, 469402. [Google Scholar] [CrossRef] [Green Version]
- Davidson, E.A.; Robertson, E.E. Alzheimer’s disease with acne rosacea in one of identical twins. J. Neurol. Neurosurg. Psychiatry 1955, 18, 72–77. [Google Scholar] [CrossRef] [Green Version]
- Lorenzl, S. Increased plasma levels of matrix metalloproteinase-9 in patients with Alzheimer’s disease. Neurochem. Int. 2003, 43, 191–196. [Google Scholar] [CrossRef]
- Kanada, K.N.; Nakatsuji, T.; Gallo, R.L. Doxycycline Indirectly Inhibits Proteolytic Activation of Tryptic Kallikrein-Related Peptidases and Activation of Cathelicidin. J. Investig. Dermatol. 2012, 132, 1435–1442. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garwood, C.J.; Cooper, J.D.; Hanger, D.P.; Noble, W. Anti-Inflammatory Impact of Minocycline in a Mouse Model of Tauopathy. Front. Psychiatry 2010, 1, 136. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cai, Z.; Yan, Y.; Wang, Y. Minocycline alleviates beta-amyloid protein and tau pathology via restraining neuroinflammation induced by diabetic metabolic disorder. Clin. Interv. Aging 2013, 8, 1089–1095. [Google Scholar] [CrossRef] [Green Version]
- Kumar, D.K.V.; Choi, S.H.; Washicosky, K.J.; Eimer, W.A.; Tucker, S.; Ghofrani, J.; Lefkowitz, A.; McColl, G.; Goldstein, L.E.; Tanzi, R.E.; et al. Amyloid-β peptide protects against microbial infection in mouse and worm models of Alzheimer’s disease. Sci. Transl. Med. 2016, 8, 340ra72. [Google Scholar] [CrossRef] [Green Version]
- Steinhoff, M.; Schauber, J.; Leyden, J.J. New insights into rosacea pathophysiology: A review of recent findings. J. Am. Acad. Dermatol. 2013, 69, S15–S26. [Google Scholar] [CrossRef]
- Gosztyla, M.L.; Brothers, H.M.; Robinson, S.R. Alzheimer’s Amyloid-β is an Antimicrobial Peptide: A Review of the Evidence. J. Alzheimer’s Dis. 2018, 62, 1495–1506. [Google Scholar] [CrossRef] [Green Version]
- Dodick, D.W. Migraine. Lancet 2018, 391, 1315–1330. [Google Scholar] [CrossRef]
- Wilkin, J.; Dahl, M.; Detmar, M.; Drake, L.; Feinstein, A.; Odom, R.; Powell, F. Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea. J. Am. Acad. Dermatol. 2002, 46, 584–587. [Google Scholar] [CrossRef] [Green Version]
- Scharschmidt, T.C.; Yost, J.M.; Truong, S.V.; Steinhoff, M.; Wang, K.C.; Berger, T.G. Neurogenic Rosacea: A Distinct Clinical Subtype Requiring a Modified Approach to Treatment. Arch. Dermatol. 2010, 147, 123–126. [Google Scholar] [CrossRef] [Green Version]
- Tan, S.G.; Cunliffe, W.J. Rosacea and migraine. BMJ 1976, 1, 21. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ramelet, A.A. Rosacea: A reaction pattern associated with ocular lesions and migraine? Arch. Dermatol. 1994, 130, 1448. [Google Scholar] [CrossRef] [PubMed]
- Al-Balbeesi, A.O.; Halawani, M.R. Unusual Features of Rosacea in Saudi Females with Dark Skin. Ochsner J. 2014, 14, 321–327. [Google Scholar] [PubMed]
- Berg, M.; Lidén, S. Postmenopausal Female Rosacea Patients Are More Disposed to React with Migraine. Dermatology 1996, 193, 73–74. [Google Scholar] [CrossRef] [PubMed]
- Christensen, C.E.; Andersen, F.S.; Wienholtz, N.; Egeberg, A.; Thyssen, J.P.; Ashina, M. The relationship between migraine and rosacea: Systematic review and meta-analysis. Cephalalgia 2017, 38, 1387–1398. [Google Scholar] [CrossRef]
- Elkind, A.H.; Friedman, A.P.; Grossman, J. Cutaneous blood flow in vascular headaches of the migraine type. Neurology 1964, 14, 24. [Google Scholar] [CrossRef]
- Drummond, P.D. Sweating and vascular responses in the face: Normal regulation and dysfunction in migraine, cluster headache and harlequin syndrome. Clin. Auton. Res. 1994, 4, 273–285. [Google Scholar] [CrossRef]
- Drummond, P.D. Disturbances in ocular sympathetic function and facial blood flow in unilateral migraine headache. J. Neurol. Neurosurg. Psychiatry 1990, 53, 121–125. [Google Scholar] [CrossRef] [Green Version]
- Del Fiacco, M.; Quartu, M.; Boi, M.; Serra, M.P.; Melis, T.; Boccaletti, R.; Shevel, E.; Cianchetti, C. TRPV1, CGRP and SP in scalp arteries of patients suffering from chronic migraine. J. Neurol. Neurosurg. Psychiatry 2014, 86, 393–397. [Google Scholar] [CrossRef]
- Sulk, M.; Seeliger, S.; Aubert, J.; Schwab, V.D.; Cevikbas, F.; Rivier, M.; Nowak, P.; Voegel, J.J.; Buddenkotte, J.; Steinhoff, M. Distribution and Expression of Non-Neuronal Transient Receptor Potential (TRPV) Ion Channels in Rosacea. J. Investig. Dermatol. 2012, 132, 1253–1262. [Google Scholar] [CrossRef] [Green Version]
- Meents, J.E.; Neeb, L.; Reuter, P.-D.D.U. TRPV1 in migraine pathophysiology. Trends Mol. Med. 2010, 16, 153–159. [Google Scholar] [CrossRef] [PubMed]
- Heisig, M.; Reich, A. Psychosocial aspects of rosacea with a focus on anxiety and depression. Clin. Cosmet. Investig. Dermatol. 2018, 11, 103–107. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bewley, A.; Fowler, J.; Schöfer, H.; Kerrouche, N.; Rives, V. Erythema of Rosacea Impairs Health-Related Quality of Life: Results of a Meta-analysis. Dermatol. Ther. 2016, 6, 237–247. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, Y.; Fu, C.; Zhang, W.; Li, C.; Zhang, J. The dermatology life quality index (DLQI) and the hospital anxiety and depression (HADS) in Chinese rosacea patients. Psychol. Heal. Med. 2017, 23, 369–374. [Google Scholar] [CrossRef]
- Uysal, P.I.; Akdogan, N.; Hayran, Y.; Oktem, A.; Yalcin, B. Rosacea associated with increased risk of generalized anxiety disorder: A case-control study of prevalence and risk of anxiety in patients with rosacea. An. Bras. Dermatol. 2019, 94, 704–709. [Google Scholar] [CrossRef]
- Singam, V.; Rastogi, S.; Patel, K.R.; Lee, H.H.; Silverberg, J.I. The mental health burden in acne vulgaris and rosacea: An analysis of the US National Inpatient Sample. Clin. Exp. Dermatol. 2019, 44, 766–772. [Google Scholar] [CrossRef]
- Su, D.; Drummond, P.D. Blushing Propensity and Psychological Distress in People with Rosacea. Clin. Psychol. Psychother. 2011, 19, 488–495. [Google Scholar] [CrossRef]
- Gravina, A.; Federico, A.; Ruocco, E.; Schiavo, A.L.; Masarone, M.; Tuccillo, C.; Peccerillo, F.; Miranda, A.; Romano, L.; De Sio, C.; et al. Helicobacter pylori infection but not small intestinal bacterial overgrowth may play a pathogenic role in rosacea. United Eur. Gastroenterol. J. 2014, 3, 17–24. [Google Scholar] [CrossRef] [Green Version]
- Inserra, A.; Rogers, G.B.; Licinio, J.; Wong, M.-L. The Microbiota-Inflammasome Hypothesis of Major Depression. BioEssays 2018, 40, e1800027. [Google Scholar] [CrossRef] [Green Version]
- Koopman, M.; El Aidy, S. Depressed gut? The microbiota-diet-inflammation trialogue in depression. Curr. Opin. Psychiatry 2017, 30, 369–377. [Google Scholar] [CrossRef] [Green Version]
- Salem, I.; Ramser, A.; Isham, N.; A Ghannoum, M. The Gut Microbiome as a Major Regulator of the Gut-Skin Axis. Front. Microbiol. 2018, 9, 1459. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Weinstock, L.B.; Steinhoff, M. Rosacea and small intestinal bacterial overgrowth: Prevalence and response to rifaximin. J. Am. Acad. Dermatol. 2013, 68, 875–876. [Google Scholar] [CrossRef] [PubMed]
- Woo, Y.R.; Lee, S.H.; Cho, S.H.; Lee, J.D.; Kim, H.S. Characterization and Analysis of the Skin Microbiota in Rosacea: Impact of Systemic Antibiotics. J. Clin. Med. 2020, 9, 185. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Arck, P.; Handjiski, B.; Hagen, E.; Pincus, M.; Bruenahl, C.; Bienenstock, J.; Paus, R. Is there a ‘gut-brain-skin axis’? Exp. Dermatol. 2010, 19, 401–405. [Google Scholar] [CrossRef]
- Ali, A.A.; Vender, R.; Vender, R. The Role of IL-17 in Papulopustular Rosacea and Future Directions. J. Cutan. Med. Surg. 2019, 23, 635–641. [Google Scholar] [CrossRef]
- Watson, W.; Paton, E.; Murray, D. SMALL-BOWEL DISEASE IN ROSACEA. Lancet 1965, 286, 47–50. [Google Scholar] [CrossRef]
- Szlachcic, A. The link between Helicobacter pylori infection and rosacea. J. Eur. Acad. Dermatol. Venereol. 2002, 16, 328–333. [Google Scholar] [CrossRef]
- Utaş, S.; Özbakir, Ö.; Turasan, A.; Utaş, C. Helicobacter pylori eradication treatment reduces the severity of rosacea. J. Am. Acad. Dermatol. 1999, 40, 433–435. [Google Scholar] [CrossRef]
- De Miquel, D.B.; Romero, M.V.; Sequeiros, E.V.; Olcina, J.R.F.; Román, A.L.S.; Villanueva, S.A.; Prados, C.M.D.A.D. Effect of Helicobacter pylori eradication therapy in rosacea patients. Revista Española de Enfermedades Digestivas 2006, 98, 501–509. [Google Scholar] [CrossRef] [Green Version]
- Egeberg, A.; Weinstock, L.; Thyssen, E.; Gislason, G. Rosacea and gastrointestinal disorders: A population-based cohort study. Br. J. Dermatol. 2016, 176, 100–106. [Google Scholar] [CrossRef]
- Jørgensen, A.-H.; Egeberg, A.; Gideonsson, R.; Weinstock, L.; Thyssen, J.P. Rosacea is associated with Helicobacter pylori: A systematic review and meta-analysis. J. Eur. Acad. Dermatol. Venereol. 2017, 31, 2010–2015. [Google Scholar] [CrossRef] [PubMed]
- Szlachcic, A.; Sliwowski, Z.; Karczewska, E.; Bielański, W.; Pytko-Polonczyk, J.; Konturek, S.J. Helicobacter pylori and its eradication in rosacea. J. Physiol. Pharmacol. Off. J. Pol. Physiol. Soc. 1999, 50, 777–786. [Google Scholar]
- Pakodi, F.; Abdel-Salam, O.M.; Debreceni, A.; Mozsik, G. Helicobacter pylori. One bacterium and a broad spectrum of human disease! An overview. J. Physiol. 2000, 94, 139–152. [Google Scholar] [CrossRef]
- Spoendlin, J.; Karatas, G.; Furlano, R.I.; Jick, S.S.; Meier, C.R. Rosacea in Patients with Ulcerative Colitis and Crohn’s Disease: A Population-based Case-control Study. Inflamm. Bowel Dis. 2016, 22, 680–687. [Google Scholar] [CrossRef] [Green Version]
- Li, W.-Q.; Cho, E.; Khalili, H.; Wu, S.; Chan, A.T.; Qureshi, A.A. Rosacea, Use of Tetracycline, and Risk of Incident Inflammatory Bowel Disease in Women. Clin. Gastroenterol. Hepatol. 2015, 14, 220–225.e1. [Google Scholar] [CrossRef] [Green Version]
- Kim, M.; Choi, K.H.; Hwang, S.W.; Lee, Y.B.; Park, H.J.; Bae, J.M. Inflammatory bowel disease is associated with an increased risk of inflammatory skin diseases: A population-based cross-sectional study. J. Am. Acad. Dermatol. 2017, 76, 40–48. [Google Scholar] [CrossRef]
- Wang, F.-Y.; Chi, C.-C. Association of rosacea with inflammatory bowel disease. Medicine 2019, 98, e16448. [Google Scholar] [CrossRef]
- Geremia, A.; Biancheri, P.; Allan, P.; Corazza, G.R.; Di Sabatino, A. Innate and adaptive immunity in inflammatory bowel disease. Autoimmun. Rev. 2014, 13, 3–10. [Google Scholar] [CrossRef]
- Safarpour, A.R.; Moini, M.; Saadat, M.; Saadat, H.; Esmailnejad, A. Association Study of Glutathione S-transferases Gene Polymorphisms (GSTM1 and GSTT1) with Ulcerative Colitis and Crohn’s Disease in the South of Iran. Adv. Biomed. Res. 2017, 6, 67. [Google Scholar] [CrossRef]
- Yazici, A.C.; Tamer, L.; Ikizoglu, G.; Kaya, T.I.; Api, H.; Yildirim, H.; Adiguzel, A. GSTM1 and GSTT1 null genotypes as possible heritable factors of rosacea. Photodermatol. Photoimmunol. Photomed. 2006, 22, 208–210. [Google Scholar] [CrossRef]
- Parodi, A.; Paolino, S.; Greco, A.; Drago, F.; Mansi, C.; Rebora, A.; Parodi, A.; Savarino, V. Small intestinal bacterial overgrowth in rosacea: Clinical effectiveness of its eradication. Clin. Gastroenterol. Hepatol. 2008, 6, 759–764. [Google Scholar] [CrossRef] [PubMed]
- Weiss, E.; Katta, R. Diet and rosacea: The role of dietary change in the management of rosacea. Dermatol. Pr. Concept. 2017, 7, 31–37. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shah, A.; Morrison, M.; Burger, D.; Martin, N.; Rich, J.; Jones, M.; A Koloski, N.; Walker, M.M.; Talley, N.J.; Holtmann, G. Systematic review with meta-analysis: The prevalence of small intestinal bacterial overgrowth in inflammatory bowel disease. Aliment. Pharmacol. Ther. 2019, 49, 624–635. [Google Scholar] [CrossRef] [PubMed]
- Rana, S.V.; Sharma, S.; Malik, A.; Kaur, J.; Prasad, K.K.; Sinha, S.K.; Singh, K. Small Intestinal Bacterial Overgrowth and Orocecal Transit Time in Patients of Inflammatory Bowel Disease. Dig. Dis. Sci. 2013, 58, 2594–2598. [Google Scholar] [CrossRef]
- Picardo, M.; Ottaviani, M. Skin Microbiome and Skin Disease. J. Clin. Gastroenterol. 2014, 48, S85–S86. [Google Scholar] [CrossRef]
- Kendall, S.N. Remission of rosacea induced by reduction of gut transit time. Clin. Exp. Dermatol. 2004, 29, 297–299. [Google Scholar] [CrossRef]
- Parodi, A.; Guarrera, M.; Drago, F. Flushing in rosacea: An experimental approach. Arch. Dermatol. Res. 1980, 269, 269–273. [Google Scholar] [CrossRef]
- Sharma, J.; Zeitlin, I.; MacKenzie, J.; Russell, R. PLASMA KININ-PRECURSOR LEVELS IN CLINICAL INTESTINAL INFLAMMATION. Fundam. Clin. Pharmacol. 1988, 2, 399–403. [Google Scholar] [CrossRef]
- Wu, C.-Y.; Chang, Y.-T.; Juan, C.-K.; Shieh, J.-J.; Lin, Y.-P.; Liu, H.-N.; Lin, J.-T.; Chen, Y.-J. Risk of inflammatory bowel disease in patients with rosacea: Results from a nationwide cohort study in Taiwan. J. Am. Acad. Dermatol. 2017, 76, 911–917. [Google Scholar] [CrossRef]
- Holmes, A.D. Potential role of microorganisms in the pathogenesis of rosacea. J. Am. Acad. Dermatol. 2013, 69, 1025–1032. [Google Scholar] [CrossRef]
- Beri, K. Perspective: Stabilizing the Microbiome Skin-Gut-Brain Axis with Natural Plant Botanical Ingredients in Cosmetics. Cosmetics 2018, 5, 37. [Google Scholar] [CrossRef] [Green Version]
| Disorder | Study | Study Population | Relative Risk of Measures |
|---|---|---|---|
| Neurologic disorder | Egeberg (2016) [7] | Rosacea: 68,053 Control: 5,404,692 | Parkinson’s disease aIRR 1.71 (1.52–1.92) |
| Mathieu (2018) [8] | Rosacea: 14,696 Control: 399,383 | Parkinson’s disease OR 1.39 (1.04–1.85) | |
| Egeberg (2016) [9] | Rosacea: 82,439 Control: 5,509,279 | Dementia aHR 1.28 (1.01–1.14); Alzheimer’s disease aHR 1.25 (1.14–1.37) | |
| Spoendlin (2013) [10] | Rosacea: 53,927 Control: 53,927 | Migraine in women aOR 1.22 (1.16–1.29) | |
| Egeberg (2016) [11] | Rosacea: 49,475 Control: 4,312,213 | Migraine aHR 1.31 (1.23–1.39); migraine in ocular rosacea aHR 1.69 (1.43–1.99) | |
| Psychiatric disorder | Gupta (2005) [12] | Rosacea visits: 13,978,704 Control: 594,766,021 | Depressive disease OR 4.81 (1.39–16.62) |
| Egeberg (2016) [13] | Rosacea: 55,437 (Mild: 30,725; moderate to severe: 24,712) Control: 4,576,904 | Depression IRR in mild rosacea 1.89 (1.82–1.96); in moderate to severe rosacea 2.04 (1.96–2.12) Anxiety disorder IRR in mild rosacea 1.80 (1.75–1.86); in moderate to severe rosacea 1.98 (1.91–2.05) | |
| Hung (2018) [14] | Rosacea: 7881 Control: 31,524 | Total psychiatric disorders aHR 2.76 (2.65–2.87); phobic disorder aHR 7.84 (7.52–8.17); obsessive-compulsive disorder aHR 7.84 (7.52–8.17); major depressive disorder aHR 3.78 (3.63–3.94); bipolar disorder aHR 3.19 (3.06–3.32); anxiety aHR 2.91 (2.79–3.03); personality disorder aHR 2.85 (2.73–2.97); manic disorder aHR 2.63 (2.52–2.74); schizophrenia aHR 2.28 (2.19–2.38); attention deficit hyperactivity disorder aHR 1.04 (1.00–1.08) |
| Study | Study Design | Study Population | Main Outcomes |
|---|---|---|---|
| Spoendlin (2016) [64] | Case–control | Rosacea: 80,957 Control: 80,957 | A history of UC is associated risk of rosacea (OR: 1.65; 95% CI: 1.43–190); a history of CD is associated with risk of rosacea (OR: 1.49; 95% CI: 1.25–1.77) |
| Li (2016) [65] | Cross-sectional | Rosacea: 1127 female nurses; Control: 95,187 female nurses | No association with UC CD (HR: 2.20; 95% CI: 1.15–4.18) |
| Egeberg (2017) [60] | Cohort | Rosacea: 49,475 Control: 4,312,213 | Celiac disease (HR: 1.46; 95% CI: 1.11–1.93); Crohn’s disease (CD) (HR: 1.45; 95% CI: 1.19–1.77); ulcerative colitis (UC) (HR: 1.19; 95% CI: 1.02–1.39); inflammatory bowel syndrome (HR: 1.34; 95% CI: 1.19–1.50) No association with SIBO and H. pylori infection |
| Wu (2017) [79] | Cohort | Rosacea: 89,356 Control: 178,712 | IBD (HR: 1.94; 95% CI: 1.04–3.63) |
| Kim (2018) [66] | Cross-sectional | IBD: 40,843 (CD: 12,646; UC: 28,197) Control: 122,529 | Rosacea (OR: 2.173; 95% CI: 1.590–2.969); rosacea risk among UC patients (OR: 1.979; 95% CI: 1.389–2.819); rosacea risk among CD patients (OR: 2.735; 95% CI: 1.708–4.380) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Woo, Y.R.; Han, Y.J.; Kim, H.S.; Cho, S.H.; Lee, J.D. Updates on the Risk of Neuropsychiatric and Gastrointestinal Comorbidities in Rosacea and Its Possible Relationship with the Gut–Brain–Skin Axis. Int. J. Mol. Sci. 2020, 21, 8427. https://doi.org/10.3390/ijms21228427
Woo YR, Han YJ, Kim HS, Cho SH, Lee JD. Updates on the Risk of Neuropsychiatric and Gastrointestinal Comorbidities in Rosacea and Its Possible Relationship with the Gut–Brain–Skin Axis. International Journal of Molecular Sciences. 2020; 21(22):8427. https://doi.org/10.3390/ijms21228427
Chicago/Turabian StyleWoo, Yu Ri, Yu Jin Han, Hei Sung Kim, Sang Hyun Cho, and Jeong Deuk Lee. 2020. "Updates on the Risk of Neuropsychiatric and Gastrointestinal Comorbidities in Rosacea and Its Possible Relationship with the Gut–Brain–Skin Axis" International Journal of Molecular Sciences 21, no. 22: 8427. https://doi.org/10.3390/ijms21228427
APA StyleWoo, Y. R., Han, Y. J., Kim, H. S., Cho, S. H., & Lee, J. D. (2020). Updates on the Risk of Neuropsychiatric and Gastrointestinal Comorbidities in Rosacea and Its Possible Relationship with the Gut–Brain–Skin Axis. International Journal of Molecular Sciences, 21(22), 8427. https://doi.org/10.3390/ijms21228427






