Cannabinoids and Prostate Cancer: A Systematic Review of Animal Studies
Abstract
1. Introduction
2. Results
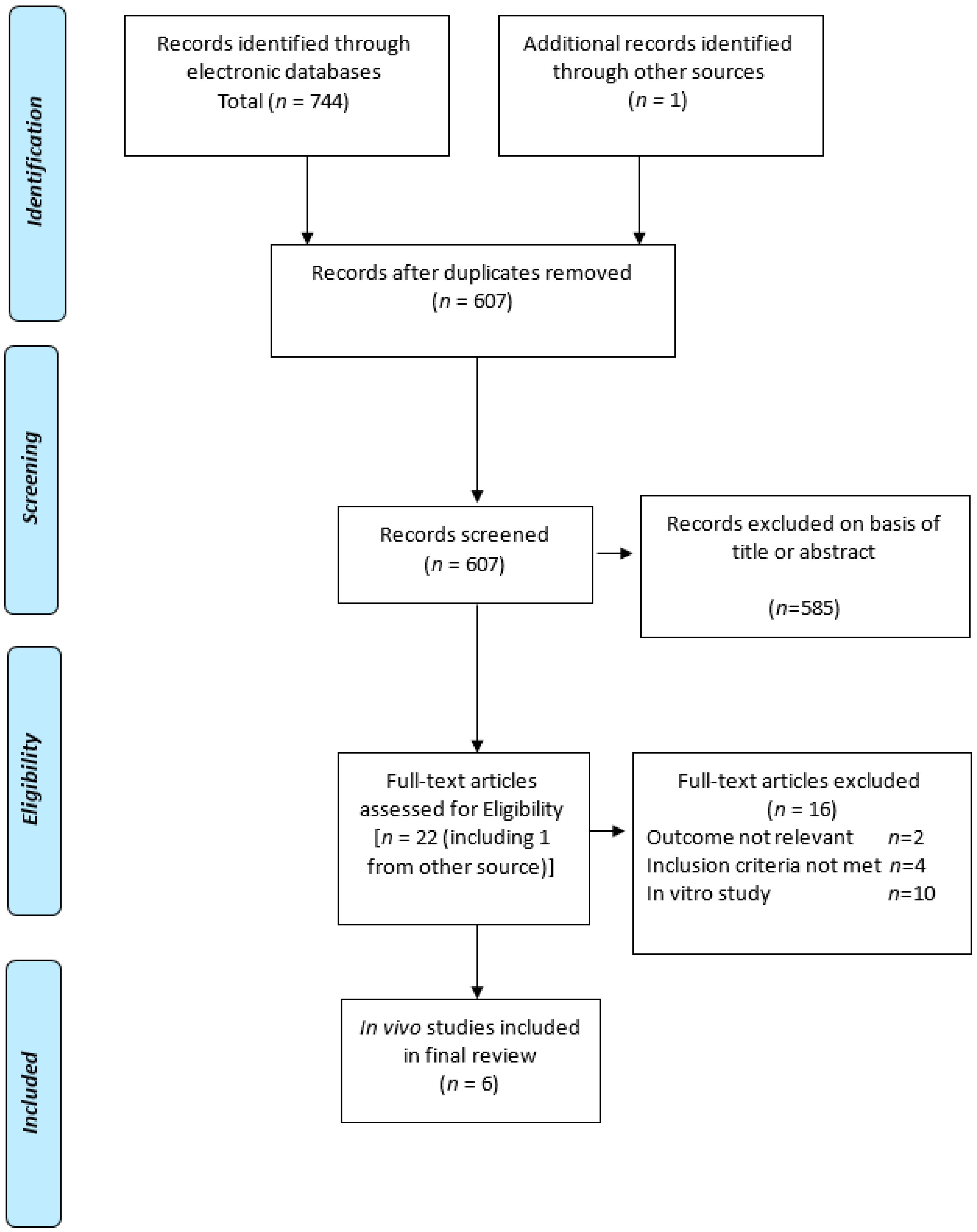
2.1. Results from the Search
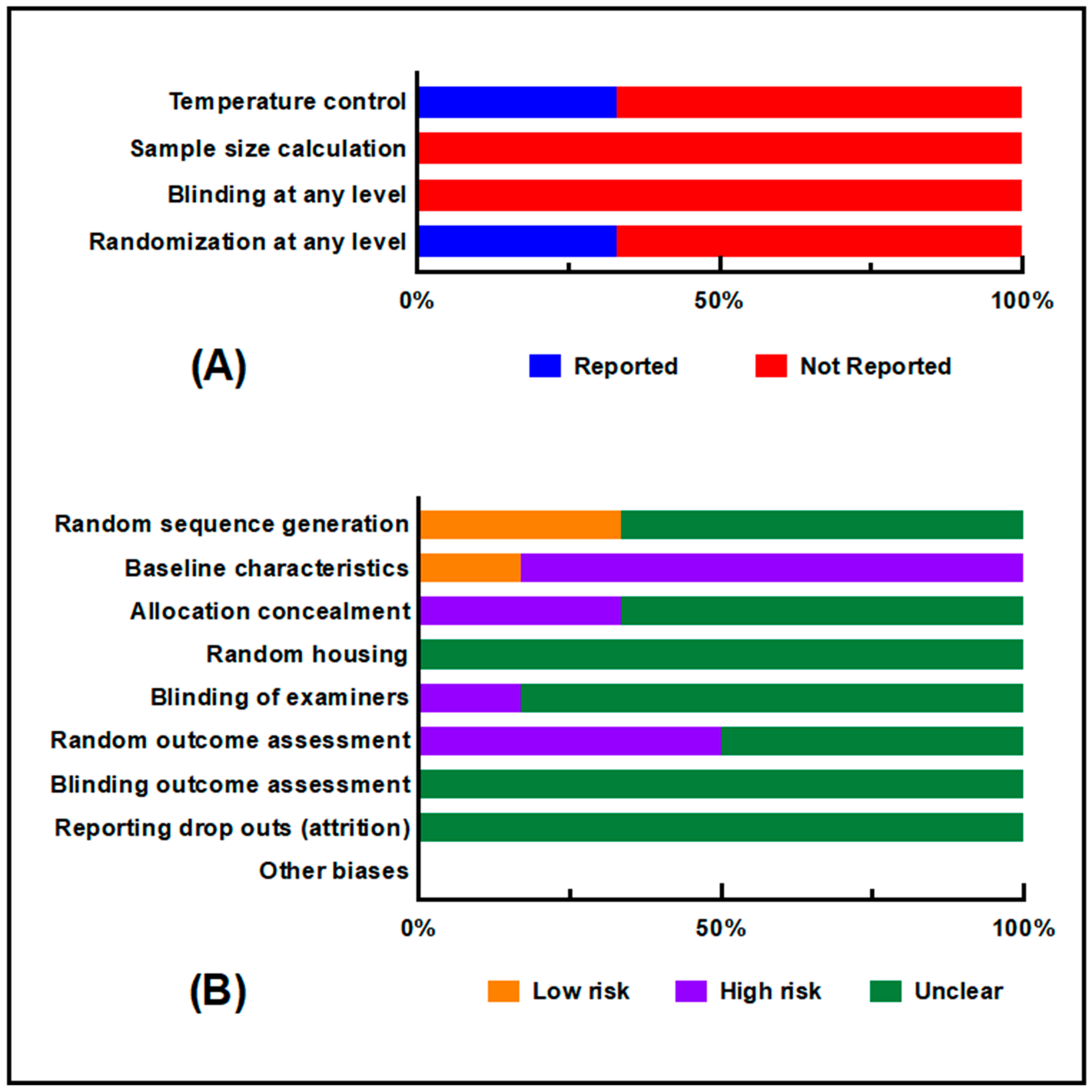
2.2. Risk of Bias Assessment
2.3. Study Characteristics
3. Discussion
4. Material and Methods
4.1. Search Strategy
4.2. Inclusion Criteria
4.3. Study Selection and Data Extraction
4.4. Risk of Bias Assessment
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef] [PubMed]
- Leitzmann, M.F.; Rohrmann, S. Risk factors for the onset of prostatic cancer: Age, location, and behavioral correlates. Clin. Epidemiol. 2012, 4, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Barbieri, C.E.; Baca, S.C.; Lawrence, M.S.; Demichelis, F.; Blattner, M.; Theurillat, J.-P.; White, T.A.; Stojanov, P.; Van Allen, E.; Stransky, N. Exome sequencing identifies recurrent SPOP, FOXA1 and MED12 mutations in prostate cancer. Nat. Genet. 2012, 44, 685–689. [Google Scholar] [CrossRef]
- Ku, S.Y.; Rosario, S.; Wang, Y.; Mu, P.; Seshadri, M.; Goodrich, Z.W.; Goodrich, M.M.; Labbé, D.P.; Gomez, E.C.; Wang, J. Rb1 and Trp53 cooperate to suppress prostate cancer lineage plasticity, metastasis, and antiandrogen resistance. Science 2017, 355, 78–83. [Google Scholar] [CrossRef] [PubMed]
- Montgomery, B.T.; Young, C.Y.F.; Bilhartz, D.L.; Andrews, P.E.; Thompson, N.F.; Tindall, D.J.; Prescott, J.L. Hormonal regulation of prostate-specific antigen (PSA) glycoprotein in the human prostatic adenocarcinoma cell line, LNCaP. Prostate 1992, 21, 63–73. [Google Scholar] [CrossRef] [PubMed]
- Sharma, M.; Hudson, J.B.; Adomat, H.; Guns, E.; Cox, M.E. In vitro anticancer activity of plant-derived cannabidiol on prostate cancer cell lines. Pharmacol. Pharm. 2014, 5, 806–820. [Google Scholar] [CrossRef]
- Lee, C.; Sutkowski, D.; Sensibar, J.; Zelner, D.; Kim, I.; Amsel, I.; Shaw, N.; Prins, G.S.; Kozlowski, J.M. Regulation of proliferation and production of prostate-specific antigen in androgen-sensitive prostatic cancer cells, LNCaP, by dihydrotestosterone. Endocrinology 1995, 136, 796–803. [Google Scholar] [CrossRef]
- Nguyen, C.; Lairson, D.R.; Swartz, M.D.; Du, X.L. Risks of major long-term side effects associated with androgen-deprivation therapy in men with prostate cancer. Pharmacotherapy 2018, 38, 999–1009. [Google Scholar] [CrossRef]
- Bhutani, K.K.; Gohil, V.M. Natural products drug discovery research in India: Status and appraisal. Indian J. Exp. Biol. 2010, 48, 199–207. [Google Scholar]
- Wang, X.; Fang, G.; Pang, Y. Chinese medicines in the treatment of prostate cancer: From formulas to extracts and compounds. Nutrients 2018, 10, 283. [Google Scholar] [CrossRef]
- Yang, H.; Chen, D.; Cui, Q.C.; Yuan, X.; Dou, Q.P. Celastrol, a triterpene extracted from the Chinese “Thunder of God Vine,” is a potent proteasome inhibitor and suppresses human prostate cancer growth in nude mice. Cancer Res. 2006, 66, 4758–4765. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.-M.; Lin, P.-H.; Hsu, R.-J.; Chang, Y.-H.; Cheng, K.-C.; Pang, S.-T.; Lin, S.-K. Complementary traditional Chinese medicine therapy improves survival in patients with metastatic prostate cancer. Medicine 2016, 95, e4475. [Google Scholar] [CrossRef] [PubMed]
- Moyad, M.; Hathaway, S.; Ni, H. Traditional Chinese medicine, acupuncture, and other alternative medicines for prostate cancer: An introduction and the need for more research. Semin. Urol. Oncol. 1999, 17, 103–110. [Google Scholar] [PubMed]
- Jiang, R.-W.; Zhou, J.-R.; Hon, P.-M.; Li, S.-L.; Zhou, Y.; Li, L.-L.; Ye, W.-C.; Xu, H.-X.; Shaw, P.-C.; But, P.P.-H. Lignans from Dysosma versipellis with inhibitory effects on prostate cancer cell lines. J. Nat. Prod. 2007, 70, 283–286. [Google Scholar] [CrossRef] [PubMed]
- Way, T.-D.; Lee, J.-C.; Kuo, D.-H.; Fan, L.-L.; Huang, C.-H.; Lin, H.-Y.; Shieh, P.-C.; Kuo, P.-T.; Liao, C.-F.; Liu, H. Inhibition of epidermal growth factor receptor signaling by Saussurea involucrata, a rare traditional Chinese medicinal herb, in human hormone-resistant prostate cancer PC-3 cells. J. Agric. Food Chem. 2010, 58, 3356–3365. [Google Scholar] [CrossRef]
- Zuardi, A.W. History of cannabis as a medicine: A review. Braz. J. Psychiatry 2006, 28, 153–157. [Google Scholar] [CrossRef]
- Ramos, J.A.; Bianco, F.J. The role of cannabinoids in prostate cancer: Basic science perspective and potential clinical applications. Indian J. Urol. 2012, 28, 9–14. [Google Scholar] [CrossRef]
- Dariš, B.; Verboten, M.T.; Knez, Ž.; Ferk, P. Cannabinoids in cancer treatment: Therapeutic potential and legislation. Bosn. J. Basic Med. Sci. 2019, 19, 14–23. [Google Scholar] [CrossRef]
- Lafaye, G.; Karila, L.; Blecha, L.; Benyamina, A. Cannabis, cannabinoids, and health. Dialogues Clin. Neurosci. 2017, 19, 309–316. [Google Scholar]
- Massi, P.; Solinas, M.; Cinquina, V.; Parolaro, D. Cannabidiol as potential anticancer drug. Br. J. Clin. Pharmacol. 2013, 75, 303–312. [Google Scholar] [CrossRef]
- Pacher, P. Towards the use of non-psychoactive cannabinoids for prostate cancer. Br. J. Pharmacol. 2013, 168, 76–78. [Google Scholar] [CrossRef]
- Bogdanović, V.; Mrdjanović, J.; Borišev, I. A review of the therapeutic antitumor potential of cannabinoids. J. Altern. Complement. Med. 2017, 23, 831–836. [Google Scholar] [CrossRef] [PubMed]
- Śledziński, P.; Zeyland, J.; Słomski, R.; Nowak, A. The current state and future perspectives of cannabinoids in cancer biology. Cancer Med. 2018, 7, 765–775. [Google Scholar] [CrossRef] [PubMed]
- Flygare, J.; Sander, B. The endocannabinoid system in cancer—Potential therapeutic target? Semin. Cancer Biol. 2008, 18, 176–189. [Google Scholar] [CrossRef] [PubMed]
- Guzmán, M. Cannabinoids: Potential anticancer agents. Nat. Rev. Cancer 2003, 3, 745–755. [Google Scholar] [CrossRef] [PubMed]
- Bifulco, M.; Laezza, C.; Pisanti, S.; Gazzerro, P. Cannabinoids and cancer: Pros and cons of an antitumour strategy. Br. J. Pharmacol. 2006, 148, 123–135. [Google Scholar] [CrossRef] [PubMed]
- Sarfaraz, S.; Adhami, V.M.; Syed, D.N.; Afaq, F.; Mukhtar, H. Cannabinoids for cancer treatment: Progress and promise. Cancer Res. 2008, 68, 339–342. [Google Scholar] [CrossRef]
- Velasco, G.; Hernández-Tiedra, S.; Dávila, D.; Lorente, M. The use of cannabinoids as anticancer agents. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2016, 64, 259–266. [Google Scholar] [CrossRef]
- Fraguas-Sanchez, A.I.; Fernandez-Carballido, A.; Torres-Suarez, A.I. Phyto-, endo- and synthetic cannabinoids: Promising chemotherapeutic agents in the treatment of breast and prostate carcinomas. Expert Opin. Investig. Drugs 2016, 25, 1311–1323. [Google Scholar] [CrossRef]
- Svíženská, I.; Dubový, P.; Šulcová, A. Cannabinoid receptors 1 and 2 (CB1 and CB2), their distribution, ligands and functional involvement in nervous system structures—A short review. Pharmacol. Biochem. Behav. 2008, 90, 501–511. [Google Scholar] [CrossRef]
- Console-Bram, L.; Marcu, J.; Abood, M.E. Cannabinoid receptors: Nomenclature and pharmacological principles. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2012, 38, 4–15. [Google Scholar] [CrossRef] [PubMed]
- Matsuda, L.A.; Lolait, S.J.; Brownstein, M.J.; Young, A.C.; Bonner, T.I. Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature 1990, 346, 561–564. [Google Scholar] [CrossRef] [PubMed]
- Morell, C.; Bort, A.; Vara, D.; Ramos-Torres, A.; Rodriguez-Henche, N.; Diaz-Laviada, I. The cannabinoid WIN 55,212-2 prevents neuroendocrine differentiation of LNCaP prostate cancer cells. Prostate Cancer Prostatic Dis. 2016, 19, 248–257. [Google Scholar] [CrossRef] [PubMed]
- Barbado, M.V.; Medrano, M.; Caballero-Velázquez, T.; Álvarez-Laderas, I.; Sánchez-Abarca, L.I.; García-Guerrero, E.; Martín-Sánchez, J.; Rosado, I.V.; Piruat, J.I.; Gonzalez-Naranjo, P. Cannabinoid derivatives exert a potent anti-myeloma activity both in vitro and in vivo. Int. J. Cancer 2017, 140, 674–685. [Google Scholar] [CrossRef]
- Khan, M.I.; Sobocinska, A.A.; Brodaczewska, K.K.; Zielniok, K.; Gajewska, M.; Kieda, C.; Czarnecka, A.M.; Szczylik, C. Involvement of the CB2 cannabinoid receptor in cell growth inhibition and G0/G1 cell cycle arrest via the cannabinoid agonist WIN 55,212-2 in renal cell carcinoma. BMC Cancer 2018, 18, 1–17. [Google Scholar] [CrossRef]
- Pietrovito, L.; Iozzo, M.; Bacci, M.; Giannoni, E.; Chiarugi, P. Treatment with Cannabinoids as a Promising Approach for Impairing Fibroblast Activation and Prostate Cancer Progression. Int. J. Mol. Sci. 2020, 21, 787. [Google Scholar] [CrossRef]
- Coke, C.J.; Scarlett, K.A.; Chetram, M.A.; Jones, K.J.; Sandifer, B.J.; Davis, A.S.; Marcus, A.I.; Hinton, C.V. Simultaneous Activation of Induced Heterodimerization between CXCR4 Chemokine Receptor and Cannabinoid Receptor 2 (CB2) Reveals a Mechanism for Regulation of Tumor Progression. J. Biol. Chem. 2016, 291, 9991–10005. [Google Scholar] [CrossRef]
- Katchan, V.; David, P.; Shoenfeld, Y. Cannabinoids and autoimmune diseases: A systematic review. Autoimmun. Rev. 2016, 15, 513–528. [Google Scholar] [CrossRef]
- Velasco, G.; Galve-Roperh, I.; Sánchez, C.; Blázquez, C.; Guzmán, M. Hypothesis: Cannabinoid therapy for the treatment of gliomas? Neuropharmacology 2004, 47, 315–323. [Google Scholar] [CrossRef]
- Hardie, D.G. AMPK—Sensing energy while talking to other signaling pathways. Cell Metab. 2014, 20, 939–952. [Google Scholar] [CrossRef]
- Hermanson, D.J.; Marnett, L.J. Cannabinoids, endocannabinoids, and cancer. Cancer Metastasis Rev. 2011, 30, 599–612. [Google Scholar] [CrossRef] [PubMed]
- Orellana-Serradell, O.; Poblete, C.; Sanchez, C.; Castellon, E.; Gallegos, I.; Huidobro, C.; Llanos, M.; Contreras, H. Proapoptotic effect of endocannabinoids in prostate cancer cells. Oncol. Rep. 2015, 33, 1599–1608. [Google Scholar] [CrossRef] [PubMed]
- Guindon, J.; Hohmann, A.G. The endocannabinoid system and cancer: Therapeutic implication. Br. J. Pharmacol. 2011, 163, 1447–1463. [Google Scholar] [CrossRef] [PubMed]
- Baram, L.; Peled, E.; Berman, P.; Yellin, B.; Besser, E.; Benami, M.; Louria-Hayon, I.; Lewitus, G.M.; Meiri, D. The heterogeneity and complexity of Cannabis extracts as antitumor agents. Oncotarget 2019, 10, 4091–4106. [Google Scholar] [CrossRef]
- De Petrocellis, L.; Ligresti, A.; Schiano Moriello, A.; Iappelli, M.; Verde, R.; Stott, C.G.; Cristino, L.; Orlando, P.; Di Marzo, V. Non-THC cannabinoids inhibit prostate carcinoma growth in vitro and in vivo: Pro-apoptotic effects and underlying mechanisms. Br. J. Pharmacol. 2013, 168, 79–102. [Google Scholar] [CrossRef]
- Roberto, D.; Klotz, L.H.; Venkateswaran, V. Cannabinoid WIN 55,212-2 induces cell cycle arrest and apoptosis, and inhibits proliferation, migration, invasion, and tumor growth in prostate cancer in a cannabinoid-receptor 2 dependent manner. Prostate 2019, 79, 151–159. [Google Scholar] [CrossRef]
- Nithipatikom, K.; Gomez-Granados, A.D.; Tang, A.T.; Pfeiffer, A.W.; Williams, C.L.; Campbell, W.B. Cannabinoid receptor type 1 (CB1) activation inhibits small GTPase RhoA activity and regulates motility of prostate carcinoma cells. Endocrinology 2012, 153, 29–41. [Google Scholar] [CrossRef]
- Milano, W.; Padricelli, U.; Capasso, A. Recent advances in research and therapeutic application of cannabinoids in cancer disease. Pharmacol. Online 2017, 3, 66–78. [Google Scholar]
- Hooijmans, C.R.; Rovers, M.M.; de Vries, R.B.; Leenaars, M.; Ritskes-Hoitinga, M.; Langendam, M.W. SYRCLE’s risk of bias tool for animal studies. BMC Med. Res. Methodol. 2014, 14, 43. [Google Scholar] [CrossRef]
- Olea-Herrero, N.; Vara, D.; Malagarie-Cazenave, S.; Diaz-Laviada, I. Inhibition of human tumour prostate PC-3 cell growth by cannabinoids R (+)-Methanandamide and JWH-015: Involvement of CB 2. Br. J. Cancer 2009, 101, 940–950. [Google Scholar] [CrossRef]
- Mukhtar, H.; Afaq, F.; Sarfaraz, S. Cannabinoid Receptors: A Novel Target for Therapy for Prostate Cancer (Award number W81XWH-04-1-0217). Defense Technical Information Center, 2008. Available online: https://apps.dtic.mil/dtic/tr/fulltext/u2/a482403.pdf (accessed on 21 March 2020).
- Morales, P.; Vara, D.; Goméz-Cañas, M.; Zúñiga, M.C.; Olea-Azar, C.; Goya, P.; Fernández-Ruiz, J.; Díaz-Laviada, I.; Jagerovic, N. Synthetic cannabinoid quinones: Preparation, in vitro antiproliferative effects and in vivo prostate antitumor activity. Eur. J. Med. Chem. 2013, 70, 111–119. [Google Scholar] [CrossRef] [PubMed]
- Roberto, D.; Klotz, L.H.; Venkateswaran, V. Cannabinoids as an Anticancer Agent for Prostate Cancer. J. Urol. Res. 2017, 4, 1090–1097. [Google Scholar]
- Gandhi, S.; Vasisth, G.; Kapoor, A. Systematic review of the potential role of cannabinoids as antiproliferative agents for urological cancers. Can. Urol. Assoc. J. 2017, 11, E138–E142. [Google Scholar] [CrossRef]
- Qamri, Z.; Preet, A.; Nasser, M.W.; Bass, C.E.; Leone, G.; Barsky, S.H.; Ganju, R.K. Synthetic cannabinoid receptor agonists inhibit tumor growth and metastasis of breast cancer. Mol. Cancer Ther. 2009, 8, 3117–3129. [Google Scholar] [CrossRef] [PubMed]
- Gholizadeh, F.; Ghahremani, M.H.; Aliebrahimi, S.; Shadboorestan, A.; Ostad, S.N. Assessment of Cannabinoids Agonist and Antagonist in Invasion Potential of K562 Cancer Cells. Iran. Biomed. J. 2019, 23, 153–158. [Google Scholar] [CrossRef]
- Englund, A.; M Stone, J.; D Morrison, P. Cannabis in the arm: What can we learn from intravenous cannabinoid studies? Curr. Pharm. Des. 2012, 18, 4906–4914. [Google Scholar] [CrossRef]
- Terry, S.; Ploussard, G.; Allory, Y.; Nicolaiew, N.; Boissière-Michot, F.; Maillé, P.; Kheuang, L.; Coppolani, E.; Ali, A.; Bibeau, F.; et al. Increased expression of class III β-tubulin in castration-resistant human prostate cancer. Br. J. Cancer 2009, 101, 951–956. [Google Scholar] [CrossRef]
- Scott, K.A.; Shah, S.; Dalgleish, A.G.; Liu, W.M. Enhancing the activity of cannabidiol and other cannabinoids in vitro through modifications to drug combinations and treatment schedules. Anticancer Res. 2013, 33, 4373–4380. [Google Scholar]
- Mueller, L.; Radtke, A.; Decker, J.; Koch, M.; Belge, G. The synthetic cannabinoid WIN 55,212-2 elicits death in human cancer cell lines. Anticancer Res. 2017, 37, 6341–6345. [Google Scholar]
- Casanova, M.L.; Blázquez, C.; Martínez-Palacio, J.; Villanueva, C.; Fernández-Aceñero, M.J.; Huffman, J.W.; Jorcano, J.L.; Guzmán, M. Inhibition of skin tumor growth and angiogenesis in vivo by activation of cannabinoid receptors. J. Clin. Investig. 2003, 111, 43–50. [Google Scholar] [CrossRef]
- Sánchez, C.; de Ceballos, M.L.; del Pulgar, T.G.; Rueda, D.; Corbacho, C.; Velasco, G.; Galve-Roperh, I.; Huffman, J.W.; y Cajal, S.R.; Guzmán, M. Inhibition of glioma growth in vivo by selective activation of the CB2 cannabinoid receptor. Cancer Res. 2001, 61, 5784–5789. [Google Scholar]
- Kis, B.; Ifrim, F.C.; Buda, V.; Avram, S.; Pavel, I.Z.; Antal, D.; Paunescu, V.; Dehelean, C.A.; Ardelean, F.; Diaconeasa, Z. Cannabidiol—From plant to human body: A promising bioactive molecule with multi-target effects in cancer. Int. J. Mol. Sci. 2019, 20, 5905. [Google Scholar] [CrossRef] [PubMed]
- Kenyon, J.; Liu, W.; Dalgleish, A. Report of objective clinical responses of cancer patients to pharmaceutical-grade synthetic cannabidiol. Anticancer Res. 2018, 38, 5831–5835. [Google Scholar] [CrossRef] [PubMed]
- Deng, L.; Ng, L.; Ozawa, T.; Stella, N. Quantitative analyses of synergistic responses between cannabidiol and DNA-damaging agents on the proliferation and viability of glioblastoma and neural progenitor cells in culture. J. Pharmacol. Exp. Ther. 2017, 360, 215–224. [Google Scholar] [CrossRef] [PubMed]
| First Author (Year) [Reference] | Selection Bias | Performance Bias | Detection Bias | Attrition Bias (Drop-Outs) | Other Biases | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Random Group Allocation | Baseline Group Characteristic | Allocation Concealed | Random Housing | Blinding of Examiners | Random Outcome Selection | Blinding of Assessor | Any Randomization | Any Blinding | Size Calculation | Temp Control | ||
| Morell (2016) [33] | L | H | H | ? | ? | H | ? | ? | Y | N | N | Y |
| De Petrocellis (2013) [45] | ? | H | H | ? | H | H | ? | ? | N | N | N | Y |
| Roberto (2019) [46] | L | H | ? | ? | ? | ? | ? | ? | Y | N | N | N |
| Olea-Herrero (2009) [50] | ? | L | ? | ? | ? | ? | ? | ? | N | N | N | N |
| Mukhtar (2007) [51] | ? | H | ? | ? | ? | ? | ? | ? | N | N | N | N |
| Morales (2013) [52] | ? | H | ? | ? | ? | H | ? | ? | N | N | N | N |
| First Author (Year) [Reference] | Study Population (Animals) | Tumor Induction (Cell Line) | Study Intervention | Cannabinoid Dose (Route) | Duration | Anticancer Outcomes | |||
|---|---|---|---|---|---|---|---|---|---|
| Strain | Age | Number | Intervention | Control | |||||
| Roberto, 2019 [46] | Male athymic nu/nu mice | 6 weeks | 10 mice (n = 5 per group) | Xenograft PC-3 cells, DU145 cells, and LNCaP cells | WIN55,212-2 | Vehicle (DMSO) | For PC3 and DU145 cell lines, dose given was 5, 10, and 20 µM. For LNCaP cell line, dose given was 20 and 30 µM. | 38 days | In PC3 xenograft, dose of 5 µM = 50%, 10 µM = 55%, and 20 µM = 64% reduction in cell proliferation. In DU145 xenograft, dose of 5 µM = 46%, 10 µM = 51%, and 20 µM = 65% reduction in cell proliferation. In LNCaP xenograft, dose of 20 µM = 69% and 30 µM = 66% reduction in cell proliferation. |
| Morell, 2016 [33] | Athymic nude-Foxn1 (nu/nu) | 4 weeks | 8 mice | Xenograft PC3 cells | WIN55,212-2 | Vehicle (not mentioned) | Daily (i.p.) 0.5 mg/kg (s.c.) | 15 days | WIN55,212-2-treated xenografts grew slower and the size of the tumor was smaller than that of vehicle-treated xenografts (% reduction in tumor size not mentioned). βIII Tub levels decreased in WIN55,212-2-treated tumors. |
| De Petrocellis, 2013 [45] | MF-1 nude mice | 4–7 weeks | 60 mice (n = 10 per group) | Xenograft LNCaP cells | Control CBD-BDS alone | Vehicle (not mentioned) | Daily (i.p.) | 35 days | CBD-BDS dose-dependently inhibited the growth of xenografts from LNCaP, but not DU145, cells. At 100 mg/kg, extract exerted a similar effect on both LNCaP and DU145 CBD-BDS plus bicalutamide significantly prolonged survival compared with bicalutamide or CBD-BDS alone. |
| Grp 1—vehicle only Grp 2—1 mg/kg daily Grp 2—10 mg/kg daily Grp 2—100 mg/kg daily | |||||||||
| Docetaxel Bicalutamide CBD-BDS + Docetaxel CBD-BDS + Bicalutamide | Grp 3—5 mg/kg (i.v.) 1× week Grp 4—25–50 mg/kg 3× week (p.o.) Grp 5—100 mg/kg (i.p.) + 5 mg/kg (i.v.) 1× week Grp 6—100 mg/kg (i.p.) + 25–50 mg/kg (p.o.) 3× week | ||||||||
| MF-1 nude mice | 4–7 weeks | 60 mice (n = 10 per group) | Xenograft DU145 cells | Control CBD-BDS alone | Vehicle (not mentioned) | Daily (i.p.) | 35 days | Tumor growth potentiation CBD-BDS + Docetaxel (exact % of reduction not mentioned). CBD-BDS + bicalutamide at 25 mg/kg significantly inhibited xenograft growth (exact % of reduction not mentioned). CBD-BDS + bicalutamide significantly prolonged survival compared with bicalutamide or CBD-BDS alone. | |
| Grp 1—vehicle only Grp 2—1 mg/kg daily Grp 2—10 mg/kg daily Grp 2—100 mg/kg daily | |||||||||
| Docetaxel Bicalutamide CBD-BDS + Docetaxel CBD-BDS + Bicalutamide | Grp 3—5 mg/kg (i.v.) 1× week Grp 4—25–50 mg/kg 3× week (p.o.) Grp 5—100 mg/kg (i.p.) + 5 mg/kg (i.v.) 1× week Grp 6—100 mg/kg (i.p.) + 25–50 mg/kg (p.o.) 3× week | ||||||||
| Morales, 2013 [52] | Athymic nu/nu mice (BALB/cOlaHsd-Foxn1nu) | 5 weeks | 16 mice (n = 8 per group) | Xenograft LNCaP cells | PM49 (synthetic cannabinoid quinone) | Control (vehicle not mentioned) | 2 mg/kg (i.p) | 15 days | Treatment with PM49 almost totally blocked the growth of LNCaP tumors. |
| Xenograft PC3 cells | 40% tumor growth inhibition and final tumor volume was smaller in all four treated mice. | ||||||||
| Olea-Herrero, 2009 [50] | Athymic nu/nu mice | 6 weeks | 24 mice (n = 8 per group) | Xenograft PC3 cells | JWH-015 | Control (saline) | 1.5 mg/mL (s.c.) | 14 days | Final tumor volume and tumor weight were significantly lower in the treatment group (exact % of reduction not mentioned). |
| 1.5 mg/mL (s.c.) | |||||||||
| JWH-015 + SR2 | 1.5 mg/mL + 1.5 mg/kg (s.c.) | ||||||||
| Mukhtar, 2007 [51] | Athymic nu/nu mice | 6–8 weeks | 24 mice (n = 8 per group) | Xenograft 22Rν1 cells | WIN55,212-2 | Control | 0.5 mg/kg (i.p) alternate day | 35 days | Inhibition of tumor growth and decrease in Serum PSA levels to 1.86 ng/mL, whereas that of control group was 7.1 ng/mL. PSA secretion was correlated with tumor growth inhibition (exact % of reduction not mentioned). |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Singh, K.; Jamshidi, N.; Zomer, R.; Piva, T.J.; Mantri, N. Cannabinoids and Prostate Cancer: A Systematic Review of Animal Studies. Int. J. Mol. Sci. 2020, 21, 6265. https://doi.org/10.3390/ijms21176265
Singh K, Jamshidi N, Zomer R, Piva TJ, Mantri N. Cannabinoids and Prostate Cancer: A Systematic Review of Animal Studies. International Journal of Molecular Sciences. 2020; 21(17):6265. https://doi.org/10.3390/ijms21176265
Chicago/Turabian StyleSingh, Kanika, Negar Jamshidi, Roby Zomer, Terrence J. Piva, and Nitin Mantri. 2020. "Cannabinoids and Prostate Cancer: A Systematic Review of Animal Studies" International Journal of Molecular Sciences 21, no. 17: 6265. https://doi.org/10.3390/ijms21176265
APA StyleSingh, K., Jamshidi, N., Zomer, R., Piva, T. J., & Mantri, N. (2020). Cannabinoids and Prostate Cancer: A Systematic Review of Animal Studies. International Journal of Molecular Sciences, 21(17), 6265. https://doi.org/10.3390/ijms21176265







