Gestational Diabetes Mellitus: A Harbinger of the Vicious Cycle of Diabetes
Abstract
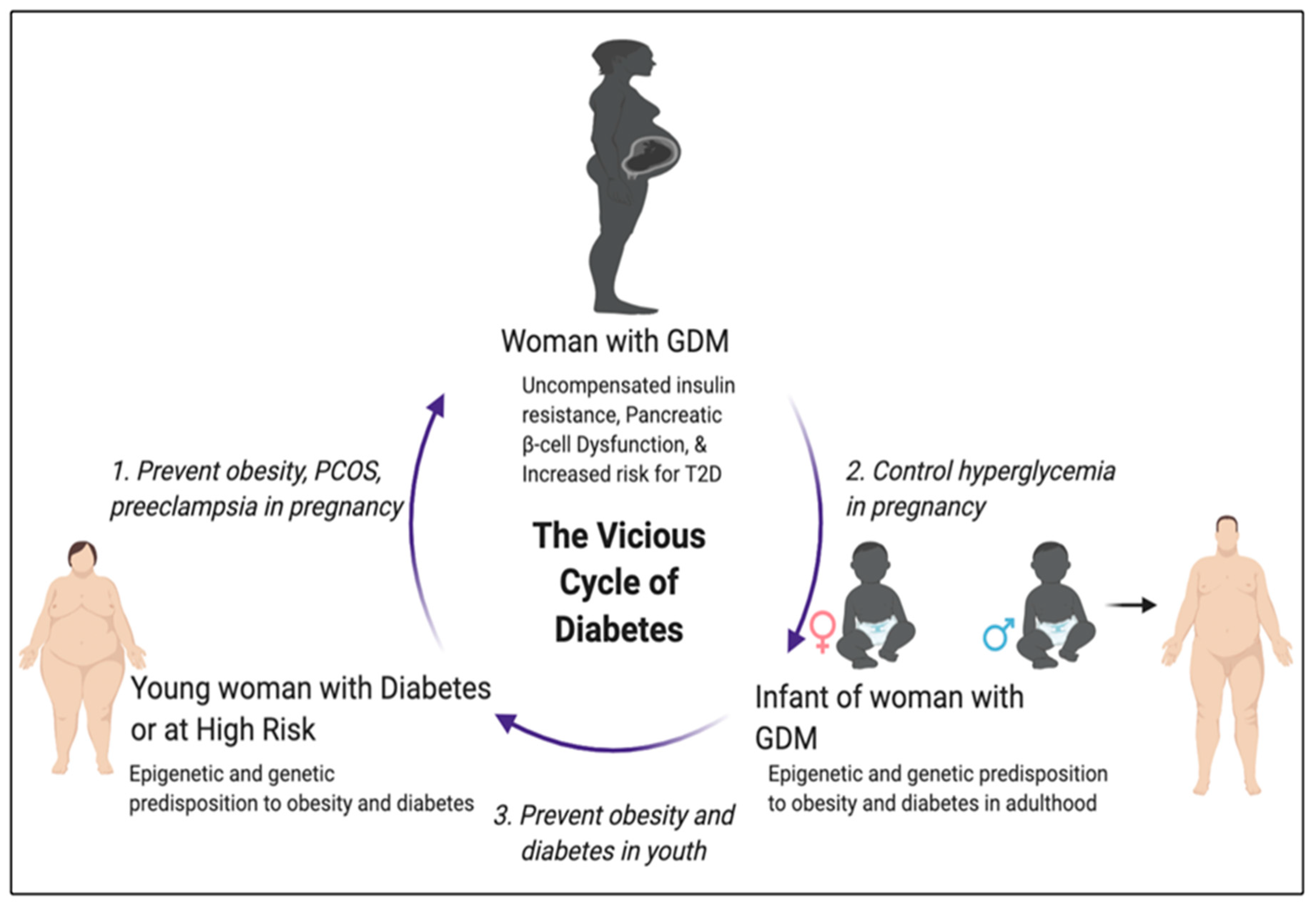
1. Introduction
2. Gestational Diabetes Mellitus
3. Risk Factors for GDM
3.1. Modifiable Risk Factors
3.1.1. Overweight, Obesity, and Pre-Pregnancy Body Mass Index (BMI)
3.1.2. Metabolic Syndrome and Nutritional Diet
3.1.3. Polycystic Ovary Syndrome (PCOS)
3.1.4. Pre-Eclampsia
3.1.5. Additional Modifiable Risk Factors for GDM
3.2. Non-Modifiable Risk Factors
3.2.1. Maternal Age
3.2.2. Gravidity and Parity
3.2.3. Ethnicity
3.2.4. Genetics and Family History of Hyperglycemia
3.3. Socioeconomic and Geographic Risk Factors
3.3.1. Climate and Geographical Location
3.3.2. Education and Socio-Economic Status
3.4. Screening and Diagnosis
3.4.1. Laboratory Evaluation
3.4.2. Criteria for GDM Diagnosis
3.5. Complications
3.5.1. Maternal Complications
3.5.2. Fetal Complications
3.5.3. Neonatal Complications
3.5.4. Childhood and Adulthood Complications
4. Preclinical Models of GDM
4.1. Surgical Models
4.2. Pharmacological Models
4.3. Diet-Induced Models
4.4. Genetic Models
4.5. Fetal Programming Models
5. Concluding Remarks
Funding
Acknowledgments
Conflicts of Interest
References
- Hanson, M.A.; Gluckman, P.D.; Ma, R.C.; Matzen, P.; Biesma, R. Early life opportunities for prevention of diabetes in low and middle income countries. BMC Public Health 2012, 12, 1025. [Google Scholar] [CrossRef]
- Poon, L.C.; Simmons, D.; Hyett, J.A.; Da Fonseca, E.B.; Hod, M. The first-trimester of pregnancy—A window of opportunity for prediction and prevention of pregnancy complications and future life. Diabetes Res. Clin. Pract. 2018, 145, 20–30. [Google Scholar] [CrossRef] [PubMed]
- Catov, J.M.; Margerison-Zilko, C. Pregnancy as a window to future health: Short-term costs and consequences. Am. J. Obstet. Gynecol. 2016, 215, 406–407. [Google Scholar] [CrossRef] [PubMed]
- Godfrey, K.M.; Barker, D.J.; Aranceta, J.; Serra-Majem, L.; Ribas, L.; Pérez-Rodrigo, C. Fetal programming and adult health. Public Health Nutr. 2001, 4, 611–624. [Google Scholar] [CrossRef]
- Hoffman, D.; Reynolds, R.M.; Hardy, D.B. Developmental origins of health and disease: Current knowledge and potential mechanisms. Nutr. Rev. 2017, 75, 951–970. [Google Scholar] [CrossRef] [PubMed]
- Diagnostic criteria and classification of hyperglycaemia first detected in pregnancy: A World Health Organization Guideline. Diabetes Res. Clin. Pract. 2014, 103, 341–363. [CrossRef]
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2013, 36 (Suppl. S1), S67–S74. [Google Scholar] [CrossRef]
- Schneider, S.; Bock, C.; Wetzel, M.; Maul, H.; Loerbroks, A. The prevalence of gestational diabetes in advanced economies. J. Périnat. Med. 2012, 40, 511–520. [Google Scholar] [CrossRef]
- McCance, D.R.; Maresh, M.; Sacks, D.A. A Practical Manual of Diabetes in Pregnancy; Wiley-Blackwell: Chichister, UK, 2010. [Google Scholar]
- Plows, J.F.; Stanley, J.L.; Baker, P.N.; Reynolds, C.; Vickers, M.H. The Pathophysiology of Gestational Diabetes Mellitus. Int. J. Mol. Sci. 2018, 19, 3342. [Google Scholar] [CrossRef]
- Parsons, J.A.; Brelje, T.C.; Sorenson, R.L. Adaptation of islets of Langerhans to pregnancy: Increased islet cell proliferation and insulin secretion correlates with the onset of placental lactogen secretion. Endocrinology 1992, 130, 1459–1466. [Google Scholar]
- Herrera, E. Implications of Dietary Fatty Acids during Pregnancy on Placental, Fetal and Postnatal Development—A Review. Placenta 2002, 23, S9–S19. [Google Scholar] [CrossRef]
- Svensson, H.; Wetterling, L.; Bosaeus, M.; Odén, B.; Odén, A.; Jennische, E.; Edén, S.; Holmäng, A.; Lönn, M. Body fat mass and the proportion of very large adipocytes in pregnant women are associated with gestational insulin resistance. Int. J. Obes. 2015, 40, 646–653. [Google Scholar] [CrossRef]
- Lau, D.C. Central Role of Adipose Tissue in Pregnancy and Lactation. In Maternal-Fetal and Neonatal Endocrinology; Elsevier BV: Amsterdam, The Netherlands, 2020; pp. 147–158. [Google Scholar]
- De Souza, L.R.; Berger, H.; Retnakaran, R.; Maguire, J.L.; Nathens, A.B.; Connelly, P.; Ray, J.G. First-Trimester Maternal Abdominal Adiposity Predicts Dysglycemia and Gestational Diabetes Mellitus in Midpregnancy. Diabetes Care 2015, 39, 61–64. [Google Scholar] [CrossRef] [PubMed]
- Vellinga, A.; Zawiejska, A.; Harreiter, J.; Buckley, B.; Di Cianni, G.; Lapolla, A.; Corcoy, R.; Simmons, D.; Adelantado, J.M.; Damm, P.; et al. Associations of Body Mass Index (Maternal BMI) and Gestational Diabetes Mellitus with Neonatal and Maternal Pregnancy Outcomes in a Multicentre European Database (Diabetes and Pregnancy Vitamin D and Lifestyle Intervention for Gestational Diabetes Mellitus Prevention). ISRN Obes. 2012, 2012, 1–4. [Google Scholar] [CrossRef]
- Chen, C.; Xu, X.; Yan, Y. Estimated global overweight and obesity burden in pregnant women based on panel data model. PLoS ONE 2018, 13, e0202183. [Google Scholar] [CrossRef]
- Cypryk, K.; Pertyńska-Marczewska, M.; Szymczak, W.; Zawodniak-Szałapska, M.; Wilczyński, J.; Lewiński, A. Overweight and obesity as common risk factors for gestational diabetes mellitus (GDM), perinatal macrosomy in offspring and type-2 diabetes in mothers. Prz. Lek. 2005, 62, 38–41. [Google Scholar]
- Miao, M.; Dai, M.; Zhang, Y.; Sun, F.; Guo, X.; Sun, G.-J. Influence of maternal overweight, obesity and gestational weight gain on the perinatal outcomes in women with gestational diabetes mellitus. Sci. Rep. 2017, 7, 305. [Google Scholar] [CrossRef]
- Cnattingius, S.; Villamor, E.; Johansson, S.; Bonamy, A.-K.E.; Persson, M.; Wikström, A.-K.; Granath, F. Maternal Obesity and Risk of Preterm Delivery. JAMA 2013, 309, 2362–2370. [Google Scholar] [CrossRef] [PubMed]
- Çınar, M.; Timur, H.; Aksoy, R.T.; Guzel, A.I.; Tokmak, A.; Findik, R.B.; Uygur, D. Evaluation of maternal and perinatal outcomes among overweight women who experienced stillbirth. J. Matern. Neonatal Med. 2016, 30, 1–20. [Google Scholar] [CrossRef]
- Boney, C.M. Metabolic Syndrome in Childhood: Association With Birth Weight, Maternal Obesity, and Gestational Diabetes Mellitus. Pediatrics 2005, 115, 290–296. [Google Scholar] [CrossRef]
- Catalano, P.M.; Shankar, K. Obesity and pregnancy: Mechanisms of short term and long term adverse consequences for mother and child. BMJ 2017, 356, 1. [Google Scholar] [CrossRef] [PubMed]
- Rasmussen, K.M.; Abrams, B.; Bodnar, L.M.; Butte, N.F.; Catalano, P.M.; Siega-Riz, A.M. Recommendations for Weight Gain During Pregnancy in the Context of the Obesity Epidemic. Obstet. Gynecol. 2010, 116, 1191–1195. [Google Scholar] [CrossRef]
- Morisset, A.-S.; Veillette, J.; Weisnagel, S.J.; Tchernof, A.; Robitaille, J.; St-Yves, A. Prevention of gestational diabetes mellitus: A review of studies on weight management. Diabetes Metab. Res. Rev. 2010, 26, 17–25. [Google Scholar] [CrossRef]
- Hopkins, S.; Artal, R. The Role of Exercise in Reducing the Risks of Gestational Diabetes Mellitus. Women’s Health 2013, 9, 569–581. [Google Scholar] [CrossRef] [PubMed]
- Qi, Y.; Sun, X.; Tan, J.; Zhang, G.; Chen, M.; Xiong, Y.; Chen, P.; Liu, C.; Zou, K.; Liu, X. Excessive gestational weight gain in the first and second trimester is a risk factor for gestational diabetes mellitus among women pregnant with singletons: A repeated measures analysis. J. Diabetes Investig. 2020. [Google Scholar] [CrossRef] [PubMed]
- Wani, K.; Sabico, S.; Alnaami, A.M.; Al-Musharaf, S.; Fouda, M.A.; Turkestani, I.Z.; Al-Ajlan, A.; Alshingetti, N.M.; Alokail, M.S.; Al-Daghri, N.M. Early-Pregnancy Metabolic Syndrome and Subsequent Incidence in Gestational Diabetes Mellitus in Arab Women. Front. Endocrinol. 2020, 11, 98. [Google Scholar] [CrossRef]
- Chatzi, L.; Plana, E.; Pappas, A.; Alegkakis, D.; Karakosta, P.; Daraki, V.; Vassilaki, M.; Tsatsanis, C.; Kafatos, A.; Koutis, A.; et al. The metabolic syndrome in early pregnancy and risk of gestational diabetes mellitus. Nutr. Ther. Interv. Diabetes Metab. Syndr. 2009, 35, 490–494. [Google Scholar] [CrossRef]
- Shin, D.; Lee, K.W.; Song, W.O. Dietary Patterns during Pregnancy Are Associated with Risk of Gestational Diabetes Mellitus. Nutrients 2015, 7, 9369–9382. [Google Scholar] [CrossRef]
- Sedaghat, F.; Akhoondan, M.; Ehteshami, M.; Aghamohammadi, V.; Ghanei, N.; Mirmiran, P.; Rashidkhani, B. Maternal Dietary Patterns and Gestational Diabetes Risk: A Case-Control Study. J. Diabetes Res. 2017, 2017, 1–8. [Google Scholar] [CrossRef]
- Moses, R.G.; Brand-Miller, J. Dietary risk factors for gestational diabetes mellitus: Are sugar-sweetened soft drinks culpable or guilty by association? Diabetes Care 2009, 32, 2314–2315. [Google Scholar] [CrossRef][Green Version]
- Saraf-Bank, S.; Tehrani, H.G.; Haghighatdoost, F.; Moosavian, S.P.; Azadbakht, L. The acidity of early pregnancy diet and risk of gestational diabetes mellitus. Clin. Nutr. 2018, 37, 2054–2059. [Google Scholar] [CrossRef]
- WHO. Diet, Nutrition and the Prevention of Chronic Diseases; WHO Technical Report Series, No. 916 (TRS 916); WHO: Geneva, Switzerland, 2003.
- Vickers, M.H.; Sloboda, D.M. Strategies for Reversing the Effects of Metabolic Disorders Induced as a Consequence of Developmental Programming. Front. Physiol. 2012, 3, 242. [Google Scholar] [CrossRef] [PubMed]
- Mooi, N.; Ncama, B.P. Evidence on nutritional therapy practice guidelines and implementation in adult critically ill patients: A systematic scoping review. Curationis 2019, 42, e1–e13. [Google Scholar] [CrossRef] [PubMed]
- Weickert, M.O.; Möhlig, M.; Koebnick, C.; Holst, J.J.; Namsolleck, P.; Ristow, M.; Osterhoff, M.; Rochlitz, H.; Rudovich, N.; Spranger, J.; et al. Impact of cereal fibre on glucose-regulating factors. Diabetology 2005, 48, 2343–2353. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Liu, S.; Solomon, C.G.; Hu, F.B. Dietary Fiber Intake, Dietary Glycemic Load, and the Risk for Gestational Diabetes Mellitus. Diabetes Care 2006, 29, 2223–2230. [Google Scholar] [CrossRef]
- Brand-Miller, J.; Colagiuri, S.; Crossman, S.; Allen, A.; Roberts, D.C.; Truswell, A.S. Low-Glycemic Index Foods Improve Long-Term Glycemic Control in NIDDM. Diabetes Care 1991, 14, 95–101. [Google Scholar] [CrossRef]
- Shyam, S.; Arshad, F.; Ghani, R.A.; Wahab, N.A.; Safii, N.S.; Yusof, B.N.M.; Chinna, K.; Kamaruddin, N.A. Low glycaemic index diets improve glucose tolerance and body weight in women with previous history of gestational diabetes: A six months randomized trial. Nutr. J. 2013, 12, 68. [Google Scholar] [CrossRef]
- Pitsavos, C.; Panagiotakos, D.B.; Weinem, M.; Stefanadis, C. Diet, Exercise and the Metabolic Syndrome. Rev. Diabet. Stud. 2006, 3, 118–126. [Google Scholar] [CrossRef]
- Filardi, T.; Panimolle, F.; Crescioli, C.; Lenzi, A.; Morano, S. Gestational Diabetes Mellitus: The Impact of Carbohydrate Quality in Diet. Nutrients 2019, 11, 1549. [Google Scholar] [CrossRef]
- Luoto, R.; Laitinen, K.; Nermes, M.; Isolauri, E. Impact of maternal probiotic-supplemented dietary counselling on pregnancy outcome and prenatal and postnatal growth: A double-blind, placebo-controlled study. Br. J. Nutr. 2010, 103, 1792–1799. [Google Scholar] [CrossRef]
- Furness, J.B.; Rivera, L.R.; Cho, H.-J.; Bravo, D.M.; Callaghan, B. The gut as a sensory organ. Nat. Rev. Gastroenterol. Hepatol. 2013, 10, 729–740. [Google Scholar] [CrossRef]
- Isolauri, E.; Rautava, S.; Collado, M.C.; Salminen, S. Role of probiotics in reducing the risk of gestational diabetes. Diabetes Obes. Metab. 2015, 17, 713–719. [Google Scholar] [CrossRef] [PubMed]
- Kalra, B.; Gupta, Y.; Singla, R.; Kalra, S. Use of Oral Anti-Diabetic Agents in Pregnancy: A Pragmatic Approach. N. Am. J. Med. Sci. 2015, 7, 6–12. [Google Scholar] [CrossRef]
- Harris, H.R.; Babic, A.; Webb, P.M.; Nagle, C.M.; Jordan, S.J.; Risch, H.A.; Rossing, M.A.; Doherty, J.A.; Goodman, M.T.; Modugno, F.; et al. Polycystic Ovary Syndrome, Oligomenorrhea, and Risk of Ovarian Cancer Histotypes: Evidence from the Ovarian Cancer Association Consortium. Cancer Epidemiol. Biomark. Prev. 2017, 27, 174–182. [Google Scholar] [CrossRef]
- Pasquali, R.; Zanotti, L.; Fanelli, F.; Mezzullo, M.; Fazzini, A.; Morselli-Labate, A.M.; Repaci, A.; Ribichini, D.; Gambineri, A. Defining Hyperandrogenism in Women With Polycystic Ovary Syndrome: A Challenging Perspective. J. Clin. Endocrinol. Metab. 2016, 101, 2013–2022. [Google Scholar] [CrossRef]
- Dunaif, A. Insulin resistance and the polycystic ovary syndrome: Mechanism and implications for pathogenesis. Endocr. Rev. 1997, 18, 774–800. [Google Scholar] [PubMed]
- Bhathena, R.K. Insulin resistance and the long-term consequences of polycystic ovary syndrome. J. Obstet. Gynaecol. 2011, 31, 105–110. [Google Scholar] [CrossRef] [PubMed]
- Mustaniemi, S.; Vääräsmäki, M.; Eriksson, J.G.; Gissler, M.; Laivuori, H.; Ijäs, H.; Bloigu, A.; Kajantie, E.; Morin-Papunen, L. Polycystic ovary syndrome and risk factors for gestational diabetes. Endocr. Connect. 2018, 7, 859–869. [Google Scholar] [CrossRef]
- Li, G.; Huang, W.; Zhang, L.; Tian, Z.; Zheng, W.; Wang, T.; Zhang, T.; Zhang, W. A prospective cohort study of early-pregnancy risk factors for gestational diabetes in polycystic ovarian syndrome. Diabetes Metab. Res. Rev. 2018, 34, e3003. [Google Scholar] [CrossRef]
- Lo, J.C.; Feigenbaum, S.L.; Escobar, G.J.; Yang, J.; Crites, Y.M.; Ferrara, A. Increased Prevalence of Gestational Diabetes Mellitus Among Women With Diagnosed Polycystic Ovary Syndrome: A population-based study. Diabetes Care 2006, 29, 1915–1917. [Google Scholar] [CrossRef]
- Norman, R.J.; Davies, M.; Lord, J.; Moran, L.J. The role of lifestyle modification in polycystic ovary syndrome. Trends Endocrinol. Metab. 2002, 13, 251–257. [Google Scholar] [CrossRef]
- Douglas, C.C.; Gower, B.A.; Darnell, B.E.; Ovalle, F.; Oster, R.; Azziz, R. Role of diet in the treatment of polycystic ovary syndrome. Fertil. Steril. 2006, 85, 679–688. [Google Scholar] [CrossRef] [PubMed]
- Radosh, L. Drug treatments for polycystic ovary syndrome. Am. Fam. Physician 2009, 79, 671–676. [Google Scholar]
- Jeyabalan, A. Epidemiology of preeclampsia: Impact of obesity. Nutr. Rev. 2013, 71, S18–S25. [Google Scholar] [CrossRef] [PubMed]
- Cho, G.J.; Kim, H.Y.; Park, J.H.; Ahn, K.-H.; Hong, S.-C.; Kim, H.-J.; Han, S.W.; Oh, M.-J. Prepregnancy Factors Are Associated with Development of Hypertension Later in Life in Women with Pre-Eclampsia. J. Women’s Health 2019, 28, 984–989. [Google Scholar] [CrossRef]
- Gutaj, P.; Zawiejska, A.; Mantaj, U.; Wender-Ożegowska, E. Determinants of preeclampsia in women with type 1 diabetes. Acta Diabetol. 2017, 54, 1115–1121. [Google Scholar] [CrossRef] [PubMed]
- Hedderson, M.; Ferrara, A. High Blood Pressure Before and During Early Pregnancy is Associated with an Increased Risk of Gestational Diabetes Mellitus. Diabetes Care 2008, 31, 2362–2367. [Google Scholar] [CrossRef]
- Lee, J.; Ouh, Y.-T.; Ahn, K.H.; Hong, S.C.; Oh, M.-J.; Kim, H.-J.; Cho, G.J. Preeclampsia: A risk factor for gestational diabetes mellitus in subsequent pregnancy. PLoS ONE 2017, 12, e0178150. [Google Scholar] [CrossRef] [PubMed]
- Kitzmiller, J.L.; Block, J.M.; Brown, F.M.; Catalano, P.M.; Conway, D.L.; Coustan, D.R.; Gunderson, E.P.; Herman, W.H.; Hoffman, L.D.; Inturrisi, M.; et al. Managing Preexisting Diabetes for Pregnancy: Summary of evidence and consensus recommendations for care. Diabetes Care 2008, 31, 1060–1079. [Google Scholar] [CrossRef] [PubMed]
- Horsch, A.; Kang, J.S.; Vial, Y.; Ehlert, U.; Borghini, A.; Marques-Vidal, P.; Jacobs, I.; Puder, J.J. Stress exposure and psychological stress responses are related to glucose concentrations during pregnancy. Br. J. Health Psychol. 2016, 21, 712–729. [Google Scholar] [CrossRef] [PubMed]
- Myoga, M.; Japan Environment and Children’s Study; Tsuji, M.; Tanaka, R.; Shibata, E.; Askew, D.J.; Aiko, Y.; Senju, A.; Kawamoto, T.; Hachisuga, T.; et al. Impact of sleep duration during pregnancy on the risk of gestational diabetes in the Japan environmental and Children’s study (JECS). BMC Pregnancy Childbirth 2019, 19, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Hosler, A.S.; Nayak, S.; Radigan, A.M. Stressful events, smoking exposure and other maternal risk factors associated with gestational diabetes mellitus. Paediatr. Périnat. Epidemiol. 2011, 25, 566–574. [Google Scholar] [CrossRef]
- Loeken, M.R. Passive smoking as an independent risk factor for gestational diabetes that synergizes with prepregnancy obesity in urban Chinese women. Diabetes Metab. Res. Rev. 2017, 33, e2910. [Google Scholar] [CrossRef]
- Lee, K.W.; Ching, S.M.; Ramachandran, V.; Yee, A.; Hoo, F.K.; Chia, Y.C.; Sulaiman, W.A.W.; Suppiah, S.; Mohamed, M.H.; Veettil, S.K. Prevalence and risk factors of gestational diabetes mellitus in Asia: A systematic review and meta-analysis. BMC Pregnancy Childbirth 2018, 18, 494. [Google Scholar] [CrossRef]
- Larrabure-Torrealva, G.; Martinez, S.; Luque-Fernández, M.-Á.; Sanchez, S.E.; Mascaro-Sánchez, P.; Ingar, H.; Castillo, W.; Zumaeta, R.; Grande, M.; Motta, V.; et al. Prevalence and risk factors of gestational diabetes mellitus: Findings from a universal screening feasibility program in Lima, Peru. BMC Pregnancy Childbirth 2018, 18, 303. [Google Scholar] [CrossRef] [PubMed]
- Abu-Heija, A.; Al-Bash, M.R.; Al-Kalbani, M.A. Effects of maternal age, parity and pre-pregnancy body mass index on the glucose challenge test and gestational diabetes mellitus. J. Taibah Univ. Med. Sci. 2017, 12, 338–342. [Google Scholar] [CrossRef]
- Mishra, S.; Shetty, A.; Rao, C.R.; Nayak, S.; Kamath, A. Risk factors for gestational diabetes mellitus: A prospective case-control study from coastal Karnataka. Clin. Epidemiol. Glob. Health 2020. [Google Scholar] [CrossRef]
- Li, Y.; Ren, X.; He, L.; Li, J.; Zhang, S.; Chen, W. Maternal age and the risk of gestational diabetes mellitus: A systematic review and meta-analysis of over 120 million participants. Diabetes Res. Clin. Pract. 2020, 162, 108044. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.-C.; Hung, C.; Ke, L.-Y.; Lin, K.-C.; Hsu, Y.-Y.; Tzeng, Y.-L. The risk factors for gestational diabetes mellitus: A retrospective study. Midwifery 2016, 42, 16–20. [Google Scholar] [CrossRef]
- Souza De Oliveira Dode, M.A.; Dos Santos, I.S. Non classical risk factors for gestational diabetes mellitus: A systematic review of the literature. Cad. Saúde Pública 2009, 25, S341–S359. [Google Scholar] [CrossRef]
- Wan, C.S.; Abell, S.; Aroni, R.; Nankervis, A.; Boyle, J.; Teede, H.J. Ethnic differences in prevalence, risk factors, and perinatal outcomes of gestational diabetes mellitus: A comparison between immigrant ethnic Chinese women and Australian-born Caucasian women in Australia. J. Diabetes 2019, 11, 809–817. [Google Scholar] [CrossRef]
- Pedula, K.L.; Hillier, T.A.; Schmidt, M.M.; Mullen, J.A.; Charles, M.A.; Pettitt, D.J. Ethnic differences in gestational oral glucose screening in a large US population. Ethn. Dis. 2009, 19, 414–419. [Google Scholar]
- Hall, L.M.L.; Moran, C.N.; Milne, G.R.; Wilson, J.; Macfarlane, N.G.; Forouhi, N.G.; Hariharan, N.; Salt, I.P.; Sattar, N.; Gill, J.M. Fat Oxidation, Fitness and Skeletal Muscle Expression of Oxidative/Lipid Metabolism Genes in South Asians: Implications for Insulin Resistance? PLoS ONE 2010, 5, e14197. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.S.; Kim, B.C.; Daily, J.; Park, S. High genetic risk scores for impaired insulin secretory capacity doubles the risk for type 2 diabetes in Asians and is exacerbated by Western-type diets. Diabetes Metab. Res. Rev. 2017, 34, e2944. [Google Scholar] [CrossRef]
- Lowe, W.L.; Scholtens, D.; Sandler, V.; Hayes, M.G.; Lowe, W.L. Genetics of Gestational Diabetes Mellitus and Maternal Metabolism. Curr. Diabetes Rep. 2016, 16, 15. [Google Scholar] [CrossRef]
- Lauenborg, J.; Grarup, N.; Damm, P.; Borch-Johnsen, K.; Jørgensen, T.; Pedersen, O.; Hansen, T. Common Type 2 Diabetes Risk Gene Variants Associate with Gestational Diabetes. J. Clin. Endocrinol. Metab. 2009, 94, 145–150. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, R.M.; Allayee, H.; Xiang, A.H.; Trigo, E.; Hartiala, J.; Lawrence, J.M.; Buchanan, T.A. Transcription factor 7-like 2 (TCF7L2) is associated with gestational diabetes mellitus and interacts with adiposity to alter insulin secretion in Mexican Americans. Diabetes 2007, 56, 1481–1485. [Google Scholar] [CrossRef] [PubMed]
- Papadopoulou, A.; Lynch, K.F.; Shaat, N.; Hakansson, R.; Ivarsson, S.A.; Berntorp, K.; Agardh, C.D.; Lernmark, Å. DiPiS Study Group Gestational diabetes mellitus is associated with TCF7L2 gene polymorphisms independent of HLA-DQB1*0602 genotypes and islet cell autoantibodies. Diabet. Med. 2011, 28, 1018–1027. [Google Scholar] [CrossRef]
- Vejražková, D.; Lukasova, P.; Vanková, M.; Vcelák, J.; Bradnova, O.; Cirmanova, V.; Andelova, K.; Krejci, H.; Bendlova, B. MTNR1B Genetic Variability Is Associated with Gestational Diabetes in Czech Women. Int. J. Endocrinol. 2014, 2014, 1–7. [Google Scholar] [CrossRef]
- Vlassi, M.; Gazouli, M.; Paltoglou, G.; Christopoulos, P.; Florentin, L.; Kassi, G.; Mastorakos, G. The rs10830963 variant of melatonin receptor MTNR1B is associated with increased risk for gestational diabetes mellitus in a Greek population. Hormones 2012, 11, 70–76. [Google Scholar] [CrossRef]
- Kwak, S.H.; Kim, S.-H.; Cho, Y.M.; Go, M.J.; Cho, Y.S.; Choi, S.H.; Moon, M.K.; Jung, H.S.; Shin, H.D.; Kang, H.M.; et al. A Genome-Wide Association Study of Gestational Diabetes Mellitus in Korean Women. Diabetes 2012, 61, 531–541. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Chen, Q.; Feng, Y.; Yang, H.; Wu, W.; Zhang, P.; Wang, Y.; Ko, J.; Zhao, F.; Du, W.; et al. Single Nucleotide Polymorphisms in CDKAL1 Gene Are Associated with Risk of Gestational Diabetes Mellitus in Chinese Population. J. Diabetes Res. 2019, 2019, 3618103–3618107. [Google Scholar] [CrossRef]
- Fatima, S.S.; Chaudhry, B.; Khan, T.A.; Farooq, S. KCNQ1 rs2237895 polymorphism is associated with Gestational Diabetes in Pakistani Women. Pak. J. Med Sci. 2016, 32, 1380–1385. [Google Scholar] [CrossRef]
- Shin, H.D.; Park, B.L.; Shin, H.J.; Kim, J.Y.; Park, S.; Kim, B.; Kim, S.-H. Association ofKCNQ1Polymorphisms with the Gestational Diabetes Mellitus in Korean Women. J. Clin. Endocrinol. Metab. 2010, 95, 445–449. [Google Scholar] [CrossRef] [PubMed]
- Alharbi, K.K.; Khan, I.A.; Abotalib, Z.; Al-Hakeem, M.M. Insulin Receptor Substrate-1 (IRS-1) Gly927Arg: Correlation with Gestational Diabetes Mellitus in Saudi Women. BioMed Res. Int. 2014, 2014, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Tok, E.C.; Ertunc, D.; Bilgin, O.; Erdal, E.M.; Kaplanoğlu, M.; Dilek, S.; Erdal, M.E. Association of insulin receptor substrate-1 G972R variant with baseline characteristics of the patients with gestational diabetes mellitus. Am. J. Obstet. Gynecol. 2006, 194, 868–872. [Google Scholar] [CrossRef] [PubMed]
- Yahaya, T.; Anyebe, D. Genes predisposing to neonatal diabetes mellitus and pathophysiology: Current findings. J. Neonatal-Perinatal Med. 2020, 1–11. [Google Scholar] [CrossRef]
- Lehnen, H.; Zechner, U.; Haaf, T. Epigenetics of gestational diabetes mellitus and offspring health: The time for action is in early stages of life. Mol. Hum. Reprod. 2013, 19, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Ding, G.-L.; Huang, H.-F. Paternal transgenerational glucose intolerance with epigenetic alterations in second generation offspring of GDM. Asian J. Androl. 2013, 15, 451–452. [Google Scholar] [CrossRef] [PubMed]
- Litwin, L.; Sundholm, J.K.M.; Rönö, K.; Koivusalo, S.B.; Eriksson, J.G.; Sarkola, T. Transgenerational effects of maternal obesity and gestational diabetes on offspring body composition and left ventricle mass: The Finnish Gestational Diabetes Prevention Study (RADIEL) 6-year follow-up. Diabet. Med. 2019, 37, 147–156. [Google Scholar] [CrossRef]
- Franzago, M.; Fraticelli, F.; Stuppia, L.; Vitacolonna, E. Nutrigenetics, epigenetics and gestational diabetes: Consequences in mother and child. Epigenetics 2019, 14, 215–235. [Google Scholar] [CrossRef]
- Huang, T.; Shu, Y.; Cai, Y. Genetic differences among ethnic groups. BMC Genom. 2015, 16, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Yuan, V.; Price, E.M.; Del Gobbo, G.; Mostafavi, S.; Cox, B.J.; Binder, A.M.; Michels, K.B.; Marsit, C.J.; Robinson, W.P. Accurate ethnicity prediction from placental DNA methylation data. Epigenet. Chromatin 2019, 12. [Google Scholar] [CrossRef] [PubMed]
- Carolan, M.; Davey, M.-A.; Biro, M.A.; Kealy, M. Maternal age, ethnicity and gestational diabetes mellitus. Midwifery 2012, 28, 778–783. [Google Scholar] [CrossRef] [PubMed]
- Jenum, A.K.; Mørkrid, K.; Sletner, L.; Vange, S.; Torper, J.L.; Nakstad, B.; Voldner, N.; Rognerud-Jensen, O.H.; Berntsen, S.; Mosdøl, A.; et al. Impact of ethnicity on gestational diabetes identified with the WHO and the modified International Association of Diabetes and Pregnancy Study Groups criteria: A population-based cohort study. Eur. J. Endocrinol. 2012, 166, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Robitaille, J.; Grant, A. The genetics of gestational diabetes mellitus: Evidence for relationship with type 2 diabetes mellitus. Genet. Med. 2008, 10, 240–250. [Google Scholar] [CrossRef]
- Yu, X.; Wang, Q.; Qin, L.; Peng, L.; Chen, Z.; Qin, X.; Wang, Y.; Shi, Q.; Yu, H. Association between a functional polymorphism rs10830963 in melatonin receptor 1B and risk of gestational diabetes mellitus: An updated meta-analysis. bioRxiv 2017. [Google Scholar] [CrossRef]
- Park, H.; He, A.; Lodhi, I.J. Lipid Regulators of Thermogenic Fat Activation. Trends Endocrinol. Metab. 2019, 30, 710–723. [Google Scholar] [CrossRef]
- Kajimura, S.; Spiegelman, B.; Seale, P. Brown and Beige Fat: Physiological Roles beyond Heat Generation. Cell Metab. 2015, 22, 546–559. [Google Scholar] [CrossRef]
- Celi, F.S.; Brychta, R.J.; Linderman, J.D.; Butler, P.W.; Alberobello, A.T.; Smith, S.; Courville, A.B.; Lai, E.W.; Costello, R.; Skarulis, M.C.; et al. Minimal changes in environmental temperature result in a significant increase in energy expenditure and changes in the hormonal homeostasis in healthy adults. Eur. J. Endocrinol. 2010, 163, 863–872. [Google Scholar] [CrossRef]
- Wolf, K.; Schneider, A.; Breitner, S.; Von Klot, S.; Meisinger, C.; Cyrys, J.; Hymer, H.; Wichmann, H.-E.; Peters, A.; for the Cooperative Health Research in the Region of Augsburg (KORA) Study Group. Air Temperature and the Occurrence of Myocardial Infarction in Augsburg, Germany. Circulation 2009, 120, 735–742. [Google Scholar] [CrossRef]
- Shi, L.; Kloog, I.; Zanobetti, A.; Liu, P.; Schwartz, J. Impacts of temperature and its variability on mortality in New England. Nat. Clim. Chang. 2015, 5, 988–991. [Google Scholar] [CrossRef] [PubMed]
- Vasileiou, V.; Kyratzoglou, E.; Paschou, S.A.; Kyprianou, M.; Anastasiou, E. The impact of environmental temperature on the diagnosis of gestational diabetes mellitus. Eur. J. Endocrinol. 2018, 178, 209–214. [Google Scholar] [CrossRef] [PubMed]
- Price, L.A.; Lock, L.J.; Archer, L.E.; Ahmed, Z. Awareness of Gestational Diabetes and its Risk Factors among Pregnant Women in Samoa. Hawai’i J. Med. Public Health 2017, 76, 48–54. [Google Scholar]
- Ansarzadeh, S.; Salehi, L.; Mahmoodi, Z.; Mohammadbeigi, A. Factors affecting the quality of life in women with gestational diabetes mellitus: A path analysis model. Health Qual. Life Outcomes 2020, 18, 1–9. [Google Scholar] [CrossRef]
- Ogu, R.N.; Maduka, O.; Agala, V.; Alamina, F.; Adebiyi, O.; Edewor, U.; Porbeni, I.; Abam, C. Gestational Diabetes Mellitus Knowledge Among Women of Reproductive Age in Southern Nigeria: Implications for Diabetes Education. Int. Q. Community Health Educ. 2019, 40, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Rönö, K.; Masalin, S.; Kautiainen, H.; Gissler, M.; Raina, M.; Eriksson, J.G.; Kainulainen, H. Impact of maternal income on the risk of gestational diabetes mellitus in primiparous women. Diabet. Med. 2019, 36, 214–220. [Google Scholar] [CrossRef]
- Nelson, K.M.; Chapko, M.K.; Reiber, G.; Boyko, E.J. The Association between Health Insurance Coverage and Diabetes Care; Data from the 2000 Behavioral Risk Factor Surveillance System. Health Serv. Res. 2005, 40, 361–372. [Google Scholar] [CrossRef]
- Hsu, C.-C.; Lee, C.-H.; Wahlqvist, M.L.; Huang, H.-L.; Chang, H.-Y.; Chen, L.; Shih, S.-F.; Shin, S.-J.; Tsai, W.-C.; Chen, T.; et al. Poverty Increases Type 2 Diabetes Incidence and Inequality of Care Despite Universal Health Coverage. Diabetes Care 2012, 35, 2286–2292. [Google Scholar] [CrossRef]
- Petkova, V.; Dimitrov, M.; Geourgiev, S. Pilot project for education of gestational diabetes mellitus (GDM) patients—Can it be beneficial? Afr. J. Pharm. Pharmacol. 2011, 5, 1282–1286. [Google Scholar] [CrossRef]
- Alayoub, H.; Curran, S.; Coffey, M.; Hatunic, M.; Higgins, M.F. Assessment of the effectiveness of group education on knowledge for women with newly diagnosed gestational diabetes. Ir. J. Med Sci. 2017, 187, 65–68. [Google Scholar] [CrossRef] [PubMed]
- Minschart, C.; Amuli, K.; Delameillieure, A.; Calewaert, P.; Mathieu, C.; Benhalima, K. Multidisciplinary Group Education for Gestational Diabetes Mellitus: A Prospective Observational Cohort Study. J. Clin. Med. 2020, 9, 509. [Google Scholar] [CrossRef] [PubMed]
- Mirfeizi, M.; Tourzani, Z.M.; Jafarabadi, M.A.; Hanjani, S.M.; Hasanzad, M. Health education in gestational diabetes mellitus and quality of life. J. Midwifery Reprod. Health 2017, 5, 1066–1074. [Google Scholar]
- Caughey, A.B.; Turrentine, M. ACOG Practice Bulletin No. 190 Summary: Gestational Diabetes Mellitus. Obstet. Gynecol. 2018, 131, 406–408. [Google Scholar]
- Rani, P.R.; Begum, J. Screening and Diagnosis of Gestational Diabetes Mellitus, Where Do We Stand. J. Clin. Diagn. Res. 2016, 10, QE01–QE04. [Google Scholar] [CrossRef]
- McIntyre, H.D.; Colagiuri, S.; Roglic, G.; Hod, M. Diagnosis of GDM: A suggested consensus. Best Pract. Res. Clin. Obstet. Gynaecol. 2015, 29, 194–205. [Google Scholar] [CrossRef]
- Hosseini, E.; Janghorbani, M.; Aminorroaya, A. Incidence, risk factors, and pregnancy outcomes of gestational diabetes mellitus using one-step versus two-step diagnostic approaches: A population-based cohort study in Isfahan, Iran. Diabetes Res. Clin. Pract. 2018, 140, 288–294. [Google Scholar] [CrossRef]
- Akgol, S.; Obut, M.; Kahveci, B.; Budak, M.S.; Baglı, I. An Evaluation of the Effect of a One or Two-Step Gestational Diabetes Mellitus Screening Program on Obstetric and Neonatal Outcomes in Pregnancies. Gynecol. Obstet. Reprod. Med. 2018, 25, 1–5. [Google Scholar] [CrossRef]
- Burtis, C.A.; Bruns, D.E. Tietz Fundamentals of Clinical Chemistry and Molecular Diagnostics, 7th ed.; Elsevier: St. Louis, MI, USA, 2015. [Google Scholar]
- Luewan, S.; Bootchaingam, P.; Tongsong, T. Comparison of the Screening Tests for Gestational Diabetes Mellitus between “One-Step” and “Two-Step” Methods among Thai Pregnant Women. Obstet. Gynecol. Int. 2018, 2018, 1–5. [Google Scholar] [CrossRef]
- Berghella, V.; Caissutti, C.; Saccone, G.; Khalifeh, A. One-Step Approach to Identifying Gestational Diabetes Mellitus. Obstet. Gynecol. 2019, 133, 383. [Google Scholar] [CrossRef]
- Brown, J.; Alwan, N.A.; West, J.; Brown, S.; McKinlay, C.; Farrar, D.; Crowther, C.A. Lifestyle interventions for the treatment of women with gestational diabetes. Cochrane Database Syst. Rev. 2017, 2017, 959. [Google Scholar] [CrossRef]
- Celen, S.; Yildiz, Y.; Kahyaoglu, S.; Kaymak, O.; Ozel, M.; Timur, H.; Danişman, N. Cost-Effectivity Analysis of One-Step Versus Two-Step Screening for Gestational Diabetes. Eurasian J. Med. 2012, 44, 84–87. [Google Scholar] [CrossRef] [PubMed]
- Meltzer, S.J.; Snyder, J.; Penrod, J.; Nudi, M.; Morin, L. Gestational diabetes mellitus screening and diagnosis: A prospective randomised controlled trial comparing costs of one-step and two-step methods. BJOG Int. J. Obstet. Gynaecol. 2010, 117, 407–415. [Google Scholar] [CrossRef] [PubMed]
- Nankervis, A.; McIntyre, H.D.; Moses, R.G.; Ross, G.P.; Callaway, L.K. Testing for Gestational Diabetes Mellitus in Australia. Diabetes Care 2013, 36, e64. [Google Scholar] [CrossRef]
- Diabetes Canada Clinical Practice Guidelines Expert Committee; Feig, D.S.; Berger, H.; Donovan, L.; Godbout, A.; Kader, T.; Keely, E.; Sanghera, R. Diabetes and Pregnancy. Can. J. Diabetes 2018, 42 (Suppl. S1), S255–S282. [Google Scholar]
- Kleinwechter, H.; Schäfer-Graf, U.; Bührer, C.; Hoesli, I.; Kainer, F.; Kautzky-Willer, A.; Pawlowski, B.; Schunck, K.; Somville, T.; Sorger, M. Gestational Diabetes Mellitus (GDM) Diagnosis, Therapy and Follow-Up Care. Exp. Clin. Endocrinol. Diabetes 2014, 122, 395–405. [Google Scholar] [CrossRef]
- Vitacolonna, E.; Succurro, E.; Lapolla, A.; Scavini, M.; Bonomo, M.; Di Cianni, G.; Di Benedetto, A.; Napoli, A.; Tumminia, A.; Festa, C.; et al. Guidelines for the screening and diagnosis of gestational diabetes in Italy from 2010 to 2019: Critical issues and the potential for improvement. Acta Diabetol. 2019, 56, 1159–1167. [Google Scholar] [CrossRef]
- Metzger, B.E.; Lowe, L.P.; Dyer, A.R.; Trimble, E.R.; Chaovarindr, U.; Coustan, D.R.; Hadden, D.R.; McCance, D.; Hod, M.; McIntyre, H.D.; et al. Hyperglycemia and Adverse Pregnancy Outcomes. N. Engl. J. Med. 2008, 358, 1991–2002. [Google Scholar] [CrossRef]
- Behboudi-Gandevani, S.; Amiri, M.; Yarandi, R.B.; Tehrani, F.R. The impact of diagnostic criteria for gestational diabetes on its prevalence: A systematic review and meta-analysis. Diabetol. Metab. Syndr. 2019, 11, 1–18. [Google Scholar] [CrossRef]
- Weinert, L.S. International Association of Diabetes and Pregnancy Study Groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy: Comment to the International Association of Diabetes and Pregnancy Study Groups Consensus Panel. Diabetes Care 2010, 33, e97. [Google Scholar] [CrossRef]
- Schmidt, M.I.; Duncan, B.B.; Reichelt, A.J.; Branchtein, L.; Matos, M.C.; Forti, A.C.E.; Spichler, E.R.; Pousada, J.M.; Teixeira, M.M.; Yamashita, T. Gestational diabetes mellitus diagnosed with a 2-h 75-g oral glucose tolerance test and adverse pregnancy outcomes. Diabetes Care 2001, 24, 1151–1155. [Google Scholar] [CrossRef] [PubMed]
- Lehmann, R.; Troendle, A.; Brandle, M. New insights into diagnosis and management of gestational diabetes mellitus: Recommendations of the Swiss Society for Endocrinology and Diabetes. Ther. Umsch. 2009, 66, 695–706. [Google Scholar] [CrossRef] [PubMed]
- Cortel, M.R.B.P.; Manalo, M.E.M.; Canivel, R.R.C.; Matias, R.S.; Dizon, A.J.B.; Bacani, M.N.S.; Dalmacio, J.S.B. Screening and Diagnosis of Gestational Diabetes Mellitus Using 75-g Oral Glucose Tolerance Test Following the WHO, ADA, and IADPSG Criteria. J. Diabetes Metab. 2018, 9, 1–4. [Google Scholar] [CrossRef]
- Stanley, J.; Cheung, C.C.; Rueda-Clausen, C.; Sankaralingam, S.; Baker, P.N.; Davidge, S.T. Effect of Gestational Diabetes on Maternal Artery Function. Reprod. Sci. 2011, 18, 342–352. [Google Scholar] [CrossRef]
- Dharmashankar, K.; Widlansky, M.E. Vascular Endothelial Function and Hypertension: Insights and Directions. Curr. Hypertens. Rep. 2010, 12, 448–455. [Google Scholar] [CrossRef]
- Sullivan, S.D.; Umans, J.G.; Ratner, R.E. Gestational Diabetes: Implications for Cardiovascular Health. Curr. Diabetes Rep. 2011, 12, 43–52. [Google Scholar] [CrossRef]
- Powe, C.E.; Levine, R.J.; Karumanchi, S.A. Preeclampsia, a disease of the maternal endothelium: The role of antiangiogenic factors and implications for later cardiovascular disease. Circulation 2011, 123, 2856–2869. [Google Scholar] [CrossRef]
- Weissgerber, T.; Mudd, L.M. Preeclampsia and diabetes. Curr. Diabetes Rep. 2015, 15, 9–579. [Google Scholar] [CrossRef]
- Miao, Z.; Wu, H.; Ren, L.; Bu, N.; Jiang, L.; Yang, H.; Zhang, J.; Guo, X. Long-Term Postpartum Outcomes of Insulin Resistance and beta-cell Function in Women with Previous Gestational Diabetes Mellitus. Int. J. Endocrinol. 2020, 2020, 7417356. [Google Scholar] [CrossRef]
- Rayanagoudar, G.; Hashi, A.A.; Zamora, J.; Khan, K.S.; Hitman, G.; Thangaratinam, S. Quantification of the type 2 diabetes risk in women with gestational diabetes: A systematic review and meta-analysis of 95,750 women. Diabetology 2016, 59, 1403–1411. [Google Scholar] [CrossRef]
- Chivese, T.; Norris, S.A.; Levitt, N.S. Progression to type 2 diabetes mellitus and associated risk factors after hyperglycemia first detected in pregnancy: A cross-sectional study in Cape Town, South Africa. PLoS Med. 2019, 16, e1002865. [Google Scholar] [CrossRef] [PubMed]
- Eades, C.; Styles, M.; Leese, G.P.; Cheyne, H.; Evans, J.M.M. Progression from gestational diabetes to type 2 diabetes in one region of Scotland: An observational follow-up study. BMC Pregnancy Childbirth 2015, 15, 11. [Google Scholar] [CrossRef]
- Noctor, E.; Dunne, F.P. Type 2 diabetes after gestational diabetes: The influence of changing diagnostic criteria. World J. Diabetes 2015, 6, 234–244. [Google Scholar] [CrossRef] [PubMed]
- Herath, H.; Herath, R.P.; Wickremasinghe, R. Gestational diabetes mellitus and risk of type 2 diabetes 10 years after the index pregnancy in Sri Lankan women—A community based retrospective cohort study. PLoS ONE 2017, 12, e0179647. [Google Scholar] [CrossRef] [PubMed]
- Coustan, D.R. Recurrent GDM and the development of type 2 diabetes have similar risk factors. Endocrine 2016, 53, 624–625. [Google Scholar] [CrossRef][Green Version]
- Kruse, A.; Darling, M.S.; Hansen, M.K.L.; Markman, M.J.; Lauszus, F.; Wielandt, H.B. Recurrence of gestational diabetes in primiparous women. Acta Obstet. Gynecol. Scand. 2015, 94, 1367–1372. [Google Scholar] [CrossRef]
- Wang, Y.-Y.; Liu, Y.; Li, C.; Lin, J.; Liu, X.-M.; Sheng, J.-Z.; Huang, H.-F. Frequency and risk factors for recurrent gestational diabetes mellitus in primiparous women: A case control study. BMC Endocr. Disord. 2019, 19, 1–7. [Google Scholar] [CrossRef]
- Kc, K.; Shakya, S.; Zhang, H. Gestational Diabetes Mellitus and Macrosomia: A Literature Review. Ann. Nutr. Metab. 2015, 66, 14–20. [Google Scholar] [CrossRef]
- Illsley, N.; Baumann, M.U. Human placental glucose transport in fetoplacental growth and metabolism. Biochim. Biophys. Acta Mol. Basis Dis. 2020, 1866, 165359. [Google Scholar] [CrossRef]
- Yoon, M.-S. The Role of Mammalian Target of Rapamycin (mTOR) in Insulin Signaling. Nutrients 2017, 9, 1176. [Google Scholar] [CrossRef]
- Rosario, F.J.; Powell, T.L.; Jansson, T. Activation of placental insulin and mTOR signaling in a mouse model of maternal obesity associated with fetal overgrowth. Am. J. Physiol. Integr. Comp. Physiol. 2016, 310, R87–R93. [Google Scholar] [CrossRef] [PubMed]
- Dimasuay, K.G.; Boeuf, P.; Powell, T.L.; Jansson, T. Placental Responses to Changes in the Maternal Environment Determine Fetal Growth. Front. Physiol. 2016, 7, 2759. [Google Scholar] [CrossRef] [PubMed]
- Hart, B.; Morgan, E.; Alejandro, E.U. Nutrient sensor signaling pathways and cellular stress in fetal growth restriction. J. Mol. Endocrinol. 2019, 62, R155–R165. [Google Scholar] [CrossRef] [PubMed]
- Catalano, P.M.; Mouzon, S.H.-D. Is it time to revisit the Pedersen hypothesis in the face of the obesity epidemic? Am. J. Obstet. Gynecol. 2011, 204, 479–487. [Google Scholar] [CrossRef] [PubMed]
- Castillo-Castrejon, M.; Powell, T.L. Placental Nutrient Transport in Gestational Diabetic Pregnancies. Front. Endocrinol. 2017, 8, 306. [Google Scholar] [CrossRef]
- Logan, K.M.; Gale, C.; Hyde, M.; Santhakumaran, S.; Modi, N. Diabetes in pregnancy and infant adiposity: Systematic review and meta-analysis. Arch. Dis. Child. Fetal Neonatal Ed. 2016, 102, F65–F72. [Google Scholar] [CrossRef] [PubMed]
- Sovio, U.; Murphy, H.R.; Smith, G.C. Accelerated Fetal Growth Prior to Diagnosis of Gestational Diabetes Mellitus: A Prospective Cohort Study of Nulliparous Women. Diabetes Care 2016, 39, 982–987. [Google Scholar] [CrossRef]
- Dunn, A.B.; Hanson, L.; VandeVusse, L.; Leslie, S. Through the Microbial Looking Glass. J. Périnat. Neonatal Nurs. 2019, 33, 35–51. [Google Scholar] [CrossRef]
- Chawanpaiboon, S.; Vogel, J.P.; Moller, A.-B.; Lumbiganon, P.; Petzold, M.; Hogan, D.; Landoulsi, S.; Jampathong, N.; Kongwattanakul, K.; Laopaiboon, M.; et al. Global, regional, and national estimates of levels of preterm birth in 2014: A systematic review and modelling analysis. Lancet Glob. Health 2018, 7, e37–e46. [Google Scholar] [CrossRef]
- Rozance, P.J.; Hay, W.W. Hypoglycemia in Newborn Infants: Features Associated with Adverse Outcomes. Neonatology 2006, 90, 74–86. [Google Scholar] [CrossRef]
- Sweet, C.B.; Grayson, S.; Polak, M. Management Strategies for Neonatal Hypoglycemia. J. Pediatr. Pharmacol. Ther. 2013, 18, 199–208. [Google Scholar] [CrossRef]
- Pettitt, D.J.; Baird, H.R.; Aleck, K.A.; Bennett, P.H.; Knowler, W.C. Excessive Obesity in Offspring of Pima Indian Women with Diabetes during Pregnancy. N. Engl. J. Med. 1983, 308, 242–245. [Google Scholar] [CrossRef] [PubMed]
- Franks, P.W.; Looker, H.C.; Kobes, S.; Touger, L.; Tataranni, P.A.; Hanson, R.L.; Knowler, W.C. Gestational Glucose Tolerance and Risk of Type 2 Diabetes in Young Pima Indian Offspring. Diabetes 2006, 55, 460–465. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Scholtens, D.M.; Kuang, A.; Lowe, L.P.; Hamilton, J.K.; Lawrence, J.M.; Lebenthal, Y.; Brickman, W.J.; Clayton, R.; Ma, R.C.; McCance, D.; et al. Hyperglycemia and Adverse Pregnancy Outcome Follow-up Study (HAPO FUS): Maternal Glycemia and Childhood Glucose Metabolism. Diabetes Care 2019, 42, 381–392. [Google Scholar] [CrossRef] [PubMed]
- Keely, E.; Malcolm, J.C.; Hadjiyannakis, S.; Gaboury, I.; Lough, G.; Lawson, M.L. Prevalence of metabolic markers of insulin resistance in offspring of gestational diabetes pregnancies. Pediatr. Diabetes 2007, 9, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Boerschmann, H.; Pflüger, M.; Henneberger, L.; Ziegler, A.-G.; Hummel, S. Prevalence and Predictors of Overweight and Insulin Resistance in Offspring of Mothers with Gestational Diabetes Mellitus. Diabetes Care 2010, 33, 1845–1849. [Google Scholar] [CrossRef] [PubMed]
- Blotsky, A.L.; Rahme, E.; Dahhou, M.; Nakhla, M.; Dasgupta, K. Gestational diabetes associated with incident diabetes in childhood and youth: A retrospective cohort study. Can. Med Assoc. J. 2019, 191, E410–E417. [Google Scholar] [CrossRef]
- Clausen, T.D.; Mathiesen, E.R.; Hansen, T.; Pedersen, O.; Jensen, D.M.; Lauenborg, J.; Damm, P. High Prevalence of Type 2 Diabetes and Pre-Diabetes in Adult Offspring of Women With Gestational Diabetes Mellitus or Type 1 Diabetes: The role of intrauterine hyperglycemia. Diabetes Care 2007, 31, 340–346. [Google Scholar] [CrossRef]
- Vohr, B.R.; Boney, C.M. Gestational diabetes: The forerunner for the development of maternal and childhood obesity and metabolic syndrome? J. Matern. Neonatal Med. 2008, 21, 149–157. [Google Scholar] [CrossRef]
- Tam, W.H.; Ma, R.C.; Ozaki, R.; Li, A.M.; Chan, M.H.M.; Yuen, L.Y.; Lao, T.T.H.; Yang, X.; Ho, C.S.; Tutino, G.E.; et al. In Utero Exposure to Maternal Hyperglycemia Increases Childhood Cardiometabolic Risk in Offspring. Diabetes Care 2017, 40, 679–686. [Google Scholar] [CrossRef]
- Pathirana, M.M.; Lassi, Z.S.; Roberts, C.T.; Andraweera, P. Cardiovascular risk factors in offspring exposed to gestational diabetes mellitus in utero: Systematic review and meta-analysis. J. Dev. Orig. Health Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- Leybovitz-Haleluya, N.; Wainstock, T.; Landau, D.; Sheiner, E. Maternal gestational diabetes mellitus and the risk of subsequent pediatric cardiovascular diseases of the offspring: A population-based cohort study with up to 18 years of follow up. Acta Diabetol. 2018, 55, 1037–1042. [Google Scholar] [CrossRef]
- Yu, Y.; Arah, O.A.; Liew, Z.; Cnattingius, S.; Olsen, J.; Sørensen, H.T.; Qin, G.; Li, J. Maternal diabetes during pregnancy and early onset of cardiovascular disease in offspring: Population based cohort study with 40 years of follow-up. BMJ 2019, 367, l6398. [Google Scholar] [CrossRef]
- Monteiro, L.J.; Norman, J.E.; Rice, G.E.; Illanes, S.E. Fetal programming and gestational diabetes mellitus. Placenta 2016, 48, S54–S60. [Google Scholar] [CrossRef]
- Catalano, P.M. The impact of gestational diabetes and maternal obesity on the mother and her offspring. J. Dev. Orig. Health Dis. 2010, 1, 208–215. [Google Scholar] [CrossRef] [PubMed]
- Pasek, R.; Gannon, M. Advancements and challenges in generating accurate animal models of gestational diabetes mellitus. Am. J. Physiol. Metab. 2013, 305, E1327–E1338. [Google Scholar] [CrossRef] [PubMed]
- Jawerbaum, A.; Catafau, J.; Gonzales, E.; Rodríguez, R.; Gelpi, E.; Gomez, G.; Gimeno, A.; Gimeno, M. Eicosanoid production by uterine strips and by embryos obtained from diabetic pregnant rats. Prostaglandins 1993, 45, 487–495. [Google Scholar] [CrossRef]
- Gillman, J.; Gilbert, C.; Epstein, E.; Allan, J.C. Endocrine Control of Blood Sugar, Lipaemia, and Ketonaemia in Diabetic Baboons. BMJ 1958, 2, 1260–1263. [Google Scholar] [CrossRef][Green Version]
- Junod, A.; Lambert, A.E.; Stauffacher, W.; Renold, A.E. Diabetogenic action of streptozotocin: Relationship of dose to metabolic response. J. Clin. Investig. 1969, 48, 2129–2139. [Google Scholar] [CrossRef]
- Lenzen, S.; Panten, U. Alloxan: History and mechanism of action. Diabetology 1988, 31, 337–342. [Google Scholar] [CrossRef]
- Kemnitz, J.; Eisele, S.; Lindsay, K.; Engle, M.; Perelman, R.; Farrell, P. Changes in food intake during menstrual cycles and pregnancy of normal and diabetic rhesus monkeys. Diabetology 1984, 26, 60–64. [Google Scholar] [CrossRef] [PubMed]
- Mintz, D.H.; Chez, R.A.; Hutchinson, D.L. Subhuman Primate Pregnancy Complicated by Streptozotocin-Induced Diabetes Mellitus. J. Clin. Investig. 1972, 51, 837–847. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Genevay, M.; Pontes, H.; Meda, P. Beta cell adaptation in pregnancy: A major difference between humans and rodents? Diabetology 2010, 53, 2089–2092. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Holemans, K.; Caluwaerts, S.; Poston, L.; Van Assche, F. Diet-induced obesity in the rat: A model for gestational diabetes mellitus. Am. J. Obstet. Gynecol. 2004, 190, 858–865. [Google Scholar] [CrossRef] [PubMed]
- Gauguier, D.; Bihoreau, M.T.; Picon, L.; Ktorza, A. Insulin Secretion in Adult Rats After Intrauterine Exposure to Mild Hyperglycemia During Late Gestation. Diabetes 1991, 40, 109–114. [Google Scholar] [CrossRef] [PubMed]
- Yamashita, H.; Shao, J.; Qiao, L.; Pagliassotti, M.; Friedman, J.E. Effect of spontaneous gestational diabetes on fetal and postnatal hepatic insulin resistance in Lepr(db/+) mice. Pediatr. Res. 2003, 53, 411–418. [Google Scholar] [CrossRef]
- Huang, C.; Snider, F.; Cross, J.C. Prolactin Receptor Is Required for Normal Glucose Homeostasis and Modulation of β-Cell Mass during Pregnancy. Endocrinology 2009, 150, 1618–1626. [Google Scholar] [CrossRef] [PubMed]
- Pereira, T.J.; Moyce, B.L.; Kereliuk, S.; Dolinsky, V.W. Influence of maternal overnutrition and gestational diabetes on the programming of metabolic health outcomes in the offspring: Experimental evidence. Biochem. Cell Biol. 2015, 93, 438–451. [Google Scholar] [CrossRef]
- Jawerbaum, A.; White, V. Animal Models in Diabetes and Pregnancy. Endocr. Rev. 2010, 31, 680–701. [Google Scholar] [CrossRef] [PubMed]
- Capobianco, E.; Fornes, D.D.; Linenberg, I.; Powell, T.L.; Jansson, T.; Jawerbaum, A. A novel rat model of gestational diabetes induced by intrauterine programming is associated with alterations in placental signaling and fetal overgrowth. Mol. Cell. Endocrinol. 2016, 422, 221–232. [Google Scholar] [CrossRef]
- Boloker, J.; Gertz, S.J.; Simmons, R.A. Gestational diabetes leads to the development of diabetes in adulthood in the rat. Diabetes 2002, 51, 1499–1506. [Google Scholar] [CrossRef]
- Szlapinski, S.K.; King, R.T.; Retta, G.; Yeo, E.; Strutt, B.J.; Hill, D. A mouse model of gestational glucose intolerance through exposure to a low protein diet during fetal and neonatal development. J. Physiol. 2019, 597, 4237–4250. [Google Scholar] [CrossRef]
- Gauguier, D.; Bihoreau, M.T.; Ktorza, A.; Berthault, M.F.; Picon, L. Inheritance of diabetes mellitus as consequence of gestational hyperglycemia in rats. Diabetes 1990, 39, 734–739. [Google Scholar] [CrossRef] [PubMed]
- McCurdy, C.E.; Bishop, J.M.; Williams, S.M.; Grayson, B.E.; Smith, M.S.; Friedman, J.E.; Grove, K.L. Maternal high-fat diet triggers lipotoxicity in the fetal livers of nonhuman primates. J. Clin. Investig. 2009, 119, 323–335. [Google Scholar] [CrossRef] [PubMed]
- Friedman, J.E. Obesity and Gestational Diabetes Mellitus Pathways for Programming in Mouse, Monkey, and Man—Where Do We Go Next? The 2014 Norbert Freinkel Award Lecture. Diabetes Care 2015, 38, 1402–1411. [Google Scholar] [CrossRef] [PubMed]
| Type of Testing | Advantages | Disadvantages |
|---|---|---|
| One-step approach | Simple to follow Better patient adherence Easy diagnosis Cost-effective for high-risk individuals Increased sensitivity Detection of milder GDM, thus less complications like pre-eclampsia, applicable to women of any gestational age, neonatal hypoglycemia, neonatal death, and NICU admission | Poor reproducibility Women need to be in a fasting state |
| Two-step approach | Fewer false positive results Avoids OGTT in more than 75% of women | Less patient compliance Requires patients to make two visits for testing Missed diagnosis: 75% sensitivity with 84% specificity as compared with the single-step, 100 g OGTT Delay in initiating treatment even for those who tested positive |
| 75-g OGTT | Glucose Threshold for Diagnosing GDM in mmol/L (mg/dL) | ||
|---|---|---|---|
| GLUCOSE MEASURE | ADA ** | IADPSG * | WHO * |
| FASTING | 5.1 (92.0) | 5.1 (≥92.5) | 5.1–6.9 (92.0–125.0) |
| 1 H | 10.0 (180.0) | 10.0 (≥180.0) | ≥10.0 (180.0) |
| 2 H | 8.5 (152.0) | 8.5 (≥153.0) | 8.5–11.0 (153.0–199.0) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alejandro, E.U.; Mamerto, T.P.; Chung, G.; Villavieja, A.; Gaus, N.L.; Morgan, E.; Pineda-Cortel, M.R.B. Gestational Diabetes Mellitus: A Harbinger of the Vicious Cycle of Diabetes. Int. J. Mol. Sci. 2020, 21, 5003. https://doi.org/10.3390/ijms21145003
Alejandro EU, Mamerto TP, Chung G, Villavieja A, Gaus NL, Morgan E, Pineda-Cortel MRB. Gestational Diabetes Mellitus: A Harbinger of the Vicious Cycle of Diabetes. International Journal of Molecular Sciences. 2020; 21(14):5003. https://doi.org/10.3390/ijms21145003
Chicago/Turabian StyleAlejandro, Emilyn U., Therriz P. Mamerto, Grace Chung, Adrian Villavieja, Nawirah Lumna Gaus, Elizabeth Morgan, and Maria Ruth B. Pineda-Cortel. 2020. "Gestational Diabetes Mellitus: A Harbinger of the Vicious Cycle of Diabetes" International Journal of Molecular Sciences 21, no. 14: 5003. https://doi.org/10.3390/ijms21145003
APA StyleAlejandro, E. U., Mamerto, T. P., Chung, G., Villavieja, A., Gaus, N. L., Morgan, E., & Pineda-Cortel, M. R. B. (2020). Gestational Diabetes Mellitus: A Harbinger of the Vicious Cycle of Diabetes. International Journal of Molecular Sciences, 21(14), 5003. https://doi.org/10.3390/ijms21145003





