Molecular Effects of FDA-Approved Multiple Sclerosis Drugs on Glial Cells and Neurons of the Central Nervous System
Abstract
1. Introduction
2. Molecular Effects of FDA-Approved MS Drugs on CNS Cells
2.1. Molecular Effects of FTY720
2.1.1. Microglia
2.1.2. Astrocytes
2.1.3. Neurons
2.1.4. Oligodendrocytes
2.2. Molecular Effects of DMF
2.2.1. Microglia
2.2.2. Astrocytes
2.2.3. Neurons
2.2.4. Oligodendrocytes
2.3. Molecular Effects of GA
2.3.1. Microglia
2.3.2. Astrocytes
2.3.3. Neurons
2.3.4. Oligodendrocytes
2.4. Molecular Effects of IFNs
2.4.1. Microglia
2.4.2. Astrocytes
2.4.3. Neurons
2.4.4. Oligodendrocytes
2.5. Molecular Effects of TF
2.5.1. Microglia
2.5.2. Astrocytes
2.5.3. Neurons
2.5.4. Oligodendrocytes
2.6. Molecular Effects of LQ
2.6.1. Microglia
2.6.2. Astrocytes
2.6.3. Neurons
2.6.4. Oligodendrocytes
2.7. Molecular Effects of NZ
2.7.1. Microglia
2.7.2. Astrocytes
2.7.3. Neurons
2.7.4. Oligodendrocytes
2.8. Molecular Effects of AZ
Microglia, Astrocytes, Neurons and Oligodendrocytes
2.9. Molecular Effects of OCR
Microglia, Astrocytes, Neurons and Oligodendrocytes
3. Discussion
3.1. FDA-Approved MS Drugs Induce the Transition from a Pro-Inflammatory into an Anti-Inflammatory Microglia Phenotype
3.2. FDA-Approved MS Drugs Induce the Transition from a Reactive into a Neuroprotective Astrocytic Phenotype
3.3. Effects of FDA-Approved MS Drugs on the Microglial and Astrocytic Phenotypes May Be Mediated through NFκB Signaling
3.4. Effects of FDA-Approved MS Drugs on Neurons and Oligodendrocytes May Be Caused Indirectly by the Attenuation of the Pro-Inflammatory States of Microglia and Astrocytes
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| 3-NT | 3-nitrotyrosine |
| AD | Alzheimer’s disease |
| ADCC | Antibody-dependent cellular cytotoxicity |
| ADCP | Antibody-dependent cellular phagocytosis |
| AhR | Aryl hydrocarbon receptor |
| AIM2 | Absent in melanoma 2 |
| AKT | Protein kinase B |
| AMD | Age-related macular degeneration |
| AMPA | α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor |
| APP | Amyloid precursor protein |
| ARG1 | Arginase 1 |
| ASC | Apoptosis-associated speck-like protein |
| AZ | Alemtuzumab |
| Aβ | Amyloid-beta |
| BAX | BCL2 associated X |
| BBB | Blood–brain barrier |
| BDNF | Brain derived neurotrophic factor |
| BrdU | Bromodeoxyuridine/5-bromo-2′-deoxyuridin |
| C3 | Complement component 3 |
| cAMP | Cyclic adenosine monophosphate |
| CAP | Compound action potentials |
| CASP | Caspase |
| CAT | Catalase |
| CCL | C-C Motif chemokine ligand |
| CD11c/ITGAX | Integrin alpha-X precursor |
| CD20 | Cluster of differentiation 20 |
| CD45 | Protein tyrosine-protein phosphatase |
| CD52 | Cluster of differentiation 52 |
| CD68 | Cluster of differentiation 68 |
| CD86 | Cluster of differentiation 86 |
| CDC | Complement-dependent cytotoxicity |
| cGAS | Cyclic GMP-AMP synthase |
| c-Fos | FBJ murine osteosarcoma viral oncogene homolog |
| CHI3L3 | Chitinase 3-like 3 |
| CHIL3 | Chitinase-like 3 |
| CHIT1 | Chitotriosidase |
| CLN | Neuronal ceroid lipofuscinosis |
| CNPase | 2′,3′-Cyclic-nucleotide 3′-phosphodiesterase |
| CNS | Central nervous system |
| CNTF | Ciliary neurotrophic factor |
| COX2 | Cyclooxygenase |
| Cr | Creatine |
| CREB | cAMP-response element binding protein |
| CSF | Cerebrospinal fluid |
| CXCL | Chemokine (C-X-C motif) ligand |
| CXCR | C-X-C Motif chemokine receptor |
| CYP1A1 | Cytochrome P450 |
| DARPP-32 | Protein phosphatase 1 regulatory subunit 1B |
| DAT | Dopamine transporter |
| DCX | Doublecortin |
| DHODH | Dihydro-orotate dehydrogenase |
| DMF | Dimethyl fumarate |
| DRG | Dorsal root ganglion |
| EAE | Experimental autoimmune encephalitis |
| EGR1/2 | Early growth response 1/2 |
| EPSC | Excitatory postsynaptic currents |
| ERK1/2 | Extracellular signal-regulated kinase 1 and 2 |
| ESC | Embryonic stem cells |
| FDA | US Food and Drug Administration |
| FGF2 | Fibroblast growth factor 2 |
| FTY720 | Fingolimod |
| FTY720-pPFTY720 | Phosphorylated FTY720 |
| GA | Glatiramer acetate |
| GABA | γ-aminobutyric acid |
| GAP43 | Growth associated protein 43 |
| GDNF | Glial cell line-derived neurotrophic factor |
| GFAP | Glial fibrillary acidic protein |
| GLI1 | GLI family zinc finger 1 |
| GM-CSF | Granulocyte-macrophage colony-stimulating factor |
| GMH | Germinal matrix hemorrhage |
| GPI | Glycosylphosphatidylinositol |
| GS | Glutamine synthetase |
| GSH | Glutathione |
| GSK3β | Glycogen synthase kinase 3 beta |
| H2O2 | Hydrogen peroxide |
| HBEGF | Heparin binding EGF-like growth factor |
| HCAR2 | Hydroxycarboxylic acid receptor 2 |
| HD | Huntington’s disease |
| HDAC | Histone deacetylase |
| HIF-1α | Hypoxia-induced factor 1α |
| HMGB1 | High mobility group box 1 |
| HO-1 | Heme oxygenase 1 |
| HSV-1 | Human herpesvirus 1 |
| IBA-1 | Allograft inflammatory factor 1 |
| ICAM-1 | Intercellular adhesion molecule 1 |
| ICH | Intracerebral hemorrhage |
| IFN | Interferons |
| IFNAR | IFN receptor |
| IFN-α | Interferon-alpha |
| IFN-β | Interferon-beta |
| IFN-γ | Interferon-gamma |
| IGF-1 | Insulin-like growth factor 1 |
| IL | Interleukin |
| iNOS | Inducible nitric oxide synthase |
| IRF | Interferon regulatory factor |
| Iκbα | NFκB inhibitor alpha |
| JAK1 | Janus kinase 1 |
| JNK | c-Jun N-terminal kinase |
| JNK1/2 | c-Jun N-terminal kinase 1 or 2 |
| LBP | LPS-binding protein |
| LCN2 | Lipocalin 2 |
| LFB | Luxol Fast Blue |
| LIF | Leukemia inhibitory factor |
| LPS | Lipopolysaccharide |
| LQ | Laquinimod |
| MAC-1/ITGAM | Integrin alpha-M precursor |
| MAC-2 | Galectin-3 |
| MAC-3/CD107b | Lysosome-associated membrane protein 2 |
| MAG | Myelin-associated glycoprotein |
| MAP2 | Microtubule-associated protein 2 |
| MAPK | p38 mitogen-activated protein kinases |
| MASH1 | Mammalian achaete-schute homolog 1 |
| MBP | Myelin basic protein |
| MHC-I | Major histocompatibility complex class I protein |
| MHC-II | Major histocompatibility complex class II protein |
| MiR-124a | MicroRNA 124a |
| MiR-155 | MicroRNA 155 |
| MMF | Monomethyl Fumarate |
| MMP | Matrix metalloproteinase |
| MnSOD | Manganese-dependent superoxide dismutase |
| MOG | Myelin oligodendrocyte glycoprotein |
| MOG-ON | MOG-induced optic neuritis |
| MPP | 1-methyl-4-phenylpyridinium |
| MPTP | 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine |
| MRC1/CD206 | Mannose receptor C-type 1 |
| MRI | Magnetic resonance imaging |
| MRS | 1H-magnetic resonance spectroscopy |
| MRTF | MKL/megakaryoblastic leukemia 1 |
| MyD88 | Myeloid differentiation primary response 88 |
| NAA | N-acetyl aspartate |
| NAWM | Normal appearing white matter |
| ND4 | NADH dehydrogenase, subunit 4 |
| NDMA | N-methyl-D-aspartate receptor |
| NeuN | Neuronal nuclei |
| NF | Neurofilament |
| NFκB | Nuclear Factor binding near the kappa-light-chain gene in B cell |
| NFκB p65 | Rel-A |
| NG2 | Neural/glial antigen 2 |
| NGF | Nerve growth factor beta |
| NLRP3 | NLR family pyrin domain containing 3 |
| NO | Nitric oxide |
| NOTCH-1 | Neurogenic locus notch homolog protein 1 |
| NQO-1 | NAD(P)H dehydrogenase quinone |
| NRF2 | Nuclear factor erythroid 2-related factor 2 |
| NSC | Neural stem cells |
| NT3 | Neurotrophin-3 |
| NZ | Natalizumab |
| OCLN | Occludin |
| OCR | Ocrelizumab |
| OGD | Oxygen–glucose deprivation |
| OLIG2 | Oligodendrocyte transcription factor |
| OPC | Oligodendrocyte precursor cell |
| p | Phosphorylated |
| P204 | Interferon-activable protein 204 |
| P25 | Tubulin polymerization-promoting protein |
| PAP | Placental alkaline phosphatase |
| PBX1 | PBX homeobox 1 |
| pCr | phosphoCr |
| PD | Parkinson’s disease |
| PDGF-A | Platelet derived growth factor subunit A |
| PI3K | Phosphoinositide 3-kinase |
| PLP1 | Proteolipid protein |
| PPMS | Primary-progressive MS |
| PS1 | Presenilin-1 |
| PSD95 | Postsynaptic density protein 95 |
| PTZ | Pentylenetetrazol |
| PYHIN | Pyrin and HIN200 domain-containing proteins |
| RETNLA | Resistin-like alpha |
| RGC | Retinal ganglion cell |
| rIFN | Recombinant interferon |
| RIP3 | Receptor-interacting protein kinase 3 |
| ROS | Reactive oxygen species |
| RRMS | Relapsing-remitting MS |
| S100β | S100 calcium-binding protein B |
| S1P | Sphingosine 1-phosphate |
| S1PR1 | S1P receptor 1 |
| SCI | Spinal cord injury |
| SE | Status epilepticus |
| SHH | Sonic hedgehog |
| SIGLEC-1 | Sialoadhesin |
| SLC1A | Solute carrier family 1 member |
| SMI32 | Neurofilament-heavy chain |
| SMO | Smoothened |
| SOCS2 | Suppressor of cytokine signaling 2 |
| SOD | Superoxide dismutase |
| SPN2S | Spinster homolog 2 |
| SREBP2 | Sterol regulatory element-binding protein 2 |
| SRF | Serum response factor |
| STAT | Signal transducer and activator of transcription |
| sTREM-2 | Triggering receptor expressed on myeloid cells 2 |
| SYP | Synaptophysin |
| TAU | Tau protein |
| TBI | Traumatic brain injury |
| TF | Teriflunomide |
| TGF-α | Transforming growth factor alpha |
| TGF-β2 | Transforming growth factor-beta 2 |
| TH | Tyrosine hydroxylase |
| TLR | Toll-like receptor |
| tMCAO | Transient middle cerebral artery occlusion |
| TMEM119 | Transmembrane protein 119 |
| TMEV | Theiler’s murine encephalomyelitis virus |
| TNF-α | Tumor necrosis factor alpha |
| TRIF | Toll like receptor adaptor molecule 1 |
| TSPO | Translocator protein |
| TYK1 | Leukocyte receptor tyrosine kinase |
| VCAM-1 | Vascular cell adhesion protein 1 |
| VEGF-B | Vascular endothelial growth factor B |
| VEGF-A | Vascular endothelial growth factor A |
| VGLUT1 | Vesicular glutamate transporter 1 |
| VIM | Vimentin |
| VLA-4/CD49d/CD29 | Very late antigen-4 |
| ZO-1 | Zonula occludens protein-1 |
| αSYN | α-synuclein |
| βIII-Tubulin | Beta-3-tubulin |
References
- Lassmann, H. Multiple Sclerosis Pathology. Cold Spring Harb Perspect Med. 2018, 8. [Google Scholar] [CrossRef] [PubMed]
- Kutzelnigg, A.; Lucchinetti, C.F.; Stadelmann, C.; Bruck, W.; Rauschka, H.; Bergmann, M.; Schmidbauer, M.; Parisi, J.E.; Lassmann, H. Cortical demyelination and diffuse white matter injury in multiple sclerosis. Brain 2005, 128, 2705–2712. [Google Scholar] [CrossRef] [PubMed]
- Zrzavy, T.; Hametner, S.; Wimmer, I.; Butovsky, O.; Weiner, H.L.; Lassmann, H. Loss of ‘homeostatic’ microglia and patterns of their activation in active multiple sclerosis. Brain 2017, 140, 1900–1913. [Google Scholar] [CrossRef] [PubMed]
- Lassmann, H. Pathogenic Mechanisms Associated With Different Clinical Courses of Multiple Sclerosis. Front Immunol. 2018, 9, 3116. [Google Scholar] [CrossRef]
- Baecher-Allan, C.; Kaskow, B.J.; Weiner, H.L. Multiple Sclerosis: Mechanisms and Immunotherapy. Neuron 2018, 97, 742–768. [Google Scholar] [CrossRef] [PubMed]
- Bachiller, S.; Jimenez-Ferrer, I.; Paulus, A.; Yang, Y.; Swanberg, M.; Deierborg, T.; Boza-Serrano, A. Microglia in Neurological Diseases: A Road Map to Brain-Disease Dependent-Inflammatory Response. Front. Cell Neurosci. 2018, 12, 488. [Google Scholar] [CrossRef] [PubMed]
- Angelova, D.M.; Brown, D.R. Microglia and the aging brain: Are senescent microglia the key to neurodegeneration? J. Neurochem. 2019, 151, 676–688. [Google Scholar] [CrossRef]
- Stys, P.K.; Zamponi, G.W.; van Minnen, J.; Geurts, J.J. Will the real multiple sclerosis please stand up? Nat. Rev. Neurosci. 2012, 13, 507–514. [Google Scholar] [CrossRef]
- Traka, M.; Podojil, J.R.; McCarthy, D.P.; Miller, S.D.; Popko, B. Oligodendrocyte death results in immune-mediated CNS demyelination. Nat. Neurosci. 2016, 19, 65–74. [Google Scholar] [CrossRef]
- Barnett, M.H.; Prineas, J.W. Relapsing and remitting multiple sclerosis: Pathology of the newly forming lesion. Ann. Neurol. 2004, 55, 458–468. [Google Scholar] [CrossRef]
- Gholamzad, M.; Ebtekar, M.; Ardestani, M.S.; Azimi, M.; Mahmodi, Z.; Mousavi, M.J.; Aslani, S. A comprehensive review on the treatment approaches of multiple sclerosis: Currently and in the future. Inflamm. Res. 2019, 68, 25–38. [Google Scholar] [CrossRef] [PubMed]
- Loleit, V.; Biberacher, V.; Hemmer, B. Current and future therapies targeting the immune system in multiple sclerosis. Curr. Pharm. Biotechnol. 2014, 15, 276–296. [Google Scholar] [CrossRef] [PubMed]
- International Multiple Sclerosis Genetics, C. Multiple sclerosis genomic map implicates peripheral immune cells and microglia in susceptibility. Science 2019, 365. [Google Scholar] [CrossRef] [PubMed]
- Graetz, C.; Groppa, S.; Zipp, F.; Siller, N. Preservation of neuronal function as measured by clinical and MRI endpoints in relapsing-remitting multiple sclerosis: How effective are current treatment strategies? Expert Rev. Neurother. 2018, 18, 203–219. [Google Scholar] [CrossRef]
- Kuhle, J.; Kropshofer, H.; Haering, D.A.; Kundu, U.; Meinert, R.; Barro, C.; Dahlke, F.; Tomic, D.; Leppert, D.; Kappos, L. Blood neurofilament light chain as a biomarker of MS disease activity and treatment response. Neurology 2019, 92, e1007–e1015. [Google Scholar] [CrossRef] [PubMed]
- Wattjes, M.P.; Rovira, A.; Miller, D.; Yousry, T.A.; Sormani, M.P.; de Stefano, M.P.; Tintore, M.; Auger, C.; Tur, C.; Filippi, M.; et al. Evidence-based guidelines: MAGNIMS consensus guidelines on the use of MRI in multiple sclerosis--establishing disease prognosis and monitoring patients. Nat. Rev. Neurol. 2015, 11, 597–606. [Google Scholar] [CrossRef]
- Kihara, Y. Systematic Understanding of Bioactive Lipids in Neuro-Immune Interactions: Lessons from an Animal Model of Multiple Sclerosis. Adv. Exp. Med. Biol. 2019, 1161, 133–148. [Google Scholar] [CrossRef]
- Candido, K.; Soufi, H.; Bandyopadhyay, M.; Dasgupta, S. Therapeutic Impact of Sphingosine 1-phosphate Receptor Signaling in Multiple Sclerosis. Mini. Rev. Med. Chem. 2016, 16, 547–554. [Google Scholar] [CrossRef]
- Groves, A.; Kihara, Y.; Chun, J. Fingolimod: Direct CNS effects of sphingosine 1-phosphate (S1P) receptor modulation and implications in multiple sclerosis therapy. J. Neurol. Sci. 2013, 328, 9–18. [Google Scholar] [CrossRef]
- Miller, L.G., Jr.; Young, J.A.; Ray, S.K.; Wang, G.; Purohit, S.; Banik, N.L.; Dasgupta, S. Sphingosine Toxicity in EAE and MS: Evidence for Ceramide Generation via Serine-Palmitoyltransferase Activation. Neurochem Res. 2017, 42, 2755–2768. [Google Scholar] [CrossRef]
- Bruck, J.; Dringen, R.; Amasuno, A.; Pau-Charles, I.; Ghoreschi, K. A review of the mechanisms of action of dimethylfumarate in the treatment of psoriasis. Exp. Dermatol. 2018, 27, 611–624. [Google Scholar] [CrossRef] [PubMed]
- Yazdi, A.; Ghasemi-Kasman, M.; Javan, M. Possible regenerative effects of fingolimod (FTY720) in multiple sclerosis disease: An overview on remyelination process. J. Neurosci. Res. 2020, 98, 524–536. [Google Scholar] [CrossRef] [PubMed]
- Hunter, S.F.; Bowen, J.D.; Reder, A.T. The Direct Effects of Fingolimod in the Central Nervous System: Implications for Relapsing Multiple Sclerosis. CNS Drugs 2016, 30, 135–147. [Google Scholar] [CrossRef] [PubMed]
- Liddell, J.R. Are Astrocytes the Predominant Cell Type for Activation of Nrf2 in Aging and Neurodegeneration? Antioxidants (Basel) 2017, 6, 65. [Google Scholar] [CrossRef] [PubMed]
- Chen-Roetling, J.; Regan, R.F. Targeting the Nrf2-Heme Oxygenase-1 Axis after Intracerebral Hemorrhage. Curr Pharm. Des. 2017, 23, 2226–2237. [Google Scholar] [CrossRef]
- Liblau, R. Glatiramer acetate for the treatment of multiple sclerosis: Evidence for a dual anti-inflammatory and neuroprotective role. J. Neurol. Sci. 2009, 287, S17–S23. [Google Scholar] [CrossRef]
- Arnon, R.; Aharoni, R. Neurogenesis and neuroprotection in the CNS--fundamental elements in the effect of Glatiramer acetate on treatment of autoimmune neurological disorders. Mol. Neurobiol. 2007, 36, 245–253. [Google Scholar] [CrossRef]
- Dhib-Jalbut, S. Mechanisms of action of interferons and glatiramer acetate in multiple sclerosis. Neurology 2002, 58, S3–S9. [Google Scholar] [CrossRef]
- Sellebjerg, F.; Cadavid, D.; Steiner, D.; Villar, L.M.; Reynolds, R.; Mikol, D. Exploring potential mechanisms of action of natalizumab in secondary progressive multiple sclerosis. Ther. Adv. Neurol. Disord. 2016, 9, 31–43. [Google Scholar] [CrossRef]
- Kieseier, B.C. Defining a role for laquinimod in multiple sclerosis. Ther. Adv. Neurol. Disord. 2014, 7, 195–205. [Google Scholar] [CrossRef]
- Bruck, W.; Wegner, C. Insight into the mechanism of laquinimod action. J. Neurol. Sci. 2011, 306, 173–179. [Google Scholar] [CrossRef] [PubMed]
- Orihuela, R.; McPherson, C.A.; Harry, G.J. Microglial M1/M2 polarization and metabolic states. Br. J. Pharmacol. 2016, 173, 649–665. [Google Scholar] [CrossRef] [PubMed]
- Tang, Y.; Le, W. Differential Roles of M1 and M2 Microglia in Neurodegenerative Diseases. Mol. Neurobiol. 2016, 53, 1181–1194. [Google Scholar] [CrossRef] [PubMed]
- Miller, S.J. Astrocyte Heterogeneity in the Adult Central Nervous System. Front Cell Neurosci. 2018, 12, 401. [Google Scholar] [CrossRef] [PubMed]
- Tsai, H.C.; Han, M.H. Sphingosine-1-Phosphate (S1P) and S1P Signaling Pathway: Therapeutic Targets in Autoimmunity and Inflammation. Drugs 2016, 76, 1067–1079. [Google Scholar] [CrossRef]
- Prager, B.; Spampinato, S.F.; Ransohoff, R.M. Sphingosine 1-phosphate signaling at the blood-brain barrier. Trends Mol. Med. 2015, 21, 354–363. [Google Scholar] [CrossRef]
- Wang, Z.; Kawabori, M.; Houkin, K. FTY720 (Fingolimod) Ameliorates Brain Injury Through Multiple Mechanisms and is a Strong Candidate for Stroke Treatment. Curr. Med. Chem. 2019. [Google Scholar] [CrossRef]
- Farez, M.F.; Correale, J. Sphingosine 1-phosphate signaling in astrocytes: Implications for progressive multiple sclerosis. J. Neurol. Sci. 2016, 361, 60–65. [Google Scholar] [CrossRef]
- Hiestand, P.C.; Rausch, M.; Meier, D.P.; Foster, C.A. Ascomycete derivative to MS therapeutic: S1P receptor modulator FTY720. Prog. Drug Res. 2008, 66, 361, 363–381. [Google Scholar] [CrossRef]
- Park, S.J.; Im, D.S. Sphingosine 1-Phosphate Receptor Modulators and Drug Discovery. Biomol. Ther. (Seoul) 2017, 25, 80–90. [Google Scholar] [CrossRef]
- Foster, C.A.; Howard, L.M.; Schweitzer, A.; Persohn, E.; Hiestand, P.C.; Balatoni, B.; Reuschel, R.; Beerli, C.; Schwartz, M.; Billich, A. Brain penetration of the oral immunomodulatory drug FTY720 and its phosphorylation in the central nervous system during experimental autoimmune encephalomyelitis: Consequences for mode of action in multiple sclerosis. J. Pharmacol. Exp. Ther. 2007, 323, 469–475. [Google Scholar] [CrossRef] [PubMed]
- Shang, K.; He, J.; Zou, J.; Qin, C.; Lin, L.; Zhou, L.Q.; Yang, L.L.; Wu, L.J.; Wang, W.; Zhan, K.B.; et al. Fingolimod promotes angiogenesis and attenuates ischemic brain damage via modulating microglial polarization. Brain Res. 2020, 1726, 146509. [Google Scholar] [CrossRef] [PubMed]
- Qin, C.; Fan, W.H.; Liu, Q.; Shang, K.; Murugan, M.; Wu, L.J.; Wang, W.; Tian, D.S. Fingolimod Protects Against Ischemic White Matter Damage by Modulating Microglia Toward M2 Polarization via STAT3 Pathway. Stroke 2017, 48, 3336–3346. [Google Scholar] [CrossRef] [PubMed]
- Zhong, L.; Jiang, X.; Zhu, Z.; Qin, H.; Dinkins, M.B.; Kong, J.N.; Leanhart, S.; Wang, R.; Elsherbini, A.; Bieberich, E.; et al. Lipid transporter Spns2 promotes microglia pro-inflammatory activation in response to amyloid-beta peptide. Glia 2019, 67, 498–511. [Google Scholar] [CrossRef] [PubMed]
- Carreras, I.; Aytan, N.; Choi, J.K.; Tognoni, C.M.; Kowall, N.W.; Jenkins, B.G.; Dedeoglu, A. Dual dose-dependent effects of fingolimod in a mouse model of Alzheimer’s disease. Sci. Rep. 2019, 9, 10972. [Google Scholar] [CrossRef] [PubMed]
- Metzdorf, J.; Hobloss, Z.; Schlevogt, S.; Ayzenberg, I.; Stahlke, S.; Pedreiturria, X.; Haupeltshofer, S.; Gold, R.; Tonges, L.; Kleiter, I. Fingolimod for Irradiation-Induced Neurodegeneration. Front Neurosci. 2019, 13, 699. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Dong, S.; Zheng, Q.; Zhang, L.; Tan, X.; Zou, J.; Yan, B.; Chen, Y. FTY720 attenuates iron deposition and glial responses in improving delayed lesion and long-term outcomes of collagenase-induced intracerebral hemorrhage. Brain Res. 2019, 1718, 91–102. [Google Scholar] [CrossRef]
- Kim, S.; Bielawski, J.; Yang, H.; Kong, Y.; Zhou, B.; Li, J. Functional antagonism of sphingosine-1-phosphate receptor 1 prevents cuprizone-induced demyelination. Glia 2018, 66, 654–669. [Google Scholar] [CrossRef]
- Groh, J.; Berve, K.; Martini, R. Fingolimod and Teriflunomide Attenuate Neurodegeneration in Mouse Models of Neuronal Ceroid Lipofuscinosis. Mol. Ther. 2017, 25, 1889–1899. [Google Scholar] [CrossRef]
- Lee, D.H.; Seubert, S.; Huhn, K.; Brecht, L.; Rotger, C.; Waschbisch, A.; Schlachetzki, J.; Klausmeyer, A.; Melms, A.; Wiese, S.; et al. Fingolimod effects in neuroinflammation: Regulation of astroglial glutamate transporters? PLoS ONE 2017, 12, e0171552. [Google Scholar] [CrossRef]
- Aytan, N.; Choi, J.K.; Carreras, I.; Brinkmann, V.; Kowall, N.W.; Jenkins, B.G.; Dedeoglu, A. Fingolimod modulates multiple neuroinflammatory markers in a mouse model of Alzheimer’s disease. Sci. Rep. 2016, 6, 24939. [Google Scholar] [CrossRef] [PubMed]
- Serdar, M.; Herz, J.; Kempe, K.; Lumpe, K.; Reinboth, B.S.; Sizonenko, S.V.; Hou, X.; Herrmann, R.; Hadamitzky, M.; Heumann, R.; et al. Fingolimod protects against neonatal white matter damage and long-term cognitive deficits caused by hyperoxia. Brain Behav. Immun. 2016, 52, 106–119. [Google Scholar] [CrossRef] [PubMed]
- Wei, Y.; Yemisci, M.; Kim, H.H.; Yung, L.M.; Shin, H.K.; Hwang, S.K.; Guo, S.; Qin, T.; Alsharif, N.; Brinkmann, V.; et al. Fingolimod provides long-term protection in rodent models of cerebral ischemia. Ann. Neurol. 2011, 69, 119–129. [Google Scholar] [CrossRef] [PubMed]
- Gao, F.; Liu, Y.; Li, X.; Wang, Y.; Wei, D.; Jiang, W. Fingolimod (FTY720) inhibits neuroinflammation and attenuates spontaneous convulsions in lithium-pilocarpine induced status epilepticus in rat model. Pharmacol. Biochem. Behav. 2012, 103, 187–196. [Google Scholar] [CrossRef]
- Ji, J.; Wang, J.; Yang, J.; Wang, X.P.; Huang, J.J.; Xue, T.F.; Sun, X.L. The Intra-nuclear SphK2-S1P Axis Facilitates M1-to-M2 Shift of Microglia via Suppressing HDAC1-Mediated KLF4 Deacetylation. Front Immunol. 2019, 10, 1241. [Google Scholar] [CrossRef]
- Gol, M.; Ghorbanian, D.; Hassanzadeh, S.; Javan, M.; Mirnajafi-Zadeh, J.; Ghasemi-Kasman, M. Fingolimod enhances myelin repair of hippocampus in pentylenetetrazol-induced kindling model. Eur. J. Pharm. Sci. 2017, 96, 72–83. [Google Scholar] [CrossRef]
- Rau, C.R.; Hein, K.; Sattler, M.B.; Kretzschmar, B.; Hillgruber, C.; McRae, B.L.; Diem, R.; Bahr, M. Anti-inflammatory effects of FTY720 do not prevent neuronal cell loss in a rat model of optic neuritis. Am. J. Pathol. 2011, 178, 1770–1781. [Google Scholar] [CrossRef]
- Yao, S.; Li, L.; Sun, X.; Hua, J.; Zhang, K.; Hao, L.; Liu, L.; Shi, D.; Zhou, H. FTY720 Inhibits MPP(+)-Induced Microglial Activation by Affecting NLRP3 Inflammasome Activation. J. Neuroimmune. Pharmacol. 2019, 14, 478–492. [Google Scholar] [CrossRef]
- Cipriani, R.; Chara, J.C.; Rodriguez-Antiguedad, A.; Matute, C. FTY720 attenuates excitotoxicity and neuroinflammation. J. Neuroinflammation 2015, 12, 86. [Google Scholar] [CrossRef]
- Balatoni, B.; Storch, M.K.; Swoboda, E.M.; Schonborn, V.; Koziel, A.; Lambrou, G.N.; Hiestand, P.C.; Weissert, R.; Foster, C.A. FTY720 sustains and restores neuronal function in the DA rat model of MOG-induced experimental autoimmune encephalomyelitis. Brain Res. Bull 2007, 74, 307–316. [Google Scholar] [CrossRef]
- Smith, P.A.; Schmid, C.; Zurbruegg, S.; Jivkov, M.; Doelemeyer, A.; Theil, D.; Dubost, V.; Beckmann, N. Fingolimod inhibits brain atrophy and promotes brain-derived neurotrophic factor in an animal model of multiple sclerosis. J. Neuroimmunol 2018, 318, 103–113. [Google Scholar] [CrossRef] [PubMed]
- Vidal-Martinez, G.; Segura-Ulate, I.; Yang, B.; Diaz-Pacheco, V.; Barragan, J.A.; De-Leon Esquivel, J.; Chaparro, S.A.; Vargas-Medrano, J.; Perez, R.G. FTY720-Mitoxy reduces synucleinopathy and neuroinflammation, restores behavior and mitochondria function, and increases GDNF expression in Multiple System Atrophy mouse models. Exp. Neurol. 2020, 325, 113120. [Google Scholar] [CrossRef] [PubMed]
- Marfia, G.; Navone, S.E.; Hadi, L.A.; Paroni, M.; Berno, V.; Beretta, M.; Gualtierotti, R.; Ingegnoli, F.; Levi, V.; Miozzo, M.; et al. The Adipose Mesenchymal Stem Cell Secretome Inhibits Inflammatory Responses of Microglia: Evidence for an Involvement of Sphingosine-1-Phosphate Signalling. Stem Cells Dev. 2016, 25, 1095–1107. [Google Scholar] [CrossRef] [PubMed]
- Bechet, S.; O’Sullivan, S.A.; Yssel, J.; Fagan, S.G.; Dev, K.K. Fingolimod Rescues Demyelination in a Mouse Model of Krabbe’s Disease. J. Neurosci. 2020, 40, 3104–3118. [Google Scholar] [CrossRef]
- Rothhammer, V.; Kenison, J.E.; Tjon, E.; Takenaka, M.C.; de Lima, K.A.; Borucki, D.M.; Chao, C.C.; Wilz, A.; Blain, M.; Healy, L.; et al. Sphingosine 1-phosphate receptor modulation suppresses pathogenic astrocyte activation and chronic progressive CNS inflammation. Proc. Natl. Acad. Sci. USA 2017, 114, 2012–2017. [Google Scholar] [CrossRef]
- Miron, V.E.; Ludwin, S.K.; Darlington, P.J.; Jarjour, A.A.; Soliven, B.; Kennedy, T.E.; Antel, J.P. Fingolimod (FTY720) enhances remyelination following demyelination of organotypic cerebellar slices. Am. J. Pathol. 2010, 176, 2682–2694. [Google Scholar] [CrossRef]
- Alme, M.N.; Nystad, A.E.; Bo, L.; Myhr, K.M.; Vedeler, C.A.; Wergeland, S.; Torkildsen, O. Fingolimod does not enhance cerebellar remyelination in the cuprizone model. J. Neuroimmunol. 2015, 285, 180–186. [Google Scholar] [CrossRef]
- Slowik, A.; Schmidt, T.; Beyer, C.; Amor, S.; Clarner, T.; Kipp, M. The sphingosine 1-phosphate receptor agonist FTY720 is neuroprotective after cuprizone-induced CNS demyelination. Br. J. Pharmacol. 2015, 172, 80–92. [Google Scholar] [CrossRef]
- Nystad, A.E.; Lereim, R.R.; Wergeland, S.; Oveland, E.; Myhr, K.M.; Bo, L.; Torkildsen, O. Fingolimod downregulates brain sphingosine-1-phosphate receptor 1 levels but does not promote remyelination or neuroprotection in the cuprizone model. J. Neuroimmunol. 2020, 339, 577091. [Google Scholar] [CrossRef]
- Anastasiadou, S.; Knoll, B. The multiple sclerosis drug fingolimod (FTY720) stimulates neuronal gene expression, axonal growth and regeneration. Exp. Neurol. 2016, 279, 243–260. [Google Scholar] [CrossRef]
- Anthony, D.C.; Dickens, A.M.; Seneca, N.; Couch, Y.; Campbell, S.; Checa, B.; Kersemans, V.; Warren, E.A.; Tredwell, M.; Sibson, N.R.; et al. Anti-CD20 inhibits T cell-mediated pathology and microgliosis in the rat brain. Ann. Clin. Transl. Neurol. 2014, 1, 659–669. [Google Scholar] [CrossRef] [PubMed]
- Noda, H.; Takeuchi, H.; Mizuno, T.; Suzumura, A. Fingolimod phosphate promotes the neuroprotective effects of microglia. J. Neuroimmunol. 2013, 256, 13–18. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, S.A.; O’Sullivan, C.; Healy, L.M.; Dev, K.K.; Sheridan, G.K. Sphingosine 1-phosphate receptors regulate TLR4-induced CXCL5 release from astrocytes and microglia. J. Neurochem. 2018, 144, 736–747. [Google Scholar] [CrossRef] [PubMed]
- Das, A.; Arifuzzaman, S.; Kim, S.H.; Lee, Y.S.; Jung, K.H.; Chai, Y.G. FTY720 (fingolimod) regulates key target genes essential for inflammation in microglial cells as defined by high-resolution mRNA sequencing. Neuropharmacology 2017, 119, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Fauser, U.; Schluesener, H.J. Early attenuation of lesional interleukin-16 up-regulation by dexamethasone and FTY720 in experimental traumatic brain injury. Neuropathol. Appl. Neurobiol. 2008, 34, 330–339. [Google Scholar] [CrossRef] [PubMed]
- Newton, K.; Dixit, V.M. Signaling in innate immunity and inflammation. Cold Spring Harb Perspect Biol. 2012, 4. [Google Scholar] [CrossRef]
- Scheiblich, H.; Schlutter, A.; Golenbock, D.T.; Latz, E.; Martinez-Martinez, P.; Heneka, M.T. Activation of the NLRP3 inflammasome in microglia: The role of ceramide. J. Neurochem. 2017, 143, 534–550. [Google Scholar] [CrossRef]
- Grivennikov, S.I.; Karin, M. Dangerous liaisons: STAT3 and NF-kappaB collaboration and crosstalk in cancer. Cytokine Growth Factor Rev. 2010, 21, 11–19. [Google Scholar] [CrossRef]
- Fan, Y.; Mao, R.; Yang, J. NF-kappaB and STAT3 signaling pathways collaboratively link inflammation to cancer. Protein Cell 2013, 4, 176–185. [Google Scholar] [CrossRef]
- Yoshino, T.; Tabunoki, H.; Sugiyama, S.; Ishii, K.; Kim, S.U.; Satoh, J. Non-phosphorylated FTY720 induces apoptosis of human microglia by activating SREBP2. Cell Mol. Neurobiol. 2011, 31, 1009–1020. [Google Scholar] [CrossRef]
- Ruiz, A.; Joshi, P.; Mastrangelo, R.; Francolini, M.; Verderio, C.; Matteoli, M. Testing Abeta toxicity on primary CNS cultures using drug-screening microfluidic chips. Lab. Chip 2014, 14, 2860–2866. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.W.; Gardell, S.E.; Herr, D.R.; Rivera, R.; Lee, C.W.; Noguchi, K.; Teo, S.T.; Yung, Y.C.; Lu, M.; Kennedy, G.; et al. FTY720 (fingolimod) efficacy in an animal model of multiple sclerosis requires astrocyte sphingosine 1-phosphate receptor 1 (S1P1) modulation. Proc. Natl. Acad. Sci. USA 2011, 108, 751–756. [Google Scholar] [CrossRef] [PubMed]
- Mullershausen, F.; Craveiro, L.M.; Shin, Y.; Cortes-Cros, M.; Bassilana, F.; Osinde, M.; Wishart, W.L.; Guerini, D.; Thallmair, M.; Schwab, M.E.; et al. Phosphorylated FTY720 promotes astrocyte migration through sphingosine-1-phosphate receptors. J. Neurochem. 2007, 102, 1151–1161. [Google Scholar] [CrossRef] [PubMed]
- Miguez, A.; Garcia-Diaz Barriga, G.; Brito, V.; Straccia, M.; Giralt, A.; Gines, S.; Canals, J.M.; Alberch, J. Fingolimod (FTY720) enhances hippocampal synaptic plasticity and memory in Huntington’s disease by preventing p75NTR up-regulation and astrocyte-mediated inflammation. Hum. Mol. Genet. 2015, 24, 4958–4970. [Google Scholar] [CrossRef]
- McManus, R.M.; Finucane, O.M.; Wilk, M.M.; Mills, K.H.G.; Lynch, M.A. FTY720 Attenuates Infection-Induced Enhancement of Abeta Accumulation in APP/PS1 Mice by Modulating Astrocytic Activation. J. Neuroimmune. Pharmacol. 2017, 12, 670–681. [Google Scholar] [CrossRef]
- Brunkhorst, R.; Kanaan, N.; Koch, A.; Ferreiros, N.; Mirceska, A.; Zeiner, P.; Mittelbronn, M.; Derouiche, A.; Steinmetz, H.; Foerch, C.; et al. FTY720 treatment in the convalescence period improves functional recovery and reduces reactive astrogliosis in photothrombotic stroke. PLoS ONE 2013, 8, e70124. [Google Scholar] [CrossRef]
- Yavuz, A.; Sezik, M.; Ozmen, O.; Asci, H. Fingolimod against endotoxin-induced fetal brain injury in a rat model. J. Obstet. Gynaecol. Res. 2017, 43, 1708–1713. [Google Scholar] [CrossRef]
- Yazdi, A.; Mokhtarzadeh Khanghahi, A.; Baharvand, H.; Javan, M. Fingolimod Enhances Oligodendrocyte Differentiation of Transplanted Human Induced Pluripotent Stem Cell-Derived Neural Progenitors. Iran J. Pharm. Res. 2018, 17, 1444–1457. [Google Scholar]
- Spampinato, S.F.; Obermeier, B.; Cotleur, A.; Love, A.; Takeshita, Y.; Sano, Y.; Kanda, T.; Ransohoff, R.M. Sphingosine 1 Phosphate at the Blood Brain Barrier: Can the Modulation of S1P Receptor 1 Influence the Response of Endothelial Cells and Astrocytes to Inflammatory Stimuli? PLoS ONE 2015, 10, e0133392. [Google Scholar] [CrossRef]
- Lee, B.J.; Kim, J.Y.; Cho, H.J.; Park, D. Sphingosine 1-phosphate receptor modulation attenuate mechanical allodynia in mouse model of chronic complex regional pain syndrome by suppressing pathogenic astrocyte activation. Reg. Anesth Pain Med. 2020. [Google Scholar] [CrossRef]
- Weinstock, L.D.; Furness, A.M.; Herron, S.S.; Smith, S.S.; Sankar, S.B.; DeRosa, S.G.; Gao, D.; Mepyans, M.E.; Scotto Rosato, A.; Medina, D.L.; et al. Fingolimod phosphate inhibits astrocyte inflammatory activity in mucolipidosis IV. Hum. Mol. Genet 2018, 27, 2725–2738. [Google Scholar] [CrossRef] [PubMed]
- Colombo, E.; Di Dario, M.; Capitolo, E.; Chaabane, L.; Newcombe, J.; Martino, G.; Farina, C. Fingolimod may support neuroprotection via blockade of astrocyte nitric oxide. Ann. Neurol. 2014, 76, 325–337. [Google Scholar] [CrossRef] [PubMed]
- Dong, Y.F.; Guo, R.B.; Ji, J.; Cao, L.L.; Zhang, L.; Chen, Z.Z.; Huang, J.Y.; Wu, J.; Lu, J.; Sun, X.L. S1PR3 is essential for phosphorylated fingolimod to protect astrocytes against oxygen-glucose deprivation-induced neuroinflammation via inhibiting TLR2/4-NFkappaB signalling. J. Cell Mol. Med. 2018, 22, 3159–3166. [Google Scholar] [CrossRef] [PubMed]
- Pang, X.; Hou, X. Synergistic protective effect of FTY720 and vitamin E against simulated cerebral ischemia in vitro. Mol. Med. Rep. 2017, 16, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, F.S.; Hofereiter, J.; Rubsamen, H.; Melms, J.; Schwarz, S.; Faber, H.; Weber, P.; Putz, B.; Loleit, V.; Weber, F.; et al. Fingolimod induces neuroprotective factors in human astrocytes. J. Neuroinflammation 2015, 12, 184. [Google Scholar] [CrossRef] [PubMed]
- Janssen, S.; Schlegel, C.; Gudi, V.; Prajeeth, C.K.; Skripuletz, T.; Trebst, C.; Stangel, M. Effect of FTY720-phosphate on the expression of inflammation-associated molecules in astrocytes in vitro. Mol. Med. Rep. 2015, 12, 6171–6177. [Google Scholar] [CrossRef]
- Groves, A.; Kihara, Y.; Jonnalagadda, D.; Rivera, R.; Kennedy, G.; Mayford, M.; Chun, J. A Functionally Defined In Vivo Astrocyte Population Identified by c-Fos Activation in a Mouse Model of Multiple Sclerosis Modulated by S1P Signaling: Immediate-Early Astrocytes (ieAstrocytes). eNeuro 2018, 5. [Google Scholar] [CrossRef]
- Trkov Bobnar, S.; Stenovec, M.; Mis, K.; Pirkmajer, S.; Zorec, R. Fingolimod Suppresses the Proinflammatory Status of Interferon-gamma-Activated Cultured Rat Astrocytes. Mol. Neurobiol. 2019, 56, 5971–5986. [Google Scholar] [CrossRef]
- Doyle, T.M.; Chen, Z.; Durante, M.; Salvemini, D. Activation of Sphingosine-1-Phosphate Receptor 1 in the Spinal Cord Produces Mechanohypersensitivity Through the Activation of Inflammasome and IL-1beta Pathway. J. Pain 2019, 20, 956–964. [Google Scholar] [CrossRef]
- Saha, R.N.; Jana, M.; Pahan, K. MAPK p38 regulates transcriptional activity of NF-kappaB in primary human astrocytes via acetylation of p65. J. Immunol. 2007, 179, 7101–7109. [Google Scholar] [CrossRef]
- Somensi, N.; Brum, P.O.; de Miranda Ramos, V.; Gasparotto, J.; Zanotto-Filho, A.; Rostirolla, D.C.; da Silva Morrone, M.; Moreira, J.C.F.; Pens Gelain, D. Extracellular HSP70 Activates ERK1/2, NF-kB and Pro-Inflammatory Gene Transcription Through Binding with RAGE in A549 Human Lung Cancer Cells. Cell Physiol. Biochem. 2017, 42, 2507–2522. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wang, J.; Lu, P.; Cai, Y.; Wang, Y.; Hong, L.; Ren, H.; Heng, B.C.; Liu, H.; Zhou, J.; et al. Local delivery of FTY720 in PCL membrane improves SCI functional recovery by reducing reactive astrogliosis. Biomaterials 2015, 62, 76–87. [Google Scholar] [CrossRef]
- van Doorn, R.; Nijland, P.G.; Dekker, N.; Witte, M.E.; Lopes-Pinheiro, M.A.; van het Hof, B.; Kooij, G.; Reijerkerk, A.; Dijkstra, C.; van van der Valk, P.; et al. Fingolimod attenuates ceramide-induced blood-brain barrier dysfunction in multiple sclerosis by targeting reactive astrocytes. Acta. Neuropathol. 2012, 124, 397–410. [Google Scholar] [CrossRef] [PubMed]
- Healy, L.M.; Sheridan, G.K.; Pritchard, A.J.; Rutkowska, A.; Mullershausen, F.; Dev, K.K. Pathway specific modulation of S1P1 receptor signalling in rat and human astrocytes. Br. J. Pharmacol. 2013, 169, 1114–1129. [Google Scholar] [CrossRef] [PubMed]
- Luchtman, D.; Gollan, R.; Ellwardt, E.; Birkenstock, J.; Robohm, K.; Siffrin, V.; Zipp, F. In vivo and in vitro effects of multiple sclerosis immunomodulatory therapeutics on glutamatergic excitotoxicity. J. Neurochem. 2016, 136, 971–980. [Google Scholar] [CrossRef]
- Cipriani, R.; Chara, J.C.; Rodriguez-Antiguedad, A.; Matute, C. Effects of FTY720 on brain neurogenic niches in vitro and after kainic acid-induced injury. J. Neuroinflammation 2017, 14, 147. [Google Scholar] [CrossRef] [PubMed]
- Cui, Q.L.; Fang, J.; Kennedy, T.E.; Almazan, G.; Antel, J.P. Role of p38MAPK in S1P receptor-mediated differentiation of human oligodendrocyte progenitors. Glia 2014, 62, 1361–1375. [Google Scholar] [CrossRef]
- Jin, Y.; Sun, L.H.; Yang, W.; Cui, R.J.; Xu, S.B. The Role of BDNF in the Neuroimmune Axis Regulation of Mood Disorders. Front Neurol. 2019, 10, 515. [Google Scholar] [CrossRef]
- Traiffort, E.; Kassoussi, A.; Zahaf, A.; Laouarem, Y. Astrocytes and Microglia as Major Players of Myelin Production in Normal and Pathological Conditions. Front Cell Neurosci. 2020, 14, 79. [Google Scholar] [CrossRef]
- Yasuda, K.; Maki, T.; Saito, S.; Yamamoto, Y.; Kinoshita, H.; Choi, Y.K.; Arumugam, T.V.; Lim, Y.A.; Chen, C.L.H.; Wong, P.T.; et al. Effect of fingolimod on oligodendrocyte maturation under prolonged cerebral hypoperfusion. Brain Res. 2019, 1720, 146294. [Google Scholar] [CrossRef]
- Yazdi, A.; Baharvand, H.; Javan, M. Enhanced remyelination following lysolecithin-induced demyelination in mice under treatment with fingolimod (FTY720). Neuroscience 2015, 311, 34–44. [Google Scholar] [CrossRef] [PubMed]
- Caprariello, A.V.; Batt, C.E.; Zippe, I.; Romito-DiGiacomo, R.R.; Karl, M.; Miller, R.H. Apoptosis of Oligodendrocytes during Early Development Delays Myelination and Impairs Subsequent Responses to Demyelination. J. Neurosci. 2015, 35, 14031–14041. [Google Scholar] [CrossRef] [PubMed]
- Dulamea, A.O. Role of Oligodendrocyte Dysfunction in Demyelination, Remyelination and Neurodegeneration in Multiple Sclerosis. Adv. Exp. Med. Biol. 2017, 958, 91–127. [Google Scholar] [CrossRef] [PubMed]
- Coelho, R.P.; Payne, S.G.; Bittman, R.; Spiegel, S.; Sato-Bigbee, C. The immunomodulator FTY720 has a direct cytoprotective effect in oligodendrocyte progenitors. J. Pharmacol. Exp. Ther. 2007, 323, 626–635. [Google Scholar] [CrossRef] [PubMed]
- Bieberich, E. There is more to a lipid than just being a fat: Sphingolipid-guided differentiation of oligodendroglial lineage from embryonic stem cells. Neurochem. Res. 2011, 36, 1601–1611. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Miron, V.E.; Jung, C.G.; Kim, H.J.; Kennedy, T.E.; Soliven, B.; Antel, J.P. FTY720 modulates human oligodendrocyte progenitor process extension and survival. Ann. Neurol. 2008, 63, 61–71. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Zhang, Z.G.; Li, Y.; Ding, X.; Shang, X.; Lu, M.; Elias, S.B.; Chopp, M. Fingolimod treatment promotes proliferation and differentiation of oligodendrocyte progenitor cells in mice with experimental autoimmune encephalomyelitis. Neurobiol. Dis. 2015, 76, 57–66. [Google Scholar] [CrossRef]
- Dasgupta, S.; Ray, S.K. Ceramide and Sphingosine Regulation of Myelinogenesis: Targeting Serine Palmitoyltransferase Using microRNA in Multiple Sclerosis. Int. J. Mol. Sci. 2019, 20, 5031. [Google Scholar] [CrossRef]
- Pritchard, A.J.; Mir, A.K.; Dev, K.K. Fingolimod attenuates splenocyte-induced demyelination in cerebellar slice cultures. PLoS ONE 2014, 9, e99444. [Google Scholar] [CrossRef]
- Osinde, M.; Mullershausen, F.; Dev, K.K. Phosphorylated FTY720 stimulates ERK phosphorylation in astrocytes via S1P receptors. Neuropharmacology 2007, 52, 1210–1218. [Google Scholar] [CrossRef]
- Segura-Ulate, I.; Yang, B.; Vargas-Medrano, J.; Perez, R.G. FTY720 (Fingolimod) reverses alpha-synuclein-induced downregulation of brain-derived neurotrophic factor mRNA in OLN-93 oligodendroglial cells. Neuropharmacology 2017, 117, 149–157. [Google Scholar] [CrossRef] [PubMed]
- Michell-Robinson, M.A.; Moore, C.S.; Healy, L.M.; Osso, L.A.; Zorko, N.; Grouza, V.; Touil, H.; Poliquin-Lasnier, L.; Trudelle, A.M.; Giacomini, P.S.; et al. Effects of fumarates on circulating and CNS myeloid cells in multiple sclerosis. Ann. Clin. Transl. Neurol. 2016, 3, 27–41. [Google Scholar] [CrossRef] [PubMed]
- Fowler, J.H.; McQueen, J.; Holland, P.R.; Manso, Y.; Marangoni, M.; Scott, F.; Chisholm, E.; Scannevin, R.H.; Hardingham, G.E.; Horsburgh, K. Dimethyl fumarate improves white matter function following severe hypoperfusion: Involvement of microglia/macrophages and inflammatory mediators. J. Cereb Blood Flow Metab. 2018, 38, 1354–1370. [Google Scholar] [CrossRef] [PubMed]
- Lin, R.; Cai, J.; Kostuk, E.W.; Rosenwasser, R.; Iacovitti, L. Fumarate modulates the immune/inflammatory response and rescues nerve cells and neurological function after stroke in rats. J. Neuroinflammation 2016, 13, 269. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Vollmer, M.K.; Ahmad, A.S.; Fernandez, V.M.; Kim, H.; Dore, S. Pretreatment with Korean red ginseng or dimethyl fumarate attenuates reactive gliosis and confers sustained neuroprotection against cerebral hypoxic-ischemic damage by an Nrf2-dependent mechanism. Free Radic. Biol. Med. 2019, 131, 98–114. [Google Scholar] [CrossRef]
- Traub, J.; Traffehn, S.; Ochs, J.; Hausser-Kinzel, S.; Stephan, S.; Scannevin, R.; Bruck, W.; Metz, I.; Weber, M.S. Dimethyl fumarate impairs differentiated B cells and fosters central nervous system integrity in treatment of multiple sclerosis. Brain Pathol. 2019, 29, 640–657. [Google Scholar] [CrossRef]
- Campolo, M.; Casili, G.; Biundo, F.; Crupi, R.; Cordaro, M.; Cuzzocrea, S.; Esposito, E. The Neuroprotective Effect of Dimethyl Fumarate in an MPTP-Mouse Model of Parkinson’s Disease: Involvement of Reactive Oxygen Species/Nuclear Factor-kappaB/Nuclear Transcription Factor Related to NF-E2. Antioxid Redox. Signal 2017, 27, 453–471. [Google Scholar] [CrossRef]
- Southwood, C.M.; Garshott, D.M.; Richardson, C.R.; Seraji-Bozorgzad, N.; Fribley, A.M.; Gow, A. Dimethyl fumarate ameliorates myoclonus stemming from protein misfolding in oligodendrocytes. J. Neurochem. 2017, 142, 103–117. [Google Scholar] [CrossRef]
- Cordaro, M.; Casili, G.; Paterniti, I.; Cuzzocrea, S.; Esposito, E. Fumaric Acid Esters Attenuate Secondary Degeneration after Spinal Cord Injury. J. Neurotrauma. 2017, 34, 3027–3040. [Google Scholar] [CrossRef]
- Iniaghe, L.O.; Krafft, P.R.; Klebe, D.W.; Omogbai, E.K.I.; Zhang, J.H.; Tang, J. Dimethyl fumarate confers neuroprotection by casein kinase 2 phosphorylation of Nrf2 in murine intracerebral hemorrhage. Neurobiol. Dis. 2015, 82, 349–358. [Google Scholar] [CrossRef]
- Cuadrado, A.; Kugler, S.; Lastres-Becker, I. Pharmacological targeting of GSK-3 and NRF2 provides neuroprotection in a preclinical model of tauopathy. Redox Biol. 2018, 14, 522–534. [Google Scholar] [CrossRef] [PubMed]
- Paraiso, H.C.; Kuo, P.C.; Curfman, E.T.; Moon, H.J.; Sweazey, R.D.; Yen, J.H.; Chang, F.L.; Yu, I.C. Dimethyl fumarate attenuates reactive microglia and long-term memory deficits following systemic immune challenge. J. Neuroinflammation 2018, 15, 100. [Google Scholar] [CrossRef] [PubMed]
- Majkutewicz, I.; Kurowska, E.; Podlacha, M.; Myslinska, D.; Grembecka, B.; Rucinski, J.; Pierzynowska, K.; Wrona, D. Age-dependent effects of dimethyl fumarate on cognitive and neuropathological features in the streptozotocin-induced rat model of Alzheimer’s disease. Brain Res. 2018, 1686, 19–33. [Google Scholar] [CrossRef] [PubMed]
- Pagani, F.; Testi, C.; Grimaldi, A.; Corsi, G.; Cortese, B.; Basilico, B.; Baiocco, P.; De Panfilis, S.; Ragozzino, D.; Di Angelantonio, S. Dimethyl Fumarate Reduces Microglia Functional Response to Tissue Damage and Favors Brain Iron Homeostasis. Neuroscience 2019. [Google Scholar] [CrossRef]
- Kronenberg, J.; Pars, K.; Brieskorn, M.; Prajeeth, C.K.; Heckers, S.; Schwenkenbecher, P.; Skripuletz, T.; Pul, R.; Pavlou, A.; Stangel, M. Fumaric Acids Directly Influence Gene Expression of Neuroprotective Factors in Rodent Microglia. Int. J. Mol. Sci. 2019, 20, 325. [Google Scholar] [CrossRef]
- Booth, L.; Cruickshanks, N.; Tavallai, S.; Roberts, J.L.; Peery, M.; Poklepovic, A.; Dent, P. Regulation of dimethyl-fumarate toxicity by proteasome inhibitors. Cancer Biol. Ther. 2014, 15, 1646–1657. [Google Scholar] [CrossRef]
- Parodi, B.; Rossi, S.; Morando, S.; Cordano, C.; Bragoni, A.; Motta, C.; Usai, C.; Wipke, B.T.; Scannevin, R.H.; Mancardi, G.L.; et al. Fumarates modulate microglia activation through a novel HCAR2 signaling pathway and rescue synaptic dysregulation in inflamed CNS. Acta. Neuropathol. 2015, 130, 279–295. [Google Scholar] [CrossRef]
- Moharregh-Khiabani, D.; Blank, A.; Skripuletz, T.; Miller, E.; Kotsiari, A.; Gudi, V.; Stangel, M. Effects of fumaric acids on cuprizone induced central nervous system de- and remyelination in the mouse. PLoS ONE 2010, 5, e11769. [Google Scholar] [CrossRef] [PubMed]
- Reick, C.; Ellrichmann, G.; Thone, J.; Scannevin, R.H.; Saft, C.; Linker, R.A.; Gold, R. Neuroprotective dimethyl fumarate synergizes with immunomodulatory interferon beta to provide enhanced axon protection in autoimmune neuroinflammation. Exp. Neurol. 2014, 257, 50–56. [Google Scholar] [CrossRef]
- Zhao, X.; Sun, G.; Zhang, J.; Ting, S.M.; Gonzales, N.; Aronowski, J. Dimethyl Fumarate Protects Brain From Damage Produced by Intracerebral Hemorrhage by Mechanism Involving Nrf2. Stroke 2015, 46, 1923–1928. [Google Scholar] [CrossRef]
- Wierinckx, A.; Breve, J.; Mercier, D.; Schultzberg, M.; Drukarch, B.; Van Dam, A.M. Detoxication enzyme inducers modify cytokine production in rat mixed glial cells. J. Neuroimmunol. 2005, 166, 132–143. [Google Scholar] [CrossRef] [PubMed]
- Wilms, H.; Sievers, J.; Rickert, U.; Rostami-Yazdi, M.; Mrowietz, U.; Lucius, R. Dimethylfumarate inhibits microglial and astrocytic inflammation by suppressing the synthesis of nitric oxide, IL-1beta, TNF-alpha and IL-6 in an in-vitro model of brain inflammation. J. Neuroinflammation 2010, 7, 30. [Google Scholar] [CrossRef] [PubMed]
- Peng, H.; Li, H.; Sheehy, A.; Cullen, P.; Allaire, N.; Scannevin, R.H. Dimethyl fumarate alters microglia phenotype and protects neurons against proinflammatory toxic microenvironments. J. Neuroimmunol. 2016, 299, 35–44. [Google Scholar] [CrossRef] [PubMed]
- Foresti, R.; Bains, S.K.; Pitchumony, T.S.; de Castro Bras, L.E.; Drago, F.; Dubois-Rande, J.L.; Bucolo, C.; Motterlini, R. Small molecule activators of the Nrf2-HO-1 antioxidant axis modulate heme metabolism and inflammation in BV2 microglia cells. Pharmacol. Res. 2013, 76, 132–148. [Google Scholar] [CrossRef] [PubMed]
- Graber, D.J.; Hickey, W.F.; Stommel, E.W.; Harris, B.T. Anti-inflammatory efficacy of dexamethasone and Nrf2 activators in the CNS using brain slices as a model of acute injury. J. Neuroimmune Pharmacol. 2012, 7, 266–278. [Google Scholar] [CrossRef]
- Ambrosius, B.; Faissner, S.; Guse, K.; von Lehe, M.; Grunwald, T.; Gold, R.; Grewe, B.; Chan, A. Teriflunomide and monomethylfumarate target HIV-induced neuroinflammation and neurotoxicity. J. Neuroinflammation 2017, 14, 51. [Google Scholar] [CrossRef]
- Pars, K.; Gingele, M.; Kronenberg, J.; Prajeeth, C.K.; Skripuletz, T.; Pul, R.; Jacobs, R.; Gudi, V.; Stangel, M. Fumaric Acids Do Not Directly Influence Gene Expression of Neuroprotective Factors in Highly Purified Rodent Astrocytes. Brain Sci. 2019, 9, 241. [Google Scholar] [CrossRef]
- Galloway, D.A.; Williams, J.B.; Moore, C.S. Effects of fumarates on inflammatory human astrocyte responses and oligodendrocyte differentiation. Ann. Clin. Transl. Neurol. 2017, 4, 381–391. [Google Scholar] [CrossRef]
- Kunze, R.; Urrutia, A.; Hoffmann, A.; Liu, H.; Helluy, X.; Pham, M.; Reischl, S.; Korff, T.; Marti, H.H. Dimethyl fumarate attenuates cerebral edema formation by protecting the blood-brain barrier integrity. Exp. Neurol. 2015, 266, 99–111. [Google Scholar] [CrossRef]
- Kalinin, S.; Polak, P.E.; Lin, S.X.; Braun, D.; Guizzetti, M.; Zhang, X.; Rubinstein, I.; Feinstein, D.L. Dimethyl fumarate regulates histone deacetylase expression in astrocytes. J. Neuroimmunol. 2013, 263, 13–19. [Google Scholar] [CrossRef]
- Murphy, T.H.; Yu, J.; Ng, R.; Johnson, D.A.; Shen, H.; Honey, C.R.; Johnson, J.A. Preferential expression of antioxidant response element mediated gene expression in astrocytes. J. Neurochem. 2001, 76, 1670–1678. [Google Scholar] [CrossRef] [PubMed]
- Gill, A.J.; Kovacsics, C.E.; Cross, S.A.; Vance, P.J.; Kolson, L.L.; Jordan-Sciutto, K.L.; Gelman, B.B.; Kolson, D.L. Heme oxygenase-1 deficiency accompanies neuropathogenesis of HIV-associated neurocognitive disorders. J. Clin. Investig. 2014, 124, 4459–4472. [Google Scholar] [CrossRef] [PubMed]
- Bombeiro, A.L.; Toledo Nunes Pereira, B.; Pires Bonfanti, A.; de Oliveira, A.L.R. Immunomodulation by dimethyl fumarate treatment improves mouse sciatic nerve regeneration. Brain Res. Bull 2020. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Assmann, J.C.; Krenz, A.; Rahman, M.; Grimm, M.; Karsten, C.M.; Kohl, J.; Offermanns, S.; Wettschureck, N.; Schwaninger, M. Hydroxycarboxylic acid receptor 2 mediates dimethyl fumarate’s protective effect in EAE. J. Clin. Investig. 2014, 124, 2188–2192. [Google Scholar] [CrossRef]
- Kumar, P.; Sharma, G.; Gupta, V.; Kaur, R.; Thakur, K.; Malik, R.; Kumar, A.; Kaushal, N.; Raza, K. Preclinical Explorative Assessment of Dimethyl Fumarate-Based Biocompatible Nanolipoidal Carriers for the Management of Multiple Sclerosis. ACS Chem. Neurosci. 2018, 9, 1152–1158. [Google Scholar] [CrossRef]
- Huang, H.; Taraboletti, A.; Shriver, L.P. Dimethyl fumarate modulates antioxidant and lipid metabolism in oligodendrocytes. Redox Biol. 2015, 5, 169–175. [Google Scholar] [CrossRef]
- Weber, M.S.; Hohlfeld, R.; Zamvil, S.S. Mechanism of action of glatiramer acetate in treatment of multiple sclerosis. Neurotherapeutics 2007, 4, 647–653. [Google Scholar] [CrossRef]
- Lalive, P.H.; Neuhaus, O.; Benkhoucha, M.; Burger, D.; Hohlfeld, R.; Zamvil, S.S.; Weber, M.S. Glatiramer acetate in the treatment of multiple sclerosis: Emerging concepts regarding its mechanism of action. CNS Drugs 2011, 25, 401–414. [Google Scholar] [CrossRef]
- Yong, V.W. Differential mechanisms of action of interferon-beta and glatiramer aetate in MS. Neurology 2002, 59, 802–808. [Google Scholar] [CrossRef]
- Maier, K.; Kuhnert, A.V.; Taheri, N.; Sattler, M.B.; Storch, M.K.; Williams, S.K.; Bahr, M.; Diem, R. Effects of glatiramer acetate and interferon-beta on neurodegeneration in a model of multiple sclerosis: A comparative study. Am. J. Pathol. 2006, 169, 1353–1364. [Google Scholar] [CrossRef]
- Gilli, F.; Navone, N.D.; Perga, S.; Marnetto, F.; Caldano, M.; Capobianco, M.; Pulizzi, A.; Malucchi, S.; Bertolotto, A. Loss of braking signals during inflammation: A factor affecting the development and disease course of multiple sclerosis. Arch. Neurol. 2011, 68, 879–888. [Google Scholar] [CrossRef] [PubMed]
- He, F.; Zou, J.T.; Zhou, Q.F.; Niu, D.L.; Jia, W.H. Glatiramer acetate reverses cognitive deficits from cranial-irradiated rat by inducing hippocampal neurogenesis. J. Neuroimmunol. 2014, 271, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Leger, T.; Grist, J.; D’Acquisto, F.; Clark, A.K.; Malcangio, M. Glatiramer acetate attenuates neuropathic allodynia through modulation of adaptive immune cells. J. Neuroimmunol. 2011, 234, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Aharoni, R.; Eilam, R.; Stock, A.; Vainshtein, A.; Shezen, E.; Gal, H.; Friedman, N.; Arnon, R. Glatiramer acetate reduces Th-17 inflammation and induces regulatory T-cells in the CNS of mice with relapsing-remitting or chronic EAE. J. Neuroimmunol. 2010, 225, 100–111. [Google Scholar] [CrossRef] [PubMed]
- Reichert, F.; Rotshenker, S. Galectin-3/MAC-2 in experimental allergic encephalomyelitis. Exp. Neurol. 1999, 160, 508–514. [Google Scholar] [CrossRef] [PubMed]
- Aharoni, R.; Arnon, R.; Eilam, R. Neurogenesis and neuroprotection induced by peripheral immunomodulatory treatment of experimental autoimmune encephalomyelitis. J. Neurosci. 2005, 25, 8217–8228. [Google Scholar] [CrossRef] [PubMed]
- Butovsky, O.; Koronyo-Hamaoui, M.; Kunis, G.; Ophir, E.; Landa, G.; Cohen, H.; Schwartz, M. Glatiramer acetate fights against Alzheimer’s disease by inducing dendritic-like microglia expressing insulin-like growth factor 1. Proc. Natl. Acad Sci. USA 2006, 103, 11784–11789. [Google Scholar] [CrossRef]
- Chabot, S.; Yong, F.P.; Le, D.M.; Metz, L.M.; Myles, T.; Yong, V.W. Cytokine production in T lymphocyte-microglia interaction is attenuated by glatiramer acetate: A mechanism for therapeutic efficacy in multiple sclerosis. Mult. Scler. 2002, 8, 299–306. [Google Scholar] [CrossRef]
- Gentile, A.; Rossi, S.; Studer, V.; Motta, C.; De Chiara, V.; Musella, A.; Sepman, H.; Fresegna, D.; Musumeci, G.; Grasselli, G.; et al. Glatiramer acetate protects against inflammatory synaptopathy in experimental autoimmune encephalomyelitis. J. Neuroimmune. Pharmacol. 2013, 8, 651–663. [Google Scholar] [CrossRef]
- Rosato Siri, M.V.; Badaracco, M.E.; Pasquini, J.M. Glatiramer promotes oligodendroglial cell maturation in a cuprizone-induced demyelination model. Neurochem. Int. 2013, 63, 10–24. [Google Scholar] [CrossRef]
- Pul, R.; Moharregh-Khiabani, D.; Skuljec, J.; Skripuletz, T.; Garde, N.; Voss, E.V.; Stangel, M. Glatiramer acetate modulates TNF-alpha and IL-10 secretion in microglia and promotes their phagocytic activity. J. Neuroimmune. Pharmacol. 2011, 6, 381–388. [Google Scholar] [CrossRef] [PubMed]
- Nau, R.; Ribes, S.; Djukic, M.; Eiffert, H. Strategies to increase the activity of microglia as efficient protectors of the brain against infections. Front Cell Neurosci. 2014, 8, 138. [Google Scholar] [CrossRef] [PubMed]
- Chan, A.; Papadimitriou, C.; Graf, W.; Toyka, K.V.; Gold, R. Effects of polyclonal immunoglobulins and other immunomodulatory agents on microglial phagocytosis of apoptotic inflammatory T-cells. J. Neuroimmunol. 2003, 135, 161–165. [Google Scholar] [CrossRef]
- Aharoni, R.; Kayhan, B.; Eilam, R.; Sela, M.; Arnon, R. Glatiramer acetate-specific T cells in the brain express T helper 2/3 cytokines and brain-derived neurotrophic factor in situ. Proc. Natl. Acad Sci. USA 2003, 100, 14157–14162. [Google Scholar] [CrossRef] [PubMed]
- Evangelidou, M.; Karamita, M.; Vamvakas, S.S.; Szymkowski, D.E.; Probert, L. Altered expression of oligodendrocyte and neuronal marker genes predicts the clinical onset of autoimmune encephalomyelitis and indicates the effectiveness of multiple sclerosis-directed therapeutics. J. Immunol. 2014, 192, 4122–4133. [Google Scholar] [CrossRef] [PubMed]
- Aharoni, R.; Schottlender, N.; Bar-Lev, D.D.; Eilam, R.; Sela, M.; Tsoory, M.; Arnon, R. Cognitive impairment in an animal model of multiple sclerosis and its amelioration by glatiramer acetate. Sci. Rep. 2019, 9, 4140. [Google Scholar] [CrossRef] [PubMed]
- Reick, C.; Ellrichmann, G.; Tsai, T.; Lee, D.H.; Wiese, S.; Gold, R.; Saft, C.; Linker, R.A. Expression of brain-derived neurotrophic factor in astrocytes - Beneficial effects of glatiramer acetate in the R6/2 and YAC128 mouse models of Huntington’s disease. Exp. Neurol. 2016, 285, 12–23. [Google Scholar] [CrossRef]
- Corey-Bloom, J.; Aikin, A.M.; Gutierrez, A.M.; Nadhem, J.S.; Howell, T.L.; Thomas, E.A. Beneficial effects of glatiramer acetate in Huntington’s disease mouse models: Evidence for BDNF-elevating and immunomodulatory mechanisms. Brain Res. 2017, 1673, 102–110. [Google Scholar] [CrossRef]
- Moore, S.; Khalaj, A.J.; Patel, R.; Yoon, J.; Ichwan, D.; Hayardeny, L.; Tiwari-Woodruff, S.K. Restoration of axon conduction and motor deficits by therapeutic treatment with glatiramer acetate. J. Neurosci. Res. 2014, 92, 1621–1636. [Google Scholar] [CrossRef]
- Gilgun-Sherki, Y.; Panet, H.; Holdengreber, V.; Mosberg-Galili, R.; Offen, D. Axonal damage is reduced following glatiramer acetate treatment in C57/bl mice with chronic-induced experimental autoimmune encephalomyelitis. Neurosci. Res. 2003, 47, 201–207. [Google Scholar] [CrossRef]
- Lee, D.H.; Geyer, E.; Flach, A.C.; Jung, K.; Gold, R.; Flugel, A.; Linker, R.A.; Luhder, F. Central nervous system rather than immune cell-derived BDNF mediates axonal protective effects early in autoimmune demyelination. Acta. Neuropathol. 2012, 123, 247–258. [Google Scholar] [CrossRef] [PubMed]
- Schori, H.; Robenshtok, E.; Schwartz, M.; Hourvitz, A. Post-intoxication vaccination for protection of neurons against the toxicity of nerve agents. Toxicol. Sci. 2005, 87, 163–168. [Google Scholar] [CrossRef] [PubMed]
- Aharoni, R.; Herschkovitz, A.; Eilam, R.; Blumberg-Hazan, M.; Sela, M.; Bruck, W.; Arnon, R. Demyelination arrest and remyelination induced by glatiramer acetate treatment of experimental autoimmune encephalomyelitis. Proc. Natl. Acad. Sci. USA 2008, 105, 11358–11363. [Google Scholar] [CrossRef] [PubMed]
- Khan, O.; Shen, Y.; Bao, F.; Caon, C.; Tselis, A.; Latif, Z.; Zak, I. Long-term study of brain 1H-MRS study in multiple sclerosis: Effect of glatiramer acetate therapy on axonal metabolic function and feasibility of long-Term H-MRS monitoring in multiple sclerosis. J. Neuroimaging 2008, 18, 314–319. [Google Scholar] [CrossRef]
- Wiebenga, O.T.; Klauser, A.M.; Schoonheim, M.M.; Nagtegaal, G.J.; Steenwijk, M.D.; van Rossum, J.A.; Polman, C.H.; Barkhof, F.; Pouwels, P.J.; Geurts, J.J. Enhanced axonal metabolism during early natalizumab treatment in relapsing-remitting multiple sclerosis. AJNR Am. J. Neuroradiol. 2015, 36, 1116–1123. [Google Scholar] [CrossRef]
- Skihar, V.; Silva, C.; Chojnacki, A.; Doring, A.; Stallcup, W.B.; Weiss, S.; Yong, V.W. Promoting oligodendrogenesis and myelin repair using the multiple sclerosis medication glatiramer acetate. Proc. Natl. Acad Sci. USA 2009, 106, 17992–17997. [Google Scholar] [CrossRef]
- Song, F.; Bandara, M.; Deol, H.; Loeb, J.A.; Benjamins, J.; Lisak, R.P. Complexity of trophic factor signaling in experimental autoimmune encephalomyelitis: Differential expression of neurotrophic and gliotrophic factors. J. Neuroimmunol. 2013, 262, 11–18. [Google Scholar] [CrossRef][Green Version]
- From, R.; Eilam, R.; Bar-Lev, D.D.; Levin-Zaidman, S.; Tsoory, M.; LoPresti, P.; Sela, M.; Arnon, R.; Aharoni, R. Oligodendrogenesis and myelinogenesis during postnatal development effect of glatiramer acetate. Glia 2014, 62, 649–665. [Google Scholar] [CrossRef]
- Zhang, Y.; Jalili, F.; Ouamara, N.; Zameer, A.; Cosentino, G.; Mayne, M.; Hayardeny, L.; Antel, J.P.; Bar-Or, A.; John, G.R. Glatiramer acetate-reactive T lymphocytes regulate oligodendrocyte progenitor cell number in vitro: Role of IGF-2. J. Neuroimmunol. 2010, 227, 71–79. [Google Scholar] [CrossRef]
- Zula, J.A.; Green, H.C.; Ransohoff, R.M.; Rudick, R.A.; Stark, G.R.; van Boxel-Dezaire, A.H. The role of cell type-specific responses in IFN-beta therapy of multiple sclerosis. Proc. Natl. Acad Sci. USA 2011, 108, 19689–19694. [Google Scholar] [CrossRef]
- Lopez de Padilla, C.M.; Niewold, T.B. The type I interferons: Basic concepts and clinical relevance in immune-mediated inflammatory diseases. Gene 2016, 576, 14–21. [Google Scholar] [CrossRef] [PubMed]
- McDonough, A.; Lee, R.V.; Weinstein, J.R. Microglial Interferon Signaling and White Matter. Neurochem. Res. 2017, 42, 2625–2638. [Google Scholar] [CrossRef] [PubMed]
- Trebst, C.; Heine, S.; Lienenklaus, S.; Lindner, M.; Baumgartner, W.; Weiss, S.; Stangel, M. Lack of interferon-beta leads to accelerated remyelination in a toxic model of central nervous system demyelination. Acta. Neuropathol. 2007, 114, 587–596. [Google Scholar] [CrossRef] [PubMed]
- Main, B.S.; Zhang, M.; Brody, K.M.; Ayton, S.; Frugier, T.; Steer, D.; Finkelstein, D.; Crack, P.J.; Taylor, J.M. Type-1 interferons contribute to the neuroinflammatory response and disease progression of the MPTP mouse model of Parkinson’s disease. Glia 2016, 64, 1590–1604. [Google Scholar] [CrossRef] [PubMed]
- Minter, M.R.; Moore, Z.; Zhang, M.; Brody, K.M.; Jones, N.C.; Shultz, S.R.; Taylor, J.M.; Crack, P.J. Deletion of the type-1 interferon receptor in APPSWE/PS1DeltaE9 mice preserves cognitive function and alters glial phenotype. Acta. Neuropathol. Commun. 2016, 4, 72. [Google Scholar] [CrossRef]
- Choi, B.Y.; Sim, C.K.; Cho, Y.S.; Sohn, M.; Kim, Y.J.; Lee, M.S.; Suh, S.W. 2’-5’ oligoadenylate synthetase-like 1 (OASL1) deficiency suppresses central nervous system damage in a murine MOG-induced multiple sclerosis model. Neurosci. Lett. 2016, 628, 78–84. [Google Scholar] [CrossRef]
- Isaksson, M.; Ardesjo, B.; Ronnblom, L.; Kampe, O.; Lassmann, H.; Eloranta, M.L.; Lobell, A. Plasmacytoid DC promote priming of autoimmune Th17 cells and EAE. Eur. J. Immunol. 2009, 39, 2925–2935. [Google Scholar] [CrossRef]
- Costello, D.A.; Lynch, M.A. Toll-like receptor 3 activation modulates hippocampal network excitability, via glial production of interferon-beta. Hippocampus 2013, 23, 696–707. [Google Scholar] [CrossRef]
- Kasper, L.H.; Reder, A.T. Immunomodulatory activity of interferon-beta. Ann. Clin. Transl. Neurol. 2014, 1, 622–631. [Google Scholar] [CrossRef]
- Cohen, B.; Novick, D.; Barak, S.; Rubinstein, M. Ligand-induced association of the type I interferon receptor components. Mol. Cell Biol. 1995, 15, 4208–4214. [Google Scholar] [CrossRef]
- Levin, D.; Harari, D.; Schreiber, G. Stochastic receptor expression determines cell fate upon interferon treatment. Mol. Cell Biol. 2011, 31, 3252–3266. [Google Scholar] [CrossRef] [PubMed]
- Esen, N.; Rainey-Barger, E.K.; Huber, A.K.; Blakely, P.K.; Irani, D.N. Type-I interferons suppress microglial production of the lymphoid chemokine, CXCL13. Glia 2014, 62, 1452–1462. [Google Scholar] [CrossRef] [PubMed]
- Konnecke, H.; Bechmann, I. The role of microglia and matrix metalloproteinases involvement in neuroinflammation and gliomas. Clin. Dev. Immunol. 2013, 2013, 914104. [Google Scholar] [CrossRef] [PubMed]
- Liuzzi, G.M.; Latronico, T.; Fasano, A.; Carlone, G.; Riccio, P. Interferon-beta inhibits the expression of metalloproteinases in rat glial cell cultures: Implications for multiple sclerosis pathogenesis and treatment. Mult. Scler. 2004, 10, 290–297. [Google Scholar] [CrossRef] [PubMed]
- Luckoff, A.; Caramoy, A.; Scholz, R.; Prinz, M.; Kalinke, U.; Langmann, T. Interferon-beta signaling in retinal mononuclear phagocytes attenuates pathological neovascularization. EMBO Mol. Med. 2016, 8, 670–678. [Google Scholar] [CrossRef] [PubMed]
- Li, P.; Zhao, G.; Ding, Y.; Wang, T.; Flores, J.; Ocak, U.; Wu, P.; Zhang, T.; Mo, J.; Zhang, J.H.; et al. Rh-IFN-alpha attenuates neuroinflammation and improves neurological function by inhibiting NF-kappaB through JAK1-STAT1/TRAF3 pathway in an experimental GMH rat model. Brain Behav. Immun. 2019, 79, 174–185. [Google Scholar] [CrossRef]
- Sattler, M.B.; Demmer, I.; Williams, S.K.; Maier, K.; Merkler, D.; Gadjanski, I.; Stadelmann, C.; Bahr, M.; Diem, R. Effects of interferon-beta-1a on neuronal survival under autoimmune inflammatory conditions. Exp. Neurol. 2006, 201, 172–181. [Google Scholar] [CrossRef]
- MacMillan, E.L.; Schubert, J.J.; Vavasour, I.M.; Tam, R.; Rauscher, A.; Taylor, C.; White, R.; Garren, H.; Clayton, D.; Levesque, V.; et al. Magnetic resonance spectroscopy evidence for declining gliosis in MS patients treated with ocrelizumab versus interferon beta-1a. Mult. Scler. J. Exp. Transl. Clin. 2019, 5, 2055217319879952. [Google Scholar] [CrossRef]
- Roy, E.R.; Wang, B.; Wan, Y.W.; Chiu, G.; Cole, A.; Yin, Z.; Propson, N.E.; Xu, Y.; Jankowsky, J.L.; Liu, Z.; et al. Type I interferon response drives neuroinflammation and synapse loss in Alzheimer disease. J. Clin. Investig. 2020. [Google Scholar] [CrossRef]
- GuhaSarkar, D.; Neiswender, J.; Su, Q.; Gao, G.; Sena-Esteves, M. Intracranial AAV-IFN-beta gene therapy eliminates invasive xenograft glioblastoma and improves survival in orthotopic syngeneic murine model. Mol. Oncol. 2017, 11, 180–193. [Google Scholar] [CrossRef]
- Ben-Yehuda, H.; Matcovitch-Natan, O.; Kertser, A.; Spinrad, A.; Prinz, M.; Amit, I.; Schwartz, M. Maternal Type-I interferon signaling adversely affects the microglia and the behavior of the offspring accompanied by increased sensitivity to stress. Mol. Psychiatry 2019. [Google Scholar] [CrossRef] [PubMed]
- Hall, G.L.; Wing, M.G.; Compston, D.A.S.; Scolding, N.J. β-interferon regulates the immunomodulatory activity of neonatal rodent microglia. J. Neuroimmunol. 1997, 72, 11–19. [Google Scholar] [CrossRef]
- Sen, T.; Saha, P.; Gupta, R.; Foley, L.M.; Jiang, T.; Abakumova, O.S.; Hitchens, T.K.; Sen, N. Aberrant ER Stress Induced Neuronal-IFNbeta Elicits White Matter Injury Due to Microglial Activation and T-Cell Infiltration after TBI. J. Neurosci. 2020, 40, 424–446. [Google Scholar] [CrossRef] [PubMed]
- Wachholz, S.; Esslinger, M.; Plumper, J.; Manitz, M.P.; Juckel, G.; Friebe, A. Microglia activation is associated with IFN-alpha induced depressive-like behavior. Brain Behav. Immun. 2016, 55, 105–113. [Google Scholar] [CrossRef]
- Nakamichi, K.; Saiki, M.; Kitani, H.; Kuboyama, Y.; Morimoto, K.; Takayama-Ito, M.; Kurane, I. Suppressive effect of simvastatin on interferon-beta-induced expression of CC chemokine ligand 5 in microglia. Neurosci. Lett. 2006, 407, 205–210. [Google Scholar] [CrossRef]
- Jin, S.; Kawanokuchi, J.; Mizuno, T.; Wang, J.; Sonobe, Y.; Takeuchi, H.; Suzumura, A. Interferon-beta is neuroprotective against the toxicity induced by activated microglia. Brain Res. 2007, 1179, 140–146. [Google Scholar] [CrossRef]
- Li, W.; Viengkhou, B.; Denyer, G.; West, P.K.; Campbell, I.L.; Hofer, M.J. Microglia have a more extensive and divergent response to interferon-alpha compared with astrocytes. Glia 2018, 66, 2058–2078. [Google Scholar] [CrossRef]
- Khatun, M.R.; Arifuzzaman, S. Selected TLR7/8 agonist and type I interferon (IFN-alpha) cooperatively redefine the microglia transcriptome. Inflammopharmacology 2019. [Google Scholar] [CrossRef]
- Cox, D.J.; Field, R.H.; Williams, D.G.; Baran, M.; Bowie, A.G.; Cunningham, C.; Dunne, A. DNA sensors are expressed in astrocytes and microglia in vitro and are upregulated during gliosis in neurodegenerative disease. Glia 2015, 63, 812–825. [Google Scholar] [CrossRef]
- Mastronardi, F.G.; Min, W.; Wang, H.; Winer, S.; Dosch, M.; Boggs, J.M.; Moscarello, M.A. Attenuation of experimental autoimmune encephalomyelitis and nonimmune demyelination by IFN-beta plus vitamin B12: Treatment to modify notch-1/sonic hedgehog balance. J. Immunol. 2004, 172, 6418–6426. [Google Scholar] [CrossRef]
- Chhatbar, C.; Detje, C.N.; Grabski, E.; Borst, K.; Spanier, J.; Ghita, L.; Elliott, D.A.; Jordao, M.J.C.; Mueller, N.; Sutton, J.; et al. Type I Interferon Receptor Signaling of Neurons and Astrocytes Regulates Microglia Activation during Viral Encephalitis. Cell Rep. 2018, 25, 118–129. [Google Scholar] [CrossRef] [PubMed]
- Rothhammer, V.; Mascanfroni, I.D.; Bunse, L.; Takenaka, M.C.; Kenison, J.E.; Mayo, L.; Chao, C.C.; Patel, B.; Yan, R.; Blain, M.; et al. Type I interferons and microbial metabolites of tryptophan modulate astrocyte activity and central nervous system inflammation via the aryl hydrocarbon receptor. Nat. Med. 2016, 22, 586–597. [Google Scholar] [CrossRef] [PubMed]
- Malik, O.; Compston, D.A.S.; Scolding, N.J. Interferon-beta inhibits mitogen induced astrocyte proliferation in vitro. J. Neuroimmunol. 1998, 86, 155–162. [Google Scholar] [CrossRef]
- Garrison, J.I.; Berens, M.E.; Shapiro, J.R.; Treasurywala, S.; Floyd-Smith, G. Interferon-beta inhibits proliferation and progression through S phase of the cell cycle in five glioma cell lines. J. Neurooncol. 1996, 30, 213–223. [Google Scholar] [CrossRef] [PubMed]
- Guthikonda, P.; Baker, J.; Mattson, D.H. Interferon-beta-1-b (IFN-B) decreases induced nitric oxide (NO) production by a human astrocytoma cell line. J. Neuroimmunol. 1998, 82, 133–139. [Google Scholar] [CrossRef]
- Latronico, T.; Brana, M.T.; Gramegna, P.; Fasano, A.; Di Bari, G.; Liuzzi, G.M. Inhibition of myelin-cleaving poteolytic activities by interferon-beta in rat astrocyte cultures. Comparative analysis between gelatinases and calpain-II. PLoS ONE 2013, 8, e49656. [Google Scholar] [CrossRef]
- Muller, M.; Frese, A.; Nassenstein, I.; Hoppen, M.; Marziniak, M.; Ringelstein, E.B.; Kim, K.S.; Schabitz, W.R.; Kraus, J. Serum from interferon-beta-1b-treated patients with early multiple sclerosis stabilizes the blood-brain barrier in vitro. Mult. Scler. 2012, 18, 236–239. [Google Scholar] [CrossRef]
- Kraus, J.; Ling, A.K.; Hamm, S.; Voigt, K.; Oschmann, P.; Engelhardt, B. Interferon-beta stabilizes barrier characteristics of brain endothelial cells in vitro. Ann. Neurol. 2004, 56, 192–205. [Google Scholar] [CrossRef]
- Vergara, D.; Martignago, R.; Bonsegna, S.; De Nuccio, F.; Santino, A.; Nicolardi, G.; Maffia, M. IFN-beta reverses the lipopolysaccharide-induced proteome modifications in treated astrocytes. J. Neuroimmunol. 2010, 221, 115–120. [Google Scholar] [CrossRef]
- Clarke, P.; Zhuang, Y.; Berens, H.M.; Leser, J.S.; Tyler, K.L. Interferon Beta Contributes to Astrocyte Activation in the Brain following Reovirus Infection. J. Virol. 2019, 93. [Google Scholar] [CrossRef]
- Inacio, R.F.; Zanon, R.G.; Castro, M.V.; Souza, H.M.; Bajgelman, M.C.; Verinaud, L.; Oliveira, A.L. Astroglioma conditioned medium increases synaptic elimination and correlates with major histocompatibility complex of class I (MHC I) upregulation in PC12Cells. Neurosci. Lett. 2016, 634, 160–167. [Google Scholar] [CrossRef] [PubMed]
- Khorooshi, R.; Owens, T. Injury-induced type I IFN signaling regulates inflammatory responses in the central nervous system. J. Immunol. 2010, 185, 1258–1264. [Google Scholar] [CrossRef] [PubMed]
- Rizzo, M.D.; Crawford, R.B.; Bach, A.; Sermet, S.; Amalfitano, A.; Kaminski, N.E. Imiquimod and interferon-alpha augment monocyte-mediated astrocyte secretion of MCP-1, IL-6 and IP-10 in a human co-culture system. J. Neuroimmunol. 2019, 333, 576969. [Google Scholar] [CrossRef] [PubMed]
- Barca, O.; Costoya, J.A.; Senaris, R.M.; Arce, V.M. Interferon-beta protects astrocytes against tumour necrosis factor-induced apoptosis via activation of p38 mitogen-activated protein kinase. Exp. Cell Res. 2008, 314, 2231–2237. [Google Scholar] [CrossRef] [PubMed]
- Barca, O.; Seoane, M.; Ferre, S.; Prieto, J.M.; Lema, M.; Senaris, R.; Arce, V.M. Mechanisms of interferon-beta-induced survival in fetal and neonatal primary astrocytes. Neuroimmunomodulation 2007, 14, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Barca, O.; Devesa-Peleteiro, P.; Seoane, M.; Senaris, R.M.; Arce, V.M. Bimodal effect of interferon-beta on astrocyte proliferation and survival: Importance of nuclear factor-kappaB. J. Neuroimmunol. 2010, 226, 73–80. [Google Scholar] [CrossRef]
- Barca, O. Interferon beta promotes survival in primary astrocytes through phosphatidylinositol 3-kinase. J. Neuroimmunol. 2003, 139, 155–159. [Google Scholar] [CrossRef]
- Parry, A.; Corkill, R.; Blamire, A.M.; Palace, J.; Narayanan, S.; Arnold, D.; Styles, P.; Matthews, P.M. Beta-Interferon treatment does not always slow the progression of axonal injury in multiple sclerosis. J. Neurol. 2003, 250, 171–178. [Google Scholar] [CrossRef]
- Takeuchi, C.; Ota, K.; Ono, Y.; Iwata, M. Interferon Beta-1b may reverse axonal dysfunction in multiple sclerosis. Neuroradiol. J. 2007, 20, 531–540. [Google Scholar] [CrossRef]
- Narayanan, S.; De Stefano, N.; Francis, G.S.; Arnaoutelis, R.; Caramanos, Z.; Collins, D.L.; Pelletier, D.; Arnason, B.G.W.; Antel, J.P.; Arnold, D.L. Axonal metabolic recovery in multiple sclerosis patients treated with interferon beta-1b. J. Neurol. 2001, 248, 979–986. [Google Scholar] [CrossRef]
- Valeria, R.; Luisa, S.; Adele, M.; Stefania, B.; Fabio, T.; Nicoletta, B.; Carmine, P.M.; Silvia, A. Changes in the NMR Metabolic Profile of Live Human Neuron-Like SH-SY5Y Cells Exposed to Interferon-alpha2. J. Neuroimmune. Pharmacol. 2016, 11, 142–152. [Google Scholar] [CrossRef]
- Low-Calle, A.M.; Prada-Arismendy, J.; Castellanos, J.E. Study of interferon-beta antiviral activity against Herpes simplex virus type 1 in neuron-enriched trigeminal ganglia cultures. Virus Res. 2014, 180, 49–58. [Google Scholar] [CrossRef] [PubMed]
- Winkler, C.W.; Woods, T.A.; Groveman, B.R.; Carmody, A.B.; Speranza, E.E.; Martens, C.A.; Best, S.M.; Haigh, C.L.; Peterson, K.E. Neuronal maturation reduces the type I IFN response to orthobunyavirus infection and leads to increased apoptosis of human neurons. J. Neuroinflammation 2019, 16, 229. [Google Scholar] [CrossRef] [PubMed]
- Kreit, M.; Paul, S.; Knoops, L.; De Cock, A.; Sorgeloos, F.; Michiels, T. Inefficient type I interferon-mediated antiviral protection of primary mouse neurons is associated with the lack of apolipoprotein l9 expression. J. Virol. 2014, 88, 3874–3884. [Google Scholar] [CrossRef] [PubMed]
- Nakashima, T.; Hori, T.; Kuriyama, K.; Kiyohara, T. Naloxone blocks the interferon-α induced changes in hypothalamic neuronal activity. Neurosci. Lett. 1987, 82, 332–336. [Google Scholar] [CrossRef]
- Inacio, R.F.; Zanon, R.G.; Verinaud, L.; de Oliveira, A.L. Interferon beta modulates major histocompatibility complex class I (MHC I) and CD3-zeta expression in PC12 cells. Neurosci. Lett. 2012, 513, 223–228. [Google Scholar] [CrossRef]
- Lafaille, F.G.; Harschnitz, O.; Lee, Y.S.; Zhang, P.; Hasek, M.L.; Kerner, G.; Itan, Y.; Ewaleifoh, O.; Rapaport, F.; Carlile, T.M.; et al. Human SNORA31 variations impair cortical neuron-intrinsic immunity to HSV-1 and underlie herpes simplex encephalitis. Nat. Med. 2019, 25, 1873–1884. [Google Scholar] [CrossRef] [PubMed]
- Dumitrascu, O.M.; Mott, K.R.; Ghiasi, H. A comparative study of experimental mouse models of central nervous system demyelination. Gene. Ther. 2014, 21, 599–608. [Google Scholar] [CrossRef][Green Version]
- Kotsiari, A.; Voss, E.V.; Pul, R.; Skripuletz, T.; Ragancokova, D.; Trebst, C.; Stangel, M. Interferon-beta treatment normalises the inhibitory effect of serum from multiple sclerosis patients on oligodendrocyte progenitor proliferation. Neurosci. Lett. 2010, 485, 107–111. [Google Scholar] [CrossRef]
- Heine, S.; Ebnet, J.; Maysami, S.; Stangel, M. Effects of interferon-beta on oligodendroglial cells. J. Neuroimmunol. 2006, 177, 173–180. [Google Scholar] [CrossRef]
- Penton-Rol, G.; Lagumersindez-Denis, N.; Muzio, L.; Bergami, A.; Furlan, R.; Fernandez-Masso, J.R.; Nazabal-Galvez, M.; Llopiz-Arzuaga, A.; Herrera-Rolo, T.; Veliz-Rodriguez, T.; et al. Comparative Neuroregenerative Effects of C-Phycocyanin and IFN-Beta in a Model of Multiple Sclerosis in Mice. J. Neuroimmune. Pharmacol. 2016, 11, 153–167. [Google Scholar] [CrossRef] [PubMed]
- Miyamoto, N.; Maki, T.; Pham, L.D.; Hayakawa, K.; Seo, J.H.; Mandeville, E.T.; Mandeville, J.B.; Kim, K.W.; Lo, E.H.; Arai, K. Oxidative stress interferes with white matter renewal after prolonged cerebral hypoperfusion in mice. Stroke 2013, 44, 3516–3521. [Google Scholar] [CrossRef] [PubMed]
- Bar-Or, A.; Pachner, A.; Menguy-Vacheron, F.; Kaplan, J.; Wiendl, H. Teriflunomide and its mechanism of action in multiple sclerosis. Drugs 2014, 74, 659–674. [Google Scholar] [CrossRef] [PubMed]
- Lu, Z.; Zhang, D.; Cui, K.; Fu, X.; Man, J.; Lu, H.; Yu, L.; Gao, Y.; Liu, X.; Liao, L.; et al. Neuroprotective Action of Teriflunomide in a Mouse Model of Transient Middle Cerebral Artery Occlusion. Neuroscience 2020, 428, 228–241. [Google Scholar] [CrossRef] [PubMed]
- Rzagalinski, I.; Hainz, N.; Meier, C.; Tschernig, T.; Volmer, D.A. Spatial and molecular changes of mouse brain metabolism in response to immunomodulatory treatment with teriflunomide as visualized by MALDI-MSI. Anal. Bioanal. Chem. 2019, 411, 353–365. [Google Scholar] [CrossRef]
- Prabhakara, K.S.; Kota, D.J.; Jones, G.H.; Srivastava, A.K.; Cox, C.S., Jr.; Olson, S.D. Teriflunomide Modulates Vascular Permeability and Microglial Activation after Experimental Traumatic Brain Injury. Mol. Ther. 2018, 26, 2152–2162. [Google Scholar] [CrossRef]
- Pol, S.; Sveinsson, M.; Sudyn, M.; Babek, N.; Siebert, D.; Bertolino, N.; Modica, C.M.; Preda, M.; Schweser, F.; Zivadinov, R. Teriflunomide’s Effect on Glia in Experimental Demyelinating Disease: A Neuroimaging and Histologic Study. J. Neuroimaging 2019, 29, 52–61. [Google Scholar] [CrossRef]
- Wostradowski, T.; Prajeeth, C.K.; Gudi, V.; Kronenberg, J.; Witte, S.; Brieskorn, M.; Stangel, M. In vitro evaluation of physiologically relevant concentrations of teriflunomide on activation and proliferation of primary rodent microglia. J. Neuroinflammation 2016, 13, 250. [Google Scholar] [CrossRef]
- Gottle, P.; Manousi, A.; Kremer, D.; Reiche, L.; Hartung, H.P.; Kury, P. Teriflunomide promotes oligodendroglial differentiation and myelination. J. Neuroinflammation 2018, 15, 76. [Google Scholar] [CrossRef]
- Varrin-Doyer, M.; Pekarek, K.L.; Spencer, C.M.; Bernard, C.C.; Sobel, R.A.; Cree, B.A.; Schulze-Topphoff, U.; Zamvil, S.S. Treatment of spontaneous EAE by laquinimod reduces Tfh, B cell aggregates, and disease progression. Neurol. Neuroimmunol. Neuroinflamm. 2016, 3, e272. [Google Scholar] [CrossRef]
- Wilmes, A.T.; Reinehr, S.; Kuhn, S.; Pedreiturria, X.; Petrikowski, L.; Faissner, S.; Ayzenberg, I.; Stute, G.; Gold, R.; Dick, H.B.; et al. Laquinimod protects the optic nerve and retina in an experimental autoimmune encephalomyelitis model. J. Neuroinflammation 2018, 15, 183. [Google Scholar] [CrossRef] [PubMed]
- Kaye, J.; Piryatinsky, V.; Birnberg, T.; Hingaly, T.; Raymond, E.; Kashi, R.; Amit-Romach, E.; Caballero, I.S.; Towfic, F.; Ator, M.A.; et al. Laquinimod arrests experimental autoimmune encephalomyelitis by activating the aryl hydrocarbon receptor. Proc. Natl. Acad. Sci. USA 2016, 113, E6145–E6152. [Google Scholar] [CrossRef] [PubMed]
- Mishra, M.K.; Wang, J.; Keough, M.B.; Fan, Y.; Silva, C.; Sloka, S.; Hayardeny, L.; Bruck, W.; Yong, V.W. Laquinimod reduces neuroaxonal injury through inhibiting microglial activation. Ann. Clin. Transl. Neurol. 2014, 1, 409–422. [Google Scholar] [CrossRef] [PubMed]
- Nyamoya, S.; Steinle, J.; Chrzanowski, U.; Kaye, J.; Schmitz, C.; Beyer, C.; Kipp, M. Laquinimod Supports Remyelination in Non-Supportive Environments. Cells 2019, 8, 1363. [Google Scholar] [CrossRef]
- Nedelcu, J.; Reinbach, C.; Riedler, P.; Brendel, M.; Rominger, A.; Kaye, J.; Behrangi, N.; Jiangshan, Z.; Schmitz, C.; Kipp, M. Laquinimod ameliorates secondary brain inflammation. Neurobiol. Dis. 2020, 134, 104675. [Google Scholar] [CrossRef]
- Moore, S.; Khalaj, A.J.; Yoon, J.; Patel, R.; Hannsun, G.; Yoo, T.; Sasidhar, M.; Martinez-Torres, L.; Hayardeny, L.; Tiwari-Woodruff, S.K. Therapeutic laquinimod treatment decreases inflammation, initiates axon remyelination, and improves motor deficit in a mouse model of multiple sclerosis. Brain Behav. 2013, 3, 664–682. [Google Scholar] [CrossRef]
- Kramann, N.; Menken, L.; Hayardeny, L.; Hanisch, U.K.; Bruck, W. Laquinimod prevents cuprizone-induced demyelination independent of Toll-like receptor signaling. Neurol. Neuroimmunol. Neuroinflamm. 2016, 3, e233. [Google Scholar] [CrossRef]
- Bruck, W.; Pfortner, R.; Pham, T.; Zhang, J.; Hayardeny, L.; Piryatinsky, V.; Hanisch, U.K.; Regen, T.; van Rossum, D.; Brakelmann, L.; et al. Reduced astrocytic NF-kappaB activation by laquinimod protects from cuprizone-induced demyelination. Acta. Neuropathol. 2012, 124, 411–424. [Google Scholar] [CrossRef]
- Ruffini, F.; Rossi, S.; Bergamaschi, A.; Brambilla, E.; Finardi, A.; Motta, C.; Studer, V.; Barbieri, F.; De Chiara, V.; Hayardeny, L.; et al. Laquinimod prevents inflammation-induced synaptic alterations occurring in experimental autoimmune encephalomyelitis. Mult. Scler. 2013, 19, 1084–1094. [Google Scholar] [CrossRef]
- Beckers, L.; Ory, D.; Geric, I.; Declercq, L.; Koole, M.; Kassiou, M.; Bormans, G.; Baes, M. Increased Expression of Translocator Protein (TSPO) Marks Pro-inflammatory Microglia but Does Not Predict Neurodegeneration. Mol. Imaging Biol. 2018, 20, 94–102. [Google Scholar] [CrossRef]
- Katsumoto, A.; Miranda, A.S.; Butovsky, O.; Teixeira, A.L.; Ransohoff, R.M.; Lamb, B.T. Laquinimod attenuates inflammation by modulating macrophage functions in traumatic brain injury mouse model. J. Neuroinflammation 2018, 15, 26. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Hong, W.; Wang, X.; Zhang, P.; Korner, H.; Tu, J.; Wei, W. MicroRNAs in Microglia: How do MicroRNAs Affect Activation, Inflammation, Polarization of Microglia and Mediate the Interaction Between Microglia and Glioma? Front Mol. Neurosci. 2019, 12, 125. [Google Scholar] [CrossRef] [PubMed]
- Kelland, E.E.; Gilmore, W.; Hayardeny, L.; Weiner, L.P.; Lund, B.T. In vitro assessment of the direct effect of laquinimod on basic functions of human neural stem cells and oligodendrocyte progenitor cells. J. Neurol. Sci. 2014, 346, 66–74. [Google Scholar] [CrossRef]
- Pittaluga, A. CCL5-Glutamate Cross-Talk in Astrocyte-Neuron Communication in Multiple Sclerosis. Front. Immunol. 2017, 8, 1079. [Google Scholar] [CrossRef] [PubMed]
- Ellrichmann, G.; Blusch, A.; Fatoba, O.; Brunner, J.; Reick, C.; Hayardeny, L.; Hayden, M.; Sehr, D.; Winklhofer, K.F.; Saft, C.; et al. Laquinimod treatment in the R6/2 mouse model. Sci. Rep. 2017, 7, 4947. [Google Scholar] [CrossRef] [PubMed]
- Ehrnhoefer, D.E.; Caron, N.S.; Deng, Y.; Qiu, X.; Tsang, M.; Hayden, M.R. Laquinimod decreases Bax expression and reduces caspase-6 activation in neurons. Exp. Neurol. 2016, 283, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Gil-Ad, I.; Amit, B.H.; Hayardeni, L.; Tarasenko, I.; Taler, M.; Gueta, R.U.; Weizman, A. Effects of the anti-multiple sclerosis immunomodulator laquinimod on anxiety and depression in rodent behavioral models. J. Mol. Neurosci. 2015, 55, 552–560. [Google Scholar] [CrossRef]
- Stassart, R.M.; Helms, G.; Garea-Rodriguez, E.; Nessler, S.; Hayardeny, L.; Wegner, C.; Schlumbohm, C.; Fuchs, E.; Bruck, W. A New Targeted Model of Experimental Autoimmune Encephalomyelitis in the Common Marmoset. Brain Pathol. 2016, 26, 452–464. [Google Scholar] [CrossRef]
- Lehotzky, A.; Lau, P.; Tokesi, N.; Muja, N.; Hudson, L.D.; Ovadi, J. Tubulin polymerization-promoting protein (TPPP/p25) is critical for oligodendrocyte differentiation. Glia 2010, 58, 157–168. [Google Scholar] [CrossRef]
- Oh, J.; O’Connor, P.W. Established disease-modifying treatments in relapsing-remitting multiple sclerosis. Curr. Opin. Neurol. 2015, 28, 220–229. [Google Scholar] [CrossRef]
- Rodi, M.; Dimisianos, N.; de Lastic, A.L.; Sakellaraki, P.; Deraos, G.; Matsoukas, J.; Papathanasopoulos, P.; Mouzaki, A. Regulatory Cell Populations in Relapsing-Remitting Multiple Sclerosis (RRMS) Patients: Effect of Disease Activity and Treatment Regimens. Int. J. Mol. Sci. 2016, 17, 1398. [Google Scholar] [CrossRef] [PubMed]
- Banisadr, G.; Schwartz, S.R.; Podojil, J.R.; Piccinini, L.A.; Lanker, S.; Miller, S.D.; Miller, R.J. Integrin/Chemokine receptor interactions in the pathogenesis of experimental autoimmune encephalomyelitis. J. Neuroimmune. Pharmacol. 2014, 9, 438–445. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Escribano, B.M.; Medina-Fernandez, F.J.; Aguilar-Luque, M.; Aguera, E.; Feijoo, M.; Garcia-Maceira, F.I.; Lillo, R.; Vieyra-Reyes, P.; Giraldo, A.I.; Luque, E.; et al. Lipopolysaccharide Binding Protein and Oxidative Stress in a Multiple Sclerosis Model. Neurotherapeutics 2017, 14, 199–211. [Google Scholar] [CrossRef] [PubMed]
- Manocha, G.; Ghatak, A.; Puig, K.; Combs, C. Anti-alpha4beta1 Integrin Antibodies Attenuated Brain Inflammatory Changes in a Mouse Model of Alzheimer’s Disease. Curr. Alzheimer Res. 2018, 15, 1123–1135. [Google Scholar] [CrossRef]
- Mindur, J.E.; Ito, N.; Dhib-Jalbut, S.; Ito, K. Early treatment with anti-VLA-4 mAb can prevent the infiltration and/or development of pathogenic CD11b+CD4+ T cells in the CNS during progressive EAE. PLoS ONE 2014, 9, e99068. [Google Scholar] [CrossRef]
- Politis, M.; Giannetti, P.; Niccolini, F.; Su, P.; Turkheimer, F.; Waldman, A.; Reynolds, R.; Nicholas, R.; Piccini, P. Decreased Microglial Activation Precedes Stabilization of Disability in Multiple Sclerosis Patients Treated with Natalizumab (S21.004). Neurology 2013, 80, S21.004. [Google Scholar]
- Sucksdorff, M.; Tuisku, J.; Matilainen, M.; Vuorimaa, A.; Smith, S.; Keitila, J.; Rokka, J.; Parkkola, R.; Nylund, M.; Rinne, J.; et al. Natalizumab treatment reduces microglial activation in the white matter of the MS brain. Neurol. Neuroimmunol. Neuroinflamm. 2019, 6, e574. [Google Scholar] [CrossRef]
- Ohrfelt, A.; Axelsson, M.; Malmestrom, C.; Novakova, L.; Heslegrave, A.; Blennow, K.; Lycke, J.; Zetterberg, H. Soluble TREM-2 in cerebrospinal fluid from patients with multiple sclerosis treated with natalizumab or mitoxantrone. Mult. Scler. 2016, 22, 1587–1595. [Google Scholar] [CrossRef]
- Olsson, B.; Malmestrom, C.; Basun, H.; Annas, P.; Hoglund, K.; Lannfelt, L.; Andreasen, N.; Zetterberg, H.; Blennow, K. Extreme stability of chitotriosidase in cerebrospinal fluid makes it a suitable marker for microglial activation in clinical trials. J. Alzheimers Dis. 2012, 32, 273–276. [Google Scholar] [CrossRef]
- Falcon, C.; Monte-Rubio, G.C.; Grau-Rivera, O.; Suarez-Calvet, M.; Sanchez-Valle, R.; Rami, L.; Bosch, B.; Haass, C.; Gispert, J.D.; Molinuevo, J.L. CSF glial biomarkers YKL40 and sTREM2 are associated with longitudinal volume and diffusivity changes in cognitively unimpaired individuals. Neuroimage Clin. 2019, 23, 101801. [Google Scholar] [CrossRef]
- Martinez-Merino, L.; Iridoy, M.; Galbete, A.; Roldan, M.; Rivero, A.; Acha, B.; Irun, P.; Canosa, C.; Pocovi, M.; Mendioroz, M.; et al. Evaluation of Chitotriosidase and CC-Chemokine Ligand 18 as Biomarkers of Microglia Activation in Amyotrophic Lateral Sclerosis. Neurodegener Dis. 2018, 18, 208–215. [Google Scholar] [CrossRef] [PubMed]
- Hailer, N.P.; Bechmann, I.; Heizmann, S.; Nitsch, R. Adhesion molecule expression on phagocytic microglial cells following anterograde degeneration of perforant path axons. Hippocampus 1997, 7, 341–349. [Google Scholar] [CrossRef]
- Lee, S.; Jha, M.K.; Suk, K. Lipocalin-2 in the Inflammatory Activation of Brain Astrocytes. Crit. Rev. Immunol. 2015, 35, 77–84. [Google Scholar] [CrossRef] [PubMed]
- Chun, B.Y.; Kim, J.H.; Nam, Y.; Huh, M.I.; Han, S.; Suk, K. Pathological Involvement of Astrocyte-Derived Lipocalin-2 in the Demyelinating Optic Neuritis. Investig. Ophthalmol. Vis. Sci. 2015, 56, 3691–3698. [Google Scholar] [CrossRef] [PubMed]
- Marques, F.; Mesquita, S.D.; Sousa, J.C.; Coppola, G.; Gao, F.; Geschwind, D.H.; Columba-Cabezas, S.; Aloisi, F.; Degn, M.; Cerqueira, J.J.; et al. Lipocalin 2 is present in the EAE brain and is modulated by natalizumab. Front Cell Neurosci. 2012, 6, 33. [Google Scholar] [CrossRef] [PubMed]
- Al Nimer, F.; Elliott, C.; Bergman, J.; Khademi, M.; Dring, A.M.; Aeinehband, S.; Bergenheim, T.; Romme Christensen, J.; Sellebjerg, F.; Svenningsson, A.; et al. Lipocalin-2 is increased in progressive multiple sclerosis and inhibits remyelination. Neurol. Neuroimmunol. Neuroinflamm. 2016, 3, e191. [Google Scholar] [CrossRef]
- Hu, Y.; Turner, M.J.; Shields, J.; Gale, M.S.; Hutto, E.; Roberts, B.L.; Siders, W.M.; Kaplan, J.M. Investigation of the mechanism of action of alemtuzumab in a human CD52 transgenic mouse model. Immunology 2009, 128, 260–270. [Google Scholar] [CrossRef]
- Rao, S.P.; Sancho, J.; Campos-Rivera, J.; Boutin, P.M.; Severy, P.B.; Weeden, T.; Shankara, S.; Roberts, B.L.; Kaplan, J.M. Human peripheral blood mononuclear cells exhibit heterogeneous CD52 expression levels and show differential sensitivity to alemtuzumab mediated cytolysis. PLoS ONE 2012, 7, e39416. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, T.; Masuyama, J.; Sohma, Y.; Inazawa, H.; Horie, K.; Kojima, K.; Uemura, Y.; Aoki, Y.; Kaga, S.; Minota, S.; et al. CD52 is a novel costimulatory molecule for induction of CD4+ regulatory T cells. Clin. Immunol. 2006, 120, 247–259. [Google Scholar] [CrossRef]
- Chatterjee, D.; Addya, S.; Khan, R.S.; Kenyon, L.C.; Choe, A.; Cohrs, R.J.; Shindler, K.S.; Sarma, J.D. Mouse hepatitis virus infection upregulates genes involved in innate immune responses. PLoS ONE 2014, 9, e111351. [Google Scholar] [CrossRef]
- Ellwardt, E.; Vogelaar, C.F.; Maldet, C.; Schmaul, S.; Bittner, S.; Luchtman, D. Targeting CD52 does not affect murine neuron and microglia function. Eur. J. Pharmacol. 2020, 871, 172923. [Google Scholar] [CrossRef] [PubMed]
- Knier, B.; Hemmer, B.; Korn, T. Novel monoclonal antibodies for therapy of multiple sclerosis. Expert Opin Biol Ther 2014, 14, 503–513. [Google Scholar] [CrossRef] [PubMed]
- Milo, R. Therapeutic strategies targeting B-cells in multiple sclerosis. Autoimmun. Rev. 2016, 15, 714–718. [Google Scholar] [CrossRef] [PubMed]
- Moreno Torres, I.; Garcia-Merino, A. Anti-CD20 monoclonal antibodies in multiple sclerosis. Expert. Rev. Neurother. 2017, 17, 359–371. [Google Scholar] [CrossRef]
- Hausler, D.; Hausser-Kinzel, S.; Feldmann, L.; Torke, S.; Lepennetier, G.; Bernard, C.C.A.; Zamvil, S.S.; Bruck, W.; Lehmann-Horn, K.; Weber, M.S. Functional characterization of reappearing B cells after anti-CD20 treatment of CNS autoimmune disease. Proc. Natl. Acad. Sci. USA 2018, 115, 9773–9778. [Google Scholar] [CrossRef]
- Szepesi, Z.; Manouchehrian, O.; Bachiller, S.; Deierborg, T. Bidirectional Microglia-Neuron Communication in Health and Disease. Front Cell Neurosci. 2018, 12, 323. [Google Scholar] [CrossRef]
- Domingues, H.S.; Portugal, C.C.; Socodato, R.; Relvas, J.B. Oligodendrocyte, Astrocyte, and Microglia Crosstalk in Myelin Development, Damage, and Repair. Front Cell Dev. Biol. 2016, 4, 71. [Google Scholar] [CrossRef]
- Przanowski, P.; Dabrowski, M.; Ellert-Miklaszewska, A.; Kloss, M.; Mieczkowski, J.; Kaza, B.; Ronowicz, A.; Hu, F.; Piotrowski, A.; Kettenmann, H.; et al. The signal transducers Stat1 and Stat3 and their novel target Jmjd3 drive the expression of inflammatory genes in microglia. J. Mol. Med. (Berl) 2014, 92, 239–254. [Google Scholar] [CrossRef]
- Liu, T.; Zhang, L.; Joo, D.; Sun, S.C. NF-kappaB signaling in inflammation. Signal Transduct Target Ther. 2017, 2. [Google Scholar] [CrossRef]
- Mussbacher, M.; Salzmann, M.; Brostjan, C.; Hoesel, B.; Schoergenhofer, C.; Datler, H.; Hohensinner, P.; Basilio, J.; Petzelbauer, P.; Assinger, A.; et al. Cell Type-Specific Roles of NF-kappaB Linking Inflammation and Thrombosis. Front Immunol. 2019, 10, 85. [Google Scholar] [CrossRef]
- Kramer, O.H.; Baus, D.; Knauer, S.K.; Stein, S.; Jager, E.; Stauber, R.H.; Grez, M.; Pfitzner, E.; Heinzel, T. Acetylation of Stat1 modulates NF-kappaB activity. Genes Dev. 2006, 20, 473–485. [Google Scholar] [CrossRef] [PubMed]
- Yao, L.; Kan, E.M.; Lu, J.; Hao, A.; Dheen, S.T.; Kaur, C.; Ling, E.A. Toll-like receptor 4 mediates microglial activation and production of inflammatory mediators in neonatal rat brain following hypoxia: Role of TLR4 in hypoxic microglia. J. Neuroinflammation 2013, 10, 23. [Google Scholar] [CrossRef] [PubMed]
- Song, M.; Jin, J.; Lim, J.E.; Kou, J.; Pattanayak, A.; Rehman, J.A.; Kim, H.D.; Tahara, K.; Lalonde, R.; Fukuchi, K. TLR4 mutation reduces microglial activation, increases Abeta deposits and exacerbates cognitive deficits in a mouse model of Alzheimer’s disease. J. Neuroinflammation 2011, 8, 92. [Google Scholar] [CrossRef] [PubMed]
- Akhmetzyanova, E.; Kletenkov, K.; Mukhamedshina, Y.; Rizvanov, A. Different Approaches to Modulation of Microglia Phenotypes After Spinal Cord Injury. Front Syst. Neurosci. 2019, 13, 37. [Google Scholar] [CrossRef]
- Ceyzeriat, K.; Ben Haim, L.; Denizot, A.; Pommier, D.; Matos, M.; Guillemaud, O.; Palomares, M.A.; Abjean, L.; Petit, F.; Gipchtein, P.; et al. Modulation of astrocyte reactivity improves functional deficits in mouse models of Alzheimer’s disease. Acta Neuropathol. Commun. 2018, 6, 104. [Google Scholar] [CrossRef]
- Nutma, E.; van Gent, D.; Amor, S.; Peferoen, L.A.N. Astrocyte and Oligodendrocyte Cross-Talk in the Central Nervous System. Cells 2020, 9, 600. [Google Scholar] [CrossRef]
- Allen, N.J.; Eroglu, C. Cell Biology of Astrocyte-Synapse Interactions. Neuron 2017, 96, 697–708. [Google Scholar] [CrossRef]
- Peferoen, L.; Kipp, M.; van der Valk, P.; van Noort, J.M.; Amor, S. Oligodendrocyte-microglia cross-talk in the central nervous system. Immunology 2014, 141, 302–313. [Google Scholar] [CrossRef]
- Oksanen, M.; Lehtonen, S.; Jaronen, M.; Goldsteins, G.; Hamalainen, R.H.; Koistinaho, J. Astrocyte alterations in neurodegenerative pathologies and their modeling in human induced pluripotent stem cell platforms. Cell Mol. Life Sci. 2019, 76, 2739–2760. [Google Scholar] [CrossRef]
- Jha, M.K.; Jo, M.; Kim, J.H.; Suk, K. Microglia-Astrocyte Crosstalk: An Intimate Molecular Conversation. Neuroscientist 2019, 25, 227–240. [Google Scholar] [CrossRef]
- Liddelow, S.A.; Guttenplan, K.A.; Clarke, L.E.; Bennett, F.C.; Bohlen, C.J.; Schirmer, L.; Bennett, M.L.; Munch, A.E.; Chung, W.S.; Peterson, T.C.; et al. Neurotoxic reactive astrocytes are induced by activated microglia. Nature 2017, 541, 481–487. [Google Scholar] [CrossRef] [PubMed]
- Rothhammer, V.; Borucki, D.M.; Tjon, E.C.; Takenaka, M.C.; Chao, C.C.; Ardura-Fabregat, A.; de Lima, K.A.; Gutierrez-Vazquez, C.; Hewson, P.; Staszewski, O.; et al. Microglial control of astrocytes in response to microbial metabolites. Nature 2018, 557, 724–728. [Google Scholar] [CrossRef] [PubMed]
- Haruwaka, K.; Ikegami, A.; Tachibana, Y.; Ohno, N.; Konishi, H.; Hashimoto, A.; Matsumoto, M.; Kato, D.; Ono, R.; Kiyama, H.; et al. Dual microglia effects on blood brain barrier permeability induced by systemic inflammation. Nat. Commun. 2019, 10, 5816. [Google Scholar] [CrossRef] [PubMed]
- Friedman, B.A.; Srinivasan, K.; Ayalon, G.; Meilandt, W.J.; Lin, H.; Huntley, M.A.; Cao, Y.; Lee, S.H.; Haddick, P.C.G.; Ngu, H.; et al. Diverse Brain Myeloid Expression Profiles Reveal Distinct Microglial Activation States and Aspects of Alzheimer’s Disease Not Evident in Mouse Models. Cell Rep. 2018, 22, 832–847. [Google Scholar] [CrossRef]
- van der Poel, M.; Ulas, T.; Mizee, M.R.; Hsiao, C.C.; Miedema, S.S.M.; Adelia; Schuurman, K.G.; Helder, B.; Tas, S.W.; Schultze, J.L.; et al. Transcriptional profiling of human microglia reveals grey-white matter heterogeneity and multiple sclerosis-associated changes. Nat. Commun. 2019, 10, 1139. [Google Scholar] [CrossRef]
- Lee, J.; Hamanaka, G.; Lo, E.H.; Arai, K. Heterogeneity of microglia and their differential roles in white matter pathology. CNS Neurosci. Ther. 2019, 25, 1290–1298. [Google Scholar] [CrossRef]
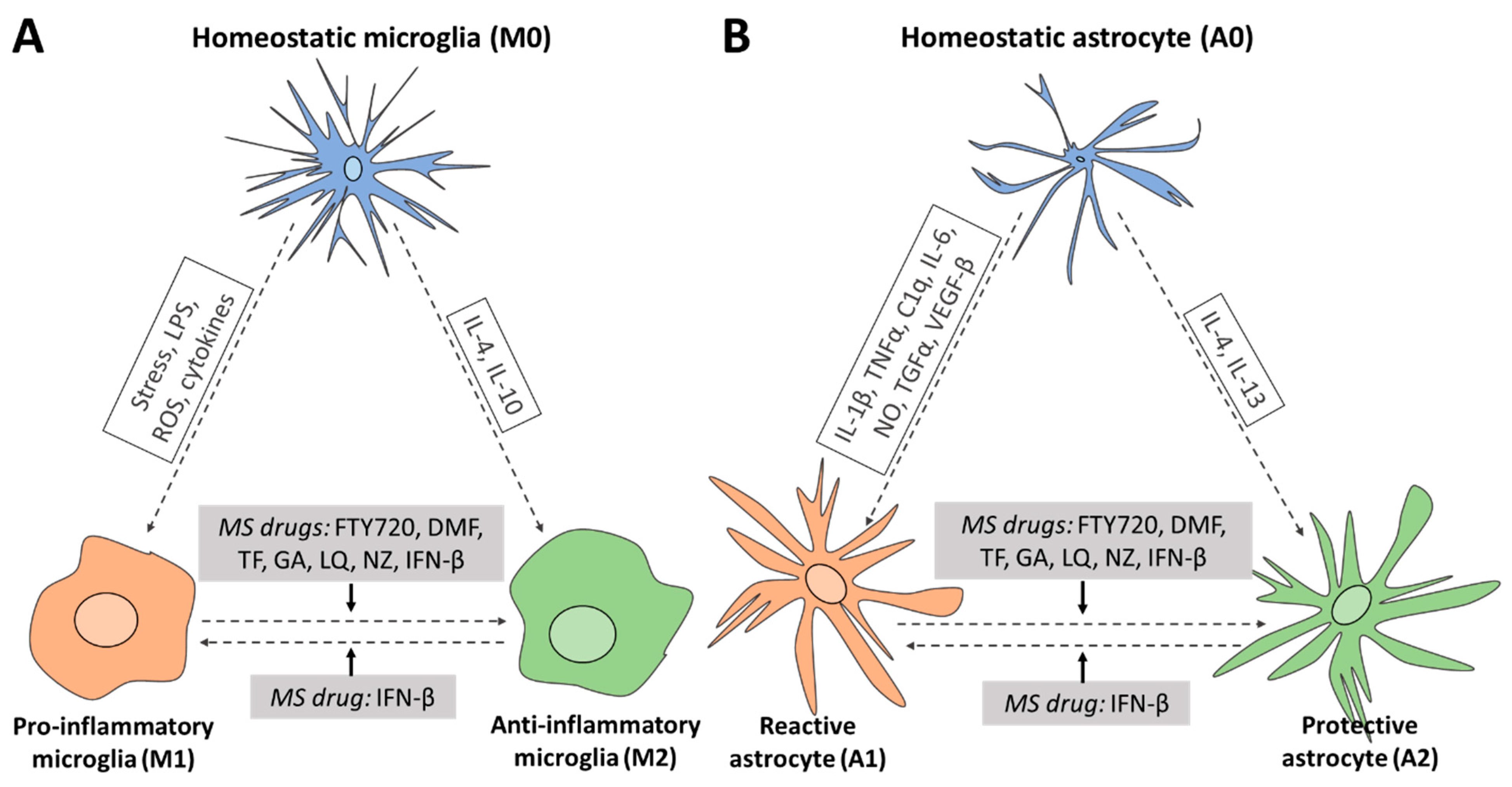
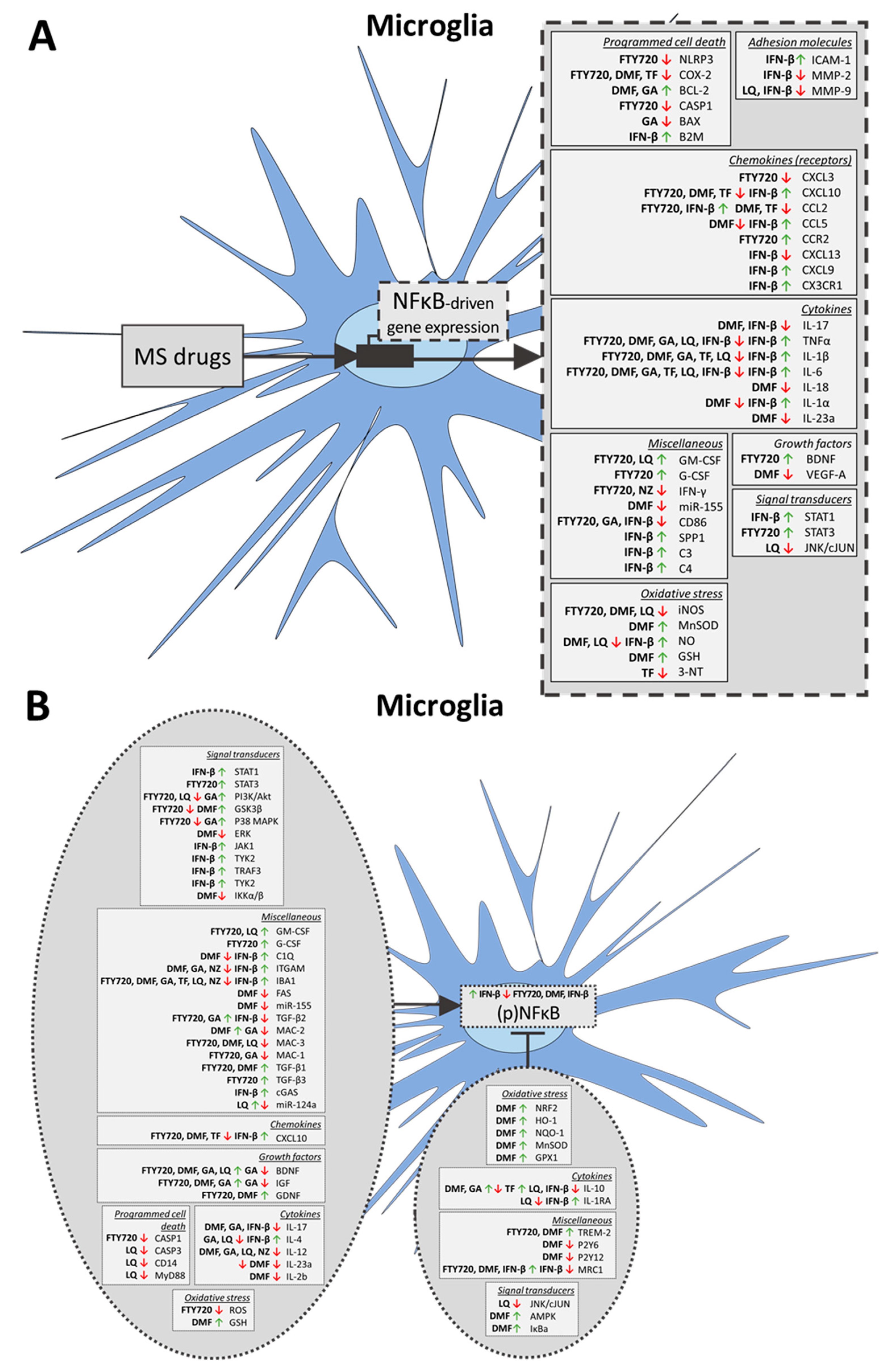
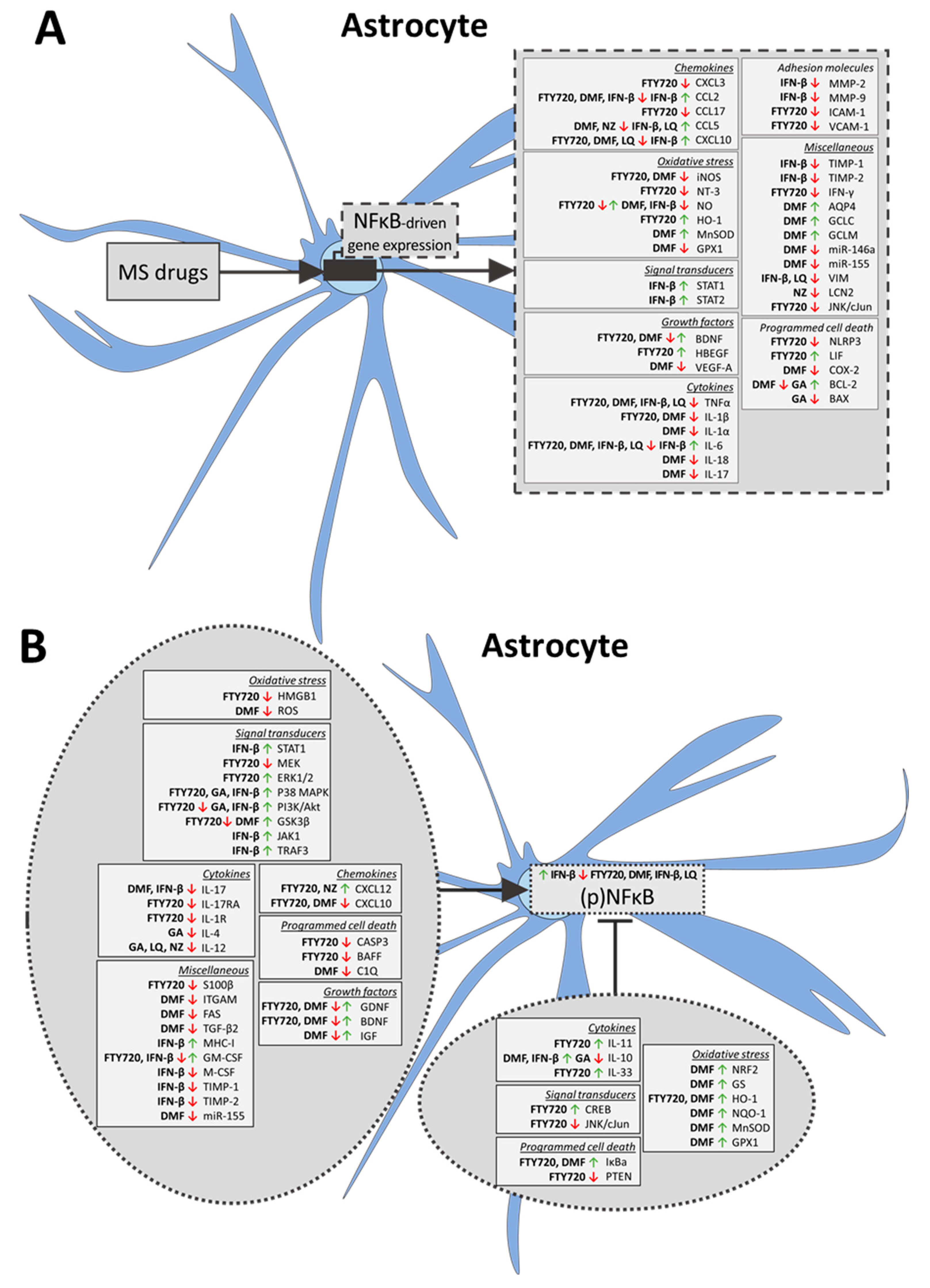
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Kleijn, K.M.A.; Martens, G.J.M. Molecular Effects of FDA-Approved Multiple Sclerosis Drugs on Glial Cells and Neurons of the Central Nervous System. Int. J. Mol. Sci. 2020, 21, 4229. https://doi.org/10.3390/ijms21124229
De Kleijn KMA, Martens GJM. Molecular Effects of FDA-Approved Multiple Sclerosis Drugs on Glial Cells and Neurons of the Central Nervous System. International Journal of Molecular Sciences. 2020; 21(12):4229. https://doi.org/10.3390/ijms21124229
Chicago/Turabian StyleDe Kleijn, Kim M. A., and Gerard J. M. Martens. 2020. "Molecular Effects of FDA-Approved Multiple Sclerosis Drugs on Glial Cells and Neurons of the Central Nervous System" International Journal of Molecular Sciences 21, no. 12: 4229. https://doi.org/10.3390/ijms21124229
APA StyleDe Kleijn, K. M. A., & Martens, G. J. M. (2020). Molecular Effects of FDA-Approved Multiple Sclerosis Drugs on Glial Cells and Neurons of the Central Nervous System. International Journal of Molecular Sciences, 21(12), 4229. https://doi.org/10.3390/ijms21124229





