Standardized Aronia melanocarpa Extract as Novel Supplement against Metabolic Syndrome: A Rat Model
Abstract
1. Introduction
2. Results
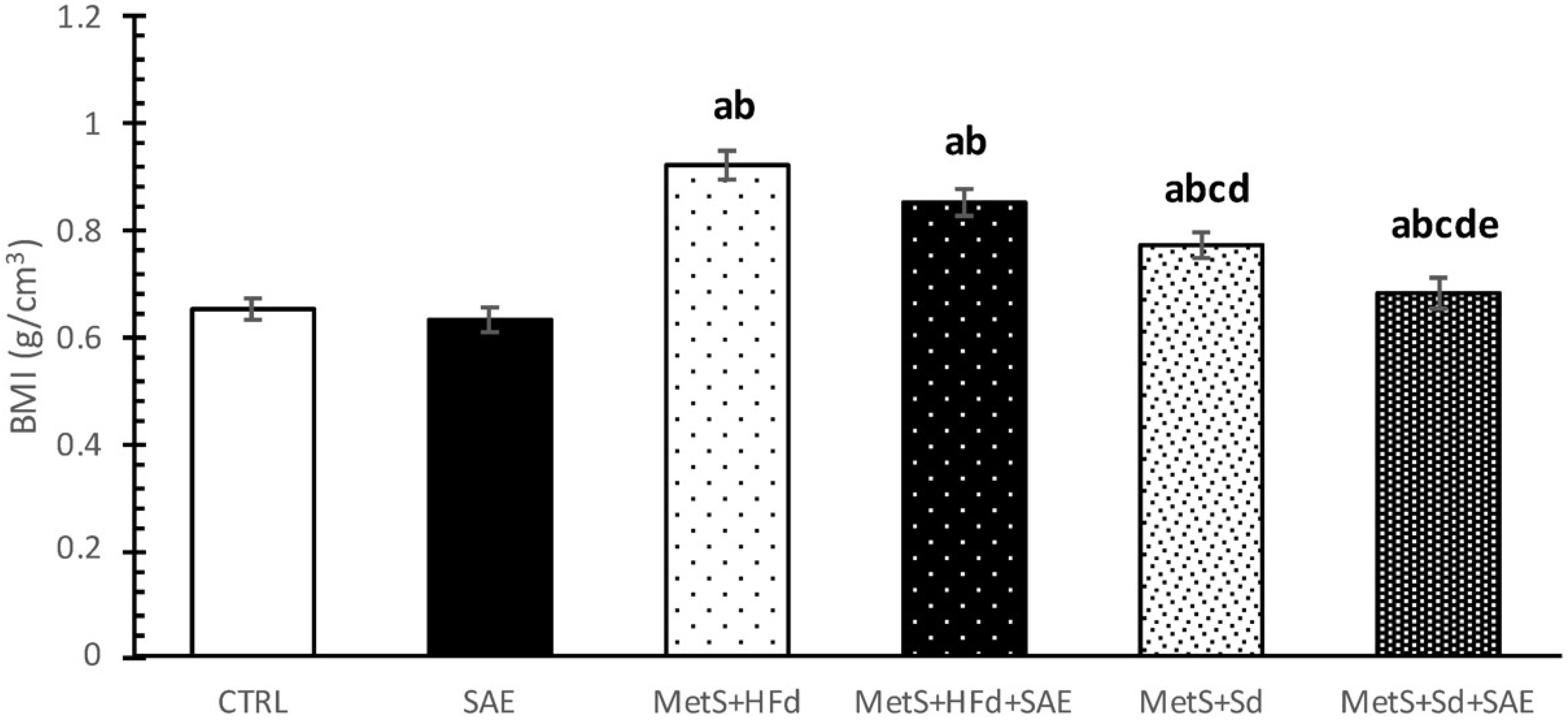
2.1. Body Mass Index (BMI) of Healthy and Rats with MetS after 4-Weeks of Dietary Changes
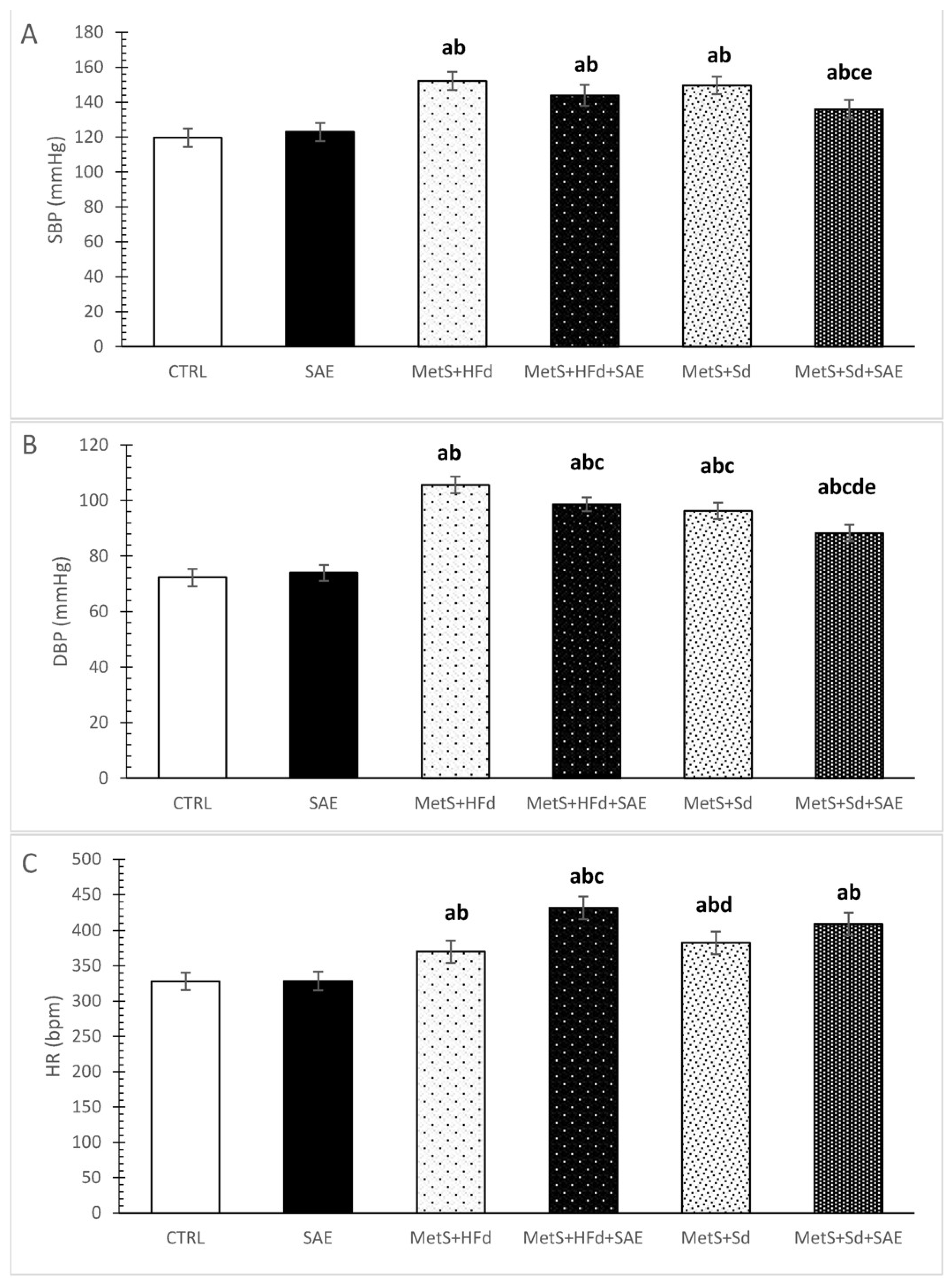
2.2. Changes in Blood Pressure and Heart Rate in Healthy and Rats with MetS on the Different Diet Regime
2.3. Effect of Dietary Changes in Healthy and Rats with MetS in In Vivo Cardiac Function
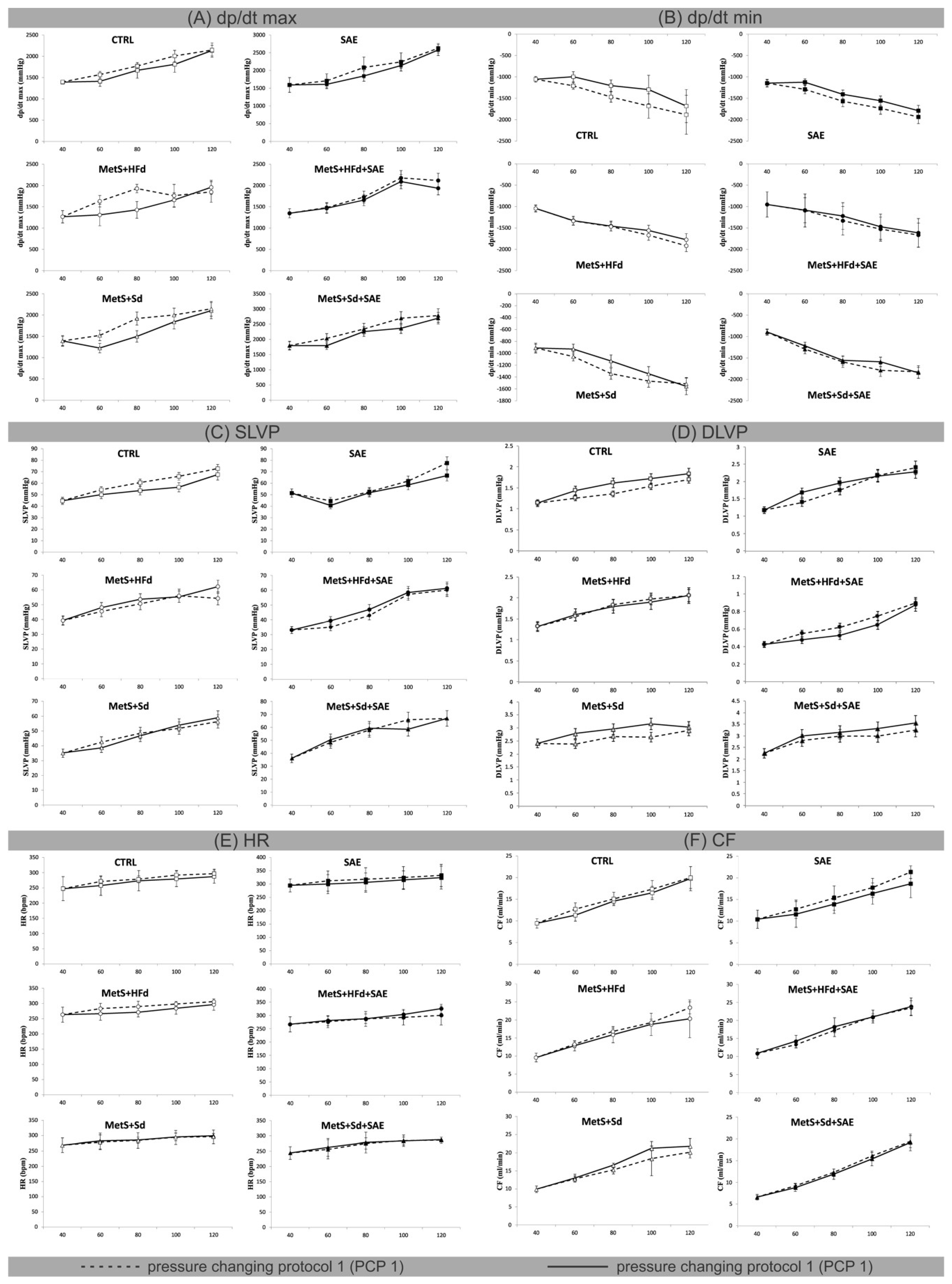
2.4. Effect of Dietary Changes in Healthy and Rats with MetS on Ex Vivo Cardiac Function
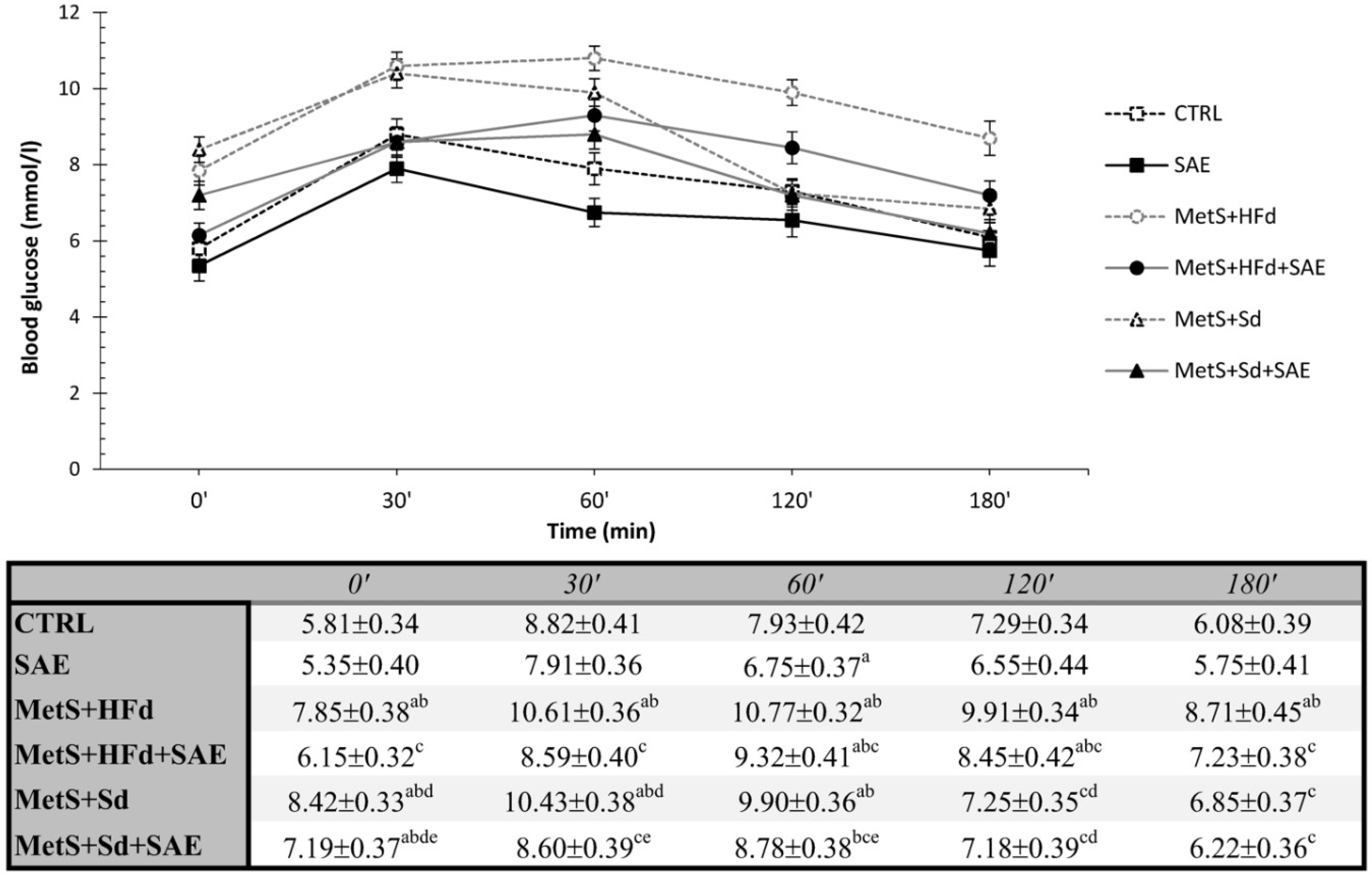
2.5. Effect of Dietary Changes in Healthy and Rats with MetS on Glucose and Insulin Levels during Oral Glucose Tolerance Test (OGTT)
2.5.1. Effects on Glucose Levels during OGTT
2.5.2. Effects on Insulin Levels during OGTT
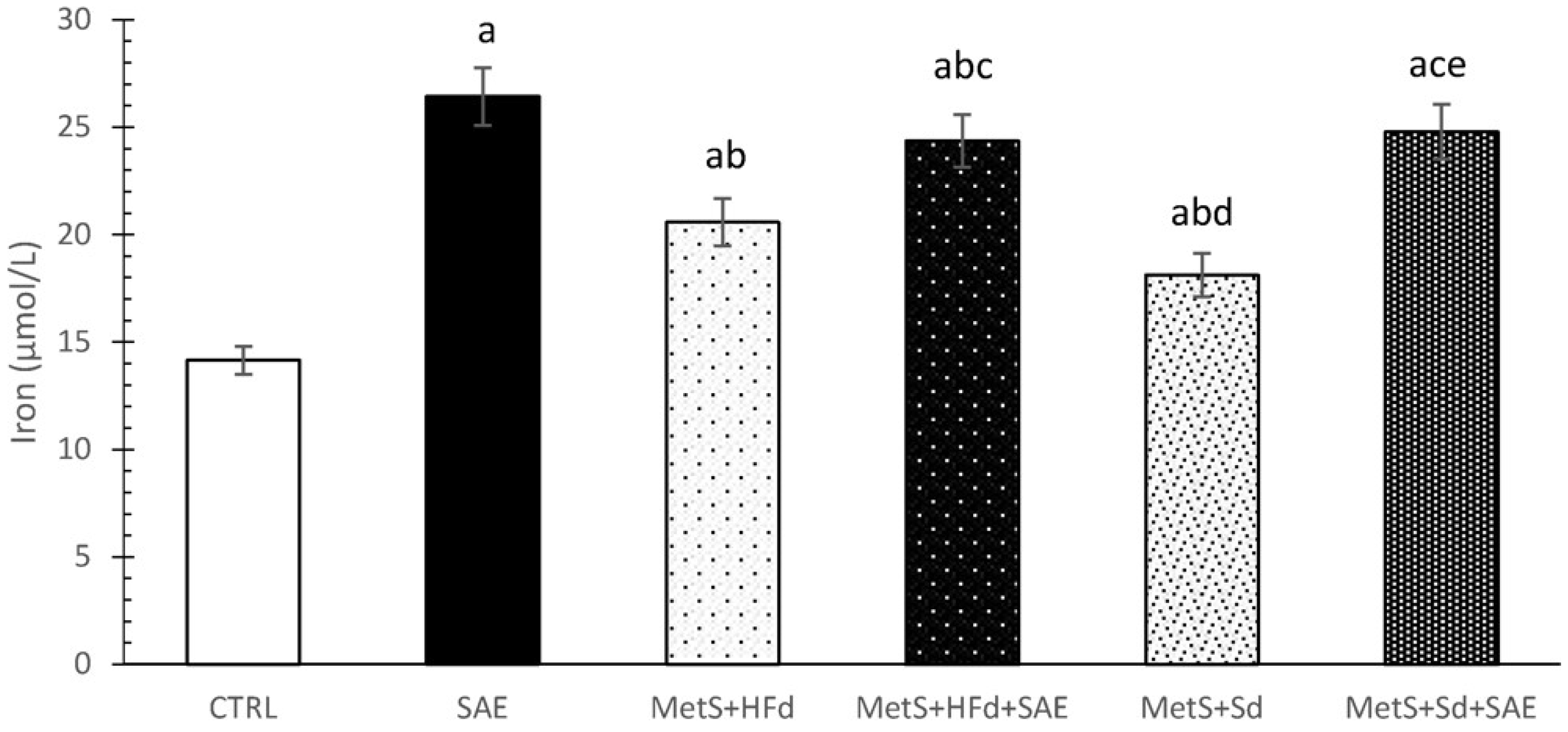
2.6. Effect of Dietary Changes in Healthy and Rats with MetS on Serum Iron Levels
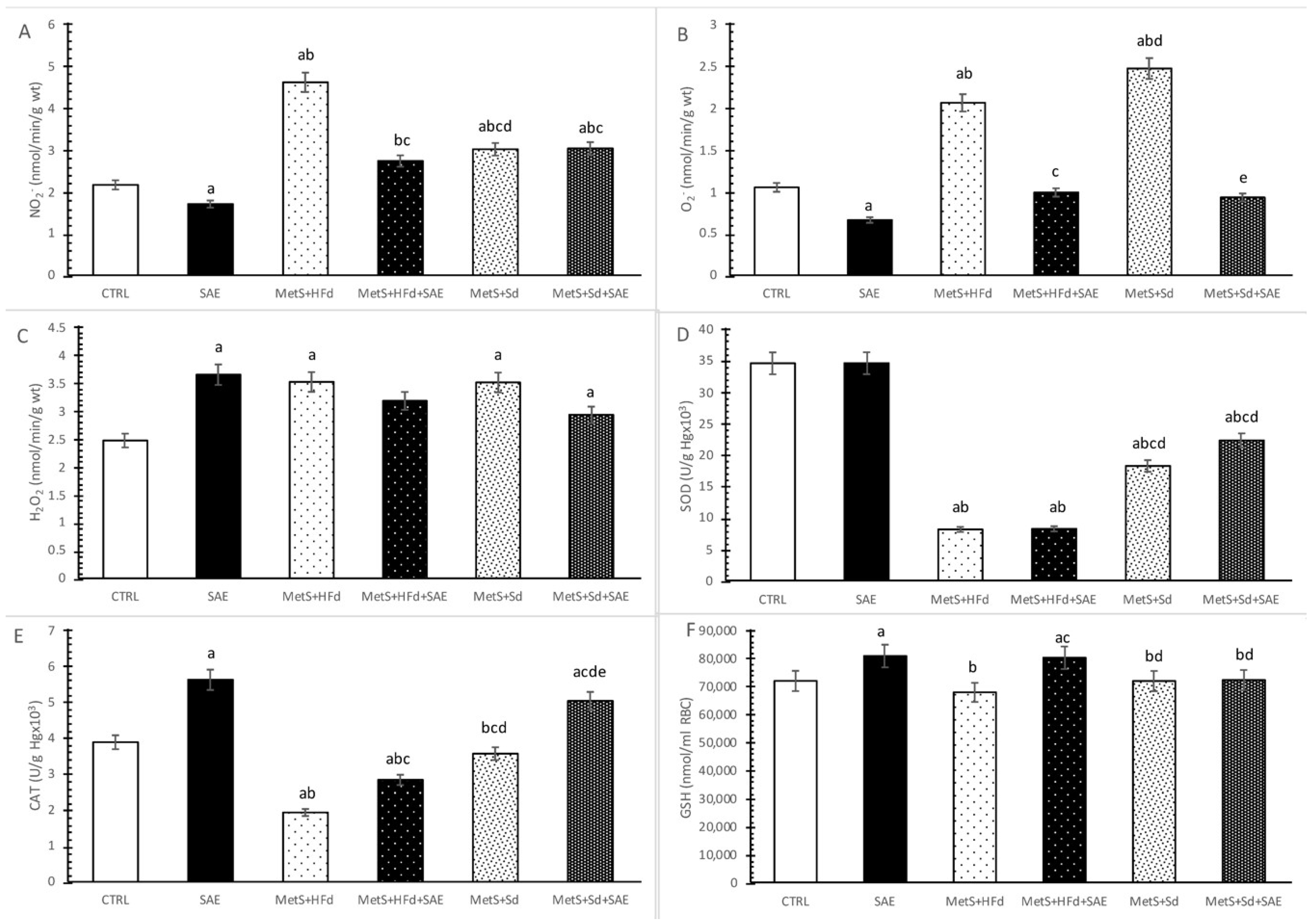
2.7. Evaluation of Systemic Redox State
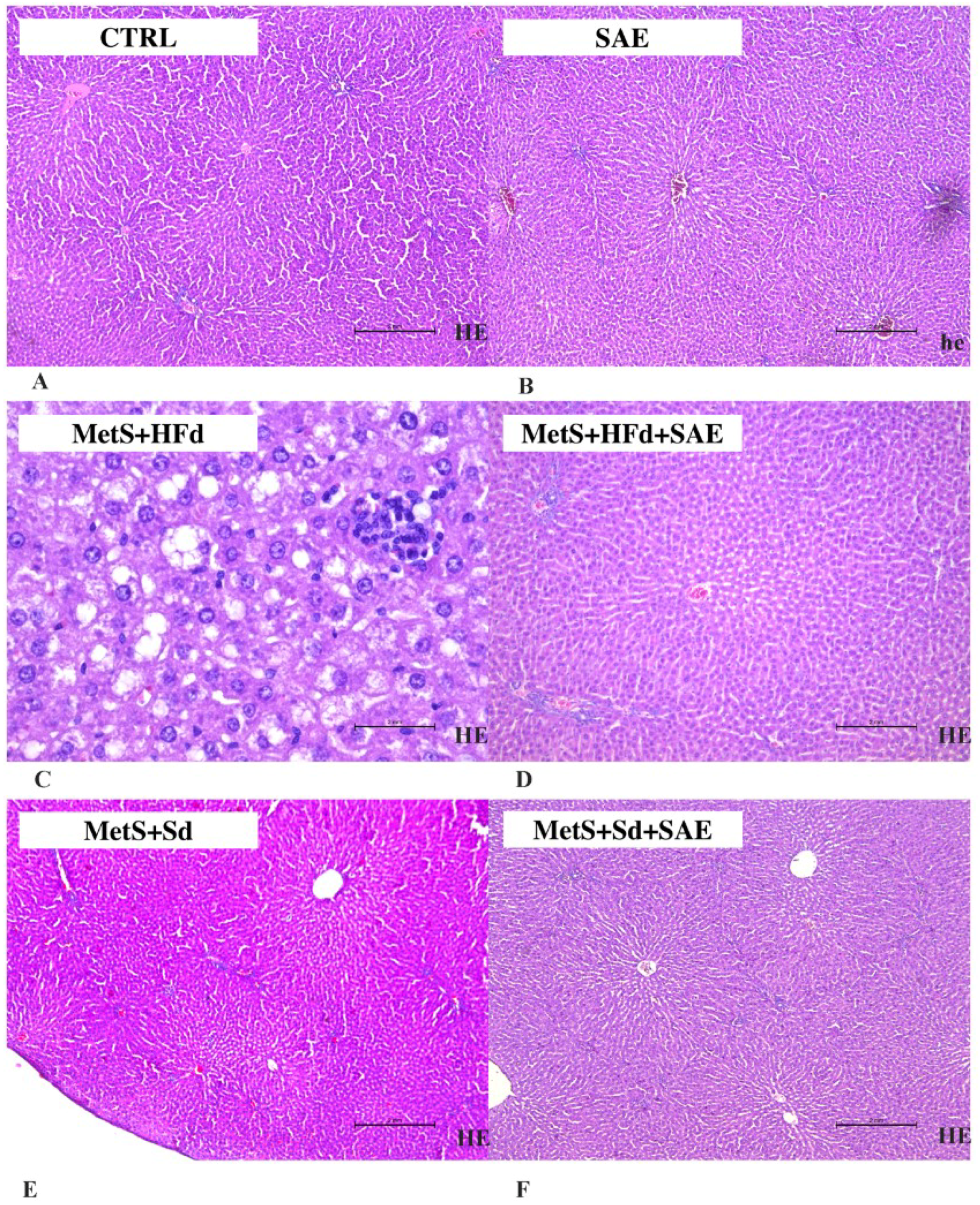
2.8. Histological Analysis of Liver Tissue
3. Discussion
4. Material and Methods
4.1. Ethical Approval
4.2. Animals
4.3. Measurement of BMI
4.4. Evaluation of Blood Pressure and Heart Rate
4.5. Evaluation of in vivo Cardiac Function
4.6. Evaluation of ex vivo Cardiac Function
4.7. Oral Glucose Tolerance Test
4.8. Evaluation of Serum Iron Levels and Systemic Redox State
4.9. Histological Analysis of Liver Tissue
4.10. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tabatabaei-Malazy, O.; Larijani, B.; Abdollahi, M. Targeting metabolic disorders by natural products. J. Diabetes Metab. Disord. 2015, 14, 57. [Google Scholar] [CrossRef] [PubMed]
- Moore, J.X.; Chaudhary, N.; Akinyemiju, T. Metabolic Syndrome Prevalence by Race/Ethnicity and Sex in the United States, National Health and Nutrition Examination Survey, 1988–2012. Prev. Chronic Dis. 2017, 14, E24. [Google Scholar] [CrossRef] [PubMed]
- Bernabé, J.; Mulero, J.; Marhuenda, J.; Cerdá, B.; Avilés, F.; Abellán, J.; Zafrilla, P. Changes in Antioxidant Enzymes in Metabolic Syndrome Patients after Consumption a Citrus-Based Juice Enriched with Aronia Melanocarpa. J. Nutr. Disorders Ther. 2015, 5, 4. [Google Scholar]
- Nammi, S.; Sreemantula, S.; Roufogalis, B.D. Protective effects of ethanolic extract of Zingiber officinale rhizome on the development of metabolic syndrome in high-fat diet-fed rats. Basic Clin. Pharmacol. Toxicol. 2009, 104, 366–373. [Google Scholar] [CrossRef] [PubMed]
- Ranasinghe, P.; Mathangasinghe, Y.; Jayawardena, R.; Hills, A.P.; Misra, A. Prevalence and trends of metabolic syndrome among adults in the asia-pacific region: A systematic review. BMC Public Health 2017, 17, 101. [Google Scholar] [CrossRef]
- De la Iglesia, R.; Loria-Kohen, V.; Zulet, M.A.; Martinez, J.A.; Reglero, G.; Ramirez de Molina, A. Dietary Strategies Implicated in the Prevention and Treatment of Metabolic Syndrome. Int. J. Mol. Sci. 2016, 17, 1877. [Google Scholar] [CrossRef] [PubMed]
- Daskalova, E.; Delchev, S.; Peeva, Y.; Vladimirova-Kitova, L.; Kratchanova, M.; Kratchanov, C.; Denev, P. Antiatherogenic and Cardioprotective Effects of Black Chokeberry (Aronia melanocarpa) Juice in Aging Rats. Evid. Based Complement Alternat. Med. 2015, 2015. [Google Scholar] [CrossRef]
- Kokotkiewicz, A.; Jaremicz, Z.; Luczkiewicz, M. Aronia plants: A review of traditional use, biological activities, and perspectives for modern medicine. J. Med. Food 2010, 13, 255–269. [Google Scholar] [CrossRef]
- Ochmian, I.; Grajkowski, J.; Smolik, M. Comparison of some morphological features, quality and chemical content of four cultivars of chokeberry fruits (Aronia melanocarpa). Not. Bot. Horti. Agrobot. Cluj Napoca 2012, 40, 253–260. [Google Scholar] [CrossRef]
- Tolić, M.T.; Landeka Jurčević, I.; Panjkota Krbavčić, I.; Marković, K.; Vahčić, N. Phenolic Content, Antioxidant Capacity and Quality of Chokeberry (Aronia melanocarpa) Products. Food Technol. Biotechnol. 2015, 53, 171–179. [Google Scholar] [CrossRef]
- Cebova, M.; Klimentova, J.; Janega, P.; Pechanova, O. Effect of Bioactive Compound of Aronia melanocarpa on Cardiovascular System in Experimental Hypertension. Oxid. Med. Cell. Longev. 2017, 2017. [Google Scholar] [CrossRef] [PubMed]
- Jurikova, T.; Mlcek, J.; Skrovankova, S.; Sumczynski, D.; Sochor, J.; Hlavacova, I.; Snopek, L.; Orsavova, J. Fruits of Black Chokeberry Aronia melanocarpa in the Prevention of Chronic Diseases. Molecules 2017, 22, 944. [Google Scholar] [CrossRef] [PubMed]
- Lupascu, N.; Cadar, E.; Cherim, M.; Erimia, C.L.; Sîrbu, R. Research Concerning the Efficiency of Aronia Melanocarpa for Pharmaceutical Purpose. Eur. J. Interdiscip. Stud. 2016, 4, 115–121. [Google Scholar] [CrossRef]
- Borowska, S.; Brzóska, M.M. Chokeberries (Aronia melanocarpa) and Their Products as a Possible Means for the Prevention and Treatment of Noncommunicable Diseases and Unfavorable Health Effects Due to Exposure to Xenobiotics. Compr. Rev. Food Sci. Food Saf. 2016, 15, 982–1017. [Google Scholar] [CrossRef]
- Finelli, C.; Sommella, L.; Gioia, S.; La Sala, N.; Tarantino, G. Should visceral fat be reduced to increase longevity? Ageing Res. Rev. 2013, 12, 996–1004. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y.; Yu, Z.; Xia, M.; Luo, X.; Lu, X.; Ling, W. Vitamin D attenuates high fat diet-induced hepatic steatosis in rats by modulating lipid metabolism. Eur. J. Clin. Investig. 2012, 42, 1189–1196. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Wang, P.Y.; Qin, L.Q.; Davaasambuu, G.; Kaneko, T.; Xu, J.; Murata, S.; Katoh, R.; Sato, A. The development of diabetes mellitus in Wistar rats kept on a high-fat/low-carbohydrate diet for long periods. Endocrine 2003, 22, 85–92. [Google Scholar] [CrossRef]
- Auberval, N.; Dal, S.; Bietiger, W.; Pinget, M.; Jeandidier, N.; Maillard-Pedracini, E.; Schini-Kerth, V.; Sigrist, S. Metabolic and oxidative stress markers in Wistar rats after 2 months on a high-fat diet. Diabetol. Metab. Syndr. 2014, 6, 130. [Google Scholar] [CrossRef] [PubMed]
- Hellström, J.K.; Shikov, A.N.; Makarova, M.N.; Pihlanto, A.M.; Pozharitskaya, O.N.; Ryhänen, E.L.; Kivijärvi, P.; Makarov, V.G.; Mattila, P.H. Blood pressure-lowering properties of chokeberry (Aronia mitchurinii var. Viking). J. Funct. Foods 2010, 2, 163–169. [Google Scholar] [CrossRef]
- Yamane, T.; Kozuka, M.; Imai, M.; Yamamoto, Y.; Ohkubo, I.; Sakamoto, T.; Nakagaki, T.; Nakano, Y. Reduction of blood pressure by aronia berries through inhibition of angiotensin-converting enzyme activity in the spontaneously hypertensive rat kidney. Funct. Food Health Dis. 2017, 7, 280–290. [Google Scholar]
- Ciocoiu, M.; Badescu, M.; Badulescu, O.; Tutunaru, D.; Badescu, L. Polyphenolic extract association with renin inhibitors in experimental arterial hypertension. J. Biomed. Sci. Eng. 2013, 6, 493–497. [Google Scholar] [CrossRef]
- Naruszewicz, M.; Laniewska, I.; Millo, B.; Dłuzniewski, M. Combination therapy of statin with flavonoids rich extract from chokeberry fruits enhanced reduction in cardiovascular risk markers in patients after myocardial infraction (MI). Atherosclerosis 2007, 194, e179–e184. [Google Scholar] [CrossRef] [PubMed]
- Tjelle, T.E.; Holtung, L.; Bøhn, S.K.; Aaby, K.; Thoresen, M.; Wiik, S.Å.; Paur, I.; Karlsen, A.S.; Retterstøl, K.; Iversen, P.O.; Blomhoff, R. Polyphenol-rich juices reduce blood pressure measures in a randomised controlled trial in high normal and hypertensive volunteers. Br. J. Nutr. 2015, 114, 1054–1063. [Google Scholar] [CrossRef] [PubMed]
- Broncel, M.; Kozirog, M.; Duchnowicz, P.; Koter-Michalak, M.; Sikora, J.; Chojnowska-Jezierska, J. Aronia melanocarpa extract reduces blood pressure, serum endothelin, lipid, and oxidative stress marker levels in patients with metabolic syndrome. Med. Sci. Monit. 2010, 16, CR28–CR34. [Google Scholar] [PubMed]
- Kanthe, P.S.; Patil, B.S.; Bagali, S.C.; Reddy, R.C.; Aithala, M.R.; Das, K.K. Protective effects of Ethanolic Extract of Emblica officinalis (amla) on Cardiovascular Pathophysiology of Rats, Fed with High Fat Diet. J. Clin. Diagn. Res. 2017, 11, CC05–CC09. [Google Scholar] [CrossRef] [PubMed]
- El-Sayyad, S.M.; Makboul, M.A.; Ali, R.M.; Farag, S.F. Hypotensive effect of Ficus sycomorus L. on the arterial blood pressure of rabbits. J. Pharmacogn. Phytochem. 2016, 4. Available online: https://www.researchgate.net/publication/309610756_Hypotensive_effect_of_Ficus_sycomorus_L_on_the_arterial_blood_pressure_of_rabbits (accessed on 28 November 2018).
- Cherniack, E.P. Polyphenols: Planting the seeds of treatment for the metabolic syndrome. Nutrition 2011, 27, 617–623. [Google Scholar] [CrossRef]
- Leung, L.; Martin, J.B.; Lawmaster, T.; Arthur, K.; Broderick, T.L.; Al-Nakkash, L. Sex-Dependent Effects of Dietary Genistein on Echocardiographic Profile and Cardiac GLUT4 Signaling in Mice. Evid. Based Complement Alternat. Med. 2016, 2016, 1796357. [Google Scholar] [CrossRef]
- Razmaraii, N.; Babaei, H.; Mohajjel Nayebi, A.; Assadnassab, G.; Ashrafi-Helan, J.; Azarmi, Y. Cardioprotective Effect of Grape Seed Extract on Chronic Doxorubicin-Induced Cardiac Toxicity in Wistar Rats. Adv. Pharm. Bull. 2016, 6, 423–433. [Google Scholar] [CrossRef]
- Yadegari, M.; Khamesipour, F.; Talebiyan, R.; Katsande, S. Echocardiography findings after intravenous injection of Achillea millefolium (Yarrow) extract in the dog. Malays. Appl. Biol. 2015, 44, 85–91. [Google Scholar]
- Parzonko, A.; Naruszewicz, M. Cardioprotective effects of Aronia melanocarpa anthocynanins. From laboratory experiments to clinical practice. Curr. Pharm. Des. 2016, 22, 174–179. [Google Scholar] [CrossRef]
- Kim, N.H.; Jegal, J.; Kim, Y.N.; Heo, J.D.; Rho, J.R.; Yang, M.H.; Jeong, E.J. Chokeberry Extract and Its Active Polyphenols Suppress Adipogenesis in 3T3-L1 Adipocytes and Modulates Fat Accumulation and Insulin Resistance in Diet-Induced Obese Mice. Nutrients 2018, 10, 1734. [Google Scholar] [CrossRef]
- Simeonov, S.B.; Botushanov, N.P.; Karahanian, E.B.; Pavlova, M.B.; Husianitis, H.K.; Troev, D.M. Effects of Aronia melanocarpa juice as part of the dietary regimen in patients with diabetes mellitus. Folia Med. 2002, 44, 20–23. [Google Scholar]
- Yamane, T.; Kozuka, M.; Konda, D.; Nakano, Y.; Nakagaki, T.; Ohkubo, I.; Ariga, H. Improvement of blood glucose levels and obesity in mice given aronia juice by inhibition of dipeptidyl peptidase IV and α-glucosidase. J. Nutr. Biochem. 2016, 31, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Imam, M.U.; Zhang, S.; Ma, J.; Wang, H.; Wang, F. Antioxidants Mediate Both Iron Homeostasis and Oxidative Stress. Nutrients 2017, 9, 671. [Google Scholar] [CrossRef]
- Lee, H.J.; Jang, H.B.; Park, J.E.; Park, K.H.; Kang, J.H.; Park, S.I.; Song, J. Relationship between Serum Levels of Body Iron Parameters and Insulin Resistance and Metabolic Syndrome in Korean Children. Osong Public Health Res. Perspect. 2014, 5, 204–210. [Google Scholar] [CrossRef] [PubMed]
- Skarpańska-Stejnborn, A.; Basta, P.; Sadowska, J.; Pilaczyńska-Szcześniak, L. Effect of supplementation with chokeberry juice on the inflammatory status and markers of iron metabolism in rowers. J. Int. Soc. Sports Nutr. 2014, 11, 48. [Google Scholar] [CrossRef]
- Mu, M.; An, P.; Wu, Q.; Shen, X.; Shao, D.; Wang, H.; Zhang, Y.; Zhang, S.; Yao, H.; Min, J.; et al. The dietary flavonoid myricetin regulates iron homeostasis by suppressing hepcidin expression. J. Nutr. Biochem. 2016, 30, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Gregório, B.M.; De Souza, D.B.; de Morais Nascimento, F.A.; Pereira, L.M.; Fernandes-Santos, C. The potential role of antioxidants in metabolic syndrome. Curr. Pharm. Des. 2016, 22, 859–869. [Google Scholar] [CrossRef]
- Louis, X.L.; Thandapilly, S.J.; Kalt, W.; Vinqvist-Tymchuk, M.; Aloud, B.M.; Raj, P.; Yu, L.; Le, H.; Netticadan, T. Blueberry polyphenols prevent cardiomyocyte death by preventing calpain activation and oxidative stress. Food Funct. 2014, 5, 1785–1794. [Google Scholar] [CrossRef]
- Mattera, R.; Benvenuto, M.; Giganti, M.G.; Tresoldi, I.; Pluchinotta, F.R.; Bergante, S.; Tettamanti, G.; Masuelli, L.; Manzari, V.; Modesti, A.; et al. Effects of Polyphenols on Oxidative Stress-Mediated Injury in Cardiomyocytes. Nutrients 2017, 9, 523. [Google Scholar] [CrossRef] [PubMed]
- Brglez Mojzer, E.; Knez Hrnčič, M.; Škerget, M.; Knez, Ž.; Bren, U. Polyphenols: Extraction Methods, Antioxidative Action, Bioavailability and Anticarcinogenic Effects. Molecules 2016, 21, 901. [Google Scholar] [CrossRef] [PubMed]
- Kotronen, A.; Westerbacka, J.; Bergholm, R.; Pietiläinen, K.H.; Yki-Järvinen, H. Liver fat in the metabolic syndrome. J. Clin. Endocrinol. Metab. 2007, 92, 3490–3497. [Google Scholar] [CrossRef] [PubMed]
- Bhaswant, M.; Shafie, S.R.; Mathai, M.L.; Mouatt, P.; Brown, L. Anthocyanins in chokeberry and purple maize attenuate diet-induced metabolic syndrome in rats. Nutrition 2017, 41, 24–31. [Google Scholar] [CrossRef] [PubMed]
- Park, C.H.; Kim, J.H.; Lee, E.B.; Hur, W.; Kwon, O.J.; Park, H.J.; Yoon, S.K. Aronia melanocarpa extract ameliorates hepatic lipid metabolism through PPARγ2 downregulation. PLoS ONE 2017, 12, e0169685. [Google Scholar] [CrossRef] [PubMed]
- Duchnowicz, P.; Ziobro, A.; Rapacka, E.; Koter-Michalak, M.; Bukowska, B. Changes in Cholinesterase Activity in Blood of Adolescent with Metabolic Syndrome after Supplementation with Extract from Aronia melanocarpa. BioMed Res. Int. 2018. [Google Scholar] [CrossRef]
- Pari, L.; Chandramohan, R. Modulatory effects of naringin on hepatic key enzymes of carbohydrate metabolism in high-fat diet/low-dose streptozotocin-induced diabetes in rats. Gen Physiol Biophys 2017, 36, 343–352. [Google Scholar] [CrossRef]
- Feng, M.; Whitesall, S.; Zhang, Y.; Beibel, M.; D′Alecy, L.; DiPetrillo, K. Validation of volume-pressure recording tail-cuff blood pressure measurements. Am. J. Hypertens. 2008, 21, 1288–1291. [Google Scholar] [CrossRef]
- Joffe, I.I.; Travers, K.E.; Perreault-Micale, C.L.; Hampton, T.; Katz, S.E.; Morgan, J.P.; Douglas, P.S. Abnormal cardiac function in the streptozotocin-induced non-insulin-dependent diabetic rat: Noninvasive assessment with Doppler echocardiography and contribution of the nitric oxide pathway. J. Am. Coll. Cardiol. 1999, 34, 2111–2119. [Google Scholar] [CrossRef]
- Zivkovic, V.; Jakovljevic, V.; Djordjevic, D.; Vuletic, M.; Barudzic, N.; Djuric, D. The effects of homocysteine-related compounds on cardiac contractility, coronary flow, and oxidative stress markers in isolated rat heart. Mol. Cell. Biochem. 2012, 370, 59–67. [Google Scholar] [CrossRef]
- Green, L.C.; Wagner, D.A.; Glogowski, J.; Skipper, P.L.; Wishnok, J.S.; Tannenbaum, S.R. Analysis of nitrate, nitrite, and [15N]nitrate in biological fluids. Anal. Biochem. 1982, 126, 131–138. [Google Scholar] [CrossRef]
- Auclair, C.; Voisin, E. Nitroblue tetrazolium reduction. In Handbook of Methods for Oxygen Radical Research; Greenvvald, R.A., Ed.; CRC Press: Boca Raton, FL, USA, 1985; pp. 123–132. [Google Scholar]
- Pick, E.; Keisari, Y. A simple colorimetric method for the measurement of hydrogen peroxide produced by cells in culture. J. Immunol. Methods. 1980, 38, 161–170. [Google Scholar] [CrossRef]
- McCord, J.M.; Fridovich, I. The utility of superoxide dismutase in studying free radical reactions. I. Radicals generated by the interaction of sulfite, dimethyl sulfoxide, and oxygen. J. Biol. Chem. 1969, 244, 6056–6063. [Google Scholar] [PubMed]
- Beutler, E. Catalase. In Red Cell Metabolism, a Manual of Biochemical Methods; Beutler, E., Ed.; Grune and Stratton: New York, NY, USA, 1982; pp. 105–106. [Google Scholar]
- Misra, H.P.; Fridovich, I. The role of superoxide-anion in the autooxidation of epinephrine and a simple assay for superoxide dismutase. J. Biol. Chem. 1972, 247, 3170–3175. [Google Scholar]
- Beutler, E. Reduced glutathione (GSH). In Red Cell Metabolism, a Manual of Biochemical Methods; Beutler, E., Ed.; Grune and Stratton: New York, NY, USA, 1975; pp. 112–114. [Google Scholar]
| Milimeters (mm) | CTRL | SAE | MetS + HFd | MetS + HFd + SAE | MetS + Sd | MetS + Sd + SAE |
|---|---|---|---|---|---|---|
| IVSd | 1.22 ± 0.2 | 1.89 ± 0.2 a | 1.28 ± 0.3 b | 1.34 ± 0.2 | 1.58 ± 0.2 | 1.59 ± 0.2 |
| LVIDd | 6.80 ± 0.4 | 5.73 ± 0.2 a | 6.23 ± 0.4 | 6.70 ± 0.4 | 5.53 ± 0.3 | 7.93 ± 0.4 e |
| LVPWd | 1.94 ± 0.4 | 3.45 ± 0.4 a | 2.22 ± 0.1 | 1.72 ± 0.1b | 1.88 ± 0.2 b | 1.93 ± 0.2 b |
| IVSs | 2.48 ± 0.3 | 3.64 ± 0.3 a | 2.33 ± 0.1 b | 2.52 ± 0.2 | 2.45 ± 0.2 b | 3.24 ± 0.1 ace |
| LVIDs | 3.20 ± 0.5 | 2.03 ± 0.2 a | 3.24 ± 0.2 b | 3.16 ± 0.1 | 2.48 ± 0.2 acd | 3.45 ± 0.2 be |
| LVPWs | 2.98 ± 0.2 | 4.97 ± 0.1 a | 3.16 ± 0.2 | 3.26 ± 0.2 | 2.76 ± 0.2 b | 3.45 ± 0.3 |
| FS (%) | 53.2 ± 4.18 | 65.7 ± 5.01 a | 49.0 ± 3.99 ab | 52.2 ± 4.32b | 51.4 ± 4.19 b | 56.3 ± 4.21 |
| CPP | CTRL | SAE | MetS + HFd | MetS + HFd + SAE | MetS + Sd | MetS + Sd + SAE |
|---|---|---|---|---|---|---|
| dp/dt max | ||||||
| 60 | −11.05 | −5.99 | −24.77 | −1.07 | −24.23 | −13.13 |
| 80 | −6.11 | −12.90 | −35.30 | −4.41 | −28.11 | −3.77 |
| 100 | −10.88 | −4.79 | −6.22 | −4.08 | −8.80 | −14.02 |
| 120 | −0.63 | −1.91 | 5.62 | −9.39 | −2.06 | −3.24 |
| dp/dt min | ||||||
| 60 | −21.25 | −14.81 | −0.46 | −0.62 | −13.64 | −6.36 |
| 80 | −22.03 | −11.53 | −0.80 | −9.03 | −18.90 | −2.32 |
| 100 | −29.70 | −11.43 | −7.04 | −3.81 | −9.14 | −12.42 |
| 120 | −12.04 | −8.14 | −8.08 | −3.15 | 2.63 | 1.16 |
| SLVP | ||||||
| 60 | −8.35 | −9.49 | 5.37 | 10.80 | −10.58 | 4.06 |
| 80 | −13.11 | −1.66 | 5.70 | 8.55 | −4.18 | 2.44 |
| 100 | −16.81 | −5.81 | −1.22 | 2.15 | 3.72 | −12.46 |
| 120 | −7.79 | −16.29 | 12.60 | 1.99 | 4.12 | −0.07 |
| DLVP | ||||||
| 60 | 12.50 | 16.67 | 2.50 | −15.79 | 14.41 | 6.67 |
| 80 | 16.05 | 10.20 | −2.22 | −19.05 | 9.32 | 4.76 |
| 100 | 10.47 | −0.93 | −4.21 | −15.38 | 15.87 | 9.09 |
| 120 | 7.61 | −5.26 | 0.00 | −2.86 | 4.13 | 8.45 |
| HR | ||||||
| 60 | −5.29 | −4.01 | −6.26 | 1.59 | 1.39 | 2.51 |
| 80 | −1.96 | −3.85 | −6.82 | 0.23 | 0.41 | 1.10 |
| 100 | −4.58 | −2.77 | −5.04 | 3.66 | 0.31 | −0.37 |
| 120 | −3.41 | −2.63 | −3.21 | 7.85 | 1.02 | 0.61 |
| CF | ||||||
| 60 | −12.37 | −10.07 | −3.11 | 6.74 | 1.93 | −4.55 |
| 80 | −3.57 | −10.40 | −5.78 | 5.48 | 7.88 | −3.36 |
| 100 | −5.10 | −8.33 | −2.55 | −0.57 | 13.44 | −4.55 |
| 120 | −1.21 | −14.66 | −14.96 | 1.51 | 7.59 | −1.04 |
| Groups | 0′ | 180′ |
|---|---|---|
| CTRL | 122.9 ± 6.76 | 123.7 ± 6.61 |
| SAE | 106.9 ± 6.04 a | 113.8 ± 6.51 |
| МetS + HFd | 185.1 ± 7.78 ab | 129.3 ± 6.38 |
| МetS + HFd + SАE | 180.3 ± 8.02 ab | 131.1 ± 7.13 b |
| МetS + Sd | 205.8 ± 9.87 abcd | 145.2 ± 7.65 b |
| МetS + Sd + SАE | 182.1 ± 9.32 abcde | 127.3 ± 6.72 e |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
JAKOVLJEVIC, V.; Milic, P.; Bradic, J.; Jeremic, J.; Zivkovic, V.; Srejovic, I.; Nikolic Turnic, T.; Milosavljevic, I.; Jeremic, N.; Bolevich, S.; et al. Standardized Aronia melanocarpa Extract as Novel Supplement against Metabolic Syndrome: A Rat Model. Int. J. Mol. Sci. 2019, 20, 6. https://doi.org/10.3390/ijms20010006
JAKOVLJEVIC V, Milic P, Bradic J, Jeremic J, Zivkovic V, Srejovic I, Nikolic Turnic T, Milosavljevic I, Jeremic N, Bolevich S, et al. Standardized Aronia melanocarpa Extract as Novel Supplement against Metabolic Syndrome: A Rat Model. International Journal of Molecular Sciences. 2019; 20(1):6. https://doi.org/10.3390/ijms20010006
Chicago/Turabian StyleJAKOVLJEVIC, Vladimir, Petar Milic, Jovana Bradic, Jovana Jeremic, Vladimir Zivkovic, Ivan Srejovic, Tamara Nikolic Turnic, Isidora Milosavljevic, Nevena Jeremic, Sergey Bolevich, and et al. 2019. "Standardized Aronia melanocarpa Extract as Novel Supplement against Metabolic Syndrome: A Rat Model" International Journal of Molecular Sciences 20, no. 1: 6. https://doi.org/10.3390/ijms20010006
APA StyleJAKOVLJEVIC, V., Milic, P., Bradic, J., Jeremic, J., Zivkovic, V., Srejovic, I., Nikolic Turnic, T., Milosavljevic, I., Jeremic, N., Bolevich, S., Labudovic Borovic, M., Mitrovic, M., & Vucic, V. (2019). Standardized Aronia melanocarpa Extract as Novel Supplement against Metabolic Syndrome: A Rat Model. International Journal of Molecular Sciences, 20(1), 6. https://doi.org/10.3390/ijms20010006








