Biomarkers for Predicting Clinical Outcomes of Chemoradiation-Based Bladder Preservation Therapy for Muscle-Invasive Bladder Cancer
Abstract
1. Introduction
2. Current Practice on Bladder Preservation Therapy in Muscle-Invasive Bladder Cancer Patients
2.1. Indications
2.2. Therapeutic Protocols
2.3. Prognosis
2.4. Clinicopathologic Factors Associated with Outcomes of Bladder Preservation Therapy
3. Biomarkers Associated with Chemoradiation Response and Prognosis
3.1. Apoptosis-Related Biomarkers
3.2. Cell Proliferation-Related Biomarkers
3.3. Receptor Tyrosine Kinases
3.4. DNA Damage Response-Related Biomarkers
3.5. Hypoxia-Related Biomarkers
3.6. Molecular Subtypes
3.7. Others
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2018. CA Cancer J. Clin. 2018, 68, 7–30. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.S.; Bochner, B.H.; Chou, R.; Dreicer, R.; Kamat, A.M.; Lerner, S.P.; Lotan, Y.; Meeks, J.J.; Michalski, J.M.; Morgan, T.M.; et al. Treatment of Non-Metastatic Muscle-Invasive Bladder Cancer: AUA/ASCO/ASTRO/SUO Guideline. J. Urol. 2017, 198, 552–559. [Google Scholar] [CrossRef] [PubMed]
- Novara, G.; Catto, J.W.; Wilson, T.; Annerstedt, M.; Chan, K.; Murphy, D.G.; Motttrie, A.; Peabody, J.O.; Skinner, E.C.; Wiklund, P.N.; et al. Systematic review and cumulative analysis of perioperative outcomes and complications after robot-assisted radical cystectomy. Eur. Urol. 2015, 67, 376–401. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, S.M.; Wood, D.P.; Dunn, R.L.; Weizer, A.Z.; Lee, C.T.; Montie, J.E.; Wei, J.T. Measuring health-related quality of life outcomes in bladder cancer patients using the Bladder Cancer Index (BCI). Cancer 2007, 109, 1756–1762. [Google Scholar] [CrossRef] [PubMed]
- Koga, F.; Kihara, K. Selective bladder preservation with curative intent for muscle-invasive bladder cancer: A contemporary review. Int. J. Urol. 2012, 19, 388–401. [Google Scholar] [CrossRef] [PubMed]
- Giacalone, N.J.; Shipley, W.U.; Clayman, R.H.; Niemierko, A.; Drumm, M.; Heney, N.M.; Michaelson, M.D.; Lee, R.J.; Saylor, P.J.; Wszolek, M.F.; et al. Long-term Outcomes After Bladder-preserving Tri-modality Therapy for Patients with Muscle-invasive Bladder Cancer: An Updated Analysis of the Massachusetts General Hospital Experience. Eur. Urol. 2017, 71, 952–960. [Google Scholar] [CrossRef] [PubMed]
- Ploussard, G.; Daneshmand, S.; Efstathiou, J.A.; Herr, H.W.; James, N.D.; Rodel, C.M.; Shariat, S.F.; Shipley, W.U.; Sternberg, C.N.; Thalmann, G.N.; et al. Critical analysis of bladder sparing with trimodal therapy in muscle-invasive bladder cancer: A systematic review. Eur. Urol. 2014, 66, 120–137. [Google Scholar] [CrossRef] [PubMed]
- Rodel, C.; Grabenbauer, G.G.; Kuhn, R.; Papadopoulos, T.; Dunst, J.; Meyer, M.; Schrott, K.M.; Sauer, R. Combined-modality treatment and selective organ preservation in invasive bladder cancer: Long-term results. J. Clin. Oncol. 2002, 20, 3061–3071. [Google Scholar] [CrossRef] [PubMed]
- Koga, F.; Numao, N.; Saito, K.; Masuda, H.; Fujii, Y.; Kawakami, S.; Kihara, K. Sensitivity to chemoradiation predicts development of metastasis in muscle-invasive bladder cancer patients. Urol. Oncol. 2013, 31, 1270–1275. [Google Scholar] [CrossRef] [PubMed]
- Coppin, C.M.; Gospodarowicz, M.K.; James, K.; Tannock, I.F.; Zee, B.; Carson, J.; Pater, J.; Sullivan, L.D. Improved local control of invasive bladder cancer by concurrent cisplatin and preoperative or definitive radiation. The National Cancer Institute of Canada Clinical Trials Group. J. Clin. Oncol. 1996, 14, 2901–2907. [Google Scholar] [CrossRef] [PubMed]
- James, N.D.; Hussain, S.A.; Hall, E.; Jenkins, P.; Tremlett, J.; Rawlings, C.; Crundwell, M.; Sizer, B.; Sreenivasan, T.; Hendron, C.; et al. Radiotherapy with or without chemotherapy in muscle-invasive bladder cancer. N. Engl. J. Med. 2012, 366, 1477–1488. [Google Scholar] [CrossRef] [PubMed]
- Choudhury, A.; Swindell, R.; Logue, J.P.; Elliott, P.A.; Livsey, J.E.; Wise, M.; Symonds, P.; Wylie, J.P.; Ramani, V.; Sangar, V.; et al. Phase II study of conformal hypofractionated radiotherapy with concurrent gemcitabine in muscle-invasive bladder cancer. J. Clin. Oncol. 2011, 29, 733–738. [Google Scholar] [CrossRef] [PubMed]
- Muller, A.C.; Diestelhorst, A.; Kuhnt, T.; Kuhn, R.; Fornara, P.; Scholz, H.J.; Dunst, J.; Zietman, A.L. Organ-sparing treatment of advanced bladder cancer: Paclitaxel as a radiosensitizer. Strahlenther. Onkol. 2007, 183, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Iwai, A.; Koga, F.; Fujii, Y.; Masuda, H.; Saito, K.; Numao, N.; Sakura, M.; Kawakami, S.; Kihara, K. Perioperative complications of radical cystectomy after induction chemoradiotherapy in bladder-sparing protocol against muscle-invasive bladder cancer: A single institutional retrospective comparative study with primary radical cystectomy. Jpn. J. Clin. Oncol. 2011, 41, 1373–1379. [Google Scholar] [CrossRef] [PubMed]
- Koga, F.; Kihara, K.; Yoshida, S.; Yokoyama, M.; Saito, K.; Masuda, H.; Fujii, Y.; Kawakami, S. Selective bladder-sparing protocol consisting of induction low-dose chemoradiotherapy plus partial cystectomy with pelvic lymph node dissection against muscle-invasive bladder cancer: Oncological outcomes of the initial 46 patients. BJU Int. 2012, 109, 860–866. [Google Scholar] [CrossRef] [PubMed]
- Koga, F.; Yoshida, S.; Kawakami, S.; Kageyama, Y.; Yokoyama, M.; Saito, K.; Fujii, Y.; Kobayashi, T.; Kihara, K. Low-dose chemoradiotherapy followed by partial or radical cystectomy against muscle-invasive bladder cancer: An intent-to-treat survival analysis. Urology 2008, 72, 384–388. [Google Scholar] [CrossRef] [PubMed]
- Azuma, H.; Inamoto, T.; Takahara, K.; Nomi, H.; Hirano, H.; Ibuki, N.; Uehara, H.; Komura, K.; Minami, K.; Uchimoto, T.; et al. Novel bladder preservation therapy with Osaka Medical College regimen. J. Urol. 2015, 193, 443–450. [Google Scholar] [CrossRef] [PubMed]
- Cahn, D.B.; Handorf, E.A.; Ghiraldi, E.M.; Ristau, B.T.; Geynisman, D.M.; Churilla, T.M.; Horwitz, E.M.; Sobczak, M.L.; Chen, D.Y.T.; Viterbo, R.; et al. Contemporary use trends and survival outcomes in patients undergoing radical cystectomy or bladder-preservation therapy for muscle-invasive bladder cancer. Cancer 2017, 123, 4337–4345. [Google Scholar] [CrossRef] [PubMed]
- Ritch, C.R.; Balise, R.; Prakash, N.S.; Alonzo, D.; Almengo, K.; Alameddine, M.; Venkatramani, V.; Punnen, S.; Parekh, D.J.; Gonzalgo, M.L. Propensity matched comparative analysis of survival following chemoradiation or radical cystectomy for muscle-invasive bladder cancer. BJU Int. 2018, 121, 745–751. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, G.S.; Hermanns, T.; Wei, Y.; Bhindi, B.; Satkunasivam, R.; Athanasopoulos, P.; Bostrom, P.J.; Kuk, C.; Li, K.; Templeton, A.J.; et al. Propensity Score Analysis of Radical Cystectomy Versus Bladder-Sparing Trimodal Therapy in the Setting of a Multidisciplinary Bladder Cancer Clinic. J. Clin. Oncol. 2017, 35, 2299–2305. [Google Scholar] [CrossRef] [PubMed]
- Coen, J.J.; Paly, J.J.; Niemierko, A.; Kaufman, D.S.; Heney, N.M.; Spiegel, D.Y.; Efstathiou, J.A.; Zietman, A.L.; Shipley, W.U. Nomograms predicting response to therapy and outcomes after bladder-preserving trimodality therapy for muscle-invasive bladder cancer. Int. J. Radiat. Oncol. Biol. Phys. 2013, 86, 311–316. [Google Scholar] [CrossRef] [PubMed]
- Rodel, C.; Grabenbauer, G.G.; Rodel, F.; Birkenhake, S.; Kuhn, R.; Martus, P.; Zorcher, T.; Fursich, D.; Papadopoulos, T.; Dunst, J.; et al. Apoptosis, p53, bcl-2, and Ki-67 in invasive bladder carcinoma: Possible predictors for response to radiochemotherapy and successful bladder preservation. Int. J. Radiat. Oncol. Biol. Phys. 2000, 46, 1213–1221. [Google Scholar] [CrossRef]
- Matsumoto, H.; Wada, T.; Fukunaga, K.; Yoshihiro, S.; Matsuyama, H.; Naito, K. Bax to Bcl-2 ratio and Ki-67 index are useful predictors of neoadjuvant chemoradiation therapy in bladder cancer. Jpn. J. Clin. Oncol. 2004, 34, 124–130. [Google Scholar] [CrossRef] [PubMed]
- Tanabe, K.; Yoshida, S.; Koga, F.; Inoue, M.; Kobayashi, S.; Ishioka, J.; Tamura, T.; Sugawara, E.; Saito, K.; Akashi, T.; et al. High Ki-67 Expression Predicts Favorable Survival in Muscle-Invasive Bladder Cancer Patients Treated with Chemoradiation-Based Bladder-Sparing Protocol. Clin. Genitourin. Cancer 2015, 13, e243-51. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, S.; Koga, F.; Kobayashi, S.; Ishii, C.; Tanaka, H.; Tanaka, H.; Komai, Y.; Saito, K.; Masuda, H.; Fujii, Y.; et al. Role of diffusion-weighted magnetic resonance imaging in predicting sensitivity to chemoradiotherapy in muscle-invasive bladder cancer. Int. J. Radiat. Oncol. Biol. Phys. 2012, 83, e21-7. [Google Scholar] [CrossRef] [PubMed]
- Chakravarti, A.; Winter, K.; Wu, C.L.; Kaufman, D.; Hammond, E.; Parliament, M.; Tester, W.; Hagan, M.; Grignon, D.; Heney, N.; et al. Expression of the epidermal growth factor receptor and Her-2 are predictors of favorable outcome and reduced complete response rates, respectively, in patients with muscle-invading bladder cancers treated by concurrent radiation and cisplatin-based chemotherapy: A report from the Radiation Therapy Oncology Group. Int. J. Radiat. Oncol. Biol. Phys. 2005, 62, 309–317. [Google Scholar] [PubMed]
- Inoue, M.; Koga, F.; Yoshida, S.; Tamura, T.; Fujii, Y.; Ito, E.; Kihara, K. Significance of ERBB2 overexpression in therapeutic resistance and cancer-specific survival in muscle-invasive bladder cancer patients treated with chemoradiation-based selective bladder-sparing approach. Int. J. Radiat. Oncol. Biol. Phys. 2014, 90, 303–311. [Google Scholar] [CrossRef] [PubMed]
- Michaelson, M.D.; Hu, C.; Pham, H.T.; Dahl, D.M.; Lee-Wu, C.; Swanson, G.P.; Vuky, J.; Lee, R.J.; Souhami, L.; Chang, B.; et al. A Phase 1/2 Trial of a Combination of Paclitaxel and Trastuzumab With Daily Irradiation or Paclitaxel Alone with Daily Irradiation After Transurethral Surgery for Noncystectomy Candidates With Muscle-Invasive Bladder Cancer (Trial NRG Oncology RTOG 0524). Int. J. Radiat. Oncol. Biol. Phys. 2017, 97, 995–1001. [Google Scholar] [CrossRef] [PubMed]
- Kawashima, A.; Nakayama, M.; Kakuta, Y.; Abe, T.; Hatano, K.; Mukai, M.; Nagahara, A.; Nakai, Y.; Oka, D.; Takayama, H.; et al. Excision repair cross-complementing group 1 may predict the efficacy of chemoradiation therapy for muscle-invasive bladder cancer. Clin. Cancer Res. 2011, 17, 2561–2569. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, H.; Yoshida, S.; Koga, F.; Toda, K.; Yoshimura, R.; Nakajima, Y.; Sugawara, E.; Akashi, T.; Waseda, Y.; Inoue, M.; et al. Impact of Immunohistochemistry-Based Subtypes in Muscle-Invasive Bladder Cancer on Response to Chemoradiotherapy. Int. J. Radiat. Oncol. Biol. Phys. 2018. [Google Scholar] [CrossRef] [PubMed]
- Urushibara, M.; Kageyama, Y.; Akashi, T.; Otsuka, Y.; Takizawa, T.; Koike, M.; Kihara, K. HSP60 may predict good pathological response to neoadjuvant chemoradiotherapy in bladder cancer. Jpn. J. Clin. Oncol. 2007, 37, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Lautenschlaeger, T.; George, A.; Klimowicz, A.C.; Efstathiou, J.A.; Wu, C.L.; Sandler, H.; Shipley, W.U.; Tester, W.J.; Hagan, M.P.; Magliocco, A.M.; et al. Bladder preservation therapy for muscle-invading bladder cancers on Radiation Therapy Oncology Group trials 8802, 8903, 9506, and 9706: Vascular endothelial growth factor B overexpression predicts for increased distant metastasis and shorter survival. Oncologist 2013, 18, 685–686. [Google Scholar] [CrossRef] [PubMed]
- Keck, B.; Wach, S.; Taubert, H.; Zeiler, S.; Ott, O.J.; Kunath, F.; Hartmann, A.; Bertz, S.; Weiss, C.; Honscheid, P.; et al. Neuropilin-2 and its ligand VEGF-C predict treatment response after transurethral resection and radiochemotherapy in bladder cancer patients. Int. J. Cancer 2015, 136, 443–451. [Google Scholar] [CrossRef] [PubMed]
- Choudhury, A.; Nelson, L.D.; Teo, M.T.; Chilka, S.; Bhattarai, S.; Johnston, C.F.; Elliott, F.; Lowery, J.; Taylor, C.F.; Churchman, M.; et al. MRE11 expression is predictive of cause-specific survival following radical radiotherapy for muscle-invasive bladder cancer. Cancer Res. 2010, 70, 7017–7026. [Google Scholar] [CrossRef] [PubMed]
- Sakano, S.; Ogawa, S.; Yamamoto, Y.; Nishijima, J.; Miyachika, Y.; Matsumoto, H.; Hara, T.; Matsuyama, H. ERCC1 and XRCC1 expression predicts survival in bladder cancer patients receiving combined trimodality therapy. Mol. Clin. Oncol. 2013, 1, 403–410. [Google Scholar] [CrossRef] [PubMed]
- Desai, N.B.; Scott, S.N.; Zabor, E.C.; Cha, E.K.; Hreiki, J.; Sfakianos, J.P.; Ramirez, R.; Bagrodia, A.; Rosenberg, J.E.; Bajorin, D.F.; et al. Genomic characterization of response to chemoradiation in urothelial bladder cancer. Cancer 2016, 122, 3715–3723. [Google Scholar] [CrossRef] [PubMed]
- Eustace, A.; Irlam, J.J.; Taylor, J.; Denley, H.; Agrawal, S.; Choudhury, A.; Ryder, D.; Ord, J.J.; Harris, A.L.; Rojas, A.M.; et al. Necrosis predicts benefit from hypoxia-modifying therapy in patients with high risk bladder cancer enrolled in a phase III randomised trial. Radiother. Oncol. 2013, 108, 40–47. [Google Scholar] [CrossRef] [PubMed]
- Hunter, B.A.; Eustace, A.; Irlam, J.J.; Valentine, H.R.; Denley, H.; Oguejiofor, K.K.; Swindell, R.; Hoskin, P.J.; Choudhury, A.; West, C.M. Expression of hypoxia-inducible factor-1alpha predicts benefit from hypoxia modification in invasive bladder cancer. Br. J. Cancer 2014, 111, 437–443. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, S.; Saito, K.; Koga, F.; Yokoyama, M.; Kageyama, Y.; Masuda, H.; Kobayashi, T.; Kawakami, S.; Kihara, K. C-reactive protein level predicts prognosis in patients with muscle-invasive bladder cancer treated with chemoradiotherapy. BJU Int. 2008, 101, 978–981. [Google Scholar] [CrossRef] [PubMed]
- Joseph, N.; Dovedi, S.J.; Thompson, C.; Lyons, J.; Kennedy, J.; Elliott, T.; West, C.M.; Choudhury, A. Pre-treatment lymphocytopaenia is an adverse prognostic biomarker in muscle-invasive and advanced bladder cancer. Ann. Oncol. 2016, 27, 294–299. [Google Scholar] [CrossRef] [PubMed]
- Zinkel, S.; Gross, A.; Yang, E. BCL2 family in DNA damage and cell cycle control. Cell Death Differ. 2006, 13, 1351–1359. [Google Scholar] [CrossRef] [PubMed]
- Margulis, V.; Lotan, Y.; Karakiewicz, P.I.; Fradet, Y.; Ashfaq, R.; Capitanio, U.; Montorsi, F.; Bastian, P.J.; Nielsen, M.E.; Muller, S.C.; et al. Multi-institutional validation of the predictive value of Ki-67 labeling index in patients with urinary bladder cancer. J. Natl. Cancer Inst. 2009, 101, 114–119. [Google Scholar] [CrossRef] [PubMed]
- Koh, D.M.; Collins, D.J. Diffusion-weighted MRI in the body: Applications and challenges in oncology. AJR Am. J. Roentgenol. 2007, 188, 1622–1635. [Google Scholar] [CrossRef] [PubMed]
- Mitsudomi, T.; Yatabe, Y. Epidermal growth factor receptor in relation to tumor development: EGFR gene and cancer. FEBS J. 2010, 277, 301–308. [Google Scholar] [CrossRef] [PubMed]
- Harris, A.L. Hypoxia—A key regulatory factor in tumour growth. Nat. Rev. Cancer 2002, 2, 38–47. [Google Scholar] [CrossRef] [PubMed]
- Thompson, L.H. Recognition, signaling, and repair of DNA double-strand breaks produced by ionizing radiation in mammalian cells: The molecular choreography. Mutat. Res. 2012, 751, 158–246. [Google Scholar] [CrossRef] [PubMed]
- Hanawalt, P.C.; Spivak, G. Transcription-coupled DNA repair: Two decades of progress and surprises. Nat. Rev. Mol. Cell Biol. 2008, 9, 958–970. [Google Scholar] [CrossRef] [PubMed]
- Iyer, G.; Balar, A.V.; Milowsky, M.I.; Bochner, B.H.; Dalbagni, G.; Donat, S.M.; Herr, H.W.; Huang, W.C.; Taneja, S.S.; Woods, M.; et al. Multicenter Prospective Phase II Trial of Neoadjuvant Dose-Dense Gemcitabine Plus Cisplatin in Patients with Muscle-Invasive Bladder Cancer. J. Clin. Oncol. 2018, 36, 1949–1956. [Google Scholar] [CrossRef] [PubMed]
- Plimack, E.R.; Dunbrack, R.L.; Brennan, T.A.; Andrake, M.D.; Zhou, Y.; Serebriiskii, I.G.; Slifker, M.; Alpaugh, K.; Dulaimi, E.; Palma, N.; et al. Defects in DNA Repair Genes Predict Response to Neoadjuvant Cisplatin-based Chemotherapy in Muscle-invasive Bladder Cancer. Eur. Urol. 2015, 68, 959–967. [Google Scholar] [CrossRef] [PubMed]
- Teo, M.Y.; Bambury, R.M.; Zabor, E.C.; Jordan, E.; Al-Ahmadie, H.; Boyd, M.E.; Bouvier, N.; Mullane, S.A.; Cha, E.K.; Roper, N.; et al. DNA Damage Response and Repair Gene Alterations Are Associated with Improved Survival in Patients with Platinum-Treated Advanced Urothelial Carcinoma. Clin. Cancer Res. 2017, 23, 3610–3618. [Google Scholar] [CrossRef] [PubMed]
- Hoskin, P.J.; Rojas, A.M.; Bentzen, S.M.; Saunders, M.I. Radiotherapy with concurrent carbogen and nicotinamide in bladder carcinoma. J. Clin. Oncol. 2010, 28, 4912–4918. [Google Scholar] [CrossRef] [PubMed]
- Cancer Genome Atlas Research Network. Comprehensive molecular characterization of urothelial bladder carcinoma. Nature 2014, 507, 315–322. [Google Scholar] [CrossRef] [PubMed]
- Choi, W.; Porten, S.; Kim, S.; Willis, D.; Plimack, E.R.; Hoffman-Censits, J.; Roth, B.; Cheng, T.; Tran, M.; Lee, I.L.; et al. Identification of distinct basal and luminal subtypes of muscle-invasive bladder cancer with different sensitivities to frontline chemotherapy. Cancer Cell 2014, 25, 152–165. [Google Scholar] [CrossRef] [PubMed]
- Sjodahl, G.; Lovgren, K.; Lauss, M.; Patschan, O.; Gudjonsson, S.; Chebil, G.; Aine, M.; Eriksson, P.; Mansson, W.; Lindgren, D.; et al. Toward a molecular pathologic classification of urothelial carcinoma. Am. J. Pathol. 2013, 183, 681–691. [Google Scholar] [CrossRef] [PubMed]
- Bellmunt, J.; de Wit, R.; Vaughn, D.J.; Fradet, Y.; Lee, J.L.; Fong, L.; Vogelzang, N.J.; Climent, M.A.; Petrylak, D.P.; Choueiri, T.K.; et al. Pembrolizumab as Second-Line Therapy for Advanced Urothelial Carcinoma. N. Engl. J. Med. 2017, 376, 1015–1026. [Google Scholar] [CrossRef] [PubMed]
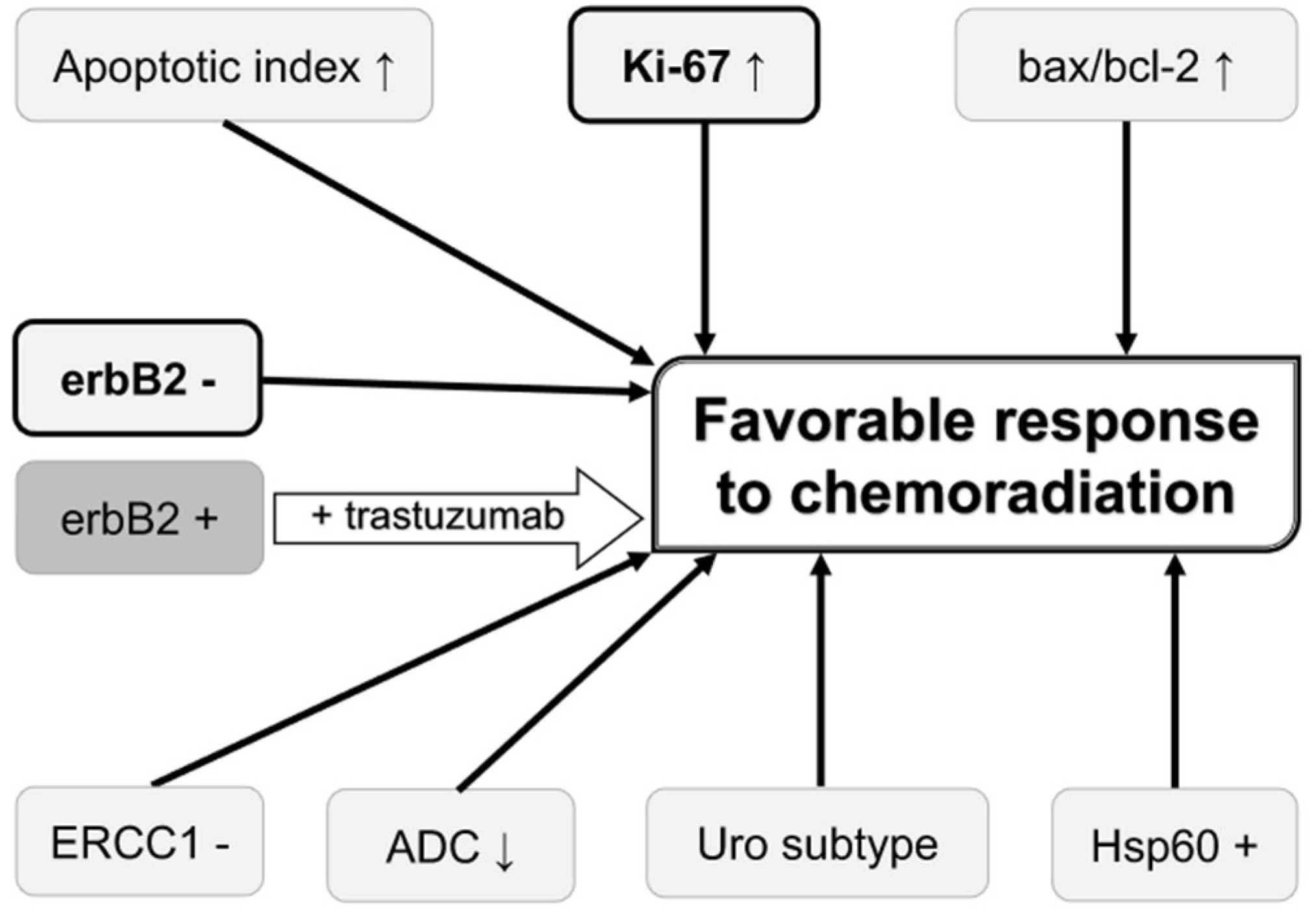
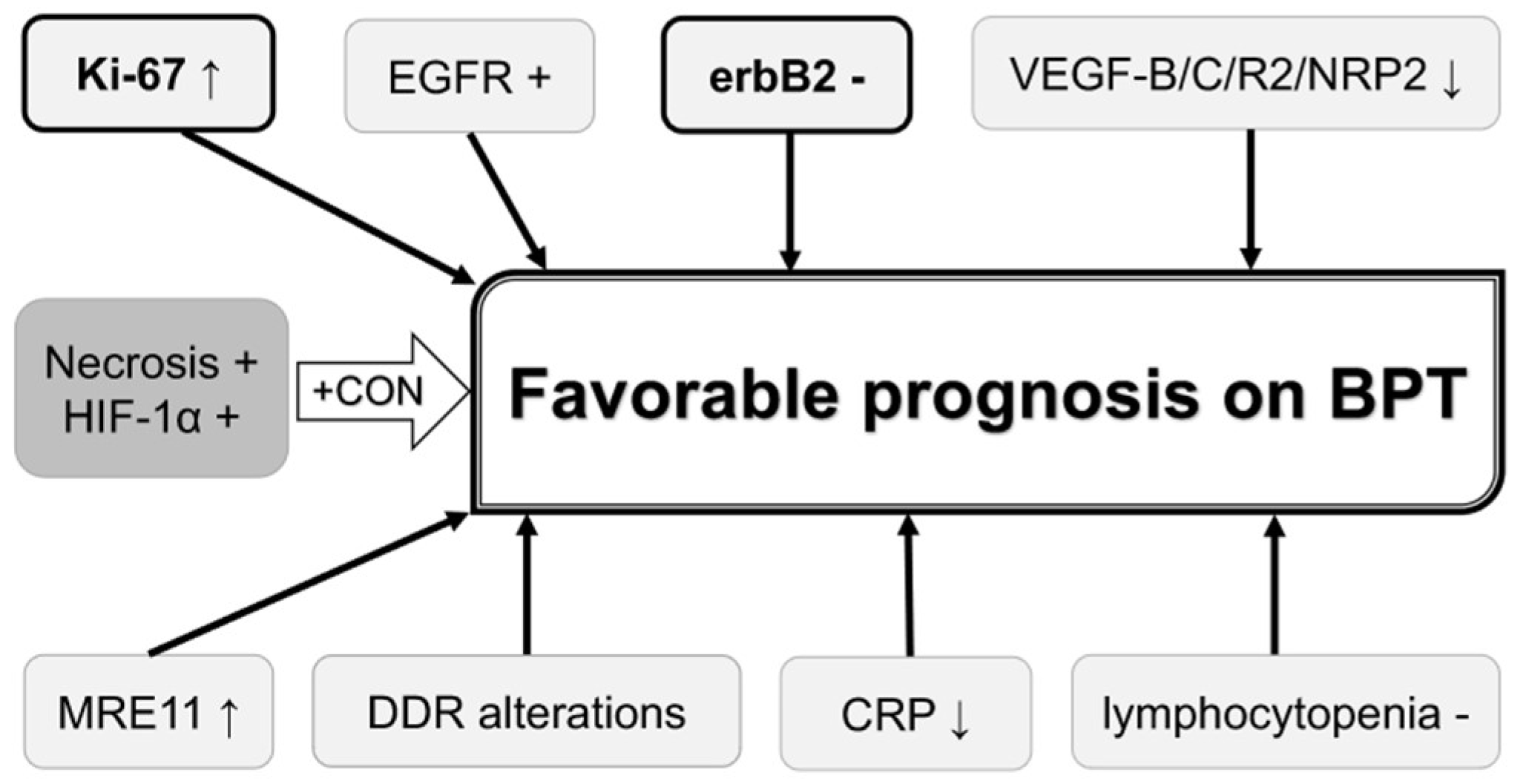
| Biomarkers | Samples Used (No. Patients) | Chemoradiation Regimen | Associations with Response | Study Type | Reference |
|---|---|---|---|---|---|
| Apoptosis-related | |||||
| Apoptotic index | Tumor tissues (n = 70) | RT 59.4 Gy + cisplatin | Higher apoptotic index was associated with a higher CR rate (86% vs. 57%, p = 0.02) | Retrospective | [22] |
| bax/bcl-2 ratio | Tumor tissues (n = 62) | RT 40.5 Gy (median) + cisplatin | Higher Bax/Bcl-2 ratio was associated with a higher CR rate (p = 0.029) | Retrospective | [23] |
| Cell proliferation-related | |||||
| Ki-67 LI | Tumor tissues (n = 70) | RT 59.4 Gy + cisplatin | Higher Ki-67 LI was associated with a higher CR rate (86% vs. 57%, p = 0.02) | Retrospective | [22] |
| Ki-67 LI | Tumor tissues (n = 94) | RT 40 Gy + cisplatin, 69 (73%) underwent partial or salvage radical cystectomy | Higher Ki-67 LI (continuous variable) was associated with a higher CR rate (p = 0.0004) | Retrospective | [24] |
| ADC value | MRI (n = 23) | RT 40 Gy + cisplatin | Sensitivity/specificity/accuracy = 92/90/91% when ADC < 0.74 × 10−3 mm2/s | Retrospective | [25] |
| RTKs | |||||
| erbB2 | Tumor tissues (n = 55) | RT 40 Gy + cisplatin + other agents | CR rates, 50% vs. 81% for positive vs. negative (p = 0.026) | Retrospective | [26] |
| erbB2 | Tumor tissues (n = 119) | RT 40 Gy + cisplatin | CR rates, 29% vs. 53% for positive vs. negative (p = 0.01) | Retrospective | [27] |
| erbB2 | Tumor tissues (n = 66) | RT 64.8 Gy + paclitaxel with (group 1: erbB2+) or without trastuzumab (group 2: erbB2-) | CR rates, 72% for group 1 and 68% for group 2 | Prospective | [28] |
| DDR-related | |||||
| ERCC1 | Tumor tissues (n = 22) | RT 40-66 Gy + cisplatin or nedaplatin | CR rates, 25% vs. 86% for positive vs. negative (p = 0.008) | Retrospective | [29] |
| Molecular subtype | |||||
| Molecular subtype | Tumor tissues (n = 118) | RT 40 Gy + cisplatin | CR rates, 52%/45%/15% for GU/SCC-like/Uro (p < 0.001) | Retrospective | [30] |
| Others | |||||
| Hsp60 | Tumor tissues (n = 54) | RT 40 Gy + cisplatin | Positive Hsp60 was associated with better response (p = 0.05) | Retrospective | [31] |
| Biomarkers | Samples Used (No. Patients) | Chemoradiation Regimen | Associations with Prognosis | Study Type | Reference |
|---|---|---|---|---|---|
| Cell proliferation-related | |||||
| Ki-67LI | Tumor tissues (n = 70) | RT 59.4 Gy + cisplatin | Better CSS with preserved bladder for higher Ki-67 LI (50% vs. 36% at 5-year, p = 0.04) | Retrospective | [22] |
| Ki-67 LI | Tumor tissues (n = 62) | RT 40.5 Gy (median) + cisplatin | Worse CSS for high Ki-67 LI of > 20% (p = 0.014) | Retrospective | [23] |
| Ki-67 LI | Tumor tissues (n = 94) | RT 40 Gy + cisplatin, 69 (73%) underwent partial or salvage radical cystectomy | Better CSS for high Ki-67 LI of > 20% (HR 0.3, p = 0.01) | Retrospective | [24] |
| RTKs | |||||
| EGFR | Tumor tissues (n = 73) | RT 40 Gy + cisplatin + other agents | Better CSS for positive EGFR (p = 0.042) | Retrospective | [26] |
| erbB2 | Tumor tissues (n = 119) | RT 40 Gy + cisplatin | Worse CSS for erbB2 overexpression (56% vs. 87%, p = 0.001) | Retrospective | [27] |
| VEGF-B/C and VEGFR2 | Tumor tissues (n = 43) | RT 64.8 Gy + cisplatin + other agents | Worse OS for high VEGF-B/C/R2 expression (p = 0.01-0.02), higher distant failure rate for high VEGF-R2 expression (p = 0.01) | Retrospective | [32] |
| VEGF-C/NRP2 | Tumor tissues (n = 247) | RT 56.3 Gy + cisplatin | Worse OS for high NRP2 or VEGFC expression (HR 4.25, p = 0.023) | Retrospective | [33] |
| DDR-related | |||||
| MRE11 | Tumor tissues (n = 179) | RT 55 Gy | Better CSS for high MRE11 expression (HR 0.36, p = 0.01) | Retrospective | [34] |
| ERCC1/XRCC1 | Tumor tissues (n = 157) | RT 48.6 Gy (median) + cisplatin | Better CSS for positive ERCC1 or XRCC1 (HR 0.64, p = 0.024) | Retrospective | [35] |
| DDR alterations | Tumor tissues (n = 48) | RT or chemoradiation (details unavailable) | Trend for better RFS for the presence of DDR alterations (HR 0.37, p = 0.07) | Retrospective | [36] |
| Hypoxia-related | |||||
| Necrosis | Tumor tissues (n = 220) | RT vs. RT + CON | The presence of necrosis predicted better OS for RT + CON than RT alone (HR 0.43, p = 0.004) | Retrospective | [37] |
| HIF-1α | Tumor tissues (n = 137) | RT vs. RT + CON | Positive HIF-1α predicted better DFS for RT + CON than RT alone (HR 0.48, p = 0.02) | Retrospective | [38] |
| Others | |||||
| CRP | Serum (n = 88) | RT 40 Gy + cisplatin | Worse CSS for high CRP of > 0.5 mg/dL (HR 1.8, p = 0.046) | Retrospective | [39] |
| Lymphocytopenia | Blood (n = 74) | RT 52.5 Gy + gemcitabine | Worse RFS for lymphocytopenia of < 1.5 × 109/L (HR 3.9, p = 0.003) | Retrospective | [40] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Koga, F.; Takemura, K.; Fukushima, H. Biomarkers for Predicting Clinical Outcomes of Chemoradiation-Based Bladder Preservation Therapy for Muscle-Invasive Bladder Cancer. Int. J. Mol. Sci. 2018, 19, 2777. https://doi.org/10.3390/ijms19092777
Koga F, Takemura K, Fukushima H. Biomarkers for Predicting Clinical Outcomes of Chemoradiation-Based Bladder Preservation Therapy for Muscle-Invasive Bladder Cancer. International Journal of Molecular Sciences. 2018; 19(9):2777. https://doi.org/10.3390/ijms19092777
Chicago/Turabian StyleKoga, Fumitaka, Kosuke Takemura, and Hiroshi Fukushima. 2018. "Biomarkers for Predicting Clinical Outcomes of Chemoradiation-Based Bladder Preservation Therapy for Muscle-Invasive Bladder Cancer" International Journal of Molecular Sciences 19, no. 9: 2777. https://doi.org/10.3390/ijms19092777
APA StyleKoga, F., Takemura, K., & Fukushima, H. (2018). Biomarkers for Predicting Clinical Outcomes of Chemoradiation-Based Bladder Preservation Therapy for Muscle-Invasive Bladder Cancer. International Journal of Molecular Sciences, 19(9), 2777. https://doi.org/10.3390/ijms19092777








