Spot-Bonding and Full-Bonding Techniques for Fiber Reinforced Composite (FRC) and Metallic Retainers
Abstract
1. Introduction
2. Results
3. Discussion
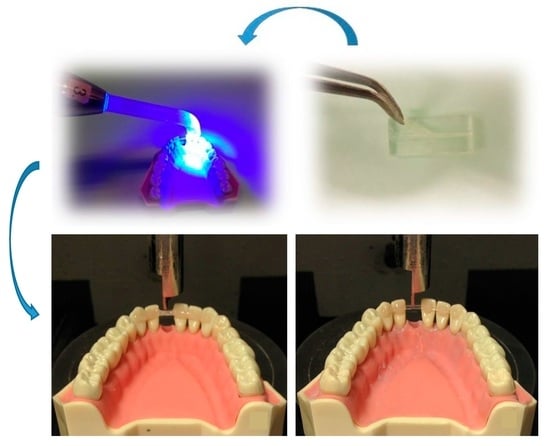
4. Materials and Methods
- -SFS: Stainless steel Flat Spot-bonded
- -SFF: Stainless steel Flat Full-bonded
- -SRS: Stainless steel Round Spot-bonded
- -SRF: Stainless steel Round Full-bonded
- -FS: FRC Spot-bonded
- -FF: FRC Full-bonded
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Goldberg, A.J.; Burstone, C.J. The use of continuous fiber reinforcement in dentistry. Dent. Mater. 1992, 8, 197–202. [Google Scholar] [CrossRef]
- Vallittu, P.K.; Lassila, V.P. Reinforcement of acrylic resin denture base material with metal or fibre strengtheners. J. Oral Rehabil. 1992, 19, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Nayar, S.; Ganesh, R.; Santhosh, S. Fiber reinforced composites in prosthodontics—A systematic review. J. Pharm. Bioallied Sci. 2015, 7 (Suppl. 1), S220–S222. [Google Scholar] [CrossRef] [PubMed]
- Freilich, M.A.; Karmaker, A.C.; Burstone, C.J.; Goldberg, A.J. Development and clinical applications of a light-polymerized fiber-reinforced composite. J. Prosthet. Dent. 1998, 80, 311–318. [Google Scholar] [CrossRef]
- Kanie, T.; Arikawa, H.; Fujii, K.; Ban, S. Light-curing reinforcement for denture base resin using a glass fiber cloth pre-impregnated with various urethane oligomers. Dent. Mater. J. 2004, 23, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Scribante, A.; Massironi, S.; Pieraccini, G.; Vallittu, P.; Lassila, L.; Sfondrini, M.F.; Gandini, P. Effects of nanofillers on mechanical properties of fiber-reinforced composites polymerized with light-curing and additional postcuring. J. Appl. Biomater. Funct. Mater. 2015, 13, e296–e299. [Google Scholar] [CrossRef] [PubMed]
- Sewón, L.A.; Ampula, L.; Vallittu, P.K. Rehabilitation of a periodontal patient with rapidly progressing marginal alveolar bone loss: 1-year follow-up. J. Clin. Periodontol. 2000, 27, 615–619. [Google Scholar] [CrossRef] [PubMed]
- Perea, L.; Matinlinna, J.P.; Tolvanen, M.; Lassila, L.V.; Vallittu, P.K. Fiber-reinforced composite fixed dental prostheses with various pontics. J. Adhes. Dent. 2014, 16, 161–168. [Google Scholar] [PubMed]
- Vallittu, P.K.; Sevelius, C. Resin-bonded, glass fiber reinforced composite fixed partial dentures—A clinical study. J. Prosthet. Dent. 2000, 84, 413–418. [Google Scholar] [CrossRef] [PubMed]
- Saker, S.; Özcan, M. Retentive strength of fiber-reinforced composite posts with composite resin cores: Effect of remaining coronal structure and root canal dentin conditioning protocols. J. Prosthet. Dent. 2015, 114, 856–861. [Google Scholar] [CrossRef] [PubMed]
- Le Bell, A.-M.; Tanner, J.; Lassila, L.V.J.; Kangasniemi, I.; Vallittu, P.K. Depth of light initiated polymerization of glass fiber reinforced composite in a simulated root canal. Int. J. Prosthodont. 2003, 16, 403–408. [Google Scholar] [PubMed]
- LeBell, A.-M.; Tanner, J.; Lassila, L.V.J.; Kangasniemi, I.; Vallittu, P.K. Bonding of composite resin luting cement to fibre-reinforced composite root canal post. J. Adhes. Dent. 2004, 6, 319–325. [Google Scholar]
- Abouelleil, H.; Pradelle, N.; Villat, C.; Attik, N.; Colon, P.; Grosgogeat, B. Comparison of mechanical properties of a new fiber reinforced composite and bulk filling composites. Restor. Dent. Endod. 2015, 40, 262–670. [Google Scholar] [CrossRef] [PubMed]
- Garoushi, S.; Vallittu, P.K.; Lassila, L.V.J. Fracture toughness, compressive strength and load-bearing capacity of short glass fiber-reinforced composite resin. Chin. J. Dent. Res. 2011, 14, 15–19. [Google Scholar] [PubMed]
- Garoushi, S.; Lassila, L.V.J.; Vallittu, P.K. Influence of nanometer scale particulate fillers on some properties of microfilled composite resin. Dent. Mater. 2011, 22, 1645–1651. [Google Scholar] [CrossRef] [PubMed]
- Garoushi, S.; Kaleem, M.; Shinya, A.; Vallittu, P.K.; Satterwaite, J.D.; Watts, D.C.; Lassila, L.V.J. Static and dynamic creep of experimental short fiber-reinforced composite resin. Dent. Mater. J. 2012, 31, 737–741. [Google Scholar] [CrossRef] [PubMed]
- Akin, H.; Turgut, M.; Coskun, M.E. Restoration of an anterior edentulous space with a unique glass fiber-reinforced composite removable partial denture: A case report. J. Esthet. Restor. Dent. 2007, 19, 193–197. [Google Scholar] [CrossRef] [PubMed]
- Narva, K.; Vallittu, P.K.; Yli-Urpo, A. Clinical survey of acrylic resin removable denture repairs with glass-fiber reinforcement. Int. J. Prosthodont. 2001, 14, 219–224. [Google Scholar] [PubMed]
- Chafaie, A.; Dahan, S.; Le Gall, M. Fiber-reinforced composite anterior bridge in pediatric traumatology: Clinical considerations. Int. Orthod. 2013, 11, 445–456. [Google Scholar]
- Sfondrini, M.F.; Fraticelli, D.; Castellazzi, L.; Scribante, A.; Gandini, P. Clinical evaluation of bond failures and survival between mandibular canine-to-canine retainers made of flexible spiral wire and fiber-reinforced composite. J. Clin. Exp. Dent. 2014, 6, e145–e149. [Google Scholar] [CrossRef] [PubMed]
- Bayani, S.; Heravi, F. Application of fiber reinforced composites in adjunctive orthodontics. Int. J. Orthod. 2012, 23, 11–13. [Google Scholar]
- Cacciafesta, V.; Sfondrini, M.F.; Lena, A.; Scribante, A.; Vallittu, P.K.; Lassila, L.V. Force levels of fiber-reinforced composites and orthodontic stainless steel wires: A 3-point bending test. Am. J. Orthod. Dentofac. Orthop. 2008, 133, 410–413. [Google Scholar] [CrossRef] [PubMed]
- Sfondrini, M.F.; Gandini, P.; Tessera, P.; Vallittu, P.K.; Lassila, L.; Scribante, A. Bending properties of fiber reinforced composites (FRC) retainers bonded with spot-composite coverage. Biomed. Res. Int. 2017, 2017, 8469090. [Google Scholar]
- Annousaki, O.; Zinelis, S.; Eliades, G.; Eliades, T. Comparative analysis of the mechanical properties of fiber and stainless steel multistranded wires used for lingual fixed retention. Dent. Mater. 2017, 33, e205–e211. [Google Scholar] [CrossRef] [PubMed]
- Oshagh, M.; Heidary, S.; Dehghani Nazhvani, A.; Koohpeima, F.; Koohi Hosseinabadi, O. Evaluation of histological impacts of three types of orthodontic fixed retainers on periodontium of rabbits. J. Dent. 2014, 15, 104–111. [Google Scholar]
- Angelopoulou, M.V.; Koletsi, D.; Vadiakas, G.; Halazonetis, D.J. Induced ankylosis of a primary molar for skeletal anchorage in the mandible as alternative to mini-implants. Prog. Orthod. 2015, 16, 18. [Google Scholar] [CrossRef] [PubMed]
- Qi, Y.; Fang, H.; Liu, W. Experimental Study of the Bending Properties and Deformation Analysis of Web-Reinforced Composite Sandwich Floor Slabs with Four Simply Supported Edges. PLoS ONE 2016, 11, e0149103. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.; Chen, H.; Cen, L.; Wang, J. Influence of abutment tooth position and adhesive point dimension on the rigidity of a dental trauma wire-composite splint. Dent. Traumatol. 2016, 32, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Schmage, P.; Nergiz, I.; Platzer, U.; Pfeiffer, P. Yield strength of fiber-reinforced composite posts with coronal retention. J. Prosthet. Dent. 2009, 101, 382–387. [Google Scholar] [CrossRef]
- Alavi, S.; Mamavi, T. Evaluation of load-deflection properties of fiber-reinforced composites and its comparison with stainless steel wires. Dent. Res. J. 2014, 11, 234–239. [Google Scholar]
- Chen, J.H.; Li, W.; Zheng, Y.P. Study on relationship between bent angles of dental fiber reinforced composites posts and their flexural properties. Zhonghua Kou Qiang Yi Xue Za Zhi 2006, 41, 331–332. [Google Scholar] [PubMed]
- Cacciafesta, V.; Sfondrini, M.F.; Lena, A.; Scribante, A.; Vallittu, P.K.; Lassila, L.V. Flexural strengths of fiber-reinforced composites polymerized with conventional light-curing and additional postcuring. Am. J. Orthod. Dentofac. Orthop. 2007, 132, 524–527. [Google Scholar] [CrossRef] [PubMed]
- Sfondrini, M.F.; Massironi, S.; Pieraccini, G.; Scribante, A.; Vallittu, P.K.; Lassila, L.V.; Gandini, P. Flexural strengths of conventional and nanofilled fiber-reinforced composites: A three-point bending test. Dent. Traumatol. 2014, 30, 32–35. [Google Scholar] [CrossRef] [PubMed]
- Scribante, A.; Sfondrini, M.F.; Broggini, S.; D'Allocco, M.; Gandini, P. Efficacy of Esthetic Retainers: Clinical Comparison between Multistranded Wires and Direct-Bond Glass Fiber-Reinforced Composite Splints. Int. J. Dent. 2011, 2011, 548356. [Google Scholar] [CrossRef] [PubMed]
- Sobouti, F.; Rakhshan, V.; Saravi, M.G.; Zamanian, A.; Shariati, M. Two-year survival analysis of twisted wire fixed retainer versus spiral wire and fiber-reinforced composite retainers: A preliminary explorative single-blind randomized clinical trial. Korean J. Orthod. 2016, 46, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Vallittu, P.K. Unpolymerized surface layer of autopolymerizing polymethyl methacrylate resin. J. Oral Rehabil. 1999, 26, 208–212. [Google Scholar] [CrossRef] [PubMed]
- Bijelic-Donova, J.; Garoushi, S.; Vallittu, P.K.; Lassila, L.V.J. Oxygen inhibition layer of composite resins: The effect of layer thickness and surface layer treatmenton the interlayer bond strength. Eur. J. Oral Sci. 2015, 123, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Foek, D.L.; Yetkiner, E.; Ozcan, M. Fatigue resistance, debonding force, and failure type of fiber-reinforced composite, polyethylene ribbon-reinforced, and braided stainless steel wire lingual retainers in vitro. Korean J. Orthod. 2013, 43, 186–192. [Google Scholar] [CrossRef] [PubMed]
- Frese, C.; Decker, C.; Rebholz, J.; Stucke, K.; Staehle, H.J.; Wolff, D. Original and repair bond strength of fiber-reinforced composites in vitro. Dent. Mater. 2014, 30, 456–462. [Google Scholar] [CrossRef] [PubMed]
- Scribante, A.; Cacciafesta, V.; Sfondrini, M.F. Effect of various adhesive systems on the shear bond strength of fiber-reinforced composite. Am. J. Orthod. Dentofac. Orthop. 2006, 130, 224–227. [Google Scholar] [CrossRef] [PubMed]
- Yanagida, H.; Tanoue, N.; Minesaki, Y.; Kamasaki, Y.; Fujiwara, T.; Minami, H. Effects of polymerization method on flexural and shear bond strengths of a fiber-reinforced composite resin. J. Oral Sci. 2017, 59, 13–21. [Google Scholar] [CrossRef] [PubMed]

| Name | Flat Stainless Steel Wire | Round Stainless Steel Wire | Fiber Reinforced Composite |
|---|---|---|---|
| Bond-a-Braid | Penta One 0155 | FRC Ortho | |
| Manufacturer | Reliance | Masel | StickTech |
| Material | Stainless steel | Stainless steel | E-glass fiber 15 μm |
| Dimensions | 0.673 mm (w) × 0.268 mm (h) | Diameter: 0.394 mm | Diameter: 0.75 mm |
| Unit Amount | 8 wires | 5 wires | 1000 fibers |
| Design | Ribbon arch | Coaxial | Unidirectional fibre bundle |
| Group | Code | Material | Shape | Bonding | Deflection (mm) | Mean | SD | Min | Mdn | Max | Lower CI | Upper CI | Post-Hoc * |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
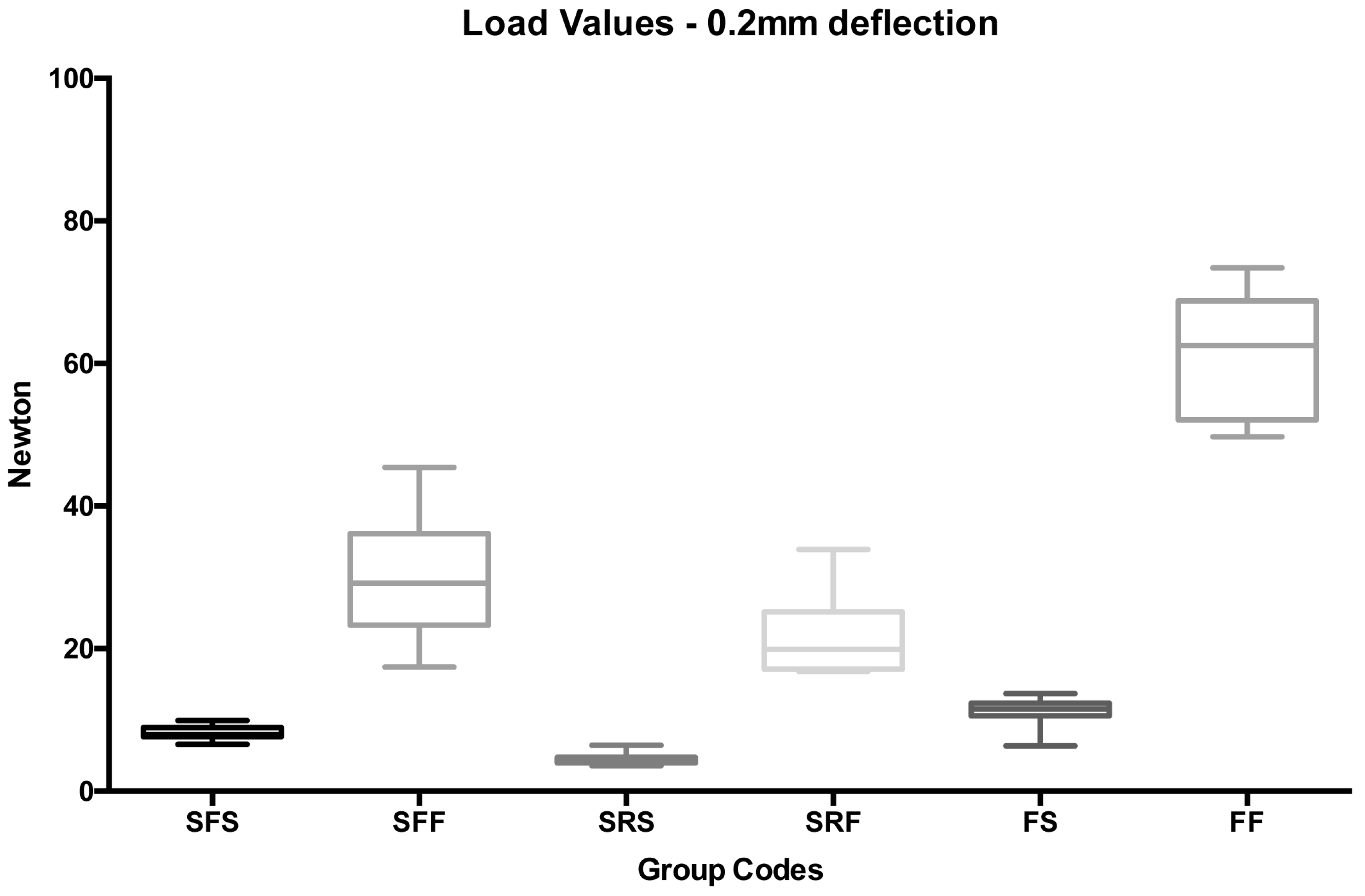
| 1 | SFS | Stainless steel | Flat | Spot bonded | 0.2 | 8.20 | 1.03 | 6.57 | 7.93 | 9.94 | 7.48 | 9.23 | A |
| 2 | SFF | Stainless steel | Flat | Full bonded | 0.2 | 30.18 | 8.91 | 17.43 | 29.17 | 45.41 | 24.01 | 39.10 | B, I |
| 3 | SRS | Stainless steel | Round | Spot bonded | 0.2 | 4.60 | 0.86 | 3.60 | 4.59 | 6.43 | 4.00 | 5.46 | A |
| 4 | SRF | Stainless steel | Round | Full bonded | 0.2 | 21.79 | 5.88 | 16.83 | 19.90 | 33.93 | 17.71 | 27.67 | B |
| 5 | FS | FRC | - | Spot bonded | 0.2 | 11.13 | 2.16 | 6.37 | 11.50 | 13.69 | 9.63 | 13.28 | A, C |
| 6 | FF | FRC | - | Full bonded | 0.2 | 61.70 | 8.75 | 49.72 | 62.53 | 73.40 | 55.64 | 70.45 | D, G, H |
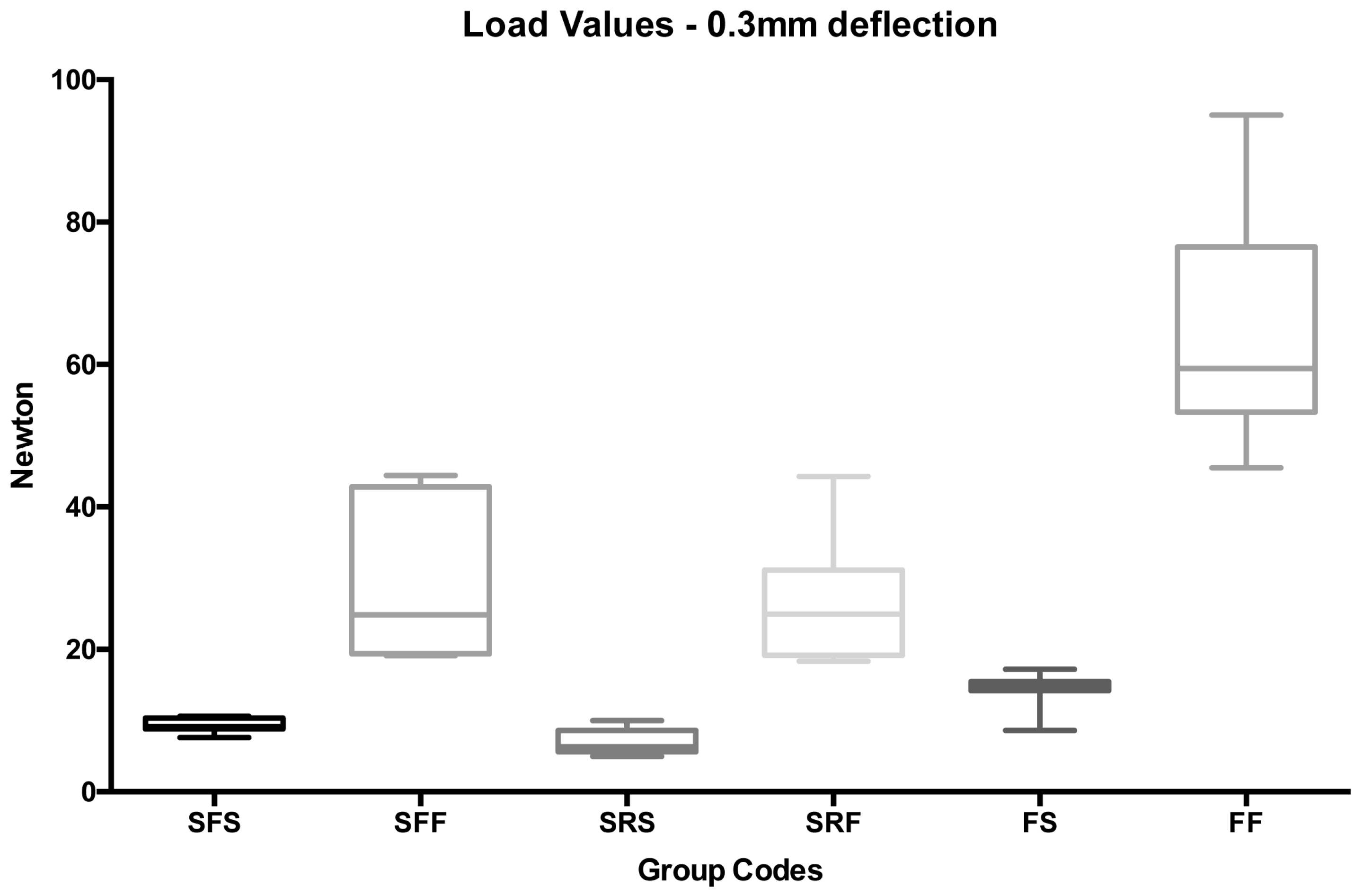
| 7 | SFS | Stainless steel | Flat | Spot bonded | 0.3 | 9.34 | 1.00 | 7.63 | 9.12 | 10.59 | 8.65 | 10.35 | A, C |
| 8 | SFF | Stainless steel | Flat | Full bonded | 0.3 | 29.37 | 11.16 | 19.12 | 24.84 | 44.43 | 21.64 | 40.53 | B, I |
| 9 | SRS | Stainless steel | Round | Spot bonded | 0.3 | 6.89 | 1.79 | 4.98 | 6.30 | 10.00 | 5.66 | 8.68 | A |
| 10 | SRF | Stainless steel | Round | Full bonded | 0.3 | 26.35 | 8.74 | 18.33 | 24.93 | 44.29 | 20.30 | 35.09 | B, C, J |
| 11 | FS | FRC | - | Spot bonded | 0.3 | 14.37 | 2.51 | 8.62 | 14.80 | 17.23 | 12.63 | 16.89 | A |
| 12 | FF | FRC | - | Full bonded | 0.3 | 64.78 | 16.29 | 45.52 | 59.42 | 95.02 | 53.49 | 81.08 | D, E, H |
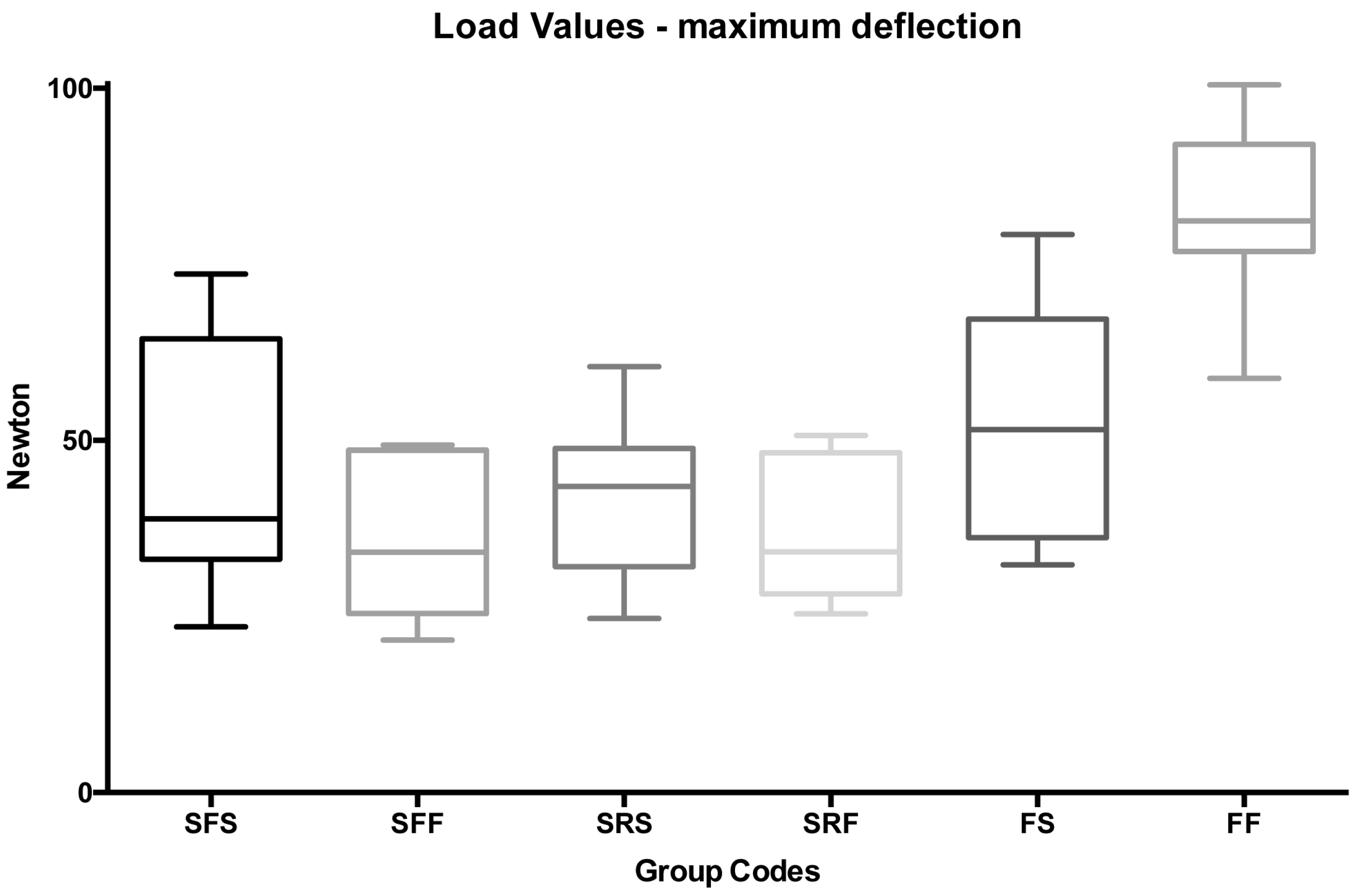
| 13 | SFS | Stainless steel | Flat | Spot bonded | Maximum Load | 46.44 | 18.21 | 23.50 | 38.88 | 73.62 | 33.82 | 64.64 | F, G, I |
| 14 | SFF | Stainless steel | Flat | Full bonded | Maximum Load | 36.17 | 11.33 | 21.66 | 34.12 | 49.32 | 28.32 | 47.50 | F, I, J |
| 15 | SRS | Stainless steel | Round | Spot bonded | Maximum Load | 41.67 | 11.40 | 24.68 | 43.45 | 60.47 | 33.77 | 53.06 | F, I, J |
| 16 | SRF | Stainless steel | Round | Full bonded | Maximum Load | 37.25 | 10.00 | 25.38 | 34.15 | 50.71 | 30.32 | 47.26 | F, I, J |
| 17 | FS | FRC | - | Spot bonded | Maximum Load | 52.20 | 16.55 | 32.30 | 51.48 | 79.19 | 40.74 | 68.75 | F, G |
| 18 | FF | FRC | - | Full bonded | Maximum Load | 81.86 | 12.56 | 58.81 | 81.15 | 100.51 | 73.16 | 94.42 | E |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scribante, A.; Gandini, P.; Tessera, P.; Vallittu, P.K.; Lassila, L.; Sfondrini, M.F. Spot-Bonding and Full-Bonding Techniques for Fiber Reinforced Composite (FRC) and Metallic Retainers. Int. J. Mol. Sci. 2017, 18, 2096. https://doi.org/10.3390/ijms18102096
Scribante A, Gandini P, Tessera P, Vallittu PK, Lassila L, Sfondrini MF. Spot-Bonding and Full-Bonding Techniques for Fiber Reinforced Composite (FRC) and Metallic Retainers. International Journal of Molecular Sciences. 2017; 18(10):2096. https://doi.org/10.3390/ijms18102096
Chicago/Turabian StyleScribante, Andrea, Paola Gandini, Paola Tessera, Pekka K. Vallittu, Lippo Lassila, and Maria Francesca Sfondrini. 2017. "Spot-Bonding and Full-Bonding Techniques for Fiber Reinforced Composite (FRC) and Metallic Retainers" International Journal of Molecular Sciences 18, no. 10: 2096. https://doi.org/10.3390/ijms18102096
APA StyleScribante, A., Gandini, P., Tessera, P., Vallittu, P. K., Lassila, L., & Sfondrini, M. F. (2017). Spot-Bonding and Full-Bonding Techniques for Fiber Reinforced Composite (FRC) and Metallic Retainers. International Journal of Molecular Sciences, 18(10), 2096. https://doi.org/10.3390/ijms18102096