Ethnobotany, Phytochemistry, and Biological Activity of Extracts and Non-Volatile Compounds from Lantana camara L. and Semisynthetic Derivatives—An Updated Review
Abstract
1. Introduction
2. Research Strategies and Literature Sources
3. Results
3.1. Ethnobotany
| Region | Country | Vernacular Name | Part of the Plant | Preparation Method | Traditional Uses | Ref. |
|---|---|---|---|---|---|---|
| Africa | Congo (Bouenza Department) | Lantana (Kunyi) | Leaves | Decoction | Antidiarrheal | [36] |
| Democratic Republic of Congo (Bukavu and Uvira) | Mwamuganga (Mashi), Mavi ya kuku (Swahili), Makereshe (Nande) | Leaves | Decoction | Antimalarial | [37] | |
| Democratic Republic of Congo (Kisantu and Mbanza-Ngungu) | Nsudi nsudi (Kikongo) | Leaves and fruits | Decoction; administered by rectal route | To treat cough by the Ntându and Ndibu ethnic groups; to treat hemorrhoids | [38] | |
| Ethiopia (Libo-Kemkem District) | NR | Leaves | Infusion | Antidiarrheal | [39] | |
| Ethiopia (Mana Angetu District) | NR | Leaves | Decoction | To treat skin infections, gonorrhea, and “evil eye” | [40] | |
| Ethiopia (Wonago Woreda) | Yewof kollo (Amharic) | Stems | Infusion | Antidiarrheal | [41] | |
| Ethiopia (Sheko District) | Michi-charo (Sheko) | Leaves | Topical | To treat “Michi”, a type of febrile illness | [42] | |
| La Réunion | Galabert, Corbeille d’or (French) | Leaves | Decoction, infusion | Antimalarial | [43] | |
| Guinea (Low, middle, upper, and forest ecological zones) | Tagani (NR) | Leaves | Decoction | Soussous, Malinké, Guerzé, Konon, and Manon ethnic groups use the plant to treat infectious diseases | [44] | |
| Kenya (Central Province) | Rûîthiki, Mûkenia (Kikuyu) | Leaves | Crushed; directly applied to the ear to treat otitis | Kikuyu ethnic group uses the plant to treat common cold by inhaling crushed leaves | [45,46] | |
| Kenya (Embu and Mbeere Districts) | Mûkenia (Kikuyu) | Leaves | Decoction | Antimalarial | [47] | |
| Kenya (Formerly: Bondo District, now Siaya County) | Nyabend winy (Luo) | Leaves and roots | Decoction | To treat cough | [48] | |
| Kenya (Msambweni District) | Mjsasa (Digo) | Leaves | Decoction | Digos, Durumas, and Kambas ethnic groups use the plant as an antimalarial | [49] | |
| Kenya (Rusinga Island and Rambira) | NR | Leaves and seeds | Burnt for fumigation | Used as a mosquito repellent | [50] | |
| Madagascar (Antsiranana) | Kalabera (NR) | Aerial parts | Decoction | To treat cough, hypertension, and fever | [51] | |
| Nigeria (Ibadan) | Wild sage (English) | Leaves | Burnt for fumigation | Used as an insect repellent | [52] | |
| Uganda (Budiope County) | Kapanga (Lusoga) | Leaves | Burnt for fumigation; decoction | Used as a mosquito repellent; antimalarial | [53] | |
| Uganda (Budondo Subcounty) | Kapanga (Lusoga), Tickberry (English) | Leaves | Burnt for fumigation | Used as a housefly and insect repellent | [54] | |
| Uganda (Otwal and Ngai Subcounties) | NR | Leaves and roots | Maceration | Used to treat ringworms, cataracts, snake bites, and epilepsy | [55] | |
| Asia | China (Xishuangbanna) | Luo-ya-min (Chinese) | Leaves | Burnt for fumigation | Used as a mosquito repellent | [56] |
| India (Assam) | Bhoot-phool (Hindi) | Bark | Burnt for fumigation; decoction | Used as an insect repellent; antimalarial | [57] | |
| India (Dharmapuri District) | NR | Leaves | Decoction, infusion | Antimalarial | [58] | |
| India (Jharkhand State) | Puttu (NR) | Leaves | Decoction, pounded | To treat several skin and respiratory diseases | [59] | |
| India (NR) | NR | Leaves | Decoction | Antiseptic, antimalarial, and antirheumatic | [60] | |
| Philippines (Paroc) | Gainis (NR) | Leaves and stems | Burnt for fumigation | Used as an insect repellent | [61] | |
| Vietnam (Hướng Hóa District) | Thục Klay (NR) | Roots | Decoction | Van Kieu ethnic group uses the plant alone or associated with roots of Mangifera indica and barks of Erythrina variegata to treat abdominal pain and diarrhea | [62] | |
| Yemen (Hajjah District) | NR | Flowers, leaves, and seeds | Burnt for fumigation | Used as an insect repellent | [63] | |
| North and Central America | Mexico (Querétaro) | Alfombrilla, Gobernadora, Ororuz (Spanish) | Leaves and stems | Decoction | To treat scorpion and insect stings; antidiarrheal and antiparasitic | [64] |
| Mexico (Chiapas) | Jøtskuy (Zoque), Cinco negritos (Spanish) | Stems | Decoction | Antidiarrheal, antiparasitic, and antirheumatic | [65] | |
| Mexico (Puebla) | Cinco negritos (Spanish) | Aerial parts | Decoction | Antidiarrheal | [66] | |
| South America | Brazil (Minas Gerais) | Cambará (Tupi) | Leaves | Decoction, infusion | To treat respiratory diseases; antipyretic and antirheumatic | [67] |
| Suriname (Pikin Slee) | NR | Leaves | Decoction | The Saramaccan Marron ethnic group uses the plant for the anti-inflammatory, antiparasitic, and depurative properties | [68] | |
| Colombia (Antioquia Department) | Venturosa (Spanish) | Stems | Decoction; steam bath | To treat snake bites | [69] | |
| The Caribbean | France (Guadeloupe) | Mille-fleurs (French) | Flowers | Decoction, infusion | To treat flu syndrome | [70] |
3.2. Phytochemistry
Triterpenoids and Steroids
| Nº | Compound Name | Molecular Formula | Molecular Weight | Skeleton Type | Part of the Plant/Solvent | Reference |
|---|---|---|---|---|---|---|
| (1) | Stigmasterol (Stigmasta-5,22-dien-3β-ol) | C29H48O | 412.702 | Stigmastane | Leaves/methanol Stems/methanol | [71] |
| (2) | 7-Oxo-β-sitosterol 3β-Hydroxy-stigmast-5-en-7-one | C29H48O2 | 428.701 | Stigmastane | Stems/methanol Roots/chloroform | [19,71] |
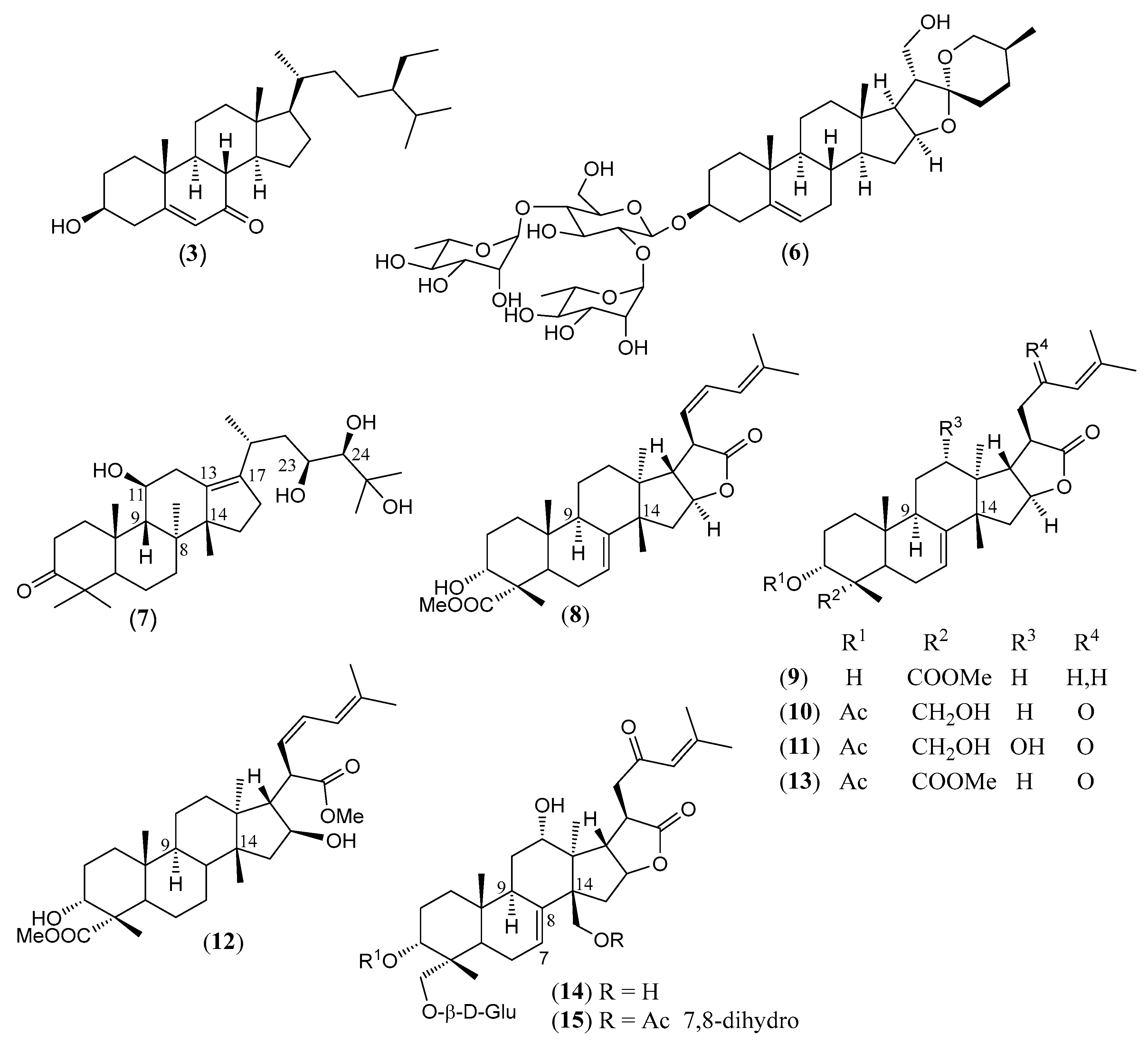
| (3) | β-Sitosterol Stigmast-5-en-3β-ol (Figure 4) | C29H50O | 414.718 | Stigmastane | Aerial parts/petroleum ether Aerial parts/96% ethanol Fruits/chloroform Leaves/methanol Stems/95% ethanol, methanol Roots/chloroform Leaves, stems, and roots/ petroleum ether | [19,72,73,74] |
| (4) | β-Sitosterol 3-O-β-D-glucopyranoside 3-O-β-D-Glucopyranosyl-stigmast-5-en-3β-ol | C35H60O6 | 576.859 | Stigmastane | Aerial parts/methanol Leaves/methanol Stems/95% ethanol, methanol | [15,71,74,75,76,77] |
| (5) | Campesterol Campest-5-en-3β-ol | C28H48O | 400.691 | Campestane | Leaves/methanol Stems/methanol | [71] |
| (6) | Yamogenin II (25S)-Spirostan-5-ene-3β,21-diol-3-O-α-L-rhamnopyranosyl-(1″33→2′)-[α-L-rhamnopyranosyl-(1‴→4′)]-β-D-glucopyranoside (Figure 4) | C45H72O17 | 885.054 | Spirostane | Leaves/methanol | [78,79] |
| Nº | Compound | Molecular Formula | Molecular Weight | Skeleton Type | Part of the Plant/Solvent | Reference |
|---|---|---|---|---|---|---|
| (7) | Alisol A | 490.725 | Protostane | Roots/chloroform | [19] | |
| (8α,9β,11β,14β,23S,24R)-11,23,24,25-tetrahydroxy-protost-13(17)-en-3-one | C30H50O5 | |||||
| (Figure 4) | ||||||
| (8) | Lantrieuphpene B (Figure 4) | C31H44O5 | 496.688 | Euphane | Aerial parts/methanol | [80] |
| (9) | Lantrieuphpene C (Figure 4) | C31H46O5 | 498.704 | Euphane | Aerial parts/methanol | [80] |
| (10) | Euphane monolactone A (Figure 4) | C32H46O6 | 526.714 | Euphane | Leaves/acetonitrile | [72] |
| (11) | Euphane monolactone B (Figure 4) | C32H46O7 | 542.713 | Euphane | Leaves/acetonitrile | [72] |
| (12) | Lantrieuphpene D (Figure 4) | C32H48O6 | 528.730 | Euphane | Aerial parts/methanol | [80] |
| (13) | Lantrieuphpene A (Figure 4) | C33H46O7 | 554.724 | Euphane | Aerial parts/methanol | [80] |
| (14) | Euphane monolactone C (Figure 4) | C40H58O14 | 762.890 | Euphane | Leaves/acetonitrile | [72,80] |
| (15) | Euphane monolactone D (Figure 4) | C42H60O15 | 804.927 | Euphane | Leaves/acetonitrile | [72] |
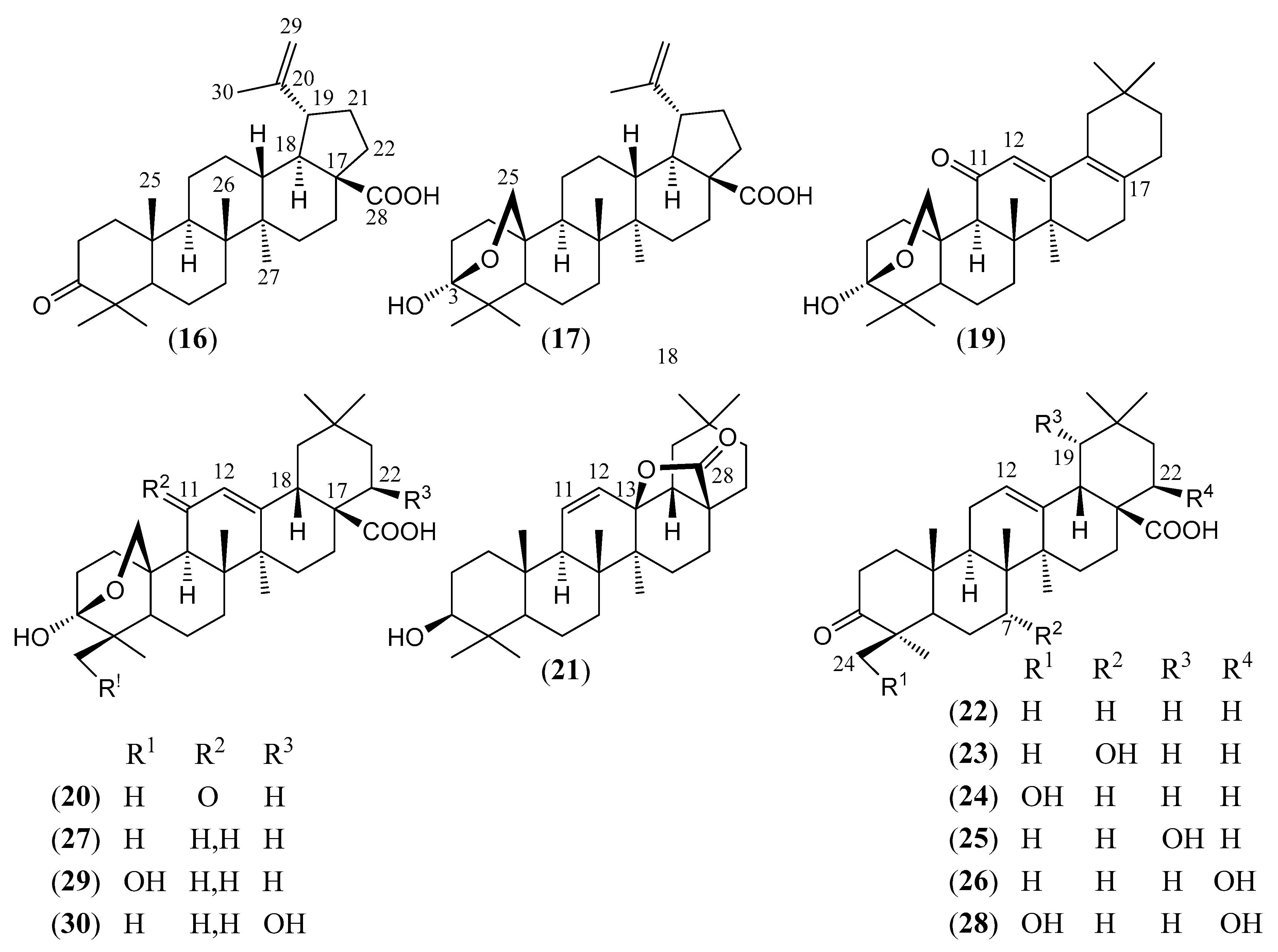
| (16) | Betulonic acid 3-oxo-lup-20(29)-en-28-oic acid (Figure 5) | C30H46O3 | 454.695 | Lupane | Leaves/methanol Stems/methanol Leaves and stems/petroleum ether | [61,71,79] |
| (17) | Lantabetulic acid 3,25-β-epoxy-3α-hydroxy-lup-20 (29)-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Lupane | Leaves and stems/petroleum ether | [81] |
| (18) | Betulinic acid 3β-hydroxy-lup-20 (29)-en-28-oic acid | C30H48O3 | 456.711 | Lupane | Aerial parts/methanol Leaves/methanol Stems/methanol Leaves and stems/petroleum ether | [71,72,78,79,82] |
| (19) | Camaradienone 3,25-β-epoxy-3α-hydroxy-28-nor-oleana-12,17-dien-11-one (Figure 5) | C29H42O3 | 438.652 | Oleanane | Aerial parts/methanol | [15] |
| (20) | Lantanoic acid 3,25-β-epoxy-3α-hydroxy-11-oxo-olean-12-en-28-oic acid (Figure 5) | C30H44O5 | 484.677 | Oleanane | Aerial parts/methanol | [83] |
| (21) | 3β-Hydroxy-olean-11-en-28,13-β-olide (Figure 5) | C30H46O3 | 454.695 | Oleanane | HD * | [74] |
| (22) | Oleanonic acid 3-Oxo-olean-12-en-28-oic acid (Figure 5) | C30H46O3 | 454.695 | Oleanane | Aerial parts/ethanol, methanol Leaves/ethanol Leaves and stems/methanol, petroleum ether Stems/ethanol, methanol Roots/ethyl acetate, methanol, n-hexane–ethyl acetate–methanol (1:1:1) | [15,71,73,74,75,76,77,78,79,81,82,83,84,85,86,87,88] |
| (23) | Camarin 7α-hydroxy-3-oxo-olean-12-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Oleanane | Aerial parts/methanol | [89,90] |
| (24) | 4-epi-Hederagonic acid 24-hydroxy-3-oxo-olean-12-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Oleanane | Aerial parts/ethanol Leaves and stems/petroleum ether | [84] |
| (25) | 19α-Hydroxy-oleanonic acid (S)-19α-hydroxy-3-oxo-olean-12-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Oleanane | Aerial parts/methanol | [80] |
| (26) | 22β-Hydroxy-oleanonic acid 22β-hydroxy-3-oxo-olean-12-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Oleanane | Aerial parts/ethanol HD Leaves/acetonitrile Leaves and stems/petroleum ether | [75,84,91,92,93,94,95,96,97] |
| (27) | Lantanolic acid 3,25-β-epoxy-3α-hydroxy-olean-12-en-28-oic acid (Figure 5) | C30H46O4 | 470.694 | Oleanane | Aerial parts/methanol HD Leaves/chloroform, methanol, petroleum ether Leaves and stems/petroleum ether Roots/ethanol | [15,75,77,79,82,84,89,90,92, 98] |
| (28) | 22β-Hydroxy-4-epi-hederagonic acid (Figure 5) | C30H46O5 | 486.693 | Oleanane | Aerial parts/ethanol | [84] |
| (29) | Lantacamaric acid A 3,25-β-epoxy-3α,24-dihydroxy-olean-12-en-28-oic acid (Figure 5) | C30H46O5 | 486.693 | Oleanane | Leaves and stems/methanol | [85] |
| (30) | Lantaninilic acid 3,25-β-epoxy-3α,22β-dihydroxy-olean-12-en-28-oic acid (Figure 5) | C30H46O5 | 486.693 | Oleanane | Aerial parts/methanol HD * Leaves and stems/methanol | [75,82,83,85,89,90] |
| (31) | Oleanolic acid 3β-hydroxy-olean-12-en-28-oic acid (Figure 6) | C30H48O3 | 456.711 | Oleanane | Aerial parts/ethanol, methanol Leaves/methanol Leaves and stems/petroleum ether Stems/ethanol, methanol Roots/ethanol, ethyl acetate, (52.5% methanol/47.5% ethyl acetate), (60% chloroform/40% methanol), n-hexane–ethyl acetate–methanol (1:1:1) | [15,19,74,75,76,77,79,80,82,84,86,87,90,91,98,99,100,101,102] |
| (32) | 22β-Hydroxy-oleanolic acid 3β,22β-dihydroxy-olean-12-en-28-oic acid (Figure 6) | C30H48O4 | 472.710 | Oleanane | Aerial parts/ethanol HD * Roots/ethanol | [84,95,96] |
| (33) | Methyl lantanoate methyl 3,25-β-epoxy-3α-hydroxy-11-oxo-olean-12-en-28-oate (Figure 6) | C31H46O5 | 498.704 | Oleanane | HD * | [83] |
| (34) | 21,22-β-Epoxy-3β-hydroxy-olean-12-en-28-oic acid, isolated as Methyl 21,22-β-epoxy-3β-hydroxy-olean-12-en-28-oate (Figure 6) | C31H48O4 | 484.721 | Oleanane | Roots/n-hexane–ethyl acetate–methanol (1:1:1) | [74] |
| (35) | Methyl 22β-hydroxy-oleanonate methyl 22β-hydroxy-3-oxo-olean-12-en-28-oate (Figure 6) | C31H48O4 | 484.721 | Oleanane | HD * | [93,94] |
| (36) | Methyl lantaninilate methyl 3,25-β-epoxy-3α,22β-dihydroxy-olean-12-en-28-oate (Figure 6) | C31H48O5 | 500.720 | Oleanane | HD * | [75] |
| (37) | 22β-Acetyloxy-oleanonic acid 22β-acetyloxy-3-oxo-olean-12-en-28-oic acid (Figure 6) | C32H48O5 | 512.731 | Oleanane | HD * | [94] |
| (38) | Lantanone 3β-acetyloxy-11-oxo-olean-12-en-28-oic acid (Figure 6) | C32H48O5 | 512.731 | Oleanane | Aerial parts/ethanol | [101] |
| (39) | Methyl 3,25-β-epoxy-3α-methoxy-22-oxo-olean-12-en-28-oate (Figure 6) | C32H48O5 | 512.731 | Oleanane | HD * | [103] |
| (40) | 22β-Acetyloxy-4-epi-hederagonic acid (Figure 6) | C32H48O6 | 528.730 | Oleanane | Aerial parts/ethanol | [104] |
| (41) | Lancamarinic acid 22β-acetyloxy-3,25-β-epoxy-3α-hydroxy-olean-12-en-28-oic acid (Figure 6) | C32H48O6 | 528.730 | Oleanane | Aerial parts/methanol | [105] |
| (42) | Lancamarolide 22β-acetyloxy-3,25-β-epoxy-3α,12α-dihydroxyolean-28,13-β-olide (Figure 6) | C32H48O7 | 544.729 | Oleanane | Aerial parts/methanol | [82] |
| (43) | Lancamaric acid 3,25-β-epoxy-3α-ethoxy-olean-12-en-28-oic acid (Figure 6) | C32H50O4 | 498.748 | Oleanane | Aerial parts/methanol | [85] |
| (44) | Oleanolic acid 3-O-acetate 3β-acetyloxy-olean-12-en-28-oic acid (Figure 6) | C32H50O4 | 498.748 | Oleanane | Aerial parts/methanol HD * Roots/n-hexane–ethyl acetate–methanol (1:1:1) | [74,77,102,106] |
| (45) | Methyl 22β-acetyloxy-oleanonate methyl 22β-acetyloxy-3-oxo-olean-12-en-28-oate (Figure 6) | C33H50O5 | 526.758 | Oleanane | HD * | [94] |
| (46) | 22β-Propanoyloxy-oleanonic acid 22β-propanoyloxy-3-oxo-olean-12-en-28-oic acid (Figure 6) | C33H50O5 | 526.758 | Oleanane | HD * | [94] |
| (47) | Methyl 22-O-acetyl-lantaninilate methyl 22β-acetyloxy-3,25-β-epoxy-3α-hydroxy-olean-12-en-28-oate (Figure 6) | C33H50O6 | 542.757 | Oleanane | HD * | [103,107] |
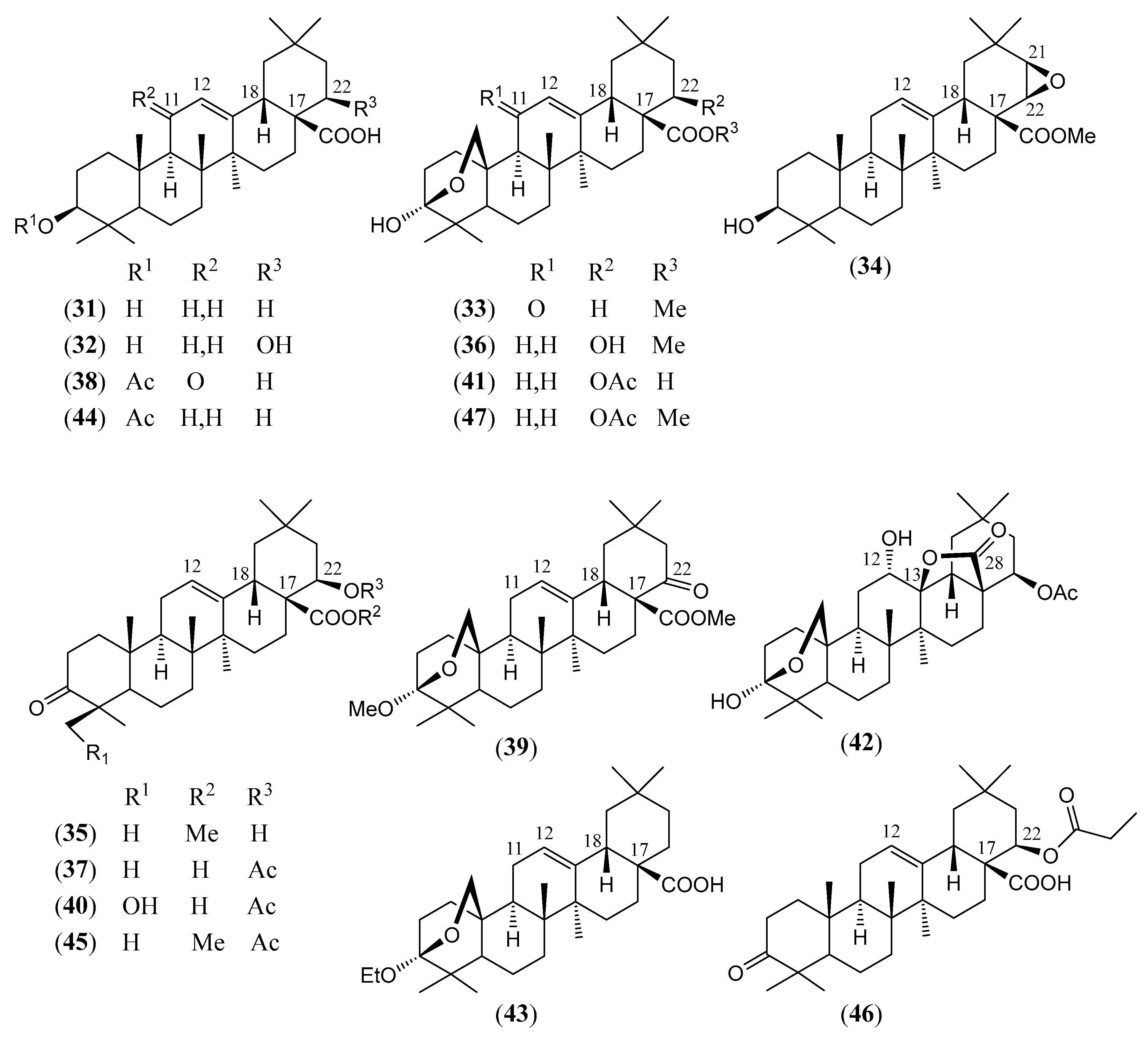
| (48) | Lantadienone 22β-angelyloxy-3,25-β-epoxy-3α-hydroxy-28-nor-oleana-12,17-dien-11-one (Figure 7) | C34H48O5 | 536.753 | Oleanane | Aerial parts/methanol | [15] |
| (49) | Lantigdienone 3,25-β-epoxy-3α-hydroxy-11-oxo-22β-senecioyloxy-28-nor-olean-12,17-diene (Figure 7) | C34H48O5 | 536.753 | Oleanane | Aerial parts/methanol | [108] |
| (50) | 22β-Butanoyloxy-oleanonic acid 22β-butanoyloxy-3-oxo-olean-12-en-28-oic acid (Figure 7) | C34H52O5 | 540.785 | Oleanane | HD * | [94] |
| (51) | Lantadene D 22β-isobutyryloxy-3-oxo-olean-12-en-28-oic acid (Figure 7) | C34H52O5 | 540.785 | Oleanane | Aerial parts/ethanol HD * Leaves/acetonitrile, methanol, petroleum ether | [19,84,94,97] |
| (52) | Methyl 22β-propanoyloxy-oleanonate methyl 22β-propanoyloxy-3-oxo-olean-12-en-28-oate (Figure 7) | C34H52O5 | 540.785 | Oleanane | HD * | [92] |
| (53) | 24-Hydroxylantadene D 22β-isobutyryloxy-24-hydroxy-3-oxo-olean-12-en-28-oic acid (Figure 7) | C34H52O6 | 556.784 | Oleanane | Aerial parts/ethanol | [84] |
| (54) | Lantrigloylic acid 3,25-β-epoxy-3α-hydroxy-22β-senecioyloxy-olea-9 (11),12-dien-28-oic acid (Figure 7) | C35H50O6 | 566.779 | Oleanane | Aerial parts/methanol | [90] |
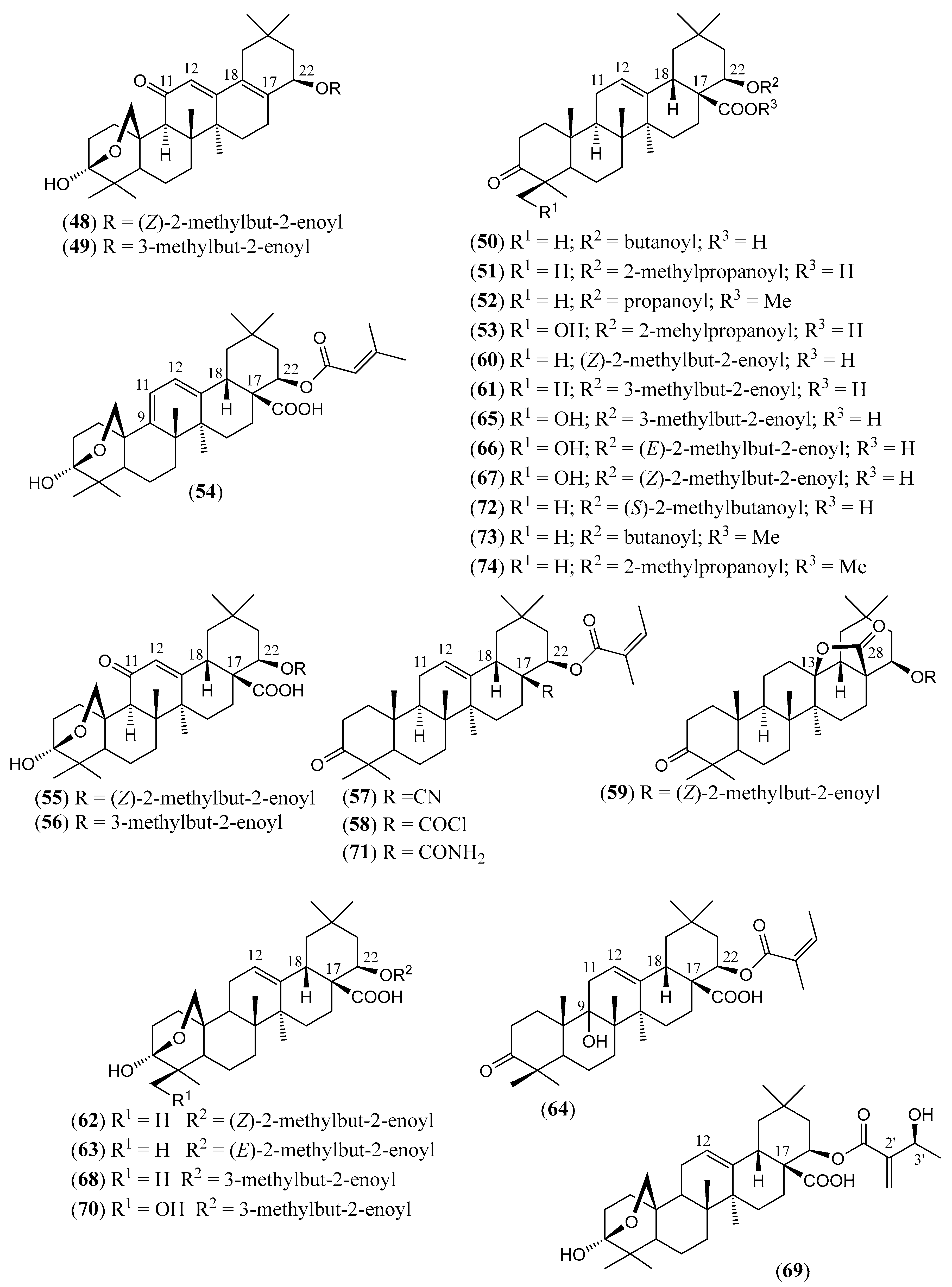
| (55) | Camangeloyl acid 3,25-β-epoxy-3α-hydroxy-22β-[(Z)-2-methyl-2-butenoyloxy]-11-oxo-olean-12-en-28-oic (Figure 7) | C35H50O7 | 582.778 | Oleanane | Aerial parts/methanol | [15,77,83,89,106] |
| (56) | Camarinin 3,25-β-epoxy-3α-hydroxy-22β-(3-methyl-2-butenoyloxy)- 11-oxo-olean-12-en-28-oic (Figure 7) | C35H50O7 | 582.778 | Oleanane | Aerial parts/methanol | [83,84,89,90,107] |
| (57) | Lantadene A nitrile 22β-angelyloxy-28-ciano-3-oxo-olean-12-ene (Figure 7) | C35H51NO3 | 533.797 | Oleanane | HD * | [93] |
| (58) | Lantadene A acyl chloride 28-chloro-22β-angelyloxy-3,28-dioxo-olean-12-ene (Figure 7) | C35H51ClO4 | 571.239 | Oleanane | HD * | [93] |
| (59) | 22β-Angelyloxy-3-oxo-olean-28,13-β-olide (Figure 7) | C35H52O5 | 552.796 | Oleanane | HD * | [108] |
| (60) | Lantadene A (Rehmannic acid) 22β-angelyloxy-3-oxo-olean-12-en-28-oic acid (Figure 7) | C35H52O5 | 552.796 | Oleanane | Aerial parts/methanol, ethanol Leaves/acetone, acetonitrile, ethanol, ethyl acetate, methanol, petroleum ether, methanol–water (70:30) Leaves and stems/methanol, petroleum ether Roots/n-hexane–ethyl acetate–methanol (1:1:1); ethanol Stems/ethanol, methanol | [108] |
| (61) | Lantadene B 3-oxo-22β-senecioyloxy- olean-12-en-28-oic acid (Figure 7) | C35H52O5 | 552.796 | Oleanane | Aerial parts/ethanol, dichloromethane, methanol, petroleum ether Leaves/acetonitrile, 96% ethanol, ethyl acetate Leaves/methanol, (70% methanol/30% water) Leaves and stems/petroleum ether Stems/methanol Roots/ethanol | [15,19,79,82,84,91,95,96,98,109,110,111,112,113,114,115,116] |
| (62) | Camaric acid 3,25-β-epoxy-3α-hydroxy-22β-[(Z)-2-methyl-2-butenoyloxy]-olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/dichloromethane, methanol Leaves and stems/methanol Roots/n-hexane–ethyl acetate–methanol (1:1:1) | [15,74,77,80,82,84,90,98,99,117,118] |
| (63) | 3,25-β-Epoxy-3α-hydroxy-22β-[(E)-2-methyl-2-butenoyloxy]-olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/ethanol | [84] |
| (64) | 9-Hydroxy-lantadene A 22β-angelyloxy-9-hydroxy-3-oxo-olean-12- en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Leaves/ethyl acetate, methanol | [119,120] |
| (65) | 24-Hydroxylantadene B ≡ 24-Hydroxy-22β-senecioyloxy-oleanonic acid 24-hydroxy-3-oxo-22β-senecioyloxy-olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/ethanol Leaves/ethyl acetate Leaves and stems/methanol | [84,99,116] |
| (66) | 24-Hydroxy lantadene X 24-hydroxy-3-oxo-22β-[(E)-2-methylbut-2-enoyloxy]- olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/ethanol | [84] |
| (67) | Icterogenin ≡ 24-Hydroxy-lantadene A ≡ 24-Hydroxy-22β-angelyloxy-oleanonic acid 24-hydroxy-3-oxo-22β-[(Z)-2-methylbut-2-enoyloxy]- olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/ethanol, methanol Leaves/acetone, ethanol Leaves/ethyl acetate, methanol Leaves and stems/methanol, petroleum ether | [19,79,80,81,82,84,99,109,116,118,121] |
| (68) | Lantanilic acid 3β,25-β-epoxy-3α-hydroxy-22β-senecioyloxy-olean-12-en-28-oic acid (Figure 7) | C35H52O6 | 568.795 | Oleanane | Aerial parts/dichloromethane, ethanol, methanol Leaves/ethanol, ethyl acetate, methanol, petroleum ether Leaves and stems/methanol Roots/chloroform | [15,19,72,77,79,81,84,85,98,99,100,109,116,122,123] |
| (69) | Camarolic acid 3,25-β-epoxy-3α-hydroxy-22β-[(S)-3-hydroxy-2-methylidenebutanoyloxy] olean- 12-en-28-oic acid (Figure 7) | C35H52O7 | 584.794 | Oleanane | Aerial parts/methanol | [82,90] |
| (70) | Lantacamaric acid B 3,25-β-epoxy-3α,24-dihydroxy-22β-senecioyloxy-olean-12-en-28-oic acid (Figure 7) | C35H52O7 | 584.794 | Oleanane | Leaves and stems/methanol | [85] |
| (71) | Lantadene A amide 28-amino-22β-angelyloxy-3,28-dioxo-olean-12-ene (Figure 7) | C35H53NO4 | 551.812 | Oleanane | HD * | [93] |
| (72) | Lantadene C 22β-[(S)-2-methylbutanoyloxy]-3-oxo-olean-12-en-28-oic acid (Figure 7) | C35H54O5 | 554.812 | Oleanane | HD * Leaves/acetonitrile, ethyl acetate, methanol Leaves and stems/petroleum ether | [91,94,109, 116,124] |
| (73) | Methyl 22β-butanoyloxy-oleanonate methyl 22β-butanoyloxy-3-oxo-olean-12-en-28-oate (Figure 7) | C35H54O5 | 554.812 | Oleanane | HD * | [94] |
| (74) | Methyl 22β-isobutyryloxy-oleanonate methyl 22β-isobutyryloxy-3-oxo-olean-12-en-28-oate (Figure 7) | C35H54O5 | 554.812 | Oleanane | HD * | [94] |
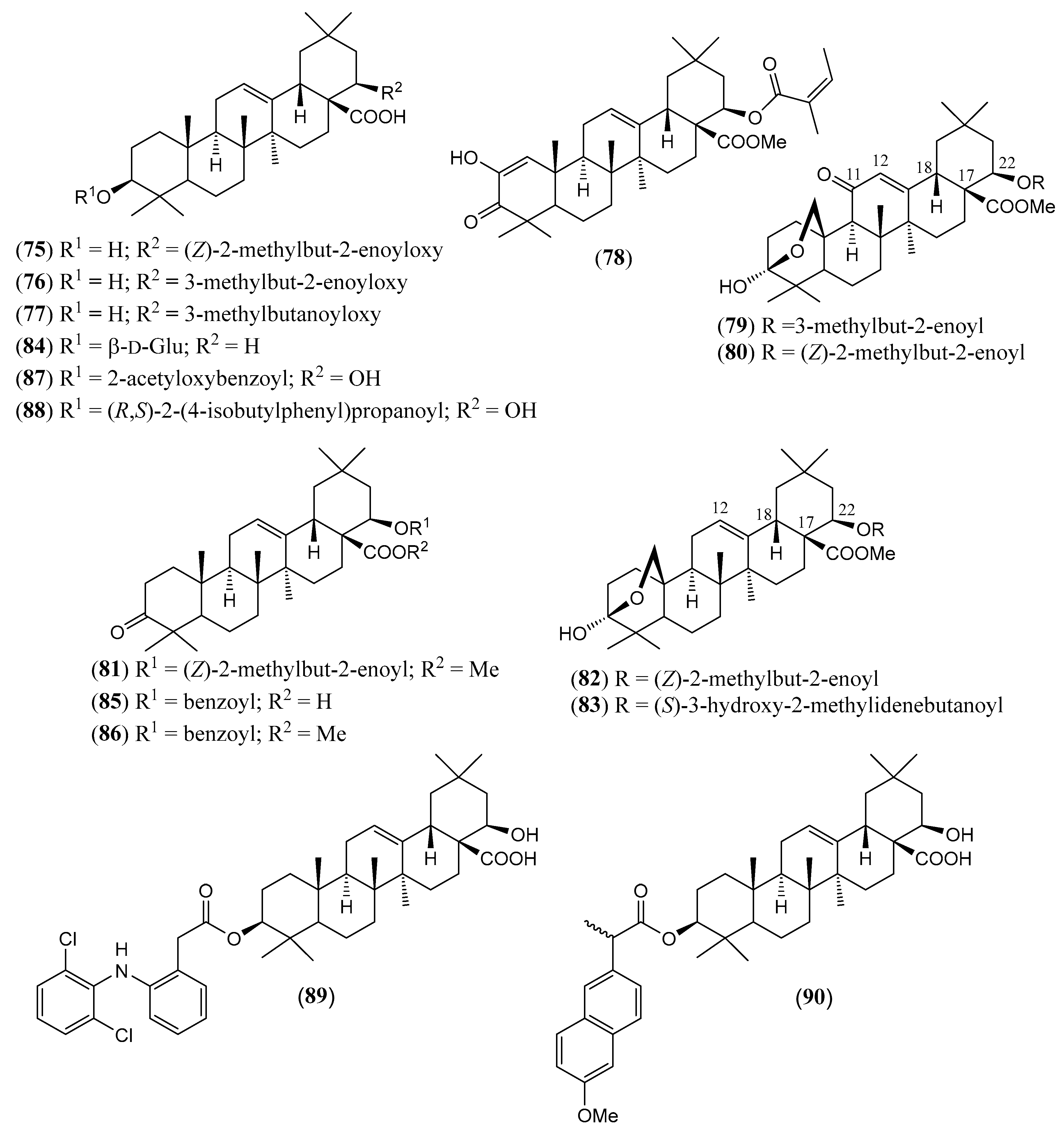
| (75) | Reduced lantadene A 22β-angelyloxy-3β-hydroxy-olean-12-en-28-oic acid (Figure 8) | C35H54O5 | 554.812 | Oleanane | Aerial parts/ethanol HD * Leaves/methanol, acetonitrile Roots/ethanol | [84,91,95] |
| (76) | Reduced lantadene B 3β-hydroxy-22β-senecioyloxy-olean-12-en-28-oic acid (Figure 8) | C35H54O5 | 554.812 | Oleanane | Aerial parts/ethanol HD * Leaves/acetonitrile, methanol Roots/ethanol | [84,91,95] |
| (77) | Reduced lantadene C 3β-hydroxy-22β-[2-methylbutanoyloxy]-olean-12-en-28-oic acid (Figure 8) | C35H56O5 | 554.812 | Oleanane | Aerial parts/ethanol | [84] |
| (78) | Methyl 22β-angelyloxy-2-hydroxy-3-oxo-olean-1,12-diene- 28-oate (Figure 8) | C36H52O6 | 580.806 | Oleanane | HD * | [124] |
| (79) | Lancamarinin methyl 3,25-β-epoxy-3α-hydroxy-11-oxo-22β-senecioyloxy-olean-12-en- 28-oate (Figure 8) | C36H52O7 | 596.805 | Oleanane | HD * Aerial parts/methanol | [105] |
| (80) | Methyl camangeloylate methyl 3,25-β-epoxy-3α-hydroxy-22β-[(Z)-2′-methyl-2′-butenoyloxy]-11-oxo-olean-12-en-28-oate (Figure 8) | C36H52O7 | 596.805 | Oleanane | HD * | [77] |
| (81) | Lantadene A methyl ester methyl 22β-angelyloxy-3-oxo-olean-12-en-28-oate (Figure 8) | C36H54O5 | 566.823 | Oleanane | HD * Leaves and stems/petroleum ether | [93,124] |
| (82) | Methyl 22-β-angelyloxy-lantanolate methyl 22β-angelyloxy-3,25-β-epoxy-3α-hydroxy-olean-12-en-28-oate (Figure 8) | C36H54O6 | 582.822 | Oleanane | HD * | [82] |
| (83) | Methyl camarolate methyl 3,25-β-epoxy-3α-hydroxy-22β-[(S)-3-hydroxy-2-methylidenebutanoyloxy] olean-12-en-28-oate (Figure 8) | C36H54O7 | 598.821 | Oleanane | HD * | [90] |
| (84) | 3-O-β-D-Glucosyl oleanolic acid 3-O-β-D-glucopyranosyloxy-olean-12-en-28-oic acid (Figure 8) | C36H58O8 | 618.852 | Oleanane | Leaves/methanol | [125,126] |
| (85) | 22β-Benzoyloxy-oleanonic acid 22β-benzoyloxy-3-oxo-olean-12-en-28-oic acid (Figure 8) | C37H50O5 | 574.802 | Oleanane | HD * | [94] |
| (86) | Methyl 22β-benzoyloxy-oleanonate methyl 22β-benzoyloxy-3-oxo-olean-12-en-28-oate (Figure 8) | C38H52O5 | 588.829 | Oleanane | HD * | [94] |
| (87) | 3β-(2-Acetyloxybenzoyloxy)-22β-hydroxy-olean-12-en-28-oic acid (Figure 8) | C39H54O7 | 634.854 | Oleanane | HD * | [96] |
| (88) | 3β-[(R,S)-2-(4-Isobutylphenyl)propanoyloxy]-22β-hydroxy-olean-12-en-28-oic acid (Figure 8) | C43H64O5 | 660.980 | Oleanane | HD * | [96] |
| (89) | 3β-{2-[2-(2,6-Dichlorophenylamino)phenyl]acetyloxy}-22β-hydroxy-olean-12-en-28-oic acid (Figure 8) | C44H57Cl2NO5 | 750.842 | Oleanane | HD * | [96] |
| (90) | 3β-[(+)-(S)-2-(6-Methoxy-2-naphthyl)propanoyloxy]-22β-hydroxy-olean-12-en-28-oic acid (Figure 8) | C44H60O6 | 684.958 | Oleanane | HD * | [96] |
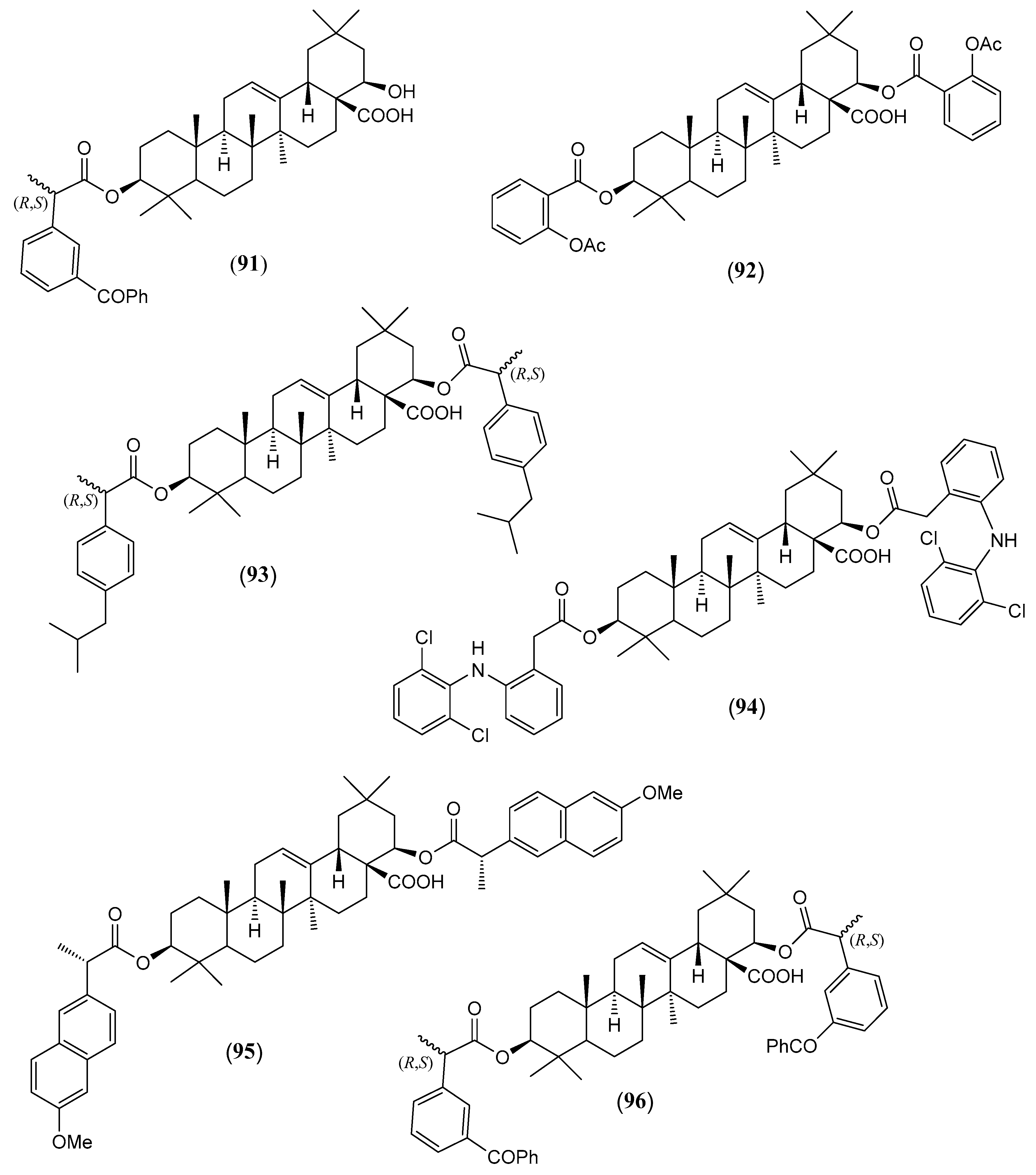
| (91) | 3β-[(R,S)-2-(3-Benzoylphenyl)propanoyloxy]-22β-hydroxy-olean-12-en-28-oic acid (Figure 9) | C46H60O6 | 708.980 | Oleanane | HD * | [96] |
| (92) | 3β,22β-Di-(2-acetyloxybenzoyloxy)-olean-12-en-28-oic acid (Figure 9) | C48H60O10 | 796.998 | Oleanane | HD * | [96] |
| (93) | 3β,22β-Di-[(R.S)-2-(4-isobutylphenyl)propanoyloxy]-olean-12-en-28-oic acid (Figure 9) | C56H80O6 | 849.250 | Oleanane | HD * | [96] |
| (94) | 3β,22β-Di-{2-[2-(2,6-dichlorophenylamino)phenyl]acetyloxy}-olean-12-en-28-oic acid (Figure 9) | C58H66Cl4N2 O6 | 1028.974 | Oleanane | HD * | [96] |
| (95) | 3β,22β-Di-[(+)-(S)-2-(6-methoxy-2-naphthyl)propanoyloxy]-olean-12-en-28-oic acid (Figure 9) | C58H72O8 | 897.206 | Oleanane | HD * | [96] |
| (96) | 3β,22β-Di-[(R,S)-2-(3-benzoylphenyl)propanoyloxy]-olean-12-en-28-oic acid (Figure 9) | C62H72O8 | 945.250 | Oleanane | HD * | [96] |
| (97) | Camarolide 3-oxo-urs-11-en-28,13-β-olide (Figure 10) | C30H44O3 | 452.679 | Ursane | Aerial parts/methanol | [85] |
| (98) | 3,24-Dioxo-urs-12-en-28-oic acid (Figure 10) | C30H44O4 | 468.678 | Ursane | Leaves/solvent not reported | [127] |
| (99) | Camaranoic acid 3,25-β-epoxy-3α-hydroxy-11-oxo-urs-12-en-28-oic acid (Figure 10) | C30H44O5 | 484.677 | Ursane | Aerial parts/methanol | [81,83,118] |
| (100) | Ursonic acid 3-oxo-urs-12-en-28-oic acid (Figure 10) | C30H46O3 | 454.695 | Ursane | Aerial parts/methanol Leaves and stems/petroleum ether | [81,83,84,85] |
| (101) | 11α-Hydroxy-3-oxo-urs-12-en-28-oic acid (Figure 10) | C30H46O4 | 470.694 | Ursane | Aerial parts/methanol | [82] |
| (102) | Lantic acid 3,25-β-epoxy-3α-hydroxy-urs-12-en-28-oic acid (Figure 10) | C30H46O4 | 470.694 | Ursane | Aerial parts/methanol Leaves/chloroform Leaves and stems/dichloromethane–methanol (1:1), petroleum ether | [75,83,98] |
| (103) | 11-Oxo-β-boswellic acid 3α-hydroxy-11-oxo-urs-12-en-24-oic acid (Figure 10) | C30H46O4 | 470.694 | Ursane | Leaves/ethyl acetate | [120] |
| (104) | Pomonic acid 19α-hydroxy-3-oxo-urs-12-en-28-oic acid (Figure 10) | C30H46O4 | 470.694 | Ursane | Aerial parts/ethanol, methanol Roots/ n-hexane–ethyl acetate–methanol (1:1:1) | [74,77,80,84] |
| (105) | Lantoic acid 3,25-β-epoxy-3α,22β-dihydroxy-urs-12-en-28-oic acid (Figure 10) | C30H46O5 | 486.693 | Ursane | Aerial parts/methanol Leaves/petroleum ether | [81,84,90,118] |
| (106) | Ursolic acid 3β-hydroxy-urs-12-en-28-oic acid; urs-12-en-3β-ol-28-oic acid (Figure 10) | C30H48O3 | 456.711 | Ursane | Aerial parts/methanol Leaves/methanol | [19,79,89,90,121,125] |
| (107) | Pomolic acid 3β,19α-dihydroxy-urs-12-en-28-oic acid (Figure 10) | C30H48O4 | 472.710 | Ursane | Aerial parts/methanol Stems/methanol Roots/chloroform, ethanol | [84,89,90,98] |
| (108) | α-Amyrin urs-12-en-3β-ol | C30H50O | 426.729 | Ursane | Aerial parts/96% ethanol, petroleum ether | [73,74] |
| (109) | 3β,19α-Dihydroxy-ursan-28-oic acid (Figure 10) | C30H50O4 | 474.726 | Ursane | Roots/ n-hexane–ethyl acetate–methanol (1:1:1) | [74] |
| (110) | Methyl camaranoate methyl 3,25-β-epoxy-3α-hydroxy-11-oxo-urs-12-en-28-oate (Figure 10) | C31H46O5 | 498.704 | Ursane | HD * | [83] |
| (111) | Ursoxy acid 3,25-β-epoxy-3α-methoxy-urs-12-en-28-oic acid (Figure 10) | C31H48O4 | 484.721 | Ursane | Aerial parts/methanol | [106] |
| (112) | Methyl 25-hydroxy-3-deoxy-ursen-12-en-28-oate (Figure 10) | C31H50O3 | 470.738 | Ursane | HD * | [128] |
| (113) | Methyl 3β,19α-dihydroxy ursan-28-oate (Figure 10) | C31H52O4 | 488.753 | Ursane | HD * | [74] |
| (114) | Camarinic acid 22β-acetyloxy-3,25-β-epoxy-3α-hydroxy-12-ursen-28-oic acid (Figure 10) | C32H48O6 | 528.730 | Ursane | Aerial parts/methanol Leaves/chloroform Leaves and stems/dichloromethane–methanol (1:1) | [16,83,98, 109] |
| (115) | Methyl ursoxylate methyl 3,25-β-epoxy-3α-methoxy-urs-12-en-28-oate (Figure 10) | C32H50O4 | 498.748 | Ursane | Aerial parts/methanol HD * | [106] |
| (116) | Ursethoxy acid 3,25-β-epoxy-3α-ethoxy-urs-12-en-28-oic acid (Figure 10) | C32H50O4 | 498.748 | Ursane | Aerial parts/methanol | [129] |
| (117) | Methyl camaralate methyl 22β-acetoxy-3,25-β-epoxy-3α-hydroxy-urs-12-en-28-oate (Figure 10) | C33H50O6 | 542.757 | Ursane | Aerial parts/methanol HD * | [77,98] |
| (118) | Methyl ursethoxylate methyl 3,25-β-epoxy-3α-ethoxy-urs-12-en-28-oate (Figure 10) | C33H52O4 | 512.775 | Ursane | Aerial parts/methanol | [129] |
| (119) | Lantacin 3β,19α-dihydroxy-22β-senecioyloxy-urs-12-en-28-oic acid (Figure 10) | C35H54O6 | 570.811 | Ursane | Aerial parts/methanol | [84,89,118] |
| (120) | Lantaiursolic acid 3β-isovaleroyloxy-19α-hydroxy-urs-12-en-28-oic acid (Figure 10) | C35H56O5 | 556.828 | Ursane | Roots/ethanol | [118] |
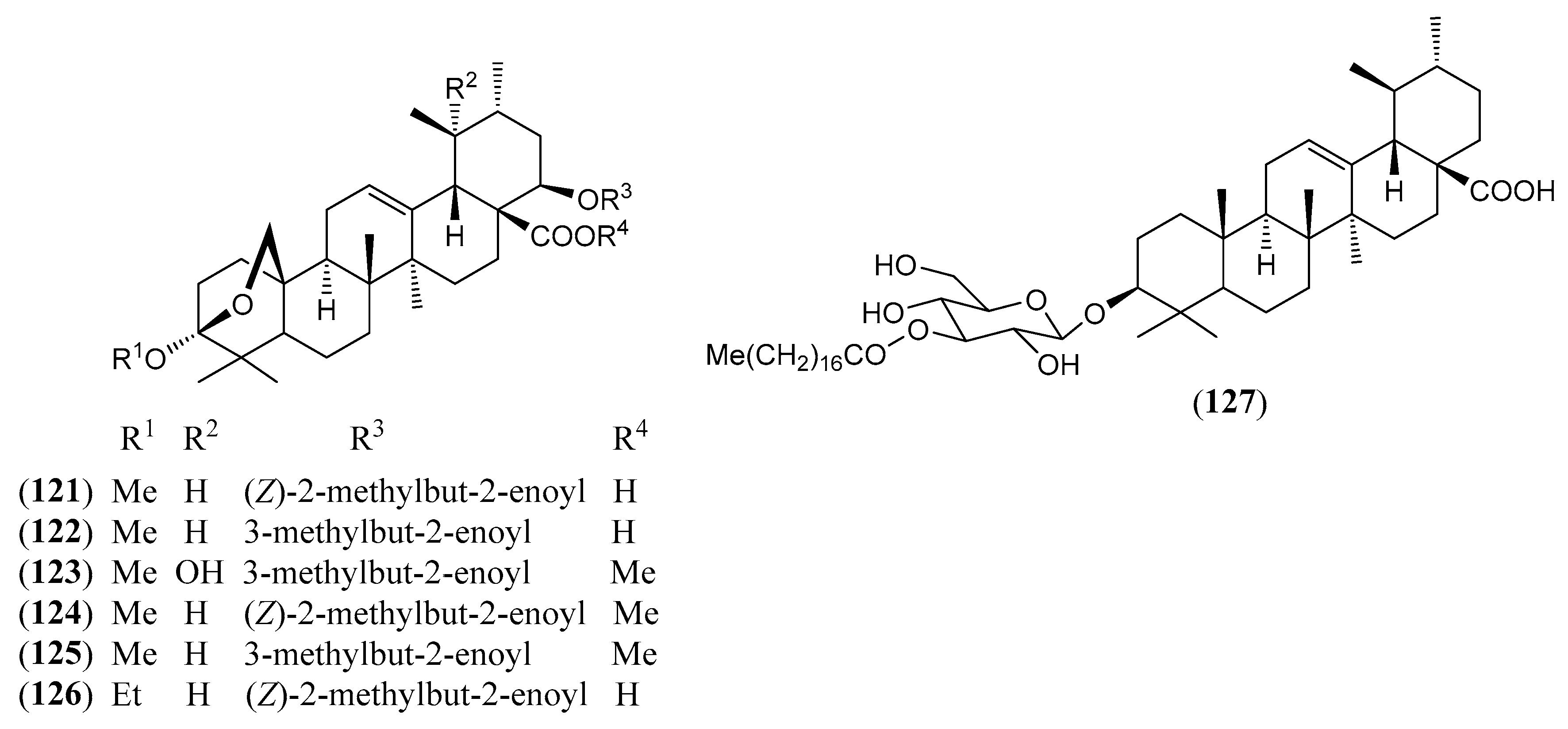
| (121) | Camaracinic acid 22β-angelyloxy-3,25-β-epoxy-3α-methoxy-12-ursen-28-oic acid (Figure 11) | C36H54O6 | 582.822 | Ursane | Aerial parts/methanol | [82] |
| (122) | Camaryolic acid 3,25-β-epoxy-3α-methoxy-22β-senecioyloxy-urs-12-en-28-oic acid (Figure 11) | C36H54O6 | 582.822 | Ursane | Aerial parts/methanol | [77,82] |
| (123) | Methyl lantacinate methyl 3β,19α-dihydroxy-22β-senecioyloxy- urs-12-en-28-oate (Figure 11) | C36H56O6 | 584.838 | Ursane | HD * | [84] |
| (124) | Methyl camaracinate methyl 22β-angelyloxy-3,25-β-epoxy-3α-methoxy-12-ursen-28-oate (Figure 11) | C37H56O6 | 596.849 | Ursane | HD * | [82] |
| (125) | Methyl camaryolate methyl 3,25-β-epoxy-3α-methoxy-22β-senecioyloxy-urs-12-en-28-oate (Figure 11) | C37H56O6 | 596.849 | Ursane | HD * | [82] |
| (126) | Ursangilic acid 22β-angelyloxy- 3,25-β-epoxy-3α-ethoxy-urs-12-en-28-oic acid (Figure 8) | C37H56O6 | 596.849 | Ursane | Aerial parts/methanol | [106] |
| (127) | Urs-12-en-3β-ol-28-oic acid 3-O-β-D-glucopyranosyl-4′- octadecanoate (Figure 11) | C54H92O9 | 885.321 | Ursane | Leaves/methanol | [125,126] |
| N.º | Compound | Molecular Formula | Molecular Weight | Flavonoid Type | Part of the Plant/Solvent | Reference |
|---|---|---|---|---|---|---|
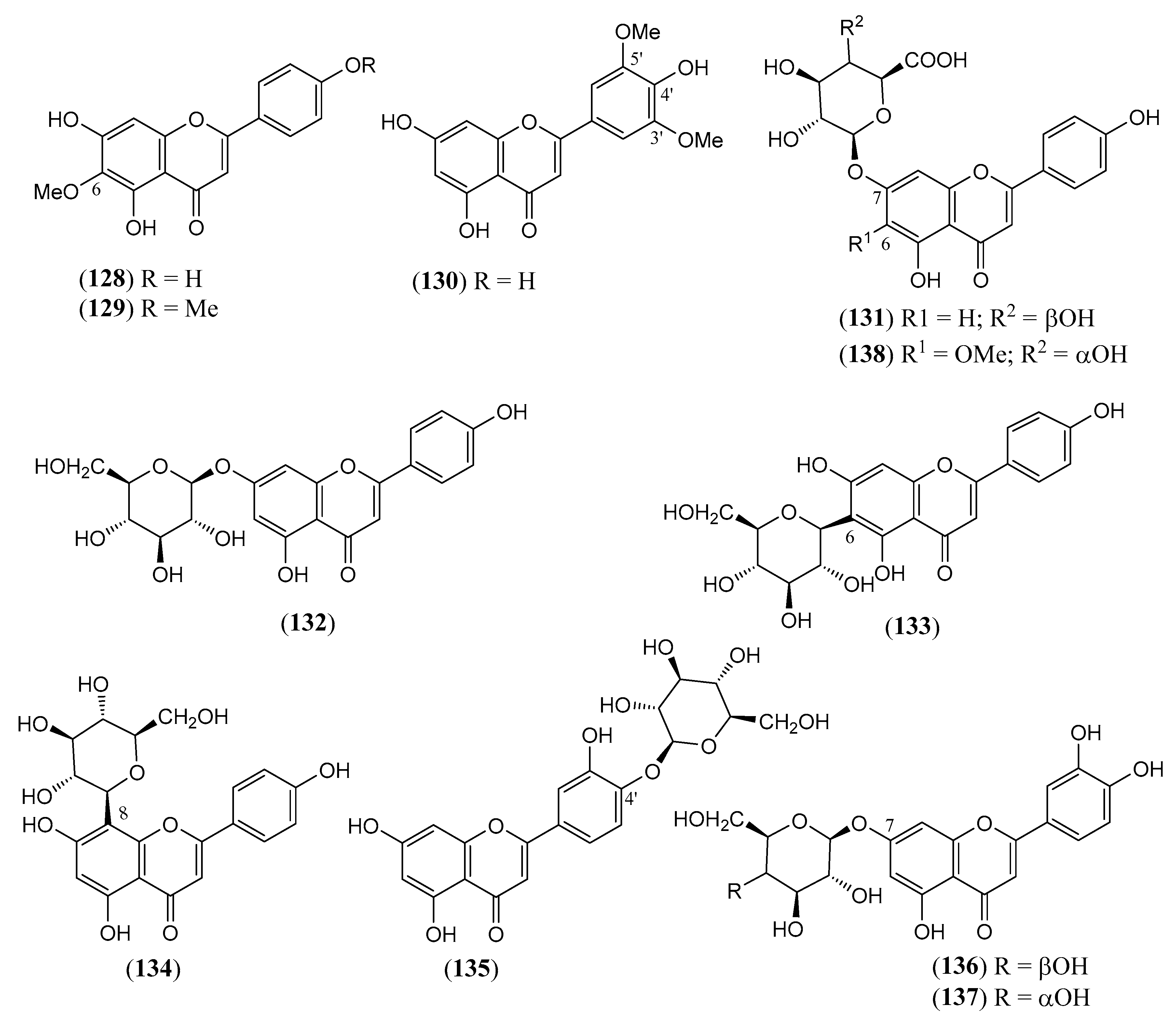
| (128) | Hispidulin 4′,5,7-trihydroxy-6-methoxyflavone (Figure 12) | C16H12O6 | 300.266 | Flavone | Leaves/ethanol Stems/methanol | [63,79,84] |
| (129) | Pectolinarigenin 5,7-dihydroxy-4′,6-dimethoxyflavone (Figure 12) | C17H14O6 | 314.293 | Flavone | Leaves/methanol | [19,79,84,130] |
| (130) | Tricin 4′,5,7-trihydroxy-3′,5′-dimethoxyflavone (Figure 12) | C17H14O7 | 330.292 | Flavone | Leaves/methanol | [79] |
| (131) | Apigenin 7-O-β-D-galacturonide 7-O-β-D-galacturonyl-4′,5,7-trihydroxyflavone (Figure 12) | C21H18O11 | 446.364 | Flavone | Flowers/methanol–water (70:30) | [131] |
| (132) | Anthemoside Apigenin 7-O-β-D-glucopyranoside 7-O-β-D-glucopyranosyl- 4′,5,7-trihydroxyflavone (Figure 12) | C21H20O10 | 432.381 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (133) | Isovitexin 6-C-β-D-glucopyranosyl-4′,5,7-trihydroxyflavone (Figure 12) | C21H20O10 | 432.381 | Flavone | Flowers/ methanol–water (70:30) | [132] |
| (134) | Vitexin 8-C-β-D-glucopyranosyl-4′,5,7-trihydroxyflavone (Figure 12) | C21H20O10 | 432.381 | Flavone | Flowers/ methanol–water (70:30) | [132,133] |
| (135) | Juncein Luteolin 4′-O-β-D-glucopyranoside 4′-O-β-D-glucopyranosyl-3′,4′,5,7-tetrahydroxyflavone (Figure 12) | C21H20O11 | 448.380 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (136) | Luteolin 7-O-β-D-galactopyranoside 7-O-β-D-galactopyranosyl-3′,4′,5,7-tetrahydroxyflavone (Figure 12) | C21H20O11 | 448.380 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (137) | Luteoloside Luteolin 7-O-β-glucopyranoside 7-O-β-D-glucopyranosyl-3′,4′,5,7-tetrahydroxyflavone (Figure 12) | C21H20O11 | 448.380 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (138) | 6-Methoxy scutellarin 7-O-β-glucuronyl-4′,5,7-trihydroxy-6-methoxyflavone (Figure 12) | C22H20O12 | 476.390 | Flavone | Leaves and stems/methanol | [85] |
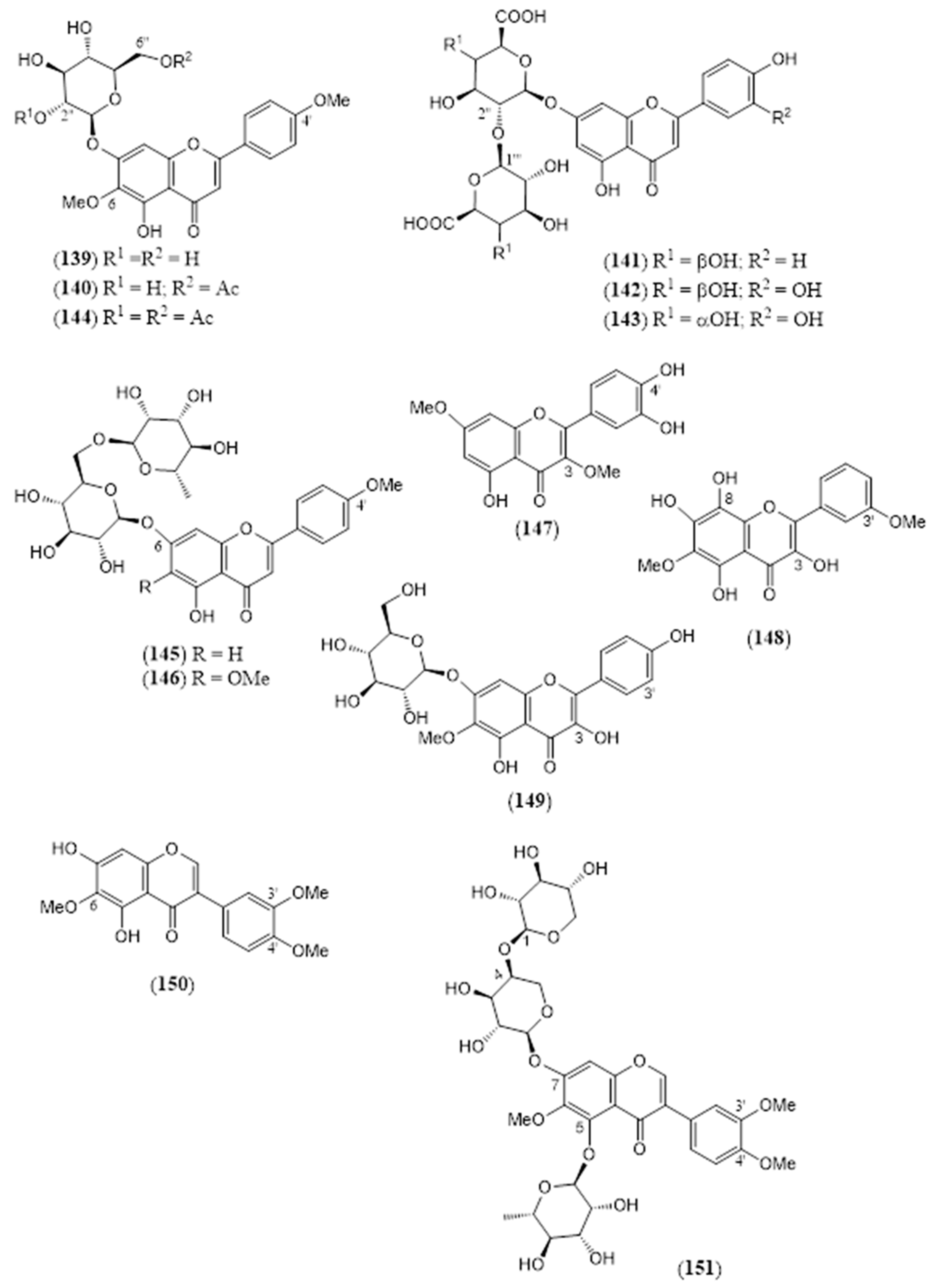
| (139) | Linaroside 7-O-β-D-glucopyranosyl-5,7-dihydroxy-4′,6-dimethoxyflavone (Figure 13) | C23H24O11 | 476.434 | Flavone | Aerial parts/ methanol Leaves/ methanol | [16,124,134] |
| (140) | Lantanoside 7-O-(6-O-acetyl-β-D-glucopyranosyl)-5,7-dihydroxy-4′,6-dimethoxyflavone (Figure 13) | C25H26O12 | 518.471 | Flavone | Aerial parts/methanol | [16,134] |
| (141) | Apigenin 7-O-β-D-galacturonyl- (2″→1‴)-O-β-D-galacturonide (Figure 13) | C27H26O17 | 622.488 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (142) | Luteolin 7-O-β-D-galacturonyl-(2″→1‴)-O-β-D-galacturonide (Figure 13) | C27H26O18 | 638.487 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (143) | Luteolin 7-O-β-D-glucuronyl-(2″→1‴)-O-β-D-glucuronide (Figure 13) | C27H26O18 | 638.487 | Flavone | Flowers/methanol–water (70:30) | [132] |
| (144) | Acetyl lantanoside 7-O-(2,6-O-diacetyl-β-D-glucopyranosyl)-5,7-dihydroxy-4′,6-dimethoxyflavone (Figure 13) | C27H28O13 | 560.508 | Flavone | HD * | [16,134] |
| (145) | Acacetin-7-O-β-D-rutinoside 7-O-β-D-rutinosyl-5,7-dihydroxy- 4′-methoxyflavone (Figure 13) | C28H32O14 | 592.550 | Flavone | Leaves/methanol | [79] |
| (146) | Pectolinarin 7-O-β-D-rutinosyl -5,7-dihydroxy-4′,6-dimethoxyflavone (Figure 13) | C29H34O15 | 622.576 | Flavone | Aerial parts/ ethanol Leaves/ ethanol, methanol | [19,84,133] |
| (147) | 3,7-O-Dimethylquercetin 3′,4′,5-trihydroxy-3,7-dimethoxyflavone (Figure 13) | C17H14O7 | 330.292 | Flavonol | Leaves/acetone | [127] |
| (148) | 3,5,7,8-Tetrahydroxy-3′,6-dimethoxyflavone (Figure 13) | C17H14O8 | 346.291 | Flavonol | Leaves/methanol | [79] |
| (149) | 6-Methoxykaempferol-7-O-β-D-glucoside 7-O-β-D-glucopyranosyl-3,4′,5,7-tetrahydroxy-6-methoxyflavone (Figure 13) | C22H22O12 | 478.406 | Flavonol | Flowers/95% methanol | [135] |
| (150) | 5,7-Dihydroxy-6,3′,4′-trimethoxy isoflavone (Figure 13) | C18H15O7 | 343.311 | Isoflavone | Leaves/methanol | [79] |
| (151) | Gautin 5,7-dihydroxy-6,3′,4′-trimethoxy isoflavone-5-O-α-L-rhamnopyranosyl-7-O-β-D-arabinopyranosyl-(1‴→4″)-O-β- D-xylopyranoside (Figure 13) | C34H42O19 | 754.691 | Isoflavone | Leaves/methanol | [79] |
| N.º | Compound | Molecular Formula | Molecular Weight | Part of the Plant/Solvent | Reference |
|---|---|---|---|---|---|
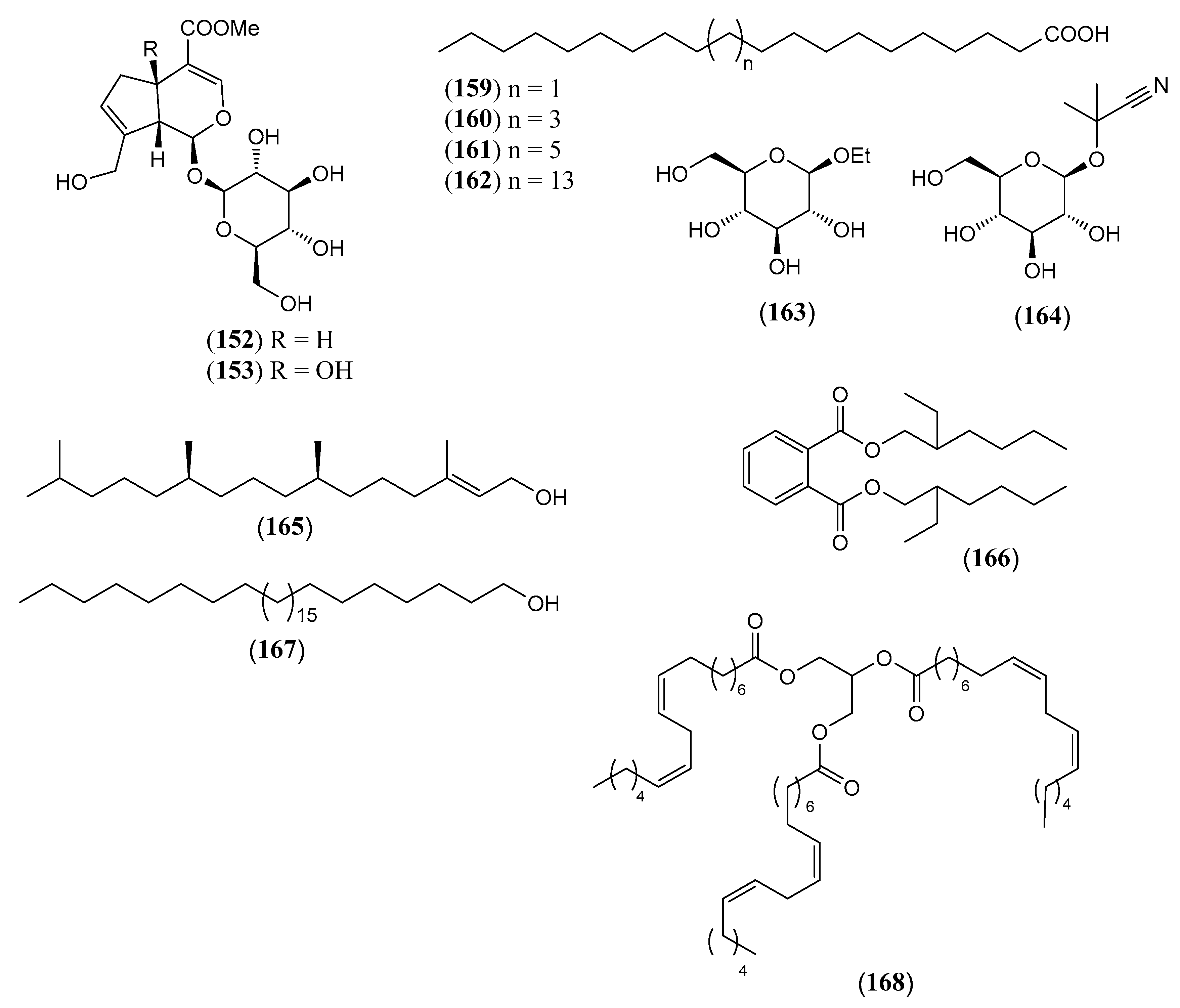
| (152) | Geniposide methyl (1S,4aS,7aS)-7-(hydroxymethyl)-1-[(2S,3R,4S,5S,6R)-3,4,5-trihydroxy-6-(hydroxymethyl) oxan-2-yl] oxy-1,4a,5,7a-tetrahydrocyclopenta[c]pyran-4-carboxylate (Figure 14) | C17H24O10 | 388.369 | Leaves and stems/ methanol Roots/ ethanol | [91] |
| (153) | Theviridoside methyl (1S,4aR,7aR)-4a-hydroxy-7-(hydroxymethyl)-1-[(2S,3R,4S,5S,6R)-3,4,5-trihydroxy-6-(hydroxymethyl) oxan-2-yl] oxy-5,7a-dihydro-1H-cyclopenta[c]pyran-4-carboxylate (Figure 14) | C17H24O11 | 404.368 | Aerial parts and roots/ ethanol Leaves and stems/ methanol Roots/ methanol | [91] |
| N.º | Compound | Molecular Formula | Molecular Weight | Part of the Plant/Solvent | References |
|---|---|---|---|---|---|
| (154) | Myristic acid tetradecanoic acid | C14H28O2 | 228.376 | Aerial parts/petroleum ether | [73] |
| (155) | Palmitic acid hexadecanoic acid | C16H32O2 | 256.430 | Aerial parts/methanol/petroleum ether Stems/ethanol | [73,77,82] |
| (156) | Linoleic acid (9Z,12Z)-octadeca-9,12-dienoic acid | C18H32O2 | 280.452 | Aerial parts/petroleum ether | [73] |
| (157) | Oleic acid (9Z)-octadec-9-enoic acid | C18H34O2 | 282.468 | Aerial parts/petroleum ether | [73] |
| (158) | Stearic acid octadecanoic acid | C18H36O2 | 284.484 | Aerial parts/methanol Stems/ethanol | [77,82] |
| (159) | Arachidic acid eicosanoid acid (Figure 14) | C20H40O2 | 312.538 | Aerial parts/petroleum ether | [73] |
| (160) | Behenic acid docosanoic acid (Figure 14) | C22H44O2 | 340.592 | Aerial parts/methanol | [77,82] |
| (161) | Lignoceric acid tetracosanoic acid (Figure 14) | C24H48O2 | 368.646 | Aerial parts/methanol | [106] |
| (162) | Lacceroic acid dotriacontanoic acid (Figure 14) | C32H64O2 | 480.862 | Aerial parts/methanol | [106] |
| N.º | Compound | Molecular Formula | Molecular Weight | Part of the Plant/Solvent | References |
|---|---|---|---|---|---|
| (163) | Ethyl-β-D-galactopyranoside (Figure 14) | C8H16O6 | 208.210 | Stems/ ethanol | [15] |
| (164) | Linamarin 2-(β-D-Glucopyranosyloxy)-2-methylpropanenitrile (Figure 14) | C10H17NO6 | 247.247 | Leaves and stems/ methanol | [99] |
| (165) | Phytol 3,7,11,15-tetramethyl-2-hexadecen-1-ol (Figure 14) | C20H40O | 296.539 | Leaves and stems/ petroleum ether | [75] |
| (166) | Di-(2-ethylhexyl) phthalate (Figure 14) | C24H38O4 | 390.564 | Fruits/ chloroform | [73] |
| (167) | Triacontan-1-ol (Figure 14) | C30H62O | 438.825 | Aerial parts/ petroleum ether | [73] |
| (168) | Trilinolein Glyceryl trilinoleate (Figure 14)) | C56H96O6 | 865.37 | Fruits/ chloroform | [73] |

3.3. Biological Activities
| Biological Activity | Part of the Plant/Solvent | Model | Results | Reference |
|---|---|---|---|---|
| Analgesic, anti-inflammatory | Leaves/water | The anti-inflammatory activity assay was carried out using carrageenan-induced lung edema and pleurisy mice. An analgesic effect assay was carried out using the formalin pain test. | Significant (p < 0.05) anti-inflammatory and analgesic activity, and minimal toxic effects. | [136] |
| Antibacterial | Leaves/ dichloromethane–methanol (1:1) | The in vitro antibacterial activity of a crude extract was screened at concentrations of 1000 μg/mL and 500 μg/mL against Bacillus cereus var mycoides (ATCC 11778), B. pumilus (ATCC 14884), B. subtilis (ATCC 6633), Bordetella bronchiseptica (ATCC 4617), Micrococcus luteus (ATCC 9341), Staphylococcus aureus (ATCC 29737), S. epidermidis (ATCC 12228), Escherichia coli (ATCC 10536), Klebsiella pneumoniae (ATCC 10031), Pseudomonas aeruginosa (ATCC 9027), and Streptococcus faecalis (MTCC 8043). | Except for E. coli and P. aeruginosa, a complete inhibition of bacterial growth was observed at both concentrations. | [60] |
| Leaves, stems, and roots/methanol | The in vitro antibacterial activity of a crude extract was screened against Bacillus cereus (ATCC 14579), Mycobacterium fortuitum (ATCC 6841), and Staphylococcus aureus (ATCC 6538). | B. cereus and M. fortuitum: MIC and MBC values > 1000 μg/mL; S. aureus: MIC = 250 μg/mL, MBC > 1000 μg/mL. | [44] | |
| Leaves/methanol | A crude extract was tested in vitro with the disk diffusion method against Escherichia coli, Proteus vulgaris, and Vibrio cholerae. | Inhibition zone diameter = 50 mm. | [121] | |
| Leaves/ methanol, ethanol, water | Crude extracts were tested against Bacillus subtilis (ATCC 6059), Klebsiella pneumoniae, Staphylococcus aureus (ATCC 6538), and Pseudomonas aeruginosa (ATCC 7221). | MIC values (mg/mL) of a methanol extract: B. subtilis and K. pneumoneae = 8; S. aureus and P. aeruginosa = 5. MIC values (mg/mL) of an ethanol extract: B. subtilis = 10, K. pneumoneae = 12, S. aureus = 6.5, P. aeruginosa = 8. MIC values (mg/mL) of an aqueous extract: B. subtilis and S. aureus = 8, P. aeruginosa = 10. | [137] | |
| Flowers/70% aqueous ethanol | A crude extract was tested against the Mycobacterium tuberculosis H37RV strain at different concentrations (25, 50, and 100 μg/mL). | All concentrations inhibited the growth of M. tuberculosis H37RV from the first to the sixth week. | [138] | |
| Leaves/methanol | Crude extracts were tested against the Mycobacterium smegmatis mc2155 strain, M. tuberculosis H37Rv strain, and rifampicin-resistant M. tuberculosis TMC-331 strain. | MIC values (μg/mL) determined for M. smegmatis mc2155 strain = 574 ± 196; M. tuberculosis H37Rv strain = 574 ± 196; M. tuberculosis TMC-331 strain = 176 ± 33. | [155] | |
| Aerial parts/methanol | The in vitro antibacterial activity of a crude extract was tested against E. coli (ATCC25922), Klebsiella pneumoniae, Pantoea sp., and Shigella flexneri. | MIC values determined for all tested bacteria = 25 μg/mL. | [156] | |
| Leaves/methanol | A crude extract was tested with the disk diffusion method against Helicobacter pylori. | Inhibition zone diameter = 20 mm. | [128] | |
| Leaves and flowers/water, methanol, acetone, benzene | Crude flower and leaf extracts showed the highest inhibitory effects against B. subtillis. Extracts separated by column chromatography displayed weaker inhibitory effects against B. subtillis than crude extracts. | Inhibition area ranging from 6 to 9 mm. Inhibition area ranging from 3 to 7 mm. | [157] | |
| Anticoagulant | Leaves, flowers, and roots/70% aqueous ethanol | The in vitro anticoagulant activity of crude extracts was tested at concentrations of 0.125, 0.25, 0.50, and 1 mg/mL. | The concentration of 1 mg/mL exhibited the highest anticoagulant activity; values expressed as prothrombin time: flowers = 21.7 ± 3 s; leaves = 16.9 ± 2.4 s; roots = 21.5 ± 2.8 s. | [158] |
| Antidiabetic | Leaves/water | Wistar albino rats (150–200 g); dose 1 = 250 mg extract/kg body weight and dose 2 = 500 mg extract/kg body weight were administered orally for 21 days. | Blood glucose levels: dose 1: at the 8th day = 183.83 ± 4.29 mg/dL; at the 14th day = 165.50 ± 4.26 mg/dL; at the 21st day = 136.83 ± 1.99 mg/dL. Dose 2: at the 8th day = 180.50 ± 3.07 mg/dL; at the 14th day = 157.83 ± 5.28 mg/dL; at the 21st day = 124.67 ± 2.40 mg/dL. | [125] |
| Antidiarrheal | Leaves/ethanol | Group II of male mice (Laca strain; 20–25 g) received 1% leaf powder for ten days; groups III–VI received a single dose of 125, 250, 500, and 1000 mg extract/kg body weight; subsequently, castor oil-induced diarrhea was evaluated. | % Intestinal transit: group II: 34.78 ± 3.52; group III: 1 ± 0.01; group IV: 26.46 ± 6.82; group V: 31.74 ± 1.49; group VI: 38.67 ± 6.60. Mean defecation in 4 h: group III: 9 ± 1.18; group IV: 9 ± 2.06; group V: 1 ± 0.05; group VI: total constipation. | [100] |
| Leaves/80% aqueous methanol | Groups III–V of Swiss albino mice (6–88 weeks; 20–30 g) received a single dose of 100, 200, and 400 mg extract/kg body weight; subsequently, castor oil-induced diarrhea was evaluated. | The most effective dose was 400 mg/kg body weight with a 67.9% inhibition of diarrhea and an antidiarrheal index of 87.6. | [159] | |
| Antifungal | Leaves/dicloromethane–methanol (1:1) | The antifungal activity of a crude extract was tested at concentrations of 1000 μg/mL and 500 μg/mL against Candida albicans (MTCC 10231), Aspergillus niger (MTCC 1344), and Saccharomyces cerevisiae (ATCC 9763). | Complete inhibition was observed at both concentrations. | [60] |
| Leaves, stems, and roots/methanol | The in vitro antifungal activity of a crude extract was tested against Candida albicans (ATCC 10231). | MIC and MBC values > 1000 μg/mL. | [44] | |
| Leaves/methanol | A crude extract was tested in vitro with the disk diffusion method against Aspergillus niger and Candida albicans. | Inhibition zone diameter = 0.5 mm. | [79] | |
| Leaves/methanol, water | Crude extracts were tested against Aspergillus fumigatus and A. flavus. | % Inhibition of the methanol extract: A. fumigatus = 71.4; A. flavus = 66.4. % Inhibition of the water extract: A. fumigatus = 61.5; A. flavus = 57.8. | [137] | |
| Antioxidant | Leaves, flowers, fruits, roots, and stems/methanol | Phytochemical analysis: Folin–Ciocalteu assay; gallic acid and ascorbic acid as reference standard. The in vitro antioxidant activity was tested by the following different methods: 1,1-diphenyl-2-picrylhydrazyl (DPPH) radical scavenging assay, with ascorbic acid as a reference standard; xanthine oxidase inhibition assay, with allopurinol as a reference standard; Griess–Ilosvay method, with allopurinol as a reference standard. | Leaves: total phenols > 100 mg/g extract; DPPH assay: IC50 = 16.02 ± 0.04 μg/mL; xanthine oxidase inhibition assay: IC50 < 20 μg/mL; Griess–Ilosvay method: IC50 < 10 ± 2 μg/mL. Flowers: total phenols > 100 mg/g extract; DPPH assay: IC50 = 28.92 ± 0.19 μg/mL; xanthine oxidase inhibition assay: IC50 > 20 μg/mL; Griess–Ilosvay method: IC50 < 10 ± 2 μg/mL. Fruits: total phenols < 100 mg/g extract; DPPH assay: IC50 = 90.11 ± 0.57 μg/mL; xanthine oxidase inhibition assay: IC50 > 20 μg/mL; Griess–Ilosvay method: IC50 > 10 ± 2 μg/mL. Roots: total phenols > 100 mg/g extract; DPPH assay: IC50 = 31.52 ± 0.74 μg/mL; xanthine oxidase inhibition assay: IC50 > 20 μg/mL; Griess–Ilosvay method: IC50 < 10 ± 2 μg/mL. Stems: total phenols > 100 mg/g extract; DPPH assay: IC50 = 46.96 ± 2.51 μg/mL; xanthine oxidase inhibition assay: IC50 < 20 μg/mL; Griess–Ilosvay method: IC50 > 10 ± 2 μg/mL. | [139] |
| Leaves and roots/ethanol | Phytochemical analyses: Folin–Ciocalteu assay, with gallic acid as a reference standard; aluminum chloride method, with quercetin as a reference standard; quantification of phenolics and flavonoids by HPLC-DAD. In vitro antioxidant activity was determined by the following different methods: thiobarbituric acid reactive substances (TBARS) assay with phospholipids; iron chelation assay; deoxyribose degradation assay; ferric-reducing antioxidant power (FRAP). | Leaves: total phenols: 227.10 ± 9.07; Gallic Acid Equivalents (GAE μg/mg), 22.7%; total flavonoids: 46.55 ± 1.50; quercetin equivalents (QuercE μg/mg), 4.6%; caffeic acid (10.75 ± 0.04 mg/g), 1.07%; quercetin (2.87 ± 0.01 mg/g, 0.28%); TBARS assay: basal IC50 = 57.69 ± 4.01 μg/mL; induced Fe2+ IC50 = 32.48 ± 3.51 μg/mL; iron chelation assay: IC50 = 214.20 ± 2.50 μg/mL; deoxyribose degradation assay: IC50 = 285.64 ± 20.63 μg/mL; FRAP assay: 8.28 ± 0.07 mM Fe 2+/g extract. Roots: total phenols = 211.80 ± 7.94 (GAE μg/mg), 21.3%; total flavonoids = 33.64 ± 1.52 (QuercE μg/mg, 3.3%); caffeic acid (8.27 ± 0.01 mg/g, 0.82%), rutin (5.35 ± 0.03 mg/g, 0.53%); TBARS assay: basal IC50 = 168.92 ± 7.36 μg/mL; induced Fe2+ IC50 = 63.84 ± 4.56 μg/mL; iron chelation assay: IC50 = 448.19 ± 4.50 μg/mL; deoxyribose degradation assay: IC50 = 276.89 ± 31.26 μg/mL; FRAP assay: 11.64 ± 0.10 mM Fe2+/g extract. | [160] | |
| Leaves/methanol | The concentration of lipid peroxides (LPOs) in the stomach mucosa of Wister albino rats used in ulcerogenic models was indirectly measured by the TBARS assay; the concentration of reduced glutathione was also determined. | LPO: 29.23 ± 0.35 and 27.7 ± 0.50 nmol/g; GSH: 181.52 ± 0.83 and 202.9 ± 1.08 μg/g. | [128] | |
| Leaves/methanol | DPPH assay. | IC50 = 74.3 μg/mL. | [130] | |
| Leaves/methanol | Quantitative analysis of phytochemicals: total phenolic content, total flavonoid content, and total tannin content. In vitro antioxidant activity (DPPH radical scavenging activity assay and hydroxyl radical scavenging activity assay). | Total phenolic content: 40.859 ± 0.017 (mg GAE/g dry sample). Total flavonoid content: 53.112 ± 0.199 (mg rutin/g dry sample). Total tannin content: 0.860 ± 0.038 (mg/g dry sample). DPPH assay: IC50 ≥ 0.2 mg/mL. Hydroxyl radical assay: IC50 ≤ 0.2 mg/mL. | [137] | |
| Leaves/ethyl acetate | Total phenolic content and DPPH assay. | Total phenolic content: 2419.6 mg/L GAE. DPPH assay: IC50 = 36.18 mg/mL. | [161] | |
| Aerial parts/methanol | The antioxidant capacity of a crude extract was evaluated by the FRAP and the DPPH assays. | FRAP: 8.17 ± 0.04 mmol/g, DPPH: IC50 = 16.13 ± 0.35 μg/mL. | [156] | |
| Leaves/water | DPPH, metal chelating activity, and FRAP assays. | DPPH assay: IC50 = 42.66 μg/mL; metal chelating activity assay: IC50 = 1036.4 μg/mL; FRAP test: dose-dependent activity. | [162] | |
| Leaves/methanol | DPPH and FRAP assays. | DPPH: IC50 = 24.80 ± 0.52 μg/mL; FRAP: IC50 = 21.61 ± 0.26 μg/mL. | [143] | |
| Antiparasitic | Leaves and stems/dichloromethane; dichloromethane–methanol (1:1); water | Leishmania amazonensis (MHOM/77BR/LTB0016) promastigotes and amastigotes. | Dichlorometane extract: IC50 = 11.7 ± 4.4 μg/mL and IC50: 21.8 ± 2.4 μg/mL; dichloromethane–methanol (1:1) and water extracts: IC50 > 200 μg/mL. | [64] |
| Leaves/methanol Aerial parts/dichloromethane | Leishmania amazonensis (MHOM/Br/75/Josefa) isolated promastigotes and L. chagasi (MHOM/Br/74/PP75) isolated promastigotes. The in vitro antiparasitic activity of a crude extract and 18 fractions obtained by open-column chromatographic separation were tested against Leishmania amazonensis (MHOM/BR/77/LTB0016) promastigotes and L. mexicana isolated amastigotes. | IC50 = 14 μg/mL and IC50 > 250 μg/mL. Crude extract: IC50 = 21.8 ± 2.4 μM and IC50 = 42.6 ± 1.9 μM. The most active fractions against L. amazonensis amastigotes were as follows: FII, IC50 = 9.1 ± 3.4 μM; FX, IC50 = 7.9 ± 0.3 μM; FXI, IC50 = 8.0 ± 1.1 μM; FXVI, IC50 = 8.5 ± 1.7 μM. | [67] [109] | |
| Leaves/dichloromethane | Dichloromethane extracts of two different batches were tested against the chloroquine-sensitive strain 3D7 and chloroquine-resistant strain W2 of Plasmodium falciparum, and by the parasite dehydrogenase lactate essay. Five female Swiss mice (10 weeks old; 25 ± 2 g), infected by Plasmodium berghei NK173, received a single dose of 50 mg extract/kg body weight daily for 4 days intraperitoneally. | 3D7: IC50 = 8.7 ± 1 and 14.1 ± 8.4 μg/mL; W2: IC50 = 5.7 ± 1.6 and 12.2 ± 2.9 μg/mL. 5% growth inhibition. | [43] | |
| Leaves/ethyl acetate | The extract was tested on chloroquine-resistant strains (3D7 and INDO) of Plasmodium falciparum. | 3D7: IC50 = 19 ± 0.57 μg/mL; INDO: IC50 = 20 ± 1.5 μg/mL. | [58] | |
| Leaves and twigs/dichloromethane–methanol (1:1); water | Crude extracts were tested in vitro against the chloroquine-sensitive strain D10 of Plasmodium falciparum and by the parasite dehydrogenase lactate assay. | IC50 = 11 μg/mL; IC50 < 1000 μg/mL. | [140] | |
| Aerial parts/methanol | The in vitro nematocidal activity of crude extract and its partitions were screened against Meloidogyne incognita larvae, at concentrations of 0.5%, 0.25%, and 0.125% after 48 h. | At a 0.5% concentration, the methanol extract: 85% mortality; ether insoluble partition: 90% mortality; methanolic acidic partition: 88% mortality; ether soluble partition: 75% mortality; n-hexane soluble partition: 60% mortality; n-hexane insoluble partition: 50% mortality. | [99] | |
| Antiulcerogenic | Leaves/methanol | Wister albino rats (150–200 g) were divided into 4 groups; groups 2 and 3 received 250 and 500 mg extract/kg orally. Aspirin-induced ulcerogenesis in a pyloric ligated system (APL); ethanol-induced ulcer model (EIM); cysteamine-induced duodenal ulcer model (Cys). | Ulcer index inhibition: APL: 46.61% and 73.97%; EIM: 55.60% and 63.39%; CYS: 41.43% and 68.90%. | [103] |
| Antiviral | Leaves and flowers/95% ethanol | The in vitro anti-COVID-19 activity of crude extracts from different cultivars were screened by the plaque reduction assay. | Spreading sunset cultivar: flowers: IC50 = 4.188 μg/mL; leaves: IC50 = 8.751 μg/mL. Chelsea gem cultivar: flowers: IC50 = 3.671 μg/mL; leaves: IC50 = 3.181 μg/mL. Nivea cultivar: flowers: IC50 = 15.050 μg/mL; leaves: IC50 = 6.820 μg/mL. Drap d’or cultivar: flowers: IC50 = 5.015 μg/mL; leaves: IC50 = 8.715 μg/mL. | [103] |
| Anxiolytic | Leaves/methanol | Ursolic acid stearyl glucoside (UASG) was isolated from the leaves of L. camara using column chromatography. The compound was administered to the animals in a dose-dependent manner to evaluate its effects at different concentrations | A dose-dependent effect, with higher doses of UASG (25 and 50 mg/kg) leading to more pronounced anxiolytic effects. UASG reduced the anxiety and increased the locomotor activity. The anxiolytic effects of UASG were comparable to those of diazepam (1 mg/kg), a standard anxiolytic drug, indicating that UASG may have a similar therapeutic potential. | [163] |
| Chemoprotective effect | Leaves/methanol | Female Swiss albino mice (6 weeks old; 18–22 g). Group III received 400 mg extract/kg body weight, which was given orally as a suspension in water and carboxymethyl cellulose, twice a week (100 nmol/100 μL), applied for 20 weeks topically. | A significant reduction in cancer (76.4%) was observed, and the survival rate was 75%. | [141] |
| Cytotoxic | Leaves and stems/dichloromethane (a); dichloromethane–methanol (1:1) (b); water (c). | BALB/c mice peritoneal macrophages. | (a): CC50 > 100 μg/mL; (b): CC50 > 200 μg/mL; (c): CC50 = 125.9 ± 3.1 μg/mL. | [64] |
| Leaves/dichloromethane | The cytotoxicity of dichloromethane extracts from two different batches was tested in vitro towards normal human fetal lung fibroblasts WI-38. | IC50 = 69.5 ± 12.1 μg/mL and IC50 = 97.2 ± 2.4 μg/mL. | [43] | |
| Leaves/ethyl acetate | HeLa cells and the MTT assay. | IC50 = 42 ± 2.3 μg/mL. | [58] | |
| Leaves/ethanol | Tested towards Hela cancer cells. | IC50 = 43.54 μg/mL. | [142] | |
| Leaves/methanol | Vero cells. | IC50 values at 24 h exposure = 361.44 ± 10.68 μg/mL; at 48 h exposure = 319.37 ± 99.80 μg/mL. | [103] | |
| DNA protection | Leaves/water | H2O2 photolysis by UV radiation in the presence of pBR322 plasmid DNA and an aqueous extract (50 g). | Treatment with the extract at the evaluated dose completely protected the plasmid DNA. | [162] |
| Hemolytic | Leaves/water | The hemolytic activity of a crude extract and the hexane–ethyl acetate (50:50), chloroform, methanolic, and ethanolic partitions were screened at different concentrations (125, 250, 500, and 1000 μg/mL). | CC50 values (μg/mL): aqueous extract = 8035.9; hexane–ethyl acetate (50:50) phase = 4470.4; chloroform phase = 2739.8; methanolic phase = 12332.0; ethanolic phase = 9496.4. | [107] |
| Hepatoprotective effect | Leaves/methanol | In vivo acetaminophen-induced hepatotoxicity on a mice model. The mice of groups III and IV received a dose of 25 and 75 mg extract/kg daily for 7 days before receiving a single dose of acetaminophen. The mice of groups V and VI received a dose of 25 and 75 mg extract/kg daily for 7 days before receiving a single dose of acetaminophen. Subsequently, the serum glutamate oxaloacetate transaminase (SGOT), serum glutamate pyruvate transaminase (SGPT), and alkaline phosphatase (ALP) activities were measured. | Among all of the tested groups, pretreatment with a 75 mg extract/kg significantly reduced the SGOT = 144.5 ± 3.74 (UI/L), SGPT = 112.4 ± 9.1 (UI/L), and ALP = 96.8 ± 3.2 (UI/L) activities compared to control groups. | [130] |
| Leaves/methanol (Lantadenes concentrated fraction) | A Ginkgo biloba methanolic extract (GBME) was evaluated against lantadenes-induced hepatic damage in guinea pigs. Guinea pigs (200–250 g) were divided into 5 groups. Group I: negative control; group II received 25 mg lantadenes/kg body weight; group III received 25 mg lantadenes/kg body weight + 100 mg GBME/kg body weight; group IV received 25 mg lantadenes/kg body weight + 200 mg GBME/kg body weight; group V: positive control, received 100 mg silymarin/kg body weight. The drugs were administered orally in gelatin capsules daily for 14 days. Analysis by HPLC of the lantadenes fraction (72.82% lantadene A). | Serum protein levels of group IV were significantly lower than group II. | [164] | |
| Insecticidal/larvicidal/termiticidal | Leaves/methanol, n-hexane | Methanol and n-hexane extracts were tested in vivo against Anopheles stephensi (Liston). | The methanol extract was more active than the n-hexane extract. The optimal dose for the repellent activity was 2 mg/mL. | [52] |
| Aerial parts/ethanol | Phthorimae operculella (Zeller). | High insecticidal effect against Phthorimae operculella (Zeller); no ovocidal effects. | [144] | |
| Leaves/ethyl acetate, methanol | Tested against Anopheles stephensi (Liston) and Culex quinquefasciatus (Say) larvae. | Ethyl acetate extract: 500 ppm, 30 min: 98% mortality and 500 ppm, 30 min: 93% mortality. Methanol extract: 500 ppm, 30 min: 82% mortality and 500 ppm, 30 min: 86% mortality. | [145] | |
| Whole plant/ethanol | The in vitro larvicidal activity of the methanol and petroleum ether partitions from extracts of different parts of the plant were assayed with the brine shrimp lethality test. | Methanol partitions: leaves: LC50 = 18 μg/mL; roots: LC50 = 17 μg/mL; twigs and stems: LC50 = 0.3 μg/mL. Petroleum ether partitions: leaves: LC50 = 54 μg/mL; roots: LC50 = 47 μg/mL; twigs: LC50 = 62 μg/mL; stems: LC50 = 3.6 μg/mL. | [86] | |
| Leaves/chloroform | The termiticidal activity of several extracts was screened against Microcerotermes beesoni. | Most active extract: LD50 = 5 μg/insect. | [146] | |
| Leaves and seeds/powder | Applied to Zea mays L. against Sitophilus zeamais. | 63.3% mortality of Sitophilus zeamais on the twenty-eighth day. | [147] | |
| Leaves/n-hexane | Different concentrations (10%, 5%, 2.5%, 1.25%, 0.1%, 0.05%, 0.025%, 0.0125%, and 0.00625%) of a crude extract were tested against Dysdercus koenigii Fabricius nymphs for 24 h and monitored for 7 days. | Survival of nymphs at 10%, 5%, 2.5%, and 1.25% concentrations = 65.33%, 66.67%, 72%, and 85.33%. Reduction in the longevity at 10% and 5% concentrations = 5.54 and 5.95 days. | [148] | |
| Leaves and flowers/ethanol | Crude extracts were tested against Anopheles arabiensis and Culex quinquefasciatus larvae. | Flowers: A. arabiensis, LC50 = 15.84 ppm; C. quinquefasciatus, LC50 = 21.37 ppm. Leaves: A. arabiensis, LC50 = 9.54 ppm; C. quinquefasciatus, LC50 = 5.01 ppm. | [149] | |
| Whole plant/water, acetone, chloroform, ethanol, and methanol | The larvicidal activity of different concentrations (25, 50, 75, 100, and 150 ppm) of crude extract was screened for 24 h against Aedes aegypti, Anopheles stephensis, and Culex quinquefasciatus. | The most active extracts: methanol: A. aegypti, LC50 = 39.54 ppm; A. stephensis, LC50 = 35.65 ppm; C. quinquefasciatus, LC50 = 35.36 ppm; ethanol: A. aegypti LC50 = 60.93 ppm; A. stephensi, LC50 = 79.03 ppm; C. quinquefasciatus, LC50 = 50.17 ppm. | [150] | |
| Leaves/diluted aqueous juice | Different concentrations (25, 50, 75, and 100 ppm) were tested against Aedes aegypti, Anopheles subpictus, and Culex quinquefasciatus larvae during 6, 12, and 24 h. | LC50 values ranged from 47.47 to 101.68 ppm. | [151] | |
| Leaves/acetone | The insecticidal activity of different concentrations (100, 200, 300, 400, and 500 ppm) of a crude extract was tested against Aedes aegypti L. larvae and pupae for 24 h. | Larvae: LC50 = 198.52 ppm; pupae: LC50 = 309.64 ppm. | [59] | |
| Leaves/water | The insecticidal activity of different concentrations (62.5, 125, 250, 500, and 1000 ppm) of a crude extract was tested against Aedes aegypti L. and Culex quinquefasciatus Say larvae for 24 h. | A. aegypti L.: LC50 = 35.48 ppm; C. quinquefasciatus: LC50 = 35.19 ppm. | [152] | |
| Leaves/95% ethanol | Different concentrations (250–3000 ppm) of a crude extract were tested against Anopheles arabiensis Patton larvae. | LC50 = 477.53 ppm. | [153] | |
| Phytotoxic | Leaves/water | Different concentrations (0%, 1.25%, 2.5%, 3.75%, and 5%, v/v) of a crude extract were tested on Bidens pilosa seeds. | The aqueous extract reduced the viability of Bidens pilosa seeds during phase III of germination. At any concentration, the aqueous extract inhibited the root and epicotyl growth. | [154] |
| Leaves/methanol–water (70:30) | A crude extract, at the concentration of 5 g/L, was tested on Eichhornia crassipes (Mart.) Solms and Microcystis aeruginosa Kütz. | E. crassipes: complete inhibition; M. aeruginosa: 66.1% inhibition. | [110] | |
| Leaves and callus/water | The inhibition of seed germination by crude extracts was tested on Brassica campestris var. chinensis, Ipomoea aquatica Forsk., Sorghum bicolor L., and Zea mays L. | Extract concentration that caused 50% inhibition of seed germination: B. campestris: leaves = 0.62%, callus = 0.65%; I. aquatica: leaves = 0.94%, callus = 0.45%; S. bicolor: leaves = 0.95%, callus = 1.19%; Z. mays: leaves = 4.39%, callus = 3.05%. | [165] | |
| Leaves/water | An aqueous leaf leachate was tested on Eichhornia crassipes (Mart.) Solms. | The concentration of 5% was the most toxic after 21 days. | [166] | |
| Callus/water | An aqueous leaf leachate was tested on Salvinia molesta Mitchell. | The concentration of 1% was the most toxic after 7 days. | [167] | |
| Callus/water | A crude extract encapsulated in calcium alginate beads was tested on Brassica campestris var. chinensis. | Beads with 5% extract had no effect on the germination rate, while beads with 1–4% extract did not reduce the total weight of fresh seedlings. | [168] | |
| Wound-healing effects | Leaves/water Leaves/ethanol | Daily topical application of 100 mg extract/kg body weight on wounds of male Sprague Dawley rats (200–220 g). Bovine dermatophilosis caused by Dermatophilus congolensis was treated with ointments containing L. camara leaf ethanolic extracts once a day for 10 days. | Mean epithelization time and % of wound healing: placebo group = 19 ± 0.14 days and 88%; tested group = 17.20 ± 0.12 days and 98%. Wound healing was observed between the third and fourth day of application without recurrence. | [169] [108] |
| Compound a,* (Nº) | Biological Activity | Reference |
|---|---|---|
| Acetyl lantanoside * (144) | In vitro antibacterial activity against Mycobacterium tuberculosis strain H37Rv (ATCC 27294): 98% inhibition, MIC < 11.15 μM. | [16,134] |
| 22β-Acetyloxy-oleanonic acid * (37) | In vitro cytotoxic activity towards human leukemia HL-60 cells: IC50 = 75.09 ± 0.09 μM; human cervical carcinoma Hela cells: IC50 = 72.75 ± 0.29 μM; colon 502,713 cells: IC50 = 67.1 ± 0.04 μM; lung carcinoma A549 cells: IC50 = 71.77 ± 0.15 μM. | [94] |
| 22β-Benzoyloxy-oleanonic acid * (85) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 88.38 ± 0.15 μM; Hela cells: IC50 = 80.55 ± 0.15 μM; colon 502,713 cells: IC50 = 89.07 ± 0.04 μM; lung A549 cells: IC50 > 100 μM. | [94] |
| 22β-Butanoyloxy-oleanonic acid * (50) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 39.94 ± 0.23 μM; Hela cells: IC50 = 42.16 ± 0.15 μM; colon 502,713 cells: IC50 = 46.6 ± 0.28 μM; lung A549 cells: IC50 = 50.11 ± 0.09 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene/12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg/kg body weight administered orally for 20 weeks: 80% mice survival and 17.2% overall papilloma incidence. | [94] |
| Camaric acid (62) | In vitro nematocidal activity towards Meloidogyne incognita larvae: 95% mortality at 0.5% concentration after 48 h. In vitro antiparasitic activity towards Leishmania mexicana promastigotes: IC50 = 2.52 ± 0.08 μM. In vitro protein tyrosine phosphatase 1B inhibition assay: IC50 = 5.1 μM [84]. In vitro cytotoxic activity towards HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 1.71 ± 0.10 μM. In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 3 μM. | [80,82,84,99,117,118] |
| Camarin (23) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at 1 mg/mL concentration after 48 h. | [90] |
| Camarinic acid (114) | In vitro antimicrobial and antifungal activity index values: E. coli = 2, S. aureus = 0.95, P. aeruginosa = 0.15, S. typhi = 0.7, C. albicans = 0.2, T. mentagrophytes = 2.3. In vivo antimutagenic evaluation: micronucleus test (2.75 mg mitomycin D/kg body weight and 6.75 mg/kg body weight given orally to Swiss strain mice, once a day-48 h): 76.7% reduction in the number of micronucleated polychromatic erythrocytes. In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at 1% concentration after 24 h. In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 89 ± 0.3 μM. | [16,78] |
| Camarinin (56) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at 1 mg/mL concentration after 48 h. | [90] |
| Di-(2-ethylhexyl) phthalate (166) | In vitro antibacterial activity (disk diffusion method), zone inhibition diameter: Escherichia coli = 20 mm, Staphylococcus aureus = 22 mm, Salmonella typhimurium = 21 mm, Pseudomonas aerugionosa = 23 mm. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 8.1 μM. | [73,84] |
| Ethyl-β-D-galactopyranoside (163) | Inactive in an in vitro antiparasitic activity assay towards Brugia malayi. | [74] |
| 3-O-β-D-Glucosyl oleanolic acid (84) | In vivo antiulcer activity: aspirin-induced and ethanol-induced ulcer models; Albino Wistar rats (150–200 g) were divided into 4 groups. Groups III and IV received 25 and 50 mg compound/kg body weight, respectively, orally once a day for 5 days. Ulcer index: 3.48± 0.83 and 1.99 ± 0.34, respectively; protection: 21.24 and 38.37%, respectively. | [126] |
| Hispidulin (128) | In vitro protein tyrosine phosphatase inhibition assay: IC50 > 33 μM. | [72,79,84] |
| 9-Hydroxy-lantadene A (64) | In vitro antifungal activity against Fusarium subglutinans (PPRI 6740), F. solani (PPRI 19147), F. graminearum (PPRI 10728), and F. semitectum (PPRI 6739): MIC ˃ 1000 μM; against F. proliferatum (PPRI 18679): MIC = 70.32 μM. In vitro cytotoxic activity towards Raw 264.7 cells: IC50 ˃ 100 μM. | [120] |
| 24-Hydroxy-lantadene B ≡ 24-Hydroxy-22β-senecioyloxy-oleanonic acid (65) | Binding affinity to the antiapoptotic protein Bcl-xL: Ki = 5.3 μM. In vitro cytotoxic activity towards papilloma KB cells: IC50 = 35.5 μM; colon carcinoma HCT-116 cells: IC50 = 11.4 μM; breast adenocarcinoma MCF7 cells: IC50 = 42.5 μM; lymphocytic leukemia L1210 cells: IC50 = 12.3 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 7.3 μM. | [84,116] |
| 24-Hydroxy-lantadene D (53) | In vitro protein tyrosine phosphatase inhibition assay: IC50 >18 μM. | [84] |
| 22β-Hydroxy- oleanolic acid (32) | In vitro cytotoxic activity: tested on multiple cancer cells. In vitro anti-inflammatory activity (TNF-α-induced NF-ΚB activation inhibitory activity): IC50 ˃10 μM; COX-2 inhibition: IC50 ˃100 μM. In vitro cytotoxic activity towards A549 cells: IC50 ˃10 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 7.9 μM. | [80,84,95,96] |
| 22β-Hydroxy-oleanonic acid (26) | In vitro antitumor activity: Epstein–Barr virus early antigen activation assay induced by 12-O-tetradecanoylphorbol-13-O-acetate (TPA) in Raji cells: 35.3% inhibition at 100 mol tested compound/1 mol TPA. In vivo hepatotoxicity evaluation (adult female guinea pigs received 125 mg compound/kg body weight orally in gelatin capsules): bilirubin: 0.67 ± 0.001 mg/100 mL, SGOT: 46.1 ± 0.4 U/L, SGPT: 39 ± 0.3 U/L; nontoxic. In vitro cytotoxic activity towards HL-60, Hela, colon 502,713, and lung A549 cells: IC50 > 100 μM; A549 cells: IC50 ˃ 10 μM [94]. In vitro anti-inflammatory activity (inhibitory activity of TNF-α-induced NF-ΚB activation): IC50 = 6.42 ± 1.24 μM; COX-2 inhibition: IC50 ˃ 100 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 6.9 μM. | [84,92,93,94,95,96] |
| 11α-Hydroxy-3-oxo-urs-12-en-28-oic acid (101) | In vitro nematocidal activity against Meloidogyne incognita larvae: 70% mortality at 0.25% concentration after 72 h. | [82] |
| Icterogenin (67) | Binding affinity to the antiapoptotic protein Bcl-xL: Ki = 7.6 μM. In vitro cytotoxic activity towards KB cells: IC50 = 15 μM; HCT-116 colon cancer cells: IC50 = 5.8 μM; MCF7 cells: IC50 = 11.3; L1210 lymphocytic leukemia cells: IC50 = 6.8 μM; HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 34.2 ± 0.7 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 11 μM. In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 3 μM. DPPH radical scavenging activity: IC50 = 169.7 μg/mL. | [109] |
| Lancamarinic acid (41) | In vitro screening against a variety of Gram-positive and Gram-negative bacteria (disk diffusion method). | [105] |
| Lancamarolide (42) | In vitro nematocidal activity against Meloidogyne incognita larvae: 80% mortality at 0.25% concentration after 48 h. | [81] |
| Lantacamaric acid A (29) | In vitro cytotoxic activity towards HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 30.8 ± 2.7 μM. | [99] |
| Lantacamaric acid B (70) | In vitro cytotoxic activity towards HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 6.60 ± 0.46 μM. | [99] |
| Lantacin (119) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at 1 mg/mL concentration after 48 h. | [81,90] |
| Lantadene A (Rehmannic acid) (60) | In vitro larvicidal activity: very toxic in the brine shrimp lethality test; insecticidal activity at 5.0 mg/mL towards Spodoptera littoralis Biosduval: 40% lethality after 48 h; fecundity inhibition assay in Clavigralla tomentosicollis Stal.: 50% fecundity suppression; inactive towards Aphis craccivora Koch. In vivo antimotility effect evaluation (Laca strain male mice (20–25 g) received a single injection of 85 and 170 mg compound/kg body weight): % intestinal transit = 39.47 ± 10.05 and 27.34 ± 4.58, respectively. Phytotoxic activity towards Eichhornia crassipes (Mart.) Solms and Microcystis aeruginosa Kutz: ErC50 = 24.78 and 21.34 mg/L, respectively. In vivo hepatotoxicity evaluation (adult female guinea pigs received 125 mg compound/kg body weight orally in gelatin capsules): bilirubin = 8.74 ± 2.5 mg/100 mL, SGOT = 696.3 ± 3.1 U/L, SGPT = 305.2 ± 3.9 U/L; toxic. In vitro cytotoxicity towards HL-60 cells: IC50 = 35.81 ± 0.40 and 35 ± 1 μM; HeLa cells: IC50 = 42.15 ± 0.09 and 42 ± 8 μM; colon 502,713 cells: IC50 = 38.53 ± 0.09 and 38 ± 5 μM μM; lung A549 cells: IC50 = 39.43 ± 0.21, 39 ± 1 μM μM, and 2.84 ± 0.72 μM; KB cells: IC50 = 15.8 μM; HCT-116 cells: IC50 = 41.8 μM; MCF7 cells: IC50 = 44.7 and ˃ 100 μM; L1210 cells: IC50 = 16.3 μM; HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 25.4 ± 3.1 μM; LNcap prostatic cancer cells: IC50 ˃ 100 μM; RWPE-1 prostatic cancer cells: IC50 ˃ 100 μM. Lantadene A-gold nanoparticles reduced MCF-7 (breast cancer cells) viability, upregulated the p53 expression, and downregulated the BCL-2 expression. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: 80–100% mice survival and 17.9–18.1% overall papilloma incidence. Binding affinity to the antiapoptotic protein Bcl-xL: Ki > 100 μM. Antioxidant activity in a dose-dependent manner. Toxicity evaluation: toxic (2 g) orally to sheep; nontoxic to lambs (167 mg compound/kg body weight administered orally in gelatin capsules) and guinea pigs (667 mg compound/kg body weight administered orally in gelatin capsules). In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 20.4 ± 0.1 μM. In vitro anti-inflammatory activity (inhibition of TNF-α-induced NF-ΚB activation): IC50 = 1.06 ± 0.46 μM; COX-2 inhibition: IC50 ˃ 100 μM. In vitro nematocidal activity towards Meloidogyne incognita larvae: 70% mortality at 0.5% concentration after 48 h. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 5.2 μM. DPPH radical scavenging activity: IC50 = 93.94 μM. | [78,82,84,86,91,92,93,94,95,96,99,100,105,109,110,111,112,113,114,115,116] |
| Lantadene A acyl chloride * (58) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 47.79 ± 0.24 μM; Hela cells: IC50 = 46.21 ± 0.17 μM; colon 502,713 cells: IC50 = 49.19 ± 0.17 μM; lung A549 cells: IC50 = 50.07 ± 0.14 μM. | [93] |
| Lantadene A methyl ester * (81) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 34.04 ± 0.26 and 34 ± 1.4 μM; Hela cells: IC50 = 37.93 ± 0.09 and 37 ± 5 μM; colon 502,713 cells: IC50 = 37.22 ± 0.15 and 37 ± 8 μM; lung A549 cells: IC50 = 33.87 ± 0.09 and 33 ± 5 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: 87.5–100% mice survival and 13.6–19.6% overall papilloma incidence. | [112] |
| Lantadene A nitrile * (57) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 70.43 ± 0.22 μM; Hela cells: IC50 = 74.0 ± 0.09 μM; colon 502,713 cells: IC50 = 78.68 ± 0.15 μM; lung A549 cells: IC50 = 82.80 ± 0.18 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight given orally for 20 weeks: 75% mice survival and 24.9% overall papilloma incidence. | [93] |
| Lantadene B (61) | Phytotoxic activity against Eichhornia crassipes (Mart.) Solms and Microcystis aeruginosa Kütz: ErC50 = 19.53 and 17.37 mM, respectively. Binding affinity to the antiapoptotic protein Bcl-xL: Ki > 100 μM. In vitro cytotoxic activity against KB cells: IC50 = 25.3 μM; HCT-116 cells: IC50 = 11.4 μM; MCF-7 cells: IC50 = 44 μM and ˃ 100 μM; L1210 cells: IC50 = 16.1 μM; A549 (lung carcinoma) cells: IC50 = 1.19 ± 0.28 μM. In vitro cytotoxic activity (MTT test) towards MCF-7 breast cancer cells: IC50 = 1.13 μM. In vitro anti-inflammatory activity (inhibition of TNF-α-induced NF-ΚB activation): IC50 = 1.56 ± 0.04 μM; COX-2 inhibition: IC50 ˃ 100 μM. In vitro nematocidal activity against Meloidogyne incognita larvae: 60% mortality at 0.25% concentration after 48 h; against Leishmania mexicana promastigotes, IC50 = 23.45 ± 2.15 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 5.5 μM. DPPH radical scavenging activity: IC50 = 76.45 μM. | [82,84,95,96,109,110,116,117,124] |
| Lantadene C (72) | Binding affinity to the antiapoptotic protein Bcl-xL: Ki > 100 μM. In vitro cytotoxic activity towards KB cells: IC50 = 15.8 μM; HCT-116 cells: IC50 = 41.8 μM; MCF7 cells: IC50 = 44.7 and ˃ 100 μM; L1210 cells: IC50 = 16.3 μM; HL-60 cells: IC50 ˃ 100 μM; Hela cells: IC50 ˃ 100 μM; colon 502,713 cells: IC50 ˃ 100 μM; lung A549 cells: IC50 ˃ 100 μM. DPPH radical scavenging activity: IC50 ˃ 100 μM. | [84,116] |
| Lantadene D (51) | In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight given orally for 20 weeks: approximately 85% mice survival and 30% overall papilloma incidence. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 7.9 μM [84]. | [84,97] |
| Lantanilic acid (68) | In vitro nematocidal activity against Meloidogyne incognita larvae: 98.66% mortality at 0.5% concentration after 48 h. In vitro antiparasitic activity against Leishmania mexicana promastigotes: IC50 = 9.50 ± 0.28 μM; L. major promastigotes: IC50 = 21.3 ± 0.02 μM; brine shrimp toxicity assay: LC50 = 49.20 μM. In vitro antibacterial and antifungal activity: diameter of inhibition zone at a concentration of 500 μg/mL against S. aureus = 1.7 mm and against C. albicans = 9.3 mm. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 7.5 μM [84]. In vitro cytotoxic activity towards HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 4.00 ± 0.67 μM. In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 3 μM. | [78,80,81,84,98,99,118,122,123] |
| Lantaninilic acid (30) | In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 164 ± 0.8 μM. In vitro nematocidal activity against Meloidogyne incognita larvae: 60% mortality at a concentration of 0.125% after 48 h. In vitro cytotoxic activity towards HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 68.4 ± 15.4 μM. | [78,82] |
| Lantanolic acid (27) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at a concentration of 1 mg/mL after 24 h. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 13 μM. | [84,90] |
| Lantanoside (140) | In vitro nematocidal activity against Meloidogyne incognita larvae: 95% mortality at a concentration of 1% after 48 h. In vitro antibacterial activity against Mycobacterium tuberculosis strain H37Rv (ATCC 27294): 37% inhibition, MIC > 12.05 μM. | [16,134] |
| Lantic acid (102) | In vitro antimicrobial activity (bioautography assays): minimum growth inhibition values for B. subtilis (ATCC 6633), M. luteus (ATCC 9341), S. aureus (ATCC 6538P), and P. mirabilis (ATCC 14153) = 0.3 μg; B. cereus (ATCC 11778) = 0.1 μg; S. faecalis (ATCC 8043) and P. aeruginosa (ATCC 25619) = 1.1 nmol; E. coli (ATCC 25922) = 0.17 nmol. In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at a concentration of 1 mg/mL after 24 h. | [90] |
| Lantoic acid (105) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at a concentration of 1 mg/mL after 24 h. In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 97 ± 0.02 μM. | [81,90] |
| Lantrieuphpene A (13) | In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 30 μM. | [80] |
| Lantrieuphpene B (8) | In vitro anti-inflammatory activity: inhibition of LPS-induced NO production in BV-2 cells, IC50 = 24 ± 0.30 μM; ROS and NO levels in LPS-stimulated zebrafish embryos significantly decreased in a concentration-dependent manner. Western blotting: iNOS protein expression decreased in a dose-dependent manner on pretreated cells. | [80] |
| Lantrieuphpene C (9) | In vitro anti-inflammatory activity: inhibition of LPS-induced NO production in BV-2 cells, IC50 = 27.98 ± 0.98 μM; ROS and NO levels in LPS-stimulated zebrafish embryos significantly decreased in a concentration-dependent manner. Western blotting: iNOS protein expression decreased in a dose-dependent manner on pretreated cells. | [80] |
| Lantrieuphpene D (12) | In vitro anti-inflammatory activity: inhibition of LPS-induced NO production in BV-2 cells, IC50 > 10 μM. | [80] |
| Linaroside (139) | In vitro nematocidal activity against Meloidogyne incognita larvae: 90% mortality at a concentration of 1% after 48 h. In vitro antibacterial activity against the Mycobacterium tuberculosis strain H37Rv (ATCC 27294): 30% inhibition, MIC = 13.12 μM. In vitro antioxidant activity (DPPH test): IC50 = 149.09 mM. | [16,134,162] |
| Methyl 22β-acetyloxy-oleanonate * (45) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 72.75 ± 0.29 μM; Hela cells: IC50 = 70.6 ± 0.10 μM; colon 502,713 cells: IC50 = 67.48 ± 0.15 μM; lung A549 cells: IC50 = 71.77 ± 0.10 μM. | [94] |
| Methyl 22β-angelyloxy-2-hydroxy-3-oxo-olean-1,12-diene-28-oate (78) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 26 ± 6 μM; HeLa cells: IC50 = 31 ± 5 μM; colon 502,713 cells: IC50 = 32 ± 1 μM; lung A549 cells: IC50 = 28 ± 4 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: approximately 100% mice survival and 17.2% overall papilloma incidence. | [124] |
| Methyl 22β-benzoyloxy-oleanonate * (86) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 81.52 ± 0.08 μM; Hela cells: IC50 = 86.10 ± 0.08 μM; colon 502,713 and lung A-549 cells: IC50 > 100 μM. | [94] |
| Methyl 22β-butanoyloxy-oleanonate * (73) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 34.79 ± 0.14 μM; Hela cells: IC50 = 36.23 ± 0.38 μM; colon 502,713 cells: IC50 = 38.03 ± 0.09 μM; lung A549 cells: IC50 = 40.37 ± 0.09 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a]anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: 80% mice survival and 12.4% overall papilloma incidence. | [94] |
| Methyl 22β-hydroxy-oleanonate * (35) | In vitro cytotoxicity towards HL-60 cells: IC50 ˃ 100 μM; Hela cells: IC50 > 100 μM; colon 502,713 cells: IC50 ˃ 100 μM; lung A549 cells: IC50 ˃ 100 μM. | [91,94] |
| Methyl 22β-isobutyryloxy-oleanonate * (74) | In vitro cytotoxicity towards HL-60 cells: IC50 = 71.19 ± 0.09 μM; Hela cells: IC50 = 74.08 ± 0.38 μM; colon 502,713 cells: IC50 = 68.67 ± 0.09 μM; lung A549 cells: IC50 = 76.06 ± 0.14 μM. | [94] |
| Methyl 22β-propanoyloxy-oleanonate * (52) | In vitro cytotoxicity towards HL-60 cells: IC50 = 44.75 ± 0.39 μM; Hela cells: IC50 = 48.81 ± 0.15 μM; colon 502,713 cells: IC50 = 41.42 ± 0.15 μM; lung A549 cells: IC50 = 52.52 ± 0.39 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a] anthracene-12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: 80% mice survival and 17.9% overall papilloma incidence. | [94] |
| Oleanolic acid (31) | In vitro larvicidal activity: 30% lethality in the brine shrimp lethality test against Spodoptera littoralis Biosduval after 48 h at a concentration of 10.95 mM. Inactive in the fecundity inhibition assay against Clavigralla tomentosicollis Stal. and Aphis craccivora Koch. In vitro nematocidal activity against Meloidogyne incognita larvae: 70.33% mortality at a concentration of 0.5% after 48 h. In vitro antifilarial activity against Brugia malayi: LC100 = 136.85 μM. In vivo antifilarial activity against Brugia malayi in rodel model Mastomys coucha (100 or 200 mg compound/kg body weight administered intraperitoneally for 5 days): macrofilaricidal efficacy = 9.09% and 18.18%, respectively; percent female sterility = 49.22 ± 10.57 and 56.50 ± 9.50, respectively. In vitro cytotoxic activity towards HCT-15 cells: IC50 = 52 μM; SW-620 cells: IC50 = 25 μM; A549 cells: IC50 = 52 μM; IGROV-1 cells: IC50 = 8 μM; IMR-32 cells: IC50 = 61 μM. In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 53 ± 0.02 μM. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 2 μM. In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 60 μM. | [75,78,80,84,86,87,118] |
| Oleanonic acid (22) | In vitro larvicidal activity: 20% lethality in the brine shrimp lethality test against Spodoptera littoralis Biosduval: after 48 h at a concentration of 10.996 mM. Inactive in the fecundity inhibition assay towards Clavigralla tomentosicollis Stal. and Aphis craccivora Koch. In vitro antifilarial activity against Brugia malayi: LC100 = 68.73 μg/mL. In vivo antifilarial activity against Brugia malayi in rodel model Mastomys coucha (100 or 200 mg compound/kg body weight administered intraperitoneally for 5 days), macrofilaricidal efficacy: inactive; % female sterility: 56.56 ± 9.49 and 29.71 ± 6.52, respectively. In vitro cytotoxic activity towards EAC cells: IC50 = 7.1 ± 1.3 μM; A375 cells: IC50 = 10.9 ± 1.5 μM; Hep2 cells: IC50 = 59.3 ± 1.1 μM; U937 cells: IC50 = 16.5 ± 1.3 μM; HL-60 human promyelocytic leukemia cells (JCRB0085): IC50 = 9.79 ± 2.13 μM; PMBC cells: IC50 > 100 μM. In vitro nematocidal activity against Meloidogyne incognita larvae: 80% mortality at a concentration of 0.5% after 48 h. In vitro protein tyrosine phosphatase inhibition essay: IC50 = 6.9 μM [84]. | [26,75,82,84,86,88,99] |
| 11-Oxo-β-boswellic acid (103) | In vitro antifungal activity against Fusarium subglutinans (PPRI 6740) and F. semitectum (PPRI 6739): MIC = 1.338 mM; F. proliferatum (PPRI 18679): MIC = 2.762 mM; F. solani (PPRI 19147) and F. graminearum (PPRI 10728): MIC = 5.311 mM. In vitro cytotoxicity towards Raw 264.7 cells: IC50 ˃ 100 μM. | [120] |
| Pomolic acid (107) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at a concentration of 1 mg/mL after 24 h. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 10.6 μM. | [84,90] |
| Pomonic acid (104) | In vitro protein tyrosine phosphatase inhibition assay: IC50 = 10.5 μM. In vitro anti-inflammatory activity (inhibition of LPS-induced NO production in BV-2 cells): IC50 > 30 μM. | [80,84] |
| 22β-Propanoyl- oxy-oleanonic acid * (46) | In vitro cytotoxic activity towards HL-60 cells: IC50 = 50.12 ± 0.32 μM; Hela cells: IC50 = 54.29 ± 0.09 μM; colon 502,713 cells: IC50 = 48.22 ± 0.09 μM; lung A549 cells: IC50 = 56.19 ± 0.26 μM. In vivo antitumor activity: squamous cell carcinogenesis induced by 7,12-dimethylbenz[a] anthracene/12-O-tetradecanoylphorbol-13-O-acetate in Swiss albino mice (LACCA/female); 50 mg compound/kg body weight administered orally for 20 weeks: 80% mice survival and 19.6% overall papilloma incidence. | [94] |
| Reduced lantadene A (22β-angelyloxy-3β-hydroxy-olean-12-en-28-oic acid) (75) | Evaluation of toxicity to sheep: 80 mg compound/kg body weight administered orally in gelatin capsules: nontoxic; 80 mg compound/kg body weight, dissolved in DMSO, intraruminal administration: toxic. Evaluation of toxicity to Wistar female rats: 15 mg compound/kg body weight administered orally in olive oil: toxic. In vitro antitumor activity: Epstein–Barr virus early antigen activation assay induced by 12-O-tetradecanoylphorbol-13-O-acetate (TPA) in Raji cells: 30.6% inhibition at a concentration of 100 mol compound/1 mol TPA. In vitro cytotoxicity was tested towards multiple cancer cells. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 7.2 μM. | [84,91,95] |
| Reduced lantadene B (3β-hydroxy-22β-senecioyloxy-olean-12-en-28-oic acid) (76) | In vitro cytotoxicity was tested towards multiple cancer cells. In vitro protein tyrosine phosphatase inhibition assay: IC50 = 5.1 μM. | [95] |
| Reduced lantadene C 3β-hydroxy-22β-[2-methylbutanoyloxy]-olean-12-en-28-oic acid (77) | In vitro protein tyrosine phosphatase 1B inhibition assay: IC50 = 7.3 μM. | [84] |
| β-Sitosterol (3) | In vitro antiparasitic activity against Brugia malayi: LC100 > 1.2 mM. Antibacterial activity (disk diffusion method): diameter of inhibition zone = 14 mm for Escherichia coli, 19 mm for Staphylococcus aureus, 17 mm for Salmonella typhimurium, 24 mm for Pseudomonas aeruginosa. The cytotoxic potential was tested in vitro by an MTT assay against T47D (breast cancer cells) and HeLa (cervical cancer cells): IC50 = 24.06 and 24.86 µM, respectively. | [73,74,170] |
| β-Sitosterol 3-O-β-D-glucopyrano-side (4) | In vitro antiparasitic activity against Brugia malayi: LC100 > 0.86 mM. | [71] |
| Stearic acid (158) | In vitro antiparasitic activity against Brugia malayi: LC100 > 1.7 mM. | [74,77] |
| Trilinolein (168) | In vitro antibacterial activity (disk diffusion method): diameter of inhibition zone = 20 mm for Escherichia coli, 19 mm for Staphylococcus aureus, 18 mm for Salmonella typhimurium, 21 mm for Pseudomonas aeruginosa. | [73] |
| Urs-12-en-3β-ol-28-oic acid 3-O-β-D-glucopyrano- syl-4′-octadecano- ate (127) | In vivo antidiabetic activity: Wistar albino rats (150–200 g) received 0.3 mg/kg body weight orally for 21 days. Blood glucose levels: 8th day = 183.56 ± 3.61 mg/dL, 14th day = 143.43 ± 2.79 mg/dL, 21st day = 118.67 ± 2.40 mg/dL. In vivo anxiolytic activity: dose-dependent effect. | [125] |
| Ursolic acid (106) | In vitro nematocidal activity against Meloidogyne incognita larvae: 100% mortality at a concentration of 1 mg/mL after 48 h. In vitro antiparasitic activity against Leishmania major promastigotes: IC50 = 12.4 ± 0.03 μM. | [78,90] |
| Compound (Nº) | Docking Value | Reference |
|---|---|---|
| Camaranoic acid (99) | Molecular docking into the active site of SARS-CoV-2 RNA-dependent RNA polymerase (RdRp): binding free energy = 1.272 kcal/mol. | [81] |
| Camaric acid (62) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −3.198 kcal/mol. | [81] |
| Camarolic acid (69) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −6.73 kcal/mol. | [81] |
| Icterogenin (67) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding energy = −2.311 kcal/mol. | [81] |
| Lantabetulic acid (17) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −2.958 kcal/mol. | [81] |
| Lantacin (119) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −2.919 kcal/mol. | [81] |
| Lantaiursolic acid (120) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −3.867 kcal/mol. | [81] |
| Lantanilic acid (68) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −3.633 kcal/mol. | [81] |
| Lantoic acid (105) | Molecular docking into the active site of SARS-CoV-2 RdRp: binding free energy = −6.07 kcal/mol. | [81] |
| Lantrieuphpene B (8) | Binding free energy = −9.8 Kcal/mol with TYR-341, TYR-367, and ASP-376 residues of iNOS (inducible Nitric Oxide Synthase). | [80] |
| Lantrieuphpene C (9) | Molecular binding free energy = −9.3 Kcal/mol with TYR-341, TYR-367, and ASP-376 residues of iNOS. | [80] |
| β-Sitosterol (3) | Molecular binding free energies towards Bcl-2 and HPV16 E7 protein receptors: −8.11 and −7.276 kcal/mol, respectively | [170] |
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Byng, J.W.; Chase, M.W.; Christenhusz, M.J.; Fay, M.F.; Judd, W.S.; Mabberley, D.J. An update of the angiosperm phylogeny group classification for the orders and families of flowering plants: APG IV. Bot. J. Linn. Soc. 2016, 181, 1–20. [Google Scholar]
- WFO Plant List. Snapshots of the Taxonomy. Search for Lantana L. WFO Plant List | World Flora Online. Available online: https://wfoplantlist.org/taxon/wfo-4000020568-2023-12?page=1 (accessed on 9 March 2024).
- Cardoso, P.H.; O’Leary, N.; Olmstead, R.G.; Moroni, P.; Thode, V.A. An update of the Verbenaceae genera and species numbers. Plant Ecol. Evol. 2021, 154, 80–86. [Google Scholar] [CrossRef]
- Lu-Irving, P.; Bedoya, A.M.; Salimena, F.R.G.; dos Santos Silva, T.R.; Viccini, L.F.; Bitencourt, C. Phylogeny of Lantana, Lippia, and related genera (Lantaneae: Verbenaceae). Am. J. Bot. 2021, 108, 1354–1373. [Google Scholar] [CrossRef]
- Babar, V.B.; Khapale, P.R.; Nagarale, S.N. Preliminary investigation and in-vitro anticancer activity of Lantana camara L. (Verbenaceae). J. Pharmacogn. Phytochem. 2019, 8, 2524–2527. [Google Scholar]
- El Baroty, G.S.; Goda, H.M.; Khalifa, E.A.; Abd El Baky, H.H. Antimicrobial and antioxidant activities of leaves and flowers essential oils of Egyptian Lantana camara L. Der Pharma Chem. 2014, 6, 246–255. [Google Scholar]
- Saraf, A.; Quereshi, S.; Sharma, K.; Khan, N.A. Antimicrobial activity of Lantana camara L. J. Exp. Sci. 2011, 2, 50–54. [Google Scholar]
- Al-Hakeim, H.K.; Al-Zabibah, R.S.; Alzihari, H.F.; Almensoori, A.K.; Al-Zubaidi, H.A.; Hassan, L.E.A.H. Anticancer and antiangiogenic activities of alkaloids isolated from Lantana camara by adsorption on the magnetic nanoparticles. Karbala Int. J. Mod. Sci. 2021, 7, 11. [Google Scholar] [CrossRef]
- Sharma, G.P.; Raghubanshi, A.S.; Singh, J.S. Lantana invasion: An overview. Weed Biol. Manag. 2005, 5, 157–165. [Google Scholar] [CrossRef]
- Day, M.D.; Zalucki, M.P. Lantana camara Linn. (Verbenaceae). In Biological Control of Tropical Weeds Using Arthropods; Cambridge University Press: Cambridge, UK, 2009; pp. 211–246. [Google Scholar]
- Thomas, S.E. Lantana camara (lantana). In CABI Compendium; CABI Digital Library: Wallingford, UK, 2022. [Google Scholar] [CrossRef]
- Goyal, N.; Sharma, G.P. Lantana camara L. (sensu lato): An enigmatic complex. NeoBiota 2015, 25, 15–26. [Google Scholar]
- Sanders, R.W. Taxonomy of Lantana Sect. Lantana (Verbenaceae): II. Taxonomic revision. J. Bot. Res. Inst. Texas 2012, 6, 403–441. [Google Scholar]
- Urban, A.J.; Simelane, D.O.; Retief, E.; Heystek, F.; Williams, H.E.; Madire, L.G. The invasive “Lantana camara L.” hybrid complex (Verbenaceae): A review of research into its identity and biological control in South Africa. Afr. Entomol. 2011, 19, 315–348. [Google Scholar] [CrossRef]
- Begum, S.; Zehra, S.Q.; Syed, I.; Hassan, S.I.; Siddiqui, B.S. Noroleanane triterpenoids from the aerial parts of Lantana camara. Helv. Chim. Acta 2008, 91, 460–467. [Google Scholar] [CrossRef]
- Begum, S.; Wahab, A.; Siddiqui, B.S.; Qamar, F. Nematocidal constituents of the aerial parts of Lantana camara. J. Nat. Prod. 2000, 63, 765–767. [Google Scholar] [CrossRef] [PubMed]
- Hussain, H.; Hussain, J.; Al-Harrasi, A.; Shinwari, Z.K. Chemistry of some species genus Lantana. Pak. J. Bot. 2011, 43, 51–62. [Google Scholar]
- Ved, A.; Arsi, T.; Prakash, O.; Gupta, A. A Review on phytochemistry and pharmacological activity of Lantana camara Linn. Int. J. Pharm. Sci. Res. 2018, 9, 37–43. [Google Scholar] [CrossRef]
- Al-Fadhli, A.A.; Nasser, J.A. Constituents from the root of Lantana camara. Asian J. Chem. 2014, 26, 8019–8021. [Google Scholar] [CrossRef]
- Madke, G.; Bhutkar, K.; Chaudhari, S.R. Overview on Lantana camara showing various pharmacological benefits. Int. Adv. Res. J. Sci. Eng. Technol. 2024, 11, 86–92. [Google Scholar] [CrossRef]
- Kumar, M.A.; Santoshi, S.; Patil, S.M.; Bhatt, S.P. A review on phytochemical and pharmacological profiling of Lantana camara Linn. W. J. Pharm. Pharm. Sci. 2023, 12, 15–25. [Google Scholar]
- Naphade, V.; Bhamre, J.S.; Avaghade, M.M.; Kale, M.S.; Bendale, A.R.; Borse, S.L.; Borse, L.B. Phytochemical and pharmacological potential of Lantana Camara Linn. Int. J. Life Sci. Pharma Res. 2023, 13, 70–80. [Google Scholar] [CrossRef]
- Shah, M.; Alharby, H.F.; Hakeem, K.R.; Munawar, M. A Comprehensive review on Lantana camara: An important medicinal and ornamental plant. Life Sci. J. 2024, 21, 10–17. [Google Scholar]
- Ghisalberti, E.L. Lantana camara L. (Verbenaceae). Fitoterapia 2000, 71, 467–486. [Google Scholar] [CrossRef]
- Beeby, P.J. Chemical modification of triterpenes from Lantana camara. 22β-Ester analogues of lantadene A. Aust. J. Chem. 1978, 31, 1313–1322. [Google Scholar] [CrossRef]
- Begum, S.; Raza, S.M.; Siddiqui, B.S.; Siddiqui, S. Triterpenoids from the aerial parts of Lantana camara. J. Nat. Prod. 1995, 58, 1570–1574. [Google Scholar] [CrossRef]
- Barua, A.K.; Chakrabarti, P.; Sanyal, P.K.; Das, B.C. Triterpenoids: XXXII. The structure of lantic acid—A new triterpene from Lantana camara. J. Indian Chem. Soc. 1969, 46, 100–101. [Google Scholar] [CrossRef]
- Sharma, O.P.; Sharma, S.; Pattabhi, V.; Mahato, S.B.; Sharma, P.D. A review of the hepatotoxic plant Lantana camara. Crit. Rev. Toxicol. 2007, 37, 313–352. [Google Scholar] [CrossRef]
- Ntalo, M.; Ravhuhali, K.E.; Moyo, B.; Hawu, O.; Msiza, N.H. Lantana camara: Poisonous species and a potential browse species for goats in southern Africa—A review. Sustainability 2022, 14, 751. [Google Scholar] [CrossRef]
- Kalita, S.; Kumar, G.; Karthik, L.; Rao, K.V.B. A review on medicinal properties of Lantana camara Linn. Res. J. Pharm. Technol. 2012, 5, 711–715. [Google Scholar]
- Reddy, N.M. Lantana camara Linn. Chemical constituents and medicinal properties: A review. Acad. J. Pharm. 2013, 2, 445–448. [Google Scholar]
- Kumar, R.; Katiyar, R.; Kumar, S.; Kumar, T.; Singh, V. Lantana camara: An alien weed, its impact on animal health and strategies to control. J. Exp. Biol. Agric. Sci. 2016, 4, 321–337. [Google Scholar] [CrossRef]
- Al-Snafi, A.E. Chemical constituents and pharmacological activities of Lantana camara—A review. Asian J. Pharm. Clin. Res. 2019, 12, 10–20. [Google Scholar] [CrossRef]
- Battase, L.; Attarde, D. Phytochemical and medicinal study of Lantana camara Linn (Verbenaceae)—A review. Asian J. Pharm. Clin. Res. 2021, 14, 20–27. [Google Scholar] [CrossRef]
- Kathuria, I.; Joshi, M.; Patel, B.M.; Dhobi, M. Phytoconstituents of Lantana camara L.: Rekindling hope in the cancer treatment. Curr. Bioact. Compd. 2022, 18, e311221199740. [Google Scholar]
- Kimpouni, V.; Mamboueni, J.C.; Tsoungould, F.G.M.; Mikoko, E.N. Ethnobotanical and phytotherapeutic study from Kouni community of the sub-prefecture of Kayes (Bouenza—Congo). Heliyon 2019, 5, e02007. [Google Scholar] [CrossRef] [PubMed]
- Manya, M.H.; Keymeulen, F.; Ngezahayo, J.; Bakari, A.S.; Kalonda, M.E.; Kahumba, B.J. Antimalarial herbal remedies of Bukavu and Uvira areas in DR Congo: An ethnobotanical survey. J. Ethnopharmacol. 2020, 249, 112422. [Google Scholar] [CrossRef] [PubMed]
- Pathy, K.K.; Flavien, N.B.; Honoré, B.K.; Vanhove, W.; Patrick, V.D. Ethnobotanical characterization of medicinal plants used in Kisantu and Mbanza-Ngungu territories, Kongo-Central Province in DR Congo. J. Ethnobiol. Ethnomed. 2021, 17, 5. [Google Scholar]
- Geremew, Y.A.; Desta, Y.D.; Kumar, P.A.; Tonjo, Z.T. Traditional medicinal plants used by people in Libo-Kemkem District, South Gondar, Ethiopia. Asian J. Agric. Sci. 2012, 4, 171–176. [Google Scholar]
- Lulekal, E.; Kelbessa, E.; Bekele, T.; Yineger, H. An ethnobotanical study of medicinal plants in Mana Angetu District, southeastern Ethiopia. J. Ethnobiol. Ethnomed. 2008, 4, 10. [Google Scholar] [CrossRef]
- Mesfin, F.; Demissew, S.; Teklehaymanot, T. An ethnobotanical study of medicinal plants in Wonago Woreda, SNNPR, Ethiopia. J. Ethnobiol. Ethnomed. 2009, 5, 28. [Google Scholar] [CrossRef]
- Giday, M.; Asfaw, Z.; Woldu, Z. Ethnomedicinal study of plants used by Sheko ethnic group of Ethiopia. J. Ethnopharmacol. 2010, 132, 75–85. [Google Scholar] [CrossRef]
- Jonville, M.C.; Kodja, H.; Humeau, L.; Fournel, J.; De Mol, P.; Cao, M. Screening of medicinal plants from Reunion Island for antimalarial and cytotoxic activity. J. Ethnopharmacol. 2008, 120, 382–386. [Google Scholar] [CrossRef] [PubMed]
- Magassouba, F.B.; Diallo, A.; Kouyaté, M.; Mara, F.; Mara, O.; Bangoura, O. Ethnobotanical survey and antibacterial activity of some plants used in Guinean traditional medicine. J. Ethnopharmacol. 2007, 114, 44–53. [Google Scholar] [CrossRef] [PubMed]
- Njoroge, G.N.; Bussmann, R.W. Traditional management of ear, nose and throat (ENT) diseases in Central Kenya. J. Ethnobiol. Ethnomed. 2006, 2, 54. [Google Scholar] [CrossRef] [PubMed]
- Njoroge, G.N.; Bussmann, R.W. Diversity and utilization of antimalarial ethnophytotherapeutic remedies among the Kikuyus (Central Kenya). J. Ethnobiol. Ethnomed. 2006, 2, 8. [Google Scholar] [CrossRef] [PubMed]
- Kareru, P.G.; Kenji, G.M.; Gachanja, A.N.; Keriko, J.M.; Mungai, G. Traditional medicines among the Embu and Mbeere people of Kenya. Afr. J. Tradit. Complement. Altern. Med. 2007, 4, 75–86. [Google Scholar] [CrossRef] [PubMed]
- Geissler, P.W.; Harris, S.A.; Prince, R.J.; Olsen, A.; Odhiambo, R.A.; Oketch-Rabah, H. Medicinal plants used by Luo mothers and children in Bondo district, Kenya. J. Ethnopharmacol. 2002, 83, 39–54. [Google Scholar] [CrossRef] [PubMed]
- Nguta, J.M.; Mbaria, J.M.; Gakuya, D.W.; Gathumbi, P.K.; Kiama, S.G. Antimalarial herbal remedies of Msambweni, Kenya. J. Ethnopharmacol. 2010, 128, 424–432. [Google Scholar] [CrossRef]
- Seyoum, A.; Pålsson, K.; Kung’a, S.; Kabiru, E.W.; Lwande, W.; Killeen, G.F. Traditional use of mosquito-repellent plants in western Kenya and their evaluation in semi-field experimental huts against Anopheles gambiae: Ethnobotanical studies and application by thermal expulsion and direct burning. Trans. R. Soc. Trop. Med. Hyg. 2002, 96, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Rivière, C.; Nicolas, J.P.; Caradec, M.L.; Désiré, O.; Schmitt, A. Les plants médicinales de la région nord de Madagascar une approche ethnopharmacologique. Ethnopharmacologia 2005, 36, 1–295. [Google Scholar]
- Egunyomi, A.; Gbadamosi, I.T.; Osiname, K.O. Comparative effectiveness of ethnobotanical mosquito repellents used in Ibadan, Nigeria. J. Appl. Biosci. 2010, 36, 2383–2388. [Google Scholar]
- Tabuti, J.R.S. Herbal medicines used in the treatment of malaria in Budiope county, Uganda. J. Ethnopharmacol. 2008, 116, 33–42. [Google Scholar] [CrossRef]
- Baana, K.; Angwech, H.; Malinga, G.M. Ethnobotanical survey of plants used as repellents against housefly, Musca domestica L. (Diptera: Muscidae) in Budondo Subcounty, Jinja District, Uganda. J. Ethnobiol. Ethnomed. 2018, 14, 35. [Google Scholar] [CrossRef]
- Kamatenesi, M.M.; Acipa, A.; Oryem-Origa, H. Medicinal plants of Otwal and Ngai Sub Counties in Oyam District, Northern Uganda. J. Ethnobiol. Ethnomed. 2011, 7, 7. [Google Scholar] [CrossRef] [PubMed]
- Gou, Y.; Li, Z.; Fan, R.; Guo, C.; Wang, L.; Sun, H.; Li, J.; Zhou, C.; Wang, C.; Wang, Y. Ethnobotanical survey and evaluation of traditional mosquito repellent plants of Dai people in Xishuangbanna, Yunnan Province, China. J. Ethnopharmacol. 2020, 262, 113124. [Google Scholar] [CrossRef]
- Namsa, N.D.; Mandal, M.; Tangjang, S. Anti-malarial herbal remedies of northeast India, Assam: An ethnobotanical survey. J. Ethnopharmacol. 2011, 133, 565–572. [Google Scholar] [CrossRef] [PubMed]
- Kamaraj, C.; Kaushik, N.K.; Rahuman, A.A.; Mohanakrishnan, D.; Bagavan, A.; Elango, G. Antimalarial activities of medicinal plants traditionally used in the villages of Dharmapuri regions of South India. J. Ethnopharmacol. 2012, 141, 796–802. [Google Scholar] [CrossRef] [PubMed]
- Rao, M.R.K. Lethal efficacy of phytochemicals as sustainable sources of insecticidal formulations derived from the leaf extracts of Indian medicinal plants to control Dengue and Zika vector, Aedes aegypti (Dipetra: Culicide). Int. Res. J. Environ. Sci. 2020, 9, 44–54. [Google Scholar]
- Kumar, V.P.; Chauhan, N.S.; Padh, H.; Rajani, M. Search for antibacterial and antifungal agents from selected Indian medicinal plants. J. Ethnopharmacol. 2006, 107, 182–188. [Google Scholar] [CrossRef] [PubMed]
- Obico, J.J.; Ragragio, E.M. A survey of plants used as repellents against hematophagous insects by the Ayta people of Porac, Pampanga province, Philippines. Philipp. Sci. Lett. 2014, 7, 179–186. [Google Scholar]
- Lee, C.; Kim, S.Y.; Eum, S.; Paik, J.H.; Bach, T.T.; Darshetkar, A.M. Ethnobotanical study on medicinal plants used by local Van Kieu ethnic people of Bac Huong Hoa nature reserve, Vietnam. J. Ethnopharmacol. 2019, 231, 283–294. [Google Scholar] [CrossRef]
- Hussein, S.; Dhabe, A. Ethnobotanical study of folk medicinal plants used by villagers in Hajjah district—Republic of Yemen. J. Med. Plants Stud. 2018, 6, 24–30. [Google Scholar]
- Delgado-Altamirano, R.; Monzote, L.; Piñón-Tápanes, A.; Vibrans, H.; Fausto Rivero-Cruz, J.; Ibarra-Alvarado, C.; Rojas-Molina, A. In vitro antileishmanial activity of Mexican medicinal plants. Heliyon 2017, 3, e00394. [Google Scholar] [CrossRef] [PubMed]
- González-Esquinca, A.R.; Luna-Cazáres, L.M.; Gispert-Cruells, M.; Schlie-Guzmán, M.A.; Gutiérrez-Jiménez, J. Plantas Medicinales Zoques: Padecimientos Gastrointestinales y Respiratorios; Colección Jaguar; UNICACH: Tuxtla Gutiérrez, Mexico, 2013; Volume 1, pp. 39–40. [Google Scholar]
- Hernández, T.; Canales, M.; Avila, J.G.; Duran, A.; Caballero, J.; Romo de Vivar, A. Ethnobotany and antibacterial activity of some plants used in traditional medicine of Zapotitlán de las Salinas, Puebla (México). J. Ethnopharmacol. 2003, 88, 181–188. [Google Scholar] [CrossRef] [PubMed]
- Braga, F.G.; Bouzada, M.L.M.; Fabri, R.L.; Matos, M.; Moreira, F.O.; Scio, E. Antileishmanial and antifungal activity of plants used in traditional medicine in Brazil. J. Ethnopharmacol. 2007, 111, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Van’t Klooster, C.; van Andel, T.; Reis, R. Patterns in medicinal plant knowledge and use in a Maroon village in Suriname. J. Ethnopharmacol. 2016, 189, 319–330. [Google Scholar] [CrossRef] [PubMed]
- Vásquez, J.; Alarcón, J.C.; Jiménez, S.L.; Jaramillo, G.I.; Gómez-Betancur, I.C.; Rey-Suárez, J.P. Main plants used in traditional medicine for the treatment of snake bites in the regions of the department of Antioquia, Colombia. J. Ethnopharmacol. 2015, 170, 158–166. [Google Scholar] [CrossRef]
- Boulogne, I.; Germosén-Robineau, L.; Ozier-Lafontaine, H.; Fleury, M.; Loranger-Merciris, G. TRAMIL ethnopharmalogical survey in Les Saintes (Guadeloupe, French West Indies): A comparative study. J. Ethnopharmacol. 2011, 133, 1039–1050. [Google Scholar] [CrossRef]
- Huang, K.F.; Huang, K.W. Constituents from the stems of Lantana camara (III). J. Chin. Med. 2004, 15, 109–114. [Google Scholar]
- Juang, F.C.; Chen, Y.F.; Lin, F.M.; Huang, K.F. Constituents from the leaves of Lantana camara (IV). J. Chin. Med. 2005, 16, 149–155. [Google Scholar]
- Gebre, Z.; Tariku, Y.; Jayakumar, V. Bio-assay guided isolation of bioactive molecules from chloroform extract of fruits of Lantana camara (L.). J. Pharmacogn. Phytochem. 2019, 8, 1335–1342. [Google Scholar] [CrossRef]
- Misra, L.; Laatsch, H. Triterpenoids, essential oil and photo-oxidative 28 → 13-lactonization of oleanolic acid from Lantana camara. Phytochemistry 2000, 54, 969–974. [Google Scholar] [CrossRef] [PubMed]
- Misra, N.; Sharma, M.; Raj, K.; Dangi, A.; Srivastava, S.; Misra-Bhattacharya, S. Chemical constituents and antifilarial activity of Lantana camara against human lymphatic filariid Brugia malayi and rodent filariid Acanthocheilonema viteae maintained in rodent hosts. Parasitol. Res. 2007, 100, 439–448. [Google Scholar] [CrossRef]
- Đậu, N.V.; Huyền, L.T. Các tritecpen oleanan từ cây bông ổi Lantana camara L. Tạp Chí Hóa Học 2009, 47, 144–148. [Google Scholar]
- Begum, S.; Wahab, A.; Siddiqui, B.S. Pentacyclic triterpenoids from the aerial parts of Lantana camara. Chem. Pharm. Bull. 2003, 51, 134–137. [Google Scholar] [CrossRef]
- Begum, S.; Ayub, A.; Zehra, S.Q.; Siddiqui, B.S.; Choudhary, M.I.; Samreen. Leishmanicidal triterpenes from Lantana camara. Chem. Biodivers. 2014, 11, 709–718. [Google Scholar] [CrossRef] [PubMed]
- Patil, G.; Khare, A.B.; Huang, K.-F.; Lin, F.-M. Bioactive chemical constituents from the leaves of Lantana camara L. Indian J. Chem. 2015, 54, 691–697. [Google Scholar]
- Wu, P.; Song, Z.; Wang, X.; Li, Y.; Li, Y.; Cui, J.; Tuerhong, M.; Jin, D.-Q.; Abudukeremu, M.; Lee, D.; et al. Bioactive triterpenoids from Lantana camara showing anti-inflammatory activities in vitro and in vivo. Bioorg. Chem. 2020, 101, 104004. [Google Scholar] [CrossRef] [PubMed]
- Darwish, R.S.; El-Banna, A.A.; Ghareeb, D.A.; El-Hosseny, M.F.; Seadawy, M.G.; Dawood, H.M. Chemical profiling and unraveling of anti-COVID-19 biomarkers of red sage (Lantana camara L.) cultivars using UPLC-MS/MS coupled to chemometric analysis, in vitro study and molecular docking. J. Ethnopharmacol. 2022, 291, 115038. [Google Scholar] [CrossRef]
- Begum, S.; Ayub, A.; Siddiqui, B.S.; Fayyaz, S.; Kazi, F. Nematocidal triterpenoids from Lantana camara. Chem. Biodivers. 2015, 12, 1435–1442. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Zehra, S.Q.; Siddiqui, B.S. Two new pentacyclic triterpenoids from Lantana camara LINN. Chem. Pharm. Bull. 2008, 56, 1317–1320. [Google Scholar] [CrossRef]
- Abdjul, D.B.; Yamazaki, H.; Maarisit, W.; Rotinsulu, H.; Wewengkang, D.S.; Sumilat, D.A.; Kapojos, M.M.; Losung, F.; Ukai, K.; Namikoshi, M. Oleanane triterpenes with protein tyrosine phosphatase 1B inhibitory activity from aerial parts of Lantana camara collected in Indonesia and Japan. Phytochemistry 2017, 144, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Siddiqui, B.S.; Wahab, A. Two new pentacyclic triterpenoids from the aerial parts of Lantana camara Linn. Heterocycles 2000, 53, 681–687. [Google Scholar] [CrossRef]
- Fatope, M.O.; Salihu, L.; Asante, S.K.; Takeda, Y. Larvicidal activity of extracts and triterpenoids from Lantana camara. Pharm. Biol. 2002, 40, 564–567. [Google Scholar] [CrossRef]
- Gupta, S.; Kalani, K.; Saxena, M.; Srivastava, S.K.; Agrawal, S.K.; Suri, N. Cytotoxic evaluation of semisynthetic ester and amide derivatives of oleanolic acid. Nat. Prod. Commun. 2010, 5, 1567–1570. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, S.; Das Sarma, M.; Patra, A.; Hazra, B. Anti-inflammatory and anticancer compounds isolated from Ventilago madraspatana Gaertn., Rubia cordifolia Linn. and Lantana camara Linn. J. Pharm. Pharmacol. 2010, 62, 1158–1166. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Zehra, S.Q.; Wahab, A.; Siddiqui, B.S. Triterpenoidal secondary metabolites from Lantana camara LINN. Helv. Chim. Acta 2006, 89, 1932–1941. [Google Scholar] [CrossRef]
- Begum, S.; Zehra, S.Q.; Siddiqui, B.S.; Fayyaz, S.; Ramzan, M. Pentacyclic triterpenoids from the aerial parts of Lantana camara and their nematocidal activity. Chem. Biodivers. 2008, 5, 1856–1866. [Google Scholar] [CrossRef] [PubMed]
- Sharma, O.P.; Singh, A.; Sharma, S. Levels of lantadenes, bioactive pentacyclic triterpenoids, in young and mature leaves of Lantana camara var. aculeata. Fitoterapia 2000, 71, 487–491. [Google Scholar] [CrossRef] [PubMed]
- Sharma, M.; Sharma, P.D. Optimization of lantadenes isolation and preparation of 22β-hydroxyoleanonic. Chem. Nat. Compd. 2006, 42, 357–358. [Google Scholar] [CrossRef]
- Sharma, M.; Sharma, P.D.; Bansal, M.P.; Singh, J. Synthesis, cytotoxicity, and antitumor activity of lantadene—A congeners. Chem. Biodivers. 2007, 4, 932–939. [Google Scholar] [CrossRef] [PubMed]
- Sharma, M.; Sharma, P.D.; Bansal, M.P. Lantadenes and their esters as potential antitumor agents. J. Nat. Prod. 2008, 71, 1222–1227. [Google Scholar] [CrossRef] [PubMed]
- Tailor, N.K.; Boon, H.L.; Sharma, M. Synthesis and in vitro anticancer studies of novel C-2 arylidene congeners of lantadenes. Eur. J. Med. Chem. 2013, 64, 285–291. [Google Scholar] [CrossRef] [PubMed]
- Suthar, S.K.; Lee, H.B.; Sharma, M. The synthesis of non-steroidal anti-inflammatory drug (NSAID)-lantadene prodrugs as novel lung adenocarcinoma inhibitors via the inhibition of cyclooxygenase-2 (COX-2), cyclin D1 and TNF-α-induced NF-κB activation. RSC Adv. 2014, 4, 19283–19293. [Google Scholar] [CrossRef]
- Sharma, M.; Sharma, P.D.; Bansal, M.P.; Singh, J. Synthesis and antitumor activity of novel pentacyclic triterpenoid lantadene D. Lett. Drug Des. Discov. 2007, 4, 201–206. [Google Scholar] [CrossRef]
- Delgado-Altamirano, R.; López-Palma, R.I.; Monzote, L.; Delgado-Domínguez, J.; Becker, I.; Rivero-Cruz, J.F.; Esturau-Escofet, N.; Vázquez-Landaverde, P.A.; Rojas-Molina, A. Chemical constituents with leishmanicidal activity from a pink-yellow cultivar of Lantana camara var. aculeata (L.) collected in Central Mexico. Int. J. Mol. Sci. 2019, 20, 872. [Google Scholar] [CrossRef]
- Ono, M.; Hashimoto, A.; Miyajima, M.; Sakata, A.; Furusawa, C.; Shimode, M. Two new triterpenoids from the leaves and stems of Lantana camara. Nat. Prod. Res. 2020, 35, 3757–3765. [Google Scholar] [CrossRef] [PubMed]
- Sagar, L.; Sehgal, R.; Ojha, S. Evaluation of antimotility effect of Lantana camara L. var. aculeata constituents on neostigmine induced gastrointestinal transit in mice. BMC Complement. Altern. Med. 2005, 5, 18. [Google Scholar] [CrossRef]
- Banik, R.M.; Pandey, D.K. Optimizing conditions for oleanolic acid extraction from Lantana camara roots using response surface methodology. Ind. Crops Prod. 2008, 27, 241–248. [Google Scholar] [CrossRef]
- Verma, S.C.; Jain, C.L.; Nigam, S.; Padhi, M.M. Rapid extraction, isolation, and quantification of oleanolic acid from Lantana camara L. roots using microwave and HPLC-PDA techniques. Acta Chromatogr. 2013, 25, 181–199. [Google Scholar] [CrossRef]
- Pour, M.B.; Latha, L.Y.; Sasidharan, S. Cytotoxicity and oral acute toxicity studies of Lantana camara leaf extract. Molecules 2011, 16, 3663–3674. [Google Scholar] [CrossRef]
- Ma, L.-h.; Wu, H.-b.; Wu, H.-b. A new oleanane triterpene with allelopathic activity from Lantana camara. Chem. Nat. Compd. 2023, 59, 709–711. [Google Scholar] [CrossRef]
- Ayub, A.; Begum, S.; Ali, S.N.; Ali, S.T.; Siddiqui, B.S. Triterpenoids from the aerial parts of Lantana camara. J. Asian Nat. Prod. Res. 2017, 21, 141–149. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Wahab, A.; Siddiqui, B.S. Three new pentacyclic triterpenoids from Lantana camara. Helv. Chim. Acta. 2002, 85, 2335–2341. [Google Scholar] [CrossRef]
- Kalita, S.; Kumar, G.; Karthik, L.; Rao, K.V.B. Phytochemical composition and in vitro hemolytic activity of Lantana Camara L. (Verbenaceae) leaves. Pharmacologyonline 2011, 1, 59–61. [Google Scholar]
- Ali-Emmanuel, N.; Moudachirou, M.; Akakpo, J.A.; Quetin-Leclercq, J. Treatment of bovine dermatophilosis with Senna alata, Lantana camara and Mitracarpus scaber leaf extracts. J. Ethnopharmacol. 2003, 86, 167–171. [Google Scholar] [CrossRef] [PubMed]
- Shamsee, Z.R.; Al-Saffar, A.Z.; Al-Shanon, A.F.; Al-Obaidi, J.R. Cytotoxic and cell cycle arrest induction of pentacyclic triterpenoides separated from Lantana camara leaves against MCF-7 cells in vitro. Mol. Biol. Rep. 2019, 46, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Kong, C.H.; Wang, P.; Zhang, C.X.; Zhang, M.X.; Hu, F. Herbicidal potential of allelochemicals from Lantana camara against Eichhornia crassipes and the alga Microcystis aeruginosa. Weed Res. 2006, 46, 290–295. [Google Scholar] [CrossRef]
- Giri, A.G.; Oza, R. Isolation, purification and characterization of triterpenes from Lantana camara. Chem. Sci. Rev. Lett. 2015, 4, 520–525. [Google Scholar]
- Sharma, M.; Rakhi, A.; Dalal, N.; Sharma, N. Design, synthesis and evaluation of lantadene A congener with hydroxyl functionality in ring A as an antitumour agent. Nat. Prod. Res. 2011, 25, 387–396. [Google Scholar] [CrossRef]
- Grace-Lynn, C.; Darah, I.; Chen, Y.; Latha, L.Y.; Jothy, S.L.; Sasidharan, S. In vitro antioxidant activity potential of lantadene A, a pentacyclic triterpenoid of Lantana plants. Molecules 2012, 17, 11185–11198. [Google Scholar] [CrossRef] [PubMed]
- Jaafar, N.D.; Al-Saffar, A.Z.; Yousif, E.A. Genotoxic and cytotoxic activities of lantadene A-loaded gold nanoparticles (LA-AuNPS) in MCF-7 cells: An in vitro assessment. Int. J. Toxicol. 2020, 39, 422–432. [Google Scholar] [CrossRef] [PubMed]
- Dawood, D.A.S.; Chua, L.S.; Tan, T.S.; Alshemary, A.F. Apoptotic mechanism of lantadene A from Lantana camara leaves against prostatic cancer cells. Egypt. J. Chem. 2021, 64, 7503–7510. [Google Scholar] [CrossRef]
- Litaudon, M.; Jolly, C.; Le Callonec, C.; Dao, D.C.; Retailleau, P.; Nosjean, O. Cytotoxic pentacyclic triterpenoids from Combretum sundaicum and Lantana camara as inhibitors of Bcl-xL/BakBH3 domain peptide interaction. J. Nat. Prod. 2009, 72, 1314–1320. [Google Scholar] [CrossRef]
- Delgado-Altamirano, R.; Rojas, A.; Esturau-Escofet, N. 1H and 13C NMR reassignment of some chemical shifts of lantanilic acid and camaric acid. Magn. Reson. Chem. 2019, 57, 320–325. [Google Scholar] [CrossRef] [PubMed]
- Qamar, F.; Begum, S.; Raza, S.M.; Wahab, A.; Siddiqui, B.S. Nematocidal natural products from the aerial parts of Lantana camara Linn. Nat. Prod. Res. 2005, 19, 609–613. [Google Scholar] [CrossRef]
- Kartika, M.Z.; Suryati, S.; Efdi, M. A triterpenoid compound from the leaves of Tahi ayam (Lantana camara Linn). Indones. J. Fundam. Appl. Chem. 2018, 3, 18–22. [Google Scholar]
- Seepe, H.A.; Raphoko, L.; Amoo, S.O.; Nxumalo, W. Lantadene A and boswellic acid isolated from the leaves of Lantana camara L. have the potential to control phytopathogenic Fusarium species. Heliyon 2022, 8, e12216. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Zehra, S.Q.; Ayub, A.; Siddiqui, B.S. A new 28-noroleanane triterpenoid from the aerial parts of Lantana camara Linn. Nat. Prod. Res. 2010, 24, 1227–1234. [Google Scholar] [CrossRef] [PubMed]
- Ediruslan, E.; Manjang, Y.; Suryati, S.; Aziz, H. Structure elucidation of brine shrimp toxic compound from Lantana camara L. leaves. J. Chem. Pharm. Res. 2015, 7, 250–255. [Google Scholar]
- Suryati; Efdi, M.; Oktavia, S.H.; Aziz, H. Antibacterial and antifungal activity of lantanilic acid isolated from Lantana camara Linn. Der Pharma Chem. 2017, 9, 105–108. [Google Scholar]
- Suryati, S.; Mardiah, E.; Efdi, M.; Kartika, M.Z.; Sari, Y.M. Bioactivity of compounds isolated from the leaves of the Lantana camara Linn plant. J. Chin. Pharm. Sci. 2019, 28, 360–368. [Google Scholar]
- Kazmi, I.; Rahman, M.; Afzal, M.; Gupta, G.; Saleem, S.; Afzal, O.; Shaharyar, M.A.; Nautiyal, U.; Ahmed, S.; Anwar, F. Anti-diabetic potential of ursolic acid stearoyl glucoside: A new triterpenic glycosidic ester from Lantana camara. Fitoterapia 2012, 83, 142–146. [Google Scholar] [CrossRef] [PubMed]
- Kazmi, I.; Saleem, S.; Ahmad, T.; Afzal, M.; Al-Abbasi, F.A.; Kumar, V.; Anwar, F. Protective effect of oleane-12-en-3β-ol-28-oic acid 3β-D-glucopyranoside in ethanol induced gastric ulcer by enhancing the prostaglandin E2 level. J. Ethnopharmacol. 2018, 211, 394–399. [Google Scholar] [CrossRef] [PubMed]
- Yadav, S.B.; Tripathi, V. A new triterpenoid from Lantana camara. Fitoterapia 2003, 74, 320–321. [Google Scholar] [CrossRef]
- Sathish, R.; Vyawahare, B.; Natarajan, K. Antiulcerogenic activity of Lantana camara leaves on gastric and duodenal ulcers in experimental rats. J. Ethnopharmacol. 2011, 134, 195–197. [Google Scholar] [CrossRef] [PubMed]
- Begum, S.; Wahab, A.; Siddiqui, B.S. Ursethoxy acid, a new triterpene from Lantana camara. Nat. Prod. Lett. 2002, 16, 235–238. [Google Scholar] [CrossRef] [PubMed]
- Yadav, S.B.; Tripathi, V. Chemical components of Lantana camara Linn. Indian J. Heterocyclic Chem. 2000, 10, 71–72. [Google Scholar]
- Xavier, M.R.; da Fonseca, A.M.; Gonçalves Cruz, B.; dos Santos Mendes, A.M.; Oliveira, L.S.; Bandeira, P.N.; Colares, R.P.; Braz-Filho, R.; Marinho, E.S.; Freitas, T.S.; et al. Modulating antibacterial activity against multidrug-resistant Escherichia coli and Staphylococcus aureus of the flavonoid pectolinarin isolated from Lantana camara leaves. J. Anal. Pharm. Res. 2021, 10, 217–220. [Google Scholar] [CrossRef]
- El-Kassem, L.T.A.; Mohammed, R.S.; El Souda, S.S.; El-Anssary, A.A.; Hawas, U.W.; Mohmoud, K. Digalacturonide flavones from Egyptian Lantana camara flowers with in vitro antioxidant and in vivo hepatoprotective activities. Z. Naturforsch. C 2012, 67, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Qureshi, H.; Anwar, T.; Ali, Q.; Haider, M.Z.; Habib, N.; Fatima, S. Isolation of natural herbicidal compound from Lantana camara. Int. J. Environ. Anal. Chem. 2019, 101, 631–638. [Google Scholar] [CrossRef]
- Begum, S.; Wahab, A.; Siddiqui, B.S. Antimycobacterial activity of flavonoids from Lantana camara Linn. Nat. Prod. Res. 2008, 22, 467–470. [Google Scholar] [CrossRef]
- Benjamin, R.; Akilan, A.; Senguttuvan, S. Isolation, characterization, and anti-cancer activity of kaempferol-6-methoxy-7-O-glucoside from Lantana camara flowers. Orient. J. Chem. 2022, 38, 72–76. [Google Scholar] [CrossRef]
- Millycent, S.A.; Mwonjoria, M.; Juma, K.K.; Ngugi, M.P.; Njagi, E. Evaluation of analgesic, anti-inflammatory and toxic effects of Lantana camara. Int. J. Phytopharm. 2017, 8, 89–97. [Google Scholar]
- Naz, R.; Bano, A. Phytochemical screening, antioxidants and antimicrobial potential of Lantana camara in different solvents. Asian Pac. J. Trop. Dis. 2013, 3, 480–486. [Google Scholar] [CrossRef]
- Indrayani, F.; Wirastuty, R.Y. In-vitro anti-tuberculosis activity and phytochemical screening of Lantana (Lantana camara L.) flower. Pharm. J. Indones. 2021, 18, 413–421. [Google Scholar] [CrossRef]
- Mahdi-Pour, B.; Jothy, S.L.; Latha, L.Y.; Chen, Y.; Sasidharan, S. Antioxidant activity of methanol extracts of different parts of Lantana camara. Asian Pac. J. Trop. Biomed. 2012, 2, 960–965. [Google Scholar] [CrossRef]
- Clarkson, C.; Maharaj, V.J.; Crouch, N.R.; Grace, O.M.; Pillay, P.; Matsabisa, M.G. In vitro antiplasmodial activity of medicinal plants native to or naturalised in South Africa. J. Ethnopharmacol. 2004, 92, 177–191. [Google Scholar] [CrossRef] [PubMed]
- Sharma, M.; Sharma, P.D.; Bansal, M.P. Chemopreventive effect of Lantana camara leaf extract on 7,12-dimethylbenz[a]anthracene-induced squamous cell carcinoma of skin in Swiss albino mice. Pharm. Biol. 2007, 45, 145–148. [Google Scholar] [CrossRef]
- Arbiastutie, Y.; Marsono, D.; Hartati, M.S.; Purwanto, R. The potential of understorey plants from Gunung Gede Pangrango National Park (West Java, Indonesia) as cervixs anticancer agents. Biodiversitas 2017, 18, 109–115. [Google Scholar] [CrossRef]
- Ruslin; Yamin; Rahma, N.A.; Imawati; Rohman, A. UPLC MS/MS profile and antioxidant activities from nonpolar fraction of patiwala (Lantana camara) leaves extract. Separations 2022, 9, 75. [Google Scholar] [CrossRef]
- Erdoğan, P.; Üstündağ, S. Lantana camara Ekstraktının Patates güvesi [Phthorimae operculella (Zeller) (Lepidoptera: Gelechiidae)]’ne İnsektisit Etkileri. Int. J. Sivas Univ. Sci. Technol. 2022, 1, 63–75. [Google Scholar]
- Kamaraj, C.; Rahuman, A.A.; Bagavan, A.; Elango, G.; Zahir, A.A.; Santhoshkumar, T. Larvicidal and repellent activity of medicinal plant extracts from Eastern Ghats of South India against malaria and filariasis vectors. Asian Pac. J. Trop. Med. 2011, 4, 698–705. [Google Scholar] [CrossRef] [PubMed]
- Verma, R.K.; Verma, S.K. Phytochemical and termiticidal study of Lantana camara var. aculeata leaves. Fitoterapia 2006, 77, 466–468. [Google Scholar] [CrossRef]
- Barre, J.; Jenber, A.J. Evaluation of selected botanicals for the management of maize weevil (Sitophilus zeamais) on maize (Zea mays L.) grain under laboratory condition in Gabilay District, Somaliland. Heliyon 2022, 8, e11859. [Google Scholar] [CrossRef]
- Kayesth, S.; Gupta, K.K. Impact of Lantana camara hexane extract on survival, growth and development of Dysdercus koenigii Fabricius (Heteroptera: Pyrrhocoriedae). Acta Ecol. Sin. 2018, 38, 187–192. [Google Scholar] [CrossRef]
- Alghamdi, A.A.; Basher, N.S.H. Efficacy of leaves and flowers ethanol extracts of the invasive species Lantana camara Linn as a mosquito larvicidal. Int. J. Mosq. Res. 2020, 7, 43–47. [Google Scholar]
- Hemalatha, P.; Elumalai, D.; Janaki, A.; Babu, M.; Velu, K.; Velayutham, K. Larvicidal activity of Lantana camara aculeata against three important mosquito species. J. Entomol. Zool. Stud. 2015, 3, 174–181. [Google Scholar]
- Sharma, M.; Alexander, A.; Nakhate, K.T.; Nagwanshi, K.K.; Ajazuddin. Evaluation of the mosquito larvicidal potential and comparative assessment of the juice of Lantana camara Linn and Ocimum gratissimum Linn. Exp. Parasitol. 2023, 249, 108521. [Google Scholar] [CrossRef]
- Kamatchi, P.A.C.; Maheswaran, R.; Ignacimuthu, S. Evaluation of larval toxicity of Lantana camara L. and Catharanthus roseus L. against Culex quinquefasciatus say and Aedes aegypti L. Entomol. Ornithol. Herpetol. 2016, 5, 170. [Google Scholar]
- Taha, K.A.; Osman, H.E.; Sidahmed, O.A.A. Larvicidal effects of some plant extracts against Anopheles arabiensis Patton Larvae (Diptera: Culicidae). J. Sci. Technol. 2011, 12, 67–74. [Google Scholar]
- Gindri, D.M.; Coelho, C.M.M.; Uarrota, V.G.; Rebelo, A.M. Herbicidal bioactivity of natural compounds from Lantana camara on the germination and seedling growth of Bidens pilosa. Pesqui. Agropecu. Trop. 2020, 50, e57746. [Google Scholar] [CrossRef]
- Tuyiringire, N.; Taremwa Mugisha, I.; Tusubira, D.; Munyampundu, J.P.; Mambo Muvunyi, C.; Vander Heyden, Y. In vitro antimycobacterial activity of medicinal plants Lantana camara, Cryptolepis sanguinolenta, and Zanthoxylum leprieurii. J. Clin. Tuberc. Other Mycobact. Dis. 2022, 27, 100307. [Google Scholar] [CrossRef] [PubMed]
- Bangou, M.J.; Almaraz-Abarca, N.; Méda, N.T.R.; Zeba, B.; Kiendrebéogo, M.; Millogo-Rasolodimby, J. Polyphenolic composition of Lantana camara and Lippia chevalieri, and their antioxidant and antimicrobial activities. Phytomedicine 2012, 4, 115–124. [Google Scholar]
- Pradeep, B.V.; Tejaswini, M.; Nishal, P.; Pardhu, G.; Shylaja, S.; Kumar, K.C. Phytochemical screening and antimicrobial activities of plant extract of Lantana camara. J. Environ. Biol. 2013, 34, 645–649. [Google Scholar]
- El Gendy, S.N.; Ezzat, M.I.; EL Sayed, A.M.; Saad, A.S.; Elmotayam, A.K. HPLC-PDA-ESI-MS-MS analysis of acids content of Lantana camara L. flower extract and its anticoagulant activity. Egypt. J. Chem. 2023, 66, 249–256. [Google Scholar]
- Mengistu, G.; Engidawork, E.; Nedi, T. Evaluation of the antidiarrhoeal activity of 80% methanol extract and solvent fractions of the leaves of Lantana camara Linn (Verbenaceae) in mice. Ethiop. Pharm. J. 2015, 31, 107–120. [Google Scholar] [CrossRef]
- Sousa, E.O.; Miranda, C.M.B.A.; Nobre, C.B.; Boligon, A.A.; Athayde, M.L.; Costa, J.G.M. Phytochemical analysis and antioxidant activities of Lantana camara and Lantana montevidensis extracts. Ind. Crops Prod. 2015, 70, 7–15. [Google Scholar] [CrossRef]
- Suryati; Santoni, A.; Kartika, M.Z.; Aziz, H. Antioxidant activity and total phenolic content of ethyl acetate extract and fractions of Lantana camara L. leaf. Der Pharma Chem. 2016, 8, 92–96. [Google Scholar]
- Kalita, S.; Kumar, G.; Karthik, L.; Rao, K.V.B. In vitro antioxidant and DNA damage inhibition activity of aqueous extract of Lantana camara L. (Verbenaceae) leaves. Asian Pac. J. Trop. Biomed. 2012, 2, 1675–1679. [Google Scholar] [CrossRef]
- Kazmi, I.; Afzal, M.; Ali, B.; Damanhouri, Z.A.; Ahmaol, A.; Anwar, F. Anxiolytic potential of ursolic acid derivative-a stearoyl glucoside isolated from Lantana camara L. (Verbanaceae). Asian Pac. J. Trop. Med. 2013, 6, 433–437. [Google Scholar] [CrossRef]
- Parimoo, H.A.; Sharma, R.; Patil, R.D.; Sharma, O.P.; Kumar, P.; Kumar, N. Hepatoprotective effect of Ginkgo biloba leaf extract on lantadenes-induced hepatotoxicity in guinea pigs. Toxicon 2014, 81, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Veraplakorn, V. In vitro micropropagation and allelopathic effect of lantana (Lantana camara L.). Agric. Nat. Resour. 2017, 51, 478–484. [Google Scholar] [CrossRef]
- Motwani, G.S.; Golani, N.; Solanki, H.A. Allelopathic effects of aqueous leaf leachates of Lantana camara on Eichhornia crassipes. Life Sci. Leaf 2013, 1, 83–90. [Google Scholar]
- Saxena, M.K.; Gupta, J.; Singh, N. Allelopathic potential of callus extract of Lantana camara. Int. J. Recent Sci. Res. 2013, 4, 1628–1630. [Google Scholar]
- Veraplakorn, V. Allelopathic hormesis and slow release of lantana (Lantana camara L.) callus extract. Agric. Nat. Resour. 2018, 52, 335–340. [Google Scholar] [CrossRef]
- Nayak, B.S.; Raju, S.S.; Eversley, M.; Ramsubhag, A. Evaluation of wound healing activity of Lantana camara L.—A preclinical study. Phytother. Res. 2009, 23, 241–245. [Google Scholar] [CrossRef]
- Suryati, A.S.; Imelda, R.V.U. Cytotoxic and molecular docking potential of β-sitosterol isolated from Lantana camara leaves against breast (T47D) and cervical cancer (HeLa) cell lines. Trop. J. Nat. Prod. Res. 2024, 8, 6911–6917. [Google Scholar]
- Wang, J.; Lu, X.; Jing, Q.; Zhang, B.; Ye, J.; Zhang, H.; Xiao, Z.; Zhang, J. Spatiotemporal characterization of heavy metal and antibiotics in the Pearl River Basin and pollutants removal assessment using invasive species-derived biochars. J. Hazard. 2023, 454, 131409. [Google Scholar] [CrossRef]
- Surya Prakash, V.; Radhakrishnan, N.; Vasantha-Srinivasan, P.; Veeramani, C.; El Newehy, A.S.; Alsaif, M.A.; Al-Numair, K.S. In silico analysis of selected nutrition rich fruit of Bunch berry (Lantana camara) constituents as human acetylcholinesterase (hAchE), carbonic anhydrase II (hCA-II) and carboxylesterase 1 (hCES-1) inhibitory agents. Saudi J. Biol. Sci. 2023, 30, 103847. [Google Scholar] [CrossRef]
- Patil, S.P.; Sahu, K.G.; Andhale, G.S. Lantana camara mediated green synthesis of metallic nanoparticles: A mini review. Inorg. Chem. Commun. 2024, 160, 111853. [Google Scholar] [CrossRef]
- Hussein, L.M.; Hasan, A.Y. Biosynthesis of zinc oxide nanoparticles by Lantana camara flowers extract characterization and their antibacterial potential against pathogenic bacteria isolated from wounds infections. J. Pharm. Negat. 2022, 13, 451–458. [Google Scholar]
- Hamdiani, S.; Shih, Y.F. Environmentally methods for the loaded of silver and zinc oxide nanoparticles on diatomite as a potential nanofiller for industrial application. AIP Conf. Proc. 2023, 2619, 040008. [Google Scholar]
- Negi, A.; Joshi, S.K.; Bhandari, N.S. Estimation of sorption-desorption characteristics of biosorbent of Lantana camara leaves for removal of Pb (II) ions from wastewater. Environ. Monit. Assess. 2023, 195, 42. [Google Scholar] [CrossRef] [PubMed]

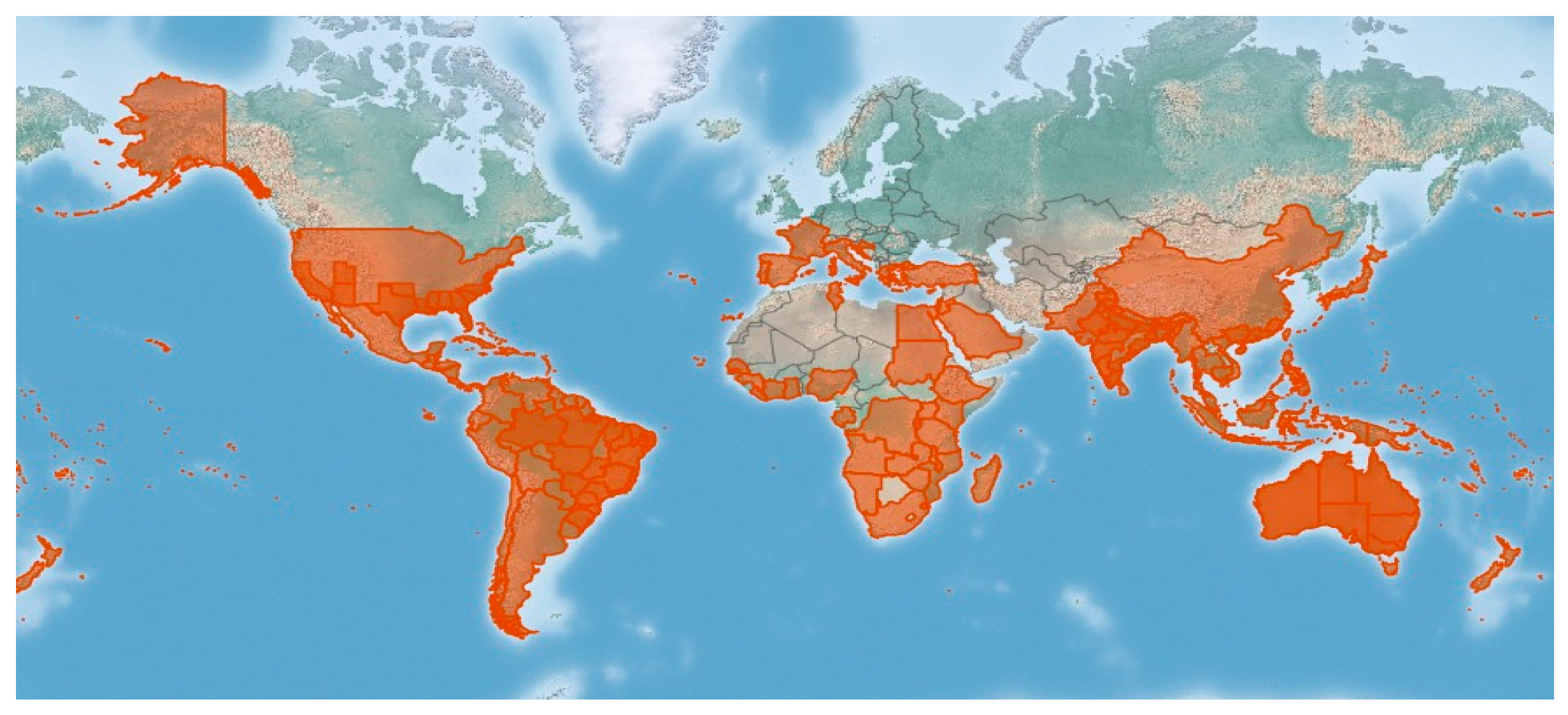
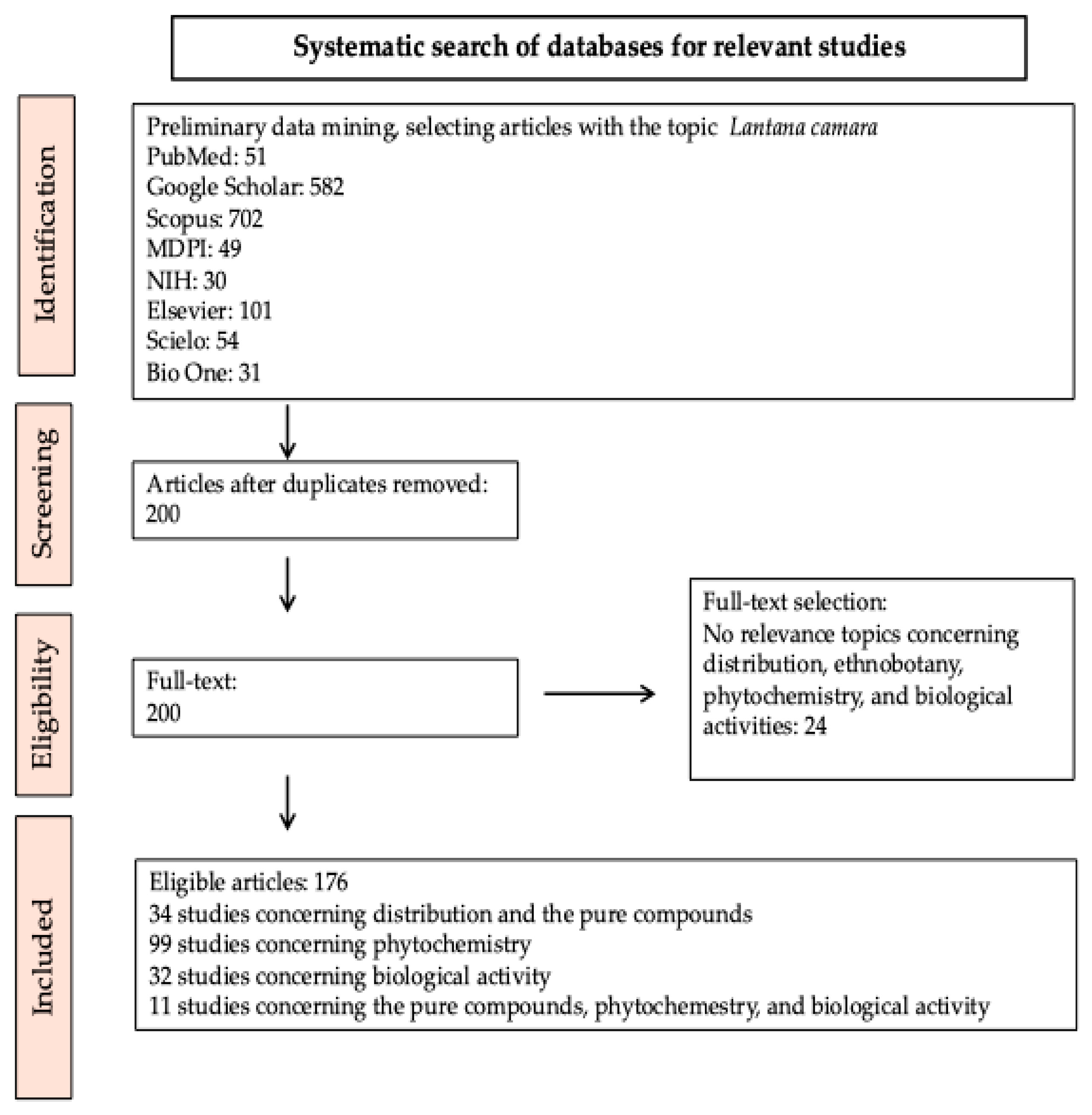
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ramírez, J.; Armijos, C.; Espinosa-Ortega, N.; Castillo, L.N.; Vidari, G. Ethnobotany, Phytochemistry, and Biological Activity of Extracts and Non-Volatile Compounds from Lantana camara L. and Semisynthetic Derivatives—An Updated Review. Molecules 2025, 30, 851. https://doi.org/10.3390/molecules30040851
Ramírez J, Armijos C, Espinosa-Ortega N, Castillo LN, Vidari G. Ethnobotany, Phytochemistry, and Biological Activity of Extracts and Non-Volatile Compounds from Lantana camara L. and Semisynthetic Derivatives—An Updated Review. Molecules. 2025; 30(4):851. https://doi.org/10.3390/molecules30040851
Chicago/Turabian StyleRamírez, Jorge, Chabaco Armijos, Nelson Espinosa-Ortega, Leydy Nathaly Castillo, and Giovanni Vidari. 2025. "Ethnobotany, Phytochemistry, and Biological Activity of Extracts and Non-Volatile Compounds from Lantana camara L. and Semisynthetic Derivatives—An Updated Review" Molecules 30, no. 4: 851. https://doi.org/10.3390/molecules30040851
APA StyleRamírez, J., Armijos, C., Espinosa-Ortega, N., Castillo, L. N., & Vidari, G. (2025). Ethnobotany, Phytochemistry, and Biological Activity of Extracts and Non-Volatile Compounds from Lantana camara L. and Semisynthetic Derivatives—An Updated Review. Molecules, 30(4), 851. https://doi.org/10.3390/molecules30040851








