Short Overview of Some Assays for the Measurement of Antioxidant Activity of Natural Products and Their Relevance in Dermatology
Abstract
1. Introduction
2. Synthetic Antioxidants vs. Natural Antioxidants
3. Assays for the Measurement of Antioxidant Activity
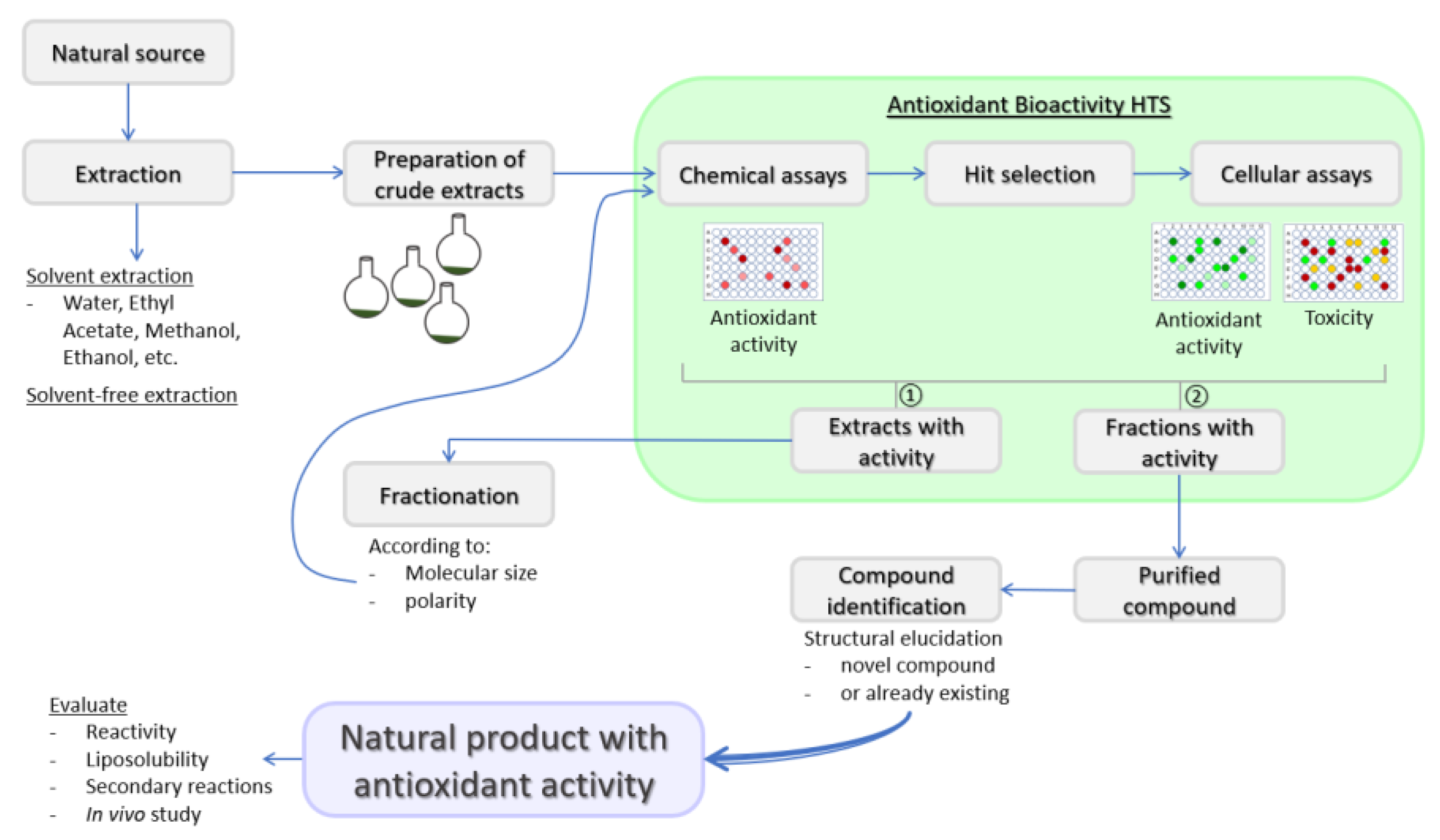
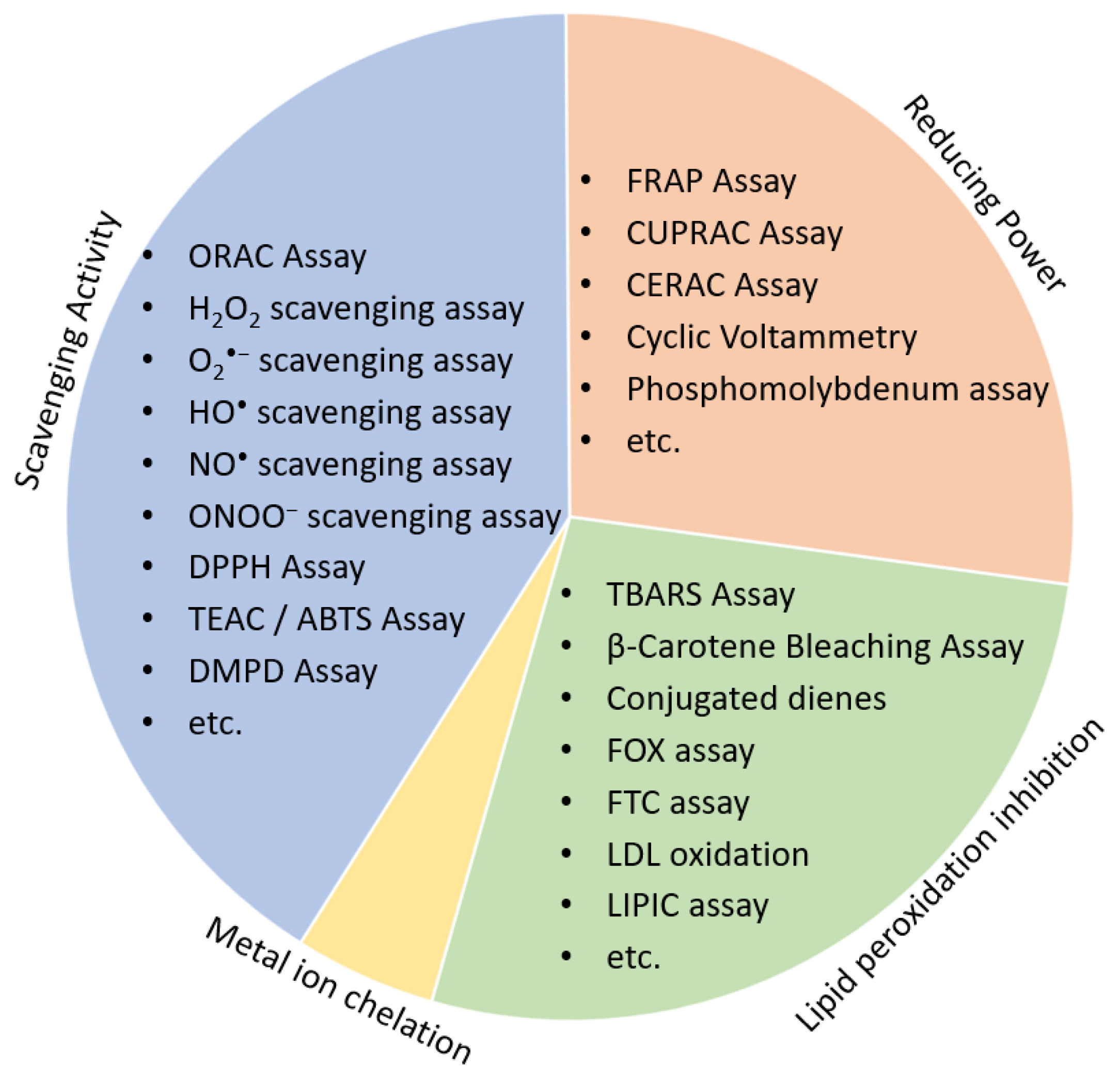
3.1. Chemical-Based Antioxidant Assays
- Scavenging activity assays are based on the ability of an antioxidant to scavenge stable free radicals. Some of the most common antioxidant assays based on scavenging activity include ORAC, DPPH, 2,2′-azinobis-(3-ethylbenzothiazole-6-sulphonate) (ABTS)/TEAC assay and N,N-dimethyl-p-phenylenediamine radical scavenging (DMPD) assay [31,32]. Although the basic principle is the same, their antioxidant solubility differs from those soluble in aqueous and alcoholic media (e.g., ABTS•+ and DMPD•+ radical) to those soluble in organic solvents (e.g., DPPH• radical). Other scavenging assays include those specific to certain ROS/RNS, such as ONOO− [33], hydroxyl radical [34], superoxide anion (O2•−) [35] or NO• scavenging assays [36].
- Reducing antioxidant power assays are based on the principle that antioxidants acts as reductants by accepting electrons, for example, from transition metals, notably iron and copper. The most frequently used reducing antioxidant power assays are FRAP, cupric ions reducing power assay (CUPRAC) and total phenolic content assay (Folin–Ciocalteu method) [32].
- Metal ion chelation is an important property of an antioxidant as transition metals, via the Fenton reaction, promote oxidative stress and lipid peroxidation [2,39,40]. Ferrous ion is commonly used to assess the metal chelation capacity of antioxidants [41]. Curcumin, resveratrol, L-carnitine and ferrozine are among many well documented antioxidants with metal chelation ability [32].
3.2. Cellular-Based Antioxidant Assays
4. Natural Products with Antioxidant Activity as Adjuvant Therapeutic Approach in Dermatology
5. Conclusions and Future Perspectives
Author Contributions
Funding
Conflicts of Interest
References
- Spoljaric, D.; Cipak, A.; Horvatic, J.; Andrisic, L.; Waeg, G.; Zarkovic, N.; Jaganjac, M. Endogenous 4-hydroxy-2-nonenal in microalga Chlorella kessleri acts as a bioactive indicator of pollution with common herbicides and growth regulating factor of hormesis. Aquat. Toxicol. 2011, 105, 552–558. [Google Scholar] [CrossRef]
- Poljak-Blazi, M.; Jaganjac, M.; Sabol, I.; Mihaljevic, B.; Matovina, M.; Grce, M. Effect of ferric ions on reactive oxygen species formation, cervical cancer cell lines growth and E6/E7 oncogene expression. Toxicol. Vitr. 2011, 25, 160–166. [Google Scholar] [CrossRef]
- Jaganjac, M.; Cipak, A.; Schaur, R.J.; Zarkovic, N. Pathophysiology of neutrophil-mediated extracellular redox reactions. Front. Biosci. Landmark 2016, 21, 839–855. [Google Scholar] [CrossRef]
- Slater, T.F. Free-radical mechanisms in tissue injury. Biochem. J. 1984, 222, 1–15. [Google Scholar] [CrossRef]
- Jaganjac, M.; Čačev, T.; Čipak, A.; Kapitanović, S.; Trošelj, K.G.; Žarković, N. Even stressed cells are individuals: Second messengers of free radicals in pathophysiology of cancer. Croat. Med. J. 2012, 53, 304–309. [Google Scholar] [CrossRef]
- Zarkovic, N.; Cipak, A.; Jaganjac, M.; Borovic, S.; Zarkovic, K. Pathophysiological relevance of aldehydic protein modifications. J. Proteom. 2013, 92, 239–247. [Google Scholar] [CrossRef]
- Jaganjac, M.; Cindrić, M.; Jakovčević, A.; Žarković, K.; Žarković, N. Lipid peroxidation in brain tumors. Neurochem. Int. 2021, 149, 105118. [Google Scholar] [CrossRef]
- Catalá, A.; Díaz, M. Editorial: Impact of lipid peroxidation on the physiology and pathophysiology of cell membranes. Front. Physiol. 2016, 7, 423. [Google Scholar] [CrossRef]
- Jaganjac, M.; Milkovic, L.; Gegotek, A.; Cindric, M.; Zarkovic, K.; Skrzydlewska, E.; Zarkovic, N. The relevance of pathophysiological alterations in redox signaling of 4-hydroxynonenal for pharmacological therapies of major stress-associated diseases. Free Radic. Biol. Med. 2020, 157, 128–153. [Google Scholar] [CrossRef]
- Awasthi, Y.C.; Sharma, R.; Cheng, J.Z.; Yang, Y.; Sharma, A.; Singhal, S.S.; Awasthi, S. Role of 4-hydroxynonenal in stress-mediated apoptosis signaling. Mol. Asp. Med. 2003, 24, 219–230. [Google Scholar] [CrossRef]
- Zarkovic, N.; Ilic, Z.; Jurin, M.; Schaur, R.J.; Puhl, H.; Esterbauer, H. Stimulation of HeLa cell growth by physiological concentrations of 4-hydroxynonenal. Cell Biochem. Funct. 1993, 11, 279–286. [Google Scholar] [CrossRef]
- Živković, M.; Žarković, K.; Škrinjar, L.; Waeg, G.; Poljak-Blaži, M.; Šunjić, S.B.; Schaur, R.J.; Žarković, N. A new method for detection of HNE-histidine conjugates in rat inflammatory cells. Croat. Chem. Acta 2005, 78, 91–98. [Google Scholar]
- Jaganjac, M.; Matijevic, T.; Cindric, M.; Cipak, A.; Mrakovcic, L.; Gubisch, W.; Zarkovic, N. Induction of CMV-1 promoter by 4-hydroxy-2-nonenal in human embryonic kidney cells. Acta Biochim. Pol. 2010, 57, 179–183. [Google Scholar] [CrossRef]
- Elrayess, M.A.; Almuraikhy, S.; Kafienah, W.; Al-Menhali, A.; Al-Khelaifi, F.; Bashah, M.; Zarkovic, K.; Zarkovic, N.; Waeg, G.; Alsayrafi, M.; et al. 4-hydroxynonenal causes impairment of human subcutaneous adipogenesis and induction of adipocyte insulin resistance. Free Radic. Biol. Med. 2017, 104, 129–137. [Google Scholar] [CrossRef]
- Greenacre, S.A.B.; Evans, P.; Halliwell, B.; Brain, S.D. Formation and loss of nitrated proteins in peroxynitrite-treated rat skin in vivo. Biochem. Biophys. Res. Commun. 1999, 262, 781–786. [Google Scholar] [CrossRef]
- Rubbo, H.; Radi, R.; Trujillo, M.; Telleri, R.; Kalyanaraman, B.; Barnes, S.; Kirk, M.; Freeman, B.A. Nitric oxide regulation of superoxide and peroxynitrite-dependent lipid peroxidation. Formation of novel nitrogen-containing oxidized lipid derivatives. J. Biol. Chem. 1994, 269, 26066–26075. [Google Scholar] [CrossRef]
- Szabó, C. DNA strand breakage and activation of poly-ADP ribosyltransferase: A cytotoxic pathway triggered by peroxynitrite. Free Radic. Biol. Med. 1996, 21, 855–869. [Google Scholar] [CrossRef]
- Møller, P.; Loft, S. Dietary antioxidants and beneficial effect on oxidatively damaged DNA. Free Radic. Biol. Med. 2006, 41, 388–415. [Google Scholar] [CrossRef]
- Harwell, B. Biochemistry of oxidative stress. Biochem. Soc. Trans. 2007, 35, 1147–1150. [Google Scholar] [CrossRef]
- Jaganjac, M.; Milkovic, L.; Sunjic, S.B.; Zarkovic, N. The NRF2, Thioredoxin, and Glutathione System in Tumorigenesis and Anticancer Therapies. Antioxidants 2020, 9, 1151. [Google Scholar] [CrossRef]
- Wu, Y.; Venier, M.; Hites, R.A. Broad Exposure of the North American Environment to Phenolic and Amino Antioxidants and to Ultraviolet Filters. Environ. Sci. Technol. 2020, 54, 9345–9355. [Google Scholar] [CrossRef]
- Wu, Y.; Venier, M.; Hites, R.A. Identification of Unusual Antioxidants in the Natural and Built Environments. Environ. Sci. Technol. Lett. 2019, 6, 443–447. [Google Scholar] [CrossRef]
- Wang, W.; Xiong, P.; Zhang, H.; Zhu, Q.; Liao, C.; Jiang, G. Analysis, occurrence, toxicity and environmental health risks of synthetic phenolic antioxidants: A review. Environ. Res. 2021, 201, 111531. [Google Scholar] [CrossRef]
- Liu, R.; Mabury, S.A. Synthetic Phenolic Antioxidants: A Review of Environmental Occurrence, Fate, Human Exposure, and Toxicity. Environ. Sci. Technol. 2020, 54, 11706–11719. [Google Scholar] [CrossRef]
- Lourenço, S.C.; Moldão-Martins, M.; Alves, V.D. Antioxidants of natural plant origins: From sources to food industry applications. Molecules 2019, 24, 4132. [Google Scholar] [CrossRef] [PubMed]
- Wakeel, A.; Jan, S.A.; Ullah, I.; Shinwari, Z.K.; Xu, M. Solvent polarity mediates phytochemical yield and antioxidant capacity of Isatis tinctoria. PeerJ 2019, 2019, e7857. [Google Scholar] [CrossRef]
- López-Alarcón, C.; Denicola, A. Evaluating the antioxidant capacity of natural products: A review on chemical and cellular-based assays. Anal. Chim. Acta 2013, 763, 1–10. [Google Scholar] [CrossRef]
- Apak, R.; Gorinstein, S.; Böhm, V.; Schaich, K.M.; Özyürek, M.; Güçlü, K. Methods of measurement and evaluation of natural antioxidant capacity/activity (IUPAC technical report). Pure Appl. Chem. 2013, 85, 957–998. [Google Scholar] [CrossRef]
- Litwinienko, G.; Ingold, K.U. Solvent effects on the rates and mechanisms of reaction of phenols with free radicals. Acc. Chem. Res. 2007, 40, 222–230. [Google Scholar] [CrossRef]
- Prior, R.L.; Wu, X.; Schaich, K. Standardized methods for the determination of antioxidant capacity and phenolics in foods and dietary supplements. J. Agric. Food Chem. 2005, 53, 4290–4302. [Google Scholar] [CrossRef]
- Shahidi, F.; Zhong, Y. Measurement of antioxidant activity. J. Funct. Foods 2015, 18, 757–781. [Google Scholar] [CrossRef]
- Gulcin, İ. Antioxidants and antioxidant methods: An updated overview. Arch. Toxicol. 2020, 94, 651–715. [Google Scholar] [CrossRef]
- Krzyżanowska-Kowalczyk, J.; Kowalczyk, M.; Ponczek, M.B.; Pecio, Ł.; Nowak, P.; Kolodziejczyk-Czepas, J. Pulmonaria obscura and pulmonaria officinalis extracts as mitigators of peroxynitrite-induced oxidative stress and cyclooxygenase-2 inhibitors–in vitro and in silico studies. Molecules 2021, 26, 631. [Google Scholar] [CrossRef]
- Kunchandy, E.; Rao, M.N.A. Oxygen radical scavenging activity of curcumin. Int. J. Pharm. 1990, 58, 237–240. [Google Scholar] [CrossRef]
- Fazilatun, N.; Nornisah, M.; Zhari, I. Superoxide radical scavenging properties of extracts and flavonoids isolated from the leaves of Blumea balsamifera. Pharm. Biol. 2004, 42, 404–408. [Google Scholar] [CrossRef]
- Asokkumar, K.; Umamaheswari, M.; Sivashanmugam, A.T.; Subhadradevi, V.; Subhashini, N.; Ravi, T.K. Free radical scavenging and antioxidant activities of Glinus oppositifolius (carpet weed) using different in vitro assay systems. Pharm. Biol. 2009, 47, 474–482. [Google Scholar] [CrossRef]
- Zhang, J.; Stanley, R.A.; Melton, L.D. Lipid peroxidation inhibition capacity assay for antioxidants based on liposomal membranes. Mol. Nutr. Food Res. 2006, 50, 714–724. [Google Scholar] [CrossRef]
- Carocho, M.; Ferreira, I.C.F.R. A review on antioxidants, prooxidants and related controversy: Natural and synthetic compounds, screening and analysis methodologies and future perspectives. Food Chem. Toxicol. 2013, 51, 15–25. [Google Scholar] [CrossRef] [PubMed]
- Tisma, V.S.; Basta-Juzbasic, A.; Jaganjac, M.; Brcic, L.; Dobric, I.; Lipozencic, J.; Tatzber, F.; Zarkovic, N.; Poljak-Blazi, M. Oxidative stress and ferritin expression in the skin of patients with rosacea. J. Am. Acad. Dermatol. 2009, 60, 270–276. [Google Scholar] [CrossRef] [PubMed]
- Sredoja Tisma, V.; Bulimbasic, S.; Galesic Ljubanovic, D.; Galesic, K.; Morovic-Vergles, J.; Mitrovic, J.; Uchida, K.; Tatzber, F.; Zarkovic, N.; Jaganjac, M. The Onset of Systemic Oxidative Stress Associated with the Accumulation of Lipid Peroxidation Product Acrolein in the Skin of Patients with Small-Vessel Vasculitis. Molecules 2021, 26, 2344. [Google Scholar] [CrossRef]
- Sadeer, N.B.; Montesano, D.; Albrizio, S.; Zengin, G.; Mahomoodally, M.F. The versatility of antioxidant assays in food science and safety—Chemistry, applications, strengths, and limitations. Antioxidants 2020, 9, 709. [Google Scholar] [CrossRef]
- Munteanu, I.G.; Apetrei, C. Analytical methods used in determining antioxidant activity: A review. Int. J. Mol. Sci. 2021, 22, 3380. [Google Scholar] [CrossRef]
- Félix, R.; Valentão, P.; Andrade, P.B.; Félix, C.; Novais, S.C.; Lemos, M.F.L. Evaluating the in vitro potential of natural extracts to protect lipids from oxidative damage. Antioxidants 2020, 9, 231. [Google Scholar] [CrossRef]
- Dikalov, S.I.; Harrison, D.G. Methods for detection of mitochondrial and cellular reactive oxygen species. Antioxid. Redox Signal. 2014, 20, 372–382. [Google Scholar] [CrossRef]
- Lao, H.K.; Tan, J.; Wang, C.; Zhang, X. Ratiometric polymer probe for detection of peroxynitrite and the application for live-cell imaging. Molecules 2019, 24, 465. [Google Scholar] [CrossRef] [PubMed]
- Peng, T.; Wong, N.-K.; Chen, X.; Chan, Y.-K.; Ho, D.H.-H.; Sun, Z.; Hu, J.J.; Shen, J.; El-Nezami, H.; Yang, D. Molecular imaging of peroxynitrite with HKGreen-4 in live cells and tissues. J. Am. Chem. Soc. 2014, 136, 11728–11734. [Google Scholar] [CrossRef]
- Peng, T.; Chen, X.; Gao, L.; Zhang, T.; Wang, W.; Shen, J.; Yang, D. A rationally designed rhodamine-based fluorescent probe for molecular imaging of peroxynitrite in live cells and tissues. Chem. Sci. 2016, 7, 5407–5413. [Google Scholar] [CrossRef]
- Zielonka, J.; Kalyanaraman, B. Hydroethidine- and MitoSOX-derived red fluorescence is not a reliable indicator of intracellular superoxide formation: Another inconvenient truth. Free Radic. Biol. Med. 2010, 48, 983–1001. [Google Scholar] [CrossRef] [PubMed]
- Al-Thani, A.M.; Voss, S.C.; Al-Menhali, A.S.; Barcaru, A.; Horvatovich, P.; Al Jaber, H.; Nikolovski, Z.; Latiff, A.; Georgakopoulos, C.; Merenkov, Z.; et al. Whole blood storage in CPDA1 blood bags alters erythrocyte membrane proteome. Oxid. Med. Cell. Longev. 2018, 2018. [Google Scholar] [CrossRef] [PubMed]
- Ludtmann, M.H.R.; Angelova, P.R.; Horrocks, M.H.; Choi, M.L.; Rodrigues, M.; Baev, A.Y.; Berezhnov, A.V.; Yao, Z.; Little, D.; Banushi, B.; et al. α-synuclein oligomers interact with ATP synthase and open the permeability transition pore in Parkinson’s disease. Nat. Commun. 2018, 9, 2293. [Google Scholar] [CrossRef]
- Esteras, N.; Kopach, O.; Maiolino, M.; Lariccia, V.; Amoroso, S.; Qamar, S.; Wray, S.; Rusakov, D.A.; Jaganjac, M.; Abramov, A.Y. Mitochondrial ROS control neuronal excitability and cell fate in frontotemporal dementia. Alzheimer’s Dement. 2021. [Google Scholar] [CrossRef]
- Robinson, K.M.; Janes, M.S.; Pehar, M.; Monette, J.S.; Ross, M.F.; Hagen, T.M.; Murphy, M.P.; Beckman, J.S. Selective fluorescent imaging of superoxide in vivo using ethidium-based probes. Proc. Natl. Acad. Sci. USA 2006, 103, 15038–15043. [Google Scholar] [CrossRef]
- Al-Menhali, A.S.; Jameela, S.A.; Latiff, A.A.; Elrayess, M.A.; Alsayrafi, M.; Jaganjac, M. Cistanche tubulosa induces reactive oxygen species-mediated apoptosis of primary and metastatic human colon cancer cells. J. Appl. Pharm. Sci. 2017, 7, 39–45. [Google Scholar] [CrossRef]
- Belousov, V.V.; Fradkov, A.F.; Lukyanov, K.A.; Staroverov, D.B.; Shakhbazov, K.S.; Terskikh, A.V.; Lukyanov, S. Genetically encoded fluorescent indicator for intracellular hydrogen peroxide. Nat. Methods 2006, 3, 281–286. [Google Scholar] [CrossRef]
- Drummen, G.P.; Van Liebergen, L.C.; Op den Kamp, J.A.; Post, J.A. C11-BODIPY581/591, an oxidation-sensitive fluorescent lipid peroxidation probe: (Micro)spectroscopic characterization and validation of methodology. Free Radic. Biol. Med. 2002, 33, 473–490. [Google Scholar] [CrossRef]
- Al-Menhali, A.S.; Banu, S.; Angelova, P.R.; Barcaru, A.; Horvatovich, P.; Abramov, A.Y.; Jaganjac, M. Lipid peroxidation is involved in calcium dependent upregulation of mitochondrial metabolism in skeletal muscle. Biochim. Biophys. Acta Gen. Subj. 2020, 1864, 129487. [Google Scholar] [CrossRef]
- Maraldi, T. Natural compounds as modulators of NADPH oxidases. Oxid. Med. Cell. Longev. 2013. [Google Scholar] [CrossRef] [PubMed]
- Acharya, P.; Mathur, M.C. Oxidative stress in alopecia areata: A systematic review and meta-analysis. Int. J. Dermatol. 2020, 59, 434–440. [Google Scholar] [CrossRef] [PubMed]
- Emre, S.; Metin, A.; Demirseren, D.D.; Akoglu, G.; Oztekin, A.; Neselioglu, S.; Erel, O. The association of oxidative stress and disease activity in seborrheic dermatitis. Arch. Dermatol. Res. 2012, 304, 683–687. [Google Scholar] [CrossRef] [PubMed]
- Kaur, S.; Zilmer, K.; Leping, V.; Zilmer, M. Allergic contact dermatitis is associated with significant oxidative stress. Dermatol. Res. Pract. 2014, 2014. [Google Scholar] [CrossRef]
- Sarici, G.; Cinar, S.; Armutcu, F.; Altinyazar, C.; Koca, R.; Tekin, N.S. Oxidative stress in acne vulgaris. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 763–767. [Google Scholar] [CrossRef]
- Luo, J.-Y.; Liu, X.; Jiang, M.; Zhao, H.-P.; Zhao, J.-J. Oxidative stress markers in blood in systemic sclerosis: A meta-analysis. Mod. Rheumatol. 2017, 27, 306–314. [Google Scholar] [CrossRef] [PubMed]
- Yesilova, Y.; Ucmak, D.; Selek, S.; Dertlioǧlu, S.B.; Sula, B.; Bozkus, F.; Turan, E. Oxidative stress index may play a key role in patients with pemphigus vulgaris. J. Eur. Acad. Dermatol. Venereol. 2013, 27, 465–467. [Google Scholar] [CrossRef] [PubMed]
- Kilinc, F.; Sener, S.; Akbaş, A.; Metin, A.; Kirbaş, S.; Neselioglu, S.; Erel, O. Oxidative stress parameters in localized scleroderma patients. Arch. Dermatol. Res. 2016, 308, 625–629. [Google Scholar] [CrossRef]
- Baek, J.-O.; Byamba, D.; Wu, W.H.; Kim, T.-G.; Lee, M.-G. Assessment of an imiquimod-induced psoriatic mouse model in relation to oxidative stress. Arch. Dermatol. Res. 2012, 304, 699–706. [Google Scholar] [CrossRef]
- Richmond, J.M.; Frisoli, M.L.; Harris, J.E. Innate immune mechanisms in vitiligo: Danger from within. Curr. Opin. Immunol. 2013, 25, 676–682. [Google Scholar] [CrossRef]
- Schallreuter, K.U.; Wood, J.M.; Berger, J. Low catalase levels in the epidermis of patients with vitiligo. J. Investig. Dermatol. 1991, 97, 1081–1085. [Google Scholar] [CrossRef]
- Vaccaro, M.; Bagnato, G.; Cristani, M.; Borgia, F.; Spatari, G.; Tigano, V.; Saja, A.; Guarneri, F.; Cannavò, S.P.; Gangemi, S. Oxidation products are increased in patients affected by non-segmental generalized vitiligo. Arch. Dermatol. Res. 2017, 309, 485–490. [Google Scholar] [CrossRef]
- Mehaney, D.A.; Darwish, H.A.; Hegazy, R.A.; Nooh, M.M.; Tawdy, A.M.; Gawdat, H.I.; El-Sawalhi, M.M. Analysis of oxidative stress status, catalase and catechol-O- Methyltransferase polymorphisms in Egyptian vitiligo patients. PLoS ONE 2014, 9, e99286. [Google Scholar] [CrossRef] [PubMed]
- Battino, M.; Greabu, M.; Totan, A.; Bullon, P.; Bucur, A.; Tovaru, S.; Mohora, M.; Didilescu, A.; Parlatescu, I.; Spinu, T.; et al. Oxidative stress markers in oral lichen planus. BioFactors 2008, 33, 301–310. [Google Scholar] [CrossRef]
- Budzyń, M.; Iskra, M.; Krasiński, Z.; Dzieciuchowicz, L.; Kasprzak, M.; Gryszczyńska, B. Serum iron concentration and plasma oxidantantioxidant balance in patients with chronic venous insufficency. Med. Sci. Monit. 2011, 17, CR719. [Google Scholar] [CrossRef]
- Li, W.C.; Mo, L.J.; Shi, X.; Lin, Z.Y.; Li, Y.Y.; Yang, Z.; Wu, C.L.; Li, X.H.; Luo, Y.Z.; Qin, L.Q.; et al. Antioxidant status of serum bilirubin, uric acid and albumin in pemphigus vulgaris. Clin. Exp. Dermatol. 2018, 43, 158–163. [Google Scholar] [CrossRef] [PubMed]
- Sivaranjani, N.; Venkata Rao, S.; Rajeev, G. Role of reactive oxygen species and antioxidants in atopic dermatitis. J. Clin. Diagn. Res. 2013, 7, 2683–2685. [Google Scholar] [CrossRef]
- Chen, J.; Li, S.; Li, C. Mechanisms of melanocyte death in vitiligo. Med. Res. Rev. 2021, 41, 1138–1166. [Google Scholar] [CrossRef]
- Botes, L.; Van Der Westhuizen, F.H.; Loots, D.T. Phytochemical contents and antioxidant capacities of two Aloe greatheadii var. davyana extracts. Molecules 2008, 13, 2169–2180. [Google Scholar] [CrossRef]
- Gao, Y.; Yuan, J.; Liang, X.; He, Y.; Li, P.; Yang, M. Artemisia anomala extracts enhance the viability and anti-oxidation capacity of human keratinocytes. Trop. J. Pharm. Res. 2019, 18, 61–67. [Google Scholar] [CrossRef]
- Kim, B.-H.; Oh, I.; Kim, J.-H.; Jeon, J.-E.; Jeon, B.; Shin, J.; Kim, T.-Y. Anti-inflammatory activity of compounds isolated from Astragalus sinicus L. in cytokine-induced keratinocytes and skin. Exp. Mol. Med. 2014, 46, e87. [Google Scholar] [CrossRef]
- Roy, S.; Khanna, S.; Alessio, H.M.; Vider, J.; Bagchi, D.; Bagchi, M.; Sen, C.K. Anti-angiogenic property of edible berries. Free Radic. Res. 2002, 36, 1023–1032. [Google Scholar] [CrossRef]
- García-Pérez, M.-E.; Royer, M.; Duque-Fernandez, A.; Diouf, P.N.; Stevanovic, T.; Pouliot, R. Antioxidant, toxicological and antiproliferative properties of Canadian polyphenolic extracts on normal and psoriatic keratinocytes. J. Ethnopharmacol. 2010, 132, 251–258. [Google Scholar] [CrossRef]
- Bader, A.; Martini, F.; Schinella, G.R.; Rios, J.L.; Prieto, J.M. Modulation of Cox-1, 5-, 12- And 15-Lox by popular herbal remedies used in Southern Italy against psoriasis and other skin diseases. Phyther. Res. 2015, 29, 108–113. [Google Scholar] [CrossRef]
- Abe, S.; Ueno, M.; Nishitani, M.; Akamatsu, T.; Sato, T.; Shimoda, M.; Kanaoka, H.; Nii, Y.; Yamasaki, H.; Yuasa, K. Citrus sudachi peel extract suppresses cell proliferation and promotes the differentiation of keratinocytes through inhibition of the EGFR-ERK signaling pathway. Biomolecules 2020, 10, 1468. [Google Scholar] [CrossRef]
- Gelmini, F.; Beretta, G.; Anselmi, C.; Centini, M.; Magni, P.; Ruscica, M.; Cavalchini, A.; Maffei Facino, R. GC-MS profiling of the phytochemical constituents of the oleoresin from Copaifera langsdorffii Desf. and a preliminary in vivo evaluation of its antipsoriatic effect. Int. J. Pharm. 2013, 440, 170–178. [Google Scholar] [CrossRef]
- Yang, B.-Y.; Cheng, Y.-G.; Liu, Y.; Liu, Y.; Tan, J.-Y.; Guan, W.; Guo, S.; Kuang, H.-X. Datura Metel L. Ameliorates imiquimod-induced psoriasis-like dermatitis and inhibits inflammatory cytokines production through TLR7/8-MyD88-NF-κB-NLRP3 inflammasome pathway. Molecules 2019, 24, 2157. [Google Scholar] [CrossRef] [PubMed]
- Bito, T.; Roy, S.; Sen, C.K.; Packer, L. Pine bark extract pycnogenol downregulates IFN-γ-induced adhesion of T cells to human keratinocytes by inhibiting inducible ICAM-1 expression. Free Radic. Biol. Med. 2000, 28, 219–227. [Google Scholar] [CrossRef]
- Singh, S.K.; Chouhan, H.S.; Sahu, A.N.; Narayan, G. Assessment of in vitro antipsoriatic activity of selected Indian medicinal plants. Pharm. Biol. 2015, 53, 1295–1301. [Google Scholar] [CrossRef]
- Dimitris, D.; Ekaterina-Michaela, T.; Christina, K.; Ioannis, S.; Ioanna, S.K.; Aggeliki, L.; Sophia, H.; Michael, R.; Helen, S. Melissa officinalis ssp. altissima extracts: A therapeutic approach targeting psoriasis in mice. J. Ethnopharmacol. 2020, 246. [Google Scholar] [CrossRef] [PubMed]
- Ampawong, S.; Kengkoom, K.; Sukphopetch, P.; Aramwit, P.; Muangkaew, W.; Kanjanapruthipong, T.; Buaban, T. Evaluating the effect of rice (Oryza sativa L.: SRNC05053-6-2) crude extract on psoriasis using in vitro and in vivo models. Sci. Rep. 2020, 10, 17618. [Google Scholar] [CrossRef] [PubMed]
- Ndjoubi, K.O.; Sharma, R.; Badmus, J.A.; Jacobs, A.; Jordaan, A.; Marnewick, J.; Warner, D.F.; Hussein, A.A. Antimycobacterial, cytotoxic, and antioxidant activities of abietane diterpenoids isolated from plectranthus madagascariensis. Plants 2021, 10, 175. [Google Scholar] [CrossRef]
- Parmar, K.M.; Itankar, P.R.; Joshi, A.; Prasad, S.K. Anti-psoriatic potential of Solanum xanthocarpum stem in Imiquimod-induced psoriatic mice model. J. Ethnopharmacol. 2017, 198, 158–166. [Google Scholar] [CrossRef]
- Abbas, A.N. Ginger (Zingiber officinale (L.) Rosc) improves oxidative stress and trace elements status in patients with alopecia areata. Niger. J. Clin. Pract. 2020, 23, 1555–1560. [Google Scholar] [CrossRef]
- Pekmezci, E.; Dundar, C.; Turkoglu, M. Proprietary Herbal Extract Downregulates the Gene Expression of IL-1α in HaCaT Cells: Possible Implications Against Nonscarring Alopecia. Med. Arch. (Sarajevobosnia Herzeg.) 2018, 72, 136–140. [Google Scholar] [CrossRef]
- León, L.M.; García, J.C.L.; Duarte, C.C.; García, K.G.; Guerra, I.R.; Marín, R.M. Antioxidant capacity of clusia minor l. Leaves | Capacidad antioxidante de las hojas de la especie clusia minor l. Rev. Cuba. Plantas Med. 2020, 25. [Google Scholar]
- Dammak, I.; Boudaya, S.; Abdallah, F.B.; Hamida, T.; Attia, H. Date seed Oil inhibits hydrogen peroxide-induced oxidative stress in normal human epidermal melanocytes. Connect. Tissue Res. 2009, 50, 330–335. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Yang, F.; Teng, L.; Katayama, I. 6-shogaol protects human melanocytes against oxidative stress through activation of the nrf2-antioxidant response element signaling pathway. Int. J. Mol. Sci. 2020, 21, 3537. [Google Scholar] [CrossRef]
- Lu, L.; Wang, S.; Fu, L.; Liu, D.; Zhu, Y.; Xu, A. Bilobalide protection of normal human melanocytes from hydrogen peroxide-induced oxidative damage via promotion of antioxidase expression and inhibition of endoplasmic reticulum stress. Clin. Exp. Dermatol. 2016, 41, 64–73. [Google Scholar] [CrossRef]
- Jeong, Y.-M.; Choi, Y.-G.; Kim, D.-S.; Park, S.-H.; Yoon, J.-A.; Kwon, S.-B.; Park, E.-S.; Park, K.-C. Cytoprotective effect of green tea extract and quercetin against hydrogen peroxide-induced oxidative stress. Arch. Pharm. Res. 2005, 28, 1251–1256. [Google Scholar] [CrossRef]
- Ning, W.; Wang, S.; Dong, X.; Liu, D.; Fu, L.; Jin, R.; Xu, A. Epigallocatechin-3-gallate (EGCG) suppresses the trafficking of lymphocytes to epidermal melanocytes via inhibition of JAK2: Its implication for vitiligo treatment. Biol. Pharm. Bull. 2015, 38, 1700–1706. [Google Scholar] [CrossRef]
- Moreira, C.G.; Carrenho, L.Z.B.; Pawloski, P.L.; Soley, B.S.; Cabrini, D.A.; Otuki, M.F. Pre-clinical evidences of Pyrostegia venusta in the treatment of vitiligo. J. Ethnopharmacol. 2015, 168, 315–325. [Google Scholar] [CrossRef]
- Ma, J.; Li, S.; Zhu, L.; Guo, S.; Yi, X.; Cui, T.; He, Y.; Chang, Y.; Liu, B.; Li, C.; et al. Baicalein protects human vitiligo melanocytes from oxidative stress through activation of NF-E2-related factor2 (Nrf2) signaling pathway. Free Radic. Biol. Med. 2018, 129, 492–503. [Google Scholar] [CrossRef]
- Lai, Y.; Feng, Q.; Zhang, R.; Shang, J.; Zhong, H. The great capacity on promoting melanogenesis of three compatible components in vernonia anthelmintica (L.) willd. Int. J. Mol. Sci. 2021, 22, 4073. [Google Scholar] [CrossRef]
- Kim, H.; Ban, I.; Choi, Y.; Yu, S.; Youn, S.J.; Baik, M.-Y.; Lee, H.; Kim, W. Puffing of turmeric (Curcuma longa L.) enhances its anti-inflammatory effects by upregulating macrophage oxidative phosphorylation. Antioxidants 2020, 9, 931. [Google Scholar] [CrossRef]
- Vaughn, A.R.; Pourang, A.; Clark, A.K.; Burney, W.; Sivamani, R.K. Dietary supplementation with turmeric polyherbal formulation decreases facial redness: A randomized double-blind controlled pilot study. J. Integr. Med. 2019, 17, 20–23. [Google Scholar] [CrossRef]
- Bhatt, L.R.; Lim, J.A.; Chai, K.Y.; Kang, J.I.; Oh, H.K.; Baek, S.H. Antioxidative and antimicrobial activities of essential oil from Artemisia vulgaris. Nat. Prod. Sci. 2006, 12, 226–231. [Google Scholar]
- Chrzaszcz, M.; Miazga-Karska, M.; Klimek, K.; Granica, S.; Tchórzewska, D.; Ginalska, G.; Szewczyk, K. Extracts from cephalaria uralensis (Murray) roem. & schult. and cephalaria gigantea (ledeb.) bobrov as potential agents for treatment of acne vulgaris: Chemical characterization and in vitro biological evaluation. Antioxidants 2020, 9, 796. [Google Scholar] [CrossRef]
- De Canha, M.N.; Kishore, N.; Kumar, V.; Meyer, D.; Nehar, S.; Singh, B.; Lall, N. The potential of Clausena anisata (Willd.) Hook.f. ex Benth against Propionibacterium acnes. S. Afr. J. Bot. 2018, 119, 410–419. [Google Scholar] [CrossRef]
- Yamaguchi, N.; Satoh-Yamaguchi, K.; Ono, M. In vitro evaluation of antibacterial, anticollagenase, and antioxidant activities of hop components (Humulus lupulus) addressing acne vulgaris. Phytomedicine 2009, 16, 369–376. [Google Scholar] [CrossRef]
- Matsubara, Y.; Matsumoto, T.; Sekiguchi, K.; Koseki, J.; Kaneko, A.; Yamaguchi, T.; Kurihara, Y.; Kobayashi, H.; Iriti, M. Oral administration of the Japanese traditional medicine Keishibukuryogan-ka-yokuinin decreases reactive oxygen metabolites in rat plasma: Identification of chemical constituents contributing to antioxidant activity. Molecules 2017, 22, 256. [Google Scholar] [CrossRef] [PubMed]
- Poomanee, W.; Chaiyana, W.; Mueller, M.; Viernstein, H.; Khunkitti, W.; Leelapornpisid, P. In-vitro investigation of anti-acne properties of Mangifera indica L. kernel extract and its mechanism of action against Propionibacterium acnes. Anaerobe 2018, 52, 64–74. [Google Scholar] [CrossRef]
- Kim, S.S.; Kim, J.E.; Hyun, C.-G.; Lee, N.H. Neolitsea aciculata essential oil inhibits drug-resistant skin pathogen growth and Propionibacterium acnes-induced inflammatory effects of human monocyte leukemia. Nat. Prod. Commun. 2011, 6, 1193–1198. [Google Scholar] [CrossRef]
- Chuang, L.-T.; Tsai, T.-H.; Lien, T.-J.; Huang, W.-C.; Liu, J.-J.; Chang, H.; Chang, M.-L.; Tsai, P.-J. Ethanolic extract of origanum vulgare suppresses propionibacterium acnes-induced inflammatory responses in human monocyte and mouse ear edema models. Molecules 2018, 23, 1987. [Google Scholar] [CrossRef]
- Kok, J.M.-L.; Jee, J.-M.; Chew, L.-Y.; Wong, C.-L. The potential of the brown seaweed Sargassum polycystum against acne vulgaris. J. Appl. Phycol. 2016, 28, 3127–3133. [Google Scholar] [CrossRef]
- Seong, S.J.; Su, K.J.; Sung, G.K.; Choi, J.-S.; Kwang, W.H.; Do, I.L. Anti-acne activity of Selaginella involvens extract and its non-antibiotic antimicrobial potential on Propionibacterium acnes. Phyther. Res. 2008, 22, 335–339. [Google Scholar] [CrossRef]
- Sharma, R.; Kishore, N.; Hussein, A.; Lall, N. Antibacterial and anti-inflammatory effects of Syzygium jambos L. (Alston) and isolated compounds on acne vulgaris. BMC Complement. Altern. Med. 2013, 13, 1–10. [Google Scholar] [CrossRef]
- Kalaskar, A.R.; Bhowate, R.R.; Kalaskar, R.R.; Ghonmode, S. Novel neem leaves extract mouthwash therapy for oral lichen planus. J. Herb. Med. 2021, 26, 100408. [Google Scholar] [CrossRef]
- Agha-Hosseini, F.; Borhan-Mojabi, K.; Monsef-Esfahani, H.-R.; Mirzaii-Dizgah, I.; Etemad-Moghadam, S.; Karagah, A. Efficacy of purslane in the treatment of oral lichen planus. Phyther. Res. 2010, 24, 240–244. [Google Scholar] [CrossRef]
- Grau, M.; Bölck, B.; Bizjak, D.A.; Stabenow, C.J.A.; Bloch, W. The red-vine-leaf extract AS195 increases nitric oxide synthase-dependent nitric oxide generation and decreases oxidative stress in endothelial and red blood cells. Pharmacol. Res. Perspect. 2016, 4, e00213. [Google Scholar] [CrossRef] [PubMed]
- De Almeida Cyrino, F.Z.G.; Balthazar, D.S.; Sicuro, F.L.; Bouskela, E. Effects of venotonic drugs on the microcirculation: Comparison between Ruscus extract and micronized diosmine. Clin. Hemorheol. Microcirc. 2018, 68, 361–370. [Google Scholar] [CrossRef]
- Akter, K.; Barnes, E.C.; Loa-Kum-Cheung, W.L.; Yin, P.; Kichu, M.; Brophy, J.J.; Barrow, R.A.; Imchen, I.; Vemulpad, S.R.; Jamie, J.F. Antimicrobial and antioxidant activity and chemical characterisation of Erythrina stricta Roxb. (Fabaceae). J. Ethnopharmacol. 2016, 185, 171–181. [Google Scholar] [CrossRef]
- Fu, R.; Zhang, Y.-T.; Guo, Y.-R.; Huang, Q.-L.; Peng, T.; Xu, Y.; Tang, L.; Chen, F. Antioxidant and anti-inflammatory activities of the phenolic extracts of Sapium sebiferum (L.) Roxb. leaves. J. Ethnopharmacol. 2013, 147, 517–524. [Google Scholar] [CrossRef] [PubMed]
- Arumugam, R.; Sarikurkcu, C.; Mutlu, M.; Tepe, B. Sophora alopecuroides var. alopecuroides: Phytochemical composition, antioxidant and enzyme inhibitory activity of the methanolic extract of aerial parts, flowers, leaves, roots, and stems. S. Afr. J. Bot. 2020. [Google Scholar] [CrossRef]
- Gveric-Ahmetasevic, S.; Sunjic, S.B.; Skala, H.; Andrisic, L.; Stroser, M.; Zarkovic, K.; Skrablin, S.; Tatzber, F.; Cipak, A.; Jaganjac, M.; et al. Oxidative stress in small-for-gestational age (SGA) term newborns and their mothers. Free Radic. Res. 2009, 43, 376–384. [Google Scholar] [CrossRef] [PubMed]
- Cesar, V.; Jozić, I.; Begović, L.; Vuković, T.; Mlinarić, S.; Lepeduš, H.; Šunjić, S.B.; Žarković, N. Cell-type-specific modulation of hydrogen peroxide cytotoxicity and 4-hydroxynonenal binding to human cellular proteins in vitro by antioxidant aloe vera extract. Antioxidant 2018, 7, 125. [Google Scholar] [CrossRef] [PubMed]


| Skin Disease | Imbalance in the Redox System | Reference |
|---|---|---|
| Psoriasis | Myeloperoxidase and GSH/GSSG ratio are increased | [65] |
| SOD level is decreased | ||
| Alopecia areata | SOD, paraoxonase and glutathione peroxidase are decreased | [58] |
| Total antioxidant capacity is decreased | ||
| Vitiligo | Advanced oxidation protein products, advanced glycation products and malondialdehyde levels are increased | [66,67,68,69] |
| Catalase is decreased | ||
| Rosacea | Serum peroxide and cutaneous ferritin are increased. | [39] |
| Total antioxidative potential is decreased | ||
| Acne vulgaris | Serum levels of malondialdehyde and xanthine oxidase activity are increased. | [61] |
| SOD and catalase activity are decreased. | ||
| Oral lichen planus | Salivary uric acid is decreased. | [70] |
| Serum gamma glutamyl transferase (GGT) and saliva total antioxidant capacity are increased. | ||
| Localized scleroderma (morphea)/systemic sclerosis | Total oxidant capacity, arylesterase and oxidative stress index are elevated. | [64] |
| Nitric oxide, malondialdehyde, asymmetric dimethylarginine, and ROOH in the blood are elevated. | ||
| Levels of SOD and vitamin C are decreased. | ||
| Chronic venous insufficiency | Malondialdehyde, serum iron and total antioxidant capacity are elevated. | [71] |
| Uric acid level in the circulation is low. | ||
| Pemphigus vulgaris | Serum bilirubin, uric acid and albumin are decreased. | [63,72] |
| Serum total oxidant capacity, lipid hydroperoxides and oxidative stress index are increased. | ||
| Eczema/dermatitis | SOD, catalase, GPX, GSH, and vitamins A, C, and E, total antioxidant status are decreased in the blood. | [59,60,73] |
| Total oxidative status, total peroxides and oxidative stress index are increased. |
| Skin Disease | Herbal Therapeutic Options | Mechanism of Action | References |
|---|---|---|---|
| Psoriasis | Aloe greatheadii var. davyana | Aqueous ethanol (95%) leaf gel extract has high polyphenol content and high antioxidant capacity. | [75] |
| Artemisia anomala S. | Extract inactivates MAPK and caspase pathway, promotes viability of human keratinocytes and increases antioxidant capacity. | [76] | |
| Astragalus sinicus L. | Aqueous and methanol extracts possess anti-inflammatory activity, and antioxidant activity by regulating cellular redox homeostasis and NF-κB, JAK/STAT and PI3/Akt signaling pathways. | [77] | |
| Berry extracts | Wild blueberry, bilberry, cranberry, elderberry, raspberry seed, and strawberry possess antioxidant activity and inhibit VEGF expression and impair angiogenesis. | [78] | |
| Canadian wood species | Yellow birch extract and black spruce extract had highest antioxidant capacity compared to other species. Black spruce extract demonstrated low toxicity and inhibited proliferation of normal human keratinocytes and non-lesional psoriatic keratinocytes but was not selective. | [79] | |
| Centella asiatica (L.) | Polar extract modulates cyclooxygenase and lipoxygenase activities suggesting its use for the treatment of psoriasis. | [80] | |
| Citrus sudachi | Peel extract demonstrated good radical scavenging activity and high ability in reducing power. It also inhibits EGFR-ERK signaling pathway, suppressing proliferation and inducing cell differentiation. | [81] | |
| Copaifera langsdorffii Desf. | Oleoresin reduces the release of pro-inflammatory cytokines by stimulated monocytes and its treatment improved typical clinical signs. | [82] | |
| Datura metel L. | Its application significantly reduced typical clinical signs of psoriasis. It also inhibited the inflammatory response which was suggested to be due to the TLR7/8–MyD88–NF-κb–NLRP3 inflammasome pathway inhibition. | [83] | |
| French maritime pine bark | High antioxidant and anti-inflammatory properties by inhibiting expression of inducible intercellular adhesion molecule-1 and interferon-gamma mediated activation of Stat1. | [84] | |
| Indian medicinal plants | Extracts from Phyllanthus simplex Retz., Crotolaria juncea Linn., Leucas aspera Linn., and Vitex glabrata R.Br. plants inhibit NO production and lipid peroxidation in keratinocytes and have promising antiproliferative activity. | [85] | |
| Melissa officinalis ssp. Altissima | The decoction showed high free radical scavenging activity and contributed to psoriasis treatment by decreasing inflammation and enhancing barrier function. | [86] | |
| Oryza sativa L. | Crude extract has an antioxidative property by enhancing Nrf2, induces expression of anti-inflammatory cytokines while reduces proinflammatory cytokines, impairs expression of psoriasis-associated genes and improves typical clinical signs of disease. | [87] | |
| Plectranthus madagascariensis | Contains abietane diterpenoids with excellent antioxidant activity. | [88] | |
| Solanum xanthocarpum Schrad. & Wendl. | Ethanolic stem extract has antioxidant properties and was found to inhibit the expression of proinflammatory cytokines and improves typical clinical signs of psoriasis. | [89] | |
| Alopecia areata | Ginger (Zingiber officinale (L.) Rosc) | Orally administered ginger powder elevated GSH level and reduced malondialdehyde level of erythrocytes and lymphocytes, and improved total antioxidant status in alopecia areata patients | [90] |
| Herbal extract | Extract prepared from Urtica dioica root, Urtica urens Leaf, Equisetum arvense leaf, Achillea millefolium aerial part, Matricaria chamomilla flower and Ceratonia siliqua fruit with known antioxidant and anti-inflammatory properties, downregulates expression of IL-1alpha a mediator for the hair loss. | [91] | |
| Vitiligo | Clusia minor L. | Extract of this plant used to treat vitiligo exhibit antioxidant activity as determined by radical scavenging activity and ferro-reducing activity. | [92] |
| Date seed | Date seed oil has radical scavenging activity, inhibits lipid peroxidation and protects against H2O2-induced cell death of melanocytes. | [93] | |
| Ginger | An active compound 6-shogaol has protective effects against H2O2-induced cell stress and activates Nrf2 pathway in epidermal melanocytes. | [94] | |
| Ginko biloba | Terpenoid bilobalide protects melanocytes from H2O2-induced apoptosis, promotes catalase and glutathione peroxidase 1. Bilobalide also exhibited immunoprotective effect by reducing the release of Hsp70. | [95] | |
| Green tea | Protects melanocytes from H2O2-induced cell death. Among the major constituents of green tea is Epigallocatechin-3-gallate with high antioxidant and anti-inflammatory potential that was also found to inhibit Janus kinase 2 thus suppressing trafficking of T lymphocytes to melanocytes. | [96,97] | |
| Pyrostegia venusta | Topical and oral administration of leaves extract has antioxidative and anti-inflammatory properties and increases epidermal melanin level in and animal vitiligo model. | [98] | |
| Scutellaria baicalensis | Baicalein extracted from the plant protects melanocytes from H2O2-induced apoptosis and promotes activation of Nrf2 pathway. | [99] | |
| Vernonia anthelmintica (L.) Willd. | The extract contains compounds with antioxidant properties and promotes melanogenesis. | [100] | |
| Rosacea | Turmeric (Curcuma longa) | Turmeric has antioxidant and anti-inflammatory properties and the administration of turmeric polyherbal formulation reduces facial redness intensity and distribution. | [101,102] |
| Acne vulgaris | Artemisia vulgaris | Essential oil has antioxidant properties with strong metal chelation activity and inhibits growth of Streptococcus pyogenes and Propionibacterium acnes. | [103] |
| Cephalaria uralensis | Ethanolic extract of aerial parts demonstrated radical scavenging activity, inhibits cyclooxygenase-1 and -2, and inhibits growth of Staphylococcus aureus, Staphylococcus epidermidis, and Propionibacterium acnes. | [104] | |
| Clausena anisata | Extract inhibits growth of Propionibacterium acnes, has potent antioxidant activity, inhibits lipase and hyaluronidase activity and decreases IL-8 production. | [105] | |
| Helichryssum kraussii | Extract inhibits growth of Propionibacterium acnes, has potent antioxidant activity | [105] | |
| Humulus lupulus L. | Hop extracts demonstrated antibacterial activity against five acne causing bacteria, anticollagenase inhibitory activity and good antioxidant capacity. | [106] | |
| Keishibukuryogan-ka-yokuinin (KBGY) | Oral administration inhibits formation of lipid hydroperoxides and scavenges ROS in plasma. | [107] | |
| Mangifera indica L. | Kernel extract inhibits growth of Propionibacterium acnes, has strong radical scavenging properties, inhibits linoleic acid peroxidation and secretion of IL-8. | [108] | |
| Neolitsea aciculata | Essential oil inhibits growth of Propionibacterium acnes and Staphylococcus epidermidis, has antioxidant properties and reduces release of inflammatory cytokines. | [109] | |
| Origanum vulgare | Ethanolic extract reduces generation of inflammatory cytokines and suppresses Propionibacterium acnes induced skin inflammation | [110] | |
| Sargassum polycystum C. Agardh | Methanolic fractions inhibit growth of Propionibacterium acnes, inhibits lipase and have high radical scavenging activities. | [111] | |
| Selaginella involvens | The extract inhibits production of NO, has NO scavenging effect and inhibits growth of Propionibacterium acnes. | [112] | |
| Syzygium jambos L. | The ethanol extract inhibits the growth of Propionibacterium acnes, exhibits strong antioxidant activity and inhibits the release of inflammatory cytokines. | [113] | |
| Oral lichen planus | Neem tree | Mouthwash with aqueous neem leaves extract improved symptoms of disease in patients. | [114] |
| Purslane | Oral administration of antioxidant-rich purslane led to partial or complete clinical improvement in majority of patients. | [115] | |
| Chronic venous insufficiency | Red-vine-leaf | Extract AS195 induces activation of endothelial and red blood cell nitric oxide synthase increasing NO bioavailability and ameliorates tert-butylhydroperoxide induced ROS. | [116] |
| Ruscus aculeatus | Ruscus extract showed significant venular constriction, antioxidative and anti-inflammatory properties. | [117] | |
| Eczema/ dermatitis | Erythrina stricta Roxb. | Erythrina extracts are active against Staphylococcus aureus and Candida albicans, and extracted erynone demonstrated significant radical scavenging activity. | [118] |
| Sapium sebiferum (L.) Roxb. | Phenolic extracts from leaves increase activities of catalase and SOD, increase GSH level and exhibit anti-inflammatory properties in an animal dermatitis model. | [119] | |
| Sophora alopecuroides L. | The root extract has strongest antioxidant activity and showed inhibitory activity for different enzymes. | [120] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jaganjac, M.; Sredoja Tisma, V.; Zarkovic, N. Short Overview of Some Assays for the Measurement of Antioxidant Activity of Natural Products and Their Relevance in Dermatology. Molecules 2021, 26, 5301. https://doi.org/10.3390/molecules26175301
Jaganjac M, Sredoja Tisma V, Zarkovic N. Short Overview of Some Assays for the Measurement of Antioxidant Activity of Natural Products and Their Relevance in Dermatology. Molecules. 2021; 26(17):5301. https://doi.org/10.3390/molecules26175301
Chicago/Turabian StyleJaganjac, Morana, Vesna Sredoja Tisma, and Neven Zarkovic. 2021. "Short Overview of Some Assays for the Measurement of Antioxidant Activity of Natural Products and Their Relevance in Dermatology" Molecules 26, no. 17: 5301. https://doi.org/10.3390/molecules26175301
APA StyleJaganjac, M., Sredoja Tisma, V., & Zarkovic, N. (2021). Short Overview of Some Assays for the Measurement of Antioxidant Activity of Natural Products and Their Relevance in Dermatology. Molecules, 26(17), 5301. https://doi.org/10.3390/molecules26175301







