Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects
Abstract
1. Introduction
2. Curcumin
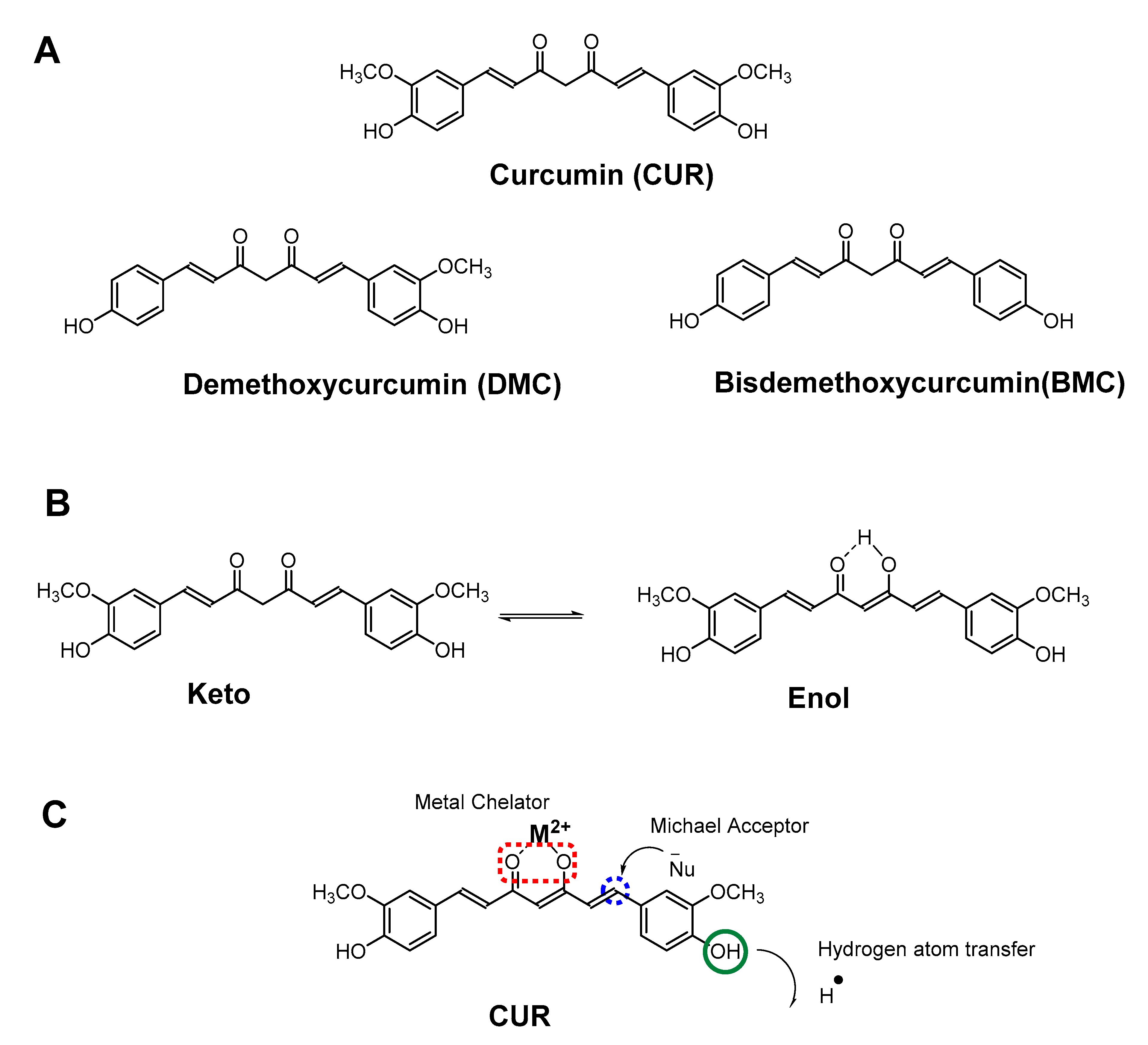
2.1. Chemistry
2.2. Bioactivity
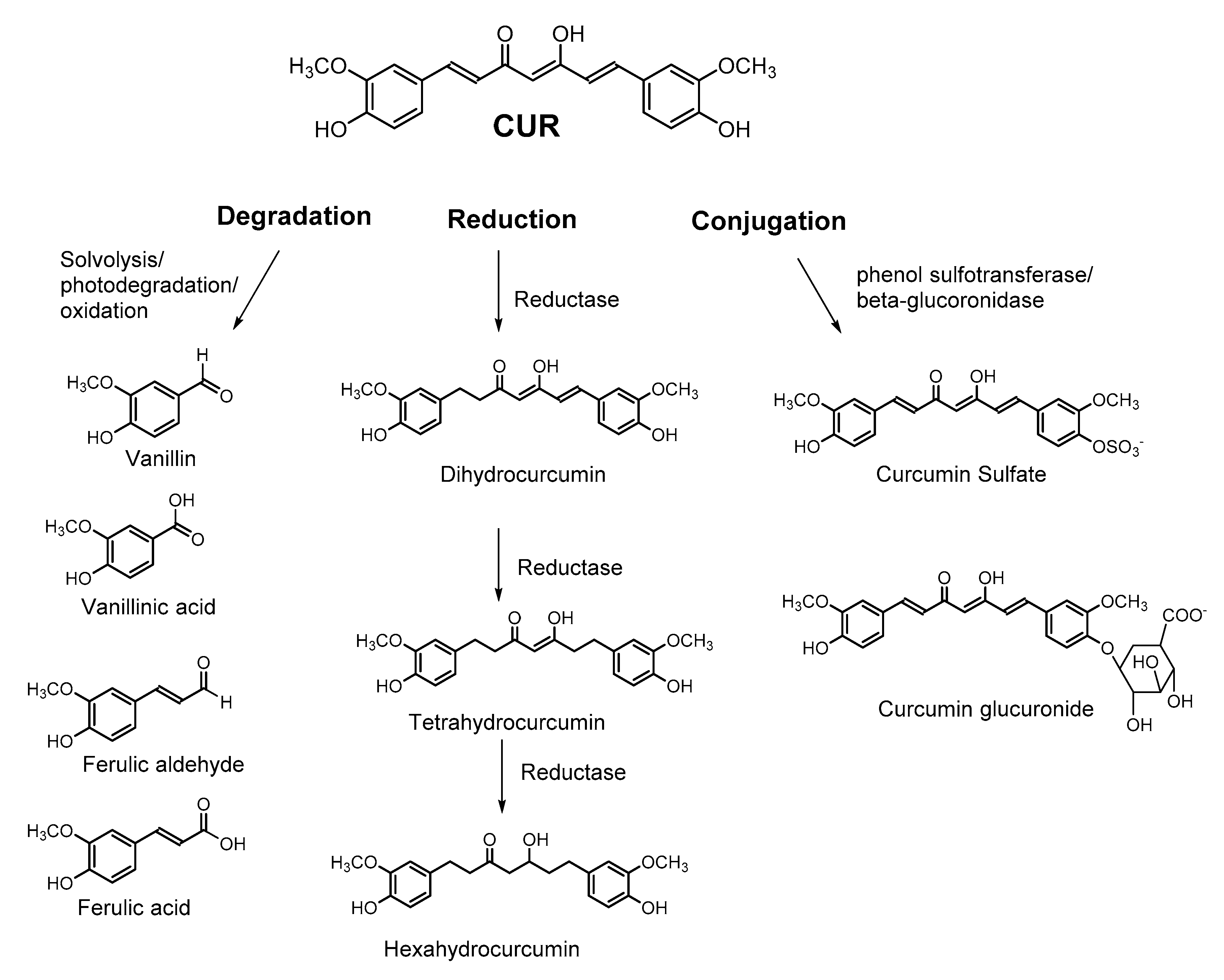
2.3. Bioavailability
3. Formulations
4. Sample Preparation for Analysis
5. Methods for Qualitative and Quantitative Analysis
6. Conclusions
Funding
Conflicts of Interest
Abbreviations
| BMC | bisdemethoxycurcumin |
| CUR | Curcumin |
| CCMs | Curcuminoids |
| DMC | Demethoxycurcumin |
| FT | Fourier transform |
| HPLC | High Performance Liquid Chromatography |
| HPTLC | High Performance Thin Layer Chromatography |
| IR | Infrared |
| LC-MS/MS | Liquid chromatography coupled with tandem mass spectrometry |
| NIR | Near-infrared |
| TLC | Thin layer chromatography |
| uHPLC | Ultra-High Performance Liquid Chromatography |
| UV-Vis | Ultraviolet/visible |
References
- Kunnumakkara, A.B.; Sailo, B.L.; Banik, K.; Harsha, C.; Prasad, S.; Gupta, S.C.; Bharti, A.C.; Aggarwal, B.B. Chronic diseases, inflammation, and spices: How are they linked? J. Transl. Med. 2018, 16, 14. [Google Scholar] [CrossRef] [PubMed]
- Hewlings, S.; Kalman, D. Curcumin: A Review of Its’ Effects on Human Health. Foods 2017, 6, 92. [Google Scholar] [CrossRef] [PubMed]
- Das, L.; Bhaumik, E.; Raychaudhuri, U.; Chakraborty, R. Role of nutraceuticals in human health. J. Food Sci. Technol. 2012, 49, 173–183. [Google Scholar] [CrossRef] [PubMed]
- Santini, A.; Tenore, G.C.; Novellino, E. Nutraceuticals: A paradigm of proactive medicine. Eur. J. Pharm. Sci. 2017, 96, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Goel, A.; Kunnumakkara, A.B.; Aggarwal, B.B. Curcumin as “Curecumin”: From kitchen to clinic. Biochem. Pharmacol. 2008, 75, 787–809. [Google Scholar] [CrossRef] [PubMed]
- Amalraj, A.; Pius, A.; Gopi, S.; Gopi, S. Biological activities of curcuminoids, other biomolecules from turmeric and their derivatives—A review. J. Tradit. Complement. Med. 2017, 7, 205–233. [Google Scholar] [CrossRef] [PubMed]
- Alves, R.C.; Fernandes, R.P.; Fonseca-Santos, B.; Victorelli, F.D.; Chorilli, M. A Critical Review of the Properties and Analytical Methods for the Determination of Curcumin in Biological and Pharmaceutical Matrices. Crit. Rev. Anal. Chem. 2019, 49, 138–149. [Google Scholar] [CrossRef]
- Araújo, C.; Leon, L. Biological activities of Curcuma longa L. Mem. Inst. Oswaldo Cruz 2001, 96, 723–728. [Google Scholar] [CrossRef]
- Prasad, S.; Aggarwal, B.B. Turmeric, the Golden Spice: From Traditional Medicine to Modern Medicine. In Herbal Medicine: Biomolecular and Clinical Aspects; Benzie, I.F.F., Wachtel-Galor, S., Eds.; CRC Press/Taylor & Francis: Boca Raton, FL, USA, 2011; ISBN 978-1-4398-0713-2. [Google Scholar]
- Herbal Supplements Market Size & Share | Industry Report, 2018–2025. Available online: https://www.grandviewresearch.com/industry-analysis/turmeric-extract-curcumin-market (accessed on 27 May 2019).
- Turmeric: Global Market Volume 2017–2027 | Statistic. Available online: https://www.statista.com/statistics/740259/global-turmeric-market-volume/ (accessed on 27 May 2019).
- Moghadamtousi, S.Z.; Kadir, H.A.; Hassandarvish, P.; Tajik, H.; Abubakar, S.; Zandi, K. A Review on Antibacterial, Antiviral, and Antifungal Activity of Curcumin. BioMed Res. Int. 2014, 2014, 186864. [Google Scholar]
- Wakte, P.S.; Sachin, B.S.; Patil, A.A.; Mohato, D.M.; Band, T.H.; Shinde, D.B. Optimization of microwave, ultra-sonic and supercritical carbon dioxide assisted extraction techniques for curcumin from Curcuma longa. Sep. Purif. Technol. 2011, 79, 50–55. [Google Scholar] [CrossRef]
- Gopi, S.; Jacob, J.; Varma, K.; Jude, S.; Amalraj, A.; Arundhathy, C.A.; George, R.; Sreeraj, T.R.; Divya, C.; Kunnumakkara, A.B.; et al. Comparative Oral Absorption of Curcumin in a Natural Turmeric Matrix with Two Other Curcumin Formulations: An Open-label Parallel-arm Study. Phytother. Res. 2017, 31, 1883–1891. [Google Scholar] [CrossRef] [PubMed]
- Gupta, S.C.; Patchva, S.; Aggarwal, B.B. Therapeutic Roles of Curcumin: Lessons Learned from Clinical Trials. AAPS J. 2013, 15, 195–218. [Google Scholar] [CrossRef] [PubMed]
- Lao, C.D.; Ruffin, M.T.; Normolle, D.; Heath, D.D.; Murray, S.I.; Bailey, J.M.; Boggs, M.E.; Crowell, J.; Rock, C.L.; Brenner, D.E. Dose escalation of a curcuminoid formulation. BMC Complement. Altern. Med. 2006, 6, 10. [Google Scholar] [CrossRef]
- Prasad, S.; Gupta, S.C.; Tyagi, A.K.; Aggarwal, B.B. Curcumin, a component of golden spice: From bedside to bench and back. Biotechnol. Adv. 2014, 32, 1053–1064. [Google Scholar] [CrossRef] [PubMed]
- Anand, P.; Kunnumakkara, A.B.; Newman, R.A.; Aggarwal, B.B. Bioavailability of Curcumin: Problems and Promises. Mol. Pharm. 2007, 4, 807–818. [Google Scholar] [CrossRef] [PubMed]
- Kunnumakkara, A.B.; Bordoloi, D.; Padmavathi, G.; Monisha, J.; Roy, N.K.; Prasad, S.; Aggarwal, B.B. Curcumin, the golden nutraceutical: Multitargeting for multiple chronic diseases. Br. J. Pharmacol. 2017, 174, 1325–1348. [Google Scholar] [CrossRef] [PubMed]
- Hussain, Z.; Thu, H.E.; Ng, S.-F.; Khan, S.; Katas, H. Nanoencapsulation, an efficient and promising approach to maximize wound healing efficacy of curcumin: A review of new trends and state-of-the-art. Colloids Surf. B Biointerfaces 2017, 150, 223–241. [Google Scholar] [CrossRef]
- Mirzaei, H.; Shakeri, A.; Rashidi, B.; Jalili, A.; Banikazemi, Z.; Sahebkar, A. Phytosomal curcumin: A review of pharmacokinetic, experimental and clinical studies. Biomed. Pharmacother. 2017, 85, 102–112. [Google Scholar] [CrossRef] [PubMed]
- Schneider, C.; Gordon, O.N.; Edwards, R.L.; Luis, P.B. Degradation of Curcumin: From Mechanism to Biological Implications. J. Agric. Food Chem. 2015, 63, 7606–7614. [Google Scholar] [CrossRef]
- Ghosh, S.; Banerjee, S.; Sil, P.C. The beneficial role of curcumin on inflammation, diabetes and neurodegenerative disease: A recent update. Food Chem. Toxicol. 2015, 83, 111–124. [Google Scholar] [CrossRef] [PubMed]
- Nelson, K.M.; Dahlin, J.L.; Bisson, J.; Graham, J.; Pauli, G.F.; Walters, M.A. The Essential Medicinal Chemistry of Curcumin: Miniperspective. J. Med. Chem. 2017, 60, 1620–1637. [Google Scholar] [CrossRef] [PubMed]
- Kunati, S.R.; Yang, S.; William, B.M.; Xu, Y. An LC-MS/MS method for simultaneous determination of curcumin, curcumin glucuronide and curcumin sulfate in a phase II clinical trial. J. Pharm. Biomed. Anal. 2018, 156, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Yang, H.; Buckley, B.; Wang, L.; Kong, A.-N. A Novel Triple Stage Ion Trap MS method validated for curcumin pharmacokinetics application: A comparison summary of the latest validated curcumin LC/MS methods. J. Pharm. Biomed. Anal. 2018, 156, 116–124. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Sun, D.; Bi, X.; Zeng, X.; Luo, W.; Cai, D.; Zeng, Q.; Xu, A. Pharmacokinetic based study on “lagged stimulation” of Curcumae Longae Rhizoma—Piper nigrum couplet in their main active components’ metabolism using UPLC-MS-MS. Phytomedicine 2017, 27, 15–22. [Google Scholar] [CrossRef] [PubMed]
- Ramalingam, P.; Ko, Y.T. A validated LC-MS/MS method for quantitative analysis of curcumin in mouse plasma and brain tissue and its application in pharmacokinetic and brain distribution studies. J. Chromatogr. B 2014, 969, 101–108. [Google Scholar] [CrossRef] [PubMed]
- Ashraf, K.; Mujeeb, M.; Ahmad, A.; Ahmad, N.; Amir, M. Determination of Curcuminoids in Curcuma longa Linn. by UPLC/Q-TOF-MS: An Application in Turmeric Cultivation. J. Chromatogr. Sci. 2015, 53, 1346–1352. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Siard, M.; Adams, A.; Keowen, M.L.; Miller, T.K.; Garza, F., Jr.; Andrews, F.M.; Seeram, N.P. Simultaneous quantification of free curcuminoids and their metabolites in equine plasma by LC-ESI-MS/MS. J. Pharm. Biomed. Anal. 2018, 154, 31–39. [Google Scholar] [CrossRef]
- Liang, S.; Zeng, Y.; Wu, J.; Li, Z.; Luo, H.; Wu, Z. Development and Validation of a Rapid and Specific UHPLC–MS/MS Method for Simultaneous Determination of 21 Bioactive Components in Tiantai No. 1 Pill and Rat Plasma. Chromatographia 2018, 81, 447–456. [Google Scholar] [CrossRef]
- Chao, I.-C.; Wang, C.-M.; Li, S.-P.; Lin, L.-G.; Ye, W.-C.; Zhang, Q.-W. Simultaneous Quantification of Three Curcuminoids and Three Volatile Components of Curcuma longa Using Pressurized Liquid Extraction and High-Performance Liquid Chromatography. Molecules 2018, 23, 1568. [Google Scholar] [CrossRef]
- Kumar, G.; Ganguly, P.; Singh, R.; Katiyar, C. Simultaneous Determination of Salicin, Curcumin and Gallic Acid in Herbal Pain Relief Tablet by High Performance Thin Layer Chromatography. Int. J. Res. Pharm. Biosci. 2018, 5, 1–6. [Google Scholar]
- Rohman, A. Analysis of curcuminoids in food and pharmaceutical products. Int. Food Res. J. 2012, 19, 19–27. [Google Scholar]
- Jude, S.; Amalraj, A.; Kunnumakkara, A.; Divya, C.; Löffler, B.-M.; Gopi, S. Development of Validated Methods and Quantification of Curcuminoids and Curcumin Metabolites and Their Pharmacokinetic Study of Oral Administration of Complete Natural Turmeric Formulation (Cureit™) in Human Plasma via UPLC/ESI-Q-TOF-MS Spectrometry. Molecules 2018, 23, 2415. [Google Scholar] [CrossRef]
- Jia, S.; Du, Z.; Song, C.; Jin, S.; Zhang, Y.; Feng, Y.; Xiong, C.; Jiang, H. Identification and characterization of curcuminoids in turmeric using ultra-high performance liquid chromatography-quadrupole time of flight tandem mass spectrometry. J. Chromatogr. A 2017, 1521, 110–122. [Google Scholar] [CrossRef]
- Huang, Y.-S.; Hsieh, T.-J.; Lu, C.-Y. Simple analytical strategy for MALDI-TOF-MS and nanoUPLC–MS/MS: Quantitating curcumin in food condiments and dietary supplements and screening of acrylamide-induced ROS protein indicators reduced by curcumin. Food Chem. 2015, 174, 571–576. [Google Scholar] [CrossRef]
- Liu, X.; Zhu, L.; Gao, X.; Wang, Y.; Lu, H.; Tang, Y.; Li, J. Magnetic molecularly imprinted polymers for spectrophotometric quantification of curcumin in food. Food Chem. 2016, 202, 309–315. [Google Scholar] [CrossRef]
- Da Silva-Buzanello, R.A.; Ferro, A.C.; Bona, E.; Cardozo-Filho, L.; De Araújo, P.H.H.; Leimann, F.V.; Gonçalves, O.H. Validation of an Ultraviolet-visible (UV-Vis) technique for the quantitative determination of curcumin in poly(l-lactic acid) nanoparticles. Food Chem. 2015, 172, 99–104. [Google Scholar] [CrossRef]
- Jayaprakasha, G.K.; Rao, L.J.M.; Sakariah, K.K. Improved HPLC Method for the Determination of Curcumin, Demethoxycurcumin, and Bisdemethoxycurcumin. J. Agric. Food Chem. 2002, 50, 3668–3672. [Google Scholar] [CrossRef]
- Dhakal, S.; Chao, K.; Schmidt, W.; Qin, J.; Kim, M.; Chan, D. Evaluation of Turmeric Powder Adulterated with Metanil Yellow Using FT-Raman and FT-IR Spectroscopy. Foods 2016, 5, 36. [Google Scholar] [CrossRef]
- Dhakal, S.; Chao, K.; Schmidt, W.; Qin, J.; Kim, M.; Huang, Q. Detection of Azo Dyes in Curry Powder Using a 1064-nm Dispersive Point-Scan Raman System. Appl. Sci. 2018, 8, 564. [Google Scholar] [CrossRef]
- Tanaka, K.; Kuba, Y.; Sasaki, T.; Hiwatashi, F.; Komatsu, K. Quantitation of Curcuminoids in Curcuma Rhizome by Near-infrared Spectroscopic Analysis. J. Agric. Food Chem. 2008, 56, 8787–8792. [Google Scholar] [CrossRef]
- Kim, Y.-J.; Lee, H.J.; Shin, H.-S.; Shin, Y. Near-infrared Reflectance Spectroscopy as a Rapid and Non-destructive Analysis Tool for Curcuminoids in Turmeric. Phytochem. Anal. 2014, 25, 445–452. [Google Scholar] [CrossRef]
- Mangolim, C.S.; Moriwaki, C.; Nogueira, A.C.; Sato, F.; Baesso, M.L.; Neto, A.M.; Matioli, G. Curcumin–β-cyclodextrin inclusion complex: Stability, solubility, characterisation by FT-IR, FT-Raman, X-ray diffraction and photoacoustic spectroscopy, and food application. Food Chem. 2014, 153, 361–370. [Google Scholar] [CrossRef]
- Gören, A.C.; Çıkrıkçı, S.; Çergel, M.; Bilsel, G. Rapid quantitation of curcumin in turmeric via NMR and LC-tandem mass spectrometry. Food Chem. 2009, 113, 1239–1242. [Google Scholar] [CrossRef]
- Kharat, S.; Namdeo, A.; Mehta, P. Development and validation of HPTLC method for simultaneous estimation of curcumin and galangin in polyherbal capsule dosage form. J. Taibah Univ. Sci. 2017, 11, 775–781. [Google Scholar] [CrossRef]
- Gad, H.A.; Bouzabata, A. Application of chemometrics in quality control of Turmeric (Curcuma longa) based on Ultra-violet, Fourier transform-infrared and 1H NMR spectroscopy. Food Chem. 2017, 237, 857–864. [Google Scholar] [CrossRef]
- Mudge, E.; Chan, M.; Venkataraman, S.; Brown, P.N. Curcuminoids in Turmeric Roots and Supplements: Method Optimization and Validation. Food Anal. Methods 2016, 9, 1428–1435. [Google Scholar] [CrossRef]
- Priyadarsini, K. The Chemistry of Curcumin: From Extraction to Therapeutic Agent. Molecules 2014, 19, 20091–20112. [Google Scholar] [CrossRef]
- Strimpakos, A.S.; Sharma, R.A. Curcumin: Preventive and Therapeutic Properties in Laboratory Studies and Clinical Trials. Antioxid. Redox Signal. 2008, 10, 511–546. [Google Scholar] [CrossRef]
- Vogel, H.A.; Pelletier, J. Curcumin-biological and medicinal properties. J. Pharma 1815, 2, 50. [Google Scholar]
- Lampe, V.; Milobedzka, J. Studien uber Curcumin. Ber. Dtsch. Chem. Ges. 1913, 46, 2235–2240. [Google Scholar] [CrossRef]
- Gupta, S.C.; Patchva, S.; Koh, W.; Aggarwal, B.B. Discovery of Curcumin, a Component of the Golden Spice, and Its Miraculous Biological Activities. Clin. Exp. Pharmacol. Physiol. 2012, 39, 283–299. [Google Scholar] [CrossRef] [PubMed]
- Priyadarsini, K.I. Photophysics, photochemistry and photobiology of curcumin: Studies from organic solutions, bio-mimetics and living cells. J. Photochem. Photobiol. C Photochem. Rev. 2009, 10, 81–95. [Google Scholar] [CrossRef]
- Payton, F.; Sandusky, P.; Alworth, W.L. NMR Study of the Solution Structure of Curcumin. J. Nat. Prod. 2007, 70, 143–146. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, B.B.; Kumar, A.; Bharti, A.C. Anticancer potential of curcumin: Preclinical and clinical studies. Anticancer Res. 2003, 23, 363–398. [Google Scholar] [PubMed]
- Banerjee, S.; Chakravarty, A.R. Metal Complexes of Curcumin for Cellular Imaging, Targeting, and Photoinduced Anticancer Activity. Acc. Chem. Res. 2015, 48, 2075–2083. [Google Scholar] [CrossRef] [PubMed]
- Wanninger, S.; Lorenz, V.; Subhan, A.; Edelmann, F.T. Metal complexes of curcumin—Synthetic strategies, structures and medicinal applications. Chem. Soc. Rev. 2015, 44, 4986–5002. [Google Scholar] [CrossRef] [PubMed]
- Mei, X.; Xu, D.; Xu, S.; Zheng, Y.; Xu, S. Gastroprotective and antidepressant effects of a new zinc(II)-curcumin complex in rodent models of gastric ulcer and depression induced by stresses. Pharmacol. Biochem. Behav. 2011, 99, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Pucci, D.; Bellini, T.; Crispini, A.; D’Agnano, I.; Liguori, P.F.; Garcia-Orduña, P.; Pirillo, S.; Valentini, A.; Zanchetta, G. DNA binding and cytotoxicity of fluorescent curcumin-based Zn(II) complexes. Med. Chem. Commun. 2012, 3, 462–468. [Google Scholar] [CrossRef]
- Baum, L.; Ng, A. Curcumin interaction with copper and iron suggests one possible mechanism of action in Alzheimer’s disease animal models. J. Alzheimers Dis. 2004, 6, 367–377. [Google Scholar] [CrossRef]
- Sood, P.K.; Nahar, U.; Nehru, B. Curcumin Attenuates Aluminum-Induced Oxidative Stress and Mitochondrial Dysfunction in Rat Brain. Neurotox. Res. 2011, 20, 351–361. [Google Scholar] [CrossRef]
- Abrahams, S.; Haylett, W.L.; Johnson, G.; Carr, J.A.; Bardien, S. Antioxidant effects of curcumin in models of neurodegeneration, aging, oxidative and nitrosative stress: A review. Neuroscience 2019, 406, 1–21. [Google Scholar] [CrossRef]
- Yang, F.; Lim, G.P.; Begum, A.N.; Ubeda, O.J.; Simmons, M.R.; Ambegaokar, S.S.; Chen, P.P.; Kayed, R.; Glabe, C.G.; Frautschy, S.A.; et al. Curcumin Inhibits Formation of Amyloid β Oligomers and Fibrils, Binds Plaques, and Reduces Amyloid in Vivo. J. Biol. Chem. 2005, 280, 5892–5901. [Google Scholar] [CrossRef]
- Nicolas, J.; Mura, S.; Brambilla, D.; Mackiewicz, N.; Couvreur, P. Design, functionalization strategies and biomedical applications of targeted biodegradable/biocompatible polymer-based nanocarriers for drug delivery. Chem. Soc. Rev. 2013, 42, 1147–1235. [Google Scholar] [CrossRef]
- García-Niño, W.R.; Pedraza-Chaverrí, J. Protective effect of curcumin against heavy metals-induced liver damage. Food Chem. Toxicol. 2014, 69, 182–201. [Google Scholar] [CrossRef]
- Yadav, A.; Lomash, V.; Samim, M.; Flora, S.J.S. Curcumin encapsulated in chitosan nanoparticles: A novel strategy for the treatment of arsenic toxicity. Chem Biol. Interact. 2012, 199, 49–61. [Google Scholar] [CrossRef]
- Shukla, P.K.; Khanna, V.K.; Khan, M.Y.; Srimal, R.C. Protective effect of curcumin against lead neurotoxicity in rat. Hum. Exp. Toxicol. 2003, 22, 653–658. [Google Scholar] [CrossRef]
- Agarwal, R.; Goel, S.K.; Behari, J.R. Detoxification and antioxidant effects of curcumin in rats experimentally exposed to mercury. J. Appl. Toxicol. 2010, 30, 457–468. [Google Scholar] [CrossRef]
- Flora, G.; Gupta, D.; Tiwari, A. Toxicity of lead: A review with recent updates. Interdiscip. Toxicol. 2012, 5, 47–58. [Google Scholar] [CrossRef]
- Oguzturk, H.; Ciftci, O.; Aydin, M.; Timurkaan, N.; Beytur, A.; Yilmaz, F. Ameliorative effects of curcumin against acute cadmium toxicity on male reproductive system in rats. Andrologia 2012, 44, 243–249. [Google Scholar] [CrossRef]
- Priyadarsini, K.I. Chemical and structural features influencing the biological activity of curcumin. Curr. Pharm. Des. 2013, 19, 2093–2100. [Google Scholar]
- Awasthi, S.; Pandya, U.; Singhal, S.S.; Lin, J.T.; Thiviyanathan, V.; Seifert, W.E., Jr.; Awasthi, Y.C.; Ansari, G.A.S. Curcumin-glutathione interactions and the role of human glutathione S-transferase P1-1. Chem Biol Interact 2000, 128, 19–38. [Google Scholar] [CrossRef]
- Jackson, P.A.; Widen, J.C.; Harki, D.A.; Brummond, K.M. Covalent Modifiers: A Chemical Perspective on the Reactivity of α,β-Unsaturated Carbonyls with Thiols via Hetero-Michael Addition Reactions. J. Med. Chem. 2017, 60, 839–885. [Google Scholar] [CrossRef]
- Fang, J.; Lu, J.; Holmgren, A. Thioredoxin Reductase Is Irreversibly Modified by Curcumin: A Novel Molecular Mechanism for its Anticancer Activity. J. Biol. Chem. 2005, 280, 25284–25290. [Google Scholar] [CrossRef]
- Lelli, D.; Sahebkar, A.; Johnston, T.P.; Pedone, C. Curcumin use in pulmonary diseases: State of the art and future perspectives. Pharmacol. Res. 2017, 115, 133–148. [Google Scholar] [CrossRef]
- Leiherer, A.; Mündlein, A.; Drexel, H. Phytochemicals and their impact on adipose tissue inflammation and diabetes. Vasc. Pharmacol. 2013, 58, 3–20. [Google Scholar] [CrossRef]
- Garcea, G.; Berry, D.P.; Jones, D.J.L.; Singh, R.; Dennison, A.R.; Farmer, P.B.; Sharma, R.A.; Steward, W.P.; Gescher, A.J. Consumption of the Putative Chemopreventive Agent Curcumin by Cancer Patients: Assessment of Curcumin Levels in the Colorectum and their Pharmacodynamic Consequences. Cancer Epidemiol. Biomark. Prev. 2005, 14, 120–125. [Google Scholar]
- He, Z.-Y.; Shi, C.-B.; Wen, H.; Li, F.-L.; Wang, B.-L.; Wang, J. Upregulation of p53 Expression in Patients with Colorectal Cancer by Administration of Curcumin. Cancer Investig. 2011, 29, 208–213. [Google Scholar] [CrossRef]
- Kim, S.G.; Veena, M.S.; Basak, S.K.; Han, E.; Tajima, T.; Gjertson, D.W.; Starr, J.; Eidelman, O.; Pollard, H.B.; Srivastava, M.; et al. Curcumin Treatment Suppresses IKKβ Kinase Activity of Salivary Cells of Patients with Head and Neck Cancer: A Pilot Study. Clin. Cancer Res. 2011, 17, 5953–5961. [Google Scholar] [CrossRef]
- Sahebkar, A. Are Curcuminoids Effective C-Reactive Protein-Lowering Agents in Clinical Practice? Evidence from a Meta-Analysis. Phytother. Res. 2014, 28, 633–642. [Google Scholar] [CrossRef]
- Aggarwal, B.B.; Shishodia, S. Suppression of the Nuclear Factor-kB Activation Pathway by Spice-Derived Phytochemicals: Reasoning for Seasoning. Ann. N. Y. Acad. Sci. 2004, 1030, 434–441. [Google Scholar] [CrossRef]
- Swamy, A.V.; Gulliaya, S.; Thippeswamy, A.; Koti, B.C.; Manjula, D.V. Cardioprotective effect of curcumin against doxorubicin-induced myocardial toxicity in albino rats. Indian J. Pharmacol. 2012, 44, 73–77. [Google Scholar] [CrossRef]
- Arun, N.; Nalini, N. Efficacy of turmeric on blood sugar and polyol pathway in diabetic albino rats. Plant Foods Hum. Nutr. 2002, 57, 41–52. [Google Scholar] [CrossRef]
- Murugan, P.; Pari, L. Influence of Tetrahydrocurcumin on Hepatic and Renal Functional Markers and Protein Levels in Experimental Type 2 Diabetic Rats. Basic Clin. Pharmacol. Toxicol. 2007, 101, 241–245. [Google Scholar] [CrossRef]
- Pagano, E.; Romano, B.; Izzo, A.A.; Borrelli, F. The clinical efficacy of curcumin-containing nutraceuticals: An overview of systematic reviews. Pharmacol. Res. 2018, 134, 79–91. [Google Scholar] [CrossRef]
- Ireson, C.R.; Jones, D.J.L.; Orr, S.; Coughtrie, M.W.H.; Boocock, D.J.; Williams, M.L.; Farmer, P.B.; Steward, W.P.; Gescher, A.J. Metabolism of the Cancer Chemopreventive Agent Curcumin in Human and Rat Intestine. Cancer Epidemiol. Biomark. Prev. 2002, 11, 105–111. [Google Scholar]
- Hoehle, S.I.; Pfeiffer, E.; Metzler, M. Glucuronidation of curcuminoids by human microsomal and recombinant UDP-glucuronosyltransferases. Mol. Nutr. Food Res. 2007, 51, 932–938. [Google Scholar] [CrossRef]
- Jäger, R.; Lowery, R.P.; Calvanese, A.V.; Joy, J.M.; Purpura, M.; Wilson, J.M. Comparative absorption of curcumin formulations. Nutr. J. 2014, 13, 11. [Google Scholar] [CrossRef]
- Prasad, S.; Tyagi, A.K.; Aggarwal, B.B. Recent Developments in Delivery, Bioavailability, Absorption and Metabolism of Curcumin: The Golden Pigment from Golden Spice. Cancer Res. Treat. 2014, 46, 2–18. [Google Scholar] [CrossRef]
- Naksuriya, O.; Okonogi, S.; Schiffelers, R.M.; Hennink, W.E. Curcumin nanoformulations: A review of pharmaceutical properties and preclinical studies and clinical data related to cancer treatment. Biomaterials 2014, 35, 3365–3383. [Google Scholar] [CrossRef]
- Purpura, M.; Lowery, R.P.; Wilson, J.M.; Mannan, H.; Münch, G.; Razmovski-Naumovski, V. Analysis of different innovative formulations of curcumin for improved relative oral bioavailability in human subjects. Eur. J. Nutr. 2018, 57, 929–938. [Google Scholar] [CrossRef]
- Yallapu, M.M.; Nagesh, P.K.B.; Jaggi, M.; Chauhan, S.C. Therapeutic Applications of Curcumin Nanoformulations. AAPS J. 2015, 17, 1341–1356. [Google Scholar] [CrossRef]
- Rahimi, H.R.; Nedaeinia, R.; Shamloo, A.S.; Nikdoust, S.; Oskuee, K. Novel delivery system for natural products: Nano-curcumin formulations. Avicenna J. Phytomed. 2016, 6, 383–398. [Google Scholar]
- Szymusiak, M.; Hu, X.; Leon Plata, P.A.; Ciupinski, P.; Wang, Z.J.; Liu, Y. Bioavailability of curcumin and curcumin glucuronide in the central nervous system of mice after oral delivery of nano-curcumin. Int. J. Pharm. 2016, 511, 415–423. [Google Scholar] [CrossRef]
- Lu, P.S.; Inbaraj, B.S.; Chen, B.H. Determination of oral bioavailability of curcuminoid dispersions and nanoemulsions prepared from Curcuma longa Linnaeus. J. Sci. Food Agric. 2018, 98, 51–63. [Google Scholar] [CrossRef]
- Desai, K. A novel Curcumin Complex with Superior Efficacy to Indomethacin and Native Curcumin in an Inflammatory Model. SF J. Orthop. Rheumatol. 2017, 1, 1. [Google Scholar]
- Stohs, S.J.; Ji, J.; Bucci, L.R.; Preuss, H.G. A Comparative Pharmacokinetic Assessment of a Novel Highly Bioavailable Curcumin Formulation with 95% Curcumin: A Randomized, Double-Blind, Crossover Study. J. Am. Coll. Nutr. 2018, 37, 51–59. [Google Scholar] [CrossRef]
- Sari, T.P.; Mann, B.; Kumar, R.; Singh, R.R.B.; Sharma, R.; Bhardwaj, M.; Athira, S. Preparation and characterization of nanoemulsion encapsulating curcumin. Food Hydrocoll. 2015, 43, 540–546. [Google Scholar] [CrossRef]
- Khan, S.; Imran, M.; Butt, T.T.; Ali Shah, S.W.; Sohail, M.; Malik, A.; Das, S.; Thu, H.E.; Adam, A.; Hussain, Z. Curcumin based nanomedicines as efficient nanoplatform for treatment of cancer: New developments in reversing cancer drug resistance, rapid internalization, and improved anticancer efficacy. Trends Food Sci. Technol. 2018, 80, 8–22. [Google Scholar] [CrossRef]
- Cuomo, J.; Appendino, G.; Dern, A.S.; Schneider, E.; McKinnon, T.P.; Brown, M.J.; Togni, S.; Dixon, B.M. Comparative Absorption of a Standardized Curcuminoid Mixture and Its Lecithin Formulation. J. Nat. Prod. 2011, 74, 664–669. [Google Scholar] [CrossRef]
- Panahi, Y.; Saadat, A.; Beiraghdar, F.; Sahebkar, A. Adjuvant Therapy with Bioavailability-Boosted Curcuminoids Suppresses Systemic Inflammation and Improves Quality of Life in Patients with Solid Tumors: A Randomized Double-Blind Placebo-Controlled Trial. Phytother. Res. 2014, 28, 1461–1467. [Google Scholar] [CrossRef]
- Sundar Dhilip Kumar, S.; Houreld, N.N.; Abrahamse, H. Therapeutic Potential and Recent Advances of Curcumin in the Treatment of Aging-Associated Diseases. Molecules 2018, 23, 835. [Google Scholar] [CrossRef]
- Steigerwalt, R.; Nebbioso, M.; Appendino, G.; Belcaro, G.; Ciammaichella, G.; Cornelli, U.; Luzzi, R.; Togni, S.; Dugall, M.; Cesarone, M.R.; et al. Meriva®, a lecithinized curcumin delivery system, in diabetic microangiopathy and retinopathy. Panminerva Med. 2012, 54, 11–16. [Google Scholar]
- Belcaro, G.; Cesarone, M.R.; Dugall, M.; Pellegrini, L.; Ledda, A.; Grossi, M.G.; Togni, S.; Appendino, G. Efficacy and Safety of Meriva®, a Curcumin-phosphatidylcholine Complex, during Extended Administration in Osteoarthritis Patients. Altern. Med. Rev. 2010, 15, 337–344. [Google Scholar]
- Mazzolani, F.; Togni, S. Oral administration of a curcumin-phospholipid delivery system for the treatment of central serous chorioretinopathy: A 12-month follow-up study. Clin. Ophthalmol. 2013, 7, 939–945. [Google Scholar]
- Cheng, K.K.; Yeung, C.F.; Ho, S.W.; Chow, S.F.; Chow, A.H.L.; Baum, L. Highly stabilized curcumin nanoparticles tested in an in vitro blood–brain barrier model and in Alzheimer’s disease Tg2576 Mice. AAPS J. 2013, 15, 324–336. [Google Scholar] [CrossRef]
- Mazzolani, F. Pilot study of oral administration of a curcumin-phospholipid formulation for treatment of central serous chorioretinopathy. Clin. Ophthalmol. 2012, 6, 801–806. [Google Scholar]
- Belcaro, G.; Cesarone, M.R.; Dugall, M.; Pellegrini, L.; Ledda, A.; Grossi, M.G.; Togni, S.; Appendino, G. Product-evaluation registry of Meriva®, a curcumin-phosphatidylcholine complex, for the complementary management of osteoarthritis. Panminerva Med. 2010, 52, 55–62. [Google Scholar]
- Appendino, G.; Belcaro, G.; Cornelli, U.; Luzzi, R.; Togni, S.; Dugall, M.; Cesarone, M.R.; Feragalli, B.; Ippolito, E.; Errichi, B.M.; et al. Potential role of curcumin phytosome (Meriva) in controlling the evolution of diabetic microangiopathy. A pilot study. Panminerva Med. 2011, 53, 43–49. [Google Scholar]
- Belcaro, G.; Hosoi, M.; Pellegrini, L.; Appendino, G.; Ippolito, E.; Ricci, A.; Ledda, A.; Dugall, M.; Cesarone, M.R.; Maione, C.; et al. A Controlled Study of a Lecithinized Delivery System of Curcumin (Meriva®) to Alleviate the Adverse Effects of Cancer Treatment. Phytother. Res. 2014, 28, 444–450. [Google Scholar] [CrossRef]
- Di Pierro, F.; Settembre, R. Safety and efficacy of an add-on therapy with curcumin phytosome and piperine and/or lipoic acid in subjects with a diagnosis of peripheral neuropathy treated with dexibuprofen. J. Pain Res. 2013, 6, 497–503. [Google Scholar] [CrossRef]
- Sasaki, H.; Sunagawa, Y.; Takahashi, K.; Imaizumi, A.; Fukuda, H.; Hashimoto, T.; Wada, H.; Katanasaka, Y.; Kakeya, H.; Fujita, M.; et al. Innovative Preparation of Curcumin for Improved Oral Bioavailability. Biol. Pharm. Bull. 2011, 34, 660–665. [Google Scholar] [CrossRef]
- Kanai, M.; Imaizumi, A.; Otsuka, Y.; Sasaki, H.; Hashiguchi, M.; Tsujiko, K.; Matsumoto, S.; Ishiguro, H.; Chiba, T. Dose-escalation and pharmacokinetic study of nanoparticle curcumin, a potential anticancer agent with improved bioavailability, in healthy human volunteers. Cancer Chemother. Pharmacol. 2012, 69, 65–70. [Google Scholar] [CrossRef]
- Nakagawa, Y.; Mukai, S.; Yamada, S.; Matsuoka, M.; Tarumi, E.; Hashimoto, T.; Tamura, C.; Imaizumi, A.; Nishihira, J.; Nakamura, T. Short-term effects of highly-bioavailable curcumin for treating knee osteoarthritis: A randomized, double-blind, placebo-controlled prospective study. J. Orthop. Sci. 2014, 19, 933–939. [Google Scholar] [CrossRef]
- Kakkar, V.; Kaur, I.P. Evaluating potential of curcumin loaded solid lipid nanoparticles in aluminium induced behavioural, biochemical and histopathological alterations in mice brain. Food Chem. Toxicol. 2011, 49, 2906–2913. [Google Scholar] [CrossRef]
- Kakkar, V.; Muppu, S.K.; Chopra, K.; Kaur, I.P. Curcumin loaded solid lipid nanoparticles: An efficient formulation approach for cerebral ischemic reperfusion injury in rats. Eur. J. Pharm. Biopharm. 2013, 85, 339–345. [Google Scholar] [CrossRef]
- Zanotto-Filho, A.; Coradini, K.; Braganhol, E.; Schröder, R.; de Oliveira, C.M.; Simões-Pires, A.; Battastini, A.M.O.; Pohlmann, A.R.; Guterres, S.S.; Forcelini, C.M.; et al. Curcumin-loaded lipid-core nanocapsules as a strategy to improve pharmacological efficacy of curcumin in glioma treatment. Eur. J. Pharm. Biopharm. 2013, 83, 156–167. [Google Scholar] [CrossRef]
- Hagl, S.; Kocher, A.; Schiborr, C.; Kolesova, N.; Frank, J.; Eckert, G.P. Curcumin micelles improve mitochondrial function in neuronal PC12 cells and brains of NMRI mice—Impact on bioavailability. Neurochem. Int. 2015, 89, 234–242. [Google Scholar] [CrossRef]
- Nayak, A.P.; Tiyaboonchai, W.; Patankar, S.; Madhusudhan, B.; Souto, E.B. Curcuminoids-loaded lipid nanoparticles: Novel approach towards malaria treatment. Colloids Surf. B Biointerfaces 2010, 81, 263–273. [Google Scholar] [CrossRef]
- Aditya, N.P.; Chimote, G.; Gunalan, K.; Banerjee, R.; Patankar, S.; Madhusudhan, B. Curcuminoids-loaded liposomes in combination with arteether protects against Plasmodium berghei infection in mice. Exp. Parasitol. 2012, 131, 292–299. [Google Scholar] [CrossRef]
- Bhatia, M.; Urolagin, S.S.; Pentyala, K.B.; Urolagin, S.B.; KB, M.; Bhoi, S. Novel Therapeutic Approach for the Treatment of Periodontitis by Curcumin. J. Clin. Diagn. Res. 2014, 8, ZC65–ZC69. [Google Scholar] [CrossRef]
- Manca, M.L.; Castangia, I.; Zaru, M.; Nácher, A.; Valenti, D.; Fernàndez-Busquets, X.; Fadda, A.M.; Manconi, M. Development of curcumin loaded sodium hyaluronate immobilized vesicles (hyalurosomes) and their potential on skin inflammation and wound restoring. Biomaterials 2015, 71, 100–109. [Google Scholar] [CrossRef]
- Karri, V.V.S.R.; Kuppusamy, G.; Talluri, S.V.; Mannemala, S.S.; Kollipara, R.; Wadhwani, A.D.; Mulukutla, S.; Raju, K.R.S.; Malayandi, R. Curcumin loaded chitosan nanoparticles impregnated into collagen-alginate scaffolds for diabetic wound healing. Int. J. Boil. Macromol. 2016, 93, 1519–1529. [Google Scholar] [CrossRef]
- Castangia, I.; Nácher, A.; Caddeo, C.; Valenti, D.; Fadda, A.M.; Díez-Sales, O.; Ruiz-Saurí, A.; Manconi, M. Fabrication of quercetin and curcumin bionanovesicles for the prevention and rapid regeneration of full-thickness skin defects on mice. Acta Biomater. 2014, 10, 1292–1300. [Google Scholar] [CrossRef]
- Gong, C.; Wu, Q.; Wang, Y.; Zhang, D.; Luo, F.; Zhao, X.; Wei, Y.; Qian, Z. A biodegradable hydrogel system containing curcumin encapsulated in micelles for cutaneous wound healing. Biomaterials 2013, 34, 6377–6387. [Google Scholar] [CrossRef]
- Ranjbar-Mohammadi, M.; Rabbani, S.; Bahrami, S.H.; Joghataei, M.T.; Moayer, F. Antibacterial performance and in vivo diabetic wound healing of curcumin loaded gum tragacanth/poly(ε-caprolactone) electrospun nanofibers. Mater. Sci. Eng. C 2016, 69, 1183–1191. [Google Scholar] [CrossRef]
- Gottumukkala, S.N.V.S.; Sudarshan, S.; Mantena, S.R. Comparative evaluation of the efficacy of two controlled release devices: Chlorhexidine chips and indigenous curcumin based collagen as local drug delivery systems. Contemp. Clin. Dent. 2014, 5, 175–181. [Google Scholar] [CrossRef]
- Yulianto, M.; Paramita, V.; Hartati, I.; Amalia, R. Response Surface Methodology of Pressurized Liquid Water Extraction of Curcumin From Curcuma Domestica Val. Rasayan J. Chem. 2018, 11, 1564–1571. [Google Scholar] [CrossRef]
- Pillai, G.K.G.; Bharate, S.S.; Awasthi, A.; Verma, R.; Mishra, G.; Singh, A.T.; Jaggi, M.; Mithal, A.; Vishwakarma, R.A. Antidiabetic potential of polyherbal formulation DB14201: Preclinical development, safety and efficacy studies. J. Ethnopharmacol. 2017, 197, 218–230. [Google Scholar] [CrossRef]
- Dandekar, D.V.; Gaikar, V.G. Microwave assisted extraction of curcuminoids from Curcuma longa. Sep. Sci. Technol. 2002, 37, 2669–2690. [Google Scholar] [CrossRef]
- Huang, Y.; Adeleye, A.S.; Zhao, L.; Minakova, A.S.; Anumol, T.; Keller, A.A. Antioxidant response of cucumber (Cucumis sativus) exposed to nano copper pesticide: Quantitative determination via LC-MS/MS. Food Chem. 2019, 270, 47–52. [Google Scholar] [CrossRef]
- Reolon, J.; Brustolin, M.; Haas, S.E.; Bender, E.A.; Malesuik, M.D.; Colomé, L.M. Development and validation of high-performance liquid chromatography method for simultaneous determination of acyclovir and curcumin in polymeric microparticles. J. Appl. Pharm. Sci. 2018, 8, 136–141. [Google Scholar]
- Peram, M.R.; Jalalpure, S.S.; Joshi, S.A.; Palkar, M.B.; Diwan, P.V. Single Robust RP-HPLC Analytical Method for Quantification of Curcuminoids in Commercial Turmeric Products, Ayurvedic Medicines, and Nanovesicular Systems. J. Liq. Chromatogr. Relat. Technol. 2017, 40, 487–498. [Google Scholar] [CrossRef]
- Ahmad, N.; Ahmad, R.; Naqvi, A.A.; Alam, M.A.; Ashafaq, M.; Iqbal, Z.; Ahmad, F.J. Isolation, Characterization and Quantification of Curcuminoids and Their Comparative Effects in Cerebral Ischemia. J. Liq. Chromatogr. Relat. Technol. 2017, 40, 133–146. [Google Scholar] [CrossRef]
- Mahale, J.; Singh, R.; Howells, L.M.; Britton, R.G.; Khan, S.M.; Brown, K. Detection of Plasma Curcuminoids from Dietary Intake of Turmeric-Containing Food in Human Volunteers. Mol. Nutr. Food Res. 2018, 62, 1800267. [Google Scholar] [CrossRef]
- Na Bhuket, P.R.; Niwattisaiwong, N.; Limpikirati, P.; Khemawoot, P.; Towiwat, P.; Ongpipattanakul, B.; Rojsitthisak, P. Simultaneous determination of curcumin diethyl disuccinate and its active metabolite curcumin in rat plasma by LC–MS/MS: Application of esterase inhibitors in the stabilization of an ester-containing prodrug. J. Chromatogr. B 2016, 1033, 301–310. [Google Scholar] [CrossRef]
- Ahmad, N.; Ahmad, R.; Ahmad, F.J. Stressed Kinetics and Pharmacokinetics of Curcumin Nanoemulsion Using Validated Ultrahigh-Performance Liquid Chromatography—Synapt Mass Spectrometry (UPLC—MS/MS-ESI-Q-TOF). Iran. J. Sci. Technol. Trans. A Sci. 2016, 40, 109–123. [Google Scholar] [CrossRef]
- Ma, W.; Wang, J.; Guo, Q.; Tu, P. Simultaneous determination of doxorubicin and curcumin in rat plasma by LC–MS/MS and its application to pharmacokinetic study. J. Pharm. Biomed. Anal. 2015, 111, 215–221. [Google Scholar] [CrossRef]
- Cao, Y.; Xu, R.X.; Liu, Z. A high-throughput quantification method of curcuminoids and curcumin metabolites in human plasma via high-performance liquid chromatography/tandem mass spectrometry. J. Chromatogr. B 2014, 949, 70–78. [Google Scholar] [CrossRef]
- Shen, Y.; Han, C.; Chen, X.; Hou, X.; Long, Z. Simultaneous determination of three Curcuminoids in Curcuma wenyujin Y.H.chen et C.Ling. by liquid chromatography–tandem mass spectrometry combined with pressurized liquid extraction. J. Pharm. Biomed. Anal. 2013, 81, 146–150. [Google Scholar] [CrossRef]
- Khalil, N.M.; Nascimento, T.C.F.D.; Casa, D.M.; Dalmolin, L.F.; De Mattos, A.C.; Hoss, I.; Romano, M.A.; Mainardes, R.M. Pharmacokinetics of curcumin-loaded PLGA and PLGA–PEG blend nanoparticles after oral administration in rats. Colloids Surfaces B Biointerfaces 2013, 101, 353–360. [Google Scholar] [CrossRef]
- Li, R.; Qiao, X.; Li, Q.; He, R.; Ye, M.; Xiang, C.; Lin, X.; Guo, D. Metabolic and pharmacokinetic studies of curcumin, demethoxycurcumin and bisdemethoxycurcumin in mice tumor after intragastric administration of nanoparticle formulations by liquid chromatography coupled with tandem mass spectrometry. J. Chromatogr. B 2011, 879, 2751–2758. [Google Scholar] [CrossRef]
- Liu, A.; Lou, H.; Zhao, L.; Fan, P. Validated LC/MS/MS assay for curcumin and tetrahydrocurcumin in rat plasma and application to pharmacokinetic study of phospholipid complex of curcumin. J. Pharm. Biomed. Anal. 2006, 40, 720–727. [Google Scholar] [CrossRef]
| Disease/Curcumin Activity | Formulations | Clinical Trial/In Vivo | Outcome | Ref |
|---|---|---|---|---|
| Curcumin with a combination of hydrophilic carrier, cellulosic derivatives, and natural antioxidants | Randomized, double-blind, crossover human study in 12 healthy volunteers | Significantly increases curcuminoid appearance in the blood in comparison to unformulated standard curcumin. | [90] | |
| Solid tumor | Meriva® (Patented and commercialized); a complex of curcumin with phosphatidylcholine | Clinical trial (80 patients undergoing chemotherapy) | Suppression of systemic inflammation via reduction of inflammatory mediators and biomarkers (TNF-α, CGRP, substance P, MCP-1, hs-CRP, and IL-6) | [103] |
| Diabetes | Meriva® | 38 patients | Significant improvement in the venoarteriolar response and a decrease in the peripheral oedema | [105] |
| Osteoarthritis | Meriva® | Clinical trial (100 patients) | Improvement of both the clinical and biochemical endpoints | [106] |
| Alzheimer’s | CUR loaded p(PEG-PLA) micelles | Tg2576 mice | Improved bioavailability in brain, and significant improvements in working and cue memory | [108] |
| Central serous chorioretinopathy | Meriva® | Clinical trial (12 patients) | Reduction in neuroretinal or retinal pigment epithelium detachment | [109] |
| Osteoarthritis | Meriva® | Clinical trial (50 patients) | Clinically effective in osteoarthritis treatment and management, while treatment costs were reduced significantly | [110] |
| Diabetes | Meriva® | 25 patients | Decrease in skin flux and edema | [111] |
| Solid tumor | Meriva® | Clinical trial (160 patients undergoing chemo- and radiotherapy) | Signs of reduced side effects of cancer chemo- and radiotherapy treatment which are attributed to an anti-oxidant and anti-inflammatory activity of curcumin | [112] |
| Peripheral neuropathy | Lipicur (a mixture of lipoic acid, curcumin phytosome and piperine) | Clinical trial (135 patients) | Reduction in neuropathic pain and usage of the drug significantly. | [113] |
| THERACURMIN (Nano-particle colloidal dispersion,) | Male Sprague-Dawley rats and 7 healthy human volunteers | Improved bioavailability than turmeric powder; 40-fold in rats and 27-fold in human | [114] | |
| THERACURMIN | 6 healthy human volunteers | Improved bioavailability | [115] | |
| Osteoarthritis | THERACURMIN | 50 patients with knee osteoarthritis | Significantly effective in decreasing pain and NSAID necessity without any major side effects | [116] |
| Reversing neuronal damage | Solid lipid nanoparticles | In vivo (male Lacca mice) | Significantly reduced the AlCl3 related neurotoxicity | [117] |
| Cerebral ischemia | Solid lipid nanoparticles | Male Wistar rats | Showed significant effect against cerebral ischemia | [118] |
| Antiglioma activity | Curcumin-loaded lipid-core nanocapsules (C-LNCs) | Male Wistar rats | Decreased the tumor size and malignance and prolonged animal survival | [119] |
| Bioavailability | Curcumin micelles | Female NMRI mice | 10–40- Folds increase in bioavailability in plasma and brain of mice | [120] |
| Antimalarial activity | Curcuminoids loaded lipid nanoparticles | Albino mice | Twofold improvement in antimalarial activity | [121] |
| Antimalarial activity | curcuminoids loaded liposomes | Albino mice | Showed lower parasitemia and higher survival than the control group | [122] |
| Periodontitis | Curcumin gel | 25 patients | Significant reduction in periopathogens | [123] |
| Wound healing | Curcumin-loaded hyalurosomes | Female CD-1 mice | Reduced inflammation and injuries, diminishing oedema formation, and myeloperoxidase activity | [124] |
| Diabetic wound healing | CUR-CSNPs impregnation into collagen scaffold | Adult male Wistar rats | accelerated the cutaneous wound healing by decreasing the inflammation | [125] |
| Wound healing | Cur- polymer micelle loaded thermosensitive hydrogel | Male Sprague-Dawley (SD) albino rats | Enhanced the cutaneous wound healing process | [127] |
| Diabetic wound healing | Curcumin-loaded nanofibers | Adult male Sprague- Dawley rats | increasing the collagen content in treating diabetic wounds and effectively promotes healing of such wounds in the early stages | [128] |
| Periodontitis | curcumin collagen sponge | 60 patients | Significant reduction in all the clinical and microbiological parameters | [129] |
| Matrix | Pretreatment/Extraction Approach | Procedure | Recovery % | Ref |
|---|---|---|---|---|
| Biological Samples | ||||
| Human plasma | Protein precipitation in methanol | 10 μL of IS mix was added to plasma, vortex-mixed for 30 s. 800 μL of methanol with 0.1% formic acid was added for protein precipitation. The resulting solution was vortex-mixed, centrifuged and the supernatant was dried under nitrogen. The residue was reconstituted in methanol: ammonium formate (1:1). | 72–84% | [25] |
| Rat plasma | Acetonitrile protein precipitation coupled with size-exclusion chromatography | 100 μL of Plasma samples were spiked with CUR-d6 IS and mixed with 300 μL of cold acetonitrile and vortex mixed for 30 s. The resulting mixture was centrifuged, and 300 μL of supernatant was transferred to an OMEGA NANOSEP 10K size exclusion tubes, centrifuged, and transferred the supernatant into LC-MS autosampler vial. | 97–109% | [26] |
| Rat plasma | Methyl-t-butyl ether extraction | 100 μL of plasma samples were taken in 1.5 mL centrifuged tube and added 10 μL of IS and 400 μL of methyl tert-butyl ether. The resulting solution was vortex-mixed for 3 min to extract curcumin. After extraction, 300 μL of upper methyl tert-butyl ether was transferred into another tube and dried under nitrogen and reconstituted the residue into 100 μL of methanol containing 0.1% formic acid. | 82.2–115.5% | [27] |
| mouse plasma and brain tissue | Mouse plasma and brain tissue; an addition of sodium hydroxide followed by liquid-liquid extraction | 10 μL of mouse plasma (or whole brain homogenate) was spiked with 10 μL of IS and 10 μL of 0.5 M sodium hydroxide for better curcumin extraction. The solution was vortex mixed for 1 min and added 250 μL of ethyl acetate for liquid-liquid extraction. After centrifugation, the organic layer was separated and dried under vacuum, and the residue was reconstituted in 20 μL of acetonitrile and 0.01% formic acid (50:50). | Plasma: 67.0–88.4% Brain tissue: 45.8–74.6% | [28] |
| Human plasma | Ethyl acetate liquid-liquid extraction | 3 mL of plasma samples were mixed with 10 μL of IS along with a phosphate buffer solution, followed by extracting with 3 mL of ethyl acetate. The upper organic layer was separated and transferred into a glass tube. The extraction procedure was repeated for two more times. All the supernatants were pooled and dried under nitrogen gas and reconstituted into 2 mL of methanol. | _ | [35] |
| Plant | ||||
| Powdered rhizome | Microwave-assisted extraction | 20 g of dry C. longa powder (with and without soaking solvent) was irradiated for a pre-defined time, followed by extraction with ethanol or acetone with different microwave power. | 68.6% (w/o soaking) 90.5% (with soaking) | [13] |
| Powdered rhizome | Powdered Turmeric rhizomes, reflux in methanol | Powdered rhizomes were refluxed with methanol for 2 h at 70 C, followed by separation of aliquots, filtered, dried and resuspended in methanol for analysis | 98.60% | [29] |
| Powdered rhizome | Pressurized liquid extraction | The optimized extractions were obtained with ethanol as extraction solvent at 100°C, pressure 1500 psi; extraction time 5 min and flush vol 60%. | 93–105% | [32] |
| Powdered rhizome | Extraction using an ultrasonic bath | Powdered rhizomes of turmeric were extracted with 5 mL of 50, 80 and 100% of methanol. All the extracts were combined, centrifuged, and filtered for analysis. | _ | [36] |
| Powdered rhizome | Dissolved acetonitrile | Turmeric powder; dissolved in 1 mg/mL in acetonitrile | _ | [37] |
| Curry powder | Ultrasonication in acetonitrile-ethanol | Samples were mixed with acetonitrile: ethanol (1:2 v/v) in a centrifuge tube and shaken for 30 s. The mixture was ultrasonicated for 5 min. The supernatant was collected and used as a prepared sample solution for the analysis. | 82.20% | [38] |
| Powdered rhizome | Pressurized liquid water extraction | Optimum extraction of the curcumin pressurized liquid water extraction was obtained at a temperature of 156.8 °C with an extraction time of 46.8 min using the solid-liquid ratio as 1:10 at a fixed 2 bar pressure. Temperature plays a vital role in extraction optimization. | _ | [130] |
| Formulation | ||||
| Tiantai No. 1 pills- contains Curcuma Longa Rhizoma and other herbal medicines | Extraction with methanol and diluted HCl | Powdered Tiantai extracted by ultrasonication with an addition of 50 mL methanol and diluted HCl. Extracts were further diluted with methanol, filtered and used for analysis | 96.85±4.2% | [31] |
| Tablet | Sonication | Powdered tablet; methanol extraction by sonication | 99.8 ± 4.4% | [33] |
| Nanoparticles | Extracted with Dichloromethane and precipitated polymer by adding methanol | The dried nanoparticles were diluted in 1 mL dichloromethane and followed by the polymer precipitation by adding 1 mL methanol. The solution was filtered, from which 1 mL of solution taken and diluted in dichloromethane: methanol 1:1 (v/v) to adjust the absorbance | 77–98% | [39] |
| Powdered rhizome in an herbal mix | 3 stage extraction using water at high temperatures | Raw herb premix was extracted in 3 stages. In the 1st stage of extraction, the raw material was mixed with water and kept for 3 h at 80–90 °C. It was then concentrated using a rotary vacuum dryer. The resulting solid was pulverized and sieved. The 2nd and 3rd stage of extractions were carried out using water. The resulting mixture was kept for 2 h at 70–80 °C, then the solution was concentrated using a rotary vacuum dryer. The final extract was prepared by mixing 1 part of the first extraction solid and 0.5 part of each 2nd and 3rd extraction solids extraction in equal proportion. | _ | [131] |
| Analytical Method | Research Objectives/Title | Matrix and Sample Preparation Method | Result | Ref |
|---|---|---|---|---|
| Magnetic molecularly imprinted technique and UV-Vis | A simple and rapid method for monitoring curcumin in food samples using a magnetic molecularly imprinted technique combined with UV–Vis. | Magnetic molecularly imprinted polymers of curcumin, trihydroxymethylpropyl trimethylacrylate, and polyvinylpyrrolidone | The recovery was between 79% and 89% with the limits of detection and quantification of 1.31 and 4.38 µg/mL, respectively. | [38] |
| UV-Vis | To develop Ultraviolet-visible spectroscopy validated method for the quantitative determination of curcumin encapsulated in poly (L-lactic acid) nanoparticles | Curcumin encapsulated in poly (L-lactic acid) nanoparticles | A UV-Vis spectroscopy method was developed to determine the concentration of curcumin on biodegradable nanoparticles and validated for linearity and inter-day, intra-day, inter-laboratory and inter-analyst precision, the limit of detection and quantification were determined. | [39] |
| FT-IR | To evaluate adulteration in turmeric | Turmeric powder | FT-IR was able to detect metanil yellow at 5% concentration, and FT-Raman was able to detect at 1% concentration | [41] |
| FT-Raman | To detect Sudan-I or metanil yellow in curry powder | Organic curry powders | The results indicated that the 1064 nm dispersive Raman system could be potentially used as a non-destructive tool for detection of chemical contaminants in a complex food matrix. | [42] |
| FT-NIR | Simultaneous quantification of curcuminoids | Turmeric powder | Partial least square regression (PLS-R) results showed a strong correlation with HPLC analysis | [43] |
| FT-NIR | To evaluate curcuminoids in turmeric powder using NIR | Crude turmeric samples | The results showed a high correlation coefficient (R2 > 0.93) and low standard error of cross-validation. | [44] |
| FT-IR, FT-Raman, and X-ray Diffraction | To compare different methods of curcumin complexation with β-cyclodextrin and to evaluate the formation of the complexes | Curcumin β-cyclodextrin complex | This complex exhibited better color stability to pH, temperature than pure colorant and had great sensorial acceptance | [45] |
| 1H NMR | A rapid, accurate, and sensitive 1H NMR method for the quantitation of curcumin isolated from turmeric extract and compare the results with a validated with LC-MS/MS method | Curcumin samples were dissolved in DMSO-d6 and added 1,3,5-trimethoxy benzene was added as an internal standard | The correlation coefficients 0.998 for 1H NMR was and 0.995 for LC-MS/MS method in the calibration range. The measurement uncertainty for curcumin via 1H NMR was 5.80% as compared to 7.38% by LC-MS/MS method. | [46] |
| HPTLC | To develop simple and precise HPTLC methods for the simultaneous estimation of two anti-inflammatory drugs (curcumin and galangin) | Polyherbal capsule | The HPTLC method was developed and validated for linearity, accuracy, precision, detection and quantitation limits, robustness and specificity were also determined. The LOD for CUR was 18.31 ng/spot. | [47] |
| HPTLC | A simple and sensitive HPTLC method to develop for the simultaneous determination of salicin, curcumin, and gallic acid in herbal pain relief tablet. | Powdered tablet | The Rf values were determined as 0.16, 0.71 and 0.61 respectively for salicin, curcumin and gallic acid with the linearity ranges; salicin: 2.0–16.0μg; curcumin: 0.20–2.5 μg; gallic acid: 0.3–3.0 μg | [33] |
| HPLC | Isolation and identification of curcuminoids from the mother liquor by reporting the HPLC separation conditions | Commercial samples of turmeric | HPLC analysis was achieved for separation of curcumin, demethoxycurcumin, and bisdemethoxycurcumin on a C18 column using three solvents, methanol, 2% AcOH, and acetonitrile, with detection at 425 nm. | [40] |
| UV, FT-IR, 1H- NMR, and HPLC analysis | UV, FT-IR, 1H NMR, and HPLC were applied to construct a metabolic fingerprint to evaluate Turmeric quality. | Powdered samples were initially extracted with hexane, centrifuged, and discarded the supernatant. The residue was extracted again with methanol. | PCA analysis of the score plot of UV and HPLC analysis showed the same discriminatory patterns based on the curcuminoids content. FT-IR failed to discriminate between the same species, and 1H-NMR showed variability between samples in the oils/fatty acids region. | [48] |
| HPLC | To address the modifications suggested by the ERP for turmeric method optimization by using factorial studies to guide the optimization. | Raw materials and finished products containing turmeric roots | A single-laboratory validated method per the AOAC International guidelines was developed for curcuminoids quantification. Column temperature and extraction solvent were determined as the two most significant factors impacting the quantitation of curcuminoids. Optimum extraction was achieved with 100% MeOH, and the best separation was achieved at 55 °C column temperature. | [49] |
| HPLC | Developed and validated an HPLC based analytical methodology for simultaneous determination of acyclovir and curcumin within microparticles. | Samples of microparticles were extracted with 20:80 of DMSO and acetonitrile | The linear range for curcumin was determined as 0.5–20 µg/mL. Detection and quantification limits for curcumin were 91.61 ng. mL−1 and 128.71 ng/mL with almost complete recovery. | [134] |
| HPLC | Quantification of curcuminoids in commercial turmeric products, Ayurvedic medicines, and nanovesicular systems. | Powdered samples were extracted with methanol | The inter and the intraday relative standard deviation was < 2% and with almost complete 100% recovery. Limit of detection and quantification were determined to be 7.4 and 24.7 ng/mL. | [135] |
| Purpose of Quantification/Title | Matrix and Sample Preparation Method | Instrumentation and Separation Column | MS Detection Instrumentation | LOD (ng/mL) | LLOQ (ng/mL) | Ref |
|---|---|---|---|---|---|---|
| Pharmacokinetic studies of curcumin in a natural turmeric matrix with two other curcumin formulations | Human plasma; Ethyl acetate extraction | Acquity High Performance LC (Waters Corporation); AQUITY BEH C18 column (2.1 × 50 mm, 1.7 μm) | Waters Xevo TQD; +ESI | 1 | 10 | [14] |
| Determination of curcumin and its metabolites simultaneously in phase II clinical trial | Human plasma; methanol protein precipitation | Shimadzu Prominence UFLC; Waters XTerra MS C18 column (2.1 mm × 50 mm, 3.5 μm) | AB Sciex API 3200 turbo-ion-spray triple quadrupole tandem mass spectrometer; -ESI | 2.5 | [25] | |
| Determination of curcumin in rat plasma for pharmacokinetics | Rat plasma; Acetonitrile protein precipitation coupled with size exclusion chromatography | Thermo Finnigan Surveyor HPLC system; Agilent Zorbax Eclipse XDB C18 column (3.5 μm, 4.6 × 50 mm) | Thermo Finnigan LTQ mass spectrometer (ITMS/MS/MS) +ESI | 0.1 | 1.0 | [26] |
| Quantification of curcumin in vivo | Rat plasma; methyl-t-butyl ether extraction | Thermo Accela pump using an Agilent Poroshell SB-C18 (4.6m m× 150m m, 2.7 μm) column | Thermo TSQ Quantum; +ESI | 0.5 | 1 | [27] |
| simultaneous determination of curcumin in mouse plasma and brain tissue | Mouse plasma; sodium hydroxide was added to plasma, followed by liquid-liquid extraction with ethyl acetate. Brain tissue; to brain homogenate sodium hydroxide was added, followed by liquid-liquid extraction with ethyl acetate | Agilent LC 1100; an analytical Sepax BR-C18 (5 µm, 120 Å 1.0 × 100 mm) column | Agilent 6490 triple quadrupole MS; +ESI | 2.5 | [28] | |
| To determine curcuminoids in Curcuma longa Linn. | Powdered rhizomes; refluxed in methanol | Waters ACQUITY UPLC; BEH C8 column (100.0 mm × 2.1 mm; 1.7 µm) | Waters Synapt Q-TOF Premier; -ve ionization | 0.32 | 1 | [29] |
| Simultaneous quantification of free curcuminoids and their metabolites in equine plasma | Equine plasma; acetonitrile protein precipitation | Shimadzu Prominence UFLC system; Waters XBridge BEH C18 column, 100 mm × 2.1 mm i.d., 2.5 um | AB Sciex QTRAP 4500 tandem mass spectrometer; ESI | 0.5 | [30] | |
| Simultaneous determination of 21 bioactive components in herbal medicine and rat plasma | Medicine; 2% HCl (v/v) and methanol extraction. Rat plasma; Added 2% HCl, followed by methanol extraction | Agilent 1290 UPLC; Agilent Zorbax Eclipse Plus C18 column (4.6 mm × 150 mm, 3.5 μm) | Agilent 6410 triple quadrupole mass spectrometer | 0.3 | 1.3 | [31] |
| Method development and validation to study the pharmacokinetics of curcuminoids and curcumin metabolites in human blood plasma after an oral administration of bioavailable curcumin—Cureit™ | Human plasma- ethyl acetate liquid-liquid extractions | Waters ACQUITY UPLC I; ACQUITY UPLC BEH C-18 (2.1 × 50 mm; 1.7 µm) column | Waters Xevo G2S Q-TOF; -ESI | 1 | [35] | |
| Identification and characterization of curcuminoids in turmeric | Powdered rhizomes of turmeric were extracted with 50, 80 and 100% of methanol | Shimadzu UHPLC; Welch Ultimate UHPLC C18 column (100mm × 2.1mm, 1.8 µm) | AB Sciex Triple TOF 5600; ESI | [36] | ||
| Quantitating curcumin in food condiments and dietary supplements | turmeric powder, curry powder, and yellow mustard; 1 mg/mL in acetonitrile | MALDI-TOF-MS system (model Autoflex III Smartbeam) equipped with a 355 nm Nd: YAG laser from Bruker Daltonics (Billerica, MA, USA); | 1000 | [37] | ||
| Analysis of different innovative formulations of curcumin to assess relative oral bioavailability in human subjects | Human plasma; Spiked with 100 μL solution containing 1000 U of β-glucuronidase/sulfatase (EC 3.2.1.31) from Helix pomatia (Sigma, St. Louis, MO) in 0.1 M phosphate buffer (pH 6.86) and 50 μL of methanol to liberate free curcumin | Agilent 1290 HPLC; Phenomenex Kinetex XB-C18 100 Å column (2.1 × 50 mm, 2.6 micron) attached to a security guard ultra, C18, 2.1 mm pre-column | HPLC-MSMS consisted of an Agilent 1290 HPLC system with an Agilent 6460 tandem mass spectrometer; +ESI | 0.5 | [93] | |
| Determine the bioavailability of curcumin in the central nervous system of mice after oral delivery of nano-curcumin | Mice plasma, brain, and spinal cord; liquid-liquid extraction with ethyl acetate | Shimadzu HPLC system; Thermo Scientific Hypersil Gold C18 column (2.1 50 mm, 5 um). | Agilent, 6410 triple quad mass spectrometer; -APCI | 0.12 | [96] | |
| Identify and quantify mangiferin, berberine, kaempferol, and curcumin in a polyherbal formulation | A three-stage extraction as described in Table 2 | Shimadzu HPLC (LC-2010 CHT); Chromolith high resolution RP-18 end-capped; 50 × 4.6 mm column | Agilent 6410B triple quad LC-MS/MS; +ESI | 3 | 12.2 | [131] |
| Quantitative analysis of curcumin and other metabolites in plant tissues | Extraction with 80:20 methanol and water with 2% formic acid | Agilent 1260 UHPLC; Agilent ZORBAX StableBond 80 Å C18 (4.6 mm × 50 mm, 3.5 μm) column | Agilent 6470 triple quadrupole mass spectrometer; −ESI | 0.004 | 0.01 | [133] |
| Separation, characterization, and quantitation along with the comparative pharmacological effect of curcuminoids in cerebral ischemia | turmeric powder; soxhlet extraction with petroleum ether | Water ACQUITY UPLC; Waters ACQUITY UPLC column BEH C-18 (2.1 mm × 100 mm; 1.7 μm) | Waters Synapt mass spectrometry (Synapt MS), −ESI | 1 | [136] | |
| Detection of curcuminoids in human plasma | Human plasma was treated with 9:1 acetone/formic acid followed by treating with 0.1% acetic acid water/acetonitrile | Waters Alliance 2695; HyPurity C18 (2.1 × 150 mm, 3 μm) column connected to a HyPurity C18 (2.1 × 10 mm, 3 μm) guard cartridge | Micromass Quattro Platinum tandem quadrupole mass spectrometer; −ESI | 0.125 nM | 1 nM | [137] |
| Simultaneous determination of curcumin diethyl disuccinate and its active metabolite curcumin in rat plasma | Rat plasma; Acetonitrile protein precipitation | Eskpert UltraLC 100 system; Halo C8 column (4.6 × 50 mm, 2.7 um) | AB SCIEX QTRAP 6500; +ESI | 1 | [138] | |
| Estimation of Curcumin in rat brain homogenate and plasma | rat brain homogenate and plasma | Waters ACQUITY UPLC; BEH C18 column (2.1 mm × 100 mm; 1.7 µm) | Waters Synapt (UHPLC/ESI-QTOF-MS/MS) | 0.017 | 0.054 | [139] |
| Simultaneous quantification of curcumin in rat plasma after intravenous administration | rat plasma; protein precipitation with methanol | Shimadzu HPLC; Waters ACQUITY UPLC BEH C18 (100 mm × 2.1 mm, 1.7 um, | AB SCIEX QTRAP® 5500 tandem mass spectrometer; +ESI | 5 | [140] | |
| to quantify curcuminoids and metabolites simultaneously in human plasma. | Human plasma; samples diluted with PBS buffer followed by ethyl acetate liquid-liquid extraction | Shimadzu HPLC; BetaBasic-8 column (2.1 mm × 50 mm, 5 µm, Thermo Hypersil-Keystone) coupled with a BetaBasic-8 guard column (2.1 mm × 10 mm, 5 µm, Thermo Hypersil-Keystone) coupled with a guard column. | AB Sciex API-3000 mass spectrometer, −ESI | 1 | 2 | [141] |
| simultaneous identification and quantification of three Curcuminoids in a medicinal herb. | Medicinal herb; PLE- the sample was mixed with diatomaceous earth and loaded with 15 mL of methanol into the cell. A 10-min heating process was performed, with the temperature increased up to 100 °C and maintained at a pressure of 1500 psi | Agilent 1200 Series LC system; Waters XBridge TM C18 column (150 mm × 2.1 mm i.d., 3.5 µm) | AB Sciex API 4000 triple quad MS with turbo ion spray; +ESI | 0.03 | 0.08 | [142] |
| to quantify curcumin in rat plasma | Sodium hydroxide was added to rat plasma sample followed by liquid-liquid extraction with ethyl acetate | Waters Alliance; Phenomenex Luna C18(2) 100A column (250 mm × 4.6 mm, 5 µm). | Quattro Micro API–Waters hexapole mass spectrometer; +ESI | 0.5 | [143] | |
| To investigate the metabolism and pharmacokinetics of curcuminoids in mice tumor | plasma sample and tumor homogenate samples were extracted with acetonitrile | Finnigan Surveyor LC; Agilent Zorbax SB-C18 column (150 mm × 2.1 mm i.d., 3.5 µm) equipped with an Agilent Zorbax SB-C18 guard column (12.5 mm × 4.6 mm i.d., 5 µm). | Finnigan TSQ Quantum triple quadrupole mass spectrometer; −ESI | 0.02 | 2 | [144] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kotha, R.R.; Luthria, D.L. Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects. Molecules 2019, 24, 2930. https://doi.org/10.3390/molecules24162930
Kotha RR, Luthria DL. Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects. Molecules. 2019; 24(16):2930. https://doi.org/10.3390/molecules24162930
Chicago/Turabian StyleKotha, Raghavendhar R., and Devanand L. Luthria. 2019. "Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects" Molecules 24, no. 16: 2930. https://doi.org/10.3390/molecules24162930
APA StyleKotha, R. R., & Luthria, D. L. (2019). Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects. Molecules, 24(16), 2930. https://doi.org/10.3390/molecules24162930





