Cannabinoid Delivery Systems for Pain and Inflammation Treatment
Abstract
1. Introduction
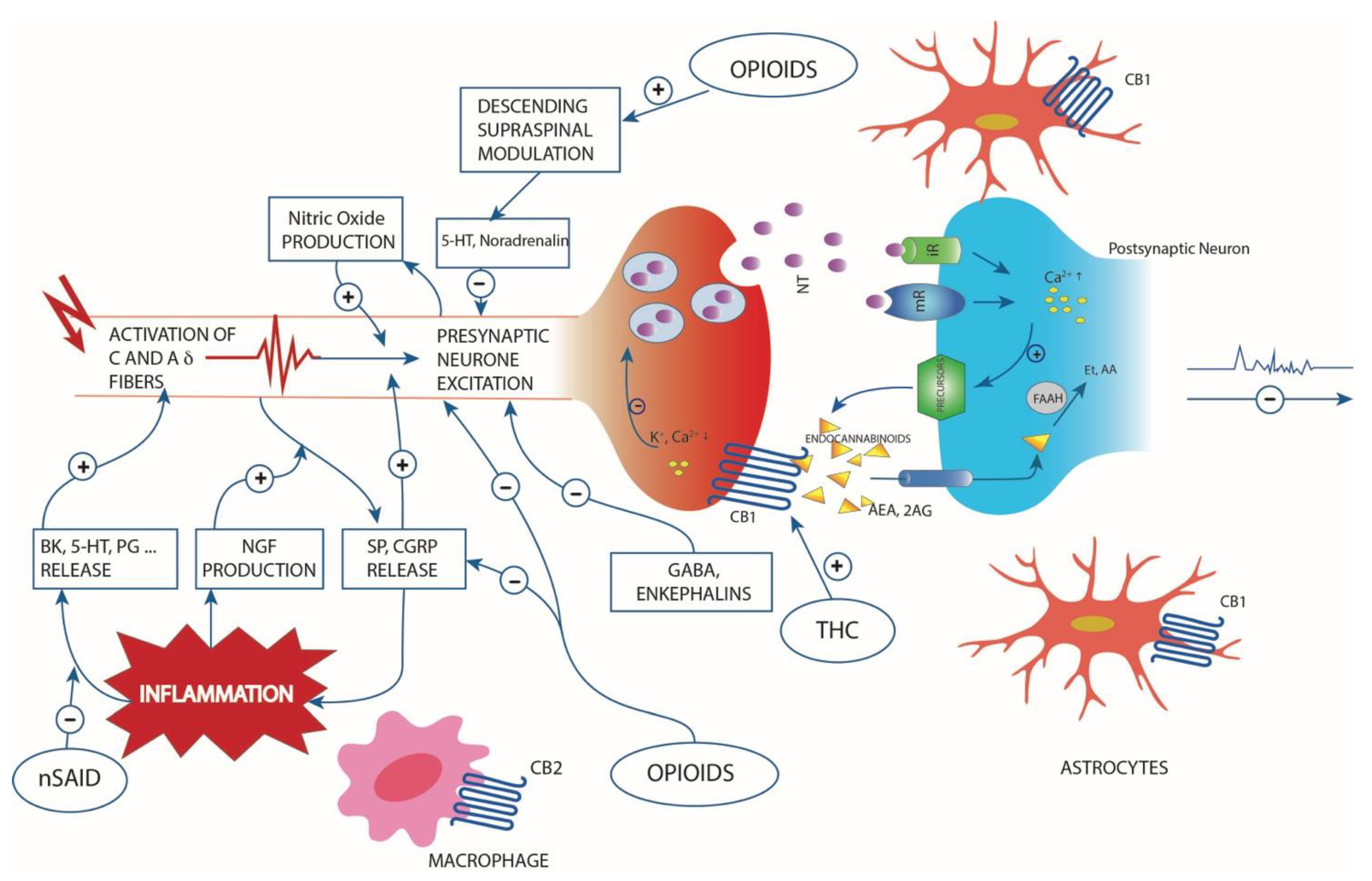
2. Role of Cannabinoids in Inflammation and Pain
3. Current Drug Dosage Forms and Novel Delivery Systems
3.1. Oral Route
3.2. Administration through Mucosa
3.3. Pulmonary Administration
3.4. Topical and Transdermal Route
3.5. Nano-Technological Approaches
3.5.1. Lipid Carriers
3.5.2. Polymeric Carriers
4. Critical Overview of Clinical Studies
5. Concluding Remarks
Funding
Acknowledgments
Conflicts of Interest
References
- Lewis, M.A.; Russo, E.B.; Smith, K.M. Pharmacological Foundations of Cannabis Chemovars. Planta Med. 2018, 84, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Gaoni, Y.; Mechoulam, R. Isolation, Structure, and Partial Synthesis of an Active Constituent of Hashish. J. Am. Chem. Soc. 1964, 86, 1646–1647. [Google Scholar] [CrossRef]
- ElSohly, M.A.; Slade, D. Chemical constituents of marijuana: The complex mixture of natural cannabinoids. Life Sci. 2005, 78, 539–548. [Google Scholar] [CrossRef] [PubMed]
- Matsuda, L.A.; Lolait, S.J.; Brownstein, M.J.; Young, A.C.; Bonner, T.I. Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature 1990, 346, 561–564. [Google Scholar] [CrossRef] [PubMed]
- Munro, S.; Thomas, K.L.; Abu-Shaar, M. Molecular characterization of a peripheral receptor for cannabinoids. Nature 1993, 365, 61–65. [Google Scholar] [CrossRef] [PubMed]
- Svíženská, I.; Dubový, P.; Šulcová, A. Cannabinoid receptors 1 and 2 (CB1 and CB2), their distribution, ligands and functional involvement in nervous system structures—A short review. Pharmacol. Biochem. Behav. 2008, 90, 501–511. [Google Scholar] [CrossRef] [PubMed]
- Di Marzo, V.; Bifulco, M.; De Petrocellis, L. The endocannabinoid system and its therapeutic exploitation. Nat. Rev. Drug Discov. 2004, 3, 771–784. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, S.; Kohsaka, H.; Takayasu, A.; Yokoyama, W.; Miyabe, C.; Miyabe, Y.; Harigai, M.; Miyasaka, N.; Nanki, T. Cannabinoid receptor 2 as a potential therapeutic target in rheumatoid arthritis. BMC Musculoskelet. Disord. 2014, 15, 275. [Google Scholar] [CrossRef] [PubMed]
- Turu, G.; Hunyady, L. Signal transduction of the CB1 cannabinoid receptor. J. Mol. Endocrinol. 2010, 44, 75–85. [Google Scholar] [CrossRef] [PubMed]
- McAllister, S.D.; Glass, M. CB1 and CB2 receptor-mediated signalling: A focus on endocannabinoids. Prostaglandins Leukot. Essent. Fatty Acids 2002, 66, 161–171. [Google Scholar] [CrossRef] [PubMed]
- Rossi, F.; Mancusi, S.; Bellini, G.; Roberti, D.; Punzo, F.; Vetrella, S.; Matarese, S.M.R.; Nobili, B.; Maione, S.; Perrotta, S. CNR2 functional variant (Q63R) influences childhood immune thrombocytopenic purpura. Haematologica 2011, 96, 1883–1885. [Google Scholar] [CrossRef] [PubMed]
- Piomelli, D.; Beltramo, M.; Giuffrida, A.; Stella, N. Endogenous cannabinoid signaling. Neurobiol. Dis. 1998, 5, 462–473. [Google Scholar] [CrossRef] [PubMed]
- Pisanti, S.; Malfitano, A.M.; Ciaglia, E.; Lamberti, A.; Ranieri, R.; Cuomo, G.; Abate, M.; Faggiana, G.; Proto, M.C.; Fiore, D.; et al. Cannabidiol: State of the art and new challenges for therapeutic applications. Pharmacol. Ther. 2017, 175, 133–150. [Google Scholar] [CrossRef] [PubMed]
- Appendino, G.; Taglialatela-Scafati, O. Cannabinoids: Chemistry and medicine. In Natural Products; Ramawat, K.G., Mérillon, J.M., Eds.; Springer: Berlin, Germany, 2013; pp. 3415–3435. [Google Scholar]
- Howlett, A.C.; Barth, F.; Bonner, T.I.; Cabral, G.; Casellas, P.; Devane, W.A.; Felder, C.C.; Herkenham, M.; Mackie, K.; Martin, B.R.; et al. International Union of Pharmacology. XXVII. Classification of cannabinoid receptors. Pharmacol. Rev. 2002, 54, 161–202. [Google Scholar] [CrossRef] [PubMed]
- Ligresti, A.; De Petrocellis, L.; Di Marzo, V. From phytocannabinoids to cannabinoid receptors and endocannabinoids: Pleiotropic physiological and pathological roles through complex pharmacology. Physiol. Rev. 2016, 96, 1593–1659. [Google Scholar] [CrossRef] [PubMed]
- Laprairie, R.B.; Bagher, A.M.; Kelly, M.E.M.; Denovan-Wright, E.M. Cannabidiol is a negative allosteric modulator of the cannabinoid CB1 receptor. Br. J. Pharmacol. 2015, 172, 4790–4805. [Google Scholar] [CrossRef] [PubMed]
- Russo, E.B.; Burnett, A.; Hall, B.; Parker, K.K. Agonistic Properties of Cannabidiol at 5-HT1a Receptors. Neurochem. Res. 2005, 30, 1037–1043. [Google Scholar] [CrossRef] [PubMed]
- Costa, B.; Giagnoni, G.; Franke, C.; Trovato, A.E.; Colleoni, M. Vanilloid TRPV1 receptor mediates the antihyperalgesic effect of the nonpsychoactive cannabinoid, cannabidiol, in a rat model of acute inflammation. Br. J. Pharmacol. 2004, 143, 247–250. [Google Scholar] [CrossRef] [PubMed]
- McPartland, J.M.; Duncan, M.; Di Marzo, V.; Pertwee, R.G. Are cannabidiol and Δ9-tetrahydrocannabivarin negative modulators of the endocannabinoid system? A systematic review. Br. J. Pharmacol. 2015, 172, 737–753. [Google Scholar] [CrossRef] [PubMed]
- Romero-Sandoval, E.A.; Kolano, A.L.; Alvarado-Vázquez, P.A. Cannabis and Cannabinoids for Chronic Pain. Curr. Rheumatol. Rep. 2017, 19. [Google Scholar] [CrossRef] [PubMed]
- Russo, E.; Guy, G.W. A tale of two cannabinoids: The therapeutic rationale for combining tetrahydrocannabinol and cannabidiol. Med. Hypotheses 2005, 66, 234–246. [Google Scholar] [CrossRef] [PubMed]
- Russo, E.B. Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br. J. Pharmacol. 2011, 163, 1344–1364. [Google Scholar] [CrossRef] [PubMed]
- Stucky, C.L.; Gold, M.S.; Zhang, X. Mechanisms of pain. Proc. Natl. Acad. Sci. USA 2001, 98, 11845–11846. [Google Scholar] [CrossRef] [PubMed]
- Pountos, I.; Georgouli, T.; Bird, H.; Giannoudis, P.V. Nonsteroidal anti-inflammatory drugs: Prostaglandins, indications, and side effects. Int. J. Interferon Cytokine Mediator Res. 2011, 3, 19–27. [Google Scholar] [CrossRef]
- Jensen, M.P.; Chodroff, M.J.; Dworkin, R.H. The impact of neuropathic pain on health-related quality of life: Review and implications. Neurology 2007, 68, 1178–1182. [Google Scholar] [CrossRef] [PubMed]
- Finnerup, N.B.; Sindrup, S.H.; Jensen, T.S. The evidence for pharmacological treatment of neuropathic pain. Pain 2010, 150, 573–581. [Google Scholar] [CrossRef] [PubMed]
- Finnerup, N.B.; Attal, N.; Haroutounian, S.; McNicol, E.; Baron, R.; Dworkin, R.H.; Gilron, I.; Haanpaa, M.; Hansson, P.; Jensen, T.S.; et al. Pharmacotherapy for neuropathic pain in adults: A systematic review and meta-analysis. Lancet Neurol. 2015, 14, 162–173. [Google Scholar] [CrossRef]
- Ohno-Shosaku, T.; Kano, M. Endocannabinoid-mediated retrograde modulation of synaptic transmission. Curr. Opin. Neurobiol. 2014, 29, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Malfait, A.M.; Gallily, R.; Sumariwalla, P.F.; Malik, A.S.; Andreakos, E.; Mechoulam, R.; Feldmann, M. The nonpsychoactive cannabis constituent cannabidiol is an oral anti-arthritic therapeutic in murine collagen-induced arthritis. Proc. Natl. Acad. Sci. USA 2000, 97, 9561–9566. [Google Scholar] [CrossRef] [PubMed]
- Akopian, A.N.; Ruparel, N.B.; Patwardhan, A.; Hargreaves, K.M. Cannabinoids desensitize capsaicin and mustard oil responses in sensory neurons via TRPA1 activation. J. Neurosci. 2008, 28, 1064–1075. [Google Scholar] [CrossRef] [PubMed]
- Schuelert, N.; McDougall, J.J. Cannabinoid-mediated antinociception is enhanced in rat osteoarthritic knees. Arthritis Rheum. 2008, 58, 145–153. [Google Scholar] [CrossRef] [PubMed]
- Sánchez Robles, E.M.; Bagües Arias, A.; Martín Fontelles, M.I. Cannabinoids and muscular pain. Effectiveness of the local administration in rat. Eur. J. Pain 2012, 16, 1116–1127. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.; Hitchcock, S.A. Targeting cannabinoid agonists for inflammatory and neuropathic pain. Expert Opin. Investig. Drugs 2007, 16, 951–965. [Google Scholar] [CrossRef] [PubMed]
- Correa, F.; Docagne, F.; Mestre, L.; Clemente, D.; Hernangómez, M.; Loría, F.; Guaza, C. A role for CB2 receptors in anandamide signalling pathways involved in the regulation of IL-12 and IL-23 in microglial cells. Biochem. Pharmacol. 2009, 77, 86–100. [Google Scholar] [CrossRef] [PubMed]
- Shang, Y.; Tang, Y. The central cannabinoid receptor type-2 (CB2) and chronic pain. Int. J. Neurosci. 2017, 127, 812–823. [Google Scholar] [CrossRef] [PubMed]
- Richardson, D.; Pearson, R.G.; Kurian, N.; Latif, M.L.; Garle, M.J.; Barrett, D.A.; Kendall, D.A.; Scammell, B.E.; Reeve, A.J.; Chapman, V. Characterisation of the cannabinoid receptor system in synovial tissue and fluid in patients with osteoarthritis and rheumatoid arthritis. Arthritis Res. Ther. 2008, 10. [Google Scholar] [CrossRef] [PubMed]
- De Vries, M.; Van Rijckevorsel, D.C.; Wilder-Smith, O.H.; Van Goor, H. Dronabinol and chronic pain: Importance of mechanistic considerations. Expert Opin. Pharmacother. 2014, 15, 1525–1534. [Google Scholar] [CrossRef] [PubMed]
- Jensen, B.; Chen, J.; Furnish, T.; Wallace, M. Medical marijuana and chronic pain: A review of basic science and clinical evidence. Curr. Pain Headache Rep. 2015, 19. [Google Scholar] [CrossRef] [PubMed]
- Lötsch, J.; Weyer-Menkhoff, I.; Tegeder, I. Current evidence of cannabinoid-based analgesia obtained in preclinical and human experimental settings. Eur. J. Pain 2018, 22, 471–484. [Google Scholar] [CrossRef] [PubMed]
- Guindon, J.; Hohmann, A.G. The endocannabinoid system and pain. CNS Neurol. Disord. Drug Targets 2009, 8, 403–421. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.C.; Ploner, M.; Wiech, K.; Bingel, U.; Wanigasekera, V.; Brooks, J.; Menon, D.K.; Tracey, I. Amygdala activity contributes to the dissociative effect of cannabis on pain perception. Pain 2013, 154, 124–134. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Echeverry, S.; Lim, T.K.; Lee, S.H.; Shi, X.Q.; Huang, H. Can modulating inflammatory response be a good strategy to treat neuropathic pain? Curr. Pharm. Des. 2015, 21, 831–839. [Google Scholar] [CrossRef] [PubMed]
- De Moulin, D.; Boulanger, A.; Clark, A.J.; Clarke, H.; Dao, T.; Finley, G.A.; Furlan, A.; Gilron, I.; Gordon, A.; Morley-Forster, P.K.; et al. Pharmacological management of chronic neuropathic pain: Revised consensus statement from the Canadian Pain Society. Pain Res. Manag. 2014, 19, 328–335. [Google Scholar] [CrossRef]
- Baron, E.P.; Lucas, P.; Eades, J.; Hogue, O. Patterns of medicinal cannabis use, strain analysis, and substitution effect among patients with migraine, headache, arthritis, and chronic pain in a medicinal cannabis cohort. J. Headache Pain 2018, 19. [Google Scholar] [CrossRef] [PubMed]
- Njoo, C.; Agarwal, N.; Lutz, B.; Kuner, R. The cannabinoid receptor cb1 interacts with the wave1 complex and plays a role in actin dynamics and structural plasticity in neurons. PLoS Biol. 2015, 13, 1–36. [Google Scholar] [CrossRef] [PubMed]
- Schoch, H.; Huerta, M.Y.; Ruiz, C.M.; Farrell, M.R.; Jung, K.M.; Huang, J.J.; Campbell, R.R.; Piomelli, D.; Mahler, S.V. Adolescent cannabinoid exposure effects on natural reward seeking and learning in rats. Psychopharmacology 2018, 235, 121–134. [Google Scholar] [CrossRef] [PubMed]
- Ananthakrishnan, A.N. Epidemiology and risk factors for IBD. Nat. Rev. Gastroenterol. Hepatol. 2015, 12, 205–217. [Google Scholar] [CrossRef] [PubMed]
- Grotenhermen, F. Pharmacokinetics and pharmacodynamics of cannabinoids. Clin. Pharmacokinet. 2003, 42, 327–360. [Google Scholar] [CrossRef] [PubMed]
- Pacifici, R.; Marchei, E.; Salvatore, F.; Guandalini, L.; Busardò, F.P.; Pichini, S. Evaluation of long-term stability of cannabinoids in standardized preparations of cannabis flowering tops and cannabis oil by ultra-high-performance liquid chromatography tandem mass spectrometry. Clin. Chem. Lab. Med. 2018, 56, e94–e96. [Google Scholar] [CrossRef] [PubMed]
- Fairbairn, J.W.; Liebmann, J.A.; Rowan, M.G. The stability of cannabis and its preparations on storage. J. Pharm. Pharmacol. 1976, 28, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kumari, A.; Yadav, S.K.; Yadav, S.C. Biodegradable polymeric nanoparticles based drug delivery systems. Colloids Surf. B Biointerfaces 2010, 75, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, M.J.; Rees, G.D. Microemulsion-based media as novel drug delivery systems. Adv. Drug Deliv. Rev. 2000, 45, 89–121. [Google Scholar] [CrossRef]
- Allen, T.M.; Cullis, P.R. Drug Delivery Systems: Entering the Mainstream. Science 2004, 303, 1818–1822. [Google Scholar] [CrossRef] [PubMed]
- Allen, T.M.; Cullis, P.R. Liposomal drug delivery systems: From concept to clinical applications. Adv. Drug Deliv. Rev. 2013, 65, 36–48. [Google Scholar] [CrossRef] [PubMed]
- Oh, D.A.; Parikh, N.; Khurana, V.; Smith, C.C.; Vetticaden, S. Effect of food on the pharmacokinetics of dronabinol oral solution versus dronabinol capsules in healthy volunteers. Clin. Pharmacol. 2017, 9, 9–17. [Google Scholar] [PubMed]
- Schimrigk, S.; Marziniak, M.; Neubauer, C.; Kugler, E.M.; Werner, G.; Abramov-Sommariva, D. Dronabinol is a safe long-term treatment option for neuropathic pain patients. Eur. Neurol. 2017, 78, 320–329. [Google Scholar] [CrossRef] [PubMed]
- Svendsen, K.B.; Jensen, T.S.; Bach, F.W. Does the cannabinoid dronabinol reduce central pain in multiple sclerosis? Randomised double blind placebo controlled crossover trial. BMJ 2004, 329, 253. [Google Scholar] [CrossRef] [PubMed]
- Schussel, V.; Kenzo, L.; Santos, A.; Bueno, J.; Yoshimura, E.; de Oliveira Cruz Latorraca, C.; Pachito, D.V.; Riera, R. Cannabinoids for nausea and vomiting related to chemotherapy: Overview of systematic reviews. Phytother. Res. 2018, 32, 567–576. [Google Scholar] [CrossRef] [PubMed]
- Toth, C.; Mawani, S.; Brady, S.; Chan, C.; Liu, C.; Mehina, E.; Garven, A.; Bestard, J.; Korngut, L. An enriched-enrolment, randomized withdrawal, flexible-dose, double-blind, placebo-controlled, parallel assignment efficacy study of nabilone as adjuvant in the treatment of diabetic peripheral neuropathic pain. Pain 2012, 153, 2073–2082. [Google Scholar] [CrossRef] [PubMed]
- Turcott, J.G.; Del Rocío Guillen Núñez, M.; Flores-Estrada, D.; Oñate-Ocaña, L.F.; Zatarain-Barrón, Z.L.; Barrón, F.; Arrieta, O. The effect of nabilone on appetite, nutritional status, and quality of life in lung cancer patients: A randomized, double-blind clinical trial. Support. Care Cancer 2018, 26, 3029–3038. [Google Scholar] [CrossRef] [PubMed]
- Devinsky, O.; Cross, J.H.; Laux, L.; Marsh, E.; Miller, I.; Nabbout, R.; Scheffer, I.E.; Thiele, E.A.; Wright, S. Trial of cannabidiol for drug-resistant seizures in the dravet syndrome. N. Engl. J. Med. 2017, 376, 2011–2020. [Google Scholar] [CrossRef] [PubMed]
- Devinsky, O.; Patel, A.D.; Cross, J.H.; Villanueva, V.; Wirrell, E.C.; Privitera, M.; Greenwood, S.M.; Roberts, C.; Checketts, D.; VanLandingham, K.E.; et al. Effect of cannabidiol on drop seizures in the lennox–gastaut syndrome. N. Engl. J. Med. 2018, 378, 1888–1897. [Google Scholar] [CrossRef] [PubMed]
- Thiele, E.A.; Marsh, E.D.; French, J.A.; Mazurkiewicz-Beldzinska, M.; Benbadis, S.R.; Joshi, C.; Lyons, P.D.; Taylor, A.; Roberts, C.; Sommerville, K.; et al. Cannabidiol in patients with seizures associated with Lennox-Gastaut syndrome (GWPCARE4): A randomised, double-blind, placebo-controlled phase 3 trial. Lancet 2018, 391, 1085–1096. [Google Scholar] [CrossRef]
- Robson, P.; Guy, G.; Pertwee, R.; Jamontt, J. Use of Tetrahydrocannabinol and/or Cannabidiol for the Treatment of Inflammatory Bowel Disease. WO2009004302A1, 8 January 2009. [Google Scholar]
- Yeshurun, M.; Sagiv, S.P. Cannabidiol for Reducing a Steroid Dose and Treating Inflammatory and Autoimmune Diseases. WO2017191630A1, 9 November 2017. [Google Scholar]
- De Vries, J.A.; Fernandez Cid, M.V.; Heredia Lopez, A.M.; Eiroa Martinez, C.M. Compressed Tablet Containing Cannabidiol, Method for Its Manufacture and Use of Such Tablet in Oral Treatment of Psychosis or Anxiety Disorders. WO2015065179A1, 7 May 2015. [Google Scholar]
- Gursoy, R.N.; Benita, S. Self-emulsifying drug delivery systems (SEDDS) for improved oral delivery of lipophilic drugs. Biomed. Pharmacother. 2004, 58, 173–182. [Google Scholar] [CrossRef] [PubMed]
- Murty, R.B.; Murty, S.B. An Improved Oral Dosage Form of Tetrahydrocannabinol and a Method of Avoiding and/or Suppressing Hepatic First Pass Metabolism via Targeted Chylomicron/Lipoprotein Delivery. WO2012033478A1, 15 March 2012. [Google Scholar]
- Murty, R.B.; Murty, S.B. Oral Dosage Form of Tetrahydrocannabinol and a Method of Avoiding and/or Suppressing Hepatic First Pass Metabolism via Targeted Chylomicron/Lipoprotein Delivery. U.S. Patent 20140357708A1, 4 December 2014. [Google Scholar]
- Murty, S.B.; Murty, R.B. Oral Gastrointestinal Dosage Form Delivery System of Cannabinoids and/or Standardized Marijuana Extracts. U.S. Patent 20160184258A1, 30 June 2016. [Google Scholar]
- Zipp, B.J.; Hardman, J.M.; Brooke, R.T. Methods for Production of Cannabinoid Glycoside Prodrugs by Glycosyltransferase-Mediated Glycosylation of Cannabinoids. WO2017053574A1, 30 March 2017. [Google Scholar]
- Hardman, J.M.; Brooke, R.T.; Zipp, B.J. Cannabinoid glycosides: In vitro production of a new class of cannabinoids with improved physicochemical properties. BioRxiv 2017. [Google Scholar] [CrossRef]
- Mercadante, S.; Radbruch, L.; Davies, A.; Poulain, P.; Sitte, T.; Perkins, P.; Colberg, T.; Camba, M.A. A comparison of intranasal fentanyl spray with oral transmucosal fentanyl citrate for the treatment of breakthrough cancer pain: an open-label, randomised, crossover trial. Curr. Med. Res. Opin. 2009, 25, 2805–2815. [Google Scholar] [CrossRef] [PubMed]
- Karschner, E.L.; Darwin, W.D.; Goodwin, R.S.; Wright, S.; Huestis, M.A. Plasma cannabinoid pharmacokinetics following controlled oral Δ9-tetrahydrocannabinol and oromucosal cannabis extract administration. Clin. Chem. 2011, 57, 66–75. [Google Scholar] [CrossRef] [PubMed]
- Tanasescu, R.; Constantinescu, C.S. Pharmacokinetic evaluation of nabiximols for the treatment of multiple sclerosis pain. Expert Opin. Drug Metab. Toxicol. 2013, 9, 1219–1228. [Google Scholar] [CrossRef] [PubMed]
- Lichtman, A.H.; Lux, E.A.; McQuade, R.; Rossetti, S.; Sanchez, R.; Sun, W.; Wright, S.; Kornyeyeva, E.; Fallon, M.T. Results of a double-blind, randomized, placebo-controlled study of nabiximols oromucosal spray as adjunctive therapy in advanced cancer patients with chronic uncontrolled pain. J. Pain Symptom Manag. 2018, 55, 179–188. [Google Scholar] [CrossRef] [PubMed]
- Nurmikko, T.J.; Serpell, M.G.; Hoggart, B.; Toomey, P.J.; Morlion, B.J.; Haines, D. Sativex successfully treats neuropathic pain characterised by allodynia: A randomised, double-blind, placebo-controlled clinical trial. Pain 2007, 133, 210–220. [Google Scholar] [CrossRef] [PubMed]
- Temtsin-Krayz, G.; Glozman, S.; Kazhdan, P. Pharmaceutical Compositions Comprising Lipophilic Compd. and Water-Sol. Polymers for Transmucosal Delivery. WO2017072774A1, 4 May 2017. [Google Scholar]
- Van Damme, P.A.; Anastassov, G.E. Chewing Gum Compositions Comprising Cannabinoids. WO2009120080A1, 1 October 2009. [Google Scholar]
- Anastassov, G.; Changoer, L. Chewing Gum Composition Comprising Cannabinoids and Opioid Agonists and/or Antagonists. WO2018075665A1, 26 April 2018. [Google Scholar]
- Paudel, K.S.; Hammell, D.C.; Agu, R.U.; Valiveti, S.; Stinchcomb, A.L. Cannabidiol bioavailability after nasal and transdermal application: Effect of permeation enhancers. Drug Dev. Ind. Pharm. 2010, 36, 1088–1097. [Google Scholar] [CrossRef] [PubMed]
- Bryson, N.; Sharma, A.C. Nasal Cannabidiol Compositions. WO2017208072A2, 7 December 2017. [Google Scholar]
- Huestis, M.A. Human Cannabinoid Pharmacokinetics. Chem. Biodivers. 2007, 4, 1770–1804. [Google Scholar] [CrossRef] [PubMed]
- Hartman, R.L.; Brown, T.L.; Milavetz, G.; Spurgin, A.; Gorelick, D.A.; Gaffney, G.; Huestis, M.A. Controlled Cannabis Vaporizer Administration: Blood and Plasma Cannabinoids with and without Alcohol. Clin. Chem. 2015, 61, 850–869. [Google Scholar] [CrossRef] [PubMed]
- Solowij, N.; Broyd, S.J.; van Hell, H.H.; Hazekamp, A. A protocol for the delivery of cannabidiol (CBD) and combined CBD and Δ9-tetrahydrocannabinol (THC) by vaporisation. BMC Pharmacol. Toxicol. 2014, 15. [Google Scholar] [CrossRef] [PubMed]
- Davidson, P.; Almog, S.; Kindler, S. Methods, Devices and Systems for Pulmonary Delivery of Active Agents. WO2016001922A1, 7 January 2016. [Google Scholar]
- Cameron, J. Hybrid Vapor Delivery System Utilizing Nebulized and Non-Nebulized Elements. WO2016187115A1, 24 November 2016. [Google Scholar]
- Raichman, Y. Vaporizing Devices and Methods for Delivering a Compound Using the Same. U.S. Patent 20180104214A1, 19 April 2018. [Google Scholar]
- McCullough, T. Methods and Devices Using Cannabis Vapors. U.S. Patent 20150223515A1, 13 August 2015. [Google Scholar]
- Mason, L.; Moore, R.A.; Derry, S.; Edwards, J.E.; McQuay, H.J. Systematic review of topical capsaicin for the treatment of chronic pain. Br. Med. J. 2004, 328, 991–994. [Google Scholar] [CrossRef] [PubMed]
- Tubaro, A.; Giangaspero, A.; Sosa, S.; Negri, R.; Grassi, G.; Casano, S.; Loggia, R.D.; Appendino, G. Comparative topical anti-inflammatory activity of cannabinoids and cannabivarins. Fitoterapia 2010, 81, 816–819. [Google Scholar] [CrossRef] [PubMed]
- Hammell, D.C.; Zhang, L.P.; Ma, F.; Abshire, S.M.; McIlwrath, S.L.; Stinchcomb, A.L.; Westlund, K.N. Transdermal cannabidiol reduces inflammation and pain-related behaviours in a rat model of arthritis. Eur. J. Pain 2016, 20, 936–948. [Google Scholar] [CrossRef] [PubMed]
- Touitou, E.; Dayan, N.; Bergelson, L.; Godin, B.; Eliaz, M. Ethosomes—Novel vesicular carriers for enhanced delivery: Characterization and skin penetration properties. J. Control. Release 2000, 65, 403–418. [Google Scholar] [CrossRef]
- Lodzki, M.; Godin, B.; Rakou, L.; Mechoulam, R.; Gallily, R.; Touitou, E. Cannabidiol—Transdermal delivery and anti-inflammatory effect in a murine model. J. Control. Release 2003, 93, 377–387. [Google Scholar] [CrossRef] [PubMed]
- Stinchcomb, A.L. Transdermal Delivery of Cannabinoids. U.S. Patent 20020111377A1, 15 August 2002. [Google Scholar]
- Stinchcomb, A.L.; Nalluri, B.N. Transdermal Delivery of Cannabinoids. U.S. Patent 20050266061A1, 1 December 2005. [Google Scholar]
- Stinchcomb, A.L.; Banks, S.L.; Golinski, M.J.; Howard, J.L.; Hammell, D.C. Use of Cannabidiol Prodrugs in Topical and Transdermal Administration with Microneedles. WO2011026144A1, 3 March 2011. [Google Scholar]
- Stinchcomb, A.L.; Valiveti, S.; Hammell, D.C.; Ramsey, D.R. Human skin permeation of Δ8-tetrahydrocannabinol, cannabidiol and cannabinol. J. Pharm. Pharmacol. 2004, 56, 291–297. [Google Scholar] [CrossRef] [PubMed]
- Chelliah, M.P.; Zinn, Z.; Khuu, P.; Teng, J.M.C. Self-initiated use of topical cannabidiol oil for epidermolysis bullosa. Pediatr. Dermatol. 2018, 35, 224–227. [Google Scholar] [CrossRef] [PubMed]
- Brooke, L.L.; Herrmann, C.C.; Yum, S.I. Cannabinoid Patch and Method for Cannabis Transdermal Delivery. U.S. Patent 6328992B1, 11 December 2001. [Google Scholar]
- Wallace, W.H. Method for Relieving Analgesia and Reducing Inflamation Using a Cannabinoid Delivery Topical Liniment. U.S. Patent 6949582B1, 27 September 2005. [Google Scholar]
- Siurkus, J. The Oleo Gel Composition and Delivery System with Active Compounds from Cannabis Sativa and Mentha Arvensis for Reduction of Inflammation and Pain in Deep Tissues. WO2017178937A1, 19 October 2017. [Google Scholar]
- Siurkus, J.; Peciura, R. The Topical Composition with Active Compounds from Cannabis Sativa and Calendula Officinalis for Reduction of Skin Lesions. WO2017175126A1, 12 October 2017. [Google Scholar]
- Jackson, D.K.; Hyatt, K. Silicone and Hyaluronic Acid (HLA) Delivery Systems for Products by Sustainable Processes for Medical Uses Including Wound Management. U.S. Patent 20130184354A1, 18 July 2013. [Google Scholar]
- Lowe, G.A.; Lowe, V. Composition of Cannabinoids, Odorous Volatile Compounds, and Emu Oil for Topical Application and Transdermal Delivery to Hypodermis. U.S. Patent 9526752B1, 27 December 2016. [Google Scholar]
- Shemanski, M.E. Formulations of Argan Oil and Cannabidiol for Treating Inflammatory Disorders Including Arthritis. WO2017160923A1, 21 September 2017. [Google Scholar]
- Skalicky, J.; Husek, J.; Hofbauerova, J.; Dittrich, M. A composition for the treatment of inflammatory diseases comprising boswellic acids and cannabidiol. European Patent Application No. 2444081A1, 25 April 2012. [Google Scholar]
- Oláh, A.; Tóth, B.I.; Borbíró, I.; Sugawara, K.; Szöllõsi, A.G.; Czifra, G.; Pál, B.; Ambrus, L.; Kloepper, J.; Camera, E.; et al. Cannabidiol exerts sebostatic and antiinflammatory effects on human sebocytes. J. Clin. Investig. 2014, 124, 3713–3724. [Google Scholar] [CrossRef] [PubMed]
- Adelli, G.R.; Bhagav, P.; Taskar, P.; Hingorani, T.; Pettaway, S.; Gul, W.; Elsohly, M.A.; Repka, M.A.; Majumdar, S. Development of a ∆9-tetrahydrocannabinol amino acid-dicarboxylate prodrug with improved ocular bioavailability. Investig. Ophthalmol. Vis. Sci. 2017, 58, 2167–2179. [Google Scholar] [CrossRef] [PubMed]
- Cairns, E.A.; Baldridge, W.H.; Kelly, M.E.M. The Endocannabinoid System as a Therapeutic Target in Glaucoma. Neural Plast. 2016, 2016, 9364091. [Google Scholar] [CrossRef] [PubMed]
- Weimann, L.J. Device and Method for the Transdermal Delivery of Cannabidiol. U.S. Patent 20160361271A1, 15 December 2016. [Google Scholar]
- Immordino, M.L.; Dosio, F.; Cattel, L. Stealth liposomes: Review of the basic science, rationale, and clinical applications, existing and potential. Int. J. Nanomed. 2006, 1, 297–315. [Google Scholar]
- Dosio, F.; Arpicco, S.; Stella, B.; Fattal, E. Hyaluronic acid for anticancer drug and nucleic acid delivery. Adv. Drug Deliv. Rev. 2016, 97, 204–236. [Google Scholar] [CrossRef] [PubMed]
- Boraschi, D.; Italiani, P.; Palomba, R.; Decuzzi, P.; Duschl, A.; Fadeel, B.; Moghimi, S.M. Nanoparticles and innate immunity: New perspectives on host defence. Semin. Immunol. 2017, 34, 33–51. [Google Scholar] [CrossRef] [PubMed]
- Park, K. Facing the truth about nanotechnology in drug delivery. ACS Nano 2013, 7, 7442–7447. [Google Scholar] [CrossRef] [PubMed]
- Hung, O.; Zamecnik, J.; Shek, P.N.; Tikuisis, P. Pulmonary Delivery of Liposome-Encapsulated Cannabinoids. WO2001003668A1, 18 January 2001. [Google Scholar]
- Donsky, M.; Winnicki, R. Terpene and Cannabinoid Liposome and Micelle Formulations. WO2015068052A2, 14 May 2015. [Google Scholar]
- Vitetta, L.; Hall, S. Protection of Plant Extracts and Compounds from Degradation. WO2017193169A1, 16 November 2017. [Google Scholar]
- Hall, S.M.; Vitetta, L.; Zhou, Y.; Rutolo, D.A., Jr.; Coulson, S.M. Transmucosal and Transdermal Delivery Systems Comprising Non-Ionic Surfactant and Polyol. WO2016141069A1, 9 September 2016. [Google Scholar]
- Pardeike, J.; Hommoss, A.; Müller, R.H. Lipid nanoparticles (SLN, NLC) in cosmetic and pharmaceutical dermal products. Int. J. Pharm. 2009, 366, 170–184. [Google Scholar] [CrossRef] [PubMed]
- Esposito, E.; Drechsler, M.; Cortesi, R.; Nastruzzi, C. Encapsulation of cannabinoid drugs in nanostructured lipid carriers. Eur. J. Pharm. Biopharm. 2016, 102, 87–91. [Google Scholar] [CrossRef] [PubMed]
- Hommoss, G.; Pyo, S.M.; Müller, R.H. Mucoadhesive tetrahydrocannabinol-loaded NLC—Formulation optimization and long-term physicochemical stability. Eur. J. Pharm. Biopharm. 2017, 117, 408–417. [Google Scholar] [CrossRef] [PubMed]
- Johnson, J.R.; Burnell-Nugent, M.; Lossignol, D.; Ganae-Motan, E.D.; Potts, R.; Fallon, M.T. Multicenter, double-blind, randomized, placebo-controlled, parallel-group study of the efficacy, safety, and tolerability of thc:cbd extract and thc extract in patients with intractable cancer-related pain. J. Pain Symptom Manag. 2010, 39, 167–179. [Google Scholar] [CrossRef] [PubMed]
- Durán-Lobato, M.; Martín-Banderas, L.; Lopes, R.; Gonçalves, L.M.D.; Fernández-Arévalo, M.; Almeida, A.J. Lipid nanoparticles as an emerging platform for cannabinoid delivery: Physicochemical optimization and biocompatibility. Drug Dev. Ind. Pharm. 2016, 42, 190–198. [Google Scholar] [CrossRef] [PubMed]
- Elgart, A.; Cherniakov, I.; Aldouby, Y.; Domb, A.J.; Hoffman, A. Improved oral bioavailability of bcs class 2 compounds by self nano-emulsifying drug delivery systems (snedds): the underlying mechanisms for amiodarone and talinolol. Pharm. Res. 2013, 30, 3029–3044. [Google Scholar] [CrossRef] [PubMed]
- Mistry, R.B.; Sheth, N.S. A review: Self emulsifying drug delivery system. Int. J. Pharm. Pharm. Sci. 2011, 3, 23–28. [Google Scholar]
- Avramoff, A.; Khan, W.; Ezra, A.; Elgart, A.; Hoffman, A.; Domb, A.J. Cyclosporin pro-dispersion liposphere formulation. J. Control. Release 2012, 160, 401–406. [Google Scholar] [CrossRef] [PubMed]
- Atsmon, J.; Cherniakov, I.; Izgelov, D.; Hoffman, A.; Domb, A.J.; Deutsch, L.; Deutsch, F.; Heffetz, D.; Sacks, H. PTL401, a new formulation based on pro-nano dispersion technology, improves oral cannabinoids bioavailability in healthy volunteers. J. Pharm. Sci. 2018, 107, 1423–1429. [Google Scholar] [CrossRef] [PubMed]
- Cherniakov, I.; Izgelov, D.; Domb, A.J.; Hoffman, A. The effect of Pro NanoLipospheres (PNL) formulation containing natural absorption enhancers on the oral bioavailability of delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD) in a rat model. Eur. J. Pharm. Sci. 2017, 109, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Cherniakov, I.; Izgelov, D.; Barasch, D.; Davidson, E.; Domb, A.J.; Hoffman, A. Piperine-pro-nanolipospheres as a novel oral delivery system of cannabinoids: Pharmacokinetic evaluation in healthy volunteers in comparison to buccal spray administration. J. Control. Release 2017, 266, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, A.; Domb, A.J.; Elgart, A.; Cherniakov, I. Formulation and Method for Increasing Oral Bioavailability of Drugs by Utilizing Pro-Nano Lipospheres Incorporating Piperine. WO2013108254A1, 25 July 2013. [Google Scholar]
- Wallis, S.W. Therapeutic Delivery Formulations and Systems Comprising Cannabinoids and Terpenes. CA2952335A1, 19 June 2017. [Google Scholar]
- Cardiol, T. Cannabidiol Nanotherapeutic—Cardiol Therapeutics. Available online: http://adisinsight.springer.com/drugs/800052179 (accessed on 25 September 2018).
- Liechty, W.B.; Kryscio, D.R.; Slaughter, B.V.; Peppas, N.A. Polymers for drug delivery systems. Ann. Rev. Chem. Biomol. Eng. 2010, 1, 149–173. [Google Scholar] [CrossRef] [PubMed]
- Mitragotri, S.; Burke, P.A.; Langer, R. Overcoming the challenges in administering biopharmaceuticals: Formulation and delivery strategies. Nat. Rev. Drug Discov. 2014, 13, 655–672. [Google Scholar] [CrossRef] [PubMed]
- Durán-Lobato, M.; Muñoz-Rubio, I.; Holgado, M.Á.; Álvarez-Fuentes, J.; Fernández-Arévalo, M.; Martín-Banderas, L. Enhanced cellular uptake and biodistribution of a synthetic cannabinoid loaded in surface-modified poly(lactic-co-glycolic acid) nanoparticles. J. Biomed. Nanotechnol. 2014, 10, 1068–1079. [Google Scholar] [CrossRef] [PubMed]
- Martín-Banderas, L.; Muñoz-Rubio, I.; Prados, J.; Álvarez-Fuentes, J.; Calderón-Montaño, J.M.; López-Lázaro, M.; Arias, J.L.; Leiva, M.C.; Holgado, M.A.; Fernández-Arévalo, M. In vitro and in vivo evaluation of Δ9-tetrahidrocannabinol/PLGA nanoparticles for cancer chemotherapy. Int. J. Pharm. 2015, 487, 205–212. [Google Scholar] [CrossRef] [PubMed]
- Hernan Perez De La Ossa, D.; Ligresti, A.; Gil-Alegre, M.E.; Aberturas, M.R.; Molpeceres, J.; Di Marzo, V.; Torres Suárez, A.I. Poly-ε-caprolactone microspheres as a drug delivery system for cannabinoid administration: Development, characterization and in vitro evaluation of their antitumoral efficacy. J. Control. Release 2012, 161, 927–932. [Google Scholar] [CrossRef] [PubMed]
- National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Population Health and Public Health Practice; Committee on the Health Effects of Marijuana: An Evidence Review and Research Agenda. The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research; National Academies Press: Washington, DC, USA, 2017. [Google Scholar]
- Whiting, P.F.; Wolff, R.F.; Deshpande, S.; Di Nisio, M.; Duffy, S.; Hernandez, A.V.; Keurentjes, J.C.; Lang, S.; Misso, K.; Ryder, S.; et al. Cannabinoids for medical use: A systematic review and meta-analysis. JAMA 2015, 313, 2456–2473. [Google Scholar] [CrossRef] [PubMed]
- Nugent, S.M.; Morasco, B.J.; O’Neil, M.E.; Freeman, M.; Low, A.; Kondo, K.; Elven, C.; Zakher, B.; Motu’apuaka, M.; Paynter, R.; et al. The effects of cannabis among adults with chronic pain and an overview of general harms a systematic review. Ann. Intern. Med. 2017, 167, 319–331. [Google Scholar] [CrossRef] [PubMed]
- Mücke, M.; Phillips, T.; Radbruch, L.; Petzke, F.; Häuser, W. Cannabis-based medicines for chronic neuropathic pain in adults. Cochrane Database Syst. Rev. 2018, 2018. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, S.; Sabioni, P.; Trigo, J.M.; Ware, M.A.; Betz-Stablein, B.D.; Murnion, B.; Lintzeris, N.; Khor, K.E.; Farrell, M.; Smith, A.; et al. Opioid-sparing effect of cannabinoids: A systematic review and meta-analysis. Neuropsychopharmacology 2017, 42, 1752–1765. [Google Scholar] [CrossRef] [PubMed]
- Campbell, G.; Hall, W.D.; Peacock, A.; Lintzeris, N.; Bruno, R.; Larance, B.; Nielsen, S.; Cohen, M.; Chan, G.; Mattick, R.P.; et al. Effect of cannabis use in people with chronic non-cancer pain prescribed opioids: Findings from a 4-year prospective cohort study. Lancet Public Health 2018, 3, e341–e350. [Google Scholar] [CrossRef]
- Esposito, G.; De Filippis, D.; Cirillo, C.; Iuvone, T.; Capoccia, E.; Scuderi, C.; Steardo, A.; Cuomo, R.; Steardo, L. Cannabidiol in inflammatory bowel diseases: A brief overview. Phytother. Res. 2013, 27, 633–636. [Google Scholar] [CrossRef] [PubMed]
- Hasenoehrl, C.; Storr, M.; Schicho, R. Cannabinoids for treating inflammatory bowel diseases: Where are we and where do we go? Expert Rev. Gastroenterol. Hepatol. 2017, 11, 329–337. [Google Scholar] [CrossRef] [PubMed]
- Goldenberg, M.; Reid, M.W.; IsHak, W.W.; Danovitch, I. The impact of cannabis and cannabinoids for medical conditions on health-related quality of life: A systematic review and meta-analysis. Drug Alcohol Depend. 2017, 174, 80–90. [Google Scholar] [CrossRef] [PubMed]
- Aviram, J.; Samuelly-Leichtag, G. Efficacy of cannabis-based medicines for pain management: A systematic review and meta-analysis of randomized controlled trials. Pain Phys. 2017, 20, E755–E796. [Google Scholar]
| Administration Route | Name | Drug | Delivery System/ Dosage Form | Disease | Application | Development Stage | References |
|---|---|---|---|---|---|---|---|
| Oral | Dronabinol | THC | Solid | HIV, chemotherapy | Anorexia, nausea | Market | [56] |
| Oral | Nabilone | THC analogue | Solid | Chemotherapy, chronic pain | Nausea, pain | Market | [59,60] |
| Oral | Epidiolex | CBD | Liquid | Lennox-Gastaud and Dravet syndromes | Epilepsy | Market | [62,63,64] |
| Oral | CBD | Solid | Crohn’s disease, GVHD | Clinical trials | [66] | ||
| Oral | THC | SEDDS | Improving dissolution, stability | Preclinical | [69,70,71] | ||
| Oral | THC-glycosides | Prodrugs | Drug-resistant inflammatory bowel disease | Inflammation | Clinical trials | [72,73] | |
| Oromucosal | Nabiximols | THC CBD 1:1 | Spray | Multiple sclerosis | Spasticity | Market | [75,78] |
| Oromucosal | Cancer | Pain | Clinical trials | [77] | |||
| Oromucosal | CBD | Powder | Formulation study | [79] | |||
| Oromucosal | THC CBD 1:1 | Chewing-gum | Several potential diseases | Pain, spasticity, dementia etc. | Preclinical | [80] | |
| Intranasal | CBD | Liquid formulations | Bioavailability study | Preclinical | [82] | ||
| Pulmonary | CBD | Solid/liquid | Formulation study | [86] | |||
| Pulmonary | Powder metered-dose inhaler | Bioavailability study | Clinical trials | [87] | |||
| Transdermal | Phytocannabinoids | Induced dermatitis | Inflammation | Preclinical | [92] | ||
| Transdermal | CBD | Gel | Arthritis | Inflammation | Preclinical | [93] | |
| Transdermal | CBD | Ethosomes | Oedema | Inflammation | Preclinical | [95] | |
| Transdermal | CBD | Gel | Epilepsy, osteoarthritis, fragile-X syndrome | Clinical trials | [96,97,98] | ||
| Transdermal | CBD | Oil, spray, cream | Epidermiolysis bullosa | Pain, blistering | Clinical treatment | [100] | |
| Transdermal | CBD | Patch | Formulation study | [112] | |||
| Transdermal | CBD + hyaluronic acid | Gel | Pain, wound management | Formulation study | [105] | ||
| Transdermal | CBD+ argan oil | Rheumatic diseases | Inflammation | Formulation study | [107] | ||
| Transdermal | CBD+boswellic acid | Inflammation | Formulation study | [108] | |||
| Topical ocular | THC analogue | Prodrugs | Glaucoma | Reduce intraocular pressure | Formulation study | [111] |
| Type | Constituents | Drug | Size (nm) | Encapsulation Efficiency | Application | Development Stage | References | |
|---|---|---|---|---|---|---|---|---|
| Lipid-based | liposomes | DPPC, cholesterol | THC | 300–500 | 0.3 mg/mL | i.v. | Pharmacokinetics | [117] |
| micelles | PC, PE plus phospholipids | Terpenes, hemp oil | n.d. | Stability evaluations | [118] | |||
| micelles | Polyethoxylated castor oil, glycerol | Cannabis oil | 100 | n.d. | oromucosal | Clinical trials | [119,120] | |
| NCL | tristearin/tricaprylin 2:1 | Cannabinoids | 100 | high | Formulation study | [122] | ||
| NCL | Cetyl palmitate or glyceryl dibehenate | THC | 200 | n.d. | nasal | Preclinical studies | [123] | |
| NCL | Glyceryl dibehenate or glyceryl palmitostearate | CB-13 | 120 | 99% | oral | Preclinical studies | [125] | |
| PNL | PTL401 | THC CBD 1:1 | <50 | 99% | oral | Preclinical studies | [130] | |
| PNL | PTL401 | Plus piperine | <50 | 99% | oral | Clinical trials | [131,132] | |
| Nanoemulsions | rectal/vaginal | n.d. | [133] | |||||
| Polymeric-based | PLGA | plus coating agents | CB-13 | 253–344 | 85% | oral | Preclinical studies | [137] |
| PLGA | plus coating agents | THC | 290–800 | 96% | oral | Preclinical studies | [138] | |
| PCL | CBD | 2000–5000 | 100% | locoregional | Preclinical studies | [139] | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bruni, N.; Della Pepa, C.; Oliaro-Bosso, S.; Pessione, E.; Gastaldi, D.; Dosio, F. Cannabinoid Delivery Systems for Pain and Inflammation Treatment. Molecules 2018, 23, 2478. https://doi.org/10.3390/molecules23102478
Bruni N, Della Pepa C, Oliaro-Bosso S, Pessione E, Gastaldi D, Dosio F. Cannabinoid Delivery Systems for Pain and Inflammation Treatment. Molecules. 2018; 23(10):2478. https://doi.org/10.3390/molecules23102478
Chicago/Turabian StyleBruni, Natascia, Carlo Della Pepa, Simonetta Oliaro-Bosso, Enrica Pessione, Daniela Gastaldi, and Franco Dosio. 2018. "Cannabinoid Delivery Systems for Pain and Inflammation Treatment" Molecules 23, no. 10: 2478. https://doi.org/10.3390/molecules23102478
APA StyleBruni, N., Della Pepa, C., Oliaro-Bosso, S., Pessione, E., Gastaldi, D., & Dosio, F. (2018). Cannabinoid Delivery Systems for Pain and Inflammation Treatment. Molecules, 23(10), 2478. https://doi.org/10.3390/molecules23102478






