Liraglutide and Exercise: A Possible Treatment for Obesity?
Abstract
:1. Introduction
2. Liraglutide Mechanism of Action
3. Liraglutide and Obesity Treatment
4. Physical Exercise and Obesity Treatment
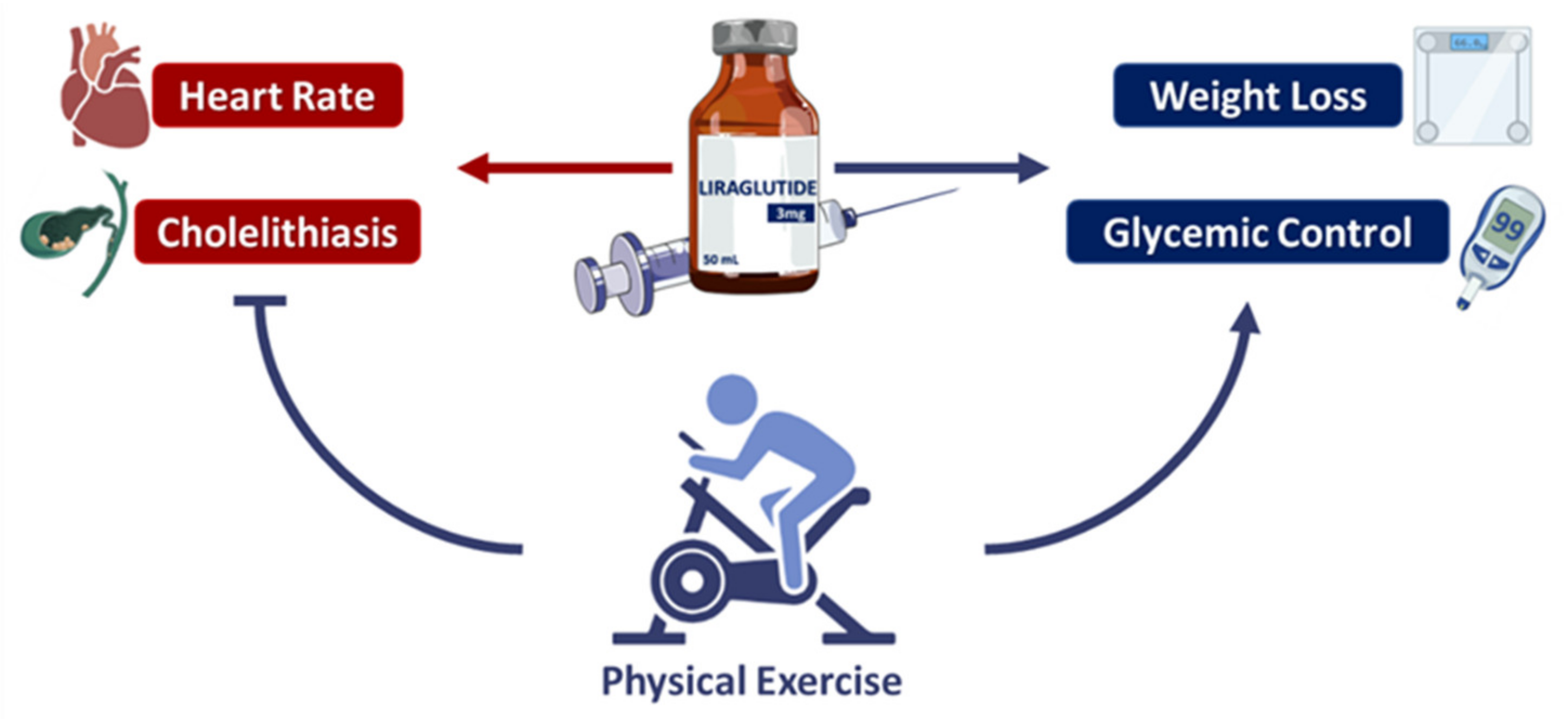
5. Liraglutide and Physical Exercise
6. Liraglutide and Pediatric Studies
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wiechert, M.; Holzapfel, C. Nutrition Concepts for the Treatment of Obesity in Adults. Nutrients 2022, 14, 169. [Google Scholar] [CrossRef] [PubMed]
- O’Neil, P.M.; Birkenfeld, A.L.; McGowan, B.; Mosenzon, O.; Pedersen, S.D.; Wharton, S.; Carson, C.G.; Jepsen, C.H.; Kabisch, M.; Wilding, J.P.H. Efficacy and Safety of Semaglutide Compared with Liraglutide and Placebo for Weight Loss in Patients with Obesity: A Randomised, Double-Blind, Placebo and Active Controlled, Dose-Ranging, Phase 2 Trial. Lancet 2018, 392, 637–649. [Google Scholar] [CrossRef]
- Lemstra, M.; Bird, Y.; Nwankwo, C.; Rogers, M.; Moraros, J. Weight Loss Intervention Adherence and Factors Promoting Adherence: A Meta-Analysis. Patient Prefer. Adherence 2016, 10, 1547–1559. [Google Scholar] [CrossRef] [PubMed]
- Dailey, M.J.; Moran, T.H. Glucagon-like Peptide 1 and Appetite. Trends Endocrinol. Metab. 2013, 24, 85–91. [Google Scholar] [CrossRef]
- Neeland, I.J.; Marso, S.P.; Ayers, C.R.; Lewis, B.; Oslica, R.; Francis, W.; Rodder, S.; Pandey, A.; Joshi, P.H. Effects of Liraglutide on Visceral and Ectopic Fat in Adults with Overweight and Obesity at High Cardiovascular Risk: A Randomised, Double-Blind, Placebo-Controlled, Clinical Trial. Lancet Diabetes Endocrinol. 2021, 9, 595–605. [Google Scholar] [CrossRef]
- Ladenheim, E.E. Liraglutide and Obesity: A Review of the Data so Far. Drug Des. Dev. Therapy. 2015, 2015, 1867–1875. [Google Scholar] [CrossRef]
- Pratley, R.; Amod, A.; Hoff, S.T.; Kadowaki, T.; Lingvay, I.; Nauck, M.; Pedersen, K.B.; Saugstrup, T.; Meier, J.J. Oral Semaglutide versus Subcutaneous Liraglutide and Placebo in Type 2 Diabetes (PIONEER 4): A Randomised, Double-Blind, Phase 3a Trial. Lancet 2019, 394, 39–50. [Google Scholar] [CrossRef]
- Rubino, D.M.; Greenway, F.L.; Khalid, U.; O’Neil, P.M.; Rosenstock, J.; Sørrig, R.; Wadden, T.A.; Wizert, A.; Garvey, W.T. Effect of Weekly Subcutaneous Semaglutide vs Daily Liraglutide on Body Weight in Adults with Overweight or Obesity Without Diabetes: The STEP 8 Randomized Clinical Trial. JAMA—J. Am. Med. Assoc. 2022, 327, 138–150. [Google Scholar] [CrossRef]
- Garvey, W.T.; Birkenfeld, A.L.; Dicker, D.; Mingrone, G.; Pedersen, S.D.; Satylganova, A.; Skovgaard, D.; Sugimoto, D.; Jensen, C.; Mosenzon, O. Efficacy and Safety of Liraglutide 3.0 Mg in Individuals with Overweight or Obesity and Type 2 Diabetes Treated with Basal Insulin: The SCALE Insulin Randomized Controlled Trial. Diabetes Care 2020, 43, 1085–1093. [Google Scholar] [CrossRef]
- Davies, M.J.; Bergenstal, R.; Bode, B.; Kushner, R.F.; Lewin, A.; Skjøth, T.V.; Andreasen, A.H.; Jensen, C.B.; DeFronzo, R.A.; Valensi, P.; et al. Efficacy of Liraglutide for Weight Loss among Patients with Type 2 Diabetes: The SCALE Diabetes Randomized Clinical Trial. JAMA—J. Am. Med. Assoc. 2015, 314, 687–699. [Google Scholar] [CrossRef]
- Gorgojo-Martínez, J.J.; Basagoiti-Carreño, B.; Sanz-Velasco, A.; Serrano-Moreno, C.; Almodóvar-Ruiz, F. Effectiveness and Tolerability of Orlistat and Liraglutide in Patients with Obesity in a Real-World Setting: The XENSOR Study. Int. J. Clin. Pract. 2019, 73, e13399. [Google Scholar] [CrossRef]
- Wharton, S.; Haase, C.L.; Kamran, E.; Liu, A.; Mancini, J.; Neish, D.; Pakseresht, A.; Power, G.S.; Christensen, R.A.G. Weight Loss and Persistence with Liraglutide 3.0 Mg by Obesity Class in the Real-World Effectiveness Study in Canada. Obes. Sci. Pract. 2020, 6, 439–444. [Google Scholar] [CrossRef]
- Lundgren, J.R.; Janus, C.; Jensen, S.B.K.; Juhl, C.R.; Olsen, L.M.; Christensen, R.M.; Svane, M.S.; Bandholm, T.; Bojsen-Møller, K.N.; Blond, M.B.; et al. Healthy Weight Loss Maintenance with Exercise, Liraglutide, or Both Combined. N. Engl. J. Med. 2021, 384, 1719–1730. [Google Scholar] [CrossRef]
- Petridou, A.; Siopi, A.; Mougios, V. Exercise in the Management of Obesity. Metab. Clin. Exp. 2019, 92, 163–169. [Google Scholar] [CrossRef]
- Bray, G.A.; Frühbeck, G.; Ryan Donna, H.; Wilding Jhon, P.H. Management of Obesity. Lancet 2016, 397, 1947–1956. [Google Scholar] [CrossRef]
- Hsu, K.J.; de Liao, C.; Tsai, M.W.; Chen, C.N. Effects of Exercise and Nutritional Intervention on Body Composition, Metabolic Health, and Physical Performance in Adults with Sarcopenic Obesity: A Meta-Analysis. Nutrients 2019, 11, 2163. [Google Scholar] [CrossRef]
- Fothergill, E.; Guo, J.; Howard, L.; Kerns, J.C.; Knuth, N.D.; Brychta, R.; Chen, K.Y.; Skarulis, M.C.; Walter, M.; Walter, P.J.; et al. Persistent Metabolic Adaptation 6 Years after “The Biggest Loser” Competition. Obesity 2016, 24, 1612–1619. [Google Scholar] [CrossRef] [PubMed]
- Hunter, G.R.; Brock, D.W.; Byrne, N.M.; Chandler-Laney, P.C.; del Corral, P.; Gower, B.A. Exercise Training Prevents Regain of Visceral Fat for 1 Year Following Weight Loss. Obesity 2010, 18, 690–695. [Google Scholar] [CrossRef] [PubMed]
- Jakicic, J.M.; Rogers, R.J.; Davis, K.K.; Collins, K.A. Role of Physical Activity and Exercise in Treating Patients with Overweight and Obesity. Clin. Chem. 2018, 64, 99–107. [Google Scholar] [CrossRef]
- Aaseth, J.; Ellefsen, S.; Alehagen, U.; Sundfør, T.M.; Alexander, J. Diets and Drugs for Weight Loss and Health in Obesity—An Update. Biomed. Pharmacother. 2021, 140, 111789. [Google Scholar] [CrossRef]
- Srivastava, G.; Apovian, C. Future Pharmacotherapy for Obesity: New Anti-Obesity Drugs on the Horizon. Curr. Obes. Rep. 2018, 7, 147–161. [Google Scholar] [CrossRef] [PubMed]
- Johansson, K.; Neovius, M.; Hemmingsson, E. Effects of Anti-Obesity Drugs, Diet, and Exercise on Weight-Loss Maintenance after a Very-Low-Calorie Diet or Low-Calorie Diet: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Am. J. Clin. Nutr. 2014, 99, 14–23. [Google Scholar] [CrossRef]
- Vieira, R.F.L.; Muñoz, V.R.; Junqueira, R.L.; de Oliveira, F.; Gaspar, R.C.; Nakandakari, S.C.B.R.; de Oliveira Costa, S.; Torsoni, M.A.; da Silva, A.S.R.; Cintra, D.E.; et al. Time-Restricted Feeding Combined with Aerobic Exercise Training Can Prevent Weight Gain and Improve Metabolic Disorders in Mice Fed a High-Fat Diet. J. Physiol. 2021, 600, 797–813. [Google Scholar] [CrossRef]
- Ropelle, E.R.; Ramos Da Silva, A.S.; Cintra, D.E.; Pereira De Moura, L.; Teixeira, A.M.; Pauli, J.R. Physical Exercise: A Versatile Anti-Inflammatory Tool Involved in the Control of Hypothalamic Satiety Signaling. Exerc. Immunol. Rev. 2021, 27, 7–21. [Google Scholar]
- Gaspar, R.C.; Pauli, J.R.; Shulman, G.I.; Muñoz, V.R. An Update on Brown Adipose Tissue Biology: A Discussion of Recent Findings. Am. J. Physiol.-Endocrinol. Metab. 2021, 230, E488–E495. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Dias, S.; Strasser, B.; Hoffmann, G. Impact of Different Training Modalities on Anthropometric and Metabolic Characteristics in Overweight/Obese Subjects: A Systematic Review and Network Meta-Analysis. PLoS ONE 2013, 8, e82853. [Google Scholar] [CrossRef]
- Bellicha, A.; van Baak, M.A.; Battista, F.; Beaulieu, K.; Blundell, J.E.; Busetto, L.; Carraça, E.V.; Dicker, D.; Encantado, J.; Ermolao, A.; et al. Effect of Exercise Training on Weight Loss, Body Composition Changes, and Weight Maintenance in Adults with Overweight or Obesity: An Overview of 12 Systematic Reviews and 149 Studies. Obes. Rev. 2021, 22, e13256. [Google Scholar] [CrossRef]
- Kelly, A.S.; Auerbach, P.; Barrientos-Perez, M.; Gies, M.; Hale, P.M.; Marcus, C.; Mastrandrea, L.D.; Prabhu, N.; Arslanian, S. A Randomized, Controlled Trial of Liraglutide for Adolescents with Obesity. N. Engl. J. Med. 2022, 382, 2117–2128. [Google Scholar] [CrossRef]
- Yin, R.; Ma, Y.; Zhang, N.; Yang, L.; Zhao, D. Combined Effects of Voluntary Running and Liraglutide on Glucose Homeostasis, Fatty Acid Composition of Brown Adipose Tissue Phospholipids, and White Adipose Tissue Browning in Db/Db Mice. Chin. J. Physiol. 2022, 65, 117. [Google Scholar] [CrossRef]
- Tamborlane, W.V.; Barrientos-Pérez, M.; Fainberg, U.; Frimer-Larsen, H.; Hafez, M.; Hale, P.M.; Jalaludin, M.Y.; Kovarenko, M.; Libman, I.; Lynch, J.L.; et al. Liraglutide in Children and Adolescents with Type 2 Diabetes. N. Engl. J. Med. 2019, 381, 637–646. [Google Scholar] [CrossRef]
- Mastrandrea, L.D.; Witten, L.; Petri Kristin, C.C.; Hale, P.M.; Hedman, H.K.; Riesenberg, R.A. Liraglutide Effects in a Pediatric (7–11 y) Population with Obesity: A Randomized, Double-Blind, Placebo-Controlled, Short-Term Trial to Assess Safety, Tolerability, Pharmacokinetics, and Pharmacodynamics. Pediatr. Obes. 2019, 14, e12495. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Macêdo, A.P.A.; Vieira, R.F.L.; Brisque, G.D.; Abud, G.F.; Pauli, J.R. Liraglutide and Exercise: A Possible Treatment for Obesity? Obesities 2022, 2, 285-291. https://doi.org/10.3390/obesities2030023
Macêdo APA, Vieira RFL, Brisque GD, Abud GF, Pauli JR. Liraglutide and Exercise: A Possible Treatment for Obesity? Obesities. 2022; 2(3):285-291. https://doi.org/10.3390/obesities2030023
Chicago/Turabian StyleMacêdo, Ana Paula Azevêdo, Renan Fudoli Lins Vieira, Guilherme Domingos Brisque, Gabriela Ferreira Abud, and José Rodrigo Pauli. 2022. "Liraglutide and Exercise: A Possible Treatment for Obesity?" Obesities 2, no. 3: 285-291. https://doi.org/10.3390/obesities2030023
APA StyleMacêdo, A. P. A., Vieira, R. F. L., Brisque, G. D., Abud, G. F., & Pauli, J. R. (2022). Liraglutide and Exercise: A Possible Treatment for Obesity? Obesities, 2(3), 285-291. https://doi.org/10.3390/obesities2030023






