Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report
Abstract
1. Introduction
2. Case Report
- Digital planning for static guided implant surgery planning;
- A lab workflow for the realization of the provisional prosthesis;
- A surgical phase of implant insertion and immediate loading of the provisional prosthesis.
- Digital implant planning was initially performed after superimposing the DICOM files of the CBCT with the STL files of the digital intraoral impressions, using a dental implant planning software (RealGuide 3Diemme, Como, Italy). Seven implants (Naturactis tapered implants, LYRA ETK, Paris, France) were virtually inserted in the upper maxilla (Figure 3a,b) based on the final prosthetic project and on the occlusion of the patient. A surgical template for static guided implant surgery was designed (Figure 4) according to the implant positions and patient anatomy. Implant dimensions and positions were specified as follows:
- Three 4 × 10 mm implants were planned in 1.5, 2.3, and 2.5 positions;
- Two 3.5 × 12 mm implants were planned in 1.3 and 1.1 positions;
- One 4 × 12 mm implant was planned in 2.1 position;
- One 4 × 8 mm implant was planned in 2.6 position.
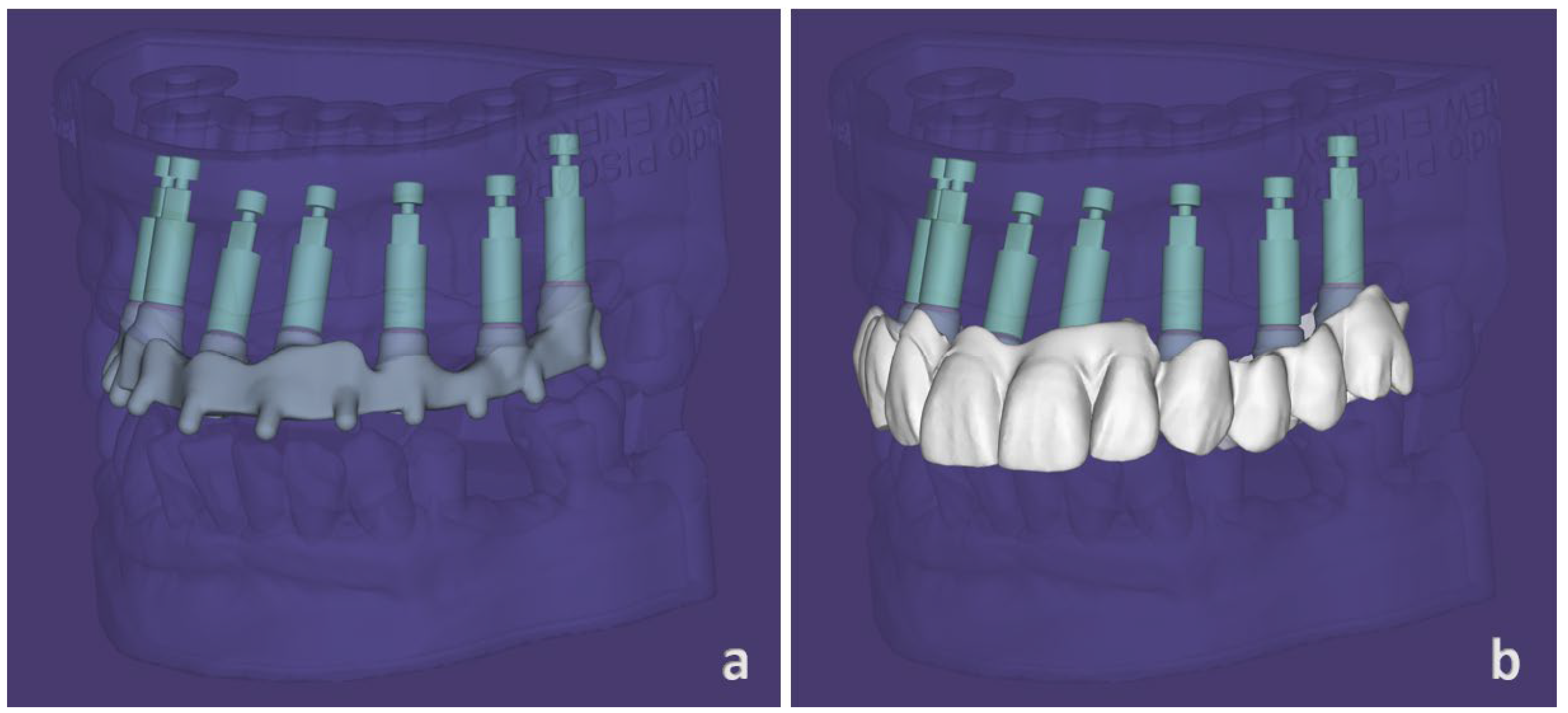
- Six low-profile attachments (OT-Equator, Rhein83, Bologna, Italy) were selected and placed in the virtual environment on the corresponding implants. The height of each OT-Equator was selected on the basis of tissue levels previously measured in the implant planning, types, and implant depth (Figure 5a).
- The digital library files of the dedicated scan abutment were applied to each OT-Equator, performing a “presurgical virtual impression” that obtained the implant’s prosthetic emergence, axis, and positions, (Figure 5b), and the STL file was then exported and sent to the technician for the project and fabrication of the provisional prosthesis.
- The dental technician worked on the STL file that was received as an intraoral digital impression, obtaining the Ti-Base (Extragrade abutment, Rhein83, Bologna, Italy) from the library file of the scan abutment (Figure 6a,b). Then, the appropriate Ti-base height for the OT-Bridge system was selected for each position (Figure 7a,b).
- A provisional prosthesis composed of a thermosetting resin reinforced with a multidirectional glass fiber framework (Trilor Arch, Bioloren, Saronno, Italy) covered by a PMMA esthetic coverage (BreCam Multicom, Bredent srl, Bolzano, Italy) was digitally designed and produced using a five-axis milling machine (PrograMill PM7, Ivoclar Vivadent, Bolzano, Italy) (Figure 8a,b). The extragrade abutments were cemented manually in the framework using a paste-paste resin-modified glass ionomer luting cement self-mixed with cartridge (FujiCEM 2, GC, Tokio, Japan). The white acetalic Seegers were inserted in the extragrade abutment undercuts and the prosthesis was then sent to the clinician (Figure 9a,b).
- A 3D-printed surgical mucosa and tooth-supported template was digitally designed and produced (RealGuide 3Diemme, Como, Italy). This was supported by the two contralateral distal molars and was provided with three labial pin holes.
- The surgical template was positioned in the upper maxilla using the tooth-supported parts and then stabilized by inserting three vestibular pins in the bone (Figure 10).
- Seven tapered implants (Naturactis LYRA ETK, Paris, France) were inserted on the upper maxilla in a flapless surgery, as planned (Figure 11a). The implant paths were prepared using a dedicated static guided surgery kit (ETK Implant Guide, LYRA ETK, Paris, France). Implants were manually inserted in an alternate way and by screwing and unscrewing movements before the final positioning. All of the implants showed final peak insertion torque values between 25 and 30 Ncm. OT-Equator attachments were mounted on implants (Figure 11b) and then the prosthesis was placed on them.
- Clinical and radiographic checks of the passive fit of the prosthesis were performed (Figure 12a–c).
3. Discussion
Author Contributions
Funding
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Maló, P.; Rangert, B.; Nobre, M. “All-on-Four” Immediate-Function Concept with Brånemark System® Implants for Completely Edentulous Mandibles: A Retrospective Clinical Study. Clin. Implant Dent. Relat. Res. 2003, 5, 2–9. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Cai, M.; Yang, J.; Aldhohrah, T.; Wang, Y. Immediate versus early or conventional loading dental implants with fixed prostheses: A systematic review and meta-analysis of randomized controlled clinical trials. J. Prosthet. Dent. 2019, 122, 516–536. [Google Scholar] [CrossRef] [PubMed]
- De Bruyn, H.; Raes, S.; Östman, P.-O.; Cosyn, J. Immediate loading in partially and completely edentulous jaws: A review of the literature with clinical guidelines. Periodontology 2000 2014, 66, 153–187. [Google Scholar] [CrossRef]
- Paleari, A.G.; Presoto, C.D.; Vasconcelos, J.A.; dos Nunes Reis, J.M.S.; Pinelli, L.A.P.; Tavares da Silva, R.H.B.; Quishida, C.C.C. An Alternative Technique for Fabrication of Frameworks in an Immediate Loading Implant Fixed Mandibular Prosthesis. Case Rep. Dent. 2015, 2015, 102189. [Google Scholar] [CrossRef]
- Pellegrino, G.; Basile, F.; Relics, D.; Ferri, A.; Grande, F.; Tarsitano, A.; Marchetti, C. Computer-Aided Rehabilitation Supported by Zygomatic Implants: A Cohort Study Comparing Atrophic with Oncologic Patients after Five Years of Follow-Up. J. Clin. Med. 2020, 9, 3254. [Google Scholar] [CrossRef]
- Pellegrino, G.; Grande, F.; Ferri, A.; Pisi, P.; Gandolfi, M.G.; Marchetti, C. Three-Dimensional Radiographic Evaluation of the Malar Bone Engagement Available for Ideal Zygomatic Implant Placement. Methods Protoc. 2020, 3, 52. [Google Scholar] [CrossRef]
- Sahin, S.; Çehreli, M.C. The Significance of Passive Framework Fit in Implant Prosthodontics: Current Status. Implant Dent. 2001, 10, 85–92. [Google Scholar] [CrossRef]
- Bousquet, P.; Carayon, D.; Durand, J.-C. Using the “One Shot” Concept for Immediate Loading Implant Protocol in Edentulous Patient Rehabilitation with a Fixed Prosthesis: A 6-Year Follow-Up. Case Rep. Dent. 2021, 2021, 8872277. [Google Scholar] [CrossRef]
- Strub, J.R.; Jurdzik, B.A.; Tuna, T. Prognosis of immediately loaded implants and their restorations: A systematic literature review: Prognosis of immediately loaded implants and restorations. J. Oral Rehabil. 2012, 39, 704–717. [Google Scholar] [CrossRef]
- Mobilio, N.; Fasiol, A.; Catapano, S. Survival Rates of Lithium Disilicate Single Restorations: A Retrospective Study. Int. J. Prosthodont. 2018, 31, 283–286. [Google Scholar] [CrossRef]
- Mobilio, N.; Catapano, S. The use of monolithic lithium disilicate for posterior screw-retained implant crowns. J. Prosthet. Dent. 2017, 118, 703–705. [Google Scholar] [CrossRef] [PubMed]
- Grande, F.; Mochi Zamperoli, E.; Pozzan, M.C.; Tesini, F.; Catapano, S. Qualitative Evaluation of the Effects of Professional Oral Hygiene Instruments on Prosthetic Ceramic Surfaces. Materials 2021, 15, 21. [Google Scholar] [CrossRef] [PubMed]
- Baldissara, P.; Koci, B.; Messias, A.M.; Meneghello, R.; Ghelli, F.; Gatto, M.R.; Ciocca, L. Assessment of impression material accuracy in complete-arch restorations on four implants. J. Prosthet. Dent. 2021, 126, 763–771. [Google Scholar] [CrossRef] [PubMed]
- Celeghin, G.; Franceschetti, G.; Mobilio, N.; Fasiol, A.; Catapano, S.; Corsalini, M.; Grande, F. Complete-Arch Accuracy of Four Intraoral Scanners: An In Vitro Study. Healthcare 2021, 9, 246. [Google Scholar] [CrossRef] [PubMed]
- Kreulen, C.M.; Wolke, J.G.C.; de Baat, C.; Creugers, N.H.J. Attaching single- and multi-unit fixed dental prostheses. Ned. Tijdschr. Voor Tandheelkd. 2013, 120, 633–640. [Google Scholar] [CrossRef]
- Hamilton, A.; Jamjoom, F.Z.; Alnasser, M.; Starr, J.R.; Friedland, B.; Gallucci, G.O.; Bdsc, D.A.H.; Bds, M.F.Z.J.; Starr, M.J.R.; BChD, M.B.F.; et al. Tilted versus axial implant distribution in the posterior edentulous maxilla: A CBCT analysis. Clin. Oral Implant. Res. 2021, 32, 1357–1365. [Google Scholar] [CrossRef]
- Pozzan, M.C.; Grande, F.; Mochi Zamperoli, E.; Tesini, F.; Carossa, M.; Catapano, S. Assessment of Preload Loss after Cyclic Loading in the OT Bridge System in an “All-on-Four” Rehabilitation Model in the Absence of One and Two Prosthesis Screws. Materials 2022, 15, 1582. [Google Scholar] [CrossRef]
- Catapano, S.; Ferrari, M.; Mobilio, N.; Montanari, M.; Corsalini, M.; Grande, F. Comparative Analysis of the Stability of Prosthetic Screws under Cyclic Loading in Implant Prosthodontics: An In Vitro Study. Appl. Sci. 2021, 11, 622. [Google Scholar] [CrossRef]
- Ceruti, P.; Mobilio, N.; Bellia, E.; Borracchini, A.; Catapano, S.; Gassino, G. Simplified edentulous treatment: A multicenter randomized controlled trial to evaluate the timing and clinical outcomes of the technique. J. Prosthet. Dent. 2017, 118, 462–467. [Google Scholar] [CrossRef]
- Ceraulo, S.; Leonida, A.; Lauritano, D.; Baldoni, A.; Longoni, S.; Baldoni, M.; Caccianiga, G. Proposal for a Clinical Approach to Geriatric Patients with Anchor Need on Implant for Removable Denture: New Technique. Prosthesis 2020, 2, 185–195. [Google Scholar] [CrossRef]
- Ortensi, L.; Fisichella, M.L.; Ortensi, M.; Grande, F.; Pellegrino, G.; Ferri, A.; LA Rosa, G.R.; Pedullà, E. A comparison of accuracy between three different facial detection systems for prosthodontic esthetic preview: A single-blinded in vitro study. Minerva Dent. Oral Sci. 2021. [Google Scholar] [CrossRef] [PubMed]
- Ortensi, L.; Ortensi, M.; Minghelli, A.; Grande, F. Implant-Supported Prosthetic Therapy of an Edentulous Patient: Clinical and Technical Aspects. Prosthesis 2020, 2, 140–152. [Google Scholar] [CrossRef]
- Lorenzetti, M.; Lorenzetti, V.; Carossa, M.; Cavagnetto, D.; Mussano, F. Using a Preoperative Scan Digital Impression and a Digital Index to Build Immediate Interim Full-Arch Implant-Supported Prosthesis. A Case Report and Proof of Concept. Appl. Sci. 2021, 11, 996. [Google Scholar] [CrossRef]
- Ortensi, L.; Sigari, G.; La Rosa, G.R.M.; Ferri, A.; Grande, F.; Pedullà, E. Digital planning of composite customized veneers using Digital Smile Design: Evaluation of its accuracy and manufacturing. Clin. Exp. Dent. Res. 2022, 8, 537–543. [Google Scholar] [CrossRef] [PubMed]
- Mobilio, N.; Fasiol, A.; Mollica, F.; Catapano, S. Effect of Different Luting Agents on the Retention of Lithium Disilicate Ceramic Crowns. Materials 2015, 8, 1604–1611. [Google Scholar] [CrossRef]
- Kero, T.; Pettersson, A.; Fäldt, J.; Andersson, M.; Gillot, L.; Cannas, B.; Nässtrom, K.; Söderberg, R. Virtual variation simulation of CAD/CAM template-guided surgeries performed on human cadavers: Part II. J. Prosthet. Dent. 2010, 104, 48–55. [Google Scholar] [CrossRef]
- Landázuri-Del Barrio, R.A.; Cosyn, J.; De Paula, W.N.; De Bruyn, H.; Marcantonio, E. A prospective study on implants installed with flapless-guided surgery using the all-on-four concept in the mandible. Clin. Oral Implant. Res. 2013, 24, 428–433. [Google Scholar] [CrossRef]
- Tahmaseb, A.; Wismeijer, D.; Coucke, W.; Derksen, W. Computer Technology Applications in Surgical Implant Dentistry: A Systematic Review. Int. J. Oral Maxillofac. Implant. 2014, 29, 25–42. [Google Scholar] [CrossRef]
- Cervino, G.; Cicciù, M.; Fedi, S.; Milone, D.; Fiorillo, L. FEM Analysis Applied to OT Bridge Abutment with Seeger Retention System. Eur. J. Dent. 2021, 15, 047–053. [Google Scholar] [CrossRef]
- Montanari, M.; Tallarico, M.; Vaccaro, G.; Ferrari, E.; Scrascia, R.; Ortensi, L.; Cicciù, M.; Meloni, S.M.; Lumbau, A.I.; Avrampou, M.; et al. Two Years after Loading Performance of Implant-Supported Overdenture with Metal Bar and Low-Profile Attachments: A Prospective Case Series Multicenter Clinical Study. Int. J. Dent. 2020, 2020, 8830722. [Google Scholar] [CrossRef]











Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Piscopo, M.; Grande, F.; Catapano, S. Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report. Prosthesis 2022, 4, 213-223. https://doi.org/10.3390/prosthesis4020021
Piscopo M, Grande F, Catapano S. Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report. Prosthesis. 2022; 4(2):213-223. https://doi.org/10.3390/prosthesis4020021
Chicago/Turabian StylePiscopo, Marco, Francesco Grande, and Santo Catapano. 2022. "Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report" Prosthesis 4, no. 2: 213-223. https://doi.org/10.3390/prosthesis4020021
APA StylePiscopo, M., Grande, F., & Catapano, S. (2022). Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report. Prosthesis, 4(2), 213-223. https://doi.org/10.3390/prosthesis4020021







