Resin-Bonded Prosthesis in Posterior Area to Prevent Early Marginal Bone Resorption in Implants Placed at Tissue Level
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Setting and Patient Selection
2.2. Inclusion Criteria
- -
- 18–75 years of age;
- -
- Presence of a single hopeless tooth which required extraction;
- -
- Possibility to be included in a hygiene recall program at 1, 3 and 12 months;
- -
- The site should allow the placement of an implant at least 10.00 mm in length;
- -
- And 3.8 mm in diameter.
2.3. Exclusion Criteria
- -
- Medical and/or general contraindications for the surgical procedures (ASA score ≥ 3);
- -
- Systemic diseases such as uncontrolled diabetes mellitus;
- -
- Pregnancy;
- -
- Poor oral hygiene and lack of motivation;
- -
- Active clinical periodontal disease in the natural dentition expressed by probing pocket depth >4 mm and bleeding on probing;
- -
- Smoking;
- -
- Malocclusion (i.e., closed bite or open bite);
- -
- Bisphosphonate and/or antidepressant therapy.
2.4. Sample Size
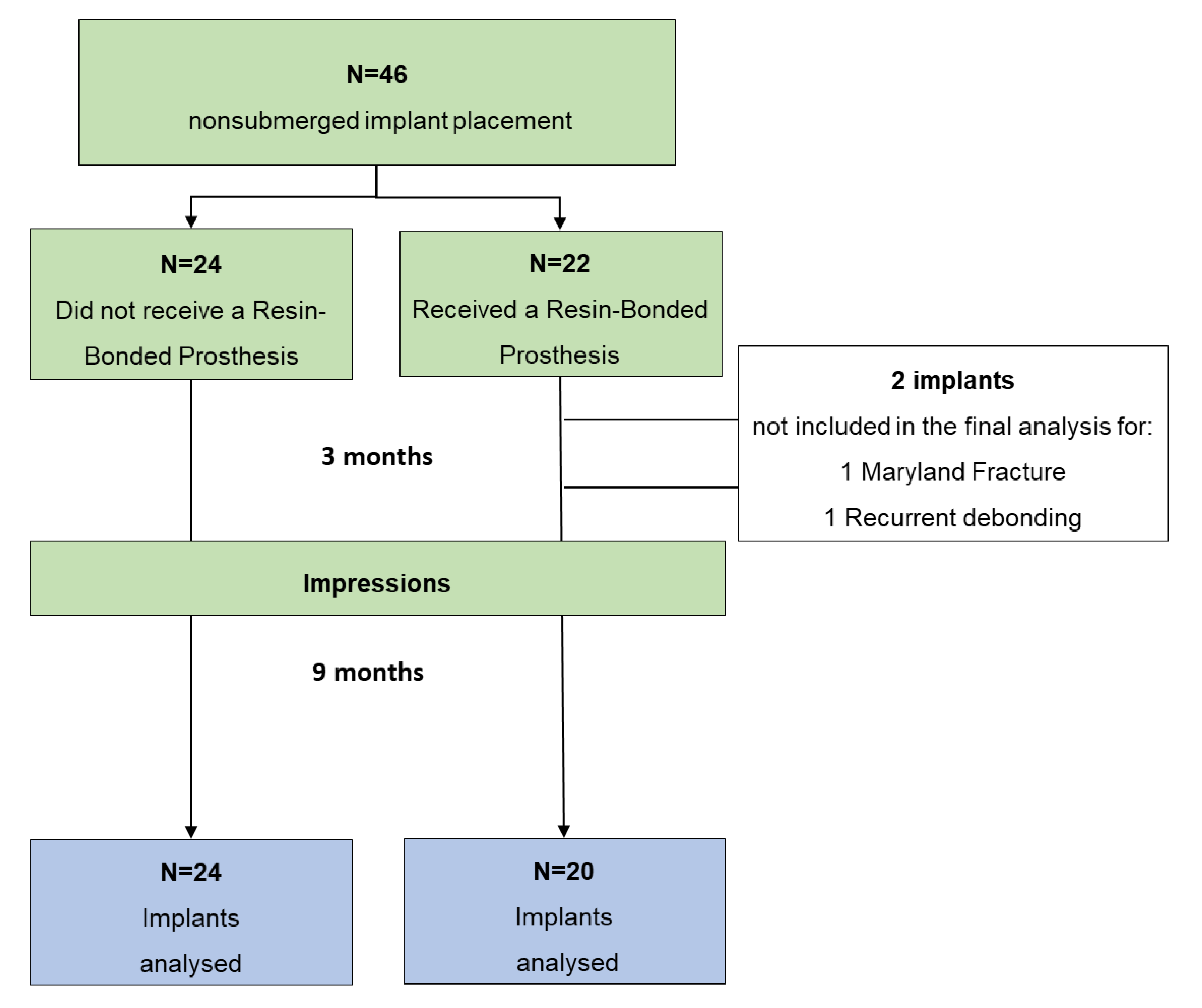
2.5. Patients Allocation and Pre-Surgical Protocol
2.6. Implant Surgery
- -
- Early implant group (Type 2 for ITI): the implant was placed 8–12 weeks after extraction. In this case, the hopeless tooth was previously removed because affected by acute periapical lesion with endodontic abscess. These teeth presented fistula, tenderness and swelling before extraction. In some cases, antibiotic therapy was scheduled 3–7 days before extraction.
- -
- Delayed implant group (Type 4 for ITI): the implant was placed in the edentulous area where cortical bone was evident on the radiograph. Tooth extraction, for any reason, was performed 10–12 months before.
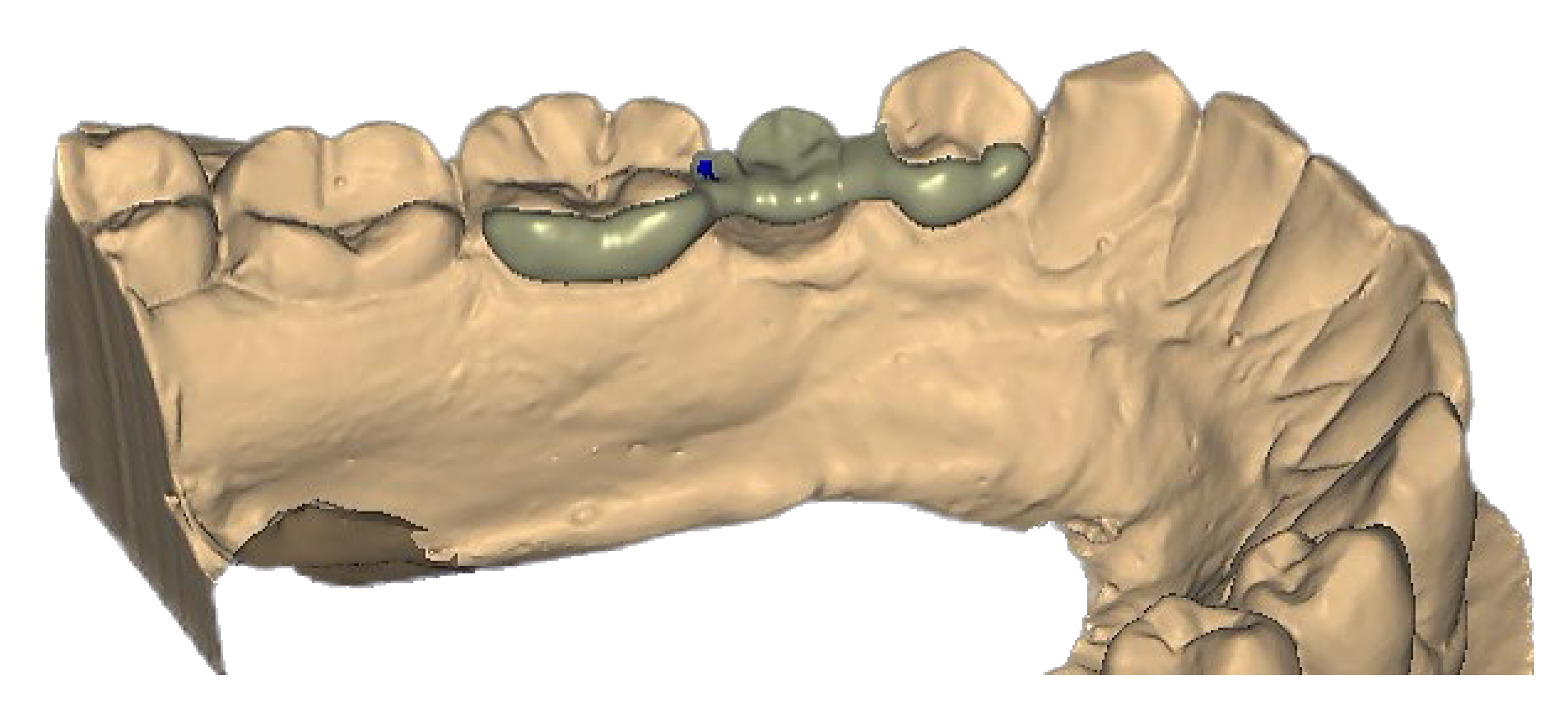
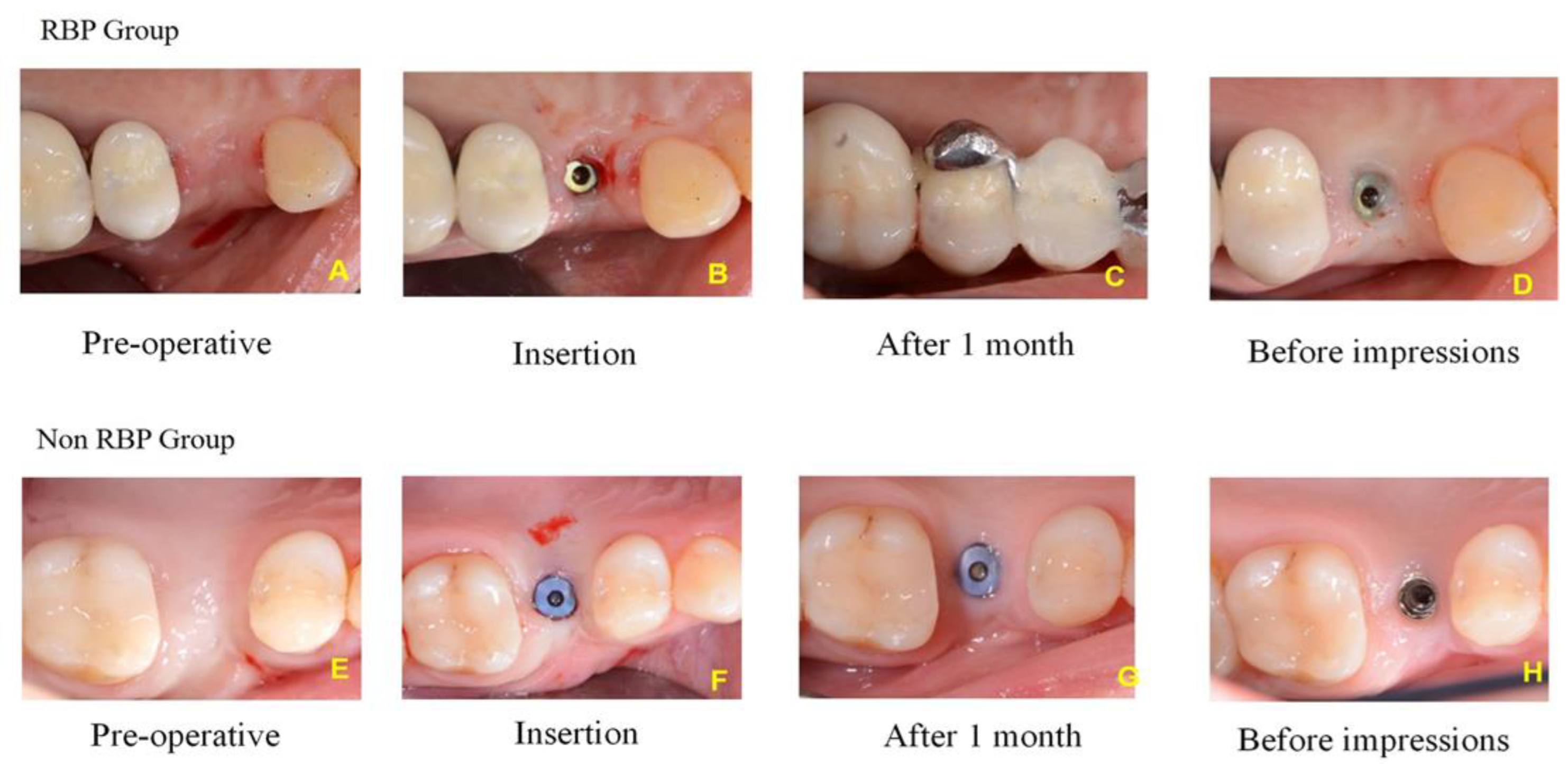
2.7. Resin-Bonded Prosthesis (RBP) Positioning
2.8. Follow-Up
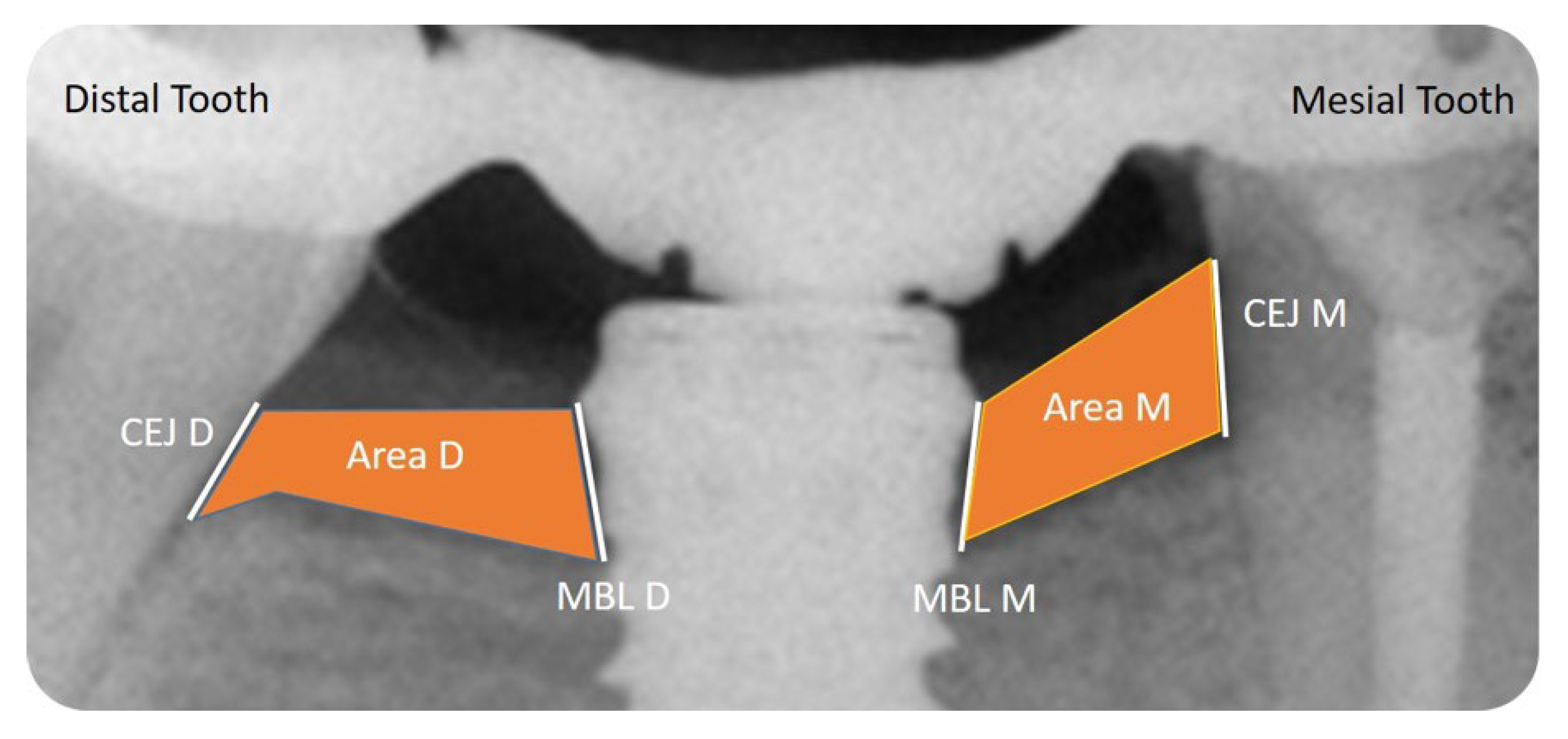
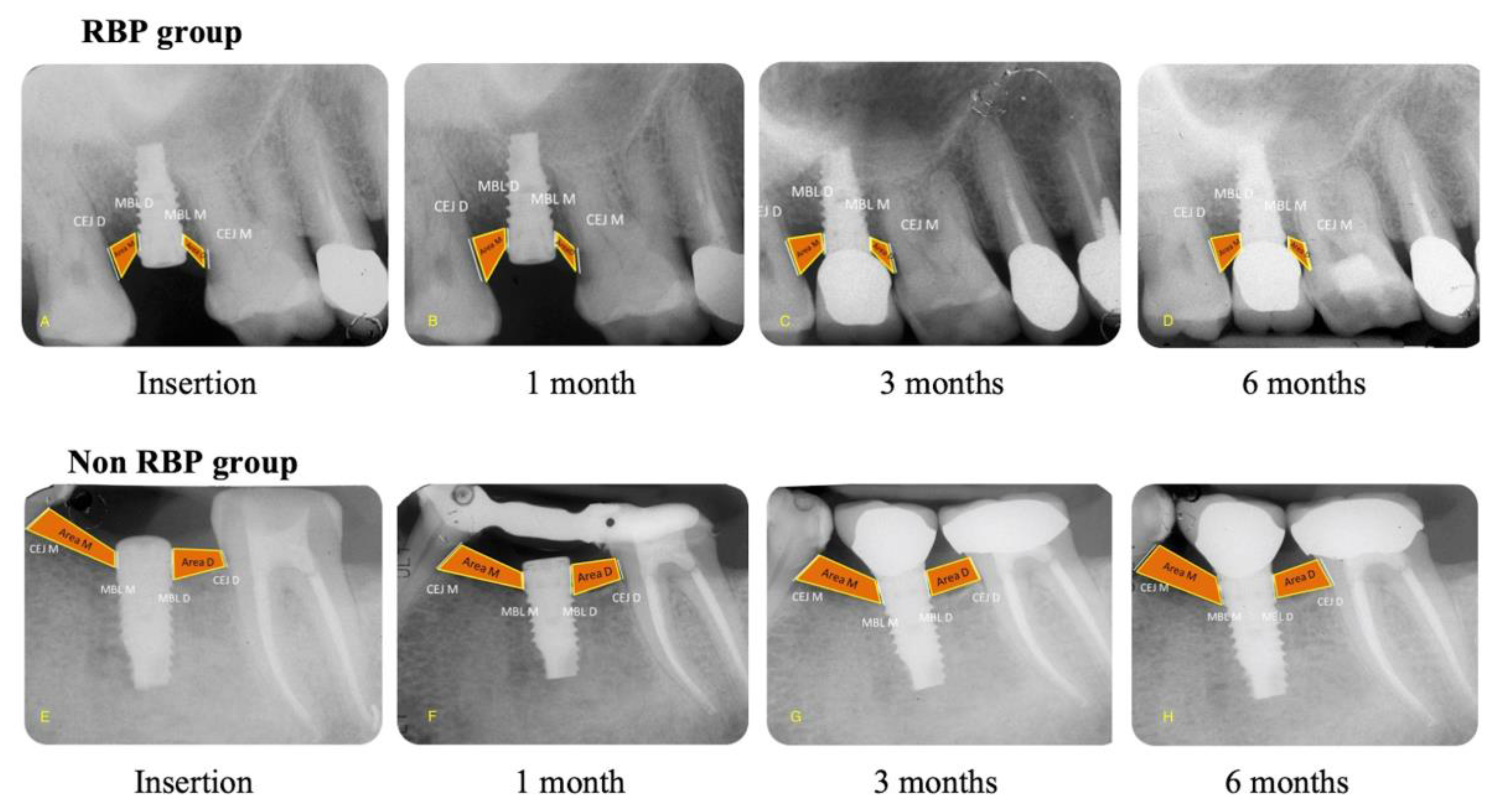
2.9. Radiographic Evaluation
- -
- Mesial and Distal Marginal Bone Levels (MBL-M and MBL-D)
- -
- Mesial and Distal Cement–Enamel Junction (CEJ-M and CEJ-D)
- -
- Mesial and Distal Bone Level Area (Area-M and Area-D)
2.10. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Crespi, R.; Capparé, P.; Polizzi, E.; Gherlone, E. Fresh-Socket Implants of Different Collar Length: Clinical Evaluation in the Aesthetic Zone. Clin. Implant Dent. Relat. Res. 2016, 17, 871–878. [Google Scholar] [CrossRef]
- Hermann, J.S.; Jones, A.A.; Bakaeen, L.G.; Buser, D.; Schoolfield, J.D.; Cochran, D.L. Influence of a Machined Collar on Crestal Bone Changes Around Titanium Implants: A Histometric Study in the Canine Mandible. J. Periodontol. 2011, 82, 1329–1338. [Google Scholar] [CrossRef]
- Valles, C.; Rodríguez-Ciurana, X.; Nart, J.; Santos, A.; Galofre, M.; Tarnow, D. Influence of Implant Neck Surface and Placement Depth on Crestal Bone Changes Around Platform-Switched Implants: A Clinical and Radiographic Study in Dogs. J. Periodontol. 2017, 88, 1200–1210. [Google Scholar] [CrossRef]
- Flores-Guillen, J.; Álvarez-Novoa, C.; Barbieri, G.; Martín, C.; Sanz, M. Five-year outcomes of a randomized clinical trial comparing bone-level implants with either submerged or transmucosal healing. J. Clin. Periodontol. 2018, 45, 125–135. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nickening, H.J.; Wichmann, M.; Schlegel, K.A.; Nkenke, E.; Eiter, S. Radiographic evaluation of marginal bone levels during healing period, adjacent to parallel-screw cilynder implants inserted in the posterior zone of the jaws, placed with flapless surgery. Clin. Oral Impl. Res. 2010, 21, 1386–1393. [Google Scholar] [CrossRef] [PubMed]
- Chrcanovic, B.R.; Albrektsson, T.; Wennerberg, A. Dental implants inserted in fresh extraction sockets versus healed sites: A systematic review and meta-analysis. J. Dent. 2015, 43, 16–41. [Google Scholar] [CrossRef] [PubMed]
- Prati, C.; Zamparini, F.; Scialabba, V.S.; Gatto, M.R.; Piattelli, A.; Montebugnoli, L.; Gandolfi, M.G. A 3-Year Prospective Cohort Study on 132 Calcium Phosphate-Blasted Implants: Flap vs Flapless Technique. Int. J. Oral Maxillofac. Implant. 2016, 31, 413–423. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Berglundh, T.; Abrahamsson, I.; Welander, M.; Lang, N.P.; Lindhe, J. Morphogenesis of the peri-implant mucosa: An experimental study in dogs. Clin. Oral Implant. Res. 2007, 18, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Baffone, G.M.; Botticelli, D.; Pereira, F.P.; Favero, G.; Schweikert, M.; Lang, N.P. Influence of buccal bony crest width on marginal dimensions of peri-implant hard and soft tissues after implant installation. An experimental study in dogs. Clin. Oral Implant. Res. 2012, 24, 250–254. [Google Scholar] [CrossRef] [PubMed]
- Cecchinato, D.; Olsson, C.; Lindhe, J. Submerged or non-submerged healing of endosseous implants to be used in the rehabilitation of partially dentate patients. J. Clin. Periodontol. 2004, 31, 299–308. [Google Scholar] [CrossRef] [PubMed]
- Abrahamsson, I.; Berglundh, T.; Moon, I.-S.; Lindhe, J. Peri-implant tissues at submerged and non-submerged titanium implants. J. Clin. Periodontol. 1999, 26, 600–607. [Google Scholar] [CrossRef]
- Galindo-Moreno, P.; León-Cano, A.; Ortega-Oller, I.; Monje, A.; O′valle, F.; Catena, A. Marginal bone loss as success criterion in implant dentistry: Beyond 2 mm. Clin. Oral Implant. Res. 2014, 26, e28–e34. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Poggio, C.E.; Salvato, A. Bonded provisional restorations for esthetic soft tissue support in single-implant treatment. J. Prosthet. Dent. 2002, 87, 688–691. [Google Scholar] [CrossRef] [PubMed]
- Siadat, H.; Alikhasi, M.; Beyabanaki, E. Interim Prosthesis Options for Dental Implants. J. Prosthodont. 2016, 26, 331–338. [Google Scholar] [CrossRef]
- Trindade, R.; Albrektsson, T.; Galli, S.; Prgomet, Z.; Tengvall, P.; Wennerberg, A. Osseointegration and foreign body reaction: Titanium implants activate the immune system and suppress bone resorption during the first 4 weeks after implantation. Clin. Implant Dent. Relat. Res. 2018, 20, 82–91. [Google Scholar] [CrossRef] [PubMed]
- Albrektsson, T.; Dahlin, C.; Jemt, T.; Sennerby, L.; Turri, A.; Wennerberg, A. Is marginal bone loss around oral implants the result of a provoked foreign body reaction? Clin. Implant Dent. Relat. Res. 2014, 16, 155–165. [Google Scholar] [CrossRef] [PubMed]
- Catapano, S.; Ortensi, L.; Mobilio, N.; Grande, F. The New Elderly Patient: A Necessary Upgrade. Prosthesis 2021, 3, 99–104. [Google Scholar] [CrossRef]
- Azizi, A.; Zamparini, F.; Spinelli, A.; Pirani, C.; Gandolfi, M.G.; Prati, C. Maryland-bridge application as a suitable technique to preserve marginal bone level of not-submerged supracrestal implants. Minerva Stomatol. 2020, 69, 335–342. [Google Scholar] [CrossRef]
- World Medical Association Declaration of Helsinki: Ethical principles for medical research involving human subjects. JAMA 2013, 310, 2191–2194. [CrossRef] [Green Version]
- Moher, D.; Hopewell, S.; Schulz, K.F.; Montori, V.; Gøtzsche, P.C.; Devereaux, P.J.; Elbourne, D.; Egger, M.; Altman, D.G. CONSORT 2010 Explanation and Elaboration: Updated guidelines for reporting parallel group randomised trials. BMJ 2010, 340, c869. [Google Scholar] [CrossRef]
- Dodson, T.B. A guide for preparing a patient-oriented research manuscript. Oral Surgery, Oral Med. Oral Pathol. Oral Radiol. Endodontology 2007, 104, 307–315. [Google Scholar] [CrossRef] [PubMed]
- Praça, L.D.F.G.; Teixeira, R.C.; Rego, R. Influence of abutment disconnection on peri-implant marginal bone loss: A randomized clinical trial. Clin. Oral Implant. Res. 2020, 31, 341–351. [Google Scholar] [CrossRef] [PubMed]
- Hämmerle, C.H.; Chen, S.T.; Wilson, T.G., Jr. Consensus statements and recommended clinical procedures regarding the placement of implants in extraction sockets. Int. J. Oral Maxillofac. Implant. 2004, 19, 26–28. [Google Scholar]
- Taxel, P.; Ortiz, D.; Shafer, D.; Pendrys, D.; Reisine, S.; Rengasamy, K.; Freilich, M. The relationship between implant stability and bone health markers in post-menopausal women with bisphosphonate exposure. Clin. Oral Investig. 2013, 18, 49–57. [Google Scholar] [CrossRef]
- Prati, C.; Zamparini, F.; Pirani, C.; Montebugnoli, L.; Canullo, L.; Gandolfi, M.G. A Multilevel Analysis of Platform-Switching Flapless Implants Placed at Tissue Level: 4-year Prospective Cohort Study. Int. J. Oral Maxillofac. Implant. 2020, 35, 330–341. [Google Scholar] [CrossRef]
- Rogers, W.H. Regression standard errors in clustered samples. Stata Tech. Bull. 1993, 13, 19–23. [Google Scholar]
- Bielemann, A.M.; Marcello-Machado, R.M.; Del Bel Cury, A.A.; Faot, F. Systematic review of wound healing biomarkers in peri-implant crevicular fluid during osseointegration. Arch. Oral Biol. 2018, 89, 107–128. [Google Scholar] [CrossRef]
- Tomasi, C.; Tessarolo, F.; Caola, I.; Wennström, J.; Nollo, G.; Berglundh, T. Morphogenesis of peri-implant mucosa revisited: An experimental study in humans. Clin. Oral Implant. Res. 2014, 25, 997–1003. [Google Scholar] [CrossRef]
- Odriguez Ciurana, X.; Navajas Acedo, A.; Vela, X.; Jimenez Garcia, J. Arrangement of peri-implant connective tissue fibers around platform-switching implant with conical abutment and its relationship to the underlying bone: A human histologic study. Int. J. Periodontics Restor. Dent 2016, 36, 533–540. [Google Scholar] [CrossRef] [Green Version]
- Rugger, A.; Franchi, M.; Marini, N.; Trisi, P.; Piattelli, A. Supracrestal circular collagen fiber network around osseointegrated nonsubmerged titanium implants. Clin. Oral Implant. Res. 1992, 3, 169–175. [Google Scholar] [CrossRef]
- Abrahamsson, I.; Berglundh, T.; Wennström, J.; Lindhe, J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin. Oral Implant. Res. 1996, 7, 212–219. [Google Scholar] [CrossRef] [PubMed]
- Van Steenberghe, D.; Naert, I.; Jacobs, R.; Quirynen, M. Influence of Inflammatory Reactions Vs. Occlusal Loading On Peri-Implant Marginal Bone Level. Adv. Dent. Res. 1999, 13, 130–135. [Google Scholar] [CrossRef] [PubMed]
- Gandolfi, M.G.; Zamparini, F.; Iezzi, G.; Degidi, M.; Botticelli, D.; Piattelli, A.; Prati, C. Microchemical and Micromorphologic ESEM-EDX Analysis of Bone Mineralization at the Thread Interface in Human Dental Implants Retrieved for Mechanical Complications After 2 Months to 17 Years. Int. J. Periodontics Restor. Dent. 2018, 38, 431–441. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yonezawa, D.; Piattelli, A.; Favero, R.; Ferri, M.; Iezzi, G.; Botticelli, D. Bone Healing at Functionally Loaded and Unloaded Screw-Shaped Implants Supporting Single Crowns: A Histomorphometric Study in Humans. Int. J. Oral Maxillofac. Implant. 2018, 33, 181–187. [Google Scholar] [CrossRef] [Green Version]
- Prati, C.; Zamparini, F.; Botticelli, D.; Ferri, M.; Yonezawa, D.; Piattelli, A.; Gandolfi, M.G. The Use of ESEM-EDX as an Innovative Tool to Analyze the Mineral Structure of Peri-Implant Human Bone. Materials 2020, 13, 1671. [Google Scholar] [CrossRef] [Green Version]
- Shah, F.A.; Ruscsák, K.; Palmquist, A. 50 years of scanning electron microscopy of bone—A comprehensive overview of the important discoveries made and insights gained into bone material properties in health, disease, and taphonomy. Bone Res. 2019, 22, 7–15. [Google Scholar] [CrossRef] [Green Version]
- Franchi, M.; Bacchelli, B.; Martini, D.; Pasquale, V.; Orsini, E.; Ottani, V.; Fini, M.; Giavaresi, G.; Giardino, R.; Ruggeri, A. Early detachment of titanium particles from various different surfaces of endosseous dental implants. Biomaterials 2003, 25, 2239–2246. [Google Scholar] [CrossRef]
- Franchi, M.; Fini, M.; Martini, D.; Orsini, E.; Leonardi, L.; Ruggeri, A.; Giavaresi, G.; Ottani, V. Biological fixation of endosseous implants. Micron 2005, 36, 665–671. [Google Scholar] [CrossRef]
| Parameters | RBP n (%) | Non-RBP n (%) | Total n (%) | |
|---|---|---|---|---|
| Gender | Males Females | 11 (25) 9 (20) | 13 (30) 11 (25) | 24 (55) 20 (45) |
| Age | <55 ≥55 | 12 (27) 8 (18) | 13 (30) 11 (25) | 25 (57) 19 (43) |
| Implant location | Maxilla Mandibular | 11 (25) 9 (20) | 12 (27) 12 (27) | 23 (53) 21 (47) |
| Implant placement timing | Early Delayed | 8 (16) 12 (27) | 11(25) 13 (29) | 19 (44) 25 (56) |
| Diameter | 3.8 4.25 5 | 5 (12) 10 (22) 5 (12) | 12 (27) 11 (25) 1 (2) | 17 (39) 21 (47) 6 (14) |
| Endo | Both vital Mesial vital Distal vital Non vital | 4 (9) 7 (16) 7 (16) 2 (6) | 14 (32) 2 (6) 5 (12) 3 (7) | 18 (41) 9 (20) 12 (27) 5 (12) |
| Total | 20 (45) | 24 (55) | 44 (100) |
| T1 | T3 | T12 | ||||
|---|---|---|---|---|---|---|
| RBP | Non-RBP | RBP | Non-RBP | RBP | Non-RBP | |
| MBL-M | 0.03 ± 0.14 aA | −0.18 ± 0.18 aA | −0.01 ± 0.24 aA | −0.36 ± 0.41 aB | −0.07 ± 0.41 aA | −0.70 ± 0.52 aB |
| MBL-D | −0.05 ± 0.17 aA | −0.21 ± 0.26 aA | −0.08 ± 0.23 aA | −0.36 ± 0.45 aB | −0.20 ± 0.40 aA | −0.81 ± 0.51 aB |
| CEJ-M | 0.01 ± 0.29 aA | −0.12 ± 0.29 aA | −0.01 ± 0.40 aA | −0.20 ± 0.35 aB | −0.08 ± 0.61 aA | −0.48 ± 0.47 aA |
| CEJ-D | 0.02 ± 0.24 aA | −0.14 ± 0.22 aA | −0.01 ± 0.29 aA | −0.30 ± 0.25 aA | −0.04 ± 0.46 aA | −0.65 ± 0.36 aA |
| Area M | −0.17 ± 0.05 aA | −0.23 ± 0.16 aA | −0.30 ± 0.06 aA | −0.13 ± 0.28 aB | −0.43 ± 0.14 aA | −0.27 ± 0.32 aA |
| Area D | −0.07 ± 0.09 aA | −0.03 ± 0.20 aA | −0.13 ± 0.13 aA | −0.16 ± 0.33 aA | −0.35 ± 0.10 aA | −0.16 ± 0.38 aB |
| T1 | T3 | T12 | |||||
|---|---|---|---|---|---|---|---|
| Parameters | RBP | Non-RBP | RBP | Non-RBP | RBP | Non-RBP | |
| Gender | Males Females | −0.05 ± 0.14 0.07 ± 0.26 | −0.16 ± 0.29 −0.25 ± 0.18 | −0.04 ± 0.24 −0.03 ± 0.41 | −0.29 ± 0.26 −0.43 ± 0.45 | −0.07 ± 0.05 −0.24 ± 0.18 | −0.44 ± 0.45 −0.54 ± 0.61 |
| Age | <55 ≥55 | −0.05 ± 0.14 −0.01 ± 0.26 | −0.18 ± 0.06 −0.12 ± 0.06 | −0.07 ± 0.18 −0.04 ± 0.14 | −0.44 ± 0.29 −0.35 ± 0.22 | −0.05 ± 0.26 −0.19 ± 0.09 | −0.90 ± 0.18 −0.78 ± 0.45 |
| Implant location | Maxilla Mandibular | −0.06 ± 0.09 −0.07 ± 0.26 | −0.17 ± 0.24 −0.20 ± 0.05 | −0.01 ± 0.09 −0.12 ± 0.26 | −0.41 ± 0.24 −0.31± 0.13 | −0.12 ± 0.05 −0.15 ± 0.14 | −0.61 ± 0.38 −0.80 ± 0.23 |
| Implant placement timing | Early Delayed | 0.01 ± 0.14 0.03 ± 0.24 | −0.13 ± 0.40 −0.14 ± 0.23 | −0.06 ± 0.06 0.00 ± 0.26 | −0.51 ± 0.45 −0.23 ± 0.38 | −0.36 ± 0.41 −0.02 ± 0.05 | −0.56 ± 0.36 −0.38 ± 0.38 |
| Diameter | 3.8 4.25 5 | 0.05 ± 0.22 −0.02 ± 0.06 −0.07 ± 0.23 | −0.18 ± 0.29 −0.19 ± 0.29 −0.12 ± 0.09 | −0.07 ± 0.06 −0.04 ± 0.14 −0.15 ± 0.05 | −0.26 ± 0.24 −0.48 ± 0.26 −0.40± 0.09 | −0.30 ± 0.13 −0.06 ± 0.61 0.40 ± 0.06 | −0.56 ± 0.40 −0.86 ± 0.18 −0.35 ± 0.41 |
| Teeth Endo status | Both vital Mesial vital Distal vital Non vital | −0.03 ± 0.14 0.10 ± 0.05 0.11 ± 0.09 −0.10 ± 0.13 | −0.16 ± 0.23 −0.30 ± 0.24 −0.45 ± 0.29 −0.06 ± 0.06 | 0.09 ± 0.22 −0.03 ± 0.26 0.05 ± 0.14 −0.30± 0.35 | −0.32 ± 0.40 −0.56 ± 0.45 −0.72 ± 0.29 −0.06 ± 0.61 | −0.03 ± 0.14 0.16 ± 0.29 −0.13 ± 0.24 −0.20 ± 0.36 | −0.65 ± 0.29 −0.68 ± 0.61 −0.88 ± 0.35 −0.20 ± 0.38 |
| Total | −0.01 ± 0.14 | −0.20 ± 0.18 | −0.04 ± 0.24 | −0.36 ± 0.41 | −0.13 ± 0.41 | −0.75 ± 0.52 | |
| T1 | T3 | T12 | |||||
|---|---|---|---|---|---|---|---|
| Parameters | RBP | Non RBP | RBP | Non RBP | RBP | Non RBP | |
| Gender | Males Females | −0.15 ± 0.29 −0.12 ± 0.31 | −0.20 ± 0.29 −0.04 ± 0.20 | −0.20 ± 0.35 −0.20 ± 0.36 | −0.14 ± 0.36 −0.14 ± 0.35 | −0.40 ± 0.47 −0.34 ± 0.51 | −0.25 ± 0.48 −0.20 ± 0.47 |
| Age | <55 ≥55 | −0.01 ± 0.01 −0.16 ± 0.29 | −0.12 ± 0.19 −0.14 ± 0.28 | 0.05 ± 0.37 −0.25 ± 0.36 | −0.15 ± 0.20 −0.16 ± 0.36 | 0.07 ± 0.52 −0.47 ± 0.47 | −0.15 ± 0.37 −0.25 ± 0.48 |
| Implant location | Maxilla Mandibular | −0.14 ± 0.29 −0.18 ± 0.31 | −0.18 ± 0.28 −0.06 ± 0.29 | −0.21 ± 0.35 −0.23 ± 0.36 | −0.24 ± 0.35 −0.06 ± 0.35 | −0.42 ± 0.47 −0.36 ± 0.51 | −0.29 ± 0.46 −0.15 ± 0.49 |
| Implant placement timing | Early Delayed | −0.31 ± 0.35 −0.11 ± 0.28 | −0.03 ± 0.35 −0.06 ± 0.28 | −0.41 ± 0.46 −0.23 ± 0.35 | 0.03 ± 0.42 −0.02 ± 0.35 | −0.51 ± 0.66 −0.33 ± 0.48 | −0.31 ± 0.54 −0.12 ± 0.47 |
| Diameter | 3.8 4.25 5 | −0.27 ± 0.32 −0.02 ± 0.28 −0.12 ± 0.31 | −0.19 ± 0.30 −0.02 ± 0.28 −0.15 ± 0.24 | −0.34 ± 0.37 −0.01 ± 0.35 −0.47 ± 0.36 | −0.14 ± 0.37 −0.16 ± 0.35 −0.20 ± 0.30 | −0.52 ± 0.48 −0.06 ± 0.47 −0.62 ±0.51 | −0.23 ± 0.50 −0.24 ± 0.46 −0.35 ± 0.33 |
| Teeth Endo Status | Both vital Mesial vital Distal vital Non vital | −0.10 ± 0.30 −0.25 ± 0.31 −0.04 ± 0.32 −0.30 ± 0.29 | −0.13 ± 0.28 0.30 ± 0.01 −0.08 ± 0.17 −0.03 ± 0.29 | −0.06 ± 0.36 −0.36 ± 0.36 −0.17 ± 0.37 −0.42 ± 0.35 | −0.22 ± 0.35 0.20 ± 0.01 −0.16 ± 0.21 0.24 ±0.31 | −0.26 ± 0.30 −0.61 ± 0.51 −0.30 ± 0.51 −0.52 ± 0.45 | −0.22 ± 0.46 0.30 ± 0.01 −0.25 ± 0.37 −0.32 ± 0.35 |
| Total | −0.09 ± 0.29 | −0.10 ± 0.29 | −0.23 ± 0.40 | −0.14 ± 0.35 | −0.39 ± 0.61 | −0.22 ± 0.47 | |
| T1 | T3 | T12 | |||||
|---|---|---|---|---|---|---|---|
| Parameters | RBP | Non-RBP | RBP | Non-RBP | RBP | Non-RBP | |
| Gender | Males Females | −0.01 ± 0.15 −0.01 ± 0.16 | −0.04 ± 0.16 −0.23 ± 0.17 | −0.03± 0.26 0.02 ± 0.28 | −0.17 ± 0.28 −0.24 ± 0.28 | −0.04 ± 0.30 −0.12 ± 0.31 | −0.42 ± 0.32 −0.53 ± 0.31 |
| Age | <55 ≥55 | −0.03 ± 0.17 0.01 ± 0.16 | 0.22 ± 0.26 −0.08 ± 0.10 | −0.01 ± 0.29 −0.02 ± 0.28 | −0.28 ± 0.24 −0.26 ± 0.28 | −0.05 ± 0.33 −0.07 ± 0.30 | −0.63 ± 0.33 −0.65 ± 0.33 |
| Implant location | Maxilla Mandibular | −0.01 ± 0.15 0.03 ± 0.16 | −0.03 ±0.16 −0.20 ± 0.17 | −0.01± 0.26 0.01 ± 0.28 | −0.12 ± 0.28 −0.29 ± 0.29 | −0.05 ± 0.30 −0.07 ± 0.31 | −0.26 ± 0.31 −0.69 ± 0.33 |
| Implant placement timing | Early Delayed | 0.01 ± 0.11 0.01 ± 0.15 | −0.09 ± 0.13 −0.12 ± 0.16 | −0.05 ± 0.11 0.01 ± 0.25 | −0.36 ± 0.35 −0.10 ±0.28 | −0.12 ± 0.15 −0.07 ± 0.29 | −0.38 ± 0.41 −0.22 ± 0.32 |
| Diameter | 3.8 4.25 5 | −0.01 ± 0.22 0.03 ± 0.15 0.01 ± 0.11 | −0.05 ± 0.11 −0.17 ± 0.16 −0.01 ± 0.10 | −0.01 ± 0.21 0.05 ± 0.25 −0.06 ± 0.28 | −0.12 ± 0.31 −0.32 ± 0.28 −0.03 ± 0.35 | −0.06 ± 0.27 −0.04 ± 0.29 −0.09 ± 0.31 | −0.28 ± 0.33 −0.71 ± 0.32 −0.06 ± 0.38 |
| Teeth Endo status | Both vital Mesial vital Distal vital Non vital | −0.02 ± 0.16 −0.01 ± 0.17 0.03 ± 0.17 −0.02 ±0.16 | −0.11 ± 0.16 −0.01 ±0.01 −0.21 ± 0.23 −0.02 ± 0.10 | −0.03 ± 0.26 −0.04 ± 0.28 −0.01 ± 0.29 −0.05 ± 0.27 | −0.21 ± 0.28 −0.10 ± 0.01 −0.41 ± 0.21 −0.01 ± 0.37 | 0.04 ± 0.30 −0.16 ± 0.32 −0.06 ± 0.33 −0.02 ± 0.31 | −0.41 ± 0.32 −0.20 ± 0.01 −0.79 ± 0.29 −0.16 ± 0.39 |
| Total | −0.02 ± 0.05 | −0.11 ± 0.16 | −0.01 ± 0.06 | −0.22 ± 0.28 | −0.06 ± 0.14 | −0.48 ± 0.32 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Prati, C.; Zamparini, F.; Azizi, A.; Spinelli, A.; Gandolfi, M.G. Resin-Bonded Prosthesis in Posterior Area to Prevent Early Marginal Bone Resorption in Implants Placed at Tissue Level. Prosthesis 2022, 4, 575-588. https://doi.org/10.3390/prosthesis4040047
Prati C, Zamparini F, Azizi A, Spinelli A, Gandolfi MG. Resin-Bonded Prosthesis in Posterior Area to Prevent Early Marginal Bone Resorption in Implants Placed at Tissue Level. Prosthesis. 2022; 4(4):575-588. https://doi.org/10.3390/prosthesis4040047
Chicago/Turabian StylePrati, Carlo, Fausto Zamparini, Arash Azizi, Andrea Spinelli, and Maria Giovanna Gandolfi. 2022. "Resin-Bonded Prosthesis in Posterior Area to Prevent Early Marginal Bone Resorption in Implants Placed at Tissue Level" Prosthesis 4, no. 4: 575-588. https://doi.org/10.3390/prosthesis4040047
APA StylePrati, C., Zamparini, F., Azizi, A., Spinelli, A., & Gandolfi, M. G. (2022). Resin-Bonded Prosthesis in Posterior Area to Prevent Early Marginal Bone Resorption in Implants Placed at Tissue Level. Prosthesis, 4(4), 575-588. https://doi.org/10.3390/prosthesis4040047












