Recovery Rates of Treated vs. Non-Treated Dairy Cows with Subclinical Mastitis
Abstract
:1. Introduction
2. Materials and Methods
Statistical Analysis
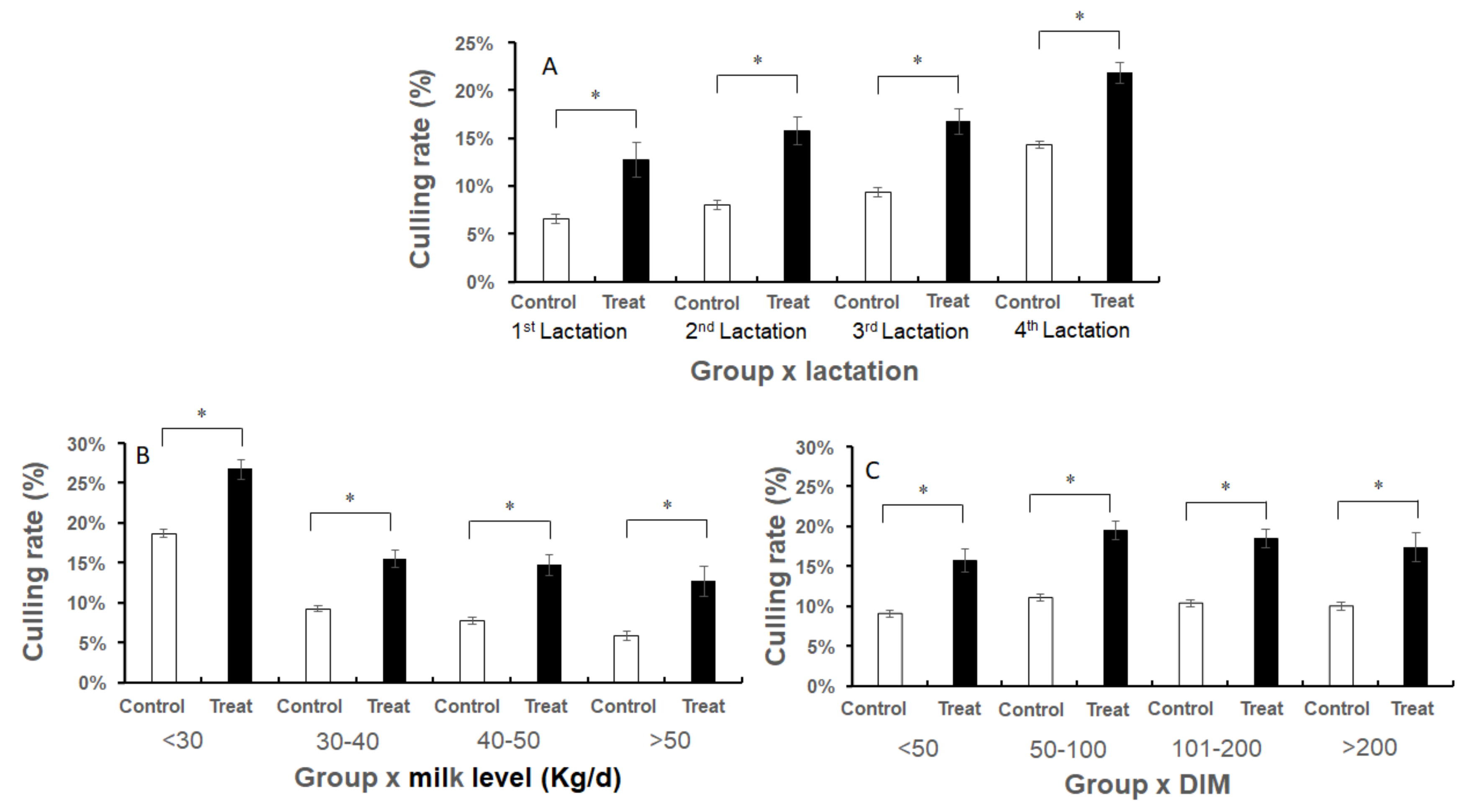
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Halasa, T.; Huijps, K.; Østerås, O.; Hogeveen, H. Economic effects of bovine mastitis and mastitis management: A review. Vet. Q. 2007, 29, 18–31. [Google Scholar] [CrossRef]
- Gröhn, Y.T.; Wilson, D.J.; González, R.N.; Hertl, J.A.; Schulte, H.; Bennett, G.; Schukken, Y.H. Effect of pathogen-specific clinical mastitis on milk yield in dairy cows. J. Dairy Sci. 2004, 87, 3358–3374. [Google Scholar] [CrossRef]
- Hertl, J.A.; Schukken, Y.H.; Welcome, F.L.; Tauer, L.W.; Gröhn, Y.T. Effects of pathogen-specific clinical mastitis on probability of conception in Holstein dairy cows. J. Dairy Sci. 2014, 97, 6942–6954. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hortet, P.; Beaudeau, F.; Seegers, H.; Fourichon, C. Reduction in milk yield associated with somatic cell counts up to 600 000 cells/mL in French Holstein cows without clinical mastitis. Live. Prod. Sci. 1999, 61, 33–42. [Google Scholar] [CrossRef]
- Halasa, T.; Nielen, M.; De Roos, A.P.W.; Van Hoorne, R.; de Jong, G.; Lam, T.J.G.M.; Van Werven, T.; Hogeveen, H. Production loss due to new subclinical mastitis in Dutch dairy cows estimated with a test-day model. J. Dairy Sci. 2009, 92, 599–606. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Smith, K.L. Standards for somatic cells in milk: Physiological and regulatory. IDF Mastit. Newsl. 1995, 144, 7–9. [Google Scholar]
- Leitner, G.; Blum, S.E.; Krifuks, O.; Edery, N.; Merin, U. Correlation between milk bacteriology, cytology, and mammary tissue histology in cows: Cure from the pathogen or recovery from the inflammation. Pathogens 2020, 9, 364. [Google Scholar] [CrossRef] [PubMed]
- Barkema, H.W.; Schukken, Y.H.; Zadoks, R.N. Invited review: The role of cow, pathogen, and treatment regimen in the therapeutic success of bovine Staphylococcus aureus mastitis. J. Dairy Sci. 2006, 89, 1877–1895. [Google Scholar] [CrossRef] [Green Version]
- Djabri, B.; Bareille, N.; Beaudeau, F.; Seegers, H. Quarter milk somatic cell count in infected dairy cows: A meta-analysis. Vet. Res. 2002, 33, 335–357. [Google Scholar] [CrossRef] [Green Version]
- Schukken, Y.H.; Wilson, D.J.; Welcome, F.; Garrison-Tikofsky, L.; Gonzalez, R.N. Monitoring udder health and milk quality using somatic cell counts. Vet. Res. 2003, 34, 579–596. [Google Scholar] [CrossRef] [Green Version]
- Owens, W.E.; Nickerson, S.C.; Boddie, R.L.; Tomita, G.M.; Ray, C.H. Prevalence of mastitis in dairy heifers and effectiveness of antibiotic therapy. J. Dairy Sci. 2001, 84, 814–817. [Google Scholar] [CrossRef]
- Murphy, J.M. Mastitis—The struggle for understanding. J. Dairy Sci. 1956, 39, 1768–1773. [Google Scholar] [CrossRef]
- Wilson, D.J.; Gonzalez, R.N.; Case, K.L.; Garrison, L.L.; Groöhn, Y.T. Comparison of seven antibiotic treatments with no treatment for bacteriological efficacy against bovine mastitis pathogens. J. Dairy Sci. 1999, 82, 1664–1670. [Google Scholar] [CrossRef]
- Apparao, D.J.; Oliviera, L.; Ruegg, P.L. Relationship between results of in vitro susceptibility tests and outcomes following treatment with pirlimycin hydrochloride in cows with subclinical mastitis associated with gram-positive pathogens. J. Am. Vet. Med. Assoc. 2009, 234, 1437–1446. [Google Scholar] [CrossRef]
- Steeneveld, W.; van Werven, T.; Barkema, H.W.; Hogeveen, H. Cow-specific treatment of clinical mastitis: An economic approach. J. Dairy Sci. 2011, 94, 174–188. [Google Scholar] [CrossRef]
- Rajala-Schultz, P.J.; Gröhn, Y.T.; McCulloch, C.E.; Guard, C.L. Effects of clinical mastitis on milk yield in dairy cows. J. Dairy Sci. 1999, 82, 1213–1220. [Google Scholar] [CrossRef]
- Schukken, Y.H.; Bennett, G.J.; Zurakowski, M.J.; Sharkey, H.L.; Rauch, B.J.; Thomas, M.J.; Ceglowski, B.; Saltman, R.L.; Belomestnykh, N.; Zadoks, R.N. Randomized clinical trial to evaluate the efficacy of a 5-day ceftiofur hydrochloride intramammary treatment on nonsevere gram-negative clinical mastitis. J. Dairy Sci. 2011, 94, 6203–6215. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Blum, S.; Heller, E.D.; Leitner, G. Long term effects of Escherichia coli. Vet. J. 2014, 201, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Rollin, E.; Dhuyvetter, K.C.; Overton, M.W. The cost of clinical mastitis in the first 30 days of lactation: An economic modeling tool. Prev. Vet. Med. 2015, 122, 257–264. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lavon, Y.; Ezra, E.; Leitner, G.; Wolfenson, D. Association of conception rate with pattern and level of somatic cell count elevation relative to time of insemination in dairy cows. J. Dairy Sci. 2011, 94, 4538–4545. [Google Scholar] [CrossRef]
- Oliver, S.P.; Gillespie, B.E.; Headrick, S.J.; Moorehead, H.; Lunn, P.; Dowlen, H.H.; Johnson, D.L.; Lamar, K.C.; Chester, S.T.; Moseley, W.M. Efficacy of extended Ceftiofur intramammary therapy for treatment of subclinical mastitis in lactating dairy cows. J. Dairy Sci. 2004, 87, 2393–2400. [Google Scholar] [CrossRef]
- Suojala, L.; Kaartinen, L.; Pyorala, S. Treatment for bovine Escherichia coli mastitis—An evidence based approach. Vet Pharm. Ther. 2013, 36, 521–531. [Google Scholar] [CrossRef]
- Boerlin, P.; White, D.G. Antimicrobial resistance and its epidemiology. In Antimicrobial Therapy in Veterinary Medicine, 5th ed.; Giguere, S., Prescott, J.F., Dowling, P.M., Eds.; Wiley Blackwell: Ames, IA, USA, 2013; pp. 21–40. [Google Scholar] [CrossRef]
- Ruegg, P.L. What is success? A narrative review of research evaluating outcomes of antibiotics used for treatment of clinical mastitis. Front. Vet. Sci. 2021, 8, 639641. [Google Scholar] [CrossRef]
- Liang, D.; Arnold, L.M.; Stowe, C.J.; Harmon, R.J.; Bewley, J.M. Estimating US dairy clinical disease costs with a stochastic simulation model. J. Dairy Sci. 2017, 100, 1472–1486. [Google Scholar] [CrossRef] [Green Version]
- Aghamohammadi, M.; Haine, D.; Kelton, D.F.; Barkema, H.W.; Hogeveen, H.; Keefe, G.P.; Dufour, S. Herd-level mastitis-associated costs on Canadian dairy farms. Front. Vet. Sci. 2018, 5, 100. [Google Scholar] [CrossRef] [PubMed]
| Cutoff Level SCC (×103/mL) | Cows | SCC (×103/mL) | Milk Yield (L/Day) | Total Cows Culled | Cows Culled Due to Mastitis (from Total) | |||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | |||
| CL1 (200–299) | 39,170 | 31.6 | 243 ± 0.03 | 39.9 ± 0.03 | 2195 | 5.6 | 965 | 44.0 |
| CL2 (300–399) | 23,390 | 18.9 | 344 ± 0.06 | 39.6 ± 0.03 | 1518 | 6.5 | 651 | 42. 9 |
| CL3 (400–499) | 15,164 | 12.2 | 444 ± 0.05 | 39.7 ± 0.04 | 1056 | 7.0 | 499 | 47.3 |
| CL4 (500–999) | 24,202 | 19.5 | 693 ± 0.20 | 39.3 ± 0.03 | 1913 | 7.9 | 959 | 50.1 |
| CL5 (≥1000) | 22,032 | 17.8 | 2785 ± 0.20 | 36.5 ± 0.04 | 2435 | 11.1 | 1487 | 61.1 |
| Cutoff Level | Cows | SR | AR | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | Treatment 1 | 100 × 103 | 250 × 103 | 100 × 103 | 250 × 103 | ||||||
| n | NT | AB | n | % | n | % | n | % | N | % | |
| CL1 (200–299) 2 | 39,169 | 37,315 | 1854 | 4676 | 12.5 | - | - | n/a | |||
| CL2 (300–399) | 23,390 | 22,221 | 1169 | 2171 | 9.8 | 7035 | 31.7 | n/a | |||
| CL3 (400–499) | 15,164 | 14,296 | 868 | 1918 | 13.4 | 3848 | 26.9 | 92 | 10.6 | 251 | 28.9 |
| CL4 (500–999) | 24,202 | 22,557 | 1645 | 2239 | 9.9 | 6133 | 27.2 | 170 | 10.3 | 433 | 26.3 |
| CL5 (≥1000) | 22,032 | 19,704 | 2328 | 2045 | 10.4 | 4988 | 25.3 | 320 | 13.8 | 701 | 30.1 |
| Variable | Level | Cows # | LSM Diff 1 | REF Level 2 | p-Value | SE | LSM Diff | REF Level | p-Value | SE |
|---|---|---|---|---|---|---|---|---|---|---|
| Recovery 3 | Culling 4 | |||||||||
| Lactation | 1 | 6974 | - | 0.391 | - | - | - | 0.02 | - | - |
| 2 | 5023 | −0.026 | 0.007 | 0.032 | 0.031 | 0.001 | 0.066 | |||
| 3 | 4726 | −0.085 | 0.001 | 0.034 | 0.04 | 0.001 | 0.065 | |||
| 4+ | 6667 | −0.155 | 0.001 | 0.030 | 0.071 | 0.001 | 0.049 | |||
| DIM | ≤50 | 3117 | - | 0.414 | - | - | - | 0.039 | - | - |
| 51–100 | 4600 | −0.056 | 0.001 | 0.032 | 0.025 | 0.001 | 0.067 | |||
| 101–200 | 8770 | −0.076 | 0.001 | 0.024 | 0.015 | 0.002 | 0.052 | |||
| >200 | 6903 | −0.215 | 0.001 | 0.033 | 0.001 | 0.818 | 0.060 | |||
| Milk yield (L/day) | ≤30 | 4090 | - | 0.256 | - | - | - | 0.173 | - | - |
| 31–40 | 8951 | 0.056 | 0.001 | 0.026 | −0.112 | 0.001 | 0.051 | |||
| 41–50 | 7103 | 0.091 | 0.001 | 0.027 | −0.144 | 0.001 | 0.067 | |||
| >50 | 3246 | 0.119 | 0.001 | 0.040 | −0.156 | 0.001 | 0.109 | |||
| Variable | Level | N | LSM Diff 1 | REF Level 2 | p-Value | SE | LSM Diff | REF Level | p-Value | SE |
|---|---|---|---|---|---|---|---|---|---|---|
| Recovery 3 | Culling 4 | |||||||||
| Treatment | Not treated | 19,704 | - | 0.254 | - | - | - | 0.076 | - | - |
| Treated | 2328 | 0.035 | 0.004 | 0.058 | 0.061 | 0.001 | 0.077 | |||
| Lactation | 1 | 4978 | - | 0.312 | - | - | - | 0.061 | - | - |
| 2 | 4484 | 0.029 | 0.096 | 0.053 | 0.035 | 0.001 | 0.075 | |||
| 3 | 4687 | −0.056 | 0.006 | 0.053 | 0.054 | 0.001 | 0.067 | |||
| 4+ | 7883 | −0.121 | 0.001 | 0.046 | 0.108 | 0.001 | 0.048 | |||
| DIM | ≤50 | 4490 | - | 0.309 | - | - | - | 0.101 | - | - |
| 51–100 | 5548 | −0.015 | 0.324 | 0.096 | 0.029 | 0.001 | 0.057 | |||
| 101–200 | 7717 | 0.004 | 0.977 | 0.093 | 0.006 | 0.485 | 0.057 | |||
| >200 | 4277 | −0.123 | 0.001 | 0.076 | −0.020 | 0.028 | 0.089 | |||
| Milk yield (L/day) | ≤30 | 4590 | - | 0.295 | - | - | - | 0.224 | - | - |
| 31–40 | 7740 | −0.011 | 0.432 | 0.044 | −0.115 | 0.001 | 0.058 | |||
| 41–50 | 6642 | −0.036 | 0.009 | 0.052 | −0.145 | 0.001 | 0.069 | |||
| >50 | 3060 | −0.045 | 0.011 | 0.078 | −0.168 | 0.001 | 0.103 | |||
| Treatment × lactation | Control × 1 | 4642 | - | 0.301 | - | - | - | 0.041 | - | - |
| Treat × 1 | 336 | 0.025 | 0.363 | 0.129 | 0.048 | 0.001 | 0.178 | |||
| Control × 2 | 4009 | - | 0.321 | - | - | - | 0.068 | - | - | |
| Treat × 2 | 475 | 0.024 | 0.081 | 0.106 | 0.064 | 0.001 | 0.136 | |||
| Control × 3 | 4144 | - | 0.242 | - | - | - | 0.088 | - | - | |
| Treat × 3 | 543 | 0.028 | 0.157 | 0.099 | 0.062 | 0.001 | 0.122 | |||
| Control × 4+ | 6909 | - | 0.172 | - | - | - | 0.141 | - | - | |
| Treat × 4+ | 974 | 0.038 | 0.005 | 0.088 | 0.06 | 0.001 | 0.087 | |||
| Treatment × DIM | Control × ≤50 | 4027 | - | 0.295 | - | - | - | 0.077 | - | - |
| Treat × ≤50 | 463 | 0.029 | 0.226 | 0.105 | 0.055 | 0.001 | 0.135 | |||
| Control × 51–100 | 4831 | - | 0.283 | - | - | - | 0.101 | - | - | |
| Treat × 51–100 | 717 | 0.025 | 0.203 | 0.087 | 0.066 | 0.011 | 0.104 | |||
| Control × 101–200 | 6879 | - | 0.284 | - | - | - | 0.08 | - | - | |
| Treat × 101–200 | 838 | 0.05 | 0.006 | 0.082 | 0.062 | 0.001 | 0.105 | |||
| Control >200 | 3967 | - | 0.171 | - | - | - | 0.057 | - | - | |
| Treat × >200 | 310 | 0.032 | 0.164 | 0.145 | 0.059 | 0.001 | 0.168 | |||
| Treatment × milk yield (L/day) | Control × ≤30 | 3937 | - | 0.257 | - | - | - | 0.198 | - | - |
| Treat × ≤30 | 653 | 0.079 | 0.001 | 0.086 | 0.055 | 0.002 | 0.094 | |||
| Control × 31–40 | 6988 | - | 0.248 | - | - | - | 0.088 | - | - | |
| Treat × 31–40 | 752 | 0.076 | 0.001 | 0.082 | 0.046 | 0.001 | 0.108 | |||
| Control × 41–50 | 6018 | - | 0.245 | - | - | - | 0.054 | - | - | |
| Treat × 41–50 | 624 | 0.026 | 0.19 | 0.104 | 0.058 | 0.001 | 0.128 | |||
| Control × >50 | 2761 | - | 0.268 | - | - | - | 0.034 | - | - | |
| Treat × >50 | 299 | −0.036 | 0.225 | 0.149 | 0.056 | 0.001 | 0.188 | |||
| Treatment | Time of Culling 1 (Days) | ||||
|---|---|---|---|---|---|
| NT | AB | NT | AB | ||
| Cows | 22,032 | 19,704 | 2328 | ||
| culled (by owner) | Total | 2018 (10.2%) | 419 (18.0%) | ||
| Reproduction | 107 (5.3%) | 13 (3.1%) | 47 | 54 | |
| Mastitis | 1229 (61.0%) | 259 (61.8%) | 47 | 49 | |
| Other | 682 (33.8%) | 147 (35.1%) | 45 | 39 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lavon, Y.; Gilad, D.; Leitner, G. Recovery Rates of Treated vs. Non-Treated Dairy Cows with Subclinical Mastitis. Dairy 2021, 2, 576-584. https://doi.org/10.3390/dairy2040045
Lavon Y, Gilad D, Leitner G. Recovery Rates of Treated vs. Non-Treated Dairy Cows with Subclinical Mastitis. Dairy. 2021; 2(4):576-584. https://doi.org/10.3390/dairy2040045
Chicago/Turabian StyleLavon, Yaniv, Dan Gilad, and Gabriel Leitner. 2021. "Recovery Rates of Treated vs. Non-Treated Dairy Cows with Subclinical Mastitis" Dairy 2, no. 4: 576-584. https://doi.org/10.3390/dairy2040045
APA StyleLavon, Y., Gilad, D., & Leitner, G. (2021). Recovery Rates of Treated vs. Non-Treated Dairy Cows with Subclinical Mastitis. Dairy, 2(4), 576-584. https://doi.org/10.3390/dairy2040045






