Accommodative Response in Patients with Central Field Loss: A Matched Case-Control Study
Abstract
1. Introduction
2. Methods
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chen, A.H.; O’Leary, D.J.; Howell, E.R. Near visual function in young children. Part I: Near point of convergence. Part II: Amplitude of accommodation. Part III: Near heterophoria. Ophthalmic Physiol. Opt. 2000, 20, 185–198. [Google Scholar] [CrossRef] [PubMed]
- Wang, B.; Ciuffreda, K.J. Depth-of-Focus of the Human Eye: Theory and Clinical Implications. Surv. Ophthalmol. 2006, 51, 75–85. [Google Scholar] [CrossRef] [PubMed]
- Coleman, D.J. Unified Model for Accommodative Mechanism. Am. J. Ophthalmol. 1970, 69, 1063–1079. [Google Scholar] [CrossRef]
- Coleman, D.; Fish, S.K. Presbyopia, accommodation, and the mature catenary. Ophthalmology 2001, 108, 1544–1551. [Google Scholar] [CrossRef]
- Poltavski, D.V.; Biberdorf, D.; Petros, T.V. Accommodative response and cortical activity during sustained attention. Vis. Res. 2012, 63, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Tarrant, J.; Roorda, A.; Wildsoet, C.F. Determining the accommodative response from wavefront aberrations. J. Vis. 2010, 10, 4. [Google Scholar] [CrossRef]
- Momeni-Moghaddam, H.; Goss, D.A.; Sobhani, M. Accommodative response under monocular and binocular conditions as a function of phoria in symptomatic and asymptomatic subjects. Clin. Exp. Optom. 2014, 97, 36–42. [Google Scholar] [CrossRef]
- Matsuo, T.; Ohtsuki, H. Follow-up results of a combination of accommodation and convergence insufficiency in school-age children and adolescents. Graefe’s Arch. Clin. Exp. Ophthalmol. 1992, 230, 166–170. [Google Scholar] [CrossRef]
- Russell, G.E.; Wick, B. A Prospective Study of Treatment of Accommodative Insufficiency. Optom. Vis. Sci. 1993, 70, 131–135. [Google Scholar] [CrossRef]
- Dwyer, P.; Wick, B. The Influence of Refractive Correction Upon Disorders of Vergence and Accommodation. Optom. Vis. Sci. 1995, 72, 224–232. [Google Scholar] [CrossRef]
- Scheiman, M.; Gallaway, M.; Coulter, R.; Reinstein, F.; Ciner, E.; Herzberg, C.; Parisi, M. Prevalence of vision and ocular disease conditions in a clinical pediatric population. J. Am. Optom. Assoc. 1996, 67, 193–202. [Google Scholar] [PubMed]
- Porcar, E.; Martinez-Palomera, A. Prevalence of General Binocular Dysfunctions in a Population of University Students. Optom. Vis. Sci. 1997, 74, 111–113. [Google Scholar] [CrossRef] [PubMed]
- Rouse, M.W.; Hyman, L.; Hussein, M.; Solan, H. Frequency of Convergence Insufficiency in Optometry Clinic Settings. Optom. Vis. Sci. 1998, 75, 88–96. [Google Scholar] [CrossRef] [PubMed]
- Lara, F.; Cacho, P.; García, Á.; Megías, R. General binocular disorders: Prevalence in a clinic population. Ophthalmic Physiol. Opt. 2001, 21, 70–74. [Google Scholar] [CrossRef]
- Campbell, F.W.; Robson, J.G.; Westheimer, G. Fluctuations of accommodation under steady viewing conditions. J. Physiol. 1959, 145, 579–594. [Google Scholar] [CrossRef] [PubMed]
- Ryu, D.-K. Comparison of clinical techniques to assess objectively accommodative response. J. Korea Acad. Coop. Soc. 2010, 11, 3406–3411. [Google Scholar] [CrossRef]
- Rosenfield, M.; Portello, J.K.; Blustein, G.H.; Jang, C. Comparison of Clinical Techniques to Assess the Near Accommodative Response. Optom. Vis. Sci. 1996, 73, 382–388. [Google Scholar] [CrossRef]
- Subbaram, M.V.; Bullimore, M.A. Visual acuity and the accuracy of the accommodative response. Ophthalmic Physiol. Opt. 2002, 22, 312–318. [Google Scholar] [CrossRef]
- Anderson, H.A.; Glasser, A.; Stuebing, K.K.; Manny, R.E. Minus Lens Stimulated Accommodative Lag as a Function of Age. Optom. Vis. Sci. 2009, 86, 685–694. [Google Scholar] [CrossRef]
- Heron, G.; Charman, W.N.; Gray, L.S. Accommodation responses and ageing. Investig. Ophthalmol. Vis. Sci. 1999, 40, 2872–2883. [Google Scholar]
- Nakatsuka, C.; Hasebe, S.; Nonaka, F.; Ohtsuki, H. Accommodative Lag Under Habitual Seeing Conditions: Comparison Between Myopic and Emmetropic Children. Jpn. J. Ophthalmol. 2005, 49, 189–194. [Google Scholar] [CrossRef]
- Xu, D.; Jiang, J.; Yan, J.; Lü, F.; Qu, J. Analyze of the accommodative response in myopia anisometropes. Zhonghua Yan Ke Za Zhi Chin. J. Ophthalmol. 2009, 45, 612–615. [Google Scholar]
- Rosenfield, M.; Gilmartin, B. Effect of Target Proximity on the Open-Loop Accommodative Response. Optom. Vis. Sci. 1990, 67, 74–79. [Google Scholar] [CrossRef] [PubMed]
- Goss, D.A.; Rainey, B.B. Relationship of Accommodative Response and Nearpoint Phoria in a Sample of Myopic Children. Optom. Vis. Sci. 1999, 76, 292–294. [Google Scholar] [CrossRef]
- Tassinari, J.T. Monocular Estimate Method Retinoscopy: Central Tendency Measures and Relationship to Refractive Status and Heterophoria. Optom. Vis. Sci. 2002, 79, 708–714. [Google Scholar] [CrossRef][Green Version]
- Scheiman, M.; Wick, B. Clinical Management of Binocular Vision: Heterophoric, Accommodative and Eye Movement Disorders; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2008; pp. 59–64, 121–123. [Google Scholar]
- Cheng, D.; Schmid, K.L.; Woo, G.C. The effect of positive-lens addition and base-in prism on accommodation accuracy and near horizontal phoria in Chinese myopic children. Ophthalmic Physiol. Opt. 2008, 28, 225–237. [Google Scholar] [CrossRef]
- Chase, C.; Tosha, C.; Borsting, E.; Ridder, W.H. Visual Discomfort and Objective Measures of Static Accommodation. Optom. Vis. Sci. 2009, 86, 883–889. [Google Scholar] [CrossRef]
- Tosha, C.; Borsting, E.; Ridder, W.H., 3rd; Chase, C. Accommodation response and visual discomfort. Ophthalmic Physiol. Opt. 2009, 29, 625–633. [Google Scholar] [CrossRef] [PubMed]
- Johnson, C.A. Effects of luminance and stimulus distance on accommodation and visual resolution. J. Opt. Soc. Am. 1976, 66, 138–142. [Google Scholar] [CrossRef] [PubMed]
- Ciuffreda, K.J. Accommodation, the Pupil and Presbyopia; Butterworth Heinemann Elsevier: St. Louis, MO, USA,, 2006; pp. 93–144. [Google Scholar]
- Manh, V.; Chen, A.M.; Tarczy-Hornoch, K.; Cotter, S.A.; Candy, T.R. Accommodative Performance of Children with Unilateral Amblyopia. Investig. Opthalmology Vis. Sci. 2015, 56, 1193–1207. [Google Scholar] [CrossRef]
- Chen, A.M.; Manh, V.; Candy, T.R. Longitudinal Evaluation of Accommodation During Treatment for Unilateral Amblyopia. Investig. Opthalmology Vis. Sci. 2018, 59, 2187–2196. [Google Scholar] [CrossRef]
- White, J.M.; Wick, B. Accommodation in humans with juvenile macular degeneration. Vis. Res. 1995, 35, 873–880. [Google Scholar] [CrossRef]
- Leat, S.J.; Mohr, A. Accommodative Response in Pre-presbyopes with Visual Impairment and Its Clinical Implications. Investig. Opthalmol. Vis. Sci. 2007, 48, 3888–3896. [Google Scholar] [CrossRef]
- Heyman, C.L. Accommodative Response in Children with Visual Impairment. Optom. Vis. Dev. 2011, 42, 10–16. [Google Scholar]
- Atchison, D.A.; Varnas, S.R. Accommodation stimulus and response determinations with autorefractors. Ophthalmic Physiol. Opt. 2017, 37, 96–104. [Google Scholar] [CrossRef]
- Montalbán, R.; Piñero, D.P.; Javaloy, J.; Alio, J.L. Correlation of the Corneal Toricity Between Anterior and Posterior Corneal Surfaces in the Normal Human Eye. Cornea 2013, 32, 791–798. [Google Scholar] [CrossRef]
- Montalbán, R.; Piñero, D.P.; Javaloy, J.; Alió, J.L. Scheimpflug photography–based clinical characterization of the correlation of the corneal shape between the anterior and posterior corneal surfaces in the normal human eye. J. Cataract. Refract. Surg. 2012, 38, 1925–1933. [Google Scholar] [CrossRef] [PubMed]
- Leat, S.J.; Gargon, J.L. Accommodative response in children and young adults using dynamic retinoscopy. Ophthalmic Physiol. Opt. 1996, 16, 375–384. [Google Scholar] [CrossRef] [PubMed]
- Garcia, A.; Cacho, P. MEM and Nott dynamic retinoscopy in patients with disorders of vergence and accommodation. Ophthalmic Physiol. Opt. 2002, 22, 214–220. [Google Scholar] [CrossRef] [PubMed]
- McBrient, N.A.; Millodot, M.; McBrien, N.A. THE EFFECT OF REFRACTIVE ERROR ON THE ACCOMMODATIVE RESPONSE GRADIENT*. Ophthalmic Physiol. Opt. 1986, 6, 145–149. [Google Scholar] [CrossRef]
- Millodot, M. The effect of refractive error on the accommodative response gradient: A summary and update. Ophthalmic Physiol. Opt. 2015, 35, 607–612. [Google Scholar] [CrossRef] [PubMed]
- Gwiazda, J.; Bauer, J.; Thorn, F.; Held, R. A dynamic relationship between myopia and blur-driven accommodation in school-aged children. Vis. Res. 1995, 35, 1299–1304. [Google Scholar] [CrossRef]
- McClelland, J.F.; Saunders, K.J. Accommodative lag using dynamic retinoscopy: Age norms for school-age children. Optom. Vis. Sci. 2004, 81, 929–933. [Google Scholar] [PubMed]
- Green, D.G.; Powers, M.K.; Banks, M.S. Depth of focus, eye size and visual acuity. Vis. Res. 1980, 20, 827–835. [Google Scholar] [CrossRef]
- Legge, G.E.; Mullen, K.T.; Woo, G.C.; Campbell, F.W. Tolerance to visual defocus. J. Opt. Soc. Am. A 1987, 4, 851–863. [Google Scholar] [CrossRef]
- Dickinson, C. Low Vision: Principles and Practice, 4th ed.; Butterworth-Heinemann: Oxford, UK, 1998. [Google Scholar]

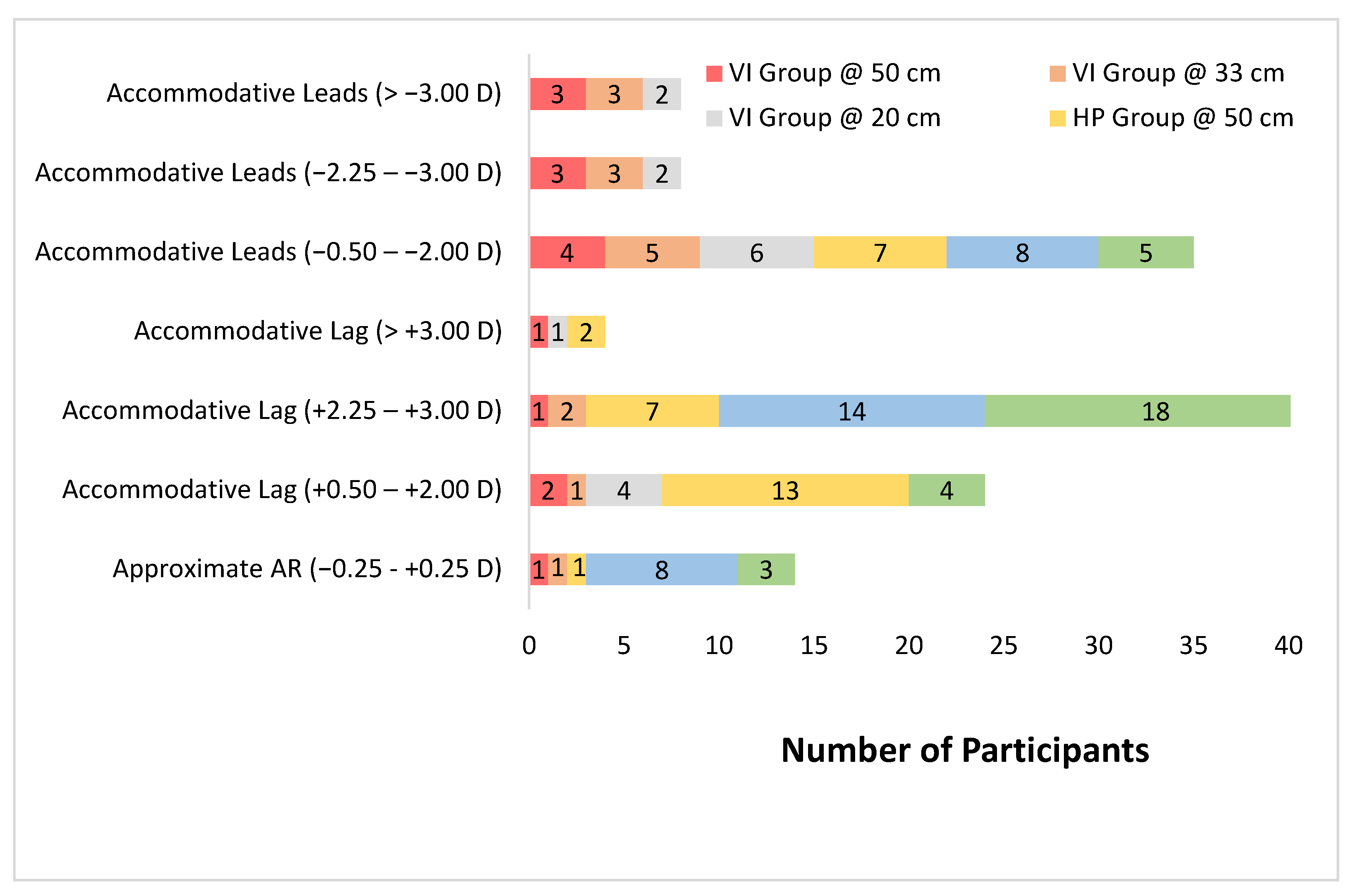
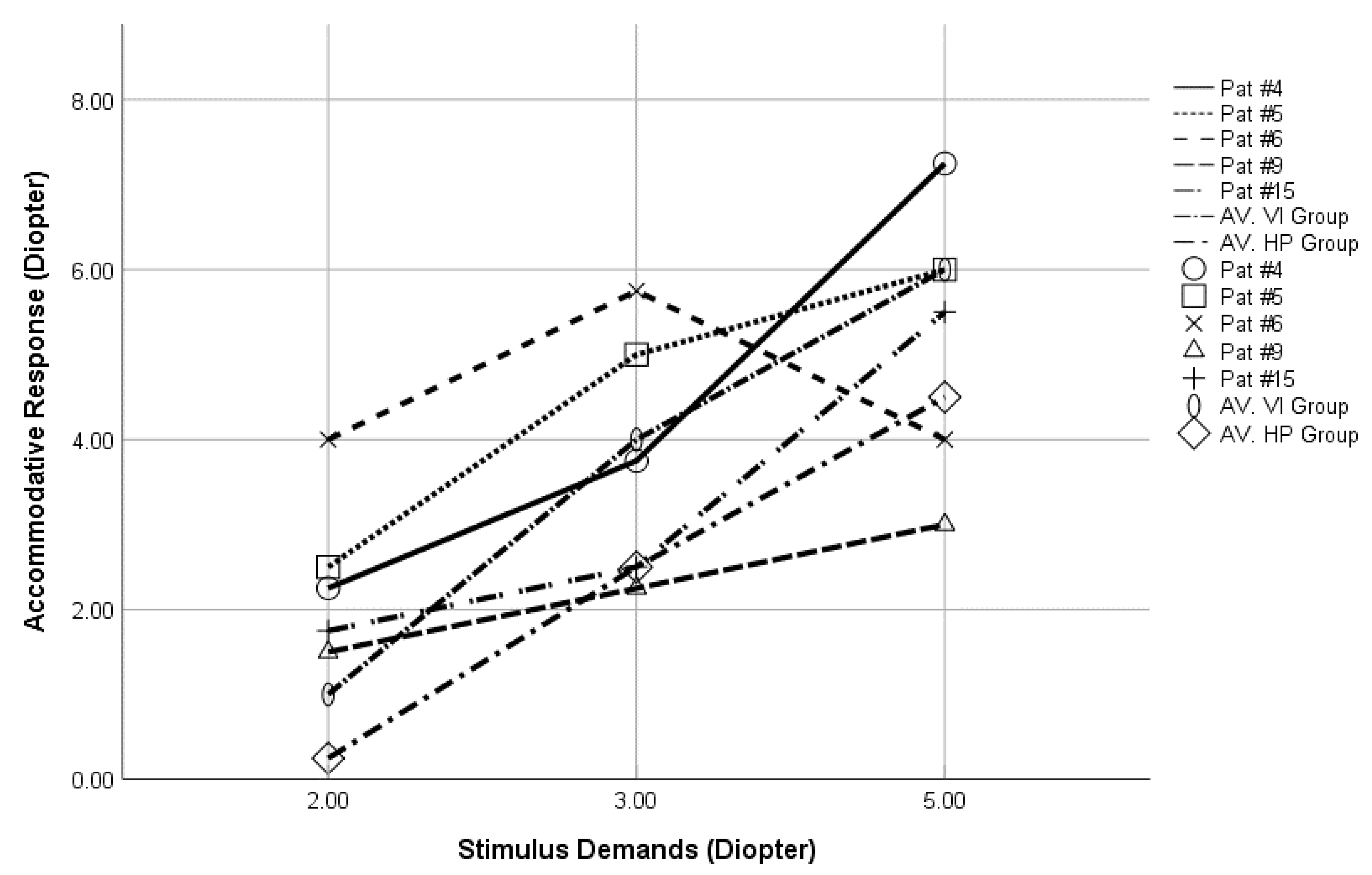
| Variable | VI Group Median ± IQ (Range) | HP Group Median ± IQ (Range) | Mann Whitney Test |
|---|---|---|---|
| Age (Years) | 14 ± 1.00 (12–15) | 14 ± 2.00 (12–15) | Z = −1.21, p = 0.23 |
| VA LogMAR | 1.3 ± 0.7 (0.70–1.8) | 0.00 ± 0.00 (0.00–0.1) | Z = −6.044, p < 0.0001 * |
| Sph.Eq | −3.25 ± 4.00 (−6.50–+6.00) | −1.25 ± 1.00 (−2.50–+1.00) | Z = −1.455, p = 0.14 |
| AR @ 50 cm | 1.14 ± 4.86 (−13.75–+3.00) | 2.45 ± 1.50 (−1.50–+3.00) | Z = −2.25, p = 0.025 * |
| AR @ 33 cm | −1.00 ± 2.90 (−14–+2.00) | 0.25 ± 1.25 (−1.25–+1.50) | Z = −2.9, p = 0.003 * |
| AR @ 20 cm | −1.00 ± 2.75 (−16–+4.00) | 0.50 ± 1.50 (−0.50–+2.25) | Z = −2.2, p = 0.03 * |
| Patient | Age | VA (LogMAR) | Error of Accommodation |
|---|---|---|---|
| 1 | 14 | 1.3 | negative slope lead |
| 2 | 12 | 1.3 | negative slope lag |
| 3 | 15 | 1.5 | variable slope |
| 4 | 14 | 1.3 | variable slope |
| 5 | 14 | 1.8 | negative slope lead |
| 6 | 12 | 1.3 | fixed lead |
| 7 | 12 | 1.3 | variable slope |
| 8 | 15 | 1.5 | fixed lead |
| 9 | 15 | 1.3 | negative slope lead |
| 10 | 15 | 1.3 | negative slope lag |
| 11 | 15 | 0.8 | negative slope lag |
| 12 | 14 | 1.8 | fixed lead |
| 13 | 15 | 0.7 | fixed accurate |
| 14 | 15 | 0.8 | fixed lead |
| 15 | 14 | 0.7 | fixed accurate |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alsaqr, A.M.; AlShareef, H.; Alhajri, F.; Abusharha, A.; Fagehi, R.; Alharbi, A.; Alanazi, S. Accommodative Response in Patients with Central Field Loss: A Matched Case-Control Study. Vision 2021, 5, 35. https://doi.org/10.3390/vision5030035
Alsaqr AM, AlShareef H, Alhajri F, Abusharha A, Fagehi R, Alharbi A, Alanazi S. Accommodative Response in Patients with Central Field Loss: A Matched Case-Control Study. Vision. 2021; 5(3):35. https://doi.org/10.3390/vision5030035
Chicago/Turabian StyleAlsaqr, Ali Mazyed, Hisham AlShareef, Faisal Alhajri, Ali Abusharha, Raied Fagehi, Ahmad Alharbi, and Saud Alanazi. 2021. "Accommodative Response in Patients with Central Field Loss: A Matched Case-Control Study" Vision 5, no. 3: 35. https://doi.org/10.3390/vision5030035
APA StyleAlsaqr, A. M., AlShareef, H., Alhajri, F., Abusharha, A., Fagehi, R., Alharbi, A., & Alanazi, S. (2021). Accommodative Response in Patients with Central Field Loss: A Matched Case-Control Study. Vision, 5(3), 35. https://doi.org/10.3390/vision5030035





