Development and Remodeling of Point-of-Care Ultrasound Education for Emergency Medicine Residents in Resource Limited Countries during the COVID-19 Pandemic
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Participants
2.3. Data Collection
2.4. Study Size
2.5. Development and Implementation of POCUS Education and POCUS Learning Tools
2.6. Remodeling of POCUS Education
2.7. Ethical Considerations
3. Results
4. Discussion
4.1. Training Program
4.2. Timing and Length of Training
4.3. Ultrasound Learning Tools
4.4. Perceived Barrier to Learning POCUS
5. Future Work
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Q1 | 1. Gender | ||||||
| 2. Age | |||||||
| 3. POCUS Experience | Yes | No | |||||
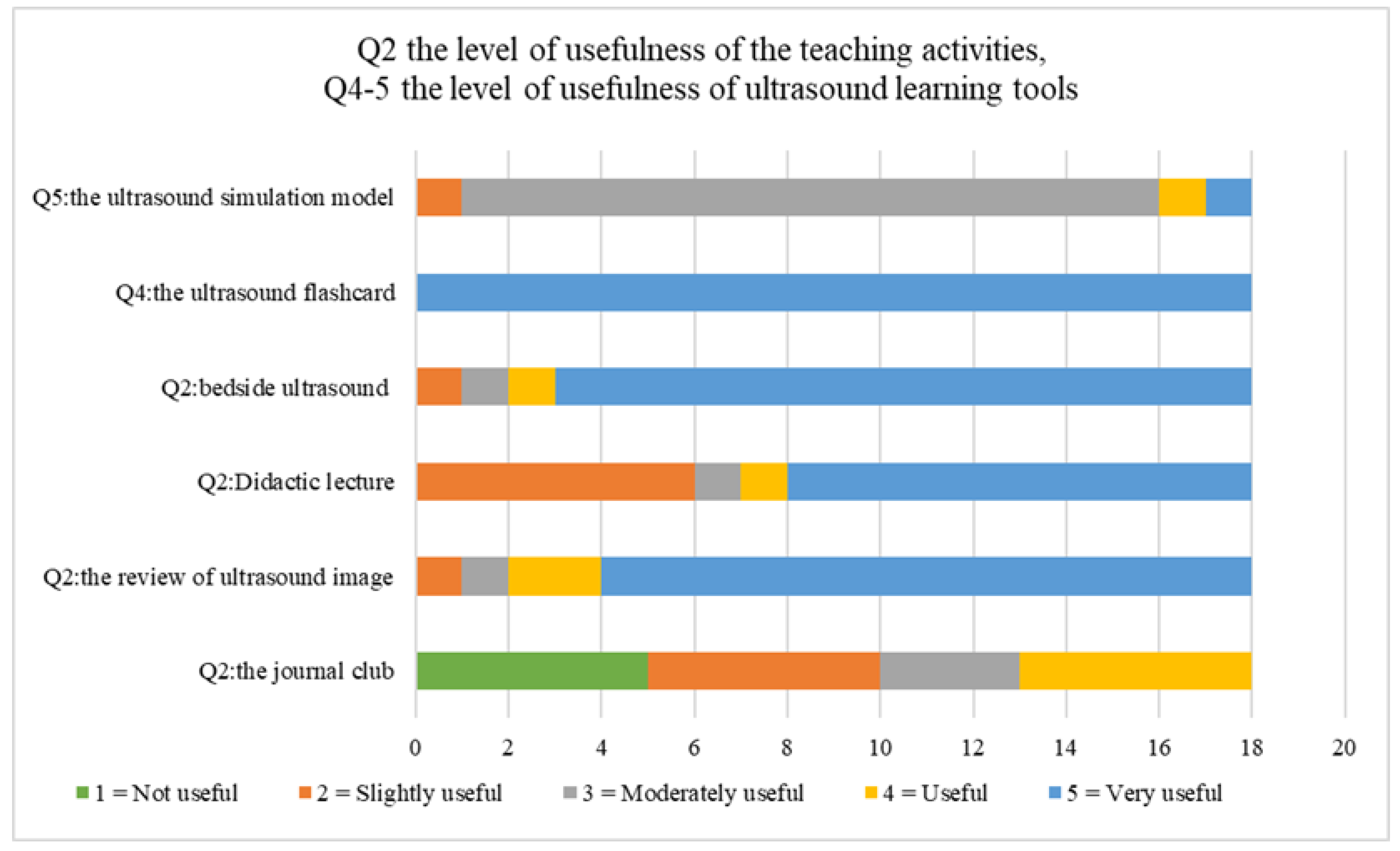
| Q2 | How useful do you think the following teaching activities are to help to improve POCUS knowledge? | 1 Not Useful | 2 Slightly Useful | 3 Moderately Useful | 4 Useful | 5 Very Useful | N/A |
| 1.The journal club | |||||||
| 2. The review of ultrasound images | |||||||
| 3. Didactic lectures | |||||||
| 4. Bedside ultrasounds | |||||||
| Q3 | How do you think the duration of time used in the following activities is for improving your POCUS knowledge? | 1 Not Suitable | 2 Slightly Suitable | 3 Moderately Suitable | 4 Suitable | 5 Very Suitable | N/A |
| 1. The journal club (1 session, 3 h) | |||||||
| 2. The review of ultrasound images (1 session, 3 h) | |||||||
| 3. Didactic lectures (3 h per week) | |||||||
| 4. Bedside ultrasounds (9 h per week) | |||||||
| Q4 | How useful do you think the ultrasound flashcards are in helping to improve POCUS knowledge? | 1 Not Useful | 2 Slightly Useful | 3 Moderately Useful | 4 Useful | 5 Very Useful | N/A |
| Q5 | How useful do you think the ultrasound simulation model is to help to improve POCUS skills? | 1 Not Useful | 2 Slightly Useful | 3 Moderately Useful | 4 Useful | 5 Very Useful | N/A |
| Q6 | Ease of use of the ultrasound devices used in this education program? | 1 Very Unsatisfied | 2 Unsatisfied | 3 Neutral | 4 Satisfied | 5 Very Satisfied | N/A |
| 1. Mindray M9 | |||||||
| 2. Sonosite M turbo | |||||||
| 3. Butterfly iQ | |||||||
| Q7 | Number of independent POCUS examinations performed in this rotation | 0–10 | 11–20 | 21–30 | 31–40 | >41 | N/A |
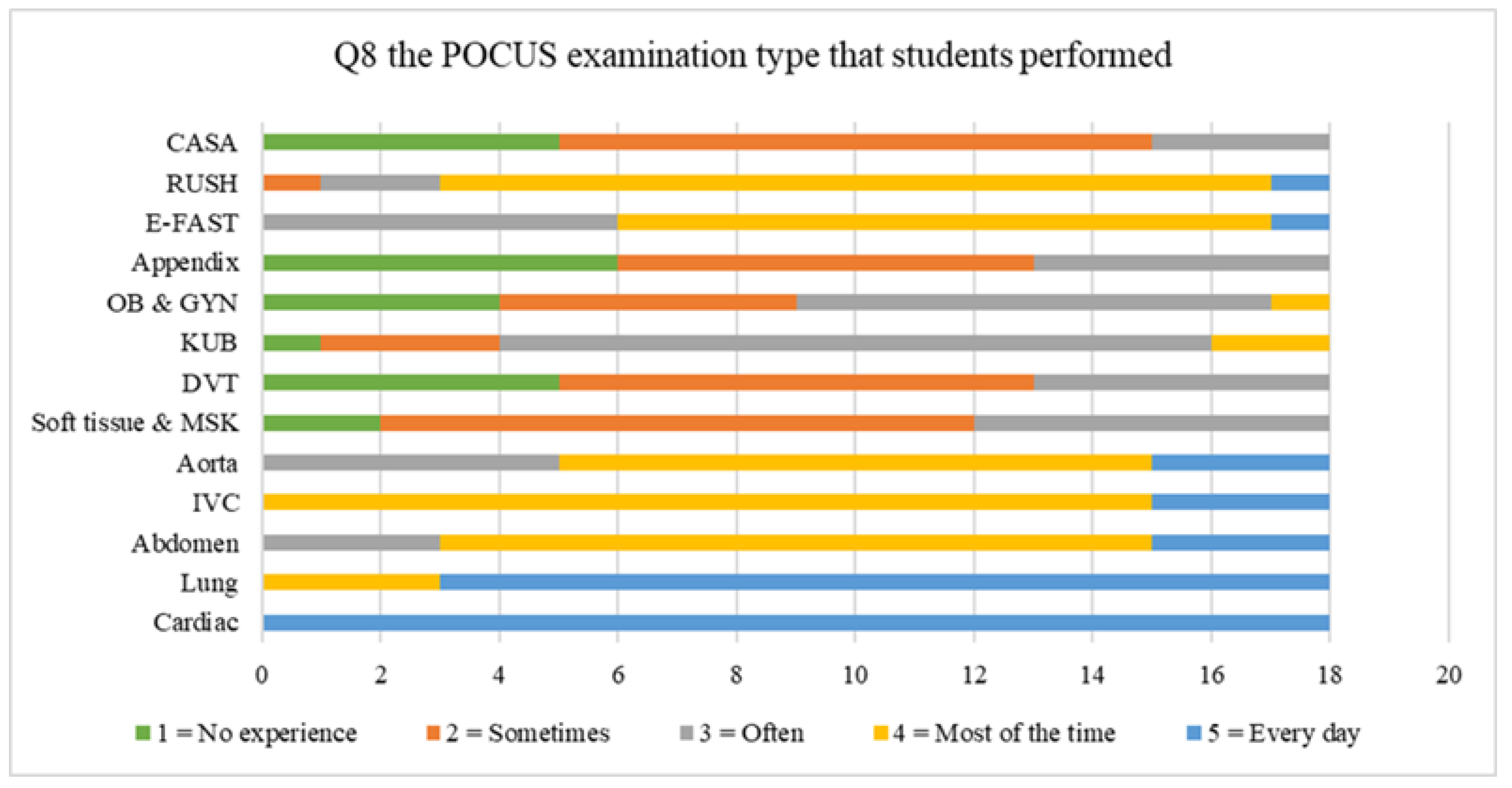
| Q8 | Type of POCUS examination that the student practiced in this class | 1 No Experience (0%) | 2 Sometimes (20%) | 3 Often (50%) | 4 Most of the Time (80%) | 5 Every Day (100%) | N/A |
| 1. Cardiac | |||||||
| 2. Lung | |||||||
| 3. Abdomen (liver, gallbladder, ascites) | |||||||
| 4. Inferior vena cava (IVC) | |||||||
| 5. Aorta | |||||||
| 6. Soft tissue and musculoskeletal (MSK) | |||||||
| 7. Deep Venous thrombosis (DVT) | |||||||
| 8.Kidney and Urinary bladder (KUB) | |||||||
| 9. Obstetrics and Gynecology | |||||||
| 10. Appendix | |||||||
| 11. E-FAST | |||||||
| 12. RUSH protocol | |||||||
| 13. CASA protocol | |||||||
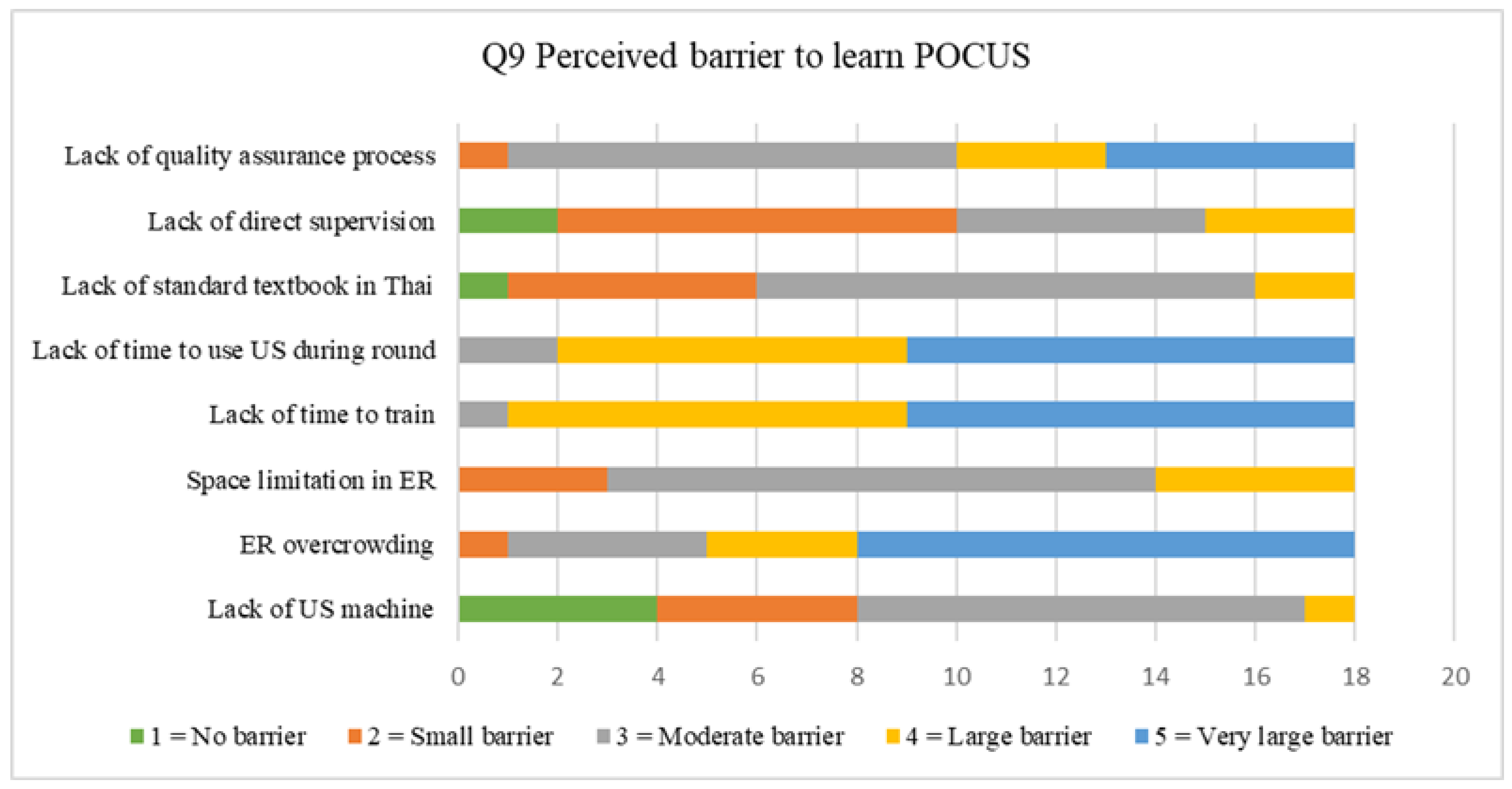
| Q9 | Perceived barrier to learn POCUS | 1 No Barrier | 2 Small Barrier | 3 Moderate Barrier | 4 Large Barrier | 5 Very Large Barrier | N/A |
| 1. Lack of ultrasound machine for learning | |||||||
| 2. ER overcrowding | |||||||
| 3. Space limitations in ER | |||||||
| 4. Lack of time to use the ultrasound during round | |||||||
| 5. Lack of time to train | |||||||
| 6. Lack of a standard POCUS textbook in the Thai language | |||||||
| 7. Lack of direct supervision | |||||||
| 8. Lack of quality assurance process | |||||||
| Q10 | How important is it to implement a POCUS education section in the Emergency Medicine residency training program? | 1 Not at All Important | 2 Slightly Important | 3 Important | 4 Very Important | 5 Extremely Important | N/A |
References
- Lichtenstein, D.; Mezière, G. A Lung Ultrasound Sign Allowing Bedside Distinction between Pulmonary Edema and COPD: The Comet-Tail Artifact. Intensive Care Med. 1998, 24, 1331–1334. [Google Scholar] [CrossRef]
- Sisley, A.C.; Rozycki, G.S.; Ballard, R.B.; Namias, N.; Salomone, J.P.; Feliciano, D.V. Rapid Detection of Traumatic Effusion Using Surgeon-Performed Ultrasonography. J. Trauma 1998, 44, 291–296; discussion 296–297. [Google Scholar] [CrossRef]
- Goldberg, B.B.; Goodman, G.A.; Clearfield, H.R. Evaluation of Ascites by Ultrasound. Radiology 1970, 96, 15–22. [Google Scholar] [CrossRef]
- Mourad, M.; Ranji, S.; Sliwka, D. A Randomized Controlled Trial of the Impact of a Teaching Procedure Service on the Training of Internal Medicine Residents. J. Grad. Med. Educ. 2012, 4, 170–175. [Google Scholar] [CrossRef] [PubMed]
- Nazeer, S.R.; Dewbre, H.; Miller, A.H. Ultrasound-Assisted Paracentesis Performed by Emergency Physicians vs the Traditional Technique: A Prospective, Randomized Study. Am. J. Emerg. Med. 2005, 23, 363–367. [Google Scholar] [CrossRef]
- Shiloh, A.L.; Savel, R.H.; Paulin, L.M.; Eisen, L.A. Ultrasound-Guided Catheterization of the Radial Artery: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Chest 2011, 139, 524–529. [Google Scholar] [CrossRef] [PubMed]
- Sibbitt, W.L.; Kettwich, L.G.; Band, P.A.; Chavez-Chiang, N.R.; DeLea, S.L.; Haseler, L.J.; Bankhurst, A.D. Does Ultrasound Guidance Improve the Outcomes of Arthrocentesis and Corticosteroid Injection of the Knee? Scand. J. Rheumatol. 2012, 41, 66–72. [Google Scholar] [CrossRef]
- Mateer, J.; Plummer, D.; Heller, M.; Olson, D.; Jehle, D.; Overton, D.; Gussow, L. Model Curriculum for Physician Training in Emergency Ultrasonography. Ann. Emerg. Med. 1994, 23, 95–102. [Google Scholar] [CrossRef]
- Hockberger, R.S.; Binder, L.S.; Graber, M.A.; Hoffman, G.L.; Perina, D.G.; Schneider, S.M.; Sklar, D.P.; Strauss, R.W.; Viravec, D.R.; Koenig, W.J.; et al. The Model of the Clinical Practice of Emergency Medicine. Ann. Emerg. Med. 2001, 37, 745–770. [Google Scholar] [CrossRef]
- Hertzberg, B.S.; Kliewer, M.A.; Bowie, J.D.; Carroll, B.A.; DeLong, D.H.; Gray, L.; Nelson, R.C. Physician Training Requirements in Sonography: How Many Cases Are Needed for Competence? AJR Am. J. Roentgenol. 2000, 174, 1221–1227. [Google Scholar] [CrossRef]
- Markowitz, J.E.; Hwang, J.Q.; Moore, C.L. Development and Validation of a Web-Based Assessment Tool for the Extended Focused Assessment with Sonography in Trauma Examination. J. Ultrasound Med. Off. J. Am. Inst. Ultrasound Med. 2011, 30, 371–375. [Google Scholar] [CrossRef] [PubMed]
- Ultrasound Guidelines: Emergency, Point-of-Care and Clinical Ultrasound Guidelines in Medicine. Ann. Emerg. Med. 2017, 69, e27–e54. [CrossRef] [PubMed] [Green Version]
- Bashir, K.; Azad, A.M.; Hereiz, A.; Bashir, M.T.; Masood, M.; Elmoheen, A. Current Use, Perceived Barriers, and Learning Preference of Point of Care Ultrasound (POCUS) in the Emergency Medicine in Qatar—A Mixed Design. Open Access Emerg. Med. OAEM 2021, 13, 177–182. [Google Scholar] [CrossRef]
- Chao, S.-L.; Chen, K.-C.; Lin, L.-W.; Wang, T.-L.; Chong, C.-F. Ultrasound Phantoms Made of Gelatin Covered with Hydrocolloid Skin Dressing. J. Emerg. Med. 2013, 45, 240–243. [Google Scholar] [CrossRef]
- LoPresti, C.M.; Schnobrich, D.J.; Dversdal, R.K.; Schembri, F. A Road Map for Point-of-Care Ultrasound Training in Internal Medicine Residency. Ultrasound J. 2019, 11, 10. [Google Scholar] [CrossRef] [Green Version]
- Janjigian, M.; Dembitzer, A.; Srisarajivakul-Klein, C.; Hardower, K.; Cooke, D.; Zabar, S.; Sauthoff, H. Design and Evaluation of the I-SCAN Faculty POCUS Program. BMC Med. Educ. 2021, 21, 22. [Google Scholar] [CrossRef]
- Russell, F.M.; Herbert, A.; Ferre, R.M.; Zakeri, B.; Echeverria, V.; Peterson, D.; Wallach, P. Development and Implementation of a Point of Care Ultrasound Curriculum at a Multi-Site Institution. Ultrasound J. 2021, 13, 9. [Google Scholar] [CrossRef]
- Safavi, A.H.; Shi, Q.; Ding, M.; Kotait, M.; Profetto, J.; Mohialdin, V.; Shali, A. Structured, Small-Group Hands-on Teaching Sessions Improve Pre-Clerk Knowledge and Confidence in Point-of-Care Ultrasound Use and Interpretation. Cureus 2018, 10, e3484. [Google Scholar] [CrossRef] [Green Version]
- Glomb, N.; D’Amico, B.; Rus, M.; Chen, C. Point-Of-Care Ultrasound in Resource-Limited Settings. Clin. Pediatr. Emerg. Med. 2015, 4, 256–261. [Google Scholar] [CrossRef]
- Haskins, S.C.; Feldman, D.; Fields, K.G.; Kirksey, M.A.; Lien, C.A.; Luu, T.H.; Nejim, J.A.; Osorio, J.A.; Yang, E.I. Teaching a Point-of-Care Ultrasound Curriculum to Anesthesiology Trainees with Traditional Didactic Lectures or an Online E-Learning Platform: A Pilot Study. J. Educ. Perioper. Med. JEPM 2018, 20, E624. [Google Scholar]
- Goldsmith, A.J.; Eke, O.F.; Alhassan Al Saud, A.; Al Mulhim, A.; Kharasch, S.; Huang, C.; Liteplo, A.S.; Shokoohi, H. Remodeling Point-of-Care Ultrasound Education in the Era of COVID-19. AEM Educ. Train. 2020, 4, 321–324. [Google Scholar] [CrossRef] [PubMed]
- Wejnarski, A.; Gajek Villebæk, P.A.; Leszczyński, P.K. Prospective evaluation of interactive project of Emergency Medicine Exam with the use of multimedia computer devices. Crit. Care Innov. 2018, 1, 1–15. [Google Scholar]
- Szucs, K.A.; Benson, J.D.; Haneman, B. Using a Guided Journal Club as a Teaching Strategy to Enhance Learning Skills for Evidence-Based Practice. Occup. Ther. Health Care 2017, 31, 143–149. [Google Scholar] [CrossRef]
- Kelm, D.J.; Ratelle, J.T.; Azeem, N.; Bonnes, S.L.; Halvorsen, A.J.; Oxentenko, A.S.; Bhagra, A. Longitudinal Ultrasound Curriculum Improves Long-Term Retention Among Internal Medicine Residents. J. Grad. Med. Educ. 2015, 7, 454–457. [Google Scholar] [CrossRef] [Green Version]
- Blans, M.J.; Pijl, M.E.J.; van de Water, J.M.; Poppe, H.J.; Bosch, F.H. The Implementation of POCUS and POCUS Training for Residents: The Rijnstate Approach. Neth. J. Med. 2020, 78, 116–124. [Google Scholar]
- Hayward, M.; Chan, T.; Healey, A. Dedicated Time for Deliberate Practice: One Emergency Medicine Program’s Approach to Point-of-Care Ultrasound (PoCUS) Training. CJEM 2015, 17, 558–561. [Google Scholar] [CrossRef] [Green Version]
- Jarwan, W.; Alshamrani, A.A.; Alghamdi, A.; Mahmood, N.; Kharal, Y.M.; Rajendram, R.; Hussain, A. Point-of-Care Ultrasound Training: An Assessment of Interns’ Needs and Barriers to Training. Cureus 2020, 12, e11209. [Google Scholar] [CrossRef]
- Shokoohi, H.; Raymond, A.; Fleming, K.; Scott, J.; Kerry, V.; Haile-Mariam, T.; Sayeed, S.; Boniface, K.S. Assessment of Point-of-Care Ultrasound Training for Clinical Educators in Malawi, Tanzania and Uganda. Ultrasound Med. Biol. 2019, 45, 1351–1357. [Google Scholar] [CrossRef] [Green Version]
- Ang, J.; Doyle, B.; Allen, P.; Cheek, C. Teaching Bedside Ultrasound to Medical Students. Clin. Teach. 2018, 15, 331–335. [Google Scholar] [CrossRef]
- Mandavia, D.P.; Aragona, J.; Chan, L.; Chan, D.; Henderson, S.O. Ultrasound Training for Emergency Physicians--a Prospective Study. Acad. Emerg. Med. Off. J. Soc. Acad. Emerg. Med. 2000, 7, 1008–1014. [Google Scholar] [CrossRef]
- Jehle, D.; Guarino, J.; Karamanoukian, H. Emergency Department Ultrasound in the Evaluation of Blunt Abdominal Trauma. Am. J. Emerg. Med. 1993, 11, 342–346. [Google Scholar] [CrossRef]
- Apiratwarakul, K.; Ienghong, K.; Tongthummachat, N.; Suzuki, T.; Tiamkao, S.; Bhudhisawasdi, V. Assessment of Competency of Point-of-Care Ultrasound in Emergency Medicine Residents during Ultrasound Rotation at the Emergency Department. Open Access Maced. J. Med. Sci. 2021, 9, 293–297. [Google Scholar] [CrossRef]
- Ienghong, K.; Kotruchin, P.; Tangpaisarn, T.; Apiratwarakul, K. Practical Emergency Ultrasound Flashcards with Augmented Reality in Teaching Point-of-Care Ultrasound in ER. Open Access Maced. J. Med. Sci. 2021, 9, 39–42. [Google Scholar] [CrossRef]
- Schwartz, C.M.; Ivancic, R.J.; McDermott, S.M.; Bahner, D.P. Designing a Low-Cost Thyroid Ultrasound Phantom for Medical Student Education. Ultrasound Med. Biol. 2020, 46, 1545–1550. [Google Scholar] [CrossRef]
- Surana, P.; Narayanan, M.K.; Parikh, D.A.; Deka, A. A Simple, Low-Cost, Customisable Ultrasound Gel-Based Phantom. Anaesth. Crit. Care Pain Med. 2020, 39, 888–890. [Google Scholar] [CrossRef]
- Selame, L.A.; Risler, Z.; Zakaria, S.J.; Hughes, L.P.; Lewiss, R.E.; Kehm, K.; Goodsell, K.; Kalwani, R.; Mirsch, D.; Kluger, S.B.; et al. A Comparison of Homemade Vascular Access Ultrasound Phantom Models for Peripheral Intravenous Catheter Insertion. J. Vasc. Access 2020, 1129729820961941. [Google Scholar] [CrossRef]
- Wong, J.; Montague, S.; Wallace, P.; Negishi, K.; Liteplo, A.; Ringrose, J.; Dversdal, R.; Buchanan, B.; Desy, J.; Ma, I.W.Y. Barriers to Learning and Using Point-of-Care Ultrasound: A Survey of Practicing Internists in Six North American Institutions. Ultrasound J. 2020, 12, 19. [Google Scholar] [CrossRef] [Green Version]
- Corell-Almuzara, A.; López-Belmonte, J.; Marín-Marín, J.-A.; Moreno-Guerrero, A.-J. COVID-19 in the Field of Education: State of the Art. Sustainability 2021, 13, 5452. [Google Scholar] [CrossRef]
- Brito, R.M.; Aparicio, J.L.; Rodríguez, C.; Beltrán, J. Sustainability Indicators in a Bachelor’s Educational Program in the Health Area. Sustainability 2021, 13, 6011. [Google Scholar] [CrossRef]
- Baribeau, Y.; Sharkey, A.; Chaudhary, O.; Krumm, S.; Fatima, H.; Mahmood, F.; Matyal, R. Handheld Point-of-Care Ultrasound Probes: The New Generation of POCUS. J. Cardiothorac. Vasc. Anesth. 2020, 34, 3139–3145. [Google Scholar] [CrossRef]
- Malik, A.N.; Rowland, J.; Haber, B.D.; Thom, S.; Jackson, B.; Volk, B.; Ehrman, R.R. The Use of Handheld Ultrasound Devices in Emergency Medicine. Curr. Emerg. Hosp. Med. Rep. 2021, 9, 73–81. [Google Scholar] [CrossRef] [PubMed]
- Varsou, O. The Use of Ultrasound in Educational Settings: What Should We Consider When Implementing This Technique for Visualisation of Anatomical Structures? Adv. Exp. Med. Biol. 2019, 1156, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Wong, C.K.; Hai, J.; Chan, K.Y.E.; Un, K.C.; Zhou, M.; Huang, D.; Cheng, Y.Y.; Li, W.H.; Yin, L.X.; Yue, W.S.; et al. Point-of-care ultrasound augments physical examination learning by undergraduate medical students. Postgrad. Med. J. 2021, 97, 10–15. [Google Scholar] [CrossRef]


| Core Emergency Ultrasound Application | Duration | Description |
|---|---|---|
| Before Pandemic (2019–2020 Academic Year) | ||
| 1. The journal club | 1 session, 3 h |
|
| 2. The review of ultrasound image | 1 session, 3 h |
|
| 3. Didactic lecture | 3 h per week |
|
| 4. Bedside ultrasound | 9 h per week |
|
| After Pandemic (2020–2021 Academic Year) | ||
| 1. The journal club | 1 session, 3 h |
|
| 2. The review of ultrasound image | 1 session, 3 h |
|
| 3. Didactic lecture | 3 h per week |
|
| 4. Bedside ultrasound | 9 h per week |
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ienghong, K.; Cheung, L.W.; Tiamkao, S.; Bhudhisawasdi, V.; Apiratwarakul, K. Development and Remodeling of Point-of-Care Ultrasound Education for Emergency Medicine Residents in Resource Limited Countries during the COVID-19 Pandemic. Tomography 2021, 7, 721-733. https://doi.org/10.3390/tomography7040060
Ienghong K, Cheung LW, Tiamkao S, Bhudhisawasdi V, Apiratwarakul K. Development and Remodeling of Point-of-Care Ultrasound Education for Emergency Medicine Residents in Resource Limited Countries during the COVID-19 Pandemic. Tomography. 2021; 7(4):721-733. https://doi.org/10.3390/tomography7040060
Chicago/Turabian StyleIenghong, Kamonwon, Lap Woon Cheung, Somsak Tiamkao, Vajarabhongsa Bhudhisawasdi, and Korakot Apiratwarakul. 2021. "Development and Remodeling of Point-of-Care Ultrasound Education for Emergency Medicine Residents in Resource Limited Countries during the COVID-19 Pandemic" Tomography 7, no. 4: 721-733. https://doi.org/10.3390/tomography7040060
APA StyleIenghong, K., Cheung, L. W., Tiamkao, S., Bhudhisawasdi, V., & Apiratwarakul, K. (2021). Development and Remodeling of Point-of-Care Ultrasound Education for Emergency Medicine Residents in Resource Limited Countries during the COVID-19 Pandemic. Tomography, 7(4), 721-733. https://doi.org/10.3390/tomography7040060








