Signed Real-Time Delay Multiply and Sum Beamforming for Multispectral Photoacoustic Imaging
Abstract
1. Introduction
- (1)
- We present a modified DMAS algorithm which we call signed DMAS (sDMAS). The modification addresses the non-linear optical and acoustic frequency response of conventional DMAS. We show linearity of sDMAS based B-Mode image reconstruction with respect to the source signal, which makes sDMAS usable for spectroscopic applications.
- (2)
- We present a graphics processing unit (GPU)-based implementation of the sDMAS algorithm which is real-time capable and therefore usable in a clinical setting. This is validated on a tissue mimicking PA characterization phantom and applied by measuring blood oxygenation in vivo on the radial artery of a healthy human volunteer.
2. Materials and Methods
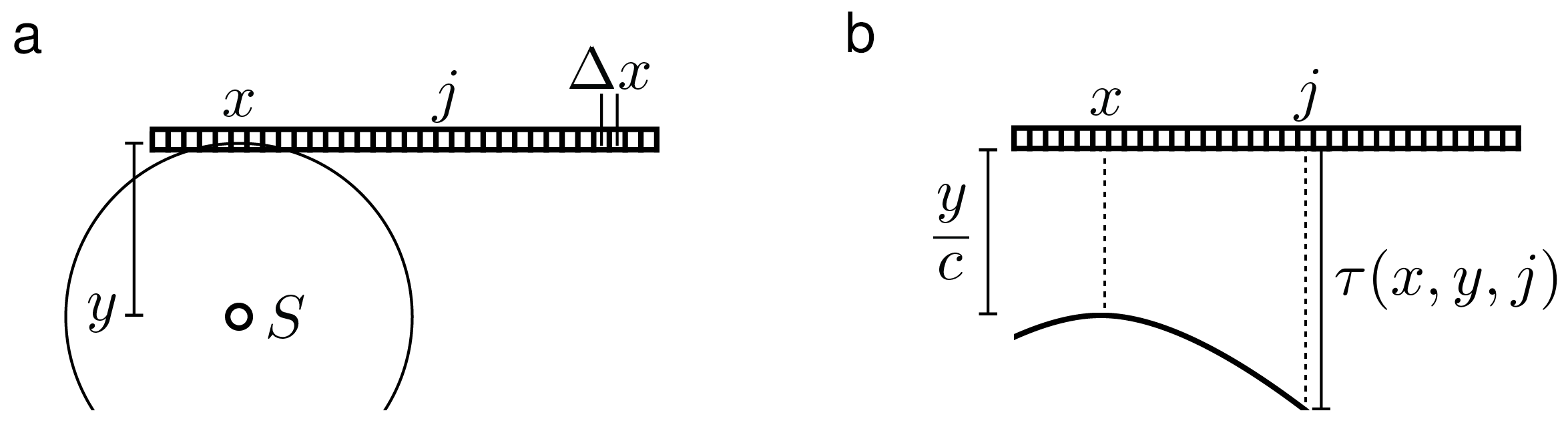
2.1. Delay and Sum Beamforming
2.2. Delay Multiply and Sum Beamforming
2.3. Signed Delay Multiply and Sum Beamforming
2.4. Linearity of Beamforming Algorithms
2.4.1. Linearity of DAS
2.4.2. Linearity of DMAS
2.4.3. Linearity of sDMAS
2.5. Implementation of Beamforming Algorithms
3. Experiments and Results
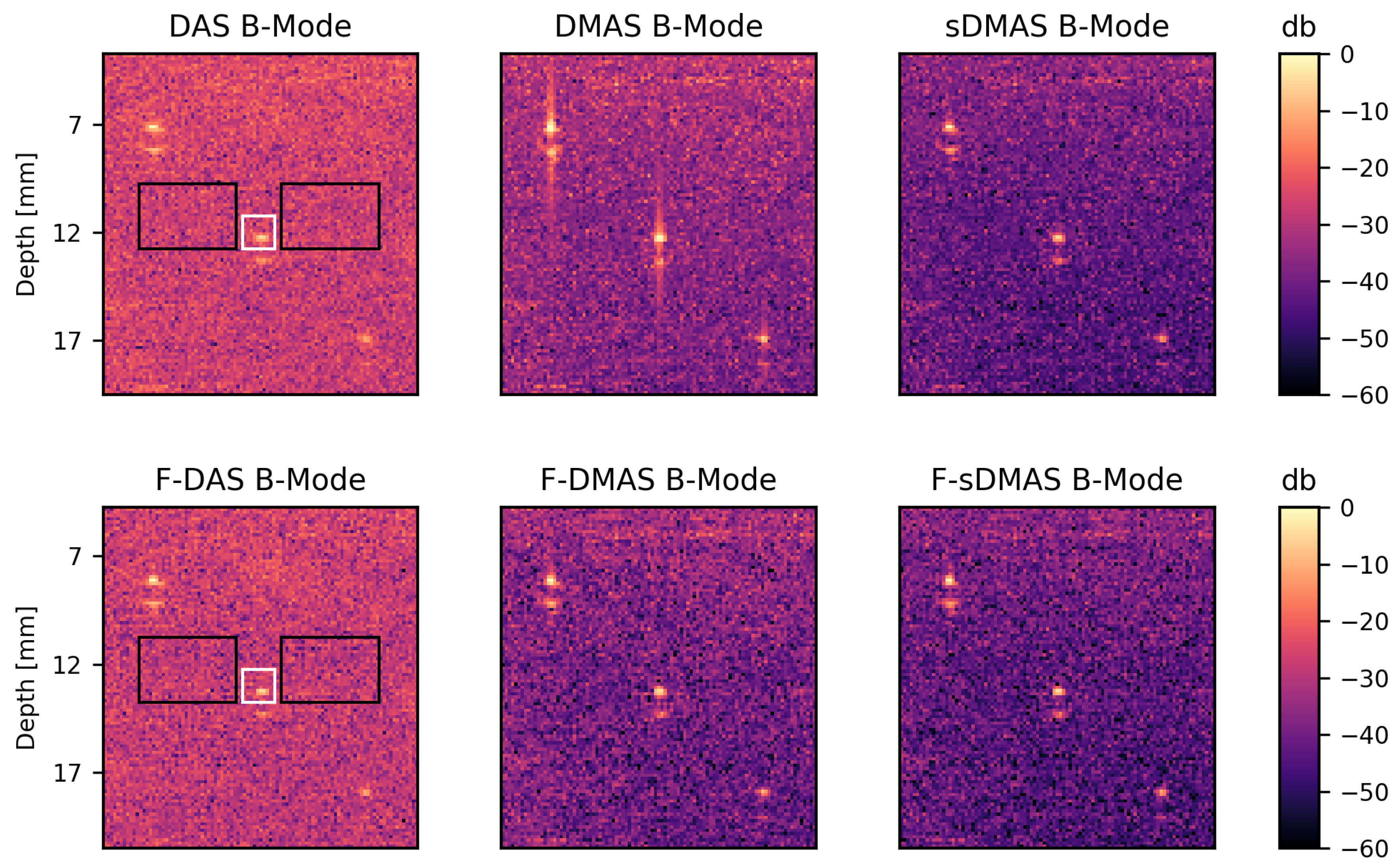
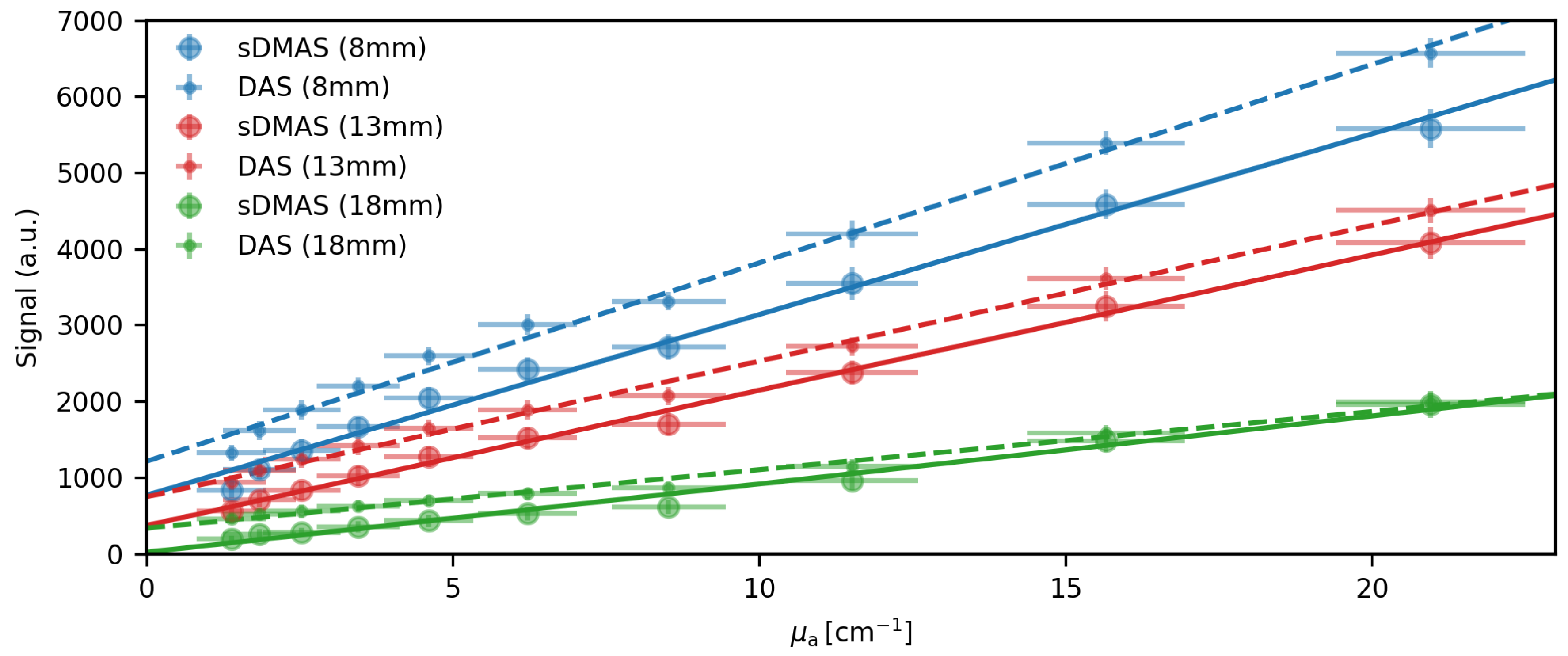
3.1. Beamforming Characterization
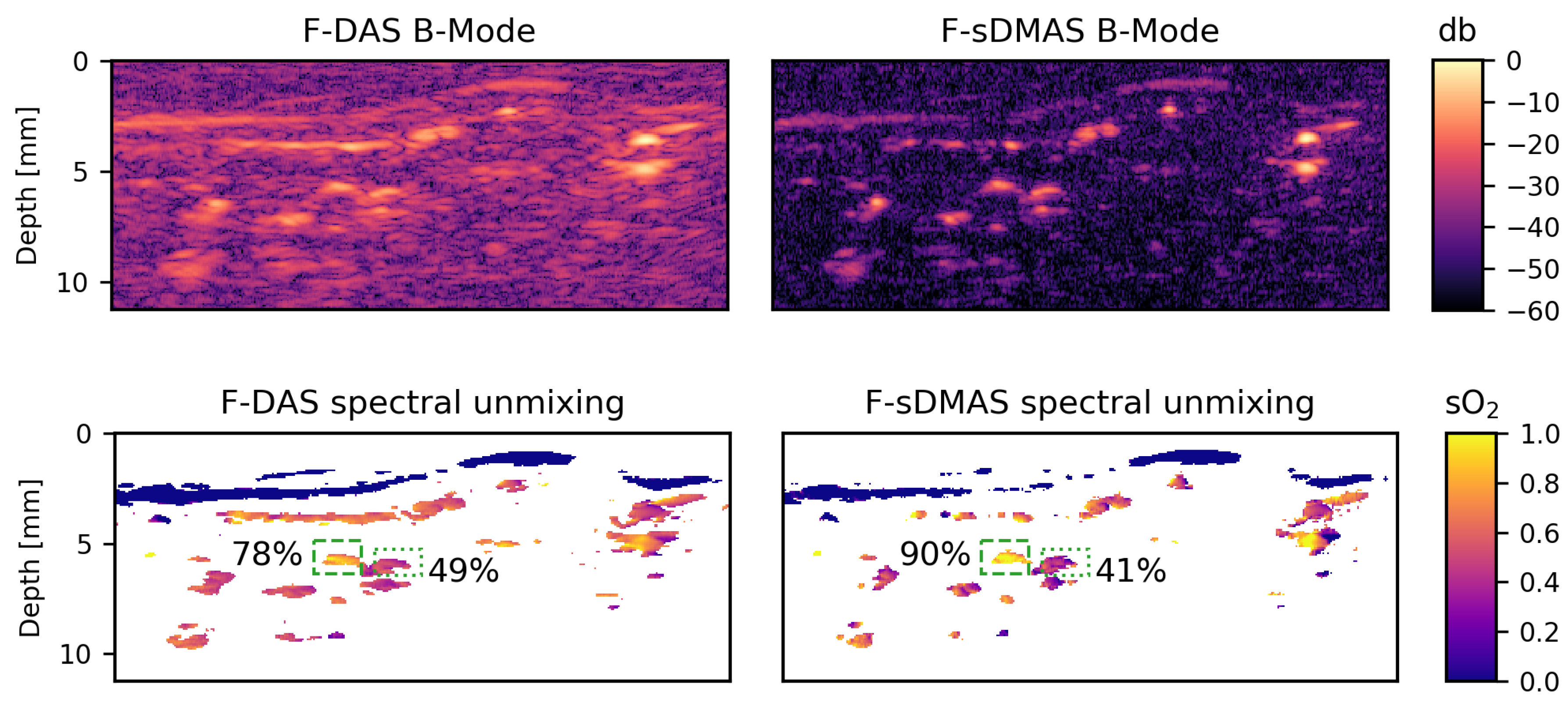
3.2. Blood Oxygenation Estimation
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| PA | photoacoustic |
| DAS | Delay and Sum |
| DMAS | Delay Multiply and Sum |
| sDMAS | signed DMAS |
| MV | Minimum Variance |
| US | ultrasonic |
| MITK | Medical Imaging Interaction Toolkit |
| SNR | Signal-to-Noise Ratio |
| CNR | Contrast-to-Noise Ratio |
| GUI | Graphical User Interface |
| API | Application Programming Interface |
| ITK | Insight Toolkit |
References
- Griffiths, L.; Jim, C. An alternative approach to linearly constrained adaptive beamforming. IEEE Trans. Antennas Propag. 1982, 30, 27–34. [Google Scholar] [CrossRef]
- Kim, J.; Park, S.; Jung, Y.; Chang, S.; Park, J.; Zhang, Y.; Lovell, J.F.; Kim, C. Programmable real-time clinical photoacoustic and ultrasound imaging system. Sci. Rep. 2016, 6. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarzadeh, M.; Mahloojifar, A.; Orooji, M.; Adabi, S.; Nasiriavanaki, M. Double Stage Delay Multiply and Sum Beamforming Algorithm: Application to Linear-Array Photoacoustic Imaging. IEEE Trans. Biomed. Eng. 2017, 65, 31–42. [Google Scholar] [CrossRef] [PubMed]
- Matrone, G.; Savoia, A.S.; Caliano, G.; Magenes, G. The Delay Multiply and Sum Beamforming Algorithm in Ultrasound B-Mode Medical Imaging. IEEE Trans. Med. Imag. 2015, 34, 940–949. [Google Scholar] [CrossRef] [PubMed]
- Park, J.; Jeon, S.; Meng, J.; Song, L.; Lee, J.S.; Kim, C. Delay-multiply-and-sum-based synthetic aperture focusing in photoacoustic microscopy. J. Biomed. Opt. 2016, 21. [Google Scholar] [CrossRef] [PubMed]
- Matrone, G.; Ramalli, A.; Savoia, A.S.; Tortoli, P.; Magenes, G. High Frame-Rate, High Resolution Ultrasound Imaging with Multi-Line Transmission and Filtered-Delay Multiply and Sum Beamforming. IEEE Trans. Med. Imag. 2017, 36, 478–486. [Google Scholar] [CrossRef] [PubMed]
- Alshaya, A.; Harput, S.; Moubark, A.M.; Cowell, D.M.; McLaughlan, J.; Freear, S. Spatial resolution and contrast enhancement in photoacoustic imaging with filter delay multiply and sum beamforming technique. In Proceedings of the 2016 IEEE International Ultrasonics Symposium (IUS), Tours, France, 18–21 September 2016; pp. 1–4. [Google Scholar]
- Treeby, B.E.; Zhang, E.Z.; Cox, B.T. Photoacoustic tomography in absorbing acoustic media using time reversal. Inverse Prob. 2010, 26. [Google Scholar] [CrossRef]
- Nolden, M.; Zelzer, S.; Seitel, A.; Wald, D.; Müller, M.; Franz, A.M.; Maleike, D.; Fangerau, M.; Baumhauer, M.; Maier-Hein, L.; et al. The Medical Imaging Interaction Toolkit: Challenges and advances. Int. J. Comput. Assist. Radiol. Surg. 2013, 8, 607–620. [Google Scholar] [CrossRef] [PubMed]
- Holfort, I.K.; Gran, F.; Jensen, J.A. Broadband minimum variance beamforming for ultrasound imaging. IEEE Trans. Ultrason. Ferroelectr. Freq. Control 2009, 56, 314–325. [Google Scholar] [CrossRef] [PubMed]
- Xu, G.; Dar, I.A.; Tao, C.; Liu, X.; Deng, C.X.; Wang, X. Photoacoustic spectrum analysis for microstructure characterization in biological tissue: A feasibility study. Appl. Phys. Lett. 2012, 101. [Google Scholar] [CrossRef] [PubMed]
- Tompson, J.; Schlachter, K. An introduction to the opencl programming model. Pers. Educ. 2012, 49, 777–780. [Google Scholar]
- Harris, F.J. On the use of windows for harmonic analysis with the discrete Fourier transform. Proc. IEEE 1978, 66, 51–83. [Google Scholar] [CrossRef]
- Laser Institute of America. American National Standard for Safe Use of Lasers; Laser Institute of America: Orlando, FL, USA, 2007. [Google Scholar]
- Kirchner, T.; Sattler, F.; Dinkelacker, S.; Goch, C.J.; Gröhl, J.; Nolden, M.; Maier-Hein, L. MITK/MITK: sDMAS-2018.07. 2018. Available online: https://zenodo.org/record/1303376#.W7_9blL3McU (accessed on 11 September 2018). [CrossRef]
- Jacques, S.L. Optical properties of biological tissues: A review. Phys. Med. Biol. 2013, 58. [Google Scholar] [CrossRef]
- Flock, S.T.; Jacques, S.L.; Wilson, B.C.; Star, W.M.; van Gemert, M.J.C. Optical properties of intralipid: A phantom medium for light propagation studies. Lasers Surg. Med. 1992, 12, 510–519. [Google Scholar] [CrossRef] [PubMed]
- Welvaert, M.; Rosseel, Y. On the Definition of Signal-To-Noise Ratio and Contrast-To-Noise Ratio for fMRI Data. PLoS ONE 2013, 8, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Zander, R. The oxygen status of arterial human blood. Scand. J. Clin. Lab. Investig. 1990, 50, 187–196. [Google Scholar] [CrossRef]
- Luke, G.P.; Nam, S.Y.; Emelianov, S.Y. Optical wavelength selection for improved spectroscopic photoacoustic imaging. Photoacoustics 2013, 1, 36–42. [Google Scholar] [CrossRef] [PubMed]
- Lawson, C.L.; Hanson, R.J. Solving Least Squares Problems; SIAM: Bangkok, Thailand, 1995. [Google Scholar]
- Mozaffarzadeh, M.; Mahloojifar, A.; Orooji, M.; Kratkiewicz, K.; Adabi, S.; Nasiriavanaki, M. Linear-array photoacoustic imaging using minimum variance-based delay multiply and sum adaptive beamforming algorithm. J. Biomed. Opt. 2018, 23. [Google Scholar] [CrossRef] [PubMed]
- Kirchner, T.; Gröhl, J.; Maier-Hein, L. Context encoding enables machine learning-based quantitative photoacoustics. J. Biomed. Opt. 2018, 23, 056008. [Google Scholar] [CrossRef] [PubMed]

| sDMAS | ||||||
|---|---|---|---|---|---|---|
| Box | Hann | |||||
| F | − | F | − | |||
| DAS | Box | F | 9 | 8 | 11 | 9 |
| − | 9 | 7 | 11 | 9 | ||
| Hann | F | 6 | 4 | 8 | 6 | |
| − | 6 | 5 | 8 | 6 | ||
| DAS | F-DMAS | sDMAS | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Box | Hann | Box | Hann | Box | Hann | |||||
| Depth | F | − | F | − | F | − | F | − | ||
| 8 mm | 5 | 5 | 8 | 7 | 10 | 11 | 12 | 10 | 14 | 11 |
| 13 mm | 4 | 5 | 8 | 7 | 12 | 14 | 14 | 13 | 17 | 15 |
| 18 mm | 0 | 0 | 6 | 8 | 8 | 6 | 10 | 8 | ||
| DAS | sDMAS | Bandpass | B-Mode | |||
|---|---|---|---|---|---|---|
| Lines | CPU | GPU | CPU | GPU | CPU | CPU |
| 128 | 29 ms | 6 ms | 502 ms | 33 ms | 9 ms | 5 ms |
| 256 | 58 ms | 18 ms | 990 ms | 63 ms | 18 ms | 10 ms |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kirchner, T.; Sattler, F.; Gröhl, J.; Maier-Hein, L. Signed Real-Time Delay Multiply and Sum Beamforming for Multispectral Photoacoustic Imaging. J. Imaging 2018, 4, 121. https://doi.org/10.3390/jimaging4100121
Kirchner T, Sattler F, Gröhl J, Maier-Hein L. Signed Real-Time Delay Multiply and Sum Beamforming for Multispectral Photoacoustic Imaging. Journal of Imaging. 2018; 4(10):121. https://doi.org/10.3390/jimaging4100121
Chicago/Turabian StyleKirchner, Thomas, Franz Sattler, Janek Gröhl, and Lena Maier-Hein. 2018. "Signed Real-Time Delay Multiply and Sum Beamforming for Multispectral Photoacoustic Imaging" Journal of Imaging 4, no. 10: 121. https://doi.org/10.3390/jimaging4100121
APA StyleKirchner, T., Sattler, F., Gröhl, J., & Maier-Hein, L. (2018). Signed Real-Time Delay Multiply and Sum Beamforming for Multispectral Photoacoustic Imaging. Journal of Imaging, 4(10), 121. https://doi.org/10.3390/jimaging4100121





