A Review of Motion-Preserving Cervical Spinal Implants and Fusion Constructs
Abstract
1. Introduction
1.1. Clinical Role of Spinal Fusion
1.2. Biomechanical Consequences of Motion Elimination
1.3. Rationale for Motion-Preserving Technologies
1.4. Knowledge Gaps in Cervical Motion Preservation
2. Methods
2.1. Study Design
2.2. Literature Identification and Scope
2.3. Evidence Selection and Narrative Synthesis
2.4. Management of Bias
2.5. Ordinal Biomechanical Scoring Framework
3. Results
3.1. Fusion Biomechanics
3.1.1. Effects of Segmental Motility and Stability
3.1.2. Effects on Adjacent Segments: Compensatory Hypermobility
3.1.3. Additional Effects on Adjacent Segments, Load Redistribution, and ASD
3.1.4. Materials and Designs of Fusion Devices
3.2. Motion-Preserving Technologies
3.2.1. Biomechanical Rationale for Cervical Disc Arthroplasty
3.2.2. Effects on Segmental and Adjacent-Level Kinematics
3.2.3. Load Redistribution and Mechanistic Insights from Finite Element Analysis
3.2.4. Implant-Dependent Global Cervical Motion Patterns
3.2.5. Long-Term Data
3.2.6. Limitations in Long-Term Data
3.3. Case Studies
3.3.1. Cadaveric Studies
3.3.2. Clinical Outcomes
3.3.3. Finite Element Analysis Complexity
3.4. Modeling and Regulatory Limitations
Regulatory Processes
4. Future Directions
4.1. Proposed Workflow
4.2. Image Acquisition and Segmentation
4.3. Biomechanical Modeling and Simulation
4.4. Implant Design Optimization
4.5. Manufacturing and Validation
4.6. Surgical Implementation
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| PU | Polyurethane |
| PE | Polyethylene |
| Ti | Titanium |
| FEA | Finite Element Analysis |
References
- Johansen, T.O.; Sundseth, J.; Fredriksli, O.A.; Andresen, H.; Zwart, J.-A.; Kolstad, F.; Pripp, A.H.; Gulati, S.; Nygaard, Ø.P. Effect of Arthroplasty vs Fusion for Patients with Cervical Radiculopathy: A Randomized Clinical Trial. JAMA Netw. Open 2021, 4, e2119606. [Google Scholar] [CrossRef]
- Carette, S.; Fehlings, M.G. Cervical Radiculopathy. N. Engl. J. Med. 2005, 353, 392–399. [Google Scholar] [CrossRef] [PubMed]
- Eck, J.C.; Humphreys, S.C.; Lim, T.-H.; Jeong, S.T.; Kim, J.G.; Hodges, S.D.; An, H.S. Biomechanical Study on the Effect of Cervical Spine Fusion on Adjacent-Level Intradiscal Pressure. Spine 2002, 27, 2431–2434. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, B.D.; Hilibrand, A.S.; Brodt, E.D.; Dettori, J.R.; Brodke, D.S. Predicting the Risk of Adjacent Segment Pathology in the Cervical Spine: A Systematic Review. Spine 2012, 37, S52. [Google Scholar] [CrossRef] [PubMed]
- Nikkhoo, M.; Lu, M.-L.; Chen, W.-C.; Fu, C.-J.; Niu, C.-C.; Lin, Y.-H.; Cheng, C.-H. Biomechanical Investigation Between Rigid and Semirigid Posterolateral Fixation During Daily Activities: Geometrically Parametric Poroelastic Finite Element Analyses. Front. Bioeng. Biotechnol. 2021, 9, 646079. [Google Scholar] [CrossRef]
- Donnally, C.J.; Patel, P.D.; Canseco, J.A.; Divi, S.N.; Goz, V.; Sherman, M.B.; Shenoy, K.; Markowitz, M.; Rihn, J.A.; Vaccaro, A.R. Current Incidence of Adjacent Segment Pathology Following Lumbar Fusion versus Motion-Preserving Procedures: A Systematic Review and Meta-Analysis of Recent Projections. Spine J. 2020, 20, 1554–1565. [Google Scholar] [CrossRef]
- Gandhi, A.A.; Kode, S.; DeVries, N.A.; Grosland, N.M.; Smucker, J.D.; Fredericks, D.C. Biomechanical Analysis of Cervical Disc Replacement and Fusion Using Single Level, Two Level, and Hybrid Constructs. Spine 2015, 40, 1578. [Google Scholar] [CrossRef]
- Finn, M.A.; Brodke, D.S.; Daubs, M.; Patel, A.; Bachus, K.N. Local and Global Subaxial Cervical Spine Biomechanics after Single-Level Fusion or Cervical Arthroplasty. Eur. Spine J. 2009, 18, 1520–1527. [Google Scholar] [CrossRef]
- Dmitriev, A.E.; Kuklo, T.R.; Lehman, R.A.; Rosner, M.K. Stabilizing Potential of Anterior, Posterior, and Circumferential Fixation for Multilevel Cervical Arthrodesis: An In Vitro Human Cadaveric Study of the Operative and Adjacent Segment Kinematics. Spine 2007, 32, E188–E196. [Google Scholar] [CrossRef]
- Farber, S.H.; Mugge, L.A.; Sawa, A.G.U.; DiDomenico, J.D.; Assefa, T.G.; Ratliff, A.C.; Crawford, N.R.; Uribe, J.S.; Kelly, B.P.; Turner, J.D. Clinical Effect of Occipitocervical and Subaxial Cervical Fusion Constructs on Range of Motion: Comprehensive Guide Based on Biomechanical Cadaveric Testing on 1009 Motion Segments. J. Neurosurg. Spine 2025, 43, 352–360. [Google Scholar] [CrossRef]
- Leahy, J.C.; Hukins, D.W. Viscoelastic Properties of Nucleus Pulposus. J. Back Musculoskelet. Rehabil. 1997, 9, 47–48. [Google Scholar] [CrossRef]
- Shoukry, H.; Elashhab, M.; Bakr, A.I.; Ahmed, A.S. Biomechanical Changes Following Cervical Disc Arthroplasty. Ortop. Traumatol. Rehabil. 2025, 27, 87–93. [Google Scholar] [CrossRef] [PubMed]
- Palepu, V.; Kodigudla, M.; Goel, V.K. Biomechanics of Disc Degeneration. Adv. Orthop. 2012, 2012, 726210. [Google Scholar] [CrossRef] [PubMed]
- Dahl, M.C.; Jacobsen, S.; Metcalf, N.; Sasso, R.; Ching, R.P. A Comparison of the Shock-Absorbing Properties of Cervical Disc Prosthesis Bearing Materials. SAS J. 2011, 5, 48–54. [Google Scholar] [CrossRef]
- Schwab, J.S.; DiAngelo, D.J.; Foley, K.T. Motion Compensation Associated with Single-Level Cervical Fusion: Where Does the Lost Motion Go? Spine 2006, 31, 2439–2448. [Google Scholar] [CrossRef] [PubMed]
- Hua, W.; Zhi, J.; Ke, W.; Wang, B.; Yang, S.; Li, L.; Yang, C. Adjacent Segment Biomechanical Changes after One- or Two-Level Anterior Cervical Discectomy and Fusion Using Either a Zero-Profile Device or Cage plus Plate: A Finite Element Analysis. Comput. Biol. Med. 2020, 120, 103760. [Google Scholar] [CrossRef]
- Chang, U.-K.; Kim, D.H.; Lee, M.C.; Willenberg, R.; Kim, S.-H.; Lim, J. Changes in Adjacent-Level Disc Pressure and Facet Joint Force after Cervical Arthroplasty Compared with Cervical Discectomy and Fusion. J. Neurosurg. Spine 2007, 7, 33–39. [Google Scholar] [CrossRef]
- Wang, Y.; Shen, Q.; Liang, C.; Shen, Y.; Tang, X.; Yi, P. Biomechanical Analysis of Adjacent Segments after Spinal Fusion Surgery Using a Geometrically Parametric Patient-Specific Finite Element Model. J. Vis. Exp. 2024, 203, e66247. [Google Scholar] [CrossRef]
- Cheng, C.-H.; Chiu, P.-Y.; Chen, H.-B.; Niu, C.-C.; Nikkhoo, M. The Influence of Over-Distraction on Biomechanical Response of Cervical Spine Post Anterior Interbody Fusion: A Comprehensive Finite Element Study. Front. Bioeng. Biotechnol. 2023, 11, 1217274. [Google Scholar] [CrossRef]
- Liang, W.; Han, B.; Hai, Y.; Yang, J.; Yin, P. Biomechanical Analysis of the Reasonable Cervical Range of Motion to Prevent Non-Fusion Segmental Degeneration After Single-Level ACDF. Front. Bioeng. Biotechnol. 2022, 10, 918032. [Google Scholar] [CrossRef]
- Seaman, S.; Kerezoudis, P.; Bydon, M.; Torner, J.C.; Hitchon, P.W. Titanium vs. Polyetheretherketone (PEEK) Interbody Fusion: Meta-Analysis and Review of the Literature. J. Clin. Neurosci. 2017, 44, 23–29. [Google Scholar] [CrossRef]
- Muthiah, N.; Yolcu, Y.U.; Alan, N.; Agarwal, N.; Hamilton, D.K.; Ozpinar, A. Evolution of Polyetheretherketone (PEEK) and Titanium Interbody Devices for Spinal Procedures: A Comprehensive Review of the Literature. Eur. Spine J. 2022, 31, 2547–2556. [Google Scholar] [CrossRef]
- Müller, U.; Imwinkelried, T.; Horst, M.; Sievers, M.; Graf-Hausner, U. Do Human Osteoblasts Grow into Open-Porous Titanium? Eur. Cell Mater. 2006, 11, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Olivares-Navarrete, R.; Hyzy, S.L.; Gittens, R.A.; Schneider, J.M.; Haithcock, D.A.; Ullrich, P.F.; Slosar, P.J.; Schwartz, Z.; Boyan, B.D. Rough Titanium Alloys Regulate Osteoblast Production of Angiogenic Factors. Spine J. 2013, 13, 1563–1570. [Google Scholar] [CrossRef] [PubMed]
- Briem, D.; Strametz, S.; Schröoder, K.; Meenen, N.M.; Lehmann, W.; Linhart, W.; Ohl, A.; Rueger, J.M. Response of Primary Fibroblasts and Osteoblasts to Plasma Treated Polyetheretherketone (PEEK) Surfaces. J. Mater. Sci. Mater. Med. 2005, 16, 671–677. [Google Scholar] [CrossRef]
- Cohen, J.D.; Kanim, L.E.; Tronits, A.J.; Bae, H.W. Allografts and Spinal Fusion. Int. J. Spine Surg. 2021, 15, 68–93. [Google Scholar] [CrossRef] [PubMed]
- Peng, Q.; Yang, S.; Zhang, Y.; Liu, H.; Meng, B.; Zhao, W.; Hu, M.; Zhang, Y.; Chen, L.; Sun, H.; et al. Effects of Structural Allograft versus Polyetheretherketone Cage in Patients Undergoing Spinal Fusion Surgery: A Systematic Review and Meta-Analysis. World Neurosurg. 2023, 178, 162–171.e7. [Google Scholar] [CrossRef]
- Choi, H.; Purushothaman, Y.; Baisden, J.L.; Rajasekaran, D.; Jebaseelan, D.; Yoganandan, N. Comparative Finite Element Modeling Study of Anterior Cervical Arthrodesis Versus Cervical Arthroplasty with Bryan Disc or Prodisc C. Mil. Med. 2021, 186, 737–744. [Google Scholar] [CrossRef]
- Dmitriev, A.E.; Cunningham, B.W.; Hu, N.; Sell, G.; Vigna, F.; McAfee, P.C. Adjacent Level Intradiscal Pressure and Segmental Kinematics Following a Cervical Total Disc Arthroplasty: An in Vitro Human Cadaveric Model. Spine 2005, 30, 1165–1172. [Google Scholar] [CrossRef]
- Abudouaini, H.; Wu, T.; Meng, Y.; Ding, C.; Liu, H.; Beiyu, W. Biomechanical Properties of a Novel Cervical Spine Implant with Elastic Deformation: A Cadaveric Study. Front. Bioeng. Biotechnol. 2023, 11, 1214877. [Google Scholar] [CrossRef]
- Gandhi, A.A.; Grosland, N.M.; Kallemeyn, N.A.; Kode, S.; Fredericks, D.C.; Smucker, J.D. Biomechanical Analysis of the Cervical Spine Following Disc Degeneration, Disc Fusion, and Disc Replacement: A Finite Element Study. Int. J. Spine Surg. 2019, 13, 491–500. [Google Scholar] [CrossRef]
- Choi, H.; Purushothaman, Y.; Baisden, J.; Yoganandan, N. Unique Biomechanical Signatures of Bryan, Prodisc C, and Prestige LP Cervical Disc Replacements: A Finite Element Modelling Study. Eur. Spine J. 2020, 29, 2631–2639. [Google Scholar] [CrossRef]
- He, J.; Li, Y.; Shen, Y.; Wang, X.; Yan, L.; Wu, T.; Ding, C.; Liu, H. Long-Term Results of Cervical Disc Arthroplasty: A Single-Center Retrospective Study with a Minimum 10-Year Follow-Up. J. Neurosurg. Spine 2025, 1, 195–204. [Google Scholar] [CrossRef]
- Kang, H.; Park, P.; La Marca, F.; Hollister, S.J.; Lin, C.-Y. Analysis of Load Sharing on Uncovertebral and Facet Joints at the C5–6 Level with Implantation of the Bryan, Prestige LP, or ProDisc-C Cervical Disc Prosthesis: An in Vivo Image-Based Finite Element Study. Neurosurg. Focus 2010, 28, E9. [Google Scholar] [CrossRef] [PubMed]
- Khalaf, K.; Nikkhoo, M. Comparative Biomechanical Analyses of Lower Cervical Spine Post Anterior Fusion versus Intervertebral Disc Arthroplasty: A Geometrically Patient-Specific Poroelastic Finite Element Investigation. J. Orthop. Transl. 2022, 36, 33–43. [Google Scholar] [CrossRef] [PubMed]
- Kowalczyk, I.; Lazaro, B.C.R.; Fink, M.; Rabin, D.; Duggal, N. Analysis of in Vivo Kinematics of 3 Different Cervical Devices: Bryan Disc, ProDisc-C, and Prestige LP Disc. J. Neurosurg. Spine 2011, 15, 630–635. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Xiong, Y.; Wang, T.; Yu, X.; Li, C.; Meng, L.; Zhao, H.; Yang, Y.; Zhao, D.; Wang, F.; et al. Kinematic Status of Bryan and Mobi-C Artificial Cervical Discs Post Cervical Hybrid Surgery: A Retrospective Study. J. Orthop. Surg. 2024, 19, 857. [Google Scholar] [CrossRef]
- Oh, H.M.; Heo, W. Preliminary Radiological Outcomes of Cervical Arthroplasty with Bryan and Prestige LP Cervical Disc Prosthesis. Age 2008, 41, 47. [Google Scholar]
- Yoganandan, N.; Purushothaman, Y.; Choi, H.; Baisden, J.; Rajasekaran, D.; Banerjee, A.; Jebaseelan, D.; Kurpad, S. Biomechanical Study of Cervical Disc Arthroplasty Devices Using Finite Element Modeling. J. Eng. Sci. Med. Diagn. Ther. 2021, 4, 021004. [Google Scholar] [CrossRef]
- Rosenthal, P.; Kim, K.D. Cervical Adjacent Segment Pathology Following Fusion: Is It Due to Fusion? World J. Orthop. 2013, 4, 112–113. [Google Scholar] [CrossRef]
- Chang, U.-K.; Kim, D.H.; Lee, M.C.; Willenberg, R.; Kim, S.-H.; Lim, J. Range of Motion Change after Cervical Arthroplasty with ProDisc-C and Prestige Artificial Discs Compared with Anterior Cervical Discectomy and Fusion. J. Neurosurg. Spine 2007, 7, 40–46. [Google Scholar] [CrossRef] [PubMed]
- Jiang, W.; Zhao, F.; Rahman, W.U.; Dong, T.; Yang, G. Comparison of the Effects of Different Artificial Discs on Hybrid Surgery: A Finite Element Analysis. Proc. Inst. Mech. Eng. Part H J. Eng. Med. 2024, 238, 78–89. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.-Y.; Kang, H.; Rouleau, J.P.; Hollister, S.J.; Marca, F.L. Stress Analysis of the Interface Between Cervical Vertebrae End Plates and the Bryan, Prestige LP, and ProDisc-C Cervical Disc Prostheses: An In Vivo Image-Based Finite Element Study. Spine 2009, 34, 1554–1560. [Google Scholar] [CrossRef] [PubMed]
- Anderson, P.A.; Sasso, R.C.; Hipp, J.; Norvell, D.C.; Raich, A.; Hashimoto, R. Kinematics of the Cervical Adjacent Segments after Disc Arthroplasty Compared with Anterior Discectomy and Fusion: A Systematic Review and Meta-Analysis. Spine 2012, 37, S85–S95. [Google Scholar] [CrossRef]
- Auerbach, J.D.; Anakwenze, O.A.; Milby, A.H.; Lonner, B.S.; Balderston, R.A. Segmental Contribution Toward Total Cervical Range of Motion: A Comparison of Cervical Disc Arthroplasty and Fusion. Spine 2011, 36, E1593. [Google Scholar] [CrossRef] [PubMed]
- Yakdan, S.; Benedict, B.; Botterbush, K.; Lagisetty, A.; Kaleem, M.I.; Alessio, R.; Hardi, A.; Javeed, S.; Ruiz-Cardozo, M.A.; Yahanda, A.T.; et al. Randomized Controlled Trials Comparing Cervical Disc Arthroplasty and Anterior Cervical Discectomy and Fusion Outcomes in Degenerative Spine Disease: A Systematic Review and Meta-Analysis. J. Neurosurg. Spine 2025, 1, 1–14. [Google Scholar] [CrossRef]
- Ghobrial, G.M.; Lavelle, W.F.; Florman, J.E.; Riew, K.D.; Levi, A.D. Symptomatic Adjacent Level Disease Requiring Surgery: Analysis of 10-Year Results From a Prospective, Randomized, Clinical Trial Comparing Cervical Disc Arthroplasty to Anterior Cervical Fusion. Neurosurgery 2019, 84, 347. [Google Scholar] [CrossRef]
- Sasso, W.R.; Ye, J.; Foley, D.P.; Vinayek, S.; Sasso, R.C. 20-Year Clinical Outcomes of Cervical Disk Arthroplasty: A Prospective, Randomized, Controlled Trial. Spine 2024, 49, 1. [Google Scholar] [CrossRef]
- Alsalek, S.; Chang, R.N.; Harary, M.; Florence, T.; Laiwalla, A.N.; Prentice, H.A.; Brara, H.S.; Harris, J.E.; Hirt, D.; Richards, H.G.; et al. Reoperation Risks Between Cervical Disc Arthroplasty and Anterior Cervical Discectomy with Fusion: It Is Not Always About Adjacent Segment Disease. Spine 2026, 51, 160–169. [Google Scholar] [CrossRef]
- Foley, D.P.; Sasso, W.R.; Ye, J.Y.; Vinayek, S.; Smucker, J.D.; McCarthy, M.H.; Boody, B.S.; Sasso, R.C. Twenty-Year Radiographic Outcomes Following Single-Level Cervical Disc Arthroplasty: Results From a Prospective Randomized Controlled Trial. Spine 2024, 49, 295. [Google Scholar] [CrossRef]
- Burkhardt, B.W.; Baumann, L.; Simgen, A.; Wagenpfeil, G.; Hendrix, P.; Reith, W.; Oertel, J.M. Long-Term Follow-up MRI Shows No Hastening of Adjacent Segment Degeneration Following Cervical Disc Arthroplasty. Sci. Rep. 2022, 12, 13318. [Google Scholar] [CrossRef]
- Kim, K.; Hoffman, G.; Bae, H.; Redmond, A.; Hisey, M.; Nunley, P.; Jackson, R.; Tahernia, D.; Araghi, A. Ten-Year Outcomes of 1- and 2-Level Cervical Disc Arthroplasty From the Mobi-C Investigational Device Exemption Clinical Trial. Neurosurgery 2021, 88, 497. [Google Scholar] [CrossRef]
- Lee, M.J.; Dumonski, M.; Phillips, F.M.; Voronov, L.I.; Renner, S.M.; Carandang, G.; Havey, R.M.; Patwardhan, A.G. Disc Replacement Adjacent to Cervical Fusion: A Biomechanical Comparison of Hybrid Construct versus Two-Level Fusion. Spine 2011, 36, 1932–1939. [Google Scholar] [CrossRef]
- Panjabi, M.M. The Stabilizing System of the Spine. Part II. Neutral Zone and Instability Hypothesis. J. Spinal Disord. 1992, 5, 390–396; discussion 397. [Google Scholar] [CrossRef] [PubMed]
- Terai, T.; Faizan, A.; Sairyo, K.; Goel, V.K. Operated and Adjacent Segment Motions for Fusion versus Cervical Arthroplasty: A Pilot Study. Clin. Orthop. 2011, 469, 682–687. [Google Scholar] [CrossRef]
- Patwardhan, A.G.; Havey, R.M. Biomechanics of Cervical Disc Arthroplasty—A Review of Concepts and Current Technology. Int. J. Spine Surg. 2020, 14, S14–S28. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.-H.; Im, Y.-J.; Kim, K.-T.; Kim, Y.-H.; Park, W.-M.; Kim, K. Comparison of Cervical Spine Biomechanics after Fixed- and Mobile-Core Artificial Disc Replacement: A Finite Element Analysis. Spine 2011, 36, 700–708. [Google Scholar] [CrossRef]
- Wang, M.C.; Kiapour, A.; Massaad, E.; Shin, J.H.; Yoganandan, N. A Guide to Finite Element Analysis Models of the Spine for Clinicians. J. Neurosurg. Spine 2024, 40, 38–44. [Google Scholar] [CrossRef] [PubMed]
- Singhal, I.; Harinathan, B.; Warraich, A.; Purushothaman, Y.; Budde, M.; Yoganandan, N.; Vedantam, A. Finite Element Modeling of the Human Cervical Spinal Cord and Its Applications: A Systematic Review. North Am. Spine Soc. J. NASSJ 2023, 15, 100246. [Google Scholar] [CrossRef]
- Alizadeh, M.; Knapik, G.G.; Mageswaran, P.; Mendel, E.; Bourekas, E.; Marras, W.S. Biomechanical Musculoskeletal Models of the Cervical Spine: A Systematic Literature Review. Clin. Biomech. 2020, 71, 115–124. [Google Scholar] [CrossRef]
- Silva, A.J.C.; Alves de Sousa, R.J.; Fernandes, F.A.O.; Ptak, M.; Parente, M.P.L. Development of a Finite Element Model of the Cervical Spine and Validation of a Functional Spinal Unit. Appl. Sci. 2022, 12, 11295. [Google Scholar] [CrossRef]
- Sasso, R.C.; Smucker, J.D.; Hacker, R.J.; Heller, J.G. Clinical Outcomes of BRYAN Cervical Disc Arthroplasty: A Prospective, Randomized, Controlled, Multicenter Trial with 24-Month Follow-Up. J. Spinal Disord. Tech. 2007, 20, 481–491. [Google Scholar] [CrossRef]
- Mummaneni, P.V.; Burkus, J.K.; Haid, R.W.; Traynelis, V.C.; Zdeblick, T.A. Clinical and Radiographic Analysis of Cervical Disc Arthroplasty Compared with Allograft Fusion: A Randomized Controlled Clinical Trial. J. Neurosurg. Spine 2007, 6, 198–209. [Google Scholar] [CrossRef]
- Shen, J.; Nemani, V.M.; Leveque, J.-C.; Sethi, R. Personalized Medicine in Orthopaedic Surgery: The Case of Spine Surgery. J. Am. Acad. Orthop. Surg. 2023, 31, 901–907. [Google Scholar] [CrossRef]
- Spetzger, U.; Frasca, M.; König, S.A. Surgical Planning, Manufacturing and Implantation of an Individualized Cervical Fusion Titanium Cage Using Patient-Specific Data. Eur. Spine J. Off. Publ. Eur. Spine Soc. Eur. Spinal Deform. Soc. Eur. Sect. Cerv. Spine Res. Soc. 2016, 25, 2239–2246. [Google Scholar] [CrossRef]
- Zhang, M.; Pu, F.; Xu, L.; Zhang, L.; Liang, H.; Li, D.; Wang, Y.; Fan, Y. Development of an Integrated CAD-FEA System for Patient-Specific Design of Spinal Cages. Comput. Methods Biomech. Biomed. Engin. 2017, 20, 355–364. [Google Scholar] [CrossRef]
- Ahmadi, M.; Chen, H.; Lin, M.; Biswas, D.; Doulgeris, J.; Tang, Y.; Engeberg, E.D.; Hashemi, J.; Pires, G.; Vrionis, F.D. Streamlined and Efficient Patient-Specific Modeling for Lumbar Spine Segmentation and Finite Element Analysis. Sci. Rep. 2025, 15, 35619. [Google Scholar] [CrossRef] [PubMed]
- Lin, M.; Shapiro, S.Z.; Engeberg, E.D.; Tsai, C.-T.; Vrionis, F.D. Finite Element Analysis of the Effect of Dynamic Plating on Two-Level Anterior Cervical Discectomy Fusion Biomechanics. World Neurosurg. 2022, 163, e43–e52. [Google Scholar] [CrossRef] [PubMed]
- Lin, M.; Paul, R.; Dhar, U.K.; Doulgeris, J.; O’Connor, T.E.; Tsai, C.-T.; Vrionis, F.D. A Review of Finite Element Modeling for Anterior Cervical Discectomy and Fusion. Asian Spine J. 2023, 17, 949–963. [Google Scholar] [CrossRef]
- Kok, J.; Shcherbakova, Y.M.; Schlösser, T.P.C.; Seevinck, P.R.; van der Velden, T.A.; Castelein, R.M.; Ito, K.; van Rietbergen, B. Automatic Generation of Subject-Specific Finite Element Models of the Spine from Magnetic Resonance Images. Front. Bioeng. Biotechnol. 2023, 11, 1244291. [Google Scholar] [CrossRef] [PubMed]
- Caprara, S.; Carrillo, F.; Snedeker, J.G.; Farshad, M.; Senteler, M. Automated Pipeline to Generate Anatomically Accurate Patient-Specific Biomechanical Models of Healthy and Pathological FSUs. Front. Bioeng. Biotechnol. 2021, 9, 636953. [Google Scholar] [CrossRef] [PubMed]
- Nispel, K.; Lerchl, T.; Gruber, G.; Moeller, H.; Graf, R.; Senner, V.; Kirschke, J.S. From MRI to FEM: An Automated Pipeline for Biomechanical Simulations of Vertebrae and Intervertebral Discs. Front. Bioeng. Biotechnol. 2024, 12, 1485115. [Google Scholar] [CrossRef] [PubMed]
- George, S.P.; Venkatesh, K.; Saravana Kumar, G. Development, Calibration and Validation of a Comprehensive Customizable Lumbar Spine FE Model for Simulating Fusion Constructs. Med. Eng. Phys. 2023, 118, 104016. [Google Scholar] [CrossRef] [PubMed]
- Kallemeyn, N.; Gandhi, A.; Kode, S.; Shivanna, K.; Smucker, J.; Grosland, N. Validation of a C2-C7 Cervical Spine Finite Element Model Using Specimen-Specific Flexibility Data. Med. Eng. Phys. 2010, 32, 482–489. [Google Scholar] [CrossRef]
- Cai, Y.; Dall’Ara, E.; Lacroix, D.; Guo, L. Deep Learning-Based Surrogate Model of Subject-Specific Finite-Element Analysis for Vertebrae. IEEE Trans. Biomed. Eng. 2025, 1–11. [Google Scholar] [CrossRef]
- Kang, J.; Dong, E.; Li, X.; Guo, Z.; Shi, L.; Li, D.; Wang, L. Topological Design and Biomechanical Evaluation for 3D Printed Multi-Segment Artificial Vertebral Implants. Mater. Sci. Eng. C Mater. Biol. Appl. 2021, 127, 112250. [Google Scholar] [CrossRef]
- Smit, T.; Aage, N.; Haschtmann, D.; Ferguson, S.J.; Helgason, B. Anatomically and Mechanically Conforming Patient-Specific Spinal Fusion Cages Designed by Full-Scale Topology Optimization. J. Mech. Behav. Biomed. Mater. 2024, 159, 106695. [Google Scholar] [CrossRef]
- Thayaparan, G.K.; Owbridge, M.G.; Thompson, R.G.; D’Urso, P.S. Designing Patient-Specific Solutions Using Biomodelling and 3D-Printing for Revision Lumbar Spine Surgery. Eur. Spine J. Off. Publ. Eur. Spine Soc. Eur. Spinal Deform. Soc. Eur. Sect. Cerv. Spine Res. Soc. 2019, 28, 18–24. [Google Scholar] [CrossRef]





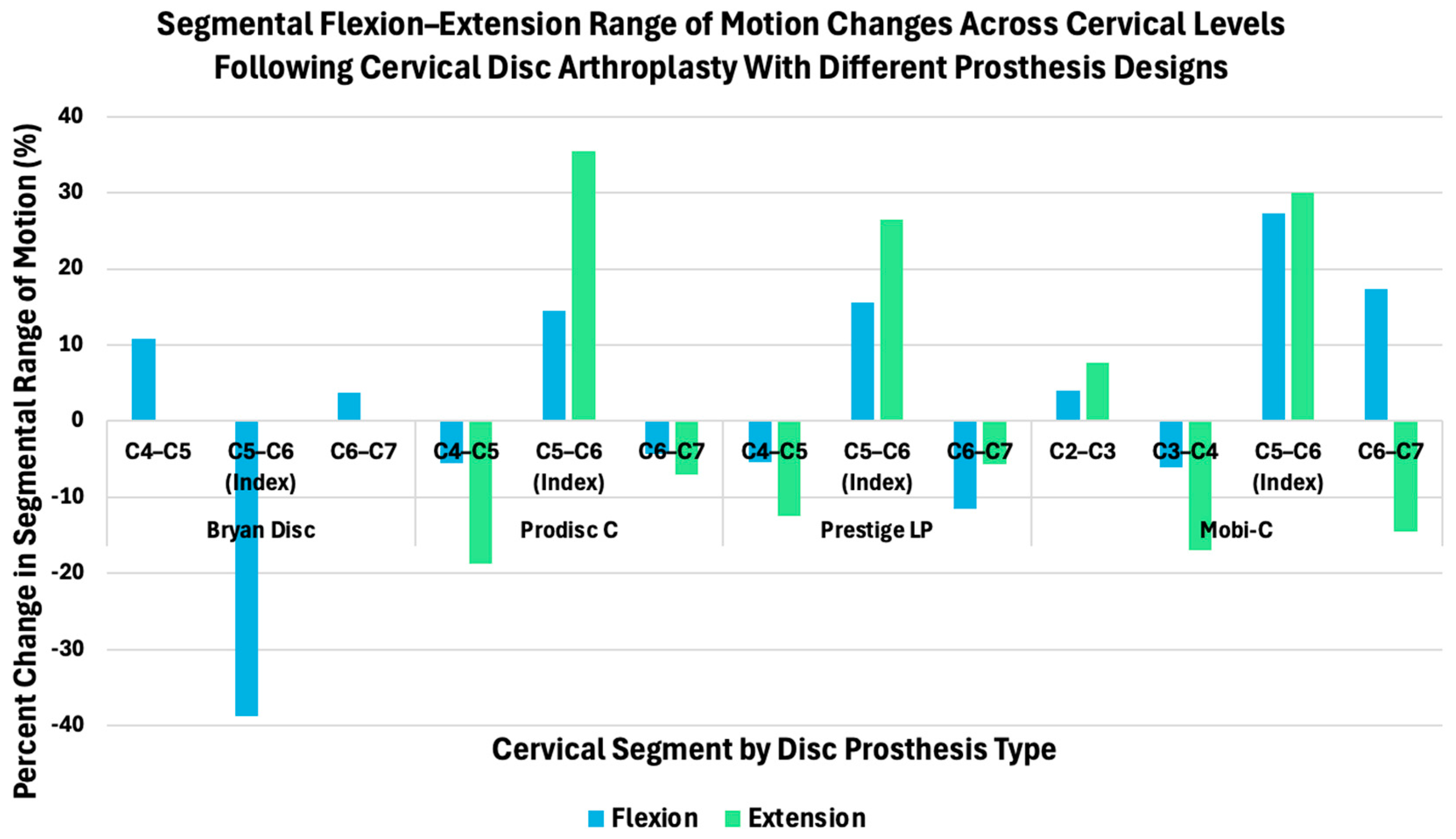
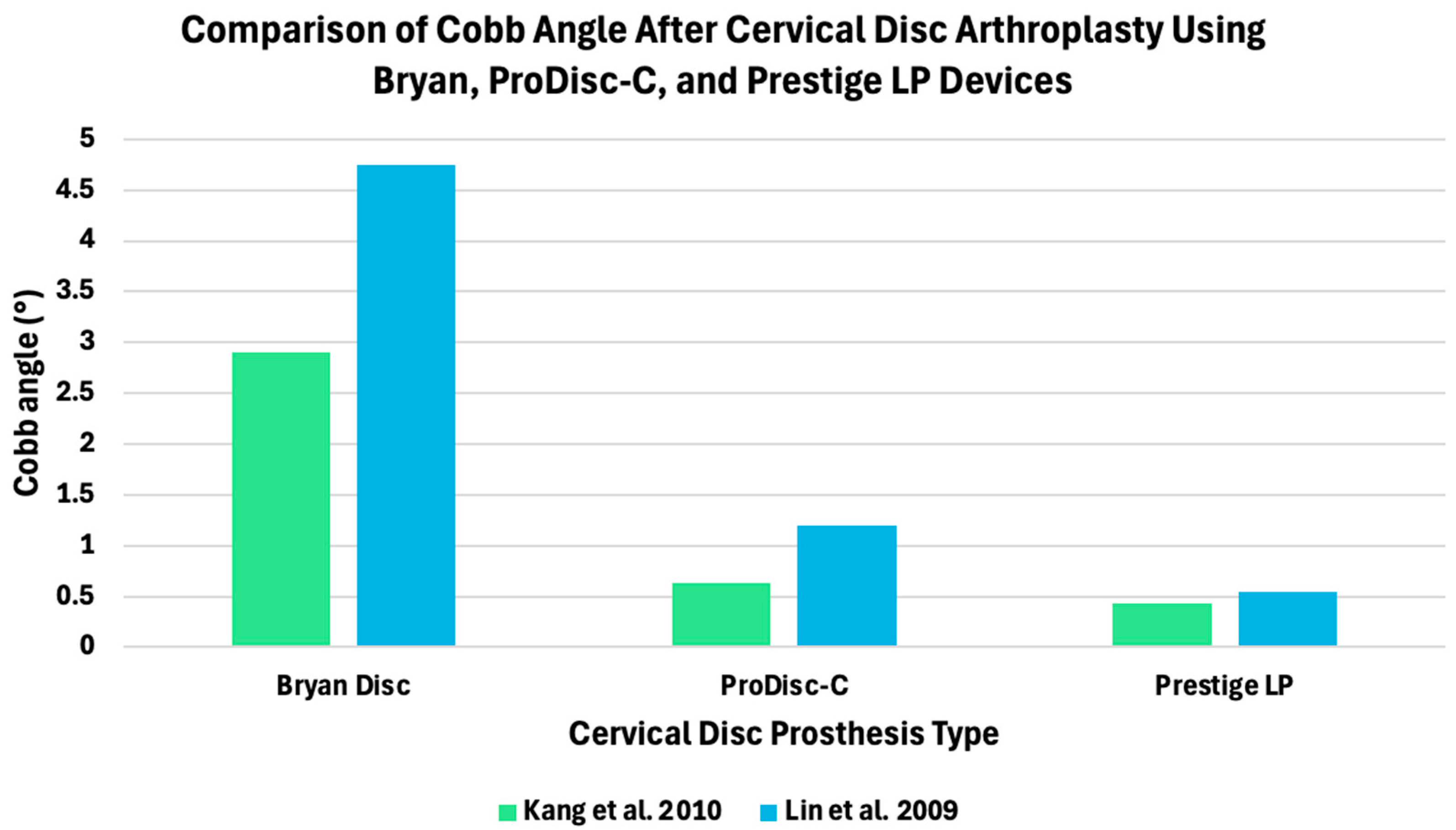
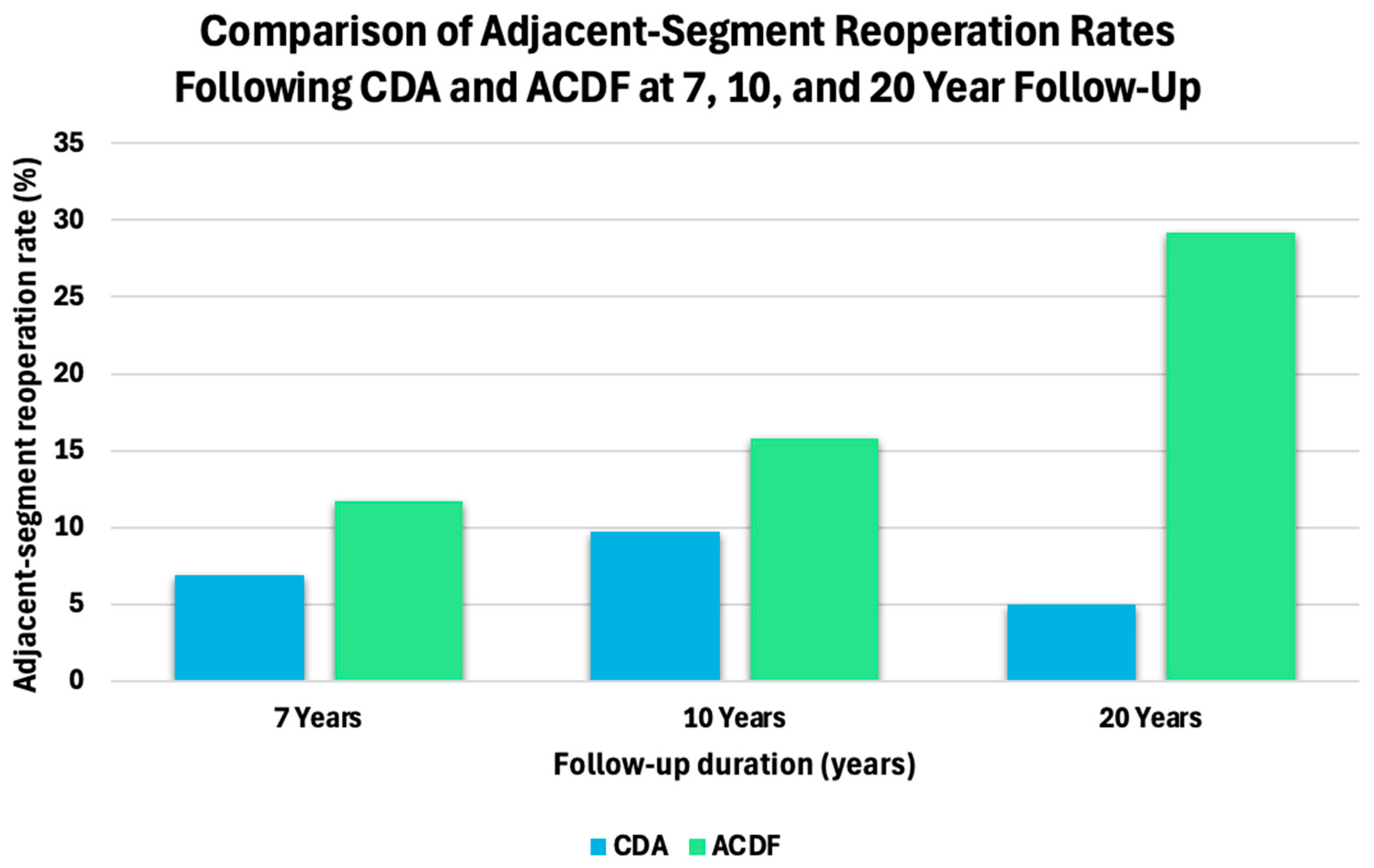

| Study | Metric | Arthroplasty/Motion-Preserving Technique | Fusion/Rigid Fixation Technique |
|---|---|---|---|
| Abudouaini et al., 2023 [30] | Index Level Flexion ROM | Maintained (near intact) | Decreased |
| Index Level Extension ROM | Maintained (near intact) | Decreased | |
| Index Level Lateral Bending ROMN | Maintained (near intact) | Decreased | |
| Index Level Axial Rotation ROM | Maintained (near intact) | Decreased | |
| Superior Adjacent Spinal. Level Flexion ROM | Maintained (no significant change in ROM) | Maintained (no significant change) | |
| Inferior Adjacent Spinal Level Flexion ROM | Maintained (no significant change in ROM) | Maintained (no significant change) | |
| Superior Adjacent Facet Joint Pressure | Slightly increased | Increased | |
| Inferior Adjacent Facet Joint Pressure | Slightly increased | Increased | |
| Superior Adjacent Intradiscal Pressure | Slightly increased | Increased | |
| Inferior Adjacent Intradiscal Pressure | Slightly increased | Increased | |
| Choi et al., 2021 [28] | Index Level Flexion ROM | Increased | Decreased |
| Index Level Extension ROM | Increased | Decreased | |
| Index Level Facet Forces | Increased | Decreased | |
| Superior Adjacent Spinal Level Flexion ROM | Maintained or Slightly Decreased (Implant-dependent) | Increased | |
| Inferior Adjacent Spinal Level Flexion ROM | Maintained or Slightly Decreased (Implant-dependent) | Increased | |
| Superior Adjacent Spinal Level Extension ROM | Maintained or Slightly Decreased (Implant-dependent) | Increased | |
| Inferior Adjacent Spinal Level Extension ROM | Maintained or Slightly Decreased (Implant-dependent) | Increased | |
| Superior Adjacent Facet Forces | Variable (Implant-dependent) | Increased | |
| Inferior Adjacent Facet Forces | Variable (Implant-dependent) | Increased | |
| Superior Adjacent Intradiscal Pressure | Increased or Decreased (Implant-Dependent) | Increased | |
| Inferior Adjacent Intradiscal Pressure | Increased or Decreased (Implant-Dependent) | Increased | |
| Gandhi et al., 2015 [7] | Index Level Flexion ROM | Increased | Decreased |
| Index Level Extension ROM | Increased | Decreased | |
| Index Level Lateral Bending ROM | Increased | Decreased | |
| Index Level Axial Rotation ROM | Increased | Decreased | |
| Superior Adjacent Spinal Level Flexion ROM | Maintained (near intact) | Increased | |
| Inferior Adjacent Spinal Level Flexion ROM | Maintained (near intact) | Increased | |
| Superior Adjacent Spinal Level Extension ROM | Maintained (near intact) | Increased | |
| Inferior Adjacent Spinal Level Extension ROM | Maintained (near intact) | Increased | |
| Superior Adjacent Spinal Level Lateral Bending ROM | Maintained (near intact) | Increased | |
| Inferior Adjacent Spinal Level Lateral Bending ROM | Maintained (near intact) | Increased | |
| Superior Adjacent Spinal Level Axial Rotation ROM | Maintained (near intact) | Increased | |
| Inferior Adjacent Spinal Level Axial Rotation ROM | Maintained (near intact) | Increased | |
| Gandhi et al., 2019 [31] | Index Level Flexion ROM | Increased | Decreased |
| Index Level Extension ROM | Increased | Decreased | |
| Index Level Lateral Bending ROM | Increased | Decreased | |
| Index Level Axial Rotation ROM | Increased | Decreased | |
| Superior Adjacent Spinal Level ROM | Maintained or Decreased | Increased | |
| Inferior Adjacent Spinal Level ROM | Maintained or Decreased | Increased | |
| Global Motion Redistribution | Concentrated at Arthroplasty Level | Shifted to Adjacent Levels |
| Factors Being Compared | Bryan Disc | Prestige LP Disc | ProDisc-C | Mobi-C Disc |
|---|---|---|---|---|
| Design Characteristics |
|
|
|
|
| Motion Mechanism | Elastic deformation of viscoelastic core and surrounding sheath | Controlled rotation through ball-in-trough metal articulation | Rotation through fixed ball-in-socket articulation | Controlled rotation through translation of mobile core |
| Pros |
|
|
|
|
| Cons |
|
|
|
|
| Trade-offs and considerations | Lower stiffness improves physiological motion and load sharing, but reduces segmental stability | Higher stiffness improves control and stability, but alters physiological load sharing | Higher stiffness improves control and stability, but alters physiological load sharing | Intermediate stiffness results in intermediate stability and load sharing compared to fully rigid and low-stiffness designs |
| Study | Metric | Arthroplasty | Fusion |
|---|---|---|---|
| Dahl et al., 2011 [14] | Implant Material Dynamic Stiffness | Decreased (PU < PE, Ti) | Increased |
| Implant Material Energy Absorption | Increased | Decreased | |
| Implant Material Viscous Damping | Increased | Decreased | |
| Axial Shock Absorption | Near intact (PU-based) | Decreased | |
| Load Transmission to Endplates | Reduced | Increased | |
| Subsidence Risk (Mechanistic) | Reduced | Increased |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Merem, I.; Vasquez, R.; Wise, J.; Beaulieu, E.; Patel, S.; Lin, M.; Pires, G.; Vrionis, F.D. A Review of Motion-Preserving Cervical Spinal Implants and Fusion Constructs. Bioengineering 2026, 13, 228. https://doi.org/10.3390/bioengineering13020228
Merem I, Vasquez R, Wise J, Beaulieu E, Patel S, Lin M, Pires G, Vrionis FD. A Review of Motion-Preserving Cervical Spinal Implants and Fusion Constructs. Bioengineering. 2026; 13(2):228. https://doi.org/10.3390/bioengineering13020228
Chicago/Turabian StyleMerem, Isabella, Rodrigo Vasquez, Jaden Wise, Elizabeth Beaulieu, Samip Patel, Maohua Lin, Gui Pires, and Frank D. Vrionis. 2026. "A Review of Motion-Preserving Cervical Spinal Implants and Fusion Constructs" Bioengineering 13, no. 2: 228. https://doi.org/10.3390/bioengineering13020228
APA StyleMerem, I., Vasquez, R., Wise, J., Beaulieu, E., Patel, S., Lin, M., Pires, G., & Vrionis, F. D. (2026). A Review of Motion-Preserving Cervical Spinal Implants and Fusion Constructs. Bioengineering, 13(2), 228. https://doi.org/10.3390/bioengineering13020228







