The Development and Biomechanical Analysis of an Allograft Interference Screw for Anterior Cruciate Ligament Reconstruction
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design of an Allograft Interference Screw for ACL Reconstruction
2.1.1. Design of the Screw Drive
2.1.2. Design of the Screw Thread
2.1.3. Design of the Screw Shape and Screw Dimensions
2.2. Biomechanical Analysis Using a Bovine Model
2.2.1. Graft Preparation
2.2.2. Graft Fixation
2.2.3. Measurement of the Ultimate Failure Load of the Graft Fixation
2.2.4. Measurement of the Ultimate Failure Torque
2.2.5. Statistical Analysis
3. Results
3.1. Results of the FEA
3.2. Results of the Biomechanical Analyses
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ACL | Anterior Cruciate Ligament |
| MRI | Magnetic Resonance Imaging |
| FEA | Finite Element Analysis |
| CAD | Computer Aided Design |
| BMD | Bone Mineral Density |
| PLLA | Polylactide |
| PU | Polyurethane |
Appendix A
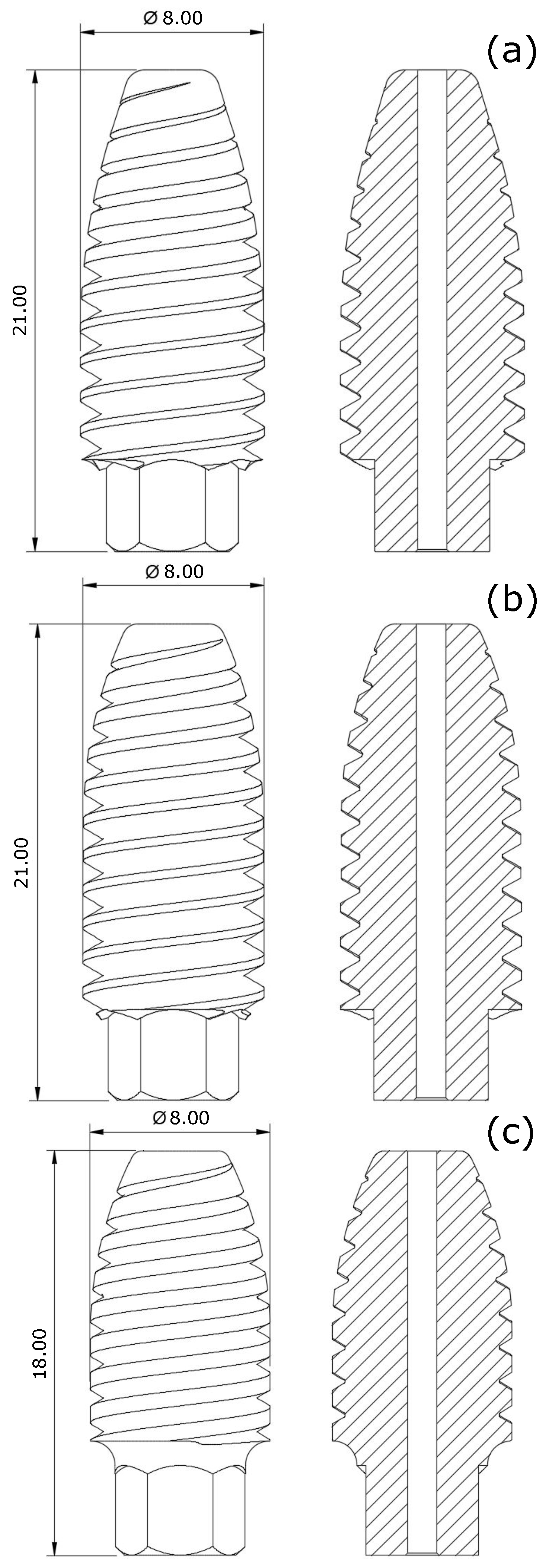
References
- Gerami, M.; Haghi, F.; Pelarak, F.; Mousavibaygei, S. Anterior cruciate ligament (ACL) injuries: A review on the newest reconstruction techniques. J. Fam. Med. Prim. Care 2022, 11, 852–856. [Google Scholar] [CrossRef]
- Rezende, F.C.; Moraes, V.Y.; Franciozi, C.E.; Debieux, P.; Luzo, M.V.; Belloti, J.C. One-incision versus two-incision techniques for arthroscopically assisted anterior cruciate ligament reconstruction in adults. Cochrane Database Syst. Rev. 2017, 12, CD010875. [Google Scholar] [CrossRef] [PubMed]
- Marieswaran, M.; Jain, I.; Garg, B.; Sharma, V.; Kalyanasundaram, D. A Review on Biomechanics of Anterior Cruciate Ligament and Materials for Reconstruction. Appl. Bionics Biomech. 2018, 2018, 4657824. [Google Scholar] [CrossRef] [PubMed]
- Sanders, T.L.; Kremers, H.M.; Bryan, A.J.; Larson, D.R.; Dahm, D.L.; Levy, B.A.; Stuart, M.J.; Krych, A.J. Incidence of Anterior Cruciate Ligament Tears and Reconstruction. Am. J. Sport. Med. 2016, 44, 1502–1507. [Google Scholar] [CrossRef] [PubMed]
- Mall, N.A.; Chalmers, P.N.; Moric, M.; Tanaka, M.J.; Cole, B.J.; Bach, B.R.; Paletta, G.A. Incidence and Trends of Anterior Cruciate Ligament Reconstruction in the United States. Am. J. Sport. Med. 2014, 42, 2363–2370. [Google Scholar] [CrossRef]
- Lam, M.H.; Fong, D.T.; Yung, P.S.; Ho, E.P.; Chan, W.Y.; Chan, K.M. Knee stability assessment on anterior cruciate ligament injury: Clinical and biomechanical approaches. BMC Sport. Sci. Med. Rehabil. 2009, 1, 20. [Google Scholar] [CrossRef]
- Chhabra, A.; Starman, J.S.; Ferretti, M.; Vidal, A.F.; Zantop, T.; Fu, F.H. Anatomic, Radiographic, Biomechanical, and Kinematic Evaluation of the Anterior Cruciate Ligament and Its Two Functional Bundles. J. Bone Jt. Surg. 2006, 88, 2–10. [Google Scholar] [CrossRef]
- Lohmander, L.S.; Englund, P.M.; Dahl, L.L.; Roos, E.M. The Long-term Consequence of Anterior Cruciate Ligament and Meniscus Injuries. Am. J. Sport. Med. 2007, 35, 1756–1769. [Google Scholar] [CrossRef]
- Lansdown, D.A.; Xiao, W.; Zhang, A.L.; Allen, C.R.; Feeley, B.T.; Li, X.; Majumdar, S.; Ma, C.B. Quantitative imaging of anterior cruciate ligament (ACL) graft demonstrates longitudinal compositional changes and relationships with clinical outcomes at 2 years after ACL reconstruction. J. Orthop. Res. 2020, 38, 1289–1295. [Google Scholar] [CrossRef]
- Buckthorpe, M. Optimising the Late-Stage Rehabilitation and Return-to-Sport Training and Testing Process After ACL Reconstruction. Sport. Med. 2019, 49, 1043–1058. [Google Scholar] [CrossRef]
- Filbay, S.R.; Ackerman, I.N.; Russell, T.G.; Crossley, K.M. Return to sport matters—longer-term quality of life after ACL reconstruction in people with knee difficulties. Scand. J. Med. Sci. Sport. 2017, 27, 514–524. [Google Scholar] [CrossRef] [PubMed]
- Gokeler, A.; Dingenen, B.; Hewett, T.E. Rehabilitation and Return to Sport Testing After Anterior Cruciate Ligament Reconstruction: Where Are We in 2022? Arthrosc. Sport. Med. Rehabil. 2022, 4, e77–e82. [Google Scholar] [CrossRef]
- Zeng, C.; Lei, G.; Gao, S.; Luo, W. Methods and devices for graft fixation in anterior cruciate ligament reconstruction. Cochrane Database Syst. Rev. 2013, 9, CD010730. [Google Scholar] [CrossRef]
- Tibor, L.; Chan, P.H.; Funahashi, T.T.; Wyatt, R.; Maletis, G.B.; Inacio, M.C.S. Surgical Technique Trends in Primary ACL Reconstruction from 2007 to 2014. JBJS 2016, 98, 1079. [Google Scholar] [CrossRef] [PubMed]
- Paschos, N.K.; Howell, S.M. Anterior cruciate ligament reconstruction: Principles of treatment. EFORT Open Rev. 2016, 1, 398–408. [Google Scholar] [CrossRef] [PubMed]
- Zainal Abidin, N.A.; Abdul Wahab, A.H.; Abdul Rahim, R.A.; Abdul Kadir, M.R.; Ramlee, M.H. Biomechanical analysis of three different types of fixators for anterior cruciate ligament reconstruction via finite element method: A patient-specific study. Med. Biol. Eng. Comput. 2021, 59, 1945–1960. [Google Scholar] [CrossRef]
- Zainal Abidin, N.A.; Ramlee, M.H.; Ab Rashid, A.M.; Ng, B.W.; Gan, H.S.; Abdul Kadir, M.R. Biomechanical effects of cross-pin’s diameter in reconstruction of anterior cruciate ligament—A specific case study via finite element analysis. Injury 2022, 53, 2424–2436. [Google Scholar] [CrossRef]
- Abidin, N.A.Z.; Kadir, M.R.A.; Ramlee, M.H. Biomechanical effects of different lengths of cross-pins in anterior cruciate ligament reconstruction: A finite element analysis. J. Mech. Med. Biol. 2020, 20, 2050047. [Google Scholar] [CrossRef]
- Athwal, K.K.; Lord, B.R.; Milner, P.E.; Gutteridge, A.; Williams, A.; Amis, A.A. Redesigning Metal Interference Screws Can Improve Ease of Insertion While Maintaining Fixation of Soft-Tissue Anterior Cruciate Ligament Reconstruction Grafts. Arthrosc. Sport. Med. Rehabil. 2020, 2, e137–e144. [Google Scholar] [CrossRef]
- Siroros, N.; Merfort, R.; Liu, Y.; Praster, M.; Migliorini, F.; Maffulli, N.; Michalik, R.; Hildebrand, F.; Eschweiler, J. Mechanical properties of a bioabsorbable magnesium interference screw for anterior cruciate ligament reconstruction in various testing bone materials. Sci. Rep. 2023, 13, 12342. [Google Scholar] [CrossRef]
- Schumacher, T.C.; Tushtev, K.; Wagner, U.; Becker, C.; große Holthaus, M.; Hein, S.B.; Haack, J.; Heiss, C.; Engelhardt, M.; El Khassawna, T.; et al. A novel, hydroxyapatite-based screw-like device for anterior cruciate ligament (ACL) reconstructions. Knee 2017, 24, 933–939. [Google Scholar] [CrossRef] [PubMed]
- Luo, Y.; Zhang, C.; Wang, J.; Liu, F.; Chau, K.W.; Qin, L.; Wang, J. Clinical translation and challenges of biodegradable magnesium-based interference screws in ACL reconstruction. Bioact. Mater. 2021, 6, 3231–3243. [Google Scholar] [CrossRef] [PubMed]
- Xu, B.; Yin, Y.; Zhu, Y.; Yin, Y.; Fu, W. Comparison of Bioabsorbable and Metallic Interference Screws for Graft Fixation During ACL Reconstruction: A Meta-analysis of Randomized Controlled Trials. Orthop. J. Sport. Med. 2021, 9, 23259671211021577. [Google Scholar] [CrossRef]
- Emond, C.E.; Woelber, E.B.; Kurd, S.K.; Ciccotti, M.G.; Cohen, S.B. A Comparison of the Results of Anterior Cruciate Ligament Reconstruction Using Bioabsorbable Versus Metal Interference Screws. J. Bone Jt. Surg.-Am. Vol. 2011, 93, 572–580. [Google Scholar] [CrossRef]
- Watson, J.N.; McQueen, P.; Kim, W.; Hutchinson, M.R. Bioabsorbable interference screw failure in anterior cruciate ligament reconstruction: A case series and review of the literature. Knee 2015, 22, 256–261. [Google Scholar] [CrossRef] [PubMed]
- Pastl, K.; Schimetta, W. The application of an allogeneic bone screw for osteosynthesis in hand and foot surgery: A case series. Arch. Orthop. Trauma Surg. 2021, 142, 2567–2575. [Google Scholar] [CrossRef]
- Pastl, K.; Pastl, E.; Flöry, D.; Borchert, G.H.; Chraim, M. Arthrodesis and Defect Bridging of the Upper Ankle Joint with Allograft Bone Chips and Allograft Cortical Bone Screws (Shark Screw®) after Removal of the Salto-Prosthesis in a Multimorbidity Patient: A Case Report. Life 2022, 12, 1028. [Google Scholar] [CrossRef]
- Brcic, I.; Pastl, K.; Plank, H.; Igrec, J.; Schanda, J.E.; Pastl, E.; Werner, M. Incorporation of an Allogenic Cortical Bone Graft Following Arthrodesis of the First Metatarsophalangeal Joint in a Patient with Hallux Rigidus. Life 2021, 11, 473. [Google Scholar] [CrossRef]
- Amann, P.; Pastl, K.; Neunteufel, E.; Bock, P. Clinical and Radiologic Results of a Human Bone Graft Screw in Tarsometatarsal II/+III Arthrodesis. Foot Ankle Int. 2022, 43, 913–922. [Google Scholar] [CrossRef]
- Lifka, S.; Baumgartner, W. A Novel Screw Drive for Allogenic Headless Position Screws for Use in Osteosynthesis—A Finite-Element Analysis. Bioengineering 2021, 8, 136. [Google Scholar] [CrossRef]
- Bi, Z. Chapter 12—Validation and Verification. In Finite Element Analysis Applications: A Systematic and Practical Approach; Academic Press: San Diego, CA, USA, 2018; pp. 455–494. [Google Scholar] [CrossRef]
- Krone, R.; Schuster, P. An Investigation on the Importance of Material Anisotropy in Finite-Element Modeling of the Human Femur. In SAE Technical Paper; SAE International: Warrendale PA, USA, 2006. [Google Scholar] [CrossRef]
- Park, Y.S.; Kwon, H.B. Three-dimensional finite element analysis of implant-supported crown in fibula bone model. J. Adv. Prosthodont. 2013, 5, 326–332. [Google Scholar] [CrossRef] [PubMed]
- Du, W.; Zhang, J.; Hu, J. A Method to Determine Cortical Bone Thickness of Human Femur and Tibia Using Clinical CT Scans. In Proceedings of the 2018 IRCOBI Conference Proceedings, Athens, Greece, 12–14 September 2018; Number IRC-18-65. pp. 388–398. [Google Scholar]
- Sadat-Ali, M.; Elshaboury, E.; Al-Omran, A.; Azam, M.Q.; Syed, A.; Gullenpet, A. Tibial cortical thickness: A dependable tool for assessing osteoporosis in the absence of dual energy X-ray absorptiopmetry. Int. J. Appl. Basic Med. Res. 2015, 5, 21–24. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.; Williams, J.; Thake, A.; Lang, Y.; Brown, J. Optimal screw diameter for interference fixation in a bone tunnel: A porcine model. Knee Surg. Sport. Traumatol. Arthrosc. 2004, 12, 486–489. [Google Scholar] [CrossRef] [PubMed]
- Mlynarek, R.A.; Bedi, A.; Brown, C.H. Intratunnel Anterior Cruciate Ligament Graft Fixation. In The Anterior Cruciate Ligament; Elsevier: Amsterdam, The Netherlands, 2018; pp. 241–244.e1. [Google Scholar] [CrossRef]
- Ezechieli, M.; Ettinger, M.; König, C.; Weizbauer, A.; Helmecke, P.; Schavan, R.; Lucas, A.; Windhagen, H.; Becher, C. Biomechanical characteristics of bioabsorbable magnesium-based (MgYREZr-alloy) interference screws with different threads. Knee Surg. Sport. Traumatol. Arthrosc. 2016, 24, 3976–3981. [Google Scholar] [CrossRef]
- Mayr, R.; Heinrichs, C.H.; Eichinger, M.; Coppola, C.; Schmoelz, W.; Attal, R. Biomechanical Comparison of 2 Anterior Cruciate Ligament Graft Preparation Techniques for Tibial Fixation: Adjustable-Length Loop Cortical Button or Interference Screw. Am. J. Sport. Med. 2015, 43, 1380–1385. [Google Scholar] [CrossRef]
- Benca, E.; van Knegsel, K.P.; Zderic, I.; Caspar, J.; Strassl, A.; Hirtler, L.; Fuchssteiner, C.; Gueorguiev, B.; Windhager, R.; Widhalm, H.; et al. Biomechanical evaluation of an allograft fixation system for ACL reconstruction. Front. Bioeng. Biotechnol. 2022, 10, 1000624. [Google Scholar] [CrossRef]
- Costi, J.J.; Kelly, A.J.; Hearn, T.C.; Martin, D.K. Comparison of Torsional Strengths of Bioabsorbable Screws for Anterior Cruciate Ligament Reconstruction. Am. J. Sport. Med. 2001, 29, 575–580. [Google Scholar] [CrossRef]
- Herrera, A.; Martínez, F.; Iglesias, D.; Cegoñino, J.; Ibarz, E.; Gracia, L. Fixation strength of biocomposite wedge interference screw in ACL reconstruction: Effect of screw length and tunnel/screw ratio. A controlled laboratory study. BMC Musculoskelet. Disord. 2010, 11, 139. [Google Scholar] [CrossRef]
- Efe, T.; Bauer, J.; Herdrich, S.; Gotzen, L.; El-Zayat, B.F.; Schmitt, J.; Schofer, M.D. Comparison between bovine bone and titanium interference screws for implant fixation in ACL reconstruction: A biomechanical study. Arch. Orthop. Trauma Surg. 2010, 130, 993–999. [Google Scholar] [CrossRef]
- Weiss, F.P.; Possoli, F.A.d.A.; Costa, I.Z.; Borges, P.C.; Stieven, E.; Kubrusly, L.F. Fixation of the Anterior Ligament Graft at the Tibial Pole: Biomechanical Analysis of Three Methods. Rev. Bras. Ortop. 2019, 54, 697–702. [Google Scholar] [CrossRef]
- Suryavanshi, A.; Khanna, K.; Sindhu, K.R.; Bellare, J.; Srivastava, R. Development of bone screw using novel biodegradable composite orthopedic biomaterial: From material design to in vitro biomechanical and in vivo biocompatibility evaluation. Biomed. Mater. 2019, 14, 045020. [Google Scholar] [CrossRef] [PubMed]
- Dong, W.; Huang, X.; Sun, Y.; Zhao, S.; Yin, J.; Chen, L. Mechanical characteristics and in vitro degradation kinetics analysis of polylactic glycolic acid/β-tricalcium phosphate (PLGA/β-TCP) biocomposite interference screw. Polym. Degrad. Stab. 2021, 186, 109421. [Google Scholar] [CrossRef]
- Aga, C.; Rasmussen, M.T.; Smith, S.D.; Jansson, K.S.; LaPrade, R.F.; Engebretsen, L.; Wijdicks, C.A. Biomechanical Comparison of Interference Screws and Combination Screw and Sheath Devices for Soft Tissue Anterior Cruciate Ligament Reconstruction on the Tibial Side. Am. J. Sport. Med. 2013, 41, 841–848. [Google Scholar] [CrossRef] [PubMed]
- Brand, J.C.; Pienkowski, D.; Steenlage, E.; Hamilton, D.; Johnson, D.L.; Caborn, D.N.M. Interference Screw Fixation Strength of a Quadrupled Hamstring Tendon Graft Is Directly Related to Bone Mineral Density and Insertion Torque. Am. J. Sport. Med. 2000, 28, 705–710. [Google Scholar] [CrossRef] [PubMed]
- Prado, M.; Martín-Castilla, B.; Espejo-Reina, A.; Serrano-Fernández, J.M.; Pérez-Blanca, A.; Ezquerro, F. Close-looped graft suturing improves mechanical properties of interference screw fixation in ACL reconstruction. Knee Surg. Sport. Traumatol. Arthrosc. 2013, 21, 476–484. [Google Scholar] [CrossRef]
- Wan, C.; Hao, Z.; Li, Z.; Lin, J. Finite element simulations of different hamstring tendon graft lengths and related fixations in anterior cruciate ligament reconstruction. Med. Biol. Eng. Comput. 2017, 55, 2097–2106. [Google Scholar] [CrossRef]
- Nyland, J.; Kocabey, Y.; Caborn, D.N. Insertion torque pullout strength relationship of soft tissue tendon graft tibia tunnel fixation with a bioabsorbable interference screw. Arthrosc. J. Arthrosc. Relat. Surg. 2004, 20, 379–384. [Google Scholar] [CrossRef]
- Yang, D.L.; Cheon, S.H.; Oh, C.W.; Kyung, H.S. A Comparison of the Fixation Strengths Provided by Different Intraosseous Tendon Lengths during Anterior Cruciate Ligament Reconstruction: A Biomechanical Study in a Porcine Tibial Model. Clin. Orthop. Surg. 2014, 6, 173. [Google Scholar] [CrossRef]
- Ariffin, A.; Chan, H.; Yusof, N.; Mohd, S.; Ramalingam, S.; Ng, W.; Mansor, A. Establishing Freeze Drying Process for Cortical and Cancellous Bone Allograft Cubes. J. Health Transl. Med. (JUMMEC) 2019, 22, 66–71. [Google Scholar] [CrossRef]
- Tecklenburg, K.; Burkart, P.; Hoser, C.; Rieger, M.; Fink, C. Prospective Evaluation of Patellar Tendon Graft Fixation in Anterior Cruciate Ligament Reconstruction Comparing Composite Bioabsorbable and Allograft Interference Screws. Arthrosc. J. Arthrosc. Relat. Surg. 2006, 22, 993–999. [Google Scholar] [CrossRef]
- Wilde, J.; Bedi, A.; Altchek, D.W. Revision Anterior Cruciate Ligament Reconstruction. Sport. Health Multidiscip. Approach 2013, 6, 504–518. [Google Scholar] [CrossRef] [PubMed]
- Persson, A.; Gifstad, T.; Lind, M.; Engebretsen, L.; Fjeldsgaard, K.; Drogset, J.O.; Forssblad, M.; Espehaug, B.; Kjellsen, A.B.; Fevang, J.M. Graft fixation influences revision risk after ACL reconstruction with hamstring tendon autografts. Acta Orthop. 2018, 89, 204–210. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.H.; Bae, K.C.; Kim, D.W.; Choi, B.C. Two-stage revision anterior cruciate ligament reconstruction. Knee Surg. Relat. Res. 2019, 31, 10. [Google Scholar] [CrossRef] [PubMed]
- Noyes, F.R.; Barber-Westin, S.D. Anterior Cruciate Ligament Revision Reconstruction. Am. J. Sport. Med. 2006, 34, 553–564. [Google Scholar] [CrossRef] [PubMed]





| Freeze-Dried Human Cortical Bone | Chromium Steel 1.4034 | |
|---|---|---|
| Density in g/cm3 | 1.022 | 7.7 |
| Young’s modulus in GPa | 5 | 215 |
| Poisson’s ratio | 0.36 | 0.3 |
| Yield strength in MPa | 108 | 650 |
| Sample Number | Graft Diameter in mm | Tunnel Diameter in mm | Max. Insertion Torque in N mm | Ultimate Failure Load Graft Fixation in N | Ultimate Failure Torque in N mm |
|---|---|---|---|---|---|
| 1 | 7 | 8 | 1600 | 203 | 2500 |
| 2 | 9 | 9.5 | 1200 | 281 | 2600 |
| 3 | 7 | 8 | 1500 | 312 | 2800 |
| 4 | 9 | 9.5 | 1600 | 362 | - |
| 5 | 7 | 8 | 900 | 160 | - |
| 6 | 7.5 | 8 | 400 | 91 | - |
| 7 | 7 | 8.5 | 1200 | 199 | - |
| 8 | 9 | 9.5 | 700 | 212 | - |
| 9 | 7 | 8 | 1000 | 359 | - |
| 10 | 7 | 7.5 | 900 | 114 | - |
| 11 | 7.5 | 8 | 1100 | 240 | - |
| 12 | 9 | 9.5 | 1400 | 288 | - |
| Mean value 7 graft | 1075 | 209.75 | - | ||
| Standard deviation 7 graft | 377.02 | 92.24 | - | ||
| Min. value 7 graft | 400 | 91 | - | ||
| Max. value 7 graft | 1600 | 359 | - | ||
| Mean value 9 graft | 1225 | 285.75 | - | ||
| Standard deviation 9 graft | 386.22 | 61.32 | - | ||
| Min. value 9 graft | 700 | 212 | - | ||
| Max. value 9 graft | 1600 | 362 | - | ||
| Mean value overall | 1125 | 235.08 | 2633.33 | ||
| Standard deviation overall | 369.58 | 88.54 | 152.75 | ||
| Min. value overall | 400 | 91 | 2500 | ||
| Max. value overall | 1600 | 362 | 2800 | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lifka, S.; Rehberger, Y.; Pastl, K.; Rofner-Moretti, A.; Reichkendler, M.; Baumgartner, W. The Development and Biomechanical Analysis of an Allograft Interference Screw for Anterior Cruciate Ligament Reconstruction. Bioengineering 2023, 10, 1174. https://doi.org/10.3390/bioengineering10101174
Lifka S, Rehberger Y, Pastl K, Rofner-Moretti A, Reichkendler M, Baumgartner W. The Development and Biomechanical Analysis of an Allograft Interference Screw for Anterior Cruciate Ligament Reconstruction. Bioengineering. 2023; 10(10):1174. https://doi.org/10.3390/bioengineering10101174
Chicago/Turabian StyleLifka, Sebastian, Yannik Rehberger, Klaus Pastl, Alexander Rofner-Moretti, Markus Reichkendler, and Werner Baumgartner. 2023. "The Development and Biomechanical Analysis of an Allograft Interference Screw for Anterior Cruciate Ligament Reconstruction" Bioengineering 10, no. 10: 1174. https://doi.org/10.3390/bioengineering10101174
APA StyleLifka, S., Rehberger, Y., Pastl, K., Rofner-Moretti, A., Reichkendler, M., & Baumgartner, W. (2023). The Development and Biomechanical Analysis of an Allograft Interference Screw for Anterior Cruciate Ligament Reconstruction. Bioengineering, 10(10), 1174. https://doi.org/10.3390/bioengineering10101174








