Farmers’ Exposure to Pesticides: Toxicity Types and Ways of Prevention
Abstract
:1. Introduction
2. Pesticide Toxicity and Risk (Hazard)
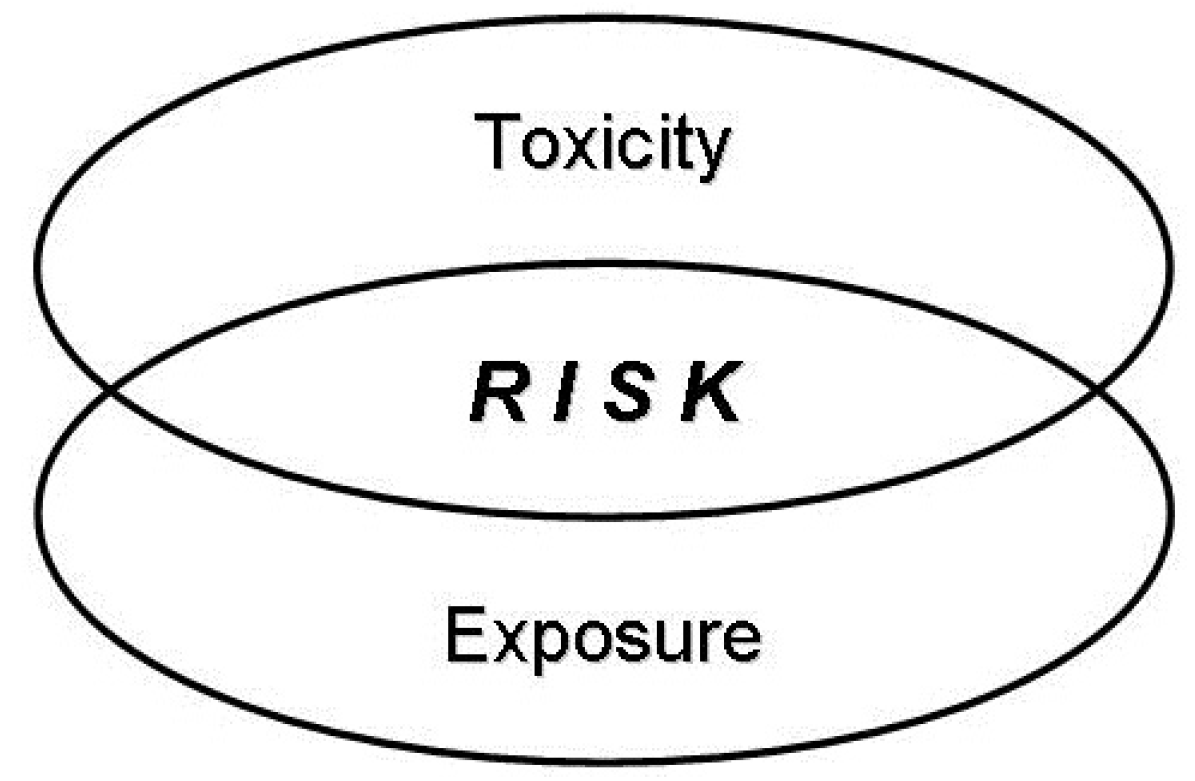
3. Classification of Toxicity by Type of Exposure
| Type | Definition |
|---|---|
| Acute toxicity | Occurring from a single incident of exposure (single short-term exposure). |
| Subchronic toxicity | Occurring from repeated incidents of exposure over several weeks or months (intermediate exposure, normally less than the lifetime of the exposed organism). |
| Chronic toxicity | Occurring from repeated incidents of exposure for many months or years (repeated long-term exposure, sometimes lasting for the entire life of the exposed organism). |
| Categories | Signal Word | Oral mg/kg | Dermal mg/kg | Inhalation mg/L |
|---|---|---|---|---|
| I—Highly toxic | POISON | 0 to 50 | 0 to 200 | 0 to 0.2 |
| II—Moderately toxic | WARNING | 50 to 500 | 200 to 2,000 | 0.2 to 2.0 |
| III—Slightly toxic | CAUTION | 500 to 5,000 | 2,000 to 20,000 | 2.0 to 20 |
| IV—Relatively non-toxic | CAUTION | 5,000+ | 20,000+ | 20+ |
4. Classification of Toxicity by Route of Entry
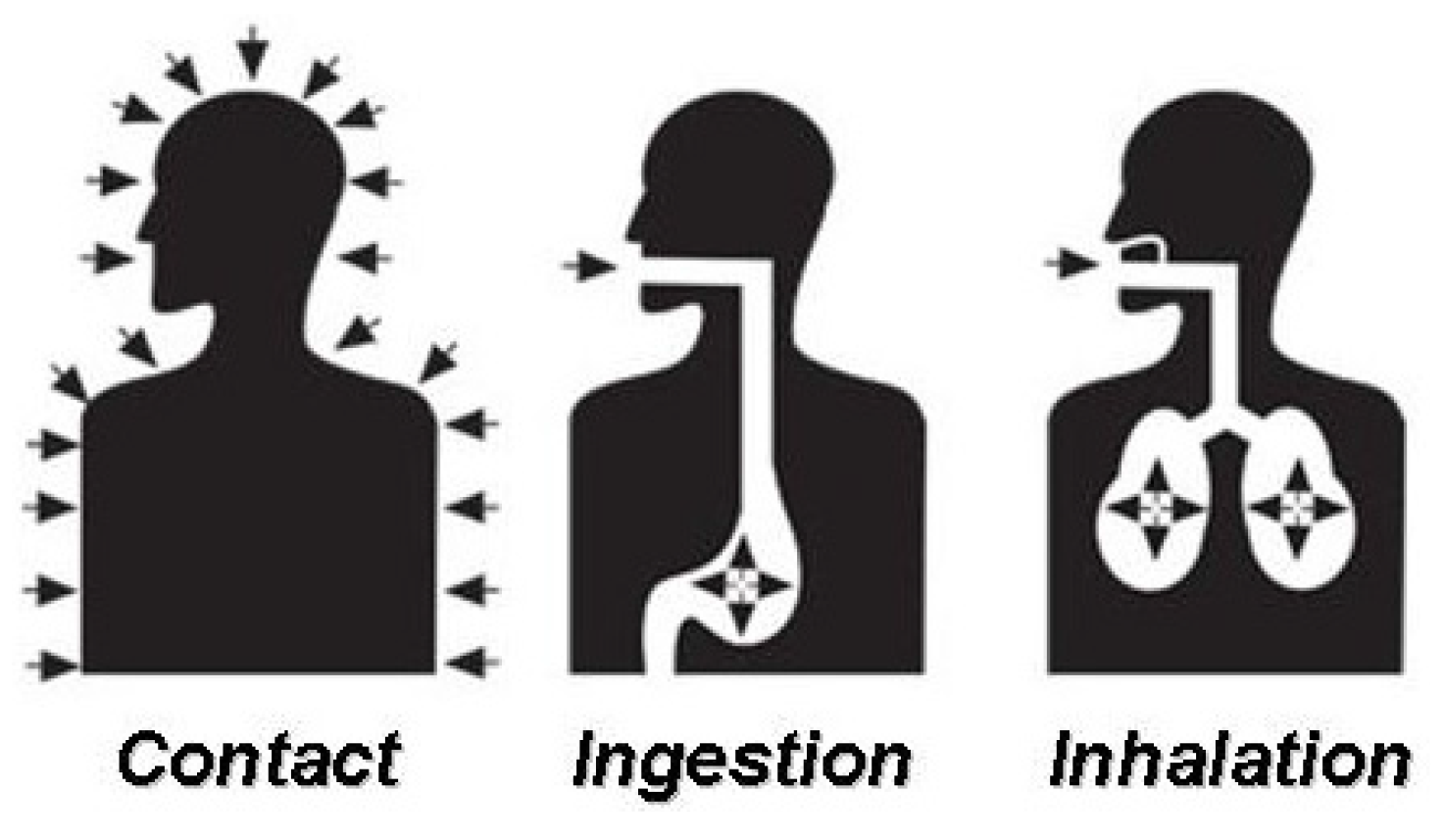
5. Pesticide-Related Work Tasks
6. Reducing Exposure to Pesticides
6.1. Alternative Cropping Systems Less Dependent on Pesticides
6.2. Use of Personal Protective Equipment (PPE)
Author Contributions
Conflicts of Interest
References
- Bao, L.-J.; Wei, Y.-L.; Yao, Y.; Ruan, Q.-Q.; Zeng, E.Y. Global trends of research on emerging contaminants in the environment and humans: A literature assimilation. Environ. Sci. Poll. Res. 2015, 22, 1635–1643. [Google Scholar] [CrossRef] [PubMed]
- Gavrilescu, M.; Demnerová, K.; Aamand, J.; Agathos, S.; Fava, F. Emerging pollutants in the environment: Present and future challenges in biomonitoring, ecological risks and bioremediation. New Biotechnol. 2015, 32, 147–156. [Google Scholar] [CrossRef] [PubMed]
- Colosio, C.; Alegakis, A.K.; Tsatsakis, A.M. Emerging health issues from chronic pesticide exposure: Innovative methodologies and effects on molecular cell and tissue level. Toxicology 2013, 307, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Moser, F.; Dondi, F. Environmental protection between chemical practice and applied ethics: A critical review. Toxicol. Environ. Chem. 2015, 6, 100–110. [Google Scholar] [CrossRef]
- Damalas, C.A. Understanding benefits and risks of pesticide use. Sci. Res. Essays 2009, 4, 945–949. [Google Scholar]
- Maroni, M.; Fanetti, A.C.; Metruccio, F. Risk assessment and management of occupational exposure to pesticides in agriculture. Med. Lav. 2006, 97, 430–437. [Google Scholar] [PubMed]
- Woodruff, T.J.; Kyle, A.D.; Bois, F.Y. Evaluating health risks from occupational exposure to pesticides and the regulatory response. Environ. Health Perspect. 1994, 102, 1088–1096. [Google Scholar] [CrossRef] [PubMed]
- Maroni, M.; Fait, A.; Colosio, C. Risk assessment and management of occupational exposure to pesticides. Toxicol. Lett. 1999, 107, 145–153. [Google Scholar] [CrossRef]
- Ye, M.; Beach, J.; Martin, J.W.; Senthilselvan, A. Occupational pesticide exposure and respiratory health. Int. J. Environ. Res. Public Health 2013, 10, 6442–6471. [Google Scholar] [CrossRef] [PubMed]
- Glass, C.R.; Machera, K. Evaluating the risks of occupational pesticide exposure. Hell. Plant Prot. J. 2009, 2, 1–9. [Google Scholar]
- Damalas, C.A.; Eleftherohorinos, I.G. Pesticide exposure, safety issues, and risk assessment indicators. Int. J. Environ. Res. Public Health 2011, 11, 1402–1408. [Google Scholar] [CrossRef] [PubMed]
- Calvert, G.M.; Karnik, J.; Mehler, L.; Beckman, J.; Morrissey, B.; Sievert, J.; Barrett, R.; Lackovic, M.; Mabee, L.; Schwartz, A.; Mitchell, Y.; Moraga-McHaley, S. Acute pesticide poisoning among agricultural workers in the United States, 1998–2005. Am. J. Ind. Med. 2008, 51, 883–898. [Google Scholar] [CrossRef] [PubMed]
- Robertson, A.; Tirado, C.; Lobstein, T.; Jermini, M.; Knai, C.; Jensen, J.H.; Ferro-Luzzi, A.; James, W.P.T. Food and Health in Europe: A New Basis for Action, European Series, No. 96; WHO Regional Publications: Geneva, Switzerland, 2004; p. 385. [Google Scholar]
- Ecobichon, D.J. Pesticide use in developing countries. Toxicology 2001, 160, 27–33. [Google Scholar] [CrossRef]
- Aktar, M.W.; Sengupta, D.; Chowdhury, A. Impact of pesticides use in agriculture: Their benefits and hazards. Interdisc. Toxicol. 2009, 2, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Hu, R.; Shi, G.; Jin, Y.; Robson, M.G.; Huang, X. Overuse or underuse? An observation of pesticide use in China. Sci. Total Environ. 2015, 538, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Ewence, A.; Brescia, S.; Johnson, I.; Rumsby, P.C. An approach to the identification and regulation of endocrine disrupting pesticides. Food Chem. Toxicol. 2015, 78, 214–220. [Google Scholar] [CrossRef] [PubMed]
- Andersen, H.R.; Cook, S.J.; Waldbillig, D. Effects of currently used pesticides in assays for estrogenicity, androgenicity, and aromatase activity in vitro. Toxicol. Appl. Pharmacol. 2002, 179, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Welshons, W.V.; Thayer, K.A.; Judy, B.M.; Taylor, J.A.; Curran, E.M.; vom Saal, F.S. Large effects from small exposures. I. Mechanisms for endocrine-disrupting chemicals with estrogenic activity. Environ. Health Perspect. 2003, 111, 994–1006. [Google Scholar] [CrossRef] [PubMed]
- Frank, P.; Ottoboni, M.A. The Dose Makes the Poison: A Plain-Language Guide to Toxicology, 3rd ed.; John Wiley and Sons Inc.: Hoboken, NJ, USA, 2011; p. 284. [Google Scholar]
- Sarwar, M. The dangers of pesticides associated with public health and preventing of the risks. Int. J. Bioinform. Biomed. Engineer. 2015, 1, 130–136. [Google Scholar]
- Klaassen, C.D. Casarett & Doull’s Toxicology: The Basic Science of Poisons, 8th ed.; McGraw-Hill Education: Columbus, OH, USA, 2013; p. 1454. [Google Scholar]
- Nesheim, O.N.; Fishel, F.M.; Mossler, M. Toxicity of Pesticides. PI-13; University of Florida (UF), Institute of Food and Agricultural Sciences (IFAS) Extension: Gainesville, FL, USA, 2014; p. 6. [Google Scholar]
- Rondeau, G.; Sánchez-Bayo, F.; Tennekes, H.A.; Decourtye, A.; Ramírez-Romero, R.; Desneux, N. Delayed and time-cumulative toxicity of imidacloprid in bees, ants and termites. Sci. Rep. 2014, 4. [Google Scholar] [CrossRef] [PubMed]
- Berthet, A.; Hopf, N.B.; Miles, A.; Spring, P.; Charrière, N.; Garrigou, A.; Baldi, I.; Vernez, D. Human skin in vitro permeation of bentazon and isoproturon formulations with or without protective clothing suit. Arch. Toxicol. 2014, 88, 77–88. [Google Scholar] [CrossRef] [PubMed]
- MacFarlane, E.; Carey, R.; Keegel, T.; El-Zaemay, S.; Fritschi, L. Dermal exposure associated with occupational end use of pesticides and the role of protective measures. Saf. Health Work 2013, 4, 136–141. [Google Scholar] [CrossRef] [PubMed]
- Baldi, I.; Lebailly, P.; Jean, S.; Rougetet, L.; Dulaurent, S.; Marquet, P. Pesticide contamination of workers in vineyards in France. J. Exp. Sci. Environ. Epidemiol. 2006, 16, 115–124. [Google Scholar] [CrossRef] [PubMed]
- Damalas, C.A. Pesticide drift: Seeking reliable environmental indicators of exposure assessment. In Environmental Indicators; Armon, R., Hänninen, O., Eds.; Springer: Dordrecht, Netherlands, 2015; pp. 251–261. [Google Scholar]
- Lebailly, P.; Bouchart, V.; Baldi, I.; Lecluse, Y.; Heutte, N.; Gislard, A.; Malas, J.-P. Exposure to pesticides in open-field farming in France. Ann. Occup. Hyg. 2009, 53, 69–81. [Google Scholar] [CrossRef] [PubMed]
- Alavanja, M.C.; Sprince, N.L.; Oliver, E.; Whitten, P.; Lynch, C.F.; Gillette, P.P.; Logsden-Sacket, N.; Zwerling, C. Nested case-control analysis of high pesticide exposure events from the Agricultural Health Study. Am. J. Ind. Med. 2001, 39, 557–563. [Google Scholar] [CrossRef] [PubMed]
- Coronado, G.D.; Thompson, B.; Strong, L.; Griffith, W.C.; Islas, I. Agricultural task and exposure to organophosphate pesticides among farmworkers. Environ. Health Perspect. 2004, 112, 142–147. [Google Scholar] [CrossRef]
- Strong, L.L.; Thompson, B.; Coronado, G.D.; Griffith, W.C.; Vigoren, E.M.; Islas, I. Health symptoms and exposure to organophosphate pesticides in farmworkers. Am. J. Ind. Med. 2004, 46, 599–606. [Google Scholar] [CrossRef] [PubMed]
- Ward, M.H.; Prince, J.R.; Stewart, P.A.; Zahm, S.H. Determining the probability of pesticide exposures among migrant farmworkers: Results from a feasibility study. Am. J. Ind. Med. 2001, 40, 538–553. [Google Scholar] [CrossRef] [PubMed]
- Burns, C.; Mahlburg, W.; Dutra, J.P.J. Pesticide exposure among farm workers. Environ. Res. 2007, 105, 285–288. [Google Scholar] [CrossRef] [PubMed]
- Cunha, J.P.; Chueca, P.; Garcerá, C.; Moltó, E. Risk assessment of pesticide spray drift from citrus applications with air-blast sprayers in Spain. Crop Prot. 2012, 116, 116–123. [Google Scholar] [CrossRef]
- Struik, P.C.; Kropff, M.J. An agricultural vision. In Pesticides: Problems, Improvements, Alternatives; den Hond, F., Groenewegen, P., van Straalen, N., Eds.; Blackwell Science: Oxford, UK, 2003; pp. 16–30. [Google Scholar]
- Ratnadass, A.; Fernandes, P.; Avelino, J.; Habib, R. Plant species diversity for sustainable management of crop pests and diseases in agroecosystems: A review. Agron. Sustain. Dev. 2012, 32, 273–303. [Google Scholar] [CrossRef] [Green Version]
- Coffman, C.W.; Stone, J.; Slocum, A.C.; Landers, A.J.; Schwab, C.V.; Olsen, L.G.; Lee, S. Use of engineering controls and personal protective equipment by certified pesticide applicators. J. Agric. Saf. Health 2009, 15, 311–326. [Google Scholar] [CrossRef] [PubMed]
- Aprea, C.; Terenzoni, B.; De Angelis, V.; Sciarra, G.; Lunghini, L.; Borzacchi, G.; Vasconi, D.; Fani, D.; Quercia, A.; Salvan, A.; Settimi, L. Evaluation of skin and respiratory doses and urinary excretion of alkylphosphates in workers exposed to dimethoate during treatment of olive trees. Arch. Environ. Contam. Toxicol. 2004, 48, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Vitali, M.; Protano, C.; Del Monte, A.; Ensabella, F.; Guidotti, M. Operative modalities and exposure to pesticides during open field treatments among a group of agricultural subcontractors. Arch. Environ. Contam. Toxicol. 2009, 57, 193–202. [Google Scholar] [CrossRef] [PubMed]
- Fenske, R.A.; Birnbaum, S.G.; Methner, M.M.; Lu, C.; Nigg, H.N. Fluorescent tracer evaluation of chemical protective clothing during pesticide applications in central Florida citrus groves. J. Agric. Saf. Health 2002, 8, 319–331. [Google Scholar] [CrossRef] [PubMed]
- Keifer, M.C. Effectiveness of interventions in reducing pesticide overexposure and poisonings. Am. J. Prev. Med. 2000, 18, 80–89. [Google Scholar] [CrossRef]
- Driver, J.; Ross, J.; Mihlan, G.; Lunchick, C.; Landenberger, B. Derivation of single layer clothing penetration factors from the pesticide handlers exposure database. Regul. Toxicol. Pharmacol. 2007, 49, 125–137. [Google Scholar] [CrossRef] [PubMed]
- Nigg, H.N.; Stamper, J.H.; Easter, E.; DeJonge, J.O. Protection afforded greenhouse pesticide applicators by coveralls: A field test. Arch. Environ. Contam. Toxicol. 1993, 25, 529–533. [Google Scholar] [CrossRef] [PubMed]
- Stewart, P.A.; Fears, T.; Kross, B.; Ogilvie, L.; Blair, A. Exposure of farmers to phosmet, a swine insecticide. Scand. J. Work Environ. Health 1999, 25, 33–38. [Google Scholar] [CrossRef] [PubMed]
- Machera, K.; Goumenou, M.; Kapetanakis, E.; Kalamarakis, A.; Glass, C.R. Determination of potential dermal and inhalation operator exposure to malathion in greenhouses with the whole body dosimetry method. Ann. Occup. Hyg. 2003, 47, 61–70. [Google Scholar] [CrossRef] [PubMed]
- Ekström, G.; Ekbom, B. Pest control in agro-ecosystems: An ecological approach. Crit. Rev. Plant Sci. 2011, 30, 74–94. [Google Scholar] [CrossRef]
- Dent, D. Overview of agrobiologicals and alternatives to synthetic pesticides. In The Pesticide Detox: Towards a More Sustainable Agriculture; Pretty, J., Ed.; Earthscan: London, UK, 2005; pp. 70–82. [Google Scholar]
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Damalas, C.A.; Koutroubas, S.D. Farmers’ Exposure to Pesticides: Toxicity Types and Ways of Prevention. Toxics 2016, 4, 1. https://doi.org/10.3390/toxics4010001
Damalas CA, Koutroubas SD. Farmers’ Exposure to Pesticides: Toxicity Types and Ways of Prevention. Toxics. 2016; 4(1):1. https://doi.org/10.3390/toxics4010001
Chicago/Turabian StyleDamalas, Christos A., and Spyridon D. Koutroubas. 2016. "Farmers’ Exposure to Pesticides: Toxicity Types and Ways of Prevention" Toxics 4, no. 1: 1. https://doi.org/10.3390/toxics4010001
APA StyleDamalas, C. A., & Koutroubas, S. D. (2016). Farmers’ Exposure to Pesticides: Toxicity Types and Ways of Prevention. Toxics, 4(1), 1. https://doi.org/10.3390/toxics4010001







