Alkenylbenzenes in Foods: Aspects Impeding the Evaluation of Adverse Health Effects
Abstract
1. Introduction
2. Current Knowledge
2.1. Occurrence of Alkenylbenzenes
2.1.1. Alkenylbenzenes in Herbs and Spices
Fennel
Basil
2.1.2. Alkenylbenzenes in Aromatized and Fortified Food Products
Essential Oils Used as Food Flavorings
2.2. Toxicity of Alkenylbenzenes
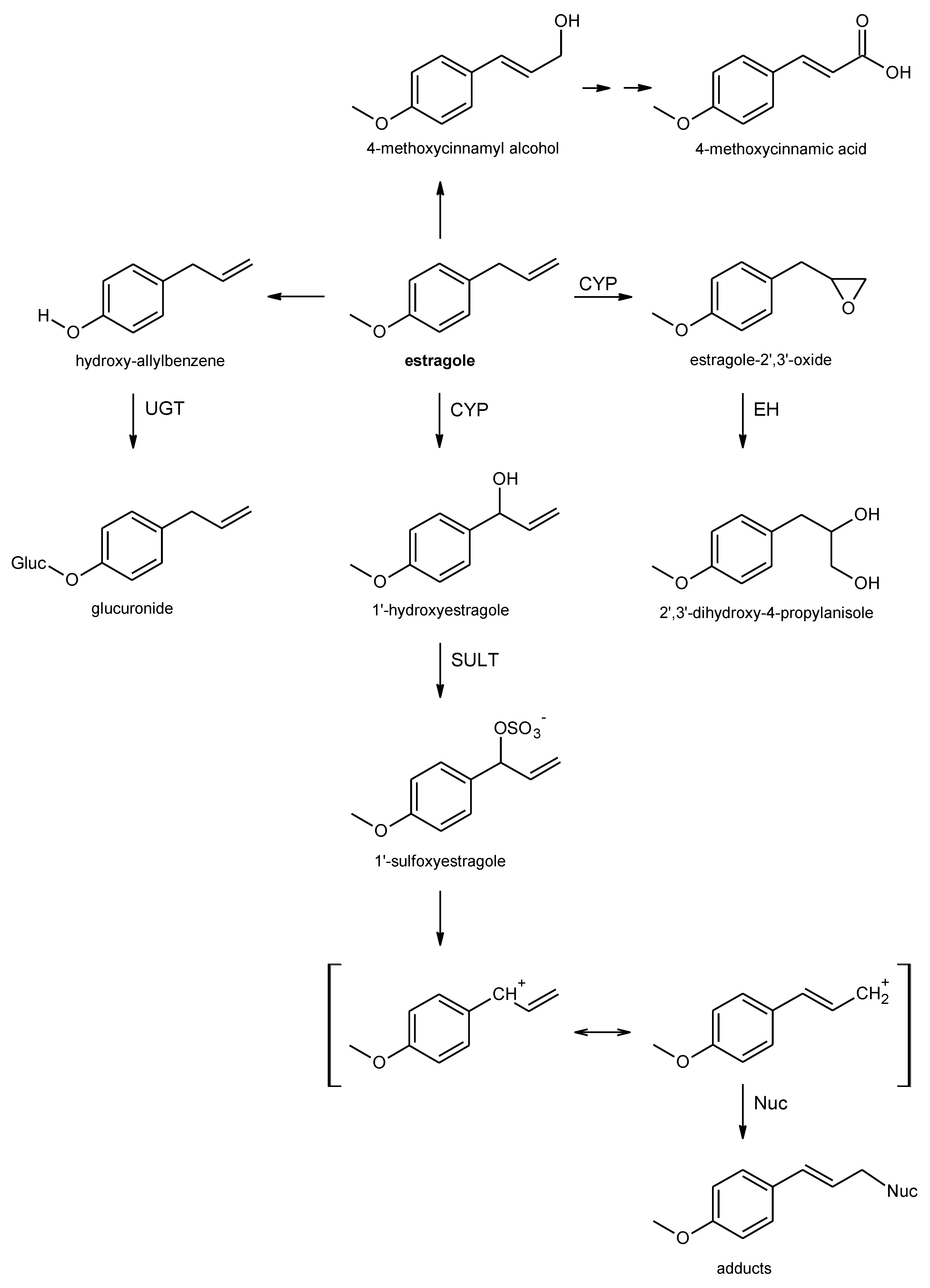
2.2.1. Toxicokinetic Impact on Toxic Properties of Alkenylbenzenes
2.2.2. Aspects Regarding Genotoxic and Carcinogenic Effects of Alkenylbenzenes
Safrole
Estragole
Methyleugenol
Other Alkenylbenzenes
2.2.3. Toxicity of Alkenylbenzenes from Complex Food Matrices
2.2.4. Genotoxicity and Carcinogenicity of Alkenylbenzenes Required Restrictions for Their Use in Foods
3. Aspects Impeding the Evaluation of Adverse Health Effects of Alkenylbenzenes
3.1. Uncertainties Regarding the Occurrence of Alkenylbenzenes
3.1.1. Conclusions Regarding Aromatized Foods and Their Potential Alkenylbenzene Contents
3.1.2. Issues Regarding Currently Available Occurrence Data for Alkenylbenzenes
3.2. Consumption of Alkenylbenzene-Containing Foodstuffs
3.2.1. Limited Availability of Data Regarding Consumption
3.2.2. Lack of Biomarker Prevents Exposure Estimation
3.3. Issues Regarding the Toxicity of Alkenylbenzenes
3.3.1. The Genotoxic and Carcinogenic Potential of Alkenylbenzenes
3.3.2. Weaknesses of Standard Genotoxicity Tests and Implications for Hazard Assessment
False-Negative Results
False-Positive Results
Possible Ways to Optimize Standard Genotoxicity Tests
Optimization of Standard Genotoxicity Tests Using the Example of the Alkenylbenzene Methyleugenol
Outlook for Future Studies and Testing
3.3.3. Toxicity of Mixtures Is Still a Controversially Debated Issue
3.3.4. Transferability of Findings in Animal Studies to Human
4. Conclusions
- valid occurrence data reflecting the occurrence of all toxicologically relevant alkenylbenzenes in different food products
- comprehensive consumption data for such alkenylbenzene-containing products, which should be collected via appropriate consumption surveys
- determination of toxicological properties of yet insufficiently investigated derivatives, such as elemicin and apiol, via adequate studies designed according to international guidelines and taking into account the alkenylbenzene-specific bioactivation (e.g., via SULTs)
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kristanc, L.; Kreft, S. European medicinal and edible plants associated with subacute and chronic toxicity part I: Plants with carcinogenic, teratogenic and endocrine-disrupting effects. Food Chem. Toxicol. 2016, 92, 150–164. [Google Scholar] [CrossRef]
- Atkinson, R.G. Phenylpropenes: Occurrence, Distribution, and Biosynthesis in Fruit. J. Agric. Food Chem. 2016, 66, 2259–2272. [Google Scholar] [CrossRef] [PubMed]
- Alajlouni, A.M.; Al-Malahmeh, A.J.; Isnaeni, F.N.; Wesseling, S.; Vervoort, J.; Rietjens, I.M. Level of Alkenylbenzenes in Parsley and Dill Based Teas and Associated Risk Assessment Using the Margin of Exposure Approach. J. Agric. Food Chem. 2016, 64, 8640–8646. [Google Scholar] [CrossRef] [PubMed]
- van den Berg, S.J.; Alhusainy, W.; Restani, P.; Rietjens, I.M. Chemical analysis of estragole in fennel based teas and associated safety assessment using the Margin of Exposure (MOE) approach. Food Chem. Toxicol. 2014, 65, 147–154. [Google Scholar] [CrossRef] [PubMed]
- Uusitalo, L.; Salmenhaara, M.; Isoniemi, M.; Garcia-Alvarez, A.; Serra-Majem, L.; Ribas-Barba, L.; Finglas, P.; Plumb, J.; Tuominen, P.; Savela, K. Intake of selected bioactive compounds from plant food supplements containing fennel (Foeniculum vulgare) among Finnish consumers. Food Chem. 2016, 194, 619–625. [Google Scholar] [CrossRef] [PubMed]
- Al-Malahmeh, A.J.; Al-Ajlouni, A.M.; Wesseling, S.; Vervoort, J.; Rietjens, I.M. Determination and risk assessment of naturally occurring genotoxic and carcinogenic alkenylbenzenes in basil-containing sauce of pesto. Toxicol. Rep. 2016, 4, 1–8. [Google Scholar] [CrossRef]
- Swanson, A.B.; Chambliss, D.D.; Blomquist, J.C.; Miller, E.C.; Miller, J.A. The mutagenicities of safrole, estragole, eugenol, trans-anethole, and some of their known or possible metabolites for Salmonella typhimurium mutants. Mutat. Res. Mol. Mech. Mutagen. 1979, 60, 143–153. [Google Scholar] [CrossRef]
- Drinkwater, N.R.; Miller, E.C.; Miller, J.A.; Pitot, H.C. Hepatocarcinogenicity of Estragole (1-Allyl-4-methoxybenzene) and 1′-Hydroxyestragole in the Mouse and Mutagenicity of 1′-Acetoxyestragole in Bacteria 2. J. Natl. Cancer Inst. 1976, 57, 1323–1331. [Google Scholar] [CrossRef]
- Dusemund, B.; Rietjens, I.M.; Abraham, K.; Cartus, A.; Schrenk, D. Chapter 16—Undesired Plant-Derived Components in Food. In Chemical Contaminants and Residues in Food, 2nd ed.; Woodhead Publishing: Southston, UK, 2017; pp. 379–424. [Google Scholar]
- van den Berg, S.J.; Klaus, V.; Alhusainy, W.; Rietjens, I.M. Matrix-derived combination effect and risk assessment for estragole from basil-containing plant food supplements (PFS). Food Chem. Toxicol. 2013, 62, 32–40. [Google Scholar] [CrossRef]
- Alhusainy, W.; Paini, A.; Berg, J.H.J.V.D.; Punt, A.; Scholz, G.; Schilter, B.; Van Bladeren, P.J.; Taylor, S.; Adams, T.B.; Rietjens, I.M. In vivo validation and physiologically based biokinetic modeling of the inhibition of SULT-mediated estragole DNA adduct formation in the liver of male Sprague-Dawley rats by the basil flavonoid nevadensin. Mol. Nutr. Food Res. 2013, 57, 1969–1978. [Google Scholar] [CrossRef]
- EFSA-ESCO. ESCO report: Advice on the EFSA guidance document for the safety assessment of botanicals and botanical preparations intended for use as food supplements, based on real case studies. In EFSA Supporting Publications; Wiley: Hoboken, NJ, USA, 2009; Volume 6, p. 280. [Google Scholar]
- EFSA. Minutes of the 23rd Plenary Meeting of the Scientific Panel on Food Additives, Flavourings, Processing Aids and Materials in Contact with Food (AFC); EFSA: Parma, Italy, 2007.
- Martinez-Velazquez, M.; Castillo-Herrera, G.A.; Rosario-Cruz, R.; Flores-Fernandez, J.M.; Lopez-Ramirez, J.; Hernandez-Gutierrez, R.; Lugo-Cervantes, E.D.C.; Rosario-Cruz, R. Acaricidal effect and chemical composition of essential oils extracted from Cuminum cyminum, Pimenta dioica and Ocimum basilicum against the cattle tick Rhipicephalus (Boophilus) microplus (Acari: Ixodidae). Parasitol. Res. 2010, 108, 481–487. [Google Scholar] [CrossRef] [PubMed]
- Padmakumari, K.; Sasidharan, I.; Sreekumar, M. Composition and antioxidant activity of essential oil of pimento (Pimenta dioica (L.) Merr.) from Jamaica. Nat. Prod. Res. 2011, 25, 152–160. [Google Scholar] [CrossRef]
- Nabney, J.; Robinson, F.V. Constituents of pimento berry oil (Pimenta dioica). Flavour Ind. 1972, 3, 50–51. [Google Scholar]
- Anastasopoulou, E.; Graikou, K.; Ganos, C.; Calapai, G.; Chinou, I. Pimpinella anisum seeds essential oil from Lesvos Island: Effect of hydrodistillation time, comparison of its aromatic profile with other samples of the Greek market. Safe use. Food Chem. Toxicol. 2019, 135, 110875. [Google Scholar] [CrossRef] [PubMed]
- Orav, A.; Raal, A.; Arak, E. Essential oil composition of Pimpinella anisum L. fruits from various European countries. Nat. Prod. Res. 2008, 22, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Bricout, J. Sur la constitution de l’huile essentielle de badiane. Bull. Société Chim. Fr. 1974, 384, 1901–1903. [Google Scholar]
- De Maack, F.; Brunet, D.; Malnati, J.-C.; Estienne, J. Étude des constituants mineurs de l’anéthole obtenu à partir d’huile essentielle de badiane—Contribution à la recherche de l’origine d’un anéthole par l’identification des sesquiterpènes. Ann. Falsif. L’expertise Chim. Toxicol. 1982, 810, 357–367. [Google Scholar]
- Tuan, D.Q.; Ilangantileket, S.G. Liquid CO2 extraction of essential oil from Star anise fruits (Illicium verum H.). J. Food Eng. 1997, 31, 47–57. [Google Scholar] [CrossRef]
- Huang, Y.; Zhao, J.; Zhou, L.; Wang, J.; Gong, Y.; Chen, X.; Guo, Z.; Wang, Q.; Jiang, W. Antifungal Activity of the Essential Oil of Illicium verum Fruit and Its Main Component trans-Anethole. Molecules 2010, 15, 7558–7569. [Google Scholar] [CrossRef] [PubMed]
- Cook, W.B.; Howard, A.S. The essential oil of illicium anisatum linn. Can. J. Chem. 1966, 44, 2461–2464. [Google Scholar] [CrossRef]
- Trenkle, K. Recent studies on fennel (Foeniculum vulgare M.) 2. The volatile oil of the fruit, herbs and roots of fruit-bearing plants. Die Pharm. 1972, 27, 319–324. [Google Scholar]
- Muráriková, A.; Ťažký, A.; Neugebauerová, J.; Planková, A.; Jampílek, J.; Mučaji, P.; Mikuš, P. Characterization of essential oil composition in different basil species and pot cultures by a GC-MS method. Molecules 2017, 22, 1221. [Google Scholar] [CrossRef] [PubMed]
- Fischer, R.; Nitzan, N.; Chaimovitsh, D.; Rubin, B.; Dudai, N. Variation in Essential Oil Composition within Individual Leaves of Sweet Basil (Ocimum basilicum L.) Is More Affected by Leaf Position than by Leaf Age. J. Agric. Food Chem. 2011, 59, 4913–4922. [Google Scholar] [CrossRef]
- Chalchat, J.-C.; Özcan, M.M. Comparative essential oil composition of flowers, leavesand stems of basil (Ocimum basilicum L.) used as herb. Food Chem. 2008, 110, 501–503. [Google Scholar] [CrossRef]
- Vani, S.R.; Cheng, S.; Chuah, C. Comparative study of volatile compounds from genus Ocimum. Am. J. Appl. Sci. 2009, 6, 523. [Google Scholar] [CrossRef]
- Tateo, F.; Santamaria, L.; Bianchi, L.; Bianchi, A. Basil Oil and Tarragon Oil: Composition and Genotoxicity Evaluation. J. Essent. Oil Res. 1989, 1, 111–118. [Google Scholar] [CrossRef]
- Vostrowsky, O.; Michaelis, K.; Ihm, H.; Zintl, R.; Knobloch, K. On the essential oil components from tarragon (Artemisia dracunculus L.). Z. Lebensm. Unters. Forschung 1981, 173, 365–367. [Google Scholar] [CrossRef]
- De Vincenzi, M.; Silano, M.; Maialetti, F.; Scazzocchio, B. Constituents of aromatic plants: II. Estragole. Fitoterapia 2000, 71, 725–729. [Google Scholar] [CrossRef]
- Lawrence, B.M. Progress in essential oils/Progrès dans le domaine des huiles essentielles. Perfum. Flavorist 1988, 13, 44–50. [Google Scholar]
- Du, S.-S.; Yang, K.; Wang, C.-F.; You, C.X.; Geng, Z.-F.; Guo, S.-S.; Deng, Z.-W.; Liu, Z.-L. Chemical constituents and activities of the essential oil from myristica fragrans against cigarette beetle lasioderma serricorne. Chem. Biodivers. 2014, 11, 1449–1456. [Google Scholar] [CrossRef] [PubMed]
- Committee, A.M. Application of gas-liquid chromatography to the analysis of essential oils. Part XIV. Monographs for five essential oils. Analyst 1988, 113, 1125–1136. [Google Scholar]
- Embong, M.B.; Hadziyev, D.; Molnar, S. Essential oils from spices grown in Alberta. Anise oil (Pimpinella anisum). Can. J. Plant Sci. 1977, 57, 681–688. [Google Scholar] [CrossRef]
- Piccaglia, R.; Marotti, M. Characterization of several aromatic plants grown in northern Italy. Flavour Fragr. J. 1993, 8, 115–122. [Google Scholar] [CrossRef]
- Simándi, B.; Deák, A.; Rónyai, E.; Yanxiang, G.; Veress, T.; Lemberkovics, E.; Then, M.; Sass-Kiss, A.; Vámos-Falusi, Z. Supercritical carbon dioxide extraction and fractionation of fennel oil. J. Agric. Food Chem. 1999, 47, 1635–1640. [Google Scholar] [CrossRef]
- Miguel, M.G.; Cruz, C.; Faleiro, L.; Simões, M.T.F.; Figueiredo, A.C.; Barroso, J.; Pedro, L. Foeniculum vulgare Essential Oils: Chemical Composition, Antioxidant and Antimicrobial Activities. Nat. Prod. Commun. 2010, 5, 319–328. [Google Scholar] [CrossRef]
- Basaglia, G.; Fiori, J.; Leoni, A.; Gotti, R. Determination of Estragole in Fennel Herbal Teas by HS-SPME and GC–MS. Anal. Lett. 2013, 47, 268–279. [Google Scholar] [CrossRef]
- Raffo, A.; Nicoli, S.; Leclercq, C. Quantification of estragole in fennel herbal teas: Implications on the assessment of dietary exposure to estragole. Food Chem. Toxicol. 2010, 49, 370–375. [Google Scholar] [CrossRef]
- Denzer, M.Y.; Kirsch, F.; Buettner, A. Are odorant constituents of herbal tea transferred into human milk? J. Agric. Food Chem. 2015, 63, 104–111. [Google Scholar] [CrossRef]
- Hausner, H.; Bredie, W.L.; Mølgaard, C.; Petersen, M.A.; Møller, P. Differential transfer of dietary flavour compounds into human breast milk. Physiol. Behav. 2008, 95, 118–124. [Google Scholar] [CrossRef] [PubMed]
- Bousova, K.; Mittendorf, K.; Senyuva, H. A solid-phase microextraction GC/MS/MS method for rapid quantitative analysis of food and beverages for the presence of legally restricted biologically active flavorings. J. Assoc. Off. Anal. Chem. 2011, 94, 1189–1199. [Google Scholar] [CrossRef]
- Siano, F.; Ghizzoni, C.; Gionfriddo, F.; Colombo, E.; Servillo, L.; Castaldo, D. Determination of estragole, safrole and eugenol methyl ether in food products. Food Chem. 2003, 81, 469–475. [Google Scholar] [CrossRef]
- Sestili, P.; Ismail, T.; Calcabrini, C.; Guescini, M.; Catanzaro, E.; Turrini, E.; Layla, A.; Akhtar, S.; Fimognari, C. The potential effects of Ocimum basilicum on health: A review of pharmacological and toxicological studies. Expert Opin. Drug Metab. Toxicol. 2018, 14, 679–692. [Google Scholar] [CrossRef]
- Surburg, H.; Panten, J. Common Fragrance and Flavor Materials: Preparation, Properties and Uses; Wiley: Hoboken, NJ, USA, 2006. [Google Scholar]
- Roohinejad, S.; Koubaa, M.; Barba, F.J.; Leong, S.Y.; Khelfa, A.; Greiner, R.; Chemat, F. Extraction Methods of Essential Oils From Herbs and Spices. In Essential Oils in Food Processing; John Wiley & Sons: Chichester, UK, 2017; pp. 21–55. [Google Scholar] [CrossRef]
- Krishnamoorty, B.; Rema, J. Nutmeg and mace. In Handbook of Herbs and Spices; Peter, K.V., Ed.; Woodhead Publishing Ltd.: Cambridge, UK, 2001; pp. 238–248. [Google Scholar]
- Raffo, A.; D’Aloise, A.; Magrì, A.L.; Leclercq, C. Quantitation of tr-cinnamaldehyde, safrole and myristicin in cola-flavoured soft drinks to improve the assessment of their dietary exposure. Food Chem. Toxicol. 2013, 59, 626–635. [Google Scholar] [CrossRef]
- Benedetti, M.S.; Malnoe, A.; Broillet, A.L. Absorption, metabolism and excretion of safrole in the rat and man. Toxicology 1977, 7, 69–83. [Google Scholar] [CrossRef]
- Caldwell, J.; Sutton, J. Influence of dose size on the disposition of trans-[methoxy-14C]anethole in human volunteers. Food Chem. Toxicol. 1988, 26, 87–91. [Google Scholar] [CrossRef]
- Monien, B.H.; Sachse, B.; Niederwieser, B.; Abraham, K. Detection of N-Acetyl-S-[3′-(4-methoxyphenyl)allyl]-l-Cys (AMPAC) in Human Urine Samples after Controlled Exposure to Fennel Tea: A New Metabolite of Estragole and trans-Anethole. Chem. Res. Toxicol. 2019, 32, 2260–2267. [Google Scholar] [CrossRef]
- Badger, D.; Smith, R.; Bao, J.; Kuester, R.; Sipes, I. Disposition and metabolism of isoeugenol in the male Fischer 344 rat. Food Chem. Toxicol. 2002, 40, 1757–1765. [Google Scholar] [CrossRef]
- Fischer, I.U.; Von Unruh, G.E.; Dengler, H.J. The metabolism of eugenol in man. Xenobiotica 1990, 20, 209–222. [Google Scholar] [CrossRef] [PubMed]
- Hong, S.P.; Fuciarelli, A.F.; Johnson, J.D.; Graves, S.W.; Bates, D.J.; Smith, C.S.; Waidyanatha, S. Toxicokinetics of Isoeugenol in F344 rats and B6C3F 1 mice. Xenobiotica 2013, 43, 1010–1017. [Google Scholar] [CrossRef] [PubMed]
- Hong, S.P.; Fuciarelli, A.F.; Johnson, J.D.; Graves, S.W.; Bates, D.J.; Waidyanatha, S.; Smith, C.S. Toxicokinetics of methyleugenol in F344 rats and B6C3F 1 mice. Xenobiotica 2012, 43, 293–302. [Google Scholar] [CrossRef]
- Sangster, S.A.; Caldwell, J.; Hutt, A.J.; Anthony, A.; Smith, R.L. The metabolic disposition of [methoxy-14c]-labelled trans-anethole, estragole and p-propylanisole in human volunteers. Xenobiotica 1987, 17, 1223–1232. [Google Scholar] [CrossRef]
- Zeller, A.; Horst, K.; Rychlik, M. Study of the Metabolism of Estragole in Humans Consuming Fennel Tea. Chem. Res. Toxicol. 2009, 22, 1929–1937. [Google Scholar] [CrossRef]
- Martins, C.; Rueff, J.; Rodrigues, A.S. Genotoxic alkenylbenzene flavourings, a contribution to risk assessment. Food Chem. Toxicol. 2018, 118, 861–879. [Google Scholar] [CrossRef] [PubMed]
- Rietjens, I.M.; Cohen, S.M.; Fukushima, S.; Gooderham, N.; Hecht, S.; Marnett, L.J.; Smith, R.L.; Adams, T.B.; Bastaki, M.; Harman, C.G.; et al. Impact of Structural and Metabolic Variations on the Toxicity and Carcinogenicity of Hydroxy- and Alkoxy-Substituted Allyl- and Propenylbenzenes. Chem. Res. Toxicol. 2014, 27, 1092–1103. [Google Scholar] [CrossRef]
- Cartus, A.; Herrmann, K.; Weishaupt, L.W.; Merz, K.-H.; Engst, W.; Glatt, H.; Schrenk, D. Metabolism of Methyleugenol in Liver Microsomes and Primary Hepatocytes: Pattern of Metabolites, Cytotoxicity, and DNA-Adduct Formation. Toxicol. Sci. 2012, 129, 21–34. [Google Scholar] [CrossRef]
- Cartus, A.T.; Merz, K.-H.; Schrenk, D. Metabolism of Methylisoeugenol in Liver Microsomes of Human, Rat, and Bovine Origin. Drug Metab. Dispos. 2011, 39, 1727–1733. [Google Scholar] [CrossRef]
- Kamienski, F.X.; Casida, J.E. Importance of demethylenation in the metabolism in vivo and in vitro of methylenedioxyphenyl synergists and related compounds in mammals. Biochem. Pharmacol. 1970, 19, 91–112. [Google Scholar] [CrossRef]
- Klungsøyr, J.; Scheline, R.R. Metabolism of safrole in the rat. Acta Pharmacol. Toxicol. 1983, 52, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Solheim, E.; Scheline, R.R. Metabolism of alkenebenzene derivatives in the rat I. P-methoxyallylbenzene (estragole) and p-methoxypropenylbenzene (anethole). Xenobiotica 1973, 3, 493–510. [Google Scholar] [CrossRef]
- Solheim, E.; Scheline, R.R. Metabolism of Alkenebenzene Derivatives in the Rat. II. Eugenol and Isoeugenol Methyl Ethers. Xenobiotica 1976, 6, 137–150. [Google Scholar] [CrossRef] [PubMed]
- Solheim, E.; Scheline, R.R. Metabolism of alkenebenzene derivatives in the rat III. Elemicin and isoelemicin. Xenobiotica 1980, 10, 371–380. [Google Scholar] [CrossRef]
- Anthony, A.; Caldwell, J.; Hutt, A.; Smith, R. Metabolism of estragole in rat and mouse and influence of dose size on excretion of the proximate carcinogen 1′-hydroxyestragole. Food Chem. Toxicol. 1987, 25, 799–806. [Google Scholar] [CrossRef]
- Guenthner, T.M.; Luo, G. Investigation of the role of the 2′,3′-epoxidation pathway in the bioactivation and genotoxicity of dietary allylbenzene analogs. Toxicology 2001, 160, 47–58. [Google Scholar] [CrossRef]
- Luo, G.; Guenthner, T.M. Detoxication of the 2′,3′-epoxide metabolites of allylbenzene and estragole: Conjugation with glutathione. Drug Metab. Dispos. 1994, 22, 731–737. [Google Scholar]
- Luo, G.; Guenthner, T.M. Covalent binding to DNA in vitro of 2′,3′-oxides derived from allylbenzene analogs. Drug Metab. Dispos. 1996, 24, 1020–1027. [Google Scholar]
- Iyer, L.V.; Ho, M.N.; Shinn, W.M.; Bradford, W.W.; Tanga, M.J.; Nath, S.S.; Green, C.E. Glucuronidation of 1′-Hydroxyestragole (1′-HE) by Human UDP-Glucuronosyltransferases UGT2B7 and UGT1A9. Toxicol. Sci. 2003, 73, 36–43. [Google Scholar] [CrossRef] [PubMed]
- Al-Subeihi, A.A.; Spenkelink, B.; Punt, A.; Boersma, M.G.; van Bladeren, P.J.; Rietjens, I.M. Physiologically based kinetic modeling of bioactivation and detoxification of the alkenylbenzene methyleugenol in human as compared with rat. Toxicol. Appl. Pharmacol. 2012, 260, 271–284. [Google Scholar] [CrossRef]
- Martati, E.; Boersma, M.G.; Spenkelink, A.; Khadka, D.B.; van Bladeren, P.J.; Rietjens, I.M.; Punt, A. Physiologically Based Biokinetic (PBBK) Modeling of Safrole Bioactivation and Detoxification in Humans as Compared With Rats. Toxicol. Sci. 2012, 128, 301–316. [Google Scholar] [CrossRef]
- Punt, A.; Paini, A.; Boersma, M.G.; Freidig, A.P.; Delatour, T.; Scholz, G.; Schilter, B.; van Bladeren, P.J.; Rietjens, I.M. Use of Physiologically Based Biokinetic (PBBK) Modeling to Study Estragole Bioactivation and Detoxification in Humans as Compared with Male Rats. Toxicol. Sci. 2009, 110, 255–269. [Google Scholar] [CrossRef]
- Bergau, N.; Herfurth, U.M.; Sachse, B.; Abraham, K.; Monien, B.H. Bioactivation of estragole and anethole leads to common adducts in DNA and hemoglobin. Food Chem. Toxicol. 2021, 153, 112253. [Google Scholar] [CrossRef] [PubMed]
- Herrmann, K.; Engst, W.; Appel, K.E.; Monien, B.H.; Glatt, H. Identification of human and murine sulfotransferases able to activate hydroxylated metabolites of methyleugenol to mutagens in Salmonella typhimurium and detection of associated DNA adducts using UPLC-MS/MS methods. Mutagenesis 2012, 27, 453–462. [Google Scholar] [CrossRef]
- NTP USNTP. NTP Technical Report on the Toxicology and Carcinogenesis Studies of Methyleugenol (CAS NO. 93-15-2) in F344/N Rats and B6C3F1 Mice (Gavage Studies); NTP TR 491; National Toxicology Program Technical Report Series (NTPTR); Environmental Health Information Service (EHS): Springfield, IL, USA, 2000; pp. 1–412.
- Miller, E.C.; Swanson, A.B.; Phillips, D.H.; Fletcher, T.L.; Liem, A.; Miller, J.A. Structure-activity studies of the carcinogenicities in the mouse and rat of some naturally occurring and synthetic alkenylbenzene derivatives related to safrole and estragole. Cancer Res. 1983, 43, 1124–1134. [Google Scholar]
- Boberg, E.W.; Miller, E.C.; Miller, J.A.; Poland, A.; Liem, A. Strong Evidence from Studies with Brachymorphic Mice and Pentachlorophenol That 1′-Sulfoöxysafrole Is the Major Ultimate Electrophilic and Carcinogenic Metabolite of 1′-Hydroxysafrole in Mouse Liver. Cancer Res. 1983, 43, 5163–5173. [Google Scholar] [PubMed]
- Punt, A.; Delatour, T.; Scholz, G.; Schilter, B.; van Bladeren, P.J.; Rietjens, I. Tandem Mass Spectrometry Analysis of N2-(trans-Isoestragol-3′-yl)-2′-deoxyguanosine as a Strategy to Study Species Differences in Sulfotransferase Conversion of the Proximate Carcinogen 1′-Hydroxyestragole. Chem. Res. Toxicol. 2007, 20, 991–998. [Google Scholar] [CrossRef]
- Al-Subeihi, A.A.; Spenkelink, B.; Rachmawati, N.; Boersma, M.G.; Punt, A.; Vervoort, J.; van Bladeren, P.J.; Rietjens, I. Physiologically based biokinetic model of bioactivation and detoxification of the alkenylbenzene methyleugenol in rat. Toxicol. Vitro. 2011, 25, 267–285. [Google Scholar] [CrossRef] [PubMed]
- Punt, A.; Freidig, A.P.; Delatour, T.; Scholz, G.; Boersma, M.G.; Schilter, B.; Van Bladeren, P.J.; Rietjens, I.M. A physiologically based biokinetic (PBBK) model for estragole bioactivation and detoxification in rat. Toxicol. Appl. Pharmacol. 2008, 231, 248–259. [Google Scholar] [CrossRef] [PubMed]
- Herrmann, K.; Schumacher, F.; Engst, W.; Appel, K.E.; Klein, K.; Zanger, U.M.; Glatt, H. Abundance of DNA adducts of methyleugenol, a rodent hepatocarcinogen, in human liver samples. Carcinogenesis 2013, 34, 1025–1030. [Google Scholar] [CrossRef] [PubMed]
- Tremmel, R.; Herrmann, K.; Engst, W.; Meinl, W.; Klein, K.; Glatt, H.; Zanger, U.M. Methyleugenol DNA adducts in human liver are associated with SULT1A1 copy number variations and expression levels. Arch. Toxicol. 2017, 91, 3329–3339. [Google Scholar] [CrossRef]
- Al-Subeihi, A.A.; Alhusainy, W.; Kiwamoto, R.; Spenkelink, B.; van Bladeren, P.J.; Rietjens, I.M.; Punt, A. Evaluation of the interindividual human variation in bioactivation of methyleugenol using physiologically based kinetic modeling and Monte Carlo simulations. Toxicol. Appl. Pharmacol. 2015, 283, 117–126. [Google Scholar] [CrossRef]
- Ning, J.; Louisse, J.; Spenkelink, B.; Wesseling, S.; Rietjens, I.M. Study on inter-ethnic human differences in bioactivation and detoxification of estragole using physiologically based kinetic modeling. Arch. Toxicol. 2017, 91, 3093–3108. [Google Scholar] [CrossRef]
- Punt, A.; Paini, A.; Spenkelink, A.; Scholz, G.; Schilter, B.; Van Bladeren, P.J.; Rietjens, I.M. Evaluation of Interindividual Human Variation in Bioactivation and DNA Adduct Formation of Estragole in Liver Predicted by Physiologically Based Kinetic/Dynamic and Monte Carlo Modeling. Chem. Res. Toxicol. 2016, 29, 659–668. [Google Scholar] [CrossRef]
- Al-Malahmeh, A.J.; Al-Ajlouni, A.; Wesseling, S.; Soffers, A.E.M.F.; Al-Subeihi, A.; Kiwamoto, R.; Vervoort, J.; Rietjens, I.M. Physiologically based kinetic modeling of the bioactivation of myristicin. Arch. Toxicol. 2016, 91, 713–734. [Google Scholar] [CrossRef]
- Martati, E.; Boersma, M.G.; Spenkelink, A.; Khadka, D.B.; Punt, A.; Vervoort, J.; Van Bladeren, P.J.; Rietjens, I.M. Physiologically Based Biokinetic (PBBK) Model for Safrole Bioactivation and Detoxification in Rats. Chem. Res. Toxicol. 2011, 24, 818–834. [Google Scholar] [CrossRef]
- van den Berg, S.J.P.L.; Punt, A.; Soffers, A.E.; Vervoort, J.; Ngeleja, S.; Spenkelink, B.; Rietjens, I.M. Physiologically based kinetic models for the alkenylbenzene elemicin in rat and human and possible implications for risk assessment. Chem. Res. Toxicol. 2012, 25, 2352–2367. [Google Scholar] [CrossRef]
- Truhaut, R.; Le Bourhis, B.; Attia, M.; Glomot, R.; Newman, J.; Caldwell, J. Chronic toxicity/carcinogenicity study of trans-anethole in rats. Food Chem. Toxicol. 1989, 27, 11–20. [Google Scholar] [CrossRef]
- Sangster, S.; Caldwell, J.; Smith, R. Metabolism of anethole. II. Influence of dose size on the route of metabolism of trans-anethole in the rat and mouse. Food Chem. Toxicol. 1984, 22, 707–713. [Google Scholar] [CrossRef]
- Sangster, S.; Caldwell, J.; Smith, R.; Farmer, P. Metabolism of anethole. I. Pathways of metabolism in the rat and mouse. Food Chem. Toxicol. 1984, 22, 695–706. [Google Scholar] [CrossRef]
- Newberne, P.; Smith, R.; Doull, J.; Goodman, J.; Munro, I.; Portoghese, P.; Wagner, B.; Weil, C.; Woods, L.; Adams, T.; et al. The FEMA GRAS Assessment of trans-Anethole Used as a Flavouring Substance. Food Chem. Toxicol. 1999, 37, 789–811. [Google Scholar] [CrossRef]
- NTP. Carcinogenesis Studies of Eugenol (CAS No. 93-15-2) in F344/N Rats and B6C3F1 Mice (Feed Studies); NTP-80-068 No. 223 (=NIH Publication No. 84-1779); National Toxicology Program Technical Report Series (NTPTR); European Commission: Brussel, Belgium, 1983; pp. 1–159. [Google Scholar]
- NTP USNTP. NTP Technical Report on the Toxicology and Carcinogenesis Studies of Isoeugenol (CAS No. 97-54-1) in F344/N Rats and B6C3F1 Mice (Gavage Studies); NTP TR 551 National Toxicology Program Technical Report Series (NTPTR); European Commission: Brussel, Belgium, 2010; pp. 1–178. [Google Scholar]
- SCF ECSCoF. Opinion of the Scientific Committee on Food on the Safety of the Presence of Safrole (1-allyl-3,4-methylene Dioxy Benzene) in Flavourings and other Food Ingredients with Flavouring Properties; European Commission: Brussel, Belgium, 2002; pp. 1–15. [Google Scholar]
- Homburger, F.; Kelley, J.T.; Friedler, G.; Russfield, A.; Homburger, H. Toxic and Possible Carcinogenic Effects of 4-AlIyl-1,2-Methylenedioxybenzene (Safrole) in Rats on Deficient Diets. Pharmacology 1961, 4, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Innes, J.R.; Ulland, B.M.; Valerio, M.G.; Petrucelli, L.; Fishbein, L.; Hart, E.R.; Pallotta, A.J.; Bates, R.R.; Falk, H.L.; Gart, J.J.; et al. Bioassay of pesticides and industrial chemicals for tumorigenicity in mice: A preliminary note. J. Natl. Cancer Inst. 1969, 42, 1101–1114. [Google Scholar]
- Bode, A.M.; Dong, Z. Toxic Phytochemicals and Their Potential Risks for Human Cancer. Cancer Prev. Res. 2014, 8, 1–8. [Google Scholar] [CrossRef]
- Borchert, P.; Miller, J.A.; Miller, E.C.; Shires, T.K. 1′-Hydroxysafrole, a proximate carcinogenic metabolite of safrole in the rat and mouse. Cancer Res. 1973, 33, 590–600. [Google Scholar]
- Jeurissen, S.M.F.; Bogaards, J.J.P.; Awad, H.M.; Boersma, M.G.; Brand, W.; Fiamegos, Y.C.; Van Beek, T.A.; Alink, G.M.; Sudhölter, E.J.R.; Cnubben, N.H.P.; et al. Human Cytochrome P450 Enzyme Specificity for Bioactivation of Safrole to the Proximate Carcinogen 1‘-Hydroxysafrole. Chem. Res. Toxicol. 2004, 17, 1245–1250. [Google Scholar] [CrossRef] [PubMed]
- Munerato, M.C.; Sinigaglia, M.; Reguly, M.L.; de Andrade, H.H.R. Genotoxic effects of eugenol, isoeugenol and safrole in the wing spot test of Drosophila melanogaster. Mutat. Res. Toxicol. Environ. Mutagen. 2005, 582, 87–94. [Google Scholar] [CrossRef]
- IARC. Overall evaluations of carcinogenicity: An updating of IARC Monographs Volumes 1 to 42—Eugenol. In IARC Monographs on the Evaluation of Carcinogenic Risk of Chemicals to Humans; IARC: Lyon, France, 1987; Volume 36, pp. 1–63. [Google Scholar]
- Suzuki, Y.; Umemura, T.; Hibi, D.; Inoue, T.; Jin, M.; Ishii, Y.; Sakai, H.; Nohmi, T.; Yanai, T.; Nishikawa, A.; et al. Possible involvement of genotoxic mechanisms in estragole-induced hepatocarcinogenesis in rats. Arch. Toxicol. 2012, 86, 1593–1601. [Google Scholar] [CrossRef]
- Smith, R.; Adams, T.; Doull, J.; Feron, V.; Goodman, J.; Marnett, L.; Portoghese, P.; Waddell, W.; Wagner, B.; Rogers, A.; et al. Safety assessment of allylalkoxybenzene derivatives used as flavouring substances—methyl eugenol and estragole. Food Chem. Toxicol. 2002, 40, 851–870. [Google Scholar] [CrossRef]
- Probert, P.M.; Palmer, J.M.; Alhusainy, W.; Amer, A.; Rietjens, I.M.; White, S.A.; Jones, D.E.; Wright, M.C. Progenitor-derived hepatocyte-like (B-13/H) cells metabolise 1′-hydroxyestragole to a genotoxic species via a SULT2B1-dependent mechanism. Toxicol. Lett. 2015, 243, 98–110. [Google Scholar] [CrossRef] [PubMed]
- SCF ECSCoF. Opinion of the Scientific Committee on Food on Estragole (1-Allyl-4-methoxybenzene); Environmental Health Information Service (EHS): Springfield, IL, USA, 2001; pp. 1–10.
- NTP. Report on Carcinogens—Background Document for Methyleugenol; National Toxicology Program Technical Report Series (NTPTR); Environmental Health Information Service (EHS): Springfield, IL, USA, 2000; pp. 1–47.
- SCF ECSCoF. Opinion of the Scientific Committee on Food on Methyleugenol (4-Allyl-1,2-dimethoxybenzene); SCF/CS/FLAV/FLAVOUR/4 ADD1 FINAL; Environmental Health Information Service (EHS): Springfield, IL, USA, 2001.
- De Vincenzi, M.; Silano, M.; Stacchini, P.; Scazzocchio, B. Constituents of aromatic plants: I. Methyleugenol. Fitoterapia 2000, 71, 216–221. [Google Scholar] [CrossRef]
- Sekizawa, J.; Shibamoto, T. Genotoxicity of safrole-related chemicals in microbial test systems. Mutat. Res. Toxicol. 1982, 101, 127–140. [Google Scholar] [CrossRef]
- Chan, V.; Caldwell, J. Comparative induction of unscheduled DNA synthesis in cultured rat hepatocytes by allylbenzenes and their 1′-hydroxy metabolites. Food Chem. Toxicol. 1992, 30, 831–836. [Google Scholar] [CrossRef]
- IARC. Methyleugenol. IARC Monographs Working Group on the Evaluation of Carcinogenic Risks to Humans, Lyon, France, 2011 IARC Monographs on the Evaluation of Carcinogenic Risk of Chemicals to Man; IARC: Geneva, Switzerland, 2013; Volume 101, pp. 407–433.
- Suparmi, S.; Ginting, A.J.; Mariyam, S.; Wesseling, S.; Rietjens, I.M. Levels of methyleugenol and eugenol in instant herbal beverages available on the Indonesian market and related risk assessment. Food Chem. Toxicol. 2019, 125, 467–478. [Google Scholar] [CrossRef] [PubMed]
- JECFA JFWECoFA. Sixty-fifth meeting of the Joint FAO/WHO Expert Committee on Food Additives. WHO Food Addit. Series 2006, 56, 155–200.
- EFSA. Consideration of eugenol and related hydroxyallylbenzene derivatives evaluated by JECFA (65th meeting) structurally related to ring-substituted phenolic substances evaluated by EFSA in FGE.22 (2006). EFSA J. 2009, 1–53. [Google Scholar] [CrossRef]
- NTP USNTP. Isoeugenol: Reproductive Assessment by Continuous Breeding when Administered to Sprague-Dawley Rats by Gavage; National Toxicology Program Technical Report Series (NTPTR); Environmental Health Information Service (EHS): Springfield, IL, USA, 2002; pp. 1–167.
- Burkey, J.L.; Sauer, J.-M.; McQueen, C.A.; Sipes, I.G. Cytotoxicity and genotoxicity of methyleugenol and related congeners—a mechanism of activation for methyleugenol. Mutat. Res. Mol. Mech. Mutagen. 2000, 453, 25–33. [Google Scholar] [CrossRef]
- Jansson, T.; Curvall, M.; Hedin, A.; Enzell, C.R. In vitro studies of biological effects of cigarette smoke condensate: II. Induction of sister-chromatid exchanges in human lymphocytes by weakly acidic, semivolatile constituents. Mutat. Res. Toxicol. 1986, 169, 129–139. [Google Scholar] [CrossRef]
- EFSA. Enzymes, Flavourings and Processing Aids (CEF). Scientific Opinion on Flavouring Group Evaluation 81 (FGE.81): Consideration of hydroxypropenylbenzenes evaluated by JECFA (61st meeting) structurally related to 2-methoxy-4-(prop-1-enyl)phenyl 3-methylbutyrate from chemical group 17 evaluated by EFSA in FGE.30. EFSA J. 2010, 8, 1899. [Google Scholar]
- EFSA. Scientific Opinion on Flavouring Group Evaluation 30, Revision 1 (FGE.30Rev1): 4-Prop-1-enylphenol and 2-methoxy-4-(prop-1-enyl)phenyl 3-methylbutyrate from chemical group 17. EFSA J. 2011, 9, 1991. [Google Scholar] [CrossRef]
- JECFA JFWECoFA. Sixty-first meeting of the Joint FAO/WHO Expert Committee on Food Addtives. WHO Tech. Rep. Ser. 2004, 922, 96. [Google Scholar]
- Gorelick, N. Genotoxicity of trans-anethole in vitro. Mutat. Res. Mol. Mech. Mutagen. 1995, 326, 199–209. [Google Scholar] [CrossRef]
- JECFA JFWECoFA. Evaluation of certain food additives. Fifty-first report of the Joint FAO/WHO Expert Committee on Food Additives. WHO Tech. Rep. Ser. 2000, 891, 1–168. [Google Scholar]
- EFSA Scientific Committee; More, S.; Bampidis, V.; Benford, D.; Boesten, J.; Bragard, C.; Halldorsson, T.; Hernandez-Jerez, A.; Hougaard-Bennekou, S.; Koutsoumanis, K.; et al. Genotoxicity assessment of chemical mixtures. EFSA J. 2019, 17, e05519. [Google Scholar] [CrossRef]
- Rietjens, I.M.; Slob, W.; Galli, C.; Silano, V. Risk assessment of botanicals and botanical preparations intended for use in food and food supplements: Emerging issues. Toxicol. Lett. 2008, 180, 131–136. [Google Scholar] [CrossRef]
- Al-Malahmeh, A.J.; Alajlouni, A.M.; Ning, J.; Wesseling, S.; Vervoort, J.; Rietjens, I.M. Determination and risk assessment of naturally occurring genotoxic and carcinogenic alkenylbenzenes in nutmeg-based plant food supplements. J. Appl. Toxicol. 2017, 37, 1254–1264. [Google Scholar] [CrossRef]
- Ning, J.; Cui, X.; Kong, X.; Tang, Y.; Wulandari, R.; Chen, L.; Wesseling, S.; Rietjens, I.M. Risk assessment of genotoxic and carcinogenic alkenylbenzenes in botanical containing products present on the Chinese market. Food Chem. Toxicol. 2018, 115, 344–357. [Google Scholar] [CrossRef] [PubMed]
- Yang, R.S.H. Toxicology of Chemical Mixtures: Case Studies, Mechanisms, and Novel Approaches; Elsevier Science: Amsterdam, The Netherlands, 2016. [Google Scholar]
- Könemann, W.; Pieters, M. Confusion of concepts in mixture toxicology. Food Chem. Toxicol. 1996, 34, 1025–1031. [Google Scholar] [CrossRef]
- EFSA. Guidance on harmonised methodologies for human health, animal health and ecological risk assessment of combined exposure to multiple chemicals. EFSA J. 2019, 17, e05634. [Google Scholar]
- Jeurissen, S.M.; Punt, A.; Delatour, T.; Rietjens, I.M. Basil extract inhibits the sulfotransferase mediated formation of DNA adducts of the procarcinogen 1′-hydroxyestragole by rat and human liver S9 homogenates and in HepG2 human hepatoma cells. Food Chem. Toxicol. 2008, 46, 2296–2302. [Google Scholar] [CrossRef] [PubMed]
- Müller, L.; Kasper, P.; Müller-Tegethoff, K.; Petr, T. The genotoxic potential in vitro and in vivo of the allyl benzene etheric oils estragole, basil oil and trans-anethole. Mutat. Res. Lett. 1994, 325, 129–136. [Google Scholar] [CrossRef]
- Alhusainy, W.; Paini, A.; Punt, A.; Louisse, J.; Spenkelink, A.; Vervoort, J.; Delatour, T.; Scholz, G.; Schilter, B.; Adams, T.; et al. Identification of nevadensin as an important herb-based constituent inhibiting estragole bioactivation and physiology-based biokinetic modeling of its possible in vivo effect. Toxicol. Appl. Pharmacol. 2010, 245, 179–190. [Google Scholar] [CrossRef]
- Alhusainy, W.; Williams, G.M.; Jeffrey, A.M.; Iatropoulos, M.J.; Taylor, S.; Adams, T.B.; Rietjens, I.M. The natural basil flavonoid nevadensin protects against a methyleugenol-induced marker of hepatocarcinogenicity in male F344 rat. Food Chem. Toxicol. 2014, 74, 28–34. [Google Scholar] [CrossRef]
- Al-Subeihi, A.A.; Alhusainy, W.; Paini, A.; Punt, A.; Vervoort, J.; van Bladeren, P.J.; Rietjens, I.M. Inhibition of methyleugenol bioactivation by the herb-based constituent nevadensin and prediction of possible in vivo consequences using physiologically based kinetic modeling. Food Chem. Toxicol. 2013, 59, 564–571. [Google Scholar] [CrossRef] [PubMed]
- Rietjens, I.M.; Tyrakowska, B.; Berg, S.J.P.L.V.D.; Soffers, A.E.M.F.; Punt, A. Matrix-derived combination effects influencing absorption, distribution, metabolism and excretion (ADME) of food-borne toxic compounds: Implications for risk assessment. Toxicol. Res. 2014, 4, 23–35. [Google Scholar] [CrossRef]
- IARC. Safrole. In IARC Monographs on the Evaluation of Carcinogenic Risk of Chemicals to Man; IARC: Geneva, Switzerland, 1972; Volume 10, pp. 169–174. [Google Scholar]
- Cohen, S.M.; Eisenbrand, G.; Fukushima, S.; Gooderham, N.J.; Guengerich, F.P.; Hecht, S.S.; Rietjens, I.M.C.M.; Harman, C.; Taylor, S.V. GRAS flavoring substances. Food Technol. 2020, 3, 45–65. [Google Scholar]
- Zhao, D.-H.; Ke, C.-L.; Liu-Dong, L.; Wang, X.-F.; Wang, Q.; Chang-Liang, K. Elimination kinetics of eugenol in grass carp in a simulated transportation setting. BMC Vet. Res. 2017, 13, 346. [Google Scholar] [CrossRef]
- Kamatou, G.P.; Vermaak, I.; Viljoen, A.M. Eugenol—From the Remote Maluku Islands to the International Market Place: A Review of a Remarkable and Versatile Molecule. Molecules 2012, 17, 6953–6981. [Google Scholar] [CrossRef]
- Priborsky, J.; Velisek, J. A Review of Three Commonly Used Fish Anesthetics. Rev. Fish. Sci. Aquac. 2018, 26, 417–442. [Google Scholar] [CrossRef]
- Tuckey, N.P.; Forster, M.E.; Gieseg, S.P. Effects of rested harvesting on muscle metabolite concentrations and K-values in Chinook salmon (Oncorhynchus tshawytscha) fillets during storage at 15 °C. J. Food Sci. 2010, 75, C459–C464. [Google Scholar] [CrossRef]
- Meinertz, J.R.; Schreier, T.M.; Porcher, S.T.; Smerud, J.R. Evaluation of a Method for Quantifying Eugenol Concentrations in the Fillet Tissue from Freshwater Fish Species. J. AOAC Int. 2016, 99, 558–564. [Google Scholar] [CrossRef]
- NTP USNTP. NTP Technical Report on the Toxicity Studies of Myristicin (CASRN 607-91-0) Administered by Gavage to F344/NTac Rats and B6C3F1/N Mice. Natl. Toxicol. Program Tech. Rep. Ser. 2019, 95, 1–65. [Google Scholar]
- The European Parliament and of the Council. Regulation (EC) No 1334/2008 of the European Parliament and of the Council of 16 December 2008 on flavourings and certain food ingredients with flavouring properties for use in and on foods and amending Council Regulation (EEC) No 1601/91, Regulations (EC) No 2232/96 and (EC) No 110/2008 and Directive 2000/13/EC. Off. J. Eur. Union 2008, L354, 1–207. [Google Scholar]
- Cao, X.; Xie, Q.; Zhang, S.; Xu, H.; Su, J.; Zhang, J.; Deng, C.; Song, G. Fabrication of functionalized magnetic microspheres based on monodispersed polystyrene for quantitation of allyl-benzodioxoles coupled with gas chromatography and mass spectrometry. J. Chromatogr. A 2019, 1607, 460402. [Google Scholar] [CrossRef] [PubMed]
- Ávila, M.; Zougagh, M.; Escarpa, A.; Ríos, A. Determination of alkenylbenzenes and related flavour compounds in food samples by on-column preconcentration-capillary liquid chromatography. J. Chromatogr. A 2009, 1216, 7179–7185. [Google Scholar] [CrossRef] [PubMed]
- López, V.; Gerique, J.; Langa, E.; Berzosa, C.; Valero, M.S.; Gómez-Rincón, C. Antihelmintic effects of nutmeg (Myristica fragans) on Anisakis simplex L3 larvae obtained from Micromesistius potassou. Res. Vet. Sci. 2015, 100, 148–152. [Google Scholar] [CrossRef] [PubMed]
- Chiu, S.; Wang, T.; Belski, M.; Abourashed, E.A. HPLC-Guided Isolation, Purification and Characterization of Phenylpropanoid and Phenolic Constituents of Nutmeg Kernel (Myristica fragrans). Nat. Prod. Commun. 2016, 11. [Google Scholar] [CrossRef]
- Dang, H.; Quirino, J. Analytical Separation of Carcinogenic and Genotoxic Alkenylbenzenes in Foods and Related Products (2010–2020). Toxins 2021, 13, 387. [Google Scholar] [CrossRef]
- Mihats, D.; Pilsbacher, L.; Gabernig, R.; Routil, M.; Gutternigg, M.; Laenger, R. Levels of estragole in fennel teas marketed in Austria and assessment of dietary exposure. Int. J. Food Sci. Nutr. 2016, 68, 569–576. [Google Scholar] [CrossRef]
- Rehm, C.; Penalvo, J.L.; Afshin, A.; Mozaffarian, D. Dietary Intake among US Adults, 1999-2012. JAMA 2016, 315, 2542–2553. [Google Scholar] [CrossRef]
- Somi, M.H.; Mousavi, S.M.; Naghashi, S.; Faramarzi, E.; Jafarabadi, M.A.; Ghojazade, M.; Majdi, A.; Alavi, S.A.N. Is there any relationship between food habits in the last two decades and gastric cancer in North-Western Iran? Asian Pac. J. Cancer Prev. 2015, 16, 283–290. [Google Scholar] [CrossRef]
- Rosi, A.; Paolella, G.; Biasini, B.; Scazzina, F.; Sinu Working Group on Nutritional Surveillance in Adolescents. Dietary habits of adolescents living in North America, Europe or Oceania: A review on fruit, vegetable and legume consumption, sodium intake, and adherence to the Mediterranean Diet. Nutr. Metab. Cardiovasc Dis. 2019, 29, 544–560. [Google Scholar] [CrossRef]
- Haufroid, V.; Lison, D. Mercapturic acids revisited as biomarkers of exposure to reactive chemicals in occupational toxicology: A minireview. Int. Arch. Occup. Environ. Health 2005, 78, 343–354. [Google Scholar] [CrossRef]
- Hartwig, A.; Arand, M.; Epe, B.; Guth, S.; Jahnke, G.; Lampen, A.; Martus, H.J.; Monien, B.; Rietjens, I.M.; Schmitz-Spanke, S.; et al. Mode of action-based risk assessment of genotoxic carcinogens. Arch Toxicol. 2020, 94, 1787–1877. [Google Scholar] [CrossRef]
- Clewell, H.J.; Tan, Y.M.; Campbell, J.L.; Andersen, M. Quantitative Interpretation of Human Biomonitoring Data. Toxicol. Appl. Pharmacol. 2008, 231, 122–133. [Google Scholar] [CrossRef] [PubMed]
- EFSA EFSASC. Scientific opinion on genotoxicity testing strategies applicable to food and feed safety assessment. EFSA J. 2011, 9, 2379. [Google Scholar]
- ICH. ICH S2 (R1) Guidance on Genotoxicity Testing and Data Interpretation for Pharmaceuticals Intended for Human Use. Step 4. ICH Harmonised Tripartite Guideline; Bibra Toxicology Advice & Consulting: Wallington, UK, 2011. [Google Scholar]
- The European Parliament and of the Council of the European Union. Regulation (EU) No 528/2012 of the European Parliament and of the Council of 22 May 2012 concerning the making available on the market and use of biocidal products. Off. J. Eur. Union 2012, L167, 1–123. [Google Scholar]
- The European Parliament and of the Council of the European Union. Regulation (EC) No 1107/2009 of the European Parliament and of the Council of 21 October 2009 concerning the placing of plant protection products on the market and repealing Council Directives 79/117/EEC and 91/414/EEC. Off. J. Eur. Union 2009, L309, 1–50. [Google Scholar]
- EC. Commission Communication in the framework of the implementation of Commission Regulation (EU) No 283/2013 of 1 March 2013 setting out the data requirements for active substances, in accordance with Regulation (EC) No 1107/2009 of the European Parliament and of the Council concerning the placing of plant protection products on the market. Off. J. Eur. Union 2013, C95, 1–20. [Google Scholar]
- OECD. OECD Test Guidelines for Chemicals. Available online: https://www.oecd.org/chemicalsafety/testing/oecdguidelinesforthetestingofchemicals.htm (accessed on 8 September 2021).
- Nestmann, E.R.; Douglas, G.R.; Kowbel, D.J.; Harrington, T.R. Solvent interactions with test compounds and recommendations for testing to avoid artifacts. Environ. Mutagen. 1985, 7, 163–170. [Google Scholar] [CrossRef] [PubMed]
- Gatehouse, D.; Haworth, S.; Cebula, T.; Gocke, E.; Kier, L.; Matsushima, T.; Melcion, C.; Nohmi, T.; Ohta, T.; Venitt, S.; et al. Recommendations for the performance of bacterial mutation assays. Mutat. Res. Mutagen. Relat. Subj. 1994, 312, 217–233. [Google Scholar] [CrossRef]
- Nesslany, F.; Zennouche, N.; Simar-Meintières, S.; Talahari, I.; Nkili-Mboui, E.-N.; Marzin, D. In vivo Comet assay on isolated kidney cells to distinguish genotoxic carcinogens from epigenetic carcinogens or cytotoxic compounds. Mutat. Res. Toxicol. Environ. Mutagen. 2007, 630, 28–41. [Google Scholar] [CrossRef] [PubMed]
- OECD. Test No. 474: Mammalian Erythrocyte Micronucleus Test; OECD Guidelines for the Testing of Chemicals, Section 4; OECD Publishing: Paris, France, 2016. [Google Scholar] [CrossRef]
- Herrmann, K.; Holzwarth, A.; Rime, S.; Fischer, B.C.; Kneuer, C. (Q)SAR tools for the prediction of mutagenic properties: Are they ready for application in pesticide regulation? Pest Manag. Sci. 2020, 76, 3316–3325. [Google Scholar] [CrossRef]
- Wislocki, P.G.; Miller, E.C.; Miller, J.A.; McCoy, E.C.; Rosenkranz, H.S. Carcinogenic and mutagenic activities of safrole, 1′-hydroxysafrole, and some known or possible metabolites. Cancer Res. 1977, 37, 1883–1891. [Google Scholar] [PubMed]
- Boberg, E.W.; Liem, A.; Miller, E.C.; Miller, J.A. Inhibition by pentachlorophenol of the initiating and promoting activities of 1′-hydroxysafrole for the formation of enzyme-altered foci and tumors in rat liver. Carcinogenesis 1987, 8, 531–539. [Google Scholar] [CrossRef]
- Groh, I.A.M.; Cartus, A.T.; Vallicotti, S.; Kajzar, J.; Merz, K.-H.; Schrenk, D.; Esselen, M. Genotoxic potential of methyleugenol and selected methyleugenol metabolites in cultured Chinese hamster V79 cells. Food Funct. 2012, 3, 428. [Google Scholar] [CrossRef] [PubMed]
- Randerath, K.; Haglund, R.E.; Phillips, D.H.; Reddy, M.V. 32P-post-labelling analysis of DNA adducts formed in the livers of animals treated with safrole, estragole and other naturally-occurring alkenylbenzenes. I. adult female CD-1 mice. Carcinogenesis 1984, 5, 1613–1622. [Google Scholar] [CrossRef]
- Daimon, H.; Sawada, S.; Asakura, S.; Sagami, F. Inhibition of sulfotransferase affecting in vivo genotoxicity and DNA adducts induced by safrole in rat liver. Teratog. Carcinog. Mutagen. 1997, 17, 327–337. [Google Scholar] [CrossRef]
- Borchert, P.; Wislocki, P.G.; Miller, J.A.; Miller, E.C. The metabolism of the naturally occurring hepatocarcinogen safrole to 1′-hydroxysafrole and the electrophilic reactivity of 1′-acetoxysafrole. Cancer Res. 1973, 33, 575–589. [Google Scholar] [PubMed]
- Schiestl, R.H.; Chan, W.-S.; Gietz, R.D.; Mehta, R.D.; Hastings, P. Safrole, eugenol and methyleugenol induce intrachromosomal recombination in yeast. Mutat. Res. Toxicol. 1989, 224, 427–436. [Google Scholar] [CrossRef]
- Mortelmans, K.; Haworth, S.; Lawlor, T.; Speck, W.; Tainer, B.; Zeiger, E. Salmonella mutagenicity tests: II. Results from the testing of 270 chemicals. Environ. Mutagen. 1986, 8, 1–119. [Google Scholar] [CrossRef]
- Herrmann, K.; Engst, W.; Meinl, W.; Florian, S.; Cartus, A.T.; Schrenk, D.; Appel, K.E.; Nolden, T.; Himmelbauer, H.; Glatt, H. Formation of hepatic DNA adducts by methyleugenol in mouse models: Drastic decrease by Sult1a1 knockout and strong increase by transgenic human SULT1A1/2. Carcinogenesis 2014, 35, 935–941. [Google Scholar] [CrossRef]
- Herrmann, K.; Engst, W.; Florian, S.; Lampen, A.; Meinl, W.; Glatt, H.R. The influence of the SULT1A status-wild-type, knockout or humanized-on the DNA adduct formation by methyleugenol in extrahepatic tissues of mice. Toxicol. Res. 2016, 5, 808–815. [Google Scholar] [CrossRef]
- Tan, K.H.; Nishida, R. Methyl Eugenol: Its Occurrence, Distribution, and Role in Nature, Especially in Relation to Insect Behavior and Pollination. J. Insect Sci. 2012, 12, 1–60. [Google Scholar] [CrossRef]
- Smith, B.; Cadby, P.; Leblanc, J.-C.; Setzer, R.W. Application of the margin of exposure (MoE) approach to substances in food that are genotoxic and carcinogenic: Example: Methyleugenol, CASRN: 93-15-2. Food Chem. Toxicol. 2010, 48, S89–S97. [Google Scholar] [CrossRef] [PubMed]
- Monien, B.H.; Schumacher, F.; Herrmann, K.; Glatt, H.; Turesky, R.J.; Chesné, C. Simultaneous Detection of Multiple DNA Adducts in Human Lung Samples by Isotope-Dilution UPLC-MS/MS. Anal. Chem. 2014, 87, 641–648. [Google Scholar] [CrossRef] [PubMed]
- Abdo, K.; Cunningham, M.; Snell, M.; Herbert, R.; Travlos, G.; Eldridge, S.; Bucher, J. 14-Week toxicity and cell proliferation of methyleugenol administered by gavage to F344 rats and B6C3F1 mice. Food Chem. Toxicol. 2001, 39, 303–316. [Google Scholar] [CrossRef]
- EFSA. Guidance on conducting repeated-dose 90-day oral toxicity study in rodents on whole food/feed. EFSA J. 2011, 9, 2438. [Google Scholar] [CrossRef]
- OECD. Test No. 407: Repeated Dose 28-day Oral Toxicity Study in Rodents. In OECD Guidelines for the Testing of Chemicals; Section 4; OECD Publishing: Paris, France, 2008. [Google Scholar]
- Sachse, B.; Meinl, W.; Sommer, Y.; Glatt, H.; Seidel, A.; Monien, B.H. Bioactivation of food genotoxicants 5-hydroxymethylfurfural and furfuryl alcohol by sulfotransferases from human, mouse and rat: A comparative study. Arch. Toxicol. 2014, 90, 137–148. [Google Scholar] [CrossRef] [PubMed]
| Safrole | Methyleugenol | Estragole (=Methylchavicol) | trans-Anethole | Myristicin | |
|---|---|---|---|---|---|
| CAS N° | 94-59-7 | 93-15-2 | 140-67-0 | 4180-23-8 | 607-91-0 |
| Structural formula | 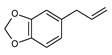 | 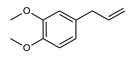 | 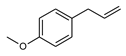 | 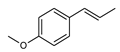 | 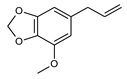 |
| IUPAC name | 5-prop-2-enyl-1,3-benzodioxole | 1,2-dimethoxy-4-prop-2-enylphenol | 1-methoxy-4-prop-2-enylbenzene | 1-methoxy-4-(E)-prop-1-enyl]benzene | 4-methoxy-6-prop-2-enyl-1,3-benzodioxole |
| Synonyms (select.) | 5-Allyl-1,3-benzodioxole Shikimole Safrene Sassafras Rhyuno oil | 4-Allyl-1,2-dimethoxybenzene 4-Allylveratrole Eugenol methyl ether Eugenyl methyl ether | 4-Allylanisole 1-Allyl-4-methoxybenzene p-Allylanisole Chavicol methyl ether Tarragon | (E)-Anethole p-Propenylanisole 4-Propenylanisole Anise camphor (E)-1-Methoxy-4-(prop-1-en-1-yl)benzene | 6-Allyl-4-methoxy-1,3-benzodioxole 5-Allyl-1-methoxy-2,3-(methylenedioxy) benzene Asaricin |
| Occurrence in essential oils (%) + (reference) | |||||
| Allspice berries | 62.7 [14] | ||||
| Allspice berries | 4–9 [15] | ||||
| Allspice berries | 8.8 [16] | ||||
| Anise seeds | 0.1–0.2 [17] | 1.44–7.08 [17] | 79.49–89.99 [17] | ||
| Anise seeds | 0.5–2.3 [18] | 76.9–93.7 [18] | |||
| Anise seeds | >90 [18] | ||||
| Chinese Star anise seeds | 0.5–5.5 [19,20] | 88.5–92 [19,21,22] | |||
| Japanese Star Anise seeds | 6.6 [23] | 9.8 [23] | 1.2 [23] | 3.5 [23] | |
| Sweet Fennel aerial parts | 2–3 [24] | 9.7–54.7 [24] | |||
| Sweet Fennel roots | 2.5–10 [24] | ||||
| Basil oil Ocimum basilicum leaves | 9.27–87.04 [25,26,27,28] | 0–81 [25,26,27,28] | |||
| Western tarragon | 0.51–28.87 [29,30] | 17.26–75 [30,31] | |||
| Eastern tarragon | no Safrole (but 21.45–38.90 Elemicin) [32] | 9.59–28.40 [32] | 0.29–0.31 [32] | ||
| Nutmeg kernel Eastern Indonesia | 1.6 (and 1.7 Elemicin) [33] | 16.7 (and 16.8. Methyl-iso-eugenol) [33] | 2.3 [33] | ||
| Nutmeg kernel Sri Lanka | 1.4 (and 2.1 Elemicin) [34] | 0.6 [34] | 4.9 [34] | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Eisenreich, A.; Götz, M.E.; Sachse, B.; Monien, B.H.; Herrmann, K.; Schäfer, B. Alkenylbenzenes in Foods: Aspects Impeding the Evaluation of Adverse Health Effects. Foods 2021, 10, 2139. https://doi.org/10.3390/foods10092139
Eisenreich A, Götz ME, Sachse B, Monien BH, Herrmann K, Schäfer B. Alkenylbenzenes in Foods: Aspects Impeding the Evaluation of Adverse Health Effects. Foods. 2021; 10(9):2139. https://doi.org/10.3390/foods10092139
Chicago/Turabian StyleEisenreich, Andreas, Mario E. Götz, Benjamin Sachse, Bernhard H. Monien, Kristin Herrmann, and Bernd Schäfer. 2021. "Alkenylbenzenes in Foods: Aspects Impeding the Evaluation of Adverse Health Effects" Foods 10, no. 9: 2139. https://doi.org/10.3390/foods10092139
APA StyleEisenreich, A., Götz, M. E., Sachse, B., Monien, B. H., Herrmann, K., & Schäfer, B. (2021). Alkenylbenzenes in Foods: Aspects Impeding the Evaluation of Adverse Health Effects. Foods, 10(9), 2139. https://doi.org/10.3390/foods10092139






