Utility of Photodynamic Therapy in Dentistry: Current Concepts
Abstract
1. Introduction, History of Photodynamic Therapy
2. The Theoretical Basis of PDT
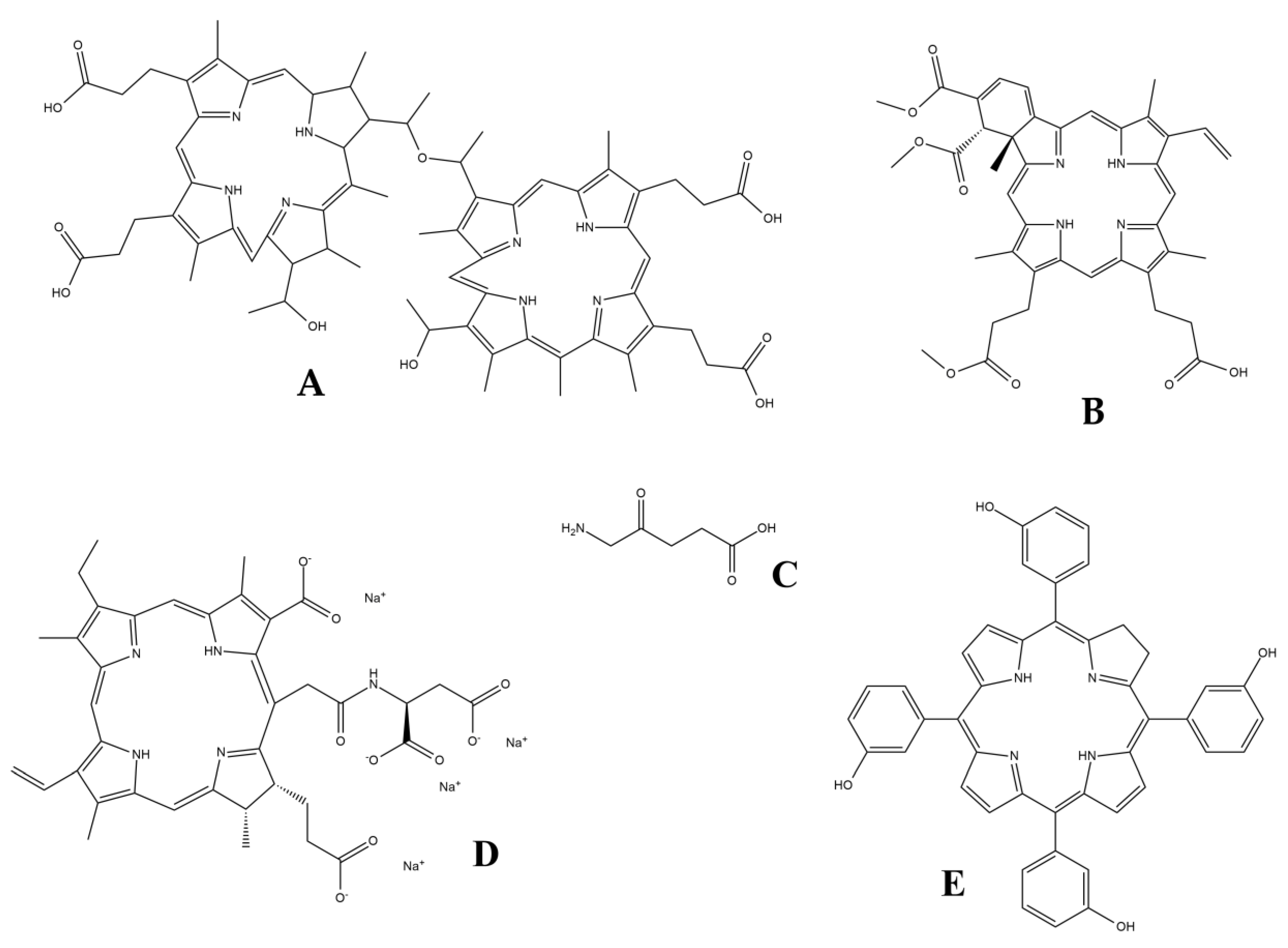
2.1. Photosensitizers (PS)
2.2. Light Source
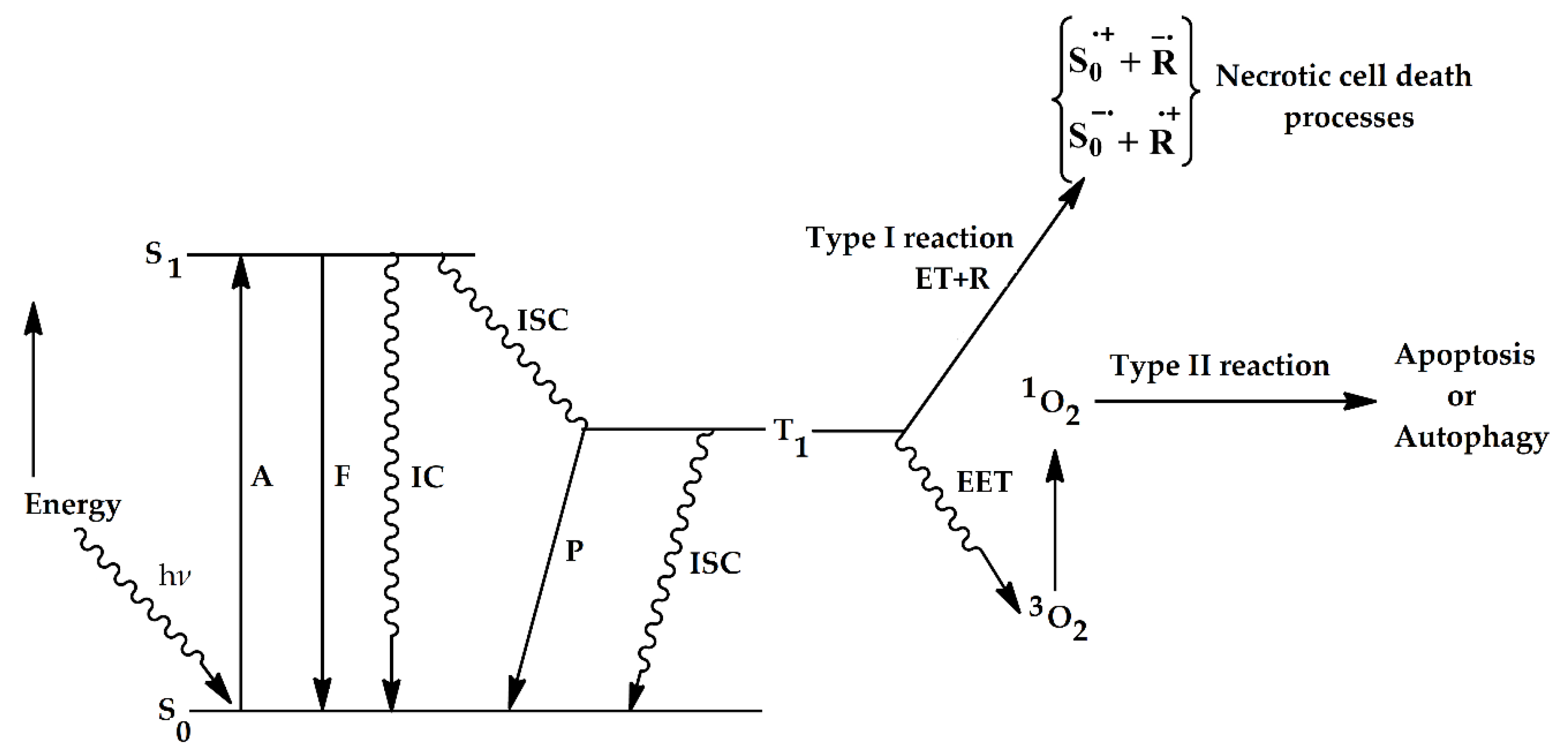
2.3. Role of Oxygen and Oxygen Species, Molecular Mechanisms of Action
3. Application of PDT in the Various Fields of Dentistry
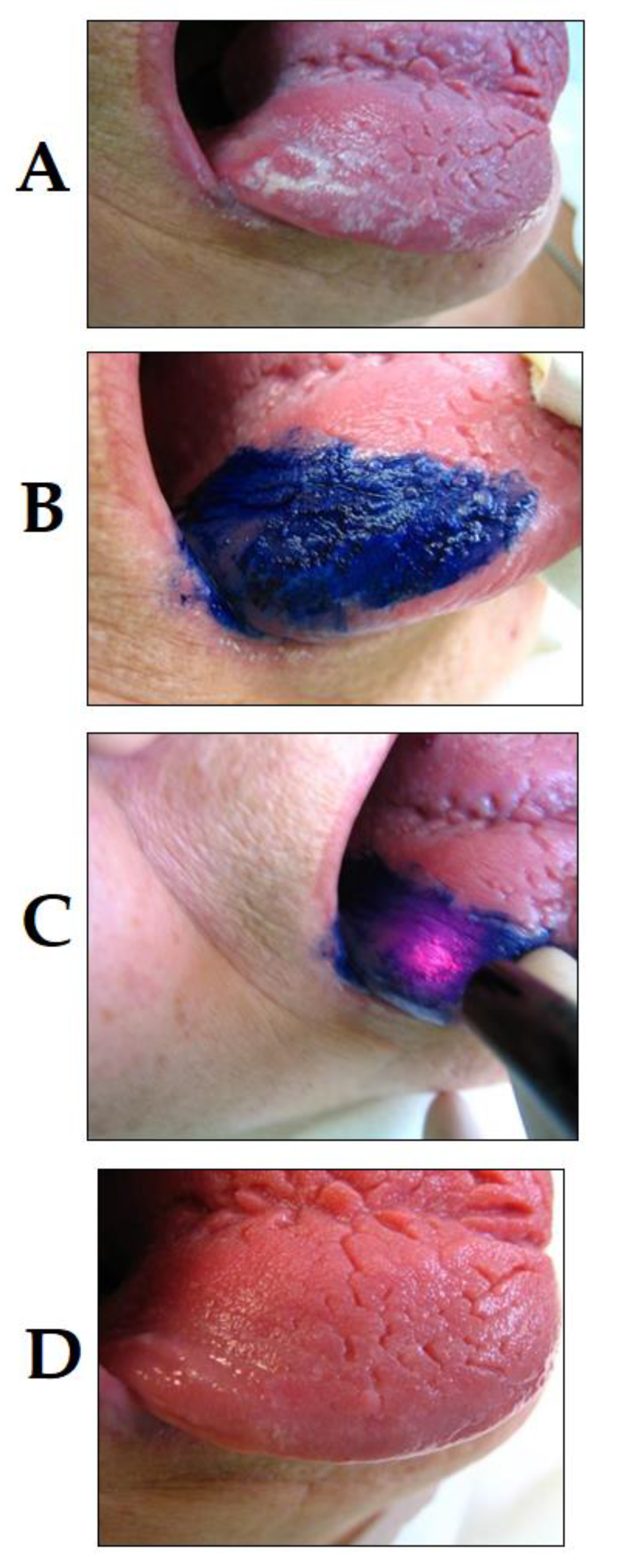
3.1. PDT in Oral and Maxillofacial Surgery, Oral Medicine and Oral Surgery
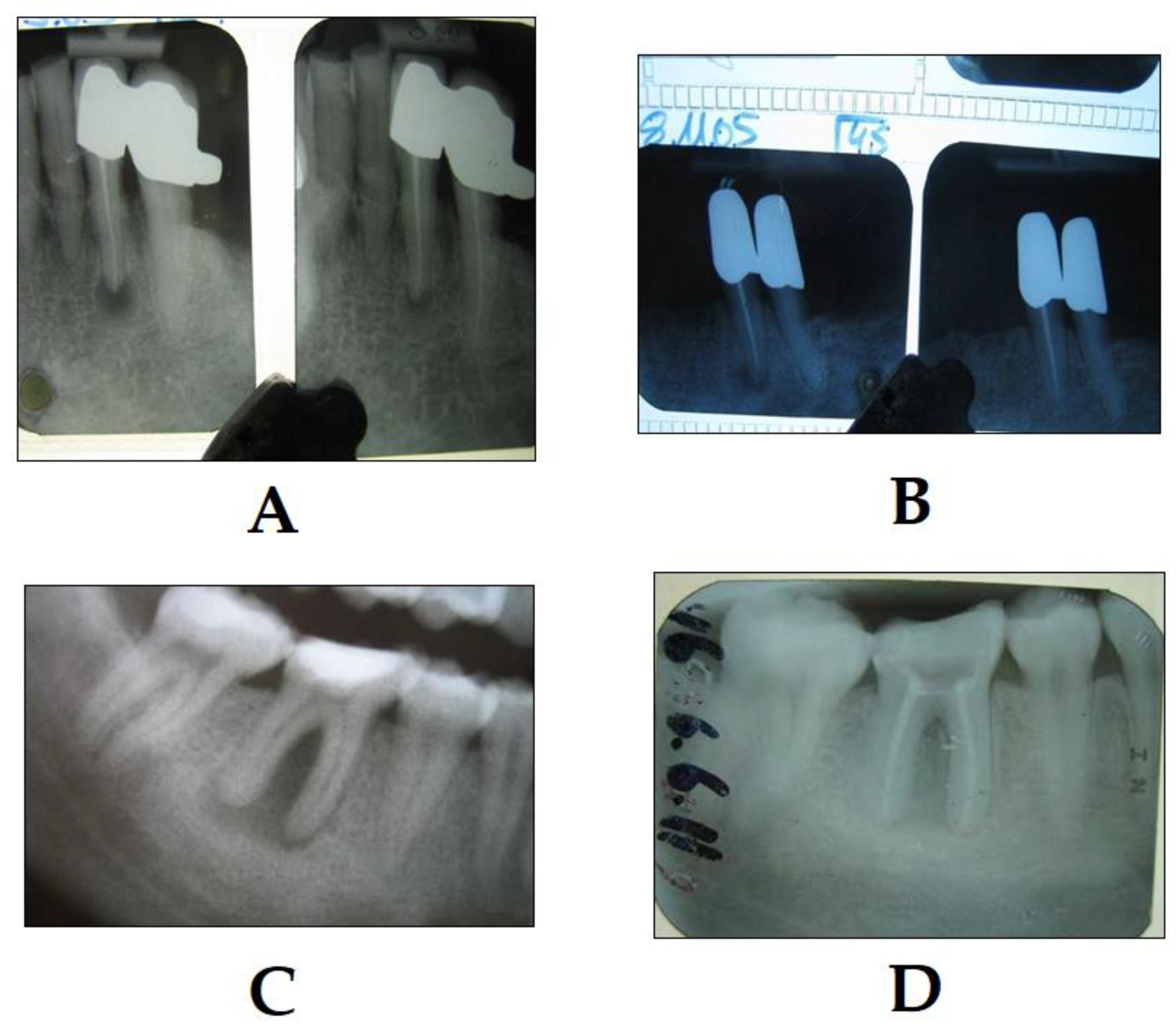
3.2. PDT in Endodontics
3.3. PDT in Preventive Dentistry
3.4. PDT in Periodontology
3.5. PDT in Implantology
4. Concluding Remarks
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Slavkin, H.C. Evolution of the scientific basis for dentistry and its impact on dental education: Past, present, and future. J. Dent. Educ. 2012, 76, 28–35. [Google Scholar]
- Polverini, P.J.; Krebsbach, P.H. Research and Discovery Science and the Future of Dental Education and Practice. J. Dent. Educ. 2017, 81, eS97–eS107. [Google Scholar] [CrossRef] [PubMed]
- Gutmann, J.L. The maturation of science within dentistry: The impact of critical milestones and visionary leaders on contemporary achievements. J. Hist. Dent. 2009, 57, 109–122. [Google Scholar] [PubMed]
- Issa, M.C.A.; Manela-Azulay, M. Photodynamic therapy: A review of the literature and image documentation. An. Bras. Dermatol. 2010, 85, 501–511. [Google Scholar] [CrossRef] [PubMed]
- Wan, M.T.; Lin, J.Y. Current evidence and applications of photodynamic therapy in dermatology. Clin. Cosmet. Investig. Dermatol. 2014, 7, 145–163. [Google Scholar] [PubMed]
- Abdel-kader, M.H. Chapter 1 The Journey of PDT Throughout History: PDT from Pharos to Present. In Photodynamic Medicine: From Bench to Clinic; Royal Society of Chemistry: London, UK, 2016; pp. 1–21. [Google Scholar]
- Kessel, D. Photodynamic Therapy: A Brief History. J. Clin. Med. 2019, 8, 1581. [Google Scholar] [CrossRef]
- Abd El-Kaream, S.A.; Abd Elsamie, G.H.; Abd-Alkareem, A.S. Sono-photodynamic modality for cancer treatment using bio-degradable bio-conjugated sonnelux nanocomposite in tumor-bearing mice: Activated cancer therapy using light and ultrasound. Biochem. Biophys. Res. Commun. 2018, 503, 1075–1086. [Google Scholar] [CrossRef]
- Abdel-Kader, M.H. (Ed.) Photodynamic Therapy: From Theory to Application; Springer-Verlag: Berlin/Heidelberg, Germany, 2014; ISBN 978-3-642-39628-1. [Google Scholar]
- Kato, H. History of photodynamic therapy--past, present and future. Cancer Chemother. 1996, 23, 8–15. [Google Scholar]
- Sotiriou, E.; Evangelou, G.; Papadavid, E.; Apalla, Z.; Vrani, F.; Vakirlis, E.; Panagiotou, M.; Stefanidou, M.; Pombou, T.; Krasagakis, K.; et al. Conventional vs. daylight photodynamic therapy for patients with actinic keratosis on face and scalp: 12-month follow-up results of a randomized, intra-individual comparative analysis. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 595–600. [Google Scholar] [CrossRef]
- Saleeby, C.W. The Advance of Heliotherapy. Available online: https://www.nature.com/articles/109663a0 (accessed on 26 March 2020).
- Møller, K.I.; Kongshoj, B.; Philipsen, P.A.; Thomsen, V.O.; Wulf, H.C. How Finsen’s light cured lupus vulgaris. Photodermatol. Photoimmunol. Photomed. 2005, 21, 118–124. [Google Scholar] [CrossRef]
- Grzybowski, A.; Pietrzak, K. From patient to discoverer--Niels Ryberg Finsen (1860–1904)—The founder of phototherapy in dermatology. Clin. Dermatol. 2012, 30, 451–455. [Google Scholar] [CrossRef] [PubMed]
- Gøtzsche, P. Niels Finsen’s treatment for lupus vulgaris. J. R. Soc. Med. 2011, 104, 41–42. [Google Scholar] [CrossRef]
- Sharma, S.K.; Mroz, P.; Dai, T.; Huang, Y.-Y.; Denis, T.G.S.; Hamblin, M.R. Photodynamic Therapy for Cancer and for Infections: What Is the Difference? Israel J. Chem. 2012, 52, 691–705. [Google Scholar] [CrossRef] [PubMed]
- Patrice, T.; Moan, J.; Peng, Q. An outline of the history of PDT. In Photodynamic Therapy; Royal Society of Chemistry: London, UK, 2003; pp. 1–18. [Google Scholar]
- Die Sensibilisierende Wirkung Fluoreszierender Substanzen—Hermann von Tappeiner (Buch)—jpc. Available online: https://www.jpc.de/jpcng/books/detail/-/art/hermann-von-tappeiner-die-sensibilisierende-wirkung-fluoreszierender-substanzen/hnum/6911897 (accessed on 26 March 2020).
- Szeimies, R.-M.; Dräger, J.; Abels, C.; Landthaler, M. Chapter 1 History of photodynamic therapy in dermatology. In Comprehensive Series in Photosciences; Calzavara-Pinton, P., Szeimies, R.-M., Ortel, B., Eds.; Photodynamic Therapy and Fluorescence Diagnosis in Dermatology; Elsevier: Amsterdam, The Netherlands, 2001; Volume 2, pp. 3–15. [Google Scholar]
- Sternberg, E.D.; Dolphin, D.; Brückner, C. Porphyrin-based photosensitizers for use in photodynamic therapy. Tetrahedron 1998, 54, 4151–4202. [Google Scholar] [CrossRef]
- Lipson, R.L.; Baldes, E.J. The photodynamic properties of a particular hematoporphyrin derivative. Arch. Dermatol. 1960, 82, 508–516. [Google Scholar] [CrossRef] [PubMed]
- Dougherty, T.J.; Gomer, C.J.; Henderson, B.W.; Jori, G.; Kessel, D.; Korbelik, M.; Moan, J.; Peng, Q. Photodynamic therapy. J. Natl. Cancer Inst. 1998, 90, 889–905. [Google Scholar] [CrossRef]
- Huang, Z. A Review of Progress in Clinical Photodynamic Therapy. Technol. Cancer Res. Treat 2005, 4, 283–293. [Google Scholar] [CrossRef]
- Toshima, K.; Tanimoto, S.; Tsumura, K.; Umezawa, K.; Takahashi, D. Target-selective degradation of cancer-related proteins by novel photosensitizers for molecular-targeted photodynamic therapy. Cancer Sci. 2009, 100, 1581–1584. [Google Scholar] [CrossRef]
- Chilakamarthi, U.; Giribabu, L. Photodynamic Therapy: Past, Present and Future. Chem. Rec. 2017, 17, 775–802. [Google Scholar] [CrossRef]
- Stokowski, L.A. Fundamentals of phototherapy for neonatal jaundice. Adv. Neonatal. Care 2011, 11, S10–S21. [Google Scholar] [CrossRef]
- Gursoy, H.; Ozcakir-Tomruk, C.; Tanalp, J.; Yilmaz, S. Photodynamic therapy in dentistry: A literature review. Clin. Oral Investig. 2013, 17, 1113–1125. [Google Scholar] [CrossRef] [PubMed]
- Malik, R.; Manocha, A.; Suresh, D.K. Photodynamic therapy—A strategic review. Indian J. Dent. Res. 2010, 21, 285–291. [Google Scholar] [CrossRef] [PubMed]
- Kou, J.; Dou, D.; Yang, L. Porphyrin photosensitizers in photodynamic therapy and its applications. Oncotarget 2017, 8, 81591–81603. [Google Scholar] [CrossRef] [PubMed]
- Kwiatkowski, S.; Knap, B.; Przystupski, D.; Saczko, J.; Kędzierska, E.; Knap-Czop, K.; Kotlińska, J.; Michel, O.; Kotowski, K.; Kulbacka, J. Photodynamic therapy—Mechanisms, photosensitizers and combinations. Biomed. Pharmacother. 2018, 106, 1098–1107. [Google Scholar] [CrossRef]
- Allison, R.R.; Downie, G.H.; Cuenca, R.; Hu, X.-H.; Childs, C.J.; Sibata, C.H. Photosensitizers in clinical PDT. Photodiagnosis Photodyn. Ther. 2004, 1, 27–42. [Google Scholar] [CrossRef]
- Detty, M.R.; Gibson, S.L.; Wagner, S.J. Current clinical and preclinical photosensitizers for use in photodynamic therapy. J. Med. Chem. 2004, 47, 3897–3915. [Google Scholar] [CrossRef] [PubMed]
- Lam, S. Photodynamic therapy of lung cancer. Semin. Oncol. 1994, 21, 15–19. [Google Scholar] [CrossRef]
- Kessel, D. More Adventures in Photodynamic Therapy. Int. J. Mol. Sci. 2015, 16, 15188–15193. [Google Scholar] [CrossRef]
- Rkein, A.M.; Ozog, D.M. Photodynamic therapy. Dermatol. Clin. 2014, 32, 415–425. [Google Scholar] [CrossRef]
- Josefsen, L.B.; Boyle, R.W. Photodynamic Therapy and the Development of Metal-Based Photosensitisers. Met. Based Drugs 2008, 2008. [Google Scholar] [CrossRef]
- Salva, K.A. Photodynamic therapy: Unapproved uses, dosages, or indications. Clin. Dermatol. 2002, 20, 571–581. [Google Scholar] [CrossRef]
- Huang, Y.-Y.; Sharma, S.K.; Yin, R.; Agrawal, T.; Chiang, L.Y.; Hamblin, M.R. Functionalized fullerenes in photodynamic therapy. J. Biomed. Nanotechnol. 2014, 10, 1918–1936. [Google Scholar] [CrossRef] [PubMed]
- Wachowska, M.; Muchowicz, A.; Firczuk, M.; Gabrysiak, M.; Winiarska, M.; Wańczyk, M.; Bojarczuk, K.; Golab, J. Aminolevulinic Acid (ALA) as a Prodrug in Photodynamic Therapy of Cancer. Molecules 2011, 16, 4140–4164. [Google Scholar] [CrossRef]
- Yang, X.; Palasuberniam, P.; Kraus, D.; Chen, B. Aminolevulinic Acid-Based Tumor Detection and Therapy: Molecular Mechanisms and Strategies for Enhancement. Int. J. Mol. Sci. 2015, 16, 25865–25880. [Google Scholar] [CrossRef]
- Abrahamse, H.; Hamblin, M.R. New photosensitizers for photodynamic therapy. Biochem. J. 2016, 473, 347–364. [Google Scholar] [CrossRef]
- Borgia, F.; Giuffrida, R.; Caradonna, E.; Vaccaro, M.; Guarneri, F.; Cannavò, S.P. Early and Late Onset Side Effects of Photodynamic Therapy. Biomedicines 2018, 6, 12. [Google Scholar] [CrossRef]
- Evans, H.H.; Horng, M.F.; Ricanati, M.; Deahl, J.T.; Oleinick, N.L. Mutagenicity of photodynamic therapy as compared to UVC and ionizing radiation in human and murine lymphoblast cell lines. Photochem. Photobiol. 1997, 66, 690–696. [Google Scholar] [CrossRef]
- Iwamoto, Y.; Mifuchi, I.; Yielding, L.W. Photodynamic mutagenic action of acridine compounds on yeast Saccharomyces cerevisiae. Mutat. Res. 1985, 158, 169–175. [Google Scholar] [CrossRef]
- Neugebauer, J.; Jozsa, M.; Kübler, A. Antimicrobial photodynamic therapy for prevention of alveolar ostitis and post-extraction pain. Mund. Kiefer Gesichtschir. 2004, 8, 350–355. [Google Scholar] [CrossRef]
- Biel, M.A. Photodynamic therapy in head and neck cancer. Curr. Oncol. Rep. 2002, 4, 87–96. [Google Scholar] [CrossRef]
- Grant, W.E.; Speight, P.M.; Hopper, C.; Bown, S.G. Photodynamic therapy: An effective, but non-selective treatment for superficial cancers of the oral cavity. Int. J. Cancer 1997, 71, 937–942. [Google Scholar] [CrossRef]
- Meisel, P.; Kocher, T. Photodynamic therapy for periodontal diseases: State of the art. J. Photochem. Photobiol. B, Biol. 2005, 79, 159–170. [Google Scholar] [CrossRef]
- Yilmaz, A.; Ozkiraz, S.; Akcan, A.B.; Canpolat, M. Low-cost Home-use Light-emitting-diode Phototherapy as an alternative to Conventional Methods. J. Trop. Pediatr. 2015, 61, 113–118. [Google Scholar] [CrossRef] [PubMed]
- Clarkson, D.M. Hazards of non coherent light sources as determined by the framework of IEC TR-60825-9. J. Med. Eng. Technol. 2004, 28, 125–131. [Google Scholar] [CrossRef] [PubMed]
- Reeds, K.B.; Ridgway, T.D.; Higbee, R.G.; Lucroy, M.D. Non-coherent light for photodynamic therapy of superficial tumours in animals. Vet. Comp. Oncol. 2004, 2, 157–163. [Google Scholar] [CrossRef] [PubMed]
- Epstein, J.H. UV-A: Biological Effects of Ultraviolet Radiation with Emphasis on Human Responses to Longwave Ultraviolet. Arch. Dermatol. 1979, 115, 648. [Google Scholar] [CrossRef]
- Ohshiro, T. New classification for single-system light treatment. Laser Ther. 2011, 20, 11–15. [Google Scholar] [CrossRef][Green Version]
- Cieplik, F.; Deng, D.; Crielaard, W.; Buchalla, W.; Hellwig, E.; Al-Ahmad, A.; Maisch, T. Antimicrobial photodynamic therapy - what we know and what we don’t. Crit. Rev. Microbiol. 2018, 44, 571–589. [Google Scholar] [CrossRef]
- Foster, T.H.; Murant, R.S.; Bryant, R.G.; Knox, R.S.; Gibson, S.L.; Hilf, R. Oxygen Consumption and Diffusion Effects in Photodynamic Therapy. Radiat. Res. 1991, 126, 296–303. [Google Scholar] [CrossRef]
- Konopka, K.; Goslinski, T. Photodynamic therapy in dentistry. J. Dent. Res. 2007, 86, 694–707. [Google Scholar] [CrossRef]
- Sitnik, T.M.; Hampton, J.A.; Henderson, B.W. Reduction of tumour oxygenation during and after photodynamic therapy in vivo: Effects of fluence rate. Br. J. Cancer 1998, 77, 1386–1394. [Google Scholar] [CrossRef] [PubMed]
- Daicoviciu, D.; Filip, A.; Ion, R.M.; Clichici, S.; Decea, N.; Muresan, A. Oxidative photodamage induced by photodynamic therapy with methoxyphenyl porphyrin derivatives in tumour-bearing rats. Folia Biol. (Praha) 2011, 57, 12–19. [Google Scholar] [PubMed]
- Romiszewska, A.; Nowak-Stępniowska, A. Photodynamic reaction and oxidative stress - influence of the photodynamic effect on the activity antioxidant enzymes. Postepy Biochem. 2014, 60, 355–364. [Google Scholar] [PubMed]
- Foote, C.S. Definition of type I and type II photosensitized oxidation. Photochem. Photobiol. 1991, 54, 659. [Google Scholar] [CrossRef] [PubMed]
- Baptista, M.S.; Cadet, J.; Di Mascio, P.; Ghogare, A.A.; Greer, A.; Hamblin, M.R.; Lorente, C.; Nunez, S.C.; Ribeiro, M.S.; Thomas, A.H.; et al. Type I and Type II Photosensitized Oxidation Reactions: Guidelines and Mechanistic Pathways. Photochem. Photobiol. 2017, 93, 912–919. [Google Scholar] [CrossRef]
- Castano, A.P.; Demidova, T.N.; Hamblin, M.R. Mechanisms in photodynamic therapy: Part two-cellular signaling, cell metabolism and modes of cell death. Photodiagnosis Photodyn. Ther. 2005, 2, 1–23. [Google Scholar] [CrossRef]
- Mallidi, S.; Anbil, S.; Lee, S.; Manstein, D.; Elrington, S.; Kositratna, G.; Schoenfeld, D.; Pogue, B.; Davis, S.J.; Hasan, T. Photosensitizer fluorescence and singlet oxygen luminescence as dosimetric predictors of topical 5-aminolevulinic acid photodynamic therapy induced clinical erythema. J. Biomed. Opt. 2014, 19, 028001. [Google Scholar] [CrossRef]
- Asgary, S.; Roghanizadeh, L. Partial Necrosis Consequence of the Infection Spreading from an Adjacent Apical Periodontitis: A Case Report. Iran Endod. J. 2018, 13, 420–423. [Google Scholar]
- Mroz, P.; Yaroslavsky, A.; Kharkwal, G.B.; Hamblin, M.R. Cell Death Pathways in Photodynamic Therapy of Cancer. Cancers 2011, 3, 2516–2539. [Google Scholar] [CrossRef]
- Kessel, D.; Reiners, J.J. Apoptosis and autophagy after mitochondrial or endoplasmic reticulum photodamage. Photochem. Photobiol. 2007, 83, 1024–1028. [Google Scholar] [CrossRef] [PubMed]
- Nishikawa, S.; Sasaki, F. Apoptosis of Dental Pulp Cells and Their Elimination by Macrophages and MHC Class II-expressing Dendritic Cells. J. Histochem. Cytochem. 1999, 47, 303–311. [Google Scholar] [CrossRef]
- Misra, A.; Rai, S.; Misra, D. Functional role of apoptosis in oral diseases: An update. J. Oral Maxillofac. Pathol. 2016, 20, 491–496. [Google Scholar] [CrossRef] [PubMed]
- de Bruijn, H.S.; Meijers, C.; van der Ploeg-van den Heuvel, A.; Sterenborg, H.J.C.M.; Robinson, D.J. Microscopic localisation of protoporphyrin IX in normal mouse skin after topical application of 5-aminolevulinic acid or methyl 5-aminolevulinate. J. Photochem. Photobiol. B Biol. 2008, 92, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Sharwani, A.; Jerjes, W.; Salih, V.; MacRobert, A.J.; El-Maaytah, M.; Khalil, H.S.M.; Hopper, C. Fluorescence spectroscopy combined with 5-aminolevulinic acid-induced protoporphyrin IX fluorescence in detecting oral premalignancy. J. Photochem. Photobiol. B Biol. 2006, 83, 27–33. [Google Scholar] [CrossRef] [PubMed]
- Bekelis, K.; Valdés, P.A.; Erkmen, K.; Leblond, F.; Kim, A.; Wilson, B.C.; Harris, B.T.; Paulsen, K.D.; Roberts, D.W. Quantitative and qualitative 5-aminolevulinic acid-induced protoporphyrin IX fluorescence in skull base meningiomas. Neurosurg. Focus 2011, 30, E8. [Google Scholar] [CrossRef]
- Sharma, P.; Wadhwan, V.; Aggarwal, P.; Sharma, A. Oral verrucous hyperplasia versus oral verrucous carcinoma: A clinicopathologic dilemma revisited using p53 as immunohistochemical marker. J. Oral Maxillofac. Pathol. 2016, 20, 362–368. [Google Scholar] [CrossRef]
- Chang, Y.-C.; Yu, C.-H. Successful treatment of a large oral verrucous hyperplasia with photodynamic therapy combined with cryotherapy. J. Dent. Sci. 2013, 8, 87–90. [Google Scholar] [CrossRef]
- Philipp-Dormston, W.G. Photodynamic therapy for aesthetic-cosmetic indications. Soc. Ital. Dermatol. Venereol 2018, 153, 817–826. [Google Scholar] [CrossRef]
- Tampa, M.; Sarbu, M.-I.; Matei, C.; Mitran, C.-I.; Mitran, M.-I.; Caruntu, C.; Constantin, C.; Neagu, M.; Georgescu, S.-R. Photodynamic therapy: A hot topic in dermato-oncology (Review). Oncol. Lett. 2019, 17, 4085–4093. [Google Scholar] [CrossRef]
- Dilkes, M.G.; DeJode, M.L.; Rowntree-Taylor, A.; McGilligan, J.A.; Kenyon, G.S.; McKelvie, P. m-THPC photodynamic therapy for head and neck cancer. Laser Med. Sci. 1996, 11, 23–29. [Google Scholar] [CrossRef]
- Dilkes, M.G.; DeJode, M.L.; Gardiner, Q.; Kenyon, G.S.; McKelvie, P. Treatment of head and neck cancer with photodynamic therapy: Results after one year. J. Laryngol. Otol. 1995, 109, 1072–1076. [Google Scholar] [CrossRef]
- Kübler, A.C.; de Carpentier, J.; Hopper, C.; Leonard, A.G.; Putnam, G. Treatment of squamous cell carcinoma of the lip using Foscan-mediated photodynamic therapy. Int. J. Oral Maxillofac. Surg. 2001, 30, 504–509. [Google Scholar] [CrossRef] [PubMed]
- Rautemaa, R.; Lauhio, A.; Cullinan, M.P.; Seymour, G.J. Oral infections and systemic disease—An emerging problem in medicine. Clin. Microbiol. Infect. 2007, 13, 1041–1047. [Google Scholar] [CrossRef] [PubMed]
- Stájer, A.; Ibrahim, B.; Gajdács, M.; Urbán, E.; Baráth, Z. Diagnosis and Management of Cervicofacial Actinomycosis: Lessons from Two Distinct Clinical Cases. Antibiotics 2020, 9, 139. [Google Scholar] [CrossRef] [PubMed]
- Gajdács, M.; Urbán, E.; Terhes, G. Microbiological and Clinical Aspects of Cervicofacial Actinomyces Infections: An Overview. Dent. J. 2019, 7, 85. [Google Scholar] [CrossRef] [PubMed]
- Komerik, N.; MacRobert, A.J. Photodynamic therapy as an alternative antimicrobial modality for oral infections. J. Environ. Pathol. Toxicol. Oncol. 2006, 25, 487–504. [Google Scholar] [PubMed]
- Singh, A.; Verma, R.; Murari, A.; Agrawal, A. Oral candidiasis: An overview. J. Oral Maxillofac. Pathol. 2014, 18, S81–S85. [Google Scholar]
- Akpan, A.; Morgan, R. Oral candidiasis. Postgrad. Med. J. 2002, 78, 455–459. [Google Scholar] [CrossRef]
- Bliss, J.M.; Bigelow, C.E.; Foster, T.H.; Haidaris, C.G. Susceptibility of Candida species to photodynamic effects of photofrin. Antimicrob. Agents Chemother. 2004, 48, 2000–2006. [Google Scholar] [CrossRef]
- Freire, F.; Ferraresi, C.; Jorge, A.O.C.; Hamblin, M.R. Photodynamic therapy of oral Candida infection in a mouse model. J. Photochem. Photobiol. B Biol. 2016, 159, 161–168. [Google Scholar] [CrossRef]
- Lotufo, M.A.; Tempestini Horliana, A.C.R.; Santana, T.; de Queiroz, A.C.; Gomes, A.O.; Motta, L.J.; Ferrari, R.A.M.; dos Santos Fernandes, K.P.; Bussadori, S.K. Efficacy of photodynamic therapy on the treatment of herpes labialis: A systematic review. Photodiagnosis Photodyn. Therapy 2020, 29, 101536. [Google Scholar] [CrossRef]
- Marotti, J.; Aranha, A.C.C.; Eduardo, C.D.P.; Ribeiro, M.S. Photodynamic Therapy Can Be Effective as a Treatment for Herpes Simplex Labialis. Photomed. Laser Surg. 2009, 27, 357–363. [Google Scholar] [CrossRef]
- Saini, R.; Lee, N.V.; Liu, K.Y.P.; Poh, C.F. Prospects in the Application of Photodynamic Therapy in Oral Cancer and Premalignant Lesions. Cancers 2016, 8, 83. [Google Scholar] [CrossRef] [PubMed]
- Persoon, I.F.; Özok, A.R. Definitions and Epidemiology of Endodontic Infections. Curr. Oral Health Rep. 2017, 4, 278–285. [Google Scholar] [CrossRef]
- Li, C.; Cui, Y.; Zhou, C.; Sun, J.; Zhou, X. Epigenetics in Odontogenesis and its Influences. Curr. Stem. Cell Res. Ther. 2018, 13, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Trindade, A.C.; De Figueiredo, J.A.P.; Steier, L.; Weber, J.B.B. Photodynamic therapy in endodontics: A literature review. Photomed. Laser Surg. 2015, 33, 175–182. [Google Scholar] [CrossRef]
- Okamoto, C.B.; Motta, L.J.; Prates, R.A.; da Mota, A.C.C.; Gonçalves, M.L.L.; Horliana, A.C.R.T.; Mesquita Ferrari, R.A.; Fernandes, K.P.S.; Bussadori, S.K. Antimicrobial Photodynamic Therapy as a Co-adjuvant in Endodontic Treatment of Deciduous Teeth: Case Series. Photochem. Photobiol. 2018, 94, 760–764. [Google Scholar] [CrossRef]
- Demidova, T.N.; Hamblin, M.R. Effect of Cell-Photosensitizer Binding and Cell Density on Microbial Photoinactivation. Antimicrob. Agents Chemother. 2005, 49, 2329–2335. [Google Scholar] [CrossRef]
- Gajdács, M.; Albericio, F. Antibiotic Resistance: From the Bench to Patients. Antibiotics 2019, 8, 129. [Google Scholar] [CrossRef]
- Fimple, J.L.; Fontana, C.R.; Foschi, F.; Ruggiero, K.; Song, X.; Pagonis, T.C.; Tanner, A.C.R.; Kent, R.; Doukas, A.G.; Stashenko, P.P.; et al. Photodynamic treatment of endodontic polymicrobial infection in vitro. J. Endod. 2008, 34, 728–734. [Google Scholar] [CrossRef]
- Gajdács, M.; Spengler, G.; Urbán, E. Identification and Antimicrobial Susceptibility Testing of Anaerobic Bacteria: Rubik’s Cube of Clinical Microbiology? Antibiotics 2017, 6, 25. [Google Scholar] [CrossRef] [PubMed]
- Petersen, J.; Glaßl, E.-M.; Nasseri, P.; Crismani, A.; Luger, A.K.; Schoenherr, E.; Bertl, K.; Glodny, B. The association of chronic apical periodontitis and endodontic therapy with atherosclerosis. Clin. Oral Investig. 2014, 18, 1813–1823. [Google Scholar] [CrossRef] [PubMed]
- Meimandi, M.; Talebi Ardakani, M.R.; Esmaeil Nejad, A.; Yousefnejad, P.; Saebi, K.; Tayeed, M.H. The Effect of Photodynamic Therapy in the Treatment of Chronic Periodontitis: A Review of Literature. J. Lasers Med. Sci. 2017, 8, S7–S11. [Google Scholar] [CrossRef]
- Garcez, A.S.; Nuñez, S.C.; Hamblin, M.R.; Ribeiro, M.S. Antimicrobial effects of photodynamic therapy on patients with necrotic pulps and periapical lesion. J. Endod. 2008, 34, 138–142. [Google Scholar] [CrossRef]
- Aas, J.A.; Griffen, A.L.; Dardis, S.R.; Lee, A.M.; Olsen, I.; Dewhirst, F.E.; Leys, E.J.; Paster, B.J. Bacteria of Dental Caries in Primary and Permanent Teeth in Children and Young Adults. J. Clin. Microbiol. 2008, 46, 1407–1417. [Google Scholar] [CrossRef]
- Faragó, I.; Nagy, G.; Márton, S.; Túry, F.; Szabó, E.; Hopcraft, M.; Madléna, M. Dental caries experience in a Hungarian police student population. Caries Res. 2012, 46, 95–101. [Google Scholar] [CrossRef]
- Stájer, A.; Urban, E.; Mihalik, E.; Rakonczay, Z.; Nagy, E.; Fazekas, A.; Turzó, K.; Radnai, M.; Nagy, K. Streptococcus mutans colonization on titanium surfaces treated with various fluoride-containing preventive solutions. Fogorv. Szle. 2009, 102, 117–122. [Google Scholar]
- Barrak, I.; Urbán, E.; Turzó, K.; Nagy, K.; Braunitzer, G.; Stájer, A. Short- and Long-Term Influence of Fluoride-Containing Prophylactics on the Growth of Streptococcus mutans on Titanium Surface. Implant Dent. 2015, 24, 675–679. [Google Scholar] [CrossRef][Green Version]
- Stájer, A.; Urbán, E.; Pelsõczi, I.K.; Mihalik, E.; Rakonczay, Z.; Nagy, K.; Turzó, K.; Radnai, M. Effect of caries preventive products on the growth of bacterial biofilm on titanium surface. Acta Microbiol. Immunol. Hung. 2012, 59, 51–61. [Google Scholar] [CrossRef]
- Ricatto, L.G.O.; Conrado, L.A.L.; Turssi, C.P.; França, F.M.G.; Basting, R.T.; Amaral, F.L.B. Comparative evaluation of photodynamic therapy using LASER or light emitting diode on cariogenic bacteria: An in vitro study. Eur. J. Dent. 2014, 8, 509–514. [Google Scholar] [CrossRef]
- Almeida, A. Photodynamic Therapy in the Inactivation of Microorganisms. Antibiotics 2020, 9, 138. [Google Scholar] [CrossRef]
- Bevilacqua, I.M.; Nicolau, R.A.; Khouri, S.; Brugnera, A.; Teodoro, G.R.; Zângaro, R.A.; Pacheco, M.T.T. The impact of photodynamic therapy on the viability of Streptococcus mutans in a planktonic culture. Photomed. Laser Surg. 2007, 25, 513–518. [Google Scholar] [CrossRef]
- Wilson, M. Bactericidal effect of laser light and its potential use in the treatment of plaque-related diseases. Int. Dent. J. 1994, 44, 181–189. [Google Scholar]
- Wilson, M. Lethal photosensitisation of oral bacteria and its potential application in the photodynamic therapy of oral infections. Photochem. Photobiol. Sci. 2004, 3, 412–418. [Google Scholar] [CrossRef]
- Gaynes, R. The Discovery of Penicillin—New Insights after More Than 75 Years of Clinical Use. Emerg. Infect. Dis. 2017, 23, 849–853. [Google Scholar] [CrossRef]
- Gajdács, M. The Concept of an Ideal Antibiotic: Implications for Drug Design. Molecules 2019, 24, 892. [Google Scholar] [CrossRef]
- How, K.Y.; Song, K.P.; Chan, K.G. Porphyromonas gingivalis: An Overview of Periodontopathic Pathogen below the Gum Line. Front. Microbiol. 2016, 7, 53. [Google Scholar] [CrossRef]
- Huang, L.; Xuan, Y.; Koide, Y.; Zhiyentayev, T.; Tanaka, M.; Hamblin, M.R. Type I and Type II mechanisms of antimicrobial photodynamic therapy: An in vitro study on Gram-negative and Gram-positive bacteria. Lasers Surg. Med. 2012, 44, 490–499. [Google Scholar] [CrossRef]
- Memar, M.Y.; Ghotaslou, R.; Samiei, M.; Adibkia, K. Antimicrobial use of reactive oxygen therapy: Current insights. Infect. Drug Resist. 2018, 11, 567–576. [Google Scholar] [CrossRef]
- Di Stasio, D.; Romano, A.; Gentile, C.; Maio, C.; Lucchese, A.; Serpico, R.; Paparella, R.; Minervini, G.; Candotto, V.; Laino, L. Systemic and topical photodynamic therapy (PDT) on oral mucosa lesions: An overview. J. Biol. Regul. Homeost. Agents 2018, 32, 123–126. [Google Scholar]
- Kumar, V.; Sinha, J.; Verma, N.; Nayan, K.; Saimbi, C.S.; Tripathi, A.K. Scope of photodynamic therapy in periodontics. Indian J. Dent. Res. 2015, 26, 439–442. [Google Scholar] [CrossRef]
- Andersen, R.; Loebel, N.; Hammond, D.; Wilson, M. Treatment of periodontal disease by photodisinfection compared to scaling and root planing. J. Clin. Dent. 2007, 18, 34–38. [Google Scholar]
- Braun, A.; Dehn, C.; Krause, F.; Jepsen, S. Short-term clinical effects of adjunctive antimicrobial photodynamic therapy in periodontal treatment: A randomized clinical trial. J. Clin. Periodontol. 2008, 35, 877–884. [Google Scholar] [CrossRef]
- Raghavendra, M.; Koregol, A.; Bhola, S. Photodynamic therapy: A targeted therapy in periodontics. Aust. Dent. J. 2009, 54 (Suppl. 1), S102–S109. [Google Scholar] [CrossRef]
- De Oliveira, R.R.; Schwartz-Filho, H.O.; Novaes, A.B.; Taba, M. Antimicrobial photodynamic therapy in the non-surgical treatment of aggressive periodontitis: A preliminary randomized controlled clinical study. J. Periodontol. 2007, 78, 965–973. [Google Scholar] [CrossRef]
- Khammissa, R.A.G.; Feller, L.; Meyerov, R.; Lemmer, J. Peri-implant mucositis and peri-implantitis: Bacterial infection. SADJ 2012, 67, 70, 72–74. [Google Scholar]
- Prathapachandran, J.; Suresh, N. Management of peri-implantitis. Dent. Res. J. (Isfahan) 2012, 9, 516–521. [Google Scholar] [CrossRef]
- Dörtbudak, O.; Haas, R.; Bernhart, T.; Mailath-Pokorny, G. Lethal photosensitization for decontamination of implant surfaces in the treatment of peri-implantitis. Clin. Oral Implants Res. 2001, 12, 104–108. [Google Scholar] [CrossRef]
- Sivaramakrishnan, G.; Sridharan, K. Photodynamic therapy for the treatment of peri-implant diseases: A network meta-analysis of randomized controlled trials. Photodiagnosis Photodyn. Ther. 2018, 21, 1–9. [Google Scholar] [CrossRef]
- Esposito, M.; Grusovin, M.G.; De Angelis, N.; Camurati, A.; Campailla, M.; Felice, P. The adjunctive use of light-activated disinfection (LAD) with FotoSan is ineffective in the treatment of peri-implantitis: 1-year results from a multicentre pragmatic randomised controlled trial. Eur. J. Oral. Implantol. 2013, 6, 109–119. [Google Scholar]

© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stájer, A.; Kajári, S.; Gajdács, M.; Musah-Eroje, A.; Baráth, Z. Utility of Photodynamic Therapy in Dentistry: Current Concepts. Dent. J. 2020, 8, 43. https://doi.org/10.3390/dj8020043
Stájer A, Kajári S, Gajdács M, Musah-Eroje A, Baráth Z. Utility of Photodynamic Therapy in Dentistry: Current Concepts. Dentistry Journal. 2020; 8(2):43. https://doi.org/10.3390/dj8020043
Chicago/Turabian StyleStájer, Anette, Szilvia Kajári, Márió Gajdács, Aima Musah-Eroje, and Zoltán Baráth. 2020. "Utility of Photodynamic Therapy in Dentistry: Current Concepts" Dentistry Journal 8, no. 2: 43. https://doi.org/10.3390/dj8020043
APA StyleStájer, A., Kajári, S., Gajdács, M., Musah-Eroje, A., & Baráth, Z. (2020). Utility of Photodynamic Therapy in Dentistry: Current Concepts. Dentistry Journal, 8(2), 43. https://doi.org/10.3390/dj8020043






