Comparison of MTA versus Biodentine in Apexification Procedure for Nonvital Immature First Permanent Molars: A Randomized Clinical Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Ethical Approval and Protocol Registration
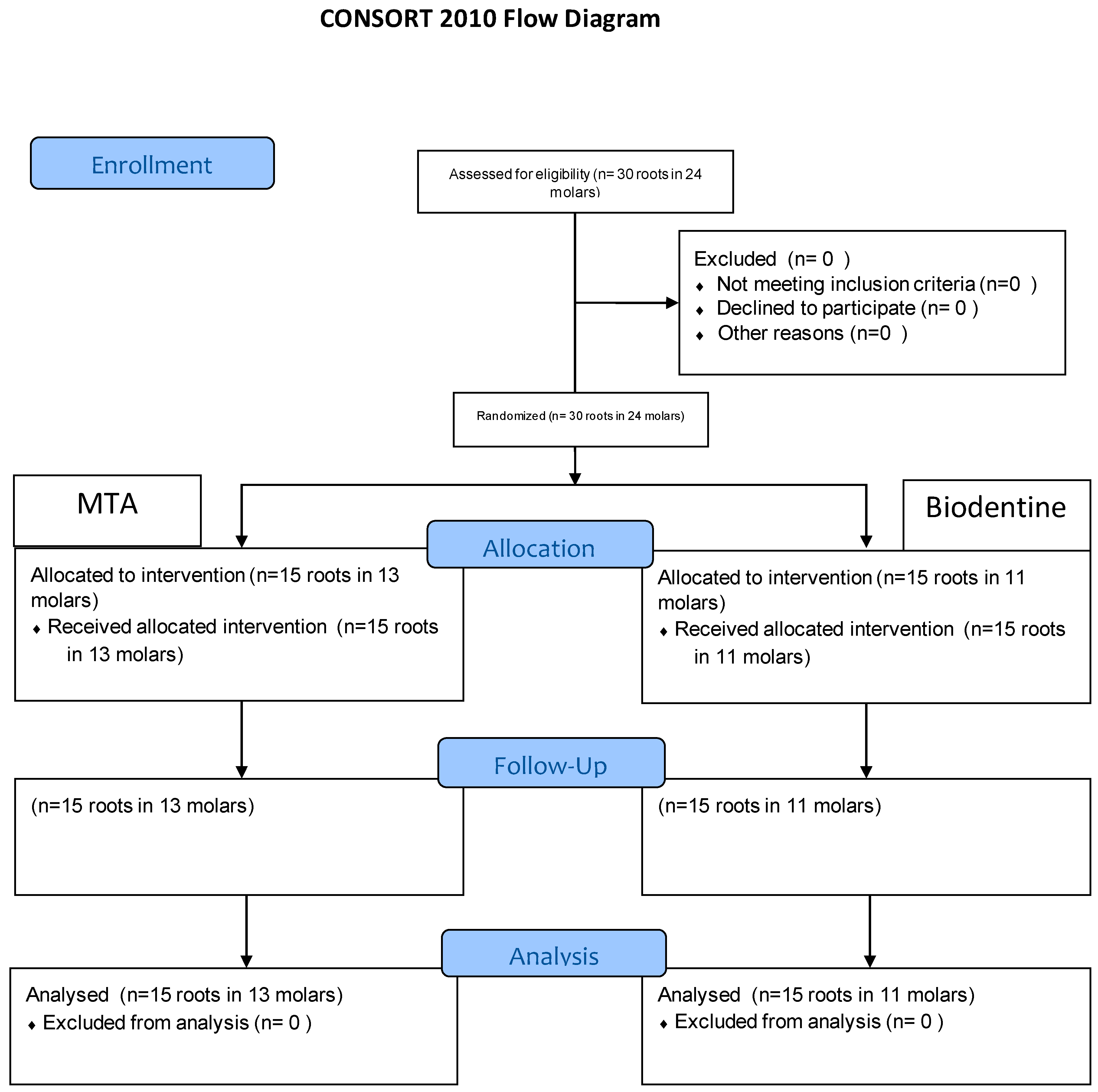
2.2. Study Design and Settings
2.3. Recruitment and Eligibility Criteria
2.4. Sample Size Calculation
2.5. Random Sequence Generation and Allocation Concealment
2.6. Blinding
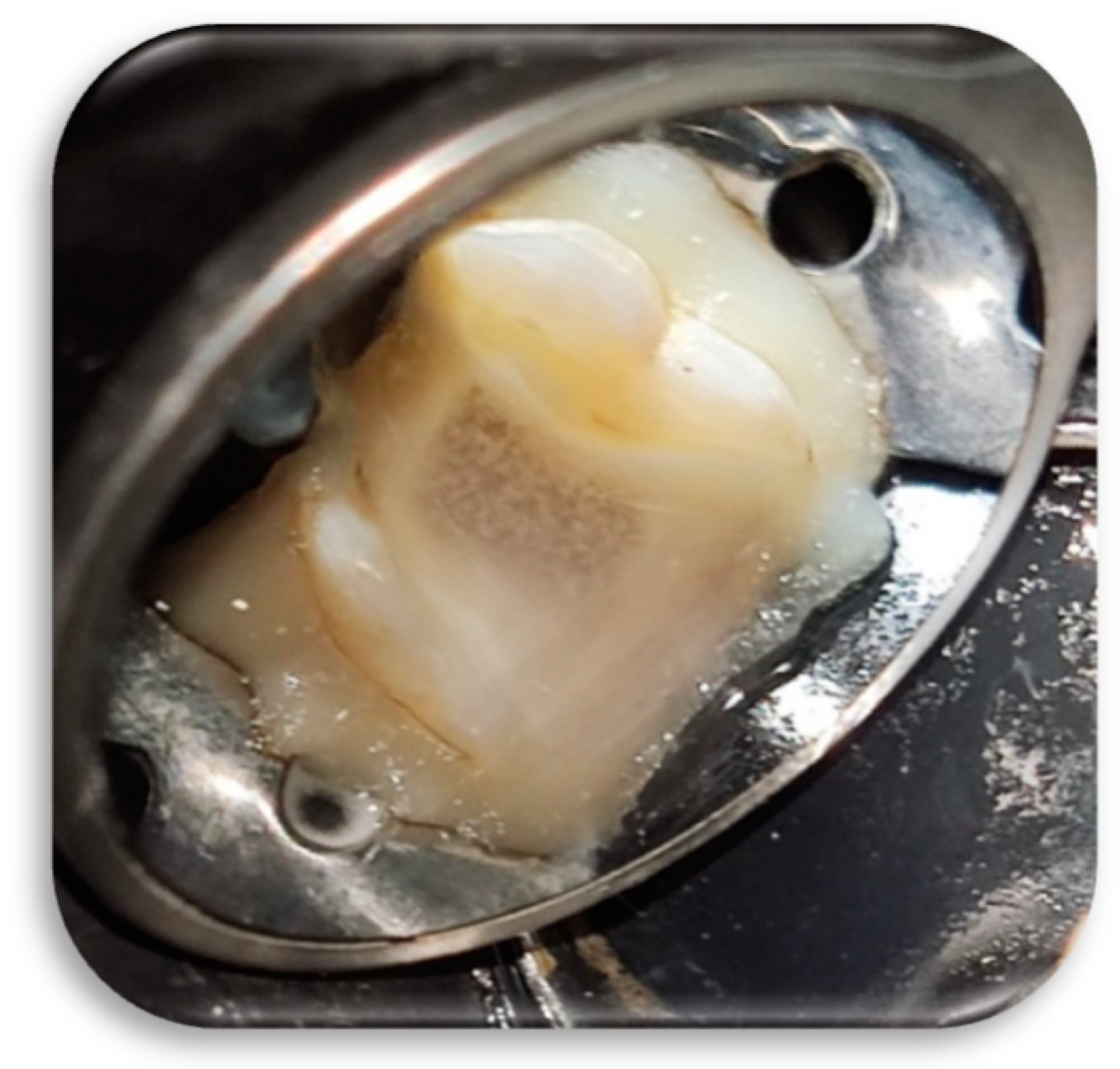
2.7. Clinical Procedures
2.8. Biomechanical Preparation
2.9. Filling of the Root Canals
2.10. Coronal Restoration
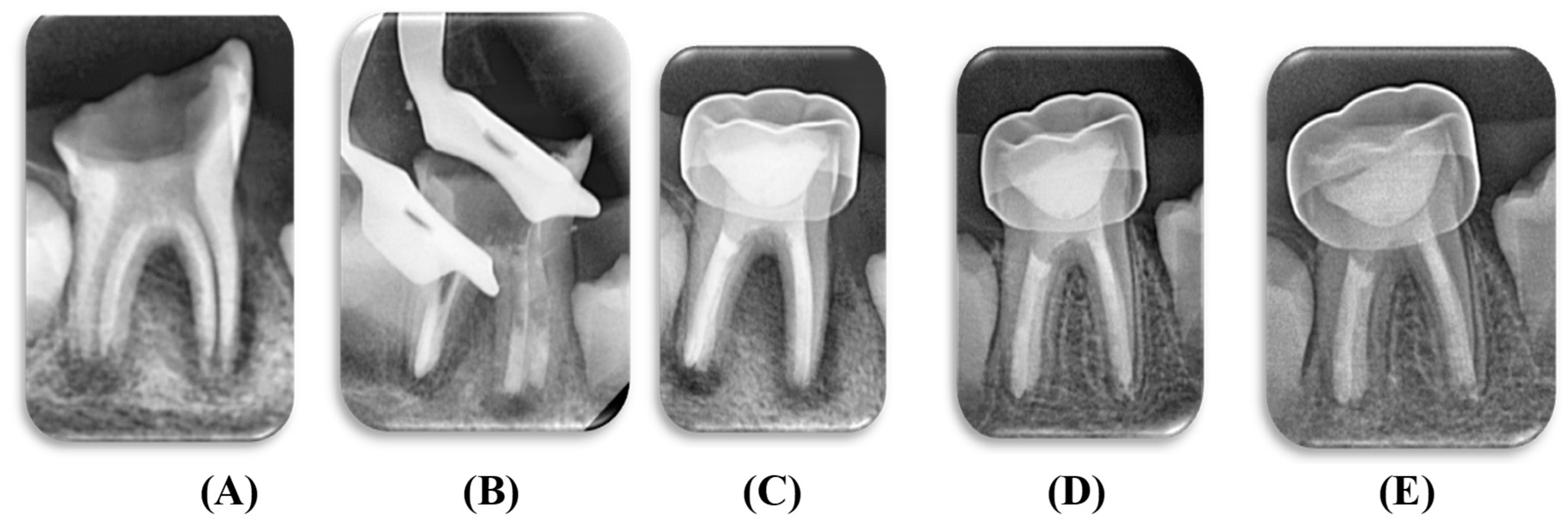
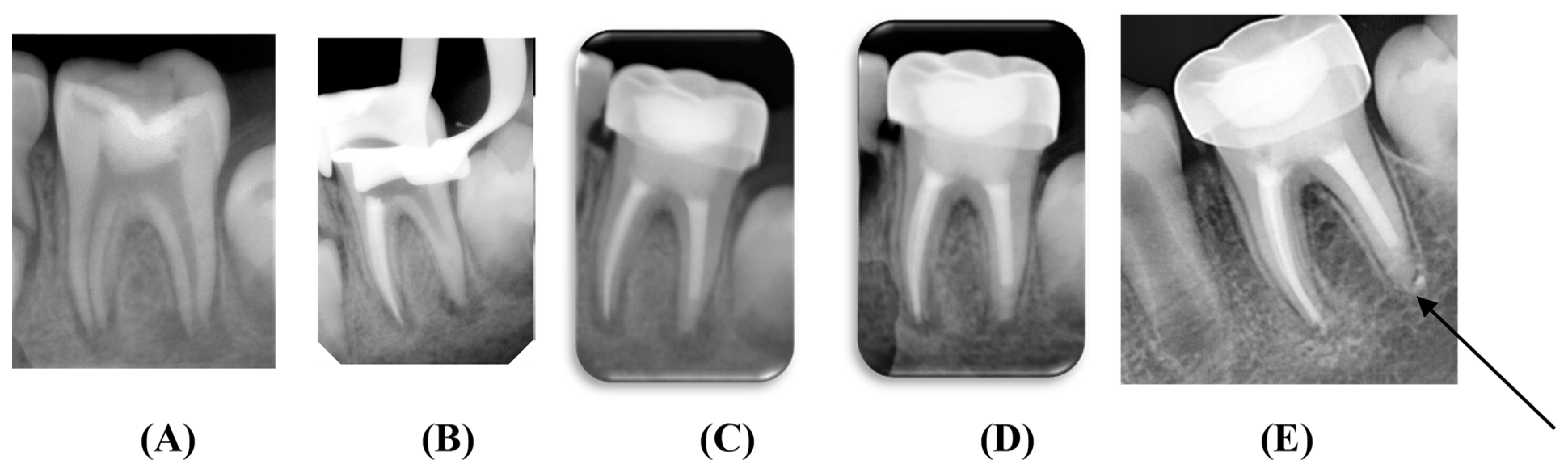
2.11. Clinical and Radiographic Evaluations
2.12. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hargreaves, K.M.; Berman, L.H. Cohen’s Pathways of the Pulp, 11th ed.; Elsevier: Saint Louis, MO, USA, 2016; pp. 913–951. [Google Scholar]
- Sheehy, E.C.; Roberts, G.J. Use of calcium hydroxide for apical barrier formation and healing in non-vital immature permanent teeth: A review. Br. Dent. J. 1997, 183, 241–246. [Google Scholar] [CrossRef]
- Felippe, M.C.S.; Felippe, W.T.; Marques, M.M.; Antoniazzi, J.H. The effect of the renewal of calcium hydroxide paste on the apexification and periapical healing of teeth with incomplete root formation. Int. Endod. J. 2005, 38, 436–442. [Google Scholar] [CrossRef]
- Andreasen, J.O.; Farik, B.; Munksgaard, E.C. Long-term calcium hydroxide as a root canal dressing may increase risk of root fracture. Dent. Traumatol. 2002, 18, 134–137. [Google Scholar] [CrossRef]
- Binnie, W.H.; Rowe, A. A Histological Study of the Periapical Tissues of Incompletely Formed Pulpless Teeth Filled with Calcium Hydroxide. J. Dent. Res. 1973, 52, 1110–1116. [Google Scholar] [CrossRef]
- Camilleri, J. Current Classification of Bioceramic Materials in Endodontics. In Bioceramic Materials in Clinical Endodontics; Springer: Cham, Switzerland, 2020; pp. 1–6. [Google Scholar] [CrossRef]
- Chung, S.H.; Chun, K.A.; Kim, H.-Y.; Kim, Y.-S.; Chang, J. Periapical Healing in Single-visit Endodontics under General Anesthesia in Special Needs Patients. J. Endod. 2019, 45, 116–122. [Google Scholar] [CrossRef]
- Camilleri, J. Biodentine™. The Dentine in a Capsule or More? Available online: https://www.septodontcorp.com/wp-content/uploads/2018/02/Biodentine-Article-0118-LOW.pdf (accessed on 1 January 2022).
- Bachoo, I.K.; Seymour, D.; Brunton, P. A biocompatible and bioactive replacement for dentine: Is this a reality? The properties and uses of a novel calcium-based cement. Br. Dent. J. 2013, 214, E5. [Google Scholar] [CrossRef]
- Kaur, M. MTA versus Biodentine: Review of Literature with a Comparative Analysis. J. Clin. Diagn. Res. 2017, 11, ZG01–ZG05. [Google Scholar] [CrossRef]
- Solanki, N.P.; Venkappa, K.K.; Shah, N.C. Biocompatibility and sealing ability of mineral trioxide aggregate and biodentine as root-end filling material: A systematic review. J. Conserv. Dent. 2018, 21, 10–15. [Google Scholar] [CrossRef]
- Johnson, E.W. Visual Analog Scale (VAS). Am. J. Phys. Med. Rehabil. 2001, 80, 717. [Google Scholar] [CrossRef]
- Orstavik, D.; Kerekes, K.; Eriksen, H.M. The periapical index: A scoring system for radiographic assessment of apical periodontitis. Dent. Traumatol. 1986, 2, 20–34. [Google Scholar] [CrossRef]
- Chauhan, A.; Saini, S.; Dua, P.; Mangla, R. Rotary Endodontics in Pediatric Dentistry: Embracing the New Alternative. Int. J. Clin. Pediatr. Dent. 2019, 12, 460–463. [Google Scholar] [CrossRef]
- Peeters, H.H.; Suardita, K.; Mooduto, L.; Gutknecht, N. Extrusion of Irrigant in Open Apex Teeth with Periapical Lesions Following Laser-Activated Irrigation and Passive Ultrasonic Irrigation. Iran. Endod. J. 2018, 13, 169–175. [Google Scholar] [CrossRef]
- Amulya, V.; Rani, V.S.; Prakash, T.J.; Ranjani, A.S.; Gayathri, C.; Chandrasekhar, V. Evaluation of biocompatibility of a new root canal irrigant Q MixTM2 in 1- An in vivo study. J. Conserv. Dent. 2013, 16, 36–40. [Google Scholar] [CrossRef] [Green Version]
- Mohammadi, Z.; Giardino, L.; Palazzi, F.; Shalavi, S.; Alikhani, M.Y.; Giudice, G.L.; Davoodpour, N. Effect of sodium hypochlorite on the sub-stantivity of chlorhexidine. Int. J. Clin. Dent. 2013, 6, 173–178. [Google Scholar]
- Attik, G.N.; Villat, C.; Hallay, F.; Pradelle-Plasse, N.; Bonnet, H.; Moreau, K.; Colon, P.; Grosgogeat, B. In vitrobiocompatibility of a dentine substitute cement on human MG63 osteoblasts cells: Biodentine™ versus MTA®. Int. Endod. J. 2014, 47, 1133–1141. [Google Scholar] [CrossRef] [PubMed]
- Hiremath, G.S.; Kulkarni, R.D.; Naik, B.D. Evaluation of minimal inhibitory concentration of two new materials using tube dilution method: An in vitro study. J. Conserv. Dent. 2015, 18, 159–162. [Google Scholar] [CrossRef] [Green Version]
- Jovanović, L.Z.; Bajkin, B.V. Scanning electron microscopy analysis of marginal adaptation of mineral trioxide aggregate, tricalcium silicate cement, and dental amalgam as a root end filling materials. Microsc. Res. Tech. 2021, 84, 2068–2074. [Google Scholar] [CrossRef]
- Nepal, M.; Shubham, S.; Tripathi, R.; Khadka, J.; Kunwar, D.; Gautam, V.; Gautam, N. Spectrophotometric analysis evaluating apical microleakage in retrograde filling using GIC, MTA and biodentine: An in-vitro study. BMC Oral Health 2020, 20, 37. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Abbas, A.; Kethineni, B.; Puppala, R.; Birapu, U.C.; Raghavendra, K.J.; Reddy, P. Efficacy of Mineral Trioxide Aggregate and Biodentine as Apical Barriers in Immature Permanent Teeth: A Microbiological Study. Int. J. Clin. Pediatr. Dent. 2020, 13, 656–662. [Google Scholar] [CrossRef]
- Torabinejad, M.; Chivian, N. Clinical applications of mineral trioxide aggregate. J. Endod. 1999, 25, 197–205. [Google Scholar] [CrossRef]
- Kumari, S.; Mittal, A.; Dadu, S.; Dhaundiyal, A.; Abraham, A.; Yendrembam, B. Comparative evaluation of physical and chemical properties of calcium silicate-based root-end filling materials (Mineral trioxide aggregate and biodentine): Anin vitrostudy. Indian J. Dent. Sci. 2018, 10, 197. [Google Scholar] [CrossRef]
- Han, L.; Okiji, T. Bioactivity evaluation of three calcium silicate-based endodontic materials. Int. Endod. J. 2013, 46, 808–814. [Google Scholar] [CrossRef] [PubMed]
- Jung, S.; Mielert, J.; Kleinheinz, J.; Dammaschke, T. Human oral cells’ response to different endodontic restorative materials: An in vitro study. Head Face Med. 2014, 10, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Miller, A.A.; Takimoto, K.; Wealleans, J.; Diogenes, A. Effect of 3 Bioceramic Materials on Stem Cells of the Apical Papilla Proliferation and Differentiation Using a Dentin Disk Model. J. Endod. 2018, 44, 599–603. [Google Scholar] [CrossRef] [PubMed]
- Apexification of Traumatically Injured Teeth: A Comparison between Biodentine and Mineral Trioxide Aggregate. Int. J. Sci. Res. (IJSR) 2017, 6, 1181–1184. [CrossRef]
- Yadav, A.; Chak, R.K.; Khanna, R. Comparative Evaluation of Mineral Trioxide Aggregate, Biodentine, and Calcium Phosphate Cement in Single Visit Apexification Procedure for Nonvital Immature Permanent Teeth: A Randomized Controlled Trial. Int. J. Clin. Pediatr. Dent. 2020, 13, S1–S13. [Google Scholar] [CrossRef]


| Follow-up | Biodentine | MTA | t-Value | p-Value | ||
|---|---|---|---|---|---|---|
| Mean ± SD | Range | Mean ± SD | Range | |||
| Baseline | 2.47 ± 1.88 | 0–7 | 1.73 ± 1.16 | 0–3 | 1.282 | 0.210 |
| 1 day | 4.27 ± 1.53 | 2–7 | 3.20 ± 1.21 | 1–5 | 2.117 | 0.043 * |
| 3 days | 2.73 ± 1.67 | 1–5 | 2.20 ± 1.57 | 0–5 | 0.903 | 0.374 |
| 1 week | 1.80 ± 1.61 | 0–4 | 0.93 ± 1.22 | 0–3 | 1.659 | 0.108 |
| 2 weeks | 1.13 ± 1.55 | 0–4 | 0.40 ± 0.74 | 0–2 | 1.653 | 0.110 |
| Follow-up Period | Plug Material | PAI Score | U-Value | p-Value | |||||
|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | Mean Rank | ||||
| Baseline | Biodentine | 0 | 0 | 0 | 14 | 1 | 4.63 | 105 | 0.317 |
| MTA | 0 | 0 | 0 | 15 | 0 | 4.77 | |||
| 6 months | Biodentine | 4 | 9 | 2 | 0 | 0 | 1.90 | 106 | 0.753 |
| MTA | 3 | 10 | 2 | 0 | 0 | 2.13 | |||
| 12 months | Biodentine | 9 | 6 | 0 | 0 | 0 | 1.30 | 90 | 0.240 |
| MTA | 12 | 3 | 0 | 0 | 0 | 1.23 | |||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tolibah, Y.A.; Kouchaji, C.; Lazkani, T.; Ahmad, I.A.; Baghdadi, Z.D. Comparison of MTA versus Biodentine in Apexification Procedure for Nonvital Immature First Permanent Molars: A Randomized Clinical Trial. Children 2022, 9, 410. https://doi.org/10.3390/children9030410
Tolibah YA, Kouchaji C, Lazkani T, Ahmad IA, Baghdadi ZD. Comparison of MTA versus Biodentine in Apexification Procedure for Nonvital Immature First Permanent Molars: A Randomized Clinical Trial. Children. 2022; 9(3):410. https://doi.org/10.3390/children9030410
Chicago/Turabian StyleTolibah, Yasser Alsayed, Chaza Kouchaji, Thuraya Lazkani, Ibrahim Ali Ahmad, and Ziad D. Baghdadi. 2022. "Comparison of MTA versus Biodentine in Apexification Procedure for Nonvital Immature First Permanent Molars: A Randomized Clinical Trial" Children 9, no. 3: 410. https://doi.org/10.3390/children9030410
APA StyleTolibah, Y. A., Kouchaji, C., Lazkani, T., Ahmad, I. A., & Baghdadi, Z. D. (2022). Comparison of MTA versus Biodentine in Apexification Procedure for Nonvital Immature First Permanent Molars: A Randomized Clinical Trial. Children, 9(3), 410. https://doi.org/10.3390/children9030410








