Role of Spanish Toddlers’ Education and Care Institutions in Achieving Physical Activity Recommendations in the COVID-19 Era: A Cross-Sectional Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design and Participants
2.2. ECEC Background Information and School Hours
2.3. ECEC and COVID-19 Regulations
2.4. Objective Physical Activity Measurement
2.5. Classroom and Playground Densities
2.6. Statistical Analysis
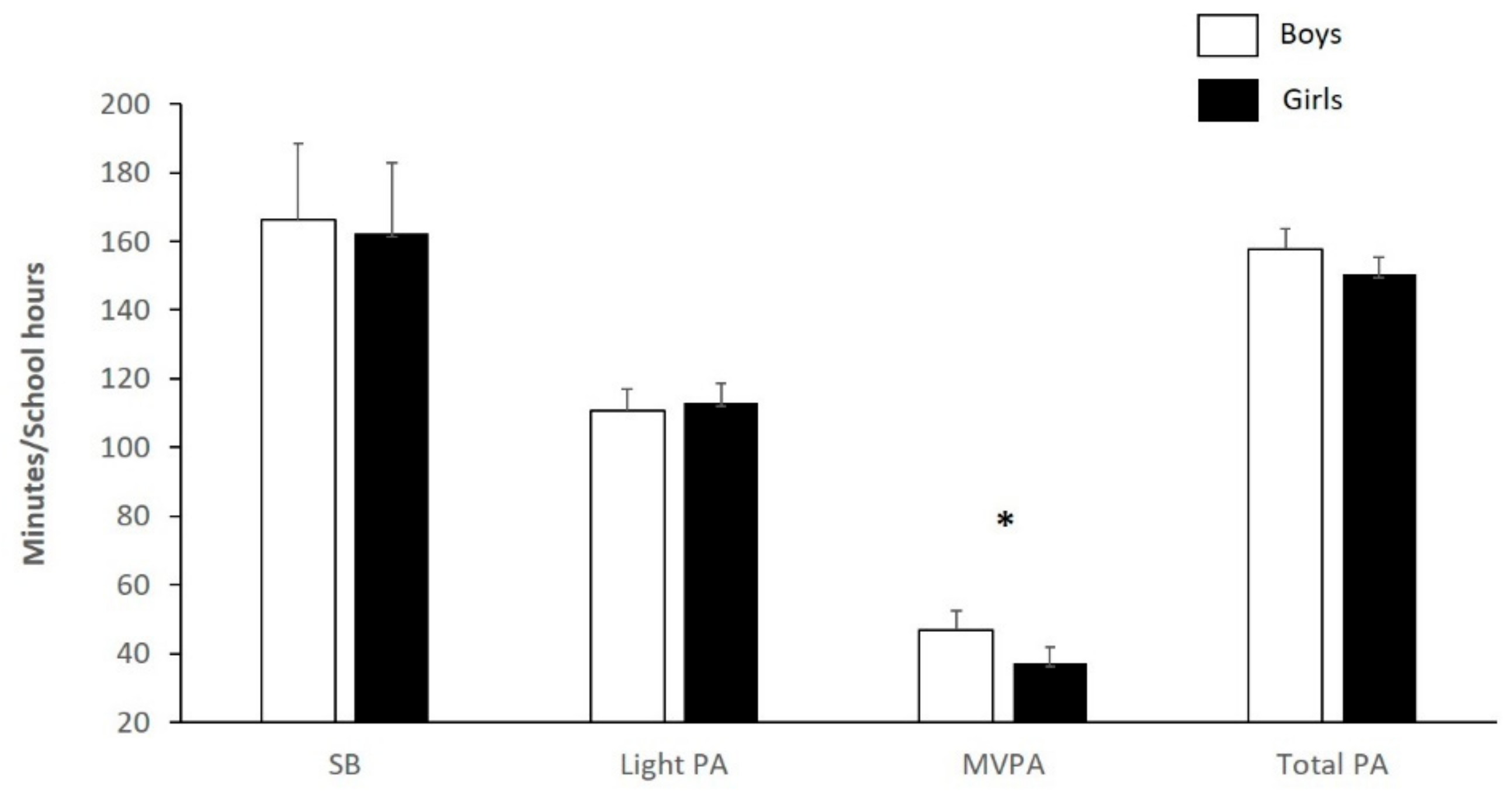
3. Results
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19-11 March 2020; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Johns Hopkins University Coronavirus COVID-19 Global Cases: Dashboard by the Center for Systems Science and Engineering (CSSE). Available online: https://coronavirus.jhu.edu/map.html (accessed on 10 August 2021).
- Saadat, S.; Rawtani, D.; Mustansar, C. Science of the Total Environment Environmental perspective of COVID-19. Sci. Total Environ. 2020, 728, 138870. [Google Scholar] [CrossRef]
- World Health Organization. Key Messages and Actions for COVID-19 Prevention and Control in Schools; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- World Health Organization. Considerations for School-Related Public Health Measures in the Context of COVID-19; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Bates, L.; Zieff, G.; Stanford, K.; Moore, J.B.; Kerr, Z.Y.; Hanson, E.D.; Barone Gibbs, B.; Kline, C.E.; Stoner, L. {COVID}-19 Impact on Behaviors across the 24-Hour Day in Children and Adolescents: Physical Activity, Sedentary Behavior, and Sleep. Children 2020, 7, 138. [Google Scholar] [CrossRef]
- Becker, S.P.; Gregory, A.M. Editorial Perspective: Perils and promise for child and adolescent sleep and associated psychopathology during the COVID-19 pandemic. J. Child Psychol. Psychiatry 2020, 7, 757–759. [Google Scholar] [CrossRef]
- Erades, N.; Morales, A.; Hernández, U.M. Impacto psicológico del confinamiento por la COVID-19 en niños españoles: Un estudio transversal. Rev. Psicol. Clín. Niños Adolesc. 2020, 7, 27–34. [Google Scholar] [CrossRef]
- Aguilar-Farias, N.; Toledo-Vargas, M.; Miranda-Marquez, S.; Cortinez-O’ryan, A.; Martino-Fuentealba, P.; Cristi-Montero, C.; Rodríguez-Rodríguez, F.; Guarda-Saavedra, P.; Pozo-Cruz, B.; Okely, A.D. Associations between movement behaviors and emotional changes in toddlers and preschoolers during early stages of the COVID-19 pandemic in Chile. Front. Pediatr. 2021. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Farias, N.; Toledo-Vargas, M.; Miranda-Marquez, S.; Cortinez-O’Ryan, A.; Cristi-Montero, C.; Rodriguez-Rodriguez, F.; Martino-Fuentealba, P.; Okely, A.D.; Del Pozo-Cruz, B. Sociodemographic Predictors of Changes in Physical Activity, Screen Time, and Sleep among Toddlers and Preschoolers in Chile during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 176. [Google Scholar] [CrossRef]
- WHO. WHO Guidelines on Physical Activity, Sedentary Behaviour; WHO: Geneva, Switzerland, 2019; ISBN 9789241550536. [Google Scholar]
- SHAPE. Active Start: A Statement of Physical Activity Guidelines for Children from Birth to Age 5, 3rd ed.; Stephen, J., Virgilio, R.C., Eds.; SHAPE America: Annapolis Junction, MD, USA, 2020. [Google Scholar]
- Institute of Medicine. Early Childhood Obesity Prevention Policies; The National Academies Press: Washington, DC, USA, 2011. [Google Scholar]
- Hesketh, K.R.; O’Malley, C.; Paes, V.M.; Moore, H.; Summerbell, C.; Ong, K.K.; Lakshman, R.; van Sluijs, E.M.F. Determinants of Change in Physical Activity in Children 0–6 years of Age: A Systematic Review of Quantitative Literature. Sports Med. 2017, 47, 1349–1374. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sallis, J.F.; Owen, N.; Fisher, E.B. Ecological Models of Health Behavior. In Health Behavior and Health Education: Theory; Jossey-Bass: San Francisco, CA, USA, 2008; pp. 465–486. [Google Scholar]
- Wijtzes, A.I.; Kooijman, M.N.; Kiefte-De Jong, J.C.; De Vries, S.I.; Henrichs, J.; Jansen, W.; Jaddoe, V.W.V.; Hofman, A.; Moll, H.A.; Raat, H. Correlates of physical activity in 2-year-old toddlers: The generation R study. J. Pediatr. 2013, 163, 791–799.e2. [Google Scholar] [CrossRef]
- Johansson, E.; Hagströmer, M.; Svensson, V.; Ek, A.; Forssén, M.; Nero, H.; Mårcus, C. Objectively measured physical activity in two-year-old children—levels, patterns and correlates. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 3. [Google Scholar] [CrossRef] [Green Version]
- Kwon, S.; Honegger, K.; Mason, M. Daily physical activity among toddlers: Hip and wrist accelerometer assessments. Int. J. Environ. Res. Public Health 2019, 16, 4244. [Google Scholar] [CrossRef] [Green Version]
- Bingham, D.D.; Costa, S.; Hinkley, T.; Shire, K.A.; Clemes, S.A.; Barber, S.E. Physical Activity During the Early Years: A Systematic Review of Correlates and Determinants. Am. J. Prev. Med. 2016, 51, 384–402. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hager, E.R.; Gormley, C.E.; Latta, L.W.; Treuth, M.S.; Caulfield, L.E.; Black, M.M. Toddler physical activity study: Laboratory and community studies to evaluate accelerometer validity and correlates. BMC Public Health 2016, 16, 936. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Prioreschi, A.; Brage, S.; Hesketh, K.D.; Hnatiuk, J.; Westgate, K.; Micklesfield, L.K. Describing objectively measured physical activity levels, patterns, and correlates in a cross sectional sample of infants and toddlers from South Africa. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 176. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gubbels, J.S.; Van Kann, D.H.H.; Jansen, M.W.J. Play Equipment, Physical Activity Opportunities, and Children ’s Activity Levels at Childcare. J. Environ. Public Health 2022, 2012, 326520. [Google Scholar] [CrossRef]
- Fees, B.S.; Fischer, E.; Haar, S.; Crowe, L.K. Toddler Activity Intensity During Indoor Free-Play: Stand and Watch. J. Nutr. Educ. Behav. 2015, 47, 170–175. [Google Scholar] [CrossRef] [PubMed]
- Ellis, Y.G.; Cliff, D.P.; Janssen, X.; Jones, R.A.; Reilly, J.J.; Okely, A.D. Sedentary time, physical activity and compliance with IOM recommendations in young children at childcare. Prev. Med. Rep. 2017, 7, 221–226. [Google Scholar] [CrossRef]
- Hunter, S.; Andrei, R.; Hesketh, K.D.; Rhodes, R.E.; Christina, M.R.; Rodgers, W.; Spence, J.C.; Carson, V. Objectively measured environmental correlates of toddlers’ physical activity and sedentary behavior. Pediatr. Exerc. Sci. 2019, 31, 480–487. [Google Scholar] [CrossRef]
- Driediger, M.; Vanderloo, L.M.; Truelove, S.; Bruijns, B.A.; Tucker, P. Encouraging kids to hop, skip, and jump: Emphasizing the need for higher-intensity physical activity in childcare. J. Sport Heal. Sci. 2018, 7, 333–336. [Google Scholar] [CrossRef]
- Zhang, Z.; Sousa-Sá, E.; Pereira, J.R.; Okely, A.D.; Feng, X.; Santos, R. The associations between environmental characteristics of early childhood education and care centers and 1-year change in toddlers’ physical activity and sedentary behavior. J. Phys. Act. Heal. 2019, 16, 1000–1006. [Google Scholar] [CrossRef]
- Zhang, Z.; Kuzik, N.; Adamo, K.B.; Ogden, N.; Goldfield, G.S.; Okely, A.D.; Crozier, M.; Hunter, S.; Predy, M.; Carson, V. Associations between the Child Care Environment and Children’s In-Care Physical Activity and Sedentary Time. Heal. Educ. Behav. 2021, 48, 42–53. [Google Scholar] [CrossRef]
- Peden, M.E.; Jones, R.; Costa, S.; Ellis, Y.; Okely, A.D. Relationship between children’s physical activity, sedentary behavior, and childcare environments: A cross sectional study. Prev. Med. Rep. 2017, 6, 171–176. [Google Scholar] [CrossRef]
- Tonge, K.L.; Jones, R.A.; Okely, A.D. Environmental Influences on Children’s Physical Activity in Early Childhood Education and Care. J. Phys. Act. Health 2020, 17, 423–428. [Google Scholar] [CrossRef]
- Carson, V.; Adamo, K.B.; Ogden, N.; Goldfield, G.S.; Okely, A.D.; Kuzik, N.; Crozier, M.; Hunter, S.; Predy, M. Sedentary Time and Physical Activity Associations Between Child Care Educators and Children. Am. J. Prev. Med. 2020, 58, e105–e111. [Google Scholar] [CrossRef]
- Lahuerta-Contell, S.; Molina-García, J.; Queralt, A.; Martínez-Bello, V.E. The Role of Preschool Hours in Achieving Physical Activity Recommendations for Preschoolers. Children 2021, 8, 82. [Google Scholar] [CrossRef]
- Tonge, K.L.; Jones, R.A.; Okely, A.D. Correlates of children’s objectively measured physical activity and sedentary behavior in early childhood education and care services: A systematic review. Prev. Med. 2016, 89, 129–139. [Google Scholar] [CrossRef] [Green Version]
- Nazaruk, S.; Marchel, J.; Kruszewska, A.; Tokarewicz, E. Physical activity of early school-age children in Poland during classes in the time of the {COVID}-19 pandemic. Education 3-13 2012, 1–13. [Google Scholar] [CrossRef]
- Lafave, L.; Webster, A.D.; Mcconnell, C. Impact of COVID—19 on Early Childhood Educator’s Perspectives and Practices in Nutrition and Physical Activity: A Qualitative Study. Early Child. Educ. J. 2021, 49, 935–945. [Google Scholar] [CrossRef]
- Pelletier, C.A.; Cornish, K.; Sanders, C. Children’ s Independent Mobility and Physical Activity during the COVID-19 Pandemic: A Qualitative Study with Families. Int. J. Environ. Res. Public Health 2021, 18, 4481. [Google Scholar] [CrossRef]
- Alonso-Martínez, A.M.; Ramírez-Vélez, R.; García-Alonso, Y.; Izquierdo, M.; García-Hermoso, A. Physical activity, sedentary behavior, sleep and self-regulation in spanish preschoolers during the COVID-19 lockdown. Int. J. Environ. Res. Public Health 2021, 18, 693. [Google Scholar] [CrossRef]
- Martínez-Bello, V.E.; Estevan, I. Physical Activity and Motor Competence in Preschool Children. Children 2021, 8, 305. [Google Scholar] [CrossRef]
- Bruijns, B.A.; Truelove, S.; Johnson, A.M.; Gilliland, J.; Tucker, P. Infants’ and toddlers’ physical activity and sedentary time as measured by accelerometry: A systematic review and meta-analysis. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 14. [Google Scholar] [CrossRef] [Green Version]
- Kuczmarski, R.; Ogden, C.; Guo, S.; Grummer-Strawn, L.M.; Flegal, K.; Mei, Z.; Wei, R.; Curtin, L.; Roche, A.; Johnson, C. CDC Growth Charts for the United States: Methods and development. Vital Health Stat. Ser. 2002, 11, 1–190. [Google Scholar]
- Pate, R.R.; Pfeiffer, K.A.; Trost, S.G.; Ziegler, P.; Dowda, M. Physical activity among children attending preschools. Pediatrics 2004, 114, 1258–1263. [Google Scholar] [CrossRef] [Green Version]
- Bisson, M.; Tremblay, F.; Pronovost, E.; Julien, A.S.; Marc, I. Accelerometry to measure physical activity in toddlers: Determination of wear time requirements for a reliable estimate of physical activity. J. Sports Sci. 2019, 37, 298–305. [Google Scholar] [CrossRef]
- Trost, S.G.; Fees, B.S.; Haar, S.J.; Murray, A.D.; Crowe, L.K. Identification and Validity of Accelerometer Cut-Points for Toddlers. Obesity 2012, 20, 2317–2319. [Google Scholar] [CrossRef]
- Ridgers, N.D.; Fairclough, S.J.; Stratton, G. Variables associated with children’s physical activity levels during recess: The A-CLASS project. Int. J. Behav. Nutr. Phys. Act. 2010, 7, 74. [Google Scholar] [CrossRef] [Green Version]
- Arufe-Giráldez, V.; Sanmiguel-Rodríguez, A.; Zagalaz-Sánchez, M.L.; Cachón-Zagalaz, J.; González-Valero, G. Sleep, physical activity and screens in 0–4 years Spanish children during the {COVID}-19 pandemic: Were the {WHO} recommendations met? J. Hum. Sport Exerc. 2020. [Google Scholar] [CrossRef]
- Spanish Government. Real Decreto 926/2020, de 25 de Octubre, Por el Que se Declara el Estado de Alarma Para Contener la Propagación de Infecciones Causadas por el SARSCoV-2; Agencia Estatal Boletín Oficial del Estado: Madrid, Spain, 2020. [Google Scholar]
- Weaver, R.G.; Hunt, E.T.; Armstrong, B.; Beets, M.W.; Brazendale, K.; Turner-Mcgrievy, G.; Pate, R.R.; Youngstedt, S.D.; Dugger, R.; Parker, H.; et al. COVID-19 Leads to Accelerated Increases in Children’s BMI z-Score Gain: An Interrupted Time-Series Study. Am. J. Prev. Med. 2021, 61, E161–E169. [Google Scholar] [CrossRef]
- Browne, N.T.; Snethen, J.A.; Greenberg, C.S.; Frenn, M.; Kilanowski, J.F.; Gance-Cleveland, B.; Burke, P.J.; Lewandowski, L. When Pandemics Collide: The Impact of COVID-19 on Childhood Obesity. J. Pediatr. Nurs. 2021, 56, 90–98. [Google Scholar] [CrossRef]
- Cadenas-Sánchez, C.; Intemann, T.; Labayen, I.; Artero, E.G.; Alvarez-Bueno, C.; Sanchis-Moysi, J.; Benito, P.J.; Beltran-Valls, M.R.; Pérez-Bey, A.; Sanchez-Delgado, G.; et al. Prevalence of severe/morbid obesity and other weight status and anthropometric reference standards in Spanish preschool children: The PREFIT project. Pediatr. Res. 2020, 87, 501–510. [Google Scholar] [CrossRef] [Green Version]
- Hesketh, K.; Griffin, S.J.; Van Sluijs, E.M.F. UK Preschool-aged children’s physical activity levels in childcare and at home: A cross-sectional exploration. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 123. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hnatiuk, J.; Ridgers, N.D.; Salmon, J.O.; Campbell, K.; Mccallum, Z.O.E.; Hesketh, K. Physical Activity Levels and Patterns of 19-month-old children. Med. Sci. Sport. Exerc. 2012, 44, 1715–1720. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Margraf, J.; Brailovskaia, J.; Schneider, S. Behavioral measures to fight {COVID}-19: An 8-country study of perceived usefulness, adherence and their predictors. PLoS ONE 2020, 15, e0243523. [Google Scholar] [CrossRef]
- Valencian Community. Plan de Contingencia y Continuidad en el Trabajo Durante las Fases de Nueva Normalidad de los Centros Docentes Públicos Dependientes de la Conselleria de Educación, Cultura y Deporte; Valencian Community: Valencia, Spain, 2020. [Google Scholar]
- Petousi, V.; Sifaki, E. Contextualising harm in the framework of research misconduct. Findings from discourse analysis of scientific publications. Int. J. Sustain. Dev. 2020, 23, 149–174. [Google Scholar]
| Variable | Measure |
|---|---|
| Age in months, mean (SD) | 31.98 (3.162) |
| Gender, n (%) | |
| Boys | 54.2% |
| Girls | 45.8% |
| BMI, mean (SD) (age and sex adjusted) | 16.04 (2.25) |
| Underweight (%) | 23.3 |
| Normal weight (%) | 51.1 |
| Overweight (%) | 11.1 |
| Obese (%) | 14.4 |
| SB | LPA | MVPA | TPA | |||||
|---|---|---|---|---|---|---|---|---|
| Predictors | Estimates (95% CI) | p | Estimates (95% CI) | p | Estimates (95% CI) | p | Estimates (95% CI) | p |
| (Intercept) | 226.93 (122.41, 331.44) | <0.001 | 132.71 (71.14, 194.28) | <0.001 | 46.16 (4.24, 88.08) | 0.031 | 233.28 (143.53, 323.04) | <0.001 |
| Gender (girl) | 6.01 (−3.27, 15.28) | 0.20 | 2.97 (−3.57, 9.51) | 0.37 | −7.97 (−13.48, −2.46) | 0.005 | −5.51 (−15.30, 4.29) | 0.27 |
| Age | 12.57 (−7.05, 32.18) | 0.21 | −15.49 (−29.15, −1.84) | 0.026 | 6.3 (−4.82, 17.42) | 0.27 | −8.92 (−29.30, 11.46) | 0.39 |
| Classroom density | −218.23 (−429.52, −6.93) | 0.043 | 58.02 (−55.05, 171.10) | 0.32 | −59.22 (−122.66, 4.23) | 0.067 | −107.01 (−268.89, 54.88) | 0.20 |
| Playground density | −208.75 (−464.31, 46.82) | 0.11 | −43.84 (−179.05, 91.38) | 0.53 | 29.47 (−44.32, 103.27) | 0.43 | −114.62 (−307.74, 78.51) | 0.25 |
| Random effects | ||||||||
| Total variance | 571.1 | 285.75 | 205.54 | 640.74 | ||||
| Random-effects variance | 444.52 | 110.65 | 20.48 | 219.51 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vega-Perona, H.; Estevan, I.; García-Ochoa, Y.C.; Martínez-Bello, D.A.; Bernabé-Villodre, M.d.M.; Martínez-Bello, V.E. Role of Spanish Toddlers’ Education and Care Institutions in Achieving Physical Activity Recommendations in the COVID-19 Era: A Cross-Sectional Study. Children 2022, 9, 51. https://doi.org/10.3390/children9010051
Vega-Perona H, Estevan I, García-Ochoa YC, Martínez-Bello DA, Bernabé-Villodre MdM, Martínez-Bello VE. Role of Spanish Toddlers’ Education and Care Institutions in Achieving Physical Activity Recommendations in the COVID-19 Era: A Cross-Sectional Study. Children. 2022; 9(1):51. https://doi.org/10.3390/children9010051
Chicago/Turabian StyleVega-Perona, Herminia, Isaac Estevan, Yolanda Cabrera García-Ochoa, Daniel A. Martínez-Bello, María del Mar Bernabé-Villodre, and Vladimir E. Martínez-Bello. 2022. "Role of Spanish Toddlers’ Education and Care Institutions in Achieving Physical Activity Recommendations in the COVID-19 Era: A Cross-Sectional Study" Children 9, no. 1: 51. https://doi.org/10.3390/children9010051
APA StyleVega-Perona, H., Estevan, I., García-Ochoa, Y. C., Martínez-Bello, D. A., Bernabé-Villodre, M. d. M., & Martínez-Bello, V. E. (2022). Role of Spanish Toddlers’ Education and Care Institutions in Achieving Physical Activity Recommendations in the COVID-19 Era: A Cross-Sectional Study. Children, 9(1), 51. https://doi.org/10.3390/children9010051






