Information and Communication Technologies to Support Early Screening of Autism Spectrum Disorder: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
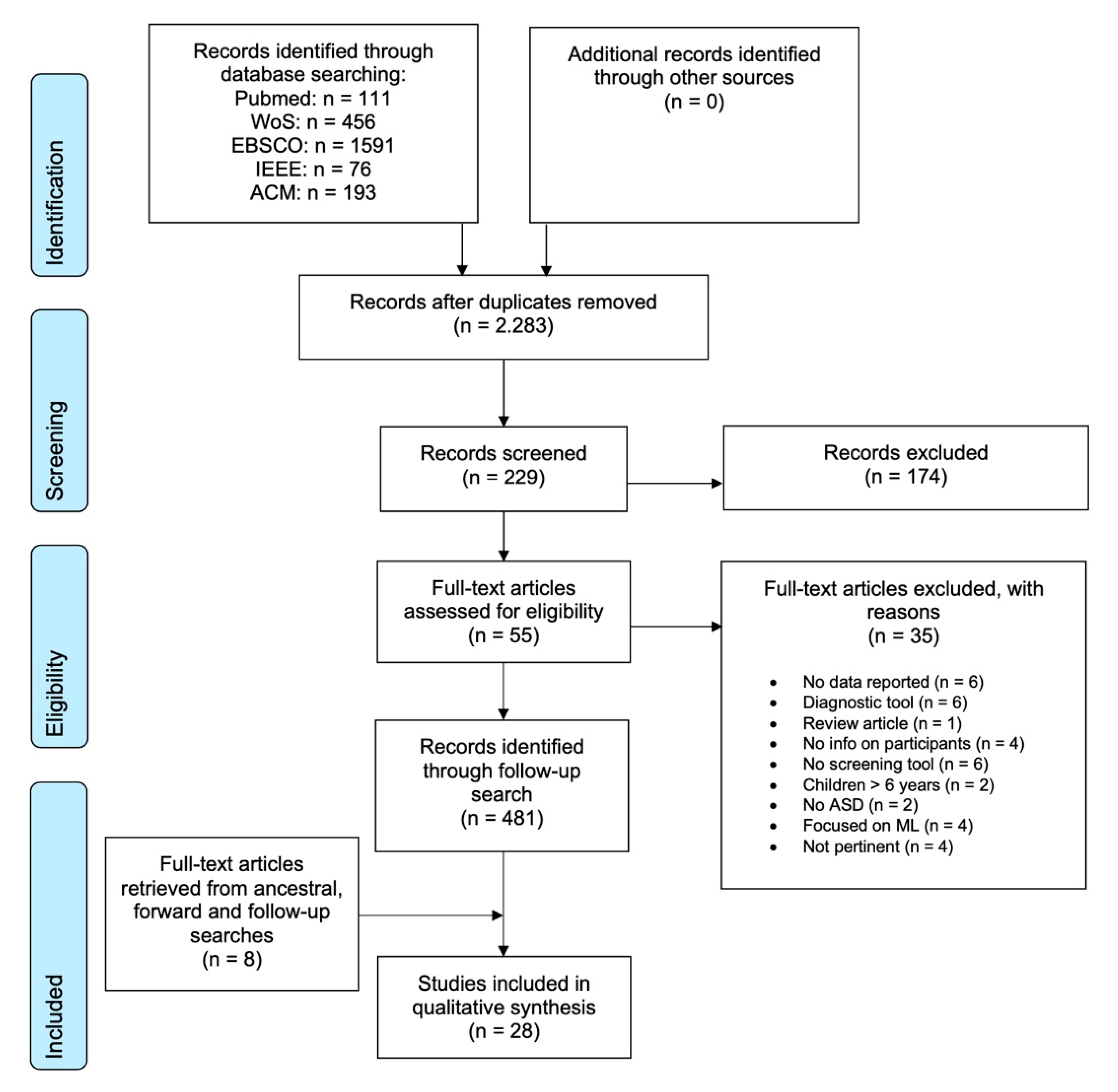
2.1. Search Strategy
2.2. Full-Texts’ Inclusion and Exclusion Criteria
- The paper had to report on the development and/or implementation of technology arrangements (whether they are commercially available or not, independently if they have been specially developed for screening or adapted from solutions available for different purposes) aimed at detecting early signs of ASD across a range of clinical (e.g., primary care; specialized clinics/services), and other settings such as laboratory, home, or school.
- The studies had to target children aged ≤6 years. Studies involving broader age ranges were included providing that they involved children within the aforementioned age group (i.e., age ≤ 6 years).
- The studies had to provide quantitative information on the capability of the technology (or the technology-based approach) of:
- Screening for ASD at the population level (Level 1 screening; L1), such as children evaluated by primary care physicians, or
- Screening for ASD in a subsample of the population identified as at risk for the disorder (Level 2 screening; L2), such as a referred clinical sample with a variety of developmental concerns, siblings of children with ASD, pre-term children, children with genetic syndromes that are usually associated with ASD, or children with a diagnosis of other neurodevelopmental disorders [29].
- Reporting on a retrospective analysis of existing databases of evaluation records which were not directly implemented in the aforementioned applied settings and/or did not involve the target users (i.e., health professionals; caregivers);
- Focusing on invasive or non-invasive techniques to investigate biological processes and structures (e.g., electroencephalography, brain imaging, electrodermal activity);
- Using technology to investigate physiological (e.g., heart rate; eye movements), behavioral (e.g., vocal or movement patterns; crying), or cognitive differences between children with/at risk of ASD and controls not for the purpose of developing a screening tool;
- Providing training to professionals on the use of a screening tool.
2.3. Data Coding and Extraction
2.4. Inter-Rater Agreement
3. Results
3.1. Overview of the Results
3.2. Types of Technologies Used
3.3. Screening Level
3.3.1. L1 Screening Tools
Solutions Tested with Children up to 30 Months
Solutions Tested with Children up to Six Years
3.3.2. L2 Screening Tools
Solutions Tested with Children up to 18 Months
Solutions Tested with Children up to 48 Months
Solutions Tested with Children up to Six Years and Older
3.4. Technology Maturity
3.5. Psychometric Properties
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Search ID | Search Terms |
|---|---|
| 1 | Child, Preschool (Mesh) |
| 2 | Infant * or baby or babies or toddler * or girl * or boy * or pre * school * |
| 3 | #1 OR #2 |
| 4 | Autism Spectrum Disorder (Mesh) |
| 5 | autis * or asperger * or pervasive or PDD or PDDNOS or pervasive develop * or autistic |
| 6 | #4 OR #5 |
| 7 | 3# AND #6 |
| 8 | Technology (Mesh) |
| 9 | Computer or mobile or digital or smart or wearable * or ICT or information technology or electronic or device or smartphone or mobile phone or virtual reality or robots or social robot * or augmented reality or speech generating device or SGD or iPad or tablet or eye tracker or gaze tracker or eye tracking or sensors or artificial intelligence or AI or voice-controlled or personal assistants or virtual assistants or smartwatch or iWatch or smartglasses or GPS or assistive technology or AT or internet of things or IOT |
| 10 | #8 OR #9 |
| 11 | Early Diagnosis (Mesh) |
| 12 | Early Medical Intervention (Mesh) |
| 13 | Early Intervention, Educational (Mesh) |
| 14 | #11 OR #12 OR #13 |
| 15 | #10 AND #14 |
| 16 | #7 AND #15 |
| Search ID | Search Terms |
|---|---|
| 1 | Infant * or baby or babies or toddler * or girl * or boy * or pre * school * |
| 2 | autis * or asperger * or pervasive or PDD or PDDNOS or pervasive develop * or autistic |
| 3 | #1 AND #2 |
| 4 | Technology or Computer or mobile or digital or smart or wearable * or ICT or information technology or electronic or device or smartphone or mobile phone or virtual reality or robots or social robot * or augmented reality or speech generating device or SGD or iPad or tablet or eye tracker or gaze tracker or eye tracking or sensor * or artificial intelligence or AI or voice-controlled or personal assistants or virtual assistants or smartwatch or iWatch or smartglasses or GPS or assistive technology or AT or internet of things or IOT |
| 5 | Diagnosis or Screening or Early Intervention or Preschool Education |
| 6 | #4 AND #5 |
| 7 | #3 AND #6 |
| Search ID | Search Terms |
|---|---|
| 1 | preschool |
| 2 | Infant * |
| 3 | #1 OR #2 |
| 4 | Autism Spectrum Disorder (Mesh) |
| 5 | autis* or pervasive |
| 6 | #4 OR #5 |
| 7 | 3# AND #6 |
| Search ID | Search Terms |
|---|---|
| 1 | (All: autism) AND (All: infant) |
Appendix B
| Score | Instructions | Examples |
|---|---|---|
| 0 points | (a) Title refers to a different age range than 0–6 OR (b) Title refers to a different term than autism (i.e., elderly or cerebral palsy, but not autism related terms) OR (c) Title refers to a different application area than Screening/ Monitoring or Intervention OR (d) Title is related to a systematic review or meta-analysis (instead of being a primary study) OR (e) Tittle is related to genetic/biochemical research | Title 1: “Digital images as meaning bridges: Case study of assimilation using avatar software in counselling with a 14-year-old boy” Explanation: The study satisfies two inclusion criteria: (1) it involves autism, (2) it refers to a technology-based intervention. However, it is explicitly mentioned that it does not focus on pre-school children. Title 2: “Technology-mediated learning in students with ASD. A bibliographical review” Explanation: The study satisfies two inclusion criteria: (a) it involves autism, (b) it refers to a technology-based intervention. However, it is a systematic review. |
| 1 point | (a) Title includes any term related to autism spectrum disorder condition (autis* or Asperger* or pervasive or PDD or PDDNOS or pervasive develop* or autistic) OR (b) Title refers to (any kind of) technology-based intervention or screening (or monitoring) AND (c) Title does not qualify for any of the 5 options that apply for 0 points | Title 1: “Sustained Community Implementation of JASPER Intervention with Toddlers with Autism” Explanation: The article refers to autism (and toddlers) which is the focus of our study. Even if we don’t know whether JASPER is a technology-based intervention, it is worth including this article in the next step. Title 2: “Factor Analysis of the Childhood Autism Rating Scale in a Sample of Two Year Olds with an Autism Spectrum Disorder” Explanation: The study satisfies two inclusion criteria: (a) it involves autism, (b) it refers to a tool for diagnosis. I know that the Childhood Autism Rating Scale is an observational tool, but I would prefer to be highly inclusive in this very first step. |
| 2 point | (a) Title includes any term related to autism spectrum disorder condition (autis* or as-perger* or pervasive or PDD or PDDNOS or pervasive develop* or autistic) AND (b) Title refers to (any kind of) technology-based intervention or screening (or monitoring) AND (c) Title does not qualify for any of the 5 options than apply for 0 points | Title 1: “Randomised controlled trial of an iPad based early intervention for autism: TOBY playpad study protocol” Explanation: The study satisfies inclusion criteria: (a) it involves autism AND (b) it refers to a technology-based intervention. Title 2: “Automatic newborn cry analysis: a non-invasive tool to help autism early diagnosis” Explanation: The article refers to autism (and newborns). We might suppose that the mentioned “tool” is a kind of digital technology. Hence, it would be better to include this title in the next step. |
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Hyman, S.L.; Levy, S.E.; Myers, S.M. Identification, evaluation, and management of children with autism spectrum disorder. Pediatrics 2020, 145. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Meeting Report: Autism Spectrum Disorders & Other Developmental Disorders: From Raising Awareness to Building Capacity; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- Rojas-Torres, L.P.; Alonso-Esteban, Y.; Alcantud-Marín, F. Early Intervention with Parents of Children with Autism Spectrum Disorders: A Review of Programs. Children 2020, 7, 294. [Google Scholar] [CrossRef] [PubMed]
- Seymour, M.; Wood, C.; Giallo, R.; Jellett, R. Fatigue, stress and coping in mothers of children with an autism spectrum disorder. J. Autism Dev. Disord. 2013, 43, 1547–1554. [Google Scholar] [CrossRef]
- Cakir, J.; Frye, R.E.; Walker, S.J. The lifetime social cost of autism: 1990–2029. Res. Autism Spectr. Disord. 2020, 72, 101502. [Google Scholar] [CrossRef]
- Tachibana, Y.; Miyazaki, C.; Ota, E.; Mori, R.; Hwang, Y.; Kobayashi, E.; Kamio, Y. A systematic review and meta-analysis of comprehensive interventions for pre-school children with autism spectrum disorder (ASD). PLoS ONE 2017, 12, e0186502. [Google Scholar] [CrossRef]
- Daniels, A.M.; Halladay, A.K.; Shih, A.; Elder, L.M.; Dawson, G. Approaches to enhancing the early detection of autism spectrum disorders: A systematic review of the literature. J. Am. Acad. Child Adolesc. Psychiatry 2014, 53, 141–152. [Google Scholar] [CrossRef]
- Zwaigenbaum, L.; Bauman, M.L.; Choueiri, R.; Kasari, C.; Carter, A.; Granpeesheh, D.; Natowicz, M.R. Early intervention for children with autism spectrum disorder under 3 years of age: Recommendations for practice and research. Pediatrics 2015, 136 (Suppl. 1), S60–S81. [Google Scholar] [CrossRef]
- Pierce, K.; Courchesne, E.; Bacon, E. To screen or not to screen universally for autism is not the question: Why the task force got it wrong. J. Pediatrics 2016, 176, 182–194. [Google Scholar] [CrossRef]
- Zwaigenbaum, L.; Brian, J.A.; Ip, A. Early detection for autism spectrum disorder in young children. Paediatr. Child Health 2019, 24, 424–432. [Google Scholar] [CrossRef]
- Lord, C.; Brugha, T.S.; Charman, T.; Cusack, J.; Dumas, G.; Frazier, T.; Veenstra-VanderWeele, J. Autism spectrum disorder. Nat. Rev. Dis. Primers 2020, 6, 1–23. [Google Scholar] [CrossRef] [PubMed]
- Petrocchi, S.; Levante, A.; Lecciso, F. Systematic Review of Level 1 and Level 2 Screening Tools for Autism Spectrum Disorders in Toddlers. Brain Sci. 2020, 10, 180. [Google Scholar] [CrossRef]
- Levy, S.E.; Wolfe, A.; Coury, D.; Duby, J.; Farmer, J.; Schor, E.; Warren, Z. Screening tools for autism spectrum disorder in primary care: A systematic evidence review. Pediatrics 2020, 145 (Suppl. 1), S47–S59. [Google Scholar] [CrossRef]
- Austin, J.; Manning-Courtney, P.; Johnson, M.L.; Weber, R.; Johnson, H.; Murray, D.; Murray, M. Improving access to care at autism treatment centers: A System analysis approach. Pediatrics 2016, 137 (Suppl. 2), S149–S157. [Google Scholar] [CrossRef]
- Bryson, S.E.; Zwaigenbaum, L.; McDermott, C.; Rombough, V.; Brian, J. The Autism Observation Scale for Infants: Scale development and reliability data. J. Autism Dev. Disord. 2008, 38, 731–738. [Google Scholar] [CrossRef]
- Zwaigenbaum, L.; Bryson, S.; Rogers, T.; Roberts, W.; Brian, J.; Szatmari, P. Behavioral manifestations of autism in the first year of life. Int. J. Dev. Neurosci. 2005, 23, 143–152. [Google Scholar] [CrossRef]
- Bejarano-Martín, Á.; Canal-Bedia, R.; Magán-Maganto, M.; Fernández-Álvarez, C.; Cilleros-Martín, M.V.; Sánchez-Gómez, M.C.; de la Paz, M.P. Early detection, diagnosis and intervention services for young children with autism spectrum disorder in the European Union (ASDEU): Family and professional perspectives. J. Autism Dev. Disord. 2020, 50, 3380–3394. [Google Scholar] [CrossRef]
- Centres for Disease, Control and Prevention. Screening and Diagnosis of Autism Spectrum Disorder. Available online: https://www.cdc.gov/ncbddd/autism/screening.html#:~:text=Diagnosing%20autism%20spectrum%20disorder%20(ASD,at%2018%20months%20or%20younger (accessed on 19 December 2020).
- García-Primo, P.; Hellendoorn, A.; Charman, T.; Roeyers, H.; Dereu, M.; Roge, B.; Canal-Bedia, R. Screening for autism spectrum disorders: State of the art in Europe. Eur. Child Adolesc. Psychiatry 2014, 23, 1005–1021. [Google Scholar] [CrossRef]
- Arunyanart, W.; Fenick, A.; Ukritchon, S.; Imjaijitt, W.; Northrup, V.; Weitzman, C. Developmental and autism screening: A survey across six states. Infants Young Child. 2012, 25, 175–187. [Google Scholar] [CrossRef]
- Bauer, N.S.; Sturm, L.A.; Carroll, A.E.; Downs, S.M. Computer decision support to improve autism screening and care in community pediatric clinics. Infants Young Child. 2013, 26, 306–317. [Google Scholar] [CrossRef]
- Bölte, S.; Bartl-Pokorny, K.D.; Jonsson, U.; Berggren, S.; Zhang, D.; Kostrzewa, E.; Marschik, P.B. How can clinicians detect and treat autism early? Methodological trends of technology use in research. Acta Paediatr. 2016, 105, 137–144. [Google Scholar] [CrossRef]
- Desideri, L.; Di Santantonio, A.; Varrucciu, N.; Bonsi, I.; Di Sarro, R. Assistive Technology for Cognition to Support Executive Functions in Autism: A Scoping Review. Adv. Neurodev. Disord. 2020, 4, 330–343. [Google Scholar] [CrossRef]
- Egger, H.L.; Dawson, G.; Hashemi, J.; Carpenter, K.L.; Espinosa, S.; Campbell, K.; Sapiro, G. Automatic emotion and attention analysis of young children at home: A ResearchKit autism feasibility study. NPJ Digit. Med. 2018, 1, 1–10. [Google Scholar] [CrossRef]
- Stephenson, J.; Limbrick, L. A review of the use of touch-screen mobile devices by people with developmental disabilities. J. Autism Dev. Disord. 2015, 45, 3777–3791. [Google Scholar] [CrossRef]
- McCarty, P.; Frye, R.E. Early Detection and Diagnosis of Autism Spectrum Disorder: Why is it so difficult? Semin. Pediatric Neurol. 2020, 100831. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef]
- Robins, D.L.; Dumont-Mathieu, T.M. Early screening for autism spectrum disorders: Update on the modified checklist for autism in toddlers and other measures. J. Dev. Behav. Pediatrics 2006, 27, S111–S119. [Google Scholar] [CrossRef]
- Kientz, J.A.; Hayes, G.R.; Goodwin, M.S.; Gelsomini, M.; Abowd, G.D. Interactive Technologies and Autism, 3rd ed.; Morgan & Claypool Publishers: San Rafael, CA, USA, 2020. [Google Scholar]
- Campbell, K.; Carpenter, K.L.; Espinosa, S.; Hashemi, J.; Qiu, Q.; Tepper, M.; Dawson, G. Use of a digital modified checklist for autism in toddlers–revised with follow-up to improve quality of screening for autism. J. Pediatri. 2017, 183, 133–139. [Google Scholar] [CrossRef]
- Downs, S.M.; Bauer, N.S.; Saha, C.; Ofner, S.; Carroll, A.E. Effect of a Computer-Based Decision Support Intervention on Autism Spectrum Disorder Screening in Pediatric Primary Care Clinics: A Cluster Randomized Clinical Trial. JAMA Netw. Open 2019, 2, e1917676. [Google Scholar] [CrossRef]
- Duda, M.; Daniels, J.; Wall, D.P. Clinical evaluation of a novel and mobile autism risk assessment. J. Autism Dev. Disord. 2016, 46, 1953–1961. [Google Scholar] [CrossRef]
- Harrington, J.W.; Bai, R.; Perkins, A.M. Screening children for autism in an urban clinic using an electronic M-CHAT. Clin. Pediatrics 2013, 52, 35–41. [Google Scholar] [CrossRef]
- Schrader, E.; Delehanty, A.D.; Casler, A.; Petrie, E.; Rivera, A.; Harrison, K.; Wetherby, A.M. Integrating a New Online Autism Screening Tool in Primary Care to Lower the Age of Referral. Clin. Pediatrics 2020, 59, 305–309. [Google Scholar] [CrossRef]
- Carpenter, K.L.; Hahemi, J.; Campbell, K.; Lippmann, S.J.; Baker, J.P.; Egger, H.L.; Dawson, G. Digital behavioral phenotyping detects atypical pattern of facial expression in toddlers with autism. Autism Res. 2020. [Google Scholar] [CrossRef]
- Abbas, H.; Garberson, F.; Glover, E.; Wall, D.P. Machine learning approach for early detection of autism by combining questionnaire and home video screening. J. Am. Med Inform. Assoc. 2018, 25, 1000–1007. [Google Scholar] [CrossRef]
- Frazier, T.W.; Klingemier, E.W.; Parikh, S.; Speer, L.; Strauss, M.S.; Eng, C.; Youngstrom, E.A. Development and Validation of objective and quantitative eye tracking− based measures of autism risk and symptom levels. J. Am. Acad. Child Adolesc. Psychiatry 2018, 57, 858–866. [Google Scholar] [CrossRef]
- Kanne, S.M.; Carpenter, L.A.; Warren, Z. Screening in toddlers and preschoolers at risk for autism spectrum disorder: Evaluating a novel mobile-health screening tool. Autism Res. 2018, 11, 1038–1049. [Google Scholar] [CrossRef]
- Moore, A.; Wozniak, M.; Yousef, A.; Barnes, C.C.; Cha, D.; Courchesne, E.; Pierce, K. The geometric preference subtype in ASD: Identifying a consistent, early-emerging phenomenon through eye tracking. Mol. Autism 2018, 9, 19. [Google Scholar] [CrossRef]
- Pierce, K.; Marinero, S.; Hazin, R.; McKenna, B.; Barnes, C.C.; Malige, A. Eye tracking reveals abnormal visual preference for geometric images as an early biomarker of an autism spectrum disorder subtype associated with increased symptom severity. Biol. Psychiatry 2016, 79, 657–666. [Google Scholar] [CrossRef]
- Young, G.S.; Constantino, J.N.; Dvorak, S.; Belding, A.; Gangi, D.; Hill, A.; Ozonoff, S. A video-based measure to identify autism risk in infancy. J. Child Psychol. Psychiatry 2020, 61, 88–94. [Google Scholar] [CrossRef]
- Talbott, M.R.; Dufek, S.; Zwaigenbaum, L.; Bryson, S.; Brian, J.; Smith, I.M.; Rogers, S.J. Brief Report: Preliminary feasibility of the TEDI: A novel parent-administered telehealth assessment for autism spectrum disorder symptoms in the first year of life. J. Autism Dev. Disord. 2020, 5, 3432–3439. [Google Scholar] [CrossRef]
- Oller, D.K.; Niyogi, P.; Gray, S.; Richards, J.A.; Gilkerson, J.; Xu, D.; Warren, S.F. Automated vocal analysis of naturalistic recordings from children with autism, language delay, and typical development. Proc. Natl. Acad. Sci. USA 2010, 107, 13354–13359. [Google Scholar] [CrossRef]
- Wedyan, M.; Al-Jumaily, A. Early diagnosis autism based on upper limb motor coordination in high risk subjects for autism. In Proceedings of the 2016 IEEE International Symposium on Robotics and Intelligent Sensors (IRIS), Tokyo, Japan, 17–20 December 2016; pp. 13–18. [Google Scholar] [CrossRef]
- Wingfield, B.; Miller, S.; Yogarajah, P.; Kerr, D.; Gardiner, B.; Seneviratne, S.; Coleman, S. A predictive model for paediatric autism screening. Health Inform. J. 2020. [Google Scholar] [CrossRef]
- Ben-Sasson, A.; Robins, D.L.; Yom-Tov, E. Risk assessment for parents who suspect their child has autism spectrum disorder: Machine learning approach. J. Med. Internet Res. 2018, 20, e134. [Google Scholar] [CrossRef]
- Anzulewicz, A.; Sobota, K.; Delafield-Butt, J.T. Toward the autism motor signature: Gesture patterns during smart tablet gameplay identify children with autism. Sci. Rep. 2016, 6, 1–13. [Google Scholar] [CrossRef]
- Vargas-Cuentas, N.I.; Roman-Gonzalez, A.; Gilman, R.H.; Barrientos, F.; Ting, J.; Hidalgo, D.; Zimic, M. Developing an eye-tracking algorithm as a potential tool for early diagnosis of autism spectrum disorder in children. PLoS ONE 2017, 12, e0188826. [Google Scholar] [CrossRef]
- Tariq, Q.; Daniels, J.; Schwartz, J.N.; Washington, P.; Kalantarian, H.; Wall, D.P. Mobile detection of autism through machine learning on home video: A development and prospective validation study. PLoS Med. 2018, 15, e1002705. [Google Scholar] [CrossRef]
- Wan, G.; Kong, X.; Sun, B.; Yu, S.; Tu, Y.; Park, J. Applying eye tracking to identify autism spectrum disorder in children. J. Autism Dev. Disord. 2019, 49, 209–215. [Google Scholar] [CrossRef]
- Crippa, A.; Salvatore, C.; Perego, P.; Forti, S.; Nobile, M.; Molteni, M.; Castiglioni, I. Use of machine learning to identify children with autism and their motor abnormalities. J. Autism Dev. Disord. 2015, 45, 2146–2156. [Google Scholar] [CrossRef]
- Gong, Y.; Yatawatte, H.; Poellabauer, C.; Schneider, S.; Latham, S. Automatic Autism Spectrum Disorder Detection Using Everyday Vocalizations Captured by Smart Devices. In Proceedings of the 2018 ACM International Conference on Bioinformatics, Computational Biology, and Health Informatics, Washington, DC, USA, 29 August–1 September 2018; pp. 465–473. [Google Scholar] [CrossRef]
- Martineau, J.; Hernandez, N.; Hiebel, L.; Roché, L.; Metzger, A.; Bonnet-Brilhault, F. Can pupil size and pupil responses during visual scanning contribute to the diagnosis of autism spectrum disorder in children? J. Psychiatr. Res. 2011, 45, 1077–1082. [Google Scholar] [CrossRef]
- Thabtah, F. An accessible and efficient autism screening method for behavioural data and predictive analyses. Health Inform. J. 2019, 25, 1739–1755. [Google Scholar] [CrossRef]
- Ramirez-Duque, A.A.; Bastos, T.; Munera, M.; Cifuentes, C.A.; Frizera-Neto, A. Robot-Assisted Intervention for children with special needs: A comparative assessment for autism screening. Robot. Auton. Syst. 2020, 103484. [Google Scholar] [CrossRef]
- Frazier, T.W.; Klingemier, E.W.; Beukemann, M.; Speer, L.; Markowitz, L.; Parikh, S.; Wexberg, S.; Giuliano, K.; Schulte, E.; Delahunty, C.; et al. Development of an objective autism risk index using remote eye tracking. J. Am. Acad. Child Adolesc. Psychiatry 2016, 55, 301–309. [Google Scholar] [CrossRef]
- Major, S.; Campbell, K.; Espinosa, S.; Baker, J.P.; Carpenter, K.L.; Sapiro, G.; Dawson, G. Impact of a digital Modified Checklist for Autism in Toddlers–Revised on likelihood and age of autism diagnosis and referral for developmental evaluation. Autism 2020, 24, 1629–1638. [Google Scholar] [CrossRef]
- Bauer, N.S.; Carroll, A.E.; Saha, C.; Downs, S.M. Computer decision support changes physician practice but not knowledge regarding autism spectrum disorders. Appl. Clin. Inform. 2015, 6, 454. [Google Scholar] [CrossRef]
- Wall, D.P.; Dally, R.; Luyster, R.; Jung, J.Y.; DeLuca, T.F. Use of artificial intelligence to shorten the behavioral diagnosis of autism. PLoS ONE 2012, 7, e43855. [Google Scholar] [CrossRef]
- Pierce, K.; Conant, D.; Hazin, R.; Stoner, R.; Desmond, J. Preference for geometric patterns early in life as a risk factor for autism. Arch. Gen. Psychiatry 2011, 68, 101–109. [Google Scholar] [CrossRef]
- Bacon, E.C.; Moore, A.; Lee, Q.; Carter Barnes, C.; Courchesne, E.; Pierce, K. Identifying prognostic markers in autism spectrum disorder using eye tracking. Autism 2020, 24, 658–669. [Google Scholar] [CrossRef]
- Morales-Hidalgo, P.; Hernández-Martínez, C.; Voltas, N.; Canals, J. EDUTEA: A DSM-5 teacher screening questionnaire for autism spectrum disorder and social pragmatic communication disorder. Int. J. Clin. Health Psychol. 2017, 17, 269–281. [Google Scholar] [CrossRef]
- Nah, Y.H. Preliminary data of a preschool teacher-screening checklist for autism spectrum disorder in Singapore. Adv. Autism 2020, 6, 303–313. [Google Scholar] [CrossRef]
- Resnick, M. Lifelong Kindergarten: Cultivating Creativity through Projects, Passion, Peers, and Play; The MIT Press: London, UK, 2017. [Google Scholar]
- Hughes-Roberts, T.; Brown, D.; Standen, P.; Desideri, L.; Negrini, M.; Rouame, A.; Hasson, C. Examining engagement and achievement in learners with individual needs through robotic-based teaching sessions. Br. J. Educ. Technol. 2019, 50, 2736–2750. [Google Scholar] [CrossRef]
- Desideri, L.; Bonifacci, P.; Croati, G.; Dalena, A.; Gesualdo, M.; Molinario, G.; Ottaviani, C. The Mind in the Machine: Mind Perception Modulates Gaze Aversion During Child–Robot Interaction. Int. J. Soc. Robot. 2020, 1–16. [Google Scholar] [CrossRef]
- Conti, E.; Chericoni, N.; Costanzo, V.; Lasala, R.; Mancini, A.; Prosperi, M.; Apicella, F. Moving Toward Telehealth Surveillance Services for Toddlers at Risk for Autism during the COVID-19 Pandemic. Front. Psychiatry 2020, 11, 565999. [Google Scholar] [CrossRef]
- Dahiya, A.V.; McDonnell, C.; DeLucia, E.; Scarpa, A. A systematic review of remote telehealth assessments for early signs of autism spectrum disorder: Video and mobile applications. Pract. Innov. 2020, 5, 150. [Google Scholar] [CrossRef]


| Study | Publication * 1 | Participants (n); Sex (M/F); Age | Diagnostic Tools | Type of Interface ** 1 | Technology Used | ASD Indicator Used | User | Context of Use/Implementation | Level of Screening | Maturity *** 1 |
|---|---|---|---|---|---|---|---|---|---|---|
| Abbas et al. (2018) [37] | CO-J | Children referring to autism centers (n = 230); (N/A); 18–72 months | ADOS | PC, M | Parent-completed questionnaires and experts’ video tagging (Cognoa) | Behavioral (parent-reported; clinical observation) | Caregivers; clinicians | Community; clinic (USA) | L1 | P (https://cognoa.com/) |
| Anzulewicz et al. (2016) [48] | SBS-J | (a) with ASD (n = 37); (24/12); 3–6 years (b) neurotypical (n = 45); (32/13); 3–6 years | Not reported | NUI | iPad-based gameplay | Behavioral (motor patterns) | Caregivers, clinicians | Laboratory (UK) | L1 | F |
| Bauer et al. (2013) [22] | MED-J | Children visited at 18- and 24-month (n = 857) (a) with MCHAT (n = 567) (b) MCHAT high-risk (n = 171) | M-CHAT | PC | HER: Child Health Improvement Through Computer Automation system (CHICA) | Behavioral (parent-reported) | Clinicians | Clinics (USA) | L1 | P (https://medicine.iu.edu/pediatrics/specialties/health-services/child-health-informatics-research-development-lab/the-chica-system) |
| Ben-Sasson et al. (2018) [47] | MED-J | Children with suspect of ASD (parental concerns) (n = 115) (a) with ASD-family member (n = 66); (N/A); 16–30 months (b) without ASD-family member (n = 49); (N/A); 16–30 months | M-CHAT-R/F; ASQ | PC, M | Automatic analysis of web-based discussion forums for parents with ASD concerns | Behavioral (parent-reported) | Caregivers | Community (Israel; USA) | L1 | F |
| Campbell et al. (2017) [31] | MED-J | Children referred to a primary care visit (n = 1191) (a) Baseline period (n = 657); (321/336); M: 21.89 (3.38) months (b) Intervention period (n = 534); (275/259); M: 21.88 (3.46) months | M-CHAT-R/F | M | Digital (tablet-based) version of M-CHAT-R/F | Behavioral (parent-reported) | Caregiver | Clinic (USA) | L1 | P (https://m-chat.org/) |
| Carpenter et al. (2020) [36] | AU-J | Children recruited at pediatric primary care visit (a) neurotypical (n = 74); (43/31); M: 21.7 (3.8) months (b) Non-ASD delay (n = 8); (5/3); M: 23.9 (3.7) months (c) ASD (n = 22); (17/5); M: 26.2 (4.1) months | M-CHAT-R/F; ADOS | M, NUI | Tablet-based facial expressions assessment | Behavioral (facial expressions) | Clinician | Clinic (USA) | L1 | F |
| Crippa et al. (2015) [52] | AU-J | Convenience sample (n = 30) (a) neurotypical (n = 15); (12/3); M: 2.6 (5.2) (b) ASD (n = 15); (13/2); M: 3.5 (7.7) 2 | Griffiths Mental Development Scales; ADOS | SW | Optoelectronic system coupled with passive markers attached to the participants’ hands and wrists | Behavioral (motor patterns) | Clinicians | Laboratory/Clinics (IT) | L1 | F |
| Downs et al. (2019) [32] | MED-J | Children referring to 4 pediatric clinics (n = 274) (a) Intervention (n = 138); (84/43); 18–24 months (b) Control (n = 136); (78/58); 18–24 months | Not reported/not relevant | PC | EHR: Child Health Improvement Through Computer Automation system (CHICA) | Behavioral (parent-reported) | Clinicians, caregivers | Clinic (USA) | L1 | P (https://medicine.iu.edu/pediatrics/specialties/health-services/child-health-informatics-research-development-lab/the-chica-system) |
| Duda et al. (2016) [33] | AU-J | Children attending a pediatrics clinic (n = 222) (a) with ASD (n = 69); (60/9); Mdn: 3.9 (3.3) (b) non-ASD (n = 153); (109/44); Mdn: 6.6 (3.9) | Bayley Scales of Infant and Toddler Development, Third Edition; DAS-II, Wechsler Intelligence Scales for Children, Fourth Edition; Vineland Adaptive Behavior Scales, Survey Interview Form; ADOS | M; PC | Mobile Autism Risk Assessment (MARA) | Behavioral (parent-reported) | Caregivers | Clinic (USA) | L1 | P (https://cognoa.com/) |
| Egger et al. (2018) [25] | MED-J | Children from general population (n = 1756); (1211/543); M: 40.4 (16.3) months MCHAT cohort (n = 407) (a) MCHAT high score (n = 159); (124/35); M: 24.1 (4.1) months (b) MCHAT low score (n = 248); (158/89); M: 23.2 (4.4) months | M-CHAT-R/F | M, NUI | iOS-based app (Autism & Beyond) | Behavioral (parent-reported and face expressions analysis) | Caregivers | Community (USA) | L1 | P (https://autismandbeyond.researchkit.duke.edu/ch) No longer available for download |
| Frazier et al. (2018) [38] | MED-J | Children referred to a tertiary-care, multi-disciplinary ASD evaluation clinic (n = 201) (a) ASD (n = 91); (75/16); 1.6–15.8 years (b) non-ASD (n = 11); (86/24); 1.8–17.6 years | ADOS-2; SRS-2; Clinical Evaluation of Language Fundamentals—Fourth Edition (or Preschool Version—Second Edition, or the Preschool Language Scales—Fifth Edition); CBCL | NUI | Eye-tacker (SMI RED250) | Social attention | Clinicians | Clinic (USA) | L2 | F |
| Gong et al. (2018) [53] | CO-C | (a) with ASD (n = 18); (14/4); 2–17 years (b) at risk (n = 8); (4/4); 3 m onths-4 years (c) neurotypical (n = 9); (2/7); 3–16 years | Not reported | NUI | iOS-based app for Apple iPod Touch | Behavioral (vocalizations) | Caregivers | Home (USA) | L1 | F |
| Harrington et al. (2013) [34] | MED-J | Children visited at a pediatric outpatient clinic (a) prospective cohort (n = 176); M: 22.1 months (b) retrospective cohort (n = 197); M: 23.1 months | M-CHAT | M | M-CHAT on the iPad | Behavioral (parent-reported) | Clinicians | Clinics (USA) | L1 | P (https://m-chat.org/) |
| Kanne et al. (2018) [39] | AU-J | Children referring to autism centers (n = 230) (a) ASD (n = 164); (133/31); 18–72 months (b) non-ASD (n = 66); (50/16); 18–72 months | MSEL; M-CHAT-R/F; DAS-II; SCQ; SRS; CBCL | M | Smartphone-based application (Cognoa) | Behavioral (parent-reported; clinical observation) | Caregivers; clinicians | Community; clinic (USA) | L1 | P (https://cognoa.com/) |
| Martineau et al. (2011) [54] | MED-J | (a) with ASD (n = 19); (16/3); M: 118 months (b) chronological age-matched controls (n = 19); (11/8); M: 116 months (range: 41 and 118 months) (c) mental age-matched controls (n = 19); (12/7); 87 months | ADI-R | NUI | Pupil-tracker (FaceLAB monitoring system) | Pupil size | Clinicians | Laboratory (FR) | L1 | F |
| Moore et al. (2018) [40] | AU-J | Referred/self-referred children (n = 227). (a) ASD (n = 76); (70/6); 12.1–47.4 months (b) with ASD features (n = 11); (10/1); 15.8–40.7 months (c) Developmental delay (n = 56); (36/20); 12.4–46.0 months (d) Neurotypical (n = 51); (30/21); 12.9–47.5 months (e) Other (n = 22); (11/11); 13.1–47.7 months (f) Typical sibling ASD (n = 11); (4/7); 12.2–44.6 | ADOS; MSEL; VABS | NUI | Eye-tracker (Tobii T-120) | Social attention | Clinician | Clinic (USA) | L2 | F |
| Oller et al. (2010) [44] | SBS-J | Children from general infant population (n = 232) (a) neurotypical (n = 106); 10–48 months (b) language delayed (n = 49); 10–44 months (c) ASD (n = 77); 16–48 months | M-CHAT | NUI | LENA (Language ENvironment Analysis) | Behavioral (vocalizations) | Clinicians | Home; community (USA) | L2 | P (https://www.lena.org/) |
| Pierce et al. (2016) [41] | MED-J | (a) with ASD (n = 115); (88/27); 12–49 months (b) with ASD symptoms (n = 20); (15/5); 11–42 months (c) with language or global DD (n = 57); (45/12); 10–46 months (d) other clinical conditions (n = 53); (26/27); 12–43 months (e) typical development (n = 64); (35/29); 12–44 months (f) ASD siblings (n = 25); (12/13); 12–31 months | ADOS; MSEL; VABS | NUI | Eye-tracker (Tobii T-120) | Social attention | Clinicians | Clinic (USA) | L2 | F |
| Ramirez-Duque et al. (2020) [56] | CO-J | (a) ASD (n = 23); (N/A); M: 6.62 (2.38) years (b) Other condition (n = 15); (N/A); M: 7.75 (2.70) years | Not reported | ROB | robot (ONO) | Social attention | Clinicians | Laboratory (Colombia) | L2 | F (https://opsoro.ugent.be/) |
| Schrader et al. (2020) [35] | MED-J | Children referred to a pediatric service (n = 391); (N/A); 18–24 months | Not reported | PC, M | EHR: Smart Early Screening for Autism and Communication Disorders (Smart ESAC) | Behavioral (parent-reported) | Caregivers | Clinic (USA) | L1 | P (https://autismnavigator.com/autism-navigator-for-primary-care/) |
| Talbott et al. (2020) [43] | AU-J | Convenience sample of at risk ASD children (n = 11); (5/6); 6–12 months | AOSI; ASQ-3/ASQ-SE-2; ECI; Infant-Toddler Checklist | PC, M | Telehealth Evaluation of Development for Infants (TEDI) | Behavioral (parent-collected) | Caregivers | Home (USA) | L2 | P |
| Tariq et al. (2018) [50] | MED-J | (a) ASD (n = 116); (78/38); M: 4.1 (2) (b) neurotypical (n = 46); (26/20) M: 2.11 (1) | ML classifier used features taken from ADI-R ADOS-2 items. | M | Video feature classifier and ML | Social attention and behavioral (expressive language, eye-contact, emotion expression, communicative engagement and echolalia) | Caregivers (they uploaded home videos) Other non-expert raters (they coded them prior to ML analysis) | Home (USA) | L1 | F |
| Thabtah et al. (2019) [55] | CO/MED-J | Children from general population (n = 20); (N/A); 4–11 years | Not reported | M | ASDtest app | Behavioral (parent-reported) | Caregivers | Community (Multiple languages) | L1 | P (https://www.asdtests.com/#home) |
| Vargas-Cuentas et al. (2017) [49] | SBS-J | (a) Neurotypical (n = 23);N/A; 2–6 years (b) with ASD (n = 8); N/A; 2–6 years | No formal diagnosis was available | NUI | Tablet displaying short videos and tracking eye gaze | Social attention | Caregiver | Ambulatory (Perù) | L1 | F |
| Wan et al. (2019) [51] | AU-J | (a) ASD (n = 37); (33/4); M: 4.7 (0.7) (b) neurotypical (n = 37); (27/10); M: 4.8 (0.4) | CARS; GDS | NUI | Eye-tacker (SMI RED250) | Social attention | Clinicians | Clinic (China) | L1 | F |
| Wedyan & Al-Jumaily (2016) [45] | CO-C | Convenience sample (n = 32) (a) High risk ASD (n = 17); (9/8); 12–36 months (b) Low risk ASD (n = 15); (8/7); 12–36 months | Not assessed (risk estimation based on presence of ASD sibling and/or family history of ASD) | SW | Wrist-worn sensors | Behavioral (motor patterns) | Clinicians | Laboratory (AUS) | L2 | F |
| Wingfield et al. (2020) [46] | CO/MED-J | Convenience sample (n = 228) (a) with ASD (n = 195); (156/39); Mdn: 2.6 years (b) neurotypical (n = 33); (28/5); Mdn: 2.3 years | Not reported | M | Pictorial autism assessment schedule (PAAS) | Behavioral (parent-reported) | Clinician | Community (Sri-Lanka) | L1 | F |
| Young et al. (2020) [42] | AU-J | (a) ASD (n = 21); (13/8); 6–18 months (b) High risk non-ASD (n = 52); (21/31); 6–18 months (c) Low risk non-ASD (n = 37); (22/15); 6–18 months | MSEL; ADOS-2 | PC, M | Self-reported video-based questionnaire | Behavioral (parent-reported) | Family/caregivers | Home/Community (USA) | L2 | F |
| Study | Screening Process Description | Screening Duration | Methodology for Screening Evaluation | Psychometric Properties * | Other Relevant Psychometric Properties | |||
|---|---|---|---|---|---|---|---|---|
| Se | Sp | PPV | NPV | |||||
| Abbas et al. (2018) [37] | System composed of (a) a short questionnaire about the child, completed by the parent, and (b) identification of specific behaviors by trained analysts after watching 2–3 short videos of the child within their natural environment that are captured by parents using a mobile device. | Not reported | Based on the responses to the questionnaire and the analysis of the videos, the authors trained two independent ML classifiers and combined their outputs into a single screening assessment | 97–98% 1 | 62–64% 1 | N/A | N/A | Performance accuracy markedly improved when combining the two classifiers into a single one. |
| Anzulewicz et al. (2016) [48] | Two commercially available gameplays running on iPad (mini) were used to record children’s movements while interacting with the device. Three machine learning algorithms were employed to differentiate gestures of children with ASD from those of children without ASD | Approximately 15 min | Proof-of-concept study aimed at assessing (1) whether ASD condition can be inferred from kinematic and (2) which motor features can be used to differentiate between the two groups | 76–83% | 67–88% | N/A | N/A | Best accuracy (AUC) was achieved using Regularized Greedy Forest approach and resulted on average of 0.93. |
| Bauer et al. (2013) [22] | Upon check-in to the clinic, CHICA administers two pre-screener questions for the parent to complete in the waiting room. MCHAT may be also administered (at 24-month visit only) and automatically scored. The results of the pre-screening process are provided to the clinician before the visit. | Not reported | To assess change in ASD screening rates after implementation of CHICA at two community-based clinics | N/A | N/A | N/A | N/A | Not reported |
| Ben-Sasson et al. (2018) [47] | System combining (a) automated text analysis relative to parental concerns with (b) minimal standard questioning taken from MCHAT-R to identify risk of ASD | Not reported | Proof-of-concept study assessing the association between the text analysis combined with standard questions and clinician’s ratings of ASD risk on a scale from 1 (no risk) to 4 (high risk). | N/A | N/A | N/A | N/A | System accuracy (AUC) range 0.74–0.88 |
| Campbell et al. (2017) [31] | The digital M-CHAT-R/F automatically scored answers provided by parents and presented and scored follow-up questions for secondary screening of medium risk results (score of 3–7). The score report was provided to the physician before the visit. | About 20 min | Prospective study assessing the uptake of the digital MCHAT on service process measures (i.e., accuracy of documentation of screening results and appropriate action for positive screens). Acceptability was also investigated with participating physicians. | N/A | N/A | N/A | N/A | |
| Carpenter et al. (2020) [36] | Short movies presented on a tablet. The embedded tablet camera recorded facial movement so that affect and head position could be subsequently analyzed by means of computer vision analysis. | About 10 min | Proof-of-concept study assessing the feasibility and accuracy of the tablet-based screening procedure. Participants were recruited at their pediatric primary care visit. | N/A | N/A | N/A | N/A | System accuracy (AUC) range 75–83 (including age as covariate) |
| Crippa et al. (2015) [52] | Optic sensors used to track children while performing reaching, grasping, and dropping movements. | No reported | Proof of concept study to test the predictive value of the ML approach comparing the performance of neurotypical children with those of children already diagnosed as autistic. | 82.2% | 89.1 | N/A | N/A | Overall mean classification accuracy (specificity/sensitivity) resulted 84.9 % |
| Downs et al. (2019) [32] | Child Health Improvement Through Computer Automation system (CHICA). Based on EHR information and pre-screen questions answered by parents, CHICA alerts the clinicians to either refer the child for an ASD evaluation or administer the M-CHAT-F (or M-CHAT-R/F). | Multi-phase process | Randomized-controlled trial involving 4 clinics (2 using CHICA with ASD module; 2 using CHICA without ASD module) to assess the percentage of children at the 18-month or 24-month visits. | N/A | N/A | N/A | N/A | None reported |
| Duda et al. (2016) [33] | Caregivers answered to a 7-item questionnaire presented on any digital device. Answers are automatically analyzed by a ML algorithm which classifies children (i.e., at risk; not at risk). | 5–10 min | Prospective study to test the predictive values of the MARA in a clinical sample of children referred for developmental/behavioral concerns and assessed for ASD using a gold standard procedure (ADOS; Bayley; WISC; Vineland). | 89.9% 2 | 79.7% 2 | 67% 2 | 95% 2 | |
| Egger et al. (2018) [25] | iOS-based app running on iPhone/iPad presenting the parents (1) brief questionnaires addressing parental and child’s status (i.e., tantrums), and (2) four short movies to the child. The camera on the device records a video of the child’s face as s/he watches the movies. Caregivers upload either the whole videos of their child or only the facial landmarks. Then, emotions (positive/negative) and attention are automatically encoded. | Not reported | Exploratory study aimed at assessing acceptability and feasibility of the app. Associations of the automatically coded emotions and behaviors with age, sex, and autism risk status (MCHAT score) were assessed. | N/A | N/A | N/A | N/A | |
| Frazier et al. (2018) [38] | Children were shown a series of scenes representing 7 distinct stimulus paradigms (e.g., gaze following and joint attention; abstract shape movement) | 5–10 min 3 | Proof-of-concept study to validate an Autism Risk Index (ARI) and an Autism Severity Index (ASI) using eye tracking metrics. | N/A | N/A | N/A | N/A | ARI test accuracy (AUC) for children < 4years and +4 years was 0.92 and 0.93 respectively. ASI resulted strongly associated with ADOS-2 total severity scores (r = 0.58–0.67) |
| Gong et al. (2018) [53] | The app recorded the vocalizations of children (a) while they played gamified exercises (e.g., reading a story, describing a picture) and (b) in their life environments during everyday communications. | Whole day, multiple days | Proof-of-concept study to assess classification accuracy based on acoustic and language features of children’s vocalization over a 17 month period of use. | N/A | N/A | N/A | N/A | Classification accuracy using unweighted average F1-score was 88.9% |
| Harrington et al. (2013) [34] | M-CHAT on the iPad provided to children’s parents while they were being triaged. | About 2 min 4 | To compare the effectiveness of the M-CHAT on an electronic format versus paper format in an outpatient clinic setting. Parents were also asked to rate their experience with the iPad M-CHAT. The study did not perform follow-up on the final diagnosis of patients who were screened | N/A | N/A | N/A | N/A | |
| Kanne et al. (2018) [39] | Cognoa tool includes (a) 15-item parent-report questionnaire; and (b) a 1–2 min. home video observation of the at-risk child captured via parent smartphone (see also Abbas et al., 2018). | Not reported | The performance of Cognoa in detecting at risk children was compared with ASD screening measures (MCHAT-R/F; SRS; SCQ; CBCL). | 75% 5 | 62% 5 | 83% 5 | 50% 5 | |
| Martineau et al. (2011) [54] | Participants’ eye gaze were monitored while looking at images on a computer screen to obtain a task-evoked pupil measurement and to test differences between dark and light conditions | No reported | Experimental study to test baseline pupil size and pupil responses to visual stimuli (faces, objects, and avatar) in three groups: (1) ASD; (2) age-matched; (3) mental age-matched. | N/A | N/A | N/A | N/A | Pupil size correctly predicted group membership classification in 89% of the participants in the ASD group; in 63% in the mental age-matched group, and in 63% in the chronological age-matched group |
| Moore et al. (2018) [40] | Replication of GeoPref Test (Pierce et al. (2016)) with the inclusion of longer and more complex social scenes. | From 60 s. (Original version) to 90 s. (Complex version) | Experimental study investigating the predictive values of two combined versions of the GeoPref test (Complex/ Original social scenes). | 35% 6 | 94% 6 | 72% 6 | 78% 6 | Classification accuracy (AUC) was 0.75 |
| Oller et al. (2010) [44] | LENA (Language ENvironment Analysis) recording device used to acquire whole day recordings of infants in their natural environments | Whole day | Proof of concept study assessing an automated procedure (i.e., algorithm) to differentiate vocal recordings from neurotypical children, children with language delay, and those with ASD | 75% | 98% | N/A | N/A | The system also differentiated the neurotypical children from a combined autism and language-delay sample (Sp = 90%). |
| Pierce et al. (2016) [41] | GeoPref Test consisting of 2 dynamic images presented side-by-side for a total of 60 s. One side featured a social stimulus (e.g., children dancing); the other side featured short sequences of moving geometric shapes. The side (left/right) of presentation scenes was randomly assigned | 60 s | Cross-sectional explorative study investigating the relationship between percent of viewing time of geometric and social scenes and clinical measures (ADOS; Mullen Scale of Early Learning, and VABS) to assess specificity, sensitivity, and positive/negative predictive values of GeoPref Test. Test-retest was also assessed. | 21% 7 | 98% 7 | 86% 7 | 70% 7 | |
| Ramirez-Duque et al. (2020) [56] | Social robot (ONO) used to elicit and assess joint attention during triadic (i.e., child-therapist-robot) interactions. | Not reported | Proof of concept study assessing differences in joint attention between children with a diagnosis of ASD and children with other neurodevelopmental disorders. | N/A | N/A | N/A | N/A | |
| Schrader et al. (2020) [35] | Smart Early Screening for Autism and Communication Disorders (Smart ESAC). A digital tool including (a) 10-question screen for communication delay, which, if positive, is followed by (b) 20 autism-specific screening questions. | 15–20 min | Pre- and post-Smart ESAC implementation data were compared to assess impact on referral and intervention timing. | 81–84% | 70–89% | N/A | N/A | |
| Talbott et al. (2020) [43] | The Telehealth Evaluation of Development for Infants (TEDI) involves parents’ delivery of semistructured parent–child play interactions using both direct coaching and written materials | Not reported | Feasibility study to assess the use of laboratory/clinical measurements (e.g., AOSI) by parents. | N/A | N/A | N/A | N/A | |
| Tariq et al. (2018) [50] | Families uploaded home videos on an internet server. Then independent non-expert raters tagged features of the videos. Then several ML classifiers were tested to evaluate and quantify risk for ASD. | Raters employed an average of 4 min to score videos. | Different ML classifiers were tested. The most effective one was a 5-feature logistic regression classifier (LR5). The features were expressive language, eye-contact, emotion expression, communicative engagement, and echolalia. | 87.8 % (independent validation) 94.5% (study) | 72.7% (independent validation) 77.4% (study) | N/A | N/A | Classification accuracy was 89% (LR5) |
| Thabtah et al. (2019) [55] | ASDTests is an app based on two short versions of the AQ and Q-CHAT screening methods. It targets 4 age ranges (≤36 months; 4–11 years; 12–16; ≥ 17 years). The app automatically computes the total score of the questionnaires compiled by the caregivers and—if the result is above a specified threshold—refers them a specialized assessment. It also produces a report in PDF. | Not reported | Not reported | 92.8–98% | 91.3–97.3% | N/A | N/A | Classification accuracy was 92.8–97.9% (Naïve Bayes—Logistic Regression). |
| Vargas-Cuentas et al. (2017) [49] | A tablet was used to present a 1-min video displaying a social scene with playing children and an abstract scene with moving shapes on either side of the screen. The child’s face was recorded while watching the video using the tablet’s front camera. Gaze preference was then calculated automatically. | 5–10 min | Proof-of-concept study exploring (a) the performance of the automatic eye gaze detection algorithm compared to manual scoring, and (b) ASD children’s scene preferences. | N/A | N/A | N/A | N/A | The correlation between the manual and the automatic classifications for left/right gaze resulted 73.2%. |
| Wan et al. (2019) [51] | Children had to attend to a muted video clip of a female speaking while their gaze were tracked. | 10 s | Proof-of-concept study comparing gaze fixations of ASD children with those of neurotypical peers to assess accuracy of the test to discriminate between the two groups by means of a machine learning method (support vector machine). | 86.5% 8 | 83.8% 8 | N/A | N/A | Classification accuracy was 85.1% [machine learning with support vector machine]. |
| Wedyan & Al-Jumaily (2016) [45] | Wrist-worn sensors track the arm movement while the infant execute two motor tasks: (a) throw a ball into a tray; (b) fitting the ball into the tube. | Not reported | Explorative study aimed at investigating the overall classification accuracy of the two tasks in classifying the participants (high risk; low risk). | 75%/76.4% | 73.3%/73.3% | N/A | N/A | Accuracy for the two tasks (correctly classified/total sample) was 74.1%/75% |
| Wingfield et al. (2020) [46] | The Pictorial autism assessment schedule (PAAS) is a mobile-based application that can be administered by non-specialist healthcare workers in LMIC at home, to advise if a clinical referral is recommended. It includes 21 yes-no questions and involves ML to automatically detect the risk of ASD. | Not reported | A descriptive study reporting on the preliminary assessment of the accuracy of the PAAC involving a selected sample of children with and without ASD | 88% | 96% | N/A | N/A | Classification accuracy (AUC) was 0.98 |
| Young et al. (2020) [42] | Infant Rating System for Autism (VIRSA) is a web-based application that presents pairs of videos of parents and infants playing together and requires parents to judge which video is most similar to their child. | Average of 56.49 s (SD = 11.49) | Parents completed VIRSA ratings when their child was 6-, 9-, 12-, and 18-months-old and again 2 weeks later to examine test–retest reliability. | 100% 9 | 53% 9 | 0.19% 9 | 100% 9 | (a) Split-half reliability (r = 0.48); (b) test–retest reliability (72% agreement); (c) convergent validity correlation with concurrent ADOS-2 [SARRB algorithm scores at 18 months] (r = −0.36) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Desideri, L.; Pérez-Fuster, P.; Herrera, G. Information and Communication Technologies to Support Early Screening of Autism Spectrum Disorder: A Systematic Review. Children 2021, 8, 93. https://doi.org/10.3390/children8020093
Desideri L, Pérez-Fuster P, Herrera G. Information and Communication Technologies to Support Early Screening of Autism Spectrum Disorder: A Systematic Review. Children. 2021; 8(2):93. https://doi.org/10.3390/children8020093
Chicago/Turabian StyleDesideri, Lorenzo, Patricia Pérez-Fuster, and Gerardo Herrera. 2021. "Information and Communication Technologies to Support Early Screening of Autism Spectrum Disorder: A Systematic Review" Children 8, no. 2: 93. https://doi.org/10.3390/children8020093
APA StyleDesideri, L., Pérez-Fuster, P., & Herrera, G. (2021). Information and Communication Technologies to Support Early Screening of Autism Spectrum Disorder: A Systematic Review. Children, 8(2), 93. https://doi.org/10.3390/children8020093






