The Relationship Between Prenatal Alcohol Exposure and Infant/Child–Caregiver Attachment: A Scoping Review
Abstract
1. Introduction
2. Methods
2.1. Eligibility Criteria
Exclusion Criteria
2.2. Information Sources
2.3. Search and Study Selection
2.4. Data Collection Process and Data Items
Critical Appraisal of Individual Sources of Evidence
2.5. Synthesis Approach
3. Results
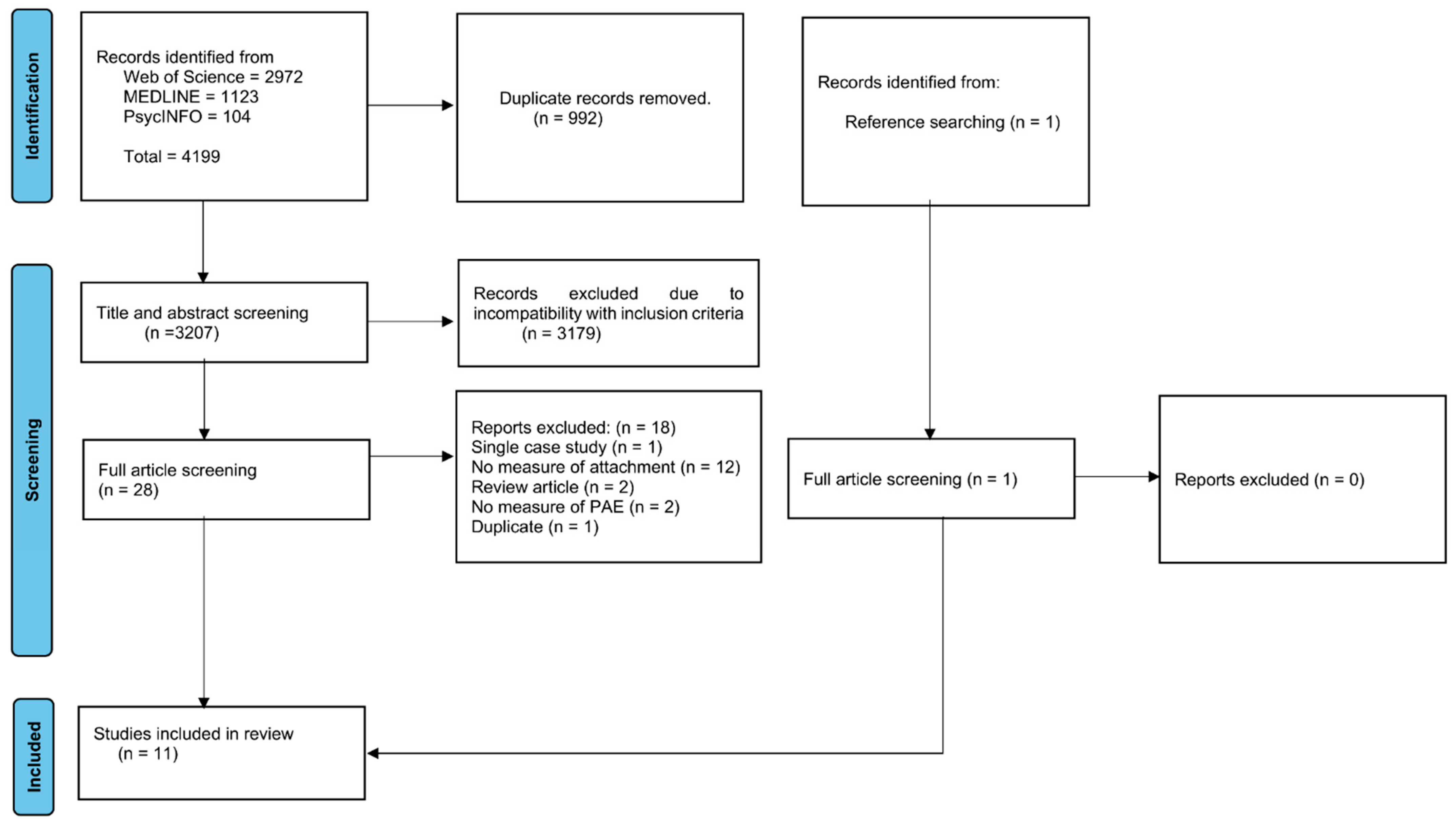
3.1. Study Selection
3.2. Quality of Studies
3.2.1. Measures of PAE and FASD
3.2.2. Measures of Attachment
3.2.3. The Relationship Between PAE/FASD and Attachment Security
3.2.4. Mediating Variables
3.2.5. Other Variables
4. Discussion
5. Practical Implications
6. Limitations and Future Directions
7. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Goodlett, C.R.; Horn, K.H.; Zhou, F.C. Alcohol teratogenesis: Mechanisms of damage and strategies for intervention. Exp. Biol. Med. 2005, 230, 394–406. [Google Scholar] [CrossRef]
- Lipinski, R.J.; Hammond, P.; O’Leary-Moore, S.K.; Ament, J.J.; Pecevich, S.J.; Jiang, Y.; Budin, F.; Parnell, S.E.; Suttie, M.; Godin, E.A. Ethanol-induced face-brain dysmorphology patterns are correlative and exposure-stage dependent. PLoS ONE 2012, 7, e43067. [Google Scholar] [CrossRef]
- Lange, S.; Probst, C.; Gmel, G.; Rehm, J.; Burd, L.; Popova, S. Global prevalence of fetal alcohol spectrum disorder among children and youth: A systematic review and meta-analysis. JAMA Pediatr. 2017, 171, 948–956. [Google Scholar] [CrossRef]
- Cook, J.L.; Green, C.R.; Lilley, C.M.; Anderson, S.M.; Baldwin, M.E.; Chudley, A.E.; Conry, J.L.; LeBlanc, N.; Loock, C.A.; Lutke, J. Fetal alcohol spectrum disorder: A guideline for diagnosis across the lifespan. Can. Med. Assoc. J. 2016, 188, 191–197. [Google Scholar] [CrossRef] [PubMed]
- Goodlett, C.R.; Horn, K.H. Mechanisms of alcohol-induced damage to the developing nervous system. Alcohol Res. Health 2001, 25, 175–184. [Google Scholar] [PubMed]
- Ungerer, M.; Knezovich, J.; Ramsay, M. In utero alcohol exposure, epigenetic changes, and their consequences. Alcohol Res. Curr. Rev. 2013, 35, 37. [Google Scholar]
- McQuire, C.; Daniel, R.; Hurt, L.; Kemp, A.; Paranjothy, S. The causal web of foetal alcohol spectrum disorders: A review and causal diagram. Eur. Child Adolesc. Psychiatry 2020, 29, 575–594. [Google Scholar] [CrossRef]
- Flannigan, K.; Wrath, A.; Ritter, C.; McLachlan, K.; Harding, K.D.; Campbell, A.; Reid, D.; Pei, J. Balancing the story of fetal alcohol spectrum disorder: A narrative review of the literature on strengths. Alcohol. Clin. Exp. Res. 2021, 45, 2448–2464. [Google Scholar] [CrossRef]
- Price, A.; Cook, P.A.; Norgate, S.; Mukherjee, R. Prenatal alcohol exposure and traumatic childhood experiences: A systematic review. Neurosci. Biobehav. Rev. 2017, 80, 89–98. [Google Scholar] [CrossRef]
- Tan, G.K.Y.; Symons, M.; Fitzpatrick, J.; Connor, S.G.; Cross, D.; Pestell, C.F. Adverse childhood experiences, associated stressors and comorbidities in children and youth with fetal alcohol spectrum disorder across the justice and child protection settings in Western Australia. BMC Pediatr. 2022, 22, 587. [Google Scholar] [CrossRef]
- Rockhold, M.N.; Handley, E.D.; Petrenko, C.L.M. Understanding the intersection of prenatal alcohol exposure and postnatal adversity: A systematic review from a developmental psychopathology lens. Alcohol Clin. Exp. Res. 2024, 49, 25–42. [Google Scholar] [CrossRef]
- Popova, S.; Lange, S.; Shield, K.; Burd, L.; Rehm, J. Prevalence of fetal alcohol spectrum disorder among special subpopulations: A systematic review and meta-analysis. Addiction 2019, 114, 1150–1172. [Google Scholar] [CrossRef]
- Del Corral Winder, S.; Rinner, A.; Dickson, A. FASD and Young Children in Foster Care. Child Welf. 2023, 101, 113–140. [Google Scholar]
- Pelech, W.; Badry, D.; Daoust, G. It takes a team: Improving placement stability among children and youth with Fetal Alcohol Spectrum Disorder in care in Canada. Child. Youth Serv. Rev. 2013, 35, 120–127. [Google Scholar] [CrossRef]
- Lange, S.; Shield, K.; Rehm, J.; Popova, S. Prevalence of fetal alcohol spectrum disorders in child care settings: A meta-analysis. Pediatrics 2013, 132, e980–e995. [Google Scholar] [CrossRef] [PubMed]
- Bower, C.; Watkins, R.E.; Mutch, R.C.; Marriott, R.; Freeman, J.; Kippin, N.R.; Safe, B.; Pestell, C.; Cheung, C.S.C.; Shield, H. Fetal alcohol spectrum disorder and youth justice: A prevalence study among young people sentenced to detention in Western Australia. BMJ Open 2018, 8, e019605. [Google Scholar] [CrossRef]
- Mela, M.; Wall, L.; Buttinger, P.; DesRoches, A.; Wrath, A.J. Rates and implications of fetal alcohol spectrum disorder among released offenders with mental disorder in Canada. Behav. Sci. Law 2022, 40, 144–158. [Google Scholar] [CrossRef]
- Brown, N.N.; Gudjonsson, G.; Connor, P. Suggestibility and Fetal Alcohol Spectrum Disorders: I’ll tell you anything you want to hear. J. Psychiatry Law 2011, 39, 39–71. [Google Scholar] [CrossRef]
- Gilbert, D.J.; Allely, C.S.; Gudjonsson, G.; Mukherjee, R.A.S.; Cook, P.A. Immediate and repeat interrogative suggestibility in a sample of adolescents with fetal alcohol spectrum disorder. Divers. Incl. Res. 2024, 1, e12007. [Google Scholar] [CrossRef]
- Gilbert, D.J.; Allely, C.; Mukherjee, R.; Gudjonsson, G.; Novick Brown, N.; Brown, J.; McGinn, V.; Cook, P. An Empirical Examination of Confabulation in Adolescents with Fetal Alcohol Spectrum Disorder (FASD). J. Pediatr. Neuropsychol. 2025. [Google Scholar] [CrossRef]
- Leszko, M.; Keenan-Devlin, L.; Adam, E.K.; Buss, C.; Grobman, W.; Simhan, H.; Wadhwa, P.; Mroczek, D.K.; Borders, A. Are personality traits associated with smoking and alcohol use prior to and during pregnancy? PLoS ONE 2020, 15, e0232668. [Google Scholar] [CrossRef] [PubMed]
- Ordenewitz, L.K.; Weinmann, T.; Schlüter, J.A.; Moder, J.E.; Jung, J.; Kerber, K.; Greif-Kohistani, N.; Heinen, F.; Landgraf, M.N. Evidence-based interventions for children and adolescents with fetal alcohol spectrum disorders–a systematic review. Eur. J. Paediatr. Neurol. 2021, 33, 50–60. [Google Scholar] [CrossRef]
- Goldberg, S.; Muir, R.; Kerry, J. Attachment theory. In Social, Developmental and Clinical Perspectives; Hillsdale: Hillsdale, MI, USA, 1995. [Google Scholar]
- Keller, H. Universality claim of attachment theory: Children’s socioemotional development across cultures. Proc. Natl. Acad. Sci. USA 2018, 115, 11414–11419. [Google Scholar] [CrossRef] [PubMed]
- Bowlby, J. Attachment and Loss; Random House: New York, NY, USA, 1969. [Google Scholar]
- Ainsworth, M.D.S.; Blehar, M.C.; Waters, E.; Wall, S.N. Patterns of Attachment: A Psychological Study of the Strange Situation; Psychology Press: London, UK, 1978. [Google Scholar]
- Main, M.; Solomon, J. Discovery of an insecure-disorganized/disoriented attachment pattern. In Affective Development in Infancy; Brazelton, T.B., Yogman, M.W., Eds.; Ablex Publishing: New York, NY, USA, 1986; pp. 95–124. [Google Scholar]
- Cyr, C.; Euser, E.M.; Bakermans-Kranenburg, M.J.; Van Ijzendoorn, M.H. Attachment security and disorganization in maltreating and high-risk families: A series of meta-analyses. Dev. Psychopathol. 2010, 22, 87–108. [Google Scholar] [CrossRef]
- Crowell, J.A.; Treboux, D. A review of adult attachment measures: Implications for theory and research. Soc. Dev. 1995, 4, 294–327. [Google Scholar] [CrossRef]
- Jewell, T.; Gardner, T.; Susi, K.; Watchorn, K.; Coopey, E.; Simic, M.; Fonagy, P.; Eisler, I. Attachment measures in middle childhood and adolescence: A systematic review of measurement properties. Clin. Psychol. Rev. 2019, 68, 71–82. [Google Scholar] [CrossRef]
- Carretero-Dios, H.; Pérez, C. Standards for the development and review of instrumental studies: Considerations about test selection in psychological research. Int. J. Clin. Health Psychol. 2007, 7, 863–882. [Google Scholar]
- Acevedo-Polakovich, I.D.; Reynaga-Abiko, G.; Garriott, P.O.; Derefinko, K.J.; Wimsatt, M.K.; Gudonis, L.C.; Brown, T.L. Beyond instrument selection: Cultural considerations in the psychological assessment of US Latinas/os. Prof. Psychol. Res. Pract. 2007, 38, 375. [Google Scholar] [CrossRef]
- Waters, E.; Hamilton, C.E.; Weinfield, N.S. The stability of attachment security from infancy to adolescence and early adulthood: General introduction. Child Dev. 2000, 71, 678–683. [Google Scholar] [CrossRef]
- Fraley, R.C.; Roisman, G.I. The development of adult attachment styles: Four lessons. Curr. Opin. Psychol. 2019, 25, 26–30. [Google Scholar] [CrossRef] [PubMed]
- Ranson, K.E.; Urichuk, L.J. The effect of parent–child attachment relationships on child biopsychosocial outcomes: A review. Early Child Dev. Care 2008, 178, 129–152. [Google Scholar] [CrossRef]
- Jethava, V.; Kadish, J.; Kakonge, L.; Wiseman-Hakes, C. Early attachment and the development of social communication: A neuropsychological approach. Front. Psychiatry 2022, 13, 838950. [Google Scholar] [CrossRef] [PubMed]
- Tryphonopoulos, P.D.; Letourneau, N.; Ditommaso, E. Attachment and caregiver-infant interaction: A review of observational-assessment tools. Infant Ment. Health J. 2014, 35, 642–656. [Google Scholar] [CrossRef]
- Delius, A.; Bovenschen, I.; Spangler, G. The inner working model as a “theory of attachment”: Development during the preschool years. Attach. Hum. Dev. 2008, 10, 395–414. [Google Scholar] [CrossRef] [PubMed]
- Biringen, Z.; Altenhofen, S.; Aberle, J.; Baker, M.; Brosal, A.; Bennett, S.; Coker, E.; Lee, C.; Meyer, B.; Moorlag, A. Emotional availability, attachment, and intervention in center-based child care for infants and toddlers. Dev. Psychopathol. 2012, 24, 23–34. [Google Scholar] [CrossRef]
- Potter-Dickey, A.; Letourneau, N.; de Koning, A.P.J. Associations between neurodevelopmental disorders and attachment patterns in preschool-aged children: Systematic review. Curr. Dev. Disord. Rep. 2020, 7, 277–289. [Google Scholar] [CrossRef]
- Beckman, L.; Janson, S.; von Kobyletzki, L. Associations between neurodevelopmental disorders and factors related to school, health, and social interaction in schoolchildren: Results from a Swedish population-based survey. Disabil. Health J. 2016, 9, 663–672. [Google Scholar] [CrossRef]
- Eiden, R.D.; Edwards, E.P.; Leonard, K.E. Predictors of effortful control among children of alcoholic and nonalcoholic fathers. J. Stud. Alcohol 2004, 65, 309–319. [Google Scholar] [CrossRef] [PubMed]
- Rockhold, M.N.; Kautz-Turnbull, C.; Handley, E.D.; Petrenko, C.L.M. The trauma experiences of children with fetal alcohol spectrum disorders: Developmental outcomes utilizing a threat/deprivation child adversity framework. Alcohol Clin. Exp. Res. 2023, 47, 1722–1735. [Google Scholar] [CrossRef]
- Kambeitz, C.; Klug, M.G.; Greenmyer, J.; Popova, S.; Burd, L. Association of adverse childhood experiences and neurodevelopmental disorders in people with fetal alcohol spectrum disorders (FASD) and non-FASD controls. BMC Pediatr. 2019, 19, 498. [Google Scholar] [CrossRef]
- Mattson, J.T.; Thorne, J.C.; Kover, S.T. Parental interaction style, child engagement, and emerging executive function in fetal alcohol spectrum disorders (FASD). Child Neuropsychol. 2022, 28, 853–877. [Google Scholar] [CrossRef] [PubMed]
- Lowe, J.; Handmaker, N.; Aragón, C. Impact of mother interactive style on infant affect among babies exposed to alcohol in utero. Infant Ment. Health J. 2006, 27, 371–382. [Google Scholar] [CrossRef] [PubMed]
- Dozier, M.; Lindhiem, O.; Lewis, E.; Bick, J.; Bernard, K.; Peloso, E. Effects of a foster parent training program on young children’s attachment behaviors: Preliminary evidence from a randomized clinical trial. Child Adolesc. Soc. Work J. 2009, 26, 321–332. [Google Scholar] [CrossRef]
- Lieberman, A.F.; Weston, D.R.; Pawl, J.H. Preventive intervention and outcome with anxiously attached dyads. Child Dev. 1991, 62, 199–209. [Google Scholar] [CrossRef]
- Kohlhoff, J.; Lieneman, C.; Cibralic, S.; Traynor, N.; McNeil, C.B. Attachment-based parenting interventions and evidence of changes in toddler attachment patterns: An overview. Clin. Child Fam. Psychol. Rev. 2022, 25, 737–753. [Google Scholar] [CrossRef]
- Spieker, S.J.; Oxford, M.L.; Kelly, J.F.; Nelson, E.M.; Fleming, C.B. Promoting first relationships: Randomized trial of a relationship-based intervention for toddlers in child welfare. Child Maltreatment 2012, 17, 271–286. [Google Scholar] [CrossRef] [PubMed]
- Munn, Z.; Peters, M.D.J.; Stern, C.; Tufanaru, C.; McArthur, A.; Aromataris, E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med. Res. Methodol. 2018, 18, 143. [Google Scholar] [CrossRef]
- Anderson, S.; Allen, P.; Peckham, S.; Goodwin, N. Asking the right questions: Scoping studies in the commissioning of research on the organisation and delivery of health services. Health Res. Policy Syst. 2008, 6, 7. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L. PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef]
- Gusenbauer, M.; Haddaway, N.R. Which academic search systems are suitable for systematic reviews or meta-analyses? Evaluating retrieval qualities of Google Scholar, PubMed, and 26 other resources. Res. Synth. Methods 2020, 11, 181–217. [Google Scholar] [CrossRef] [PubMed]
- Babineau, J. Product review: Covidence (systematic review software). J. Can. Health Libr. Assoc. 2014, 35, 68–71. [Google Scholar] [CrossRef]
- O’Connor, M.J.; Sigman, M.; Brill, N. Disorganization of attachment in relation to maternal alcohol consumption. J. Consult. Clin. Psychol. 1987, 55, 831–836. [Google Scholar] [CrossRef]
- Wilson, J. Stability of Attachment Classification from One to Six Years of Age in a Sample at Risk for Disorganized Attachment; University of California, Los Angeles: Los Angeles, CA, USA, 1990. [Google Scholar]
- O’Connor, M.J.; Sigman, M.; Kasari, C. Attachment behavior of infants exposed prenatally to alcohol: Mediating effects of infant affect and mother-infant interaction. Dev. Psychopathol. 1992, 4, 243–256. [Google Scholar] [CrossRef]
- Swanson, K.; Beckwith, L.; Howard, J. Intrusive caregiving and quality of attachment in prenatally drug-exposed toddlers and their primary caregivers. Attach. Hum. Dev. 2000, 2, 130–148. [Google Scholar] [CrossRef]
- O’Connor, M.J.; Kogan, N.; Findlay, R. Prenatal alcohol exposure and attachment behavior in children. Alcohol. Clin. Exp. Res. 2002, 26, 1592–1602. [Google Scholar] [CrossRef]
- Farina, L.; Leifer, M.; Chasnoff, I.J. Attachment and behavioural difficulties in internationally adopted Russian children. Adopt. Foster. 2004, 28, 38–49. [Google Scholar] [CrossRef]
- Yumoto, C. Attachment representation in inner-city African American adolescents. Diss. Abstr. Int. Sect. B Sci. Eng. 2008, 68, 7682. [Google Scholar]
- Bergin, C.; McCollough, P. Attachment in substance-exposed toddlers: The role of caregiving and exposure. Infant Ment. Health J. Off. Publ. World Assoc. Infant Ment. Health 2009, 30, 407–423. [Google Scholar] [CrossRef]
- Rossen, L.; Hutchinson, D.; Wilson, J.; Burns, L.; Olsson, C.A.; Allsop, S.; Elliott, E.J.; Jacobs, S.; Macdonald, J.A.; Mattick, R.P. Predictors of postnatal mother-infant bonding: The role of antenatal bonding, maternal substance use and mental health. Arch. Womens Ment. Health 2016, 19, 609–622. [Google Scholar] [CrossRef]
- Kornaszewska-Polak, M.; Klecka, M.; Janas-Kozik, M.; Palicka, I. Quality of attachment in adults diagnosed with foetal alcohol syndrome. Psychiatr. Psychol. Klin. J. Psychiatry Clin. Psychol. 2019, 19, 165–176. [Google Scholar] [CrossRef]
- Kemp, A. Attachment and Emotion Regulation in Adolescents with FAS-Dysmorphism; University of CapeTown: Cape Town, South Africa, 2021. [Google Scholar]
- NIH. Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies. 2013. Available online: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools (accessed on 15 May 2021).
- Lisy, K.; Porritt, K. Narrative synthesis: Considerations and challenges. JBI Evid. Implement. 2016, 14, 201. [Google Scholar] [CrossRef]
- Popay, J.; Roberts, H.; Sowden, A.; Petticrew, M.; Arai, L.; Rodgers, M.; Britten, N.; Roen, K.; Duffy, S. Guidance on the conduct of narrative synthesis in systematic reviews. Prod. ESRC Methods Progr. Version 2006, 1, b92. [Google Scholar]
- Trombetta, T.; Giordano, M.; Santoniccolo, F.; Vismara, L.; Della Vedova, A.M.; Rollè, L. Pre-natal attachment and parent-to-infant attachment: A systematic review. Front. Psychol. 2021, 12, 620942. [Google Scholar] [CrossRef] [PubMed]
- Day, N.L.; Robles, N. Methodological issues in the measurement of substance use. Ann. N. Y. Acad. Sci. 1989, 562, 8–13. [Google Scholar] [CrossRef] [PubMed]
- Astley, S.J. Diagnostic Guide for Fetal Alcohol Spectrum Disorders: The 4-Digit Diagnostic Code; University of Washington: Washington, DC, USA, 2004. [Google Scholar]
- Hoyme, H.E.; May, P.A.; Kalberg, W.O.; Kodituwakku, P.; Gossage, J.P.; Trujillo, P.M.; Buckley, D.G.; Miller, J.H.; Aragon, A.S.; Khaole, N. A practical clinical approach to diagnosis of fetal alcohol spectrum disorders: Clarification of the 1996 institute of medicine criteria. Pediatrics 2005, 115, 39–47. [Google Scholar] [CrossRef]
- Klagsbrun, M.; Bowlby, J. Responses to separation from parents: A clinical test for young children. Br. J. Proj. Psychol. Personal. Study 1976, 21, 7–27. [Google Scholar]
- Crawley, S.B.; Spiker, D. Mother-child interactions involving two-year-olds with Down syndrome: A look at individual differences. Child Dev. 1983, 54, 1312–1323. [Google Scholar] [CrossRef]
- Waters, E.; Deane, K.E. Defining and assessing individual differences in attachment relationships: Q-methodology and the organization of behavior in infancy and early childhood. Monogr. Soc. Res. Child Dev. 1985, 50, 41–65. [Google Scholar] [CrossRef]
- Chisholm, K. A three year follow-up of attachment and indiscriminate friendliness in children adopted from Romanian orphanages. Child Dev. 1998, 69, 1092–1106. [Google Scholar] [CrossRef]
- Target, M.; Fonagy, P.; Shmueli-Goetz, Y. Attachment representations in school-age children: The development of the Child Attachment Interview (CAI). J. Child Psychother. 2003, 29, 171–186. [Google Scholar] [CrossRef]
- Condon, J.T. The assessment of antenatal emotional attachment: Development of a questionnaire instrument. Br. J. Med. Psychol. 1993, 66, 167–183. [Google Scholar] [CrossRef] [PubMed]
- Condon, J.T.; Corkindale, C.J. The assessment of parent-to-infant attachment: Development of a self-report questionnaire instrument. J. Reprod. Infant Psychol. 1998, 16, 57–76. [Google Scholar] [CrossRef]
- Lubiewska, K.; Głogowska, K.; Mickiewicz, K.; Wojtynkiewicz, E.; Izdebski, P.; Wiśniewski, C. Skala Experience in Close Relationships-Revised: Struktura, rzetelność oraz skrócona wersja skali w polskiej próbie. Psychol. Rozw. 2016, 21, 49. [Google Scholar]
- Roque, L.; Veríssimo, M.; Fernandes, M.; Rebelo, A. Emotion regulation and attachment: Relationships with children’s secure base, during different situational and social contexts in naturalistic settings. Infant Behav. Dev. 2013, 36, 298–306. [Google Scholar] [CrossRef]
- Creeden, K. How trauma and attachment can impact neurodevelopment: Informing our understanding and treatment of sexual behaviour problems. J. Sex. Aggress. 2009, 15, 261–273. [Google Scholar] [CrossRef]
- Shaw, S.K.; Dallos, R. Attachment and adolescent depression: The impact of early attachment experiences. Attach. Hum. Dev. 2005, 7, 409–424. [Google Scholar] [CrossRef]
- Rutgers, A.H.; Bakermans-Kranenburg, M.J.; van Ijzendoorn, M.H.; van Berckelaer-Onnes, I.A. Autism and attachment: A meta-analytic review. J. Child Psychol. Psychiatry 2004, 45, 1123–1134. [Google Scholar] [CrossRef]
- Rutgers, A.H.; Van Ijzendoorn, M.H.; Bakermans-Kranenburg, M.J.; Swinkels, S.H.N.; Van Daalen, E.; Dietz, C.; Naber, F.B.A.; Buitelaar, J.K.; Van Engeland, H. Autism, attachment and parenting: A comparison of children with autism spectrum disorder, mental retardation, language disorder, and non-clinical children. J. Abnorm. Child Psychol. 2007, 35, 859–870. [Google Scholar] [CrossRef][Green Version]
- Gregory, G.; Reddy, V.; Young, C. Identifying children who are at risk of FASD in Peterborough: Working in a community clinic without access to gold standard diagnosis. Adopt. Foster. 2015, 39, 225–234. [Google Scholar] [CrossRef]
- Mukherjee, R.; Wray, E.; Commers, M.; Hollins, S.; Curfs, L. The impact of raising a child with FASD upon carers: Findings from a mixed methodology study in the UK. Adopt. Foster. 2013, 37, 43–56. [Google Scholar] [CrossRef]
- Mohamed, Z.; Carlisle, A.C.S.; Livesey, A.C.; Mukherjee, R.A.S. Carer stress in Fetal Alcohol Spectrum Disorders: The implications of data from the UK national specialist FASD clinic for training carers. Adopt. Foster. 2020, 44, 242–254. [Google Scholar] [CrossRef]
- Price, A.D.; Mukherjee, R.A.S.; Webster, A.; Tate, D.; Allely, C.S.; Brown, S.; Buckard, J.; Burd, L.; Butcher, S.; Shields, J. Development and pre-feasibility testing of specific: A psychoeducation programme for caregivers of children with fetal alcohol spectrum disorder (FASD). J. Child Fam. Stud. 2023, 32, 3026–3041. [Google Scholar] [CrossRef]
- Kodituwakku, P.; Kodituwakku, E. Cognitive and behavioral profiles of children with fetal alcohol spectrum disorders. Curr. Dev. Disord. Rep. 2014, 1, 149–160. [Google Scholar] [CrossRef]
- Pidano, A.E.; Allen, A.R. The Incredible Years series: A review of the independent research base. J. Child Fam. Stud. 2015, 24, 1898–1916. [Google Scholar] [CrossRef]
- Petrenko, C.L.M.; Pandolfino, M.E.; Roddenbery, R. The Association Between Parental Attributions of Misbehavior and Parenting Practices in Caregivers Raising Children with Prenatal Alcohol Exposure: A Mixed-Methods Study. Res. Dev. Disabil. 2016, 59, 255–267. [Google Scholar] [CrossRef] [PubMed]
- Cheang, R.T.S.; Skjevling, M.; Blakemore, A.I.F.; Kumari, V.; Puzzo, I. Do you feel me? Autism, empathic accuracy and the double empathy problem. Autism 2024, 29, 2315–2327. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, P.; Sheppard, E.; Cassidy, S. Autism and the double empathy problem: Implications for development and mental health. Br. J. Dev. Psychol. 2021, 39, 1–18. [Google Scholar] [CrossRef]
- Price, A.; Allely, C.; Mukherjee, R. Fetal alcohol spectrum disorders: Where we have come from, trends, and future directions. Minerva Pediatr. 2024, 77, 68–86. [Google Scholar] [CrossRef]
- Patel, M.; Agnihotri, S.; Hawkins, C.; Levin, L.; Goodman, D.; Simpson, A. Identifying Fetal Alcohol Spectrum Disorder and psychiatric comorbidity for children and youth in care: A community approach to diagnosis and treatment. Child. Youth Serv. Rev. 2020, 108, 104606. [Google Scholar] [CrossRef]
- Popova, S.; Lange, S.; Shield, K.; Mihic, A.; Chudley, A.E.; Mukherjee, R.A.S.; Bekmuradov, D.; Rehm, J. Comorbidity of fetal alcohol spectrum disorder: A systematic review and meta-analysis. Lancet 2016, 387, 978–987. [Google Scholar] [CrossRef]
- Minnis, H. Abuse, neglect and neurodevelopment across the life course: What can paediatricians and child psychiatrists do about this together? The Illingworth-Rees keynote lecture 2023. Arch. Dis. Child. 2024, 109, 533–535. [Google Scholar] [CrossRef] [PubMed]
- Corrales-Gutierrez, I.; Gomez-Baya, D.; Leon-Larios, F.; Medero-Canela, R.; Marchei, E.; Mendoza-Berjano, R.; García-Algar, Ó. Alcohol consumption assessed by a biomarker and self-reported drinking in a sample of pregnant women in the south of Europe: A comparative study. Toxics 2023, 11, 930. [Google Scholar] [CrossRef]
- Gilbert, D.J.; Mukherjee, R.A.S.; Kassam, N.; Cook, P.A. Exploring the experiences of social workers in working with children suspected to have fetal alcohol spectrum disorders. Adopt. Foster. 2021, 45, 155–172. [Google Scholar] [CrossRef]
- HomeOffice. Advisory Council on the Misuse of Drugs. Hidden Harm—Responding to the Needs of Children of Problem Drug Users. 2003. Available online: https://www.gov.uk/government/publications/amcd-inquiry-hidden-harm-report-on-children-of-drug-users (accessed on 17 February 2025).
- Petrenko, C.L.M.; Tahir, N.; Mahoney, E.C.; Chin, N.P. Prevention of Secondary Conditions in Fetal Alcohol Spectrum Disorders: Identification of Systems-Level Barriers. Matern. Child Health J. 2014, 18, 1496–1505. [Google Scholar] [CrossRef] [PubMed]
- Streissguth, A.P.; Bookstein, F.L.; Barr, H.M.; Sampson, P.D.; O’Malley, K.; Young, J.K. Risk factors for adverse life outcomes in fetal alcohol syndrome and fetal alcohol effects. J. Dev. Behav. Pediatr. 2004, 25, 228–238. [Google Scholar] [CrossRef] [PubMed]
- Kautz-Turnbull, C.; Adams, T.R.; Petrenko, C.L.M. The strengths and positive influences of children with fetal alcohol spectrum disorders. Am. J. Intellect. Dev. Disabil. 2022, 127, 355–368. [Google Scholar] [CrossRef]
- Kully-Martens, K.; McNeil, A.; Pei, J.; Rasmussen, C. Toward a strengths-based cognitive profile of children with fetal alcohol spectrum disorders: Implications for intervention. Curr. Dev. Disord. Rep. 2022, 9, 53–62. [Google Scholar] [CrossRef]
| Reference Location | Sample | Design | Aims | Measures | Results |
|---|---|---|---|---|---|
| [56] California, USA | N = 46 mother–infant dyads. Infants aged 12 months, mothers aged 30+ Predominantly white (92%), highly educated (72% college or more education) and middle class (100%). | Cross-sectional | To assess relationships between amount of alcohol consumed by mothers before and during pregnancy and attachment styles in infants at 12 months | Alcohol consumption in pregnancy was measured by self-report questionnaire at 12 months postpartum. Attachment was determined using the SSP—infants were categorised as either securely attached, insecure–resistant, insecure–avoidant, or disorganised. | Higher PAE scores in insecure attachment group. |
| [57] California, USA | 41 mother (30+ years) child (5–6 years) dyads from the same sample as [56]. Mothers were 88% white, 64% college educated, 100% middle class, and their average IQ score was 117. | Follow-up, cross-sectional. | To assess the consistency of attachment classifications measured at 12 months using the Strange Situation Procedure and at 5–6 years using the Separation Anxiety Test (SAT). To measure the relationship between prenatal alcohol exposure and attachment style in children aged 5–6 using the SAT. | Attachment style was measured with the Separation Anxiety Test. PAE was measured by maternal self-report. | SSP at 1 year and SAT at 6 years did not result in the same attachment categorisations. No relationship between SAT classifications and PAE. |
| [58] California, USA | N = 44 firstborn infants (aged 1 year) of middle-class (100%) mothers aged 30+. English-speaking (first language), highly educated participants, with 70% who have achieved college or postgraduate education | Cross-sectional | To investigate possible mechanisms between PAE and insecure/disorganised attachment using structural equation modelling, including infant irritability, postnatal alcohol consumption, and mother-infant interaction. Attachment category was the dependant variable. | Alcohol consumption during and after pregnancy was measured by self-report questionnaire and operationalised as average drinks per drinking occasion. Child and maternal behaviours were rated using the Mother–Child Rating Scales. Attachment style was determined using the SSP. Attachment was dichotomous (secure or not), and alcohol was measured as average drinks per drinking occasion. Smoking and caffeine use during pregnancy were also measured. | Best-fitting model identified through structural equation modelling: PAE, negative infant affect, maternal responsiveness, less secure attachment. |
| [59] California, USA | N = 51 mother–toddler (aged 18 months) dyads. Participants’ mean age was 27.80 (range: 19–45), with time spent in education (mean: 11.24; range: 7–14). 39.2% were employed, and 82.4% were from minoritised ethnic groups. | Cross-sectional | To examine the relationships between prenatal substance exposure, current substance use, caregiver sensitivity and hostility, and attachment styles. | Substance use was measured using self-report. Attachment was determined using the SSP. | PAE by maternal report was not associated with attachment classification. |
| [60] California, USA | 42 children (aged 4–5 years) of low-income ‘high-risk’ mothers. Mothers were English-speaking with age range of 21–44 years. Majority were high school graduates (38%), followed by those who have had some college education (31%). Five percent were college graduates, and 26% were non-high school graduates. Ethnicity-wise, 83% were African Americans, followed by seven percent Hispanics and 10% from ‘other’ ethnicities. | Cross-sectional | Used structural equation modelling to test the hypothesis that higher PAE would be related to insecure/disorganised attachment styles via infant negative affect and less-optimal mother–child interaction. | PAE was measured by interview and operationalised as maximum number of drinks per drinking session. Attachment style was measured using the Attachment Q-Set. Mother supportive presence, child negative affect, and child coping were measured using the Family Interaction Puzzle Task. | PAE predicted negative child affect, insecure attachment and lower levels of maternal emotional support of the child. When mothers of PAE children provided high levels of support, children had better coping skills and more secure attachment. |
| [61] Illinois, USA | 29 Russian children (age 1–7) adopted by US families. 10 of the children were diagnosed with “an ARND”. 21% of the mothers completed high school (12th grade), followed by 14% who undertook one or two years of undergraduate studies; 21% had four years of undergraduate education, and 43% completed graduate education (one to three years). | Cross-sectional | To assess relationships between parenting stress, attachment security, child behavioural difficulties, length of institutionalisation, and ARNDs. | Attachment was measured using the caregiver-report Attachment Security Questionnaire. The children either had a diagnosis of ARND or they did not. But it is unclear how/when/where they were assessed, which criteria were used, or whether any of the non-diagnosed children had PAE. | Parenting stress was significantly correlated with insecure attachment and increased child behavioural difficulties. Attachment insecurity was significantly correlated with the severity of behaviour problems. No differences were found with regard to gender or diagnosis of ARND. |
| [62] Michigan, USA | N = 130 inner-city, African American adolescents (mean age = 14.3 years). Mothers were Low SES, 75% were unmarried, and their average number of years of education was 12.6. | Cross-sectional follow-up. Mothers had been recruited during pregnancy. | To assess the relationships between PAE, childhood trauma, attachment, and behavioural functioning in adolescents. | PAE measured by maternal interview during pregnancy. Attachment measured in adolescents using the Child Attachment Interview. | PAE was not related to attachment classification, but severity of maternal drinking problems during pregnancy did predict disorganised attachment. |
| [63] Ohio, USA | Low-income (“high risk”) mothers (n = 41) with their substance-exposed 12-month-olds. Majority of participants with substance exposed toddlers received Medicaid due to poverty (93%) and were of African American origin (86%). | Matched pairs | Substance-exposed infants were compared with a nonexposed group matched for other risk factors (poverty, race, gender, gestational age, birth weight, mothers’ age at delivery, and parity). Outcomes measured were attachment, maternal sensitivity, quality of caregiving. | PAE was measured with urine toxicology at antenatal care and postnatally, as well as by interview. Maternal sensitivity and involvement were analysed from 2 h of videotaped interaction. Attachment was assessed using the Attachment Q-Set. | Attachment security and quality of caregiving were quite low for both groups, with no significant differences. Regression analyses revealed that quality of caregiving predicted attachment, but amount of alcohol and cocaine exposure did not. |
| [64] Rossen 2016 New South Wales and Western Australia, Australia | 372 pregnant women (data collected throughout pregnancy and at 8 weeks postpartum) Maternal age (median) was 33.0 years; 1.1% had indigenous background and 2.5% were indigenous, and 41.1% were born overseas. | Cross-sectional | To assess the relationships between pre- and post-natal bonding between mothers and infants, and the impact of substance use on bonding. | Mothers’ feelings of attachment towards their infant were measured using the Maternal Antenatal Attachment Scale, and Maternal Postnatal Attachment Scale. Depression and anxiety were measured using the Edinburgh Antenatal and Postnatal Depression Scale and the Depression and Anxiety Scales. Information about alcohol and drug use was collected from mothers at each trimester and eight weeks postpartum. | Higher antenatal bonding predicted higher postnatal bonding. Maternal depressive symptoms in pregnancy predicted better mother-infant bonding 8 weeks. No evidence that alcohol use during pregnancy is associated with postpartum bonding (alcohol tended to be low level). |
| [65] Silesian Voivodeship, Poland | Young adults with foetal alcohol syndrome (n = 30) and control group without FAS (n = 30, although in places n = 39) Participants with confirmed FASD | Case-control with longitudinal follow-up | Longitudinal design. | FAS in children was diagnosed using the 4-digit code system between 1990 and 2000. Attachment style in young adults was assessed with the Polish version of the Experience in Close Relationships—Revised questionnaire in 2017. | Adults diagnosed with FAS achieved higher scores in insecure attachment than adults without FAS. |
| [66] Western Cape, South Africa | N = 77 adolescents in total: 50 with FASD, 27 controls with minimal or no PAE. | Cross-sectional follow-up study | To examine the association between FASD facial dysmorphism and insecure, as well as disorganised, attachment. To examine the extent to which FASD facial dysmorphism was associated with emotion regulation difficulties in adolescence after controlling for the effects of attachment security in infancy. | Attachment measured using the Strange Situation Procedure. FASD dysmorphism assessed clinically by specialist dysmorphologists using the Institute of Medicine Criteria. | No difference in attachment security between dysmorphic and non-dysmorphic groups. Did not compare FASD and control groups on attachment security using a statistical test, but the control group did have the highest rate of secure attachment. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gilbert, D.J.; Price, A.D.; Cook, P.A.; Mukherjee, R.A.S. The Relationship Between Prenatal Alcohol Exposure and Infant/Child–Caregiver Attachment: A Scoping Review. Children 2025, 12, 1133. https://doi.org/10.3390/children12091133
Gilbert DJ, Price AD, Cook PA, Mukherjee RAS. The Relationship Between Prenatal Alcohol Exposure and Infant/Child–Caregiver Attachment: A Scoping Review. Children. 2025; 12(9):1133. https://doi.org/10.3390/children12091133
Chicago/Turabian StyleGilbert, David J., Alan D. Price, Penny A. Cook, and Raja A. S. Mukherjee. 2025. "The Relationship Between Prenatal Alcohol Exposure and Infant/Child–Caregiver Attachment: A Scoping Review" Children 12, no. 9: 1133. https://doi.org/10.3390/children12091133
APA StyleGilbert, D. J., Price, A. D., Cook, P. A., & Mukherjee, R. A. S. (2025). The Relationship Between Prenatal Alcohol Exposure and Infant/Child–Caregiver Attachment: A Scoping Review. Children, 12(9), 1133. https://doi.org/10.3390/children12091133






