Defining Goal-Directed Training for Children with Cerebral Palsy: A Scoping Review and Framework for Implementation
Abstract
Highlights
- Defines and synthesizes the core components of Goal-Directed Therapy (GDT) for children with cerebral palsy through a comprehensive scoping review.
- Identifies measurable benefits of GDT across ICF domains, including motor function, self-care, communication, and participation, based on evidence from 112 intervention studies.
- Proposes a structured eight-step GDT framework to support therapists in implementing GDT with fidelity across settings and severity levels.
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol and Registration
2.2. Eligibility Criteria
2.3. Information Sources
2.4. Search Strategy
2.5. Selection of Sources of Evidence
2.6. Data Charting Process
2.7. Synthesis of Results
3. Results
3.1. Selection of Sources of Evidence
3.2. Characteristics of Sources of Evidence
3.3. Study Participants
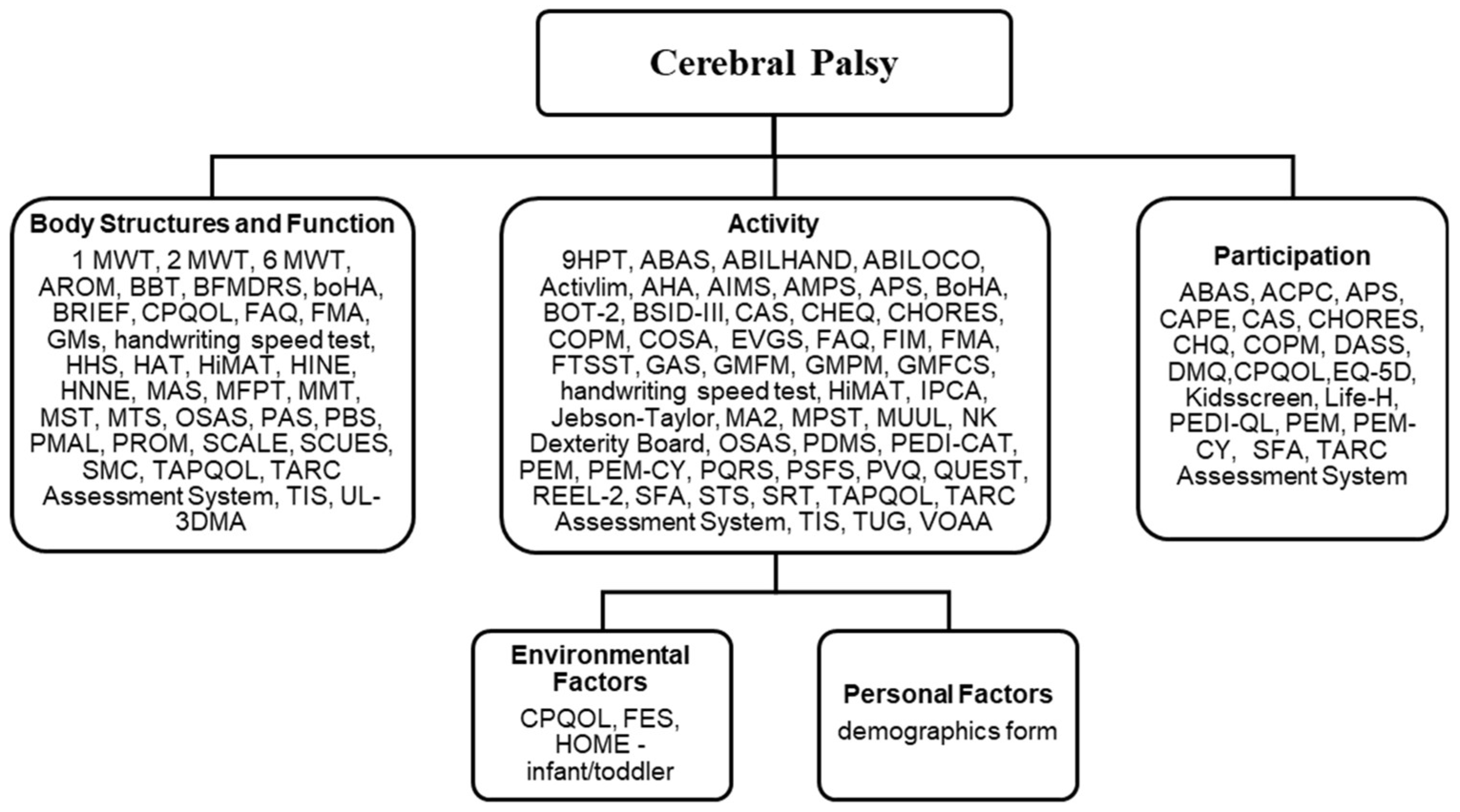
3.4. Outcome Measures and ICF Domains
3.5. Impact of GDT
3.6. Key Themes Identified in GDT Intervention
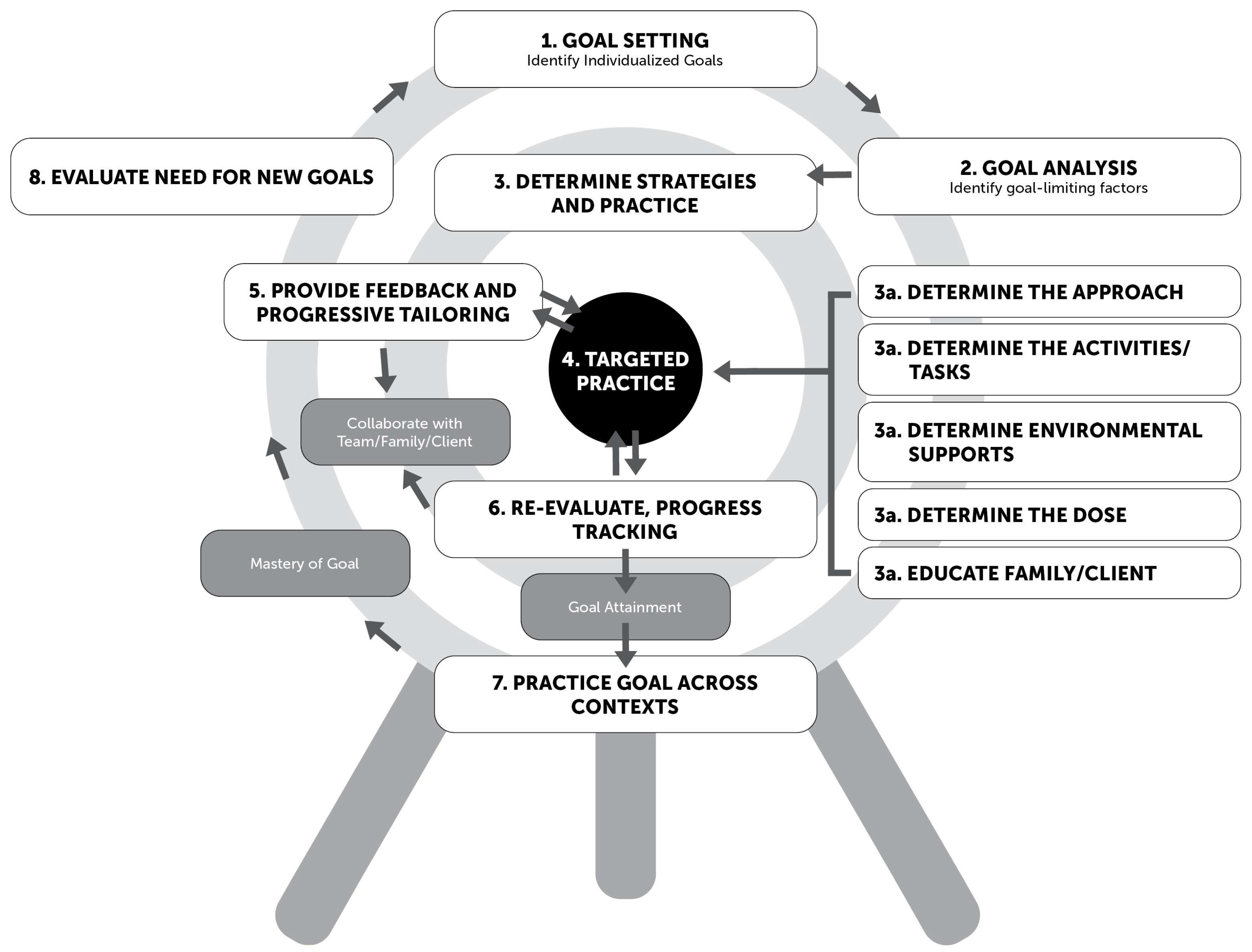
3.7. GDT Framework
4. Discussion
4.1. Collaborative Goal Setting
4.2. Family-Centered Practice
4.3. Specific Training Techniques
4.4. Therapy Dose
4.5. Social Engagement
4.6. Multidisciplinary Approaches
4.7. Outcome Monitoring and Alignment with ICF Domains
4.8. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rosenbaum, P.; Paneth, N.; Leviton, A.; Goldstein, M.; Bax, M.; Damiano, D.; Dan, B.; Jacobsson, B. A report: The definition and classification of cerebral palsy April 2006. Dev. Med. Child Neurol. Suppl. 2007, 109, 8–14. [Google Scholar] [PubMed]
- Jackman, M.; Sakzewski, L.; Morgan, C.; Boyd, R.N.; Brennan, S.E.; Langdon, K.; Toovey, R.A.M.; Greaves, S.; Thorley, M.; Novak, I. Interventions to improve physical function for children and young people with cerebral palsy: International clinical practice guideline. Dev. Med. Child Neurol. 2022, 64, 536–549. [Google Scholar] [CrossRef] [PubMed]
- Novak, I.; Paton, M.C.; Finch-Edmondson, M.; Badawi, N.; Fahey, M.; Velde, A.; Hines, A.; Dark, L.; Khamis, A.; Mc Namara, M. Commentary and clinical implications of “state of the evidence traffic lights 2019: Systematic review of interventions for preventing and treating children with cerebral palsy”. J. Exp. Neurol. 2021, 2, 112. [Google Scholar]
- Jackman, M.; Thorley, M.; Toovey, R.; Burgess, A.; Blatch-Williams, R.; Sakzewski, L.; Boyd, R.N.; Novak, I. Implementing Clinical Practice Guidelines for Improving Function in Cerebral Palsy: Development of a Fidelity Tool. Pediatr. Phys. Ther. 2025, 37, 4–13. [Google Scholar] [CrossRef]
- Ogilvie, L.; Garbellini, S.; Sakzewski, L.; Davidson, S.-A.; Elliottt, C. Key elements of Goal-Directed Training for children with cerebral palsy: A qualitative content analysis. Br. J. Occup. Ther. 2025, 88, 17–24. [Google Scholar] [CrossRef]
- Hoffmann, T.C.; Glasziou, P.P.; Boutron, I.; Milne, R.; Perera, R.; Moher, D.; Altman, D.G.; Barbour, V.; Macdonald, H.; Johnston, M.; et al. Better reporting of interventions: Template for intervention description and replication (TIDieR) checklist and guide. BMJ 2014, 348, g1687. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Shierk, A.; Roberts, H.; O’Brien, A.; Thias, B.B. Scoping Review of Goal Directed Therapy for Youth with Cerebral Palsy. 2023. Available online: https://osf.io/5t3bq (accessed on 1 April 2023).
- Novak, I.; McIntyre, S.; Morgan, C.; Campbell, L.; Dark, L.; Morton, N.; Stumbles, E.; Wilson, S.A.; Goldsmith, S. A systematic review of interventions for children with cerebral palsy: State of the evidence. Dev. Med. Child Neurol. 2013, 55, 885–910. [Google Scholar] [CrossRef]
- Novak, I.; Morgan, C.; Fahey, M.; Finch-Edmondson, M.; Galea, C.; Hines, A.; Langdon, K.; Namara, M.M.; Paton, M.C.; Popat, H.; et al. State of the Evidence Traffic Lights 2019: Systematic Review of Interventions for Preventing and Treating Children with Cerebral Palsy. Curr. Neurol. Neurosci. Rep. 2020, 20, 3. [Google Scholar] [CrossRef]
- Lambert, V.A.; Lambert, C.E. Qualitative Descriptive Research: An Acceptable Design. Pac. Rim Int. J. Nurs. Res. 2013, 16, 255–256. [Google Scholar]
- World Health Organization. International Classification of Functioning, Disability and Health: ICF; World Health Organization: Geneva, Switzerland, 2001. [Google Scholar]
- Aarts, P.B.; Jongerius, P.H.; Geerdink, Y.A.; Van Limbeek, J.; Geurts, A.C. Effectiveness of modified constraint-induced movement therapy in children with unilateral spastic cerebral palsy: A randomized controlled trial. Neurorehabilit. Neural. Repair. 2010, 24, 509–518. [Google Scholar] [CrossRef] [PubMed]
- Aarts, P.B.; van Hartingsveldt, M.; Anderson, P.G.; van den Tillaar, I.; van der Burg, J.; Geurts, A.C. The pirate group intervention protocol: Description and a case report of a modified constraint-induced movement therapy combined with bimanual training for young children with unilateral spastic cerebral palsy. Occup. Ther. Int. 2012, 19, 76–87. [Google Scholar] [CrossRef] [PubMed]
- Morgan, C.; Novak, I.; Dale, R.; Badawi, N. Optimising motor learning for infants at high risk of cerebral palsy: A pilot study. BMC Pediatr. 2015, 15, 30. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, E.; Kentish, M.; Boyd, R.; Horan, S.; Carty, C. A randomized controlled trial of functional electrical stimulation powered cycling, goaldirected training and adapted cycling in children with cerebral palsy. Dev. Med. Child Neurol. 2020, 62, 7–8. [Google Scholar] [CrossRef]
- Armstrong, E.L.; Boyd, R.N.; Horan, S.A.; Kentish, M.J.; Ware, R.S.; Carty, C.P. Maintenance of Functional Gains Following a Goal-Directed and FES-Assisted Cycling Program for Children With Cerebral Palsy. Pediatr. Phys. Ther. 2022, 34, 480–487. [Google Scholar] [CrossRef]
- Arnevik Austrheim, K.; Skagen, C.; Rieber, J.; Melfald Tveten, K. Practice, play, repeat–individualized outcomes after the “intensity matters!”-program for children with disabilities–a descriptive multicase study. Disabil. Rehabil. 2024, 46, 2847–2852. [Google Scholar] [CrossRef]
- Bleyenheuft, Y.; Ebner-Karestinos, D.; Surana, B.; Paradis, J.; Sidiropoulos, A.; Renders, A.; Friel, K.M.; Brandao, M.; Rameckers, E.; Gordon, A.M. Intensive upper-and lower-extremity training for children with bilateral cerebral palsy: A quasi-randomized trial. Dev. Med. Child Neurol. 2017, 59, 625–633. [Google Scholar] [CrossRef]
- Bono, G.L.P.; Achermann, P.; Rückriem, B.; Lieber, J.; van Hedel, H.J.A. Goal-directed personalized upper limb intensive therapy (PULIT) for children with hemiparesis: A retrospective analysis. Am. J. Occup. Ther. 2022, 76, 7606205050. [Google Scholar] [CrossRef]
- Brandão, M.B.; Ferre, C.; Kuo, H.C.; Rameckers, E.A.A.; Bleyenheuft, Y.; Hung, Y.C.; Friel, K.; Gordon, A.M. Comparison of structured skill and unstructured practice during intensive bimanual training in children with unilateral spastic cerebral palsy. Neurorehabilit. Neural. Repair. 2014, 28, 452–461. [Google Scholar] [CrossRef]
- Branjerdporn, N.; Ziviani, J.; Sakzewski, L. Goal-directed occupational therapy for children with unilateral cerebral palsy: Categorising and quantifying session content. Br. J. Occup. Ther. 2018, 81, 138–146. [Google Scholar] [CrossRef]
- Cusick, A.; McIntyre, S.; Novak, I.; Lannin, N.; Lowe, K. A comparison of goal attainment scaling and the Canadian Occupational Performance Measure for paediatric rehabilitation research. Pediatr. Rehabil. 2006, 9, 149–157. [Google Scholar] [CrossRef]
- de Brito Brandao, M.; Gordon, A.M.; Mancini, M.C. Functional impact of constraint therapy and bimanual training in children with cerebral palsy: A randomized controlled trial. AJOT Am. J. Occup. Ther. 2012, 66, 672. [Google Scholar] [CrossRef]
- Feitosa, A.M.; Mancini, M.C.; Silvério, A.P.M.; Gordon, A.M.; Brandão, M.B. “help me to improve my own priorities!”: A feasibility study of an individualized intensive goal training for adolescents with cerebral palsy. Phys. Occup. Ther. Pediatr. 2021, 41, 601–619. [Google Scholar] [CrossRef]
- Ferre, C.L.; Brandão, M.; Surana, B.; Dew, A.P.; Moreau, N.G.; Gordon, A.M. Caregiver-directed home-based intensive bimanual training in young children with unilateral spastic cerebral palsy: A randomized trial. Dev. Med. Child Neurol. 2017, 59, 497–504. [Google Scholar] [CrossRef] [PubMed]
- Figueiredo, P.R.P.; Mancini, M.C.; Feitosa, A.M.; Teixeira, C.M.M.F.; Guerzoni, V.P.D.; Elvrum, A.K.G.; Ferre, C.L.; Gordon, A.M.; BrandÃo, M.B. Hand–arm bimanual intensive therapy and daily functioning of children with bilateral cerebral palsy: A randomized controlled trial. Dev. Med. Child Neurol. 2020, 62, 1274–1282. [Google Scholar] [CrossRef] [PubMed]
- Geerdink, Y.; Aarts, P.; van der Burg, J.; Steenbergen, B.; Geurts, A. Intensive upper limb intervention with self-management training is feasible and promising for older children and adolescents with unilateral cerebral palsy. Res. Dev. Disabil. 2015, 43, 97–105. [Google Scholar] [CrossRef] [PubMed]
- Ghorbani, N.; Rassafiani, M.; Izadi-Najafabadi, S.; Yazdani, F.; Akbarfahimi, N.; Havaei, N.; Gharebaghy, S. Effectiveness of cognitive orientation to (daily) occupational performance (CO-OP) on children with cerebral palsy: A mixed design. Res. Dev. Disabil. 2017, 71, 24–34. [Google Scholar] [CrossRef]
- Gimeno, H.; Polatajko, H.J.; Cornelius, V.; Lin, J.P.; Brown, R.G. Rehabilitation in childhood-onset hyperkinetic movement disorders including dystonia: Treatment change in outcomes across the ICF and feasibility of outcomes for full trial evaluation. Eur. J. Paediatr. Neurol. 2021, 33, 159–167. [Google Scholar] [CrossRef]
- Haddon, M.; West, L.; Elliott, C.; Walmsley, C.; Valentine, J.; Bear, N.; Pool, D. Kindy Moves: The feasibility of an intensive interdisciplinary programme on goal and motor outcomes for preschool-aged children with neurodisabilities requiring daily equipment and physical assistance. BMJ Open 2023, 13, e068816. [Google Scholar] [CrossRef]
- Hoare, B.; Imms, C.; Carey, L. Intensive Upper Limb Therapy Following Botulinum-A in Young Children with Hemiplegic Cerebral Palsy: Results from a Randomised Controlled Trial. Dev. Med. Child Neurol. 2010, 52, 13. [Google Scholar]
- Imms, C.; Mathews, S.; Nicola Richmond, K.; Law, M.; Ullenhag, A. Optimising leisure participation: A pilot intervention study for adolescents with physical impairments. Disabil. Rehabil. 2016, 38, 963–971. [Google Scholar] [CrossRef] [PubMed]
- Jackman, M.; Novak, I.; Lannin, N.; Froude, E.; Miller, L.; Galea, C. Effectiveness of cognitive orientation to daily occupational performance over and above functional hand splints for children with cerebral palsy or brain injury: A randomized controlled trial. BMC Pediatr. 2018, 18, 248. [Google Scholar] [CrossRef] [PubMed]
- Jackman, M.; Novak, I.; Lannin, N.A.; Galea, C.; Froude, E. The Cognitive Orientation to daily Occupational Performance (CO-OP) Approach: Best responders in children with cerebral palsy and brain injury. Res. Dev. Disabil. 2018, 78, 103–113. [Google Scholar] [CrossRef] [PubMed]
- Janssen-Potten, Y.J.M.; Roks, L.; Roijen, R.; Vermeulen, R.J.; Adelante Study, G.; Rameckers, E.E.A. Effectiveness of functional intensive therapy on mobility and self-care activities in children and adolescents with cerebral palsy–a prospective clinical study. Disabil. Rehabil. 2023, 45, 3529–3538. [Google Scholar] [CrossRef]
- Lammi, B.M.; Law, M. The effects of family-centred functional therapy on the occupational performance of children with cerebral palsy. Can. J. Occup. Ther. 2003, 70, 285–297. [Google Scholar] [CrossRef]
- Lidman, G.; Nachemson, A.; Peny-Dahlstrand, M.; Himmelmann, K. Botulinum toxin A injections and occupational therapy in children with unilateral spastic cerebral palsy: A randomized controlled trial. Dev. Med. Child Neurol. 2015, 57, 754–761. [Google Scholar] [CrossRef]
- Lowe, K.; Novak, I.; Cusick, A. Low-dose/high-concentration localized botulinum toxin A improves upper limb movement and function in children with hemiplegic cerebral palsy. Dev. Med. Child Neurol. 2006, 48, 170–175. [Google Scholar] [CrossRef]
- Novak, I.; Cusick, A.; Lannin, N. Occupational therapy home programs for cerebral palsy: Double-blind, randomized, controlled trial. Pediatrics 2009, 124, e606–e614. [Google Scholar] [CrossRef]
- Ödman, P.E.; Öberg, B.E. Effectiveness and expectations of intensive training: A comparison between child and youth rehabilitation and conductive education. Disabil. Rehabil. 2006, 28, 561–570. [Google Scholar] [CrossRef]
- Öhrvall, A.-M.; Hofgren, C.; Lindquist, B.; Bergqvist, L.; Himmelmann, K.; Opheim, A.; Sjöwall, D.; Brock, K.; Peny-Dahlstrand, M. Intervention with the CO-OP Approach leads to a transfer effect over time to untrained goals for children with cerebral palsy or spina bifida. Disabil. Rehabil. 2024, 46, 2512–2521. [Google Scholar] [CrossRef]
- Olesch, C.A.; Greaves, S.; Imms, C.; Reid, S.M.; Graham, H.K. Repeat botulinum toxin-A injections in the upper limb of children with hemiplegia: A randomized controlled trial. Dev. Med. Child Neurol. 2010, 52, 79–86. [Google Scholar] [CrossRef]
- Palisano, R.J.; Chiarello, L.A.; King, G.A.; Novak, I.; Stoner, T.; Fiss, A. Participation-based therapy for children with physical disabilities. Disabil. Rehabil. 2012, 34, 1041–1052. [Google Scholar] [CrossRef]
- Pollock, N.; Sharma, N.; Christenson, C.; Law, M.; Gorter, J.W.; Darrah, J. Change in parent-identified goals in young children with cerebral palsy receiving a context-focused intervention: Associations with child, goal and intervention factors. Phys. Occup. Ther. Pediatr. 2014, 34, 62–74. [Google Scholar] [CrossRef]
- Roelofsma, R.; Rameckers, E. The effect of a functional intensive intervention program on self-care in children with cerebral palsy: A case study. Int. J. Brain Disord. Treat 2017, 3, 21. [Google Scholar]
- Sakzewski, L.; Provan, K.; Ziviani, J.; Boyd, R.N. Comparison of dosage of intensive upper limb therapy for children with unilateral cerebral palsy: How big should the therapy pill be? Res. Dev. Disabil. 2015, 37, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Sakzewski, L.; Ziviani, J.; Abbott, D.F.; Macdonell, R.A.; Jackson, G.D.; Boyd, R.N. Participation Outcomes in a Randomized Trial of 2 Models of Upper-Limb Rehabilitation for Children With Congenital Hemiplegia. Arch. Phys. Med. Rehabil. 2011, 92, 531–539. [Google Scholar] [CrossRef]
- Sakzewski, L.; Ziviani, J.; Boyd, R.N. Best responders after intensive upper-limb training for children with unilateral cerebral palsy. Arch. Phys. Med. Rehabil. 2011, 92, 578–584. [Google Scholar] [CrossRef] [PubMed]
- Sanli, B.B.; Janssen-Potten, Y.J.M.; Meeuwsen, I.; Coenen, M.; Caponi, L.; Roijen, R.; Teeuwen, L.; van den Berge, G.; de Haan, C.; Steinbusch, C. Effect on quality of life in children and adolescents with disabilities after a functional intensive therapy approach. Biomed. J. Sci. Tech. Res. 2020, 31, 24146–24151. [Google Scholar] [CrossRef]
- Saussez, G.; Bailly, R.; Araneda, R.; Paradis, J.; Ebner-Karestinos, D.; Klöcker, A.; Sogbossi, E.S.; Riquelme, I.; Brochard, S.; Bleyenheuft, Y. Efficacy of integrating a semi-immersive virtual device in the HABIT-ILE intervention for children with unilateral cerebral palsy: A non-inferiority randomized controlled trial. J. Neuroeng. Rehabil. 2023, 20, 98. [Google Scholar] [CrossRef]
- Sel, S.A.; Günel, M.K.; Erdem, S.; Tunçdemir, M. Effects of Telerehabilitation-Based Structured Home Program on Activity, Participation and Goal Achievement in Preschool Children with Cerebral Palsy: A Triple-Blinded Randomized Controlled Trial. Children 2023, 10, 424. [Google Scholar] [CrossRef]
- Speth, L.; Janssen-Potten, Y.; Rameckers, E.; Defesche, A.; Winkens, B.; Becher, J.; Smeets, R.; Vles, H. Effects of botulinum toxin A and/or bimanual task-oriented therapy on upper extremity activities in unilateral Cerebral Palsy: A clinical trial. BMC Neurol. 2015, 15, 143. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Steinbusch, C.V.M.; Defesche, A.; van der Leij, B.; Rameckers, E.A.A.; Knijnenburg, A.C.S.; Vermeulen, J.R.J.; Janssen-Potten, Y.J.M. The Effect of Bimanual Intensive Functional Training on Somatosensory Hand Function in Children with Unilateral Spastic Cerebral Palsy: An Observational Study. J. Clin. Med. 2023, 12, 1595. [Google Scholar] [CrossRef] [PubMed]
- Thomas, R.E.; Johnston, L.M.; Sakzewski, L.; Kentish, M.J.; Boyd, R.N. Evaluation of group versus individual physiotherapy following lower limb intra-muscular Botulinum Toxin-Type A injections for ambulant children with cerebral palsy: A single-blind randomized comparison trial. Res. Dev. Disabil. 2016, 53, 267–278. [Google Scholar] [CrossRef] [PubMed]
- Wallen, M.; Ziviani, J.; Naylor, O.; Evans, R.; Novak, I.; Herbert, R.D. Modified constraint-induced therapy for children with hemiplegic cerebral palsy: A randomized trial. Dev. Med. Child Neurol. 2011, 53, 1091–1099. [Google Scholar] [CrossRef]
- Balci, N.C.; Günel, M.K.; Erden, Z.; Tekindal, M.A. Effect of Goal Directed Phys-iotherapy vs a Goal Directed Home Program in At-Risk Infants: A Randomized Clinical Trial. Adv. Neurol. Neurosci. 2021, 4, 29–35. [Google Scholar]
- Elliott, C.M.; Reid, S.L.; Alderson, J.A.; Elliott, B.C. Lycra arm splints in conjunction with goal-directed training can improve movement in children with cerebral palsy. NeuroRehabilitation 2011, 28, 47–54. [Google Scholar] [CrossRef]
- Franki, I.; Van den Broeck, C.; De Cat, J.; Tijhuis, W.; Molenaers, G.; Vanderstraeten, G.; Desloovere, K. A randomized, single-blind cross-over design evaluating the effectiveness of an individually defined, targeted physical therapy approach in treatment of children with cerebral palsy. Clin. Rehabil. 2014, 28, 1039–1052. [Google Scholar] [CrossRef]
- Gibson, N.; Chappell, A.; Blackmore, A.M.; Morris, S.; Williams, G.; Bear, N.; Allison, G. The effect of a running intervention on running ability and participation in children with cerebral palsy: A randomized controlled trial. Disabil. Rehabil. 2018, 40, 3041–3049. [Google Scholar] [CrossRef]
- Gordon, A.M.; Hung, Y.C.; Brandao, M.; Ferre, C.L.; Kuo, H.C.; Friel, K.; Petra, E.; Chinnan, A.; Charles, J.R. Bimanual training and constraint-induced movement therapy in children with hemiplegic cerebral palsy: A randomized trial. Neurorehabilit. Neural. Repair. 2011, 25, 692–702. [Google Scholar] [CrossRef]
- Kawamura, A.; Campbell, K.; Lam-Damji, S. A Randomized Controlled Trial Comparing Botulinum Toxin A Dosage in the Upper Extremity of Children with Spasticity. Dev. Med. Child Neurol. 2007, 49, 331–337. [Google Scholar] [CrossRef]
- Knight, S.; Fetters, L. Intensive Motor Skills Training Program Combining Group and Individual Sessions for Children With Cerebral Palsy. Pediatr. Phys. Ther. 2010, 22, 160. [Google Scholar] [CrossRef] [PubMed]
- Lööwing, K.; Hamer, E.G.; Bexelius, A.; Carlberg, E.B. Exploring the relationship of family goals and scores on standardized measures in children with cerebral palsy, using the ICF-CY. Dev. Neurorehabilit. 2011, 14, 79–86. [Google Scholar] [CrossRef] [PubMed]
- Löwing, K.; Bexelius, A.; Brogren Carlberg, E. Activity focused and goal directed therapy for children with cerebral palsy—Do goals make a difference? Disabil. Rehabil. 2009, 31, 1808–1816. [Google Scholar] [CrossRef]
- Löwing, K.; Bexelius, A.; Carlberg, E.B. Goal-directed functional therapy: A longitudinal study on gross motor function in children with cerebral palsy. Disabil. Rehabil. 2010, 32, 908–916. [Google Scholar] [CrossRef] [PubMed]
- Novak, I.; Cusick, A.; Lowe, K. A pilot study on the impact of occupational therapy home programming for young children with cerebral palsy. Am. J. Occup. Ther. 2007, 61, 463–468. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Palee, S.; Ploypetch, T.; Pajareya, K.; Timdang, S. Goal-Directed Therapy to Improve Gross Motor Function and the Quality of Life of Children with Cerebral Palsy: A Randomized Controlled Trial. Siriraj Med. J. 2022, 74, 1–10. [Google Scholar] [CrossRef]
- Salavati, M.; Rameckers, E.; Waninge, A.; Krijnen, W.; van der Schans, C.; Steenbergen, B. Evaluating the outcome of an individual functional therapy program focused on children with cerebral palsy and cerebral visual impairment: A multiple case study. Eur. J. Physiother. 2018, 20, 92–100. [Google Scholar] [CrossRef]
- Seyhan, K.; GÜNel, M.K.; AkyÜZ, E.Ü. Family-centred, goal-directed multidisciplinary approach for lower extremity botulinum toxin with physical therapy and rehabilitation in cerebral palsy. Türk Fiz. Ve Rehabil. Derg. 2020, 31, 1–10. [Google Scholar] [CrossRef]
- Sørensen, K.; Vestrheim, I.E.; Lerdal, B.; Skranes, J. Functional Skills among Preschool Children with Cerebral Palsy–Assessment before and after Early Intervention. Dev. Neurorehabilit. 2020, 23, 519–525. [Google Scholar] [CrossRef]
- Sorsdahl, A.B.; Moe-Nilssen, R.; Kaale, H.K.; Rieber, J.; Strand, L.I. Change in basic motor abilities, quality of movement and everyday activities following intensive, goal-directed, activity-focused physiotherapy in a group setting for children with cerebral palsy. BMC Pediatr. 2010, 10, 26. [Google Scholar] [CrossRef]
- Türker, D.; Korkem, D.; Özal, C.; Günel, M.K.; Karahan, S. The effects of neurodevelopmental (Bobath) therapy based goal directed therapy on gross motor function and functional status of children with cerebral palsy. Int. J. Ther. Rehabil. Res. 2015, 4, 9–16. [Google Scholar] [CrossRef]
- Wu, C.-L.; Liao, S.-F.; Liu, C.-H.; Hsieh, Y.-T.; Lin, Y.-R. A pilot study of two different constraint-induced movement therapy interventions in children with hemiplegic cerebral palsy after botulinum toxin injection during preschool education. Front. Pediatr. 2020, 8, 557. [Google Scholar] [CrossRef] [PubMed]
- Ahl, L.E.; Johansson, E.; Granat, T.; Carlberg, E.B. Functional therapy for children with cerebral palsy: An ecological approach. Dev. Med. Child Neurol. 2005, 47, 613–619. [Google Scholar] [CrossRef] [PubMed]
- Akbari, A.; Javadzadeh, M.; Shahraki, G.; Jahanshahi, J.P. The effects of functional therapy on motor development in children with cerebral palsy. Iran. J. Child Neurol. 2009, 3, 23–32. [Google Scholar]
- Al Imam, M.H.; Jahan, I.; Das, M.C.; Bashar, S.M.K.; Khan, A.; Muhit, M.; Power, R.; Akbar, D.; Badawi, N.; Khandaker, G. SUpporting People in extreme POverty with Rehabilitation and Therapy (SUPPORT CP): A trial among families of children with cerebral palsy in Bangladesh. Dev. Med. Child Neurol. 2023, 65, 773–782. [Google Scholar] [CrossRef]
- Bower, E.; Michell, D.; Burnett, M.; Campbell, M.J.; McLellan, D.L. Randomized controlled trial of physiotherapy in 56 children with cerebral palsy followed for 18 months. Dev. Med. Child Neurol. 2001, 43, 4–15. [Google Scholar] [CrossRef]
- Brit Sorsdahl, A.; Moe-Nilssen, R.; Larsen, E.M.; Lundal, S.H.; Rieber, J.; Skarstein, E.; Kaale, H.K.; Strand, L.I. Long-term change of gross motor function in children with cerebral palsy; an observational study of repeated periods of intensive physiotherapy in a group setting. Eur. J. Physiother. 2020, 22, 148–154. [Google Scholar] [CrossRef]
- Crompton, J.; Imms, C.; McCoy, A.T.; Randall, M.; Eldridge, B.; Scoullar, B.; Galea, M.P. Group-based task-related training for children with cerebral palsy: A pilot study. Phys. Occup. Ther. Pediatr. 2007, 27, 43–65. [Google Scholar] [CrossRef]
- Heathcock, J.C.; Baranet, K.; Ferrante, R.; Hendershot, S. Daily Intervention for Young Children with Cerebral Palsy in GMFCS Level V: A Case Series. Pediatr. Phys. Ther. 2015, 27, 285–292. [Google Scholar] [CrossRef]
- Ketelaar, M.; Vermeer, A.; Hart, H.t.; van Petegem-van Beek, E.; Helders, P.J.M. Effects of a functional therapy program on motor abilities of children with cerebral palsy. Phys. Ther. 2001, 81, 1534–1545. [Google Scholar] [CrossRef]
- Ko, E.J.; Sung, I.Y.; Moon, H.J.; Yuk, J.S.; Kim, H.-S.; Lee, N.H. Effect of group-task-oriented training on gross and fine motor function, and activities of daily living in children with spastic cerebral palsy. Phys. Occup. Ther. Pediatr. 2020, 40, 18–30. [Google Scholar] [CrossRef]
- Law, M.C.; Darrah, J.; Pollock, N.; Wilson, B.; Russell, D.J.; Walter, S.D.; Rosenbaum, P.; Galuppi, B. Focus on function: A cluster, randomized controlled trial comparing child-versus context-focused intervention for young children with cerebral palsy. Dev. Med. Child Neurol. 2011, 53, 621–629. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Shim, J.S.; Kim, K.; Moon, J.; Kim, M. Gross motor function outcome after intensive rehabilitation in children with bilateral spastic cerebral palsy. Ann. Rehabil. Med. 2015, 39, 624–629. [Google Scholar] [CrossRef] [PubMed]
- Myrhaug, H.T.; Odgaard-Jensen, J.; Jahnsen, R. The long-term effects of conductive education courses in young children with cerebral palsy: A randomized controlled trial. Dev. Neurorehabilit. 2019, 22, 111–119. [Google Scholar] [CrossRef]
- Sah, A.K.; Balaji, G.K.; Agrahara, S. Effects of task-oriented activities based on neurodevelopmental therapy principles on trunk control, balance, and gross motor function in children with spastic diplegic cerebral palsy: A single-blinded randomized clinical trial. J. Pediatr. Neurosci. 2019, 14, 120. [Google Scholar]
- Saquetto, M.B.; de Santana Bispo, A.; da Silva Barreto, C.; Gonçalves, K.A.; Queiroz, R.S.; da Silva, C.M.; Gomes Neto, M. Addition of an educational programme for primary caregivers to rehabilitation improves self-care and mobility in children with cerebral palsy: A randomized controlled trial. Clin. Rehabil. 2018, 32, 878–887. [Google Scholar] [CrossRef]
- Sousa, L.K.; Brandão, M.B.; Curtin, C.M.; Magalhães, L.C. A collaborative and cognitive-based intervention for young people with cerebral palsy. Can. J. Occup. Ther. 2020, 87, 319–330. [Google Scholar] [CrossRef]
- Stark, C.; Duran, I.; Martakis, K.; Spiess, K.; Semler, O.; Schoenau, E. Effect of long-term repeated interval rehabilitation on the gross motor function measure in children with cerebral palsy. Neuropediatrics 2020, 51, 407–416. [Google Scholar] [CrossRef]
- Bar-Haim, S.; Harries, N.; Nammourah, I.; Oraibi, S.; Malhees, W.; Loeppky, J.; Perkins, N.J.; Belokopytov, M.; Kaplanski, J.; Lahat, E. Effectiveness of motor learning coaching in children with cerebral palsy: A randomized controlled trial. Clin. Rehabil. 2010, 24, 1009–1020. [Google Scholar] [CrossRef]
- Wang, L.; Zhang, N.; Fang, L.; Cui, Z.; Niu, H.; Lv, F.; Hu, D.; Wu, D. Effect of hip CPM on gross motor function and development of the hip joint: A single-center randomized controlled study on spastic cerebral palsy children with hip dysplasia. Front. Pediatr. 2023, 11, 1090919. [Google Scholar] [CrossRef]
- Bleyenheuft, Y.; Bleyenheuft, C.; Arnould, C.; Brandao, M.B.; Gordon, A.M. Hand and Arm Bimanual Intensive Therapy Including Lower Extremity (HABIT-ILE) in Children With Unilateral Spastic Cerebral Palsy: A Randomized Trial. Neurorehabilit. Neural. Repair. 2015, 29, 645–657. [Google Scholar] [CrossRef]
- Gelkop, N.; Burshtein, D.G.; Lahav, A.; Brezner, A.; Al-Oraibi, S.; Ferre, C.L.; Gordon, A.M. Efficacy of constraint-induced movement therapy and bimanual training in children with hemiplegic cerebral palsy in an educational setting. Phys. Occup. Ther. Pediatr. 2015, 35, 24–39. [Google Scholar] [CrossRef]
- Gordon, A.M.; Schneider, J.A.; Chinnan, A.; Charles, J.R. Efficacy of a hand–arm bimanual intensive therapy (HABIT) in children with hemiplegic cerebral palsy: A randomized control trial. Dev. Med. Child Neurol. 2007, 49, 830–838. [Google Scholar] [CrossRef]
- Kirton, A.; Andersen, J.; Herrero, M.; Nettel-Aguirre, A.; Carsolio, L.; Damji, O.; Keess, J.; Mineyko, A.; Hodge, J.; Hill, M.D. Brain stimulation and constraint for perinatal stroke hemiparesis: The PLASTIC CHAMPS Trial. Neurology 2016, 86, 1659–1667. [Google Scholar] [CrossRef] [PubMed]
- Klevberg, G.L.; Zucknick, M.; Jahnsen, R.; Eliasson, A.C. Development of Hand Use with and Without Intensive Training Among Children with Unilateral Cerebral Palsy in Scandinavia. Dev. Neurorehabilit. 2023, 26, 163–171. [Google Scholar] [CrossRef] [PubMed]
- Lieber, J.; Dittli, J.; Lambercy, O.; Gassert, R.; Meyer-Heim, A.; Hubertus, J.A.v.H. Clinical utility of a pediatric hand exoskeleton: Identifying users, practicability, and acceptance, and recommendations for design improvement. J. Neuroeng. Rehabil. 2022, 19, 17. [Google Scholar] [CrossRef] [PubMed]
- Palomo-Carrión, R.; Lirio-Romero, C.; Ferri-Morales, A.; Jovellar-Isiegas, P.; Cortés-Vega, M.-D.; Romay-Barrero, H. Combined intensive therapies at home in spastic unilateral cerebral palsy with high bimanual functional performance. What do they offer? A comparative randomised clinical trial. Ther. Adv. Chronic Dis. 2021, 12, 20406223211034996. [Google Scholar] [CrossRef]
- Roldán-Pérez, P.; Abuín-Porras, V.; Buesa-Estéllez, A.; Ortiz-Lucas, M. Functional Splinting efficacy in a Specific Task Home Program for Children with Cerebral Palsy. A Randomized Controlled Trial. Dev. Neurorehabilit. 2022, 25, 469–478. [Google Scholar] [CrossRef]
- Sakzewski, L.; Miller, L.; Ziviani, J.; Abbott, D.F.; Rose, S.; Macdonell, R.A.L.; Boyd, R.N. Randomized comparison trial of density and context of upper limb intensive group versus individualized occupational therapy for children with unilateral cerebral palsy. Dev. Med. Child Neurol. 2015, 57, 539–547. [Google Scholar] [CrossRef]
- Smorenburg, A.R.P.; Gordon, A.M.; Kuo, H.-C.; Ferre, C.L.; Brandao, M.; Bleyenheuft, Y.; Carmel, J.B.; Friel, K.M. Does corticospinal tract connectivity influence the response to intensive bimanual therapy in children with unilateral cerebral palsy? Neurorehabilit. Neural. Repair. 2017, 31, 250–260. [Google Scholar] [CrossRef]
- Green, D.; Wilson, P.H. Use of virtual reality in rehabilitation of movement in children with hemiplegia—A multiple case study evaluation. Disabil. Rehabil. 2012, 34, 593–604. [Google Scholar] [CrossRef]
- Song, C.-S. Effects of task-oriented approach on affected arm function in children with spastic hemiplegia due to cerebral palsy. J. Phys. Ther. Sci. 2014, 26, 797–800. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sakzewski, L.; Ziviani, J.; Abbott, D.F.; Macdonell, R.A.L.; Jackson, G.D.; Boyd, R.N. Randomized trial of constraint-induced movement therapy and bimanual training on activity outcomes for children with congenital hemiplegia. Dev. Med. Child Neurol. 2011, 53, 313–320. [Google Scholar] [CrossRef] [PubMed]
- Kanitkar, A.; Szturm, T.; Parmar, S.; Gandhi, D.B.; Rempel, G.R.; Restall, G.; Sharma, M.; Narayan, A.; Pandian, J.; Naik, N.; et al. The Effectiveness of a Computer Game-Based Rehabilitation Platform for Children With Cerebral Palsy: Protocol for a Randomized Clinical Trial. JMIR Res. Protoc. 2017, 6, e93. [Google Scholar] [CrossRef] [PubMed]
- Glavić, J.; Rutović, S.; Cvitanović, N.K.; Burić, P.; Petrović, A. Technology-enhanced upper limb physical rehabilitation in hemiplegic cerebral palsy. Int. J. Neurorehabilit. 2016, 3, 2376–0281.1000225. [Google Scholar] [CrossRef]
- Rameckers, E.A.; Duysens, J.; Speth, L.A.; Vles, H.J.; Smits-Engelsman, B.C. Effect of addition of botulinum toxin-A to standardized therapy for dynamic manual skills measured with kinematic aiming tasks in children with spastic hemiplegia. J. Rehabil. Med. 2010, 42, 332–338. [Google Scholar] [CrossRef]
- Simon-Martinez, C.; Mailleux, L.; Jaspers, E.; Ortibus, E.; Desloovere, K.; Klingels, K.; Feys, H. Effects of combining constraint-induced movement therapy and action-observation training on upper limb kinematics in children with unilateral cerebral palsy: A randomized controlled trial. Sci. Rep. 2020, 10, 10421. [Google Scholar] [CrossRef]
- Blundell, S.W.; Shepherd, R.B.; Dean, C.M.; Adams, R.D.; Cahill, B.M. Functional strength training in cerebral palsy: A pilot study of a group circuit training class for children aged 4-8 years. Clin. Rehabil. 2003, 17, 48–57. [Google Scholar] [CrossRef]
- Schasfoort, F.; Pangalila, R.; Sneekes, E.; Catsman, C.; Becher, J.; Horemans, H.; Stam, H.; Dallmeijer, A.; Bussmann, H. Intramuscular botulinum toxin prior to comprehensive rehabilitation has no added value for improving motor impairments, gait kinematics and goal attainment in walking children with spastic cerebral palsy. J. Rehabil. Med. 2018, 50, 732–742. [Google Scholar] [CrossRef]
- Melamalai, S.; Amalraj, C.; Alanazi, A.O.K.; Vadivel, S.; Senapati, A. Splints And a Task-Oriented Approach Improve Upper Extremity Function in Children with Spastic Quadriplegic Cerebral Palsy. Int. J. Multidiscip. Res. 2023, 5, 1–8. [Google Scholar]
- Chen, Y.; Garcia-Vergara, S.; Howard, A.M. Effect of a home-based virtual reality intervention for children with cerebral palsy using super pop VR evaluation metrics: A feasibility study. Rehabil. Res. Pract. 2015, 2015, 812348. [Google Scholar] [CrossRef]
- Gimeno, H.; Polatajko, H.J.; Lin, J.P.; Cornelius, V.; Brown, R.G. Cognitive Strategy Training in Childhood-Onset Movement Disorders: Replication Across Therapists. Front. Pediatr. 2020, 8, 600337. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, E.L.; Boyd, R.N.; Carty, C.P.; Kentish, M.J.; Goodlich, B.I.; Horan, S.A. A qualitative analysis of the experiences of children with cerebral palsy and their caregivers in a goal-directed cycling programme. Disabil. Rehabil. 2022, 44, 2715–2722. [Google Scholar] [CrossRef] [PubMed]
- Miller, L.; Ziviani, J.; Ware, R.S.; Boyd, R.N. Does context matter? Mastery motivation and therapy engagement of children with cerebral palsy. Phys. Occup. Ther. Pediatr. 2016, 36, 155–170. [Google Scholar] [CrossRef]
- Vroland-Nordstrand, K.; Eliasson, A.-C.; Krumlinde-Sundholm, L.; Johansson, U. Parents’ experiences of conducting a goal-directed intervention based on children’s self-identified goals, a qualitative study. Scand. J. Occup. Ther. 2018, 25, 243–251. [Google Scholar] [CrossRef] [PubMed]
- Al Imam, M.H.; Jahan, I.; Muhit, M.; Das, M.C.; Power, R.; Khan, A.; Akbar, D.; Badawi, N.; Khandaker, G. Supporting Ultra Poor People with Rehabilitation and Therapy among families of children with Cerebral Palsy in rural Bangladesh (SUPPORT CP): Protocol of a randomised controlled trial. PLoS ONE 2021, 16, e0261148. [Google Scholar] [CrossRef]
- Armstrong, E.L.; Boyd, R.N.; Kentish, M.J.; Carty, C.P.; Horan, S.A. Effects of a training programme of functional electrical stimulation (FES) powered cycling, recreational cycling and goal-directed exercise training on children with cerebral palsy: A randomised controlled trial protocol. BMJ Open 2019, 9, e024881. [Google Scholar] [CrossRef]
- Aydin, R.; Nur, H. Family-centered approach in the management of children with cerebral palsy. Turk. J. Phys. Med. Rehabil./Turk. Fiz. Tip Ve Rehabil. Derg. 2012, 58, 229–235. [Google Scholar] [CrossRef]
- Boyd, R.; Sakzewski, L.; Provan, K.; Abbott, D.F.; Badawy, R.; Gilmore, R.; Tournier, J.; Macdonell, R.A.L.; Jackson, G.D.; Ziviani, J. INCITE: A randomised trial comparing constraint induced movement therapy and bimanual training in children with congenital hemiplegia. BMC Neurol. 2010, 10, 4. [Google Scholar] [CrossRef]
- Hoare, B.; Greaves, S. Unimanual versus bimanual therapy in children with unilateral cerebral palsy: Same, same, but different. J. Pediatr. Rehabil. Med. 2017, 10, 47–59. [Google Scholar] [CrossRef]
- Imms, C.; Cowan, R.; Ertekin, E.; Klein, G.-L.; Galvin, J. Eight weeks of occupational therapy home programme, compared to no programme, resulted in improved achievement of child and family-selected goals by children with cerebral palsy. Aust. Occup. Ther. J. 2010, 57, 444–445. [Google Scholar] [CrossRef] [PubMed]
- Jackman, M.; Novak, I.; Lannin, N. Effectiveness of functional hand splinting and the cognitive orientation to occupational performance (CO-OP) approach in children with cerebral palsy and brain injury: Two randomised controlled trial protocols. BMC Neurol. 2014, 14, 144. [Google Scholar] [CrossRef]
- Klevberg, G.L.; Østensjø, S.; Elkjær, S.; Kjeken, I.; Jahnsen, R.B. Hand function in young children with cerebral palsy: Current practice and parent-reported benefits. Phys. Occup. Ther. Pediatr. 2017, 37, 222–237. [Google Scholar] [CrossRef] [PubMed]
- McLean, B.; Blakeman, M.; Carey, L.; Ward, R.; Novak, I.; Valentine, J.; Blair, E.; Taylor, S.; Bear, N.; Bynevelt, M. Discovering the sense of touch: Protocol for a randomised controlled trial examining the efficacy of a somatosensory discrimination intervention for children with hemiplegic cerebral palsy. BMC Pediatr. 2018, 18, 252. [Google Scholar] [CrossRef] [PubMed]
- Milton, Y.M.; Roe, S.A.; Newby, K.V. Home programmes based on evidence of best practice for children with unilateral cerebral palsy: Occupational therapists’ perceptions. Br. J. Occup. Ther. 2020, 83, 447–457. [Google Scholar] [CrossRef]
- Morgan, C.; Novak, I.; Dale, R.C.; Guzzetta, A.; Badawi, N. GAME (Goals-Activity-Motor Enrichment): Protocol of a single blind randomised controlled trial of motor training, parent education and environmental enrichment for infants at high risk of cerebral palsy. BMC Neurol. 2014, 14, 203. [Google Scholar] [CrossRef]
- Myrhaug, H.T.; Østensjø, S. Motor training and physical activity among preschoolers with cerebral palsy: A survey of parents’ experiences. Phys. Occup. Ther. Pediatr. 2014, 34, 153–167. [Google Scholar] [CrossRef]
- Novak, I. Evidence-based diagnosis, health care, and rehabilitation for children with cerebral palsy. J. Child Neurol. 2014, 29, 1141–1156. [Google Scholar] [CrossRef]
- Novak, I.; Berry, J. Home program intervention effectiveness evidence. Phys. Occup. Ther. Pediatr. 2014, 34, 384–389. [Google Scholar] [CrossRef]
- Novak, I.; Cusick, A. Home programmes in paediatric occupational therapy for children with cerebral palsy: Where to start? Aust. Occup. Ther. J. 2006, 53, 251–264. [Google Scholar] [CrossRef]
- Oh, T.-Y. Overview of Physical Therapy for Children with Cerebral Palsy. J. Korean Soc. Neurother. 2019, 23, 31–38. [Google Scholar] [CrossRef]
- Öhrvall, A.-M.; Bergqvist, L.; Hofgren, C.; Peny-Dahlstrand, M. “With CO-OP I’m the boss”–experiences of the cognitive orientation to daily occupational performance approach as reported by young adults with cerebral palsy or spina bifida. Disabil. Rehabil. 2020, 42, 3645–3652. [Google Scholar] [CrossRef]
- Palomo-Carrión, R.; Pinero-Pinto, E.; Romay-Barrero, H.; Escobio-Prieto, I.; Lillo-Navarro, C.; Romero-Galisteo, R.-P. Shall we start? Ready, set, go! Toward early intervention in infants with unilateral cerebral palsy. A randomized clinical trial protocol. Ther. Adv. Chronic Dis. 2022, 13, 20406223221136059. [Google Scholar] [CrossRef] [PubMed]
- Pritchard-Wiart, L.; Thompson-Hodgetts, S.; McKillop, A.B. A review of goal setting theories relevant to goal setting in paediatric rehabilitation. Clin. Rehabil. 2019, 33, 1515–1526. [Google Scholar] [CrossRef]
- Reedman, S.E.; Boyd, R.N.; Elliott, C.; Sakzewski, L. ParticiPAte CP: A protocol of a randomised waitlist controlled trial of a motivational and behaviour change therapy intervention to increase physical activity through meaningful participation in children with cerebral palsy. BMJ Open 2017, 7, e015918. [Google Scholar] [CrossRef] [PubMed]
- Sakzewski, L.; Bleyenheuft, Y.; Boyd, R.N.; Novak, I.; Elliott, C.; Reedman, S.; Morgan, C.; Pannek, K.; Fripp, J.; Golland, P. Protocol for a multisite randomised trial of Hand–Arm Bimanual Intensive Training Including Lower Extremity training for children with bilateral cerebral palsy: HABIT-ILE Australia. BMJ Open 2019, 9, e032194. [Google Scholar] [CrossRef] [PubMed]
- Sakzewski, L.; Pool, D.; Armstrong, E.; Reedman, S.E.; Boyd, R.N.; Elliott, C.; Novak, I.; Trost, S.; Ware, R.S.; Comans, T. ACTIVE STRIDES-CP: Protocol for a randomised trial of intensive rehabilitation (combined intensive gait and cycling training) for children with moderate-to-severe bilateral cerebral palsy. BMJ Open 2023, 13, e068774. [Google Scholar] [CrossRef]
- Sakzewski, L.; Ziviani, J.; Boyd, R.N. Delivering evidence-based upper limb rehabilitation for children with cerebral palsy: Barriers and enablers identified by three pediatric teams. Phys. Occup. Ther. Pediatr. 2014, 34, 368–383. [Google Scholar] [CrossRef]
- Sakzewski, L.; Ziviani, J.; Boyd, R.N. Translating evidence to increase Quality and Dose of Upper Limb therapy for children with unilateral cerebral palsy: A pilot study. Phys. Occup. Ther. Pediatr. 2016, 36, 305–329. [Google Scholar] [CrossRef]
- Saloojee, G. The Akwenda cerebral palsy intervention programme. BMJ Open 2022, 11, e047634. [Google Scholar]
- Sansare, A.; Xanthopoulos, M. Commentary on “Maintenance of Functional Gains Following a Goal-Directed and FES-Assisted Cycling Program for Children With Cerebral Palsy”. Pediatr. Phys. Ther. 2022, 34, 488. [Google Scholar] [CrossRef]
- Saussez, G.; Brandão, M.B.; Gordon, A.M.; Bleyenheuft, Y. Including a lower-extremity component during hand-arm bimanual intensive training does not attenuate improvements of the upper extremities: A retrospective study of randomized trials. Front. Neurol. 2017, 8, 495. [Google Scholar] [CrossRef]
- Schnackers, M.; Beckers, L.; Janssen-Potten, Y.; Aarts, P.; Rameckers, E.; van der Burg, J.; de Groot, I.; COAD Focus Group; Smeets, R.; Geurts, S.; et al. Home-based bimanual training based on motor learning principles in children with unilateral cerebral palsy and their parents (the COAD-study): Rationale and protocols. BMC Pediatr. 2018, 18, 139. [Google Scholar] [CrossRef]
- Størvold, G.V.; Jahnsen, R.B. Current physical therapy practice in Norway for children with cerebral palsy. Pediatr. Phys. Ther. 2021, 33, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Tait, K.; Sigafoos, J.; Woodyatt, G.; O’Reilly, M.; Lancioni, G. Evaluating parent use of functional communication training to replace and enhance prelinguistic behaviours in six children with developmental and physical disabilities. Disabil. Rehabil. 2004, 26, 1241–1254. [Google Scholar] [CrossRef] [PubMed]
- Toovey, R.; Harvey, A.R.; McGinley, J.L.; Lee, K.J.; Shih, S.T.F.; Spittle, A.J. Bike skills training for children with cerebral palsy: Protocol for a randomised controlled trial. BMJ Open 2018, 8, e019898. [Google Scholar] [CrossRef]
- Toovey, R.; Spittle, A.J.; Nicolaou, A.; McGinley, J.L.; Harvey, A.R. Training two-wheel bike skills in children with cerebral palsy: A practice survey of therapists in Australia. Phys. Occup. Ther. Pediatr. 2019, 39, 580–597. [Google Scholar] [CrossRef]
- Ullenhag, A.; Jahnsen, R.; Klove, N.; Smedvig, S.; Hoberg, A. How did youth with cerebral palsy perceive participation in everyday life after participating in a periodical intensive rehabilitation program based on adapted physical activity in groups? A qualitative interview study. Disabil. Rehabil. 2024, 46, 58–66. [Google Scholar] [CrossRef]
- van Vulpen, L.F.; de Groot, S.; Rameckers, E.A.A.; Becher, J.G.; Dallmeijer, A.J. Effectiveness of Functional Power Training on Walking Ability in Young Children With Cerebral Palsy: Study Protocol of a Double-Baseline Trial. Pediatr. Phys. Ther. 2017, 29, 275–282. [Google Scholar] [CrossRef]
- Adiguzel, H.; Sarikabadayi, Y.U.; Elbasan, B. Investigation of the effectiveness of family collaborative physiotherapy programs applied to high-risk infants. Physiother. Theory Pract. 2023, 39, 1871–1887. [Google Scholar] [CrossRef]
- Andrews, C.; Kakooza-Mwesige, A.; Kamusiime, S.; Forssberg, H.; Eliasson, A.C. A Goal-Directed Program for Wheelchair Use for Children and Young People with Cerebral Palsy in Uganda: An Explorative Intervention Study. J. Clin. Med. 2023, 12, 2325. [Google Scholar] [CrossRef]
- Araneda, R.; Sizonenko, S.V.; Newman, C.J.; Dinomais, M.; Le Gal, G.; Ebner-Karestinos, D.; Paradis, J.; Klöcker, A.; Saussez, G.; Demas, J. Protocol of changes induced by early Hand-Arm Bimanual Intensive Therapy Including Lower Extremities (e-HABIT-ILE) in pre-school children with bilateral cerebral palsy: A multisite randomized controlled trial. BMC Neurol. 2020, 20, 243. [Google Scholar] [CrossRef] [PubMed]
- Boyd, R.N.; Novak, I.; Morgan, C.; Bora, S.; Sakzewski, L.; Ware, R.S.; Comans, T.; Fahey, M.C.; Whittingham, K.; Trost, S. Protocol: School readiness of children at high risk of cerebral palsy randomised to early neuroprotection and neurorehabilitation: Protocol for a follow-up study of participants from four randomised clinical trials. BMJ Open 2023, 13, e068675. [Google Scholar] [CrossRef] [PubMed]
- Darrah, J.; Law, M.C.; Pollock, N.; Wilson, B.; Russell, D.J.; Walter, S.D.; Rosenbaum, P.; Galupp, B. Context therapy: A new intervention approach for children with cerebral palsy. Dev. Med. Child Neurol. 2011, 53, 615–620. [Google Scholar] [CrossRef]
- Johari, S.; Kahjoogh, M.A.; Nezhad, Z.M.; Hosseini, S.A.; Zamani, Z.P.; Shati, M.; Haghgoo, H.A. Effects of transcranial direct current stimulation combined with cognitive orientation to daily occupational performance in children with cerebral palsy: A protocol for a randomised controlled trial. Int. J. Ther. Rehabil. 2020, 27, 1–15. [Google Scholar] [CrossRef]
- Ödman, P.; Krevers, B.; Öberg, B. Parents’ perceptions of the quality of two intensive training programmes for children with cerebral palsy. Dev. Med. Child Neurol. 2007, 49, 93–100. [Google Scholar] [CrossRef]
- Bailes, A.F.; Greve, K.; Long, J.; Kurowski, B.; Vargus-Adams, J.; Aronow, B.; Mitelpunkt, A. Describing the delivery of evidence-based physical therapy intervention to individuals with cerebral palsy. Pediatr. Phys. Ther. Off. Publ. Sect. Pediatr. Am. Phys. Ther. Assoc. 2021, 33, 65. [Google Scholar] [CrossRef]
- Buitrago, J.A.; Bolaños, A.M.; Caicedo Bravo, E. A motor learning therapeutic intervention for a child with cerebral palsy through a social assistive robot. Disabil. Rehabil. Assist. Technol. 2020, 15, 357–362. [Google Scholar] [CrossRef]
- Ferro, A.M.; Quinn, L. A structured goal-setting process to promote functional and measurable outcomes in school-based physical therapy: A knowledge translation study. Pediatr. Phys. Ther. 2020, 32, 211–217. [Google Scholar] [CrossRef]
- Moreau, N.G.; Gannotti, M.E. Addressing muscle performance impairments in cerebral palsy: Implications for upper extremity resistance training. J. Hand Ther. 2015, 28, 91–100. [Google Scholar] [CrossRef]
- Fancourt, D.; Wee, J.; Lorencatto, F. Identifying mechanisms of change in a magic-themed hand-arm bimanual intensive therapy programme for children with unilateral spastic cerebral palsy: A qualitative study using behaviour change theory. BMC Pediatr. 2020, 20, 363. [Google Scholar] [CrossRef] [PubMed]
- Smidt, K.B.; Klevberg, G.L.; Oftedal, B.F. Home Programme to Improve Hand Function for Children with Bilateral Cerebral Palsy: Beneficial but Challenging. Phys. Occup. Ther. Pediatr. 2020, 40, 410–422. [Google Scholar] [CrossRef]

| (n = 4708) | n | % |
|---|---|---|
| Gender | ||
| Male | 2560 | 54% |
| Female | 1738 | 37% |
| Not reported | 410 | 9% |
| GMFCS | ||
| I | 735 | 16% |
| II | 597 | 13% |
| III | 515 | 11% |
| IV | 355 | 8% |
| V | 190 | 4% |
| Not reported | 2316 | 49% |
| MACS | ||
| I | 433 | 9% |
| II | 916 | 19% |
| III | 327 | 7% |
| IV | 68 | 1% |
| V | 63 | 1% |
| Not reported | 2901 | 62% |
| Mean | SD | |
| Age | 6.8 years | 1.3 months |
| Outcome Measure | Count | Citations |
|---|---|---|
| Canadian Occupational Performance Measure (COPM) | 44 | [13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56] |
| Goal Attainment Scale (GAS) | 39 | [13,14,15,20,23,29,30,31,32,33,34,35,36,39,40,43,44,46,52,53,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74] |
| Gross Motor Function Measure (GMFM) | 37 | [16,17,19,31,36,41,45,46,52,55,59,63,64,65,66,68,69,72,73,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92] |
| Pediatric Evaluation of Disability Inventory (PEDI) | 31 | [16,17,19,21,24,25,27,30,32,37,39,41,45,51,52,62,63,64,65,67,69,71,72,74,75,82,83,84,86,88,93] |
| Assisting Hand Assessment (AHA) | 25 | [13,14,21,26,32,38,47,48,49,51,53,54,56,61,63,93,94,95,96,97,98,99,100,101,102] |
| Box and Block Test (BBT) | 15 | [19,20,25,26,27,28,51,63,80,89,98,100,101,103,104] |
| Jebson-Taylor Hand Function Test (JTHFT) | 12 | [27,32,46,47,51,61,95,100,101,102,103,105] |
| ABILHAND-kids | 12 | [13,14,19,21,28,36,46,51,53,96,102,103] |
| Quality of Upper Extremity Skills Test (QUEST) | 10 | [32,39,40,43,61,62,67,72,94,106] |
| The Modified Ashworth Scale (MAS) | 8 | [39,56,73,76,98,107,108,109] |
| The Melbourne Assessment of Unilateral Upper Limb Function (MUUL) | 7 | [13,14,48,49,96,101,108] |
| Minute Walk Test (1, 2, 6, or 10) | 6 | [19,55,80,93,110,111] |
| Peabody Developmental Motor Scales (PDMS) | 5 | [15,43,74,106,112] |
| Bruininks-Oseretsky Test of Motor Proficiency (BOT) | 5 | [29,80,83,95,113] |
| Performance Quality Rating Scale (PQRS) | 5 | [30,37,42,89,114] |
| Steps | Specific Guidelines | Associated Themes |
|---|---|---|
| 1. Goal Setting: Identify individualized goals | 1a: The collaborative approach begins with multiple stakeholders, including the client, parent, teacher, and therapy team. | Collaborative goal setting, Family-centered, Multidisciplinary approaches |
| 1b: The goals should have a functional focus and should target meaningful activities. | ||
| 1c: The goals should be defined and measurable. | ||
| 2. Goal Analysis: Identify goal limiting factors | 2a: It is important to determine what skills are needed, which skills are difficult, and which skills are strengths. These will be assessed through baseline measurements. | Family-centered, Social engagement, Multidisciplinary Approach, Outcome monitoring (2a) |
| 2b: Task analysis will need to be performed to determine any barriers and facilitators. The provider will need to consider multiple domains which can include motor, cognition, social, communication, and the environment. | ||
| 3. Determine Strategies and Practice | 3a: The provider will then need to determine the approach. The approach can be remedial, accommodative, include modifications, mixed, evidence-based, or family preference depending on their needs. | Family-centered, Specific training techniques, Therapy dose (3d), Social engagement (3c), Multidisciplinary approach |
| 3b: When determining the activities and tasks, the provider will need to provide the family and child with motivation, seeking out the best way to engage them, and finding the just right challenge. | ||
| 3c: The provider will then need to determine the environmental supports including the different domains of social, physical, modifications, products, and technology. | ||
| 3d: The provider will determine the dose, which is the amount of time to practice the skill or goal together. | ||
| 3e: The provider will need to educate the family and client on the intervention strategies through practicing the skill or goal together. | ||
| 4. Targeted Practice of the Skill/Goal | Family-centered (especially at home), Specific training techniques, Therapy dose, Social engagement (depending on if their goal is social or performed in social contexts), Multidisciplinary approach | |
| 5. Provide Feedback and Progressive Tailoring | Continue step 4 throughout this process while in collaboration with the therapy team, the family, and the client. | Family-centered, Specific training techniques, Therapy dose, Social engagement (depending on if their goal is social or performed in social contexts), Multidisciplinary approach, Outcome monitoring |
| 6. Re-evaluate, Progress Tracking | Continue to collaborate with the therapy team, the family, and the client. At this time, it is important to re-evaluate Step 2 ‘Goal Analysis’ as needed, depending on the client’s progress with the skill or goal. | Family-centered, Specific training techniques, Therapy dose, Social engagement (because you go back to step 2), Multidisciplinary approach, Outcome monitoring |
| 7. Practice Goal Across Contexts | Continue practice until mastery of the goal is achieved within different contexts of their daily life. | Family-centered, Specific training techniques, Therapy dose, Social engagement, Multidisciplinary approach |
| 8. Evaluate Need for New Goals | Collaborative goal setting, Family-centered, Multidisciplinary approach, Outcome monitoring |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shierk, A.; Barry Thias, B.; Becker, H.; Allen, B.; Chaiprasert, B.; Lampe, K.C.; Wallace-McCollom, A.; O’Brien, A.; Roberts, H. Defining Goal-Directed Training for Children with Cerebral Palsy: A Scoping Review and Framework for Implementation. Children 2025, 12, 1039. https://doi.org/10.3390/children12081039
Shierk A, Barry Thias B, Becker H, Allen B, Chaiprasert B, Lampe KC, Wallace-McCollom A, O’Brien A, Roberts H. Defining Goal-Directed Training for Children with Cerebral Palsy: A Scoping Review and Framework for Implementation. Children. 2025; 12(8):1039. https://doi.org/10.3390/children12081039
Chicago/Turabian StyleShierk, Angela, Bridget Barry Thias, Haley Becker, Baylee Allen, Benjamin Chaiprasert, Katherine C. Lampe, Ava Wallace-McCollom, Aidan O’Brien, and Heather Roberts. 2025. "Defining Goal-Directed Training for Children with Cerebral Palsy: A Scoping Review and Framework for Implementation" Children 12, no. 8: 1039. https://doi.org/10.3390/children12081039
APA StyleShierk, A., Barry Thias, B., Becker, H., Allen, B., Chaiprasert, B., Lampe, K. C., Wallace-McCollom, A., O’Brien, A., & Roberts, H. (2025). Defining Goal-Directed Training for Children with Cerebral Palsy: A Scoping Review and Framework for Implementation. Children, 12(8), 1039. https://doi.org/10.3390/children12081039






