MGMT Promoter Methylation as a Prognostic Factor in Primary Glioblastoma: A Single-Institution Observational Study
Abstract
1. Introduction
2. Materials and Methods
Statistical Analysis
3. Results
4. Discussion
4.1. MGMT Methylation Assessing Methods’ Limitations
4.2. Mismatch Repair (MMR) Deficiency
4.3. MGMT Inhibitors
4.4. Practical Application of MGMT Promoter Methylation Status
4.5. Limitations to This Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Louis, D.N.; Ohgaki, H.; Wiestler, O.D.; Cavenee, W.K.; Burger, P.C.; Jouvet, A.; Scheithauer, B.W.; Kleihues, P. The 2007 WHO Classification of Tumours of the Central Nervous System. Acta Neuropathol. 2007, 114, 97–109. [Google Scholar] [CrossRef] [PubMed]
- Müller Bark, J.; Kulasinghe, A.; Chua, B.; Day, B.W.; Punyadeera, C. Circulating Biomarkers in Patients with Glioblastoma. Br. J. Cancer 2020, 122, 295–305. [Google Scholar] [CrossRef] [PubMed]
- Furtak, J.; Kwiatkowski, A.; Śledzińska, P.; Bebyn, M.; Krajewski, S.; Szylberg, T.; Birski, M.; Druszcz, A.; Krystkiewicz, K.; Gasiński, P.; et al. Survival after Reoperation for Recurrent Glioblastoma Multiforme: A Prospective Study. Surg. Oncol. 2022, 42, 101771. [Google Scholar] [CrossRef] [PubMed]
- Miranda, A.; Blanco-Prieto, M.; Sousa, J.; Pais, A.; Vitorino, C. Breaching Barriers in Glioblastoma. Part I: Molecular Pathways and Novel Treatment Approaches. Int. J. Pharm. 2017, 531, 372–388. [Google Scholar] [CrossRef]
- Li, H.; Li, J.; Cheng, G.; Zhang, J.; Li, X. IDH Mutation and MGMT Promoter Methylation Are Associated with the Pseudoprogression and Improved Prognosis of Glioblastoma Multiforme Patients Who Have Undergone Concurrent and Adjuvant Temozolomide-Based Chemoradiotherapy. Clin. Neurol. Neurosurg. 2016, 151, 31–36. [Google Scholar] [CrossRef]
- Esteller, M.; Garcia-Foncillas, J.; Andion, E.; Goodman, S.N.; Hidalgo, O.F.; Vanaclocha, V.; Baylin, S.B.; Herman, J.G. Inactivation of the DNA-Repair Gene MGMT and the Clinical Response of Gliomas to Alkylating Agents. N. Engl. J. Med. 2000, 343, 1350–1354. [Google Scholar] [CrossRef]
- Hegi, M.E.; Diserens, A.-C.; Gorlia, T.; Hamou, M.-F.; de Tribolet, N.; Weller, M.; Kros, J.M.; Hainfellner, J.A.; Mason, W.; Mariani, L.; et al. MGMT Gene Silencing and Benefit from Temozolomide in Glioblastoma. N. Engl. J. Med. 2005, 352, 997–1003. [Google Scholar] [CrossRef]
- Villano, J.L.; Seery, T.E.; Bressler, L.R. Temozolomide in Malignant Gliomas: Current Use and Future Targets. Cancer Chemother. Pharmacol. 2009, 64, 647–655. [Google Scholar] [CrossRef]
- Kaina, B.; Christmann, M. DNA Repair in Personalized Brain Cancer Therapy with Temozolomide and Nitrosoureas. DNA Repair 2019, 78, 128–141. [Google Scholar] [CrossRef]
- Silber, J.R.; Blank, A.; Bobola, M.S.; Mueller, B.A.; Kolstoe, D.D.; Ojemann, G.A.; Berger, M.S. Lack of the DNA Repair Protein O6-Methylguanine-DNA Methyltransferase in Histologically Normal Brain Adjacent to Primary Human Brain Tumors. Proc. Natl. Acad. Sci. USA 1996, 93, 6941–6946. [Google Scholar] [CrossRef]
- Bobola, M.S.; Alnoor, M.; Chen, J.Y.-S.; Kolstoe, D.D.; Silbergeld, D.L.; Rostomily, R.C.; Blank, A.; Chamberlain, M.C.; Silber, J.R. O6-Methylguanine-DNA Methyltransferase Activity Is Associated with Response to Alkylating Agent Therapy and with MGMT Promoter Methylation in Glioblastoma and Anaplastic Glioma. BBA Clin. 2015, 3, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Yuan, G.; Niu, L.; Zhang, Y.; Wang, X.; Ma, K.; Yin, H.; Dai, J.; Zhou, W.; Pan, Y. Defining Optimal Cutoff Value of MGMT Promoter Methylation by ROC Analysis for Clinical Setting in Glioblastoma Patients. J. Neurooncol. 2017, 133, 193–201. [Google Scholar] [CrossRef] [PubMed]
- Binabaj, M.M.; Bahrami, A.; ShahidSales, S.; Joodi, M.; Joudi Mashhad, M.; Hassanian, S.M.; Anvari, K.; Avan, A. The Prognostic Value of MGMT Promoter Methylation in Glioblastoma: A Meta-Analysis of Clinical Trials. J. Cell. Physiol. 2018, 233, 378–386. [Google Scholar] [CrossRef] [PubMed]
- Cabrini, G.; Fabbri, E.; Lo Nigro, C.; Dechecchi, M.C.; Gambari, R. Regulation of Expression of O6-Methylguanine-DNA Methyltransferase and the Treatment of Glioblastoma (Review). Int. J. Oncol. 2015, 47, 417–428. [Google Scholar] [CrossRef] [PubMed]
- Verbeek, B.; Southgate, T.D.; Gilham, D.E.; Margison, G.P. O6-Methylguanine-DNA Methyltransferase Inactivation and Chemotherapy. Br. Med. Bull. 2008, 85, 17–33. [Google Scholar] [CrossRef] [PubMed]
- Wiewrodt, D.; Nagel, G.; Dreimüller, N.; Hundsberger, T.; Perneczky, A.; Kaina, B. MGMT in Primary and Recurrent Human Glioblastomas after Radiation and Chemotherapy and Comparison with P53 Status and Clinical Outcome. Int. J. Cancer 2008, 122, 1391–1399. [Google Scholar] [CrossRef]
- Chiang, J.; Harreld, J.H.; Tinkle, C.L.; Moreira, D.C.; Li, X.; Acharya, S.; Qaddoumi, I.; Ellison, D.W. A Single-Center Study of the Clinicopathologic Correlates of Gliomas with a MYB or MYBL1 Alteration. Acta Neuropathol. 2019, 138, 1091–1092. [Google Scholar] [CrossRef]
- Yang, P.; Zhang, W.; Wang, Y.; Peng, X.; Chen, B.; Qiu, X.; Li, G.; Li, S.; Wu, C.; Yao, K.; et al. IDH Mutation and MGMT Promoter Methylation in Glioblastoma: Results of a Prospective Registry. Oncotarget 2015, 6, 40896–40906. [Google Scholar] [CrossRef]
- Roszkowski, K.; Furtak, J.; Zurawski, B.; Szylberg, T.; Lewandowska, M.A. Potential Role of Methylation Marker in Glioma Supporting Clinical Decisions. Int. J. Mol. Sci. 2016, 17, 1876. [Google Scholar] [CrossRef]
- Stupp, R.; Hegi, M.E.; Mason, W.P.; van den Bent, M.J.; Taphoorn, M.J.B.; Janzer, R.C.; Ludwin, S.K.; Allgeier, A.; Fisher, B.; Belanger, K.; et al. Effects of Radiotherapy with Concomitant and Adjuvant Temozolomide versus Radiotherapy Alone on Survival in Glioblastoma in a Randomised Phase III Study: 5-Year Analysis of the EORTC-NCIC Trial. Lancet Oncol. 2009, 10, 459–466. [Google Scholar] [CrossRef]
- Zhao, H.; Wang, S.; Song, C.; Zha, Y.; Li, L. The Prognostic Value of MGMT Promoter Status by Pyrosequencing Assay for Glioblastoma Patients’ Survival: A Meta-Analysis. World J. Surg. Oncol. 2016, 14, 261. [Google Scholar] [CrossRef] [PubMed]
- Zawlik, I.; Vaccarella, S.; Kita, D.; Mittelbronn, M.; Franceschi, S.; Ohgaki, H. Promoter Methylation and Polymorphisms of the MGMT Gene in Glioblastomas: A Population-Based Study. Neuroepidemiology 2009, 32, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Abhinav, K.; Aquilina, K.; Gbejuade, H.; La, M.; Hopkins, K.; Iyer, V. A Pilot Study of Glioblastoma Multiforme in Elderly Patients: Treatments, O-6-Methylguanine-DNA Methyltransferase (MGMT) Methylation Status and Survival. Clin. Neurol. Neurosurg. 2013, 115, 1375–1378. [Google Scholar] [CrossRef] [PubMed]
- Jovanović, N.; Mitrović, T.; Cvetković, V.J.; Tošić, S.; Vitorović, J.; Stamenković, S.; Nikolov, V.; Kostić, A.; Vidović, N.; Jevtović-Stoimenov, T.; et al. Prognostic Significance of MGMT Promoter Methylation in Diffuse Glioma Patients. Biotechnol. Biotechnol. Equip. 2019, 33, 639–644. [Google Scholar] [CrossRef]
- Śledzińska, P.; Bebyn, M.G.; Furtak, J.; Kowalewski, J.; Lewandowska, M.A. Prognostic and Predictive Biomarkers in Gliomas. Int. J. Mol. Sci. 2021, 22, 10373. [Google Scholar] [CrossRef]
- Péus, D.; Newcomb, N.; Hofer, S. Appraisal of the Karnofsky Performance Status and Proposal of a Simple Algorithmic System for Its Evaluation. BMC Med. Inform. Decis. Mak. 2013, 13, 72. [Google Scholar] [CrossRef]
- Park, J.-H.; Kim, D.-H.; Kim, B.-R.; Kim, Y.-W. The American Society of Anesthesiologists Score Influences on Postoperative Complications and Total Hospital Charges after Laparoscopic Colorectal Cancer Surgery. Medicine 2018, 97, e0653. [Google Scholar] [CrossRef]
- Thon, N.; Kreth, S.; Kreth, F.-W. Personalized Treatment Strategies in Glioblastoma: MGMT Promoter Methylation Status. OncoTargets Ther. 2013, 6, 1363–1372. [Google Scholar] [CrossRef]
- Iaccarino, C.; Orlandi, E.; Ruggeri, F.; Nicoli, D.; Torricelli, F.; Maggi, M.; Cerasti, D.; Pisanello, A.; Pedrazzi, G.; Froio, E.; et al. Prognostic Value of MGMT Promoter Status in Non-Resectable Glioblastoma after Adjuvant Therapy. Clin. Neurol. Neurosurg. 2015, 132, 1–8. [Google Scholar] [CrossRef]
- Radke, J.; Koch, A.; Pritsch, F.; Schumann, E.; Misch, M.; Hempt, C.; Lenz, K.; Löbel, F.; Paschereit, F.; Heppner, F.L.; et al. Predictive MGMT Status in a Homogeneous Cohort of IDH Wildtype Glioblastoma Patients. Acta Neuropathol. Commun. 2019, 7, 89. [Google Scholar] [CrossRef]
- Dunn, J.; Baborie, A.; Alam, F.; Joyce, K.; Moxham, M.; Sibson, R.; Crooks, D.; Husband, D.; Shenoy, A.; Brodbelt, A.; et al. Extent of MGMT Promoter Methylation Correlates with Outcome in Glioblastomas given Temozolomide and Radiotherapy. Br. J. Cancer 2009, 101, 124–131. [Google Scholar] [CrossRef] [PubMed]
- Ohgaki, H.; Dessen, P.; Jourde, B.; Horstmann, S.; Nishikawa, T.; Di Patre, P.-L.; Burkhard, C.; Schüler, D.; Probst-Hensch, N.M.; Maiorka, P.C.; et al. Genetic Pathways to Glioblastoma: A Population-Based Study. Cancer Res. 2004, 64, 6892–6899. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Yu, L.; Gaiteri, C.; Srivastava, G.P.; Chibnik, L.B.; Leurgans, S.E.; Schneider, J.A.; Meissner, A.; De Jager, P.L.; Bennett, D.A. Association of DNA Methylation in the Brain with Age in Older Persons Is Confounded by Common Neuropathologies. Int. J. Biochem. Cell Biol. 2015, 67, 58–64. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wood, J.R.; Green, S.B.; Shapiro, W.R. The Prognostic Importance of Tumor Size in Malignant Gliomas: A Computed Tomographic Scan Study by the Brain Tumor Cooperative Group. J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol. 1988, 6, 338–343. [Google Scholar] [CrossRef] [PubMed]
- Lacroix, M.; Abi-Said, D.; Fourney, D.R.; Gokaslan, Z.L.; Shi, W.; DeMonte, F.; Lang, F.F.; McCutcheon, I.E.; Hassenbusch, S.J.; Holland, E.; et al. A Multivariate Analysis of 416 Patients with Glioblastoma Multiforme: Prognosis, Extent of Resection, and Survival. J. Neurosurg. 2001, 95, 190–198. [Google Scholar] [CrossRef]
- McGirt, M.J.; Chaichana, K.L.; Gathinji, M.; Attenello, F.J.; Than, K.; Olivi, A.; Weingart, J.D.; Brem, H.; Quiñones-Hinojosa, A.R. Independent Association of Extent of Resection with Survival in Patients with Malignant Brain Astrocytoma. J. Neurosurg. 2009, 110, 156–162. [Google Scholar] [CrossRef]
- Cancer Genome Atlas Research Network; Brat, D.J.; Verhaak, R.G.W.; Aldape, K.D.; Yung, W.K.A.; Salama, S.R.; Cooper, L.A.D.; Rheinbay, E.; Miller, C.R.; Vitucci, M.; et al. Comprehensive, Integrative Genomic Analysis of Diffuse Lower-Grade Gliomas. N. Engl. J. Med. 2015, 372, 2481–2498. [Google Scholar] [CrossRef]
- Shu, C.; Wang, Q.; Yan, X.; Wang, J. The TERT Promoter Mutation Status and MGMT Promoter Methylation Status, Combined with Dichotomized MRI-Derived and Clinical Features, Predict Adult Primary Glioblastoma Survival. Cancer Med. 2018, 7, 3704–3712. [Google Scholar] [CrossRef]
- Reis Prognostic Value of MGMT Promoter Methylation in Glioblastoma Patients Treated with Temozolomide-Based Chemoradiation: A Portuguese Multicentre Study. Oncol. Rep. 2010, 23, 1655–1662. [CrossRef]
- Zhang, K.; Wang, X.; Zhou, B.; Zhang, L. The Prognostic Value of MGMT Promoter Methylation in Glioblastoma Multiforme: A Meta-Analysis. Fam. Cancer 2013, 12, 449–458. [Google Scholar] [CrossRef]
- SongTao, Q.; Lei, Y.; Si, G.; YanQing, D.; HuiXia, H.; XueLin, Z.; LanXiao, W.; Fei, Y. IDH Mutations Predict Longer Survival and Response to Temozolomide in Secondary Glioblastoma. Cancer Sci. 2012, 103, 269–273. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Liang, R.; Song, C.; Xiang, Y.; Liu, Y. Prognostic and Clinicopathological Significance of Long Non-Coding RNA in Glioma. Neurosurg. Rev. 2020, 43. [Google Scholar] [CrossRef] [PubMed]
- Chai, R.; Li, G.; Liu, Y.; Zhang, K.; Zhao, Z.; Wu, F.; Chang, Y.; Pang, B.; Li, J.; Li, Y.; et al. Predictive Value of MGMT Promoter Methylation on the Survival of TMZ Treated IDH-Mutant Glioblastoma. Cancer Biol. Med. 2021, 18, 271–282. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, H.N.; Lie, A.; Li, T.; Chowdhury, R.; Liu, F.; Ozer, B.; Wei, B.; Green, R.M.; Ellingson, B.M.; Wang, H.; et al. Human TERT Promoter Mutation Enables Survival Advantage from MGMT Promoter Methylation in IDH1 Wild-Type Primary Glioblastoma Treated by Standard Chemoradiotherapy. Neuro-Oncology 2017, 19, 394–404. [Google Scholar] [CrossRef] [PubMed]
- Dahlrot, R.H.; Larsen, P.; Boldt, H.B.; Kreutzfeldt, M.S.; Hansen, S.; Hjelmborg, J.B.; Kristensen, B.W. Posttreatment Effect of MGMT Methylation Level on Glioblastoma Survival. J. Neuropathol. Exp. Neurol. 2019, 78, 633–640. [Google Scholar] [CrossRef]
- Uno, M.; Oba-Shinjo, S.M.; Camargo, A.A.; Moura, R.P.; de Aguiar, P.H.; Cabrera, H.N.; Begnami, M.; Rosemberg, S.; Teixeira, M.J.; Marie, S.K.N. Correlation of MGMT Promoter Methylation Status with Gene and Protein Expression Levels in Glioblastoma. Clinics 2011, 66, 1747–1755. [Google Scholar] [CrossRef]
- Lalezari, S.; Chou, A.P.; Tran, A.; Solis, O.E.; Khanlou, N.; Chen, W.; Li, S.; Carrillo, J.A.; Chowdhury, R.; Selfridge, J.; et al. Combined Analysis of O6-Methylguanine-DNA Methyltransferase Protein Expression and Promoter Methylation Provides Optimized Prognostication of Glioblastoma Outcome. Neuro-Oncology 2013, 15, 370–381. [Google Scholar] [CrossRef]
- Brell, M.; Ibáñez, J.; Tortosa, A. O6-Methylguanine-DNA Methyltransferase Protein Expression by Immunohistochemistry in Brain and Non-Brain Systemic Tumours: Systematic Review and Meta-Analysis of Correlation with Methylation-Specific Polymerase Chain Reaction. BMC Cancer 2011, 11, 35. [Google Scholar] [CrossRef]
- Melguizo, C.; Prados, J.; González, B.; Ortiz, R.; Concha, A.; Alvarez, P.J.; Madeddu, R.; Perazzoli, G.; Oliver, J.A.; López, R.; et al. MGMT Promoter Methylation Status and MGMT and CD133 Immunohistochemical Expression as Prognostic Markers in Glioblastoma Patients Treated with Temozolomide plus Radiotherapy. J. Transl. Med. 2012, 10, 250. [Google Scholar] [CrossRef]
- Wang, L.; Li, Z.; Liu, C.; Chen, L.; Liu, L.; Hu, Z.; Zhao, L.; Lu, D.; Teng, L. Comparative Assessment of Three Methods to Analyze MGMT Methylation Status in a Series of 350 Gliomas and Gangliogliomas. Pathol. Res. Pract. 2017, 213, 1489–1493. [Google Scholar] [CrossRef]
- Kreth, S.; Thon, N.; Eigenbrod, S.; Lutz, J.; Ledderose, C.; Egensperger, R.; Tonn, J.C.; Kretzschmar, H.A.; Hinske, L.C.; Kreth, F.W. O-Methylguanine-DNA Methyltransferase (MGMT) MRNA Expression Predicts Outcome in Malignant Glioma Independent of MGMT Promoter Methylation. PLoS ONE 2011, 6, e17156. [Google Scholar] [CrossRef] [PubMed]
- Riemenschneider, M.J.; Hegi, M.E.; Reifenberger, G. MGMT Promoter Methylation in Malignant Gliomas. Target. Oncol. 2010, 5, 161–165. [Google Scholar] [CrossRef]
- Weller, M.; Stupp, R.; Reifenberger, G.; Brandes, A.A.; van den Bent, M.J.; Wick, W.; Hegi, M.E. MGMT Promoter Methylation in Malignant Gliomas: Ready for Personalized Medicine? Nat. Rev. Neurol. 2010, 6, 39–51. [Google Scholar] [CrossRef]
- Christians, A.; Hartmann, C.; Benner, A.; Meyer, J.; von Deimling, A.; Weller, M.; Wick, W.; Weiler, M. Prognostic Value of Three Different Methods of MGMT Promoter Methylation Analysis in a Prospective Trial on Newly Diagnosed Glioblastoma. PLoS ONE 2012, 7, e33449. [Google Scholar] [CrossRef] [PubMed]
- Weller, M.; van den Bent, M.; Preusser, M.; Le Rhun, E.; Tonn, J.C.; Minniti, G.; Bendszus, M.; Balana, C.; Chinot, O.; Dirven, L.; et al. EANO Guidelines on the Diagnosis and Treatment of Diffuse Gliomas of Adulthood. Nat. Rev. Clin. Oncol. 2021, 18, 170–186. [Google Scholar] [CrossRef] [PubMed]
- Quillien, V.; Lavenu, A.; Karayan-Tapon, L.; Carpentier, C.; Labussière, M.; Lesimple, T.; Chinot, O.; Wager, M.; Honnorat, J.; Saikali, S.; et al. Comparative Assessment of 5 Methods (Methylation-Specific Polymerase Chain Reaction, MethyLight, Pyrosequencing, Methylation-Sensitive High-Resolution Melting, and Immunohistochemistry) to Analyze O6-Methylguanine-DNA-Methyltranferase in a Series of 100 Glioblastoma Patients. Cancer 2012, 118, 4201–4211. [Google Scholar] [CrossRef]
- Mason, S.; McDonald, K. MGMT Testing for Glioma in Clinical Laboratories: Discordance with Methylation Analyses Prevents the Implementation of Routine Immunohistochemistry. J. Cancer Res. Clin. Oncol. 2012, 138, 1789–1797. [Google Scholar] [CrossRef]
- Preusser, M.; Charles Janzer, R.; Felsberg, J.; Reifenberger, G.; Hamou, M.-F.; Diserens, A.-C.; Stupp, R.; Gorlia, T.; Marosi, C.; Heinzl, H.; et al. Anti-O6-Methylguanine-Methyltransferase (MGMT) Immunohistochemistry in Glioblastoma Multiforme: Observer Variability and Lack of Association with Patient Survival Impede Its Use as Clinical Biomarker. Brain Pathol. 2008, 18, 520–532. [Google Scholar] [CrossRef]
- Liu, L.; Spiro, T.P.; Qin, X.; Majka, S.; Haaga, J.; Schupp, J.; Willson, J.K.; Gerson, S.L. Differential Degradation Rates of Inactivated Alkyltransferase in Blood Mononuclear Cells and Tumors of Patients after Treatment with O(6)-Benzylguanine. Clin. Cancer Res. Off. J. Am. Assoc. Cancer Res. 2001, 7, 2318–2324. [Google Scholar]
- Reifenberger, G.; Hentschel, B.; Felsberg, J.; Schackert, G.; Simon, M.; Schnell, O.; Westphal, M.; Wick, W.; Pietsch, T.; Loeffler, M.; et al. Predictive Impact of MGMT Promoter Methylation in Glioblastoma of the Elderly. Int. J. Cancer 2012, 131, 1342–1350. [Google Scholar] [CrossRef]
- Gurrieri, L.; De Carlo, E.; Gerratana, L.; De Maglio, G.; Macerelli, M.; Pisa, F.E.; Masiero, E.; Aprile, G.; Follador, A.; Puglisi, F.; et al. MGMT Pyrosequencing-Based Cut-off Methylation Level and Clinical Outcome in Patients with Glioblastoma Multiforme. Future Oncol. 2018, 14, 699–707. [Google Scholar] [CrossRef] [PubMed]
- Mansouri, A.; Hachem, L.D.; Mansouri, S.; Nassiri, F.; Laperriere, N.J.; Xia, D.; Lindeman, N.I.; Wen, P.Y.; Chakravarti, A.; Mehta, M.P.; et al. MGMT Promoter Methylation Status Testing to Guide Therapy for Glioblastoma: Refining the Approach Based on Emerging Evidence and Current Challenges. Neuro-Oncology 2019, 21, 167–178. [Google Scholar] [CrossRef] [PubMed]
- Jiapaer, S.; Furuta, T.; Tanaka, S.; Kitabayashi, T.; Nakada, M. Potential Strategies Overcoming the Temozolomide Resistance for Glioblastoma. Neurol. Med. Chir. 2018, 58, 405–421. [Google Scholar] [CrossRef] [PubMed]
- Nagel, Z.D.; Kitange, G.J.; Gupta, S.K.; Joughin, B.A.; Chaim, I.A.; Mazzucato, P.; Lauffenburger, D.A.; Sarkaria, J.N.; Samson, L.D. DNA Repair Capacity in Multiple Pathways Predicts Chemoresistance in Glioblastoma Multiforme. Cancer Res. 2017, 77, 198–206. [Google Scholar] [CrossRef] [PubMed]
- Blumenthal, D.T.; Rankin, C.; Stelzer, K.J.; Spence, A.M.; Sloan, A.E.; Moore, D.F.; Padula, G.D.A.; Schulman, S.B.; Wade, M.L.; Rushing, E.J. A Phase III Study of Radiation Therapy (RT) and O6-Benzylguanine + BCNU versus RT and BCNU Alone and Methylation Status in Newly Diagnosed Glioblastoma and Gliosarcoma: Southwest Oncology Group (SWOG) Study S0001. Int. J. Clin. Oncol. 2015, 20, 650–658. [Google Scholar] [CrossRef]
- Misawa, K.; Mochizuki, D.; Imai, A.; Mima, M.; Misawa, Y.; Mineta, H. Analysis of Site-Specific Methylation of Tumor-Related Genes in Head and Neck Cancer: Potential Utility as Biomarkers for Prognosis. Cancers 2018, 10, 27. [Google Scholar] [CrossRef]
- Wu, S.; Li, X.; Gao, F.; de Groot, J.F.; Koul, D.; Yung, W.K.A. PARP-Mediated PARylation of MGMT Is Critical to Promote Repair of Temozolomide-Induced O6-Methylguanine DNA Damage in Glioblastoma. Neuro-Oncology 2021, 23, 920–931. [Google Scholar] [CrossRef]
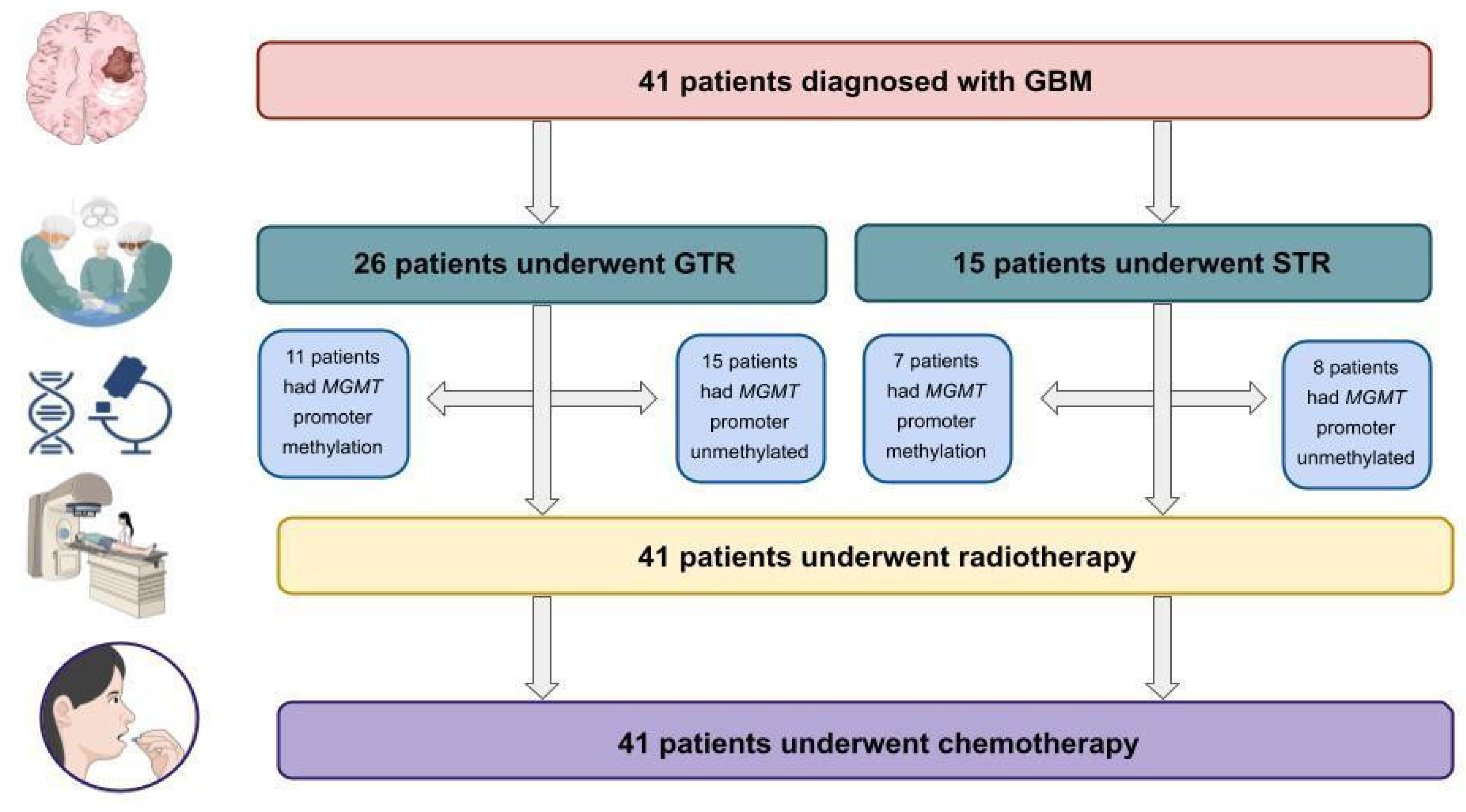
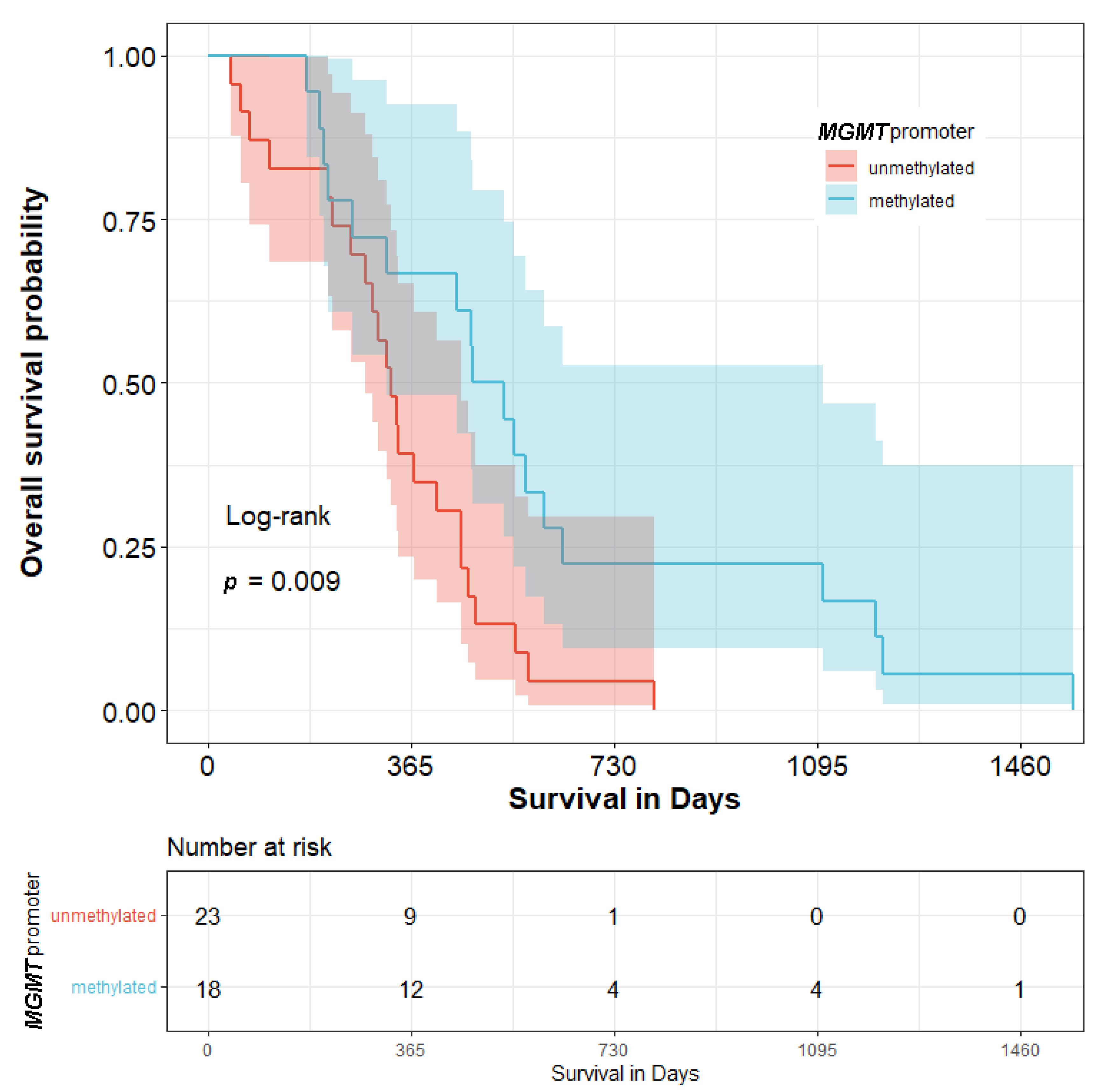

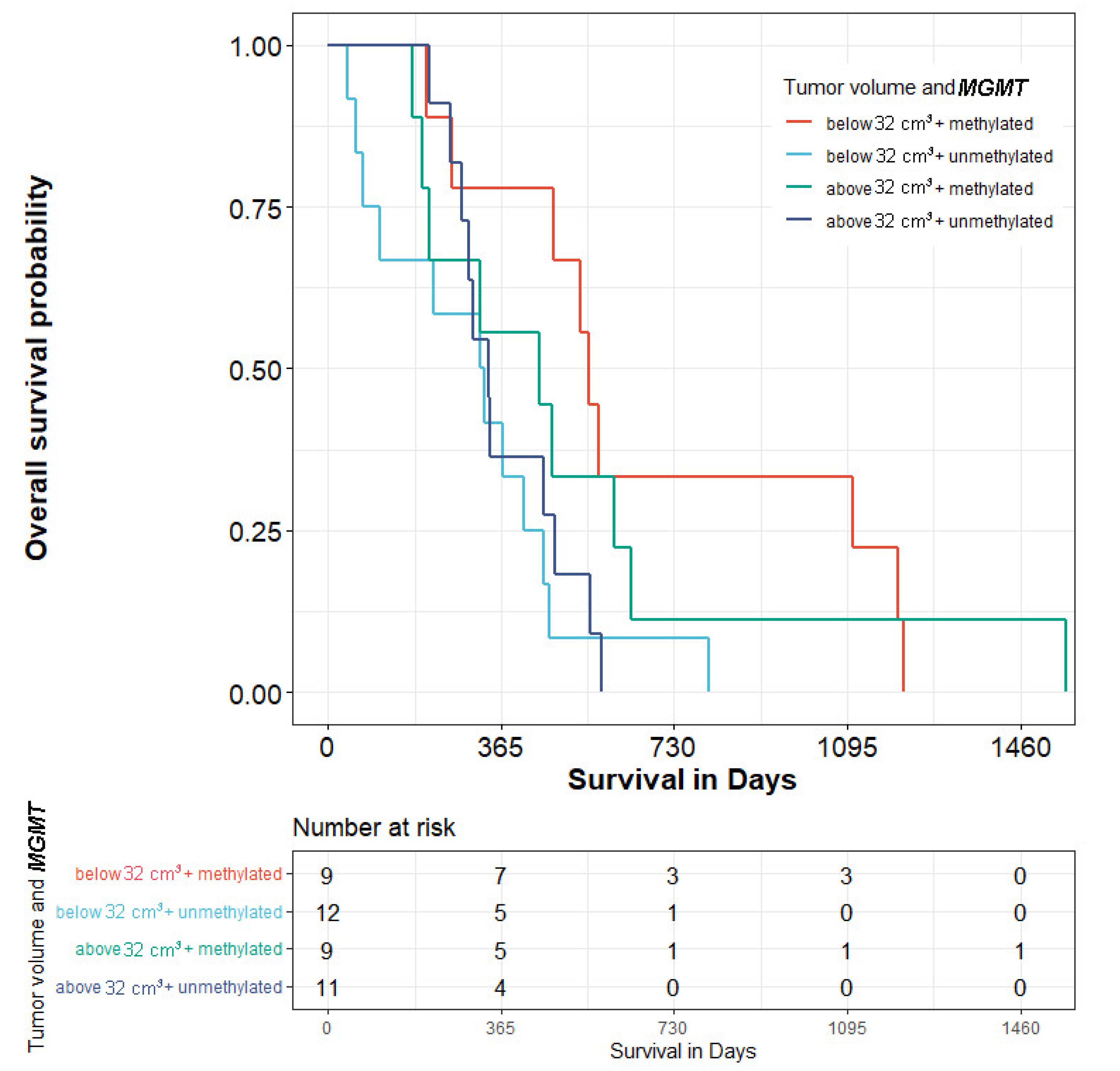
| N | % | ||
|---|---|---|---|
| Age, mean ± SD | 53 | 12 | |
| Sex | Female | 9 | 22% |
| Male | 32 | 78% | |
| Tumor Volume [cm3], mean ± SD | 38.1 | 24.6 | |
| The Extent of Resection | |||
| GTR | 26 | 63.4% | |
| STR | 15 | 36.6% | |
| KPS, mean ± SD | 90 | 7 | |
| MGMT Methylation Status | |||
| Unmethylated | 23 | 56.1% | |
| Methylated | 18 | 43.9% | |
| ASA score | |||
| 1 | 28 | 68.3% | |
| 2 | 10 | 24.4% | |
| 3 | 3 | 7.3% | |
| Location | |||
| Frontal | 8 | 19.5% | |
| Temporal | 25 | 61% | |
| Parietal | 6 | 14.6% | |
| Occipital | 1 | 2.4% | |
| Multifocal | 1 | 2.4% | |
| Variable | Number of Patients | MGMT Methylation | |
|---|---|---|---|
| Sex | Female | 9 | 5 |
| Male | 32 | 13 | |
| Age | ≤53 | 21 | 9 |
| >53 | 20 | 9 | |
| Tumor size (cm3) | ≤32 | 21 | 10 |
| >32 | 20 | 8 | |
| Resection rate | Gross total resection | 26 | 11 |
| Subtotal resection | 15 | 7 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Szylberg, M.; Sokal, P.; Śledzińska, P.; Bebyn, M.; Krajewski, S.; Szylberg, Ł.; Szylberg, A.; Szylberg, T.; Krystkiewicz, K.; Birski, M.; et al. MGMT Promoter Methylation as a Prognostic Factor in Primary Glioblastoma: A Single-Institution Observational Study. Biomedicines 2022, 10, 2030. https://doi.org/10.3390/biomedicines10082030
Szylberg M, Sokal P, Śledzińska P, Bebyn M, Krajewski S, Szylberg Ł, Szylberg A, Szylberg T, Krystkiewicz K, Birski M, et al. MGMT Promoter Methylation as a Prognostic Factor in Primary Glioblastoma: A Single-Institution Observational Study. Biomedicines. 2022; 10(8):2030. https://doi.org/10.3390/biomedicines10082030
Chicago/Turabian StyleSzylberg, Mateusz, Paweł Sokal, Paulina Śledzińska, Marek Bebyn, Stanisław Krajewski, Łukasz Szylberg, Aneta Szylberg, Tadeusz Szylberg, Kamil Krystkiewicz, Marcin Birski, and et al. 2022. "MGMT Promoter Methylation as a Prognostic Factor in Primary Glioblastoma: A Single-Institution Observational Study" Biomedicines 10, no. 8: 2030. https://doi.org/10.3390/biomedicines10082030
APA StyleSzylberg, M., Sokal, P., Śledzińska, P., Bebyn, M., Krajewski, S., Szylberg, Ł., Szylberg, A., Szylberg, T., Krystkiewicz, K., Birski, M., Harat, M., Włodarski, R., & Furtak, J. (2022). MGMT Promoter Methylation as a Prognostic Factor in Primary Glioblastoma: A Single-Institution Observational Study. Biomedicines, 10(8), 2030. https://doi.org/10.3390/biomedicines10082030







