Inter-Professional Collaboration and Occupational Well-Being of Physicians Who Work in Adverse Working Conditions
Abstract
:1. Introduction
2. Methods
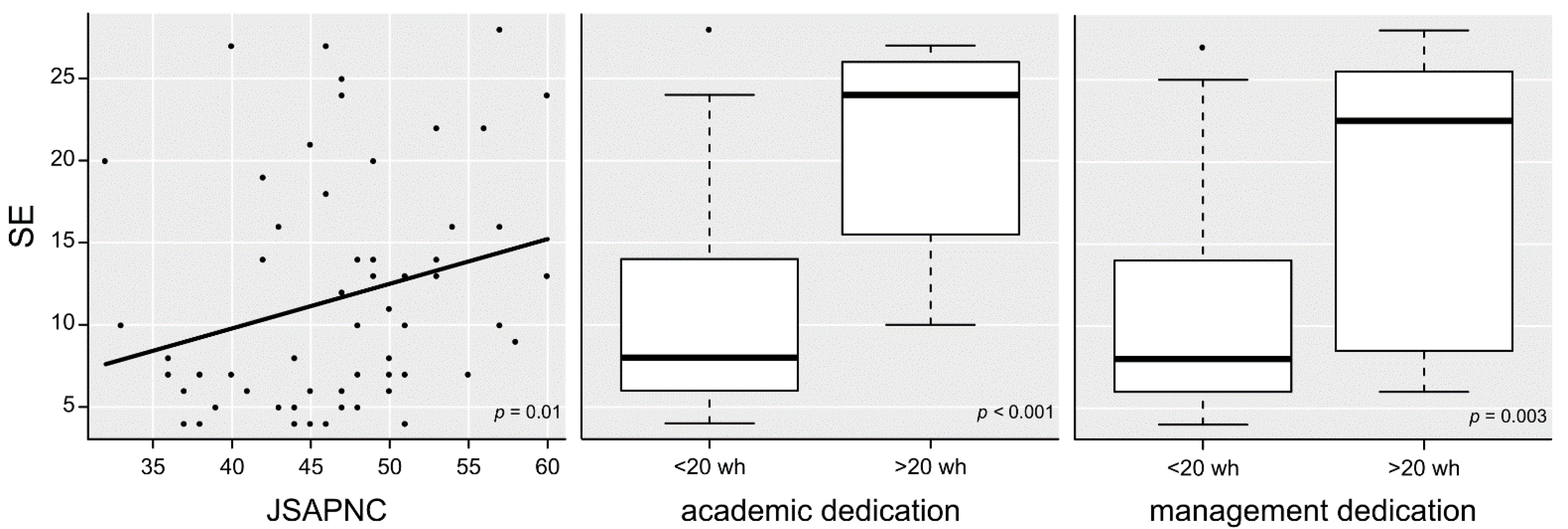
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stern, D.T. What is medical professionalism? In Measuring Medical Professionalism; Stern, D.T., Ed.; Oxford University Press: New York, NY, USA, 2006; pp. 15–38. [Google Scholar]
- Siegrist, J. Effort-Reward Imbalance Model. In Stress: Concepts, Cognition, Emotion, and Behavior; Fink, G., Ed.; Elsevier: Amsterdam, The Netherlands, 2016; pp. 81–86. ISBN 9780128009512. [Google Scholar]
- West, C.P.; Shanafelt, T.D. Physician well-being and professionalism. Minn. Med. 2007, 90, 44–46. [Google Scholar]
- Cole, T.R.; Carlin, N. The suffering of physicians. Lancet 2009, 374, 1414–1415. [Google Scholar] [CrossRef]
- Karasek, R.A.; Theorell, T. Healthy Work: Stress Productivity and the Reconstruction of Working Life; Basic Books: New York, NY, USA, 1992; ISBN 978-0465028979. [Google Scholar]
- San-Martín, M.; Delgado-Bolton, R.; Vivanco, L. Professionalism and occupational well-being: Similarities and differences among latin american health professionals. Front. Psychol. 2017, 8, 1–10. [Google Scholar] [CrossRef] [Green Version]
- Grau Martín, A.; Flichtentrei, D.; Suñer, R.; Prats, M.; Braga, F. Influence of personal, professional and cross-national factors in burnout syndrome in Hispanic Americans and Spanish health workers (2007). Rev. Esp. Salud Publica 2009, 83, 215–230. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Atun, R.; De Andrade, L.O.M.; Almeida, G.; Cotlear, D.; Dmytraczenko, T.; Frenz, P.; Garcia, P.; Gómez-Dantés, O.; Knaul, F.M.; Muntaner, C.; et al. Health-system reform and universal health coverage in Latin America. Lancet 2015, 385, 1230–1247. [Google Scholar] [CrossRef]
- Dal Poz, M.R.; Sepulveda, H.R.; Costa Couto, M.H.; Godue, C.; Padilla, M.; Cameron, R.; Vidaurre Franco, T.D.A. Assessment of human resources for health programme implementation in 15 Latin American and Caribbean countries. Hum. Resour. Health 2015, 13, 24. [Google Scholar] [CrossRef] [Green Version]
- Vian, T. Review of corruption in the health sector: Theory, methods and interventions. Health Policy Plan. 2008, 23, 83–94. [Google Scholar] [CrossRef] [Green Version]
- Pastrana, T.; Torres-Vigil, I.; De Lima, L. Palliative care development in Latin America: An analysis using macro indicators. Palliat. Med. 2014, 28, 1231–1238. [Google Scholar] [CrossRef] [Green Version]
- Alvarez, F.N.; Leys, M.; Mérida, H.E.R.; Guzmán, G.E. Primary health care research in Bolivia: Systematic review and analysis. Health Policy Plan. 2016, 31, 114–128. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zapana, V. El Defensor denuncia “pésimo estado” del Hospital de Clínicas. Diario Página Siete. Available online: https://www.paginasiete.bo/sociedad/2016/3/11/defensor-denuncia-pesimo-estado-hospital-clinicas-89454.html (accessed on 8 September 2021).
- Villena-Villegas, R. Informe de la gestión del Defensor del Pueblo (2010–2016); Defensoría del Pueblo: La Paz, Bolivia, 2016. [Google Scholar]
- Bendezu-Quispe, G.; León, F.; Moreno, J.; Inga-Berrospi, F. Characteristics of compulsory service programs for medical professionals in the Andean states. Medwave 2020, 20, e7848. [Google Scholar] [CrossRef]
- Cruz Tarifa, N. Informe Defensorial: Salud, Derechos Humanos y COVID-19 en Bolivia; Defensoria del Pueblo: La Paz, Bolivia, 2021. [Google Scholar]
- Blanch, J.M.; Sahagun, M.; Cantera, L.; Cervantes, G. Cuestionario de Bienestar Laboral General: Estructura y Propiedades Psicométricas. Rev. Psicol. Trab. Organ. 2010, 26, 157–170. [Google Scholar] [CrossRef] [Green Version]
- Hojat, M.; Fields, S.K.; Veloski, J.J.; Griffiths, M.; Cohen, M.J.M.; Plumb, J.D. Psychometric Properties of an Attitude Scale Measuring Physician-Nurse Collaboration. Eval. Health Prof. 1999, 22, 208–220. [Google Scholar] [CrossRef]
- Alcorta-Garza, A.; San-Martín, M.; Delgado-Bolton, R.; Soler-González, J.; Roig, H.; Vivanco, L. Cross-Validation of the Spanish HP-Version of the Jefferson Scale of Empathy Confirmed with Some Cross-Cultural Differences. Front. Psychol. 2016, 7, 1002. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hojat, M.; Veloski, J.J.; Gonnella, J.S. Measurement and correlates of physicians’ lifelong learning. Acad. Med. 2009, 84, 1066–1074. [Google Scholar] [CrossRef] [PubMed]
- Frost, M.H.; Reeve, B.B.; Liepa, A.M.; Stauffer, J.W.; Hays, R.D.; Sloan, J.A. What is sufficient evidence for the reliability and validity of patient-reported outcome measures? Value Health 2007, 10, 94–105. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fritz, C.O.; Morris, P.E.; Richler, J.J. Effect size estimates: Current use, calculations, and interpretation. J. Exp. Psychol. Gen. 2012, 141, 2–18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tomczak, M.; Tomczak, E. The need to report effect size estimates revisited. An overview of some recommended measures of effect size. Trends Sport Sci. 2014, 1, 19–25. [Google Scholar]
- Hojat, M.; Xu, G. A visitor’s guide to effect sizes: Statistical significance versus practical (clinical) importance of research findings. Adv. Health Sci. Educ. Theory Pract. 2004, 9, 241–249. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates Publishers: New York, NY, USA, 1988. [Google Scholar]
- Bliese, P. Multilevel: Multilevel Functions. Available online: https://cran.r-project.org/web/packages/multilevel/index.html (accessed on 8 September 2021).
- Kassambara, A. Rstatix: Pipe-Friendly Framework for Basic Statistical Tests. Available online: https://cran.r-project.org/web/packages/rstatix/index.html (accessed on 8 September 2021).
- Navarro, D. lsr: Companion to “Learning Statistics with R”. Available online: https://cran.r-project.org/web/packages/lsr/ (accessed on 8 September 2021).
- Gross, J. nortest: Tests for Normality. Available online: https://cran.r-project.org/web/packages/nortest/index.html (accessed on 22 January 2021).
- San-Martín, M.; Roig-Carrera, H.; Villalonga-Vadell, R.M.; Benito-Sevillano, C.; Torres-Salinas, M.; Claret-Teruel, G.; Robles, B.; Sans-Boix, A.; Alcorta-Garza, A.; Vivanco, L. Empathy, inter-professional collaboration, and lifelong medical learning in Spanish and Latin-American physicians-in-training who start their postgraduate training in hospitals in Spain. Preliminary outcomes. Aten. Primaria 2017, 49, 6–12. [Google Scholar] [CrossRef] [Green Version]
- Zapana, V. Galenos y Víctimas de Negligencia Intercambian Insultos en Marchas. Diario Página Siete. Available online: https://www.paginasiete.bo/sociedad/2016/7/21/galenos-victimas-negligencia-intercambian-insultos-marchas-103508.html (accessed on 8 September 2021).
- Berduzco-Torres, N.; Choquenaira-Callañaupa, B.; Medina, P.; Chihuantito-Abal, L.A.; Caballero, S.; Gallegos, E.; San-Martín, M.; Delgado Bolton, R.C.; Vivanco, L. Factors Related to the Differential Development of Inter-Professional Collaboration Abilities in Medicine and Nursing Students. Front. Psychol. 2020, 11, 432. [Google Scholar] [CrossRef]
- Muliira, J.K.; Etyang, C.; Muliira, R.S.; Kizza, I.B. Nurses’ orientation toward lifelong learning: A case study of Uganda’s national hospital. J. Contin. Educ. Nurs. 2012, 43, 90–96. [Google Scholar] [CrossRef] [PubMed]
- Pisanti, R.; Van der Doef, M.; Maes, S.; Meier, L.L.; Lazzari, D.; Violani, C. How Changes in Psychosocial Job Characteristics Impact Burnout in Nurses: A Longitudinal Analysis. Front. Psychol. 2016, 7, 1082. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Statistics | JSE | JSAPNC | JeffSPLL | SS | SE | SA |
|---|---|---|---|---|---|---|
| Range possible | 20–140 | 15–60 | 14–56 | 5–35 | 4–28 | 4–28 |
| Range observed | 81–134 | 32–60 | 31–56 | 5–33 | 4–28 | 4–24 |
| Mean | 101 | 47 | 47 | 13 | 12 | 9 |
| Standard deviation (SD) | 15 | 7 | 6 | 8 | 7 | 5 |
| Quartile | ||||||
| 1st | 88 | 42 | 44 | 8 | 6 | 5 |
| 2nd (Median) | 94 | 47 | 48 | 10 | 10 | 7 |
| 3rd | 114 | 51 | 51 | 18 | 16 | 13 |
| Reliability | 0.82 | 0.84 | 0.87 | 0.90 | 0.92 | 0.87 |
| JSE | JSAPNC | JeffSPLL | SS | SE | SA | Age | |
|---|---|---|---|---|---|---|---|
| JSE | 1 | ||||||
| JSAPNC | +0.32 * | 1 | |||||
| JeffSPLL | +0.48 *** | +0.45 *** | 1 | ||||
| SS | +0.19 | +0.24 | +0.19 | 1 | |||
| SE | +0.13 | +0.29 * | +0.21 | +0.83 *** | 1 | ||
| SA | +0.00 | +0.21 | +0.03 | +0.54 *** | +0.65 *** | 1 | |
| Age | −0.19 | +0.07 | +0.11 | −0.13 | −0.19 | −0.07 | 1 |
| Study Groups | n | Somatization (SS) | Exhaustion (SE) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Mdn | M (SD) | p | r | Mdn | M (SD) | p | r | ||
| Gender | |||||||||
| Male group | 41 | 12 | 13 (7) | 0.85 | -- | 8 | 11 (7) | 0.50 | -- |
| Female group | 19 | 9 | 13 (8) | 10 | 12 (7) | ||||
| Specialty | |||||||||
| Medical branch | 41 | 14 | 15 (8) | 0.03 | 0.29 | 12 | 13 (7) | 0.009 | 0.34 |
| Surgical branch | 19 | 9 | 10 (4) | 7 | 8 (4) | ||||
| Salary | |||||||||
| Less than USD 2000 | 42 | 9.5 | 12 (6) | 0.03 | 0.27 | 7 | 10 (6) | 0.01 | 0.33 |
| USD 2000 or more | 18 | 16 | 17 (9) | 13.5 | 16 (8) | ||||
| Dedication to clinics | |||||||||
| Less than 20 weekly hours | 47 | 10 | 12 (7) | 0.02 | 0.31 | 7 | 11 (7) | 0.03 | 0.28 |
| 20 weekly hours or more | 13 | 19 | 19 (9) | 14 | 15 (7) | ||||
| Dedication to academics | |||||||||
| Less than 20 weekly hours | 53 | 10 | 12 (7) | 0.004 | 0.37 | 8 | 10 (6) | 0.002 | 0.40 |
| 20 weekly hours or more | 7 | 25 | 23 (10) | 24 | 21 (7) | ||||
| Dedication to management | |||||||||
| Less than 20 weekly hours | 52 | 10 | 13 (7) | 0.10 | -- | 8 | 11 (6) | 0.02 | 0.30 |
| 20 weekly hours or more | 8 | 17 | 18 (10) | 22.5 | 18 (9) | ||||
| Professional experience | |||||||||
| Less than 10 years | 43 | 10 | 14 (8) | 0.62 | 0.06 | 10 | 11 (6) | 0.92 | -- |
| 10 years or more | 17 | 10 | 13 (8) | 9 | 12 (8) | ||||
| Source of Variation | Somatization | |||
|---|---|---|---|---|
| F(1,58) | η2 | ηp2 | p | |
| Academic dedication (<20 weekly hours vs. >20) | 14.52 | 0.20 | 0.20 | <0.001 |
| Source of variation | Exhaustion | |||
| F(1,56) | η2 | ηp2 | p | |
| Specialty (surgery vs. medicine) | 5.58 | 0.06 | 0.09 | 0.02 |
| Academic dedication (<20 weekly hours vs. >20) | 13.28 | 0.15 | 0.19 | <0.001 |
| Management dedication (<20 weekly hours vs. >20) | 6.73 | 0.07 | 0.11 | 0.01 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Viruez-Soto, J.; Delgado Bolton, R.C.; San-Martín, M.; Vivanco, L. Inter-Professional Collaboration and Occupational Well-Being of Physicians Who Work in Adverse Working Conditions. Healthcare 2021, 9, 1210. https://doi.org/10.3390/healthcare9091210
Viruez-Soto J, Delgado Bolton RC, San-Martín M, Vivanco L. Inter-Professional Collaboration and Occupational Well-Being of Physicians Who Work in Adverse Working Conditions. Healthcare. 2021; 9(9):1210. https://doi.org/10.3390/healthcare9091210
Chicago/Turabian StyleViruez-Soto, José, Roberto C. Delgado Bolton, Montserrat San-Martín, and Luis Vivanco. 2021. "Inter-Professional Collaboration and Occupational Well-Being of Physicians Who Work in Adverse Working Conditions" Healthcare 9, no. 9: 1210. https://doi.org/10.3390/healthcare9091210
APA StyleViruez-Soto, J., Delgado Bolton, R. C., San-Martín, M., & Vivanco, L. (2021). Inter-Professional Collaboration and Occupational Well-Being of Physicians Who Work in Adverse Working Conditions. Healthcare, 9(9), 1210. https://doi.org/10.3390/healthcare9091210








