Abstract
Bright light therapy (BLT) has demonstrated positive short- and long-term effects in people with cognitive impairment or dementia; however, the immediate impact of BLT sessions has been scarcely investigated. In this study, we aimed to explore the immediate effects of BLT on behavior, mood, and physiological parameters (oxygen saturation/heart rate) in a sample of institutionalized older adults with moderate to very severe dementia, with a median age of 85.0 (interquartile range, IQR, 82.0–90.0), being higher in men (87.0 years, IQR 80.0–94.0) than in women (84.5 years, IQR 82.0–89.5). The BLT protocol consisted of 30-min morning sessions of 10,000 lux, Monday through Friday, for 4 weeks. The physiological parameters were recorded immediately before and after each session by pulse oximetry. Mood and behavior were assessed before, after, and during the sessions using the Interact scale. Post-session Interact scores showed a significant decrease in the items Tearful/sad and Talked spontaneously, and a significant increase in the items Enjoying self, active or alert, and Relaxed, content or sleeping appropriately. Interact scores during the sessions reflected a significant decrease in the speech-related items. Both physiological parameters changed positively from before to after sessions. Our results suggest that BLT provides immediate positive effects on mood, stimulation level, and physiological parameters, as well as a trend toward decreased speech. More robust research is needed to further explore the immediate impact of BLT. This study is registered with Clinicaltrials.gov (NCT04949984).
1. Introduction
Dementia is one of the main causes of disability and dependence among older adults worldwide, constituting a public health priority due to its significant human and financial costs to society [1]. Oxidative stress, mitochondrial damage, and synaptic damage are all implicated in dementia pathogenesis, playing an important role in the cognitive impairment and memory loss of older individuals with Alzheimer’s disease (AD) [2,3,4]. Neurotransmitters are essential to maintain synaptic and cognitive function, and are also involved in altering the mood, depression, or anxiety of AD patients [5,6]. Aside from cognitive decline, dementia progression leads to the appearance of at least one neuropsychiatric symptom (NPS) in most individuals at some point during the course of their disease [7,8]. NPS, also known as behavioral and psychological symptoms of dementia (BPSD) [9], are defined as a series of signs and symptoms of disturbed perception, thought content, mood, and behavior that frequently occur in dementia and constitute part of the expression of the disease [10]. These symptoms mainly comprise delusions, hallucinations, agitation, depression, anxiety, apathy, irritability, euphoria, disinhibition, aberrant motor behavior, sleep and nighttime behavior disturbances, and changes in appetite and eating behaviors [11,12].
Treatment development for BPSD includes both pharmacological and nonpharmacological therapies. In clinical settings, pharmacological agents are frequently used in the management of these symptoms but show modest efficacy and significant serious side-effects [13,14], including increased risks of hospitalization, falls, and mortality [15]. Numerous guidelines and expert recommendations favor nonpharmacological interventions for the treatment of BPSD due to their significant impact on global BPSD outcome measurements and the lack of adverse events [16]. In fact, the American Geriatrics Society Beers Criteria Update Expert Panel recommends the use of nonpharmacological approaches as the first course of action, unless they have previously failed, are not feasible, or there is a substantial risk of harm to self or others [17]. Therefore, nonpharmacological therapies should be considered to be the first choice of treatment. Nonpharmacological interventions include cognitive stimulation, reminiscence therapy, reality orientation, validation therapy, animal-assisted therapy, exercise or physical activity, Snoezelen/multisensory stimulation, aromatherapy, music therapy, and light therapy, among others [18,19]. It is necessary for further research to continue to strengthen the evidence of their effectiveness [16].
In this study, we focus on bright light therapy (BLT). This therapy consists of the controlled application of certain levels of light that can be administered in different ways, including outdoor sunlight, light boxes, light visors worn on the head, ceiling lights, or dawn-dusk simulation [20]. BLT is reported to have positive effects in the management of BPSD, sleep disturbances, and circadian rhythms (see recent reviews [21,22]). Although numerous studies address the short- and long-term effects of this therapy in people with cognitive impairment or dementia, there is little research on its immediate effects. Furthermore, other sensory therapies—such as multisensory stimulation in a Snoezelen room or music therapy—are shown to provide immediate positive effects on measures of behavior and mood disturbances, as well as on certain physiological parameters such as heart rate or blood oxygen saturation [23,24,25]. Thus, it could be expected that BLT, as a sensory therapy, would also lead to improvements in mood, behavior, and physiological parameters. Therefore, the main objective pursued in this study was to explore the immediate effects of bright light therapy on behavior, mood, and physiological parameters (oxygen saturation and heart rate) in a sample of institutionalized older people with moderate to very severe dementia.
2. Materials and Methods
2.1. Design
This study was designed as a randomized controlled trial. Participants were stratified according to their cognitive status and were subsequently randomly assigned to the experimental group (BLT) or control group. In the analysis and exploitation of results, we only considered the response of the BLT group with regard to the stated objective since the control group did not undergo the intervention needed to complete Interact assessment during the study.
2.2. Participants
Participants were recruited from among the residents of a gerontological complex specializing in dementia (78.7% with cognitive impairment) and located in A Coruña, Spain. The gerontological complex has 70 older people in a day care-setting and 64 institutionalized older people in a nursing home. We selected all institutionalized participants (n = 64, with a mean age of 88.4 ± 8.0 years and a median age of 89.0 (interquartile range, IQR, 84.0–94.0)); 29.7% were men, with a mean age of 88.5 ± 9.4 years and a median age of 91.0 (interquartile range, IQR, 84.5–94.0), and 70.3% were women, with a mean age of 88.4 ± 7.5 years and a median age of 88.0 (interquartile range, IQR, 84.0–94.0). To delimit the sample, before the recruitment process, inclusion and exclusion criteria were established according to the existing literature. As inclusion criteria, participants were required to satisfy the conditions of being 65 years or older, diagnosed with dementia, scoring ≥4 points on the global deterioration scale (GDS) [26], and having signed the informed consent (directly or through their legal guardians). Based on a recent systematic review on the ocular safety of light therapy [27], individuals with increased ocular sensitivity to light (photosensitivity) or those with preexisting ocular abnormalities were excluded from the study. Residents who had any severe eye disorder that did not allow them to open their eyes, or involved very low visual acuity, were also excluded since light needed to enter the participant’s eyes to achieve the desired effects [28].
2.3. Procedure
The research protocol (code 2017/408) received favorable authorization from the Galician Research Ethics Committee of Xunta de Galicia, Spain, and was developed in accordance with the Declaration of Helsinki. The participants and their legal guardians were informed about the study and signed the corresponding informed consent. All the information transmitted was adapted to the level of comprehension of the participants to facilitate their understanding and comfort throughout the study.
The study was retrospectively registered with ClinicalTrials.gov (NCT04949984) on 2 July 2021. The study protocol was based on the implementation guidelines that we described in a recent review [22]. The BLT sessions were carried out in a quiet room of the gerontological complex especially enabled for their proper implementation and were conducted by two research psychologists specialized in gerontology. The devices used for the intervention were bright white light lamps providing an intensity of 10,000 lux. Four users participated in each session, with two users per lamp, seated in a comfortable chair with armrests which was 70 cm from the lamp. The sessions were 30 min/day, between 10:30 a.m. and noon, 5 days a week (Monday to Friday), for 4 weeks (total 20 sessions). During the sessions, while exposed to light, participants watched documentaries on neutral topics. Each session lasted 30 min, unless the participant expressed the desire to leave the room and could not be convinced to remain without generating agitation. Participants who responded negatively to light exposure were immediately withdrawn from the intervention. Only those sessions in which the participant remained for at least 80% of the expected time (≥22.5 min) were considered as sessions performed.
In every session, the researchers supervised the participants to ensure full compliance with the treatment and evaluated the physiological parameters, mood, and behavior of the participants. Once in the room, the investigators measured the heart rate (beats per minute) and blood oxygen saturation (SpO2) of each participant using a mobile finger pulse oximeter before and after the session.
Mood and behavior were assessed during the sessions and in the 10 min periods immediately before and after each session using the Interact scale [29] and its shortened version, named Interact short. The Interact scale, hereinafter referred to as Interact during, is made up of 22 Likert-scale items that score the frequency of occurrence (ranging from 1 (Not at all) to 5 (Nearly all the time)) of each type of mood and behavior during the sessions. Additionally, as qualitative information, any comments made by the participants about their session were recorded, as well as the sensation that the researchers believe the participants experienced during the session (relaxing, stimulating, leisure, improving communication, arousing curiosity, or unpleasant). The Interact short includes 12 Likert-scale items, with the same range as in the Interact during, recording the occurrence of each type of mood and behavior of the participants in the 10 min periods immediately preceding and following the session to measure any observable change.
2.4. Statistical Analysis
All data were analyzed using the SPSS statistical software package (version 26.0) (IBM, Armonk, NY, USA) and statistical significance was set at p < 0.05. The normal distribution of the variables was tested using the Shapiro–Wilk test. For subsequent analyses, we applied parametric or nonparametric tests depending on whether the assumption of normality was met or not for each measured variable. The Wilcoxon signed-rank test or paired t-test were employed to measure significant changes between the Interact short scores before and after the intervention sessions for each of the assessed mood and behavior items. Likewise, these same tests were used to analyze the evolution of the Interact during scores by comparing the average scores of the first week with those of the fourth week. In addition, the evolution of mood and behavior scores throughout the four weeks of treatment was analyzed with the Friedman test for related samples. The paired t-test was also used to determine the existence of any differences between before and after the sessions in the physiological parameters investigated. In the variables in which statistically significant differences were found, Cohen’s d or r values were used to report the effect size (ES) of these changes. The interpretation of the importance of the ES was made according to the benchmarks defined by Cohen [30] as follows: small ES (d = 0.2 or r = 0.1), medium ES (d = 0.5 or r = 0.3), and large ES (d = 0.8 or r = 0.5).
3. Results
3.1. Sample Characteristics
After applying inclusion and exclusion criteria, the total sample was reduced from 64 to 39 institutionalized older people (20 participants assigned to the control group and 19 to the BLT group). Table 1 shows their sociodemographic characteristics and their level of cognitive decline based on the scores obtained in the GDS. The categorical variables (gender, marital status, educational level, level of cognitive impairment) are expressed in terms of frequency and percentage, and age, as a continuous variable, is presented as the mean plus standard deviation (SD), along with the range of minimum and maximum values. The mean age of the participants was 86.3 ± 6 years, ranging from 75 to 98, with a median age of 85.0 (interquartile range, IQR, 82.0–90.0), being higher in men (87.0 years, IQR 80.0–94.0) than in women (84.5 years, IQR 82.0–89.5). The group was composed mostly of women (73.7%), and most participants were widowed (68.4%). Concerning educational level, few of the participants had higher education since most of them had received formal education for eight or fewer years (73.7%). Regarding the cognitive impairment measured by GDS, 31.6% of the sample presented moderate decline, 26.3% presented moderate to severe decline, another 26.3% presented severe decline, and finally, 15.8% of the participants presented very severe decline.

Table 1.
Sociodemographic characteristics of the study population.
3.2. Mood and Behavior
Significant effects were detected between before and after the intervention sessions in 4 of the 12 items evaluated in the Interact short (see Table 2). The results of the Wilcoxon signed-rank test showed a significant reduction in the prevalence of the Tearful/sad item (p = 0.044) with a medium effect size (r = −0.32). The results of the paired t-test showed significant changes in the score of the Talked spontaneously item (p = 0.035) with a medium effect size (d = 0.52). Moreover, two items of the Stimulation level construct showed a significant increase in scores: Enjoying self, active or alert (p = 0.034) and Relaxed, content or sleeping appropriately (p = 0.001), with medium (d = −0.52) and large (d = −0.94) effect sizes, respectively.

Table 2.
Means (SDs) of Interact short scores before and after light therapy sessions.
To analyze the significance of the changes in the evolution of behavioral and psychological symptoms during the sessions, a comparison was made between the mean/median scores of the Interact during items of the four weeks of intervention. As can be seen in Table 3, scores reflected a significant decrease in the speech-related items, with large effect sizes. Scores were significantly lower for the Comments or questions about activities/objects item of the Relating to the environment construct. The results did not differ when analyzing the evolution of the four weeks versus the evolution between only the first and last week, with the same variables being significant in both comparisons.

Table 3.
Means (SDs) of Interact during session scores for each week.
Regarding the type of experience felt by the participants during the sessions, the evaluators recorded most of the sessions as leisure (32.98%), followed by relaxing (34.23%), stimulating (23.35), arousing curiosity (16.18%), and improving communication (6.43%). The researchers only perceived 6.32% of the sessions as unpleasant for the participants.
3.3. Physiological Parameters
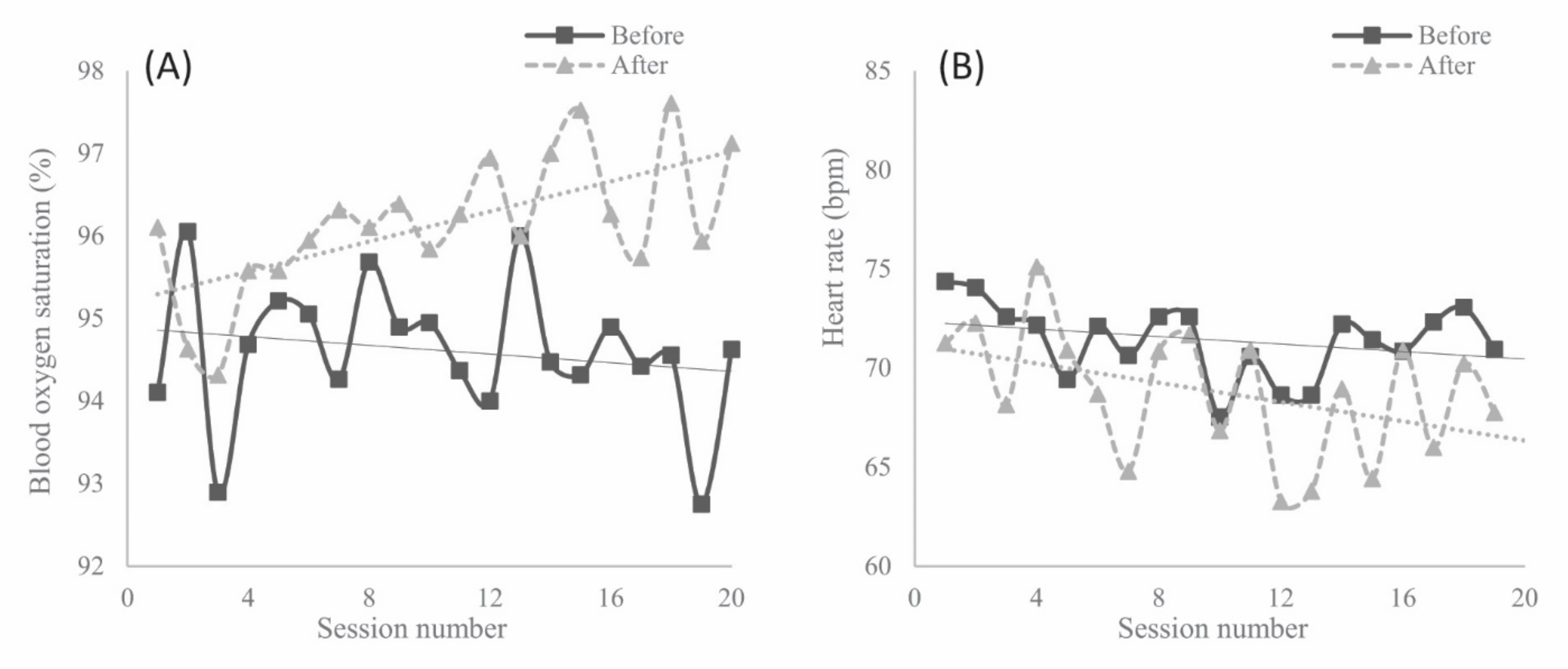
There were significant changes between before and after the sessions in both physiological parameters (see Figure 1). Participants demonstrated an increase in mean SpO2 values (p < 0.001, Figure 1A) and a decrease in mean heart rate (p < 0.001, Figure 1B) at the end of the sessions, with a large effect size of both changes measured (d = −1.33 and d = 1.10, respectively).
Figure 1.
Records of biomedical parameters before and after light therapy intervention from session 0 (baseline) to 20 (post-trial): (A) blood hemoglobin oxygen saturation (%); (B) heart rate—beats per minute (bpm).
4. Discussion
The purpose of this study was to examine the immediate effects of a four-week BLT intervention program on the behavior, mood, oxygen saturation, and heart rate of institutionalized older patients with moderate to very severe dementia. The main results revealed promising evidence of the benefits of BLT on specific aspects of mood and behavior in participants both during and after the sessions, as well as positive effects on the physiological parameters analyzed.
As previously stated, mood and behavior were assessed using the Interact scale [29]. Although this scale was initially developed for the assessment of mood and behavior of patients with dementia during multisensory stimulation sessions in a Snoezelen room, its use has been extended to other nonpharmacological interventions such as music [24], art [31], and reminiscence therapies [32,33]. On this basis, the Interact scale was chosen for this study since its structure and form of application are also appropriate and compatible with the procedure of light therapy sessions.
The Interact short scores obtained by the participants before and after BLT sessions revealed, on the one hand, a significant decrease in the items of Tearful/sad and Talked spontaneously, and, on the other hand, a significant change in their stimulation level—specifically in the items Enjoying self, active or alert, and Relaxed, content or sleeping appropriately. Therefore, participants were less sad and less spontaneously talkative immediately after BLT sessions, which in turn could be related to the fact that they were also more relaxed, content, or sleeping appropriately. Concurring with some of these findings, other authors [34] investigating the immediate effects of BLT versus dim red light sessions found an immediate decrease in sleepiness and a tendency for mood improvement upon exposure to bright light. Other studies using 30-min BLT sessions found short-term positive effects on mood and agitation in people with dementia [35,36,37], with greater benefits observed in patients with severe dementia than in those with mild/moderate dementia [36].
The Interact during showed a significant decrease in the score of the Making comments or asking questions about the activity item, which makes sense due to the habituation of the participants to the intervention program as it progressed. Scores on the Interact during also reflected that as the weeks of intervention progressed, the participants talked less clearly, sensibly, and spontaneously and with shorter sentences, i.e., an overall decrease in speech during the sessions. These results may also be linked to the lower post-session scores on the Talked spontaneously item of the Interact short. None of the existing studies on BLT in the literature address the immediate effects that occur within sessions, so we cannot discuss our results from the perspective of previous studies.
Regarding physiological parameters, the measurements showed positive changes between before and after the sessions in the two analyzed parameters, with a significant increase in mean SpO2 and a significant reduction in mean heart rate. These changes may be related to the fact that participants were more relaxed, as shown by the Interact scores, since these biological responses are considered physiological indicators of a relaxation response [38,39]. Consistent with our findings, Choi et al. [40], who studied the immediate influence of different dim-colored lights—white, red, and blue—in healthy adults, also found a decrease in heart rate after exposure to the illumination. In the existing literature, another physiological parameter that has been studied with respect to light therapy is heart rate variability (HRV). A group of authors [41,42] found immediate positive effects of evening BLT on HRV in a sample of healthy young women. Similar findings were reported by Rechlin et al. [43] in patients diagnosed with major depression. Our results differ from another previous study in which no immediate effects of morning BLT on any of the physiological parameters analyzed were found [34]. Following the initial hypothesis of this study, our findings on the effects of BLT on the physiological parameters analyzed coincide with the positive effects of other sensory interventions reported in the existing literature, such as music therapy [24,25,44,45] and multisensory stimulation [23,24].
To the best of our knowledge, the immediate impact of BLT sessions on mood and behavior has been virtually unexamined previously, so the present study provides novel and relevant data for clinical practice. However, the results of this work should be regarded as preliminary and interpreted with caution due to certain existing limitations. This study is one part of a larger and more comprehensive BLT investigation. The current study only analyzed the immediate effects during and after BLT sessions, and the long-term effects should be further established. Therefore, these limitations stem mainly from the small sample size and the use of a single-arm intervention with no control group, both of which limit the generalizability of the results found. Additionally, mood and behavior were measured based on the observations of unblinded researchers, which may have resulted in researcher bias. Future research should address these limitations by employing a double-blind design in controlled studies with larger sample sizes. Another physiological parameter (determination of blood pressure at least three times during the sessions) could also be used to further assess the impact of bright light therapy.
5. Conclusions
The results of the present study suggest that a bright light therapy intervention program of 30-min sessions provides promising outcomes and immediate positive effects on mood, stimulation level, blood oxygen saturation, and heart rate. On the other hand, there was a tendency for a decrease in speech both during and after the intervention sessions. Further research is needed to strengthen these findings and to explore in depth the possible immediate effects of BLT.
Author Contributions
Conceptualization: N.C., A.M., and J.C.M.-C.; Methodology: N.C., A.M., and J.C.M.-C.; Formal analysis: N.C., L.L.-L., and A.M.; Investigation: N.C., I.G.-A., R.L.-L., and J.L.R.-V.; Resources: J.C.M.-C., N.C., and J.L.R.-V.; Data curation: N.C.; Writing—original draft preparation: N.C. and A.M.; Writing—review and editing: all authors; Visualization: N.C. and A.M.; Supervision: A.M. and J.C.M.-C.; Project administration: A.M. and J.C.M.-C.; Funding acquisition: J.C.M.-C. and L.L.-L. All authors have read and agreed to the final version of the manuscript.
Funding
This research was funded by the Xunta de Galicia (grant numbers ED431C 2017/49, ED431F 2017/09, FrailNet network IN607C 2016/08, and REGIDEM network IN607C 2017/02); and the Spanish Ministry of Economy and Competitiveness, co-financed by the European Social Fund (grant number RYC-2015-18394).
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Galician Research Ethics Committee of Xunta de Galicia, Spain (protocol code 2017/408, approved on 25 October 2017).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgments
We would like to express our sincere gratitude to the residents and staff of the gerontological complex La Milagrosa (A Coruña, Spain) who were essential in making this study possible.
Conflicts of Interest
The authors declare no conflict of interest.
References
- World Health Organization. Global Action Plan on the Public Health Response to Dementia 2017–2025; WHO Document Production Services: Geneva, Switzerland, 2017; ISBN 978-92-4-151348-7. [Google Scholar]
- Pradeppkiran, J.A.; Reddy, P.H. Defective mitophagy in Alzheimer’s disease. Ageing Res. Rev. 2020, 64, 101191. [Google Scholar] [CrossRef]
- Reddy, P.H.; Beal, M.F. Amyloid beta, mitochondrial dysfunction and synaptic damage: Implications for cognitive decline in aging and Alzheimer’s disease. Trends Mol. Med. 2008, 14, 45–53. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reddy, P.H.; Tonk, S.; Kumar, S.; Vijayan, M.; Kandimalla, R.; Kuruva, C.S.; Reddy, A.P. A Critical Evaluation of Neuroprotective and Neurodegenerative MicroRNAs in Alzheimer’s Disease. Biochem. Biophys. Res. Commun. 2017, 483, 1156–1165. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bethea, C.L.; Reddy, A.P.; Christian, F.L. How studies of the serotonin system in macaque models of menopause relate to Alzheimer’s disease. J. Alzheimer’s Dis. 2017, 57, 1001–1015. [Google Scholar] [CrossRef] [Green Version]
- Reddy, C.L. A Critical Assessment of Research on Neurotransmitters in Alzheimer’s Disease. J. Alzheimer’s Dis. 2017, 57, 969–974. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lyketsos, C.G.; Steinberg, M.; Tschanz, J.T.; Norton, M.C.; Steffens, D.C.; Breitner, J.C.S. Mental and behavioral disturbances in dementia: Findings from the Cache County study on memory in aging. Am. J. Psychiatry 2000, 157, 708–714. [Google Scholar] [CrossRef]
- Steinberg, M.; Shao, H.; Lyketsos, C.G.; Welsh-Bohmer, K.A.; Norton, M.C.; Breitner, J.C.S.; Steffens, D.C.; Tschanz, J.T.; Cache Country Investigators. Point and 5-year period prevalence of neuropsychiatric symptoms in dementia: The Cache County Study. Int. J. Geriatr. Psychiatry 2008, 23, 170–177. [Google Scholar] [CrossRef] [Green Version]
- Aalten, P.; Verhey, F.R.J.; Boziki, M.; Bullock, R.; Byrne, E.J.; Camus, V.; Caputo, M.; Collins, D.; De Deyn, P.P.; Elina, K.; et al. Neuropsychiatric Syndromes in Dementia Results from the European Alzheimer Disease Consortium: Part I. Dement. Geriatr. Cogn. Disord. 2007, 24, 457–463. [Google Scholar] [CrossRef] [PubMed]
- Finkel, S.I.; Costa e Silva, J.; Cohen, G.; Miller, S.; Sartorius, N. Behavioral and psychological signs and symptoms of dementia: A consensus statement on current knowledge and implications for research and treatment. Int. Psychogeriatr. 1996, 8, 497–500. [Google Scholar] [CrossRef] [PubMed]
- Cummings, J.L.; Mega, M.; Gray, K.; Rosenberg-Thompson, S.; Carusi, D.A.; Gornbein, J. The Neuropsychiatric Inventory: Comprehensive assessment of psychopathology in dementia. Neurology 1994, 44, 2308–2314. [Google Scholar] [CrossRef] [Green Version]
- Cummings, J.L. The Neuropsychiatric Inventory: Assessing psychopathology in dementia patients. Neurology 1997, 48, 10S–16S. [Google Scholar] [CrossRef] [Green Version]
- Kales, H.C.; Gitlin, L.N.; Lyketsos, C.G. Management of neuropsychiatric symptoms of dementia in clinical settings: Recommendations from a multidisciplinary expert panel. J. Am. Geriatr. Soc. 2014, 62, 762–769. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sink, K.M.; Holden, K.F.; Yaffe, K. Pharmacological treatment of neuropsychiatric symptoms of dementia. JAMA 2005, 293, 596–608. [Google Scholar] [CrossRef] [PubMed]
- Chiu, Y.; Bero, L.; Hessol, N.A.; Lexchin, J.; Harrington, C. A literature review of clinical outcomes associated with antipsychotic medication use in North American nursing home residents. Health Policy 2015, 119, 802–813. [Google Scholar] [CrossRef] [PubMed]
- Dyer, S.M.; Harrison, S.L.; Laver, K.; Whitehead, C.; Crotty, M. An overview of systematic reviews of pharmacological and non-pharmacological interventions for the treatment of behavioral and psychological symptoms of dementia. Int. Psychogeriatr. 2018, 30, 295–309. [Google Scholar] [CrossRef]
- American Geriatrics Society Beers Criteria Update Expert Panel. American Geriatrics Society 2019 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults. J. Am. Geriatr. Soc. 2019, 67, 674–694. [Google Scholar] [CrossRef]
- Abraha, I.; Rimland, J.M.; Trotta, F.M.; Dell’Aquila, G.; Cruz-Jentoft, A.; Petrovic, M.; Gudmundsson, A.; Soiza, R.; O’Mahony, D.; Guaita, A.; et al. Systematic review of systematic reviews of non-pharmacological interventions to treat behavioural disturbances in older patients with dementia. The SENATOR-OnTop series. BMJ Open 2017, 7, e012759. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Takeda, M.; Tanaka, T.; Okochi, M.; Kazui, H. Non-pharmacological intervention for dementia patients. Psychiatry Clin. Neurosci. 2012, 66, 1–7. [Google Scholar] [CrossRef]
- Forbes, D.; Blake, C.M.; Thiessen, E.J.; Peacock, S.; Hawranik, P. Light therapy for improving cognition, activities of daily living, sleep, challenging behaviour, and psychiatric disturbances in dementia. Cochrane Database Syst. Rev. 2014, 2, CD003946. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hjetland, G.J.; Pallesen, S.; Thun, E.; Kolberg, E.; Nordhus, I.H.; Flo, E. Light interventions and sleep, circadian, behavioral, and psychological disturbances in dementia: A systematic review of methods and outcomes. Sleep Med. Rev. 2020, 52, 101310. [Google Scholar] [CrossRef]
- Cibeira, N.; Maseda, A.; Lorenzo-López, L.; Rodríguez-Villamil, J.L.; López-López, R.; Millán-Calenti, J.C. Application of light therapy in older adults with cognitive impairment: A systematic review. Geriatr. Nurs. 2020, 41, 970–983. [Google Scholar] [CrossRef]
- Maseda, A.; Sánchez, A.; Marante, M.P.; González-Abraldes, I.; De Labra, C.; Millán-Calenti, J.C. Multisensory stimulation on mood, behavior, and biomedical parameters in people with dementia: Is it more effective than conventional one-to-one stimulation? Am. J. Alzheimer’s Dis. Other Demen. 2014, 29, 637–647. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maseda, A.; Cibeira, N.; Lorenzo-López, L.; González-Abraldes, I.; Buján, A.; de Labra, C.; Millán-Calenti, J.C. Multisensory stimulation and individualized music sessions on older adults with severe dementia: Effects on mood, behavior, and biomedical parameters. J. Alzheimer’s Dis. 2018, 63, 1415–1425. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Raglio, A.; Oasi, O.; Gianotti, M.; Manzoni, V.; Bolis, S.; Ubezio, M.C.; Gentile, S.; Villani, D.; Stramba-Badiale, M. Effects of music therapy on psychological symptoms and heart rate variability in patients with dementia. A pilot study. Curr. Aging Sci. 2010, 3, 242–246. [Google Scholar] [CrossRef] [PubMed]
- Reisberg, B.; Ferris, S.H.; de León, M.J.; Crook, T. The Global Deterioration Scale for assessment of primary degenerative dementia. Am. J. Psychiatry 1982, 139, 1136–1139. [Google Scholar] [CrossRef] [Green Version]
- Brouwer, A.; Nguyen, H.T.; Snoek, F.J.; van Raalte, D.H.; Beekman, A.T.F.; Moll, A.C.; Bremmer, M.A. Light therapy: Is it safe for the eyes? Acta Psychiatr. Scand. 2017, 136, 534–548. [Google Scholar] [CrossRef] [PubMed]
- Skene, D.J.; Lockley, S.W.; Thapan, K.; Arendt, J. Effects of light on human circadian rhythms. Reprod. Nutr. Dev. 1999, 39, 295–304. [Google Scholar] [CrossRef] [PubMed]
- Baker, R.; Dowling, Z. INTERACT; Research and Development Support Unit, Poole Hospital: Dorset, UK, 1995. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: New York, NY, USA, 1988. [Google Scholar]
- Hendriks, I.; Meiland, F.J.M.; Slotwinska, K.; Kroeze, R.; Weinstein, H.; Gerritsen, D.L.; Dröes, R.M. How do people with dementia respond to different types of art? An explorative study into interactive museum programs. Int. Psychogeriatr. 2019, 31, 857–868. [Google Scholar] [CrossRef]
- Baillon, S.; van Diepen, E.; Prettyman, R.; Redman, J.; Rooke, N.; Campbell, R. A comparison of the effects of Snoezelen and reminiscence therapy on the agitated behaviour of patients with dementia. Int. J. Geriatr. Psychiatry 2004, 19, 1047–1052. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baillon, S.; van Diepen, E.; Prettyman, R.; Rooke, N.; Redman, J.; Campbell, R. Variability in response to older people with dementia to both Snoezelen and reminiscence. Br. J. Occup. Ther. 2005, 68, 367–374. [Google Scholar] [CrossRef] [Green Version]
- Ivanova, I.A.; Danilenko, K.V.; Aftanas, L.I. Investigation of an immediate effect of bright light on oxygen consumption, heart rate, cortisol, and α-amylase in seasonal affective disorder subjects and healthy controls. Neuropsychobiology 2016, 74, 219–225. [Google Scholar] [CrossRef]
- Onega, L.L.; Pierce, T.W.; Epperly, L. Effect of bright light exposure on depression and agitation in older adults with dementia. Issues Ment. Health Nurs. 2016, 37, 660–667. [Google Scholar] [CrossRef]
- Onega, L.L.; Pierce, T.W.; Epperly, L. Bright light therapy to treat depression in individuals with mild/moderate or severe dementia. Issues Ment. Health Nurs. 2018, 39, 370–373. [Google Scholar] [CrossRef]
- Haffmans, P.M.J.; Sival, R.C.; Lucius, S.A.P.; Cats, Q.; van Gelder, L. Bright light therapy and melatonin in motor restless behaviour in dementia: A placebo-controlled study. Int. J. Geriatr. Psychiatry 2001, 16, 106–110. [Google Scholar] [CrossRef]
- Benson, H.; Beary, J.F.; Carol, M.P. The relaxation response. Psychiatry 1974, 37, 37–46. [Google Scholar] [CrossRef]
- Han, L.; Li, J.P.; Sit, J.W.H.; Chung, L.; Jiao, Z.Y.; Ma, W.G. Effects of music intervention on physiological stress response and anxiety level of mechanically ventilated patients in China: A randomised controlled trial. J. Clin. Nurs. 2010, 19, 978–987. [Google Scholar] [CrossRef] [PubMed]
- Choi, C.J.; Kim, K.S.; Kim, C.M.; Kim, S.H.; Choi, W.S. Reactivity of heart rate variability after exposure to colored lights in healthy adults with symptoms of anxiety and depression. Int. J. Psychophysiol. 2011, 79, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Kohsaka, M.; Kohsaka, S.; Fukuda, N.; Honma, H.; Sakakibara, S.; Kawai, I.; Miyamoto, T.; Kobayashi, R. Effects of bright light exposure on heart rate variability during sleep in young women. Psychiatry Clin. Neurosci. 2001, 55, 283–284. [Google Scholar] [CrossRef] [PubMed]
- Sakakibara, S.; Honma, H.; Kohsaka, M.; Fukuda, N.; Kawai, I.; Kobayashi, R.; Koyama, T. Autonomic nervous function after evening bright light therapy: Spectral analysis of heart rate variability. Psychiatry Clin. Neurosci. 2000, 54, 363–364. [Google Scholar] [CrossRef]
- Rechlin, T.; Weis, M.; Schneider, K.; Zimmermann, U.; Kaschka, W.P. Does bright-light therapy influence autonomic heart-rate parameters? J. Affect. Disord. 1995, 35, 131–137. [Google Scholar] [CrossRef]
- Chlan, L.L. Psychophysiologic responses of mechanically ventilated patients to music: A pilot study. Am. J. Crit. Care 1995, 4, 233–238. [Google Scholar] [CrossRef] [PubMed]
- Gök Ugur, H.; Aktaş, Y.Y.; Orak, O.S.; Saglambilen, O.; Avci, İ.A. The effect of music therapy on depression and physiological parameters in elderly people living in a Turkish nursing home: A randomized-controlled trial. Aging Ment. Health 2017, 21, 1280–1286. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).