Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients and Healthy Controls
2.2. Sitting Test
2.3. Cerebral Blood Flow Determination by Extracranial Doppler Echography
2.4. Statistical Analysis
3. Results
Patient Clinical and Echo Doppler Data
4. Discussion
4.1. Clinical Implications
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
References
- Institute of Medicine (IOM) (Ed.) Beyond Mayalgic Cncephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness; The National Academies Press: Washington, DC, USA, 2015. [Google Scholar]
- van Campen, C.M.C.; Verheugt, F.W.A.; Rowe, P.C.; Visser, F.C. Cerebral blood flow is reduced in ME/CFS during head-up tilt testing even in the absence of hypotension or tachycardia: A quantitative, controlled study using Doppler echography. Clin. Neurophysiol. Pract. 2020, 5, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Miwa, K.; Inoue, Y. The etiologic relation between disequilibrium and orthostatic intolerance in patients with myalgic encephalomyelitis (chronic fatigue syndrome). J. Cardiol. 2018, 72, 261–264. [Google Scholar] [CrossRef] [PubMed]
- Carruthers, B.M.; van de Sande, M.I.; De Meirleir, K.L.; Klimas, N.G.; Broderick, G.; Mitchell, T.; Staines, D.; Powles, A.C.P.; Speight, N.; Vallings, R.; et al. Myalgic encephalomyelitis: International Consensus Criteria. J. Intern. Med. 2011, 270, 327–338. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, K.; Straus, S.E.; Hickie, I.; Sharpe, M.C.; Dobbins, J.G.; Komaroff, A. The chronic Fatigue syndrome: A comprehensive approach to its definition and study. Ann. Intern. Med. 1994, 121, 953–959. [Google Scholar] [CrossRef] [PubMed]
- van Campen, C.M.C.; Verheugt, F.W.A.; Visser, F.C. Cerebral blood flow changes during tilt table testing in healthy volunteers, as assessed by Doppler imaging of the carotid and vertebral arteries. Clin. Neurophysiol. Pract. 2018, 3, 91–95. [Google Scholar] [CrossRef] [PubMed]
- van Campen, C.M.C.; Rowe, P.C.; Visser, F.C. Cerebral Blood Flow Is Reduced in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients During Mild Orthostatic Stress Testing: An Exploratory Study at 20 Degrees of Head-Up Tilt Testing. Healthcare 2020, 8, 169. [Google Scholar] [CrossRef] [PubMed]
- van Campen, C.M.C.; Rowe, P.C.; Visser, F.C. Blood Volume Status in ME/CFS Correlates With the Presence or Absence of Orthostatic Symptoms: Preliminary Results. Front. Pediatr. 2018, 6, 4. [Google Scholar] [CrossRef] [PubMed]
- Streeten, D.H.P.; Bell, D.S. Circulating Blood Volume in Chronic Fatigue Syndrome. J. Chronic Fatigue Syndr. 1998, 4, 3–11. [Google Scholar] [CrossRef]
- Lin, Y.; Liu, H.L.; Fang, J.; Yu, C.H.; Xiong, Y.K.; Yuan, K. Anti-fatigue and vasoprotective effects of quercetin-3-O-gentiobiose on oxidative stress and vascular endothelial dysfunction induced by endurance swimming in rats. Food Chem. Toxicol. 2014, 68, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Hurwitz, B.E.; Coryell, V.T.; Parker, M.; Martín, P.; Laperriere, A.; Klimas, N.G.; Sfakianakis, G.N.; Bilsker, M.S. Chronic fatigue syndrome: Illness severity, sedentary lifestyle, blood volume and evidence of diminished cardiac function. Clin. Sci. 2010, 118, 125–135. [Google Scholar] [CrossRef] [PubMed]
- van Campen, C.M.C.; Visser, F.C. The abnormal Cardiac Index and Stroke Volume Index changes during a normal Tilt Table Test in ME/CFS patients compared to healthy volunteers, are not related to deconditioning. J. Thromb. Circ. 2018, 2018, 1–8. [Google Scholar]
- Carter, S.E.; Draijer, R.; Holder, S.M.; Brown, L.; Thijssen, D.H.J.; Hopkins, N.D. Regular walking breaks prevent the decline in cerebral blood flow associated with prolonged sitting. J. Appl. Physiol. 2018, 125, 790–798. [Google Scholar] [CrossRef] [PubMed]
- Wheeler, M.J.; Dunstan, D.W.; Smith, B.; Smith, K.J.; Scheer, A.; Lewis, J.; Naylor, L.H.; Heinonen, I.; Ellis, K.A.; Cerin, E.; et al. Morning exercise mitigates the impact of prolonged sitting on cerebral blood flow in older adults. J. Appl. Physiol. 2019, 126, 1049–1055. [Google Scholar] [CrossRef] [PubMed]
- Perdomo, S.J.; Gibbs, B.B.; Kowalsky, R.J.; Taormina, J.M.; Balzer, J.R. Effects of Alternating Standing and Sitting Compared to Prolonged Sitting on Cerebrovascular Hemodynamics. Sport Sci. Health 2019, 15, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Ocon, A.J.; Medow, M.S.; Taneja, I.; Clarke, D.; Stewart, J.M. Decreased upright cerebral blood flow and cerebral autoregulation in normocapnic postural tachycardia syndrome. Am. J. Physiol. Heart Circ. Physiol. 2009, 297, H664–H673. [Google Scholar] [CrossRef] [PubMed]
- Stewart, J.M.; Medow, M.S.; Messer, Z.R.; Baugham, I.L.; Terilli, C.; Ocon, A.J. Postural neurocognitive and neuronal activated cerebral blood flow deficits in young chronic fatigue syndrome patients with postural tachycardia syndrome. Am. J. Physiol. -Heart Circ. Physiol. 2012, 302, H1185–H1194. [Google Scholar] [CrossRef] [PubMed]
- Lewis, I.; Pairman, J.; Spickett, G.; Newton, J.L. Clinical characteristics of a novel subgroup of chronic fatigue syndrome patients with postural orthostatic tachycardia syndrome. J. Intern. Med. 2013, 273, 501–510. [Google Scholar] [CrossRef] [PubMed]
- Reynolds, G.K.; Lewis, D.P.; Richardson, A.M.; Lidbury, B.A. Comorbidity of postural orthostatic tachycardia syndrome and chronic fatigue syndrome in an Australian cohort. J. Intern. Med. 2014, 275, 409–417. [Google Scholar] [CrossRef] [PubMed]
- Sato, K.; Ogoh, S.; Hirasawa, A.; Oue, A.; Sadamoto, T. The distribution of blood flow in the carotid and vertebral arteries during dynamic exercise in humans. J. Physiol. 2011, 589 (Pt 11), 2847–2856. [Google Scholar] [CrossRef]
| A minimum of 1 h sitting was required (including travel, time spent in the waiting room, and history taking) |
| Transfer to the research table and start sitting test |
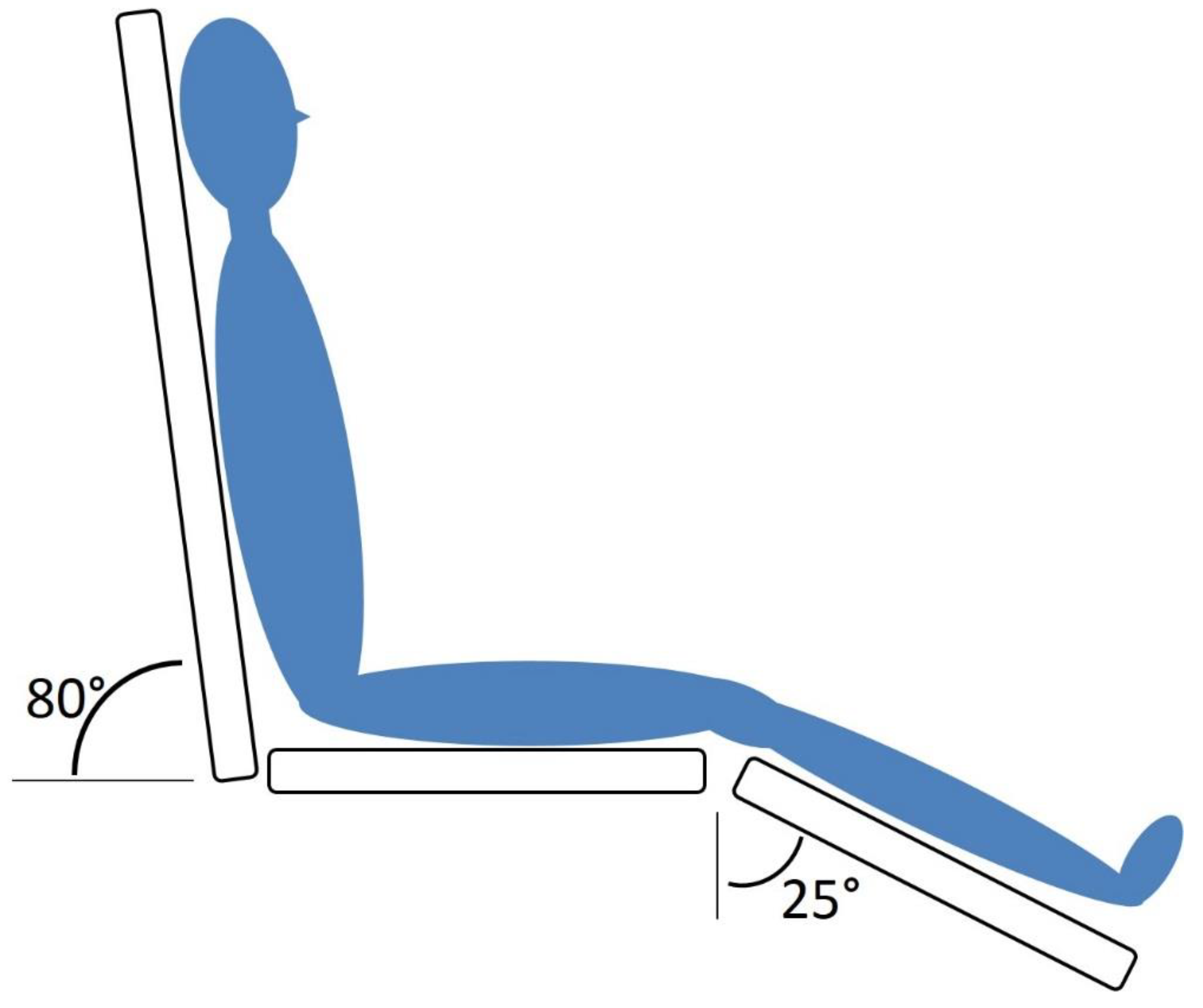
| Measurement of heart rate and blood pressure in sitting position as shown in Figure 1 |
| Cerebral blood flow measurements in sitting position |
| Lying down for 10–15 min |
| Measurement of heart rate and blood pressuring in supine position |
| Cerebral blood flow measurements in supine position |
| End of the sitting test |
| HC (n = 15) | Severe ME/CFS (n = 100) | p-Value | |
|---|---|---|---|
| Male/female | 2/13 | 12/88 | 0.88 |
| Age (years) | 38 (15) | 38 (12) | 0.94 |
| Height (cm) | 172 (9) | 174 (8) | 0.44 |
| Weight (kg) | 68 (15) | 73 (16) | 0.27 |
| BMI (kg/m2) | 22.9 (3.4) | 24.3 (5.5) | 0.33 |
| Heart rate supine (bpm) | 70 (14) | 75 (15) | 0.34 |
| Heart rate sitting (bpm) | 75 (10) | 87 (19) | 0.08 |
| Systolic blood pressure supine (mmHg) | 119 (14) | 124 (17) | 0.40 |
| Systolic blood pressure sitting (mmHg) | 122 (18) | 134 (18) | 0.05 |
| Diastolic blood pressure supine (mmHg) | 75 (12) | 80 (11) | 0.20 |
| Diastolic blood pressure sitting (mmHg) | 83 (10) | 88 (11) | 0.22 |
| Cerebral blood flow supine (mL/min) | 630 (85) | 631 (121) | 0.96 |
| Cerebral blood flow sitting (mL/min) | 627 (89) | 474 (96) | <0.0001 |
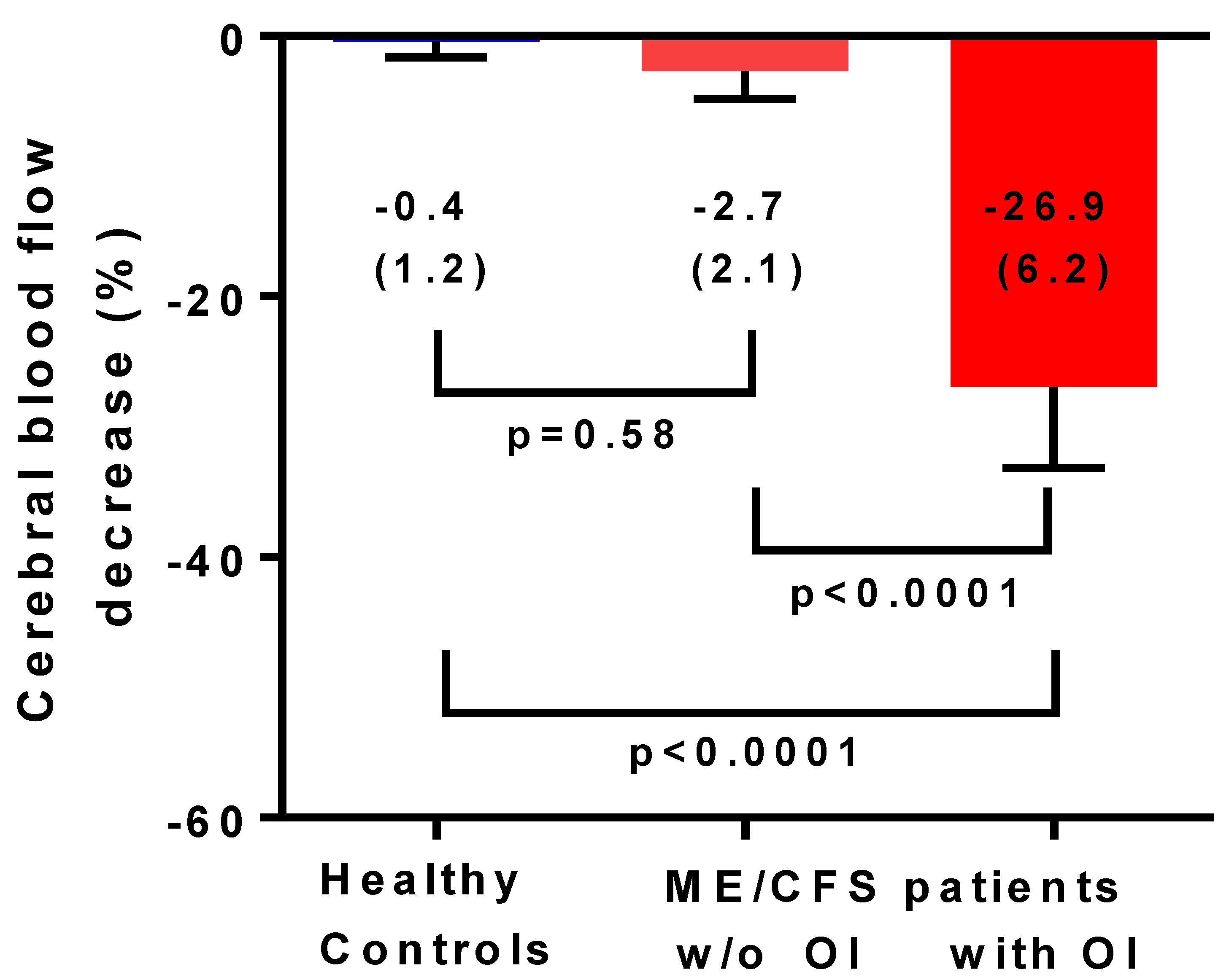
| Cerebral blood flow % change sitting vs. supine | −0.4 (1.2) | −24.5 (9.4) | <0.0001 |
| FM Plus (n = 37) | FM Minus (n = 63) | p-Value | |
|---|---|---|---|
| Male/female | 2/35 | 10/53 | 0.12 |
| Age (years) | 43 (13) | 36 (11) | <0.01 |
| Disease duration (years) # | 15 (8.5–23.5) | 13 (8–19) | 0.46 |
| Height (cm) | 172 (7) | 174 (8) | 0.15 |
| Weight (kg) | 78 (17) | 70 (15) | 0.02 |
| BMI (kg/m2) | 26.3 (5.5) | 23.1 (5.2) | <0.01 |
| Heart rate supine (bpm) | 71 (10) | 78 (17) | 0.02 |
| Heart rate sitting (bpm) | 81 (12) | 91 (21) | 0.02 |
| Systolic blood pressure supine (mmHg) | 125 (19) | 124 (16) | 0.95 |
| Systolic blood pressure sitting (mmHg) | 138 (20) | 132 (16) | 0.15 |
| Diastolic blood pressure supine (mmHg) | 82 (11) | 79 (11) | 0.24 |
| Diastolic blood pressure sitting (mmHg) | 90 (12) | 86 (10) | 0.09 |
| Cerebral blood flow supine (mL/min) | 639 (131) | 627 (116) | 0.62 |
| Cerebral blood flow sitting (mL/min) | 481 (88) | 470 (101) | 0.56 |
| Cerebral blood flow % change sitting vs. supine | −23.9 (9.4) | −24.9 (9.5) | 0.60 |
| With POTS (n = 34) | Without POTS (n = 66) | p-Value | |
|---|---|---|---|
| Male/female | 2/32 | 10/56 | 0.18 |
| Age (years) | 31 (9) | 42 (12) | <0.0001 |
| Disease duration (years) # | 13 (8–18.5) | 14.5 (–23) | 0.47 |
| Orthostatic intolerance in daily life | 34 (100%) | 56 (85%) | 0.02 # |
| Height (cm) | 174 (7) | 174 (8) | 0.98 |
| Weight (kg) | 74 (18) | 72 (15) | 0.63 |
| BMI (kg/m2) | 24.7 (6.3) | 24.1 (5.1) | 0.59 |
| Heart rate supine (bpm) | 77 (18) | 74 (13) | 0.30 |
| Heart rate sitting (bpm) | 89 (21) | 86 (17) | 0.48 |
| Systolic blood pressure supine (mmHg) | 126 (16) | 124 (18) | 0.67 |
| Systolic blood pressure sitting (mmHg) | 136 (15) | 134 (19) | 0.64 |
| Diastolic blood pressure supine (mmHg) | 82 (12) | 79 (10) | 0.30 |
| Diastolic blood pressure sitting (mmHg) | 89 (11) | 87 (10) | 0.64 |
| Cerebral blood flow supine (mL/min) | 656 (121) | 619 (121) | 0.15 |
| Cerebral blood flow sitting (mL/min) | 466 (96) | 478 (96) | 0.57 |
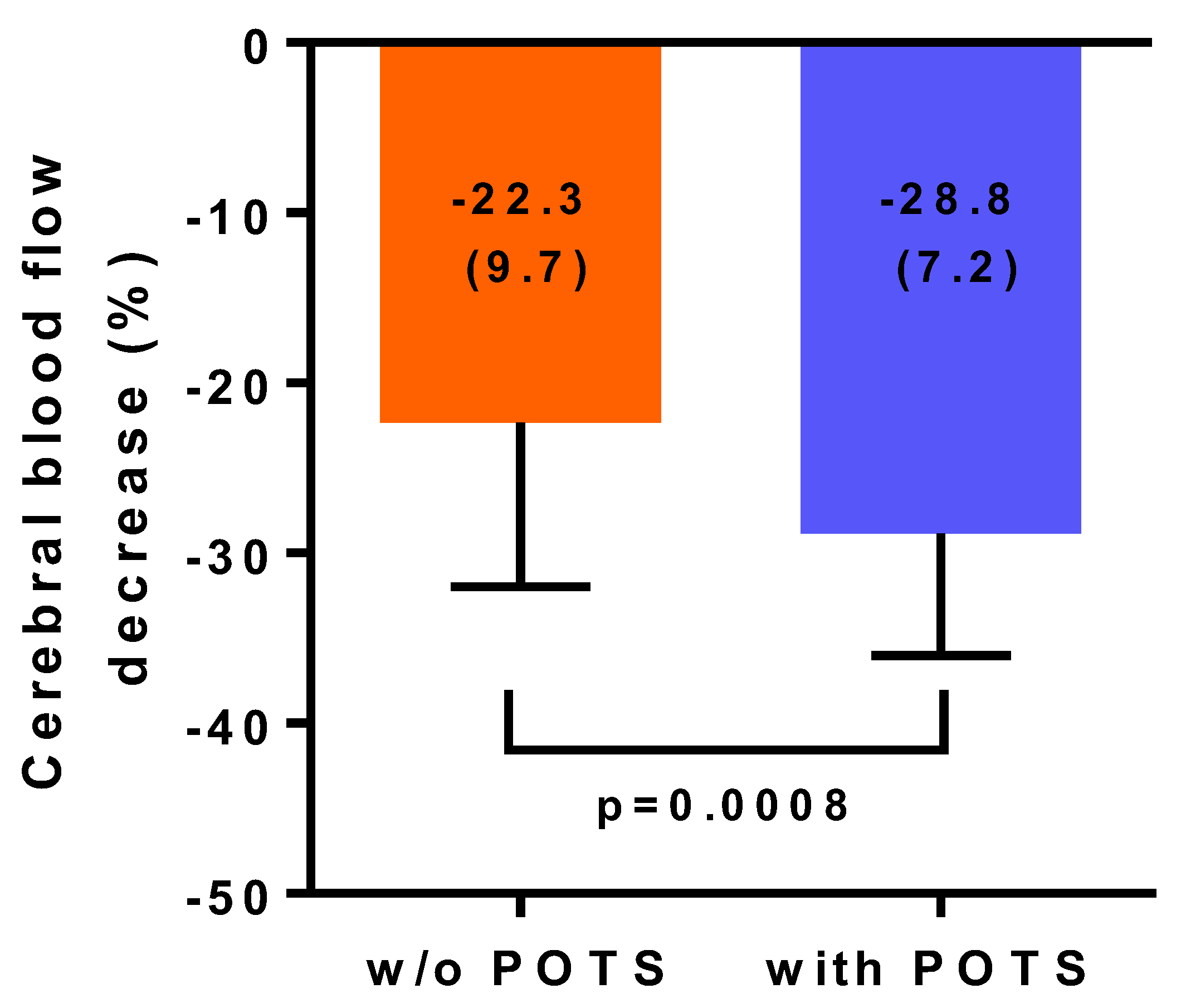
| Cerebral blood flow % change sitting vs. supine | −28.8 (7.2) | −22.3 (9.7) | <0.001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Campen, C.M.v.; Rowe, P.C.; Visser, F.C. Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients. Healthcare 2020, 8, 394. https://doi.org/10.3390/healthcare8040394
Campen CMv, Rowe PC, Visser FC. Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients. Healthcare. 2020; 8(4):394. https://doi.org/10.3390/healthcare8040394
Chicago/Turabian StyleCampen, C (Linda) MC van, Peter C. Rowe, and Frans C Visser. 2020. "Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients" Healthcare 8, no. 4: 394. https://doi.org/10.3390/healthcare8040394
APA StyleCampen, C. M. v., Rowe, P. C., & Visser, F. C. (2020). Reductions in Cerebral Blood Flow Can Be Provoked by Sitting in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients. Healthcare, 8(4), 394. https://doi.org/10.3390/healthcare8040394





