Decision Conflicts in Clinical Care during COVID-19: A Multi-Perspective Inquiry
Abstract
:1. Introduction
2. Materials and Methods
2.1. Questionnaire Development
2.2. Sample
2.3. Variables
2.4. Data Analysis
3. Results
3.1. Questionnaire Responses
3.2. Decisional Uncertainty and Conflicts
3.3. Consequences of Decisional Uncertainty and Conflicts
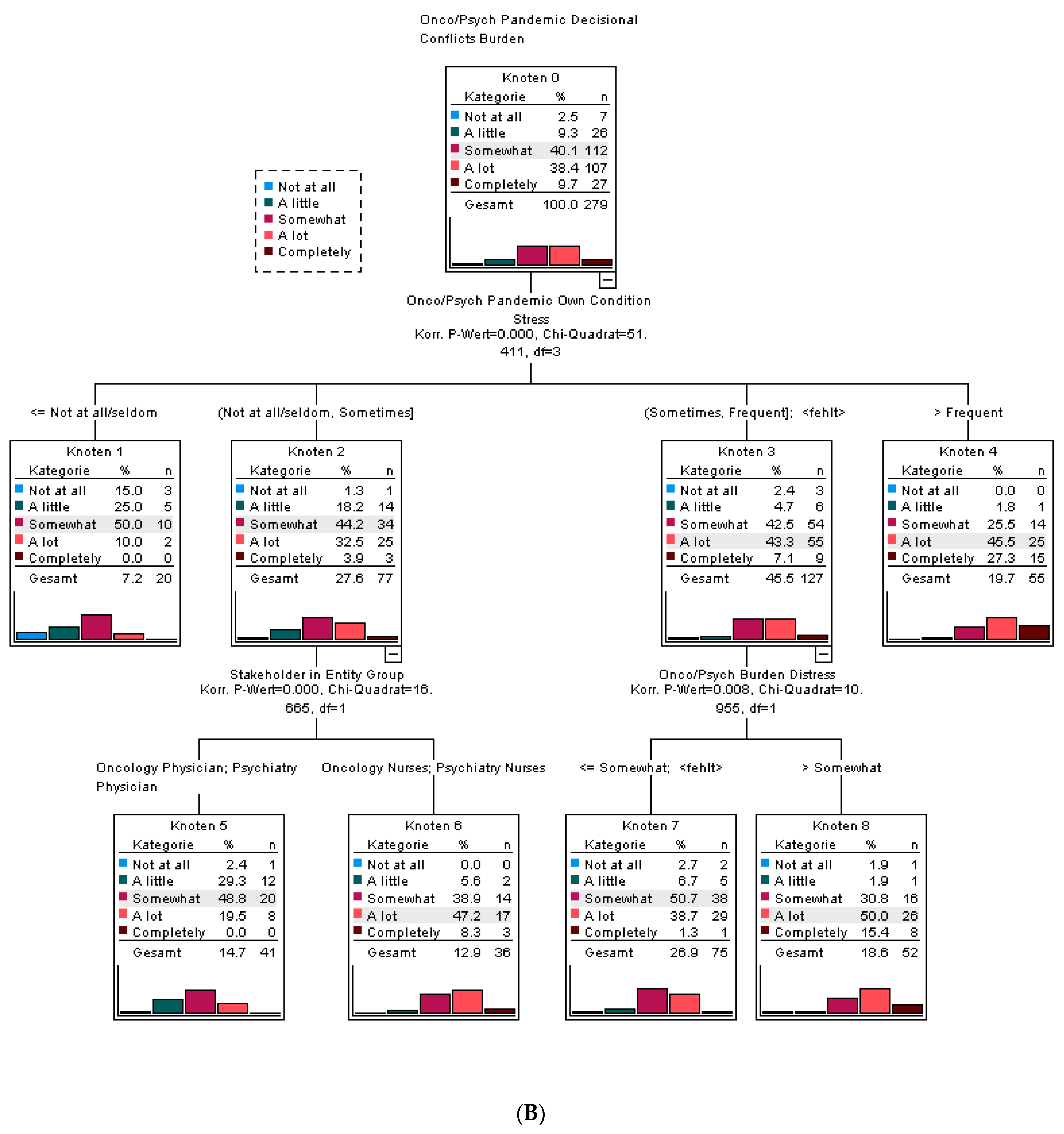
3.4. Reasons and Vulnerability
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Beller, J.; Schäfers, J.; Geyer, S.; Haier, J.; Epping, J. Patterns of Changes in Oncological Care due to COVID-19: Results of a Survey of Oncological Nurses and Physicians from the Region of Hanover, Germany. Healthcare 2021, 10, 15. [Google Scholar] [CrossRef]
- Beller, J.; Schäfers, J.; Haier, J.; Geyer, S.; Epping, J. Trust in Healthcare during COVID-19 in Europe: Vulnerable groups trust the least. J. Public Health 2022, 1–10. [Google Scholar] [CrossRef]
- Wamkpah, N.S.; Gerndt, S.P.; Kallogjeri, D.; Piccirillo, J.F.; Chi, J.J. Patients’ Views of Shared Decision-making and Decisional Conflict in Otolaryngologic Surgery During the COVID-19 Pandemic. JAMA Otolaryngol. Neck Surg. 2021, 147, 879. [Google Scholar] [CrossRef] [PubMed]
- Deml, M.J.; Minnema, J.; Dubois, J.; Senn, O.; Streit, S.; Rachamin, Y.; Jungo, K.T. The impact of the COVID-19 pandemic on the continuity of care for at-risk patients in Swiss primary care settings: A mixed-methods study. Soc. Sci. Med. 2022, 298, 114858. [Google Scholar] [CrossRef]
- Koren, O.; Abu Rajab, S.; Barbour, M.; Shachar, M.; Shahar, A.; Zubidat, K.; Slim, W.; Igbariya, D.; Rozner, E.; Turgeman, Y.; et al. The impact of anxiety level on decision to seek medical care of non-COVID cardiac patients during the pandemic outbreak—single-center experience in Israel. Rev. Cardiovasc. Med. 2022, 23, 50. [Google Scholar] [CrossRef]
- Géa, L.P.; Upfold, C.; Qureshi, A.; Moulden, H.M.; Mamak, M.; Bradford, J.M.W.; Chaimowitz, G.A. Public perceptions of psychiatric, justice-involved, and elderly populations during the COVID-19 pandemic. J. Psychiatr. Res. 2021, 146, 67–76. [Google Scholar] [CrossRef] [PubMed]
- Giwa, A.; Crutchfield, D.; Fletcher, D.; Gemmill, J.; Kindrat, J.; Smith, A.; Bayless, P. Addressing Moral Injury in Emergency Medicine. J. Emerg. Med. 2021, 61, 782–788. [Google Scholar] [CrossRef] [PubMed]
- Seino, Y.; Aizawa, Y.; Kogetsu, A.; Kato, K. Ethical and Social Issues for Health Care Providers in the Intensive Care Unit during the Early Stages of the COVID-19 Pandemic in Japan: A Questionnaire Survey. Asian Bioeth. Rev. 2021, 14, 115–131. [Google Scholar] [CrossRef] [PubMed]
- Rashid, S.; Reeder, C.; Sahu, S.; Rashid, S. Psychological distress and moral injury to oncologists and their patients during COVID-19 pandemic. Curr. Psychol. 2021, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Mulet, C.; Sansó, N.; Carrero-Planells, A.; López-Deflory, C.; Galiana, L.; García-Pazo, P.; Borràs-Mateu, M.M.; Miró-Bonet, M. The Impact of the COVID-19 Pandemic on ICU Healthcare Professionals: A Mixed Methods Study. Int. J. Environ. Res. Public Health 2021, 18, 9243. [Google Scholar] [CrossRef] [PubMed]
- Azoulay, E.; De Waele, J.; Ferrer, R.; Staudinger, T.; Borkowska, M.; Povoa, P.; Iliopoulou, K.; Artigas, A.; Schaller, S.J.; Hari, M.S.; et al. Symptoms of burnout in intensive care unit specialists facing the COVID-19 outbreak. Ann. Intensiv. Care 2020, 10, 1–8. [Google Scholar] [CrossRef]
- Romdhani, M.; Kohler, S.; Koskas, P.; Drunat, O. Ethical dilemma for healthcare professionals facing elderly dementia patients during the COVID-19 pandemic. L’Encéphale 2021, 48, 595–598. [Google Scholar] [CrossRef]
- Sukhera, J.; Kulkarni, C.; Taylor, T. Structural distress: Experiences of moral distress related to structural stigma during the COVID-19 pandemic. Perspect. Med. Educ. 2021, 10, 222–229. [Google Scholar] [CrossRef] [PubMed]
- Haier, J.; Beller, J.; Adorjan, K.; Bleich, S.; De Greck, M.; Griesinger, F.; Hein, A.; Hurlemann, R.; Mees, S.T.; Philipsen, A.; et al. Decision Conflicts in Clinical Care during COVID-19: A Patient Perspective. Healthcare 2022, 10, 1019. [Google Scholar] [CrossRef]
- Monaco, A.; Blanco, A.C.; Cobain, M.; Costa, E.; Guldemond, N.; Hancock, C.; Onder, G.; Pecorelli, S.; Silva, M.; Tournoy, J.; et al. The role of collaborative, multistakeholder partnerships in reshaping the health management of patients with noncommunicable diseases during and after the COVID-19 pandemic. Aging Clin. Exp. Res. 2021, 33, 2899–2907. [Google Scholar] [CrossRef]
- Donkers, M.A.; Gilissen, V.J.H.S.; Candel, M.J.J.M.; van Dijk, N.M.; Kling, H.; Heijnen-Panis, R.; Pragt, E.; van der Horst, I.; Pronk, S.A.; van Mook, W.N.K.A. Moral distress and ethical climate in intensive care medicine during COVID-19: A nationwide study. BMC Med Ethic. 2021, 22, 73. [Google Scholar] [CrossRef]
- Haier, J.; Mayer, M.; Schaefers, J.; Geyer, S.; Feldner, D. A pyramid model to describe changing decision making under high uncertainty during the COVID-19 pandemic. BMJ Glob. Health 2022, 7, e008854. [Google Scholar] [CrossRef] [PubMed]
- Austin, E.J.; Blacker, A.; Kalia, I. “Watching the tsunami come”: A case study of female healthcare provider experiences during the COVID-19 pandemic. Appl. Psychol. Health Well-Being 2021, 13, 781–797. [Google Scholar] [CrossRef]
- Dutour, M.; Kirchhoff, A.; Janssen, C.; Meleze, S.; Chevalier, H.; Levy-Amon, S.; Detrez, M.-A.; Piet, E.; Delory, T. Family medicine practitioners’ stress during the COVID-19 pandemic: A cross-sectional survey. BMC Fam. Pract. 2021, 22, 36. [Google Scholar] [CrossRef] [PubMed]
- Vanni, G.; Materazzo, M.; Santori, F.; Pellicciaro, M.; Costesta, M.; Orsaria, P.; Cattadori, F.; Pistolese, C.A.; Perretta, T.; Chiocchi, M.; et al. The Effect of Coronavirus (COVID-19) on Breast Cancer Teamwork: A Multicentric Survey. Vivo 2020, 34, 1685–1694. [Google Scholar] [CrossRef] [PubMed]
- Luoto, S.; Varella, M.A.C. Pandemic Leadership: Sex Differences and Their Evolutionary–Developmental Origins. Front. Psychol. 2021, 12, 633862. [Google Scholar] [CrossRef]
- Bacigalupe, A.; Cabezas-Rodríguez, A.; Giné-March, A.; Carrillo, M.J. Gender invisibility in the COVID-19 management: Who are the policy decision-makers during the pandemic? Gac. Sanit. 2021, 36, 156–159. [Google Scholar] [CrossRef]
- Monge-Rodríguez, F.; Jiang, H.; Zhang, L.; Alvarado-Yepez, A.; Cardona-Rivero, A.; Huaman-Chulluncuy, E.; Torres-Mejía, A. Psychological Factors Affecting Risk Perception of COVID-19: Evidence from Peru and China. Int. J. Environ. Res. Public Health 2021, 18, 6513. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Sanz, J.; Pérez-Molina, J.A.; Moreno, S.; Zamora, J.; Serrano-Villar, S. Understanding clinical decision-making during the COVID-19 pandemic: A cross-sectional worldwide survey. eClinicalMedicine 2020, 27, 100539. [Google Scholar] [CrossRef] [PubMed]
- Pololi, L.H.; Vasiliou, V.; Bloom-Feshbach, K. Midcareer Medical School Research Faculty Perspectives on Vitality and Professionalism During the COVID-19 Pandemic. JAMA Netw. Open 2021, 4, e2120642. [Google Scholar] [CrossRef]
- Haier, J.; Sleeman, J.; Schäfers, J. Sociocultural incentives for cancer care implementation. Clin. Exp. Metastasis 2020, 37, 561–563. [Google Scholar] [CrossRef]
- Banks, L.; Randhawa, V.K.; Colella, T.J.; Dhanvantari, S.; Connelly, K.A.; Robinson, L.; Mak, S.; Ouzounian, M.; Mulvagh, S.L.; Straus, S.; et al. Cardiovascular Physicians, Scientists, and Trainees Balancing Work and Caregiving Responsibilities in the COVID-19 Era: Sex and Race-Based Inequities. CJC Open 2021, 3, 627–630. [Google Scholar] [CrossRef]





| # Respondents | Female/Male a | Age b | Experience c | % Respond | |
|---|---|---|---|---|---|
| Oncology Physicians | 207 | 97/109 | 43.3 ± 10.3 | 15.2 ± 10.5 | 16.8 |
| Oncology Nurses | 241 | 202/35 | 42.3 ± 12.3 | 19.1 ± 12.3 | 19.6 |
| Oncology Patients | 386 | 197/183 | 59.7 ± 15.6 | 31.4 | |
| Psychiatry Physicians | 115 | 63/51 | 38.5 ± 10.5 | 9.9 ± 9.2 | 9.3 |
| Psychiatry Nurses | 128 | 85/33 | 43.4 ± 19.3 | 19.3 ± 12.6 | 10.4 |
| Psychiatry Patients | 154 | 86/62 | 39.3 ± 15.6 | 12.5 | |
| Total | 1231 | 730/473 | 47.4 ± 15.9 | 16.4 ± 11.8 | 100.0 |
| (A) | |||||||
| Effect | −2 Log-Likelihood for Reduced Model | Likelihood-Quotient Tests | |||||
| Chi-Square | dF | Significance | |||||
| Constant term | 1086.079 | 0.000 | 0 | 0.000 | |||
| Stakeholder in entity group | 1111.436 | 25.357 | 12 | 0.013 | |||
| Age | 1094.640 | 8.562 | 4 | 0.073 | |||
| Gender | 1101.177 | 15.098 | 12 | 0.236 | |||
| Availability of professional information | 1120.034 | 33.955 | 16 | 0.006 | |||
| Modification of own decisions | 1262.868 | 176.789 | 16 | 0.000 | |||
| Burden due to distress | 1598.556 | 512.477 | 16 | 0.000 | |||
| Burden due to own risk | 1110.867 | 24.788 | 16 | 0.074 | |||
| Own condition stress | 1120.687 | 34.608 | 12 | 0.001 | |||
| Pandemic workload | 1112.688 | 26.609 | 16 | 0.046 | |||
| (B) | |||||||
| Observed | Predicted | ||||||
| Not at All | A Little | Somewhat | A Lot | Completely | % Correct | % Correct with Neighbor | |
| Not at all | 55 | 35 | 5 | 0 | 0 | 57.9% | 94.7% |
| A little | 24 | 137 | 41 | 11 | 3 | 63.4% | 93.5% |
| Somewhat | 4 | 37 | 113 | 12 | 1 | 67.7% | 97.0% |
| A lot | 2 | 16 | 29 | 40 | 2 | 44.9% | 79.8% |
| Completely | 0 | 0 | 2 | 2 | 13 | 76.5% | 88.2% |
| % Total | 14.6% | 38.5% | 32.5% | 11.1% | 3.3% | 61.3% | 92.5% |
| (A) | |||||||
| Effect | −2 Log-Likelihood for Reduced Model | Likelihood-Quotient Tests | |||||
| Chi-Square | dF | Significance | |||||
| Constant term | 428.226 | 0.000 | 0 | 0.000 | |||
| Age | 1101.176 | 672.950 | 4 | 0.000 | |||
| Gender | 434.342 | 6.117 | 8 | 0.634 | |||
| Stakeholder in entity group | 515.481 | 87.256 | 12 | 0.000 | |||
| Modification of own decisions | 500.931 | 72.705 | 16 | 0.000 | |||
| Burden due to own risk | 526.510 | 98.284 | 16 | 0.000 | |||
| Burden due to distress | 442.304 | 14.078 | 16 | 0.593 | |||
| Own condition stress | 502.116 | 73.891 | 12 | 0.000 | |||
| Pandemic workload | 511.219 | 82.993 | 16 | 0.000 | |||
| (B) | |||||||
| Observed | Predicted | ||||||
| Not at All | A Little | Somewhat | A Lot | Completely | % Correct | % Correct with Neighbor | |
| Not at all | 4 | 0 | 1 | 1 | 0 | 66.7% | 66.7% |
| A little | 0 | 11 | 6 | 8 | 0 | 44.0% | 68.0% |
| Somewhat | 0 | 3 | 72 | 24 | 2 | 71.3% | 98.0% |
| A lot | 0 | 2 | 28 | 55 | 4 | 61.8% | 97.8% |
| Completely | 0 | 0 | 4 | 5 | 17 | 65.4% | 84.6% |
| % Total | 1.6% | 6.5% | 44.9% | 37.7% | 9.3% | 64.4% | 92.7% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Haier, J.; Beller, J.; Adorjan, K.; Bleich, S.; de Greck, M.; Griesinger, F.; Heppt, M.; Hurlemann, R.; Mees, S.T.; Philipsen, A.; et al. Decision Conflicts in Clinical Care during COVID-19: A Multi-Perspective Inquiry. Healthcare 2022, 10, 1914. https://doi.org/10.3390/healthcare10101914
Haier J, Beller J, Adorjan K, Bleich S, de Greck M, Griesinger F, Heppt M, Hurlemann R, Mees ST, Philipsen A, et al. Decision Conflicts in Clinical Care during COVID-19: A Multi-Perspective Inquiry. Healthcare. 2022; 10(10):1914. https://doi.org/10.3390/healthcare10101914
Chicago/Turabian StyleHaier, Joerg, Johannes Beller, Kristina Adorjan, Stefan Bleich, Moritz de Greck, Frank Griesinger, Markus Heppt, René Hurlemann, Soeren Torge Mees, Alexandra Philipsen, and et al. 2022. "Decision Conflicts in Clinical Care during COVID-19: A Multi-Perspective Inquiry" Healthcare 10, no. 10: 1914. https://doi.org/10.3390/healthcare10101914
APA StyleHaier, J., Beller, J., Adorjan, K., Bleich, S., de Greck, M., Griesinger, F., Heppt, M., Hurlemann, R., Mees, S. T., Philipsen, A., Rohde, G., Schilling, G., Trautmann, K., Combs, S. E., Geyer, S., & Schaefers, J. (2022). Decision Conflicts in Clinical Care during COVID-19: A Multi-Perspective Inquiry. Healthcare, 10(10), 1914. https://doi.org/10.3390/healthcare10101914









