Kidney Transplant: Survival Analysis and Prognostic Factors after 10 Years of Follow-Up
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Data Collection
2.3. Statistical Analysis
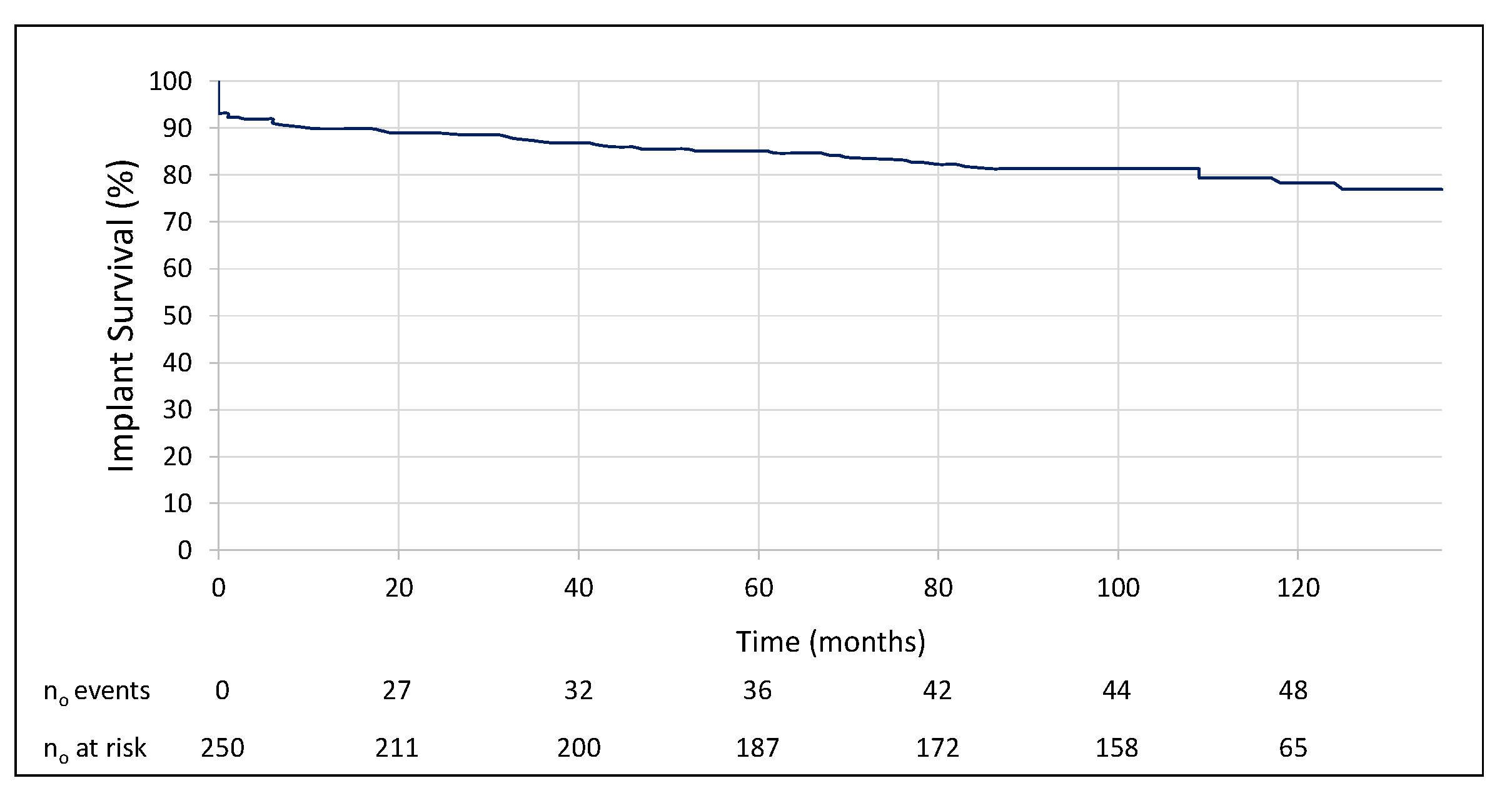
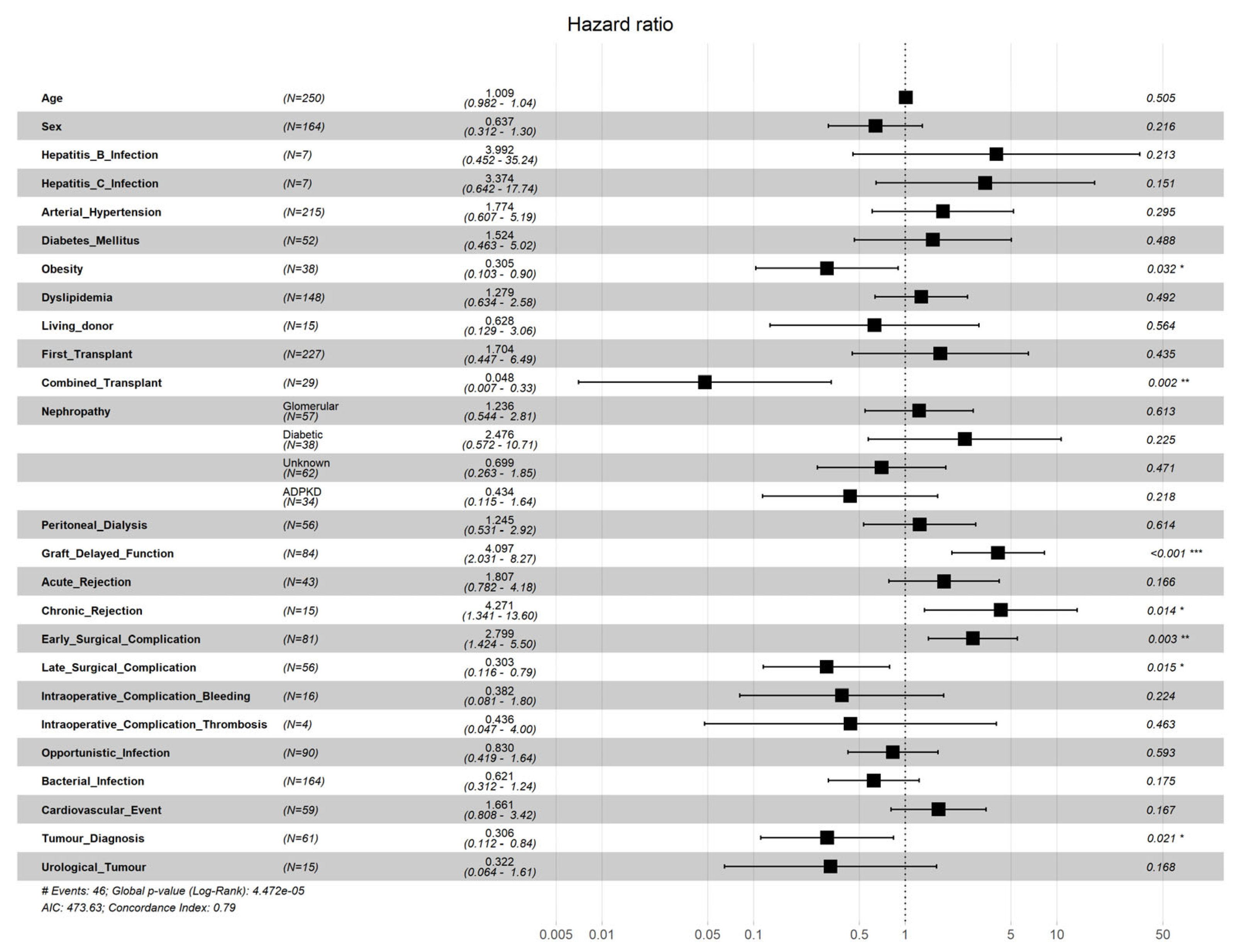
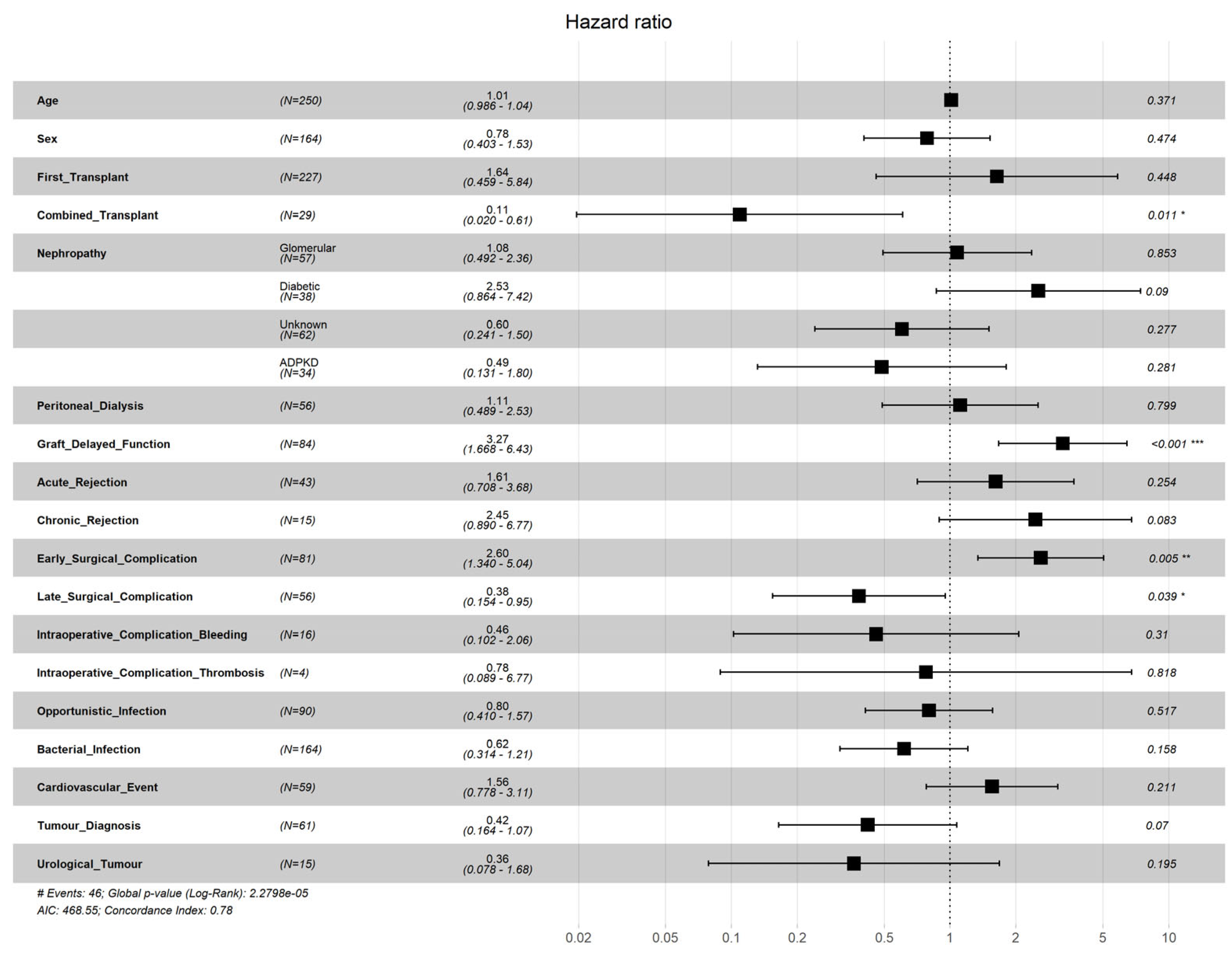
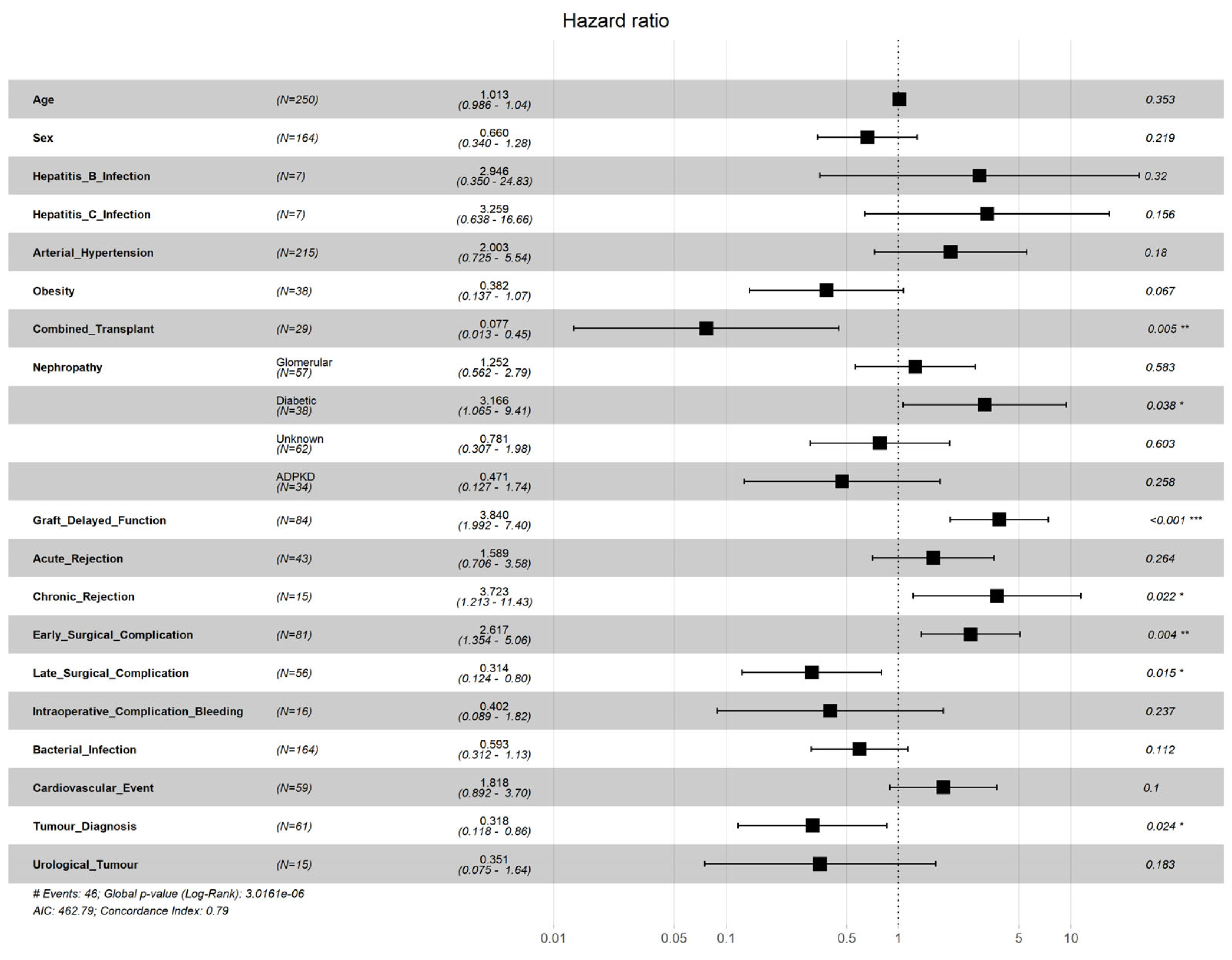
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Axelrod, D.A.; Schnitzler, M.A. An economic assessment of contemporary kidney transplant practice. Am. J. Transpl. 2018, 18, 1168–1176. [Google Scholar] [CrossRef] [PubMed]
- Querard, A.H.; Foucher, Y. Comparison of survival outcomes between Expanded Criteria Donor and Standard Criteria Donor kidney transplant recipients: A systematic review and meta-analysis. Transpl. Int. 2016, 29, 403–415. [Google Scholar] [CrossRef] [PubMed]
- Wolfe, R.A.; Ashby, V.B. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N. Engl. J. Med. 1999, 341, 1725–1730. [Google Scholar] [CrossRef] [PubMed]
- Organización Nacional de Trasplantes. Ministerio de Sanidad. Balance de actividad del 2021. Comunicado de Prensa, 2021 Gen, Madrid. Available online: http://www.ont.es/Documents/Balance%20de%20actividad%20Donaci%C3%B3n%20y%20Trasplante%202021_ONT.pdf (accessed on 28 November 2022).
- Van Loon, E.; Senev, A. Assessing the Complex Causes of Kidney Allograft Loss. Transplantation 2020, 104, 2557–2566. [Google Scholar] [CrossRef] [PubMed]
- Gondos, A.; Döhler, B. Kidney Graft Survival in Europe and the United States. Strikingly Different Long-Term Outcomes. Transpl. J. 2013, 95, 267–274. [Google Scholar] [CrossRef]
- Douglas, S.K.; Demattos, A. Effect of donor recipient age match on survival after first deceased donor renal transplantation. J. Am. Soc. Nephrol. 2004, 15, 1086–1091. [Google Scholar]
- Morath, C.; Döhler, B. Pre-transplant HLA Antibodies and Delayed Graft Function in the Current Era of Kidney Transplantation. Front Immunol. 2020, 11, 1886. [Google Scholar] [CrossRef]
- Chih-Yuan, L.; Ching-Yao, Y. Prognostic factors for renal transplant graft survival in a retrospective cohort of 1000 cases: The role of desensitization therapy. J. Formos. Med. Assoc. 2020, 119, 829–837. [Google Scholar]
- Jeon, J.Y.; Kim, S.J. Trends in the effects of pre-transplant diabetes on mortality and cardiovascular events after kidney transplantation. J. Diabetes Investig. 2021, 12, 811–818. [Google Scholar] [CrossRef]
- Erturk, T.; Berber, I. Effect of Obesity on Clinical Outcomes of Kidney Transplant Patients. Transpl. Proc. 2019, 51, 1093–1095. [Google Scholar] [CrossRef]
- Fellmann, M.; Loïc, B. Effects of Obesity on Postoperative Complications and Graft Survival After Kidney Transplantation. Transpl. Proc. 2020, 52, 3153–3159. [Google Scholar] [CrossRef]
- Prezelin, M.; Combe, C. Prolonged dialysis duration is associated with graft failure and mortality after kidney transplantation: Results from the French transplant database. Nephrol. Dial. Transpl. 2019, 34, 538–545. [Google Scholar] [CrossRef]
- Torres, A.; Hernández, D. Randomized Controlled Trial Assessing the Impact of Tacrolimus Versus Cyclosporine on the Incidence of Posttransplant Diabetes Mellitus. Kidney Int. Rep. 2018, 3, 1304–1315. [Google Scholar] [CrossRef]
- Barba, J.; Rinco, A. Complicaciones quirúrgicas en el trasplante renal y su influencia en la supervivencia del injerto. Actas Urológicas Españolas 2010, 34, 266–273. [Google Scholar] [CrossRef]
- Kramer, A.; Pippias, M. The European Renal Association – European Dialysis and Transplant Association (ERA-EDTA) Registry Annual Report 2016: A summary. Clin. Kidney J. 2019, 12, 702–720. [Google Scholar] [CrossRef]
- Álvarez, L.E.; Martínez, P. Supervivencia del paciente y del injerto a largo plazo en receptores de trasplante renal. Rev. Med. Inst. Mex. Seguro Soc. 2019, 57, 348–356. [Google Scholar]
- Sexton, D.J.; O’Kelly, P. Progressive improvement in short-, medium- and long-term graft survival in kidney transplantation patients in Ireland—A retrospective study. Transpl. Int. 2019, 32, 974–984. [Google Scholar] [CrossRef] [PubMed]
- Saucedo, H.; Haakinson, D.J. Prognostic factors in kidney transplantation in the septuagenarian: A multicenter analysis. Clin. Transpl. 2016, 30, 828–835. [Google Scholar] [CrossRef]
- Gopalakrishnan, V.; Agarwal, S.K. Infection is the chief cause of mortality and non-death censored graft loss in the first year after renal transplantation in a resource limited population: A single centre study. Nephrology 2019, 24, 456–463. [Google Scholar] [CrossRef]
- Noguchi, H.; Kitada, H. Outcome of renal transplantation in patients with type 2 diabetic nephropathy: A single-center experience. Transpl. Proc. 2015, 47, 608–611. [Google Scholar] [CrossRef]
- Butala, N.M.; Reese, P.P. Is delayed graft function causally associated with long-term outcomes after kidney transplantation? Instrumental variable analysis. Transplantation 2013, 95, 1008–1014. [Google Scholar] [CrossRef] [PubMed]
- Redfield, R.R.; Scalea, J.R. Predictors and outcomes of delayed graft function after living-donor kidney transplantation. Transpl. Int. 2016, 29, 81–87. [Google Scholar] [CrossRef]
- Kim, S.J.; Lee, H.H. Prognostic factors affecting graft and patient survival in cadaveric and living kidney transplantation. Transpl. Proc. 2004, 36, 2038–2039. [Google Scholar] [CrossRef] [PubMed]
- Vnucak, M.; Granak, K. The impact of different induction immunosuppression protocols on patient survival, graft survival and acute graft rejection after kidney transplantation. Bratisl. Lek. Listy 2022, 123, 730–735. [Google Scholar] [CrossRef]
- Pillot, P.; Bardonnaud, N. Risk factors for surgical complications after renal transplantation and impact on patient and graft survival. Transpl. Proc. 2012, 44, 2803–2808. [Google Scholar] [CrossRef]
- Tisserand, B.; Doré, B. Impact à long terme des complications chirurgicales sur la survie du transplant rénal. Progrès Urol. 2013, 23, 113–120. [Google Scholar] [CrossRef]
| Demographic Variables | n (%) |
|---|---|
| Age at transplant in years [µ ± SD] | 52.3 ± 14.0 |
| Sex | |
| Female | 86 (34.4) |
| Male | 164 (65.6) |
| Comorbidity | n (%) |
| Arterial Hypertension | 215 (86.0) |
| Diabetes Mellitus | 52 (20.8) |
| Obesity | 38 (15.2) |
| Dyslipidemia | 148 (59.2) |
| Hepatitis B Virus Infection | 7 (2.8) |
| Hepatitis C Virus Infection | 7 (2.8) |
| Aetiology of Chronic Kidney Disease | |
| Glomerular Nephropathy | 57 (22.8) |
| Diabetic nephropathy | 38 (12.2) |
| Autosomal Dominant Polycystic Kidney Disease | 34 (13.6) |
| Unknown | 62 (24.8) |
| Renal Replacement Therapy | |
| Type 1 | |
| Haemodialysis | 159 (64.1) |
| Peritoneal dialysis | 48 (19.4) |
| Both | 34 (13.7) |
| Pre-dialysis | 7 (2.8) |
| Mean time (years) in replacement therapy [µ± SD] | 4.4 ± 4.2 |
| Type of Complication | n (%) |
|---|---|
| Intraoperative Complication | 31 (12.4) |
| Bleeding | 16 (6.4) |
| Thrombosis | 4 (1.6) |
| Early Surgical Complication | 81 (32.4) |
| Late Surgical Complication | 56 (22.4) |
| Acute Rejection | 42 (16.8) |
| Chronic Rejection | 15 (6.0) |
| Graft Delayed Function | 84 (33.6) |
| Opportunistic Infection | 90 (36.0) |
| Bacterial Infection | 164 (65.6) |
| Cardiovascular Event | 59 (23.6) |
| Tumour Diagnosis | 61 (24.4) |
| Urological Tumour | 15 (6.0) |
| Graft loss | 49 (19.6) |
| Death | 55 (22.0) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Beviá-Romero, Á.; Quereda-Flores, F.; Díaz-Carnicero, J.; Gómez-Palomo, F.; Ramos-Cebrián, M.; Espinosa-Vañó, J.; Castillo-Antón, D.J.; Broseta-Rico, E.; Vivas-Consuelo, D.; Budía-Alba, A. Kidney Transplant: Survival Analysis and Prognostic Factors after 10 Years of Follow-Up. Mathematics 2023, 11, 1640. https://doi.org/10.3390/math11071640
Beviá-Romero Á, Quereda-Flores F, Díaz-Carnicero J, Gómez-Palomo F, Ramos-Cebrián M, Espinosa-Vañó J, Castillo-Antón DJ, Broseta-Rico E, Vivas-Consuelo D, Budía-Alba A. Kidney Transplant: Survival Analysis and Prognostic Factors after 10 Years of Follow-Up. Mathematics. 2023; 11(7):1640. https://doi.org/10.3390/math11071640
Chicago/Turabian StyleBeviá-Romero, Álvaro, Francisco Quereda-Flores, Javier Díaz-Carnicero, Francisco Gómez-Palomo, María Ramos-Cebrián, Joaquín Espinosa-Vañó, Dario J. Castillo-Antón, Enrique Broseta-Rico, David Vivas-Consuelo, and Alberto Budía-Alba. 2023. "Kidney Transplant: Survival Analysis and Prognostic Factors after 10 Years of Follow-Up" Mathematics 11, no. 7: 1640. https://doi.org/10.3390/math11071640
APA StyleBeviá-Romero, Á., Quereda-Flores, F., Díaz-Carnicero, J., Gómez-Palomo, F., Ramos-Cebrián, M., Espinosa-Vañó, J., Castillo-Antón, D. J., Broseta-Rico, E., Vivas-Consuelo, D., & Budía-Alba, A. (2023). Kidney Transplant: Survival Analysis and Prognostic Factors after 10 Years of Follow-Up. Mathematics, 11(7), 1640. https://doi.org/10.3390/math11071640







