Development and Student Perception of Virtual Reality for Implant Surgery
Abstract
1. Introduction
2. Material and Methods
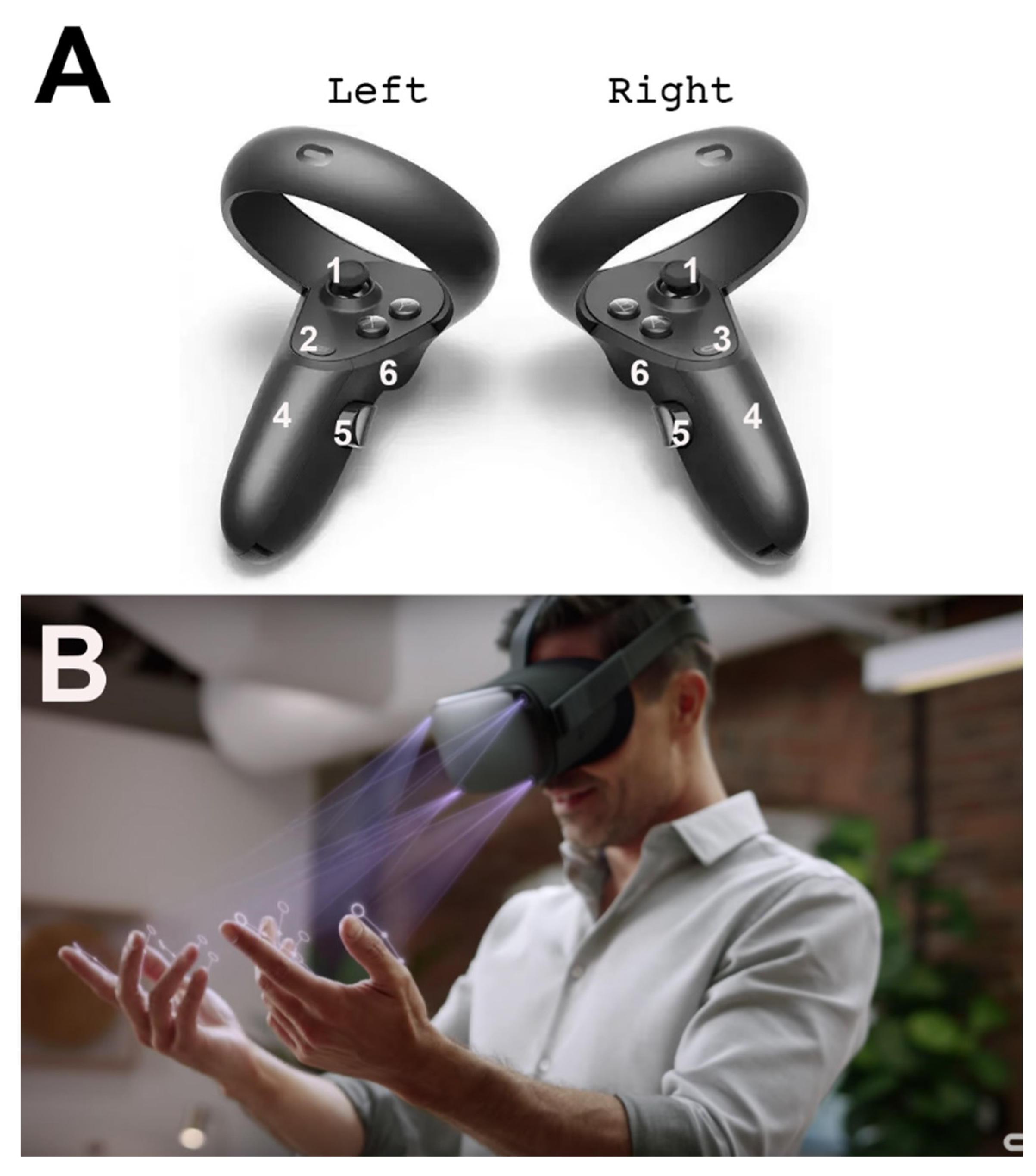
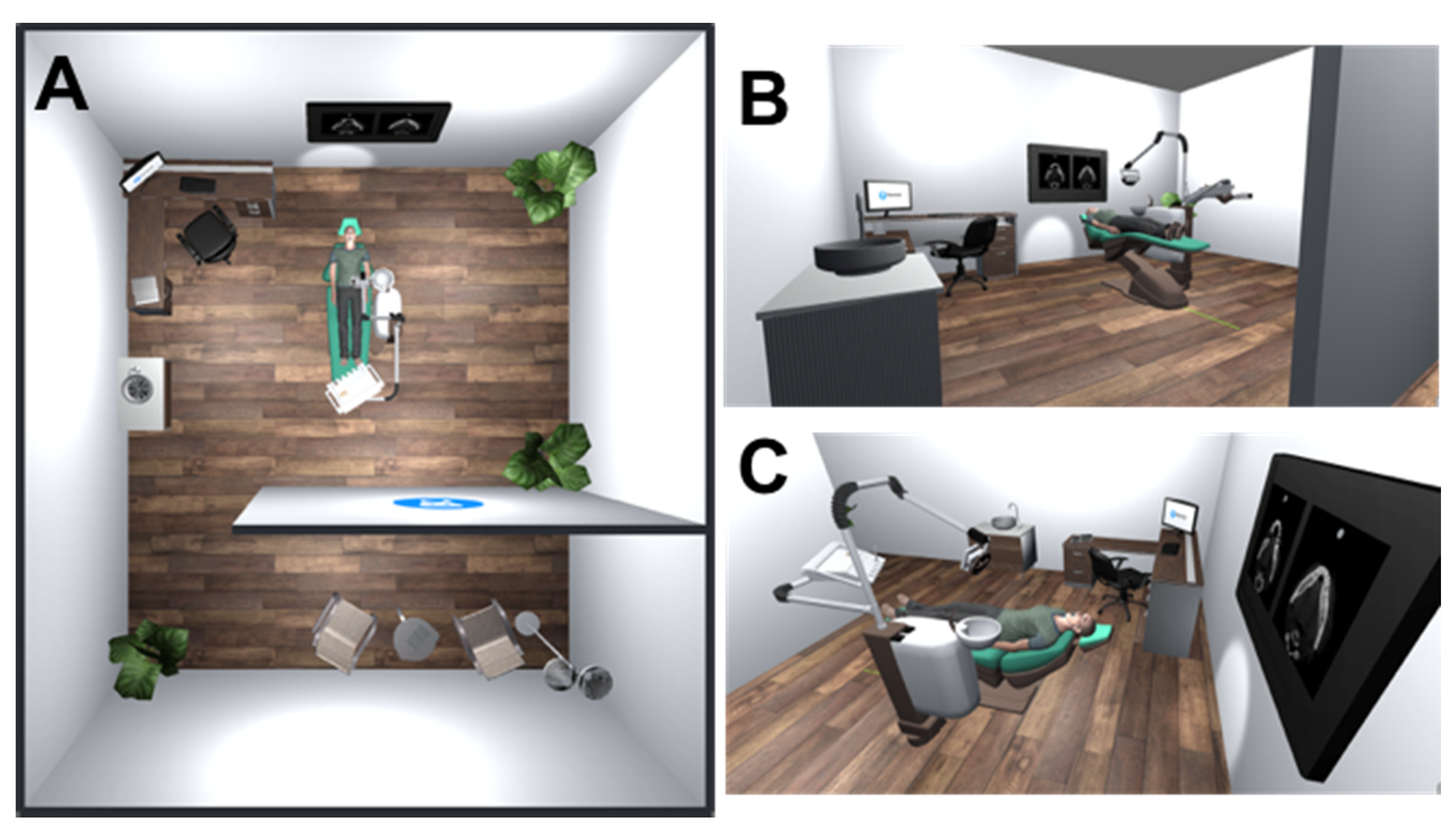
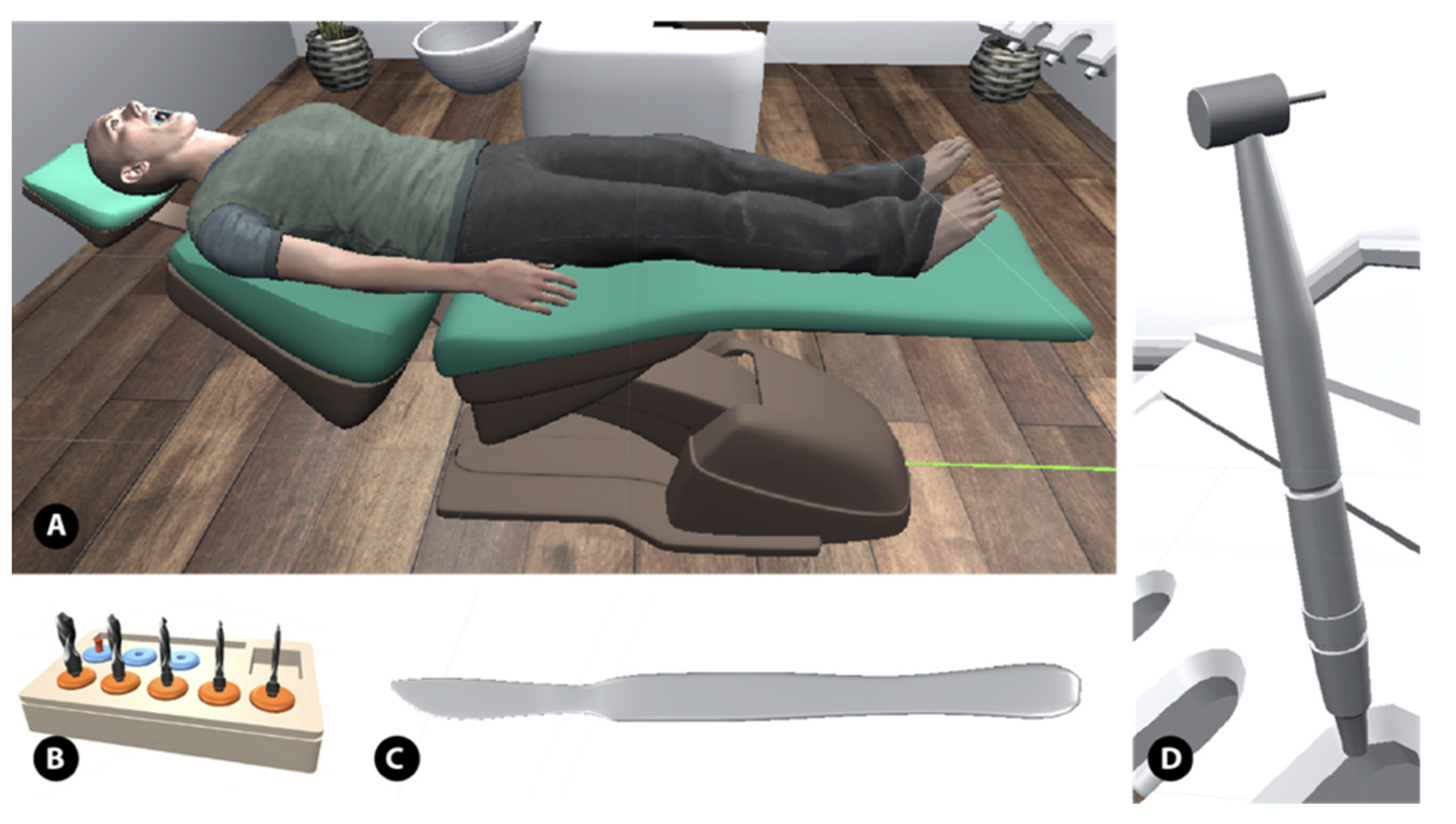
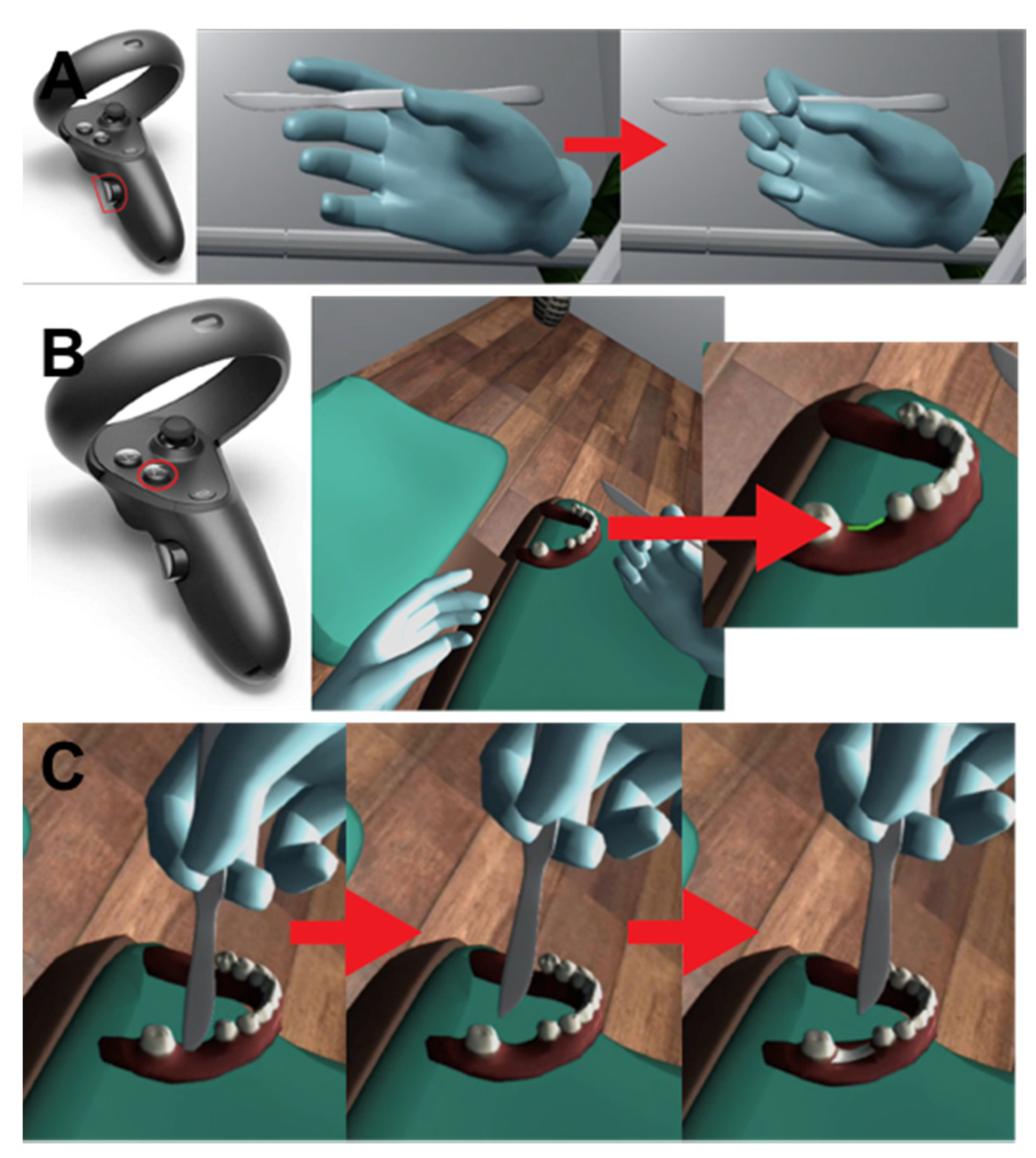
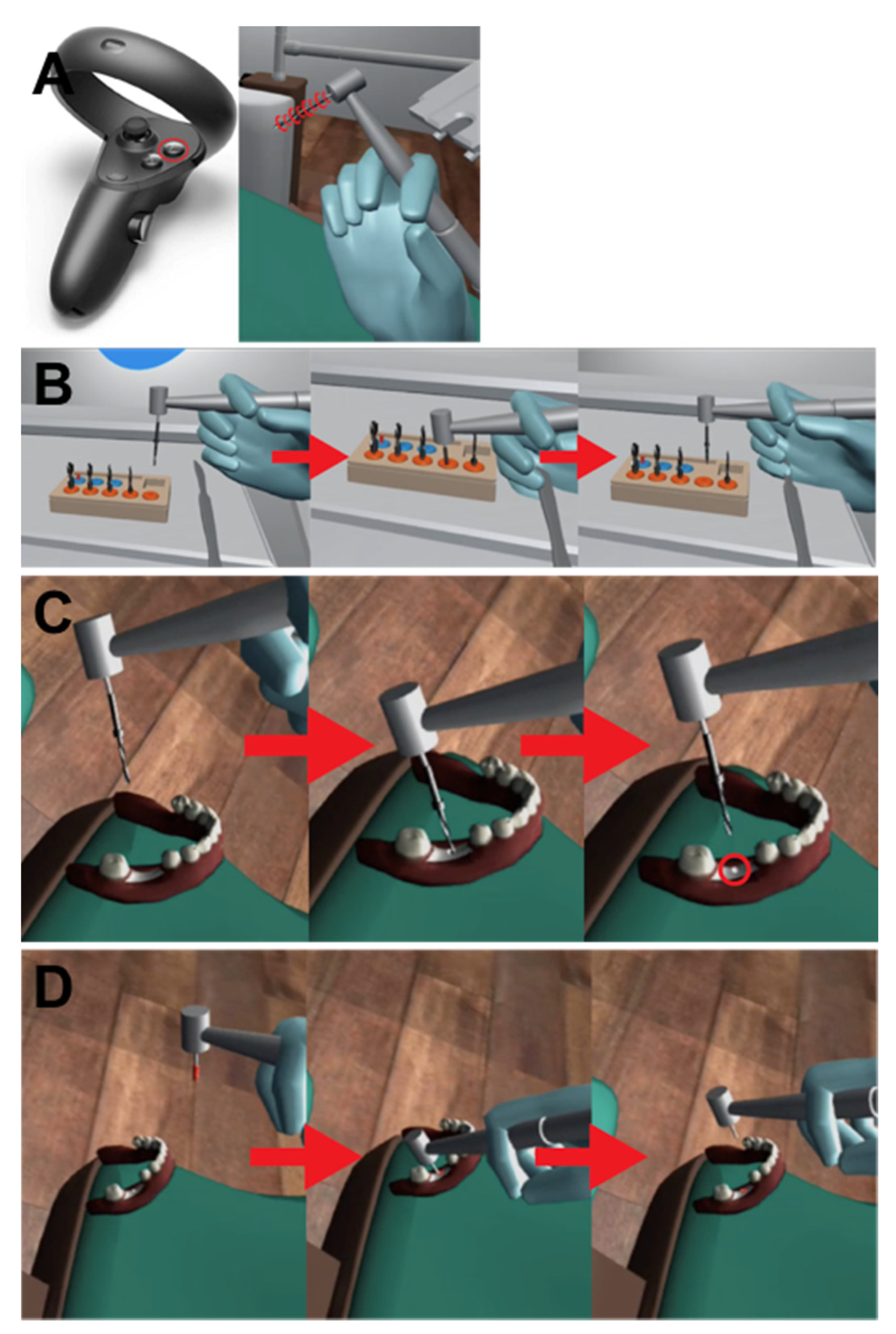
2.1. Development of Virtual Reality for Implant Surgery
2.2. Students’ Perception of the VR Implant Surgery
2.3. Focus Group Discussion (FGD)
3. Results
3.1. Students Perception on the VR Implant Surgery
3.2. FGD Result
3.2.1. Student Perceptions of Immersive Experiences
3.2.2. Advantages and Disadvantages of VR
3.2.3. Features to Add or Delete from Application
3.2.4. VR in the Curriculum and VR as the Future of Dental Education
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Ferrini, F.; Sannino, G.; Chiola, C.; Capparé, P.; Gastaldi, G.; Gherlone, E.F. Influence of intra-oral scanner (I.O.S.) on the marginal accuracy of CAD/CAM single crowns. Int. J. Environ. Res. Public Health 2019, 16, 544. [Google Scholar] [CrossRef]
- Gherlone, E.F.; Ferrini, F.; Crespi, R.; Gastaldi, G.; Cappare, P. Digital impressions for fabrication of definitive "all-on-four" restorations. Implant Dent. 2015, 24, 125–129. [Google Scholar] [CrossRef]
- Cattoni, F.; Teté, G.; Calloni, A.M.; Manazza, F.; Gastaldi, G.; Capparè, P. Milled versus moulded mock-ups based on the superimposition of 3D meshes from digital oral impressions: A comparative in vitro study in the aesthetic area. BMC Oral Health 2019, 19, 230. [Google Scholar] [CrossRef]
- Pagano, S.; Moretti, M.; Marsili, R.; Ricci, A.; Barraco, G.; Cianetti, S. Evaluation of the accuracy of four digital methods by linear and volumetric analysis of dental impressions. Materials 2019, 12, 1958. [Google Scholar] [CrossRef]
- Sberna, M.T.; Rizzo, G.; Zacchi, E.; Cappare, P.; Rubinacci, A. A preliminary study of the use of peripheral quantitative computed tomography for investigating root canal anatomy. Int. Endod. J. 2009, 42, 66–75. [Google Scholar] [CrossRef]
- Liebermann, A.; Erdelt, K. Virtual education: Dental morphologies in a virtual teaching environment. J. Dent. Educ. 2020, 84, 1143–1150. [Google Scholar] [CrossRef] [PubMed]
- Kim-Berman, H.; Karl, E.; Sherbel, J.; Sytek, L.; Ramaswamy, V. Validity and user experience in an augmented reality virtual tooth identification test. J. Dent. Educ. 2019, 83, 1345–1352. [Google Scholar] [CrossRef] [PubMed]
- Joda, T.; Gallucci, G.O.; Wismeijer, D.; Zitzmann, N.U. Augmented and virtual reality in dental medicine: A systematic review. Comput. Biol. Med. 2019, 108, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Pulijala, Y.; Ma, M.; Pears, M.; Peebles, D.; Ayoub, A. An innovative virtual reality training tool for orthognathic surgery. Int. J. Oral Maxillofac. Surg. 2018, 47, 1199–1205. [Google Scholar] [CrossRef] [PubMed]
- Raghav, K.; Van Wijk, A.J.; Abdullah, F.; Islam, M.N.; Bernatchez, M.; De Jongh, A. Efficacy of virtual reality exposure therapy for treatment of dental phobia: A randomized control trial. BMC Oral Health 2016, 16, 25. [Google Scholar] [CrossRef]
- Custodio, N.B.; Costa, F.D.S.; Cademartori, M.G.; da Costa, V.P.P.; Goettems, M.L. Effectiveness of Virtual reality glasses as a distraction for children during dental care. Pediatr. Dent. 2020, 42, 93–102. [Google Scholar]
- Touati, R.; Richert, R.; Millet, C.; Farges, J.C.; Sailer, I.; Ducret, M. Comparison of two innovative strategies using augmented reality for communication in aesthetic dentistry: A pilot study. J. Healthc. Eng. 2019, 2019, 7019046. [Google Scholar] [CrossRef]
- Zafar, S.; Zachar, J.J. Evaluation of HoloHuman augmented reality application as a novel educational tool in dentistry. Eur. J. Dent. Educ. 2020, 24, 259–265. [Google Scholar] [CrossRef] [PubMed]
- Murbay, S.; Neelakantan, P.; Chang, J.W.W.; Yeung, S. Evaluation of the introduction of a dental virtual simulator on the performance of undergraduate dental students in the pre-clinical operative dentistry course. Eur. J. Dent. Educ. 2020, 24, 5–16. [Google Scholar] [CrossRef] [PubMed]
- de Boer, I.R.; Lagerweij, M.D.; Wesselink, P.R.; Vervoorn, J.M. The effect of variations in force feedback in a virtual reality environment on the performance and satisfaction of dental students. Simul. Healthc. 2019, 14, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Jerald, J. The VR Book: Human-Centered Design for Virtual Reality: Association for Computing Machinery; Morgan & Claypool: San Rafel, CA, USA, 2015. [Google Scholar]
- Milgram, P.; Kishino, F. A taxonomy of mixed reality visual displays. IEICE Trans. Inf. Syst. 1994, 77, 1–15. [Google Scholar]
- Kim, N.; Phan, A.H.; Erdenebat, M.U.; Alam, A.; Kwon, K.C.; Piao, M.L.; Lee, J.H. 3D display technology. Disp. Imag. 2013, 1, 73–95. [Google Scholar]
- Kiyokawa, K. An Introduction to Head Mounted Display for Augmented Reality; IGI Global: Hershey, PA, USA, 2007. [Google Scholar]
- Goodacre, C.J. Digital learning resources for prosthodontic education: The perspectives of a long-term dental educator regarding 4 key factors. J. Prosthodont. 2018, 27, 791–797. [Google Scholar] [CrossRef]
- Afshari, F.S.; Yuan, J.C.; Quimby, A.; Harlow, R.; Campbell, S.D.; Sukotjo, C. Advanced predoctoral implant program at UIC: Description and qualitative analysis. J. Dent. Educ. 2014, 78, 770–778. [Google Scholar] [CrossRef]
- Rogers, L. Developing simulations in multi-user virtual environments to enhance healthcare education. Br. J. Educ. Technol. 2011, 42, 608–615. [Google Scholar] [CrossRef]
- Hu-Au, E.; Lee, J.J. Virtual reality in education: A tool for learning in the experience age. Int. J. Innov. Educ. 2017, 4, 215–226. [Google Scholar] [CrossRef]
- Delialioglu, O. Student engagement in blended learning environments with lecture-based and problem-based instructional approaches. J. Educ. Technol. Soc. 2012, 15, 310–322. [Google Scholar]
- Bailenson, J.N.; Yee, N.; Blascovich, J.; Beall, A.C.; Lundblad, N.; Jin, M. The use of immersive virtual reality in the learning sciences: Digital transformations of teachers, students and social context. J. Learn. Sci. 2008, 17, 102–141. [Google Scholar] [CrossRef]
- Dalgarno, B.; Lee, M.J.W. What are the learning affordances of 3-D virtual environments? Br. J. Educ. Technol. 2009, 40, 10–32. [Google Scholar] [CrossRef]
- Gamage, V.; Tretiakov, A.; Crump, B. Teacher perceptions of learning affordances of multi-user virtual environments. Comput. Educ. 2011, 57, 2406–2413. [Google Scholar] [CrossRef]
- Pantelidis, V.S. Reasons to use virtual reality in education and training courses and a model to determine when to use virtual reality. Themes Sci. Technol. Educ. 2009, 2, 59–70. [Google Scholar]
- Lorenzo, C.-M.; Ángel Sicilia, M.; Sánchez, S. Studying the effectiveness of multi-user immersive environments for collaborative evaluation tasks. Comput. Educ. 2012, 59, 1361–1376. [Google Scholar] [CrossRef]


| Pre Mean ± SD | Post Mean ± SD | |
|---|---|---|
| I found this “VR” application very interesting. | 4.3 ± 0.5 | 5.0 ± 0.0 |
| I think the use of “VR” has aided my learning of implant surgical placement. | 3.9 ± 0.7 | 4.6 ± 0.5 |
| I think I would prefer traditional lectures over use of the “VR” in class. | 3.0 ± 0.8 | 2.9 ± 1.3 |
| I believe that the “VR” should be used without any classroom discussion. | 2.3 ± 0.5 | 2.6 ± 0.5 |
| I think the use of the “VR” encouraged me to actively participate more in class. | 3.3 ± 0.5 | 4.3 ± 0.8 |
| I am very interested to use the “VR” outside of class. | 4.0 ± 0.0 | 4.9 ± 0.4 |
| I think the “VR” helped me develop my three-dimensional visualization skills (ability to visualize three-dimensional shapes). | 3.3 ± 0.5 | 4.6 ± 0.8 |
| I benefitted from the imagery and visualizations of implant surgical placement that the “VR” provides. | 3.7 ± 0.8 | 4.9 ± 0.4 |
| I think use of the “VR” improved my enthusiasm and motivation toward learning. | 3.6 ± 0.5 | 4.7 ± 0.5 |
| I think the “VR” provided easier access to learning materials than traditional lectures and textbooks. | 3.4 ± 0.5 | 4.4 ± 1.0 |
| I think the “VR” helped me to prepare for clinical applications of implant surgical placement. | 3.6 ± 0.5 | 4.7 ± 0.5 |
| I think I can use the “VR” as supplement to the traditional lectures. | 3.9 ± 0.4 | 4.9 ± 0.4 |
| I think the “VR” can provide outstanding visualization that isn’t possible in the traditional classroom. | 3.9 ± 0.7 | 4.9 ± 0.4 |
| I think the “VR” increases students’ engagement via an immersive experience. | 4.0 ± 0.0 | 4.9 ± 0.4 |
| I think the “VR” can enhance my education through “learning by doing it”. | 4.1 ± 0.4 | 4.7 ± 0.5 |
| I think this “VR” application will increase the confidence of surgical trainees before they perform a real surgery in the operating room. | 4.0 ± 0.6 | 4.9 ± 0.4 |
| I want to see more implant treatment procedures developed into VR procedures. | 4.1 ± 0.9 | 5.0 ± 0.0 |
| I think the “VR” can improve the quality of implant education in general. | 4.1 ± 0.4 | 4.9 ± 0.4 |
| Mean ± SD | |
|---|---|
| I found the headset comfortable to wear throughout the application usage. | 4.3 ± 0.5 |
| I found the quality of the audio to be excellent. | 4.0 ± 0.6 |
| I found the quality of the images to be excellent. | 4.1 ± 0.7 |
| I could interact with the user interfaces as I expected. | 4.3 ± 0.5 |
| I could touch the virtual objects appropriately. | 4.6 ± 0.5 |
| I could not tract my hands in the application accurately. | 1.9 ± 0.7 |
| I did not experience nausea, dizziness, or headache using this “VR” application. | 3.6 ± 1.3 |
| It was comfortable to use the “VR” surgery application. | 4.4 ± 0.5 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sukotjo, C.; Schreiber, S.; Li, J.; Zhang, M.; Chia-Chun Yuan, J.; Santoso, M. Development and Student Perception of Virtual Reality for Implant Surgery. Educ. Sci. 2021, 11, 176. https://doi.org/10.3390/educsci11040176
Sukotjo C, Schreiber S, Li J, Zhang M, Chia-Chun Yuan J, Santoso M. Development and Student Perception of Virtual Reality for Implant Surgery. Education Sciences. 2021; 11(4):176. https://doi.org/10.3390/educsci11040176
Chicago/Turabian StyleSukotjo, Cortino, Stephanie Schreiber, Jingyao Li, Menghan Zhang, Judy Chia-Chun Yuan, and Markus Santoso. 2021. "Development and Student Perception of Virtual Reality for Implant Surgery" Education Sciences 11, no. 4: 176. https://doi.org/10.3390/educsci11040176
APA StyleSukotjo, C., Schreiber, S., Li, J., Zhang, M., Chia-Chun Yuan, J., & Santoso, M. (2021). Development and Student Perception of Virtual Reality for Implant Surgery. Education Sciences, 11(4), 176. https://doi.org/10.3390/educsci11040176







