Smart Device Development for Gait Monitoring: Multimodal Feedback in an Interactive Foot Orthosis, Walking Aid, and Mobile Application
Abstract
1. Introduction
- SRQ1 (System Feasibility): How accurately does the developed SFO measure plantar pressure and gait parameters compared to a clinical reference system, as a foundation for reliable real-time multimodal feedback?
- SRQ2 (Application Usability): How do users evaluate the usability of the accompanying mobile application for interpreting gait and pressure information within the integrated system?
- MRQ (Feedback Evaluation): How do different vibrotactile feedback types (continuous vs. pattern-based), delivered through the orthosis and the walking aid, influence user perception in terms of noticeability, intrusiveness, perceived usefulness, and intended use?
2. Related Work
2.1. Smart Footwear for Mobile Gait Analysis and Monitoring Health Parameters
2.2. Foot Augmentation with Multimodal Feedback for Patient Device Interaction
2.3. Smart Walking Aids and Applied Sensor Technologies
2.4. Research Gap
3. Method
3.1. System Overview
3.2. Hardware Architecture and Concept Development
3.2.1. Smart Orthosis
3.2.2. Smart Walking Aid
3.3. Software Architecture and Data Processing
3.3.1. Smart Orthosis—Mobile Gait Analysis
3.3.2. Smart Walking Aid—Haptic Feedback and Motion Data
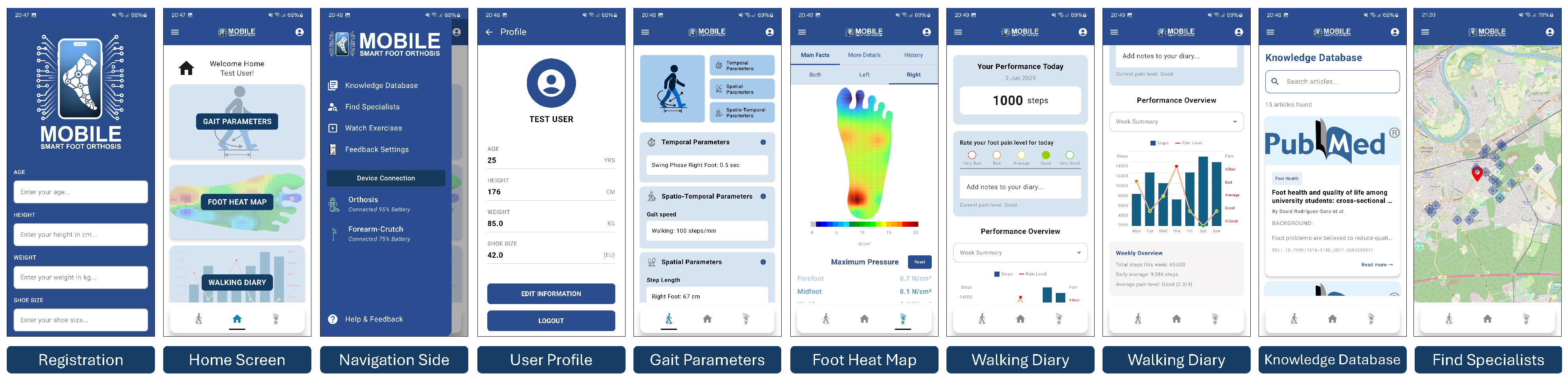
3.3.3. Smartphone Application
3.4. Prototype Validation Study: Experimental Setup
- System Feasibility: Validation of the SFO plantar pressure and spatial/temporal gait data against an instrumented treadmill.
- Application Usability: User experience evaluation of the smartphone app based on the System Usability Scale (SUS) [105].
- Feedback Evaluation: Assessment of two feedback mechanisms applied within the SFO and forearm crutch using a customized questionnaire.
3.4.1. Study Design
3.4.2. Apparatus
3.4.3. Procedure and Tasks
3.4.4. Measurement and Data Analysis
System Feasibility: Accuracy of Plantar Pressure and Gait Parameters (Smart Orthosis)
Application Usability: Evaluation of Smartphone App Usability
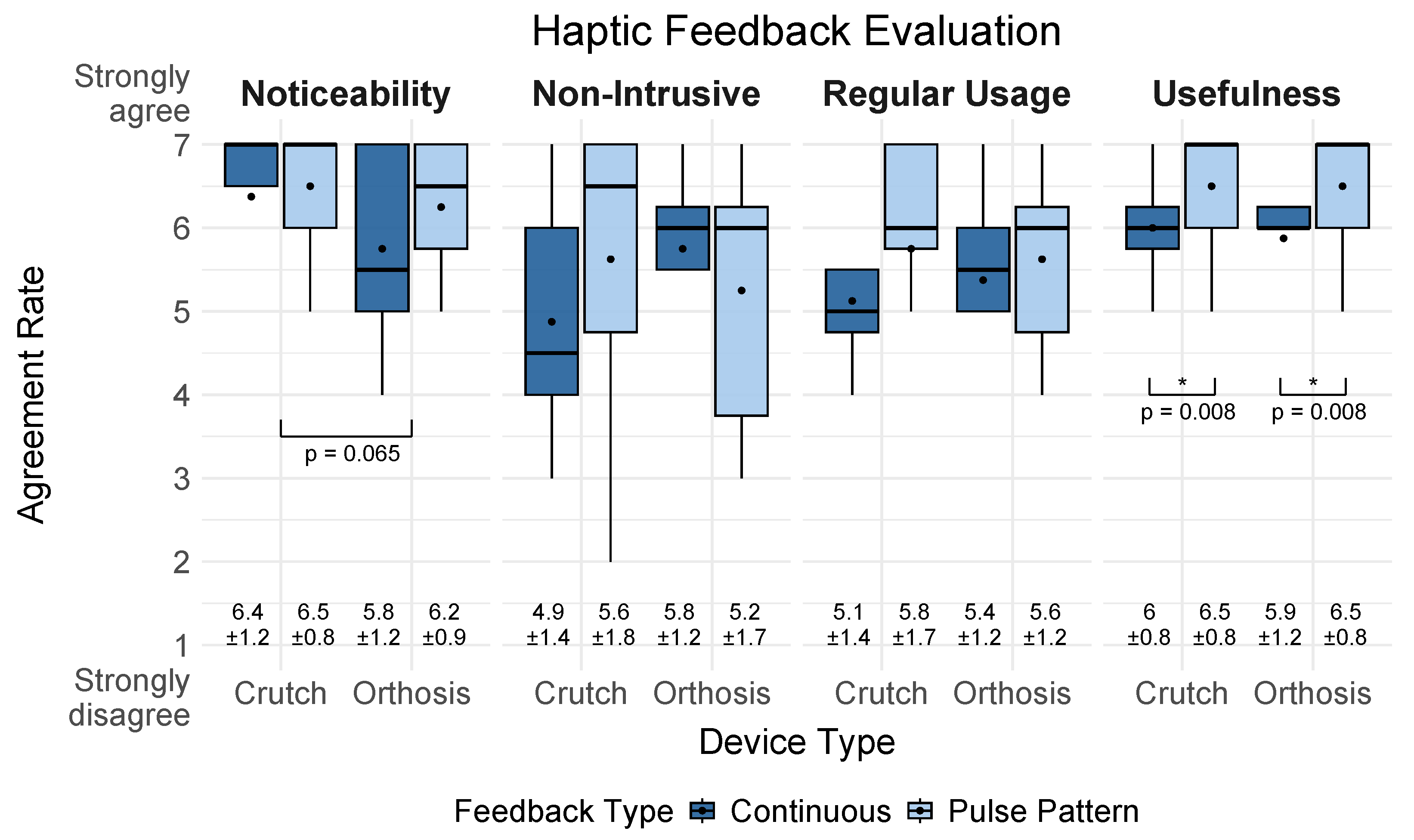
Feedback Evaluation: User Perception of Haptic Feedback (Orthosis and Walking Aid)
- Noticeability: “The haptic feedback was clearly noticeable during use.”
- Non-Intrusiveness “I found the feedback comfortable and non-intrusive.”
- Regular Usage “I could imagine using such feedback during everyday mobility tasks.”
- Usefulness “The feedback would be useful in real-life situations (e.g., alerting me of incorrect foot placement or walking posture).”
3.5. Participants
- Footwear size: European shoe size between 38 and 43.
- Current or past foot-related conditions, including either acute or chronic conditions
- Current or previous use of foot-related orthopedic products, such as shoe insoles, foot orthoses, bandages, or foot casts.
- Right foot affected or bilateral condition (but not solely left foot), as the sensor insole was configured specifically for the right foot.
4. Results
4.1. System Feasibility: Accuracy of Plantar Pressure and Gait Parameters (Smart Orthosis)
4.1.1. Gait Data Measurement
Temporal Parameters
Spatial Parameters
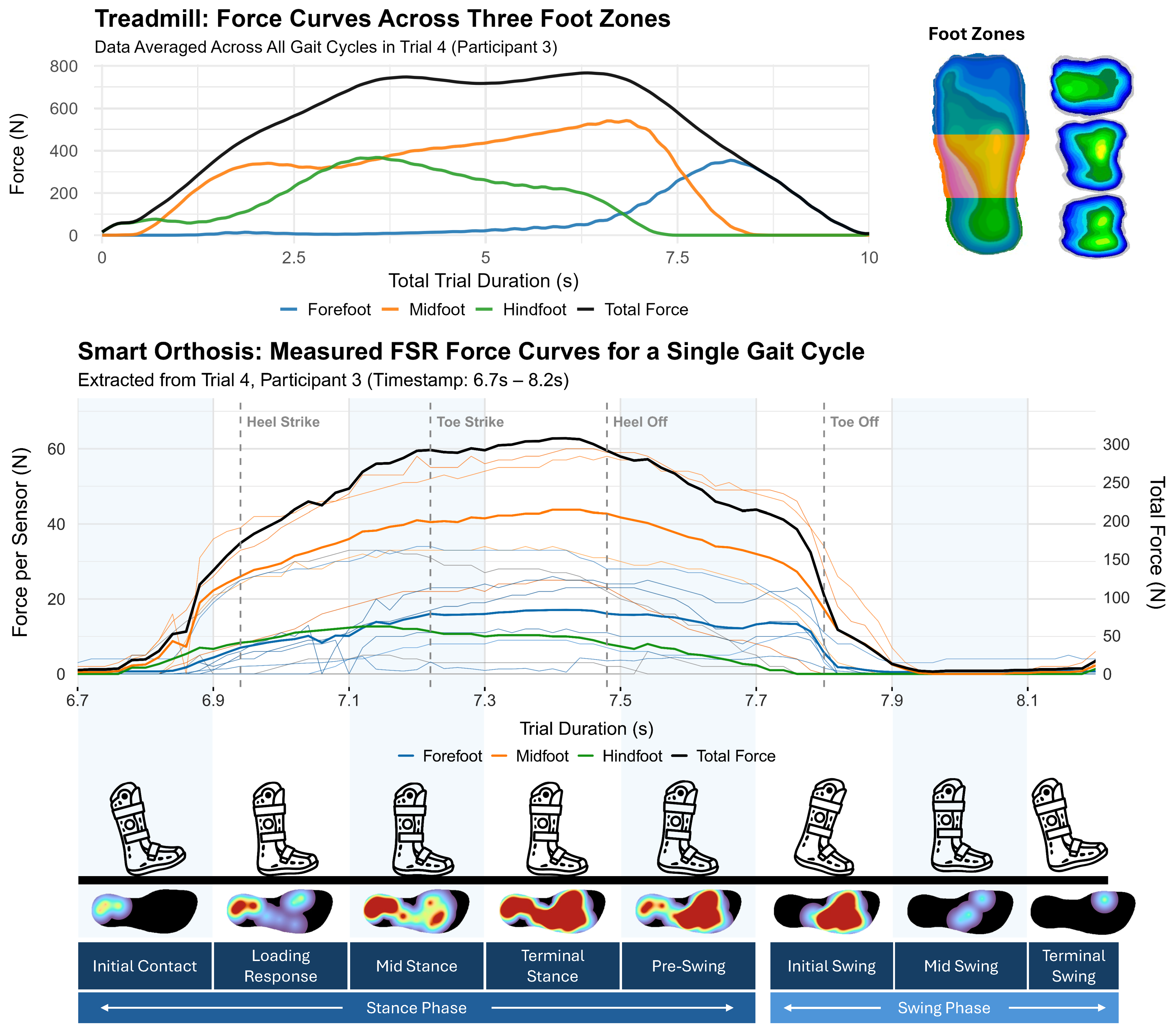
4.1.2. Pressure Data Measurement
4.2. Application Usability: Evaluation of Smartphone App Usability
4.3. Feedback Evaluation: User Perception of Haptic Feedback (Smart Orthosis and Walking Aid)
4.3.1. Correlation of Ratings Across Devices
4.3.2. Post-Experiment Questionnaire
5. Discussion
5.1. System Feasibility and Application Usability
5.1.1. System Feasibility: Accuracy of Plantar Pressure and Gait Parameters (SRQ1)
5.1.2. Application Usability: Evaluation of Smartphone App Usability (SRQ2)
5.2. Feedback Evaluation: User Perception of Haptic Feedback (MRQ)
5.3. Implications
5.4. Limitations
5.5. Future Work
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Software Architecture and Data Processing—Smart Orthosis
Appendix A.1. Raw Data Acquisition
Appendix A.2. Pre-Processing
Appendix A.3. Signal Processing
Appendix A.4. Sensor Fusion
Appendix A.5. Extraction of Gait Parameters
- Pressure variability: Temporal fluctuations in total plantar pressure across all FSR channels.
- Anterior-posterior pressure ratio: Relative distribution of pressure between forefoot and rearfoot regions.
References
- Barbara, A.M.; Grobelna, A. Orthopedic Footwear for People with Lower-Limb Conditions. Can. J. Health Technol. 2022, 2, 1–42. [Google Scholar] [CrossRef]
- Bertrand, K.; Raymond, M.H.; Miller, W.C.; Ginis, K.A.M.; Demers, L. Walking aids for enabling activity and participation: A systematic review. Am. J. Phys. Med. Rehabil. 2017, 96, 894–903. [Google Scholar] [CrossRef]
- Burns, J.; Wegener, C.; Begg, L.; Vicaretti, M.; Fletcher, J. Randomized trial of custom orthoses and footwear on foot pain and plantar pressure in diabetic peripheral arterial disease. Diabet. Med. 2009, 26, 893–899. [Google Scholar] [CrossRef]
- de Jong, L.A.; Kerkum, Y.L.; Altmann, V.C.; Geurts, A.C.; Keijsers, N.L. Orthopedic footwear has a positive influence on gait adaptability in individuals with hereditary motor and sensory neuropathy. Gait Posture 2023, 106, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Arch, E.S.; Stanhope, S.J. Orthotic Device Research. In Full Stride: Advancing the State of the Art in Lower Extremity Gait Systems; Springer: New York, NY, USA, 2017; pp. 99–116. [Google Scholar] [CrossRef]
- Resch, S.; Carroll, A. Influence of Virtual Footwear on Gait Behavior, Embodiment, and Workload While Walking on a Treadmill in Virtual Reality. In Proceedings of the 2025 31st ACM Symposium on Virtual Reality Software and Technology, Montreal, QC, Canada, 12–14 November 2025; VRST ‘25. [Google Scholar] [CrossRef]
- Salis, F.; Bertuletti, S.; Bonci, T.; Caruso, M.; Scott, K.; Alcock, L.; Buckley, E.; Gazit, E.; Hansen, C.; Schwickert, L.; et al. A multi-sensor wearable system for the assessment of diseased gait in real-world conditions. Front. Bioeng. Biotechnol. 2023, 11, 1143248. [Google Scholar] [CrossRef]
- Almuteb, I.; Hua, R.; Wang, Y. Smart insoles review (2008–2021): Applications, potentials, and future. Smart Health 2022, 25, 100301. [Google Scholar] [CrossRef]
- Okoduwa, S.I.; Igiri, B.E.; Tagang, J.I.; Okoduwa, U.J.; Adeyi, A.O. Therapeutic smart-footwear approach for management of neuropathic diabetic foot ulcers: Current challenges and focus for future perspective. Med. Nov. Technol. Devices 2024, 23, 100311. [Google Scholar] [CrossRef]
- Hutabarat, Y.; Owaki, D.; Hayashibe, M. Recent Advances in Quantitative Gait Analysis Using Wearable Sensors: A Review. IEEE Sens. J. 2021, 21, 26470–26487. [Google Scholar] [CrossRef]
- Kim, H.; Kang, Y.; Valencia, D.R.; Kim, D. An integrated system for gait analysis using FSRs and an IMU. In Proceedings of the 2018 Second IEEE International Conference on Robotic Computing (IRC), Laguna Hills, CA, USA, 31 January–2 February 2018; pp. 347–351. [Google Scholar] [CrossRef]
- Grech, J.; Mizzi, S.; Falzon, O. A technical review of foot temperature measurement systems. J. Am. Podiatr. Med. Assoc. 2022, 112, 21–65. [Google Scholar] [CrossRef]
- Frykberg, R.G.; Lavery, L.A.; Pham, H.; Harvey, C.; Harkless, L.; Veves, A. Role of neuropathy and high foot pressures in diabetic foot ulceration. Diabetes Care 1998, 21, 1714–1719. [Google Scholar] [CrossRef]
- Subramaniam, S.; Majumder, S.; Faisal, A.I.; Deen, M.J. Insole-based systems for health monitoring: Current solutions and research challenges. Sensors 2022, 22, 438. [Google Scholar] [CrossRef]
- Resch, S.; Röll, A.; Malech, A.; Schwind, V.; Sanchez-Morillo, D.; Völz, D. Walking aid with haptic feedback for combined use with a smart foot orthosis. Gerontechnology 2024, 23, 2. [Google Scholar] [CrossRef]
- Alam, U.; Riley, D.R.; Jugdey, R.S.; Azmi, S.; Rajbhandari, S.; D’Août, K.; Malik, R.A. Diabetic neuropathy and gait: A review. Diabetes Ther. 2017, 8, 1253–1264. [Google Scholar] [CrossRef] [PubMed]
- Rogers, L.C.; Frykberg, R.G.; Armstrong, D.G.; Boulton, A.J.; Edmonds, M.; Van, G.H.; Hartemann, A.; Game, F.; Jeffcoate, W.; Jirkovska, A.; et al. The Charcot foot in diabetes. J. Am. Podiatr. Med. Assoc. 2011, 101, 437–446. [Google Scholar] [CrossRef]
- Finco, M.G.; Cay, G.; Lee, M.; Garcia, J.; Salazar, E.; Tan, T.W.; Armstrong, D.G.; Najafi, B. Taking a Load Off: User Perceptions of Smart Offloading Walkers for Diabetic Foot Ulcers Using the Technology Acceptance Model. Sensors 2023, 23, 2768. [Google Scholar] [CrossRef]
- Park, C.; Mishra, R.; Vigano, D.; Macagno, M.; Rossotti, S.; D’Huyvetter, K.; Garcia, J.; Armstrong, D.G.; Najafi, B. Smart offloading boot system for remote patient monitoring: Toward adherence reinforcement and proper physical activity prescription for diabetic foot ulcer patients. J. Diabetes Sci. Technol. 2023, 17, 42–51. [Google Scholar] [CrossRef]
- Zhou, C.; Yang, L.; Liao, H.; Liang, B.; Ye, X. Ankle foot motion recognition based on wireless wearable sEMG and acceleration sensors for smart AFO. Sens. Actuators A Phys. 2021, 331, 113025. [Google Scholar] [CrossRef]
- Najafi, B.; Mohseni, H.; Grewal, G.S.; Talal, T.K.; Menzies, R.A.; Armstrong, D.G. An optical-fiber-based smart textile (smart socks) to manage biomechanical risk factors associated with diabetic foot amputation. J. Diabetes Sci. Technol. 2017, 11, 668–677. [Google Scholar] [CrossRef]
- Isezaki, T.; Kadone, H.; Niijima, A.; Aoki, R.; Watanabe, T.; Kimura, T.; Suzuki, K. Sock-Type Wearable Sensor for Estimating Lower Leg Muscle Activity Using Distal EMG Signals. Sensors 2019, 19, 1954. [Google Scholar] [CrossRef]
- Zhang, Z.; He, T.; Zhu, M.; Sun, Z.; Shi, Q.; Zhu, J.; Dong, B.; Yuce, M.R.; Lee, C. Deep learning-enabled triboelectric smart socks for IoT-based gait analysis and VR applications. npj Flex. Electron. 2020, 4, 29. [Google Scholar] [CrossRef]
- Drăgulinescu, A.; Drăgulinescu, A.M.; Zincă, G.; Bucur, D.; Feieș, V.; Neagu, D.M. Smart socks and in-shoe systems: State-of-the-art for two popular technologies for foot motion analysis, sports, and medical applications. Sensors 2020, 20, 4316. [Google Scholar] [CrossRef]
- Semjonova, G.; Davidovica, A.; Kozlovskis, N.; Okss, A.; Katashevs, A. Smart Textile Sock System for Athletes’ Self-Correction during Functional Tasks: Formative Usability Evaluation. Sensors 2022, 22, 4779. [Google Scholar] [CrossRef] [PubMed]
- Morley, R.; Richter, E.; Klaesner, J.; Maluf, K.; Mueller, M. In-shoe multisensory data acquisition system. IEEE Trans. Biomed. Eng. 2001, 48, 815–820. [Google Scholar] [CrossRef]
- Eskofier, B.M.; Lee, S.I.; Baron, M.; Simon, A.; Martindale, C.F.; Gaßner, H.; Klucken, J. An overview of smart shoes in the internet of health things: Gait and mobility assessment in health promotion and disease monitoring. Appl. Sci. 2017, 7, 986. [Google Scholar] [CrossRef]
- Sunarya, U.; Sun Hariyani, Y.; Cho, T.; Roh, J.; Hyeong, J.; Sohn, I.; Kim, S.; Park, C. Feature analysis of smart shoe sensors for classification of gait patterns. Sensors 2020, 20, 6253. [Google Scholar] [CrossRef] [PubMed]
- Gokalgandhi, D.; Kamdar, L.; Shah, N.; Mehendale, N. A review of smart technologies embedded in shoes. J. Med. Syst. 2020, 44, 150. [Google Scholar] [CrossRef] [PubMed]
- Ullrich, M.; Kuderle, A.; Hannink, J.; Din, S.D.; Gasner, H.; Marxreiter, F.; Klucken, J.; Eskofier, B.M.; Kluge, F. Detection of Gait from Continuous Inertial Sensor Data Using Harmonic Frequencies. IEEE J. Biomed. Health Inform. 2020, 24, 1869–1878. [Google Scholar] [CrossRef] [PubMed]
- Lin, F.; Wang, A.; Zhuang, Y.; Tomita, M.R.; Xu, W. Smart insole: A wearable sensor device for unobtrusive gait monitoring in daily life. IEEE Trans. Ind. Inform. 2016, 12, 2281–2291. [Google Scholar] [CrossRef]
- Xu, W.; Huang, M.C.; Amini, N.; Liu, J.J.; He, L.; Sarrafzadeh, M. Smart insole: A wearable system for gait analysis. In Proceedings of the 5th International Conference on Pervasive Technologies Related to Assistive Environments, Heraklion, Crete, Greece, 6–8 June 2012; pp. 1–4. [Google Scholar] [CrossRef]
- Duong, T.T.; Goldman, S.; Zhang, H.; Salazar, R.; Beenders, S.; Cornett, K.M.; Bain, J.M.; Montes, J.; Zanotto, D. Validation of Insole-based Gait Analysis System in Young Children with a Neurodevelopmental Disorder and Autism Traits. In Proceedings of the IEEE RAS and EMBS International Conference on Biomedical Robotics and Biomechatronics, New York, NY, USA, 29 November–1 December 2020; pp. 715–720. [Google Scholar] [CrossRef]
- Shefa, F.R.; Sifat, F.H.; Shah, S.C.; Kibria, M.G. IoT-Based Smart Ankle-Foot Orthosis for Patients with Gait Imbalance. In Proceedings of the International Conference on Control, Automation and Systems, Yeosu, Republic of Korea, 17–20 October 2023; pp. 969–974. [Google Scholar] [CrossRef]
- Shefa, F.R.; Sifat, F.H.; Uddin, J.; Ahmad, Z.; Kim, J.M.; Kibria, M.G. Deep Learning and IoT-Based Ankle–Foot Orthosis for Enhanced Gait Optimization. Healthcare 2024, 12, 2273. [Google Scholar] [CrossRef]
- Han, P.; Wang, K.; Yan, C.; Wang, L. Design and Experimental Research of an Intelligent Ankle-Foot Orthosis System for Strephenopodia. In Proceedings of the 2023 4th International Symposium on Artificial Intelligence for Medicine Science, Chengdu, China, 20–22 October 2023; ISAIMS ’23, pp. 985–991. [Google Scholar] [CrossRef]
- Mustufa, Y.S.; Barton, J.; O’Flynn, B.; Davies, R.; McCullagh, P.; Zheng, H. Design of a smart insole for ambulatory assessment of gait. In Proceedings of the 2015 IEEE 12th International Conference on Wearable and Implantable Body Sensor Networks, BSN 2015, Cambridge, MA, USA, 9–12 June 2015. [Google Scholar] [CrossRef]
- Roth, N.; Martindale, C.F.; Gaßner, H.; Kohl, Z.; Klucken, J.; Eskofer, B.M. Synchronized sensor insoles for clinical gait analysis in home-monitoring applications. Curr. Dir. Biomed. Eng. 2018, 4, 433–437. [Google Scholar] [CrossRef]
- Farid, L.; Jacobs, D.; Santos, J.D.; Simon, O.; Gracies, J.M.; Hutin, E. FeetMe® Monitor-connected insoles are a valid and reliable alternative for the evaluation of gait speed after stroke. Top. Stroke Rehabil. 2021, 28, 127–134. [Google Scholar] [CrossRef]
- Chen, D.; Asaeikheybari, G.; Chen, H.; Xu, W.; Huang, M.C. Ubiquitous Fall Hazard Identification with Smart Insole. IEEE J. Biomed. Health Inform. 2021, 25, 2768–2776. [Google Scholar] [CrossRef] [PubMed]
- D’arco, L.; Mccalmont, G.; Wang, H.; Zheng, H. Application of Smart Insoles for Recognition of Activities of Daily Living: A Systematic Review. ACM Trans. Comput. Healthc. 2024, 5, 1–34. [Google Scholar] [CrossRef]
- Djamaa, B.; Bessa, M.M.; Diaf, B.; Rouigueb, A.; Yachir, A. BoostSole: Design and Realization of a Smart Insole for Automatic Human Gait Classification. In Proceedings of the 2020 Federated Conference on Computer Science and Information Systems, FedCSIS 2020, Sofia, Bulgaria, 6–9 September 2020; pp. 35–43. [Google Scholar] [CrossRef]
- Razak, A.H.A.; Zayegh, A.; Begg, R.K.; Wahab, Y. Foot Plantar Pressure Measurement System: A Review. Sensors 2012, 12, 9884–9912. [Google Scholar] [CrossRef] [PubMed]
- Shu, L.; Hua, T.; Wang, Y.; Li, Q.; Feng, D.D.; Tao, X. In-Shoe Plantar Pressure Measurement and Analysis System Based on Fabric Pressure Sensing Array. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 767–775. [Google Scholar] [CrossRef]
- Senanayake, C.M.; Senanayake, S.M.N.A. Computational Intelligent Gait-Phase Detection System to Identify Pathological Gait. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 1173–1179. [Google Scholar] [CrossRef] [PubMed]
- Gujarathi, T.; Bhole, K. GAIT ANALYSIS USING IMU SENSOR. In Proceedings of the 2019 10th International Conference on Computing, Communication and Networking Technologies, ICCCNT 2019, Kanpur, India, 6–8 July 2019. [Google Scholar] [CrossRef]
- Aggarwal, A.; Gupta, R.; Agarwal, R. Design and Development of Integrated Insole System for Gait Analysis. In Proceedings of the 2018 11th International Conference on Contemporary Computing, IC3 2018, Noida, India, 2–4 August 2018. [Google Scholar] [CrossRef]
- Sabatini, A.M.; Martelloni, C.; Scapellato, S.; Cavallo, F. Assessment of walking features from foot inertial sensing. IEEE Trans. Biomed. Eng. 2005, 52, 486–494. [Google Scholar] [CrossRef]
- Küderle, A.; Roth, N.; Zlatanovic, J.; Zrenner, M.; Eskofier, B.; Kluge, F. The placement of foot-mounted IMU sensors does affect the accuracy of spatial parameters during regular walking. PLoS ONE 2022, 17, e0269567. [Google Scholar] [CrossRef]
- Zhang, Z.; Poslad, S. Improved use of foot force sensors and mobile phone GPS for mobility activity recognition. IEEE Sens. J. 2014, 14, 4340–4347. [Google Scholar] [CrossRef]
- Matijevich, E.; Minty, E.; Bray, E.; Bachus, C.; Hajizadeh, M.; Liden, B. A Multi-Faceted Digital Health Solution for Monitoring and Managing Diabetic Foot Ulcer Risk: A Case Series. Sensors 2024, 24, 2675. [Google Scholar] [CrossRef]
- Hong, S.; Park, K.S. Unobtrusive photoplethysmographic monitoring under the foot sole while in a standing posture. Sensors 2018, 18, 3239. [Google Scholar] [CrossRef] [PubMed]
- Joseph, A.M.; Kian, A.; Begg, R. State-of-the-Art Review on Wearable Obstacle Detection Systems Developed for Assistive Technologies and Footwear. Sensors 2023, 23, 2802. [Google Scholar] [CrossRef] [PubMed]
- Manna, S.K.; Azhar, M.A.H.B.; Greace, A. Optimal locations and computational frameworks of FSR and IMU sensors for measuring gait abnormalities. Heliyon 2023, 9, e15210. [Google Scholar] [CrossRef] [PubMed]
- Prasanth, H.; Caban, M.; Keller, U.; Courtine, G.; Ijspeert, A.; Vallery, H.; von Zitzewitz, J. Wearable Sensor-Based Real-Time Gait Detection: A Systematic Review. Sensors 2021, 21, 2727. [Google Scholar] [CrossRef]
- Han, Y.C.; Wong, K.I.; Murray, I. Gait Phase Detection for Normal and Abnormal Gaits Using IMU. IEEE Sens. J. 2019, 19, 3439–3448. [Google Scholar] [CrossRef]
- Manupibul, U.; Tanthuwapathom, R.; Jarumethitanont, W.; Kaimuk, P.; Limroongreungrat, W.; Charoensuk, W. Integration of force and IMU sensors for developing low-cost portable gait measurement system in lower extremities. Sci. Rep. 2023, 13, 10653. [Google Scholar] [CrossRef]
- Benocci, M.; Rocchi, L.; Farella, E.; Chiari, L.; Benini, L. A wireless system for gait and posture analysis based on pressure insoles and inertial measurement units. In Proceedings of the 3rd International Conference on Pervasive Computing Technologies for Healthcare-Pervasive Health 2009, London, UK, 1–3 April 2009. [Google Scholar] [CrossRef]
- Jakob, V.; Küderle, A.; Kluge, F.; Klucken, J.; Eskofier, B.M.; Winkler, J.; Winterholler, M.; Gassner, H. Validation of a Sensor-Based Gait Analysis System with a Gold-Standard Motion Capture System in Patients with Parkinson’s Disease. Sensors 2021, 21, 7680. [Google Scholar] [CrossRef]
- Donath, L.; Faude, O.; Lichtenstein, E.; Nuesch, C.; Mündermann, A. Validity and reliability of a portable gait analysis system for measuring spatiotemporal gait characteristics: Comparison to an instrumented treadmill. J. Neuroeng. Rehabil. 2016, 13, 6. [Google Scholar] [CrossRef] [PubMed]
- Jagos, H.; Pils, K.; Haller, M.; Wassermann, C.; Chhatwal, C.; Rafolt, D.; Rattay, F. Mobile gait analysis via eSHOEs instrumented shoe insoles: A pilot study for validation against the gold standard GAITRite®. J. Med. Eng. Technol. 2017, 41, 375–386. [Google Scholar] [CrossRef]
- Raghuvanshi, A.; Mitra, P.; Rane, D.; Kumar, S.D.; Lahiri, U. GaitWEAR: An Augmented Wearable System for Gait Quantification. IEEE Sens. J. 2024, 24, 35673–35685. [Google Scholar] [CrossRef]
- Santos, V.M.; Gomes, B.B.; Neto, M.A.; Amaro, A.M. A Systematic Review of Insole Sensor Technology: Recent Studies and Future Directions. Appl. Sci. 2024, 14, 6085. [Google Scholar] [CrossRef]
- Saboor, A.; Kask, T.; Kuusik, A.; Alam, M.M.; Moullec, Y.L.; Niazi, I.K.; Zoha, A.; Ahmad, R. Latest research trends in gait analysis using wearable sensors and machine learning: A systematic review. IEEE Access 2020, 8, 167830–167864. [Google Scholar] [CrossRef]
- Resch, S.; Zoufal, K.; Akhouaji, I.; Abbou, M.A.; Schwind, V.; Völz, D. Augmented Smart Insoles-Prototyping a Mobile Application: Usage Preferences of Healthcare Professionals and People with Foot Deformities. Curr. Dir. Biomed. Eng. 2023, 9, 698–701. [Google Scholar] [CrossRef]
- Resch, S.; Zimmermann, L.; Kunkel, A.; Gerstung, D.; Schwind, V.; Völz, D.; Sanchez-Morillo, D. Usability Evaluation of a Mobile Application for Foot Health Monitoring of Smart Insoles: A Mixed Methods Study. In Proceedings of the MobileHCI 2024 Adjunct Proceedings-Publication of the 26th International Conference on Mobile Human-Computer Interaction, Melbourne, VIC, Australia, 30 September–3 October 2024; 2024. [Google Scholar] [CrossRef]
- Crea, S.; Cipriani, C.; Donati, M.; Carrozza, M.C.; Vitiello, N. Providing Time-Discrete Gait Information by Wearable Feedback Apparatus for Lower-Limb Amputees: Usability and Functional Validation. IEEE Trans. Neural Syst. Rehabil. Eng. 2015, 23, 250–257. [Google Scholar] [CrossRef] [PubMed]
- Oates, A.R.; Hauck, L.; Moraes, R.; Sibley, K.M. The effects of haptic input on biomechanical and neurophysiological parameters of walking: A scoping review. Gait Posture 2017, 58, 232–239. [Google Scholar] [CrossRef] [PubMed]
- Berengueres, J.; Fritschi, M.; McClanahan, R. A smart pressure-sensitive insole that reminds you to walk correctly: An orthotic-less treatment for over pronation. In Proceedings of the 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, EMBC 2014, Chicago, IL, USA, 26–30 August 2014; pp. 2488–2491. [Google Scholar] [CrossRef]
- Biesmans, S.; Markopoulos, P. Design and Evaluation of SONIS, a Wearable Biofeedback System for Gait Retraining. Multimodal Technol. Interact. 2020, 4, 60. [Google Scholar] [CrossRef]
- Pacilli, A.; Mileti, I.; Germanotta, M.; Di Sipio, E.; Imbimbo, I.; Aprile, I.; Padua, L.; Rossi, S.; Palermo, E.; Cappa, P. A wearable setup for auditory cued gait analysis in patients with Parkinson’s Disease. In Proceedings of the 2016 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Benevento, Italy, 15–18 May 2016; pp. 1–6. [Google Scholar] [CrossRef]
- Ma, C.C.; Wei, S.Y.; Lin, J.H. Smart footwear feedback interface analysis and design. In Proceedings of the 2015 International Conference on Computational Science and Computational Intelligence, CSCI 2015, Las Vegas, NV, USA, 7–9 December 2015; pp. 766–770. [Google Scholar] [CrossRef]
- Redd, C.B.; Bamberg, S.J. A wireless sensory feedback device for real-time gait feedback and training. IEEE/ASME Trans. Mechatronics 2012, 17, 425–433. [Google Scholar] [CrossRef]
- Elvitigala, D.S.; Matthies, D.J.; David, L.; Weerasinghe, C.; Nanayakkara, S. GymSoles: Improving Squats and Dead-Lifts by Visualizing the User’s Center of Pressure. In Proceedings of the 2019 CHI Conference on Human Factors in Computing Systems, New York, NY, USA, 4–9 May 2019; CHI ’19, pp. 1–12. [Google Scholar] [CrossRef]
- Yan, Q.; Huang, J.; Tao, C.; Chen, X.; Xu, W.X. Intelligent mobile walking-aids: Perception, control and safety. Adv. Robot. 2020, 34, 2–18. [Google Scholar] [CrossRef]
- Resch, S.; Zirari, A.; Tran, T.D.Q.; Bauer, L.M.; Sanchez-Morillo, D. Smart Walking Aids with Sensor Technology for Gait Support and Health Monitoring: A Scoping Review. Technologies 2025, 13, 346. [Google Scholar] [CrossRef]
- Srinivasan, S.; Rajesh, M. Smart walking stick. In Proceedings of the International Conference on Trends in Electronics and Informatics, ICOEI 2019, Tirunelveli, India, 23–25 April 2019; pp. 576–579. [Google Scholar] [CrossRef]
- Yang, Z.; Gao, M.; Choi, J. Smart walking cane based on triboelectric nanogenerators for assisting the visually impaired. Nano Energy 2024, 124, 109485. [Google Scholar] [CrossRef]
- Chamorro-Moriana, G.; Sevillano, J.L.; Ridao-Fernández, C. A Compact Forearm Crutch Based on Force Sensors for Aided Gait: Reliability and Validity. Sensors 2016, 16, 925. [Google Scholar] [CrossRef]
- Shah, M.M.; Khan, M.N.R.; Khan, M.R.A.; Plabon, M.M.H.; Razzak, M.A. A Cost-Effective Smart Walking Stick for Visually Impaired People. In Proceedings of the 6th International Conference on Communication and Electronics Systems, ICCES 2021, Coimbatre, India, 8–10 July 2021; pp. 1582–1585. [Google Scholar] [CrossRef]
- Bansal, M.; Malik, S.; Kumar, M.; Meena, N. Arduino based Smart Walking Cane for Visually Impaired People. In Proceedings of the 4th International Conference on Inventive Systems and Control, ICISC 2020, Coimbatore, India, 8–10 January 2020; pp. 462–465. [Google Scholar] [CrossRef]
- Ikbal, M.A.; Rahman, F.; Kabir, M.H. Microcontroller based smart walking stick for visually impaired people. In Proceedings of the 4th International Conference on Electrical Engineering and Information and Communication Technology, iCEEiCT 2018, Dhaka, Bangladesh, 13–15 September 2018; pp. 255–259. [Google Scholar] [CrossRef]
- Gallo, S.; Chapuis, D.; Santos-Carreras, L.; Kim, Y.; Retornaz, P.; Bleuler, H.; Gassert, R. Augmented white cane with multimodal haptic feedback. In Proceedings of the 2010 3rd IEEE RAS and EMBS International Conference on Biomedical Robotics and Biomechatronics, BioRob 2010, Tokyo, Japan, 26–29 September 2010; pp. 149–155. [Google Scholar] [CrossRef]
- Di, P.; Hasegawa, Y.; Nakagawa, S.; Sekiyama, K.; Fukuda, T.; Huang, J.; Huang, Q. Fall Detection and Prevention Control Using Walking-Aid Cane Robot. IEEE/ASME Trans. Mechatron. 2016, 21, 625–637. [Google Scholar] [CrossRef]
- Tsuda, N.; Hayashi, A.; Tounai, M.; Akutagawa, S. Visualization system of crutch walking based on internal sensors. In Proceedings of the IEEE/ASME International Conference on Advanced Intelligent Mechatronics, AIM, Montreal, QC, Canada, 6–9 July 2010; pp. 19–24. [Google Scholar] [CrossRef]
- Trujillo-León, A.; de Guzmán-Manzano, A.; Velázquez, R.; Vidal-Verdú, F. Generation of gait events with a fsr based cane handle. Sensors 2021, 21, 5632. [Google Scholar] [CrossRef]
- Murali, S.; Shrivatsan, R.; Sreenivas, V.; Vijjappu, S.; Gladwin, S.J.; Rajavel, R. Smart walking cane for the visually challenged. In Proceedings of the IEEE Region 10 Humanitarian Technology Conference 2016, R10-HTC 2016-Proceedings, Agra, India, 21–23 December 2016. [Google Scholar] [CrossRef]
- Merrett, G.V.; Ettabib, M.A.; Peters, C.; Hallett, G.; White, N.M. Augmenting forearm crutches with wireless sensors for lower limb rehabilitation. Meas. Sci. Technol. 2010, 21, 124008. [Google Scholar] [CrossRef]
- Schuster, E.; Routson, R.L.; Hinchcliff, M.; Benoff, K.; Suri, P.; Richburg, C.; Muir, B.C.; Czerniecki, J.M.; Aubin, P.M. A novel walking cane with haptic biofeedback reduces knee adduction moment in the osteoarthritic knee. J. Biomech. 2021, 114, 110150. [Google Scholar] [CrossRef] [PubMed]
- Mohapatra, S.; Rout, S.H.; Tripathi, V.; Saxena, T.; Karuna, Y. Smart Walking Stick for Blind Integrated with SOS Navigation System. In Proceedings of the 2nd International Conference on Trends in Electronics and Informatics, ICOEI 2018, Tirunelveli, India, 11–12 May 2018; pp. 441–447. [Google Scholar] [CrossRef]
- Suman, S.; Mishra, S.; Sahoo, K.S.; Nayyar, A. Vision navigator: A smart and intelligent obstacle recognition model for visually impaired users. Mob. Inf. Syst. 2022, 2022, 9715891. [Google Scholar] [CrossRef]
- Lancini, M.; Serpelloni, M.; Pasinetti, S.; Guanziroli, E. Healthcare Sensor System Exploiting Instrumented Crutches for Force Measurement during Assisted Gait of Exoskeleton Users. IEEE Sens. J. 2016, 16, 8228–8237. [Google Scholar] [CrossRef]
- Enovis. AIRCAST® AIRSELECT™ Elite Walker. Available online: https://www.enovis-medtech.de/AIRCAST-AIRSELECT-Elite-Walker (accessed on 15 August 2025).
- ISO 11334-1:2007; Assistive Products for Walking Manipulated by One Arm—Requirements and Test Methods—Part 1: Elbow Crutches. Deutsches Institut für Normung e.V. (DIN): Berlin, Germany, 2007. [CrossRef]
- Interlink Electronics. FSR® 400 Short. Available online: https://www.interlinkelectronics.com/fsr-400-short (accessed on 15 August 2025).
- Interlink Electronics. FSR® Integration Guide; Interlink Electronics: Camarillo, CA, USA, 2013. [Google Scholar]
- Bosch Sensortec GmbH. Small. Low Power. Optimized for Wearables—Inertial Measurement Unit: BMI270. Available online: https://www.bosch-sensortec.com/products/motion-sensors/imus/bmi270/ (accessed on 15 August 2025).
- Bosch Sensortec GmbH. BMI270 Datasheet, revision 1.5 ed.; Bosch Sensortec GmbH: Reutlingen, Germany, 2023. [Google Scholar]
- Ballesteros, J.; Tudela, A.; Caro-Romero, J.R.; Urdiales, C. A cane-based low cost sensor to implement attention mechanisms in telecare robots. In Proceedings of the 2019 International Conference on Robotics and Automation (ICRA), Montreal, QC, Canada, 20–24 May 2019; pp. 1473–1478. [Google Scholar] [CrossRef]
- Mariani, B.; Rouhani, H.; Crevoisier, X.; Aminian, K. Quantitative estimation of foot-flat and stance phase of gait using foot-worn inertial sensors. Gait Posture 2013, 37, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Sardini, E.; Serpelloni, M.; Lancini, M. Wireless Instrumented Crutches for Force and Movement Measurements for Gait Monitoring. IEEE Trans. Instrum. Meas. 2015, 64, 3369–3379. [Google Scholar] [CrossRef]
- Mikhailov, A. Turbo, An Improved Rainbow Colormap for Visualization. Google. 2019. Available online: https://research.google/blog/turbo-an-improved-rainbow-colormap-for-visualization/ (accessed on 15 August 2025).
- Android Studio. Android Studio–The Official IDE for Android Development. Available online: https://developer.android.com/studio (accessed on 15 August 2025).
- Developers. Build Better Apps Faster with Jetpack Compose. Available online: https://developer.android.com/compose (accessed on 15 August 2025).
- Brooke, J. SUS-A Quick and Dirty Usability Scale. In Usability Evaluation in Industry; CRC Press: Boca Raton, FL, USA, 1996; Volume 189, pp. 4–7. [Google Scholar]
- Schwind, V.; Resch, S.; Sehrt, J. The HCI User Studies Toolkit: Supporting Study Designing and Planning for Undergraduates and Novice Researchers in Human-Computer Interaction. In Proceedings of the Extended Abstracts of the 2023 CHI Conference on Human Factors in Computing Systems, New York, NY, USA, 23–28 April 2023; CHI EA ’23. [Google Scholar] [CrossRef]
- Kassambara, A. rstatix: Pipe-Friendly Framework for Basic Statistical Tests, R Package Version 0.7.2. 2023. Available online: https://rpkgs.datanovia.com/rstatix/ (accessed on 15 August 2025).
- Likert, R. A technique for the measurement of attitudes. Arch. Psychol. 1932, 140, 1–55. [Google Scholar]
- Bangor, A.; Kortum, P.; Miller, J. Determining what individual SUS scores mean: Adding an adjective rating scale. J. Usability Stud. 2009, 4, 114–123. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Routledge: London, UK, 2013. [Google Scholar]
- Ganguly, A.; Olmanson, B.A.; Knowlton, C.B.; Wimmer, M.A.; Ferrigno, C. Accuracy of the fully integrated Insole3’s estimates of spatiotemporal parameters during walking. Med. Eng. Phys. 2023, 111, 103925. [Google Scholar] [CrossRef]
- Hyzy, M.; Bond, R.; Mulvenna, M.; Bai, L.; Dix, A.; Leigh, S.; Hunt, S. System Usability Scale Benchmarking for Digital Health Apps: Meta-analysis. JMIR mHealth uHealth 2022, 10, e37290. [Google Scholar] [CrossRef] [PubMed]
- Alzghoul, B. The Effectiveness of Gamification in Changing Health-related Behaviors: A Systematic Review and Meta-analysis. Open Public Health J. 2024, 17. [Google Scholar] [CrossRef]
- Gurari, N.; Smith, K.; Madhav, M.; Okamura, A.M. Environment discrimination with vibration feedback to the foot, arm, and fingertip. In Proceedings of the 2009 IEEE International Conference on Rehabilitation Robotics, Kyoto, Japan, 23–26 June 2009; pp. 343–348. [Google Scholar] [CrossRef]
- Choi, S.; Kuchenbecker, K.J. Vibrotactile Display: Perception, Technology, and Applications. Proc. IEEE 2013, 101, 2093–2104. [Google Scholar] [CrossRef]
- Nikodelis, T.; Moscha, D.; Metaxiotis, D.; Kollias, I. Commercial video frame rates can produce reliable results for both normal and CP spastic gait’s spatiotemporal, angular, and linear displacement variables. J. Appl. Biomech. 2011, 27, 266–271. [Google Scholar] [CrossRef]
- Santos, J.P.; Ferreira, J.P.; Crisóstomo, M.; Paulo Coimbra, A. Instrumented Shoes for 3D GRF Analysis and Characterization of Human Gait. In Proceedings of the Bioinformatics and Biomedical Engineering: 7th International Work-Conference, IWBBIO 2019, Granada, Spain, 8–10 May 2019; Proceedings, Part II 7. Springer: Berlin/Heidelberg, Germany, 2019; pp. 51–62. [Google Scholar]
- Majumder, S.; Deen, M.J. Wearable IMU-based system for real-time monitoring of lower-limb joints. IEEE Sens. J. 2020, 21, 8267–8275. [Google Scholar] [CrossRef]
- Kalman, R.E. A new approach to linear filtering and prediction problems. J. Basic Eng. 1960, 82, 35–45. [Google Scholar] [CrossRef]
- Shankar, P.S.U.; Raveendranathan, N.; Gans, N.R.; Jafari, R. Towards power optimized kalman filter for gait assessment using wearable sensors. In Proceedings-Wireless Health 2010; Association for Computing Machinery: New York, NY, USA, 2010; pp. 137–144. [Google Scholar] [CrossRef]
- Bennett, T.; Jafari, R.; Gans, N. An extended Kalman filter to estimate human gait parameters and walking distance. In Proceedings of the American Control Conference, Washington, DC, USA, 17–19 June 2013; pp. 752–757. [Google Scholar] [CrossRef]
- Mahony, R.; Hamel, T.; Pflimlin, J.M. Nonlinear Complementary Filters on the Special Orthogonal Group. IEEE Trans. Autom. Control 2008, 53, 1203–1218. [Google Scholar] [CrossRef]
- SensorFusion: A Simple Implementation of Some Complex Sensor Fusion Algorithms. 2023. GitHub Repository. Available online: https://github.com/aster94/SensorFusion (accessed on 5 July 2025).
- Skog, I.; Handel, P.; Nilsson, J.O.; Rantakokko, J. Zero-Velocity Detection—An Algorithm Evaluation. IEEE Trans. Biomed. Eng. 2010, 57, 2657–2666. [Google Scholar] [CrossRef]
- Perry, J.; Burnfield, J.M.; Cabico, L.M. Gait Analysis: Normal and Pathological Function. J. Sport. Sci. Med. 2010, 9, 353. [Google Scholar]
- Lovecchio, N.; Zago, M.; Sforza, C. Gait Analysis in the Rehabilitation Process. In Rehabilitation After Limb Salvage Surgery; Springer International Publishing: Cham, Switzerland, 2021; pp. 109–118. [Google Scholar] [CrossRef]







| Parameter Type | Parameter | Unit |
|---|---|---|
| Temporal | Stance Duration | s |
| Swing Duration | s | |
| Cycle Duration | s | |
| Spatial | Stride/Cycle Length | m |
| Kinetic | Mean Plantar Pressure | N/cm2 |
| Parameter Type | Parameter | Mean Accuracy | SD Accuracy |
|---|---|---|---|
| Temporal | Stance Phase Duration | 96.7% | ±3.1 |
| Swing Phase Duration | 60.3% | ±12.6 | |
| Cycle Phase Duration | 85.2% | ±1.6 | |
| Spatial | Stride/Cycle Length | 83.4% | ±13.3 |
| No. | Item | M | SD |
|---|---|---|---|
| 1 | Frequency of Use | 3.63 | 0.92 |
| 2 | Complexity * | 1.88 | 0.83 |
| 3 | Ease of Use | 4.50 | 0.53 |
| 4 | Need for Support * | 1.38 | 0.74 |
| 5 | Integration of Functions | 4.13 | 0.99 |
| 6 | Inconsistency * | 1.88 | 0.64 |
| 7 | Learnability | 4.75 | 0.46 |
| 8 | Cumbersomeness * | 1.75 | 1.04 |
| 9 | Confidence | 4.25 | 0.71 |
| 10 | Prior Learning Required * | 2.13 | 1.36 |
| ART RM ANOVA | Pairwise Comparisons (Wilcoxon) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Measure | Factor | F | Df | p | Sig. | Statistic | p | Magnitude | |||
| Noticeability | Device | 4.49 | 1, 21 | 0.046 | * | 0.176 | 25.0 | 0.065 | 0.483 | moderate | |
| Feedback | 1.80 | 1, 21 | 0.194 | 0.079 | 22.0 | 0.187 | 0.310 | moderate | |||
| Device × Feedback | 1.60 | 1, 21 | 0.220 | 0.071 | — | — | — | — | |||
| Non-Intrusiveness | Device | 0.06 | 1, 21 | 0.815 | 0.003 | 27.5 | 0.653 | 0.106 | small | ||
| Feedback | 0.50 | 1, 21 | 0.487 | 0.023 | 42.5 | 0.811 | 0.046 | small | |||
| Device × Feedback | 2.24 | 1, 21 | 0.150 | 0.096 | — | — | — | — | |||
| Regular Usage | Device | 0.00 | 1, 21 | 0.966 | 0.000 | 42.5 | 0.807 | 0.099 | small | ||
| Feedback | 2.57 | 1, 21 | 0.124 | 0.109 | 50.0 | 0.129 | 0.326 | moderate | |||
| Device × Feedback | 0.77 | 1, 21 | 0.390 | 0.035 | — | — | — | — | |||
| Usefulness | Device | 0.00 | 1, 21 | 1.000 | 0.000 | 24.5 | 0.851 | 0.076 | small | ||
| Feedback | 6.01 | 1, 21 | 0.023 | * | 0.220 | 36.0 | 0.008 | 0.703 | large | ||
| Device × Feedback | 0.00 | 1, 21 | 1.000 | 0.000 | — | — | — | — | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Resch, S.; Kousha, A.; Carroll, A.; Severinghaus, N.; Rehberg, F.; Zatschker, M.; Söyleyici, Y.; Sanchez-Morillo, D. Smart Device Development for Gait Monitoring: Multimodal Feedback in an Interactive Foot Orthosis, Walking Aid, and Mobile Application. Technologies 2025, 13, 588. https://doi.org/10.3390/technologies13120588
Resch S, Kousha A, Carroll A, Severinghaus N, Rehberg F, Zatschker M, Söyleyici Y, Sanchez-Morillo D. Smart Device Development for Gait Monitoring: Multimodal Feedback in an Interactive Foot Orthosis, Walking Aid, and Mobile Application. Technologies. 2025; 13(12):588. https://doi.org/10.3390/technologies13120588
Chicago/Turabian StyleResch, Stefan, André Kousha, Anna Carroll, Noah Severinghaus, Felix Rehberg, Marco Zatschker, Yunus Söyleyici, and Daniel Sanchez-Morillo. 2025. "Smart Device Development for Gait Monitoring: Multimodal Feedback in an Interactive Foot Orthosis, Walking Aid, and Mobile Application" Technologies 13, no. 12: 588. https://doi.org/10.3390/technologies13120588
APA StyleResch, S., Kousha, A., Carroll, A., Severinghaus, N., Rehberg, F., Zatschker, M., Söyleyici, Y., & Sanchez-Morillo, D. (2025). Smart Device Development for Gait Monitoring: Multimodal Feedback in an Interactive Foot Orthosis, Walking Aid, and Mobile Application. Technologies, 13(12), 588. https://doi.org/10.3390/technologies13120588









