Suaeda vermiculata Aqueous-Ethanolic Extract-Based Mitigation of CCl4-Induced Hepatotoxicity in Rats, and HepG-2 and HepG-2/ADR Cell-Lines-Based Cytotoxicity Evaluations
Abstract
1. Introduction
2. Results
2.1. LC-MS-Based Chemical Fingerprinting of Suaeda vermiculata aq.-Ethanolic Extract
2.2. Estimations of the Total Phenolics and Flavonoid Contents in the aq.-Ethanolic Extract, and Fractions of the aq.-Ethanolic Extract Obtained from Suaeda vermiculata
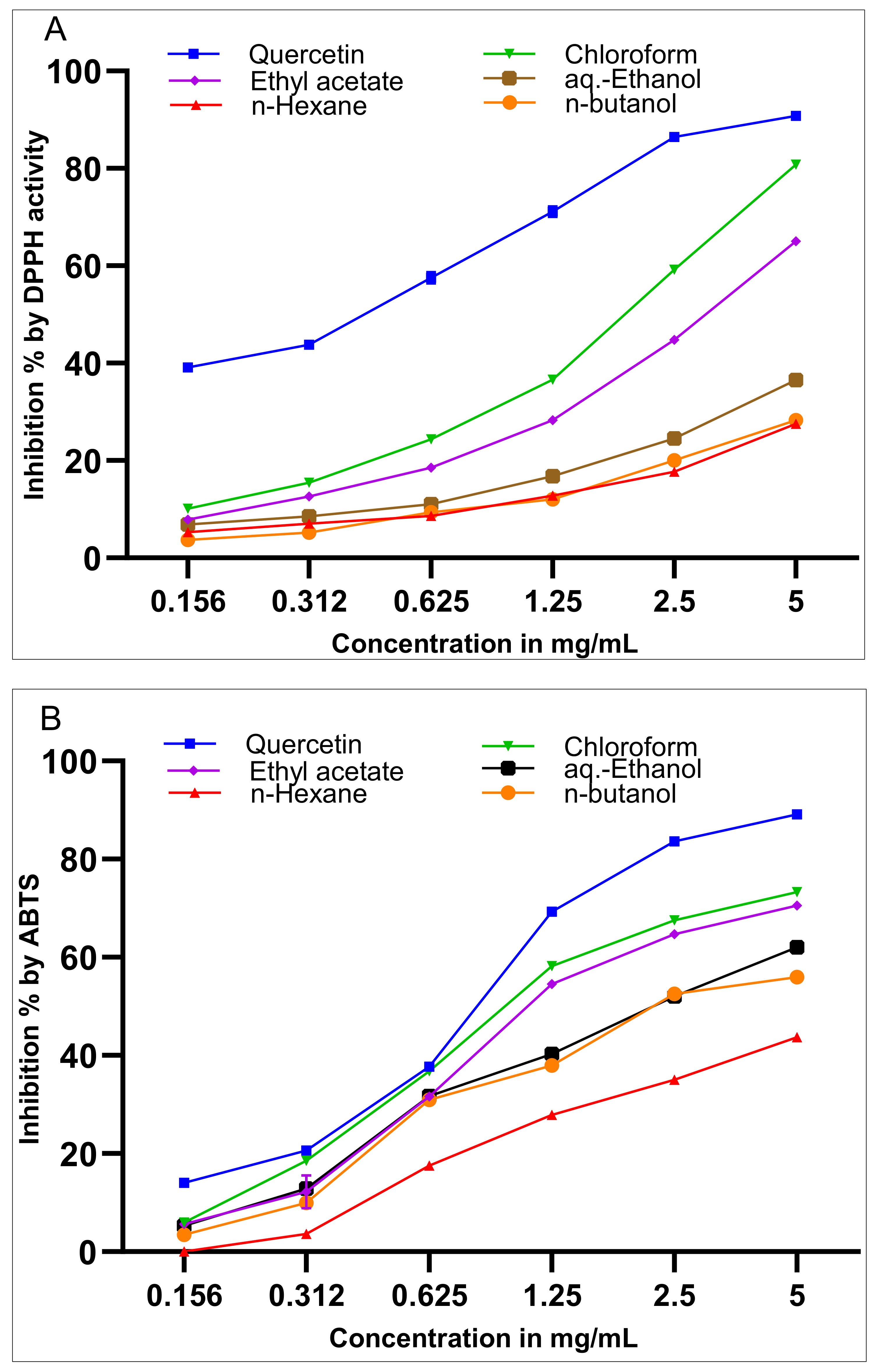
2.3. Determination of Antioxidant Potentials Through Measurement of Free-Radical Scavenging Activity
2.4. Acute Toxicity Study and Dose Selection
2.5. Safety Determination of aq.-Ethanolic Extract on Liver, Heart, and Kidney
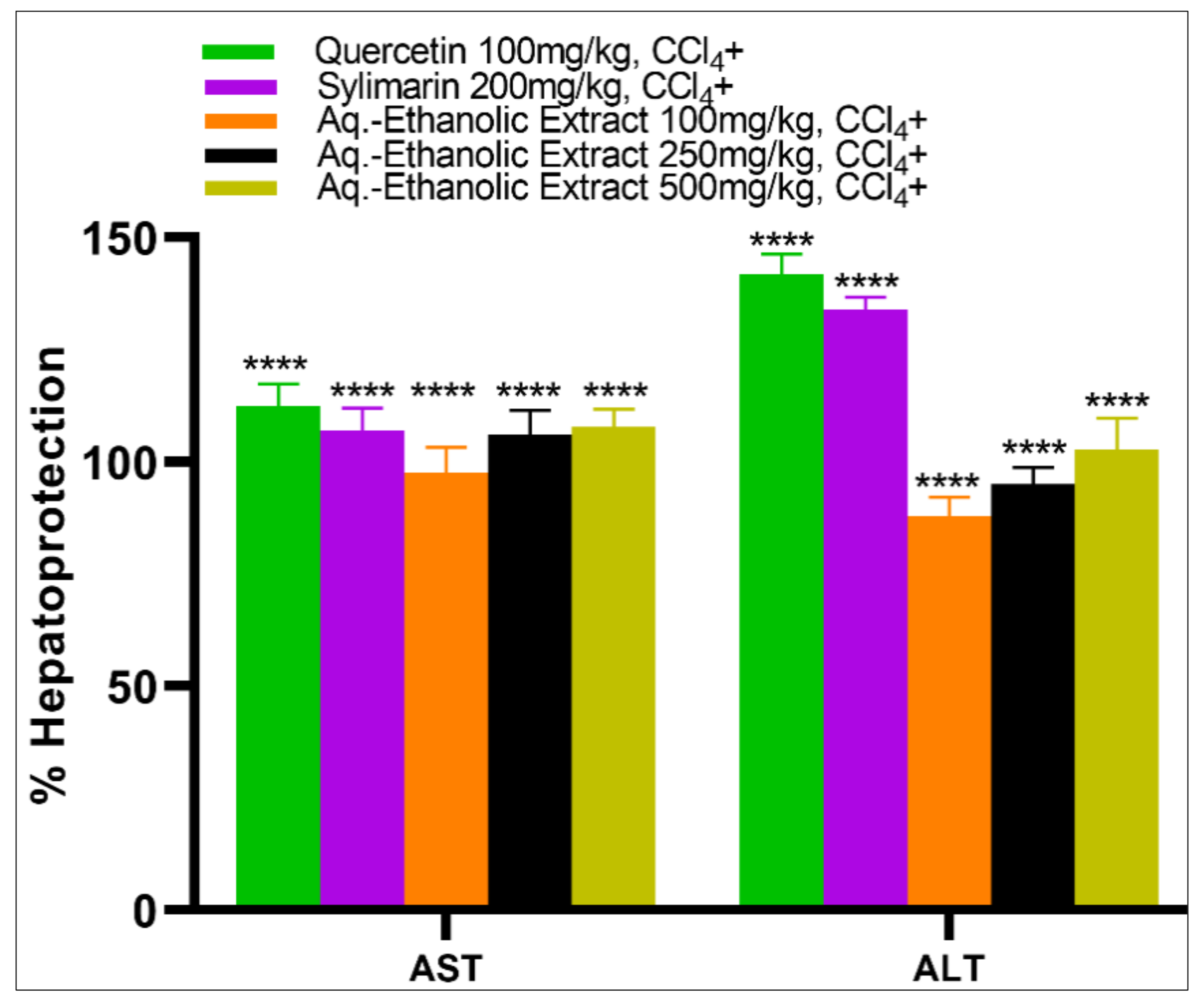
2.6. Hepatoprotective Activity of the aq.-Ethanolic Extract
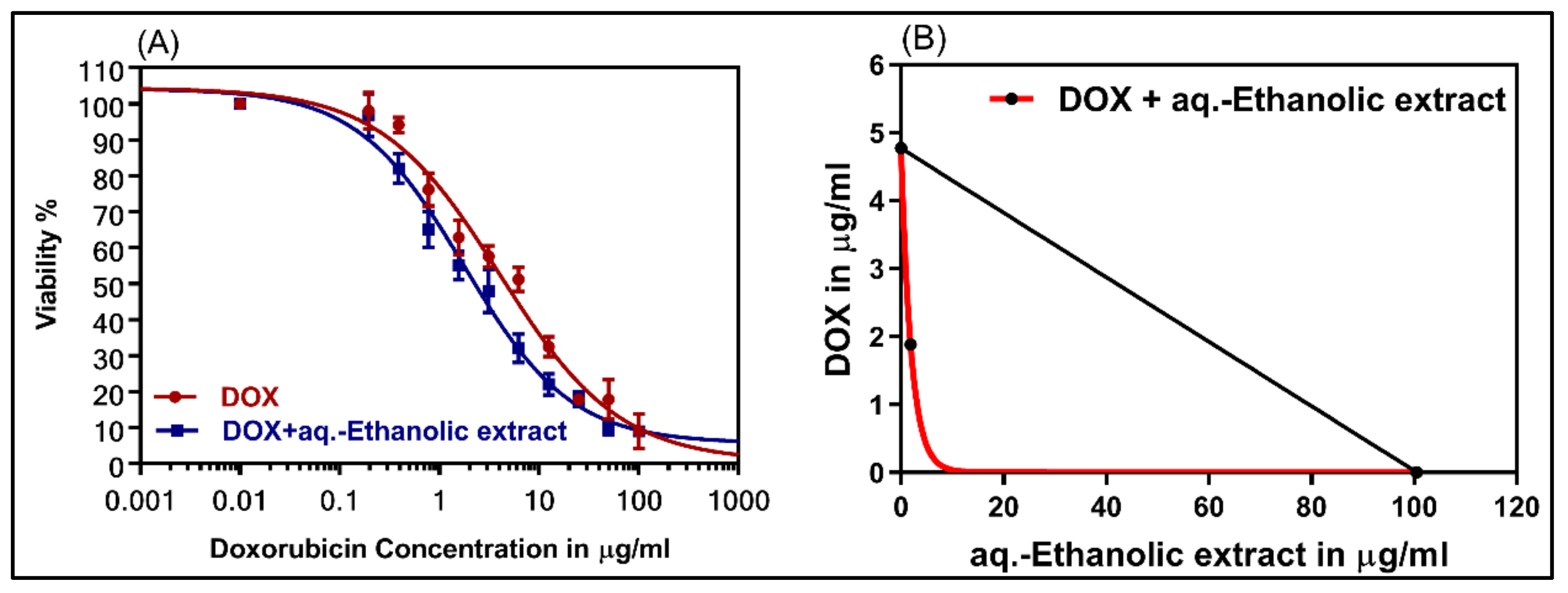
2.7. Cytotoxicity of Suaeda vermiculata Extract in Wild Type Sensitive and Resistant Hepatic Cell-Lines
2.8. Suaeda vermiculata aq.-Ethanolic Extract Reverses DOX Cytotoxicity in Resistant Hepatic Cell-Lines
3. Discussion
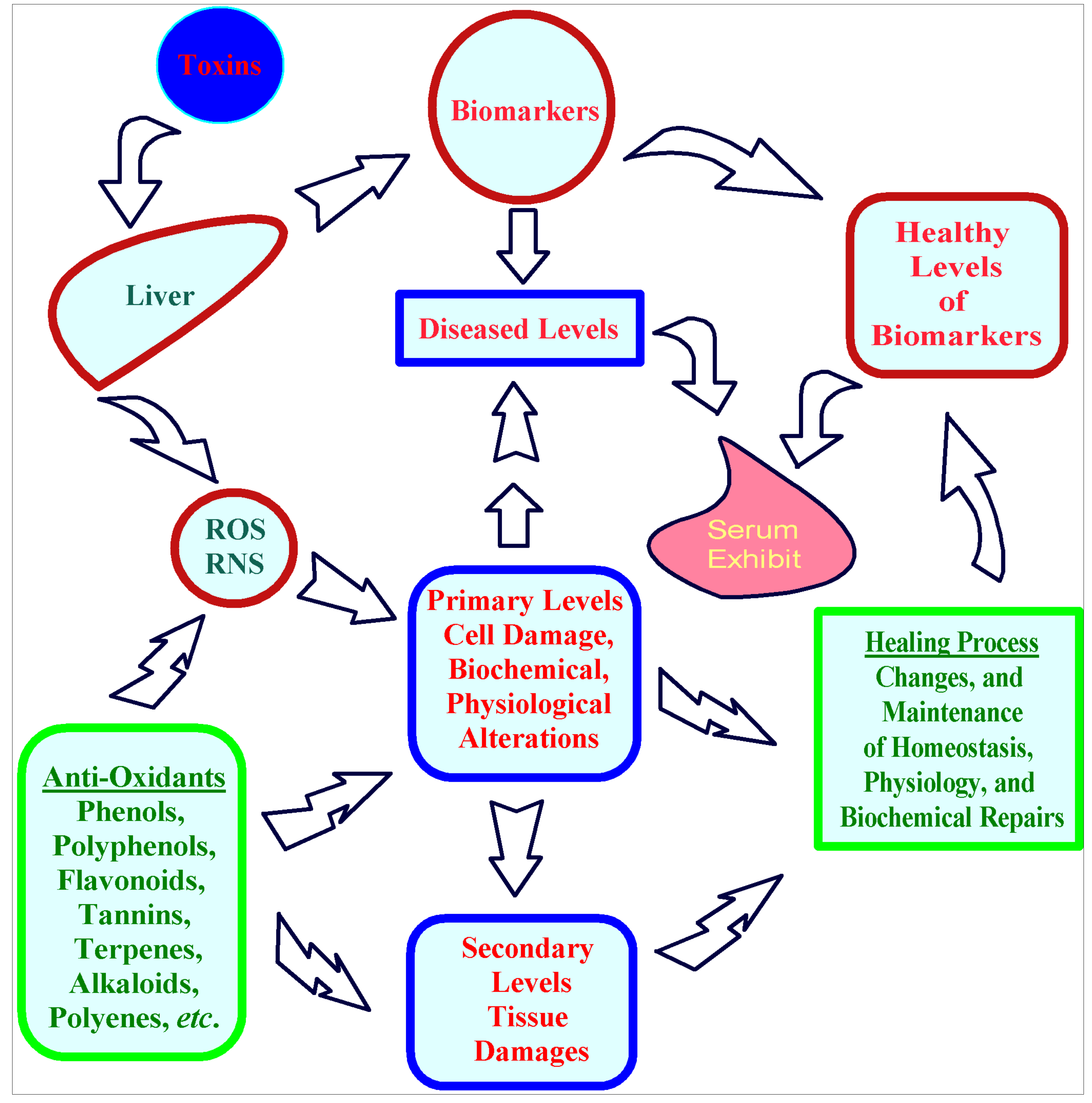
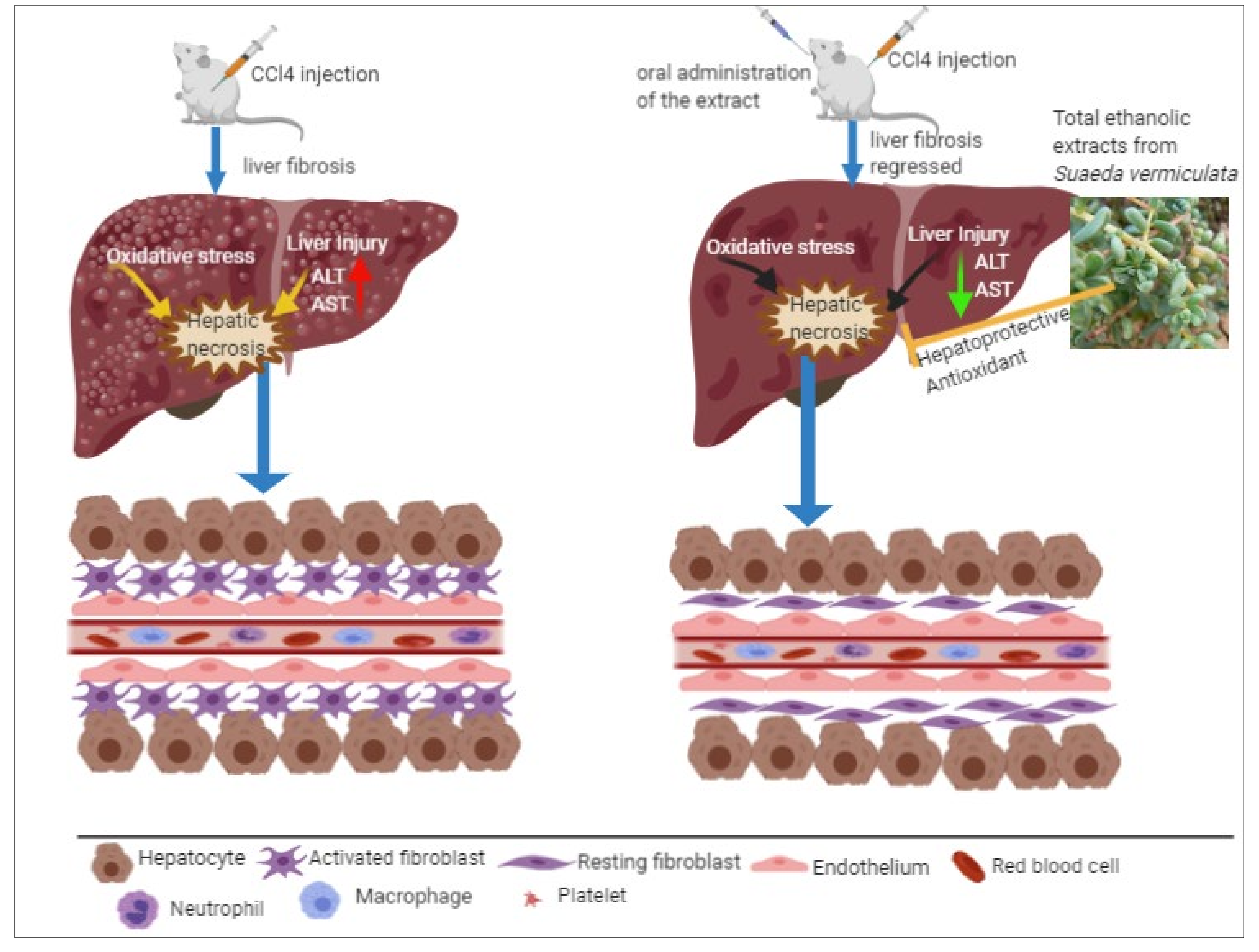
3.1. A Plausible Biomechanistic Aspect of Liver Toxicity and Its Amelioration
4. Materials and Methods
4.1. Chemicals and Reagents
4.2. Plant Material Collection and Extraction
4.3. LC-MS Experimental Design
4.3.1. High-Pressure Chromatography (HPLC): The Chemical Fingerprinting
4.3.2. Mass Spectrometer
4.4. Determination of Total Phenolic Contents
4.5. Determination of Total Flavonoid Contents
4.6. Evaluation of Free-Radical Scavenging Activity
4.6.1. DPPH Assay
4.6.2. ABTS Assay
4.7. Acute Toxicity Studies and Sample Size
4.8. Effect of aq.-Ethanolic Extract on Liver and Kidney Enzymes in Addition to Lipid and Sugar Levels
4.8.1. Experimental Animal Groups
4.8.2. Determination of Levels AST, ALT, TP, and Creatinine
4.8.3. Determination of Plasma Level of Glucose, Cholesterol, and Triglycerides
4.9. Cell-Lines
4.10. Cytotoxicity and Reversal Assay
4.11. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Asrani, S.K.; Devarbhavi, H.; Eaton, J.; Kamath, P.S. Burden of liver diseases in the world. J. Hepatol. 2019, 70, 151–171. [Google Scholar] [CrossRef] [PubMed]
- Everhart, J.E.; Ruhl, C.E. Burden of Digestive Diseases in the United States Part III: Liver, Biliary Tract, and Pancreas. Gastroenterology 2009, 136, 1134–1144. [Google Scholar] [CrossRef] [PubMed]
- Al-Anazi, M.R.; Matou-Nasri, S.; Al-Qahtani, A.A.; Alghamdi, J.; Abdo, A.A.; Sanai, F.M.; Al-Hamoudi, W.K.; Alswat, K.A.; Al-Ashgar, H.I.; Khan, M.Q.; et al. Association between IL-37 gene polymorphisms and risk of HBV-related liver disease in a Saudi Arabian population. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Al-Johani, J.J.; Aljehani, S.M.; Alzahrani, G.S. Assessment of Knowledge about Liver Cirrhosis among Saudi Population. Egypt. J. Hosp. Med. 2018, 71, 2443–2446. [Google Scholar] [CrossRef]
- Alsabaani, A.; Mahfouz, A.; Awadalla, N.; Musa, M.; Humayed, S. Al Non-Alcoholic Fatty Liver Disease among Type-2 Diabetes Mellitus Patients in Abha City, South Western Saudi Arabia. Int. J. Environ. Res. Public Health 2018, 15, 2521. [Google Scholar] [CrossRef]
- Arhoghro, E.M.; Ekpo, K.E.; Anosike, E.O.; Ibeh, G.O. Effect of Aqueous Extract of Bitter Leaf (Vernonia Amygdalina Del) on Carbon Tetrachloride (CCl4) Induced Liver Damage in Albino Wistar Rats. Eur. J. Sci. Res. 2009, 26, 122–130. [Google Scholar]
- Mohammed, H.A.; Abdel-Aziz, M.M.; Hegazy, M.M. Anti-Oral Pathogens of Tecoma stans (L.) and Cassia javanica (L.) Flower Volatile Oils in Comparison with Chlorhexidine in Accordance with Their Folk Medicinal Uses. Medicina (B. Aires). 2019, 55, 301. [Google Scholar] [CrossRef]
- Jeong, E.; Yang, M.; Kim, N.-H.; Heo, J.-D.; Sung, S. Hepatoprotective effects of Limonium tetragonum, edible medicinal halophyte growing near seashores. Pharmacogn. Mag. 2014, 10, 563. [Google Scholar] [CrossRef]
- Souid, A.; Croce, C.M.D.; Pozzo, L.; Ciardi, M.; Giorgetti, L.; Gervasi, P.G.; Abdelly, C.; Magné, C.; Hamed, K.B.; Longo, V. Antioxidant properties and hepatoprotective effect of the edible halophyte Crithmum maritimum L. against carbon tetrachloride-induced liver injury in rats. Eur. Food Res. Technol. 2020, 246, 1393–1403. [Google Scholar] [CrossRef]
- Gnanadesigan, M.; Ravikumar, S.; Inbaneson, S.J. Hepatoprotective and antioxidant properties of marine halophyte Luminetzera racemosa bark extract in {CCL}4 induced hepatotoxicity. Asian Pac. J. Trop. Med. 2011, 4, 462–465. [Google Scholar] [CrossRef]
- Modarresi, M.; Moradian, F.; Nematzadeh, G. Antioxidant responses of halophyte plant Aeluropus littoralis under long-term salinity stress. Biologia (Bratisl). 2014, 69. [Google Scholar] [CrossRef]
- Boestfleisch, C.; Papenbrock, J. Changes in secondary metabolites in the halophytic putative crop species Crithmum maritimum L., Triglochin maritima L. and Halimione portulacoides (L.) Aellen as reaction to mild salinity. PLOS ONE 2017, 12, e0176303. [Google Scholar] [CrossRef] [PubMed]
- Grigore, M.-N.; Oprica, L. Halophytes as possible source of antioxidant compounds, in a scenario based on threatened agriculture and food crisis. Iran. J. Public Health 2015, 44, 1153. [Google Scholar] [PubMed]
- Soundararajan, P.; Manivannan, A.; Jeong, B.R. Different Antioxidant Defense Systems in Halophytes and Glycophytes to Overcome Salinity Stress. In Sabkha Ecosystems; Springer International Publishing: Berlin, Germany, 2019; pp. 335–347. [Google Scholar]
- Cichoż-Lach, H. Oxidative stress as a crucial factor in liver diseases. World J. Gastroenterol. 2014, 20, 8082. [Google Scholar] [CrossRef]
- McRae, C.A.; Agarwal, K.; Mutimer, D.; Bassendine, M.F. Hepatitis associated with Chinese herbs. Eur. J. Gastroenterol. Hepatol. 2002, 14, 559–562. [Google Scholar] [CrossRef]
- Pak, E.; Esrason, K.; Wu, V. Hepatotoxicity of herbal remedies: an emerging dilemma. Prog. Transplant. 2004, 14, 91–96. [Google Scholar] [CrossRef]
- Woolbright, B.L.; Williams, C.D.; McGill, M.R.; Jaeschke, H. Liver Toxicity. In Reference Module in Biomedical Sciences; Elsevier: Amsterdam, The Netherlands, 2014. [Google Scholar]
- Masarone, M.; Rosato, V.; Dallio, M.; Gravina, A.G.; Aglitti, A.; Loguercio, C.; Federico, A.; Persico, M. Role of Oxidative Stress in Pathophysiology of Nonalcoholic Fatty Liver Disease. Oxid. Med. Cell. Longev. 2018, 2018, 1–14. [Google Scholar] [CrossRef]
- Ostapowicz, G. Results of a Prospective Study of Acute Liver Failure at 17 Tertiary Care Centers in the United States. Ann. Intern. Med. 2002, 137, 947. [Google Scholar] [CrossRef]
- Yen, F.-L.; Wu, T.-H.; Lin, L.-T.; Cham, T.-M.; Lin, C.-C. Naringenin-Loaded Nanoparticles Improve the Physicochemical Properties and the Hepatoprotective Effects of Naringenin in Orally-Administered Rats with {CCl}4-Induced Acute Liver Failure. Pharm. Res. 2008, 26, 893–902. [Google Scholar] [CrossRef]
- Chávez, E.; Reyes-Gordillo, K.; Segovia, J.; Shibayama, M.; Tsutsumi, V.; Vergara, P.; Moreno, M.G.; Muriel, P. Resveratrol prevents fibrosis, NF-kappaB activation and TGF-beta increases induced by chronic CCl4 treatment in rats. J. Appl. Toxicol. 2007, 28, 35–43. [Google Scholar] [CrossRef]
- Casas-Grajales, S. Antioxidants in liver health. World J. Gastrointest. Pharmacol. Ther. 2015, 6, 59. [Google Scholar] [CrossRef] [PubMed]
- Gillessen, A.; Schmidt, H.H.-J. Silymarin as supportive treatment in liver diseases: A narrative review. Adv. Ther. 2020, 1–23. [Google Scholar] [CrossRef] [PubMed]
- Nwidu, L.L.; Oboma, Y.I.; Elmorsy, E.; Carter, W.G. Hepatoprotective effect of hydromethanolic leaf extract of Musanga cecropioides (Urticaceae) on carbon tetrachloride-induced liver injury and oxidative stress. J. Taibah Univ. Med. Sci. 2018, 13, 344–354. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.; Zhou, Z.; Li, J.; Luo, Y.; Zhou, Y.; Ke, X.; Huang, K. {CCl}4-Induced Liver Injury Was Ameliorated by Qi-Ge Decoction through the Antioxidant Pathway. Evidence-Based Complement. Altern. Med. 2019, 2019, 1–12. [Google Scholar] [CrossRef]
- Chao, W.-W.; Chen, S.-J.; Peng, H.-C.; Liao, J.-W.; Chou, S.-T. Antioxidant Activity of Graptopetalum paraguayense E. Walther Leaf Extract Counteracts Oxidative Stress Induced by Ethanol and Carbon Tetrachloride Co-Induced Hepatotoxicity in Rats. Antioxidants 2019, 8, 251. [Google Scholar] [CrossRef]
- Nwidu, L.L.; Elmorsy, E.; Oboma, Y.I.; Carter, W.G. Hepatoprotective and antioxidant activities of Spondias mombin leaf and stem extracts against carbon tetrachloride-induced hepatotoxicity. J. Taibah Univ. Med. Sci. 2018, 13, 262–271. [Google Scholar] [CrossRef]
- Kuriakose, G.C.; Kurup, M.G. Antioxidant and antihepatotoxic effect of Spirulina laxissima against carbon tetrachloride induced hepatotoxicity in rats. Food Funct. 2011, 2, 190. [Google Scholar] [CrossRef]
- Abdou, R.H.; Basha, W.A.; Khalil, W.F. Subacute Toxicity of Nerium oleander Ethanolic Extract in Mice. Toxicol. Res. 2019, 35, 233–239. [Google Scholar] [CrossRef]
- Alhdad, G.M.; Seal, C.E.; Al-Azzawi, M.J.; Flowers, T.J. The effect of combined salinity and waterlogging on the halophyte Suaeda maritima: the role of antioxidants. Environ. Exp. Bot. 2013, 87, 120–125. [Google Scholar] [CrossRef]
- Pareek, A.; Godavarthi, A.; Issarani, R.; Nagori, B.P. Antioxidant and hepatoprotective activity of Fagonia schweinfurthii (Hadidi) Hadidi extract in carbon tetrachloride induced hepatotoxicity in {HepG}2 cell line and rats. J. Ethnopharmacol. 2013, 150, 973–981. [Google Scholar] [CrossRef]
- Dahiru, D.; Obidoa, O. Evaluation of the antioxidant effects of Ziziphus mauritiana leaf extracts against chronic ethanol-induced hepatotoxicity in rat liver. African J. Tradit. Complement. Altern. Med. 2008, 5. [Google Scholar] [CrossRef] [PubMed]
- Li, A.-N.; Li, S.; Zhang, Y.-J.; Xu, X.-R.; Chen, Y.-M.; Li, H.-B. Resources and Biological Activities of Natural Polyphenols. Nutrients 2014, 6, 6020–6047. [Google Scholar] [CrossRef] [PubMed]
- Chu, X.; Wang, H.; Jiang, Y.; Zhang, Y.; Bao, Y.; Zhang, X.; Zhang, J.; Guo, H.; Yang, F.; Luan, Y.; et al. Ameliorative effects of tannic acid on carbon tetrachloride-induced liver fibrosis in~vivo and in~vitro. J. Pharmacol. Sci. 2016, 130, 15–23. [Google Scholar] [CrossRef]
- Chen, L.; Hu, C.; Hood, M.; Kan, J.; Gan, X.; Zhang, X.; Zhang, Y.; Du, J. An Integrated Approach Exploring the Synergistic Mechanism of Herbal Pairs in a Botanical Dietary Supplement: A Case Study of a Liver Protection Health Food. Int. J. Genomics 2020, 2020, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Rasool, M.; Iqbal, J.; Malik, A.; Ramzan, H.S.; Qureshi, M.S.; Asif, M.; Qazi, M.H.; Kamal, M.A.; Chaudhary, A.G.A.; Al-Qahtani, M.H.; et al. Hepatoprotective Effects of Silybum marianum (Silymarin) and Glycyrrhiza glabra (Glycyrrhizin) in Combination: A Possible Synergy. Evidence-Based Complement. Altern. Med. 2014, 2014, 1–9. [Google Scholar] [CrossRef]
- Ming, Z.; Fan, Y.; Yang, X.; Lautt, W.W. Synergistic protection by S-adenosylmethionine with vitamins C and E on liver injury induced by thioacetamide in rats. Free Radic. Biol. Med. 2006, 40, 617–624. [Google Scholar] [CrossRef] [PubMed]
- Singh, H.; Prakash, A.; Kalia, A.N.; Majeed, A.B.A. Synergistic hepatoprotective potential of ethanolic extract of Solanum xanthocarpum and Juniperus communis against paracetamol and azithromycin induced liver injury in rats. J. Tradit. Complement. Med. 2016, 6, 370–376. [Google Scholar] [CrossRef]
- Yadav, N.P.; Pal, A.; Shanker, K.; Bawankule, D.U.; Gupta, A.K.; Darokar, M.P.; Khanuja, S.P.S. Synergistic effect of silymarin and standardized extract of Phyllanthus amarus against {CCl}4-induced hepatotoxicity in Rattus norvegicus. Phytomedicine 2008, 15, 1053–1061. [Google Scholar] [CrossRef]
- Chen, P.; Wang, Y.; Chen, L.; Jiang, W.; Niu, Y.; Shao, Q.; Gao, L.; Zhao, Q.; Yan, L.; Wang, S. Comparison of the anti-inflammatory active constituents and hepatotoxic pyrrolizidine alkaloids in two Senecio plants and their preparations by LC–UV and LC–MS. J. Pharm. Biomed. Anal. 2015, 115, 260–271. [Google Scholar] [CrossRef]
- Quirós-Guerrero, L.; Albertazzi, F.; Araya-Valverde, E.; Romero, R.M.; Villalobos, H.; Poveda, L.; Chavarría, M.; Tamayo-Castillo, G. Phenolic variation among Chamaecrista nictitans subspecies and varieties revealed through UPLC-ESI (-)-MS/MS chemical fingerprinting. Metabolomics 2019, 15, 14. [Google Scholar] [CrossRef]
- Mohammed, H.A. The Valuable Impacts of Halophytic Genus Suaeda; Nutritional, Chemical, and Biological Values. Med. Chem. 2020. [Google Scholar] [CrossRef] [PubMed]
- Hou, M.-L.; Chang, L.-W.; Lin, C.-H.; Lin, L.-C.; Tsai, T.-H. Determination of bioactive components in Chinese herbal formulae and pharmacokinetics of rhein in rats by UPLC-MS/MS. Molecules 2014, 19, 4058–4075. [Google Scholar] [CrossRef] [PubMed]
- Dai, W.; Li, H.; Cong, W.; Zhao, W.; Wang, Q. Two New Eremophilane Sesquiterpenes and One New Resorcinol from Ligularia knorringiana. Nat. Prod. Commun. 2016, 11, 1934578X1601100201. [Google Scholar] [CrossRef]
- Madan, S.; Pannakal, S.T.; Ganapaty, S.; Singh, G.N.; Kumar, Y. Phenolic glucosides from Flacourtia indica. Nat. Prod. Commun. 2009, 4, 1934578X0900400313. [Google Scholar] [CrossRef]
- n-Hexadecanoic Acid. Available online: https://webbook.nist.gov/cgi/cbook.cgi?ID=C57103&Mask=200 (accessed on 14 September 2020).
- Mohammed, H.A.; Al-Omar, M.S.; El-Readi, M.Z.; Alhowail, A.H.; Aldubayan, M.A.; Abdellatif, A.A.H. Formulation of Ethyl Cellulose Microparticles Incorporated Pheophytin A Isolated from Suaeda vermiculata for Antioxidant and Cytotoxic Activities. Molecules 2019, 24, 1501. [Google Scholar] [CrossRef] [PubMed]
- OECD. OECD Test No. 425: Acute Oral Toxicity: Up-and-Down Procedure; OECD: Paris, France, 2008. [Google Scholar]
- Jun, H.-I.; Wiesenborn, D.P.; Kim, Y.-S. Antioxidant Activity of Phenolic Compounds from Canola (Brassica napus) Seed. Food Sci. Biotechnol 2014, 23, 1753–1760. [Google Scholar] [CrossRef]
- Kaur, D.; Kaur, A.; Arora, S. Delineation of attenuation of oxidative stress and mutagenic stress by Murraya exotica L. leaves. Springerplus 2016, 5. [Google Scholar] [CrossRef] [PubMed]
- Routray, W.; Orsat, V. Microwave-assisted extraction of flavonoids: a review. Food Bioprocess Technol. 2012, 5, 409–424. [Google Scholar] [CrossRef]
- Stalikas, C.D. Extraction, separation, and detection methods for phenolic acids and flavonoids. J. Sep. Sci. 2007, 30, 3268–3295. [Google Scholar] [CrossRef]
- Mohammed, H.A.; Al-Omar, M.S.; Aly, M.S.A.; Hegazy, M.M. Essential Oil Constituents and Biological Activities of the Halophytic Plants, Suaeda Vermiculata Forssk and Salsola Cyclophylla Bakera Growing in Saudi Arabia. J. Essent. Oil Bear. Plants 2019, 1–12. [Google Scholar] [CrossRef]
- Mohammadi Motamed, S.; Bush, S.; Hosseini Rouzbahani, S.; Karimi, S.; Mohammadipour, N. Total phenolic and flavonoid contents and antioxidant activity of four medicinal plants from Hormozgan province, Iran. Res. J. Pharmacogn. 2016, 3, 17–26. [Google Scholar]
- Popoviç, M.; Kaurinoviç, B.; Jakovljeviç, V.; Mimica-Dukic, N.; Bursaç, M.; Popovic, M. PARSLEY ON OXIDATIVE STRESS 717 Effect of Parsley (Petroselinum crispum (Mill.) Nym. ex A.W. Hill, Apiaceae) Extracts on some Biochemical Parameters of Oxidative Stress in Mice treated with CCl 4. Phytother. Res 2007, 21, 717–723. [Google Scholar] [CrossRef] [PubMed]
- Hafez, M.M.; Hamed, S.S.; El-Khadragy, M.F.; Hassan, Z.K.; Al Rejaie, S.S.; Sayed-Ahmed, M.M.; Al-Harbi, N.O.; Al-Hosaini, K.A.; Al-Harbi, M.M.; Alhoshani, A.R.; et al. Effect of ginseng extract on the TGF-β1 signaling pathway in CCl4-induced liver fibrosis in rats. BMC Complement. Altern. Med. 2017, 17, 45. [Google Scholar] [CrossRef]
- Araya, E.M.; Adamu, B.A.; Periasamy, G.; Sintayehu, B.; Gebrelibanos Hiben, M. In vivo hepatoprotective and In vitro radical scavenging activities of Cucumis ficifolius A. rich root extract. J. Ethnopharmacol. 2019, 242, 112031. [Google Scholar] [CrossRef] [PubMed]
- Jabit, M.L.; Wahyuni, F.S.; Khalid, R.; Israf, D.A.; Shaari, K.; Lajis, N.H.; Stanslas, J. Cytotoxic and nitric oxide inhibitory activities of methanol extracts of Garcinia species. Pharm. Biol. 2009, 47, 1019–1026. [Google Scholar] [CrossRef]
- Li, S.; Zhao, Q.; Wang, B.; Yuan, S.; Wang, X.; Li, K. Quercetin reversed MDR in breast cancer cells through down-regulating P-gp expression and eliminating cancer stem cells mediated by YB-1 nuclear translocation. Phyther. Res. 2018, 32, 1530–1536. [Google Scholar] [CrossRef]
- Borska, S.; Chmielewska, M.; Wysocka, T.; Drag-Zalesinska, M.; Zabel, M.; Dziegiel, P. In vitro effect of quercetin on human gastric carcinoma: Targeting cancer cells death and MDR. Food Chem. Toxicol. 2012, 50, 3375–3383. [Google Scholar] [CrossRef]
- Kumar, M.; Sharma, G.; Misra, C.; Kumar, R.; Singh, B.; Katare, O.P.; Raza, K. N-desmethyl tamoxifen and quercetin-loaded multiwalled CNTs: A synergistic approach to overcome MDR in cancer cells. Mater. Sci. Eng. C 2018, 89, 274–282. [Google Scholar] [CrossRef]
- Mohana, S.; Ganesan, M.; Rajendra Prasad, N.; Ananthakrishnan, D.; Velmurugan, D. Flavonoids modulate multidrug resistance through wnt signaling in P-glycoprotein overexpressing cell lines. BMC Cancer 2018, 18, 1168. [Google Scholar] [CrossRef]
- Mohana, S.; Ganesan, M.; Agilan, B.; Karthikeyan, R.; Srithar, G.; Beaulah Mary, R.; Ananthakrishnan, D.; Velmurugan, D.; Rajendra Prasad, N.; Ambudkar, S.V. Screening dietary flavonoids for the reversal of P-glycoprotein-mediated multidrug resistance in cancer. Mol. Biosyst. 2016, 12, 2458–2470. [Google Scholar] [CrossRef]
- Qureshi, N.N.; Kuchekar, B.S.; Logade, N.A.; Haleem, M.A. Antioxidant and hepatoprotective activity of Cordia macleodii leaves. Saudi Pharm. J. 2009, 17, 299–302. [Google Scholar] [CrossRef] [PubMed]
- Delgado-Montemayor, C.; Cordero-Pérez, P.; Salazar-Aranda, R.; Waksman-Minsky, N. Models of hepatoprotective activity assessment. Med. Univ. 2015, 17, 222–228. [Google Scholar] [CrossRef]
- Ritesh, K.R.; Suganya, A.; Dileepkumar, H.V.; Rajashekar, Y.; Shivanandappa, T. A single acute hepatotoxic dose of CCl4 causes oxidative stress in the rat brain. Toxicol. Rep. 2015, 2, 891–895. [Google Scholar] [CrossRef] [PubMed]
- Hogade, M.G.; Patil, K.S.; Wadkar, G.H.; Mathapati, S.S.; Dhumal, P.B. Hepatoprotective activity of Morus alba (Linn.) leaves extract against carbon tetrachloride induced hepatotoxicity in rats. African J. Pharm. Pharmacol. 2010, 4, 731–734. [Google Scholar]
- Boll, M.; Weber, L.W.D.; Becker, E.; Stampfl, A. Mechanism of carbon tetrachloride-induced hepatotoxicity. Hepatocellular damage by reactive carbon tetrachloride metabolites. Zeitschrift Naturforsch. Sect. C J. Biosci. 2001, 56, 649–659. [Google Scholar] [CrossRef]
- Recknagel, R.O.; Glende, E.A.; Dolak, J.A.; Waller, R.L. Mechanisms of carbon tetrachloride toxicity. Pharmacol. Ther. 1989, 43, 139–154. [Google Scholar] [CrossRef]
- He, Q.; Guoming, S.; Liu, K.; Zhang, F.; Jiang, Y.; Gao, J.; Liu, L.; Jiang, Z.; Jin, M.; Xie, H. Sex-specific reference intervals of hematologic and biochemical analytes in Sprague-Dawley rats using the nonparametric rank percentile method. PLoS ONE 2017, 12, e0189837. [Google Scholar] [CrossRef]
- Sallie, R.; Michael Tredger, J.; Williams, R. Drugs and the liver part 1: Testing liver function. Biopharm. Drug Dispos. 1991, 12, 251–259. [Google Scholar] [CrossRef]
- Zhou, D.; Ruan, J.; Cai, Y.; Xiong, Z.; Fu, W.; Wei, A. Antioxidant and hepatoprotective activity of ethanol extract of Arachniodes exilis (Hance) Ching. J. Ethnopharmacol. 2010, 129, 232–237. [Google Scholar] [CrossRef]
- Alhassan, A.J.; Sule, M.J.; Aliyu, S.A.; Aliyu, M.D. Ideal hepatotoxicity model in rats using Carbon Tetrachloride (CCl4). Bayero J. Pure Appl. Sci. 2011, 2. [Google Scholar] [CrossRef]
- Singh, A.; Bhat, T.; Sharma, O. Clinical Biochemistry of Hepatotoxicity. J. Clin. Toxicol. 2011, 04. [Google Scholar] [CrossRef]
- Shaker, E.; Mahmoud, H.; Mnaa, S. Silymarin, the antioxidant component and Silybum marianum extracts prevent liver damage. Food Chem. Toxicol. 2010, 48, 803–806. [Google Scholar] [CrossRef] [PubMed]
- Shalan, M.G.; Mostafa, M.S.; Hassouna, M.M.; El-Nabi, S.E.H.; El-Refaie, A. Amelioration of lead toxicity on rat liver with Vitamin C and silymarin supplements. Toxicology 2005, 206, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Flora, K.; Hahn, M.; Rosen, H.; Benner, K. Milk thistle (Silybum marianum) for the therapy of liver disease. Am. J. Gastroenterol. 1998, 93, 139–143. [Google Scholar] [CrossRef]
- Miltonprabu, S.; Tomczyk, M.; Skalicka-Woźniak, K.; Rastrelli, L.; Daglia, M.; Nabavi, S.F.; Alavian, S.M.; Nabavi, S.M. Hepatoprotective effect of quercetin: From chemistry to medicine. Food Chem. Toxicol. 2017, 108, 365–374. [Google Scholar] [CrossRef]
- Elsawaf, A.; Faras, A. El Hepatoprotective activity of quercetin against paracetamol-induced liver toxicity in rats. Tanta Med. J. 2017, 45, 92. [Google Scholar] [CrossRef]
- Oueslati, S.; Trabelsi, N.; Boulaaba, M.; Legault, J.; Abdelly, C.; Ksouri, R. Evaluation of antioxidant activities of the edible and medicinal Suaeda species and related phenolic compounds. Ind. Crops Prod. 2012, 36, 513–518. [Google Scholar] [CrossRef]
- Mohammed, H.A. Behavioral Evaluation for Aqueous and Ethanol Extracts of Suaeda vermiculata Forssk. Cent. Nerv. Syst. Agents Med. Chem. 2020. [Google Scholar] [CrossRef]
- Benwahhoud, M.; Jouad, H.; Eddouks, M.; Lyoussi, B. Hypoglycemic effect of Suaeda fruticosa in streptozotocin-induced diabetic rats. J. Ethnopharmacol. 2001, 76, 35–38. [Google Scholar] [CrossRef]
- Issa, M.; Agbon, A.; Balogun, S.; Mahdi, O.; Bobbo, K.; Ayegbusi, F. Hepatoprotective effect of methanol fruit pulp extract of Musa paradisiaca on carbon tetrachloride-induced liver toxicity in Wistar rats. J. Exp. Clin. Anat. 2018, 17, 1. [Google Scholar] [CrossRef]
- Khan, R.A.; Khan, M.R.; Sahreen, S. CCl4-induced hepatotoxicity: Protective effect of rutin on p53, CYP2E1 and the antioxidative status in rat. BMC Complement. Altern. Med. 2012, 12, 178. [Google Scholar] [CrossRef] [PubMed]
- Rahman, T.M.; Hodgson, H.J.F. Animal models of acute hepatic failure. Int. J. Exp. Pathol. 2000, 81, 145–157. [Google Scholar] [CrossRef] [PubMed]
- Lima, L.C.D.; Miranda, A.S.; Ferreira, R.N.; Rachid, M.A.; e Silva, A.C.S. Hepatic encephalopathy: Lessons from preclinical studies. World J. Hepatol. 2019, 11, 173–185. [Google Scholar] [CrossRef] [PubMed]
- Tuñón, M.J.; Alvarez, M.; Culebras, J.M.; González-Gallego, J. An overview of animal models for investigating the pathogenesis and therapeutic strategies in acute hepatic failure. World J. Gastroenterol. 2009, 15, 3086–3098. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Chou, P.; Hsu, C.; Hung, J.; Wu, Y.; Lin, J. Fermented Citrus Lemon Reduces Liver Injury Induced by Carbon Tetrachloride in Rats. Evid. Based. Complement. Alternat. Med. 2018, 2018. [Google Scholar] [CrossRef]
- Fouad, D.; Badr, A.; Attia, H.A. Hepatoprotective activity of raspberry ketone is mediated: Via inhibition of the NF-κB/TNF-α/caspase axis and mitochondrial apoptosis in chemically induced acute liver injury. Toxicol. Res. (Camb). 2019, 8, 663–676. [Google Scholar] [CrossRef]
- Kaur, C.; Kapoor, H.C. Anti-oxidant activity and total phenolic content of some Asian vegetables. Int. J. Food Sci. Technol. 2002, 37, 153–161. [Google Scholar] [CrossRef]
- Chantiratikul, P.; Meechai, P.; Nakbanpotec, W. Antioxidant Activities and Phenolic Contents of Extracts from Salvinia molesta and Eichornia crassipes. Res. J. Biol. Sci. 2009, 4, 1113–1117. [Google Scholar]
- Mohammed, H.A.; Al-Omar, M.S.; Mohammed, S.A.A.; Aly, M.S.A.; Alsuqub, A.N.A.; Khan, R.A. Drying Induced Impact on Composition and Oil Quality of Rosemary Herb, Rosmarinus Officinalis Linn. Molecules 2020, 25, 2830. [Google Scholar] [CrossRef]
- Floegel, A.; Kim, D.O.; Chung, S.J.; Koo, S.I.; Chun, O.K. Comparison of ABTS/DPPH assays to measure antioxidant capacity in popular antioxidant-rich US foods. J. Food Compos. Anal. 2011, 24, 1043–1048. [Google Scholar] [CrossRef]
- Organization for Economic Cooperation and Development (OECD) Guidelines for Testing of Chemicals, Guideline 425: Acute Oral Toxicity--Up-And-Down Procedure. Organ. Econ. Coop. Dev. Paris 2006.
- Ali, E.; Mohamed, H.; Lim, C.P.; Saad-Ebrika, O.; Asmawi, M.Z.; Sadikun, A.; Yam, F.; Mohamed, E.A.H.; Lim, C.P.; Ebrika, O.S.; et al. Toxicity evaluation of a standardised 50% ethanol extract of Orthosiphon stamineus. J. Ethnopharmacol. 2011, 133, 358–363. [Google Scholar] [CrossRef]
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. In Proceedings of the Behavior Research Methods; Psychonomic Society Inc.: Madisson, WI, USA, 2007; Volume 39, pp. 175–191. [Google Scholar]
- Kilkenny, C.; Browne, W.J.; Cuthill, I.C.; Emerson, M.; Altman, D.G. Improving bioscience research reporting: The arrive guidelines for reporting animal research. PLoS Biol. 2010, 8. [Google Scholar] [CrossRef]
- Wang, L.; Huang, Q.H.; Li, Y.X.; Huang, Y.F.; Xie, J.H.; Xu, L.Q.; Dou, Y.X.; Su, Z.R.; Zeng, H.F.; Chen, J.N. Protective effects of Silymarin on triptolide-induced acute hepatotoxicity in rats. Mol. Med. Rep. 2018, 17, 789–800. [Google Scholar] [CrossRef] [PubMed]
- Freitag, A.F.; Cardia, G.F.E.; Da Rocha, B.A.; Aguiar, R.P.; Silva-Comar, F.M.D.S.; Spironello, R.A.; Grespan, R.; Caparroz-Assef, S.M.; Bersani-Amado, C.A.; Cuman, R.K.N. Hepatoprotective effect of silymarin (silybum marianum) on hepatotoxicity induced by acetaminophen in spontaneously hypertensive rats. Evidence-based Complement. Altern. Med. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Li, C.C.; Hsiang, C.Y.; Wu, S.L.; Ho, T.Y. Identification of novel mechanisms of silymarin on the carbon tetrachloride-induced liver fibrosis in mice by nuclear factor-κB bioluminescent imaging-guided transcriptomic analysis. Food Chem. Toxicol. 2012, 50, 1568–1575. [Google Scholar] [CrossRef]
- Hassan, A. moniem S.; Abo El-Ela, F.I.; Abdel-Aziz, A.M. Investigating the potential protective effects of natural product quercetin against imidacloprid-induced biochemical toxicity and DNA damage in adults rats. Toxicol. Reports 2019, 6, 727–735. [Google Scholar] [CrossRef]
- El-Nekeety, A.A.; Abdel-Azeim, S.H.; Hassan, A.M.; Hassan, N.S.; Aly, S.E.; Abdel-Wahhab, M.A. Quercetin inhibits the cytotoxicity and oxidative stress in liver of rats fed aflatoxin-contaminated diet. Toxicol. Reports 2014, 1, 319–329. [Google Scholar] [CrossRef]
- Szende, B.; Timár, F.; Hargitai, B. Olive oil decreases liver damage in rats caused by carbon tetrachloride (CCl4). Exp. Toxicol. Pathol. 1994, 46, 355–359. [Google Scholar] [CrossRef]
- Bhat, S.H.; Shrivastava, R.; Malla, M.Y.; Iqbal, M.; Anjum, T.; Mir, A.H.; Sharma, M. Hepatoprotective activity of Argemone Mexicana Linn against toxic effects of carbon tetrachloride in rats. World J. Pharm. Res. 2014, 3, 4037–4048. [Google Scholar]
- Meharie, B.G.; Amare, G.G.; Belayneh, Y.M. Evaluation of Hepatoprotective Activity of the Crude Extract and Solvent Fractions of Clutia abyssinica (Euphorbiaceae) Leaf Against CCl 4-Induced Hepatotoxicity in Mice. J. Exp. Pharmacol. 2020, 12, 137–150. [Google Scholar] [CrossRef]
- Thefeld, W.; Hoffmeister, H.; Busch, E.-W.; Koller, P.; Vollmar, J. Referenzwerte für die Bestimmungen der Transaminasen GOT und GPT sowie der alkalischen Phosphatase im Serum mit optimierten Standardmethoden. DMW Dtsch. Medizinische Wochenschrift 1974, 99, 343–351. [Google Scholar] [CrossRef] [PubMed]
- Weichselbaum, C.T.E. An accurate and rapid method for the determination of proteins in small amounts of blood serum and plasma. Am. J. Clin. Pathol. 1946, 10, 40–49. [Google Scholar] [CrossRef]
- Fabiny, D.L.; Ertingshausen, G. Automated Reaction-Rate Method for Determination of Serum Creatinine with the CentrifiChem. Clin. Chem. 1971, 17. [Google Scholar] [CrossRef]
- Trinder, P. Determination of blood glucose using 4-amino phenazone as oxygen acceptor. J. Clin. Pathol. 1969, 22, 246. [Google Scholar] [CrossRef] [PubMed]
- Trinder, P. Enzymatic calorimetric determination of triglycerides by GOP-PAP method. Ann. ClinBiochem 1969, 6, 24–27. [Google Scholar]
- Carmichael, J.; DeGraff, W.G.; Gazdar, A.F.; Minna, J.D.; Mitchell, J.B. Evaluation of a Tetrazolium-based Semiautomated Colorimetric Assay: Assessment of Chemosensitivity Testing. Cancer Res. 1987, 47. [Google Scholar]
- Saito, J.; Okamura, A.; Takeuchi, K.; Hanioka, K.; Okada, A.; Ohata, T. High content analysis assay for prediction of human hepatotoxicity in HepaRG and HepG2 cells. Toxicol. Vitr. 2016, 33, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Danhof, M.; de Jongh, J.; De Lange, E.C.M.; Della Pasqua, O.; Ploeger, B.A.; Voskuyl, R.A. Mechanism-Based Pharmacokinetic-Pharmacodynamic Modeling: Biophase Distribution, Receptor Theory, and Dynamical Systems Analysis. Annu. Rev. Pharmacol. Toxicol. 2007, 47, 357–400. [Google Scholar] [CrossRef]
- Kirkwood, B.R.; Sterne, J.A.C. Essential Medical Statistics; Essentials; Wiley: Hoboken, NJ, USA, 2010; ISBN 9781444392845. [Google Scholar]

| Sr. | RT (min) | Mol. Formula | Calc. Mass | Obsrvd. Mass | Mass Fragments | Error (Δ ppm) | Compound Name | * R% | Refer |
|---|---|---|---|---|---|---|---|---|---|
| 1. | 16.11 | C10H16O5 | 217.1076 | 217.10656 [M + H] | 239.0883 [M+ + Na]; 455.1877 [2M + Na] | −2.265 | Senecic acid | 0.84 | [41] |
| 2. | 20.24 | C28H30O16 | 623.1612 | 623.1611 [M + H]+ | 446.9041[M-Pentose-acetyl];582.8751 [M-acetyl + 2H] | −1.007 | Kaempferol-O- (acetyl) hexoside-pentoside | 4.37 | [42] |
| 3. | 21.66 | C15H10O7 | 303.2443 | 303.0492 [M + H]+ | 289.1404 [M-CH2] | 0 | Quercetin | 12.45 | [43] |
| 4. | 23.45 | C15H8O6 | 285.0399 | 285.04069 [M + H]+ | 284.99585 [M]; 286.04395 [M + 2H] | 0.810 | Rhein | 1.26 | [44] |
| 5. | 24.18 | C12O14O4 | 223.0970 | 223.09634 [M + H]+ | 177.0543 [M + H-C2H10O]; 245.0782 [M + Na];467.16744 [2M + Na] | −0.957 | 4-Acetyl-6-(2-methylpropionyl)-1,3-resorcinol | 2.32 | [45] |
| 6. | 29.30 | C16H22O4 | 279.1596 | 279.15900 [M + H]+ | 301.1407 [M + Na]; 579.2921 [2M + Na] | −0.323 | (2E)-Heptyl-3-(3,4-dihydroxyphenyl) acrylate | 3.37 | [46] |
| 7. | 30.15 | C16H30O4 | 287.2222 | 287.22140 [M + H]+ | 199.16898 [M-C4H10O2]; 309.20324 [M + Na]; 595.41675 [2M + Na] | −1.260 | Hexadecanedioic acid | 1.57 | [47] |
| 8. | 31.70 | C55H74N4O5 | 872.5815 | 872.1408 [M + H]+ | 256.26268 [Phytyl-C2H5 + H];280.26241 [phytyl moiety];593.15607 [M-phytyl];577.12459 [M-phytyl–methyl];615.13623 [M-phytyl + Na] | 0.240 | Pheophytin-a | 23.69 | [48] |
| 9. | 31.75 | C27H30O16 | 633.1431 | 633.14559 [M + Na]+ | 634.14630 [M + H + Na] | 4.719 | Quercetin-3-O-rutinoside (Rutin) | 7.80 | [43] |
| Extracts | Extractive Values * | Total Phenolic Contents (mg GAE/g) | Total Flavonoid Contents (mg QE/g) |
|---|---|---|---|
| n-Hexane fraction | 1.06 | 15.1 ± 0.60 E | nd |
| Ethyl acetate fraction | 4.37 | 317.5 ± 0.17 A | 13.80 ± 0.04 BC |
| Chloroform fraction | 1.27 | 140.0 ± 1.02 D | 17.47 ± 0.02 A |
| n-Butanolic fraction | 6.25 | 192.6 ± 0.97 C | 11.55 ± 0.02 C |
| aq.-Ethanolic extract (mother liquor) | 20.00 | 200.6 ± 2.14 B | 16.70 ±1.56 AB |
| Groups | AST IU/L | ALT IU/L | TP g/dL | Creatinine mg/dL |
|---|---|---|---|---|
| 62.83 ±2.21 B | 67.42 ± 4.66 B | 7.39 ± 0.17 A | 0.91 ± 0.02 A |
| 54.36 ± 3.64 B | 55.19 ± 3.47 B | 6.14 ± 0.34 BC | 0.80 ± 0.04 A |
| 169.57 ± 12.68 A | 103.38 ± 4.86 A | 7.23 ± 0.17 AB | 0.82 ± 0.03 A |
| 55.40 ± 2.45 B | 55.25 ± 2.91 B | 5.32 ± 0.14 BC | 0.82 ± 0.04 A |
| 65.35 ± 3.92 B | 71.77 ± 4.25 B | 7.64 ± 0.23 A | 0.80 ± 0.03 A |
| 56.29 ± 3.30 B | 69.21 ± 3.79 B | 7.23 ± 0.27AB | 0.86 ± 0.03 A |
| 54.59 ± 1.67 B | 66.45 ± 7.05 B | 7.56 ± 0.32 A | 0.87 ± 0.02 A |
| 49.54 ± 1.23 B | 52.39 ± 4.56 B | 8.05 ± 0.18 A | 0.82 ± 0.03 A |
| Groups | Glucose mg/dL | Cholesterol mg/dL | Triglycerides mg/dL |
|---|---|---|---|
| 122.46 ± 2.66 A | 85.06 ± 1.85 A | 86.26 ± 2.24 BC |
| 101.82 ± 4.47 AB | 78.73 ± 3.87 AB | 74.11 ± 2.95 C |
| 111.23 ± 3.23 AB | 61.70 ± 1.42 D | 100.20 ± 6.80 AB |
| 110.43 ± 6.43 AB | 65.94 ± 2.17 CD | 99.54 ± 4.28 AB |
| 99.86 ± 4.15 B | 59.46 ± 1.66 D | 76.56 ± 3.25 C |
| 99.49 ± 7.00 B | 80.93 ± 2.08 AB | 97.53 ± 3.58 AB |
| 98.79 ± 6.70 B | 66.66 ± 2.20 CD | 78.16 ± 2.62 C |
| 115.46 ± 3.58 AB | 72.83 ± 1.57 BC | 3.02 A |
| Groups | IC50 (µg/mL) * | RR | |
|---|---|---|---|
| HepG-2 | HepG-2/ADR | ||
| aq.-Ethanolic extract | 56.19 ± 2.55 | 78.40 ± 0.32 *** | 1.39 |
| Doxorubicin | 1.3 ± 0.064 | 4.77 ± 1.05 *** | 3.67 |
| Groups | IC50 (µg/mL) | Synergistic Parameters | |||
|---|---|---|---|---|---|
| HepG-2/ADR | FR | CI | r | IB | |
| Doxorubicin (DOX) | 4.77 ± 1.05 | -- | -- | -- | -- |
| DOX + aq.-ethanolic extract | 1.72 ± 0.07 *** | 2.77 | 0.56 | 0.99 | Synergism |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mohammed, S.A.A.; Khan, R.A.; El-Readi, M.Z.; Emwas, A.-H.; Sioud, S.; Poulson, B.G.; Jaremko, M.; Eldeeb, H.M.; Al-Omar, M.S.; Mohammed, H.A. Suaeda vermiculata Aqueous-Ethanolic Extract-Based Mitigation of CCl4-Induced Hepatotoxicity in Rats, and HepG-2 and HepG-2/ADR Cell-Lines-Based Cytotoxicity Evaluations. Plants 2020, 9, 1291. https://doi.org/10.3390/plants9101291
Mohammed SAA, Khan RA, El-Readi MZ, Emwas A-H, Sioud S, Poulson BG, Jaremko M, Eldeeb HM, Al-Omar MS, Mohammed HA. Suaeda vermiculata Aqueous-Ethanolic Extract-Based Mitigation of CCl4-Induced Hepatotoxicity in Rats, and HepG-2 and HepG-2/ADR Cell-Lines-Based Cytotoxicity Evaluations. Plants. 2020; 9(10):1291. https://doi.org/10.3390/plants9101291
Chicago/Turabian StyleMohammed, Salman A. A., Riaz A. Khan, Mahmoud Z. El-Readi, Abdul-Hamid Emwas, Salim Sioud, Benjamin G. Poulson, Mariusz Jaremko, Hussein M. Eldeeb, Mohsen S. Al-Omar, and Hamdoon A. Mohammed. 2020. "Suaeda vermiculata Aqueous-Ethanolic Extract-Based Mitigation of CCl4-Induced Hepatotoxicity in Rats, and HepG-2 and HepG-2/ADR Cell-Lines-Based Cytotoxicity Evaluations" Plants 9, no. 10: 1291. https://doi.org/10.3390/plants9101291
APA StyleMohammed, S. A. A., Khan, R. A., El-Readi, M. Z., Emwas, A.-H., Sioud, S., Poulson, B. G., Jaremko, M., Eldeeb, H. M., Al-Omar, M. S., & Mohammed, H. A. (2020). Suaeda vermiculata Aqueous-Ethanolic Extract-Based Mitigation of CCl4-Induced Hepatotoxicity in Rats, and HepG-2 and HepG-2/ADR Cell-Lines-Based Cytotoxicity Evaluations. Plants, 9(10), 1291. https://doi.org/10.3390/plants9101291







