Investigating the Spatiotemporal Relationship between the Built Environment and COVID-19 Transmission
Abstract
:1. Introduction
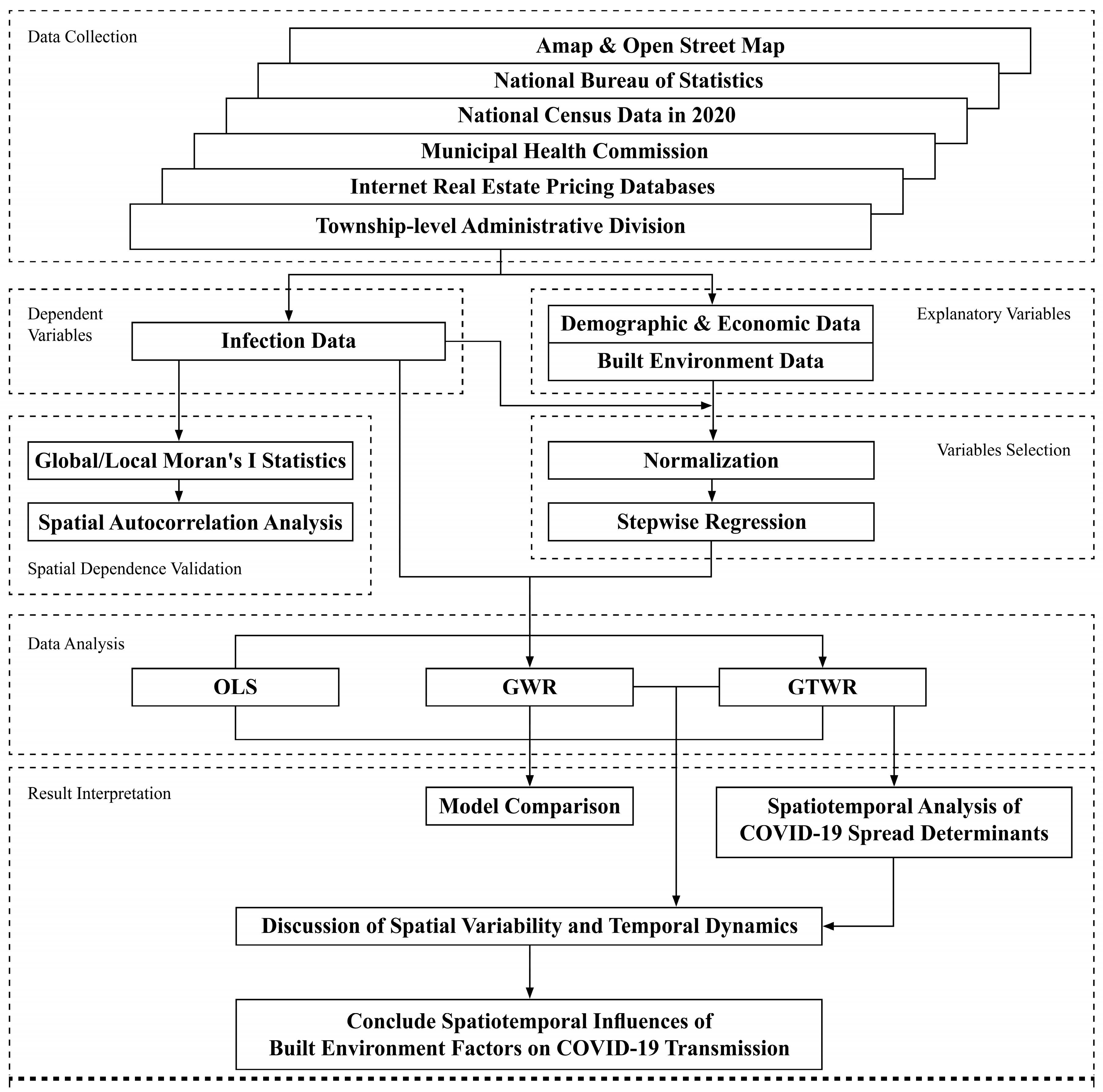
2. Methodology
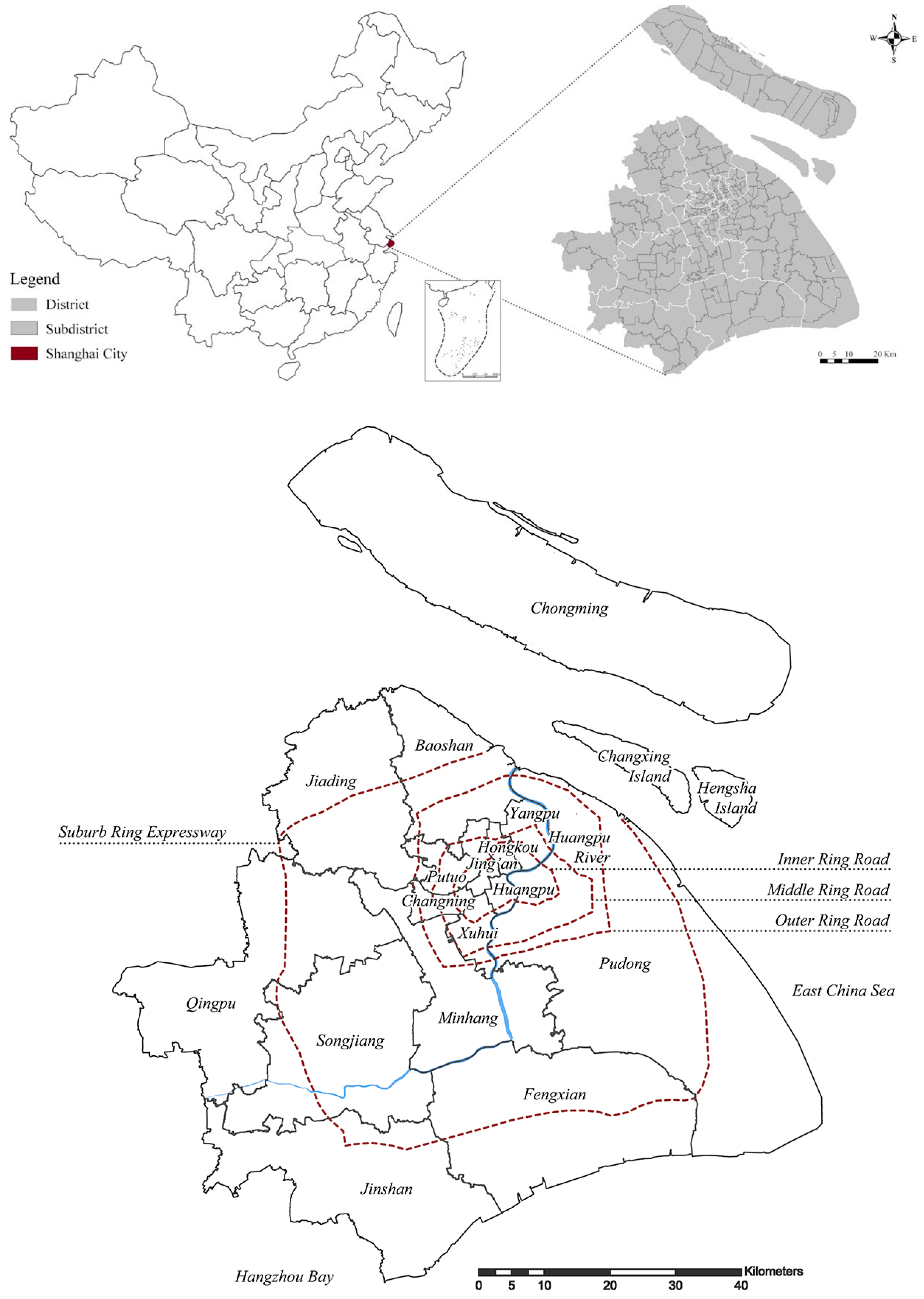
2.1. Study Area
2.2. Datasets
2.2.1. Infection Data
2.2.2. Demographic and Economic Variables
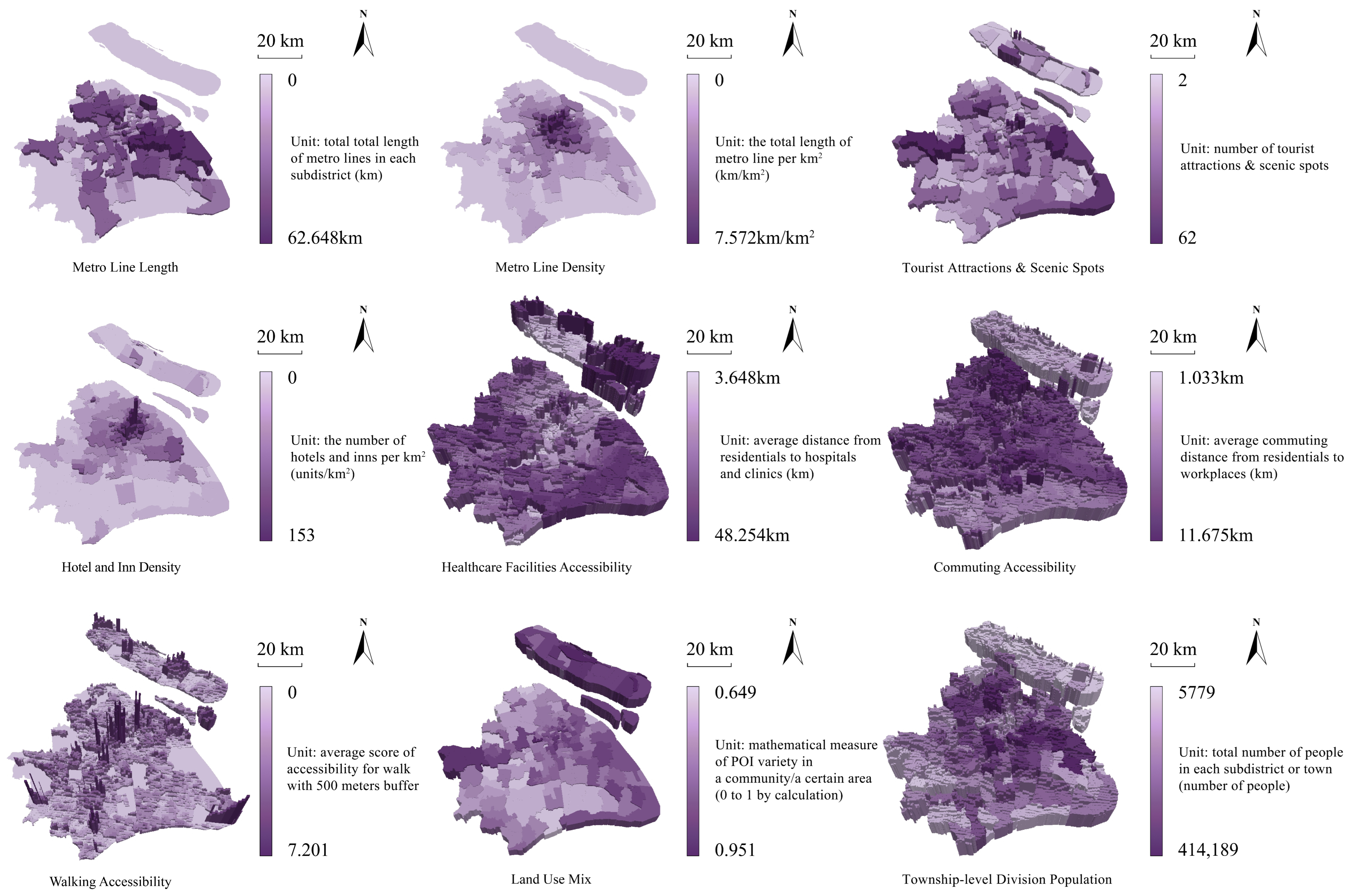
2.2.3. Built Environment Variables
2.3. Methods
3. Results
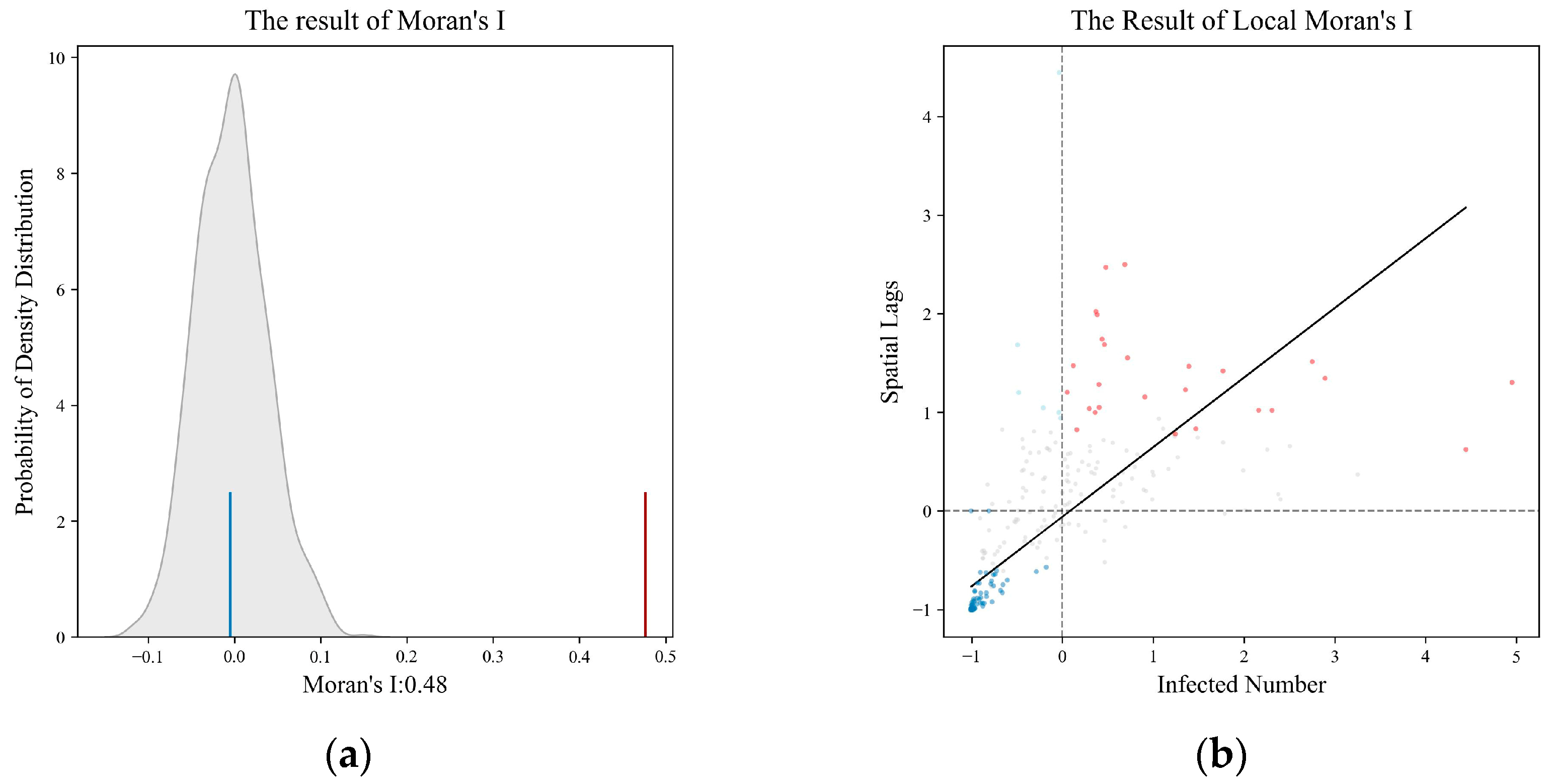
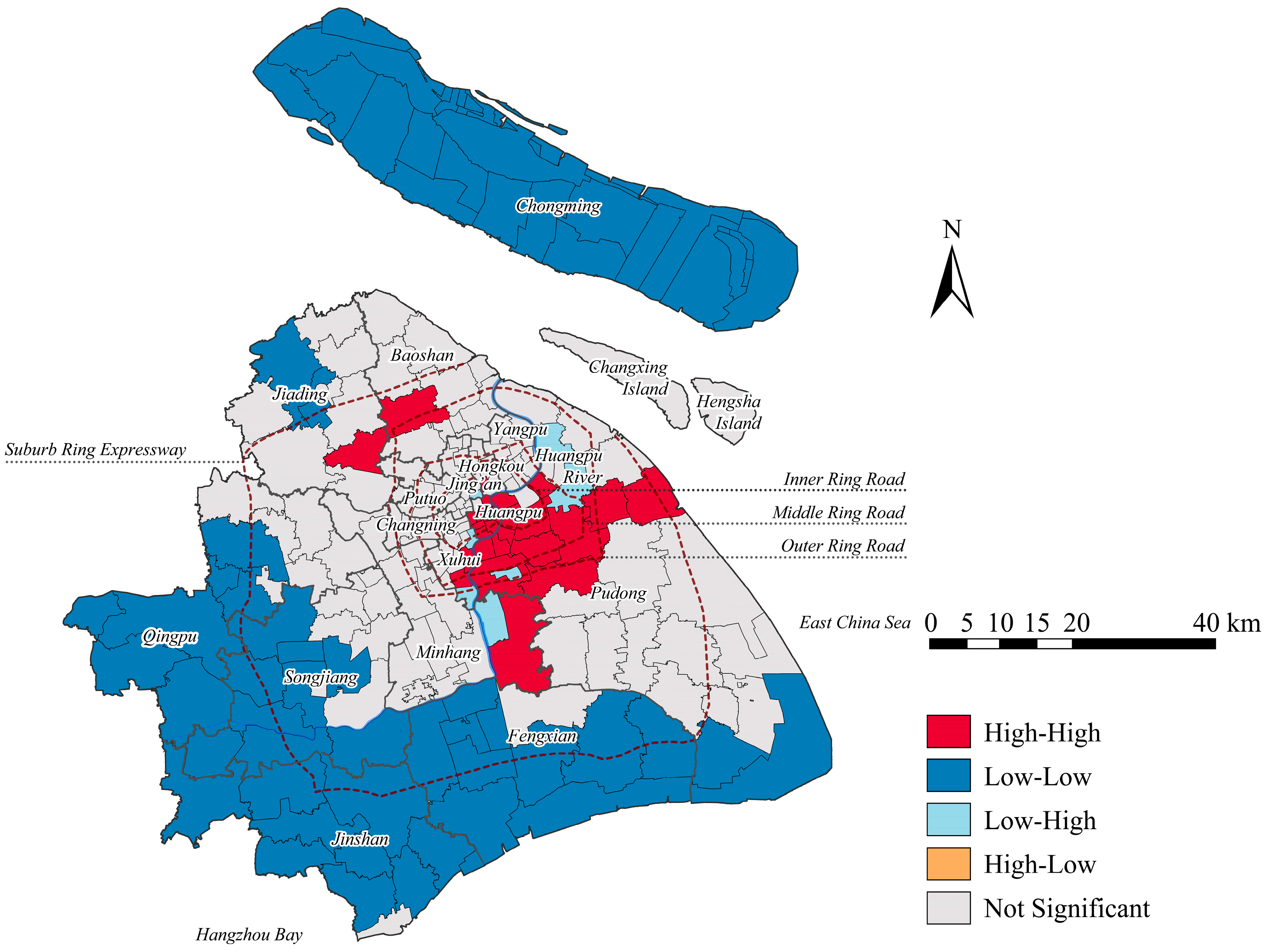
3.1. Spatial Patterns: Cluster Analysis
3.2. Regression Results and Comparison
3.3. Spatial Variation of Estimated Coefficients
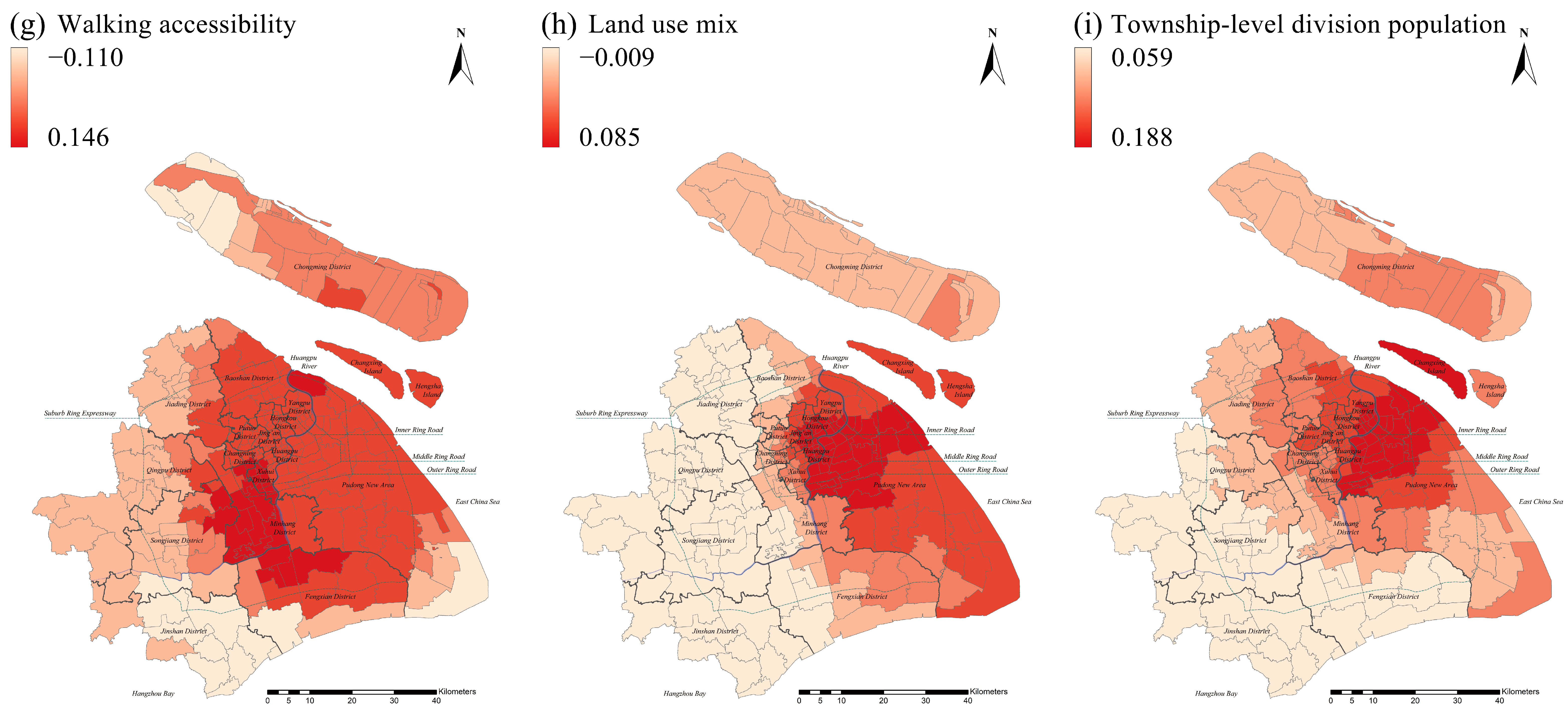
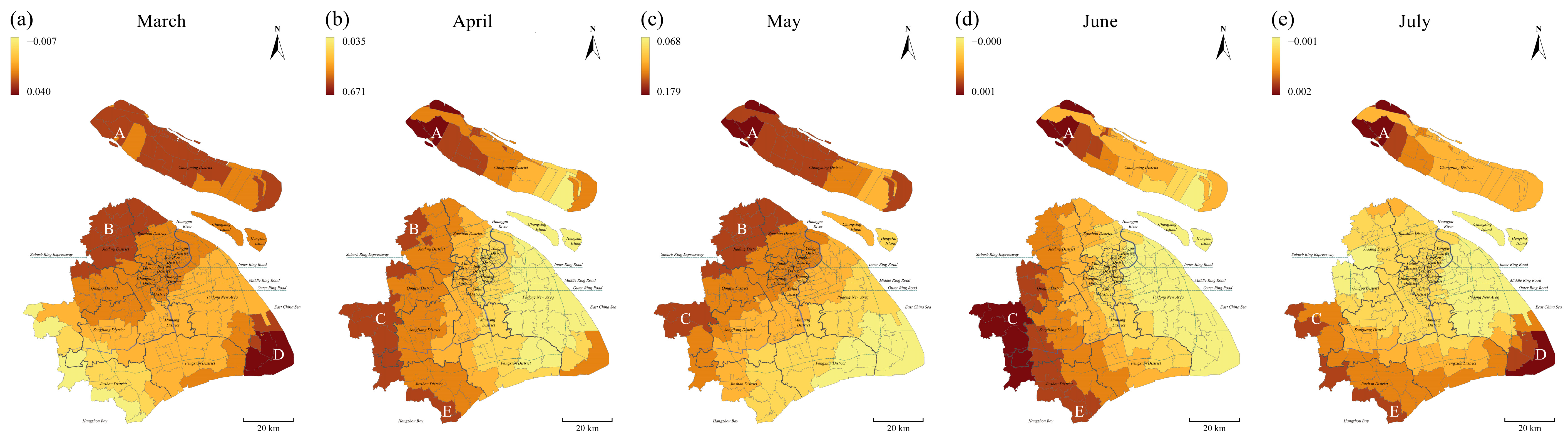
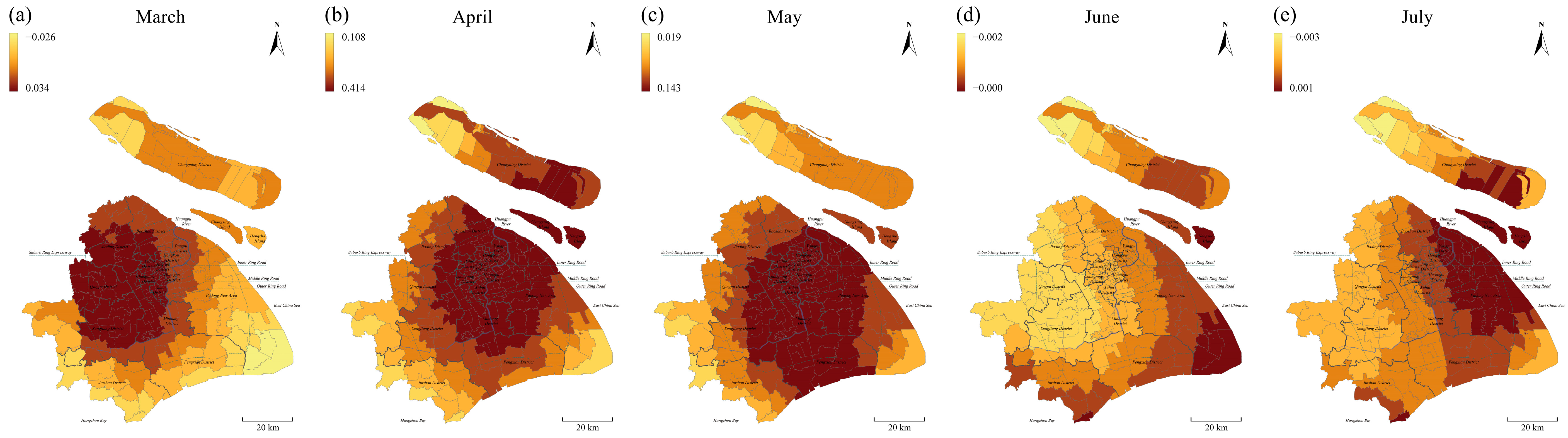
3.3.1. Spatial Distribution by Environmental Variables
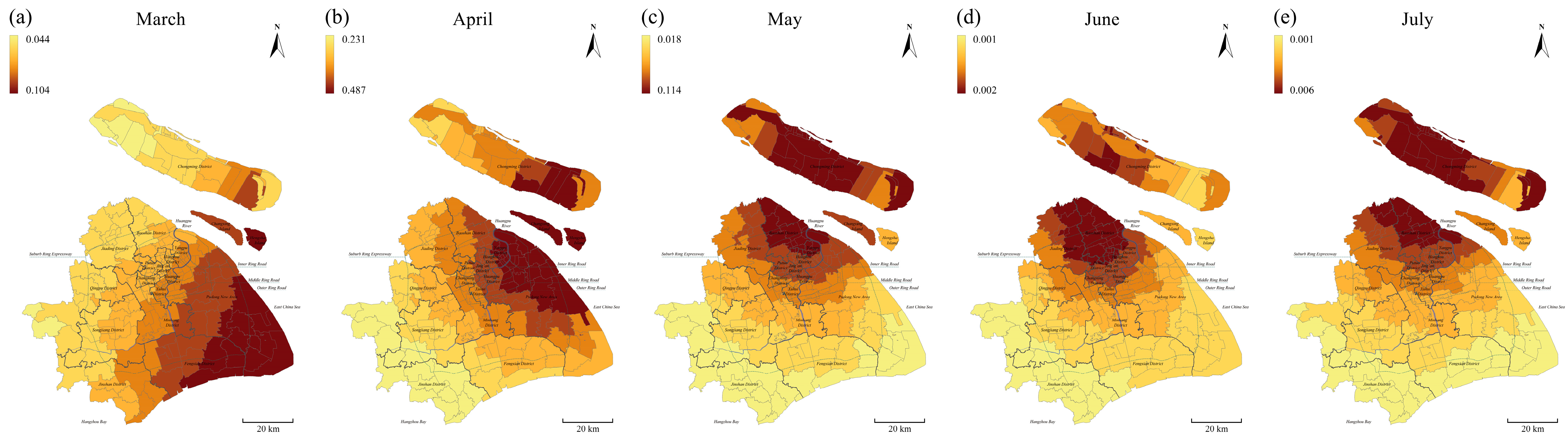
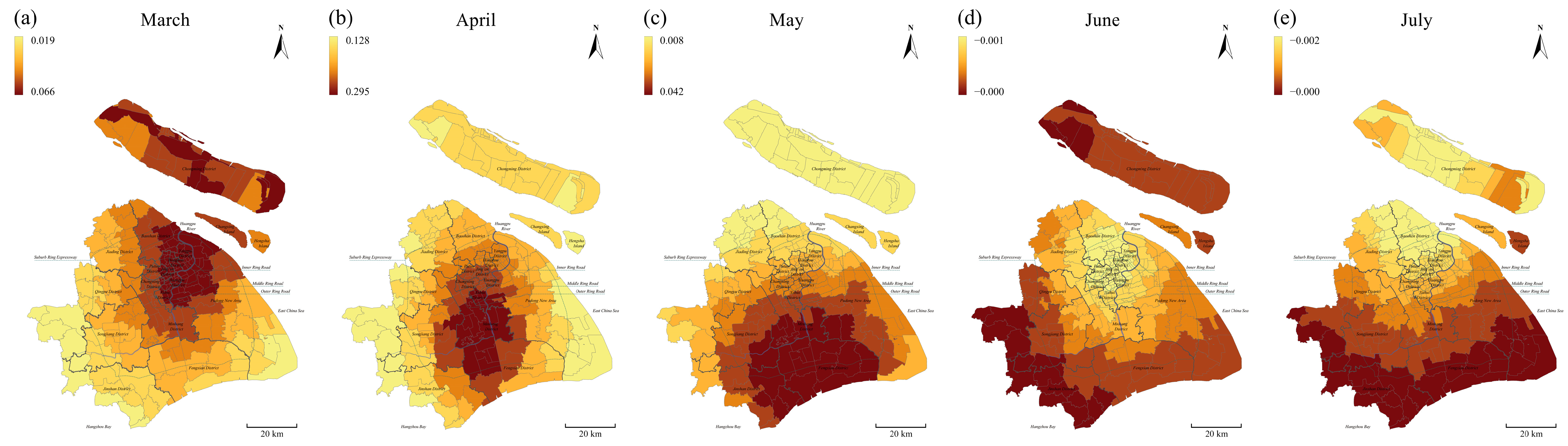
3.3.2. Spatial Distribution by Temporal Scale
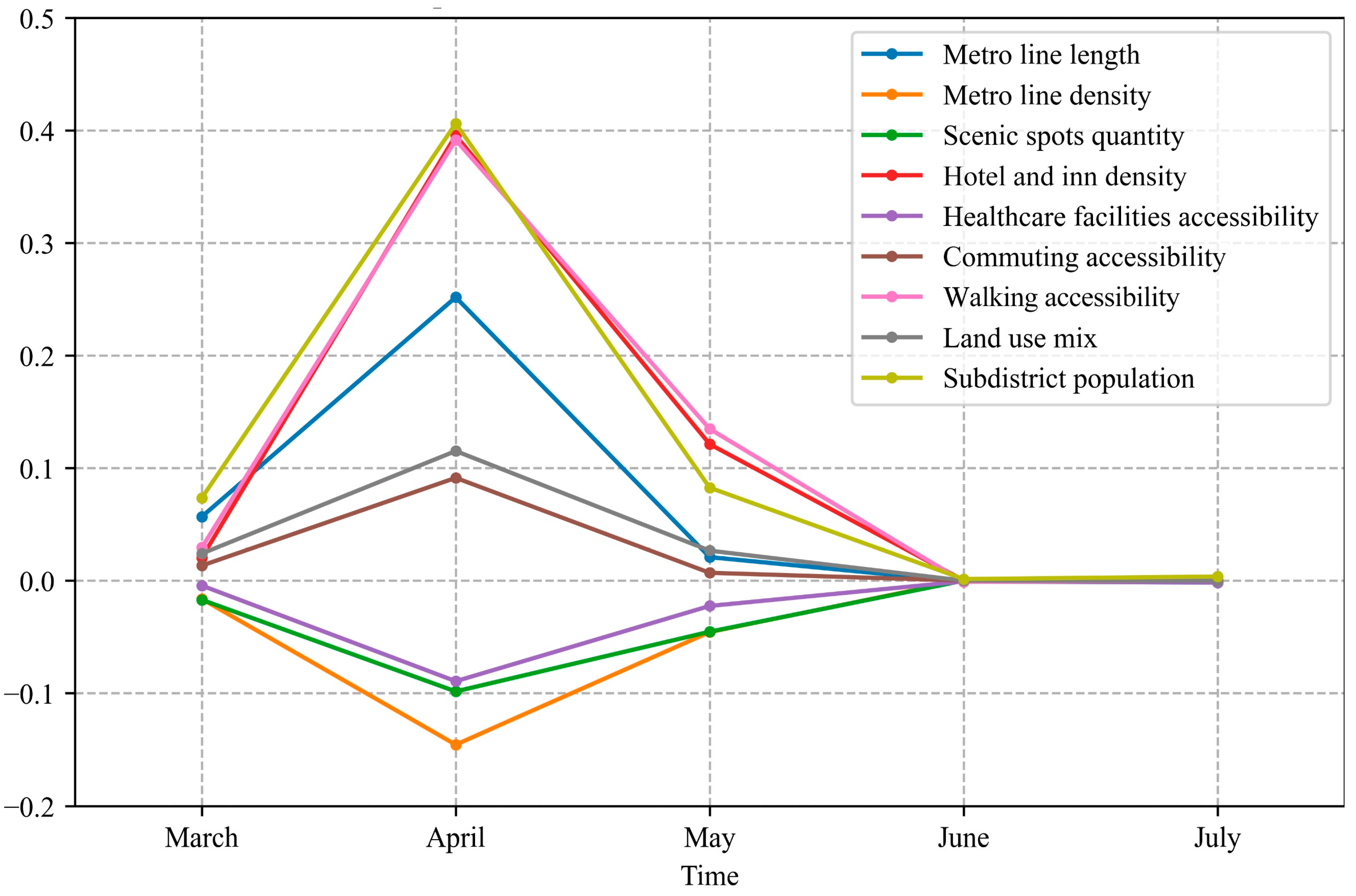
3.3.3. Temporal Variation in Estimated Coefficients
4. Discussion
4.1. Spatial Variability
4.1.1. Population, Transmission, and COVID-19 Policies
4.1.2. Mobility and Urban Transport System
4.1.3. COVID-19 Distribution and Accessibility Disparity
4.1.4. Epidemics and Land Mixing
4.2. Temporal Dynamics
4.2.1. Overall Temporal Variation in Built Environment Variables
4.2.2. Human Behaviors and Public Transportation
4.2.3. Temporal Variation in Accessibility
4.2.4. Hotel Density and COVID-19 Transmission
4.3. Limitations and Assumptions
4.4. Implications and Future Perspectives
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Ascher, K.; Marech, W.; Alexander, I. The Works: Anatomy of a City; Penguin Press: New York, NY, USA, 2005; ISBN 1-59420-071-8. [Google Scholar]
- Santiago-Alarcon, D.; MacGregor-Fors, I. Cities and Pandemics: Urban Areas Are Ground Zero for the Transmission of Emerging Human Infectious Diseases. J. Urban Ecol. 2020, 6, juaa012. [Google Scholar] [CrossRef]
- Liu, C.; Liu, Z.; Guan, C. The Impacts of the Built Environment on the Incidence Rate of COVID-19: A Case Study of King County, Washington. Sustain. Cities Soc. 2021, 74, 103144. [Google Scholar] [CrossRef] [PubMed]
- Li, R.; Huang, Y. COVID-19 Pandemic and Minority Health Disparities in New York City: A Spatial and Temporal Perspective. Environ. Plan. B Urban Anal. City Sci. 2023, 50, 1194–1211. [Google Scholar] [CrossRef]
- Nazroo, J.; Murray, K.; Taylor, H.; Bécares, L.; Field, Y.; Kapadia, D.; Rolston, Y. Rapid Evidence Review: Inequalities in Relation to COVID-19 and Their Effects on London; University of Manchester: London, UK; The Ubele Initiative: London, UK; University of Sussex: Brighton, UK, 2020. [Google Scholar]
- Chakraborty, I.; Maity, P. COVID-19 Outbreak: Migration, Effects on Society, Global Environment and Prevention. Sci. Total Environ. 2020, 728, 138882. [Google Scholar] [CrossRef]
- Sobczak, M.; Pawliczak, R. Factors That Affect the COVID-19 Pandemic in Summer 2022 Compared to Summer 2021. Int. J. Environ. Res. Public Health 2022, 19, 12561. [Google Scholar] [CrossRef]
- Andreucci, M.B.; Marvuglia, A. Investigating, Implementing and Funding Regenerative Urban Design in a Post-COVID-19 Pandemic Built Environment: A Reading through Selected UN Sustainable Development Goals and the European Green Deal. In Rethinking Sustainability towards a Regenerative Economy; Andreucci, M.B., Marvuglia, A., Baltov, M., Hansen, P., Eds.; Future City; Springer International Publishing: Cham, Switzerland, 2021; Volume 15, pp. 395–413. ISBN 978-3-030-71818-3. [Google Scholar]
- Fenner, R.; Cernev, T. The Implications of the COVID-19 Pandemic for Delivering the Sustainable Development Goals. Futures 2021, 128, 102726. [Google Scholar] [CrossRef]
- Whyte, W.H. The Social Life of Small Urban Spaces; 7. print.; Project for Public Spaces: New York, NY, USA, 2010; ISBN 978-0-9706324-1-8. [Google Scholar]
- Yip, T.L.; Huang, Y.; Liang, C. Built Environment and the Metropolitan Pandemic: Analysis of the COVID-19 Spread in Hong Kong. Build. Environ. 2021, 188, 107471. [Google Scholar] [CrossRef]
- DiMaggio, C.; Klein, M.; Berry, C.; Frangos, S. Black/African American Communities Are at Highest Risk of COVID-19: Spatial Modeling of New York City ZIP Code–Level Testing Results. Ann. Epidemiol. 2020, 51, 7–13. [Google Scholar] [CrossRef]
- Fortaleza, C.M.C.B.; Guimarães, R.B.; De Almeida, G.B.; Pronunciate, M.; Ferreira, C.P. Taking the Inner Route: Spatial and Demographic Factors Affecting Vulnerability to COVID-19 among 604 Cities from Inner São Paulo State, Brazil. Epidemiol. Infect. 2020, 148, e118. [Google Scholar] [CrossRef]
- Dutta, I.; Basu, T.; Das, A. Spatial Analysis of COVID-19 Incidence and Its Determinants Using Spatial Modeling: A Study on India. Environ. Chall. 2021, 4, 100096. [Google Scholar] [CrossRef]
- Klompmaker, J.O.; Hart, J.E.; Holland, I.; Sabath, M.B.; Wu, X.; Laden, F.; Dominici, F.; James, P. County-Level Exposures to Greenness and Associations with COVID-19 Incidence and Mortality in the United States. Environ. Res. 2021, 199, 111331. [Google Scholar] [CrossRef] [PubMed]
- López-Gay, A.; Spijker, J.; Cole, H.V.S.; Marques, A.G.; Triguero-Mas, M.; Anguelovski, I.; Marí-Dell’Olmo, M.; Módenes, J.A.; Álamo-Junquera, D.; López-Gallego, F.; et al. Sociodemographic Determinants of Intraurban Variations in COVID-19 Incidence: The Case of Barcelona. J. Epidemiol. Community Health 2022, 76, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Md Iderus, N.H.; Lakha Singh, S.S.; Mohd Ghazali, S.; Yoon Ling, C.; Cia Vei, T.; Md Zamri, A.S.S.; Ahmad Jaafar, N.; Ruslan, Q.; Ahmad Jaghfar, N.H.; Gill, B.S. Correlation between Population Density and COVID-19 Cases during the Third Wave in Malaysia: Effect of the Delta Variant. Int. J. Environ. Res. Public Health 2022, 19, 7439. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Liu, Y.; Chen, F.; Mi, B.; Zeng, L.; Pei, L. The Effect of Sociodemographic Factors on COVID-19 Incidence of 342 Cities in China: A Geographically Weighted Regression Model Analysis. BMC Infect. Dis. 2021, 21, 428. [Google Scholar] [CrossRef] [PubMed]
- Liu, L. Emerging Study on the Transmission of the Novel Coronavirus (COVID-19) from Urban Perspective: Evidence from China. Cities 2020, 103, 102759. [Google Scholar] [CrossRef] [PubMed]
- Barak, N.; Sommer, U.; Mualam, N. Urban Attributes and the Spread of COVID-19: The Effects of Density, Compliance and Socio-Political Factors in Israel. Sci. Total Environ. 2021, 793, 148626. [Google Scholar] [CrossRef]
- Huang, J.; Kwan, M.-P.; Kan, Z.; Wong, M.; Kwok, C.; Yu, X. Investigating the Relationship between the Built Environment and Relative Risk of COVID-19 in Hong Kong. IJGI 2020, 9, 624. [Google Scholar] [CrossRef]
- Li, X.; Zhou, L.; Jia, T.; Peng, R.; Fu, X.; Zou, Y. Associating COVID-19 Severity with Urban Factors: A Case Study of Wuhan. Int. J. Environ. Res. Public Health 2020, 17, 6712. [Google Scholar] [CrossRef]
- You, H.; Wu, X.; Guo, X. Distribution of COVID-19 Morbidity Rate in Association with Social and Economic Factors in Wuhan, China: Implications for Urban Development. Int. J. Environ. Res. Public Health 2020, 17, 3417. [Google Scholar] [CrossRef]
- Li, B.; Peng, Y.; He, H.; Wang, M.; Feng, T. Built Environment and Early Infection of COVID-19 in Urban Districts: A Case Study of Huangzhou. Sustain. Cities Soc. 2021, 66, 102685. [Google Scholar] [CrossRef]
- Ma, S.; Li, S.; Zhang, J. Diverse and Nonlinear Influences of Built Environment Factors on COVID-19 Spread across Townships in China at Its Initial Stage. Sci. Rep. 2021, 11, 12415. [Google Scholar] [CrossRef] [PubMed]
- Kan, Z.; Kwan, M.-P.; Wong, M.S.; Huang, J.; Liu, D. Identifying the Space-Time Patterns of COVID-19 Risk and Their Associations with Different Built Environment Features in Hong Kong. Sci. Total Environ. 2021, 772, 145379. [Google Scholar] [CrossRef]
- Schmiege, D.; Haselhoff, T.; Ahmed, S.; Anastasiou, O.E.; Moebus, S. Associations Between Built Environment Factors and SARS-CoV-2 Infections at the Neighbourhood Level in a Metropolitan Area in Germany. J. Urban Health 2023, 100, 40–50. [Google Scholar] [CrossRef] [PubMed]
- Hu, T.; Yue, H.; Wang, C.; She, B.; Ye, X.; Liu, R.; Zhu, X.; Guan, W.W.; Bao, S. Racial Segregation, Testing Site Access, and COVID-19 Incidence Rate in Massachusetts, USA. Int. J. Environ. Res. Public Health 2020, 17, 9528. [Google Scholar] [CrossRef] [PubMed]
- Guan, C.; Tan, J.; Hall, B.; Liu, C.; Li, Y.; Cai, Z. The Effect of the Built Environment on the COVID-19 Pandemic at the Initial Stage: A County-Level Study of the USA. Sustainability 2022, 14, 3417. [Google Scholar] [CrossRef]
- Nguyen, Q.C.; Huang, Y.; Kumar, A.; Duan, H.; Keralis, J.M.; Dwivedi, P.; Meng, H.-W.; Brunisholz, K.D.; Jay, J.; Javanmardi, M.; et al. Using 164 Million Google Street View Images to Derive Built Environment Predictors of COVID-19 Cases. Int. J. Environ. Res. Public Health 2020, 17, 6359. [Google Scholar] [CrossRef]
- Li, S.; Ma, S.; Zhang, J. Association of Built Environment Attributes with the Spread of COVID-19 at Its Initial Stage in China. Sustain. Cities Soc. 2021, 67, 102752. [Google Scholar] [CrossRef]
- Wang, J.; Wu, X.; Wang, R.; He, D.; Li, D.; Yang, L.; Yang, Y.; Lu, Y. Review of Associations between Built Environment Characteristics and Severe Acute Respiratory Syndrome Coronavirus 2 Infection Risk. Int. J. Environ. Res. Public Health 2021, 18, 7561. [Google Scholar] [CrossRef]
- Wang, S.; Liu, Y.; Lam, J.; Kwan, M.-P. The Effects of the Built Environment on the General Health, Physical Activity and Obesity of Adults in Queensland, Australia. Spat. Spatio-Temporal Epidemiol. 2021, 39, 100456. [Google Scholar] [CrossRef]
- Xiao, Y.; Chen, S.; Miao, S.; Yu, Y. Exploring the Mediating Effect of Physical Activities on Built Environment and Obesity for Elderly People: Evidence from Shanghai, China. Front. Public Health 2022, 10, 853292. [Google Scholar] [CrossRef]
- Ewing, R.; Cervero, R. Travel and the Built Environment: A Meta-Analysis. J. Am. Plan. Assoc. 2010, 76, 265–294. [Google Scholar] [CrossRef]
- Witten, K.; Blakely, T.; Bagheri, N.; Badland, H.; Ivory, V.; Pearce, J.; Mavoa, S.; Hinckson, E.; Schofield, G. Neighborhood Built Environment and Transport and Leisure Physical Activity: Findings Using Objective Exposure and Outcome Measures in New Zealand. Environ. Health Perspect. 2012, 120, 971–977. [Google Scholar] [CrossRef]
- Liu, L.; Zhang, M.; Xu, T. A Conceptual Framework and Implementation Tool for Land Use Planning for Corridor Transit Oriented Development. Cities 2020, 107, 102939. [Google Scholar] [CrossRef]
- Carozzi, F. Urban Density and COVID-19. SSRN J. 2020. [Google Scholar] [CrossRef]
- Rahman, M.H.; Zafri, N.M.; Ashik, F.; Waliullah, M. Gis-Based Spatial Modeling to Identify Factors Affecting COVID-19 Incidence Rates in Bangladesh. SSRN J. 2020. [Google Scholar] [CrossRef]
- Kim, B.; Rundle, A.G.; Goodwin, A.T.S.; Morrison, C.N.; Branas, C.C.; El-Sadr, W.; Duncan, D.T. COVID-19 Testing, Case, and Death Rates and Spatial Socio-Demographics in New York City: An Ecological Analysis as of June 2020. Health Place 2021, 68, 102539. [Google Scholar] [CrossRef]
- Yang, T.-C.; Kim, S.; Zhao, Y.; Choi, S.E. Examining Spatial Inequality in COVID-19 Positivity Rates across New York City ZIP Codes. Health Place 2021, 69, 102574. [Google Scholar] [CrossRef]
- Ma, S.; Li, S.; Zhang, J. The Spread of COVID-19 in China at Its Initial Stage: A Township-Level Analysis in Association with the Built Environment. SSRN J. 2020. [Google Scholar] [CrossRef]
- Scarpone, C.; Brinkmann, S.T.; Große, T.; Sonnenwald, D.; Fuchs, M.; Walker, B.B. A Multimethod Approach for County-Scale Geospatial Analysis of Emerging Infectious Diseases: A Cross-Sectional Case Study of COVID-19 Incidence in Germany. Int. J. Health Geogr. 2020, 19, 32. [Google Scholar] [CrossRef]
- Fischer, M.M. Spatial Analysis in Geography. In International Encyclopedia of the Social & Behavioral Sciences; Elsevier: Amsterdam, The Netherlands, 2015; pp. 94–99. ISBN 978-0-08-097087-5. [Google Scholar]
- Lin, Y.; Yang, B.; Cobey, S.; Lau, E.H.Y.; Adam, D.C.; Wong, J.Y.; Bond, H.S.; Cheung, J.K.; Ho, F.; Gao, H.; et al. Incorporating Temporal Distribution of Population-Level Viral Load Enables Real-Time Estimation of COVID-19 Transmission. Nat. Commun. 2022, 13, 1155. [Google Scholar] [CrossRef]
- Chen, Y.; Chen, M.; Huang, B.; Wu, C.; Shi, W. Modeling the Spatiotemporal Association Between COVID-19 Transmission and Population Mobility Using Geographically and Temporally Weighted Regression. GeoHealth 2021, 5, e2021GH000402. [Google Scholar] [CrossRef]
- Ling, L.; Qian, X.; Guo, S.; Ukkusuri, S.V. Spatiotemporal Impacts of Human Activities and Socio-Demographics during the COVID-19 Outbreak in the US. BMC Public Health 2022, 22, 1466. [Google Scholar] [CrossRef]
- Sy, K.T.L.; White, L.F.; Nichols, B.E. Population Density and Basic Reproductive Number of COVID-19 across United States Counties. PLoS ONE 2021, 16, e0249271. [Google Scholar] [CrossRef]
- Credit, K. Neighbourhood Inequity: Exploring the Factors Underlying Racial and Ethnic Disparities in COVID-19 Testing and Infection Rates Using ZIP Code Data in Chicago and New York. Reg. Sci. Policy Pract. 2020, 12, 1249–1271. [Google Scholar] [CrossRef]
- Wong, D.W.S.; Li, Y. Spreading of COVID-19: Density Matters. PLoS ONE 2020, 15, e0242398. [Google Scholar] [CrossRef]
- Teller, J. Urban Density and COVID-19: Towards an Adaptive Approach. Build. Cities 2021, 2, 150–165. [Google Scholar] [CrossRef]
- Chung, C.K.L.; Xu, J.; Zhang, M. Geographies of COVID-19: How Space and Virus Shape Each Other. Asian Geogr. 2020, 37, 99–116. [Google Scholar] [CrossRef]
- He, Q.; He, W.; Song, Y.; Wu, J.; Yin, C.; Mou, Y. The Impact of Urban Growth Patterns on Urban Vitality in Newly Built-Up Areas Based on an Association Rules Analysis Using Geographical ‘Big Data’. Land Use Policy 2018, 78, 726–738. [Google Scholar] [CrossRef]
- Wu, C.; Ye, X.; Ren, F.; Du, Q. Check-in Behaviour and Spatio-Temporal Vibrancy: An Exploratory Analysis in Shenzhen, China. Cities 2018, 77, 104–116. [Google Scholar] [CrossRef]
- Wang, J.; McDonald, N.; Cochran, A.L.; Oluyede, L.; Wolfe, M.; Prunkl, L. Health Care Visits during the COVID-19 Pandemic: A Spatial and Temporal Analysis of Mobile Device Data. Health Place 2021, 72, 102679. [Google Scholar] [CrossRef]
- Peng, J.; Liu, H.; Tang, J.; Peng, C.; Yang, X.; Deng, M.; Xu, Y. Exploring Crowd Travel Demands Based on the Characteristics of Spatiotemporal Interaction between Urban Functional Zones. IJGI 2023, 12, 225. [Google Scholar] [CrossRef]
- Qu, J.; Zhang, J. Validating Mobile Designs with Agile Testing in China: Based on Baidu Map for Mobile. In Design, User Experience, and Usability: Design Thinking and Methods; Marcus, A., Ed.; Lecture Notes in Computer Science; Springer International Publishing: Cham, Switzerland, 2016; Volume 9746, pp. 491–498. ISBN 978-3-319-40408-0. [Google Scholar]
- Dong, G.; Li, R.; Wu, H.; Chen, W.; Huang, W.; Zhang, H. Browsing Behavior Modeling and Browsing Interest Extraction in the Trajectories on Web Map Service Platforms. Expert Syst. Appl. 2022, 195, 116590. [Google Scholar] [CrossRef]
- Wachs, M.; Kumagai, T.G. Physical Accessibility as a Social Indicator. Socio-Econ. Plan. Sci. 1973, 7, 437–456. [Google Scholar] [CrossRef]
- Higgins, C.; Palm, M.; DeJohn, A.; Xi, L.; Vaughan, J.; Farber, S.; Widener, M.; Miller, E. Calculating Place-Based Transit Accessibility: Methods, Tools and Algorithmic Dependence. JTLU 2022, 15, 95–116. [Google Scholar] [CrossRef]
- Khahro, S.H.; Talpur, M.A.H.; Bhellar, M.G.; Das, G.; Shaikh, H.; Sultan, B. GIS-Based Sustainable Accessibility Mapping of Urban Parks: Evidence from the Second Largest Settlement of Sindh, Pakistan. Sustainability 2023, 15, 6228. [Google Scholar] [CrossRef]
- Talpur, M.A.H.; Khahro, S.H.; Ali, T.H.; Waseem, H.B.; Napiah, M. Computing Travel Impendences Using Trip Generation Regression Model: A Phenomenon of Travel Decision-Making Process of Rural Households. Environ. Dev. Sustain. 2023, 25, 5973–5996. [Google Scholar] [CrossRef]
- Cooper, C.H.V.; Chiaradia, A.J.F. sDNA: 3-d Spatial Network Analysis for GIS, CAD, Command Line & Python. SoftwareX 2020, 12, 100525. [Google Scholar] [CrossRef]
- Shi, H.; Zhao, M.; Simth, D.A.; Chi, B. Behind the Land Use Mix: Measuring the Functional Compatibility in Urban and Sub-Urban Areas of China. Land 2021, 11, 2. [Google Scholar] [CrossRef]
- Carver, S.J. Integrating Multi-Criteria Evaluation with Geographical Information Systems. Int. J. Geogr. Inf. Syst. 1991, 5, 321–339. [Google Scholar] [CrossRef]
- Mazziotta, M.; Pareto, A. Methods for Constructing Composite Indices: One for All or All for One. Riv. Ital. Econ. Demogr. Stat. 2013, 67, 67–80. [Google Scholar]
- Libório, M.P.; Diniz, A.M.A.; Rabiei-Dastjerd, H.; Martinuci, O.D.S.; Martins, C.A.P.D.S.; Ekel, P.I. A Decision Framework for Identifying Methods to Construct Stable Composite Indicators That Capture the Concept of Multidimensional Social Phenomena: The Case of Social Exclusion. Sustainability 2023, 15, 6171. [Google Scholar] [CrossRef]
- Thompson, B. Stepwise Regression and Stepwise Discriminant Analysis Need Not Apply Here: A Guidelines Editorial. Educ. Psychol. Meas. 1995, 55, 525–534. [Google Scholar] [CrossRef]
- Saltelli, A.; Ratto, M.; Tarantola, S.; Campolongo, F. Sensitivity Analysis Practices: Strategies for Model-Based Inference. Reliab. Eng. Syst. Saf. 2006, 91, 1109–1125. [Google Scholar] [CrossRef]
- Wang, M.; Wright, J.; Brownlee, A.; Buswell, R. A Comparison of Approaches to Stepwise Regression on Variables Sensitivities in Building Simulation and Analysis. Energy Build. 2016, 127, 313–326. [Google Scholar] [CrossRef]
- Whittingham, M.J.; Stephens, P.A.; Bradbury, R.B.; Freckleton, R.P. Why Do We Still Use Stepwise Modelling in Ecology and Behaviour? Stepwise Modelling in Ecology and Behaviour. J. Anim. Ecol. 2006, 75, 1182–1189. [Google Scholar] [CrossRef]
- Sisman, S.; Aydinoglu, A.C. A Modelling Approach with Geographically Weighted Regression Methods for Determining Geographic Variation and Influencing Factors in Housing Price: A Case in Istanbul. Land Use Policy 2022, 119, 106183. [Google Scholar] [CrossRef]
- Craney, T.A.; Surles, J.G. Model-Dependent Variance Inflation Factor Cutoff Values. Qual. Eng. 2002, 14, 391–403. [Google Scholar] [CrossRef]
- Christopher, J.; Kutner, M.H.; Li, W.; Neter, J.; Kutner, M. Applied Linear Statistical Models, 5th ed.; Kutner, M.H., Ed.; The McGraw-Hill/Irwin Series Operations and Decision Sciences; McGraw-Hill Irwin: Boston, UK, 2005; ISBN 978-0-07-238688-2. [Google Scholar]
- Miles, J. Tolerance and Variance Inflation Factor. In Wiley StatsRef: Statistics Reference Online; Balakrishnan, N., Colton, T., Everitt, B., Piegorsch, W., Ruggeri, F., Teugels, J.L., Eds.; Wiley: Hoboken, NJ, USA, 2014; ISBN 978-1-118-44511-2. [Google Scholar]
- An, R.; Wu, Z.; Tong, Z.; Qin, S.; Zhu, Y.; Liu, Y. How the Built Environment Promotes Public Transportation in Wuhan: A Multiscale Geographically Weighted Regression Analysis. Travel Behav. Soc. 2022, 29, 186–199. [Google Scholar] [CrossRef]
- Huang, B.; Wu, B.; Barry, M. Geographically and Temporally Weighted Regression for Modeling Spatio-Temporal Variation in House Prices. Int. J. Geogr. Inf. Sci. 2010, 24, 383–401. [Google Scholar] [CrossRef]
- Ma, X.; Zhang, J.; Ding, C.; Wang, Y. A Geographically and Temporally Weighted Regression Model to Explore the Spatiotemporal Influence of Built Environment on Transit Ridership. Comput. Environ. Urban Syst. 2018, 70, 113–124. [Google Scholar] [CrossRef]
- Chu, H.-J.; Huang, B.; Lin, C.-Y. Modeling the Spatio-Temporal Heterogeneity in the PM10-PM2.5 Relationship. Atmos. Environ. 2015, 102, 176–182. [Google Scholar] [CrossRef]
- Fu, X.; Zhai, W. Examining the Spatial and Temporal Relationship between Social Vulnerability and Stay-at-Home Behaviors in New York City during the COVID-19 Pandemic. Sustain. Cities Soc. 2021, 67, 102757. [Google Scholar] [CrossRef]
- Chen, L.; Zhao, L.; Xiao, Y.; Lu, Y. Investigating the Spatiotemporal Pattern between the Built Environment and Urban Vibrancy Using Big Data in Shenzhen, China. Comput. Environ. Urban Syst. 2022, 95, 101827. [Google Scholar] [CrossRef]
- Fotheringham, A.S.; Brunsdon, C.; Charlton, M. Geographically Weighted Regression: The Analysis of Spatially Varying Relationships; Wiley: Chichester, UK; Hoboken, NJ, USA, 2002; ISBN 978-0-471-49616-8. [Google Scholar]
- Alcântara, E.; Mantovani, J.; Rotta, L.; Park, E.; Rodrigues, T.; Campos Carvalho, F.; Roberto Souza Filho, C. Investigating Spatiotemporal Patterns of the COVID-19 in São Paulo State, Brazil. Geospat. Health 2020, 15, 925. [Google Scholar] [CrossRef]
- Ghosh, P.; Cartone, A. A Spatio-temporal Analysis of COVID-19 Outbreak in Italy. Reg. Sci. Policy Pract. 2020, 12, 1047–1062. [Google Scholar] [CrossRef]
- Moran, P.A. The Interpretation of Statistical Maps. J. R. Stat. Soc. Ser. B (Methodol.) 1948, 10, 243–251. [Google Scholar] [CrossRef]
- Anselin, L. The Moran Scatterplot as an ESDA Tool to Assess Local Instability in Spatial Association. In Spatial Analytical Perspectives on GIS; Routledge: London, UK, 2019; pp. 111–126. [Google Scholar]
- Anselin, L. Spatial Econometrics: Methods and Models; Springer Science & Business Media: Berlin, Germany, 1988; Volume 4, ISBN 90-247-3735-4. [Google Scholar]
- Anselin, L. Local Indicators of Spatial Association—LISA. Geogr. Anal. 1995, 27, 93–115. [Google Scholar] [CrossRef]
- Scardaccione, G.; Scorza, F.; Casas, G.L.; Murgante, B. Spatial Autocorrelation Analysis for the Evaluation of Migration Flows: The Italian Case. In Proceedings of the Computational Science and Its Applications–ICCSA 2010: International Conference, Fukuoka, Japan, 23–26 March 2010; Part I 10. Springer: Berlin/Heidelberg, Germany, 2010; pp. 62–76. [Google Scholar]
- Leung, Y.; Mei, C.-L.; Zhang, W.-X. Testing for Spatial Autocorrelation among the Residuals of the Geographically Weighted Regression. Environ. Plan. A 2000, 32, 871–890. [Google Scholar] [CrossRef]
- Chen, Y. Spatial Autocorrelation Approaches to Testing Residuals from Least Squares Regression. PLoS ONE 2016, 11, e0146865. [Google Scholar] [CrossRef]
- Ma, X.; Ji, Y.; Yuan, Y.; Van Oort, N.; Jin, Y.; Hoogendoorn, S. A Comparison in Travel Patterns and Determinants of User Demand between Docked and Dockless Bike-Sharing Systems Using Multi-Sourced Data. Transp. Res. Part A Policy Pract. 2020, 139, 148–173. [Google Scholar] [CrossRef]
- Ma, J.; Zhu, H.; Li, P.; Liu, C.; Li, F.; Luo, Z.; Zhang, M.; Li, L. Spatial Patterns of the Spread of COVID-19 in Singapore and the Influencing Factors. IJGI 2022, 11, 152. [Google Scholar] [CrossRef]
- Zhang, L.; Ma, Z.; Guo, L. An Evaluation of Spatial Autocorrelation and Heterogeneity in the Residuals of Six Regression Models. For. Sci. 2009, 55, 533–548. [Google Scholar]
- Griffith, D.; Chun, Y. Evaluating Eigenvector Spatial Filter Corrections for Omitted Georeferenced Variables. Econometrics 2016, 4, 29. [Google Scholar] [CrossRef]
- Burnham, K.P.; Anderson, D.R.; Huyvaert, K.P. AIC Model Selection and Multimodel Inference in Behavioral Ecology: Some Background, Observations, and Comparisons. Behav. Ecol. Sociobiol. 2011, 65, 23–35. [Google Scholar] [CrossRef]
- Baguley, T. Serious Stats: A Guide to Advanced Statistics for the Behavioral Sciences; Palgrave Macmillan: Basingstoke, UK; New York, NY, USA, 2012; ISBN 978-0-230-57717-6. [Google Scholar]
- Liu, J.; Liu, M.; Liang, W.; School of Public Health, Peking University, Beijing, China; Vanke School of Public Health, Tsinghua University, Beijing, China; Institute for Healthy China, Tsinghua University, Beijing, China. The Dynamic COVID-Zero Strategy in China. China CDC Wkly. 2022, 4, 74–75. [Google Scholar] [CrossRef]
- Zhang, X.; Zhang, W.; Chen, S. Shanghai’s Life-Saving Efforts against the Current Omicron Wave of the COVID-19 Pandemic. Lancet 2022, 399, 2011–2012. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Jiang, H.; Wang, Q.; Yang, M.; Chen, Y.; Jiang, Q. Use of Contact Tracing, Isolation, and Mass Testing to Control Transmission of COVID-19 in China. BMJ 2021, 375, n2330. [Google Scholar] [CrossRef]
- Cheshmehzangi, A.; Zou, T.; Su, Z. Commentary: China’s Zero-COVID Approach Depends on Shanghai’s Outbreak Control. Front. Public Health 2022, 10, 912992. [Google Scholar] [CrossRef]
- Chen, Z.; Deng, X.; Fang, L.; Sun, K.; Wu, Y.; Che, T.; Zou, J.; Cai, J.; Liu, H.; Wang, Y.; et al. Epidemiological Characteristics and Transmission Dynamics of the Outbreak Caused by the SARS-CoV-2 Omicron Variant in Shanghai, China: A Descriptive Study. Lancet Reg. Health—West. Pac. 2022, 29, 100592. [Google Scholar] [CrossRef]
- Cai, J.; Deng, X.; Yang, J.; Sun, K.; Liu, H.; Chen, Z.; Peng, C.; Chen, X.; Wu, Q.; Zou, J.; et al. Modeling Transmission of SARS-CoV-2 Omicron in China. Nat. Med. 2022, 28, 1468–1475. [Google Scholar] [CrossRef]
- Baobeid, A.; Koç, M.; Al-Ghamdi, S.G. Walkability and Its Relationships With Health, Sustainability, and Livability: Elements of Physical Environment and Evaluation Frameworks. Front. Built Environ. 2021, 7, 721218. [Google Scholar] [CrossRef]
- Lee, K.O.; Mai, K.M.; Park, S. Green Space Accessibility Helps Buffer Declined Mental Health during the COVID-19 Pandemic: Evidence from Big Data in the United Kingdom. Nat. Ment. Health 2023, 1, 124–134. [Google Scholar] [CrossRef]
- Jiang, B.; Yang, Y.; Chen, L.; Liu, X.; Wu, X.; Chen, B.; Webster, C.; Sullivan, W.C.; Larsen, L.; Wang, J.; et al. Green Spaces, Especially Nearby Forest, May Reduce the SARS-CoV-2 Infection Rate: A Nationwide Study in the United States. Landsc. Urban Plan. 2022, 228, 104583. [Google Scholar] [CrossRef]
- Almagro, M.; Orane-Hutchinson, A. JUE Insight: The Determinants of the Differential Exposure to COVID-19 in New York City and Their Evolution over Time. J. Urban Econ. 2022, 127, 103293. [Google Scholar] [CrossRef]
- Malik, O.; Gong, B.; Moussawi, A.; Korniss, G.; Szymanski, B.K. Modelling Epidemic Spread in Cities Using Public Transportation as a Proxy for Generalized Mobility Trends. Sci. Rep. 2022, 12, 6372. [Google Scholar] [CrossRef] [PubMed]
- Hu, M.; Roberts, J.D.; Azevedo, G.P.; Milner, D. The Role of Built and Social Environmental Factors in COVID-19 Transmission: A Look at America’s Capital City. Sustain. Cities Soc. 2021, 65, 102580. [Google Scholar] [CrossRef]
- Jin, X.; Leng, Y.; Gong, E.; Xiong, S.; Yao, Y.; Vedanthan, R.; Wu, C.; Yan, L.L. Neighborhood-Level Public Facilities and COVID-19 Transmission: A Nationwide Geospatial Study in China. medRxiv 2020. [Google Scholar]
- Li, W.; Zhao, S.; Ji, X.; Ma, J. Impact of Traffic Exposure and Land Use Patterns on the Risk of COVID-19 Spread at the Community Level. China J. Highw. Transp. 2020, 33, 43–54. [Google Scholar] [CrossRef]
- Wali, B.; Frank, L.D. Neighborhood-Level COVID-19 Hospitalizations and Mortality Relationships with Built Environment, Active and Sedentary Travel. Health Place 2021, 71, 102659. [Google Scholar] [CrossRef]
- Johnson, T.F.; Hordley, L.A.; Greenwell, M.P.; Evans, L.C. Associations between COVID-19 Transmission Rates, Park Use, and Landscape Structure. Sci. Total Environ. 2021, 789, 148123. [Google Scholar] [CrossRef]
- You, Y.; Pan, S. Urban Vegetation Slows down the Spread of Coronavirus Disease (COVID-19) in the United States. Geophys. Res. Lett. 2020, 47, e2020GL089286. [Google Scholar] [CrossRef]
- Angel, S.; Lamson-Hall, P.; Salazar Tamayo, M.M. Coronavirus and the Cities: Explaining Variations in the Onset of Infection and in the Number of Reported Cases and Deaths in US Metropolitan Areas as of 27 March 2020; New York University, Marron Institute of Urban Management: New York, NY, USA, 2020. [Google Scholar]
- Gatto, M.; Bertuzzo, E.; Mari, L.; Miccoli, S.; Carraro, L.; Casagrandi, R.; Rinaldo, A. Spread and Dynamics of the COVID-19 Epidemic in Italy: Effects of Emergency Containment Measures. Proc. Natl. Acad. Sci. USA 2020, 117, 10484–10491. [Google Scholar] [CrossRef] [PubMed]
- Pierantoni, I.; Pierantozzi, M.; Sargolini, M. COVID 19—A Qualitative Review for the Reorganization of Human Living Environments. Appl. Sci. 2020, 10, 5576. [Google Scholar] [CrossRef]
- Andersen, L.M.; Harden, S.R.; Sugg, M.M.; Runkle, J.D.; Lundquist, T.E. Analyzing the Spatial Determinants of Local COVID-19 Transmission in the United States. Sci. Total Environ. 2021, 754, 142396. [Google Scholar] [CrossRef] [PubMed]
- Yu, D.; Li, X.; Yu, J.; Shi, X.; Liu, P.; Tian, P. Whether Urbanization Has Intensified the Spread of Infectious Diseases—Renewed Question by the COVID-19 Pandemic. Front. Public Health 2021, 9, 699710. [Google Scholar] [CrossRef] [PubMed]
- Zhang, N.; Jia, W.; Wang, P.; Dung, C.-H.; Zhao, P.; Leung, K.; Su, B.; Cheng, R.; Li, Y. Changes in Local Travel Behaviour before and during the COVID-19 Pandemic in Hong Kong. Cities 2021, 112, 103139. [Google Scholar] [CrossRef]
- Thaithatkul, P.; Sanghatawatana, P.; Anuchitchanchai, O.; Laosinwattana, W.; Liang, J.; Chalermpong, S. Travel Behavior Change of Public Transport Users during the COVID-19 Pandemic: Evidence from Bangkok. Asian Transp. Stud. 2023, 9, 100102. [Google Scholar] [CrossRef]
- Aydin, N.; Kuşakcı, A.O.; Deveci, M. The Impacts of COVID-19 on Travel Behavior and Initial Perception of Public Transport Measures in Istanbul. Decis. Anal. J. 2022, 2, 100029. [Google Scholar] [CrossRef]
- Oishi, S.; Cha, Y.; Schimmack, U. The Social Ecology of COVID-19 Cases and Deaths in New York City: The Role of Walkability, Wealth, and Race. Soc. Psychol. Personal. Sci. 2021, 12, 1457–1466. [Google Scholar] [CrossRef]
- Wang, Y.; Tsai, T.C.; Duncan, D.; Ji, J. Association of City-Level Walkability, Accessibility to Biking and Public Transportation and Socio-Economic Features with COVID-19 Infection in Massachusetts, USA: An Ecological Study. Geospat. Health 2022, 17, s1. [Google Scholar] [CrossRef]
- Wang, S.; Luo, X. The Evolution of Government Behaviors and Urban Expansion in Shanghai. Land Use Policy 2022, 114, 105973. [Google Scholar] [CrossRef]
- Hamidi, S.; Ewing, R.; Sabouri, S. Longitudinal Analyses of the Relationship between Development Density and the COVID-19 Morbidity and Mortality Rates: Early Evidence from 1,165 Metropolitan Counties in the United States. Health Place 2020, 64, 102378. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, A.; Nundy, S.; Ghosh, S.; Mallick, T.K. Study of COVID-19 Pandemic in London (UK) from Urban Context. Cities 2020, 106, 102928. [Google Scholar] [CrossRef] [PubMed]
- Mansour, S.; Al Kindi, A.; Al-Said, A.; Al-Said, A.; Atkinson, P. Sociodemographic Determinants of COVID-19 Incidence Rates in Oman: Geospatial Modelling Using Multiscale Geographically Weighted Regression (MGWR). Sustain. Cities Soc. 2021, 65, 102627. [Google Scholar] [CrossRef]
- Gaskin, D.J.; Zare, H.; Delarmente, B.A. Geographic Disparities in COVID-19 Infections and Deaths: The Role of Transportation. Transp. Policy 2021, 102, 35–46. [Google Scholar] [CrossRef] [PubMed]
- Tribby, C.P.; Hartmann, C. COVID-19 Cases and the Built Environment: Initial Evidence from New York City. Prof. Geogr. 2021, 73, 365–376. [Google Scholar] [CrossRef]
- Kim, D. Exploratory Study on the Spatial Relationship between Emerging Infectious Diseases and Urban Characteristics: Cases from Korea. Sustain. Cities Soc. 2021, 66, 102672. [Google Scholar] [CrossRef]



| Classification | Variable | Calculation Process | |
|---|---|---|---|
| Density | Population density | Total population divided by area. | |
| Building density | Building square footage divided by area. | ||
| Green space density | (1) | ||
| where Xk (k = 1, 2, …, n) denotes the area of a single green space, n indicates the number of green spaces within the same subdistrict/town, and Aj measures the area of subdistrict/town j. | |||
| Density of road length | (2) | ||
| where Xk (k = 1, 2, …, n) denotes the length of a single road segment after being divided by administrative boundaries of subdistrict/town j, n indicates the number of roads within the same subdistrict/town, and Aj measures the area of subdistrict/town j. | |||
| Density of bus line length | (3) | ||
| where Xk (k = 1, 2, …, n) denotes the length of a single bus line segment after being divided by administrative boundaries of subdistrict/town j, n indicates the number of bus lines within the same subdistrict/town, and Aj measures the area of subdistrict/town j. | |||
| Density of metro line length | (4) | ||
| where Xk (k = 1, 2, …, n) denotes the length of a single metro line segment after being divided by administrative boundaries of subdistrict/town j, n indicates the number of metro lines within the same subdistrict/town, and Aj measures the area of subdistrict/town j. | |||
| Density of bus stop/metro station/road intersection | (5) | ||
| where N indicates the number of bus stops/metro stations/road intersections within the subdistrict/town j, and Aj measures the area (unit: km2) of subdistrict/town j. The unit used is number/km2. | |||
| Density of 12 categories * of POI datasets | (6) | ||
| where N indicates the number of category k points within the subdistrict/town j, and Aj measures the area (unit: km2) of subdistrict/town j. The unit used number/km2. | |||
| Design | Quantity of road length/bus line/metro line/bust stop/metro station/road intersection | The quantity of road length/bus line length/metro line length was measured as the total length of road/bus line/metro line within each subdistrict or town, while the quantity of bus stop/metro station/street intersection was the number of street intersections in each subdistrict. | |
| Green space area, waterbody area | The total area of polygons with green space and waterbody attributes was calculated within the subdistrict/town area. | ||
| Quantity of 12 categories * of POI datasets | The amount of 12 categories of POIs within each subdistrict was counted separately. | ||
| Destination accessibility | Accessibility to hospital/clinic, accessibility to kindergarten/school, commuting accessibility, accessibility to park | Opportunity-based measures could simply be to find the nearest destinations to an origin and calculate their distances or to count the number of destinations or opportunities available within a specified distance from an origin [59,60,61,62]. | |
| (7) | |||
| Walk accessibility, drive accessibility, radius setting: 500 meters and 10 kilometers | Betweenness was utilized to describe the road network accessibility [63]. It computes the number of times each street x is traversed by the shortest path between any two street segments, y and z, within a defined analysis radius. | ||
| (8) | |||
| where | (9) | ||
| Distance to transit | Distance to bus stop/metro station | (10) | |
| p(y) represents the weight of node y within a radius of R in the equation, where p(y) takes on values between 0 and 1. d (x, y) is the minimum topological distance between nodes x and y. In our study, p(x) indicates the community, p(y) depicts the metro station or bus stop, and R is 1 kilometer or 15 minutes of walking. | |||
| Diversity of land use | Land use mix | The Shannon Entropy Index was used to quantify the land use mix [64]: | |
| (11) | |||
| where Pk, i is the quantity of POIs within subdistrict k, which belongs to sub-category i as a percentage of the total amount of POIs in subdistrict k and denotes the number of POI sub-categories in subdistrict k. | |||
| OLS | GWR | GTWR | |
|---|---|---|---|
| Moran’s Index: | 0.050 | −0.022 | −0.001 |
| Expected Index: | −0.005 | −0.005 | −0.001 |
| Variance: | 0.000 | 0.000 | 0.000 |
| z-score: | 4.112 | −1.924 | 0.160 |
| p-value: | 0.000 | 0.054 | 0.873 |
| Pattern: | Clustered | Dispersed | Random |
| Unstandardized Coefficients | Standardized Coefficients | ||||||
|---|---|---|---|---|---|---|---|
| Variable | B | SE | Beta | t | Sig. | Tolerance | VIF |
| (Constant) | −0.139 | 0.053 | −2.630 | 0.009 ** | |||
| Walking accessibility | 0.463 | 0.075 | 0.510 | 6.166 | 0.000 *** | 0.220 | 4.542 |
| Population of subdistrict | 0.444 | 0.062 | 0.469 | 7.114 | 0.000 *** | 0.348 | 2.876 |
| Healthcare accessibility | −0.083 | 0.038 | −0.129 | −2.183 | 0.300 * | 0.430 | 2.327 |
| Length of metro lines | 0.265 | 0.063 | 0.263 | 4.236 | 0.000 *** | 0.392 | 2.554 |
| Density of hotel and inn | 0.434 | 0.103 | 0.326 | 4.217 | 0.000 *** | 0.253 | 3.954 |
| Density of metro lines | −0.172 | 0.056 | −0.243 | −3.046 | 0.003 ** | 0.237 | 4.216 |
| Number of scenic spots | −0.137 | 0.045 | −0.154 | −3.060 | 0.003 ** | 0.596 | 1.677 |
| Land use mix | 0.138 | 0.052 | 0.127 | 2.649 | 0.009 ** | 0.657 | 1.522 |
| Commuting accessibility | 0.100 | 0.045 | 0.109 | 2.217 | 0.028 * | 0.624 | 1.603 |
| OLS | GWR | GTWR | |
|---|---|---|---|
| R2 | 0.688 | 0.787 | 0.854 |
| Adjusted R2 | 0.673 | 0.776 | 0.853 |
| RSS | 1.915 | 1.314 | 1.714 |
| AICc 1 | −391.54 | −392.81 | −3610.16 |
| Variable | AVG | MIN | MAX | LQ | MED | UQ | SD |
|---|---|---|---|---|---|---|---|
| Intercept | −0.032 | −0.197 | 0.011 | −0.030 | −0.015 | 0.000 | 0.049 |
| Length of metro lines | 0.065 | −0.008 | 0.295 | −0.001 | 0.021 | 0.065 | 0.097 |
| Density of metro lines | −0.041 | −0.162 | 0.007 | −0.050 | −0.018 | 0.000 | 0.056 |
| Number of scenic spots | −0.032 | −0.168 | 0.000 | −0.053 | −0.018 | 0.000 | 0.039 |
| Hotel and inn density | 0.107 | −0.007 | 0.671 | 0.000 | 0.021 | 0.126 | 0.152 |
| Healthcare facilities accessibility | −0.024 | −0.181 | 0.002 | −0.024 | −0.002 | −0.001 | 0.037 |
| Commuting accessibility | −0.022 | −0.005 | 0.149 | 0.000 | 0.005 | 0.018 | 0.036 |
| Walking accessibility | 0.111 | −0.026 | 0.141 | 0.000 | 0.032 | 0.141 | 0.150 |
| Land use mix | 0.033 | −0.014 | 0.203 | −0.000 | 0.020 | 0.031 | 0.048 |
| Population of Subdistrict or Town | 0.114 | 0.001 | 0.487 | 0.003 | 0.070 | 0.100 | 0.153 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, H.; Shi, H.; Zordan, M.; Lo, S.M.; Tsou, J.Y. Investigating the Spatiotemporal Relationship between the Built Environment and COVID-19 Transmission. ISPRS Int. J. Geo-Inf. 2023, 12, 390. https://doi.org/10.3390/ijgi12100390
Huang H, Shi H, Zordan M, Lo SM, Tsou JY. Investigating the Spatiotemporal Relationship between the Built Environment and COVID-19 Transmission. ISPRS International Journal of Geo-Information. 2023; 12(10):390. https://doi.org/10.3390/ijgi12100390
Chicago/Turabian StyleHuang, Hao, Haochen Shi, Mirna Zordan, Siu Ming Lo, and Jin Yeu Tsou. 2023. "Investigating the Spatiotemporal Relationship between the Built Environment and COVID-19 Transmission" ISPRS International Journal of Geo-Information 12, no. 10: 390. https://doi.org/10.3390/ijgi12100390
APA StyleHuang, H., Shi, H., Zordan, M., Lo, S. M., & Tsou, J. Y. (2023). Investigating the Spatiotemporal Relationship between the Built Environment and COVID-19 Transmission. ISPRS International Journal of Geo-Information, 12(10), 390. https://doi.org/10.3390/ijgi12100390








