The Longevity Protein Klotho: A Promising Tool to Monitor Lifestyle Improvements
Abstract
1. Introduction
2. A Marker to Rule them All: Klotho, the Longevity Protein
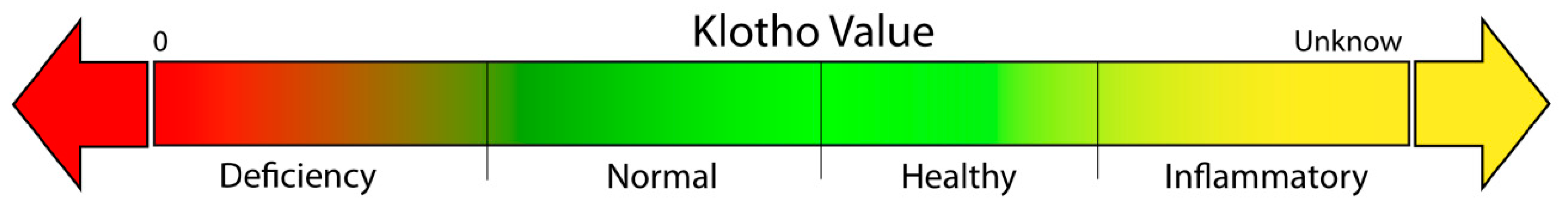
2.1. Potential Healthspan Biomarker
2.2. Molecular Biology of Klotho
2.3. Klotho and the Pillars of Lifestyle Medicine
2.3.1. Nutrition
2.3.2. Physical Activity
2.3.3. Stress Management
2.3.4. Restorative Sleep
2.3.5. Social Connection
2.3.6. Avoidance of Risky Substances
Tobacco
Alcohol
Drugs
2.3.7. Holistic Integration of Klotho
3. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- World Health Statistics 2022: Monitoring Health for the SDGs, Sustainable Development Goals; World Health Organization: Geneva, Switzerland, 2022; p. 125.
- Health and Economic Costs of Chronic Diseases. Available online: https://www.cdc.gov/chronicdisease/about/costs/index.htm (accessed on 6 July 2023).
- Li, Y.; Pan, A.; Wang, D.D.; Liu, X.; Dhana, K.; Franco, O.H.; Kaptoge, S.; Di Angelantonio, E.; Stampfer, M.; Willett, W.C.; et al. Impact of Healthy Lifestyle Factors on Life Expectancies in the US Population. Circulation 2018, 138, 345–355. [Google Scholar] [CrossRef]
- Hu, Y.; He, H.; Ou, Q.; Nai, J.; Pan, L.; Chen, X.; Tu, J.; Zeng, X.; Pei, G.; Wang, L.; et al. Prevalence of common chronic disease and multimorbidity patterns in Guangdong province with three typical cultures: Analysis of data from the Diverse Life-Course Cohort study. Front. Public Health 2023, 11, 1163791. [Google Scholar] [CrossRef] [PubMed]
- Longo, P.L.; de Aquino, R.C.; Ortiz, S.R.M.; de Oliveira, R.S.; Gavioli, A.; do Amaral, J.B.; Monteiro, F.R.; de Almeida Franco, R.R.; Mereu, G.R.; Bachi, A.L.L.; et al. Effects of physical distancing by COVID-19 pandemic on diet quality, neurological and immunological markers, and fecal microbiota of Brazilian older women. Front. Nutr. 2022, 9, 972100. [Google Scholar] [CrossRef] [PubMed]
- McHugh, J.; Dalal, M.; Agarwal, N. From Preconception Care to the First Day of School: Transforming the Health of New Families with Lifestyle Medicine. Am. J. Lifestyle Med. 2020, 14, 532–540. [Google Scholar] [CrossRef] [PubMed]
- Furrer, R.; Handschin, C. Drugs, clocks and exercise in ageing: Hype and hope, fact and fiction. J. Physiol. 2023, 601, 2057–2068. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Schoufour, J.; Wang, D.D.; Dhana, K.; Pan, A.; Liu, X.; Song, M.; Liu, G.; Shin, H.J.; Sun, Q.; et al. Healthy lifestyle and life expectancy free of cancer, cardiovascular disease, and type 2 diabetes: Prospective cohort study. BMJ 2020, 368, l6669. [Google Scholar] [CrossRef] [PubMed]
- Garmany, A.; Yamada, S.; Terzic, A. Longevity leap: Mind the healthspan gap. NPJ Regen. Med. 2021, 6, 57. [Google Scholar] [CrossRef]
- Levine, M.E.; Lu, A.T.; Quach, A.; Chen, B.H.; Assimes, T.L.; Bandinelli, S.; Hou, L.; Baccarelli, A.A.; Stewart, J.D.; Li, Y.; et al. An epigenetic biomarker of aging for lifespan and healthspan. Aging 2018, 10, 573–591. [Google Scholar] [CrossRef]
- Wang, S.; Prizment, A.; Moshele, P.; Vivek, S.; Blaes, A.H.; Nelson, H.H.; Thyagarajan, B. Aging measures and cancer: Findings from the Health and Retirement Study. medRxiv 2023. [Google Scholar] [CrossRef]
- Branca, F.; Hanley, A.B.; Pool-Zobel, B.; Verhagen, H. Biomarkers in disease and health. Br. J. Nutr. 2001, 86 (Suppl. S1), S55–S92. [Google Scholar] [CrossRef]
- Dorcely, B.; Katz, K.; Jagannathan, R.; Chiang, S.S.; Oluwadare, B.; Goldberg, I.J.; Bergman, M. Novel biomarkers for prediabetes, diabetes, and associated complications. Diabetes Metab. Syndr. Obes. 2017, 10, 345–361. [Google Scholar] [CrossRef] [PubMed]
- Patschan, D.; Patschan, S.; Matyukhin, I.; Ritter, O.; Dammermann, W. Metabolomics in Acute Kidney Injury: The Clinical Perspective. J. Clin. Med. 2023, 12, 4083. [Google Scholar] [CrossRef]
- Goevaerts, W.F.; Tenbult-van Limpt, N.; Kop, W.J.; Birk, M.V.; Liu, Y.; Brouwers, R.W.M.; Lu, Y.; Kemps, H.M.C. Adherence to a lifestyle monitoring system in patients with heart disease: Protocol for the care-on prospective observational trial. BMC Cardiovasc. Disord. 2023, 23, 196. [Google Scholar] [CrossRef] [PubMed]
- Schaefer, E.J.; Tsunoda, F.; Diffenderfer, M.; Polisecki, E.; Thai, N.; Asztalos, B. The Measurement of Lipids, Lipoproteins, Apolipoproteins, Fatty Acids, and Sterols, and Next Generation Sequencing for the Diagnosis and Treatment of Lipid Disorders. In Endotext; Feingold, K.R., Anawalt, B., Blackman, M.R., Boyce, A., Chrousos, G., Corpas, E., de Herder, W.W., Dhatariya, K., Dungan, K., Hofland, J., et al., Eds.; MDText.com Inc.: South Dartmouth, MA, USA, 2000. [Google Scholar]
- Casadei, K.; Kiel, J. Anthropometric Measurement; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Mathew, T.K.; Zubair, M.; Tadi, P. Blood Glucose Monitoring; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Kong, L.J.; Ye, C.J.; Wang, Y.Y.; Hou, T.Z.C.; Zheng, J.; Zhao, Z.Y.; Li, M.; Xu, Y.; Lu, J.L.; Chen, Y.H.; et al. Genetic Evidence for Causal Effects of Socioeconomic, Lifestyle, and Cardiometabolic Factors on Epigenetic-Age Acceleration. J. Gerontol.-Biol. 2023, 78, 1083–1091. [Google Scholar] [CrossRef]
- Donate-Correa, J.; Martin-Carro, B.; Cannata-Andia, J.B.; Mora-Fernandez, C.; Navarro-Gonzalez, J.F. Klotho, Oxidative Stress, and Mitochondrial Damage in Kidney Disease. Antioxidants 2023, 12, 239. [Google Scholar] [CrossRef]
- Arroyo, E.; Troutman, A.D.; Moorthi, R.N.; Avin, K.G.; Coggan, A.R.; Lim, K. Klotho: An Emerging Factor with Ergogenic Potential. Front. Rehabil. Sci. 2021, 2, 807123. [Google Scholar] [CrossRef] [PubMed]
- Espuch-Oliver, A.; Vazquez-Lorente, H.; Jurado-Fasoli, L.; de Haro-Munoz, T.; Diaz-Alberola, I.; Lopez-Velez, M.D.S.; de Haro-Romero, T.; Castillo, M.J.; Amaro-Gahete, F.J. References Values of Soluble alpha-Klotho Serum Levels Using an Enzyme-Linked Immunosorbent Assay in Healthy Adults Aged 18–85 Years. J. Clin. Med. 2022, 11, 2415. [Google Scholar] [CrossRef]
- Prud’homme, G.J.; Kurt, M.; Wang, Q. Pathobiology of the Klotho Antiaging Protein and Therapeutic Considerations. Front. Aging 2022, 3, 931331. [Google Scholar] [CrossRef]
- Abraham, C.R.; Li, A. Aging-suppressor Klotho: Prospects in diagnostics and therapeutics. Ageing Res. Rev. 2022, 82, 101766. [Google Scholar] [CrossRef]
- Amaro-Gahete, F.J.; de-la-O, A.; Jurado-Fasoli, L.; Ruiz, J.R.; Castillo, M.J.; Gutierrez, A. Role of Exercise on S-Klotho Protein Regulation: A Systematic Review. Curr. Aging Sci. 2018, 11, 100–107. [Google Scholar] [CrossRef]
- Trošt, N.; Peña-Llopis, S.; Koirala, S.; Stojan, J.; Potts, P.R.; Fon Tacer, K.; Martinez, E.D. Correction: γKlotho is a novel marker and cell survival factor in a subset of triple negative breast cancers. Oncotarget 2019, 10, 916. [Google Scholar] [CrossRef]
- Aczel, D.; Torma, F.; Jokai, M.; McGreevy, K.; Boros, A.; Seki, Y.; Boldogh, I.; Horvath, S.; Radak, Z. The Circulating Level of Klotho Is Not Dependent upon Physical Fitness and Age-Associated Methylation Increases at the Promoter Region of the Klotho Gene. Genes 2023, 14, 525. [Google Scholar] [CrossRef]
- Fung, T.Y.; Iyaswamy, A.; Sreenivasmurthy, S.G.; Krishnamoorthi, S.; Guan, X.J.; Zhu, Z.; Su, C.F.; Liu, J.; Kan, Y.X.; Zhang, Y.; et al. Klotho an Autophagy Stimulator as a Potential Therapeutic Target for Alzheimer’s Disease: A Review. Biomedicines 2022, 10, 705. [Google Scholar] [CrossRef] [PubMed]
- Jurado-Fasoli, L.; Amaro-Gahete, F.J.; De-la-O, A.; Gutierrez, A.; Castillo, M.J. Alcohol consumption and S-Klotho plasma levels in sedentary healthy middle-aged adults: A cross sectional study. Drug Alcohol. Depend. 2019, 194, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Kundu, P.; Zimmerman, B.; Quinn, J.F.; Kaye, J.; Mattek, N.; Westaway, S.K.; Raber, J. Serum Levels of alpha-Klotho Are Correlated with Cerebrospinal Fluid Levels and Predict Measures of Cognitive Function. J. Alzheimers Dis. 2022, 86, 1471–1481. [Google Scholar] [CrossRef]
- Kuro-o, M.; Matsumura, Y.; Aizawa, H.; Kawaguchi, H.; Suga, T.; Utsugi, T.; Ohyama, Y.; Kurabayashi, M.; Kaname, T.; Kume, E.; et al. Mutation of the mouse klotho gene leads to a syndrome resembling ageing. Nature 1997, 390, 45–51. [Google Scholar] [CrossRef]
- Zelazniewicz, A.; Nowak-Kornicka, J.; Pawlowski, B. S-Klotho level and physiological markers of cardiometabolic risk in healthy adult men. Aging 2022, 14, 708–727. [Google Scholar] [CrossRef] [PubMed]
- Kurosu, H.; Yamamoto, M.; Clark, J.D.; Pastor, J.V.; Nandi, A.; Gurnani, P.; McGuinness, O.P.; Chikuda, H.; Yamaguchi, M.; Kawaguchi, H.; et al. Suppression of aging in mice by the hormone Klotho. Science 2005, 309, 1829–1833. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Zhang, Z.; Li, J.; Deng, L.; Geng, J.; Jin, K.; Zheng, X.; Qiu, S.; Dong, B. Association between Dietary Inflammatory Index and serum Klotho concentration among adults in the United States. BMC Geriatr. 2022, 22, 528. [Google Scholar] [CrossRef] [PubMed]
- Du, S.; Zheng, H. Role of FoxO transcription factors in aging and age-related metabolic and neurodegenerative diseases. Cell Biosci. 2021, 11, 188. [Google Scholar] [CrossRef] [PubMed]
- Du, C.H.; Wang, X.M.; Wu, Y.D.; Liao, W.N.; Xiong, J.C.; Zhu, Y.G.; Liu, C.N.; Han, W.H.; Wang, Y.; Han, S.L.; et al. Renal Klotho and inorganic phosphate are extrinsic factors that antagonistically regulate hematopoietic stem cell maintenance. Cell Rep. 2022, 38, 110392. [Google Scholar] [CrossRef] [PubMed]
- Benigas, S.; Shurney, D.; Stout, R. Making the Case for Lifestyle Medicine. J. Fam. Pract. 2022, 71, S2–S4. [Google Scholar] [CrossRef]
- Chen, Y.; Michalak, M.; Agellon, L.B. Importance of Nutrients and Nutrient Metabolism on Human Health. Yale J. Biol. Med. 2018, 91, 95–103. [Google Scholar] [PubMed]
- Cui, J.W.; Yang, Z.Z.; Wang, J.H.; Yin, S.; Xiao, Y.F.; Bai, Y.J.; Wang, J. A cross-sectional analysis of association between visceral adiposity index and serum anti-aging protein Klotho in adults. Front. Endocrinol. 2023, 14, 1082504. [Google Scholar] [CrossRef]
- Shen, W.; Punyanitya, M.; Chen, J.; Gallagher, D.; Albu, J.; Pi-Sunyer, X.; Lewis, C.E.; Grunfeld, C.; Heshka, S.; Heymsfield, S.B. Waist circumference correlates with metabolic syndrome indicators better than percentage fat. Obesity 2006, 14, 727–736. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.W.; Hung, C.C.; Fang, W.H.; Chen, W.L. Association between Soluble alpha-Klotho Protein and Metabolic Syndrome in the Adult Population. Biomolecules 2022, 12, 70. [Google Scholar] [CrossRef] [PubMed]
- Goel, K.; Misra, A.; Vikram, N.K.; Poddar, P.; Gupta, N. Subcutaneous abdominal adipose tissue is associated with the metabolic syndrome in Asian Indians independent of intra-abdominal and total body fat. Heart 2010, 96, 579–583. [Google Scholar] [CrossRef] [PubMed]
- Ozhan, H.; Alemdar, R.; Caglar, O.; Ordu, S.; Kaya, A.; Albayrak, S.; Turker, Y.; Bulur, S.; Investigators, M. Performance of bioelectrical impedance analysis in the diagnosis of metabolic syndrome. J. Investig. Med. 2012, 60, 587–591. [Google Scholar] [CrossRef]
- Holmes, C.J.; Racette, S.B. The Utility of Body Composition Assessment in Nutrition and Clinical Practice: An Overview of Current Methodology. Nutrients 2021, 13, 2493. [Google Scholar] [CrossRef]
- Ostojic, S.M.; Engeset, D. Improving Brain Creatine Uptake by Klotho Protein Stimulation: Can Diet Hit the Big Time? Front. Nutr. 2021, 8, 795599. [Google Scholar] [CrossRef] [PubMed]
- Ma, T.C.; Zhou, J.; Wang, C.X.; Lin, Z.Z.; Gao, F. Associations between the Healthy Eating Index-2015 and S-Klotho plasma levels: A cross-sectional analysis in middle-to-older aged adults. Front. Nutr. 2022, 9, 904745. [Google Scholar] [CrossRef] [PubMed]
- Krebs-Smith, S.M.; Pannucci, T.E.; Subar, A.F.; Kirkpatrick, S.I.; Lerman, J.L.; Tooze, J.A.; Wilson, M.M.; Reedy, J. Update of the Healthy Eating Index: HEI-2015. J. Acad. Nutr. Diet. 2018, 118, 1591–1602. [Google Scholar] [CrossRef]
- Wu, S.E.; Chen, Y.J.; Chen, W.L. Adherence to Mediterranean Diet and Soluble Klotho Level: The Value of Food Synergy in Aging. Nutrients 2022, 14, 3910. [Google Scholar] [CrossRef] [PubMed]
- Jurado-Fasoli, L.; Amaro-Gahete, F.J.; De-la-O, A.; Martinez-Tellez, B.; Ruiz, J.R.; Gutierrez, A.; Castillo, M.J. Adherence to the Mediterranean diet, dietary factors, and S-Klotho plasma levels in sedentary middle-aged adults. Exp. Gerontol. 2019, 119, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Mou, L.; Yang, F.; Tu, H.; Lin, W. Curcumin attenuates cyclosporine A-induced renal fibrosis by inhibiting hypermethylation of the klotho promoter. Mol. Med. Rep. 2016, 14, 3229–3236. [Google Scholar] [CrossRef] [PubMed][Green Version]
- He, H.; Chen, X.; Miao, D.; Zhang, H.; Wang, Y.; He, X.; Chen, X.; Dai, N. Composite Dietary Antioxidant Index and Plasma Levels of Soluble Klotho: Insights from NHANES. Oxid. Med. Cell Longev. 2023, 2023, 3524611. [Google Scholar] [CrossRef]
- Forster, R.E.; Jurutka, P.W.; Hsieh, J.C.; Haussler, C.A.; Lowmiller, C.L.; Kaneko, I.; Haussler, M.R.; Kerr Whitfield, G. Vitamin D receptor controls expression of the anti-aging klotho gene in mouse and human renal cells. Biochem. Biophys. Res. Commun. 2011, 414, 557–562. [Google Scholar] [CrossRef]
- Azimzadeh, M.J.; Shidfar, F.; Jazayeri, S.; Hosseini, A.F.; Ranjbaran, F. Effect of vitamin D supplementation on klotho protein, antioxidant status and nitric oxide in the elderly: A randomized, double-blinded, placebo-controlled clinical trial. Eur. J. Integr. Med. 2020, 35, 101089. [Google Scholar] [CrossRef]
- Dermaku-Sopjani, M.; Kurti, F.; Xuan, N.T.; Sopjani, M. Klotho-Dependent Role of 1,25(OH)(2)D(3) in the Brain. Neurosignals 2021, 29, 14–23. [Google Scholar] [CrossRef]
- Luthra, N.S.; Clow, A.; Corcos, D.M. The Interrelated Multifactorial Actions of Cortisol and Klotho: Potential Implications in the Pathogenesis of Parkinson’s Disease. Brain Sci. 2022, 12, 1695. [Google Scholar] [CrossRef]
- Tsujikawa, H.; Kurotaki, Y.; Fujimori, T.; Fukuda, K.; Nabeshima, Y. Klotho, a gene related to a syndrome resembling human premature aging, functions in a negative regulatory circuit of vitamin D endocrine system. Mol. Endocrinol. 2003, 17, 2393–2403. [Google Scholar] [CrossRef]
- Ramsey, K.A.; Meskers, C.G.M.; Maier, A.B. Every step counts: Synthesising reviews associating objectively measured physical activity and sedentary behaviour with clinical outcomes in community-dwelling older adults. Lancet Healthy Longev. 2021, 2, e764–e772. [Google Scholar] [CrossRef] [PubMed]
- Pelletier, C.; Gagnon, M.P.; Almeras, N.; Despres, J.P.; Poirier, P.; Tremblay, A.; Chabot, C.; Rheaume, C. Using an activity tracker to increase motivation for physical activity in patients with type 2 diabetes in primary care: A randomized pilot trial. Mhealth 2021, 7, 59. [Google Scholar] [CrossRef] [PubMed]
- Choi, B.C.; Pak, A.W.; Choi, J.C.; Choi, E.C. Daily step goal of 10,000 steps: A literature review. Clin. Investig. Med. 2007, 30, E146–E151. [Google Scholar] [CrossRef]
- Sorensen, A.; Aune, T.K.; Rangul, V.; Dalen, T. The Validity of Functional Threshold Power and Maximal Oxygen Uptake for Cycling Performance in Moderately Trained Cyclists. Sports 2019, 7, 217. [Google Scholar] [CrossRef]
- Ji, N.; Luan, J.; Hu, F.; Zhao, Y.; Lv, B.; Wang, W.; Xia, M.; Zhao, X.; Lao, K. Aerobic exercise-stimulated Klotho upregulation extends life span by attenuating the excess production of reactive oxygen species in the brain and kidney. Exp. Ther. Med. 2018, 16, 3511–3517. [Google Scholar] [CrossRef]
- Rao, Z.; Zheng, L.; Huang, H.; Feng, Y.; Shi, R. alpha-Klotho Expression in Mouse Tissues Following Acute Exhaustive Exercise. Front. Physiol. 2019, 10, 1498. [Google Scholar] [CrossRef] [PubMed]
- Corrêa, H.L.; Raab, A.T.O.; Araújo, T.M.; Deus, L.A.; Reis, A.L.; Honorato, F.S.; Rodrigues-Silva, P.L.; Neves, R.V.P.; Brunetta, H.S.; Mori, M.; et al. A systematic review and meta-analysis demonstrating Klotho as an emerging exerkine. Sci. Rep. 2022, 12, 17587. [Google Scholar] [CrossRef] [PubMed]
- Beckner, M.E.; Conkright, W.R.; Eagle, S.R.; Martin, B.J.; Sinnott, A.M.; LaGoy, A.D.; Proessl, F.; Lovalekar, M.; Jabloner, L.R.; Roma, P.G.; et al. Impact of simulated military operational stress on executive function relative to trait resilience, aerobic fitness, and neuroendocrine biomarkers. Physiol. Behav. 2021, 236, 113413. [Google Scholar] [CrossRef]
- Laddu, D.R.; Rana, J.S.; Murillo, R.; Sorel, M.E.; Quesenberry, C.P., Jr.; Allen, N.B.; Gabriel, K.P.; Carnethon, M.R.; Liu, K.; Reis, J.P.; et al. 25-Year Physical Activity Trajectories and Development of Subclinical Coronary Artery Disease as Measured by Coronary Artery Calcium: The Coronary Artery Risk Development in Young Adults (CARDIA) Study. Mayo Clin. Proc. 2017, 92, 1660–1670. [Google Scholar] [CrossRef]
- Merghani, A.; Malhotra, A.; Sharma, S. The U-shaped relationship between exercise and cardiac morbidity. Trends Cardiovasc. Med. 2016, 26, 232–240. [Google Scholar] [CrossRef] [PubMed]
- Harkanen, T.; Kuulasmaa, K.; Sares-Jaske, L.; Jousilahti, P.; Peltonen, M.; Borodulin, K.; Knekt, P.; Koskinen, S. Estimating expected life-years and risk factor associations with mortality in Finland: Cohort study. BMJ Open 2020, 10, e033741. [Google Scholar] [CrossRef] [PubMed]
- Noushad, S.; Ahmed, S.; Ansari, B.; Mustafa, U.H.; Saleem, Y.; Hazrat, H. Physiological biomarkers of chronic stress: A systematic review. Int. J. Health Sci. 2021, 15, 46–59. [Google Scholar]
- Kroenke, K.; Wu, J.W.; Yu, Z.S.; Bair, M.J.; Kean, J.; Stump, T.; Monahan, P.O. Patient Health Questionnaire Anxiety and Depression Scale: Initial Validation in Three Clinical Trials. Psychosom. Med. 2016, 78, 716–727. [Google Scholar] [CrossRef] [PubMed]
- Hannibal, K.E.; Bishop, M.D. Chronic stress, cortisol dysfunction, and pain: A psychoneuroendocrine rationale for stress management in pain rehabilitation. Phys. Ther. 2014, 94, 1816–1825. [Google Scholar] [CrossRef] [PubMed]
- James, K.A.; Stromin, J.I.; Steenkamp, N.; Combrinck, M.I. Understanding the relationships between physiological and psychosocial stress, cortisol and cognition. Front. Endocrinol. 2023, 14, 1085950. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.J.; Wu, W.N.; Fan, H.; Liu, L.E.; Zhan, J.Q.; Li, Y.H.; Chen, C.N.; Jiang, S.Z.; Xiong, J.W.; Yu, Z.M.; et al. Life extension factor klotho regulates behavioral responses to stress via modulation of GluN2B function in the nucleus accumbens. Neuropsychopharmacology 2022, 47, 1710–1720. [Google Scholar] [CrossRef]
- Nakanishi, K.; Nishida, M.; Taneike, M.; Yamamoto, R.; Adachi, H.; Moriyama, T.; Yamauchi-Takihara, K. Implication of alpha-Klotho as the predictive factor of stress. J. Investig. Med. 2019, 67, 1082–1086. [Google Scholar] [CrossRef]
- Nakanishi, K.; Nishida, M.; Harada, M.; Ohama, T.; Kawada, N.; Murakami, M.; Moriyama, T.; Yamauchi-Takihara, K. Klotho-related Molecules Upregulated by Smoking Habit in Apparently Healthy Men: A Cross-sectional Study. Sci. Rep. 2015, 5, 14230. [Google Scholar] [CrossRef]
- Prather, A.A.; Epel, E.S.; Arenander, J.; Broestl, L.; Garay, B.I.; Wang, D.; Dubal, D.B. Longevity factor klotho and chronic psychological stress. Transl. Psychiat. 2015, 5, e585. [Google Scholar] [CrossRef]
- Gautam, S.; Kumar, U.; Kumar, M.; Rana, D.; Dada, R. Yoga improves mitochondrial health and reduces severity of autoimmune inflammatory arthritis: A randomized controlled trial. Mitochondrion 2021, 58, 147–159. [Google Scholar] [CrossRef] [PubMed]
- Sambou, M.L.; Zhao, X.Y.; Hong, T.T.; Naveed, M.; Sambou, A.; El Hafa, F.; Basnet, T.B.; Dai, J.C. Investigation of the relationships between sleep behaviors and risk of healthspan termination: A prospective cohort study based on 323,373 UK-Biobank participants. Sleep Breath. 2022, 26, 205–213. [Google Scholar] [CrossRef]
- Masters, A.; Pandi-Perumal, S.R.; Seixas, A.; Girardin, J.L.; McFarlane, S.I. Melatonin, the Hormone of Darkness: From Sleep Promotion to Ebola Treatment. Brain Disord. Ther. 2014, 4, 1000151. [Google Scholar] [CrossRef] [PubMed]
- Huang, D.D.; Wang, S.B. Association between the Anti-Aging Protein Klotho and Sleep Duration in General Population. Int. J. Gen. Med. 2021, 14, 10023–10030. [Google Scholar] [CrossRef]
- Dikeos, D.; Wichniak, A.; Ktonas, P.Y.; Mikoteit, T.; Cronlein, T.; Eckert, A.; Koprivova, J.; Ntafouli, M.; Spiegelhalder, K.; Hatzinger, M.; et al. The potential of biomarkers for diagnosing insomnia: Consensus statement of the WFSBP Task Force on Sleep Disorders. World J. Biol. Psychiatry 2023, 24, 614–642. [Google Scholar] [CrossRef] [PubMed]
- Fabbri, M.; Beracci, A.; Martoni, M.; Meneo, D.; Tonetti, L.; Natale, V. Measuring Subjective Sleep Quality: A Review. Int. J. Environ. Res. Public Health 2021, 18, 1082. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Qin, G. Irregular sleep and cardiometabolic risk: Clinical evidence and mechanisms. Front. Cardiovasc. Med. 2023, 10, 1059257. [Google Scholar] [CrossRef]
- Hackett, R.A.; Dal, Z.; Steptoe, A. The relationship between sleep problems and cortisol in people with type 2 diabetes. Psychoneuroendocrinology 2020, 117, 104688. [Google Scholar] [CrossRef] [PubMed]
- Cappuccio, F.P.; D’Elia, L.; Strazzullo, P.; Miller, M.A. Sleep duration and all-cause mortality: A systematic review and meta-analysis of prospective studies. Sleep 2010, 33, 585–592. [Google Scholar] [CrossRef] [PubMed]
- Mochón-Benguigui, S.; Carneiro-Barrera, A.; Castillo, M.J.; Amaro-Gahete, F.J. Is Sleep Associated with the S-Klotho Anti-Aging Protein in Sedentary Middle-Aged Adults? The FIT-AGEING Study. Antioxidants 2020, 9, 738. [Google Scholar] [CrossRef]
- Holt-Lunstad, J.; Smith, T.B.; Layton, J.B. Social relationships and mortality risk: A meta-analytic review. PLoS Med. 2010, 7, e1000316. [Google Scholar] [CrossRef] [PubMed]
- Lee, R.M.; Draper, M.; Lee, S. Social connectedness, dysfunctional interpersonal behaviors, and psychological distress: Testing a mediator model. J. Couns. Psychol. 2001, 48, 310–318. [Google Scholar] [CrossRef]
- Thayer, C.; Anderson, G.O. Loneliness and Social Connections: A National Survey of Adults 45 and Older. AARP Res. 2018. [Google Scholar] [CrossRef]
- Social Connectedness. Available online: https://www.cdc.gov/emotional-wellbeing/social-connectedness/index.htm (accessed on 5 June 2023).
- Social Determinants of Health at CDC. Available online: https://www.cdc.gov/about/sdoh/index.html (accessed on 1 August 2023).
- Coan, J.A.; Sbarra, D.A. Social Baseline Theory: The social regulation of risk and effort. Curr. Opin. Psychol. 2015, 1, 87–91. [Google Scholar] [CrossRef] [PubMed]
- Holt-Lunstad, J. Loneliness and Social Isolation as Risk Factors: The Power of Social Connection in Prevention. Am. J. Lifestyle Med. 2021, 15, 567–573. [Google Scholar] [CrossRef] [PubMed]
- Hawkley, L.C.; Thisted, R.A.; Cacioppo, J.T. Loneliness Predicts Reduced Physical Activity: Cross-Sectional & Longitudinal Analyses. Health Psychol. 2009, 28, 354–363. [Google Scholar] [CrossRef] [PubMed]
- Beckes, L.; Sbarra, D.A. Social baseline theory: State of the science and new directions. Curr. Opin. Psychol. 2022, 43, 36–41. [Google Scholar] [CrossRef] [PubMed]
- Cacioppo, S.; Grippo, A.J.; London, S.; Goossens, L.; Cacioppo, J.T. Loneliness: Clinical import and interventions. Perspect. Psychol. Sci. 2015, 10, 238–249. [Google Scholar] [CrossRef]
- Dote-Montero, M.; De-la-O, A.; Castillo, M.J.; Amaro-Gahete, F.J. Predictors of Sexual Desire and Sexual Function in Sedentary Middle-Aged Adults: The Role of Lean Mass Index and S-Klotho Plasma Levels. The FIT-AGEING Study. J. Sex. Med. 2020, 17, 665–677. [Google Scholar] [CrossRef]
- Okorare, O.; Evbayekha, E.O.; Adabale, O.K.; Daniel, E.; Ubokudum, D.; Olusiji, S.A.; Antia, A.U. Smoking Cessation and Benefits to Cardiovascular Health: A Review of Literature. Cureus J. Med. Sci. 2023, 15, e35966. [Google Scholar] [CrossRef]
- Onmaz, M.; Demirbas, N.; Eryavuz Onmaz, D.; Kutlu, R.; Unlu, A. Effect of cigarette smoking on serum methylarginine and alpha-klotho levels. Nutr. Metab. Cardiovasc. Dis. 2023, 33, 602–609. [Google Scholar] [CrossRef] [PubMed]
- Kamizono, Y.; Shiga, Y.; Suematsu, Y.; Imaizumi, S.; Tsukahara, H.; Noda, K.; Kuwano, T.; Fujimi, K.; Saku, K.; Miura, S.I. Impact of cigarette smoking cessation on plasma alpha-klotho levels. Medicine 2018, 97, e11947. [Google Scholar] [CrossRef]
- Akbaraly, T.N.; Hamer, M.; Ferrie, J.E.; Lowe, G.; Batty, G.D.; Hagger-Johnson, G.; Singh-Manoux, A.; Shipley, M.J.; Kivimäki, M. Chronic inflammation as a determinant of future aging phenotypes. CMAJ 2013, 185, E763–E770. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Zeng, X.; He, F.; Huang, X. Inflammatory biomarkers of frailty: A review. Exp. Gerontol. 2023, 179, 112253. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Long, Y.; Du, F.W.; Zhao, Y.; Luo, X.B. Association between serum cotinine and α-Klotho levels among adults: Findings from the National Health and Nutrition Examination Survey 2007–2016. Tob. Induc. Dis. 2022, 20, 57. [Google Scholar] [CrossRef] [PubMed]
- Martin-Gonzalez, C.; Gonzalez-Reimers, E.; Quintero-Platt, G.; Martinez-Riera, A.; Santolaria-Fernandez, F. Soluble alpha-Klotho in Liver Cirrhosis and Alcoholism. Alcohol Alcohol. 2019, 54, 204–208. [Google Scholar] [CrossRef] [PubMed]
- Ding, M.; Fitzmaurice, G.M.; Arvizu, M.; Willett, W.C.; Manson, J.E.; Rexrode, K.M.; Hu, F.B.; Chavarro, J.E. Associations between patterns of modifiable risk factors in mid-life to late life and longevity: 36 year prospective cohort study. BMJ Med. 2022, 1, e000098. [Google Scholar] [CrossRef]
- Gonzalez-Reimers, E.; Romero-Acevedo, L.; Espelosin-Ortega, E.; Martin-Gonzalez, M.C.; Quintero-Platt, G.; Abreu-Gonzalez, P.; Jose de-la-Vega-Prieto, M.; Martinez-Martinez, D.; Santolaria-Fernandez, F. Soluble Klotho and Brain Atrophy in Alcoholism. Alcohol Alcohol. 2018, 53, 503–510. [Google Scholar] [CrossRef] [PubMed]
- Santos-Buelga, C.; Gonzalez-Manzano, S.; Gonzalez-Paramas, A.M. Wine, Polyphenols, and Mediterranean Diets. What Else Is There to Say? Molecules 2021, 26, 5537. [Google Scholar] [CrossRef]
- Yazici, A.B.; Guzel, D.; Kurt, E.M.; Turkmen, B.; Yazici, E. Klotho, BDNF, NGF, GDNF Levels and Related Factors in Withdrawal Period in Chronic Cannabinoid Users. Indian J. Clin. Biochem. 2022, 37, 139–148. [Google Scholar] [CrossRef]
- Wang, Z.; Zheng, P.; Chen, X.; Xie, Y.; Weston-Green, K.; Solowij, N.; Chew, Y.L.; Huang, X.F. Cannabidiol induces autophagy and improves neuronal health associated with SIRT1 mediated longevity. Geroscience 2022, 44, 1505–1524. [Google Scholar] [CrossRef]
- Trivedi, M.K.; Mondal, S.; Gangwar, M.; Jana, S. Effects of Cannabidiol Interactions with CYP2R1, CYP27B1, CYP24A1, and Vitamin D(3) Receptors on Spatial Memory, Pain, Inflammation, and Aging in Vitamin D(3) Deficiency Diet-Induced Rats. Cannabis Cannabinoid Res. 2022. ahead of print. [Google Scholar] [CrossRef] [PubMed]
- Comander, A.; Frates, B.; Tollefson, M. PAVING the Path to Wellness for Breast Cancer Survivors: Lifestyle Medicine Education and Group Interventions. Am. J. Lifestyle Med. 2021, 15, 242–248. [Google Scholar] [CrossRef] [PubMed]
- Marti, B.; Abelin, T.; Minder, C.E.; Vader, J.P. Smoking, alcohol consumption, and endurance capacity: An analysis of 6500 19-year-old conscripts and 4100 joggers. Prev. Med. 1988, 17, 79–92. [Google Scholar] [CrossRef]
- Colyer-Patel, K.; Kuhns, L.; Weidema, A.; Lesscher, H.; Cousijn, J. Age-dependent effects of tobacco smoke and nicotine on cognition and the brain: A systematic review of the human and animal literature comparing adolescents and adults. Neurosci. Biobehav. Rev. 2023, 146, 105038. [Google Scholar] [CrossRef] [PubMed]
- Kresovich, J.K.; Bulka, C.M. Low Serum Klotho Associated with All-cause Mortality Among a Nationally Representative Sample of American Adults. J. Gerontol. Biol. Sci. Med. Sci. 2022, 77, 452–456. [Google Scholar] [CrossRef] [PubMed]
- Sanz, B.; Arrieta, H.; Rezola-Pardo, C.; Fernandez-Atutxa, A.; Garin-Balerdi, J.; Arizaga, N.; Rodriguez-Larrad, A.; Irazusta, J. Low serum klotho concentration is associated with worse cognition, psychological components of frailty, dependence, and falls in nursing home residents. Sci. Rep. 2021, 11, 9098. [Google Scholar] [CrossRef]

| Lifestyle Pillar | Effect on Klotho | Type of Studies | References |
|---|---|---|---|
| Nutrition | |||
| Mediterranean diet Low-carb diet Low fat diet Healthy Eating Index | Increase No effect No effect Increase | Observational Observational Observational Observational | [48,49] [48] [48] [46] |
| Physical activity | |||
| Low intensity High intensity | Increase Decrease | Observational, RCT RCT | [5,61,63] [62,64] |
| Stress Management | |||
| Acute stress Chronic stress Yoga | Decrease Increase/Decrease Increase | Observational Observational RCT | [64] [73,75] [76] |
| Restorative sleep | |||
| 5.5–7.5 h ≤ 5.5–≥ 7.5 h | Increase Decrease | Observational, RCT Observational | [79,85] [79] |
| Social connection | |||
| Sexual | Increase | Observational | [96] |
| Risky substance | |||
| Tobacco Alcohol Drug | Increase/Decrease Decrease/Increase Decrease/Increase | Observational, RCT Observational, Literature survey Observational, Interventional | [74,98,99] [29,105] [107,108,109] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Paquette, J.-S.; Rhéaume, C.; Cordeau, P.; Moulin, J.-A.; Audet-Walsh, E.; Blanchette, V.; Drouin-Chartier, J.-P.; Toi, A.-K.; Tremblay, A. The Longevity Protein Klotho: A Promising Tool to Monitor Lifestyle Improvements. Metabolites 2023, 13, 1157. https://doi.org/10.3390/metabo13111157
Paquette J-S, Rhéaume C, Cordeau P, Moulin J-A, Audet-Walsh E, Blanchette V, Drouin-Chartier J-P, Toi A-K, Tremblay A. The Longevity Protein Klotho: A Promising Tool to Monitor Lifestyle Improvements. Metabolites. 2023; 13(11):1157. https://doi.org/10.3390/metabo13111157
Chicago/Turabian StylePaquette, Jean-Sébastien, Caroline Rhéaume, Pierre Cordeau, Julie-Alexandra Moulin, Etienne Audet-Walsh, Virginie Blanchette, Jean-Philippe Drouin-Chartier, Alfred-Kodjo Toi, and Angelo Tremblay. 2023. "The Longevity Protein Klotho: A Promising Tool to Monitor Lifestyle Improvements" Metabolites 13, no. 11: 1157. https://doi.org/10.3390/metabo13111157
APA StylePaquette, J.-S., Rhéaume, C., Cordeau, P., Moulin, J.-A., Audet-Walsh, E., Blanchette, V., Drouin-Chartier, J.-P., Toi, A.-K., & Tremblay, A. (2023). The Longevity Protein Klotho: A Promising Tool to Monitor Lifestyle Improvements. Metabolites, 13(11), 1157. https://doi.org/10.3390/metabo13111157







