Innovative Multi-Site Photoplethysmography Analysis for Quantifying Pulse Amplitude and Timing Variability Characteristics in Peripheral Arterial Disease
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Datasets
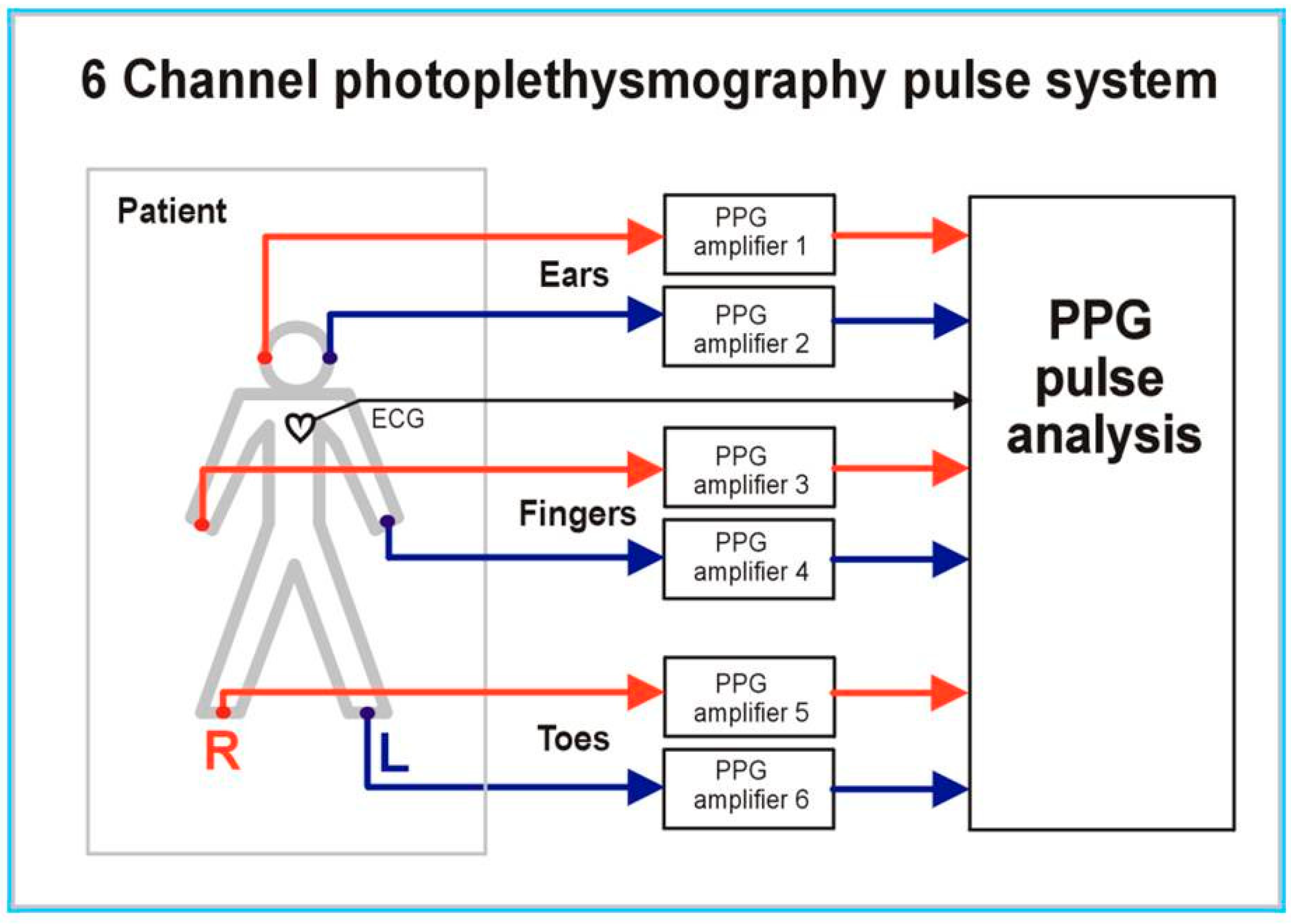
2.2. Multi-Site PPG System and Measurements
2.3. Pulse Wave Analysis and Signal Quality Control
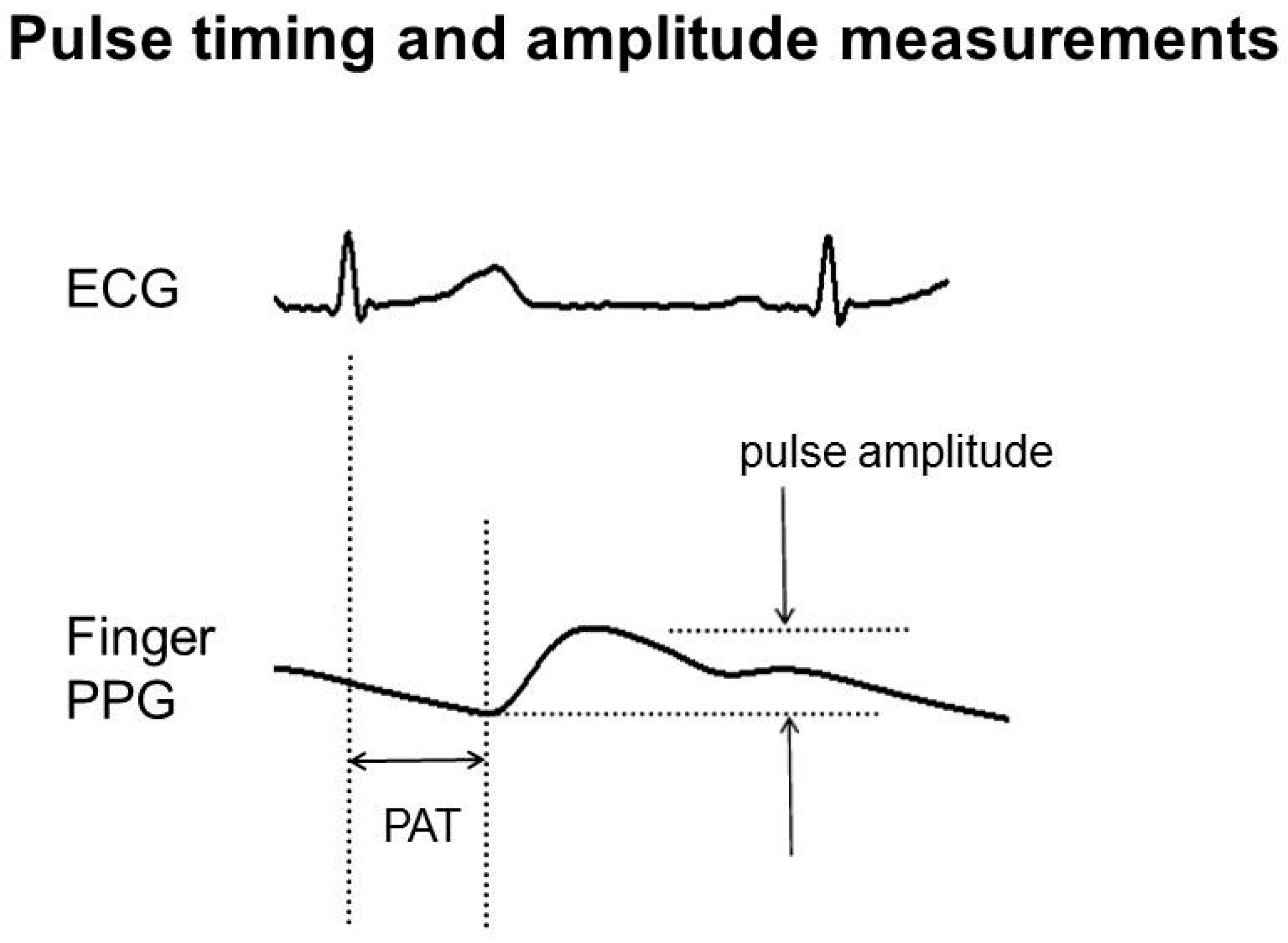
2.3.1. Time-Domain Analysis
2.3.2. Frequency-Domain Analysis
2.4. Statistical Analysis
3. Results
3.1. Subject Demographics
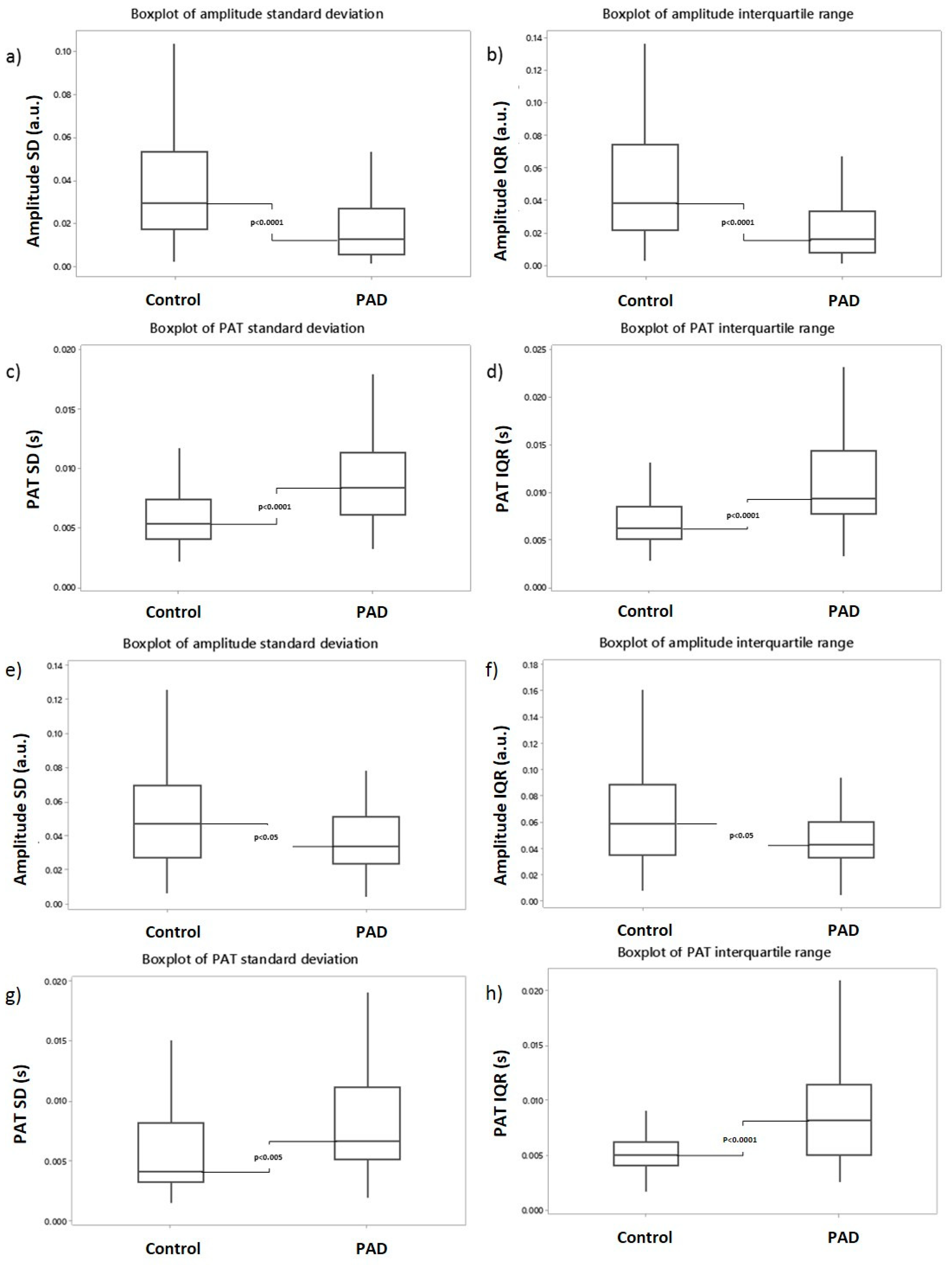
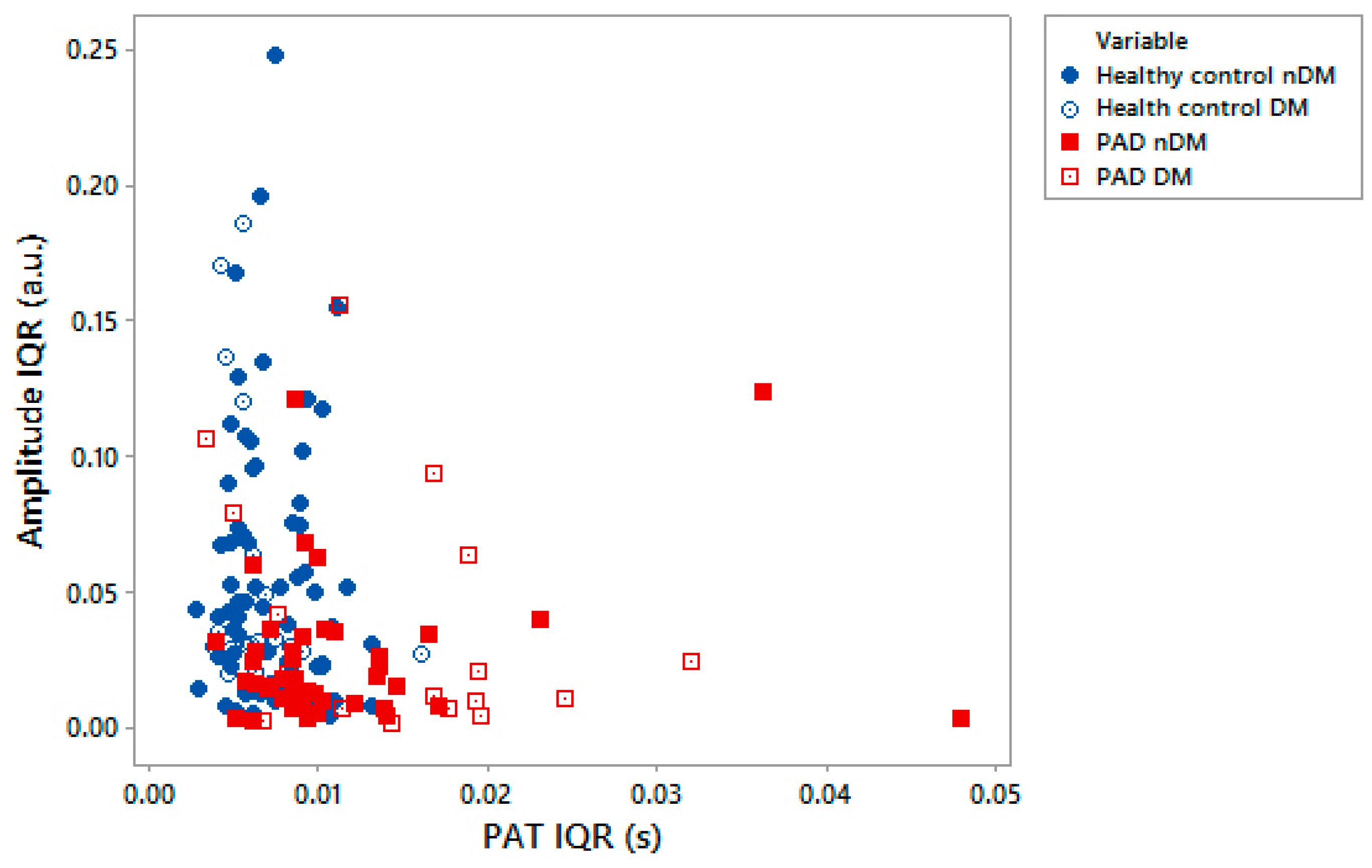
3.2. Toe Site PPG Variability in the Time-Domain Comparing PAD to Healthy Controls
3.3. Changes in the Frequency-Domain with PAD for the Toe Site
3.4. Finger Site PPG Variability in the Time-Domain Comparing PAD to Healthy Controls
3.5. Changes in the Frequency-Domain with PAD for the Fingers
4. Discussion
4.1. Variability in Time-Domain Measures in Health and Peripheral Arterial Disease
4.2. Variability in the Frequency-Domain in Health and in PAD
4.3. Study Limitations
4.4. Future Directions of the Research
5. Summary
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Allen, J. Photoplethysmography and its application in clinical physiological measurement. Physiol. Meas. 2007, 28, R1. [Google Scholar] [PubMed]
- Fischer, C.; Dömer, B.; Wibmer, T.; Penzel, T. An algorithm for real-time pulse waveform segmentation and artifact detection in photoplethysmograms. IEEE J. Biomed. Health Inf. 2017, 21, 372–381. [Google Scholar] [CrossRef] [PubMed]
- Chua, C.P.; Heneghan, C. Continuous Blood Pressure Monitoring using ECG and Finger Photoplethysmogram. In Proceedings of the 2006 International Conference of the IEEE Engineering in Medicine and Biology Society, New York, NY, USA, 30 August–3 September 2006; pp. 5117–5120. [Google Scholar]
- Chua, E.C.-P.; Redmond, S.J.; McDarby, G.; Heneghan, C. Towards using photo-plethysmogram amplitude to measure blood pressure during sleep. Ann. Biomed. Eng. 2010, 38, 945–954. [Google Scholar] [PubMed]
- Lokharan, M.; Lokesh Kumar, K.C.; Harish Kumar, V.; Kayalvizhi, N.; Aryalekshmi, R. Measurement of Pulse Transit Time (PTT) Using Photoplethysmography. In Proceedings of the 16th International Conference on Biomedical Engineering (IFMBE), Singapore, 7–10 December 2016; Goh, J., Lim, C., Leo, H., Eds.; Springer: Berlin, Germany, 2017; Volume 61. [Google Scholar]
- Payne, R.A.; Symeonides, C.N.; Webb, D.J.; Maxwell, S.R.J. Pulse transit time measured from the ECG: An unreliable marker of beat-to-beat blood pressure. J. Appl. Physiol. 2006, 100, 136–141. [Google Scholar] [CrossRef] [PubMed]
- Stavros, L.; Rex, D.; Nirree, P.; Christopher, N.M.; Stephen, E.G. Validation of a device to measure arterial pulse wave velocity by a photoplethysmographic method. Physiol. Meas. 2002, 23, 581. [Google Scholar]
- McCall, C.; Rostosky, R.; Wiard, R.M.; Inan, O.T.; Giovangrandi, L.; Cuttino, C.M.; Gregory, T.A.K. Noninvasive pulse transit time measurement for arterial stiffness monitoring in microgravity. In Proceedings of the 2015 37th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Milan, Italy, 25–29 August 2015; pp. 6429–6432. [Google Scholar]
- Zhang, Y.-L.; Zheng, Y.-Y.; Ma, Z.-C.; Sun, Y.-N. Radial pulse transit time is an index of arterial stiffness. Hypertens. Res. 2011, 34, 884. [Google Scholar] [CrossRef] [PubMed]
- Allen, J.; Oates, C.P.; Lee, T.A.; Murray, A. Photoplethysmography detection of lower limb peripheral arterial occlusive disease: A comparison of pulse timing, amplitude and shape characteristics. Physiol. Meas. 2005, 26, 811. [Google Scholar] [PubMed]
- Awad, A.A.; Haddadin, A.S.; Tantawy, H.; Badr, T.M.; Stout, R.G.; Silverman, D.G.; Kirk, H.S. The relationship between the photoplethysmographic waveform and systemic vascular resistance. J. Clin. Monit. Comput. 2007, 21, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Pickwell-MacPherson, E.; Liang, Y.P.; Zhang, Y.T. Noninvasive cardiac output estimation using a novel photoplethysmogram index. In Proceedings of the 2009 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Minneapolis, MN, USA, 3–6 September 2009; pp. 1746–1749. [Google Scholar]
- Allen, J.; Murray, A. Similarity in bilateral photoplethysmographic peripheral pulse wave characteristics at the ears, thumbs and toes. Physiol. Meas. 2000, 21, 369–377. [Google Scholar] [CrossRef] [PubMed]
- Stefanovska, A.; Bracic, M. Physics of the human cardiovascular system. Contemp. Phys. 1999, 40, 31–55. [Google Scholar] [CrossRef]
- Bernjak, A.; Clarkson, P.B.M.; McClintock, P.V.E.; Stefanovska, A. Low-frequency blood flow oscillations in congestive heart failure and after β1-blockade treatment. Microvasc. Res. 2008, 76, 224–232. [Google Scholar] [CrossRef] [PubMed]
- Khanoka, B.; Slovik, Y.; Landau, D.; Nitzan, M. Sympathetically induced spontaneous fluctuations of the photoplethysmographic signal. Med. Biol. Eng. Comput. 2004, 42, 80–85. [Google Scholar] [CrossRef]
- Nitzan, M.; Babchenko, A.; Khanokh, B.; David, L. The variability of the photoplethysmographic signal—A potential method for the evaluation of the autonomic nervous system. Physiol. Meas. 1998, 19, 93. [Google Scholar] [CrossRef] [PubMed]
- Nitzan, M.; Babchenko, A.; Shemesh, D.; Alberton, J. Influence of thoracic sympathectomy on cardiac induced oscillations in tissue blood volume. Med. Biol. Eng. Comput. 2001, 39, 579–583. [Google Scholar] [CrossRef] [PubMed]
- Buchs, A.; Slovik, Y.; Rapoport, M.; Rosenfeld, C.; Khanokh, B.; Nitzan, M. Right-left correlation of the sympathetically induced fluctuations of photoplethysmographic signal in diabetic and non-diabetic subjects. Med. Biol. Eng. Comput. 2005, 43, 252–257. [Google Scholar] [CrossRef] [PubMed]
- Cea-Soriano, L.; Fowkes, F.G.R.; Johansson, S.; Allum, A.M.; García Rodriguez, L.A. Time trends in peripheral artery disease incidence, prevalence and secondary preventive therapy: A cohort study in the Health Improvement Network UK. BMJ Open 2018, 8, e018184. [Google Scholar] [CrossRef] [PubMed]
- Norgren, L.; Hiatt, W.R.; Dormandy, J.A.; Nehler, M.R.; Harris, K.A.; Fowkes, F.G.R. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J. Vasc. Surg. 2007, 45, S5–S67. [Google Scholar] [CrossRef] [PubMed]
- Burns, P.; Gough, S.; Bradbury, A.W. Management of peripheral arterial disease in primary care. BMJ 2003, 326, 584–588. [Google Scholar] [CrossRef] [PubMed]
- Hennion, D.R.; Siano, K.A. Diagnosis and treatment of peripheral arterial disease. Am. Fam. Physician 2013, 88, 306–310. [Google Scholar] [PubMed]
- Wilkes, S.; Stansby, G.; Sims, A.; Haining, S.; Allen, J. Peripheral arterial disease: Diagnostic challenges and how photoplethysmography may help. Br. J. Gen. Pract. 2015, 65, 323–324. [Google Scholar] [CrossRef] [PubMed]
- Hodnett, P.A.; Koktzoglou, I.; Davarpanah, A.H.; Scanlon, T.G.; Collins, J.D.; Sheehan, J.J.; Eugene, E.D.; Navyash, G.; James, C.C.; Robert, R. Edelman Evaluation of Peripheral Arterial Disease with Nonenhanced Quiescent-Interval Single-Shot MR Angiography. Radiology 2011, 260, 282–293. [Google Scholar] [CrossRef] [PubMed]
- Abdulhannan, P.; Russell, D.A.; Homer-Vanniasinkam, S. Peripheral arterial disease: A literature review. Br. Med. Bull. 2012, 104, 21–39. [Google Scholar] [CrossRef] [PubMed]
- Pollak, A.W.; Norton, P.; Kramer, C.M. Multimodality imaging of lower extremity peripheral arterial disease: Current role and future directions. Circ. Cardiovasc. Imaging 2012, 5, 797–807. [Google Scholar] [CrossRef] [PubMed]
- Ro, D.H.; Moon, H.J.; Kim, J.H.; Lee, K.M.; Kim, S.J.; Lee, D.Y. Photoplethysmography and continuous-wave Doppler ultrasound as a complementary test to Ankle–Brachial Index in detection of stenotic peripheral arterial disease. Angiology 2013, 64, 314–320. [Google Scholar] [CrossRef] [PubMed]
- Beutner, F.; Teren, A.; Gielen, S.; Schuler, G.; Wirkner, K.; Tiller, D.; Markus, L.; Markus, S. Automated photoplethysmography-based determination of ankle-brachial index: A validation study against Doppler sonography. Clin. Res. Cardiol. 2012, 101, 875–883. [Google Scholar] [CrossRef] [PubMed]
- Danescu, L.; Roe, C.; Johnson, L. Photoplethysmography: A simplified method for the office measurement of Ankle Brachial Index in individuals with diabetes. Endocr. Pract. 2013, 19, 439–443. [Google Scholar] [CrossRef] [PubMed]
- Peltokangas, M.; Vehkaoja, A.; Matti, H.; Verho, J.; Mattila, V.M.; Juha, R.; Pekka, R.; Jukka, L.; Niku, O. Combining finger and toe photoplethysmograms for the detection of atherosclerosis. Physiol. Meas. 2017, 38, 139–154. [Google Scholar] [CrossRef] [PubMed]
- Peltokangas, M.; Verho, J.; Mattila, V.M.; Pekka, R.; Vehkaoja, A.; Jukka, L.; Niku, O. Areas under peripheral pulse waves: A potential marker of atherosclerotic changes. Physiol. Meas. 2018, 39, 025003. [Google Scholar] [CrossRef] [PubMed]
- Peltokangas, M.; Telembeci, A.A.; Verho, J.; Mattila, V.M.; Romsi, P.; Vehkaoja, A.; Jukka, L.; Niku, O. Parameters extracted from arterial pulse waves as markers of atherosclerotic changes: Performance and repeatability. IEEE J. Biomed. Health Inf. 2018, 22, 750–757. [Google Scholar] [CrossRef] [PubMed]
- Nath, A.F. Screening for Peripheral Arterial Disease in Patients with Diabetes: A Study Comparing Multi-Site Photoplethysmography Pulse Assessments with Gold Standard Ankle Brachial Pressure Index (ABPI) and Toe Brachial Pressure Index (TBPI) Assessments; Newcastle University: Newcastle upon Tyne, UK, 2013. [Google Scholar]
- Allen, J.; Overbeck, K.; Nath, A.F.; Murray, A.; Stansby, G. A prospective comparison of bilateral photoplethysmography versus the ankle-brachial pressure index for detecting and quantifying lower limb peripheral arterial disease. J. Vasc. Surg. 2008, 47, 794–802. [Google Scholar] [CrossRef] [PubMed]
- Dhaliwal, G.; Mukherjee, D. Peripheral arterial disease: Epidemiology, natural history, diagnosis and treatment. Int. J. Angiol. 2007, 16, 36–44. [Google Scholar] [CrossRef] [PubMed]
- Allen, J.; Murray, A. Age-related changes in the characteristics of the photoplethysmographic pulse shape at various body sites. Physiol. Meas. 2003, 24, 297–307. [Google Scholar] [CrossRef] [PubMed]
- Magnitude-Squared Coherence. Available online: https://uk.mathworks.com/help/signal/ref/mscohere.html (accessed on 1 May 2015).
- Kvandal, P.; Landsverk, S.A.; Bernjak, A.; Stefanovska, A.; Kvernmo, H.D.; Kirkebøen, K.A. Low-frequency oscillations of the laser Doppler perfusion signal in human skin. Microvasc. Res. 2006, 72, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Kvernmo, H.D.; Stefanovska, A.; Bracic, M.; Kirkebøen, K.A.; Kvernebo, K. Spectral analysis of the laser Doppler perfusion signal in human skin before and after exercise. Microvasc. Res. 1998, 56, 173–182. [Google Scholar] [CrossRef] [PubMed]
- Allen, J.; Murray, A. Variability of photoplethysmography peripheral pulse measurements at the ears, thumbs and toes. IEE Proc. Sci. Meas. Technol. 2000, 147, 403–407. [Google Scholar] [CrossRef]

| Frequency Band | Frequency (Hz) | Physiological Origin |
|---|---|---|
| Alternating Current (AC) | 0.6–2.0 | Heartbeat |
| High frequency (HF) | 0.145–0.6 | Respiratory activity |
| Medium frequency (MF) | 0.052–0.145 | Intrinsic myogenic activity |
| Low frequency (LF) | 0.021–0.052 | Neurogenic (sympathetic) activity |
| Very low frequency (VLF) | 0.0095–0.021 | NO-dependent endothelial activity |
| Variable | Healthy Control (n = 43) | PAD (n = 31) | p-Value |
|---|---|---|---|
| Age (years) | 68 (55–77) | 69 (64–75) | NS |
| Sex (male) | 20 | 15 | NS |
| Height (cm) | 169 (162–174) | 167 (159–172) | NS |
| Heart-rate (bpm) | 69 (64–77) | 70 (61–79) | NS |
| Systolic BP (mmHg) | 142 (124–158) | 158 (144–177) | <0.001 |
| Minimum side ABPI | 1.07 (1.01–1.15) | 0.59 (0.53–0.69) | <0.001 |
| Measure | Healthy Control Legs (n = 86) | PAD Legs (n = 62) | p-Value |
|---|---|---|---|
| SD amplitude (a.u.) | 0.0295 (0.0172–0.0536) | 0.0124 (0.0056–0.0270) | <0.0001 |
| IQR amplitude (a.u.) | 0.0384 (0.0217–0.0744) | 0.0160 (0.0080–0.0338) | <0.0001 |
| SD PAT (s) | 0.0054 (0.0041–0.0074) | 0.0085 (0.0061–0.0114) | <0.0001 |
| IQR PAT (s) | 0.0063 (0.0052–0.0086) | 0.0093 (0.0078–0.0144) | <0.0001 |
| Frequency Band | Healthy Control Legs (n = 86) | PAD Legs (n = 62) | p-Value |
|---|---|---|---|
| Amplitude VLF | 0.685 (0.514–0.835) | 0.466 (0.394–0.685) | <0.005 |
| Amplitude LF | 0.704 (0.563–0.799) | 0.484 (0.342–0.704) | <0.005 |
| Amplitude MF | 0.611 (0.430–0.707) | 0.536 (0.394–0.656) | NS |
| Amplitude HF | 0.684 (0.545–0.839) | 0.551 (0.444–0.735) | <0.05 |
| Amplitude AC | 0.526 (0.446–0.653) | 0.497 (0.415–0.567) | NS |
| PAT VLF | 0.870 (0.727–0.937) | 0.701 (0.543–0.899) | <0.05 |
| PAT LF | 0.704 (0.546–0.882) | 0.445 (0.269–0.646) | <0.001 |
| PAT MF | 0.631 (0.479–0.865) | 0.435 (0.377–0.557) | <0.001 |
| PAT HF | 0.755 (0.575–0.904) | 0.517 (0.468–0.699) | <0.005 |
| PAT AC | 0.685 (0.467–0.838) | 0.426 (0.373–0.767) | <0.01 |
| Measure | Healthy Control Arms (n = 78) | PAD Patient Arms (n = 62) | p-Value |
|---|---|---|---|
| Amplitude SD (a.u.) | 0.0473 (0.0275–0.0695) | 0.0336 (0.0239–0.0511) | <0.05 |
| Amplitude IQR (a.u.) | 0.0591 (0.0353–0.0890) | 0.0435 (0.0331–0.0603) | <0.05 |
| PAT SD (s) | 0.0041 (0.0033–0.0082) | 0.0066 (0.0051–0.0111) | <0.005 |
| PAT IQR (s) | 0.0050 (0.0041–0.0062) | 0.0082 (0.0050–0.0114) | <0.0001 |
| Frequency Band | Healthy Control arms (n = 78) | PAD arms (n = 62) | p-Value |
|---|---|---|---|
| Amplitude VLF | 0.804 (0.573–0.931) | 0.696 (0.500–0.922) | NS |
| Amplitude LF | 0.834 (0.664–0.924) | 0.680 (0.487–0.787) | <0.005 |
| Amplitude MF | 0.673 (0.548–0.768) | 0.532 (0.404–0.694) | <0.01 |
| Amplitude HF | 0.631 (0.515–0.782) | 0.573 (0.458–0.699) | NS |
| Amplitude AC | 0.492 (0.440–0.622) | 0.486 (0.402–0.580) | NS |
| PAT VLF | 0.750 (0.468–0.939) | 0.633 (0.464–0.858) | NS |
| PAT LF | 0.518 (0.325–0.746) | 0.514 (0.380–0.637) | NS |
| PAT MF | 0.581 (0.378–0.808) | 0.439 (0.349–0.557) | <0.05 |
| PAT HF | 0.644 (0.499–0.833) | 0.492 (0.398–0.733) | <0.05 |
| PAT AC | 0.540 (0.409–0.822) | 0.434 (0.363–0.661) | NS |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bentham, M.; Stansby, G.; Allen, J. Innovative Multi-Site Photoplethysmography Analysis for Quantifying Pulse Amplitude and Timing Variability Characteristics in Peripheral Arterial Disease. Diseases 2018, 6, 81. https://doi.org/10.3390/diseases6030081
Bentham M, Stansby G, Allen J. Innovative Multi-Site Photoplethysmography Analysis for Quantifying Pulse Amplitude and Timing Variability Characteristics in Peripheral Arterial Disease. Diseases. 2018; 6(3):81. https://doi.org/10.3390/diseases6030081
Chicago/Turabian StyleBentham, Michael, Gerard Stansby, and John Allen. 2018. "Innovative Multi-Site Photoplethysmography Analysis for Quantifying Pulse Amplitude and Timing Variability Characteristics in Peripheral Arterial Disease" Diseases 6, no. 3: 81. https://doi.org/10.3390/diseases6030081
APA StyleBentham, M., Stansby, G., & Allen, J. (2018). Innovative Multi-Site Photoplethysmography Analysis for Quantifying Pulse Amplitude and Timing Variability Characteristics in Peripheral Arterial Disease. Diseases, 6(3), 81. https://doi.org/10.3390/diseases6030081






