Self-Medication with Antibiotics, Attitude and Knowledge of Antibiotic Resistance among Community Residents and Undergraduate Students in Northwest Nigeria
Abstract
:1. Introduction
2. Methods
2.1. Study Site
2.2. Study Design and Data Collection
2.3. Data Analysis
2.4. Ethical Considerations
3. Results
3.1. Socio-Demographics of Respondents
3.2. Socio-Demographic Characteristics among the University Students
3.3. Socio-Demographic Characteristics of Community Members
3.4. Frequency, Types and Place of Purchase of Commonly Used Antibiotics
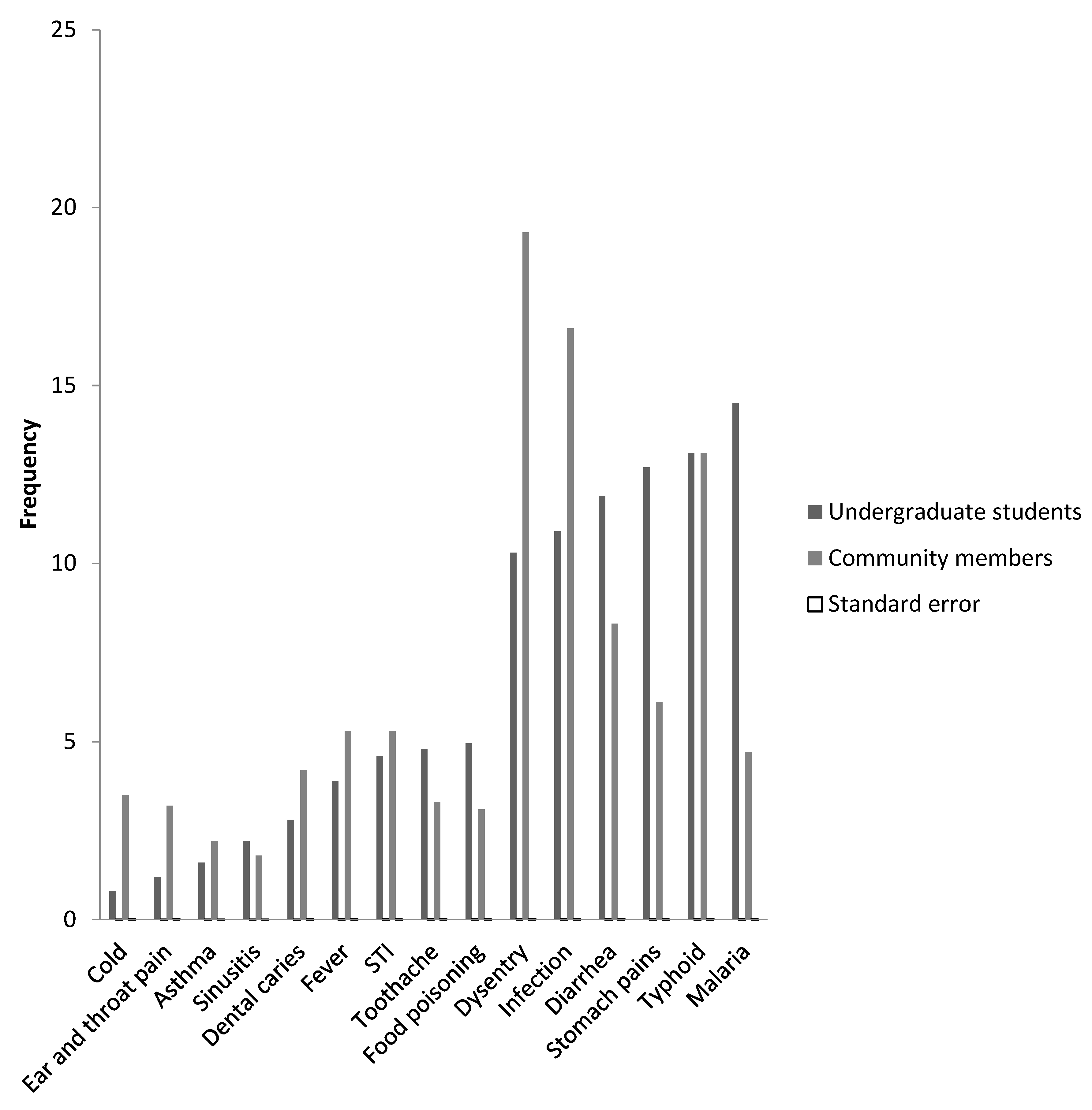
3.5. Commonly Treated Illnesses
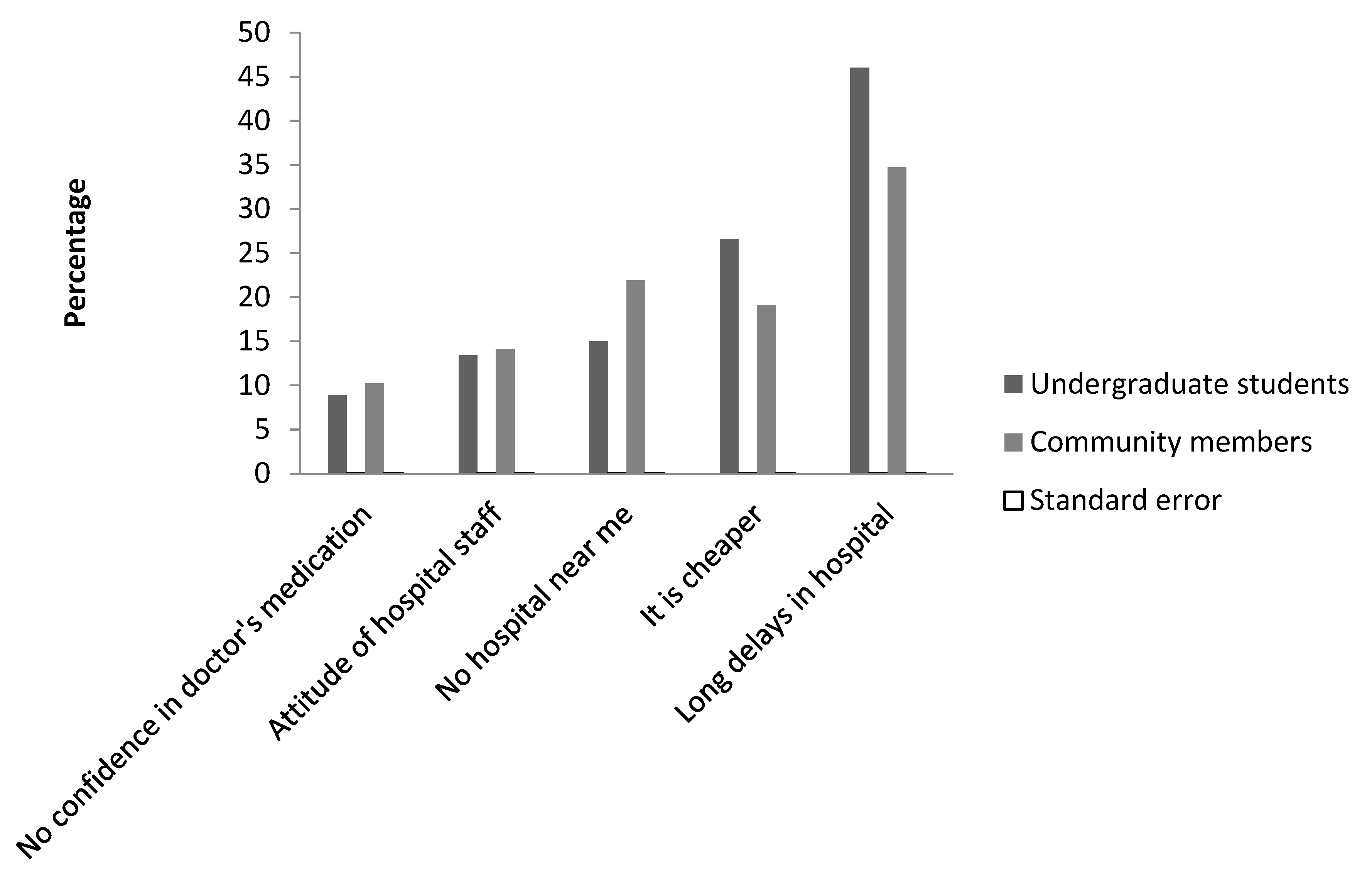
3.6. Source of Antibiotic Choice
3.7. Knowledge of Antibiotic Resistance among Undergraduate Students and Community Residents
3.8. Attitude towards the Use of Antibiotics
4. Discussion
Author Contributions
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Antimicrobial Resistance; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Ventola, C.L. The Antibiotic Resistance Crisis. Pharm. Ther. 2015, 40, 277–283. [Google Scholar]
- World Health Organization. Antibiotic Resistance: Multi-Country Public Awareness Survey; World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Ayukekbong, J.A.; Ntemgwa, M.; Atabe, A.N. The threat of antimicrobial resistance in developing countries: Causes and control strategies. Antimicrob. Resist. Infect. Control 2017, 6, 47. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. The Role of the Pharmacist in Self-Care and Self-Medication; World Health Organization: Geneva, Switzerland, 1998. [Google Scholar]
- Loyola Filho, A.I.; Lima-Costa, M.F.; Uchôa, E. Bambuí Project: A qualitative approach to self-medication. Cad. Saude Publica 2004, 20, 1661–1669. [Google Scholar] [CrossRef] [PubMed]
- Ehigiator, O.; Azodo, C.C.; Ehizele, A.O.; Ezeja, E.B.; Ehigiator, L.; Madukwe, I.U. Self-medication practices among dental, midwifery and nursing students. Eur. J. Gen. Dent. 2013, 2, 54–57. [Google Scholar] [CrossRef]
- Selley, P. Self-prescribing by doctors. Health Trends 1988, 20, 128–129. [Google Scholar] [PubMed]
- Umeora, O.U.J.; Egwuatu, V.E. Menstruation in rural Igbo women of south east Nigeria: Attitudes, beliefs and practices. Afr. J. Reprod. Health 2008, 12, 109–115. [Google Scholar] [PubMed]
- Bello, F.A.; Morhason-Bello, I.O.; Olayemi, O.; Adekunle, A.O. Patterns and predictors of self-medication amongst antenatal clients in Ibadan, Nigeria. Niger. Med. J. 2011, 52, 153–157. [Google Scholar] [CrossRef] [PubMed]
- Babatunde, O.A.; Fadare, J.O.; Ojo, O.J.; Durowade, K.A.; Atoyebi, O.A.; Olaniyan, P.O.A.T. Self-medication among health workers in a tertiary institution in South-West Nigeria. Pan Afr. Med. J. 2016, 24, 312. [Google Scholar] [CrossRef] [PubMed]
- Abdulraheem, I.S.; Adegboye, A.; Fatiregun, A.A. Self-medication with Antibiotics: Empirical Evidence from a Nigerian Rural Population. Br. J. Pharm. Res. 2016, 11, 1–13. [Google Scholar] [CrossRef]
- Leopold, S.J.; van Leth, F.; Tarekegn, H.; Schultsz, C. Antimicrobial drug resistance among clinically relevant bacterial isolates in sub-Saharan Africa: A systematic review. J. Antimicrob. Chemother. 2014, 69, 2337–2353. [Google Scholar] [CrossRef] [PubMed]
- Bernabé, K.J.; Langendorf, C.; Ford, N.; Ronat, J.-B.; Murphy, R.A. Antimicrobial resistance in West Africa: A systematic review and meta-analysis. Int. J. Antimicrob. Agents 2017, 50, 629–639. [Google Scholar] [CrossRef] [PubMed]
- Williams, D.N. Antimicrobial resistance: Are we at the dawn of the post-antibiotic era? J. R. Coll. Physicians Edinb. 2016, 46, 150–156. [Google Scholar] [CrossRef] [PubMed]
- Dresser, G.K.; Bailey, D.G. The effects of fruit juices on drug disposition: A new model for drug interactions. Eur. J. Clin. Investig. 2003, 33 (Suppl. S2), 10–16. [Google Scholar] [CrossRef]
- PMHDEV. Using Medication: Using Antibiotics Correctly and Avoiding Resistance. 2013. Available online: https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0087079/ (accessed on 14 April 2018).
- Li, M.; Andrew, M.A.; Wang, J.; Salinger, D.H.; Vicini, P.; Grady, R.W.; Phillips, B.; Shen, D.D.; Anderson, G.D. Effects of Cranberry Juice on Pharmacokinetics of β-Lactam Antibiotics following Oral Administration. Antimicrob. Agents Chemother. 2009, 53, 2725–2732. [Google Scholar] [CrossRef] [PubMed]
- World Medical Association. World Medical Association Declaration of Helsinki: Ethical principles for medical research involving human subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef]
- Okonko, I.O.; Ijandipe, L.A.; Ilusanya, O.A.; Donbraye-Emmanuel, O.B.; Ejembi, J.; Udeze, A.O.; Egun, O.C.; Fowotade, A.; Nkang, A.O. Incidence of urinary tract infection (UTI) among pregnant women in Ibadan, South-Western Nigeria. Afr. J. Biotechnol. 2009, 8, 6649–6657. [Google Scholar]
- Olayemi, J.O.; Olayinka, B.O.; Musa, A.I. Evaluation of Antibiotic Self-Medication Pattern Amongst Undergraduate Students of Ahmadu Bello University (Main Campus), Zaria. Res. J. Appl. Sci. Eng. Technol. 2010, 2, 35–38. [Google Scholar]
- Fakeye, T.O.; Adisa, R.; Olatunji, E. Self medication among hospitalized patients in selected secondary health facilities in South Western Nigeria. Pharm. Pract. 2010, 8, 233–237. [Google Scholar] [CrossRef]
- Biswas, M.; Roy, M.N.; Manik, M.I.N.; Hossain, M.S.; Tapu, S.M.T.A.; Moniruzzaman, M.; Sultana, S. Self medicated antibiotics in Bangladesh: A cross-sectional health survey conducted in the Rajshahi City. BMC Public Health 2014, 14, 847. [Google Scholar] [CrossRef] [PubMed]
- Shah, S.J.; Ahmad, H.; Rehan, R.B.; Najeeb, S.; Mumtaz, M.; Jilani, M.H.; Rabbani, M.S.; Alam, M.Z.; Farooq, S.; Kadir, M.M. Self-medication with antibiotics among non-medical university students of Karachi: A cross-sectional study. BMC Pharmacol. Toxicol. 2014, 15, 74. [Google Scholar] [CrossRef] [PubMed]
- Togoobaatar, G.; Ikeda, N.; Ali, M.; Sonomjamts, M.; Dashdemberel, S.; Mori, R.; Shibuya, K. Survey of non-prescribed use of antibiotics for children in an urban community in Mongolia. Bull. World Health Organ. 2010, 88, 930–936. [Google Scholar] [CrossRef] [PubMed]
- Abasaeed, A.; Vlcek, J.; Abuelkhair, M.; Kubena, A. Self-medication with antibiotics by the community of Abu Dhabi Emirate, United Arab Emirates. J. Infect. Dev. Ctries. 2009, 3, 491–497. [Google Scholar] [CrossRef] [PubMed]
- Chattaway, M.A.; Aboderin, A.O.; Fashae, K.; Okoro, C.K.; Opintan, J.A.; Okeke, I.N. Fluoroquinolone-Resistant Enteric Bacteria in Sub-Saharan Africa: Clones, Implications and Research Needs. Front. Microbiol. 2016, 7, 558. [Google Scholar] [CrossRef] [PubMed]
- Namboodiri, S.S.; Opintan, J.A.; Lijek, R.S.; Newman, M.J.; Okeke, I.N. Quinolone resistance in Escherichia coli from Accra, Ghana. BMC Microbiol. 2011, 11, 44. [Google Scholar] [CrossRef] [PubMed]
- Gelayee, D.A. Self-Medication Pattern among Social Science University Students in Northwest Ethiopia. J. Pharm. 2017, 2017, 8680714. [Google Scholar] [CrossRef] [PubMed]
- Sapkota, A.R.; Coker, M.E.; Rosenberg Goldstein, R.E.; Atkinson, N.L.; Sweet, S.J.; Sopeju, P.O.; Ojo, M.T.; Otivhia, E.; Ayepola, O.O.; Olajuyigbe, O.O.; et al. Self-medication with antibiotics for the treatment of menstrual symptoms in southwest Nigeria: A cross-sectional study. BMC Public Health 2010, 10, 610. [Google Scholar] [CrossRef] [PubMed]
- Major, C.; Vincze, Z.; Meskó, A.; Balogh, J.; Zelkó, R.; Németh, E. Medicating outside the consulting room. Orv. Hetil. 2007, 148, 291–298. [Google Scholar] [CrossRef] [PubMed]
- Afolabi, A.O. Factors influencing the pattern of self-medication in an adult Nigerian population. Ann. Afr. Med. 2008, 7, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Adinma, E.D.; Adinma, J.I.B. Perceptions and practices on menstruation amongst Nigerian secondary school girls. Afr. J. Reprod. Health 2008, 12, 74–83. [Google Scholar] [PubMed]
- Kimang’a, A.N. A Situational Analysis of Antimicrobial Drug Resistance in Africa: Are We Losing the Battle? Ethiop. J. Health Sci. 2012, 22, 135–143. [Google Scholar] [PubMed]
- Thriemer, K.; Katuala, Y.; Batoko, B.; Alworonga, J.-P.; Devlieger, H.; Van Geet, C.; Ngbonda, D.; Jacobs, J. Antibiotic prescribing in DR Congo: A knowledge, attitude and practice survey among medical doctors and students. PLoS ONE 2013, 8, e55495. [Google Scholar] [CrossRef] [PubMed]


| Characteristics | Frequency (N) | Percentage (%) | Characteristics | NDHS 2013 Men (%) | NDHS 2013 Women (%) |
|---|---|---|---|---|---|
| Sex | Sex | ||||
| Male | 173 | 48 | Male | NA | NA |
| Female | 185 | 52 | Female | NA | NA |
| Total | 358 | 100 | Total | ||
| Age group | Age group | ||||
| 14–19 | 23 | 7 | 15–19 | 20.9 | 20.1 |
| 20–25 | 204 | 60 | 20–24 | 16.7 | 17.3 |
| 26–31 | 111 | 33 | 25–29 | 15.9 | 18.3 |
| 32–37 | 1 | 0.3 | 30–34 | 13.9 | 14.0 |
| Others | 1 | 0.3 | 35–39 | 12.5 | 12.1 |
| Total | 340 | 100 | |||
| Academic Year | Level of education | ||||
| 1 | 122 | 35 | No education | 21.2 | 37.8 |
| 2 | 138 | 40 | Primary | 16.7 | 17.3 |
| 3 | 88 | 25 | Secondary | 47.7 | 35.8 |
| Total | 348 | 100 | More than secondary | 14.3 | 9.1 |
| Characteristics | Frequency (N) | Percentage (%) | Characteristics | NDHS 2013 Men (%) | NDHS 2013 Women (%) |
|---|---|---|---|---|---|
| Sex | Sex | ||||
| Male | 351 | 40 | Male | NA | NA |
| Female | 521 | 60 | Female | NA | NA |
| Total | 872 | 100 | Total | ||
| Age group | Age group | ||||
| 14–19 | 82 | 9.5 | 15–19 | 20.9 | 20.1 |
| 20–25 | 228 | 26 | 20–24 | 16.7 | 17.3 |
| 26–31 | 216 | 25 | 25–29 | 15.9 | 18.3 |
| 32–37 | 161 | 19 | 30–34 | 13.9 | 14.0 |
| 38–43 | 118 | 13.6 | 35–39 | 12.5 | 12.1 |
| 44–49 | 50 | 5.8 | 40–44 | 10.2 | 9.3 |
| >49 | 11 | 1.3 | 45–49 | 9.9 | 8.8 |
| Total | 866 | 100 | |||
| Occupation | Occupation | ||||
| Farmer | 111 | 14 | Agriculture | 33.7 | 15.6 |
| Housewife | 174 | 22 | Unskilled manual | 4.9 | 0.5 |
| Office job | 241 | 30.5 | Professional/technical | 11.3 | 7.4 |
| Self-employed | 150 | 19 | Skilled manual | 23.0 | 14.3 |
| Unemployed | 115 | 14.5 | |||
| Total | 791 | 100 | |||
| Marital status | Marital status | ||||
| Divorced | 34 | 41 | Divorced/separated | 1.2 | 2.1 |
| Married | 537 | 65 | Married | 49.1 | 69.4 |
| Single | 255 | 31 | Never married | 48.3 | 23.9 |
| Total | 826 | 100 | |||
| Educational status | Level of education | ||||
| None | 40 | 4.7 | No education | 21.2 | 37.8 |
| Primary | 59 | 7 | Primary | 16.7 | 17.3 |
| Secondary | 260 | 30.8 | Secondary | 47.7 | 35.8 |
| Tertiary | 484 | 57.5 | More than secondary | 14.3 | 9.1 |
| Total | 843 | 100 |
| Characteristics | Undergraduates | Community Members | Chi-Square |
|---|---|---|---|
| N (%) | N (%) | ||
| Frequency of antibiotics use | |||
| Weekly | 150 (43.2) | 231 (26.3) | |
| Monthly | 60 (17.3) | 237 (27) | |
| Once in two months | 65 (18.2) | 147 (16.7) | 53.3 *** |
| Every 3 months | 53 (15.3) | 128 (14.6) | |
| Others | 19 (6) | 137 (15.6) | |
| Total | 347 (100) | 880 (100) | |
| Who prescribed it? | |||
| Doctor | 65 (33.5) | 411 (57) | |
| Nurse | 56 (28.9) | 147 (20.4) | |
| Pharmacist | 49 (25.2) | 112 (15.5) | 34.6 *** |
| Others | 24 (12.4) | 51 (7.1) | |
| Total | 194 (100) | 721 (100) | |
| Place of purchase | |||
| Local chemist | 100 (33.3) | 350 (48.4) | |
| Patent medicine store | 119 (39.7) | 297 (41.1) | |
| Local drug hawkers | 68 (22.7) | 68 (9.4) | 49.9 *** |
| Others | 13 (4.3) | 8 (1.1) | |
| Total | 300 (100) | 723 (100) | |
| Did you comply with the duration of use of the antibiotics? | |||
| Yes | 288 (85.2) | 705 (83.5) | |
| No | 50 (14.8) | 139 (16.5) | 0.50 |
| Total | 338 (100) | 844 (100) | |
| Were there any side effects? | |||
| Yes | 92 (27.5) | 322 (39.6) | |
| No | 243 (72.5) | 492 (60.4) | 15.0 *** |
| Total | 335 (100) | 814 (100) | |
| Was the antibiotic effective in resolving the illness? | |||
| Excellent | 46 (13.7) | 172 (21.1) | |
| Satisfactory | 85 (25.3) | 327 (40.2) | |
| Good | 146 (43.4) | 274 (33.7) | 70.8 *** |
| No results | 59 (17.6) | 41 (5) | |
| Total | 336 (100) | 814 (100) |
| Characteristics | Undergraduates N (%) | Community Residents N (%) | Chi-Square |
|---|---|---|---|
| Antibiotics can cure all infections | |||
| True | 170 (47) | 509 (57.6) | 11.8 ** |
| False | 192 (53) | 374 (42.4) | |
| Total | 362 (100) | 883 (100) | |
| Antibiotics can be used for cold | |||
| True | 188 (52.4) | 440 (50) | 0.69 |
| False | 171 (47.6) | 444 (50) | |
| Total | 359 (100) | 884 (100) | |
| When I have cold, I should always take antibiotics | |||
| True | 153 (42.5) | 392 (44.7) | 0.50 |
| False | 207 (57.5) | 485 (55.3) | |
| Total | 360 (100) | 877 (100) | |
| Antibiotics can be used for body pains | |||
| True | 226 (62.8) | 357 (40.9) | 49.0 *** |
| False | 134 (37.2) | 516 (59.1) | |
| Total | 360 (100) | 873 (100) | |
| Antibiotics might be effective even if I don’t complete the dosage | |||
| True | 202 (56.1) | 412 (47.1) | 8.3 ** |
| False | 158 (43.9) | 463 (52.9) | |
| Total | 360 (100) | 875 (100) | |
| Unnecessary use of antibiotics makes them ineffective | |||
| True | 247 (68.4) | 542 (62.9) | 3.4 |
| False | 114 (31.6) | 320 (37.1) | |
| Total | 361 (100) | 862 (100) | |
| Have you heard of resistance to antibiotics | |||
| Yes | 239 (67) | 453 (53.4) | 18.8 *** |
| No | 118 (33) | 395 (46.6) | |
| Total | 357 (100) | 848 (100) | |
| Resistance to antibiotics can be caused by | |||
| Self-medication | 85 (32.6) | 310 (42.2) | 8.5 * |
| Not completing the dosage | 42 (16.1) | 118 (16) | |
| Using antibiotics repeatedly | 134 (51.3) | 307 (41.8) | |
| Total | 261 (100) | 735 (100) | |
| Level of awareness of antibiotics resistance | |||
| Low | 31 (12.1) | 65 (10) | 11.6 ** |
| Moderate | 156 (60.7) | 478 (72) | |
| High | 70 (27.2) | 121 (18) | |
| Total | 257 (100) | 664 (100) |
| Characteristics | Undergraduates N (%) | Community Residents N (%) | Chi-Square |
|---|---|---|---|
| With what do you take your antibiotics? | |||
| Water | 242 (71) | 718 (81.8) | 22.1 *** |
| Tea | 32 (9.4) | 44 (5) | |
| Juice | 15 (4.4) | 26 (3) | |
| Soft drinks | 34 (10) | 44 (5) | |
| Others | 18 (5.2) | 46 (5.2) | |
| Total | 341 (100) | 878 (100) | |
| Do you use left-over antibiotics from friends or family without doctor’s consultation? | |||
| Always | 42 (12.5) | 73 (8.5) | 43.7 *** |
| Sometimes | 193 (57.4) | 347 (40.3) | |
| Never | 101 (30.1) | 441 (51.2) | |
| Total | 336 (100) | 861 (100) | |
| Do you use antibiotics based on relative’s advice? | |||
| Always | 89 (25.4) | 160 (18.3) | 105.4 *** |
| Sometimes | 215 (61.4) | 329 (37.7) | |
| Never | 46 (13.2) | 384 (44) | |
| Total | 350 (100) | 873 (100) | |
| Do you use another family member’s antibiotics? | |||
| Always | 60 (17.2) | 121 (13.8) | 73.0 *** |
| Sometimes | 197 (56.5) | 294 (33.5) | |
| Never | 92 (26.4) | 462 (52.7) | |
| Total | 349 (100) | 877 (100) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ajibola, O.; Omisakin, O.A.; Eze, A.A.; Omoleke, S.A. Self-Medication with Antibiotics, Attitude and Knowledge of Antibiotic Resistance among Community Residents and Undergraduate Students in Northwest Nigeria. Diseases 2018, 6, 32. https://doi.org/10.3390/diseases6020032
Ajibola O, Omisakin OA, Eze AA, Omoleke SA. Self-Medication with Antibiotics, Attitude and Knowledge of Antibiotic Resistance among Community Residents and Undergraduate Students in Northwest Nigeria. Diseases. 2018; 6(2):32. https://doi.org/10.3390/diseases6020032
Chicago/Turabian StyleAjibola, Olumide, Olusola Akintoye Omisakin, Anthonius Anayochukwu Eze, and Semeeh Akinwale Omoleke. 2018. "Self-Medication with Antibiotics, Attitude and Knowledge of Antibiotic Resistance among Community Residents and Undergraduate Students in Northwest Nigeria" Diseases 6, no. 2: 32. https://doi.org/10.3390/diseases6020032
APA StyleAjibola, O., Omisakin, O. A., Eze, A. A., & Omoleke, S. A. (2018). Self-Medication with Antibiotics, Attitude and Knowledge of Antibiotic Resistance among Community Residents and Undergraduate Students in Northwest Nigeria. Diseases, 6(2), 32. https://doi.org/10.3390/diseases6020032





