A Systematic Review of the Use of Art in Virtual Reality
Abstract
:1. Introduction
2. Objectives
- What is the feasibility for non-adolescent brain injury patients to experience art therapy for motor neurorehabilitation in a virtual environment?
- What are the limitations of performing art therapy in VR?
3. Methods
3.1. Inclusion Criteria
3.2. Exclusion Criteria
3.3. Study Selection
4. Search Results
4.1. Article Exclusion
4.2. Data Extraction
5. Traditional Art Therapy
5.1. Digital Art Application
5.2. Art-Making Changes Brain Connectivity
5.3. Art Therapy for Parkinson’s Disease
5.4. Personal Journey Back to Mobility
6. Art Therapy in Virtual Reality: Brain Injury
6.1. Traditional Art-Making vs. Virtual Reality Art-Making
6.2. Art Improves Performance in Virtual Reality
6.3. Digital Art Program in Virtual Reality
7. Art Therapy in Virtual Reality: Healthy
7.1. Experiencing Art Therapy in Virtual Reality
7.2. Expert Art Therapists on Art Therapy in Virtual Reality
8. Discussion
9. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Van Lith, T.; Fenner, P.; Schofield, M.J. Art Therapy in Rehabilitation. In International Encyclopaedia of Rehabilitation; Stone, J.H., Blouin, M., Eds.; Center for International Rehabilitation Research Information and Exchange (CIRRIE): Buffalo, NY, USA, 2009. [Google Scholar]
- The Daily Californian. Available online: https://www.dailycal.org/2019/02/28/art-therapy-rehab/ (accessed on 4 August 2021).
- Perrin, T. Don’t Despise the Fluffy Bunny: A Reflection from Practice. Br. J. Occup. Ther. 2001, 64, 129–134. [Google Scholar] [CrossRef]
- Kline, T. Art Therapy for Individuals With Traumatic Brain Injury: A Comprehensive Neurorehabilitation-Informed Approach to Treatment. J. Abbr. 2016, 33, 67–73. [Google Scholar] [CrossRef]
- McGraw, M.K. Art therapy with brain-injured patients. Am. J. Art Ther. 1989, 28, 37–44. [Google Scholar]
- Kolb, B. Synaptic plasticity and the organization of behaviour after early and late brain injury. Can. J. Exp. Psychol. 1999, 10, 62–76. [Google Scholar] [CrossRef] [PubMed]
- Stepankova, H.; Lukavsky, J.; Buschkuehl, M.; Kopecek, M.; Ripova, D.; Jaeggi, S.M. The malleability of working memory and visuospatial skills: A randomized controlled study in older adults. Dev. Psychol. 2014, 50, 1049–1059. [Google Scholar] [CrossRef]
- Csikszentmihalyi, M.; Csikszentmihalyi, I.S. Optimal Experience: Psychological Studies of Flow in Consciousness, 1st ed.; Cambridge University Press: New York, NY, USA, 1992; pp. 1–31. [Google Scholar]
- Jung, R.E.; Segall, J.M.; Bockholt, H.J.; Flores, R.A.; Smith, S.M.; Chavez, R.S.; Haier, R.J. Neuroanatomy of creativity. Hum. Brain Mapp. 2010, 31, 398–409. [Google Scholar] [CrossRef] [PubMed] [Green Version]
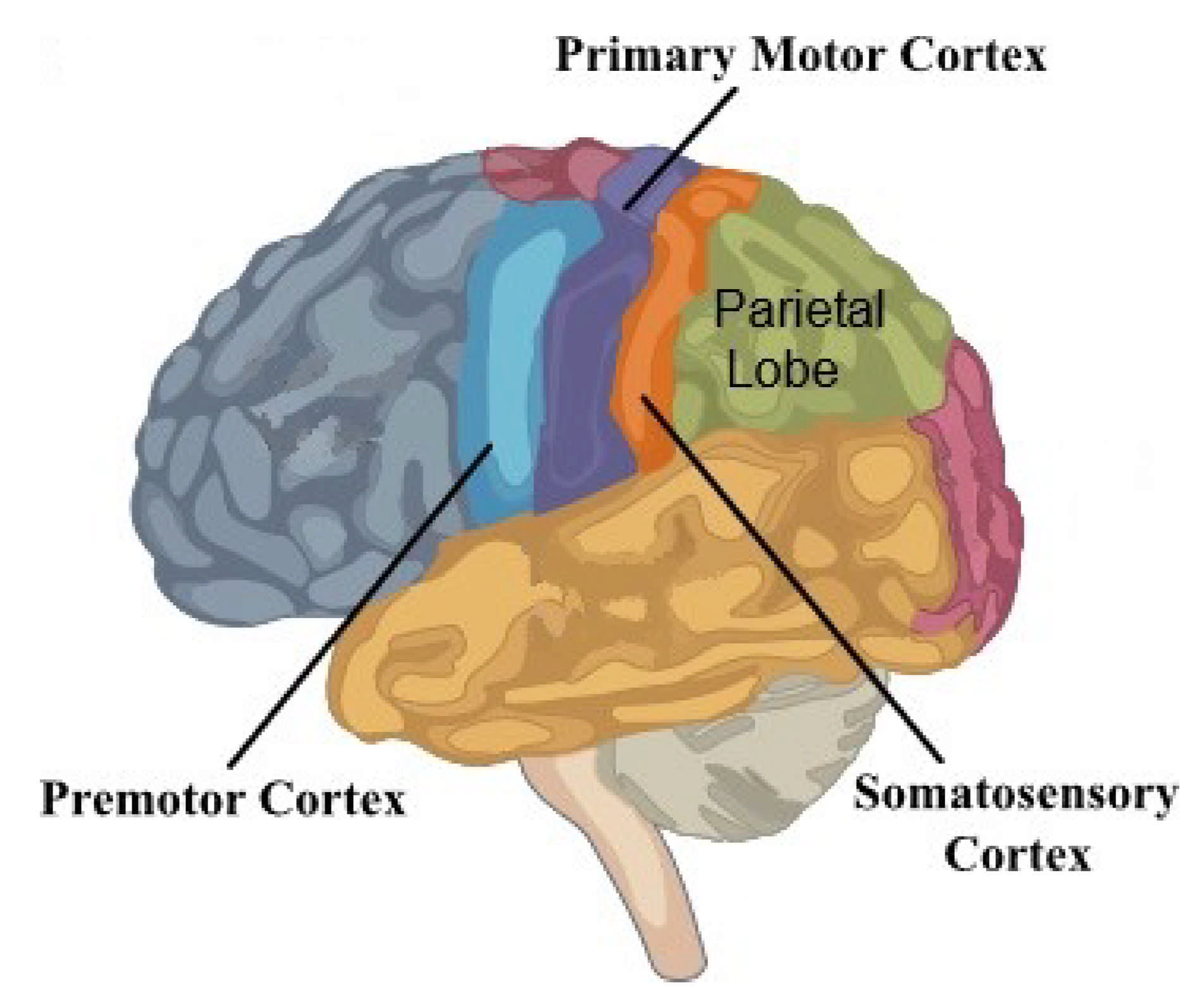
- Makuuchi, M.; Kaminaga, T.; Sugishita, M. Both parietal lobes are involved in drawing: A functional MRI study and implications for constructional apraxia. Cogn. Brain Res. 2003, 16, 338–347. [Google Scholar] [CrossRef]
- Hoshi, E.; Tanji, J. Distinctions between dorsal and ventral premotor areas: Anatomical connectivity and functional properties. Curr. Opin. Neurobiol. 2007, 17, 234–242. [Google Scholar] [CrossRef]
- Chegg. Diagram of Premotor Cortex. Available online: https://www.chegg.com/learn/biology/anatomy-physiology-in-biology/diagram-of-premotor-cortex (accessed on 5 September 2021).
- James, S.L.; Theadom, A. Global, regional, and national burden of traumatic brain injury and spinal cord injury, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019, 18, 56–87. [Google Scholar] [CrossRef] [Green Version]
- Brain Injury Association of America. Brain Injury Facts & Statistics. Available online: https://www.biausa.org/public-affairs/public-awareness/brain-injury-awareness (accessed on 4 August 2021).
- Smith, C. Innovative rehabilitation after head injury: Examining the use of a creative intervention. J. Soc. Work Pract. 2007, 21, 297–309. [Google Scholar] [CrossRef]
- Adamovich, S.V.; Merians, A.S.; Boian, R.; Tremaine, M.; Burdea, G.S.; Recce, M.; Poizner, H. A virtual reality based exercise system for hand rehabilitation post-stroke: Transfer to function. In Proceedings of the 26th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Francisco, CA, USA, 1–5 September 2004; pp. 4936–4939. [Google Scholar] [CrossRef]
- Jang, S.H.; You, S.H.; Hallett, M.; Cho, Y.W.; Park, C.M.; Cho, S.H.; Lee, H.Y.; Kim, T.H. Cortical reorganization and associated functional motor recovery after virtual reality in patients with chronic stroke: An experimenter-blind preliminary study. Arch. Phys. Med. Rehabil. 2005, 86, 2218–2223. [Google Scholar] [CrossRef]
- Holden, M.K.; Dyar, T. Virtual Environment Training: A New Tool for Neurorehabilitation. Neurol. Rep. 2002, 26, 62–71. [Google Scholar] [CrossRef]
- Merians, A.S.; Jack, D.; Boian, R.; Tremaine, M.; Burdea, G.C.; Adamovich, S.V.; Recce, M.; Poizner, H. Virtual Reality–Augmented Rehabilitation for Patients Following Stroke. Phys. Ther. 2002, 82, 898–915. [Google Scholar] [CrossRef] [Green Version]
- Broeren, J.; Rydmark, M.; Sunnerhagen, K.S. Virtual reality and haptics as a training device for movement rehabilitation after stroke: A single-case study. Arch. Phys. Med. Rehabil. 2004, 85, 1247–1250. [Google Scholar] [CrossRef] [PubMed]
- Bermudez i Badia, S.; Fluet, G.G.; Llorens, R.; Deutsch, J.E. Virtual Reality for Sensorimotor Rehabilitation Post Stroke: Design Principles and Evidence. In Neurorehabilitation Technology; Reinkensmeyer, D., Dietz, V., Eds.; Springer: Cham, Switzerland, 2016; pp. 573–603. [Google Scholar] [CrossRef]
- Vourvopoulos, A.; Jorge, C.; Abreu, R.; Figueiredo, P.; Fernandes, J.C.; Bermudez i Badia, S. Efficacy and Brain Imaging Correlates of an Immersive Motor Imagery BCI-Driven VR System for Upper Limb Motor Rehabilitation: A Clinical Case Report. Front. Hum. Neurosci. 2019, 13, 244. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Piron, L.; Tonin, P.; Piccione, F.; Iaia, V.; Trivello, E.; Dam, M. Virtual Environment Training Therapy for Arm Motor Rehabilitation. Presence 2005, 14, 732–740. [Google Scholar] [CrossRef]
- Tawfik, G.M.; Dila, K.A.S.; Mohamed, M.Y.F.; Tam, D.N.H.; Kien, N.D.; Ahmed, A.M.; Huy, N.T. A step by step guide for conducting a systematic review and meta-analysis with simulation data. Trop. Med. Health 2019, 47, 46. [Google Scholar] [CrossRef]
- Jones, J.P.; Drass, J.M.; Kaimal, G. Art therapy for military service members with post-traumatic stress and traumatic brain injury: Three case reports highlighting trajectories of treatment and recovery. Arts Psychother. 2019, 63, 18–30. [Google Scholar] [CrossRef]
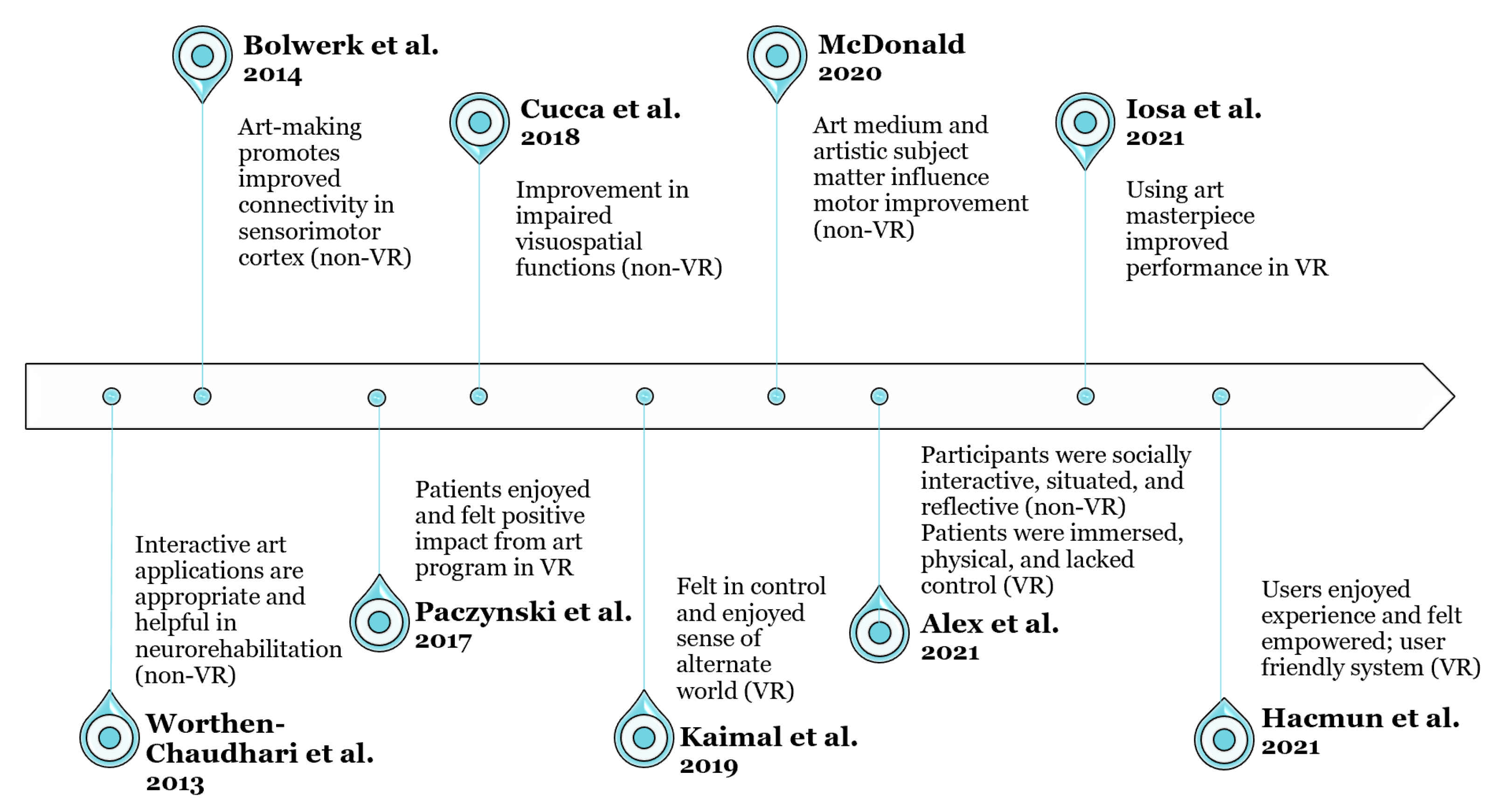
- Worthen-Chaudhari, L.; Whalen, C.N.; Swendal, C.; Bockbrader, M.; Haserodt, S.; Smith, R.; Bruce, M.K.; Mysiw, W.J. A feasibility study using interactive graphic art feedback to augment acute neurorehabilitation therapy. NeuroRehabilitation 2013, 33, 481–490. [Google Scholar] [CrossRef]
- Bolwerk, A.; Mack-Andrick, J.; Lang, F.R.; Dorfler, A.; Maihofner, C. How Art Changes Your Brain: Differential Effects of Visual Art Production and Cognitive Art Evaluation on Functional Brain Connectivity. PLoS ONE 2014, 9, e116548. [Google Scholar] [CrossRef]
- Paczynski, A.; Diment, L.; Hobbs, D.; Reynolds, K. Using Technology to Increase Activity, Creativity and Engagement for Older Adults Through Visual Art. In Mobile e-Health. Human-Computer Interaction Series; Marston, H., Freeman, S., Musselwhite, C., Eds.; Springer: Cham, Switzerland, 2017; pp. 97–114. [Google Scholar] [CrossRef]
- Cucca, A.; Acosta, I.; Berberian, M.; Lemen, A.C.; Rizzo, J.R.; Ghilardi, M.F.; Quartarone, A.; Feigin, A.S.; Di Rocco, A.; Biagioni, M.C. Visuospatial exploration and art therapy intervention in patients with Parkinson’s disease: An exploratory therapeutic protocol. Complement. Ther. Med. 2018, 40, 70–76. [Google Scholar] [CrossRef] [PubMed]
- Kaimal, G.; Carroll-Haskins, K.; Berberian, M.; Dougherty, A.; Carlton, N.; Ramakrishnan, A. Virtual Reality in Art Therapy: A Pilot Qualitative Study of the Novel Medium and Implications for Practice. J. Am. Art Ther. Assoc. 2019, 37, 16–24. [Google Scholar] [CrossRef]
- McDonald, B. My Journey Using Art as Physical Therapy. J. Humanit. Rehabil. 2020. Available online: https://www.jhrehab.org/2020/05/08/my-journey-using-art-as-physical-therapy/ (accessed on 1 May 2020).
- Alex, M.; Wunsche, B.C.; Lottridge, D. Virtual reality art-making for stroke rehabilitation: Field study and technology probe. Int. J. Hum.-Comput. Stud. 2021, 145, 102481. [Google Scholar] [CrossRef]
- Iosa, M.; Aydin, M.; Candelise, C.; Coda, N.; Morone, G.; Antonucci, G.; Marinozzi, F.; Bini, F.; Paolucci, S.; Gaetano, T. The Michelangelo Effect: Art Improves the Performance in a Virtual Reality Task Developed for Upper Limb Neurorehabilitation. Front. Psychol. 2021, 11, 1–8. [Google Scholar] [CrossRef]
- Hacmun, I.; Regev, D.; Salomon, R. Artistic creation in virtual reality for art therapy: A qualitative study with expert art therapists. Arts Psychother. 2021, 72, 101745. [Google Scholar] [CrossRef]
- Smith, D.; Wright, C.J.; Lakhani, A.; Zeeman, H. Art processes: A research tool for acquired brain injury and residential design. Arts Health 2017, 9, 251–268. [Google Scholar] [CrossRef]
- Park, D.C.; Reuter-Lorenz, P. The Adaptive Brain: Aging and Neurocognitive Scaffolding. Annu. Rev. Psychol. 2009, 60, 173–196. [Google Scholar] [CrossRef] [Green Version]
- Dickstein, R.; Dunsky, A.; Marcovitz, E. Motor Imagery for Gait Rehabilitation in Post-Stroke Hemiparesis. Phys. Ther. 2004, 84, 1167–1177. [Google Scholar] [CrossRef] [PubMed]
- Jackson, P.L.; Doyon, J.; Richards, C.L.; Malouin, F. The Efficacy of Combined Physical and Mental Practice in the Learning of a Foot-Sequence Task after Stroke: A Case Report. Neurorehabil. Neural Repair 2004, 18, 106–111. [Google Scholar] [CrossRef] [PubMed]
- Page, S.J. Imagery Improves Upper Extremity Motor Function in Chronic Stroke Patients: A Pilot Study. Occup. Ther. J. Res. 2000, 20, 200–215. [Google Scholar] [CrossRef]
- Page, S.J.; Levine, P.; Sisto, S.A.; Johnston, M.V. Mental Practice Combined with Physical Practice in Upper-Limb Motor Deficit in Subacute Stroke. Phys. Ther. 2001, 81, 1455–1462. [Google Scholar] [CrossRef]
- Yoo, E.; Park, E.; Chung, B. Mental practice effect on line-tracing accuracy in persons with hemiparetic stroke: A preliminary study. Arch. Phys. Med. Rehabil. 2001, 82, 1213–1218. [Google Scholar] [CrossRef]
- Crosbie, J.H.; McDonough, S.M.; Gilmore, D.H.; Wiggman, M.I. The adjunctive role of mental practice in the rehabilitation of the upper limb after hemiplegic stroke: A pilot study. Clin. Rehabil. 2004, 18, 60–68. [Google Scholar] [CrossRef]
- Stevens, J.A.; Stoykov, M.E.P. Using Motor Imagery in the Rehabilitation of Hemiparesis. Arch. Phys. Med. Rehabil. 2003, 84, 1090–1092. [Google Scholar] [CrossRef]
- Dijkerman, H.C.; Ietswaart, M.; Johnston, M.; MacWalter, R.S. Does motor imagery training improve hand function in chronic stroke patients? A pilot study. Clin. Rehabil. 2004, 18, 538–549. [Google Scholar] [CrossRef]
- Tilt Brush by Google. 2018. Available online: https://www.tiltbrush.com (accessed on 16 September 2021).
- Symons, J.; Clark, H.; Williams, K.; Hansen, E.; Orpin, P. Visual Art in Physical Rehabilitation: Experiences of People with Neurological Conditions. Br. J. Occup. Ther. 2011, 74, 44–52. [Google Scholar] [CrossRef]
- Chantios, E. Art Therapy. In Proceedings of the Frontiers of Clinical Practice—Environments for Recovery (3rd VBIRA Workshop); Victorian Brain Injury Recovery Association: Melbourne, Australia, 2005; pp. 56–61. [Google Scholar]
- Agnihotri, S.; Gray, J.; Colantonio, A.; Polatajko, H.; Cameron, D.; Wiseman-Hakes, C.; Rumney, P.; Keightley, M. Arts-based social skills interventions for adolescents with acquired brain injuries: Five case reports. Dev. Neurorehabil. 2014, 17, 44–63. [Google Scholar] [CrossRef] [PubMed]
- Zeki, S. Neural Concept Formation & Art: Dante, Michelangelo, Wagner. J. Conscious. Stud. 2002, 9, 53–76. [Google Scholar] [CrossRef]
- Lusebrink, V.B. Art Therapy and the Brain: An Attempt to Understand the Underlying Processes of Art Expression in Therapy. J. Am. Art Ther. Assoc. 2014, 21, 125–135. [Google Scholar] [CrossRef]
- King, J.L.; Knapp, K.E.; Shaikh, A.; Li, F.; Sabau, D.; Pascuzzi, R.M.; Osburn, L.L. Cortical Activity Changes after Art Making and Rote Motor Movement as Measured by EEG: A Preliminary Study. Biomed. J. Sci. Tech. Res. 2017, 1, 1062–1075. [Google Scholar] [CrossRef]
- Fugl-Meyer, A.R.; Laasko, L.; Leyman, I.; Olsson, S.; Steglind, S. The post-stroke hemiplegic patient. 1. A method for evaluation of physical performance. Scand. J. Rehabil. Med. 1975, 7, 13–31. [Google Scholar] [PubMed]

| Author (Year) | Pop Size (Avg Age) | Condition | Setting | Art Medium |
|---|---|---|---|---|
| Worthen-Chaudhari et al. (2013) [26] | 21 (57 ± 18) | motor impaired | non-VR | digital drawing |
| Bolwerk et al. (2014) [27] | 28 (64 ± 4) | healthy | non-VR | mixed media |
| Paczynski et al. (2017) [28] | 5 (84 ± 8) | stroke | VR | 3D painting (Splashboard) |
| Cucca et al. (2018) [29] | 20 (45–80) * 20 (45–80) * | Parkinson’s Disease, age-matched healthy | non-VR | mixed media |
| Kaimal et al. (2019) [30] | 17 (18–65) * | healthy | VR | 3D painting (GTB) |
| McDonald (2020) [31] | 1 (64–65) * | stroke | non-VR | mixed media |
| Alex et al. (2021) [32] | 14 (55–84) * | stroke | non-VR VR | mixed media, 3D painting (GTB) |
| Iosa et al. (2021) [33] | 4 (60 ± 13) | stroke | VR | 2D painting |
| Hacmun et al. (2021) [34] | 7 (42–75) * | expert art therapists | VR | 3D painting (GTB) |
| Author (Year) | Pop Size (Avg Age) | Condition | Art Medium | Results |
|---|---|---|---|---|
| Worthen-Chaudhari et al. (2013) [26] | 21 (57 ± 18) | motor impaired | digital drawing | Interactive art applications are appropriate and helpful in neurorehabilitation |
| Bolwerk et al. (2014) [27] | 28 (64 ± 4) | healthy | mixed media | Art-making promotes improved connectivity in sensorimotor cortex |
| Cucca et al. (2018) [29] | 20 (45–80) * 20 (45–80) * | Parkinson’s Disease, age-matched healthy | mixed media | Improvement in impaired visuospatial functions |
| McDonald (2020) [31] | 1 (64–65) * | stroke | mixed media | Art medium and artistic subject matter influenced motor improvement |
| Alex et al. (2021) [32] (non-VR) | 14 (55–84) * | stroke | mixed media | Participants were socially interactive, situated, and reflective |
| Author (Year) | Pop Size (Avg Age) | Condition | Art Medium | Results |
|---|---|---|---|---|
| Alex et al. (2021) [32] (VR) | 14 (55–84) * | stroke | 3D painting (GTB) | Patients were immersed, physical, and lacked control |
| Iosa et al. (2021) [33] | 4 (60 ± 13) | stroke | 2D painting | Significant improvements in art masterpiece group compared to control |
| Paczynski et al. (2017) [28] | 5 (84 ± 8) | stroke | 3D painting (Splashboard) | Patients enjoyed art program and showed above average velocities in upper body movement |
| Author (Year) | Pop Size (Avg Age) | Condition | Art Medium | Results |
|---|---|---|---|---|
| Kaimal et al. (2019) [30] | 17 (18–65) * | healthy | 3D painting (GTB) | Felt in control and free; enjoyed sense of alternate world |
| Hacmun et al. (2021) [34] | 7 (42–75) * | expert art therapists | 3D painting (GTB) | Enjoyed experience; user-friendly; felt empowered |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aldridge, A.; Bethel, C.L. A Systematic Review of the Use of Art in Virtual Reality. Electronics 2021, 10, 2314. https://doi.org/10.3390/electronics10182314
Aldridge A, Bethel CL. A Systematic Review of the Use of Art in Virtual Reality. Electronics. 2021; 10(18):2314. https://doi.org/10.3390/electronics10182314
Chicago/Turabian StyleAldridge, Audrey, and Cindy L. Bethel. 2021. "A Systematic Review of the Use of Art in Virtual Reality" Electronics 10, no. 18: 2314. https://doi.org/10.3390/electronics10182314
APA StyleAldridge, A., & Bethel, C. L. (2021). A Systematic Review of the Use of Art in Virtual Reality. Electronics, 10(18), 2314. https://doi.org/10.3390/electronics10182314






