Crossover-Use of Human Antibiotics in Livestock in Agricultural Communities: A Qualitative Cross-Country Comparison between Uganda, Tanzania and India
Abstract
1. Introduction
2. Results
2.1. Characterising the Practice of Human Antibiotic Crossover-Use
2.1.1. How Medicine-Providers and Livestock-Keepers Describe Crossover-Use
“People use these drugs interchangeably, so we have a very big problem.”—MP5-Veterinary drug shop, Uganda
“The role of these people [veterinary drug shops] is to health educate clients [on] the danger of using human medicine to treat animals… So, their role is to tell people …not to go to human drugs shops to buy drugs to treat animals.”—MP1-Human drug shop Uganda
“Like that he will tell you ‘give me doxy, I am going to give to chickens’. Now I am not sure because when he takes things like that you don’t know if he is going to consume [himself] or treat his chicken.”—MP3-Human drug shop, Tanzania
“Interviewer: Are there cases where one will buy human medicine, like chloramphenicol to give to poultry?
Respondent 1: (Laughter) It’s there and so common.”—MP2-Veterinary drug shop, Uganda
“They [livestock-keeper] will say ‘Musawo [doctor], give me medicine for chicken’. You will ask them what that medicine looks like. He will even know the colour of the drug, saying ‘I want the white capsules to give to chicken or a goat’.”—MP7-Human drug shop, Uganda
2.1.2. Animals Treated and Human Antibiotics Used in Crossover-Use
“Some people have HIV so they will share ARVs with pigs at home because they have the mentality that when the human takes ARVs they grow fat, so they also try it on pigs.”—MP6–Veterinary drug shop, Uganda
2.2. Factors Influencing Antibiotic Crossover-Use
2.2.1. Medicine-Providers’ and Livestock-Keepers’ Perceptions of the Effectiveness and Safety of Antibiotics
Human and Animal Antibiotics Are the Same
“We just think that if it works for humans, it might work in the cows for the same problem. That’s what we think.”—LK7, India
Human Antibiotics Are More Effective and Better Quality
“Even people who rear chicken on large scale do this [use human antibiotics] but what brings this about is using antibiotics when chickens are not sick so when they use enrofloxacin for human they will be trying to look for an antibiotic that can cover the diseases they want to treat, because these [veterinary antibiotics] are over used and the [chicken’s] bodies are now used to them.”—MP6-Veterinary drug shop, Uganda
“I have seen some human medicine works very much in animals. I have seen in mastitis my medicine is not working but [brand name redacted], amoxicillin and clavulanic acid (human antibiotic) works. Quality of human antibiotics is better.”—MP9-Para-vet, India
Safety Considerations
"A person came to me and asked, ‘Doctor my goat is having loose motion, what can we do?’ If I see the condition of the goat is really bad and it might die without a treatment, I may ask him to have a human medicine of a low dose.”—MP1-Informal human health provider, India
“We don’t want to take that risk. Maybe the cow was going to die anyway, but if it dies after taking medicines from my store it could create a problem. We still give medicine if there’s an emergency. Otherwise, it’s preferred that you have a prescription from a veterinarian…In case he isn’t there, we try and give medicines understanding the symptoms, we suggest the dose.”—MP17-Human drug shop, India
2.2.2. Livestock-Keepers’ Sources of Information
Trial and Error and Word of Mouth
“Even me when we were still young, we bought human antibiotics and gave it to chicken…The veterinary doctor came and immunized our chickens and they failed to respond, so the neighbours to mammy told her to buy CAF [chloramphenicol] and give it to them or else they will die. Mummy bought the drug, and we gave them, and they got healed. Since we never called the veterinary doctor again.”—MP4-Human drug shop, Uganda
“She will come and place an order for more drugs and tries to explain how the capsules look like, if you ask why she’s taking them, and then she will tell you ‘that I give to poultry, and they respond well to it’.”—MP3-Human drug shop, Uganda
Advice from Medicine-Providers
“I don’t know much about medicines. The veterinary doctor tells me that some medicines work the same for animals and humans. So, they give the medicines.”—LK5, India
2.2.3. Differences in Availability of Human and Veterinary Services and Antibiotics
Veterinary Services Less Easily Accessible than Human
Lack of Desired Veterinary Antibiotic Formulations
“Suppose my oxytetracycline get finished I have to go [to] Sarisha then. But if there is human oxytetracycline nearby then I use that.”—MP12-Animal development volunteer, India
"The government is giving medicines in a limited way. So that is how the human thing is coming to veterinary practice.”—MP14-Private veterinarian, India
Unsuitable Packaging Size
“Another challenge is that when we go to treat animals, once you open an ampoule of a given drug it must be used within 7 days before it goes bad or it gets spilt, yet we do not use it all at once, so it usually goes bad, and we tend to exploit the farmers in terms of cost recovery in the business aspect.”—MP2-Veterinary drug shop, Uganda
Human Antibiotics Easy to Acquire over the Counter
“You don’t need a prescription to dispense… there are many shops, human chemist shops, that deal with [human] antibiotics, and they will take it out and give it to the para-vets. It is very easily available, it’s easily available.”—MP14-Private veterinarian, India
“For me, what I think would be our role as both human and veterinary system is to guide our clients before we sell the drugs to them. More so the human drugs would only be sold on prescription only, but this open system of ours is the one causing problems, where people come in as they wish, buy drugs, and take.”—MP2-Veterinary drug shop, Uganda
2.2.4. Economic Incentives and Pressures
Human Antibiotics Are Cheaper
“The human medicine costs lesser than animals, like the medicine for loose motion for human costs 2 rupees while tablet for cow one tablet costs 40–80 rupees. Why would we use that?”—LK1, India
Economic Incentives and Pressures for Selling Human Antibiotics for Animals
“They will say, ‘Give me chloramphenicol. Give me amoxicillin’… ‘I am going to give it to chicken.’ And you will tell them that it is not for chicken. And they will say, ‘Just give me. Me I want to use it.’ Because we are in a competitive society and people have to look for bread, you end up giving out. Because if you don’t, what will you eat? What will you use to pay the bills?”—MP7-Human drug shop, Uganda
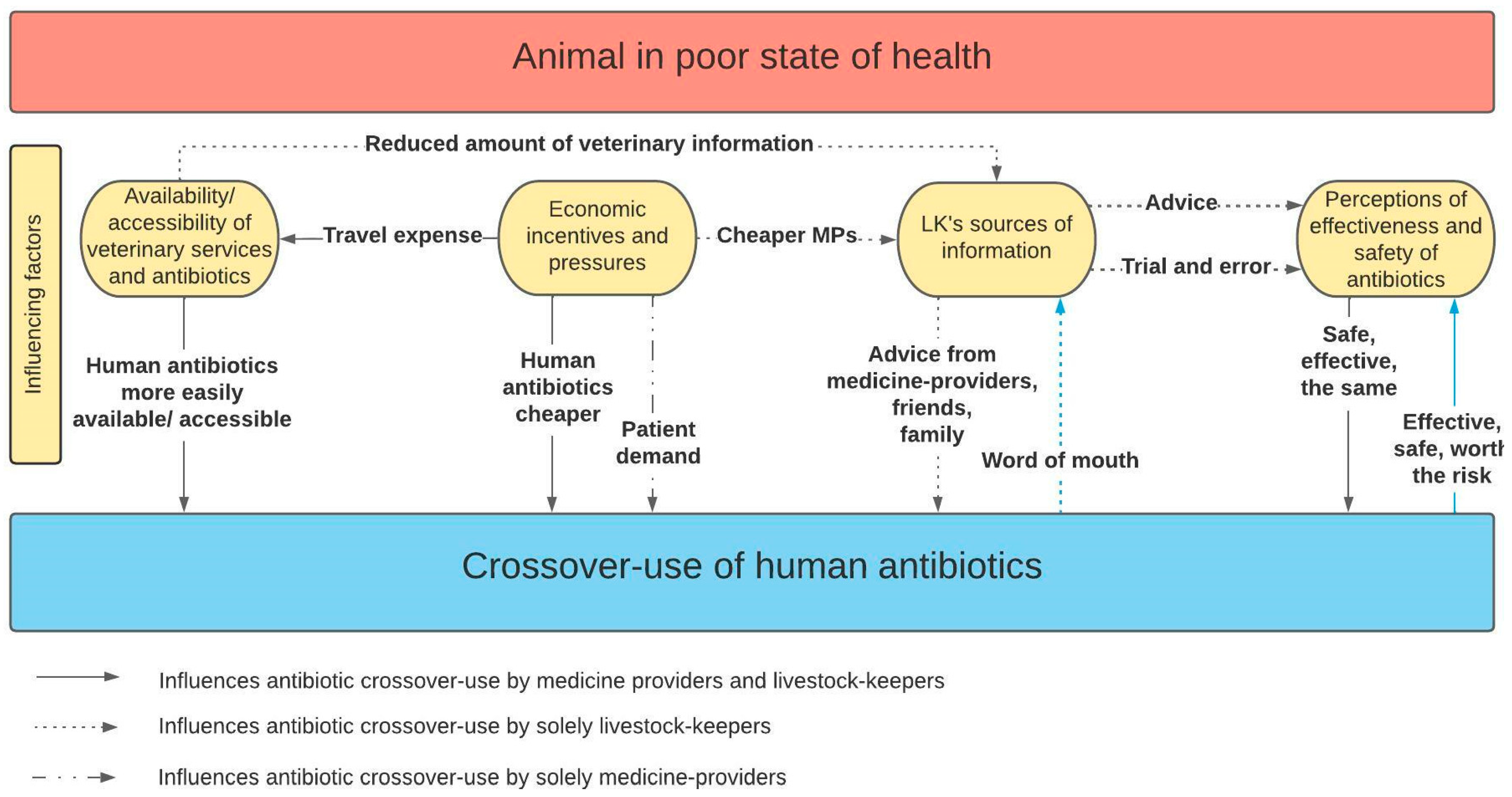
2.2.5. Summary of Factors Influencing Crossover-Use
Human Antibiotics Used in Crossover-Use
3. Discussion
4. Materials and Methods
4.1. Study Design
4.2. Study Setting
4.2.1. Study Sites
4.2.2. Study Respondents
4.3. Data Collection
4.4. Data Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Murray, C.J.; Ikuta, K.S.; Sharara, F.; Swetschinski, L.; Robles Aguilar, G.; Gray, A.; Han, C.; Bisignano, C.; Rao, P.; Wool, E.; et al. Global burden of bacterial antimicrobial resistance in 2019: A systematic analysis. Lancet 2022, 399, 629–655. [Google Scholar] [CrossRef]
- Beović, B. The issue of antimicrobial resistance in human medicine. Int. J. Food Microbiol. 2006, 112, 280–287. [Google Scholar] [CrossRef] [PubMed]
- Holmes, A.H.; Moore, L.S.; Sundsfjord, A.; Steinbakk, M.; Regmi, S.; Karkey, A.; Guerin, P.J.; Piddock, L.J. Understanding the mechanisms and drivers of antimicrobial resistance. Lancet 2016, 387, 176–187. [Google Scholar] [CrossRef]
- Wistrand-Yuen, E.; Knopp, M.; Hjort, K.; Koskiniemi, S.; Berg, O.G.; Andersson, D.I. Evolution of high-level resistance during low-level antibiotic exposure. Nat. Commun. 2018, 9, 1599. [Google Scholar] [CrossRef] [PubMed]
- Klein, E.Y.; Van Boeckel, T.P.; Martinez, E.M.; Pant, S.; Gandra, S.; Levin, S.A.; Goossens, H.; Laxminarayan, R. Global increase and geographic convergence in antibiotic consumption between 2000 and 2015. Proc. Natl. Acad. Sci. USA 2018, 115, E3463–E3470. [Google Scholar] [CrossRef]
- James, S.L.; Murray, C.J.L.; Abate, D.; Abate, K.H.; Abay, S.M.; Abbafati, C.; Abbasi, N.; Abbastabar, H.; Abd-Allah, F.; Abdela, J.; et al. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1789–1858. [Google Scholar] [CrossRef]
- Klein, E.Y.; Milkowska-Shibata, M.; Tseng, K.K.; Sharland, M.; Gandra, S.; Pulcini, C.; Laxminarayan, R. Assessment of WHO antibiotic consumption and access targets in 76 countries, 2000–2015: An analysis of pharmaceutical sales data. Lancet Infect. Dis. 2021, 21, 107–115. [Google Scholar] [CrossRef]
- Jacobs, T.G.; Robertson, J.; van den Ham, H.A.; Iwamoto, K.; Bak Pedersen, H.; Mantel-Teeuwisse, A.K. Assessing the impact of law enforcement to reduce over-the-counter (OTC) sales of antibiotics in low- and middle-income countries; a systematic literature review. BMC Health Serv. Res. 2019, 19, 536. [Google Scholar] [CrossRef]
- Van Boeckel, T.P.; Brower, C.; Gilbert, M.; Grenfell, B.T.; Levin, S.A.; Robinson, T.P.; Teillant, A.; Laxminarayan, R. Global trends in antimicrobial use in food animals. Proc. Natl. Acad. Sci. USA 2015, 112, 5649–5654. [Google Scholar] [CrossRef] [PubMed]
- Laxminarayan, R.; Matsoso, P.; Pant, S.; Brower, C.; Røttingen, J.-A.; Klugman, K.; Davies, S. Access to effective antimicrobials: A worldwide challenge. Lancet 2016, 387, 168–175. [Google Scholar] [CrossRef]
- World Organisation for Animal Health (WOAH). OIE Fifth Annual Report Factsheet: Antimicrobial Agents Intended for Use in Animals; World Organisation for Animal Health (WOAH): Paris, France, 2021. [Google Scholar]
- Lowder, S.K.; Sánchez, M.V.; Bertini, R. Which farms feed the world and has farmland become more concentrated? World Dev. 2021, 142, 105455. [Google Scholar] [CrossRef]
- Herrero, M.; Thornton, P.K.; Power, B.; Bogard, J.R.; Remans, R.; Fritz, S.; Gerber, J.S.; Nelson, G.; See, L.; Waha, K.; et al. Farming and the geography of nutrient production for human use: A transdisciplinary analysis. Lancet Planet. Health 2017, 1, e33–e42. [Google Scholar] [CrossRef]
- Centre for Disease Control | One Health. Available online: https://www.cdc.gov/onehealth/index.html (accessed on 5 May 2021).
- World Health Organisation. Global Action Plan on Antimicrobial Resistance; WHO: Geneva, Switzerland, 2015; Available online: https://www.who.int/publications/i/item/9789241509763 (accessed on 5 July 2021).
- Ministry of Health and Family Welfare. National Action Plan on Antimicrobial Resistance; Government of India: New Delhi, India, 2017.
- Ministry of Health Tanzania. The National Action Plan on Antimicrobial Resistance 2017–2022; The United Republic of Tanzania: Dar es Salaam, Tanzania, 2017. Available online: https://www.afro.who.int/publications/national-action-plan-antimicrobial-resistance-2017-2022 (accessed on 29 April 2021).
- Government of Uganda. Antimicrobial Resistance National Action Plan 2018–2023; Government of Uganda: Kampala, Uganda, 2018. Available online: https://cddep.org/wp-content/uploads/2018/12/GoU_AMR-NAP.pdf (accessed on 29 April 2021).
- McCubbin, K.D.; Ramatowski, J.W.; Buregyeya, E.; Hutchinson, E.; Kaur, H.; Mbonye, A.K.; Mateus, A.L.P.; Clarke, S.E. Unsafe “crossover-use” of chloramphenicol in Uganda: Importance of a One Health approach in antimicrobial resistance policy and regulatory action. J. Antibiot. 2021, 74, 417–420. [Google Scholar] [CrossRef]
- Omeiza, G.K.; Kabir, J.; Mamman, M.; Ibrahim, H.; Fagbamila, I.O. Response of Nigerian farmers to a questionnaire on chloramphenicol application in commercial layers. Vet. Ital. 2012, 48, 87–93. [Google Scholar] [PubMed]
- Om, C.; McLaws, M.L. Antibiotics: Practice and opinions of Cambodian commercial farmers, animal feed retailers and veterinarians. Antimicrob Resist. Infect Control. 2016, 5, 42. [Google Scholar] [CrossRef]
- Rimi, N.A.; Sultana, R.; Ishtiak-Ahmed, K.; Haider, N.; Azziz-Baumgartner, E.; Nahar, N.; Luby, S.P. Where backyard poultry raisers seek care for sick poultry: Implications for avian influenza prevention in Bangladesh. BMC Public Health 2018, 18, 969. [Google Scholar] [CrossRef]
- Snively-Martinez, A.E. Ethnographic Decision Modeling to Understand Smallholder Antibiotic Use for Poultry in Guatemala. Med. Anthr. 2019, 38, 295–310. [Google Scholar] [CrossRef]
- Suy, S.; Rego, S.; Bory, S.; Chhorn, S.; Phou, S.; Prien, C.; Heng, S.; Wu, S.; Legido-Quigley, H.; Hanefeld, J.; et al. Invisible medicine sellers and their use of antibiotics: A qualitative study in Cambodia. BMJ Glob. Health 2019, 4, e001787. [Google Scholar] [CrossRef] [PubMed]
- Gemeda, B.A.; Amenu, K.; Magnusson, U.; Dohoo, I.; Hallenberg, G.S.; Alemayehu, G.; Desta, H.; Wieland, B. Antimicrobial Use in Extensive Smallholder Livestock Farming Systems in Ethiopia: Knowledge, Attitudes, and Practices of Livestock Keepers. Front. Vet. Sci. 2020, 7, 55. [Google Scholar] [CrossRef]
- Arnold, J.-C.; Day, D.; Hennessey, M.; Alarcon, P.; Gautham, M.; Samanta, I.; Mateus, A. “If It Works in People, Why Not Animals?”: A Qualitative Investigation of Antibiotic Use in Smallholder Livestock Settings in Rural West Bengal, India. Antibiotics 2021, 10, 1433. [Google Scholar] [CrossRef] [PubMed]
- Musoke, D.; Namata, C.; Lubega, G.B.; Kitutu, F.E.; Mugisha, L.; Amir, S.; Brandish, C.; Gonza, J.; Ikhile, D.; Niyongabo, F.; et al. Access, use and disposal of antimicrobials among humans and animals in Wakiso district, Uganda: A qualitative study. J. Pharm. Policy Pract. 2021, 14, 69. [Google Scholar] [CrossRef]
- Bennani, H.; Mateus, A.; Mays, N.; Eastmure, E.; Stärk, K.D.C.; Häsler, B. Overview of Evidence of Antimicrobial Use and Antimicrobial Resistance in the Food Chain. Antibiotics 2020, 9, 49. [Google Scholar] [CrossRef] [PubMed]
- WHO Releases the 2019 AWaRe Classification Antibiotics. Available online: https://www.who.int/news/item/01-10-2019-who-releases-the-2019-aware-classification-antibiotics (accessed on 29 March 2022).
- Boothe, D. Phenicols. Veterinary Maual. 2015. Available online: https://www.merckvetmanual.com/pharmacology/antibacterial-agents/phenicols (accessed on 28 July 2021).
- National Toxicology Program, Department of Health and Human Services. Report on Carcinogens Background Document for Chloramphenicol; National Institutes of Health: Bethesda, MD, USA, 2000.
- World Health Organization. WHO List of Critically Important Antimicrobials for Human Medicine (WHO CIA List); World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- Iwu, C.D.; Korsten, L.; Okoh, A.I. The incidence of antibiotic resistance within and beyond the agricultural ecosystem: A concern for public health. Microbiolyopen 2020, 9, e1035. [Google Scholar] [CrossRef]
- Hoelzer, K.; Wong, N.; Thomas, J.; Talkington, K.; Jungman, E.; Coukell, A. Antimicrobial drug use in food-producing animals and associated human health risks: What, and how strong, is the evidence? BMC Vet. Res. 2017, 13, 211. [Google Scholar] [CrossRef] [PubMed]
- Mukonzo, J.K.; Namuwenge, P.M.; Okure, G.; Mwesige, B.; Namusisi, O.K.; Mukanga, D. Over-the-counter suboptimal dispensing of antibiotics in Uganda. J. Multidiscip. Healthc. 2013, 6, 303–310. [Google Scholar] [CrossRef] [PubMed]
- Dillip, A.; Embrey, M.; Shekalaghe, E.; Ross-Degnan, D.; Vialle-Valentin, C.; Kimatta, S.; Liana, J.; Rutta, E.; Valimba, R.; Chalker, J. What motivates antibiotic dispensing in accredited drug dispensing outlets in Tanzania? A qualitative study. Antimicrob. Resist. Infect. Control. 2015, 4, 30. [Google Scholar] [CrossRef]
- Barker, A.K.; Brown, K.; Ahsan, M.; Sengupta, S.; Safdar, N. Social determinants of antibiotic misuse: A qualitative study of community members in Haryana, India. BMC Public Health 2017, 17, 333. [Google Scholar] [CrossRef] [PubMed]
- Mayora, C.; Kitutu, F.E.; Kandala, N.-B.; Ekirapa-Kiracho, E.; Peterson, S.S.; Wamani, H. Private retail drug shops: What they are, how they operate, and implications for health care delivery in rural Uganda. BMC Health Serv. Res. 2018, 18, 532. [Google Scholar] [CrossRef]
- Matin, M.A.; Khan, W.A.; Karim, M.M.; Ahmed, S.; John-Langba, J.; Sankoh, O.A.; Gyapong, M.; Kinsman, J.; Wertheim, H. What influences antibiotic sales in rural Bangladesh? A drug dispensers’ perspective. J. Pharm. Policy Pract. 2020, 13, 20. [Google Scholar] [CrossRef]
- Ndaki, P.; Mushi, M.; Mwanga, J.; Konje, E.; Ntinginya, N.; Mmbaga, B.; Keenan, K.; Sabiiti, W.; Kesby, M.; Benitez-Paez, F.; et al. Dispensing Antibiotics without Prescription at Community Pharmacies and Accredited Drug Dispensing Outlets in Tanzania: A Cross-Sectional Study. Antibiotics 2021, 10, 1025. [Google Scholar] [CrossRef]
- Do, N.T.T.; Vu, H.T.L.; Nguyen, C.T.K.; Punpuing, S.; Khan, W.A.; Gyapong, M.; Asante, K.P.; Munguambe, K.; Gómez-Olivé, F.X.; John-Langba, J.; et al. Community-based antibiotic access and use in six low-income and middle-income countries: A mixed-method approach. Lancet Glob. Health 2021, 9, e610–e619. [Google Scholar] [CrossRef]
- Horumpende, P.G.; Sonda, T.B.; van Zwetselaar, M.; Antony, M.L.; Tenu, F.F.; Mwanziva, C.E.; Shao, E.R.; Mshana, S.E.; Mmbaga, B.T.; Chilongola, J.O. Prescription and non-prescription antibiotic dispensing practices in part I and part II pharmacies in Moshi Municipality, Kilimanjaro Region in Tanzania: A simulated clients approach. PLoS ONE 2018, 13, e0207465. [Google Scholar] [CrossRef]
- Dione, M.M.; Amia, W.C.; Ejobi, F.; Ouma, E.A.; Wieland, B. Supply Chain and Delivery of Antimicrobial Drugs in Smallholder Livestock Production Systems in Uganda. Front. Vet. Sci. 2021, 8, 611076. [Google Scholar] [CrossRef]
- Ministry of Health and FamilyWelfare. The Drugs and Cosmetics Act and Rules; Government of India: New Delhi, India, 2016. [Google Scholar]
- The United Republic of Tanzania. The Tanzania Food, Drugs and Cosmetics (Scheduling of Medicines) (Amendment) Regulations 2018, 63rd ed.; The United Republic of Tanzania: Dar es Salaam, Tanzania, 2018. Available online: https://www.tmda.go.tz/uploads/publications/en1545378328-The%20Tanzania%20Food,%20Drugs%20and%20Cosmetics%20(Scheduling%20of%20Medicines)%20(Amendments)%20%20Regulations,%202018%20.pdf (accessed on 31 January 2022).
- National Drug Authority. Licensing Renewal and New Licences for Class C Drug Shops; National Drug Authority: Kampala, Uganda, 2018. Available online: https://www.nda.or.ug/nda/files/downloads/Professional%20licensing%20Guidelines%202018-Licensing%20Renewal%20and%20new%20Licenses%20%20for%20class%20C%20drug%20shops.pdf (accessed on 28 January 2022).
- National Drug Authority. The National Drug Policy and Authority Act; Uganda Legal Information Institute: Kampala, Uganda, 1993; p. 52. Available online: https://www.nda.or.ug/wp-content/uploads/2022/03/National-Drug-Policy-Authority-Act-Cap-206.pdf (accessed on 4 January 2022).
- The United Republic of Tanzania. The Tanzania Food, Drugs and Cosmetics (Scheduling of Medicines) Regulations 2015, 63rd ed.; The United Republic of Tanzania: Dar es Salaam, Tanzania, 2015. Available online: https://www.tanzania.go.tz/egov_uploads/documents/THE_TANZANIA_FOOD,_DRUGS_AND_COSMETICS_(SCHEDULING_OF_MEDICINES)_sw.pdf (accessed on 31 January 2022).
- Mikecz, O.; Pica-Ciamarra, U.; Felis, A.; Nizeyimana, G.; Okello, P.; Brunelli, C. Data on antimicrobial use in livestock: Lessons from Uganda. One Health 2020, 10, 100165. [Google Scholar] [CrossRef]
- Queenan, K.; Chandler, C.I.R.; Goodman, C. A Review of Methods and Metrics for Studying Human and Livestock Antibiotic Use at the Granular Level; A Pre-Read for Roundtable Discussion in London: Lodon, UK, 2017; Available online: https://amr.lshtm.ac.uk/researchprojects/metrics-and-methods-for-assessing-antibiotic-use/ (accessed on 1 September 2022).
- Ming, A.; Puddle, J.; Wilson, H. Antimicrobial Resistance: The Role of Regulation; University College London: London, UK, 2019. [Google Scholar]
- Food and Agricultural Organisation; PRASARI. Livelihood Zones Analysis in West Bengal; FAO: Rome, Italy, 2011; Available online: http://www.fao.org/3/bl063e/bl063e.pdf (accessed on 12 June 2021).
- Gautham, M.; Shyamprasad, K.M.; Singh, R.; Zachariah, A.; Singh, R.; Bloom, G. Informal rural healthcare providers in North and South India. Health Policy Plan 2014, 29, i20–i29. [Google Scholar] [CrossRef]
- Embrey, M.; Vialle-Valentin, C.; Dillip, A.; Kihiyo, B.; Mbwasi, R.; Semali, I.A.; Chalker, J.C.; Liana, J.; Lieber, R.; Johnson, K.; et al. Understanding the Role of Accredited Drug Dispensing Outlets in Tanzania’s Health System. PLoS ONE 2016, 11, e0164332. [Google Scholar] [CrossRef]
- Mbonye, A.K.; Buregyeya, E.; Rutebemberwa, E.; Clarke, S.E.; Lal, S.; Hansen, K.S.; Magnussen, P.; Larussa, P. Prescription for antibiotics at drug shops and strategies to improve quality of care and patient safety: A cross-sectional survey in the private sector in Uganda. BMJ Open 2016, 6, e010632. [Google Scholar] [CrossRef][Green Version]
- Caudell, M.A.; Dorado-Garcia, A.; Eckford, S.; Creese, C.; Byarugaba, D.K.; Afakye, K.; Chansa-Kabali, T.; Fasina, F.O.; Kabali, E.; Kiambi, S.; et al. Towards a bottom-up understanding of antimicrobial use and resistance on the farm: A knowledge, attitudes, and practices survey across livestock systems in five African countries. PLoS ONE 2020, 15, e0220274. [Google Scholar] [CrossRef]
- Gautham, M.; Spicer, N.; Chatterjee, S.; Goodman, C. What are the challenges for antibiotic stewardship at the community level? An analysis of the drivers of antibiotic provision by informal healthcare providers in rural India. Soc. Sci. Med. 2021, 275, 113813. [Google Scholar] [CrossRef]
- Caudell, M.A.; Mair, C.; Subbiah, M.; Matthews, L.; Quinlan, R.J.; Quinlan, M.B.; Zadoks, R.; Keyyu, J.; Call, D.R. Identification of risk factors associated with carriage of resistant Escherichia coli in three culturally diverse ethnic groups in Tanzania: A biological and socioeconomic analysis. Lancet Planet. Health 2018, 2, e489–e497. [Google Scholar] [CrossRef]
- Kakkar, M.; Walia, K.; Vong, S.; Chatterjee, P.; Sharma, A. Antibiotic resistance and its containment in India. BMJ 2017, 358, j2687. [Google Scholar] [CrossRef]
- Hounmanou, G.; Mdegela, H. Current situation for antimicrobial use, antimicrobial resistance and antimicrobial residues in the food and agriculture sectors in Tanzania: A review. Tanzan. Vet. J. 2017, 35, 58–62. [Google Scholar]
- Laxminarayan, R.; Chaudhury, R.R. Antibiotic Resistance in India: Drivers and Opportunities for Action. PLoS Med. 2016, 13, e1001974. [Google Scholar] [CrossRef]
- Porter, G.; Kotwani, A.; Bhullar, L.; Joshi, J. Over-the-counter sales of antibiotics for human use in India: The challenges and opportunities for regulation. Med. Law Int. 2021, 21, 147–173. [Google Scholar] [CrossRef]
- Olaniran, A.; Smith, H.; Unkels, R.; Bar-Zeev, S.; van den Broek, N. Who is a community health worker?—A systematic review of definitions. Glob. Health Action 2017, 10, 1272223. [Google Scholar] [CrossRef]
- Dillip, A.; Kimatta, S.; Embrey, M.; Chalker, J.C.; Valimba, R.; Malliwah, M.; Meena, J.; Lieber, R.; Johnson, K. Can formalizing links among community health workers, accredited drug dispensing outlet dispensers, and health facility staff increase their collaboration to improve prompt access to maternal and child care? A qualitative study in Tanzania. BMC Health Serv. Res. 2017, 17, 416. [Google Scholar] [CrossRef]
- Manzi, F.; Schellenberg, J.A.; Hutton, G.; Wyss, K.; Mbuya, C.; Shirima, K.; Mshinda, H.; Tanner, M.; Schellenberg, D. Human resources for health care delivery in Tanzania: A multifaceted problem. Hum. Resour. Health 2012, 10, 3. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Thematic Analysis-A Practical Guide; SAGE publications Ltd.: Newbury Park, CA, USA, 2022. [Google Scholar]
- Terry, G.; Hayfield, N.; Clarke, V.; Braun, V. Thematic Analysis. In The SAGE Handbook of Qualitative Research in Psychology; SAGE Publications Ltd.: London, UK, 2017. [Google Scholar]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Nvivo Qualitative Data Analysis Software, NVivo, 12; QSR International Pty Ltd.: Doncaster, VIC, Australia, 2020.
| Species of Animal | Country | ||
|---|---|---|---|
| Uganda | Tanzania | India | |
| Chicken | ✓ | ✓ | ✓ |
| Goat | ✓ | ✓ | ✓ |
| Turkey | ✓ | - | - |
| Duck | ✓ | - | - |
| Cow | - | - | ✓ |
| Dog | - | - | ✓ |
| Cat | - | - | ✓ |
| Sheep | - | - | ✓ |
| Not-specified | - | - | ✓ |
| Theme | Sub-Theme | Quotes | ||
|---|---|---|---|---|
| Uganda | Tanzania | India | ||
| Medicine-providers’ and livestock-keepers’ perceptions of the effectiveness and safety of antibiotics | Human and animal antibiotics are the same | “People do not differentiate between drug shops, for one can come to a human drug shop and ask for combitic [penicillin & streptomycin], or for poultry drugs.”—MP4-Human drug shop | “You find one using medicines, which he has bought from the human being’s pharmacy shop. Because he just believes in antibiotic, then even human being antibiotic he goes to give to livestock.” –MP1-Veterinary drug shop | “Most of the medicines are same. Our medicines and cow’s medicines and dog’s medicines are the same. If they have fever, and we have fever, the medicine for the fever is the same.”—LK5 |
| Human antibiotics are more effective | “They [customers] will tell you they are going to give them to the chicken. They will tell you that antibiotics meant for chicken don’t work…human antibiotics tend to work on chicken more effectively.”— MP1-Human drug shop | “Chicken may be sick, cold/influenza… and these medicines from the veterinary officer…they do not get well. You use the one called doxy [doxycycline] which are human medicines, and the chicken get well.”—LK2 | Interviewer: “Why Norfloxacin [human formulation] is used?” Respondent: “Norfloxacin gets some better result in case of goat.”—MP15-Veterinarian | |
| Safety considerations | “At times they give animals overdose because they don’t know the weight…so they don’t give them medicines basing on their weight, so they end up giving them overdose when they give them human drugs.”—MP5-Human drug shop | “He [customer] wanted two tablets of doxy… he says he is going to give to chickens… he will ask you for a half dose.” —MP3-Human drug shop | “A person came to me and asked, ‘Doctor my goat is having loose motion, what can we do?’ If I see the condition of the goat is really bad and it might die without a treatment, I may ask him to have a human medicine of a low dose… as I am not aware of the treatments, so I just give a low one.” —MP1-Informal human health provider | |
| Livestock-keepers’ sources of information | Trial and error (personal experience) | “They [customers] do it as a discovery, they try it and see it working then they come and tell you their success stories that ‘Doctor for me I gave chloramphenicol to poultry, and it got better’.”—MP2-Veterinary drug shop | Not mentioned | “Sometimes when they don’t get meds then approach me. [Veterinary] Doctors said they don’t have so we came to you for the meds. And they worked.”—MP4-Informal human health provider |
| Word of mouth (Other livestock-keeper’s experience) | Interviewer: “Now which diseases do farmers normally treat using the human drugs?” Respondent: “It should be fowl typhoid, because they usually develop diarrhoea with a white colour of their droppings and therefore if A used chloramphenicol and it worked for his poultry, he tells B and at times they don’t even know the name, but they say that ‘I gave white capsules’.”—MP2-Veterinary drug shop | Interviewer: “Right what other human medicine we use to treat animals?” Respondent: “All I know is that my fellow member, mother and my colleague talked about it.”—LK4 | Not mentioned | |
| Differences in availability of human and veterinary services and antibiotics | Veterinary services less easily accessible | “There are few veterinary drug shops compared to human drug shops.”—MP3-Human drug shop | “Livestock is near, a veterinary doctor is very far, if I find someone who can work on the problem that my livestock has, I will ask him to help.”—LK1 | “If I find the antibiotic is not available in veterinary, then I use the human one.”—MP10-Veterinarian, India |
| Economic incentives and pressures | Human antibiotics are cheaper | “They say ‘Doctor your packaging is big and expensive, I will use 200 to buy [human] chloramphenicol capsule yet for you, you will sell to me 5,000 to 8,000’…that’s why they basically do it.”—MP2-Veterinary drug shop | “Some time you find he has no money to pay the expert when he comes to see his livestock…. That is why you find most of them using their own medicines… Because the human being’s medicines are cheap.”—MP1-Veterinary drug shop | “The human medicine costs lesser than animals like the medicine for loose motion for human costs 2 rupees while tablet for cow one tablet costs 40–80 rupees. Why would we use that?”—LK1 |
| Economic incentives for selling human antibiotics for animals | “Some people go and buy human antibiotics and they treat animals for example Caf [chloramphenicol] people give it to chicken…—And if you refuse the customer will never come back.”—MP1-Human drug shop | Not mentioned | “We are only supposed to do vaccination, and artificial insemination. But if we did just that we won’t make enough money, so we, on our own, have learnt how to use antibiotics from other veterinary doctors.“—MP16-Veterinary paraprofessional (pranibandhu) | |
| Theme | Sub-Theme | Driver or Barrier to Antibiotic Crossover-Use | Reported in The Data | ||
|---|---|---|---|---|---|
| Uganda | Tanzania | India | |||
| Medicine-providers’ and livestock-keepers’ perceptions of the effectiveness and safety of antibiotics | Human and animal antibiotics are the same | Driver | ✓ | ✓ | ✓ |
| Human antibiotics are more effective | Driver | ✓ | ✓ | ✓ | |
| Human antibiotics are better quality | Driver | - | - | ✓ | |
| Safety considerations | ✓ | ✓ | ✓ | ||
| Human antibiotics are safe in animals | Driver | ✓ | ✓ | ✓ | |
| Human antibiotics are dangerous in animals | Barrier | ✓ | ✓ | ✓ | |
| Livestock-keepers’ sources of information | Trial and error (personal experience) | Driver | ✓ | - | ✓ |
| Word of mouth (other livestock-keeper’s experience) | Driver | ✓ | ✓ | - | |
| Advice from medicine-providers (‘expert’ opinion) | Driver | - | - | ✓ | |
| Differences in availability of human and veterinary services and antibiotics | Veterinary services less easily accessible | Driver | ✓ | ✓ | ✓ |
| Veterinary antibiotics less easily available | Driver | - | - | ✓ | |
| Unsuitable packaging size | Driver | ✓ | - | - | |
| Economic incentives and pressures | Human antibiotics are cheaper | Driver | ✓ | ✓ | ✓ |
| Economic incentives for selling human antibiotics for animals | Driver | ✓ | - | ✓ | |
| Country | ||||||
|---|---|---|---|---|---|---|
| Uganda (N = 7) | India (N = 29) | Tanzania (N = 22) | Total (N = 58) | |||
| Number of Different Antibiotics Mentioned | 8 | 25 | 8 | 26 | ||
| Average number of different antibiotics mentioned per transcript (range) | 2.86 (1–4) | 1.66 (1–5) | 1.5 (1–3) | 1.74 (1–5) | ||
| Antibiotic class | Antibiotic | Number of transcripts each antibiotic is mentioned in per country | WHO list of critically important AM | |||
| Uganda n (%) | India n (%) | Tanzania n (%) | Total n (%) | |||
| Fluoroquinolones | Ciprofloxacinw | 1 (10) | 1 (3) | 2 (3) | Highest priority CIA | |
| Norfloxacin w | 2 (7) | 2 (3) | Highest priority CIA | |||
| Enrofloxacin | 1 (10) | 1 (3) | 2 (3) | Highest priority CIA | ||
| Ofloxacinw | 1 (3) | 1 (2) | Highest priority CIA | |||
| Macrolides | Azithromycinw | 1 (3) | 1 (2) | Highest priority CIA | ||
| Erythromycin w | 4 (18) | 2 (3) | Highest priority CIA | |||
| Cephalosporins (3rd, 4th and 5th generation) | Ceftriaxone w | 2 (6) | 2 (3) | Highest priority CIA | ||
| Cefotaximew | 1 (3) | 1 (2) | ||||
| Aminoglycosides | GentamicinA | 2 (7) | 2 (3) | High priority CIA | ||
| AmikacinA | 1 (3) | 1 (2) | High priority CIA | |||
| Penicillin | AmoxicillinA | 3 (43) | 4 (14) | 13 (59) | 18 (31) | High priority CIA |
| PenicillinA | 1 (10) | 1 (3) | 1 (5) | 3 (5) | ||
| Amoxicillin-Clavulanic AcidA | 1 (3) | 1 (2) | High priority CIA | |||
| AmpicillinA | 2 (7) | 2 (9) | 4 (7) | High priority CIA | ||
| Cephalosporins (1st and 2nd generation) | CephalexinA | 3 (10) | 3 (5) | HIA | ||
| Chloramphenicol | Chloramphenicol 1 | 7 (100) | 1 (3) | 8 (14) | HIA | |
| Sulphonamides | Trimethoprim-sulfamethoxazoleA | 1 (10) | 2 (7) | 3 (5) | HIA | |
| SulfadimidineA | 2 (7) | 2 (3) | HIA | |||
| Tetracyclines | TetracyclineA | 5 (71) | 2 (7) | 4 (18) | 11 (19) | HIA |
| Oxytetracyclinew | 2 (7) | 2 (9) | 4 (7) | |||
| DoxycyclineA | 2 (7) | 11 (50) | 12 (20) | HIA | ||
| Nitroimidazole | Metronidazole A | 5 (17) | 1 (5) | 6 (10) | ||
| OrnidazoleA | 1 (3) | 1 (2) | ||||
| Combination | Ofloxacin-ornidazoleNR | 3 (10) | 3 (5) | Highest priority CIA | ||
| Norfloxacin-Tinidazole | 3 (10) | 3 (5) | Highest priority CIA | |||
| Ampicillin-cloxacillinNR | 1 (10) | 2 (7) | 3 (5) | |||
| Country | Type of Medicine-Provider | Definition |
|---|---|---|
| Uganda | Human or veterinary drug shops | Recognised drug outlets in the private for-profit sector, registered and licensed by the National Drug Authority to sell class “C” medicines (a restricted list of medicines including some antibiotic formulations) [38]. These drug outlets are licensed to provide either human or veterinary medicines exclusively. |
| Tanzania | Human or veterinary drug shops | The Tanzanian system distinguishes between type 1 (working under the supervision of a registered pharmacist) or type 2 (supervised by any person who has attended a five weeks’ accredited drug dispensing outlet training course) drug providers [40]. Type 1 providers can sell prescription only (including antibiotics), pharmacy only and general sale list (GSL) drugs. Type 2 providers can dispense GSL drugs and some antibiotics with prescription. Both type 1 and type 2 sell exclusively human or veterinary drugs. |
| Community health worker | Community residents who have a close understanding of key aspects of the community (e.g., language, socio-economic status, and life and health experiences) [63]. They receive pre-service training to perform activities related to health promotion and disease prevention in the community. They cannot administer medicines but can refer patients to health facilities and accredited drug dispensing outlets to receive treatment, including antibiotics [64]. | |
| Nurse | Nurses include nursing officers, nurse midwives, public health nurses. Training requirements include four years of secondary education followed by three years of professional training [65]. | |
| India | Private veterinarian | A self-employed worker who has received a university degree in veterinary medicine |
| Public-private veterinary paraprofessionals (Pranibandhu and Animal Development Volunteer) | Public capacity – provide artificial insemination and livestock development services, paid on commission Private capacity – delivered livestock healthcare informally (including provision of antibiotics) and are paid directly by livestock-keepers | |
| Para-vet | A self-employed animal health worker informally trained in primary veterinary care | |
| Veterinary drug shop | A shop that sells allopathic medicines that are manufactured with the intention of animal consumption | |
| Human drug shop | A shop that sells allopathic medicines that are manufactured with the intention of human consumption | |
| Informal provider of human health | A self-employed health worker who does not hold a medical degree but is informally trained in the practice of human medicine | |
| Homeopath | A self-employed health worker in homeopathic medicine |
| Type of Interviewee | Number of Transcripts Received and Interview Method | Number of Transcripts with Crossover-Use Mentioned and Interview Method | ||||||
|---|---|---|---|---|---|---|---|---|
| Total | Uganda | Tanzania | India | Total | Uganda | Tanzania | India | |
| Medicine-provider | 41 | 7 FGD | 8 IDI | 26 IDI | 30 | 7 FGD | 6 IDI | 17 IDI |
| Livestock-keeper | 53 | - | 16 FGD 2 IDI | 34 IDI 1FGD | 23 | - | 11 FGD 1 IDI | 10 IDI 1 FGD |
| Key informant | 6 | - | - | 6 IDI | 2 | - | - | 2 IDI |
| Community health worker | 8 | - | 8 IDI | - | 4 | - | 4 IDI | - |
| Total | 108 | 7 | 34 | 67 | 59 | 7 | 22 | 30 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Myers, J.; Hennessey, M.; Arnold, J.-C.; McCubbin, K.D.; Lembo, T.; Mateus, A.; Kitutu, F.E.; Samanta, I.; Hutchinson, E.; Davis, A.; et al. Crossover-Use of Human Antibiotics in Livestock in Agricultural Communities: A Qualitative Cross-Country Comparison between Uganda, Tanzania and India. Antibiotics 2022, 11, 1342. https://doi.org/10.3390/antibiotics11101342
Myers J, Hennessey M, Arnold J-C, McCubbin KD, Lembo T, Mateus A, Kitutu FE, Samanta I, Hutchinson E, Davis A, et al. Crossover-Use of Human Antibiotics in Livestock in Agricultural Communities: A Qualitative Cross-Country Comparison between Uganda, Tanzania and India. Antibiotics. 2022; 11(10):1342. https://doi.org/10.3390/antibiotics11101342
Chicago/Turabian StyleMyers, Jessica, Mathew Hennessey, Jean-Christophe Arnold, Kayley D. McCubbin, Tiziana Lembo, Ana Mateus, Freddy Eric Kitutu, Indranil Samanta, Eleanor Hutchinson, Alicia Davis, and et al. 2022. "Crossover-Use of Human Antibiotics in Livestock in Agricultural Communities: A Qualitative Cross-Country Comparison between Uganda, Tanzania and India" Antibiotics 11, no. 10: 1342. https://doi.org/10.3390/antibiotics11101342
APA StyleMyers, J., Hennessey, M., Arnold, J.-C., McCubbin, K. D., Lembo, T., Mateus, A., Kitutu, F. E., Samanta, I., Hutchinson, E., Davis, A., Mmbaga, B. T., Nasuwa, F., Gautham, M., & Clarke, S. E. (2022). Crossover-Use of Human Antibiotics in Livestock in Agricultural Communities: A Qualitative Cross-Country Comparison between Uganda, Tanzania and India. Antibiotics, 11(10), 1342. https://doi.org/10.3390/antibiotics11101342








