Continuous Glucose Monitoring and Exercise in Type 1 Diabetes: Past, Present and Future
Abstract
1. Introduction
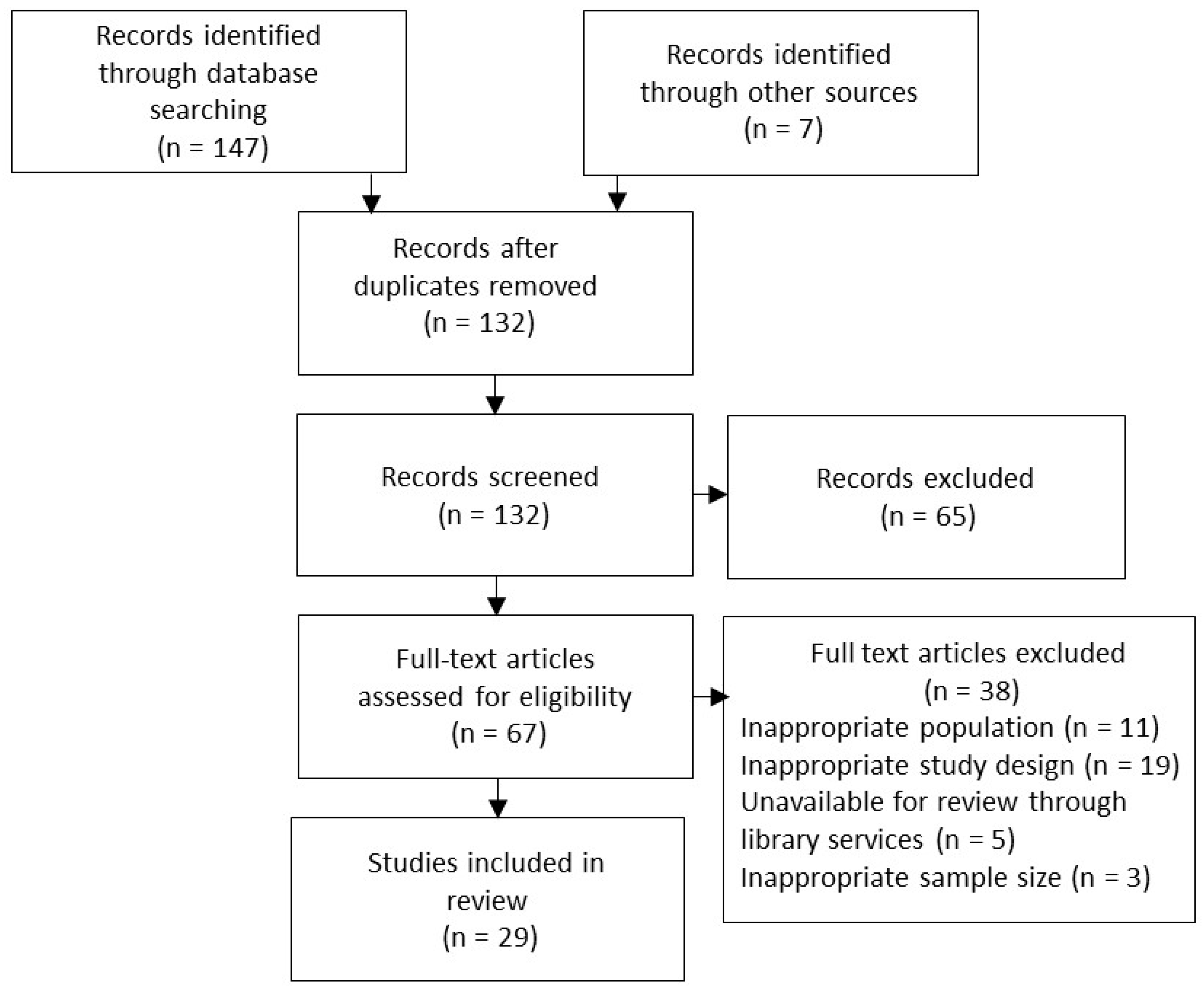
2. Materials and Methods
3. Discussion
3.1. CGM-Derived Contributions to the T1D Exercise Research Literature
3.1.1. Aerobic Exercise
3.1.2. High Intensity Intermittent Exercise
3.1.3. Resistance Exercise
3.2. CGM Accuracy during Exercise
3.3. CGM and Diabetes Management during Exercise
3.4. Using CGM as a Tool for Patients to Learn about Exercise
3.5. Where CGM Technology Is Leading
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Zinman, B.; Murray, F.T.; Vranic, M.; Albisser, A.M.; Leibel, B.S.; McClean, P.A.; Marliss, E.B. Glucoregulation during moderate exercise in insulin treated diabetics. J. Clin. Endocrinol. Metab. 1977, 45, 641–652. [Google Scholar] [CrossRef] [PubMed]
- Hubinger, A.; Ridderskamp, I.; Lehmann, E.; Gries, F.A. Metabolic response to different forms of physical exercise in type I diabetics and the duration of the glucose lowering effect. Eur. J. Clin. Investig. 1985, 15, 197–203. [Google Scholar] [CrossRef]
- Meinders, A.E.; Willekens, F.L.; Heere, L.P. Metabolic and hormonal changes in IDDM during long-distance run. Diabetes Care 1988, 11, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Moser, O.; Tschakert, G.; Mueller, A.; Groeschl, W.; Pieber, T.R.; Obermayer-Pietsch, B.; Koehler, G.; Hofmann, P. Effects of High-Intensity Interval Exercise versus Moderate Continuous Exercise on Glucose Homeostasis and Hormone Response in Patients with Type 1 Diabetes Mellitus Using Novel Ultra-Long-Acting Insulin. PLoS ONE 2015, 10, e0136489. [Google Scholar] [CrossRef] [PubMed]
- Yamanouchi, K.; Abe, R.; Takeda, A.; Atsumi, Y.; Shichiri, M.; Sato, Y. The effect of walking before and after breakfast on blood glucose levels in patients with type 1 diabetes treated with intensive insulin therapy. Diabetes Res. Clin. Pract. 2002, 58, 11–18. [Google Scholar] [CrossRef]
- Ruegemer, J.J.; Squires, R.W.; Marsh, H.M.; Haymond, M.W.; Cryer, P.E.; Miles, J.M. Differences between prebreakfast and late afternoon glycemic responses to exercise in IDDM patients. Diabetes Care 1990, 13, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Kenny, G.P.; Perkins, B.A.; Riddell, M.C.; Balaa, N.; Malcolm, J.; Boulay, P.; Khandwala, F.; Sigal, R.J. Resistance versus aerobic exercise: Acute effects on glycemia in type 1 diabetes. Diabetes Care 2013, 36, 537–542. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Kenny, G.P.; Perkins, B.A.; Riddell, M.C.; Malcolm, J.; Boulay, P.; Khandwala, F.; Sigal, R.J. Effects of performing resistance exercise before versus after aerobic exercise on glycemia in type 1 diabetes. Diabetes Care 2012, 35, 669–675. [Google Scholar] [CrossRef] [PubMed]
- Turner, D.; Luzio, S.; Kilduff, L.P.; Gray, B.J.; Dunseath, G.; Bain, S.C.; Campbell, M.D.; West, D.J.; Bracken, R.M. Reductions in resistance exercise-induced hyperglycaemic episodes are associated with circulating interleukin-6 in type 1 diabetes. Diabet. Med. 2014, 31, 1009–1013. [Google Scholar] [CrossRef] [PubMed]
- Turner, D.; Gray, B.J.; Luzio, S.; Dunseath, G.; Bain, S.C.; Hanley, S.; Richards, A.; Rhydderch, D.C.; Ayles, M.; Kilduff, L.P.; et al. Similar magnitude of post-exercise hyperglycemia despite manipulating resistance exercise intensity in type 1 diabetes individuals. Scand. J. Med. Sci. Sports 2016, 26, 404–412. [Google Scholar] [CrossRef] [PubMed]
- Turner, D.; Luzio, S.; Gray, B.J.; Dunseath, G.; Rees, E.D.; Kilduff, L.P.; Campbell, M.D.; West, D.J.; Bain, S.C.; Bracken, R.M. Impact of single and multiple sets of resistance exercise in type 1 diabetes. Scand. J. Med. Sci. Sports 2015, 25, e99–e109. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, T.H.; Abraham, G.; Schiffrin, A.; Leiter, L.A.; Marliss, E.B. Hyperglycemia after intense exercise in IDDM subjects during continuous subcutaneous insulin infusion. Diabetes Care 1988, 11, 311–317. [Google Scholar] [CrossRef] [PubMed]
- Purdon, C.; Brousson, M.; Nyveen, S.L.; Miles, P.D.; Halter, J.B.; Vranic, M.; Marliss, E.B. The roles of insulin and catecholamines in the glucoregulatory response during intense exercise and early recovery in insulin-dependent diabetic and control subjects. J. Clin. Endocrinol. Metab. 1993, 76, 566–573. [Google Scholar] [PubMed]
- Sigal, R.J.; Purdon, C.; Fisher, S.J.; Halter, J.B.; Vranic, M.; Marliss, E.B. Hyperinsulinemia prevents prolonged hyperglycemia after intense exercise in insulin-dependent diabetic subjects. J. Clin. Endocrinol. Metab. 1994, 79, 1049–1057. [Google Scholar] [PubMed]
- Bussau, V.A.; Ferreira, L.D.; Jones, T.W.; Fournier, P.A. A 10-s sprint performed prior to moderate-intensity exercise prevents early post-exercise fall in glycaemia in individuals with type 1 diabetes. Diabetologia 2007, 50, 1815–1818. [Google Scholar] [CrossRef] [PubMed]
- Fahey, A.J.; Paramalingam, N.; Davey, R.J.; Davis, E.A.; Jones, T.W.; Fournier, P.A. The effect of a short sprint on postexercise whole-body glucose production and utilization rates in individuals with type 1 diabetes mellitus. J. Clin. Endocrinol. Metab. 2012, 97, 4193–4200. [Google Scholar] [CrossRef] [PubMed]
- Bussau, V.A.; Ferreira, L.D.; Jones, T.W.; Fournier, P.A. The 10-s maximal sprint: A novel approach to counter an exercise-mediated fall in glycemia in individuals with type 1 diabetes. Diabetes Care 2006, 29, 601–606. [Google Scholar] [CrossRef] [PubMed]
- Guelfi, K.J.; Jones, T.W.; Fournier, P.A. The decline in blood glucose levels is less with intermittent high-intensity compared with moderate exercise in individuals with type 1 diabetes. Diabetes Care 2005, 28, 1289–1294. [Google Scholar] [CrossRef] [PubMed]
- Guelfi, K.J.; Jones, T.W.; Fournier, P.A. Intermittent high-intensity exercise does not increase the risk of early postexercise hypoglycemia in individuals with type 1 diabetes. Diabetes Care 2005, 28, 416–418. [Google Scholar] [CrossRef] [PubMed]
- Iscoe, K.E.; Riddell, M.C. Continuous moderate-intensity exercise with or without intermittent high-intensity work: Effects on acute and late glycaemia in athletes with type 1 diabetes mellitus. Diabet. Med. 2011, 28, 824–832. [Google Scholar] [CrossRef] [PubMed]
- Campbell, M.D.; West, D.J.; Bain, S.C.; Kingsley, M.I.; Foley, P.; Kilduff, L.; Turner, D.; Gray, B.; Stephens, J.W. Simulated games activity vs continuous running exercise: A novel comparison of the glycemic and metabolic responses in T1DM patients. Scand. J. Med. Sci. Sports 2015, 25, 216–222. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Colberg, S.R. Update on Management of Type 1 Diabetes and Type 2 Diabetes in Athletes. Curr. Sports Med. Rep. 2017, 16, 38–44. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.; Mollard, R.; MacIntosh, A.; Macmillan, F.; Wicklow, B.; Berard, L.; Hurd, C.; Marks, S.; McGavock, J. Vigorous intensity exercise for glycemic control in patients with type 1 diabetes. Can. J. Diabetes. 2013, 37, 427–432. [Google Scholar] [CrossRef] [PubMed]
- Riddell, M.C.; Gallen, I.W.; Smart, C.E.; Taplin, C.E.; Addolfsson, P.; Lumb, A.N.; Kowalski, A.; Rabasa-Lhoret, R.; McCrimmon, R.J.; Hume, C.; et al. Exercise management in type 1 diabetes: A consensus statement. Lancet Diabetes Endocrinol. 2017, 5, 377–390. [Google Scholar] [CrossRef]
- Colberg, S.R.; Sigal, R.J.; Yardley, J.E.; Riddell, M.C.; Dunstan, D.W.; Dempsey, P.C.; Horton, E.S.; Castorino, K.; Tate, D.F. Physical Activity/Exercise and Diabetes: A Position Statement of the American Diabetes Association. Diabetes Care 2016, 39, 2065–2079. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Sigal, R.J.; Perkins, B.A.; Riddell, M.C.; Kenny, G.P. Resistance exercise in type 1 diabetes. Can. J. Diabetes 2013, 37, 420–426. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services, Physical Activity Guidelines Advisory Committee. Physical Activity Guidelines Advisory Committee Report; Government Printing Office: Washington, DC, USA, 2008; p. 683.
- Davidson, H. Aerobic Exercise. In Gale Encyclopaedia of Senior Health; Longe, J., Ed.; Gale: Detroit, MI, USA, 2009; pp. 36–39. [Google Scholar]
- Pal, S.; Radavelli-Bagatini, S.; Ho, S. Potential benefits of exercise on blood pressure and vascular function. J. Am. Soc. Hypertens. 2013, 7, 494–506. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Zaharieva, D.P.; Jarvis, C.; Riddell, M.C. The “ups” and “downs” of a bike race in people with type 1 diabetes: Dramatic differences in strategies and blood glucose responses in the Paris-to-Ancaster Spring Classic. Can. J. Diabetes 2015, 39, 105–110. [Google Scholar] [CrossRef] [PubMed]
- Maran, A.; Pavan, P.; Bonsembiante, B.; Brugin, E.; Ermolao, A.; Avogaro, A.; Zaccaria, M. Continuous glucose monitoring reveals delayed nocturnal hypoglycemia after intermittent high-intensity exercise in nontrained patients with type 1 diabetes. Diabetes Technol. Ther. 2010, 12, 763–768. [Google Scholar] [CrossRef] [PubMed]
- Reddy, R.; El Youssef, J.; Winters-Stone, K.; Branigan, D.; Leitschuh, J.; Castle, J.; Jacobs, P.G. The effect of exercise on sleep in adults with type 1 diabetes. Diabetes Obes. Metab. 2018, 20, 443–447. [Google Scholar] [CrossRef] [PubMed]
- Zaharieva, D.P.; Miadovnik, L.A.; Rowan, C.P.; Gumieniak, R.J.; Jamnik, V.K.; Riddell, M.C. Effects of acute caffeine supplementation on reducing exercise-associated hypoglycaemia in individuals with Type 1 diabetes mellitus. Diabet. Med. 2016, 33, 488–496. [Google Scholar] [CrossRef] [PubMed]
- Iscoe, K.E.; Campbell, J.E.; Jamnik, V.; Perkins, B.A.; Riddell, M.C. Efficacy of Continuous Real-Time Blood Glucose Monitoring During and After Prolonged High-Intensity Cycling Exercise: Spinning with a Continuous Glucose Monitoring System. Diabetes Technol. Ther. 2006, 8, 627–635. [Google Scholar] [CrossRef] [PubMed]
- Lerner, K.L.; Lerner, B.W. (Eds.) World of Sport Science; Gale: Detroit, MI, USA, 2007. [Google Scholar]
- Wan, W.; Skandari, M.R.; Minc, A.; Nathan, A.G.; Winn, A.; Zarei, P.; O’Grady, M.; Huang, E.S. Cost-effectiveness of Continuous Glucose Monitoring for Adults with Type 1 Diabetes Compared With Self-Monitoring of Blood Glucose: The DIAMOND Randomized Trial. Diabetes Care 2018, 41, 1227–1234. [Google Scholar] [CrossRef] [PubMed]
- Bode, B.W. Clinical Utility of the Continuous Glucose Monitoring System. Diabetes Technol. Ther. 2000, 2, S35–S41. [Google Scholar] [CrossRef] [PubMed]
- Aberer, F.; Hajnsek, M.; Rumpler, M.; Zenz, S.; Baumann, P.M.; Elsayed, H.; Puffing, A.; Treiber, G.; Pieber, T.R.; Sourij, H.; et al. Evaluation of subcutaneous glucose monitoring systems under routine environmental conditions in patients with type 1 diabetes. Diabetes Obes. Metab. 2017, 19, 1051–1055. [Google Scholar] [CrossRef] [PubMed]
- Bally, L.; Zueger, T.; Pasi, N.; Carlos, C.; Paganini, D.; Stettler, C. Accuracy of continuous glucose monitoring during differing exercise conditions. Diabetes Res. Clin. Pract. 2016, 112, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Moser, O.; Mader, J.K.; Tschakert, G.; Mueller, A.; Groeschl, W.; Pieber, T.R.; Koehler, G.; Messerschmidt, J.; Hofmann, P. Accuracy of continuous glucose monitoring (CGM) during continuous and high-intensity interval exercise in patients with type 1 diabetes mellitus. Nutrients 2016, 8, 489. [Google Scholar] [CrossRef] [PubMed]
- Radermecker, R.P.; Fayolle, C.; Brun, J.F.; Bringer, J.; Renard, E. Accuracy assessment of online glucose monitoring by a subcutaneous enzymatic glucose sensor during exercise in patients with type 1 diabetes treated by continuous subcutaneous insulin infusion. Diabetes Metab. 2013, 39, 258–262. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Sigal, R.J.; Kenny, G.P.; Riddell, M.C.; Lovblom, L.E.; Perkins, B.A. Point accuracy of interstitial continuous glucose monitoring during exercise in type 1 diabetes. Diabetes Technol. Ther. 2013, 15, 46–49. [Google Scholar] [CrossRef] [PubMed]
- Campbell, M.D.; Walker, M.; Trenell, M.I.; Jakovljevic, D.G.; Stevenson, E.J.; Bracken, R.M.; Bain, S.C.; West, D.J. Large pre- and postexercise rapid-acting insulin reductions preserve glycemia and prevent early- but not late-onset hypoglycemia in patients with type 1 diabetes. Diabetes Care 2013, 36, 2217–2224. [Google Scholar] [CrossRef] [PubMed]
- Campbell, M.D.; Walker, M.; Trenell, M.I.; Stevenson, E.J.; Turner, D.; Bracken, R.M.; Shaw, J.A.; West, D.J. A low-glycemic index meal and bedtime snack prevents postprandial hyperglycemia and associated rises in inflammatory markers, providing protection from early but not late nocturnal hypoglycemia following evening exercise in type 1 diabetes. Diabetes Care 2014, 37, 1845–1853. [Google Scholar] [CrossRef] [PubMed]
- Franc, S.; Daoudi, A.; Pochat, A.; Petit, M.H.; Randazzo, C.; Petit, C.; Duclos, M.; Penfornis, A.; Pussard, E.; Not, D.; et al. Insulin-based strategies to prevent hypoglycaemia during and after exercise in adult patients with type 1 diabetes on pump therapy: The DIABRASPORT randomized study. Diabetes Obes. Metab. 2015, 17, 1150–1157. [Google Scholar] [CrossRef] [PubMed]
- Kilbride, L.; Charlton, J.; Aitken, G.; Hill, G.W.; Davison, R.C.; McKnight, J.A. Managing blood glucose during and after exercise in Type 1 diabetes: Reproducibility of glucose response and a trial of a structured algorithm adjusting insulin and carbohydrate intake. J. Clin. Nurs. 2011, 20, 3423–3429. [Google Scholar] [CrossRef] [PubMed]
- Zaharieva, D.; Yavelberg, L.; Jamnik, V.; Cinar, A.; Turksoy, K.; Riddell, M.C. The effects of basal insulin suspension at the start of exercise on blood glucose levels during continuous versus circuit-based exercise in individuals with type 1 diabetes on continuous subcutaneous insulin infusion. Diabetes Technol. Ther. 2017, 19, 370–378. [Google Scholar] [CrossRef] [PubMed]
- Pickup, J.C.; Holloway, M.F.; Samsi, K. Real-Time Continuous Glucose Monitoring in Type 1 Diabetes: A Qualitative Framework Analysis of Patient Narratives. Diabetes Care 2015, 38, 544–550. [Google Scholar] [CrossRef] [PubMed]
- Dyck, R.A.; Kleinman, N.J.; Funk, D.R.; Yeung, R.O.; Senior, P.; Yardley, J.E. We can work (it) out together: Type 1 diabetes boot camp for adult patients and providers improves exercise self-efficacy. Can. J. Diabetes 2018. [Google Scholar] [CrossRef] [PubMed]
- Tumminia, A.; Crimi, S.; Sciacca, L.; Buscema, M.; Frittitta, L.; Squatrito, S.; Vigneri, R.; Tomaselli, L. Efficacy of real-time continuous glucose monitoring on glycemia control and glucose varibility in type 1 diabetic patients treated with either insulin pumps or multiple insulin injection therapy: A randomized controlled crossover trial. Diabetes Metab. Res. Rev. 2015, 31, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Breton, M.D.; Patek, S.D.; Lv, D.; Schertz, E.; Robic, J.; Pinnata, J.; Kollar, L.; Barnett, C.; Wakeman, C.; Oliveri, M.; et al. Continuous Glucose Monitoring and Insulin Informed Advisory System with Automated Titration and Dosing of Insulin Reduces Glucose Variability in Type 1 Diabetes Mellitus. Diabetes Technol. Ther. 2018, 20. [Google Scholar] [CrossRef] [PubMed]
- Brazeau, A.S.; Rabasa-Lhoret, R.; Strychar, I.; Sircescu, H. Barriers to physical activity among patients with type 1 diabetes. Diabetes Care 2008, 31, 2108–2109. [Google Scholar] [CrossRef] [PubMed]
- Colberg, S.R.; Laan, R.; Dassau, E.; Kerr, D. Physical activity and type 1 diabetes: Time for a rewire? J. Diabetes Sci. Technol. 2015, 9, 609–618. [Google Scholar] [CrossRef] [PubMed]
- Riddell, M.C.; Zaharieva, D.P.; Yavelberg, L.; Cinar, A.; Jamnik, V.K. Exercise and the Development of the Artificial Pancreas: One of the More Difficult Series of Hurdles. J. Diabetes Sci. Technol. 2015, 9, 1217–1226. [Google Scholar] [CrossRef] [PubMed]
- Moser, O.; Yardley, J.E.; Bracken, R.M. Interstitial glucose and physical exercise in type 1 diabetes: Integrative physiology, technology, and the gap in-between. Nutrients 2018, 10, 93. [Google Scholar] [CrossRef] [PubMed]
- Abraham, M.B.; Davey, R.; O’Grady, M.J.; Ly, T.T.; Paramalingam, N.; Fournier, P.A.; Roy, A.; Grosman, B.; Kurtz, N.; Fairchild, J.M.; et al. Effectiveness of a predictive algorithm in the prevention of exercise-induced hypoglycemia in type 1 diabetes. Diabetes Technol. Ther. 2016, 18, 543–550. [Google Scholar] [CrossRef] [PubMed]
- Breton, M.D.; Brown, M.D.; Hughes Karvetski, C.; Kollar, L.; Topchyan, K.A.; Anderson, S.M.; Kovatchev, B.P. Adding Heart Rate Signal to a Control-to-Range Artificial Pancreas System Improves the Protection Against Hypoglycemia During Exercise in Type 1 Diabetes. Diabetes Technol. Ther. 2014, 16, 506–511. [Google Scholar] [CrossRef] [PubMed]
- Turksoy, K.; Quinn, L.T.; Littlejohn, E.; Cinar, A. An Integrated Multivariable Artificial Pancreas Control System. J. Diabetes Sci. Technol. 2014, 8, 498–507. [Google Scholar] [CrossRef] [PubMed]
- Jayawardene, D.C.; McAuley, S.A.; Horsburgh, J.C.; Gerche, A.; Jenkins, A.J.; Ward, G.M.; MacIsaac, R.J.; Roberts, T.J.; Grosman, B.; Kurtz, N.; et al. Closed-Loop Insulin delivery for adults with type 1 diabetes undertaking high-intensity interval exercise versus moderate-intensity exercise: A randomized, crossover study. Diabetes Technol. Ther. 2017, 19, 340–348. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, P.G.; El Youssef, J.; Reddy, R.; Resalat, N.; Branigan, D.; Condon, J.; Preiser, N.; Ramsey, K.; Jones, M.; Edwards, C.; et al. Randomized trial of a dual-hormone artificial pancreas with dosing adjustment during exercise compared with no adjustment and sensor-augmented pump therapy. Diabetes Obes. Metab. 2016, 18, 1110–1119. [Google Scholar] [CrossRef] [PubMed]
- Van Bon, A.C.; Jonker, L.D.; Koebrugge, R.; Koops, R.; Hoekstra, J.B.; DeVries, J.H. Feasibility of a bihormonal closed-loop system to control postexercise and postprandial glucose excursions. J. Diabetes Sci. Technol. 2012, 6, 1114–1122. [Google Scholar] [CrossRef] [PubMed]
- Taleb, N.; Emami, A.; Suppere, C.; Messier, V.; Legault, L.; Ladouceur, M.; Chiasson, J.L.; Haidar, A.; Rabasa-Lhoret, R. Efficacy of single-hormone and dual-hormone artificial pancreas during continuous and interval exercise in adult patients with type 1 diabetes: Randomised controlled crossover trial. Diabetologia 2016, 59, 2561–2571. [Google Scholar] [CrossRef] [PubMed]
- Castle, J.R.; El Youssef, J.; Wilson, L.M.; Reddy, R.; Resalat, N.; Branigan, D.; Ramsey, K.; Leitschuh, J.; Rajhbeharrysingh, U.; Senf, B.; et al. Randomized Outpatient Trial of Single- and Dual-Hormone Closed-Loop Systems That Adapt to Exercise Using Wearable Sensors. Diabetes Care 2018, 41, dc180228. [Google Scholar] [CrossRef] [PubMed]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Houlder, S.K.; Yardley, J.E. Continuous Glucose Monitoring and Exercise in Type 1 Diabetes: Past, Present and Future. Biosensors 2018, 8, 73. https://doi.org/10.3390/bios8030073
Houlder SK, Yardley JE. Continuous Glucose Monitoring and Exercise in Type 1 Diabetes: Past, Present and Future. Biosensors. 2018; 8(3):73. https://doi.org/10.3390/bios8030073
Chicago/Turabian StyleHoulder, Shaelyn K., and Jane E. Yardley. 2018. "Continuous Glucose Monitoring and Exercise in Type 1 Diabetes: Past, Present and Future" Biosensors 8, no. 3: 73. https://doi.org/10.3390/bios8030073
APA StyleHoulder, S. K., & Yardley, J. E. (2018). Continuous Glucose Monitoring and Exercise in Type 1 Diabetes: Past, Present and Future. Biosensors, 8(3), 73. https://doi.org/10.3390/bios8030073




