Incorporation of Nanomaterials in Glass Ionomer Cements—Recent Developments and Future Perspectives: A Narrative Review
Abstract
1. Introduction
| Polymeric Acids | Glasses | Additives | Water | Physical Requirements According to ISO 9917-1 [9] |
|---|---|---|---|---|
| poly(acrylic acid) (homopolymer), 2:1 copolymer of acrylic acid/maleic acid | Alumino-silicates (particle size up to 45 μm), zinc silicates, niobium silicates with inclusion of CaF2, SrO, SrF2, Fe2O3, etc. | Chelating agents: (+)− tartaric acid, citric acid (5–10%); | 11–24% | Luting cement: setting time 2.5–8 min; compressive strength min 70 MPa; acid-soluble As 2 mg/kg; acid-soluble Pb 100 mg/kg; Restorative cement: setting time 2–6 min; compressive strength min 130 MPa; max. 0.05 mm/h; opacity 0.35–0.9; acid erosion acid-soluble As 2 mg/kg; acid-soluble Pb 100 mg/kg |
- (a)
- Luting/bonding cements (Type I)
- -
- used for cementation, inlays and orthodontic applications;
- -
- powder/liquid ratio = 1.5/1 … 3.8/1);
- -
- low setting times;
- -
- good early resistance to water;
- -
- radiopaque.
- (b)
- Restorative cements for anterior repairs (Type II i), when aesthetic characteristics are important
- -
- powder/liquid ratio = 3/1 … 6.8/1;
- -
- corresponding color match;
- -
- not resistant to water (protection needed);
- -
- most often radiopaque.
- (c)
- Restorative cements for posterior repairs (Type II ii), when aesthetic characteristics are not important
- -
- powder/liquid ratio = 3/1 … 4/1;
- -
- low setting times, resistance to water uptake;
- -
- radiopaque.
- (d)
- Base cements and lining (Type III)
- -
- powder/liquid ratio = 1.5/1 (for lining), 3/1 … 6.8/1 (for base cements);
- -
- radiopaque.
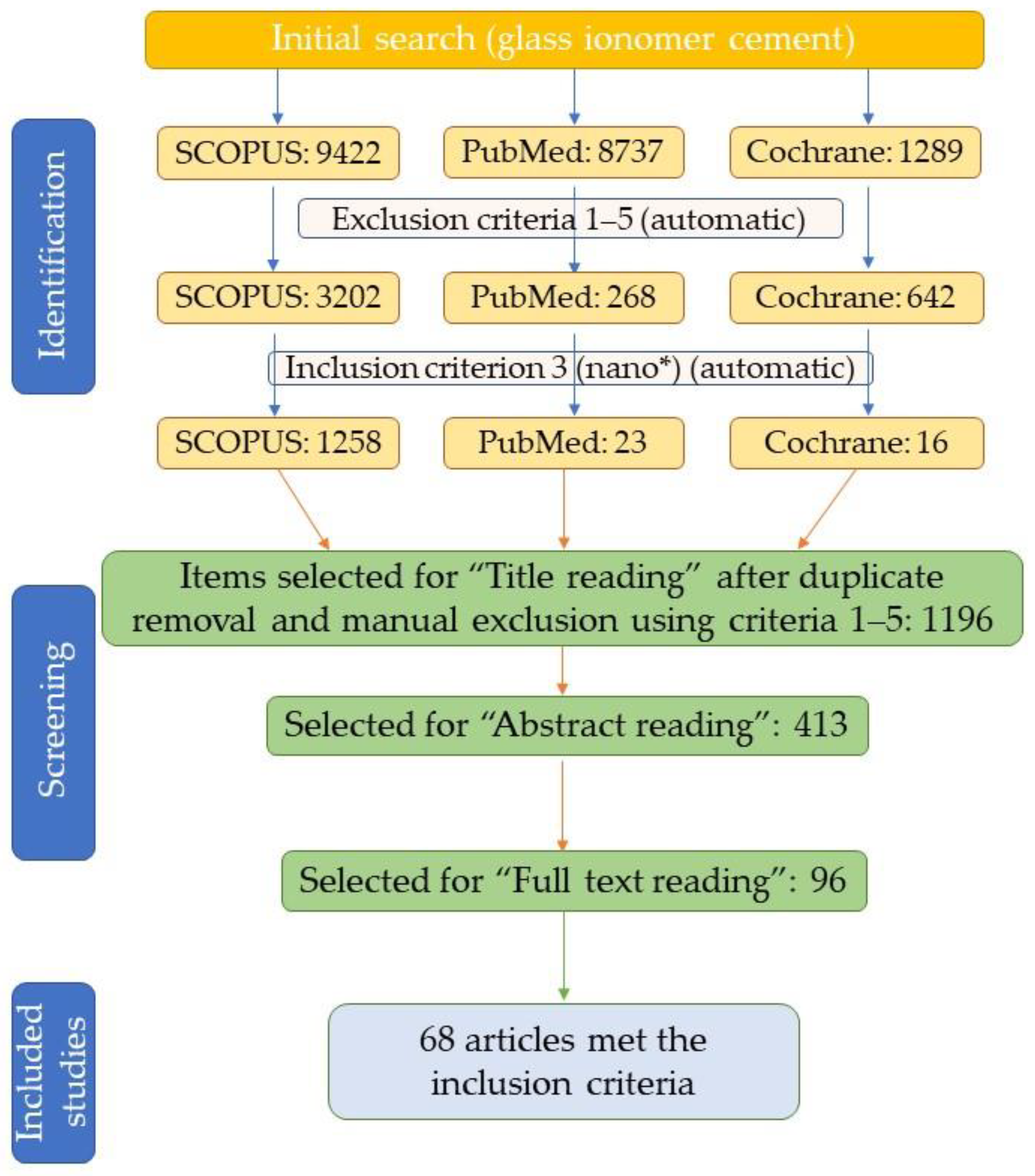
2. Methodology
- -
- research articles published in the time interval 2011–present, full text;
- -
- articles published or available in English;
- -
- incorporation of nanomaterials (either commercial or obtained in the laboratory);
- -
- randomized clinical trials;
- -
- quantitative and/or qualitative evaluation of mechanical or antimicrobial properties of GIC;
- -
- relevance for the review topic (new information provided).
- -
- articles published before 2011;
- -
- book chapters or book;
- -
- review or systematic review articles;
- -
- conference paper, note, letter, short survey, erratum or conference review;
- -
- articles published in languages other than English;
- -
- incorporation of exclusively organic materials or carbon nanomaterials in GICs.
3. Results and Discussion
3.1. Metallic Nanoparticles in Glass Ionomer Cements
| NPs, Ref. | NPs Characteristics | GIC | Experimental Study | Findings |
|---|---|---|---|---|
| CuNP [44] | Phytosynthesized using Thymus vulgaris extract, spherical, 10-25 nm | GC Fuji IX GP ® (type II ii) | 0.5% NPs, respectively 0.5% NPs + 1.5% metronidazole in GIC, antimicrobial effect tested against Staphylococcus aureus and Streptococcus mutans; compressive strength measurements | Addition of CuNPs enhanced antimicrobial properties, while not affecting the mechanical properties: IZ = 20/29 mm (S. aureus), 19/26 mm (S. mutans) after 1 day, 15/19 mm (S. aureus), 13/18 mm (S. mutans) after 1 month; CS = 44.2/43.9 MPa |
| AgNP [44] | Commercially available, 20–50 nm | Addition of AgNPs led to superior antimicrobial properties compared with other variants (including CuNPs), while not affecting the mechanical properties: IZ = 24/30 mm (S. aureus), 20/27 mm (S. mutans) after 1 day, 16/18 mm (S. aureus), 14/17 mm (S. mutans) after 1 month; CS = 45.9/45.0 MPa | ||
| AgNP [45] | Commercially available, under 100 nm | GC Fuji II GP ® (type II ii) | 0.2, 0.4, respectively 0.6%NPs in GIC, evaluation of the quality of the chemical bond of GIC to primary dentin by FTIR | Concentrations above 0.4% AgNP in GIC altered the bond quality with dentin interaction; addition of AgNPs at low level improves the mechanical properties while maintaining the bond quality |
| AgNP [46] | Phytosynthesized using Cupressus macrocarpa extract, spherical, 13.5–25.8 nm | GC Fuji IX GP ® (type II ii) | 0.5%NPs, respectively 0.5%NPs + amoxicillin in GIC, antimicrobial effect tested against Staphylococcus aureus and Streptococcus mutans; compressive strength measurements | Addition of AgNPs showed a synergistic antimicrobial effect with amoxicillin: IZ = 20/30 mm (S. aureus), 18/29 mm (S. mutans) after 1 day, compared with GIC 9/8 mm, 12/16 mm (S. aureus), 11/15 mm (S. mutans) after 3 weeks, compared with GIC 0/0 mm; the influence on compressive strength was insignificant: CS = 45.6/45.3 MPa, compared to GIC 44.4 MPa |
| AgNP [47] | Phytosynthesized using Zingiber officinale extract, spherical, 10.5–14.12 nm | GC Fuji IX GP ® (type II ii) | 0.5% NPs, respectively 0.5%NPs+1% chlorhexidine in GIC, evaluation of antimicrobial activity (against Staphylococcus aureus, Streptococcus mutans, and Candida albicans), CS | The addition of AgNPs and chlorhexidine enhanced antimicrobial efficacy and compressive strength compared with individual components. IZ = 21.3/25.2 (S. aureus), 19.4/26.2 (S. mutans), 16.3/20.4 (C. albicans) at 24 h; IZ = 13.3/18.3 (S. aureus), 12.1/19.1 (S. mutans), 9.2/16.3 (C. albicans) at 3 weeks; CS = 44.7/45.8, compared with 42.4 MPa (control) |
| AgNP [49] | Commercially available, 20 nm | GC Ortho LC, Fuji ® (type I) | 0.15% NPs in GIC, followed by addition of N-acetylcysteine (NAC) at 20% and 2-methacryloyloxyethyl Phosphorylcholine (MPC) 1-3%; evaluation of the bond strength, cytotoxicity, and antimicrobial potential against Streptococcus mutans | Cement with AgNP presented strong antibacterial capability, protein-repellent ability, and acceptable biocompatibility. Cell viability 81.3% (day 7), CS = 8.13 MPa (at MPC 2%), suppressed metabolic activity by 59.03% and lactic acid production of biofilms by 70.02%, reduced biofilm CFU by 2 logs, reduced protein adsorption by 76.87%. |
| AgNP [50] | Chitosan-mediated, hydrodynamic diameter 122 nm | Ketac™ CEM, Easymix,3M (Type I) | 10, 30, 50%NPs in GIC, evaluation of mechanical properties and color stability | The addition of AgNPs (10%) induced significant increase in CS = 37 MPa (compared with control 27MPa); the addition of AgNPs also led to significant color change (ΔE = >3.3) and appearance of pores in the cement |
| AgNP [51] | Commercially available | GC Fuji II GP ® (type II ii) | 5%NPs in GIC, evaluation of μSBS | Addition of AgNPs increases the bond strength of the restoration: μSBS = 6.96 MPa, compared with control 3.77 MPa |
| CuNP [48] | Synthesized using ascorbic acid, 10.87 nm | GC Fuji IX GP ® (type II ii) | 1, 2, 3, 4%NPs in GIC, evaluation of antimicrobial potential against Streptococcus mutans and Streptococcus sanguinis | Addition of 2–4% CuNPs provided antimicrobial potential to the GIC: HDPFs viability = 68-72% (after 48 h), <10 CFU S. mutans (3 and 4%), <20 CFU S. sanguinis (4%) |
| AgNP [52] | Commercially available, 25 nm | Harvard Ionoglas Cem ® (type I) | 5%NPs in GIC, evaluation of physico-mechanical properties | Addition of AgNPs significantly increased most of the physico-mechanical parameters: CS~150 MPa, DTS~11 MPa, FS = 29 MPa, H = 90.4 VHN; control CS = 117 MPa, DTS = 7.2 MPa, FS = 27.4 MPa, H = 56.6 VHN; |
| AgNP [53] | Commercially available | GC Fuji II GP ® (type II ii) | 0.1%NPs, used as a pretreatment (after the conditioner), evaluation of μSBS | Dentin pretreatment with the nanoparticles after applying the conditioner enhanced the bond strength: μSBS = 3.24 MPa, compared with control 2.17 MPa |
| AgNP [54] | Commercially available, 20 nm | GC Fuji II GP ® (type II ii) | 0.1, 0.2%NPs in GIC, evaluation of μSBS, CS, FS, H | GICs with 0.1% and 0.2% AgNPs significantly improved the mechanical properties compared to the unmodified GIC: μSBS = 7.22 MPa, CS = 37.67, FS = 13.03, H = 66.01; control μSBS = 2.14 MPa, CS = 26, FS = 10.92, H = 58.63 |
| AgNP [55] | - | GC Ortho LC, Fuji ® (type I) | 1%, 2% NPs in GIC, evaluation of cell viability, H, Ra | Addition of AgNPs led to insignificant differences in cell viability and to significant differences in terms of microhardness and surface roughness compared with control; H = 50.2/33.45 (1/2% NP), control = 54.48 VHN, Ra = 14.76/17.19 μm (1/2% NP), control = 23.45 μm |
| AgNP [56] | In situ synthesized in poly(acrylic acid) and L-(+)-tartaric acid, 6–11 nm | Fluoro-alumino-silicate ionomer glass powder, poly(acrylic acid) and L-(+)-tartaric acid | Final concentration 0.10–0.50% in GIC, evaluation of CS and antibacterial effect (against Escherichia coli) | The addition of 0.5% AgNPs led to significant increase in compressive strength and antimicrobial properties: 32% increase in CS; IZ = 76.1 mm2, inhibition of S. mutans biofilm |
| AgNP [57] | Commercially available, <100 nm | GC Fuji IX GP ® (type II ii) | 1, 3, and 5% NPs in GIC, evaluation of minimum inhibitory concentration and minimum bactericidal concentration (against S. aureus), biofilm reduction (against S. aureus and S. mutans), CS, and H | Addition of silver nanoparticles limits biofilm formation with an insignificant effect on mechanical properties: MIC/MBC = 25/50 μg/mL (S. aureus), 25 μg/mL (S. mutans); H = 83 (at 1 and 3%), 74 (at 5%), control 85 g/μm2. CS = 136/134/132/126 N/mm2 (control, 1, 3, 5%NP) |
| AgNP [58] | Phytosynthesized using Mangifera indica leaves, 32 nm | GC Fuji Gold Label Type 9 Glass Ionomer Cement (type I) | 3% NPs in GIC, evaluation of H, NPs antimicrobial potential against E. coli and S. aureus | Incorporation of AgNPs led to improvement of the low wear of GIC and prevented the formation of bacterial colonies. H: 82 (Vickers-VHN), 14.2 (Monsanto-kg/cm2), control 54 (Vickers-VHN), 9.5 (Monsanto-kg/cm2); IZ = 1.2/1.5 at 8 μg/mL |
| AgNP [59] | Chemical synthesis, 12 nm | GC Gold Label 1 (type I) | 0.1, 0.2% NPs in GIC, evaluation of cytotoxicity (MTT and Trypan Blue assays) | NPs did not affect the cytotoxicity of the GIC (no significant differences being observed). |
| AgNP [60] | Commercially available, 5–10 nm | GC Ortho LC, Fuji ® (type I) | 1, 3, 5, 10, 15% NPs in GIC, evaluation of antimicrobial potential (against S. mutans), μSBS | Initially, the incorporation of AgNPs led to significant antibacterial properties, gradually lost with aging time; no antimicrobial effect observed after 8 weeks. A gradual decrease in bond strength was observed with the increasing incorporation of AgNPs, although the results were in the ideal bond strength range: μSBS: 9.58/9.47/9.30/9.07/8.64/7.80 MPa (control, 1/3/ 5/10/15%NP) Addition of AgNPs can decrease the demineralization rate without affecting bond strength |
3.2. Metal and Metalloid Oxide Nanoparticles in Glass Ionomer Cements
| NM | NM Characteristics | GIC | Experimental Study | Findings |
|---|---|---|---|---|
| TiO2 [63] | Biosynthesized using Bacillus subtilis, 70.17 nm | GC Fuji II GP ® (type II ii) | 0–10%NM in GIC, evaluation of CS, FS | Addition of TiO2 to GIC revealed no observable cytotoxic effect. An increase in the compressive strength and flexural strength was observed for addition of NMs up to 5%. Best results (at 5%NP): CS = 15.51 MPa (control 7.63), FS = 26.39 MPa (control 16.11) |
| TiO2 [51] | Commercially available | GC Fuji II GP ® (type II ii) | 5% NM in GIC, evaluation of μSBS | TiO2 can be incorporated in GIC without compromising the bond strength: μSBS = 4.15 MPa, compared with control 3.77 MPa |
| ZnO [51] | Commercially available | 5% NM in GIC, evaluation of μSBS | Incorporation of ZnO affected the bond strength: μSBS = 2.93 MPa, compared with control 3.77 MPa | |
| TiO2 [52] | Commercially available, 21 nm | Harvard Ionoglas Cem ® (type I) | 5% NM in GIC, evaluation of physico-mechanical properties | Addition of TiO2NMs significantly increased the physico-mechanical parameters: CS = 154.2 MPa, DTS = 13.2 MPa, FS ~28.5 MPa, H ~89 VHN; control CS = 117 MPa, DTS = 7.2 MPa, FS = 27.4 MPa, H = 56.6 VHN |
| TiO2 [53] | Commercially available | GC Fuji II GP ® (type II ii) | 0.1% NM, used as a pretreatment (after the conditioner), evaluation of μSBS | Dentin pretreatment with the nanoparticles after applying the conditioner enhanced the bond strength: μSBS = 4.81 MPa, compared with control 2.17 MPa |
| ZnO [53] | Commercially available | Dentin pretreatment with the nanoparticles after applying the conditioner enhanced the bond strength: μSBS = 4.07 MPa, compared with control 2.17 MPa | ||
| TiO2 [64] | Nanotubes, chemically synthesized, particle size 20 nm, diameter 10 nm | Ketac Molar EasyMix™ (type II ii) | 3, 5, 7% NM in GIC, evaluation of antimicrobial potential (against Streptococcus mutans) | Increased antimicrobial effect with incorporation of 5% NMs: IZ = 8.77/9.06 mm (1 day/7 days) compared with CIG control 8.49/8.41 mm (1 day/7 days). Incorporation of NMs affected S. mutans viability and the expression of key genes for bacterial survival and growth. Anticariogenic properties were improved |
| ZnO [65] | Phytosynthesized using Syzygium aromaticum extract | GC Fuji II GP ® (type II ii) | 50% NM in GIC, evaluation of antimicrobial potential (against Streptococcus mutans) | Incorporation of NMs provided antimicrobial activity to the GIC: IZ ~10.5 to 15.5 mm (depending on the S. mutans isolate) |
| TiO2 [66] | Nanotubes, chemically synthesized, particle size 20 nm, diameter 10 nm | Ketac Molar EasyMix™ (type II ii) | 3, 5, 7% NM in GIC, evaluation of CS, FS, μSBS, Ra, WL (after brushing simulation) | Incorporation of NMs improved the mechanical properties and decreased weight loss after surface wear, without affecting adhesiveness to dentin. Best results at 5% NM: CS = 105.23 MPa, FS = 7.41 MPa, μSBS = 5.30 MPa, Ra = 0.3997/0.3851 μm (after/before brushing simulation), WL = 1.4%; control CS = 89.46 MPa, FS = 6.41 MPa, μSBS = 4.76 MPa, Ra = 0.4213/0.3127μm (after/before brushing simulation), WL = 3.8% |
| MgO [67] | Commercially available | Ketac Molar EasyMix™ (type II ii) | 1, 2.5, 5, 10% NM in GIC, evaluation of ST, CS, DTS, μSBS | Addition of NMs for up to 2.5% kept the setting time within the requirements of ISO standard, and increased cement strength, without affecting the adhesiveness. Best results at 1% NM: ST ~5.5 min, CS ~240 MPa, DTS ~8 MPa, μSBS (dentin) ~6.2 MPa, μSBS (enamel) ~5.5 MPa |
| MgO [68] | Commercially available, 20 nm | Ketac Molar EasyMix™ (type II ii) | 1, 2.5, 5, 10% NM in GIC, evaluation of antibacterial and antibiofilm potential against Streptococcus mutans and S. sobrinus | Addition of NMs above 2.5% led to the development of materials with antimicrobial activity. Best results at 10% NM: IZ ~8.5/8.8 mm; log10 (CFU/mL) ~6 |
| ZnO [69] | Commercially available | GC Fuji II GP ® (type II ii) | 1, 5, 10, 15% NM in GIC, evaluation of μSBS, FS, WT, ST | Marginal increase in mechanical properties, no significant differences recorded for any studied parameter |
| TiO2 [70] | Nanotubes, chemically synthesized, particle size 20 nm, diameter 10 nm | Ketac Molar EasyMix™ (type II ii) | 3, 5, 7% NM in GIC, evaluation of Ra, SH, cytotoxicity | Addition of NMs improved the physico-chemical properties, increased fluoride release, and positively influenced morphology/spreading and extracellular matrix composition. Best results at 5% NM: Ra = 0.49 μm, SH = 118.25 KHN, ECM collagenous and non-collagenous content: 2.94/54.6 μg/well (14 days) control Ra = 0.41 μm, SH = 81.48 KHN, ECM collagenous and non-collagenous content: 2.81/53.3 μg/well (14 days) |
| TiO2 [71] | Commercially available, 21 nm | GC Gold Label 1 (type I) | 3%NM in GIC, evaluation of CS, FS, SH | Addition of NMs significantly improved the mechanical properties: FS ~30 MPa, CS ~240 SH ~75 VHN |
| ZnO [72] | - | GC Fuji II GP ® (type II ii) | 1 and 2% NM in GIC, evaluation of antibacterial activity (S. mutans) | No improvement of antibacterial activity observed |
| Al2O3 [73] | Commercially available, <50 nm | 3M™ Vitremer™ (type II ii) | 3.9, 6.1% NM in GIC, evaluation of CL | Addition of NMs improved mechanical properties, without being affected by thermal cycling in artificial saliva; cracks and pores were detected in the modified cement. CL (max. for 3.9%) ~2350 N |
| ZrO2 [73] | Commercially available, <50 nm | 4.7, 9.4, 11, 15.8% NM in GIC, evaluation of CL | Addition of NMs improved mechanical properties, without being affected by thermal cycling in artificial saliva; cracks and pores were detected in the modified cement. CL (max. for 4.7 and 9.4%) ~2150 N | |
| TiO2 [74] | Commercially available, <25 nm | Dental Shofu FX-II Enhanced Direct Restorative (Type II i) | 3 and 5% NM in GIC, evaluation of antibacterial activity (S. mutans), CS, H, FS, μSBS | Addition of NMs significantly improved mechanical properties and antibacterial activity, without affecting the enamel and dentin adhesion. IZ = 2.11/1.53 mm (control 0.92 mm); CS = 7.3/8.6 MPa, H = 64.2/63.8 VHN, FS = 20.2/21.4 MPa, μSBS dentin = 1.5/0.99, μSBS enamel = 1.96/2.2; control: CS = 5.6 MPa, H = 54.3 VHN, FS = 15.1 MPa, μSBS dentin = 1.32, μSBS enamel = 1.89 |
| SiO2 [75] | 20–70 nm | Medicem (Type I) | 0.01, 0.02, 0.04% NM in GIC, evaluation of bioactivity | Addition of NMs led to the enhancement of the GIC’s bioactivity. Development of a calcium phosphate phase after 1 week immersion in SBF was observed |
| TiO2 [76] | Commercially available, 21 nm | Kavitan ® Plus (Type III) | 3, 5, 7% NM in GIC, evaluation of antibacterial activity (S. mutans), ST, FT, CS, H, FS, μSBS | Addition of up to 5% NMs improved the mechanical properties without affecting bond strength with dentin or fluoride release. Materials developed possess antimicrobial activity. FT = 1.29/1.33/1.57 MPa/m2, CS = 176.27/157.53/92.75 MPa, H = 48.34/36.54/ 28.3 VHN, FS = 23.17/ 19.65/9.12 MPa, ST = 217/204/178 s μSBS = 11.54/10.48/10.14 MPa; control: FT = 0.69 MPa/m2, CS = 149.06 MPa, H = 46.3 VHN, FS = 13.57 MPa, ST = 268 s μSBS = 9.46 MPa; BGR = 0.122/0.117/0.112, control = 1.49. Most promising material was proposed to contain 3% NMs |
3.3. Incorporation of Apatitic Materials in Glass Ionomer Cements
- (a)
- increase the compressive strength by filling the voids in the composite, thus preventing the appearance of defects (such as pores and cracks);
- (b)
- increase flexural strength, due to its porosity;
- (c)
- influence the microhardness of the GIC, usually by increasing it (with superior results for hydroxyapatite in its nanoform compared with microcrystalline material);
- (d)
- improve biocompatibility;
- (e)
- minimize microleakage;
- (f)
- increase fluoride ion release;
- (g)
- increase the antimicrobial properties.
| AN | AN Characteristic | GIC | Experimental Study | Findings |
|---|---|---|---|---|
| HAP [81] | Commercially available | Ketac Molar EasyMix™ (type II ii) | 5% AM in GIC, evaluation of Ra, H, WL after 60 days of brushing simulation cycles | Addition of AM generated significant changes in the studied parameters: Ra = 1.17 mm (control 0.99), H = 41.19 MPa (control 50.96), WL = −0.00205 g (control 0.00010) |
| HAP [82] | Commercially available, 20 nm | GC Fuji II GP ® (type II ii) | 2, 4, 6, 8, 10% AM in GIC, evaluation of ST, CS, H, ML | ST: at concentration above 6%, exceeded imposed limits; at 6%: CS = 158.3 MPa, H = 126.4 MPa, ML = 15.33 (control = 40). No significant changes in the cytotoxicity were observed |
| HAP [83] | Commercially available | GC Fuji II GP ® (type II ii) | 1, 2, 5, 7, 10% AM in GIC, evaluation of cytotoxicity | Increased cell viability at 10–99.8% (at 72h, compared with control −91%) |
| HAP [84] | Obtained by co-precipitation from egg-shells, 39.15 nm | GC Fuji IX GP ® (type II ii) | 3, 5, 7, 9% AM in GIC, evaluation of H | Higher concentration of AM increased the GIC surface harness. H = 70.21/74.68/ 76.16/79.27 VHN (control – 61.86) |
| HAP, FHAP [85] | Obtained by microwave-assisted precipitation, different degrees of fluoridation, crystallite size 16.69–22.68 nm | GC Fuji IX GP ® (type II ii) | 5, 7.5, 10% AM in GIC, evaluation of H | Addition of AM in certain amounts increased microhardness; the difference in fluoridation degrees with the addition of the same mass percentage does not significantly influences the microhardness. Best results: HAP 7.5% (H = 112.17 VHN), 35FHAP 5% (H = 81.23 VHN), 65FHAP 7.5% (H = 80.5 VHN), 95FHAP 5% (H = 81.23 VHN), control 48.94 VHN |
| HAP [86] | Obtained by co-precipitation, hexagonal, 80–150 nm | GC Fuji I® (type I) | 1, 2, 4, 6, 8% AM in GIC at different powder/liquid ratios, evaluation of FS, μSBS | Addition of AM led to the increase in mechanical properties and adhesion potential. Best results at 6% HAP, 3:1 powder/liquid ratio: FS = 30.97 MPa (control 11.65 MPa), μSBS = 0.97 MPa (control 0.39 MPa) |
| HAP [87] | Commercially available, <200 nm | SDI Riva Self Cure GIC (type I) | 1, 3, 5, 8, 10% AM in GIC, evaluation of fluoride release, CS, antibacterial effect (against S. mutans) | Addition of HAP increased release up to 8% HAP (0.36 μg/mm2), while CS increased for 3–10% HAP (147.12–149.72 MPa), IZ (best results at 8% HAP) ~8.5 mm |
| HAP [88] | Obtained by co-precipitation, 24 nm | GC Fuji II GP ® (type II ii) | 5, 8% in GIC, evaluation of CS, DTS, H, ST, WT | Addition of HAP increased mechanical properties: ST = 150/153 s (control 187), WT = 110/108 (control 125), CS ~70/70 (control ~65 MPa), DTS ~9.5/11 (control ~8 MPa), H = 69.3/75.4 (control = 65.3 VHN) |
| FAP [88] | Obtained by co-precipitation, 30 nm | Addition of FAP increased mechanical properties: ST = 138/135 s (control 187), WT = 98/95 (control 125), CS = ~72/72 (control ~65 MPa), DTS ~11/12 (control ~8 MPa), H = 74.2/77.3 (control = 65.3 VHN) | ||
| HAP [89] | Commercially available | GC Fuji II GP ® (type II ii) | 25% AM in GIC, evaluation of microleakage at enamel and dentin/cementum interface | Microleakage of occlusal margin was significantly lower than that of gingival margin |
| HAP [90] | Obtained by co-precipitation, 24 nm | GC Fuji II ® (type II ii) | 5, 8% in GIC, evaluation of CS, DTS, H, ST, WT | Addition of HAP led to an increase in the mechanical properties: ST = 295/215 s (control 340), WT = 215/198 (control 235), CS ~110/112 (control ~105 MPa), DTS ~15/15.5 (control ~12.5 MPa), H = 161.5/168 (control = 158 VHN) |
| FAP [90] | Obtained by co-precipitation, 30 nm | Addition of FAP led to the increase in the mechanical properties: ST = 275/225 s (control 340), WT = 210/198 (control 235), CS = ~120/120 (control ~105 MPa), DTS ~17.5/19 (control ~12.5 MPa), H = 176.6/201 (control = 158 VHN) | ||
| FAP [91] | Obtained by sol-gel, ~100–200 nm | GC Fuji IX GP ® (type II ii) | Glass powder/FAP ratio = 20:1, powder/liquid ratio = 3.6/1, evaluation of H, fluoride release, cytotoxicity | Addition of FAP improved surface hardness; H at 7 days = 53.29 kg/mm2 (control 46.89); no significant influence on fluoride release and cell proliferation, compared with control, were recorded |
| HAP [92] | Commercially available, 10–20 nm | Not declared | 8% AM in GIC, evaluation of μSBS | Addition of HAP interfered with the bonding ability: 3.28 MPa (control 5.25 MPa); a mixed type of failure was observed for the developed material, while for GIC, a cohesive failure |
| HAP [93] | Microwave synthesized, calcium deficient, 24 nm | Not declared | 5, 10, 15% AM in GIC, evaluation of H, WL, CS, ionic release | The ionic release percentage, weight loss, and compressive strength increased with HAP addition. H ~80/66/58 (control 85 VHN); CS ~102/92/80 (control 68 MPa), increased weight loss and ionic release |
3.4. Other Types of Nanomaterials Used in Glass Ionomer Cements
| NM | NM Characteristics | GIC | Experimental Study | Findings |
|---|---|---|---|---|
| BN-TiO2 [95] | Chemically synthesized, BN nanosheets (200 nm-1μm) with TiO2 grown in situ (20-200 nm); max. thickness of the nanocomposite – 4 nm | China GIC (Chang Shu Shang Chi Dental Materials) (type I) | 0.3, 0.7, 1.1, 1.5% NM in GIC, evaluation of H, CS, CoF, So, antibacterial properties (against Streptococcus mutans), cytotoxicity (L-929) | The NM served as a reinforcing material for GIC. Data compared with control: H increase: 25.6/77.9/149.65/56.5%; CS increase: 32.8/64.5/ 80.2/52.6%; CoF and So decrease; antibacterial effect increase: 14.5/38.4/67.2/93.4/76.9%; no significant influence on the L-929 cells |
| Mg2SiO4 [96] | Sol-gel synthesized, 70–80 nm | GC Fuji II GP ® (type II ii) | 2, 4, 6% NM in GIC, evaluation of H, CS, FT, fluoride release | Addition of NM led to the improvement of mechanical properties, optimal fluoride release and bioactivity. CS = 850/630/480 MPa (control 350), H = 152/144/131 VHN (control 114), FT = 6.1/4.2/4.3 MPa/m2 (control 2.7), slight fluoride-release reduction |
| ZrO2-SiO2-HAP [97] | Sol-gel synthesized, 21.62 nm | GC Fuji IX GP ® (type II ii) | 3, 5, 7, 9% NM in GIC, evaluation of FT, color stability, So, Sp | Addition of NM (especially at 5%) significantly enhanced GIC physico-mechanical properties. FT = 1.16/1.35/1.09/1.05 MPa/m2 (control 0.78); ΔE (28 days) = 2.75 (5%, control 3.56), So – 66.46 μg/mm3 (control), Sp – 23.64 μg/mm3 (control 36.28) |
| SiO2-HAP [98] | Sol-gel synthesized | GC Fuji IX GP ® (type II ii) | 10% NM in GIC, evaluation of ionic exchange with human enamel and dentin | The addition of NM could provide increased remineralization. Superior levels at ion exchange layer for Sr and Al (enamel), Si, P, Ca (dentin); at 0.1 mm for Ca, Sr (enamel), Al (dentin); at 0.5 mm Si, Sr (enamel), Si (dentin) |
| SiO2-HAP [99] | Sol-gel synthesized, elongated HAP (100–150 nm) covered with SiO2 (40 nm) | GC Fuji IX GP ® (type II ii) | 10% NM in GIC, evaluation of Ra, So, Sp | Addition of NM enhances the GIC physical properties and slightly increased sol-sorption properties. Ra = 0.22 (control 0.22) after 28 days, Sp = 48.38 μg/mm3 (control 42.64), So = 63.66 μg/mm3 (control 56.65) |
| rGn-Ag [100] | Synthesized by a chemical method | GC Fuji IX GP ® (type II ii) | 0.05, 0.1, 0.5, 1, 2%NM in GIC, evaluation of antimicrobial potential, cytotoxicity, FS, H | Addition of 1 and 2% NM significantly decreased the percentage of viable bacteria, without negatively influencing the mechanical properties. FS and H significant increase at 0.1% |
| Cellulose/ TiO2 [101] | Commercial cellulose nanowhiskers, chemically synthesized TiO2 (50 nm). | China GIC (Chang Shu Shang Chi Dental Materials) (type I) | 2%TiO2+1% cellulose in GIC, evaluation of CS, H, enamel μSBS, WR, D, antimicrobial potential (Candida albicans), cytotoxicity (L-929) | Addition of NM led to an increase in mechanical properties: CS = 112.7 MPa (control 94.4), no influence on H, enamel μSBS = 14.61 MPa (control 9.69), no significant influence on WR and D; antifungal activity = 92.3% (70 control); slight cytotoxic effect |
| ZrO2-SiO2-HAP [102] | Sol-gel synthesized, HAP nanorods—length 114 nm, SiO2 18 nm, ZrO2 39 nm | GC Fuji IX GP ® (type II ii) | 3, 5, 7, 9%NM in GIC, evaluation of CS, FS, Ra | Incorporation of NM resulted in considerable improvement in the mechanical properties. Best results at 5%: CS = 144.12 MPa (control 117.64), FS = 18.12 MPa (control 14.38). Ra = 0.13/0.15/0.33/0.65 μm (control 0.151) |
| ZrO2-SiO2-HAP [103] | Sol-gel synthesized | GC Fuji IX GP ® (type II ii) | NM concentration in GIC not disclosed, evaluation of microleakage | Modified GIC had more microleakage than the unmodified cement: 0.96 (control 0.58) |
| SiO2-HAP [104] | Sol-gel synthesized, elongated HAP (100–150 nm) covered with SiO2 (~50 nm), different SiO2 content (11, 21, 35) | GC Fuji IX GP ® (type II ii) | 5, 10, 15, 20% NM in GIC, evaluation of H, CS, FS, μSBS | Addition of NM significantly enhanced the mechanical properties of the GIC. Best results for 10% 35SiO2-HAP: H = 64.77 VHN (control), CS = 143, 42 MPa (control 119.82), FS = 17.68 MPa (control 11.53), μSBS = 7.85 MPa (control 6.69) |
| SiO2-HAP [105] | Sol-gel synthesized | GC Fuji IX GP ® (type II ii) | 5% NM in GIC, evaluation of cytotoxicity (MTT assay) | Addition of NM led to an increase in cytotoxicity at 200 mg/mL (cell viability 21.27% at 72 h, compared with control, 57.83%), while no significant differences to control at lower concentrations were observed |
| ZrO2-SiO2-HAP [106] | One-pot synthesized SiO2-HAP, commercially available ZrO2; HAP nanorods: length 140 nm, SiO2 21 nm, ZrO2 40 nm; ZrO2 added at different concentration (5, 15, 20, 25% in nanocomposite) | GC Fuji IX GP ® (type II ii) | 1, 3, 5, 7, 9, 15, 20% NM in GIC, evaluation of H, ΔE | Addition of NM led to the significant improvement of hardness and aesthetic features. Best results at 5% 25ZrO2-SiO2-HAP: H = 79.38 VHN; ΔE = 4.09 (control 1.99) |
| Nanoclay [107] | Commercially available, medical grade, 1 nm thickness, 300–600 nm surface dimensions | HiFi glass powder (alumino-silicate glass) and HiFi polyacrylic acid (PAA) powder (Advanced Healthcare Limited) | 1, 2, 4% NM in GIC, evaluation of WR, H | No significant influence on WR and H; marginal increase in H at 4% NM |
| HAP-Ag [108] | HAP commercially available, composite synthesis assisted by γ radiation, 55–65 nm | Transbond XT paste 3M (type I) | 1, 5, 10%NM in GIC, evaluation of antimicrobial properties (against Streptococcus mutans, Lactobacillus acidophilus and S. sanguinis) | Addition of NMs led to a concentration-dependent increase in the mechanical properties: IZ (at 10%) = 8.66/7.66/ 9.66 mm; IZ (at 5%) = 6.33/5.66/7.66 mm; eluted component test: S. mutans, significant decrease colony count with concentration increase. S. sanguinis, no significant differences between 1 and 5%. Significant reduction at 10%. L. acidophilus, no significant differences between 1 and 5%. Biofilm inhibition: S. mutans, significant differences between all groups (except 5/10%). S. sanguinis and L. acidophilus, significant differences between all groups (except between 1/5%, 5/10%) |
| SiO2-HAP [109] | Sol-gel synthesis, elongated HAP (~103 nm), SiO2 (~30 nm), different SiO2 content (11, 21, 35) | GC Fuji IX GP ® (type II ii) | 1, 3, 5, 7, 9, 15, 20% NM in GIC, evaluation of H | Addition of NMs led to denser and stronger GIC. Best results at 5% 35SiO2-HAP: H = 70.8 VHN (control 40.6) |
| Nanoclay [110] | Purified nanomer/polymer-grade montmorillonite, (PGV/PGN) | GC Fuji IX GP ® (type II ii) | 2%NM in GIC, evaluation of CS, DTS, FS, Ef, WT, ST | Addition of nanoclay led to the enhancement of mechanical properties, without negatively influencing the nature of polyacid neutralization. 1-month results: PGV: CS = 122 MPa, DTS = 17 MPa, FS = 24 MPa, Ef = 13 GPa, WT = 4.15 min, ST = 6.55 min; PGN: CS = 130 MPa, DTS = 19 MPa, FS = 28 MPa, Ef = 12 GPa, WT = 4.50 min, ST = 6.50 min; control: CS = 124 MPa, DTS = 16 MPa, FS = 20 MPa, Ef = 11 GPa, WT=4.16 min, ST = 6.35 min |
| Nanoclay [111] | Polymer-grade montmorillonite | HiFi, Advanced Healthcare (type I) | 1, 2, 4%NM in GIC, evaluation of CS, DTS, FS, Ef, WT, ST | Addition of 1/2% NM increased mechanical properties, while 2/4% NM reduced working and setting times. Best 1-month results were recorded at 2%: CS = 134 MPa, DTS = 20 MPa, FS = 43 MPa, Ef = 11 GPa, WT=3.05. Control: CS = 124 MPa, DTS = 18 MPa, FS = 36 MPa, Ef = 14 GPa, WT=3.28 min, ST = 6.30 min |
| Mg2SiO4 [112] | Sol-gel synthesized, 36 nm | GC Fuji II GP ® (type II ii) | 1, 2, 3, 4%NM in GIC, evaluation of CS, FS, DTS | Addition of 1% NM is recommended for applications in which the maximum strength in all three modes of loading is required. CS = 74.4/94.1/106.3/ 38 MPa (control 42.4), FS = 93.7/71.1/31.3/- MPa (control 52,4), DTS = 13/11.7/9.6/- MPa (control 10) |
| Al2O3/ ZrO2 [113] | Spray pyrolysis, 26 nm | Qingpu NiKang Dental Instrument Manufactory (type I) | Incorporation in GIC alongside HAP and NBG, evaluation of ST, H, YM, W, So, antimicrobial potential (Pseudomonas, Bacillus) | Addition of the nanocomposite led to the improvement of mechanical properties, setting time, bioactivity, and antimicrobial activity: ST = 55 s, H = 0.67 MPa, YM = 15.6 GPa, W (after 6 h) = 0.508, initial 0.598 g, So = 15.05%, IZ = 15/14 mm. Control: ST = 110 s, H = 0.43 MPa, YM = 7.77 GPa, W (after 6 h) = 0.478, initial 0.598 g, So = 20.067%. |
4. Implications and Future Perspectives
5. Conclusions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Zaura, E.; ten Cate, J.M. Towards understanding oral health. Caries Res. 2015, 49, 55–61. [Google Scholar] [CrossRef]
- Marsh, P.D.; Head, D.A.; Devine, D.A. Ecological approaches to oral bioflms: Control without killing. Caries Res. 2015, 49, 46–54. [Google Scholar] [CrossRef]
- Petersen, P.E.; Lennon, M.A. Effective use of fluorides for the prevention of dental caries in the 21st century: The WHO approach. Community Dent. Oral. Epidemiol. 2004, 32, 319–321. [Google Scholar] [CrossRef]
- World Health Organization. Oral Health. Available online: https://www.who.int/news-room/fact-sheets/detail/oral-health (accessed on 1 August 2022).
- Balhaddad, A.A.; Kansara, A.A.; Hidan, D.; Weir, M.D.; Xu, H.H.K.; Melo, M.A.S. Toward dental caries: Exploring nanoparticle-based platforms and calcium phosphate compounds for dental restorative materials. Bioact. Mater. 2019, 4, 43–55. [Google Scholar] [CrossRef]
- Lazăr, V.; Dițu, L.M.; Curuțiu, C.; Gheorghe, I.; Holban, A.; Popa, P.; Chifiriuc, C. Impact of Dental Plaque Biofilms in Periodontal Disease: Management and Future Therapy. In Periodontitis—A Useful Reference; Arjunan, P., Ed.; IntechOpen: London, UK, 2017; pp. 11–42. [Google Scholar] [CrossRef]
- Silva, E.J.N.L.; De-Deus, G.; Souza, E.M.; Belladonna, F.G.; Cavalcante, D.M.; Simões-Carvalho, M.; Versiani, M.A. Present status and future directions—Minimal endodontic access cavities. Int. Endod. J. 2022, 55, 531–587. [Google Scholar] [CrossRef]
- Cubas, G.B.; Camacho, G.B.; Pereira-Cenci, T.; Nonaka, T.; Barbin, E.L. Influence of cavity design and restorative material on the fracture resistance of maxillary premolars. Gen. Dent. 2010, 58, e84–e88. [Google Scholar]
- ISO 9917-1. Dental Water Based Cements. International Organization for Standardization: Geneva, Switzerland, 2003.
- Wilson, A.D. Glass-ionomer cement–origins, development and future. Clin. Mater. 1991, 7, 275–282. [Google Scholar] [CrossRef]
- Mustafa, H.A.; Soares, A.P.; Paris, S.; Elhennawy, K.; Zaslansky, P. The forgotten merits of GIC restorations: A systematic review. Clin. Oral. Investig. 2020, 24, 2189–2201. [Google Scholar] [CrossRef]
- Smith, D.C. Development of glass-ionomer cement systems. Biomaterials 1998, 19, 467–478. [Google Scholar] [CrossRef]
- Wilson, A.D.; Kent, B.E. The glass-ionomer cement, a new translucent dental filling material. J. Appl. Chem. Biotechnol. 1971, 21, 313. [Google Scholar] [CrossRef]
- Yan, Z.; Sidhu, S.K.; Carrick, T.E.; McCabe, J.F. Response to thermal stimuli of glass ionomer cements. Dent. Mater. 2007, 23, 597–600. [Google Scholar] [CrossRef] [PubMed]
- Sakaguchi, R.L.; Powers, J.M. Craig’s Restorative Dental Materials; Elsevier/Mosby: St. Louis, MO, USA, 2012. [Google Scholar]
- European Commission, Directorate-General for Health and Consumers, The Safety of Dental Amalgam and Alternative Dental Restoration Materials for Patients and Users. Available online: https://data.europa.eu/doi/10.2772/42641 (accessed on 1 August 2022).
- Fricker, J.P. Therapeutic properties of glass-ionomer cements: Their application to orthodontic treatment. Aust. Dent. J. 2022, 67, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Dezanetti, J.M.P.; Nascimento, B.N.; Orsi, J.S.R.; Souza, E.M. Effectiveness of glass ionomer cements in the restorative treatment of radiation-related caries—A systematic review. Support Care Cancer, 2022; online ahead of print. [Google Scholar] [CrossRef]
- Iaculli, F.; Salucci, A.; Di Giorgio, G.; Luzzi, V.; Ierardo, G.; Polimeni, A.; Bossù, M. Bond Strength of Self-Adhesive Flowable Composites and Glass Ionomer Cements to Primary Teeth: A Systematic Review and Meta-Analysis of In Vitro Studies. Materials 2021, 14, 6694. [Google Scholar] [CrossRef] [PubMed]
- Peric, T.; Markovic, E.; Markovic, D.; Petrovic, B. Meta-Analysis of In-Vitro Bonding of Glass-Ionomer Restorative Materials to Primary Teeth. Materials 2021, 14, 3915. [Google Scholar] [CrossRef] [PubMed]
- Sidhu, S.K.; Nicholson, J.W. A Review of Glass-Ionomer Cements for Clinical Dentistry. J. Funct. Biomater. 2016, 7, 16. [Google Scholar] [CrossRef]
- Pagano, S.; Lombardo, G.; Costanzi, E.; Balloni, S.; Bruscoli, S.; Flamini, S.; Coniglio, M.; Valenti, C.; Cianetti, S.; Marinucci, L. Morpho-functional effects of different universal dental adhesives on human gingival fibroblasts: An in vitro study. Odontology 2021, 109, 524–539. [Google Scholar] [CrossRef]
- Sasanaluckit, P.; Albustany, K.R.; Doherty, P.J.; Williams, D.F. Biocompatibility of glass ionomer cements. Biomaterials 1993, 14, 906–916. [Google Scholar] [CrossRef]
- Sidhu, S.K.; Schmalz, G. The biocompatibility of glass-ionomer cement materials. A status report for the American Journal of Dentistry. Am. J. Dent. 2001, 14, 387–396. [Google Scholar]
- Bapat, R.A.; Parolia, A.; Chaubal, T.; Dharamadhikari, S.; Abdulla, A.M.; Sakkir, N.; Arora, S.; Bapat, P.; Sindi, A.M.; Kesharwani, P. Recent update on potential cytotoxicity, biocompatibility and preventive measures of biomaterials used in dentistry. Biomater. Sci. 2021, 9, 3244–3283. [Google Scholar] [CrossRef]
- Elibol, C.; Atalay, E.G.; Sagir, K.; Yoruc, A.B.H. Effect of water absorption and hydroxyapatite addition on mechanical and microstructural properties of dental luting cements. Mat. Test. 2022, 64, 303–313. [Google Scholar] [CrossRef]
- Ali, M.; Okamoto, M.; Watanabe, M.; Huang, H.; Matsumoto, S.; Komichi, S.; Takahashi, Y.; Hayashi, M. Biological properties of lithium-containing surface pre-reacted glass fillers as direct pulp-capping cements. Dent. Mat. 2022, 38, 294–308. [Google Scholar] [CrossRef] [PubMed]
- Meneses, I.H.C.; Sampaio, G.A.M.; Vieira, R.A.; Campos, M.J.D.S.; Alves, P.M.; Pithon, M.M.; Lacerda-Santos, R. Effect of Yellow Propolis on Biocompatibility of Cements: Morphological and Immunohistochemistry Analysis. Eur. J. Dent. 2022, 16, 130–136. [Google Scholar] [CrossRef] [PubMed]
- Wilson, N.H.; Mjor, I.A. The teaching of class I and class II direct composite restorations in European dental schools. J. Dent. 2000, 28, 15–21. [Google Scholar] [CrossRef]
- Peng, C.F.; Yang, Y.; Zhao, Y.M.; Liu, H.; Xu, Z.; Zhao, D.H.; Qin, M. Long-term treatment outcomes in immature permanent teeth by revascularisation using MTA and GIC as canal-sealing materials: A retrospective study. Int. J. Paediatr. Dent. 2017, 27, 454–462. [Google Scholar] [CrossRef]
- Thomas, B.; Gupta, K. In vitro biocompatibility of hydroxyapatite-added GIC: An SEM study using human periodontal ligament fibroblasts. J. Esthet. Restor. Dent. 2017, 29, 435–441. [Google Scholar] [CrossRef]
- Lorenzetti, C.C.; Bortolatto, J.F.; Ramos, A.T.P.R.; Shinohara, A.L.; Saad, J.R.C.; Kuga, M.C. The effectiveness of glass ionomer cement as a fiber post cementation system in endodontically treated teeth. Microsc. Res. Tech. 2019, 82, 1191–1197. [Google Scholar] [CrossRef]
- Vahid-Dastjerdi, E.; Borzabadi-Farahani, A.; Pourmofidi-Neistanak, H.; Amini, N. An in-vitro assessment of weekly cumulative fluoride release from three glass ionomer cements used for orthodontic banding. Prog. Orthod. 2012, 13, 49–56. [Google Scholar] [CrossRef]
- Beauchamp, J.; Caufield, P.W.; Crall, J.J.; Donly, K.; Feigal, R.; Gooch, B.; Ismail, A.; Kohn, W.; Siegal, M.; Simonsen, R.; et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants—A report of the American Dental Association Council on Scientific Affairs. J. Am. Dent. Assoc. 2008, 139, 257–268. [Google Scholar] [CrossRef]
- Aboush, Y.E.; Torabzadeh, H. Clinical performance of Class II restorations in which resin composite is laminated over resinmodified glass-ionomer. Oper. Dent. 2000, 25, 367–373. [Google Scholar]
- Banerjee, A.; Frencken, J.E.; Schwendicke, F.; Innes, N.P.T. Contemporary operative caries management: Consensus recommendations on minimally invasive caries removal. Br. Dent. J. 2017, 223, 215–222. [Google Scholar] [CrossRef]
- Nicholson, J.; Czarnecka, B. Conventional glass-ionomer cements. In Materials for the Direct Restoration of Teeth; Nicholson, J., Czarnecka, B., Eds.; Woodhead Publishing: Duxford, UK, 2016; pp. 107–136. [Google Scholar] [CrossRef]
- Gorseta, K.; Borzabadi-Farahani, A.; Moshaverinia, A.; Glavina, D.; Lynch, E. Effect of different thermo-light polymerization on flexural strength of two glass ionomer cements and a glass carbomer cement. J. Prosthet. Dent. 2017, 118, 102–107. [Google Scholar] [CrossRef] [PubMed]
- Gavic, L.; Gorseta, K.; Borzabadi-Farahani, A.; Tadin, A.; Glavina, D.; van Duinen, R.N.; Lynch, E. Influence of Thermo-Light Curing with Dental Light-Curing Units on the Microhardness of Glass-Ionomer Cements. Int. J. Periodontics Restor. Dent. 2016, 36, 425–430. [Google Scholar] [CrossRef] [PubMed]
- Nicholson, J.W.; Sidhu, S.K.; Czarnecka, B. Enhancing the Mechanical Properties of Glass-Ionomer Dental Cements: A Review. Materials 2020, 13, 2510. [Google Scholar] [CrossRef] [PubMed]
- Gupta, A.A.; Mulay, S.; Mahajan, P.; Raj, A.T. Assessing the effect of ceramic additives on the physical, rheological and mechanical properties of conventional glass ionomer luting cement—An in-vitro study. Heliyon 2019, 5, e02094. [Google Scholar] [CrossRef] [PubMed]
- Lardani, L.; Derchi, G.; Marchio, V.; Carli, E. One-Year Clinical Performance of Activa™ Bioactive-Restorative Composite in Primary Molars. Children 2022, 9, 433. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The Prisma 2020 statement: An updated guideline for reporting systematic reviews. PLoS Med. 2021, 18, e1003583. [Google Scholar] [CrossRef]
- Ashour, A.A.; Felemban, M.F.; Felemban, N.H.; Enan, E.T.; Basha, S.; Hassan, M.M.; Gad El-Rab, S.M.F. Comparison and Advanced Antimicrobial Strategies of Silver and Copper Nanodrug-Loaded Glass Ionomer Cement against Dental Caries Microbes. Antibiotics 2022, 11, 756. [Google Scholar] [CrossRef]
- Abed, F.M.; Kotha, S.B.; AlShukairi, H.; Almotawah, F.N.; Alabdulaly, R.A.; Mallineni, S.K. Effect of Different Concentrations of Silver Nanoparticles on the Quality of the Chemical Bond of Glass Ionomer Cement Dentine in Primary Teeth. Front. Bioeng. Biotechnol. 2022, 10, 816652. [Google Scholar] [CrossRef]
- Enan, E.T.; Ashour, A.A.; Basha, S.; Felemban, N.H.; Gad El-Rab, S.M.F. Antimicrobial activity of biosynthesized silver nanoparticles, amoxicillin, and glass-ionomer cement against Streptococcus mutans and Staphylococcus aureus. Nanotechnology 2021, 32, 215101. [Google Scholar] [CrossRef]
- Ashour, A.A.; Basha, S.; Felemban, N.H.; Enan, E.T.; Alyamani, A.A.; Gad El-Rab, S.M.F. Molecules Antimicrobial Efficacy of Glass Ionomer Cement in Incorporation with Biogenic Zingiber officinale Capped Silver-Nanobiotic, Chlorhexidine Diacetate and Lyophilized Miswak. Molecules 2022, 27, 528. [Google Scholar] [CrossRef]
- Aguilar-Perez, D.; Vargas-Coronado, R.; Cervantes-Uc, J.M.; Rodriguez-Fuentes, N.; Aparicio, C.; Covarrubias, C.; Alvarez-Perez, M.; Garcia-Perez, V.; Martinez-Hernandez, M.; Cauich-Rodriguez, J.V. Antibacterial activity of a glass ionomer cement doped with copper nanoparticles. Dent. Mater. J. 2020, 39, 389–396. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.; Yi, J.; Zhao, Z. Biocompatible orthodontic cement with antibacterial capability and protein repellency. BMC Oral. Health 2021, 21, 412. [Google Scholar] [CrossRef]
- Qasim, S.S.B.; Ali, D.; Soliman, M.S.; Zafiropoulos, G.G. The effect of chitosan derived silver nanoparticles on mechanical properties, color stability of glass ionomer luting cements. Mater. Res. Express 2021, 8, 085401. [Google Scholar] [CrossRef]
- Fattah, Z.; Jowkar, Z.; Rezaeian, S. Microshear Bond Strength of Nanoparticle-Incorporated Conventional and Resin-Modified Glass Ionomer to Caries-Affected Dentin. Int. J. Dent. 2021, 2021, 5565556. [Google Scholar] [CrossRef] [PubMed]
- Assery, M.K.A.; Abdulrahman, A.; AlWaleed, A.; Nawaf, L.; Mohamed, H. Nanoparticles as void fillers in glass ionomer cement for enhanced physicomechanical properties. Mater. Express 2020, 10, 1960–1964. [Google Scholar] [CrossRef]
- Jowkar, Z.; Fattah, Z.; Ghanbarian, S.; Shafiei, F. The Effects of Silver, Zinc Oxide, and Titanium Dioxide Nanoparticles Used as Dentin Pretreatments on the Microshear Bond Strength of a Conventional Glass Ionomer Cement to Dentin. Int. J. Nanomed. 2020, 15, 4755–4762. [Google Scholar] [CrossRef]
- Jowkar, Z.; Jowkar, M.; Shafiei, F. The Mechanical and dentin bond strength properties of the nanosilver enriched glass ionomer cement. J. Clin. Exp. Dent. 2019, 11, 275–281. [Google Scholar] [CrossRef] [PubMed]
- Munguía-Moreno, S.; Martínez-Castañón, G.A.; Patiño-Marín, N.; Cabral-Romero, C.; Zavala-Alonso, N.V. Biocompatibility and Surface Characteristics of Resin-Modified Glass Ionomer Cements with Ammonium Quaternary Compounds or Silver Nanoparticles: An In Vitro Study. J. Nanomat. 2018, 2018, 6401747. [Google Scholar] [CrossRef]
- Paiva, L.; Fidalgo, T.K.S.; da Costa, L.P.; Maia, L.C.; Balan, L.; Anselme, K.; Ploux, L.; Thiré, R.M.S.M. Antibacterial properties and compressive strength of new one-step preparation silver nanoparticles in glass ionomer cements (NanoAg-GIC). J. Dent. 2018, 69, 102–109. [Google Scholar] [CrossRef]
- El-Wassefy, N.A.; El-Mahdy, R.H.; El-Kholany, N.R. The impact of silver nanoparticles integration on biofilm formation and mechanical properties of glass ionomer cement. J. Esthet. Restor. Dent. 2018, 30, 146–152. [Google Scholar] [CrossRef]
- Sundeep, D.; Vijaya Kumar, T.; Rao, P.; Ravikumar, R.; Gopala Krishna, A. Green synthesis and characterization of Ag nanoparticles from Mangifera indica leaves for dental restoration and antibacterial applications. Progr. Biomat. 2017, 6, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Siqueira, P.C.; Magalhães, A.P.R.; Pires, V.C.; Pereira, F.C.; Silveira-Lacerda, E.P.; Carrião, M.S.; Bakuzis, A.F.; Souza-Costa, C.A.; Lopes, L.G.; Estrela, C. Cytotoxicity of glass ionomer cements containing silver nanoparticles. J. Clin. Exp. Dent. 2015, 7, e622–e627. [Google Scholar] [CrossRef] [PubMed]
- Li, F.; Li, Z.; Liu, G.; He, H. Long-term antibacterial properties and bond strength of experimental nano silver-containing orthodontic cements. J. Wuhan Univ. Technol.-Mat. Sci. Edit. 2013, 28, 849–855. [Google Scholar] [CrossRef]
- Fierascu, I.; Fierascu, I.C.; Brazdis, R.I.; Baroi, A.M.; Fistos, T.; Fierascu, R.C. Phytosynthesized Metallic Nanoparticles—Between Nanomedicine and Toxicology. A Brief Review of 2019′s Findings. Materials 2020, 13, 574. [Google Scholar] [CrossRef] [PubMed]
- Coutinho, E.; Cardoso, M.V.; DeMunck, J.; Neves, A.A.; Van Landuyt, K.L.; Poitevin, A.; Peumans, M.; Lambrechts, P.; Van Meerbeek, B. Bonding effectiveness and interfacial characterization of a nano-filled resin-modified glass-ionomer. Dent. Mater. 2009, 25, 1347–1357. [Google Scholar] [CrossRef]
- Mansoor, A.; Khan, M.T.; Mehmood, M.; Khurshid, Z.; Ali, M.I.; Jamal, A. Synthesis and Characterization of Titanium Oxide Nanoparticles with a Novel Biogenic Process for Dental Application. Nanomaterials 2022, 12, 1078. [Google Scholar] [CrossRef]
- de Souza Araújo, I.J.; Ricardo, M.G.; Gomes, O.P.; Giovani, P.A.; Puppin-Rontani, J.; Pecorari, V.A.; Martinez, E.F.; Napimoga, M.H.; Nociti Junior, F.H.; Puppin-Rontani, R.M.; et al. Titanium dioxide nanotubes added to glass ionomer cements affect S. mutans viability and mechanisms of virulence. Braz. Oral. Res. 2021, 35, 062. [Google Scholar] [CrossRef]
- Ahalya, N.; Dhamodhar, P.; Vaishnavi, A.D. Green Synthesis, Characterization of Zinc Oxide Nanoparticles and their Incorporation into Glass Ionomer Cement for Inhibition of Streptococcus mutans. Asian J. Chem. 2021, 33, 515–520. [Google Scholar] [CrossRef]
- Kantovitz, K.R.; Fernandes, F.P.; Feitosa, I.V.; Lazzarini, M.O.; Denucci, G.C.; Gomes, O.P.; Giovani, P.A.; Silva Moreira, K.M.; Arias Pecorari, V.G.; Sanches Borges, A.F.; et al. TiO2 nanotubes improve physico-mechanical properties of glass ionomer cement. Dent. Mater. 2020, 36, 85–92. [Google Scholar] [CrossRef]
- Noori, A.J.; Kareem, F.A. Setting time, mechanical and adhesive properties of magnesium oxide nanoparticles modified glass-ionomer cement. J. Mater. Res. Technol. 2020, 9, 1809–1818. [Google Scholar] [CrossRef]
- Noori, A.J.; Kareem, F.A. The effect of magnesium oxide nanoparticles on the antibacterial and antibiofilm properties of glass-ionomer cement. Heliyon 2019, 5, e02568. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, P.; Nayak, R.; Upadhya, P.N.; Ginjupalli, K.; Gupta, L. Evaluation of properties of Glass Ionomer Cement reinforced with Zinc Oxide nanoparticles—An in vitro study. Mat. Today Proc. 2018, 5, 16065–16072. [Google Scholar] [CrossRef]
- Cibim, D.D.; Saito, M.T.; Giovani, P.A.; Sanches Borges, A.F.; Arias Pecorari, V.G.; Gomes, O.P.; Lisboa-Filho, P.N.; Nociti-Junior, F.H.; Puppin-Rontani, R.M.; Kantovitz, K.R. Novel Nanotechnology of TiO2 Improves Physical-Chemical and Biological Properties of Glass Ionomer Cement. Int. J. Biomat. 2017, 2017, 7123919. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, M.A.; Priyadarshini, B.M.; Neo, J.; Fawzy, A.S. Characterization of Chitosan/TiO2 Nano-Powder Modified Glass-Ionomer Cement for Restorative Dental Applications. J. Esthet. Restor. Dent. 2017, 29, 146–156. [Google Scholar] [CrossRef] [PubMed]
- Sasso Garcia, P.P.N.; Cardia, M.F.B.; Francisconi, R.S.; Dovigo, L.N.; Palomari Spolidório, D.M.; de Souza Rastelli, A.N.; Botta, A.C. Antibacterial activity of glass ionomer cement modified by zinc oxide nanoparticles. Microsc. Res. Tech. 2017, 80, 456–461. [Google Scholar] [CrossRef]
- Souza, J.C.M.; Silva, J.B.; Aladim, A.; Carvalho, O.; Nascimento, R.M.; Silva, F.S.; Martinelli, A.E.; Henriques, B. Effect of Zirconia and Alumina Fillers on the Microstructure and Mechanical Strength of Dental Glass Ionomer Cements. Open Dent. J. 2016, 10, 58–68. [Google Scholar] [CrossRef]
- Garcia-Contreras, R.; Scougall-Vilchis, R.J.; Contreras-Bulnes, R.; Sakagami, H.; Morales-Luckie, R.A.; Nakajima, H. Mechanical, antibacterial and bond strength properties of nano-titanium-enriched glass ionomer cement. J. Appl. Oral. Sci. 2015, 23, 321–328. [Google Scholar] [CrossRef]
- Mabrouk, M.; Selim, M.M.; Beherei, H.; El-Gohary, M.I. Effect of incorporation of nano bioactive silica into commercial Glass Ionomer Cement (GIC). J. Genet. Eng. Biotechnol. 2012, 10, 113–119. [Google Scholar] [CrossRef]
- Elsaka, S.E.; Hamouda, I.M.; Swain, M.V. Titanium dioxide nanoparticles addition to a conventional glass-ionomer restorative: Influence on physical and antibacterial properties. J. Dent. 2011, 39, 589–598. [Google Scholar] [CrossRef]
- Fierascu, R.C.; Fierascu, I.; Lungulescu, E.M.; Nicula, N.; Somoghi, R.; Diţu, L.M.; Ungureanu, C.; Sutan, A.N.; Drăghiceanu, O.A.; Paunescu, A.; et al. Phytosynthesis and radiation-assisted methods for obtaining metal nanoparticles. J. Mat. Sci. 2020, 55, 1915–1932. [Google Scholar] [CrossRef]
- Saghiri, M.A.; Vakhnovetsky, J.; Vakhnovetsky, A. Functional role of inorganic trace elements in dentin apatite—Part II: Copper, manganese, silicon, and lithium. J. Trace Elem. Med. Biol. 2022, 72, 126995. [Google Scholar] [CrossRef] [PubMed]
- Fierascu, I.; Fierascu, R.C.; Somoghi, R.; Ion, R.M.; Moanta, A.; Avramescu, S.M.; Damian, C.M.; Ditu, L.M. Tuned apatitic materials: Synthesis, characterization and potential antimicrobial applications. Appl. Surf. Sci. 2018, 438, 127–135. [Google Scholar] [CrossRef]
- Murugan, R.; Yazid, F.; Nasruddin, N.S.; Anuar, N.N.M. Effects of Nanohydroxyapatite Incorporation into Glass Ionomer Cement (GIC). Minerals 2022, 12, 9. [Google Scholar] [CrossRef]
- Martins, R.A.; Marti, L.M.; Mendes, A.C.B.; Fragelli, C.; Cilense, M.; Zuanon, A.C.C. Brushing Effect on the Properties of Glass Ionomer Cement Modified by Hydroxyapatite Nanoparticles or by Bioactive Glasses. Int. J. Dent. 2022, 2022, 1641041. [Google Scholar] [CrossRef] [PubMed]
- Zhu, K.; Zheng, L.; Xing, J.; Chen, S.; Chen, R.; Ren, L. Mechanical, antibacterial, biocompatible and microleakage evaluation of glass ionomer cement modified by nanohydroxyapatite/polyhexamethylene biguanide. Dent. Mater. J. 2022, 41, 197–208. [Google Scholar] [CrossRef]
- Golkar, P.; Omrani, L.R.; Zohourinia, S.; Ahmadi, E.; Asadian, F. Cytotoxic Effect of Addition of Different Concentrations of Nanohydroxyapatite to Resin Modified and Conventional Glass Ionomer Cements on L929 Murine Fibroblasts. Front. Dent. 2021, 18, 17. [Google Scholar] [CrossRef]
- Effendi, M.C.; Pratiwi, A.R.; Afifah, F.; Taufiq, A. The Role of Chicken Egg-Shell Nano-Hydroxyapatite as Fillers on the Surface Hardness of Glass Ionomer Cement. Malays. J. Fundam. Appl. Sci. 2021, 17, 475–484. [Google Scholar] [CrossRef]
- Caesarianto, F.P.; Nurlely. The enhancement of glass ionomer cement mechanical strength through the incorporation of fluorhydroxyapatite nanocrystals. AIP Conf. Proc. 2021, 2346, 020004. [Google Scholar] [CrossRef]
- Kheur, M.; Kantharia, N.; Iakha, T.; Kheur, S.; Al-Haj Husain, N.; Özcan, M. Evaluation of mechanical and adhesion properties of glass ionomer cement incorporating nano-sized hydroxyapatite particles. Odontology 2020, 108, 66–73. [Google Scholar] [CrossRef]
- Alatawi, R.A.S.; Elsayed, N.H.; Mohamed, W.S. Influence of hydroxyapatite nanoparticles on the properties of glass ionomer cement. J. Mat. Res. Technol. 2019, 8, 344–349. [Google Scholar] [CrossRef]
- Barandehfard, F.; Kianpour Rad, M.; Hosseinnia, A.; Rashidi, A.; Tahriri, M.; Tayebi, L. The evaluation of the mechanical characteristics of the synthesized glass-ionomer cements (GICs): The effect of hydroxyapatite and fluorapatite nanoparticles and glass powders. J. Aust. Ceram. Soc. 2019, 55, 507–517. [Google Scholar] [CrossRef]
- Sharafeddin, F.; Feizi, N. Evaluation of the effect of adding micro-hydroxyapatite and nano-hydroxyapatite on the microleakage of conventional and resin-modified Glass-ionomer Cl V restorations. J. Clin. Exp. Dent. 2017, 9, 242–248. [Google Scholar] [CrossRef] [PubMed]
- Barandehfard, F.; Kianpour Rad, M.; Hosseinnia, A.; Khoshroo, K.; Tahriri, M.; Jazayeri, H.E.; Moharamzadeh, K.; Tayebi, L. The addition of synthesized hydroxyapatite and fluorapatite nanoparticles to a glass-ionomer cement for dental restoration and its effects on mechanical properties. Ceramic. Int. 2016, 42, 17866–17875. [Google Scholar] [CrossRef]
- Moshaverinia, M.; Borzabadi-Farahani, A.; Sameni, A.; Moshaverinia, A.; Ansari, S. Effects of incorporation of nano-fluorapatite particles on microhardness, fluoride releasing properties, and biocompatibility of a conventional glass ionomer cement (GIC). Dent. Mater. J. 2016, 35, 817–821. [Google Scholar] [CrossRef]
- Choudhary, K.; Nandlal, B. Comparative evaluation of shear bond strength of nano-hydroxyapatite incorporated glass ionomer cement and conventional glass ionomer cement on dense synthetic hydroxyapatite disk: An in vitro study. Indian J. Dent. Res. 2015, 26, 170–175. [Google Scholar] [CrossRef]
- Goenka, S.; Balu, R.; Kumar, T.S.S. Effects of nanocrystalline calcium deficient hydroxyapatite incorporation in glass ionomer cements. J. Mech. Behav. Biomed. Mater. 2012, 7, 69–76. [Google Scholar] [CrossRef]
- Mirghaderi, F.; Monshi, A.; Kasiri, M.; Doostmohammadi, A.; Khaghani, M. A Short Study on the Experimental Glass-Ionomer Cement Containing P2O5. Phosphorus Sulfur Silicon Relat. Elem. 2014, 189, 74–80. [Google Scholar] [CrossRef]
- Ma, Y.; Guo, Y.Z.; Liu, Y.; Wang, Y.R.; Yang, J.C.; Kong, X.Z.; Jia, H.L.; Li, R.Z.; Han, Q.Z.; Zheng, C.D.; et al. Mechanical and Antibacterial Properties of h-BN-TiO2 Nanocomposite-Modified Glass Ionomer Cement. Front. Mater. 2022, 9, 883027. [Google Scholar] [CrossRef]
- Nojehdehi, A.M.; Moghaddam, F.; Hamedani, M.T. Mechanical properties of glass ionomer cement incorporating forsterite nanoparticles synthesized by the sol-gel method. J. Sol-Gel. Sci. Technol, 2022; 1–9, in press. [Google Scholar] [CrossRef]
- Aldhuwayhi, S.D.; Sajjad, A.; Bakar, W.Z.W.; Mohamad, D.; Kannan, T.P.; Moheet, I.A. Evaluation of Fracture Toughness, Color Stability, and Sorption Solubility of a Fabricated Novel Glass Ionomer Nano Zirconia-Silica-Hydroxyapatite Hybrid Composite Material. Int. J. Polym. Sci. 2021, 2021, 6626712. [Google Scholar] [CrossRef]
- Moheet, I.A.; Luddin, N.; Ab Rahman, I.; Masudi, S.M.; Kannan, T.P.; Nik Abd Ghani, N.R. Analysis of Ionic-Exchange of Selected Elements between Novel Nano-Hydroxyapatite-Silica Added Glass Ionomer Cement and Natural Teeth. Polymers 2021, 13, 3504. [Google Scholar] [CrossRef]
- Moheet, I.A.; Luddin, N.; Ab Rahman, I.; Masudi, S.M.; Kannan, T.P.; Abd Ghani, N.R.N. Novel nano-hydroxyapatite-silica–added glass ionomer cement for dental application: Evaluation of surface roughness and sol-sorption. Polym. Polym. Compos. 2020, 28, 299–308. [Google Scholar] [CrossRef]
- Chen, J.; Zhao, Q.; Peng, J.; Yang, X.; Yu, D.; Zhao, W. Antibacterial and mechanical properties of reduced graphene-silver nanoparticle nanocomposite modified glass ionomer cements. J. Dent. 2020, 96, 103332. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.; Xu, Y.; Zhu, B.; Gao, G.; Ren, J.; Wang, H.; Lin, Y.; Cao, B. Synergistic effects of titanium dioxide and cellulose on the properties of glassionomer cement. Dent. Mater. J. 2019, 38, 41–51. [Google Scholar] [CrossRef] [PubMed]
- Sajjad, A.; Bakar, W.Z.W.; Mohamad, D.; Kannan, T.P. Characterization and enhancement of physico-mechanical properties of glass ionomer cement by incorporating a novel nano zirconia silica hydroxyapatite composite synthesized via sol-gel. AIMS Mat. Sci. 2019, 6, 730–747. [Google Scholar] [CrossRef]
- Hussin, H.M.; Bakar, W.Z.; Ghazali, N.A.; Sajjad, A. Microleakage assessment of a new modified glass ionomer cement-nanozirconia-silica-hydroxyapatite restorative material. J. Int. Oral. Health 2018, 10, 138–142. [Google Scholar] [CrossRef]
- Moheet, I.A.; Luddin, N.; Ab Rahman, I.; Masudi, S.M.; Kannan, T.P.; Abd Ghani, N.R.N. Evaluation of mechanical properties and bond strength of nano-hydroxyapatite-silica added glass ionomer cement. Ceramics Int. 2018, 44, 9899–9906. [Google Scholar] [CrossRef]
- Noorani, T.Y.; Luddin, N.; Ab Rahman, I.; Masudi, S.M. In Vitro Cytotoxicity Evaluation of Novel Nano-Hydroxyapatite-Silica Incorporated Glass Ionomer Cement. J. Clin. Diagn. Res. 2017, 11, ZC105–ZC109. [Google Scholar] [CrossRef]
- AbRahman, I.; Ghazali, N.A.M.; Bakar, W.Z.W.; Masudi, S.M. Modification of glass ionomer cement by incorporating nanozirconia-hydroxyapatite-silica nano-powder composite by the one-pot technique for hardness and aesthetics improvement. Ceram. Int. 2017, 43, 13247–13253. [Google Scholar] [CrossRef]
- Fareed, M.A.; Stamboulis, A. Nanoclay-Reinforced Glass-Ionomer Cements: In Vitro Wear Evaluation and Comparison by Two Wear-Test Methods. Dent. J. 2017, 5, 28. [Google Scholar] [CrossRef]
- Sodagar, A.; Akhavan, A.; Hashemi, E.; Arab, S.; Pourhajibagher, M.; Sodagar, K.; Kharrazifard, M.J.; Bahador, A. Evaluation of the antibacterial activity of a conventional orthodontic composite containing silver/hydroxyapatite nanoparticles. Prog. Orthod. 2016, 17, 40. [Google Scholar] [CrossRef]
- Rahman, I.A.; Masudi, S.M.; Luddin, N.; Shiekh, R.A. One-pot synthesis of hydroxyapatite–silica nanopowder composite for hardness enhancement of glass ionomer cement (GIC). Bull. Mater. Sci. 2014, 37, 213–219. [Google Scholar] [CrossRef]
- Fareed, M.A.; Stamboulis, A. Effect of Nanoclay Dispersion on the Properties of a Commercial Glass Ionomer Cement. Int. J. Biomat. 2014, 2014, 685389. [Google Scholar] [CrossRef] [PubMed]
- Fareed, M.A.; Stamboulis, A. Nanoclay addition to a conventional glass ionomer cements: Influence on physical properties. Eur. J. Dent. 2014, 8, 456–463. [Google Scholar] [CrossRef] [PubMed]
- Sayyedan, F.S.; Fathi, M.H.; Edris, H.; Doostmohammadi, A.; Mortazavi, V.; Hanifi, A. Effect of forsterite nanoparticles on mechanical properties of glass ionomer cements. Ceram. Int. 2014, 40, 10743–10748. [Google Scholar] [CrossRef]
- Anusha Thampi, V.V.; Prabhu, M.; Kavitha, K.; Manivasakan, P.; Prabu, P.; Rajendran, V.; Shankar, S.; Kulandaivelu, P. Hydroxyapatite, alumina/zirconia, and nanobioactive glass cement for tooth-restoring applications. Ceram. Int. 2014, 40, 14355–14365. [Google Scholar] [CrossRef]
- Shiekh, R.A.; Ab Rahman, I.; Masudi, S.M.; Luddin, N. Modification of glass ionomer cement by incorporating hydroxyapatite-silica nano-powder composite: Sol–gel synthesis and characterization. Ceram. Int. 2014, 40, 3165–3170. [Google Scholar] [CrossRef]
- Fareed, M.A.; Stamboulis, A. Nanoclays reinforced glass ionomer cements: Dispersion and interaction of polymer grade (PG) montmorillonite with poly(acrylic acid). J. Mater. Sci. Mater. Med. 2014, 25, 91–99. [Google Scholar] [CrossRef]
- Cheetham, J.J. The Future of Glass-Ionomers. In Glass-Ionomers in Dentistry; Sidhu, S., Ed.; Springer: Cham, Switzerland, 2016; pp. 125–148. [Google Scholar] [CrossRef]
- Kumar, A. Clinical Performance of Reinforced Glass Ionomer Materials in Class-II Restorations—A 12 Month Randomized Controlled Clinical Trial. 2022. Available online: http://www.ctri.nic.in/Clinicaltrials/pmaindet2.php?trialid=66470 (accessed on 18 August 2022).
- Swarup, S.J.; Rao, A.; Boaz, K.; Srikant, N.; Shenoy, R. Pulpal response to nano hydroxyapatite, mineral trioxide aggregate and calcium hydroxide when used as a direct pulp capping agent: An in vivo study. J. Clin. Pediatr. Dent. 2014, 38, 201–206. [Google Scholar] [CrossRef]
- Zaki, Z. Effect of Nano-hydroxyapatite Incorporation into Conventional and Resin Modified Glass Ionomer Cements on Shear Bond Strength to Sound and Caries-Affected Dentin (An In-Vitro/In-Vivo Study). 2022. Available online: https://pactr.samrc.ac.za/TrialDisplay.aspx?TrialID=8259 (accessed on 18 August 2022).
- Mahmoud, R.N. Clinical Evaluation of Nano Hydroxyapatite Reinforced Glass Ionomer in Treatment of Root Caries in Geriatric Patients. 2021. Available online: https://clinicaltrials.gov/ct2/show/record/NCT04701320?term=glass+ionomer+cement+nano&draw=2&rank=1 (accessed on 18 August 2022).
| P (Problem) | The need for improving the properties of GICs |
| I (Intervention) | Incorporation of inorganic nanomaterials in GIC |
| C (Comparison) | Unmodified GIC; GICs modified with other types of materials |
| O (Outcome) | Improvement of mechanical properties and antimicrobial activity of GICs |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fierascu, R.C. Incorporation of Nanomaterials in Glass Ionomer Cements—Recent Developments and Future Perspectives: A Narrative Review. Nanomaterials 2022, 12, 3827. https://doi.org/10.3390/nano12213827
Fierascu RC. Incorporation of Nanomaterials in Glass Ionomer Cements—Recent Developments and Future Perspectives: A Narrative Review. Nanomaterials. 2022; 12(21):3827. https://doi.org/10.3390/nano12213827
Chicago/Turabian StyleFierascu, Radu Claudiu. 2022. "Incorporation of Nanomaterials in Glass Ionomer Cements—Recent Developments and Future Perspectives: A Narrative Review" Nanomaterials 12, no. 21: 3827. https://doi.org/10.3390/nano12213827
APA StyleFierascu, R. C. (2022). Incorporation of Nanomaterials in Glass Ionomer Cements—Recent Developments and Future Perspectives: A Narrative Review. Nanomaterials, 12(21), 3827. https://doi.org/10.3390/nano12213827








