Understanding Telehealth Adoption among the Elderly: An Empirical Investigation
Abstract
1. Introduction
2. Theoretical Underpinnings
2.1. Behavioral Reasoning Theory (BRT)
2.2. Reason for and against Adoption
3. Hypotheses Development
3.1. Value (Openness to Change)
3.2. Attitude and Adoption Behavior
3.3. Reasons against the Adoption of Telehealth Adoption among the Elderly
3.4. Reasons for the Adoption of Telehealth Adoption among the Elderly
4. Method
4.1. Instrument
4.2. Data Collection and Sample
4.3. Initial Data Quality Checks
5. Results and Findings
5.1. Measurement Model
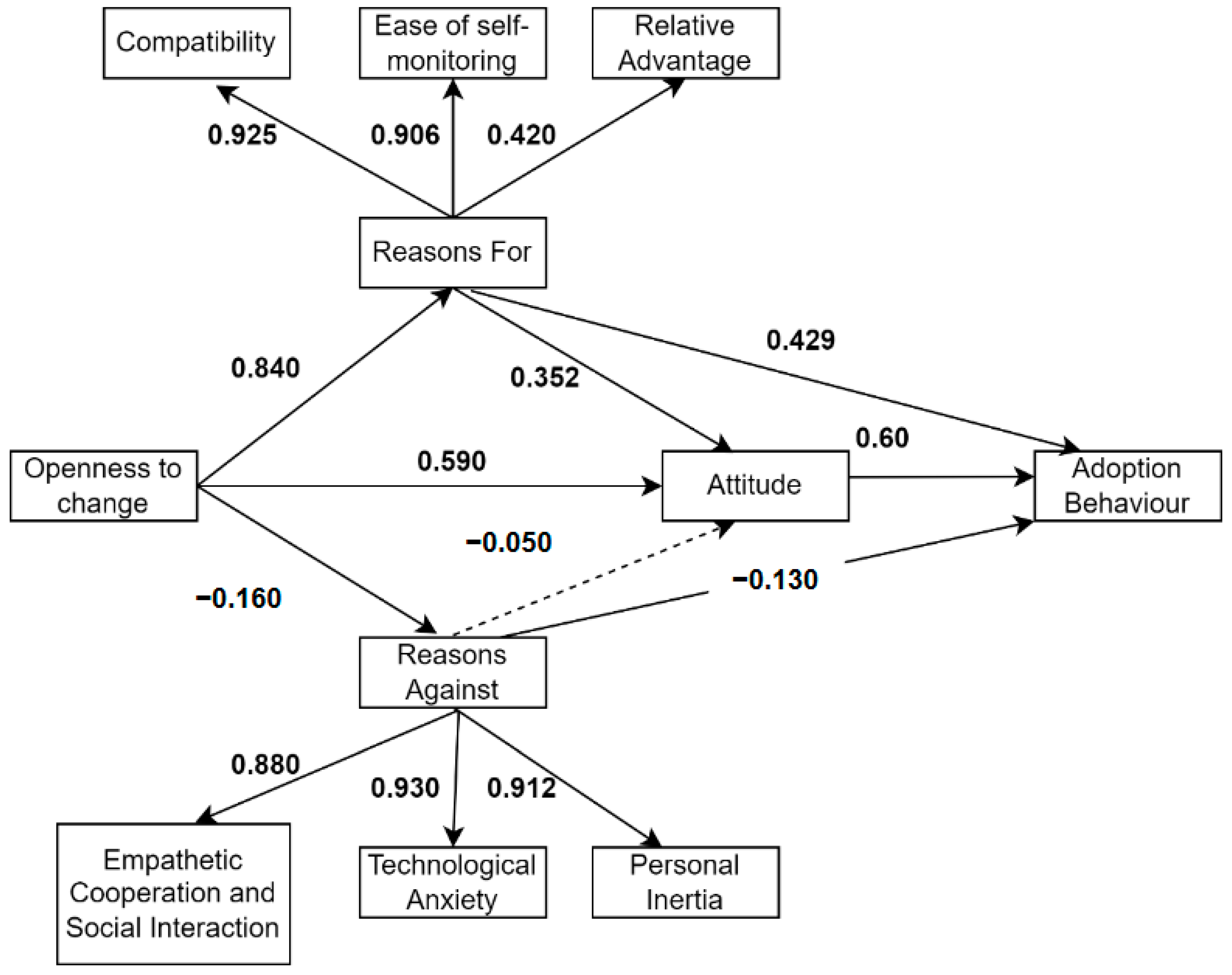
5.2. Structural Model
6. Conclusions
7. Implications of This Study
8. Limitations and Future Scope
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Scale Items and Their Source | |
|---|---|
| Main Construct | Indicator/Item |
| Relative Advantage | Compared to personal visits to the doctor, telehealth can save money. |
| Compared with offline health services, getting teleconsultation on time is more convenient for me. | |
| Compared with offline health services, I think telehealth services (such as appointments, medical treatment, and taking medicine) are more efficient. | |
| Compatibility | The service provided by telehealth can satisfy my demands regarding health management. |
| [1] | Services provided by telehealth connect with my daily life. |
| Applying telehealth services does not create any conflicts with my living habits. | |
| Ease of Self-monitoring | The instructions provided for self-monitoring through telehealth are clear. |
| [54,55] | I can easily access support if I encounter difficulties with self-monitoring using telehealth. |
| The instructions provided for self-monitoring through telehealth are easy to understand. | |
| Value of openness to change | I always look for new things in telehealth to do. |
| [18] | I look for adventure while using telehealth. |
| I am open to new experiences. | |
| Personal Inertia | I will continue to apply traditional physical measurement tools because they are part of my life. |
| [1,12] | Even though traditional physical measurement tools are not effective, I will continue to apply them. |
| I am already used to these traditional physical measurement tools. | |
| Technological Anxiety | I feel afraid to use telehealth. |
| [1] | I feel nervous about using telehealth. |
| I feel uncomfortable using telehealth. | |
| Empathetic Cooperation and Social Interaction | Using telehealth weakens my emotional bonds with healthcare providers. |
| [12,35] | Telehealth decreases my scope to interact socially. |
| I feel social detachment while using telehealth. | |
| Attitude | I feel comfortable using telehealth. |
| [1] | Using telehealth provides lots of benefits over the conventional healthcare system. |
| Using telehealth in the near future adds a lot of value. | |
| Adoption Intention | I will use telehealth in the near future. |
| [1] | I will try to replace my current physical mode of health checkup with telehealth. |
| I plan to use telehealth. | |
References
- Tsai, J.M.; Cheng, M.J.; Tsai, H.H.; Hung, S.W.; Chen, Y.L. Acceptance and resistance of telehealth: The perspective of dual-factor concepts in technology adoption. Int. J. Inf. Manag. 2019, 49, 34–44. [Google Scholar] [CrossRef]
- Nagaraja, V.H.; Dastidar, B.G.; Suri, S.; Jani, A.R. Perspectives and use of telemedicine by doctors in India: A cross-sectional study. Health Policy Technol. 2024, 13, 100845. [Google Scholar] [CrossRef]
- Sajid, M.; Zakkariya, K.A.; Peethambaran, M. Predicting virtual care continuance intention in the post-Covid world: Empirical evidence from an emerging economy. Int. J. Healthc. Manag. 2023, 16, 327–335. [Google Scholar] [CrossRef]
- Haimi, M.; Goren, U.; Grossman, Z. Barriers and challenges to telemedicine usage among the elderly population in Israel in light of the COVID-19 era: A qualitative study. Digit. Health 2024, 10, 20552076241240235. [Google Scholar] [CrossRef] [PubMed]
- Turcotte, S.; Bouchard, C.; Rousseau, J.; DeBroux Leduc, R.; Bier, N.; Kairy, D.; Dang-Vu, T.T.; Sarimanukoglu, K.; Dubé, F.; Bourgeois Racine, C.; et al. Factors influencing older adults’ participation in telehealth interventions for primary prevention and health promotion: A rapid review. Australas. J. Ageing 2024, 43, 11–30. [Google Scholar] [CrossRef]
- Rana, S.; Tandon, U.; Kumar, H. Understanding medical service quality, system quality and information quality of Tele-Health for sustainable development in the Indian context. Kybernetes 2023. ahead of print. [Google Scholar] [CrossRef]
- Ferguson, J.M.; Jacobs, J.; Yefimova, M.; Greene, L.; Heyworth, L.; Zulman, D.M. Virtual care expansion in the Veterans health administration during the COVID-19 pandemic: Clinical services and patient characteristics associated with utilization. J. Am. Med. Inform. Assoc. 2021, 28, 453–462. [Google Scholar] [CrossRef]
- WHO Global Observatory for eHealth. Telemedicine: Opportunities and Developments in Member States: Report on the Second Global Survey on eHealth; World Health Organization: Geneva, Switzerland, 2010; Available online: https://apps.who.int/iris/handle/10665/44497 (accessed on 20 April 2020).
- Sajid, M.; Zakkariya, K.A.; Surira, M.D.; Thomas, L. Why are Indian Digital Natives Resisting Telemedicine Innovation Resistance Theory Perspective. Int. J. Bus. Inf. Syst. 2023, 1. [Google Scholar] [CrossRef]
- Joshi, A.; Generalla, J.; Thompson, B.; Haidet, P. Facilitating the feedback process on a clinical clerkship using a smartphone application. Acad. Psychiatry 2017, 41, 651–655. [Google Scholar] [CrossRef]
- Yadav, R.; Giri, A.; Chatterjee, S. Understanding the users’ motivation and barriers in adopting healthcare apps: A mixed-method approach using behavioral reasoning theory. Technol. Forecast. Soc. Chang. 2022, 183, 121932. [Google Scholar] [CrossRef]
- Tandon, U.; Ertz, M.; Shashi. Continued Intention of mHealth Care Applications among the Elderly: An Enabler and Inhibitor Perspective. Int. J. Hum. Comput. Interact. 2023, 1–16. [Google Scholar] [CrossRef]
- Talukder, M.S.; Laato, S.; Islam, A.N.; Bao, Y. Continued use intention of wearable health technologies among the elderly: An enablers and inhibitors perspective. Internet Res. 2021, 31, 1611–1640. [Google Scholar] [CrossRef]
- Choi, N.G.; DiNitto, D.M.; Marti, C.N.; Choi, B.Y. Telehealth use among older adults during COVID-19: Associations with sociodemographic and health characteristics, technology device ownership, and technology learning. J. Appl. Gerontol. 2022, 41, 600–609. [Google Scholar] [CrossRef] [PubMed]
- Westaby, J.D. Behavioral reasoning theory: Identifying new linkages underlying intentions and behavior. Organ. Behav. Hum. Decis. Process. 2005, 98, 97–120. [Google Scholar] [CrossRef]
- Virmani, N.; Sharma, S.; Kumar, A.; Luthra, S. Adoption of industry 4.0 evidence in emerging economy: Behavioral reasoning theory perspective. Technol. Forecast. Soc. Chang. 2023, 188, 122317. [Google Scholar] [CrossRef]
- Lalicic, L.; Weismayer, C. Consumers’ reasons and perceived value co-creation of using artificial intelligence-enabled travel service agents. J. Bus. Res. 2021, 129, 891–901. [Google Scholar] [CrossRef]
- Claudy, M.C.; Garcia, R.; O’Driscoll, A. Consumer resistance to innovation—A behavioral reasoning perspective. J. Acad. Mark. Sci. 2015, 43, 528–544. [Google Scholar] [CrossRef]
- Dhir, A.; Koshta, N.; Goyal, R.K.; Sakashita, M.; Almotairi, M. Behavioral reasoning theory (BRT) perspectives on E-waste recycling and management. J. Clean. Prod. 2021, 280, 124269. [Google Scholar] [CrossRef]
- Westaby, J.D.; Probst, T.M.; Lee, B.C. Leadership decision-making: A behavioral reasoning theory analysis. Leadersh. Q. 2010, 21, 481–495. [Google Scholar] [CrossRef]
- Banbury, A.; Smith, A.C.; Mehrotra, A.; Page, M.; Caffery, L.J. A comparison study between metropolitan and rural hospital-based telehealth activity to inform adoption and expansion. J. Telemed. Telecare 2023, 29, 540–551. [Google Scholar] [CrossRef]
- Zhou, M.; Li, X.; Burtch, G. Healthcare across boundaries: Urban-rural differences in the consequences of telehealth adoption. Inf. Syst. Res. 2023. [Google Scholar] [CrossRef]
- Yuen, K.F.; Chua, J.Y.; Li, X.; Wang, X. The determinants of users’ intention to adopt telehealth: Health belief, perceived value and self-determination perspectives. J. Retail. Consum. Serv. 2023, 73, 103346. [Google Scholar] [CrossRef]
- Alarabyat, I.A.; Al-Nsair, N.; Alrimawi, I.; Al-Yateem, N.; Shudifat, R.M.; Saifan, A.R. Perceived barriers to effective use of telehealth in managing the care of patients with cardiovascular diseases: A qualitative study exploring healthcare professionals’ views in Jordan. BMC Health Serv. Res. 2023, 23, 452. [Google Scholar] [CrossRef] [PubMed]
- Bakshi, S.; Tandon, U. Understanding barriers of telemedicine adoption: A study in North India. Syst. Res. Behav. Sci. 2022, 39, 128–142. [Google Scholar] [CrossRef]
- Lee, J.C.; Chen, L.; Zhang, H. Exploring the adoption decisions of mobile health service users: A behavioral reasoning theory perspective. Ind. Manag. Data Syst. 2023, 123, 2241–2266. [Google Scholar] [CrossRef]
- Schwartz, S.H. Universals in the Content and Structure of Values: Theoretical Advances and Empirical Tests in 20 Countries. Advances in Experimental Social Psychology; Academic Press: Cambridge, MA, USA, 1992. [Google Scholar]
- Sivathanu, B. Adoption of Internet of things (IOT) based wearables for healthcare of older adults–a behavioural reasoning theory (BRT) approach. J. Enabling Technol. 2018, 12, 169–185. [Google Scholar] [CrossRef]
- Kruse, P.; Wach, D.; Costa, S.; Moriano, J.A. Values matter, Don’t They?–combining theory of planned behavior and personal values as predictors of social entrepreneurial intention. J. Soc. Entrep. 2019, 10, 55–83. [Google Scholar] [CrossRef]
- Steg, L.; Perlaviciute, G.; Van der Werff, E.; Lurvink, J. The significance of hedonic values for environmentally relevant attitudes, preferences, and actions. Environ. Behav. 2014, 46, 163–192. [Google Scholar] [CrossRef]
- Gupta, P.; Gupta, A.; Dixit, S.; Kumar, H. Knowledge, attitude, and practices regarding COVID-19: A cross-sectional study among rural population in a northern Indian District. J. Fam. Med. Prim. Care 2020, 9, 4769–4773. [Google Scholar]
- Liu, Y.; Liang, Z.; Li, C.; Guo, J.; Zhao, G. An investigation into the adoption behavior of mhealth users: From the perspective of the push-pull-mooring framework. Sustainability 2022, 14, 14372. [Google Scholar] [CrossRef]
- Huang, Y.; Qian, L. Understanding the potential adoption of autonomous vehicles in China: The perspective of behavioral reasoning theory. Psychol. Mark. 2021, 38, 669–690. [Google Scholar] [CrossRef]
- Yang, J.; Liu, Z.; Cheng, X.; Ye, G. Understanding the keyword adoption behavior patterns of researchers from a functional structure perspective. Scientometrics 2024, 129, 3359–3384. [Google Scholar] [CrossRef]
- Shareef, M.A.; Kumar, V.; Dwivedi, Y.K.; Kumar, U.; Akram, M.S.; Raman, R. A new health care system enabled by machine intelligence: Elderly people’s trust or losing self control. Technol. Forecast. Soc. Chang. 2021, 162, 120334. [Google Scholar] [CrossRef]
- Dwivedi, A.D.; Malina, L.; Dzurenda, P.; Srivastava, G. Optimized blockchain model for Internet of things based healthcare applications. In Proceedings of the 2019 42nd International Conference on Telecommunications and Signal Processing (TSP), Budapest, Hungary, 1–3 July 2019; pp. 135–139. [Google Scholar]
- Bell, R.K.; Badger, K.; Barton, K.L.; Kohut, M.; Clark, M. The implementation of telemedicine in the COVID-19 Era. J. Maine Med. Cent. 2021, 3, 6. [Google Scholar] [CrossRef]
- Korber, S.; McNaughton, R.B. Resilience and entrepreneurship: A systematic literature review. Int. J. Entrep. Behav. Res. 2018, 24, 1129–1154. [Google Scholar] [CrossRef]
- Kamal, S.A.; Shafiq, M.; Kakria, P. Investigating acceptance of telemedicine services through an extended technology acceptance model (TAM). Technol. Soc. 2020, 60, 101212. [Google Scholar] [CrossRef]
- Werner, P. Willingness to use telemedicine for psychiatric care. Telemed. J. e-Health 2004, 10, 286–293. [Google Scholar] [CrossRef]
- Ahmad, S.Z.; Khalid, K. The adoption of M-government services from the user’s perspectives: Empirical evidence from the United Arab Emirates. Int. J. Inf. Manag. 2017, 37, 367–379. [Google Scholar] [CrossRef]
- Lucia-Palacios, L.; Pérez-López, R.; Polo-Redondo, Y. Enemies of cloud services usage: Inertia and switching costs. Serv. Bus. 2016, 10, 447–467. [Google Scholar] [CrossRef]
- Samuelson, W.; Zeckhauser, R. Status quo bias in decision making. J. Risk Uncertain. 1988, 1, 7–59. [Google Scholar] [CrossRef]
- Polites, G.L.; Karahanna, E. Shackled to the status quo: The inhibiting effects of incumbent system habit, switching costs, and inertia on new system acceptance. MIS Q. 2012, 36, 21–42. [Google Scholar] [CrossRef]
- Prakash, A.V.; Das, S. Medical practitioner’s adoption of intelligent clinical diagnostic decision support systems: A mixed-methods study. Inf. Manag. 2021, 58, 103524. [Google Scholar] [CrossRef]
- Rahman, R.; Bandyopadhyay, S. An observable effect of spin inertia in slow magneto-dynamics: Increase of the switching error rates in nanoscale ferromagnets. J. Phys. Condens. Matter 2021, 33, 355801. [Google Scholar] [CrossRef]
- Cohen-Mansfield, J.; Muff, A.; Meschiany, G.; Lev-Ari, S. Adequacy of web-based activities as a substitute for in-person activities for older persons during the COVID-19 pandemic: Survey study. J. Med. Internet Res. 2021, 23, e25848. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Zhang, X. How environmental uncertainty moderates the effect of relative advantage and perceived credibility on the adoption of mobile health services by Chinese organizations in the big data era? Int. J. Telemed. Appl. 2016, 2016, 3618402. [Google Scholar] [CrossRef]
- Rogers, E.M. Lessons for guidelines from the diffusion of innovations. Jt. Comm. J. Qual. Improv. 1995, 21, 324–328. [Google Scholar] [CrossRef]
- Tung, F.C.; Chang, S.C.; Chou, C.M. An extension of trust and TAM model with IDT in the adoption of the electronic logistics information system in HIS in the medical industry. Int. J. Med. Inform. 2008, 77, 324–335. [Google Scholar] [CrossRef]
- Asua, J.; Orruño, E.; Reviriego, E.; Gagnon, M.P. Healthcare professional acceptance of telemonitoring for chronic care patients in primary care. BMC Med. Inform. Decis. Mak. 2012, 12, 139. [Google Scholar] [CrossRef]
- Foster, M.V.; Sethares, K.A. Facilitators and barriers to the adoption of telehealth in older adults: An integrative review. CIN Comput. Inform. Nurs. 2014, 32, 523–533. [Google Scholar] [CrossRef]
- Cimperman, M.; Brenčič, M.M.; Trkman, P.; Stanonik, M.D.L. Older adults’ perceptions of home telehealth services. Telemed. e-Health 2013, 19, 786–790. [Google Scholar] [CrossRef]
- Kruse, C.; Fohn, J.; Wilson, N.; Patlan, E.N.; Zipp, S.; Mileski, M. Utilization barriers and medical outcomes commensurate with the use of telehealth among older adults: Systematic review. JMIR Med. Inform. 2020, 8, e20359. [Google Scholar] [CrossRef]
- Ma, J.; Xiao, L.; Blonstein, A.C. Measurement of self-monitoring web technology acceptance and use in an e-health weight-loss trial. Telemed. e-Health 2013, 19, 739–745. [Google Scholar] [CrossRef] [PubMed]
- Bentler, P.M.; Chou, C.-P. Practical Issues in Structural Modeling. Sociol. Methods Res. 1987, 16, 78–117. [Google Scholar] [CrossRef]
- Byrne, B.M. Structural Equation Modeling with Mplus: Basic Concepts, Applications, and Programming; Routledge: London, UK, 2013. [Google Scholar]
- Hair, J.F.; Ringle, C.M.; Sarstedt, M. PLS-SEM: Indeed a silver bullet. J. Mark. Theory Pract. 2011, 19, 139–152. [Google Scholar] [CrossRef]
- Hajiheydari, N.; Delgosha, M.S.; Olya, H. Scepticism and resistance to IoMT in healthcare: Application of behavioural reasoning theory with configurational perspective. Technol. Forecast. Soc. Chang. 2021, 169, 120807. [Google Scholar] [CrossRef]
- Ashfaq, M.; Yun, J.; Yu, S. My smart speaker is cool! Perceived coolness, perceived values, and users’ attitude toward smart speakers. Int. J. Hum. Comput. Interact. 2021, 37, 560–573. [Google Scholar] [CrossRef]
- Sreen, N.; Dhir, A.; Talwar, S.; Tan, T.M.; Alharbi, F. Behavioral reasoning perspectives to brand love toward natural products: Moderating role of environmental concern and household size. J. Retail. Consum. Serv. 2021, 61, 102549. [Google Scholar] [CrossRef]
- Chowdhury, A.; Hafeez-Baig, A.; Gururajan, R.; Chakraborty, S. Conceptual framework for telehealth adoption in Indian healthcare. In Proceedings of the 24th Annual Conference of the Asia Pacific Decision Sciences Institute: Full Papers, Asia-Pacific Decision Sciences Institute (APDSI), New Orleans, LA, USA, 23–25 November 2019. [Google Scholar]
- Chellaiyan, V.G.; Nirupama, A.Y.; Taneja, N. Telemedicine in India: Where do we stand? J. Fam. Med. Prim. Care 2019, 8, 1872–1876. [Google Scholar] [CrossRef]
- Dandachi, D.; Dang, B.N.; Lucari, B.; Teti, M.; Giordano, T.P. Exploring the attitude of patients with HIV about using telehealth for HIV care. AIDS Patient Care STDs 2020, 34, 166–172. [Google Scholar] [CrossRef]
- Bhatia, R. Telehealth and COVID-19: Using technology to accelerate the curve on access and quality healthcare for citizens in India. Technol. Soc. 2021, 64, 101465. [Google Scholar] [CrossRef]
- Arora, M.; Mittal, A. Employees’ change in perception when artificial intelligence integrates with human resource management: A mediating role of AI-tech trust. Benchmarking Int. J. 2024. ahead-of-print. [Google Scholar] [CrossRef]
- Duplaga, M. A cross-sectional study assessing determinants of the attitude to the introduction of eHealth services among patients suffering from chronic conditions. BMC Med. Inform. Decis. Mak. 2015, 15, 33. [Google Scholar] [CrossRef]
- Manohar, S.; Mittal, A.; Marwah, S. Service innovation, corporate reputation and word-of-mouth in the banking sector: A test on multigroup-moderated mediation effect. Benchmarking Int. J. 2020, 27, 406–429. [Google Scholar] [CrossRef]
- Rasekaba, T.M.; Pereira, P.; Rani, G.V.; Johnson, R.; McKechnie, R.; Blackberry, I. Exploring telehealth readiness in a resource limited setting: Digital and health literacy among older people in Rural India (DAHLIA). Geriatrics 2022, 7, 28. [Google Scholar] [CrossRef] [PubMed]
- Kumar, B.S.; Shalini, S.P.; Rao, Y.M.; Hedberg, P.; Liljegren, P.D.; Edin-Liljegren, A. Challenges for Technology Adoption Towards Primary Geriatrics Services. DY Patil J. Health Sci. 2022, 10, 89–93. [Google Scholar] [CrossRef]
- Davis, F.D.; Bagozzi, R.; Warshaw, P. Technology acceptance model. J. Manag. Sci. 1989, 35, 982–1003. [Google Scholar]
- Audrain-Pontevia, A.F.; Menvielle, L.; Ertz, M. Effects of three antecedents of patient compliance for users of peer-to-peer online health communities: Cross-sectional study. J. Med. Internet Res. 2019, 21, e14006. [Google Scholar] [CrossRef]
- Menvielle, L.; Ertz, M.; François, J.; Audrain-Pontevia, A.F. User-Involved Design of Digital Health Products. In Revolutions in Product Design for Healthcare: Advances in Product Design and Design Methods for Healthcare; Springer: Singapore, 2022; pp. 1–19. [Google Scholar]
| Std. Estimate | Std. Error | Critical Ratio | Average Variance Extracted | Composite Reliability | Cronbach’s Alpha | ||
|---|---|---|---|---|---|---|---|
| Openness to change | OTC1 | 0.665 | 0.503 | 0.751 | 0.749 | ||
| OTC2 | 0.706 | 0.102 | 11.020 | ||||
| OTC3 | 0.753 | 0.11 | 11.636 | ||||
| Compatibility | COM1 | 0.814 | 0.563 | 0.794 | 0.791 | ||
| COM2 | 0.715 | 0.068 | 14.079 | ||||
| COM3 | 0.718 | 0.059 | 14.659 | ||||
| Ease of Self-monitoring | SLF1 | 0.716 | 0.556 | 0.789 | 0.764 | ||
| SLF2 | 0.72 | 0.077 | 12.776 | ||||
| SLF3 | 0.798 | 0.263 | 7.937 | ||||
| Relative Advantage | REA1 | 0.756 | 0.545 | 0.782 | 0.769 | ||
| REA2 | 0.708 | 0.084 | 12.07 | ||||
| REA3 | 0.749 | 0.06 | 13.49 | ||||
| Attitude | ADA1 | 0.769 | 0.580 | 0.846 | 0.831 | ||
| ADA2 | 0.784 | 0.062 | 15.233 | ||||
| ADA3 | 0.797 | 0.059 | 15.508 | ||||
| ADA4 | 0.691 | 0.074 | 12.018 | ||||
| Adoption Behavior | ABH1 | 0.743 | 0.634 | 0.874 | 0.858 | ||
| ABH2 | 0.814 | 0.064 | 15.331 | ||||
| ABH3 | 0.846 | 0.072 | 15.883 | ||||
| ABH4 | 0.779 | 0.072 | 14.671 | ||||
| Empathetic Cooperation and Social Interaction | ECS1 | 0.709 | 0.652 | 0.848 | 0.819 | ||
| ECS2 | 0.847 | 0.075 | 15.148 | ||||
| ECS3 | 0.858 | 0.073 | 15.298 | ||||
| Technological Anxiety | TRD1 | 0.899 | 0.675 | 0.861 | 0.842 | ||
| TRD2 | 0.845 | 0.044 | 21.596 | ||||
| TRD3 | 0.709 | 0.057 | 13.048 | ||||
| Personal Inertia | PEN1 | 0.866 | 0.729 | 0.890 | 0.856 | ||
| PEN2 | 0.878 | 0.042 | 22.497 | ||||
| PEN3 | 0.817 | 0.045 | 19.885 |
| Openness to Change | Compatibility | Ease of Self-Monitoring | Relative Advantage | Attitude | Adoption Behavior | Empathetic Cooperation and Social Interaction | Personal Inertia | Technological Anxiety | |
|---|---|---|---|---|---|---|---|---|---|
| Openness to Change | 0.709 | ||||||||
| Compatibility | 0.630 ** | 0.750 | |||||||
| Ease of self-monitoring | 0.580 ** | 0.701 ** | 0.745 | ||||||
| Relative Advantage | 0.292 ** | 0.289 ** | 0.235 ** | 0.738 | |||||
| Attitude | 0.456 ** | 0.466 ** | 0.381 ** | 0.642 ** | 0.761 | ||||
| Adoption Behavior | 0.466 ** | 0.519 ** | 0.400 ** | 0.304 ** | 0.482 ** | 0.796 | |||
| Empathetic Cooperation and Social Interaction | −0.048 | −0.082 | −0.120 * | 0.256 ** | −0.028 | −0.104 * | 0.807 | ||
| Personal Inertia | −0.095 | −0.130 * | −0.132 * | 0.299 ** | −0.002 | −0.062 | 0.703 ** | 0.853 | |
| Technological Anxiety | −0.060 | −0.100 | −0.067 | 0.336 ** | 0.052 | −0.102 * | 0.699 ** | 0.705 ** | 0.810 |
| Second-Order Estimated Path | Path Coefficients | Critical Ratio | p-Value (*** p < 0.001) | Result |
|---|---|---|---|---|
| Reasons for → Compatibility | 0.925 | 16.256 | *** | Supported |
| Reasons for → Relative Advantage | 0.420 | 6.106 | *** | Supported |
| Reasons for → Ease of Self-monitoring | 0.906 | 11.969 | *** | Supported |
| Reasons against → Lack of Empathetic cooperation and social interaction | 0.880 | 16.613 | *** | Supported |
| Reasons against → Personal Inertia | 0.912 | 13.289 | *** | Supported |
| Reasons against → Technological Anxiety | 0.930 | 11.141 | *** | Supported |
| Hypothesized path (First order model) | ||||
| Openness to change → Reasons for | 0.84 | 10.015 | *** | Supported |
| Openness to change → Reasons against | −0.16 | −4.659 | 0.04 | Supported |
| Openness to change → Attitude | 0.59 | 7.645 | *** | Supported |
| Reasons Against → Attitude | −0.05 | 0.911 | 0.362 | Not Supported |
| Reasons Against → Adoption Behavior | −0.13 | −2.567 | 0.029 | Supported |
| Reasons For → Attitude | 0.352 | 3.459 | 0.015 | Supported |
| Reasons For → Adoption Behavior | 0.429 | 4.931 | *** | Supported |
| Attitude → Adoption Behavior | 0.60 | 9.222 | *** | Supported |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tandon, U.; Ertz, M.; Sajid, M.; Kordi, M. Understanding Telehealth Adoption among the Elderly: An Empirical Investigation. Information 2024, 15, 552. https://doi.org/10.3390/info15090552
Tandon U, Ertz M, Sajid M, Kordi M. Understanding Telehealth Adoption among the Elderly: An Empirical Investigation. Information. 2024; 15(9):552. https://doi.org/10.3390/info15090552
Chicago/Turabian StyleTandon, Urvashi, Myriam Ertz, Muhammed Sajid, and Mehrdad Kordi. 2024. "Understanding Telehealth Adoption among the Elderly: An Empirical Investigation" Information 15, no. 9: 552. https://doi.org/10.3390/info15090552
APA StyleTandon, U., Ertz, M., Sajid, M., & Kordi, M. (2024). Understanding Telehealth Adoption among the Elderly: An Empirical Investigation. Information, 15(9), 552. https://doi.org/10.3390/info15090552






