Gender Differences in Health-Related Quality of Life in Patients with Systolic Heart Failure: Results of the VIDA Multicenter Study
Abstract
:1. Introduction
2. Methods
2.1. Study Design
2.2. Study Population and Inclusion-Exclusion Criteria
2.3. Assessment of Patient-Centred Health Outcomes in Quality of Life
2.4. Statistical Analysis
3. Results
4. Discussion
Limitations of the Study
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Comin-Colet, J.; Anguita, M.; Formiga, F.; Almenar, L.; Crespo-Leiro, M.G.; Manzano, L.; Muñiz, J.; Chaves, J.; De Frutos, T.; Enjuanes, C. Health-related Quality of Life of Patients With Chronic Systolic Heart Failure in Spain: Results of the VIDA-IC Study. Rev. Esp. Cardiol. (Engl. Ed.) 2016, 69, 256–271. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Comín-Colet, J.; Enjuanes, C.; Gonzalez, G.; Torrens, A.; Cladellas, M.; Meroño, O.; Ribas, N.; Ruiz, S.; Gómez, M.; Verdú, J.M.; et al. Iron deficiency is a key determinant of health-related quality of life in patients with chronic heart failure regardless of anaemia status. Eur. J. Hear. Fail. 2013, 15, 1164–1172. [Google Scholar] [CrossRef]
- Nieminen, M.S.; Dickstein, K.; Fonseca, C.; Serrano, J.M.; Parissis, J.; Fedele, F.; Wikström, G.; Agostoni, P.; Atar, S.; Baholli, L.; et al. The patient perspective: Quality of life in advanced heart failure with frequent hospitalisations. Int. J. Cardiol. 2015, 191, 256–264. [Google Scholar] [CrossRef]
- Volz, A.; Schmid, J.-P.; Zwahlen, M.; Kohls, S.; Saner, H.; Barth, J. Predictors of readmission and health related quality of life in patients with chronic heart failure: A comparison of different psychosocial aspects. J. Behav. Med. 2010, 34, 13–22. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chandra, A.; Vaduganathan, M.; Lewis, E.F.; Claggett, B.L.; Rizkala, A.R.; Wang, W.; Lefkowitz, M.P.; Shi, V.C.; Anand, I.S.; Ge, J.; et al. Health-Related Quality of Life in Heart Failure With Preserved Ejection Fraction: The PARAGON-HF Trial. JACC Hear. Fail. 2019, 7, 862–874. [Google Scholar] [CrossRef] [PubMed]
- Feldman, D.E.; Ducharme, A.; Giannetti, N.; Frenette, M.; Michel, C.; Grondin, F.; Sheppard, R.; Lauriers, J.D.; Behlouli, H.; Pilote, L. Severity at Entry to Specialized Heart Failure Clinics: Discrepancies Between Health-Related Quality of Life and Function in Men and Women. Can. J. Cardiol. 2011, 27, 382–387. [Google Scholar] [CrossRef] [PubMed]
- Lesman-Leegte, I.; Jaarsma, T.; Coyne, J.C.; Hillege, H.L.; Van Veldhuisen, D.J.; Sanderman, R. Quality of Life and Depressive Symptoms in the Elderly: A Comparison Between Patients With Heart Failure and Age- and Gender-Matched Community Controls. J. Card. Fail. 2009, 15, 17–23. [Google Scholar] [CrossRef] [Green Version]
- Dewan, P.; Rørth, R.; Jhund, P.S.; Shen, L.; Raparelli, V.; Petrie, M.C.; Abraham, W.T.; Desai, A.S.; Dickstein, K.; Køber, L.; et al. Differential Impact of Heart Failure With Reduced Ejection Fraction on Men and Women. J. Am. Coll. Cardiol. 2019, 73, 29–40. [Google Scholar] [CrossRef]
- Faxén, U.L.; Hage, C.; Donal, E.; Daubert, J.-C.; Linde, C.; Lund, L. Patient reported outcome in HFpEF: Sex-specific differences in quality of life and association with outcome. Int. J. Cardiol. 2018, 267, 128–132. [Google Scholar] [CrossRef]
- Heo, S.; Moser, D.K.; Widener, J. Gender Differences in the Effects of Physical and Emotional Symptoms on Health-Related Quality of Life in Patients with Heart Failure. Eur. J. Cardiovasc. Nurs. 2007, 6, 146–152. [Google Scholar] [CrossRef]
- Friedman, M.M. Gender differences in the health related quality of life of older adults with heart failure. Hear. Lung 2003, 32, 320–327. [Google Scholar] [CrossRef]
- Piepenburg, S.M.; Faller, H.; Störk, S.; Ertl, G.; Angermann, C.E. Symptom patterns and clinical outcomes in women versus men with systolic heart failure and depression. Clin. Res. Cardiol. 2018, 108, 244–253. [Google Scholar] [CrossRef]
- Riegel, B.; Mosra, D.K.; Carlson, B.; Deaton, C.; Armolla, R.; Sethares, K.; Shively, M.; Evangelista, L.; Albert, N. Gender differences in quality of life are minimal in patients with heart failure. J. Card. Fail. 2003, 9, 42–48. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Anguita, M.; Comin-Colet, J.; Formiga, F.; Almenar, L.; Crespo-Leiro, M.; Manzano, L. Tratamiento de la insuficiencia cardiaca con función sistólica deprimida: Situación actual en España. Resultados del estudio VIDA–IC. Rev. Esp. Cardiol. 2014, 67, 769–770. [Google Scholar] [CrossRef] [PubMed]
- Green, C.; Porter, C.B.; Bresnahan, D.R.; Spertus, J.A. Development and evaluation of the Kansas City Cardiomyopathy Questionnaire: A new health status measure for heart failure. J. Am. Coll. Cardiol. 2000, 35, 1245–1255. [Google Scholar] [CrossRef] [Green Version]
- Badia, X.; Roset, M.; Herdman, M.; Kind, P. A Comparison of United Kingdom and Spanish General Population Time Trade-off Values for EQ-5D Health States. Med Decis. Mak. 2001, 21, 7–16. [Google Scholar] [CrossRef] [PubMed]
- Comín-Colet, J.; Garín, O.; Lupón, J.; Manito, N.; Crespo-Leiro, M.G.; Gómez-Bueno, M.; Ferrer, M.; Artigas, R.; Zapata, A.; Elosua, R. Validación de la versión española del Kansas City Cardiomyopathy Questionnaire. Revista Española de Cardiología 2011, 64, 51–58. [Google Scholar] [CrossRef] [PubMed]
- Townsend, N.; Nichols, M.; Scarborough, P.; Rayner, M. Cardiovascular disease in Europe — epidemiological update 2015. Eur. Hear. J. 2015, 36, 2696–2705. [Google Scholar] [CrossRef] [Green Version]
- Bucholz, E.M.; Butala, N.M.; Rathore, S.S.; Dreyer, R.P.; Lansky, A.J.; Krumholz, H.M. Sex differences in long-term mortality after myocardial infarction: A systematic review. Circulation 2014, 130, 757–767. [Google Scholar] [CrossRef] [Green Version]
- Loehr, L.R.; Rosamond, W.D.; Chang, P.P.; Folsom, A.R.; Chambless, L.E. Heart Failure Incidence and Survival (from the Atherosclerosis Risk in Communities Study). Am. J. Cardiol. 2008, 101, 1016–1022. [Google Scholar] [CrossRef]
- Sillars, A.; Ho, F.K.; Pell, G.P.; Gill, J.M.R.; Sattar, N.; Gray, S.; Celis-Morales, C. Sex differences in the association of risk factors for heart failure incidence and mortality. Heart 2019. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lichtman, J.H.; Leifheit, E.C.; Safdar, B.; Bao, H.; Krumholz, H.M.; Lorenze, N.P.; Daneshvar, M.; Spertus, J.A.; D’Onofrio, G. Sex Differences in the Presentation and Perception of Symptoms Among Young Patients With Myocardial Infarction: Evidence from the VIRGO Study (Variation in Recovery: Role of Gender on Outcomes of Young AMI Patients). Circulation 2018, 137, 781–790. [Google Scholar] [CrossRef] [PubMed]
- Heras, M. Cardiopatía isquémica en la mujer: Presentación clínica, pruebas diagnósticas y tratamiento de los síndromes coronarios agudos. Rev. Esp. Cardiol. 2006, 59, 371–381. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leon, D.A. Trends in European life expectancy: A salutary view. Int. J. Epidemiol. 2011, 40, 271–277. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Masoudi, F.A.; Havranek, E.P.; Smith, G.; Fish, R.H.; Steiner, J.F.; Ordin, D.L.; Krumholz, H.M. Gender, age, and heart failure with preserved left ventricular systolic function. J. Am. Coll Cardiol 2003, 41, 217–223. [Google Scholar] [CrossRef]
- Bozkurt, B.; Khalaf, S. Heart Failure in Women. Methodist DeBakey Cardiovasc. J. 2017, 13, 216–223. [Google Scholar]
- Beale, A.L.; Meyer, P.; Marwick, T.H.; Lam, C.S.; Kaye, D.M. Sex Differences in Cardiovascular Pathophysiology. Circulation 2018, 138, 198–205. [Google Scholar] [CrossRef]
- Norris, C.M.; Spertus, J.A.; Jensen, L.; Johnson, J.A.; Hegadoren, K.; Ghali, W.A. Investigators Sex and Gender Discrepancies in Health-Related Quality of Life Outcomes Among Patients with Established Coronary Artery Disease. Circ. Cardiovasc. Qual. Outcomes 2008, 1, 123–130. [Google Scholar] [CrossRef] [Green Version]
- Walfridsson, U.; Hansen, P.S.; Charitakis, E.; Almroth, H.; Jönsson, A.; Karlsson, L.O.; Liuba, I.; Ayou, R.S.; Poci, D.; Holmqvist, F.; et al. Gender and age differences in symptoms and health-related quality of life in patients with atrial fibrillation referred for catheter ablation. Pacing Clin. Electrophysiol. 2019, 42, 1431–1439. [Google Scholar] [CrossRef]
- Strømnes, L.A.; Ree, H.; Gjesdal, K.; Ariansen, I. Sex Differences in Quality of Life in Patients with Atrial Fibrillation: A Systematic Review. J. Am. Hear. Assoc. 2019, 8, e010992. [Google Scholar] [CrossRef] [Green Version]
- McMurray, J.J.; Solomon, S.D.; Inzucchi, S.E.; Køber, L.; Kosiborod, M.N.; Martinez, F.A.; Ponikowski, P.; Sabatine, M.S.; Anand, I.S.; Bělohlávek, J.; et al. Dapagliflozin in Patients with Heart Failure and Reduced Ejection Fraction. N. Engl. J. Med. 2019, 381, 1995–2008. [Google Scholar] [CrossRef] [PubMed] [Green Version]

| n | Overall n = 1028 | Women n = 309 (30%) | Men n = 719 (70%) | p Value | |
|---|---|---|---|---|---|
| Age (years) | 1015 | 71 ± 11 | 73 ± 10 | 70 ± 11 | <0.0001 |
| BMI (kg/m2) | 997 | 27.7 ± 3,9 | 28.2 ± 4,4 | 27.5 ± 3.6 | 0.010 |
| Systolic Blood Pressure (mmHg) | 1022 | 127 ± 19 | 129 ± 20 | 126 ± 18 | 0.092 |
| Heart rate (bpm) | 1021 | 74 ± 16 | 76 ± 16 | 73 ± 15 | 0.017 |
| NYHA Functional class I-II vs. III-IV | 994 | 546 (54.9)/448 (45.1) | 158 (53.4)/138 (54.6) | 388(55.6)/310 (44.4) | 0.531 |
| Previous HF admission, | 1028 | 860 (83.7) | 262 (84.8) | 598 (83.2) | 0.581 |
| HF admission <6 months, | 1028 | 507 (49.3) | 148 (47.9) | 359 (49.9) | 0.586 |
| Time from diagnosis (years) | 936 | 2.7 (0.9–5.9) | 2.8 (0.9–6.3) | 2.7 (0.9–5.7) | 0.690 |
| LVEF (%) | 993 | 33.7 ± 6.8 | 34.4 ± 6.7 | 33.4 ± 6.8 | 0.027 |
| Ischemic etiology of HF | 1028 | 521 (50.7) | 100 (32.4) | 421 (58.6) | <0.0001 |
| Comorbidities | |||||
| Hypertension | 1028 | 815 (79.3) | 240 (77.7) | 575 (80.0) | 0.403 |
| Diabetes mellitus | 1028 | 450 (43.8) | 141 (45.6) | 309 (43.0) | 0.451 |
| Previous AMI | 1028 | 447 (43.5) | 91 (29.4) | 356 (49.5) | <0.0001 |
| Dislipidemia | 1028 | 704 (68.5) | 196 (63.4) | 508 (70.7) | 0.023 |
| Chronic kidney disease | 1028 | 242 (23.5) | 63 (20.4) | 179 (24.9) | 0.128 |
| Atrial Fibrillation | 1028 | 443 (45.5) | 150 (51.5) | 293 (43.0) | 0.017 |
| Anemia | 1028 | 194 (18.9) | 80 (25.9) | 114 (15.9) | 0.0003 |
| COPD | 1028 | 199 (19.4) | 28 (9.1) | 171 (23.8) | <0.0001 |
| TIA/Stroke | 1028 | 142 (13.8) | 47 (15.2) | 95 (13.2) | 0.430 |
| Anemia | 1028 | 204 (19.8) | 44 (14.2) | 160 (22.3) | 0.003 |
| Cancer | 1028 | 81 (7.9) | 30 (9.7) | 51 (7.1) | 0.165 |
| Chronic Hepatopathy | 1028 | 43 (4.2) | 7 (2.3) | 36 (5.0) | 0.060 |
| Obesity | 1028 | 239 (23.2) | 98 (31.7) | 141 (19.6) | <0.0001 |
| Low weight | 1028 | 13 (1.3) | 6 (1.9) | 7 (1.0) | 0.227 |
| Overweight | 1028 | 801 (77.9) | 239 (77.3) | 562 (78.2) | 0.806 |
| Sleep Apnea | 1028 | 94 (9.1) | 13 (4.2) | 81 (11.3) | 0.0002 |
| Comorbidities (n) | 1028 | 3.5 ± 1.9 | 3.2 ± 1.8 | 3.7 ± 1.9 | 0.0002 |
| Charlson index (points) | 527 | 4.4 ± 2.8 | 3.98 ± 2.4 | 4.6 ± 3.0 | 0.009 |
| Medications | |||||
| ACEIs or ARBs | 1028 | 922 (89.7) | 274 (88.7) | 648 (90.1) | 0.503 |
| Beta-blockers | 1028 | 787 (76.6) | 224 (72.5) | 563 (78.3) | 0.045 |
| MRAs | 1028 | 684 (66.5) | 202 (65.4) | 482 (67.0) | 0.614 |
| Ivabradine | 1028 | 91 (8.9) | 21 (6.8) | 70 (9.7) | 0.151 |
| Digoxin | 1028 | 221 (21.5) | 82 (26.5) | 139 (19.3) | 0.013 |
| Diuretics | 1028 | 917 (89.2) | 281 (90.9) | 636 (88.5) | 0.273 |
| Statins | 1028 | 779 (75.8) | 214 (69.3) | 565 (78.6) | 0.002 |
| Antiplatelets | 1028 | 618 (60.1) | 154 (49.8) | 464 (64.5) | <0.0001 |
| Anticoagulants | 1028 | 410 (39.9) | 143 (46.3) | 267 (37.1) | 0.007 |
| Laboratory parameters | |||||
| Hemoglobin (g/dL) | 971 | 12.9 ± 1.7 | 12.4 ± 1.4 | 13.1 ± 1.7 | <0.0001 |
| eGFR (mL/min/1.73 m2) | 573 | 60.0 (45.0–70.0) | 60.0 (45.0–70.5) | 60.0 (45.0–70.0) | 0.542 |
| Creatinine clearance <60 mL/min | 573 | 259 (45.2) | 85 (48.9) | 174 (43.6) | 0.274 |
| NT-proBNP (pg/mL) | 238 | 1345 (504–2390) | 1348 (422–2333) | 1333 (537–2411) | 0.600 |
| BNP (pg/mL) | 154 | 216 (124–430) | 211 (125–397) | 232 (124–453) | 0.258 |
| n | Overall n = 1028 | Women n = 309 | Men n = 719 | p Value | |
|---|---|---|---|---|---|
| KCCQ Subdomain Score | |||||
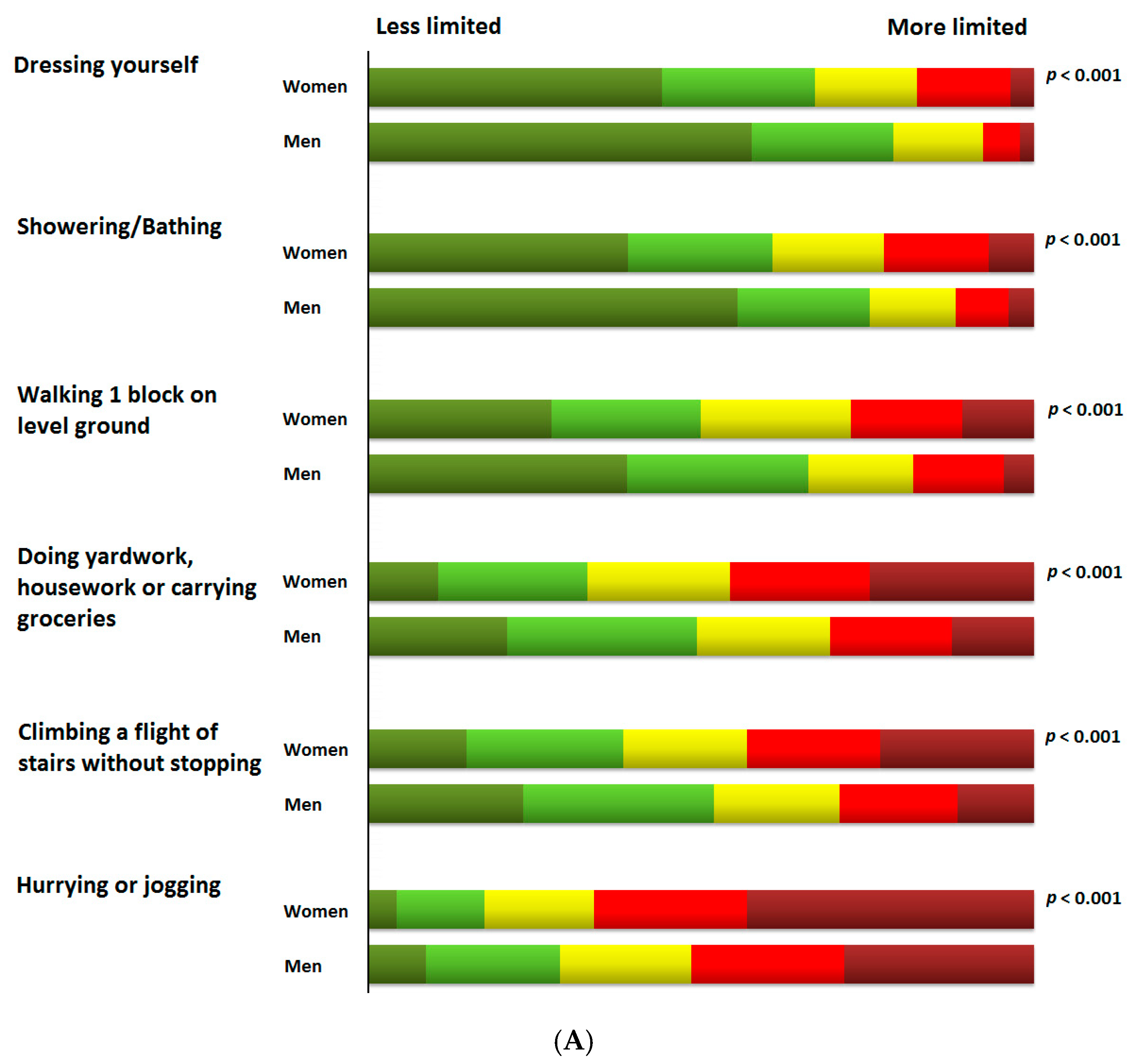
| Physical Limitation | 1023 | 61.1 ± 28.0 | 53.3 ± 29.1 | 64.5 ± 26.9 | <0.0001 |
| Symptom Stability | 1022 | 59.5 ± 23.2 | 59.2 ± 24.0 | 59.7 ± 22.9 | 0.761 |
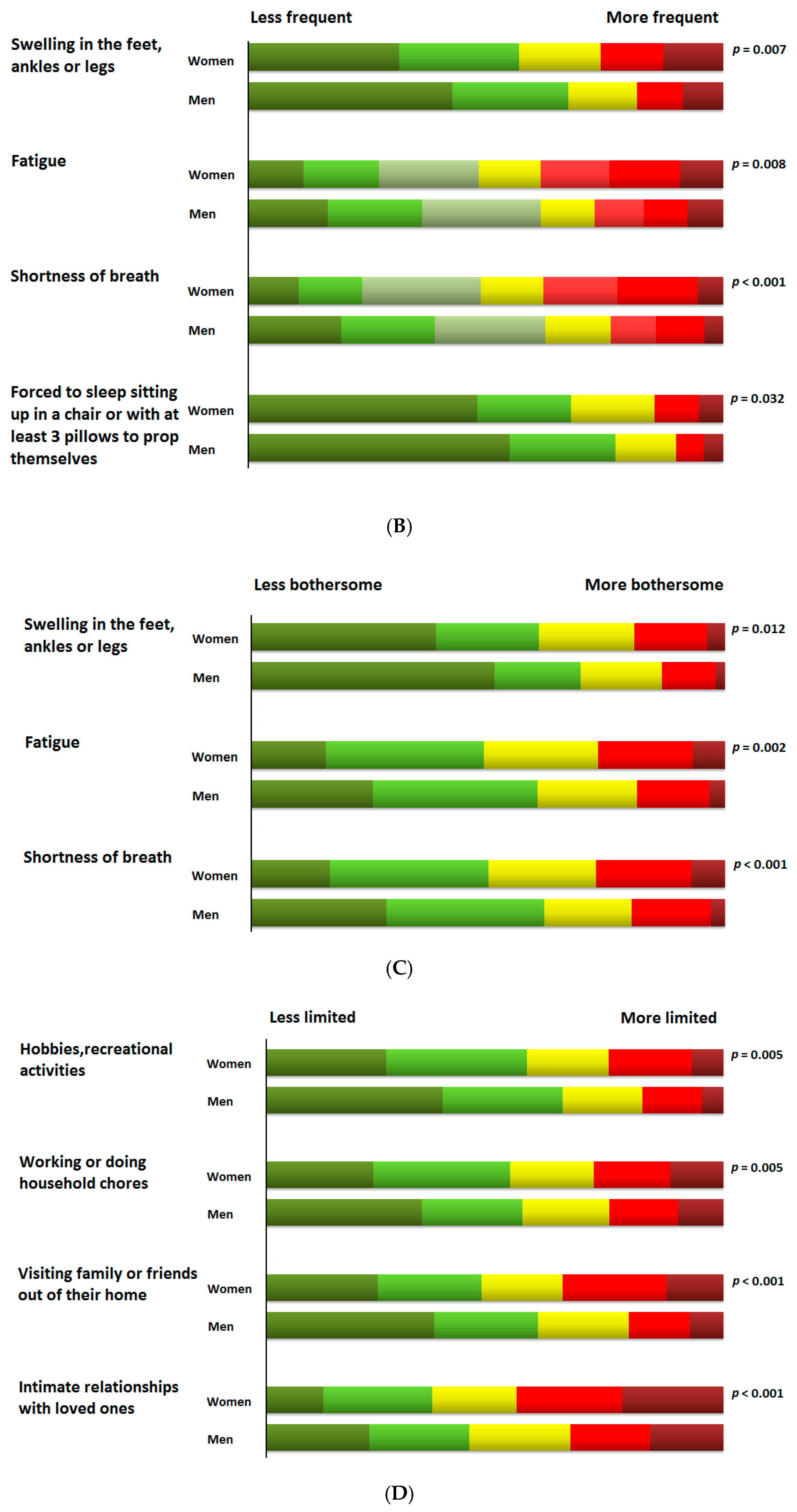
| Symptom Frequency | 1027 | 66.4 ± 26.0 | 60.8 ± 26.7 | 68.7 ± 25.4 | <0.0001 |
| Symptom Burden | 1027 | 67.2 ± 26.0 | 61.6 ± 26.5 | 69.6 ± 25.5 | <0.0001 |
| Self-Efficacy | 1026 | 69.1 ± 22.5 | 67.9 ± 22.8 | 69.6 ± 22.3 | 0.262 |
| Quality of Life | 1026 | 54.4 ± 24.1 | 50.8 ± 24.0 | 55.9 ± 24.0 | 0.002 |
| Social Limitation | 1018 | 61.6 ± 29.4 | 55.8 ± 29.5 | 64.1 ± 29.0 | <0.0001 |
| KCCQ, Summary Scores | |||||
| Overall Summary Score | 1014 | 60.9 ± 24.5 | 55.0 ± 24.6 | 63.4 ± 24.0 | <0.0001 |
| Clinical Summary Score | 1023 | 63.9 ± 25.1 | 57.3 ± 25.7 | 66.8 ± 24.4 | <0.0001 |
| Total Symptom Score | 1027 | 66.8 ± 25.4 | 61.2 ± 25.9 | 69.2 ± 25.5 | <0.0001 |
| EQ 5D, % patients reporting issues | |||||
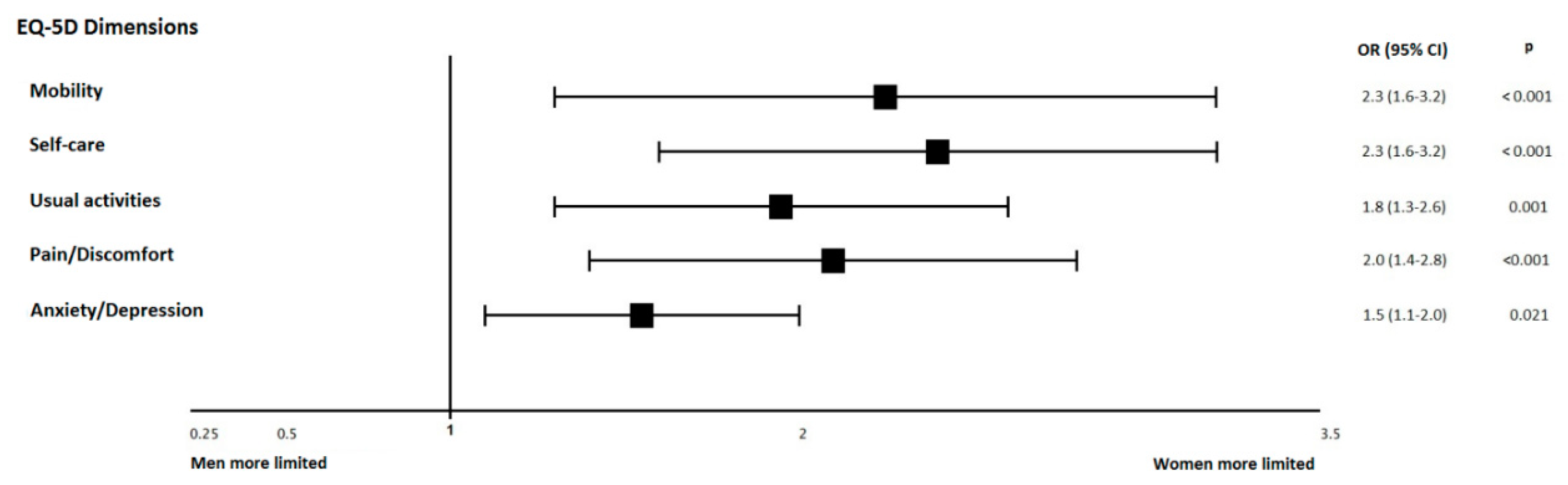
| Mobility | 1001 | 581 (58.0) | 212 (69.3) | 369 (53.1) | <0.0001 |
| Self-Care | 1001 | 581 (58.0) | 212 (69.3) | 369 (53.1) | <0.0001 |
| Usual Activities | 1000 | 615 (61.5) | 217 (70.9) | 398 (57.3) | <0.0001 |
| Pain/Discomfort | 999 | 506 (50.7) | 192 (62.7) | 314 (45.3) | <0.0001 |
| Anxiety/Depression | 999 | 490 (59.0) | 166 (54.2) | 324 (46.8) | 0.033 |
| EQ 5D Summary Scores | |||||
| EQ 5D Index | 993 | 0.65 ± 0.26 | 0.58 ± 0.26 | 0.67 ± 0.25 | <0.0001 |
| Visual analogue scale | 1013 | 60.8 ± 20.0 | 57.5 ± 20.8 | 62.2 ± 19.4 | 0.001 |
| Women | Men | p Value | |
|---|---|---|---|
| LVEF >30% | 56.0 ± 1.5 | 63.3 ± 1.0 | <0.001 |
| LVEF <30% | 52.8 ± 2.1 | 61.3 ± 1.4 | 0.003 |
| p value for interaction | 0.669 * | ||
| Age <75 years | 56.1 ± 1.8 | 64.2 ± 1.0 | <0.001 |
| Age >75 years | 53.0 ± 1.7 | 60.3 ± 1.3 | 0.001 |
| p value for interaction | 0.766 * | ||
| NYHA I-II | 66.2 ± 1.8 | 72.7 ± 1.1 | 0.003 |
| NYHA III-IV | 42.1 ± 1.8 | 51.2 ± 1.2 | <0.001 |
| p value for interaction | 0.364 * | ||
| Comorbidities number <5 | 54.9 ± 1.8 | 64.4 ± 1.3 | <0.001 |
| Comorbidities number >5 | 55.3 ± 2.0 | 61.0 ± 1.2 | 0.005 |
| p value for interaction | 0.193 * | ||
| Ischemic etiology: yes | 55.3 ± 1.5 | 62.9 ± 1.3 | <0.001 |
| Ischemic etiology: no | 54.5 ± 2.1 | 62.3 ± 1.0 | <0.001 |
| p value for interaction | 0.959 * | ||
| Recent admission: yes | 58.3 ± 1.8 | 66.2 ± 1.1 | <0.001 |
| Recent admission: no | 51.4 ± 1.7 | 59.0 ± 1.2 | <0.001 |
| p value for interaction | 0.902 * | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garay, A.; Tapia, J.; Anguita, M.; Formiga, F.; Almenar, L.; Crespo-Leiro, M.G.; Manzano, L.; Muñiz, J.; Chaves, J.; De Frutos, T.; et al. Gender Differences in Health-Related Quality of Life in Patients with Systolic Heart Failure: Results of the VIDA Multicenter Study. J. Clin. Med. 2020, 9, 2825. https://doi.org/10.3390/jcm9092825
Garay A, Tapia J, Anguita M, Formiga F, Almenar L, Crespo-Leiro MG, Manzano L, Muñiz J, Chaves J, De Frutos T, et al. Gender Differences in Health-Related Quality of Life in Patients with Systolic Heart Failure: Results of the VIDA Multicenter Study. Journal of Clinical Medicine. 2020; 9(9):2825. https://doi.org/10.3390/jcm9092825
Chicago/Turabian StyleGaray, Alberto, Javier Tapia, Manuel Anguita, Francesc Formiga, Luis Almenar, María G. Crespo-Leiro, Luis Manzano, Javier Muñiz, José Chaves, Trinidad De Frutos, and et al. 2020. "Gender Differences in Health-Related Quality of Life in Patients with Systolic Heart Failure: Results of the VIDA Multicenter Study" Journal of Clinical Medicine 9, no. 9: 2825. https://doi.org/10.3390/jcm9092825
APA StyleGaray, A., Tapia, J., Anguita, M., Formiga, F., Almenar, L., Crespo-Leiro, M. G., Manzano, L., Muñiz, J., Chaves, J., De Frutos, T., Moliner, P., Corbella, X., Enjuanes-Grau, C., Comín-Colet, J., & on Behalf of VIDA-IC Multicenter Study Investigators. (2020). Gender Differences in Health-Related Quality of Life in Patients with Systolic Heart Failure: Results of the VIDA Multicenter Study. Journal of Clinical Medicine, 9(9), 2825. https://doi.org/10.3390/jcm9092825






